Phototherapy Protocols. Contents
|
|
|
- Wesley Scott
- 9 years ago
- Views:
Transcription
1 Classification: Protocols Lead Author: Dr Tsui Ling Additional author(s): N/A Authors Division: Dermatology Unique ID: GSCDerm02(13) Issue number: 2 Expiry Date: February 2017 Contents Section Page Intro Who should read this document 3 Key practice points 3 Policy TREATMENT PROTOCOL No. 1: Narrowband UVB (TL-01) 4 Phototherapy 2 TREATMENT PROTOCOL No. 2: Systemic PUVA Phototherapy 7 3 TREATMENT PROTOCOL No. 3: Hand and foot PUVA soaks 11 4 TREATMENT PROTOCOL No. 4: Hand and foot oral PUVA 13 5 TREATMENT PROTOCOL No. 5: Bath PUVA Phototherapy 16 6 TREATMENT PROTOCOL No. 6: Missed treatments for UVB, 18 PUVA, hand and foot PUVA 7 TREATMENT PROTOCOL No. 7: Accidental overdose UV 19 protocol 8 TREATMENT PROTOCOL No. 8: Protocol for management of 20 minor adverse events 9 PROTOCOL NO. 9: MED tester protocol PROTOCOL NO. 10: Discharge protocol Appendix 23 Document control information (Published as separate document) Document Control 24 Policy Implementation Plan 25 Monitoring and Review 25 Endorsement 25 Equality analysis 26 Page 1 of 22
2 Who should read this document? Phototherapy Unit staff All Dermatology Staff All medical and nursing staff involved in the care of Phototherapy patients Key Practice Points Phototherapy protocols (UVB, PUVA, bath PUVA, hand and foot oral PUVA, hand and foot PUVA soaks), including incremental regimes, are shown. Protocol for management for missed treatments is listed. Protocol for management of accidental UV burns is listed. Protocol for management of minor adverse events is listed. Protocol for use of MED tester is listed. What is new in this version? PROTOCOL no. 9: Discharge protocol added. Page 2 of 22
3 Treatment Protocol TREATMENT PROTOCOL No. 1: Narrowband UVB (TL-01) Phototherapy 1. Initial irradiation dose: Determine MED (minimal erythema dose) with readings at 24 hours, +/- 3 hours (see Protocol no.9: Narrowband UVB MED testing), except for vitiligo patients or where the patient s skin condition or other circumstances makes testing impractical. 2. Initial irradiation dose: 70% of MED 3. NBUVB to be given three times weekly for most cases, with 2 days between treatments. 4. All patients to wear UV opaque goggles in the cabin. A face shield should also be worn unless significant lesions on face. Males must wear a sock for genital protection. 5. Incremental regime and action to be taken: see also TL01 UVB whole body cabins dose schedule Grade Definition Action E0 No erythema and no report 20% increment of erythema after last treatment E0+1 Patient reports erythema 20% increment but if previous E0+ after last treatment but now then hold dose or 10% increment resolved E1 (mild) Barely perceptible Repeat previous dose then consider E2 (moderate) E3 (severe) E4 (very severe) asymptomatic erythema Well-defined erythema, possibly causing slight manageable discomfort Well-defined symptomatic/painful erythema Painful erythema usually with blistering 10% increments Postpone one treatment if not completely settled; if settled, repeat previous dose and thereafter consider 10% increments No treatment and reviewed by Doctor when possible. When completely settled, 50% of previous dose and then 10% increments No treatment and review by Doctor Page 3 of 22
4 6. Usual course: treatments. Maximum number of treatments per course: 30. Maximum dose per treatment: 4.3 J/cm 2. Lifetime limit of 300 treatments. 7. If develop small areas of erythema: repeat previous dose and apply high factor sunscreen to affected area for one treatment. 8. If develop facial erythema or unacceptable facial pigmentation, a face shield or sunscreen should be used for each treatment. 9. If develop pruritus: encourage use of emollients and antihistamines. 10. If develop Polymorphic Light Eruption (PLE): treat with emollients and very potent topical steroids (eg. Dermovate) immediately after treatment. Postpone treatment if troublesome and reduce to 10 % increments. 11. Cancellation/ missed treatments: see missed treatment protocol. 12. Discharge: see discharge protocol. 13. Documentation: Copies of Treatment summary to be sent to responsible consultant and entered on EPR. 14. Eczema UVB Initiating dose: 0.20J/cm End of phototherapy course taper treatment, with 20% reduction in dose for each treatment: -use last dose at 2/week for 6 weeks, -followed by at 1/week for 6 weeks, -then discharge. 15. Vitiligo UVB Initiating dose dose: 0.20J/cm UVB increment: 10% Minimum 3 monthly treatment. If no response discontinue Follow up by doctor every 3 months Maximum 12 months treatment Clinical photographs at the start of treatment and every three months. 16. Polymorphic Light Eruption (or other photosensitivity disorder) UVB Initiating dose: 0.20J/cm UVB increment: 20% /week for 5 weeks, i.e. 15 treatments in total If develop PLE during treatment, Page 4 of 22
5 -If mild, continue with treatment in combination with emollients and topical steroids (eg. Dermovate ointment for body, Eumovate for face). -If severe, treat with emollients and topical steroids AND stop treatment until rash clears, then recommence at a lower dose. -Very severe flares may require oral prednisolone discuss with doctor /book into clinic Encourage patients to keep their sun tolerance topped-up by regular sun exposure throughout spring/summer. 17. Mycosis Fungoides UVB initiating dose and incremental doses: as with standard protocol UVB suitable for patch stage MF (systemic PUVA for plaque stage MF) Continue until skin clear no limit to number of treatments each course or lifetime If maintenance phototherapy is required once skin is clear, consider 1/week or less. Review every 20 maintenance treatments. Page 5 of 22
6 TREATMENT PROTOCOL No. 2: Systemic PUVA Phototherapy 1. Initial irradiation dose: Skin phototype Start dose J/cm 2 I (Always burn, never tan) 0.5 II (Usually burn, sometimes tan) 1.0 III (Usually tan, sometimes burn) 1.4 IV (Never burn, always tan) 2.0 V (Brown skin) 2.0 VI (Black skin) PUVA to be given twice weekly for most cases, with 3 days between treatments Methoxypsoralen (8-MOP) tablets are to be taken 2 hours before irradiation. The dose is calculated according to body surface area(m 2 ) (refer EPR / patient information/ body surface area, or body surface area nomogram). Dose of 8 MOP is 25 mg/m 2 ; dose of 5-MOP is 50 mg/m All patients to wear UV opaque goggles in the cabin. A face shield should also be worn unless significant lesions on face. Males must wear a sock for genital protection. 4. Incremental regime and action to be taken: Grade Definition Action E0 No erythema and no report of erythema after last treatment E0+1 Patient reports erythema after last treatment but now resolved E1 (mild) Barely perceptible asymptomatic erythema E2 Well-defined erythema, (moderate) E3 (severe) E4 (very severe) possibly causing slight manageable discomfort Well-defined symptomatic/painful erythema Painful erythema usually with blistering 40% increment; for 1/week treatment use 20% 40% increment but if previous E0+ then hold dose or 20% increment Repeat previous dose then consider 20% increments Postpone one treatment if not completely settled; if settled, repeat previous dose and thereafter consider 20% increments No treatment and reviewed by Doctor when possible. When completely settled, 50% of previous dose and then 20% increments No treatment and review by Doctor Page 6 of 22
7 5. Usual course: treatments. Maximum number of treatments per course: 30. Maximum dose per treatment: 15 J/cm 2. Lifetime limit of 200 treatments. 6. If develop small areas of erythema: repeat previous dose and apply high factor sunscreen to affected area for one treatment. 7. If develop facial erythema or unacceptable facial pigmentation, a face shield or sunscreen should be used for each treatment. 8. If develop pruritus: encourage use of emollients and antihistamines. 9. If develop Polymorphic Light Eruption (PLE): treat with emollients and very potent topical steroids (eg. Dermovate) immediately after treatment. Postpone treatment if troublesome and reduce to 20 % increments. 10. Cancellation/ missed treatments: see missed treatment protocol. 11. Discharge: see discharge protocol. 13. Documentation: Copies of Treatment summary to be sent to responsible consultant and entered on EPR. 14. Eczema PUVA Initiating dose: 0.5J/cm PUVA increments: 40%. If E1 erythema develops, change to 20% increment End of phototherapy course taper treatment, with 20% reduction in dose for each treatment: -use last dose at 1/week for 6 weeks, -then discharge. 15. Vitiligo PUVA Initiating dose dose: 0.5J/cm PUVA increment: 0.5J/cm 2 until vitiligo is just pink, then maintain or increase by 0.1J/cm Minimum 3 monthly treatment. If no response discontinue Follow up by doctor every 20 treatments Maximum 12 months treatment Clinical photographs at the start of treatment and every three months. 16. Polymorphic Light Eruption (or other photosensitivity disorder) PUVA Initiating dose: 0.5J/cm 2 Page 7 of 22
8 16.2. PUVA increment: 40% of previous dose over 4 weeks /week for 4 weeks, i.e. 8 treatments in total TREATMENT NUMBER SYSTEMIC PUVA J/cm If develop PLE during treatment, -If mild, continue with treatment in combination with emollients and topical steroids (eg. Dermovate ointment for body, eumovate for face). -If severe, treat with emollients and topical steroids AND stop treatment until rash clears, then recommence at a lower dose. -Very severe flares may require oral prednisolone discuss with doctor /book into clinic Encourage patients to keep their sun tolerance topped-up by regular sun exposure throughout spring/summer. 17. Mycosis Fungoides Systemic PUVA for plaque stage MF (UVB suitable for patch stage MF) Initiating dose and increments as for standard protocol Continue until skin clear no limit to number of treatments each course or lifetime If maintenance phototherapy is required once skin is clear, consider 1/week or less. Review every 20 maintenance treatments. 18. Palmoplantar Pustulosis Systemic PUVA with or without retinoids If initiating Acitretin midway during phototherapy, hold UV dose for three sessions before increasing dose as per regime. Consider Acitretin dose of mg daily Initial irradiation dose: as per standard protocol Maximum no. of treatments: 30 for hands, 40 for feet. 19. Palmoplantar Eczema/ Psoriasis Consider hand and foot oral PUVA for hyperkeratotic conditions Maximum no. of treatments: 30 for hands, 40 for feet. Page 8 of 22
9 Page 9 of 22
10 TREATMENT PROTOCOL No. 3: Hand and foot PUVA soaks ml of 8-MOP 1.2% lotion in 2L water (concentration of 3mg/L). 2. Soak for 15 minutes, with a delay of 30 minutes before UVA exposure. 3. For gel (0.005% 8-MOP solution in aqueous gel), apply a thin layer over the affected areas, taking care to avoid applying to surrounding unaffected skin. Then wait for a further 15 minutes prior to treatment. 4. Initial irradiation dose: Skin phototype SOAKS GEL I (Always burn, never tan) II (Usually burn, sometimes tan) III (Usually tan, sometimes burn) IV (Never burn, always tan) V (Brown skin) VI (Black skin) Topical PUVA to be given twice weekly for most cases, with 3 days between treatments. 6. All patients to wear UV opaque goggles when having UV irradiation to their hands or feet. 7. Incremental regime and action to be taken: see also Dose to Time Conversion Table Grade Definition Action E0 No erythema and no report of erythema after last treatment E0+1 Patient reports erythema after last treatment but now resolved E1 (mild) Barely perceptible asymptomatic erythema E2 Well-defined erythema, (moderate) E3 (severe) E4 (very severe) possibly causing slight manageable discomfort Well-defined symptomatic/painful erythema Painful erythema usually with blistering 40% increment; for 1/week treatment use 20% 40% increment but if previous E0+ then hold dose or 20% increment Repeat previous dose then consider 20% increments Postpone one treatment if not completely settled; if settled, repeat previous dose and thereafter consider 20% increments No treatment and reviewed by Doctor when possible. When completely settled, 50% of previous dose and then 20% increments No treatment and review by Doctor Page 10 of 22
11 8. Usual course: 30 treatments. Maximum number of treatments per course: 40. Maximum dose per treatment: 10 J/cm 2. Lifetime limit of 200 treatments. 9. If develop small areas of erythema: repeat previous dose and apply high factor sunscreen to affected area for one treatment. 10. If develop pruritus: encourage use of emollients and antihistamines. 11. If develop Polymorphic Light Eruption (PLE): treat with emollients and very potent topical steroids (eg. Dermovate) immediately after treatment. Postpone treatment if troublesome and reduce to 20 % increments. 12. Cancellation/ missed treatments: see missed treatment protocol. 13. Discharge: see discharge protocol. 14. Documentation: Treatment summary to be entered on EPR and copies to be sent to responsible consultant. Page 11 of 22
12 TREATMENT PROTOCOL No. 4: Hand and foot oral PUVA 1. Initial irradiation dose: Skin phototype Start dose (J/cm 2 ) I (Always burn, never tan) 0.5 II (Usually burn, sometimes tan) 0.5 III (Usually tan, sometimes burn) 0.5 IV (Never burn, always tan) 0.5 V (Brown skin) 0.5 VI (Black skin) PUVA to be given twice weekly for most cases, with 3 days between treatments Methoxypsoralen (8-MOP) tablets are to be taken 2 hours before irradiation. The dose is calculated according to body surface area(m 2 ) (refer EPR / patient information/ body surface area, or body surface area nomogram). Dose of 8 MOP is 25 mg/m 2 ; dose of 5-MOP is 50 mg/m Incremental regime and action to be taken: (ref: Dose to Time Conversion Table) Grade Definition Action E0 No erythema and no report of erythema after last treatment E0+1 Patient reports erythema after last treatment but now resolved E1 (mild) E2 (moderate) E3 (severe) E4 (very severe) Barely perceptible asymptomatic erythema Well-defined erythema, possibly causing slight manageable discomfort Well-defined symptomatic/painful erythema Painful erythema usually with blistering 40% increment; for 1/week treatment use 20% 40% increment but if previous E0+ then hold dose or 20% increment Repeat previous dose then consider 20% increments Postpone one treatment if not completely settled; if settled, repeat previous dose and thereafter consider 20% increments No treatment and reviewed by Doctor when possible. When completely settled, 50% of previous dose and then 20% increments No treatment and review by Doctor Page 12 of 22
13 5. Usual course: 30 treatments. Maximum number of treatments per course: 40. Maximum dose per treatment: 10 J/cm 2. Lifetime limit of 200 treatments. 6. If develop small areas of erythema: repeat previous dose and apply high factor sunscreen to affected area for one treatment. 7. If develop pruritus: encourage use of emollients and antihistamines. 8. If develop Polymorphic Light Eruption (PLE): treat with emollients and very potent topical steroids (eg. Dermovate) immediately after treatment. Postpone treatment if troublesome and reduce to 20 % increments. 9. Cancellation/ missed treatments: see missed treatment protocol. 10. Discharge: see discharge protocol. 11. Documentation: Treatment summary to be entered on EPR and copies to be sent to responsible consultant. Page 13 of 22
14 Page 14 of 22
15 TREATMENT PROTOCOL No. 5: Bath PUVA Phototherapy 1. 30ml of 8-MOP 1.2% lotion in 140L water (concentration of 2.6mg/L). 2. Bathe for 15 minutes, followed by immediate UVA exposure. 3. Initial irradiation dose: Skin phototype Start dose J/cm 2 I (Always burn, never tan) 0.2 II (Usually burn, sometimes tan) 0.3 III (Usually tan, sometimes burn) 0.4 IV (Never burn, always tan) 0.5 V (Brown skin) 0.5 VI (Black skin) Topical PUVA to be given twice weekly for most cases, with 3 days between treatments. 5. All patients to wear UV opaque goggles in the cabin. Face shield should also be worn unless significant lesions present on face. 6. Incremental regime and action to be taken: Grade Definition Action E0 No erythema and no report of erythema after last treatment E0+1 Patient reports erythema after last treatment but now resolved E1 (mild) E2 (moderate) E3 (severe) E4 (very severe) Barely perceptible asymptomatic erythema Well-defined erythema, possibly causing slight manageable discomfort Well-defined symptomatic/painful erythema Painful erythema usually with blistering 40% increment; for 1/week treatment use 20% 40% increment but if previous E0+ then hold dose or 20% increment Repeat previous dose then consider 20% increments Postpone one treatment if not completely settled; if settled, repeat previous dose and thereafter consider 20% increments No treatment and reviewed by Doctor when possible. When completely settled, 50% of previous dose and then 20% increments No treatment and review by Doctor Page 15 of 22
16 7. Usual course: 24 treatments. Maximum number of treatments per course: 30. Maximum dose per treatment: 10 J/cm 2. Lifetime limit of 200 treatments. 8. If develop small areas of erythema: repeat previous dose and apply high factor sunscreen to affected area for one treatment. 9. If develop pruritus: encourage use of emollients and antihistamines. 10. If develop Polymorphic Light Eruption (PLE): treat with emollients and very potent topical steroids (eg. Dermovate) immediately after treatment. Postpone treatment if troublesome and reduce to 20 % increments. 11. Cancellation/ missed treatments: see missed treatment protocol. 12. Discharge: see discharge protocol. 13. Documentation: Treatment summary to be entered on EPR and copies to be sent to responsible consultant. Page 16 of 22
17 TREATMENT PROTOCOL No. 6: Missed treatments for UVB, PUVA, hand and foot PUVA Ensure treatments have not been cancelled or missed due to erythema, if so follow appropriate protocol incremental regime. Missed 1 treatment Missed 2 treatments Missed 3 treatments Missed 4-6 treatments Missed >6 treatments UVB: Continue with previous increments. PUVA: Repeat previous dose. Repeat previous dose. Give dose before previous dose. Give 50% of previous dose. Refer back to consultant. Missed >3 weeks due to holiday or sickness Consult starting dose. Page 17 of 22
18 TREATMENT PROTOCOL No. 7: ACCIDENTAL UV OVERDOSE PROTOCOL 1. General points 1.1. Contact patient immediately and explain Make all efforts for patient to re-attend the phototherapy unit immediately for assessment and treatment. Prompt action will minimise UV damage Phototherapy Consultant, on call registrar, and GP to be informed Where a large error has occurred ( eg.>50% UVB dose, or >75% UVA dose), consider hospital admission for overnight observation and treatment If patient can be treated at home, frequent contact should be maintained Accurate documentation is vital; ensure all discussions are documented. All details to be entered in phototherapy notes and a copy sent for filing in main hospital notes; 1.7. Complete Trust incident form UVB-induced burns reach maximum intensity at hours, and fade thereafter. UVA-induced burns reach maximum intensity at 2-3 days for oral PUVA, or 3-5 days for bath PUVA. 2. Specific Treatment (give hospital prescription) 2.1. Oral Prednisolone to be given: 40 mg stat, followed by 30 mg /day for five days. 2.2 Topical treatment Dermovate ointment B.D. An emollient QID 2.3 Prescribe analgesics. 3. Follow-up 3.1. Offer daily dressings / nursing assessment to patient Review by medical staff within three days. Page 18 of 22
19 TREATMENT PROTOCOL No. 8: PROTOCOL for MANAGEMENT OF MINOR ADVERSE EVENTS 1. Acute adverse effects of PUVA 1.1. Severe burns - see Protocol Mild/localized burning emollients, Dermovate ointment, apply sunscreens to affected area 1.3. Erythema grade level of erythema and manage accordingly 1.4. PUVA itch uncommon, usually chest and arms. Emollients and antihistamines to tide patients over the first couple of week of PUVA. Occasionally this may be painful ; PUVA-pain consider changing to 5 MOP or bath PUVA PUVA blisters this is usually a phototoxic reaction, involving hands and feet. Consider concomitant photosensitizing drugs (eg. NSAID, thiazides, diuretics, tetracyclines, Neotigason) Tanning people with skin type IV and V may not consider tanning to be desirable. Patients with vitiligo may find tanning of normal skin worsening the overall appearance Provocation of PLE Prophylactic application of Dermovate ointment after each treatment session Reaction of Cold Sores If susceptible to cold sores, apply lip sunscreen or visor throughout duration of treatment. If develop cold sores early application of acyclovir cream five times a day Facial seborrhoeic dermatitis - affects about 5% of patients and is not very responsive to topical corticosteroids Other side effects photo-onycholysis, nail pigmentation facial hair growth in women, scalp hair growth in men curling of previous straight hair folliculitis and milia pseudoporphyria lichenoid eruption 2. Acute adverse events of UVB 2.1. Severe burns see protocol Transient erythema common; starts a few minutes after treatment and persist for up to 8 hours. It clears completely. Next erythemal assessment prior to the next dose of UVB should not be affected i.e. E0+ reaction Itch usually during first 2 weeks of treatment. Emollients and antihistamines Cold sores susceptibility to this should be prevented with lip sunscreen or visor. Treat with topical or oral acyclovir Blistering occurs at the margins of psoriasis plaques, especially on plaques around the mid and lower abdomen and buttocks. Page 19 of 22
20 PROTOCOL No. 9: MED Tester protocol MED (Minimum Erythema Dose) testing should be carried out on all patients prior to a course of narrowband UVB (TL01) phototherapy, except for vitiligo patients or where the patient's skin condition or other circumstances makes testing impractical. 1. Confirm that the patient will be able to return for evaluation of their skin response 24 hours (+/- 3 hours) after the test exposure. 2. Indentify a suitable skin area to which the MED tester can be applied. The area should have limited normal sun exposure, such as the inner surface of the forearm, and be clear of skin rashes or other skin surface changes that might complicate the assessment of the MED test. Ensure that the full area of the face of the MED tester will lie in contact with the patient's skin without undue pressure. 3. Select the test exposure time to be used on depending on the assessment of the patient's skin type. A shorter exposure time is used for Skin Types I and II, and a longer time for Skin Type III and above. 4. Prepare the MED tester and give the test exposure according to the local operating instructions. 5. Immediately the test exposure ends, mark the patient's skin beside the test area to indicate the orientation of the test area. Use a waterproof marker. Avoid marks within the actual test area. 6. In the patient's record, note the exposure time used. 7. After use, clean the MED tester with SaniCloth Detergent Wipes. 8. When the patient returns for the 24 hour response reading, examine the test area in a good light and decide which of the 10 individual test patches is just showing an erythema response. 9. From the comparison table for MEDs and phototherapy start doses, read off the MED for the appropriate test patch. Note the MED in the patient's record. 10. Also read off the corresponding phototherapy start dose and note this in the patient's record. Start doses are approximately 70% of the MED. 11. If the MED test result is unclear, e.g. all test patches with higher doses than the apparent MED patch do not also show erythema, use the standard starting doses based on skin type and skin disease. 12. Once the start dose has been determined, commence phototherapy treatment that same day. Page 20 of 22
21 PROTOCOL No. 10: Discharge protocol Treatment usually continues until the patient is clear, condition is no longer improving, has 4 treatments at MRA (minimal residual activity) or is stopped on medical advice. A phototherapy summary is sent to the referring clinician on completion of treatment. The following is a guide to follow-up care: 1. Patients completing treatment having incurred no problems discharge to referring clinician. 2. Patients who have failed to attend discharge to referring clinician. If patient has had mitigating circumstances, consider discussing with referring clinician. 3. Patients who are known to flare quickly when treatment is completed should be advised to contact the referring clinician if they develop a flare up or have concerns. 4. Patients attending for desensitisation who may require repeated treatment should be reviewed early the following year by the phototherapy clinic as appropriate. Page 21 of 22
22 Standards (section number should follow on from the preceding section) Minimum service provision standards using the Phototherapy Review toolkit, as well as recommended Phototherapy Guidelines, as suggested by the British Association of Dermatologists can be viewed here: Explanation of terms Terms as described in document. References and Supporting Documents For recommended phototherapy guidelines, see British Association Dermatologists website/phototherapy/phototherapy Service Provision in the UK Roles and responsibilities Lead Clinician: Dr Tsui Ling Lead Nurse: Sister Melanie Casey Medical Physicist: Dr Donald Allan Page 22 of 22
Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB)
 Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB) Your doctor has referred you to the Dowling Day Treatment Centre for a course of narrow band ultraviolet treatment for your
Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB) Your doctor has referred you to the Dowling Day Treatment Centre for a course of narrow band ultraviolet treatment for your
Department of Dermatology, Churchill Hospital PUVA Treatment
 Oxford University Hospitals NHS Trust Department of Dermatology, Churchill Hospital PUVA Treatment information for patients CONTENTS What is PUVA 3 What conditions are treated with PUVA? 3 How is PUVA
Oxford University Hospitals NHS Trust Department of Dermatology, Churchill Hospital PUVA Treatment information for patients CONTENTS What is PUVA 3 What conditions are treated with PUVA? 3 How is PUVA
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement
 Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
TOPICAL TREATMENTS FOR PSORIASIS
 TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
TREATMENTS FOR MODERATE OR SEVERE PSORIASIS
 TREATMENTS FOR MODERATE OR SEVERE PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with creams and ointments, which are applied to the skin. These are discussed
TREATMENTS FOR MODERATE OR SEVERE PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with creams and ointments, which are applied to the skin. These are discussed
Guide to PUVA Therapy
 Guide to PUVA Therapy Elisabeth Richard, MD Light Therapy for Skin Disease lightandlaser.com 410-847-3700!1 OVERVIEW PUVA therapy consists of taking a medication called psoralen (pronounced soralen with
Guide to PUVA Therapy Elisabeth Richard, MD Light Therapy for Skin Disease lightandlaser.com 410-847-3700!1 OVERVIEW PUVA therapy consists of taking a medication called psoralen (pronounced soralen with
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Treatment options a simple guide
 Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
VITILIGO Charles Camisa, MD 1/24/12. Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural
 VITILIGO Charles Camisa, MD 1/24/12 What is vitiligo? Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural brown pigment in the skin called melanin. It affects about 1%
VITILIGO Charles Camisa, MD 1/24/12 What is vitiligo? Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural brown pigment in the skin called melanin. It affects about 1%
NEHSNORTH EASTERN HEALTH SPECIALISTS
 COSMETIC DERMATOLOGY NEHSNORTH EASTERN HEALTH SPECIALISTS nehs.com.au CONSENT FORM ACNE Treatment I, DOB:, of authorize of North Eastern Health Specialist to perform hair removal with the BBL / Nd-Yag
COSMETIC DERMATOLOGY NEHSNORTH EASTERN HEALTH SPECIALISTS nehs.com.au CONSENT FORM ACNE Treatment I, DOB:, of authorize of North Eastern Health Specialist to perform hair removal with the BBL / Nd-Yag
Laser hair removal. Birmingham Regional Skin Laser Centre
 What is laser hair removal? involves removing unwanted hair using laser. The high level of energy in the laser is taken up by the pigment within the hair (melanin), which converts the energy into heat
What is laser hair removal? involves removing unwanted hair using laser. The high level of energy in the laser is taken up by the pigment within the hair (melanin), which converts the energy into heat
PACKAGE LEAFLET: INFORMATION FOR THE USER. Elidel 10 mg/g Cream. pimecrolimus
 PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
Oxford University Hospitals. NHS Trust. Dermatology Department Frontal Fibrosing Alopecia. Information for patients
 Oxford University Hospitals NHS Trust Dermatology Department Frontal Fibrosing Alopecia Information for patients What is Frontal Fibrosing Alopecia (FFA)? FFA is a condition which causes hair loss, mainly
Oxford University Hospitals NHS Trust Dermatology Department Frontal Fibrosing Alopecia Information for patients What is Frontal Fibrosing Alopecia (FFA)? FFA is a condition which causes hair loss, mainly
Laser Tattoo Removal. Birmingham Regional Skin Laser Centre
 What is laser tattoo removal? Laser tattoo removal is a treatment to help fade and remove unwanted tattoos. We are able to remove the following types of tattoos: Amateur tattoos - normally formed using
What is laser tattoo removal? Laser tattoo removal is a treatment to help fade and remove unwanted tattoos. We are able to remove the following types of tattoos: Amateur tattoos - normally formed using
What are spider veins? What is the best treatment for spider veins?
 Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac
 PUBLIC SUMMARY DOCUMENT Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac Sponsor: Genepharm Australasia Ltd Date of PBAC Consideration: July 2007 1. Purpose
PUBLIC SUMMARY DOCUMENT Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac Sponsor: Genepharm Australasia Ltd Date of PBAC Consideration: July 2007 1. Purpose
Laser Treatment for Acne
 Laser Treatment for Acne Exceptional healthcare, personally delivered Welcome to the Laser Centre of the South West We are part of the Plastic Surgery Department at North Bristol NHS Trust, and were set
Laser Treatment for Acne Exceptional healthcare, personally delivered Welcome to the Laser Centre of the South West We are part of the Plastic Surgery Department at North Bristol NHS Trust, and were set
COSMETIC LASER AND AESTHETICS CENTER
 COSMETC LASER AND AESTHETCS CENTER LGHT SHEAR LASER HAR REMOVAL NFORMATON AND CONSENT understand that the purpose of this procedure is to reduce and/or remove unwanted hair. There are several alternatives
COSMETC LASER AND AESTHETCS CENTER LGHT SHEAR LASER HAR REMOVAL NFORMATON AND CONSENT understand that the purpose of this procedure is to reduce and/or remove unwanted hair. There are several alternatives
1g cream or ointment contains 1 mg methylprednisolone aceponate.
 CONSUMER MEDICINE INFORMATION ADVANTAN 1g cream or ointment contains 1 mg methylprednisolone aceponate. What is in this leaflet Please read this leaflet carefully before you start using ADVANTAN. It will
CONSUMER MEDICINE INFORMATION ADVANTAN 1g cream or ointment contains 1 mg methylprednisolone aceponate. What is in this leaflet Please read this leaflet carefully before you start using ADVANTAN. It will
PSORIASIS AND ITS. Learn how vitamin D medications play an important role in managing plaque psoriasis
 PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
Skin care guidelines for patients receiving radiotherapy
 Skin care guidelines for patients receiving radiotherapy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Skin care guidelines for patients receiving radiotherapy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
HIRSUTISM. What are the aims of this leaflet?
 HIRSUTISM What are the aims of this leaflet? This leaflet has been written to help you understand more about hirsutism. It tells you what it is, what causes it, what can be done about it, and provides
HIRSUTISM What are the aims of this leaflet? This leaflet has been written to help you understand more about hirsutism. It tells you what it is, what causes it, what can be done about it, and provides
Save Face Laser & IPL Fact Sheet
 Save Face Laser & IPL Fact Sheet Patient information Laser & IPL (Intensed Pulse light) What is laser & IPL (Intensed Pulse light)? Over the last decade the use of light such as Lasers and Intense Pulsed
Save Face Laser & IPL Fact Sheet Patient information Laser & IPL (Intensed Pulse light) What is laser & IPL (Intensed Pulse light)? Over the last decade the use of light such as Lasers and Intense Pulsed
Systematic Review of UV-Based Therapy for Psoriasis
 Am J Clin Dermatol (2013) 14:87 109 DOI 10.1007/s40257-013-0015-y EVIDENCE-BASED REVIEW ARTICLE Systematic Review of UV-Based Therapy for Psoriasis Fahad Almutawa Naif Alnomair Yun Wang Iltefat Hamzavi
Am J Clin Dermatol (2013) 14:87 109 DOI 10.1007/s40257-013-0015-y EVIDENCE-BASED REVIEW ARTICLE Systematic Review of UV-Based Therapy for Psoriasis Fahad Almutawa Naif Alnomair Yun Wang Iltefat Hamzavi
Cutaneous Lymphoma FAST FACTS
 Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes Information for patients Introduction This leaflet is for people who have had surgery for
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall and lymph nodes Information for patients Introduction This leaflet is for people who have had surgery for
Radiotherapy to the chest wall
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall Information for patients Introduction This leaflet is for people who have had surgery for breast cancer
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the chest wall Information for patients Introduction This leaflet is for people who have had surgery for breast cancer
ECZEMA: YOUR GP THE SECRETS WON T TELL YOU
 ECZEMA: THE SECRETS YOUR GP WON T TELL YOU As a sufferer of eczema or dry skin, it s likely that you ll understand the frustrations associated with trying various creams and lotions that are supposed to
ECZEMA: THE SECRETS YOUR GP WON T TELL YOU As a sufferer of eczema or dry skin, it s likely that you ll understand the frustrations associated with trying various creams and lotions that are supposed to
Case Scenarios. Case Scenario 1 Group A
 Case Scenarios Prior to the workshop please work through the following scenario and be prepared to present this to the rest of the group. You can work in groups of 3-4. Specialist nurses, phototherapy
Case Scenarios Prior to the workshop please work through the following scenario and be prepared to present this to the rest of the group. You can work in groups of 3-4. Specialist nurses, phototherapy
Psoriasis. Student's Name. Institution. Date of Submission
 Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
Professor Andrew Wright,
 Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Although the flush is the classic menopausal symptom that we ve
 24 MENOPAUSE: ANSWERS AT YOUR FINGERTIPS HOW LONG DO SYMPTOMS LAST? The duration of early symptoms is very variable from a few months to many years and the severity varies between individuals. On average,
24 MENOPAUSE: ANSWERS AT YOUR FINGERTIPS HOW LONG DO SYMPTOMS LAST? The duration of early symptoms is very variable from a few months to many years and the severity varies between individuals. On average,
MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%
![MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%](/thumbs/27/10084771.jpg) MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
STUDY. Pravit Asawanonda, MD, DSc; Akkrawat Chingchai, MD; Pawinee Torranin, MD
 STUDY Targeted UV-B Phototherapy for Plaque-type Psoriasis Pravit Asawanonda, MD, DSc; Akkrawat Chingchai, MD; Pawinee Torranin, MD Objective: To determine whether targeted UV-B phototherapy is efficacious
STUDY Targeted UV-B Phototherapy for Plaque-type Psoriasis Pravit Asawanonda, MD, DSc; Akkrawat Chingchai, MD; Pawinee Torranin, MD Objective: To determine whether targeted UV-B phototherapy is efficacious
Psoriasis Treatment Transition Pathway
 Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Science > MultiClear. How the MultiClear works?
 Science > MultiClear How the MultiClear works? Treatment of Psoriasis by UVB is a common, effective and respected therapy for more than 100 years.[1] Narrow band UVB light (peak 296-313 nm) has been clinically
Science > MultiClear How the MultiClear works? Treatment of Psoriasis by UVB is a common, effective and respected therapy for more than 100 years.[1] Narrow band UVB light (peak 296-313 nm) has been clinically
BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU)
 BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU) What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinoma in situ (Bowen s disease). It
BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU) What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinoma in situ (Bowen s disease). It
Patient Guide. Important information for patients starting therapy with LEMTRADA (alemtuzumab)
 Patient Guide Important information for patients starting therapy with LEMTRADA (alemtuzumab) This medicinal product is subject to additional monitoring. This will allow quick identification of new safety
Patient Guide Important information for patients starting therapy with LEMTRADA (alemtuzumab) This medicinal product is subject to additional monitoring. This will allow quick identification of new safety
SHINGLES (Herpes zoster infection)
 SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
PSORIASISforum. Initiating Narrow-band UVB for the Treatment of Psoriasis. Alice N. Do, D.O. a and John Y.M. Koo, M.D. b
 PSORIASISforum Spring 2004 Vol. 10, No. 1 R E P R I N T E D F R O M A JOURNAL FOR N A T I O N A L P S O R I A S I S F O U N D A T I O N P R O F E S S I O N A L M E M B E R S Initiating Narrow-band UVB
PSORIASISforum Spring 2004 Vol. 10, No. 1 R E P R I N T E D F R O M A JOURNAL FOR N A T I O N A L P S O R I A S I S F O U N D A T I O N P R O F E S S I O N A L M E M B E R S Initiating Narrow-band UVB
Prescribing advice for the management and treatment of psoriasis
 Prescribing advice for the management and treatment of psoriasis This guidance contains suggested advice for the management and treatment of patients presenting with psoriasis. This guidance applies to
Prescribing advice for the management and treatment of psoriasis This guidance contains suggested advice for the management and treatment of patients presenting with psoriasis. This guidance applies to
Neutral Superoxidized solution vs. benzoyl peroxide gel 5% in the treatment of. Superoxidized solution (SOS) is an electrochemically processed aqueous
 Neutral Superoxidized solution vs. benzoyl peroxide gel 5% in the treatment of acne vulgaris: a randomized open-label clinical trial. Summary. Superoxidized solution (SOS) is an electrochemically processed
Neutral Superoxidized solution vs. benzoyl peroxide gel 5% in the treatment of acne vulgaris: a randomized open-label clinical trial. Summary. Superoxidized solution (SOS) is an electrochemically processed
about Why You Should Know Melanoma
 about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC)
 Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
PACKAGE LEAFLET: INFORMATION FOR THE USER PROPECIA 1 mg film-coated Tablets (finasteride)
 PACKAGE LEAFLET: INFORMATION FOR THE USER PROPECIA 1 mg film-coated Tablets (finasteride) This medicine is for use in men only Read all of this leaflet carefully before you start to take this medicine.
PACKAGE LEAFLET: INFORMATION FOR THE USER PROPECIA 1 mg film-coated Tablets (finasteride) This medicine is for use in men only Read all of this leaflet carefully before you start to take this medicine.
Leukocytoclastic Vasculitis and Stasis Dermatitis With Id Reaction
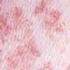 Id Reaction December 01, 2007 By David L. Kaplan, MD [1] A Photo Quiz to Hone Dermatologic Skills Case 1: A slightly pruritic eruption developed on the lower legs of a 39-year-old woman after she had an
Id Reaction December 01, 2007 By David L. Kaplan, MD [1] A Photo Quiz to Hone Dermatologic Skills Case 1: A slightly pruritic eruption developed on the lower legs of a 39-year-old woman after she had an
Nail Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
Treating psoriasis and psoriatic arthritis. A booklet for patients and carers
 Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Welcome to Bella! Give the Gift of Bella. A few tips to prepare you for your first visit: Gift Certificates are just $100 for a $150 value!
 Welcome to Bella! We are glad to have you as our guest. We encourage you to visit our website to see all of the exciting new laser and skincare treatments that we offer. Please be aware of our 24 hour
Welcome to Bella! We are glad to have you as our guest. We encourage you to visit our website to see all of the exciting new laser and skincare treatments that we offer. Please be aware of our 24 hour
National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 E-Mail: nmic@stjames.
 VOLUME 6 NUMBER 6 2000 PSORIASIS National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 E-Mail: [email protected] SUMMARY The aim of treatment is
VOLUME 6 NUMBER 6 2000 PSORIASIS National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 E-Mail: [email protected] SUMMARY The aim of treatment is
Informed Consent For Laser Hair Removal
 Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
LEFLUNOMIDE (Adults)
 Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Guidelines of care for the management of psoriasis and psoriatic arthritis
 FROM THE ACADEMY Guidelines of care for the management of psoriasis and psoriatic arthritis Section 5. Guidelines of care for the treatment of psoriasis with phototherapy and photochemotherapy Alan Menter,
FROM THE ACADEMY Guidelines of care for the management of psoriasis and psoriatic arthritis Section 5. Guidelines of care for the treatment of psoriasis with phototherapy and photochemotherapy Alan Menter,
The challenge of herpes
 The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis
 1 The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis ผ ว จ ย Rutsanee Akaraphanth MD, Yotsinee Kittipavara MD, Nataya Voravutinon MD, Usa Wachiratarapadorn
1 The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis ผ ว จ ย Rutsanee Akaraphanth MD, Yotsinee Kittipavara MD, Nataya Voravutinon MD, Usa Wachiratarapadorn
Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS
 Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS 2 Proudly supported by Disclaimer: Some photographs and models used in this booklet are for illustrative purposes only and
Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS 2 Proudly supported by Disclaimer: Some photographs and models used in this booklet are for illustrative purposes only and
The Radiotherapy Department Radiotherapy to the breast Information for patients
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the breast Information for patients page 2 Introduction This leaflet is for people who have had surgery for breast cancer
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy to the breast Information for patients page 2 Introduction This leaflet is for people who have had surgery for breast cancer
X-Plain Alopecia Reference Summary
 X-Plain Alopecia Reference Summary Introduction Hair loss is very common in both men and women. You or someone you love may be experiencing hair loss. Hair follicle Learning about normal hair growth is
X-Plain Alopecia Reference Summary Introduction Hair loss is very common in both men and women. You or someone you love may be experiencing hair loss. Hair follicle Learning about normal hair growth is
Ultraviolet (UV) Radiation Safety
 Ultraviolet (UV) Radiation Safety April 2005 Compiled by Myung Chul Jo Environmental Health and Safety University of Nevada Reno Page 1 of 8 Table of Contents 1. UVRadiation 3 2. Common sources of UV radiation
Ultraviolet (UV) Radiation Safety April 2005 Compiled by Myung Chul Jo Environmental Health and Safety University of Nevada Reno Page 1 of 8 Table of Contents 1. UVRadiation 3 2. Common sources of UV radiation
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Teriflunomide (Aubagio) 14mg once daily tablet
 Teriflunomide (Aubagio) 14mg once daily tablet Exceptional healthcare, personally delivered Your Consultant Neurologist has suggested that you may benefit from treatment with Teriflunomide. The decision
Teriflunomide (Aubagio) 14mg once daily tablet Exceptional healthcare, personally delivered Your Consultant Neurologist has suggested that you may benefit from treatment with Teriflunomide. The decision
Preetha selva et al. / International Journal of Phytopharmacology. 6(1), 2015, 42-46. International Journal of Phytopharmacology
 International Journal of Phytopharmacology Journal homepage: www.onlineijp.com 42 e- ISSN 0975 9328 Print ISSN 2229 7472 IJP A CLINICAL STUDY TO EVALUATE THE EFFECT OF TOPICAL TAZAROTENE IN THE TREATMENT
International Journal of Phytopharmacology Journal homepage: www.onlineijp.com 42 e- ISSN 0975 9328 Print ISSN 2229 7472 IJP A CLINICAL STUDY TO EVALUATE THE EFFECT OF TOPICAL TAZAROTENE IN THE TREATMENT
Dry skin, eczema, psoriasis and flare-ups
 Dry skin, eczema, psoriasis and flare-ups Let s feel comfortable in our skin FL4368_1000031525 BTS LFGT Specialist Skin A5LFT 12pp V7.indd 1 21/02/2014 09:58 Some of us live with a dry or sore skin condition.
Dry skin, eczema, psoriasis and flare-ups Let s feel comfortable in our skin FL4368_1000031525 BTS LFGT Specialist Skin A5LFT 12pp V7.indd 1 21/02/2014 09:58 Some of us live with a dry or sore skin condition.
Nurse Practitioner, Dermatology
 Melissa O Neill, O MS, APRN Nurse Practitioner, Dermatology Three Types of Skin Cancer > Basal Cell Carcinoma > Squamous Cell Carcinoma > Malignant Melanoma Basal Cell Carcinoma > Most common skin cancer
Melissa O Neill, O MS, APRN Nurse Practitioner, Dermatology Three Types of Skin Cancer > Basal Cell Carcinoma > Squamous Cell Carcinoma > Malignant Melanoma Basal Cell Carcinoma > Most common skin cancer
Ear Infections Chickenpox chickenpox
 Ear Chickenpox Infections chickenpox Chickenpox Chickenpox is a common, very contagious viral infection that over 90% of people get during childhood unless they have been immunised. After an infection,
Ear Chickenpox Infections chickenpox Chickenpox Chickenpox is a common, very contagious viral infection that over 90% of people get during childhood unless they have been immunised. After an infection,
Staff Skin Care Policy
 This is an official Northern Trust policy and should not be edited in any way Staff Skin Care Policy Reference Number: NHSCT/10/350 Target audience: All Trust staff and in particular those involved in
This is an official Northern Trust policy and should not be edited in any way Staff Skin Care Policy Reference Number: NHSCT/10/350 Target audience: All Trust staff and in particular those involved in
X-Plain Acne Reference Summary
 X-Plain Acne Reference Summary Introduction Nearly 17 million people in the United States have acne, making it one of the most common skin diseases in the USA. Although acne is not a serious health threat,
X-Plain Acne Reference Summary Introduction Nearly 17 million people in the United States have acne, making it one of the most common skin diseases in the USA. Although acne is not a serious health threat,
Treatments for allergy are usually straightforward, safe and effective. Common treatments include:
 Allergy Medications The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient
Allergy Medications The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient
Eastern Health MS Service. Tysabri Therapy. Information for People with MS and their Families
 Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Additional information >>> HERE <<< How To scalp psoriasis treatment philippines Scam or Work?
 Additional information >>> HERE http://urlzz.org/psoriasis7/pdx/fph1
Additional information >>> HERE http://urlzz.org/psoriasis7/pdx/fph1
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la]
![READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la] READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la]](/thumbs/35/17235501.jpg) READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr NUCALA [new-ka la] mepolizumab lyophilized powder for subcutaneous injection Read this carefully before you start
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr NUCALA [new-ka la] mepolizumab lyophilized powder for subcutaneous injection Read this carefully before you start
A guide for people with genital herpes
 A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
Lasers that emit short pulses of UV light in
 Handheld roadband UV Phototherapy Module for the Treatment of Patients With Psoriasis and Vitiligo Peter P. Rullan, MD Cosmetic Technique Short pulses of UV light in the 300- to 380-nm wavelength have
Handheld roadband UV Phototherapy Module for the Treatment of Patients With Psoriasis and Vitiligo Peter P. Rullan, MD Cosmetic Technique Short pulses of UV light in the 300- to 380-nm wavelength have
Atopic Dermatitis/Eczema
 Atopic Dermatitis/Eczema Symptoms Eczema, also known as atopic eczema or atopic dermatitis, is a skin condition causing inflammation and intense irritation. Eczema symptoms tend to be caused by dry skin.
Atopic Dermatitis/Eczema Symptoms Eczema, also known as atopic eczema or atopic dermatitis, is a skin condition causing inflammation and intense irritation. Eczema symptoms tend to be caused by dry skin.
Ruthenium Plaque Treatment
 Information for patients Department of Ophthalmology Royal Hallamshire Hospital Ruthenium Plaque Treatment What is Ruthenium Plaque treatment? This is a treatment whereby a plaque is surgically placed
Information for patients Department of Ophthalmology Royal Hallamshire Hospital Ruthenium Plaque Treatment What is Ruthenium Plaque treatment? This is a treatment whereby a plaque is surgically placed
PACT. PACT Nail Fungus Therapy Treatment Instructions. Photodynamic therapy for nail fungus using light, safely and gently.
 PACT PACT Nail Fungus Therapy Treatment Instructions Photodynamic therapy for nail fungus using light, safely and gently. PACT Nail Fungus Therapy Treatment Instructions Contents 1. Introduction 2. Nail
PACT PACT Nail Fungus Therapy Treatment Instructions Photodynamic therapy for nail fungus using light, safely and gently. PACT Nail Fungus Therapy Treatment Instructions Contents 1. Introduction 2. Nail
Psoriasis is a skin condition that causes scaly red patches on your skin. There's no cure for psoriasis, but there are treatments that can help.
 Patient information from the BMJ Group Psoriasis What is it? What are the symptoms? How is it diagnosed? How common is it? What treatments work? What will happen? Questions to ask Psoriasis If you get
Patient information from the BMJ Group Psoriasis What is it? What are the symptoms? How is it diagnosed? How common is it? What treatments work? What will happen? Questions to ask Psoriasis If you get
Vitamin-D User's Manual Supplement
 Vitamin-D User's Manual Supplement For use with all Solarc/SolRx UVB-Narrowband (UVB-NB) and UVB-Broadband (UVB) Phototherapy Devices E-Series, 1000-Series, 500-Series, 100-Series Solarc Systems Inc. 1515
Vitamin-D User's Manual Supplement For use with all Solarc/SolRx UVB-Narrowband (UVB-NB) and UVB-Broadband (UVB) Phototherapy Devices E-Series, 1000-Series, 500-Series, 100-Series Solarc Systems Inc. 1515
Common Skin Conditions in Children. Liz Moore and Emma King Dermatology Nurse Consultants
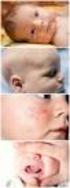 Common Skin Conditions in Children Liz Moore and Emma King Dermatology Nurse Consultants Diagnosis? Nummular Dermatitis Disc pattern rash (discoid eczema) Clearly demarcated edges Occurs at any age Can
Common Skin Conditions in Children Liz Moore and Emma King Dermatology Nurse Consultants Diagnosis? Nummular Dermatitis Disc pattern rash (discoid eczema) Clearly demarcated edges Occurs at any age Can
Radiation Oncology Patient information. Radiation Therapy for breast cancers
 Radiation Oncology Patient information Radiation Therapy for breast cancers Radiation Therapy for breast cancers 1 Radiation therapy for breast cancer Radiation therapy plays a vital role in treating and
Radiation Oncology Patient information Radiation Therapy for breast cancers Radiation Therapy for breast cancers 1 Radiation therapy for breast cancer Radiation therapy plays a vital role in treating and
Gel Manicures and Pedicures
 Gel Manicures and Pedicures Gel Manicures and Pedicures While gel systems for manicures and pedicures have been available for more than three decades, their recent popularity is driven by technological
Gel Manicures and Pedicures Gel Manicures and Pedicures While gel systems for manicures and pedicures have been available for more than three decades, their recent popularity is driven by technological
Acne (Acne Vulgaris) A common type of bacteria that lives on the skin, known as Propionibacterium acnes, sometimes
 Acne (Acne Vulgaris) Acne, clinically known as acne vulgaris, is the most common skin disease. It affects 85% of teenagers, some as young as 12, and often continues into adulthood. It is also called pimples,
Acne (Acne Vulgaris) Acne, clinically known as acne vulgaris, is the most common skin disease. It affects 85% of teenagers, some as young as 12, and often continues into adulthood. It is also called pimples,
Hydrozole Cream Hydrocortisone (microfine) 1% w/w and Clotrimazole 1% w/w
 CONSUMER MEDICINE INFORMATION What is in this leaflet? This leaflet answers some common questions about Hydrozole It does not contain all the available information. It does not take the place of talking
CONSUMER MEDICINE INFORMATION What is in this leaflet? This leaflet answers some common questions about Hydrozole It does not contain all the available information. It does not take the place of talking
Summary Acne vulgaris is a chronic, treatable disease but response to treatment may be delayed.
 TREATMENT OF ACNE VULGARIS Summary Acne vulgaris is a chronic, treatable disease but response to treatment may be delayed. Topical agents are useful as monotherapy for mild acne and in combination with
TREATMENT OF ACNE VULGARIS Summary Acne vulgaris is a chronic, treatable disease but response to treatment may be delayed. Topical agents are useful as monotherapy for mild acne and in combination with
Intravenous Methyl Prednisolone in Multiple Sclerosis
 Intravenous Methyl Prednisolone in Multiple Sclerosis Exceptional healthcare, personally delivered Relapse management in multiple sclerosis Relapses in multiple sclerosis (MS) are common and caused by
Intravenous Methyl Prednisolone in Multiple Sclerosis Exceptional healthcare, personally delivered Relapse management in multiple sclerosis Relapses in multiple sclerosis (MS) are common and caused by
light therapy > UVB phototherapy > Home phototherapy > Lasers > PUVA > Sunlight
 light therapy > UVB phototherapy > Home phototherapy > Lasers > PUVA > Sunlight introduction to psoriasis what is psoriasis? Psoriasis is a noncontagious, genetic disease of the immune system, which affects
light therapy > UVB phototherapy > Home phototherapy > Lasers > PUVA > Sunlight introduction to psoriasis what is psoriasis? Psoriasis is a noncontagious, genetic disease of the immune system, which affects
Additional information >>> HERE <<< How To scalp psoriasis treatment philippines Scam or Work?
 Additional information >>> HERE http://urlzz.org/psoriasis7/pdx/fph1
Additional information >>> HERE http://urlzz.org/psoriasis7/pdx/fph1

 More information >>> HERE
More information >>> HERE