Respiratory distress in the newborn
|
|
|
- Shawn Walton
- 7 years ago
- Views:
Transcription
1 Respiratory distress in the newborn Respiratory distress in newborn is one of the commonest conditions requiring admission in newborn nursery and it contributes to 30-40% of admissions in NICU. 1 Respiratory distress occurs in 2.2% of all newborns and in almost 60% of the infants below 1000 gm (ELBW infants). 2 A neonate can develop respiratory distress due to a wide variety of conditions, which are not limited to respiratory or cardiovascular causes. Management of respiratory distress may vary from providing warmth and oxygen to maximum respiratory support such as high frequency ventilation or inhaled nitric oxide therapy. Appropriate management includes proper assessment of the infant for the cause, and precise decision making about the need for and the level of respiratory support required and other supportive measures. Definition Respiratory distress is defined according to the National Neonatal Perinatal Database (NNPD) 3 as presence of any two of the following features: 1. Respiratory rate >60/minute 2. Subcostal/intercostal recessions 3. Expiratory grunt/groaning In addition to the above features, presence of nasal flaring, suprasternal retractions, decreased air entry on auscultation of the chest also will indicate the presence of respiratory distress. An infant who has an advanced degree of respiratory distress may exhibit additional signs, such as cyanosis, gasping, choking, apnea, and stridor. 4 Incidence Respiratory distress occurs in almost % of the live born infants. 2,5 According to the NNPD data ( ), 5.8% of the live born infants had respiratory morbidities. 3 The incidence also varies with the gestational age of the infants with the incidence being inversely proportional to the gestational age and birth weight. In a prospective study, it was found that almost 58% of the ELBW infants (birth weight <1000 g) developed respiratory distress but it was only 0.7% in infants who were of normal weight ( g). Causes Respiratory distress in a newborn can be due to a wide variety of conditions, majority of which are uncommon and should be considered in cases with unusual presentations (Table 1). The frequency of a particular condition as the cause of respiratory distress in an infant depends on various factors with gestation being the most important one. In preterm infants, respiratory distress syndrome (RDS) being AK Deorari 23/7/12 1:06 PM Formatted: Tabs:Not at 2.05 cm AK Deorari 23/7/12 1:06 PM Deleted: 2
2 the most common cause (almost 90%) while in the late preterm and term infants transient tachypnea of newborn (TTN) is the predominant cause (68%). 2 Table 1 Causes of respiratory distress in the newborn. Upper Airway Obstruction Choanal atresia Nasal stenosis Pierre Robin sequence Laryngeal stenosis or atresia Hemangioma Vocal cord paralysis Vascular rings Tracheobronchial stenosis Cleft palate Pulmonary Diseases Respiratory distress syndrome (RDS) Transient tachypnea of the newborn (TTN) Aspiration (including meconium aspiration syndrome; MAS) Pneumonia Pneumothorax Pneumomediastinum Primary pulmonary hypertension Tracheoesophageal fistula (TEF) Pulmonary hemorrhage Pulmonary hypoplasia Pulmonary agenesis Cystic adenomatoid malformation Pleural effusion Chylothorax Neoplasm Bronchopulmonary sequestration Pulmonary arteriovenous malformation Pulmonary interstitial emphysema Pulmonary edema Congenital alveolar proteinosis Congenital lobar emphysema Cardiac Diseases Cyanotic congenital heart disease Acyanotic congenital heart disease Arrhythmia Congestive cardiac failure Cardiomyopathy Thoracic Causes Chest wall deformity Thoracic mass AK Deorari 12/7/12 12:36 PM Deleted: AK Deorari 12/7/12 12:36 PM Deleted: Masses... [1] AK Deorari 12/7/12 12:36 PM Deleted: Nasal stuffiness AK Deorari 12/7/12 12:38 PM Comment [1]: Can we just mention important cause and reduce list AK Deorari 12/7/12 12:38 PM Deleted: Pneumopericardium AK Deorari 12/7/12 12:39 PM Deleted: M
3 Metabolic Disorders Hypoglycemia Infant of a diabetic mother Inborn errors of metabolism Diaphragmatic Causes Hernia Paralysis Neuromuscular Diseases Central nervous system damage (birth trauma, hemorrhage) Medication (maternal sedation, narcotic withdrawal) Muscular disease (myasthenia gravis) Intraventricular hemorrhage Meningitis Hypoxic- ischemic encephalopathy Seizure disorder Obstructed hydrocephalus Infantile botulism Spinal cord injury Infectious Causes Sepsis Pneumonia (especially group B Streptococcus) Hematological Causes Anemia Polycythemia Abnormal hemoglobin Miscellaneous Causes Asphyxia Acidosis Hypo/hyperthermia Hypo/hypernatremia Assessment of respiratory distress Initial assessment Initial assessment of respiratory distress in the delivery room should be done to find out life threatening conditions, which require immediate management such as inadequate or obstructed airway (gasping, choking, stridor) or circulatory collapse (bradycardia, hypotension, poor perfusion). If such features are present then emergency measures such as bag and mask ventilation or intubation should be carried out as necessary. 4 History A detailed history is important in assigning a cause to the respiratory distress in a given infant (Table 2).
4 Table 2: Relevant history in a neonate with respiratory distress 6 Antenatal Diabetes mellitus Fever, UTI Polyhydramnios/oligohydramnios Rh isoimmunization Drug abuse Antenatal steroids status Intranatal PPROM/ PROM Intrapartum fever/ Chorioamnionitis Sedative use Meconium stained liquor Abnormal fetal monitoring Instrumental delivery/ Birth trauma Need for bag& mask ventilation Postnatal Gestational age Shake test Onset/ Course of respiratory distress Radiological features AK Deorari 12/7/12 12:44 PM Formatted: Font:Bold General examination It should be done to identify any feature which may give a clue to the etiology such as dysmorphic features, anomalies, features of intrauterine growth restriction, single umbilical artery, scaphoid abdomen, drooling of saliva etc. Assessment of respiratory distress Respiratory rate Respiratory rate (RR) should be counted for full one minute with a timer and when the baby is quiet and preferably when baby is not hungry or immediately after feeds. 3 A normal neonate has a RR of 40-60/min. RR above 60/min is considered as tachypnea. But at times, baby can have respiratory rates well below 60/min but with significant retractions or has apneic episodes interspersed, which may signify severe respiratory distress with impending respiratory failure. Grunting Infants develop an expiratory groaning noise called grunting when they have significant respiratory distress. Grunting happens when the infant attempts to keep the alveoli open to maintain the functional residual capacity by partially closing the glottis during expiration. 4 Grunting generally disappears first when the baby starts improving but it can also disappear in a baby who is worsening because of exhaustion. Hence it has to be assessed in the context of other features such as oxygen saturation, color and activity of the infant.
5 Stridor Stridor is produced due to narrowing of the major airways. It is often inspiratory but can be expiratory or biphasic. Stridor can occur in newborn due to laryngomalacia, Pierre Robin sequence etc. Chest retractions Retractions have to be assessed in the suprasternal, intercostal, subcostal and xiphoid area. Retractions can be mild to severe depending on the severity of respiratory distress. Suprasternal recession more often suggests upper airway obstruction and may be a pointer toward upper airway anomaly in neonates. Intercostal retraction suggests alveolar involvement. Nasal flaring also has to be looked for when assessing for chest retractions. Oxygen saturation Oxygen saturation has to be checked preferentially both preductal and postductal. Preductal SpO2 is checked by applying the pulse oximeter probe to the right hand and postductal by putting the probe on the legs. A preductal- postductal difference of more than 5% to 10% indicates probable right- to- left shunt through patent ductus arteriosus (PDA) in the setting of persistent pulmonary hypertension of the newborn (PPHN). 7 Respiratory system examination Respiratory system examination includes inspection of the chest for symmetry of chest movements bilaterally, auscultation for the symmetry of breath sound and for the presence of any adventitious sounds such as crepitations. When there is suspicion of pneumothorax, transillumination of the chest should be carried out. Scoring the severity of respiratory distress Scoring the respiratory distress is essential as it provides an objective way of assessing the severity, and also monitoring the score at regular intervals helps in deciding the course of the illness either improvement or deterioration. Silverman score 8 (Table 2) and Downe s score 9 (Table 3) are used to assess the severity of the respiratory distress.
6 Table 2 Silverman score Feature Score 0 Score 1 Score 2 Upper chest movement None Respiratory lag See- Saw respiration Lower chest retractions None Minimal Marked Xiphoid retractions None Minimal Marked Nasal flaring None Minimal Marked Grunting None Audible with stethoscope Audible without stethoscope Chest movement: Upper chest movement Upper chest movement is assessed by observing the synchrony of the movement with the abdomen. Upper chest is the part of the chest anterior to the mid axillary line. Synchronized movement of upper chest with abdomen is scored 0, while lag of upper chest behind the abdomen is scored as 1 and see- saw movement of the chest and abdomen as 2. Lower chest retractions Lower chest retractions are assessed by observing the retractions between the ribs below the mid axillary line and is rated as none, minimal or marked. This indicates loss of FRC of lungs. Xiphoid retractions Similarly, retraction below the xiphoid process are rated as none, minimal or marked. Nasal flaring Normally, there should be no nasal flaring. Minimal flaring is scored as 1 and marked flaring is scored as 2. Expiratory grunting Grunting that is audible with a stethoscope is scored 1, and grunting that is audible without using a stethoscope is scored 2. The higher the score, more severe is the respiratory distress. A score greater than 7 indicates that the baby is in respiratory failure. AK Deorari 23/7/12 1:07 PM Deleted: rectractions Table 3 Downe s score Feature Score 0 Score 1 Score 2 Cyanosis None In room air In 40% FiO 2 Retractions None Mild Severe Grunting None Audible with stethoscope Audible without stethoscope Air entry Normal Decreased Barely audible Respiratory rate < >80 or apnea Score: > 4 = Clinical respiratory distress- monitor arterial blood gases > 7 = Impending respiratory failure
7 In a recent study it was found that Downe s score of 5 had a sensitivity of 88%, specificity of 81%, positive predictive value of 72% and negative predictive value of 92% for detecting hypoxemia in neonates with respiratory distress. 10 Hemodynamic stability Pulse rate, blood pressure and capillary refill time have to be monitored to identify hypoperfusion which can be secondary to prolonged hypoxemia. Causes Respiratory distress syndrome RDS also called as hyaline membrane disease (HMD) is seen almost exclusively in preterm infants. The risk of RDS decreases with increasing gestational age: 60% of babies born at fewer than 28 weeks gestation, 30% of babies born between 28 and 34 weeks gestation, and fewer than 5% of babies born after 34 weeks gestation develop RDS. 11 Other factors that increase the risk of RDS include male sex, maternal gestational diabetes, perinatal asphyxia, hypothermia, and multiple gestations. Antenatal steroids and prolonged rupture of membranes decrease the risk of RDS. RDS presents at the time of or soon after birth, and symptoms worsen over time. Shake test done from the gastric aspirate may be negative. 12 Along with the history and physical examination, a chest radiograph is needed for the diagnosis of RDS. The typical chest radiograph shows diffuse atelectasis and the classic ground glass appearance of the lung fields. Air bronchograms, which are air- filled bronchi superimposed on the relatively airless parenchyma of the lung tissue, also are seen commonly on chest radiograph. Transient tachypnea of newborn (TTN) This relatively benign, self- limited disease also is known as RDS type 2 or wet lungs. It occurs in approximately 11 per 1,000 live births and appears more often in boys, in infants delivered by cesarean section, and in infants who have perinatal asphyxia, or maternal complications such as asthma, diabetes, or analgesia or anesthesia during labor. 13,14 Respiratory morbidity in elective caesarean section is inversely related to gestational age: 73.8/1000 in the 37 th week, 42.3/1000 in the 38 th week, and 17.8/1000 in the 39 th week of gestation (therefore elective cesarean sections should be delayed until 39 to 40 wk). 15 It represents transient pulmonary edema resulting from delayed clearance of fetal lung liquid. It can occur in both term and preterm neonates. Lung liquid is produced actively in utero by a chloride pump that causes influx of chloride and water from the interstitium into the alveolar space. Approximately 2 to 3 days before delivery, lung liquid starts to clear due to transformation of the secretory channels to absorptive ones under the hormonal changes which occur with the onset of
8 labor. 16 Because this liquid contains very little protein, low oncotic pressure also favors the movement of water from the alveolar spaces into the interstitium. At this time, prostaglandin secretion by the feto- placental unit increases to trigger labor. Prostaglandins are responsible for the lymphatic dilatation that accelerates clearance of liquid from the interstitium. After birth, when the lungs expand with air, water moves rapidly from air spaces to connective tissue, to be removed gradually from the lungs by the lymphatic system and pulmonary blood vessels. Infants who have TTN present clinically with tachypnea and occasionally grunting and nasal flaring immediately after birth. Typically, arterial blood gases reveal respiratory acidosis and mild- to- moderate hypoxemia. 17 Chest radiography reveals hyperinflation, perihilar streaking due to dilated lymphatics, increased interstitial markings, fluid in the interlobar fissures and occasionally pleural effusion and mild cardiomegaly. TTN is generally a benign, self- limited disease that usually responds well to oxygen therapy. Mechanical ventilation seldom is needed, although many infants require nasal continuous positive airway pressure (ncpap) support. The CPAP may assist in maintaining alveolar surface area as well as absorbing the retained intra- alveolar fluid. Infants whose disease is uncomplicated usually recover without long term pulmonary sequelae. Full recovery is expected within 2 to 5 days. Meconium aspiration syndrome (MAS) MAS is defined as respiratory distress in an infant born through meconium stained amniotic fluid whose symptoms cannot otherwise be explained. Approximately 13% of all live births are complicated by meconium stained amniotic fluid, and of these, 4% to 5% of infants develop MAS. 18 Passage of meconium in utero may represent fetal hypoxemia. Meconium can be aspirated before, during, or after delivery. Once aspirated, meconium can cause obstruction of the air passages, chemical pneumonitis with activation of several inflammatory mediators, and inactivation of lung surfactant. The infant who has MAS may present with varying degrees of respiratory distress and is likely to have a barrel chest with audible rales or rhonchi on auscultation. The chest radiograph usually shows patchy areas of atelectasis alternating with areas of overinflation. Pneumothorax may be seen in 10% to 20% of infants who have MAS. 19
9 Pneumonia Pneumonia may be acquired in utero, during delivery (or perinatally), or postnatally in the nursery or at home. At autopsies of both stillbirths and live born neonatal deaths, pneumonia was found to be present in 20% to 60% in different centers. 20 Pneumonia which presents before 72 hours of life is almost synonymous with early onset sepsis (EOS) and the risk factors include maternal fever, chorioamnionitis, prolonged rupture of membranes (PROM), unclean vaginal examination and prematurity. The causative agent varies, depending on whether the infection is acquired before, during, or after birth in the nursery or at home. Congenital pneumonia is a severe disease that frequently results in either stillbirth or death within the first 24 hours after birth. Pneumonias that are acquired later present most often as systemic disease. In neonatal pneumonia, the chest radiograph may reveal classical patchy infiltrates, but the findings also may be indistinguishable from RDS. The presence of a pleural effusion supports the diagnosis of pneumonia; it has been reported in up to 67% of cases, but essentially never in uncomplicated RDS. 20 Mild cardiac enlargement in the absence of cardiac anomalies also is seen more often in pneumonia than in RDS. Management includes oxygen therapy, ventilatory support, antibiotics, and often vasopressor support such as dopamine and dobutamine. Congenital heart disease Infants who have CHD may present with cyanosis or heart failure. Signs that generally are consistent with CHD include: visibly hyperactive precordial impulse, gallop rhythm, poor capillary refill, weak pulses, decreased or delayed pulses in lower extremities, hepatomegaly, and abnormal vascularity or cardiomegaly on chest radiography. 21 A single second heart sound without split also may be indicative of CHD. Nada s criteria also can be applied to identify infants with congenital heart disease. A neonate who has cyanosis without marked respiratory distress and an O 2 saturation of less than 85% in both room air and 100% oxygen likely has an intracardiac shunt. If the O 2 saturation increases to more than 85% on 100% oxygen, a full hyperoxia test should be performed. The test consists of obtaining a baseline right radial (preductal) arterial blood gas measurement with the child breathing room air and repeating the measurement while the infant is receiving 100% O2. Arterial PaO 2 measurement greater than 250 mm Hg on 100% oxygen rules out cyanotic CHD, between 100 and 250 mm Hg suggests cyanotic CHD with good mixing or pulmonary disease, and less than 100 mm Hg suggests cyanotic CHD (or severe pulmonary hypertension). 22 Echocardiography needs to be done to confirm the diagnosis.
10 Table 4: Comparison of common causes of respiratory distress in neonates Condition Risk factors Clinical course Radiological features Respiratory distress syndrome (RDS) Transient tachypnea of newborn (TTN) Early onset sepsis (EOS)/ pneumonia Meconium aspiration syndrome (MAS) Prematurity (usually <34 weeks) Lack of antenatal steroids Infant of diabetic mother Birth asphyxia Rh isoimmunization Predominantly late preterm and term infants Born by Caesarean section Maternal diabetes Risk factors such as PROM,chorioamnionitis, maternal fever, unclean vaginal examinations Meconium stained amniotic fluid Onset at or soon after birth Progresses till 48 hours, static for 48 hrs and improves later. FiO 2 requirement often more than 40% Surfactant modifies the typical course Onset at or soon after birth Maximum severity at birth and improves gradually FiO 2 requirement seldom more than 40% Onset at birth or delayed May fail to improve with oxygen/ CPAP Onset may be at birth or delayed Meconium staining of cord/ skin Hyperinflated chest Features of PPHN Low volume lungs Fine reticulo- granular pattern- Ground glass appearance Air bronchograms White- out lungs Hyperinflated lungs Perihilar sreaking Fluid in minor fissure Pleural effusion Mild cardiomegaly Homogeneous/ Non- homogeneous opacities bilaterally Hyperinflated lungs Coarse nodular opacities Patchy atelactasis Areas of overinflation Management: Investigations Often the diagnosis requires appropriate history along with the reports of antenatal investigations, clinical examination and a proper chest x ray. Sepsis screen, blood cultures may be required when sepsis is strongly suspected. CSF examination is warranted in the presence of clinical sepsis or positive blood culture. Other investigations specific to the suspected clinical condition such as CT thorax in case of lung anomalies, or echocardiography in PPHN or congenital heart disease may be required. Treatment The basic principles of treatment include 1. Supportive care 2. Respiratory support
11 3. Monitoring for and management of complications 4. Specific therapy Supportive care This includes maintenance of thermo- neutral environment by caring the infant under radiant warmer or in incubator, ensuring normal blood glucose levels with intravenous fluids and monitoring the vital parameters such as heart rate, respiratory rate and scoring of the respiratory distress. Respiratory support Respiratory support provided to the infant depends on many factors such as the size of the infant, hemodynamic stability, the pathologic condition under treatment, the severity of respiratory distress and the presence of complication if any. The objective is to ensure adequate oxygenation and ventilation, and thereby decrease the work of breathing. The aim would be to maintain ph>7.25, po mm Hg, pco 2 <50 mmhg and SpO 2 88%- 93%. Supplemental oxygen Most often babies with conditions such as TTN or mild RDS may require only supplemental oxygen which is delivered through head box. The FiO 2 requirement of the baby has to be monitored at regular intervals so that any increase in requirement to maintain the SpO 2 in the optimal range can be identified early and thereby the worsening of the lung condition, or consequent complications developing if any. CPAP Infants who fail to maintain adequate oxygenation and ventilation on supplemental oxygen or those who have significant respiratory distress with Silverman or Downe s score more than 4 will require CPAP. CPAP is generally used in preterm infants with mild to moderate respiratory distress. It may be also be used in late preterm and term infants with TTN or pneumonia if tolerated. 23 Mechanical ventilation Infants who fail to maintain oxygenation and ventilation on CPAP will require mechanical ventilation. Mode of ventilation and the settings will vary based on the weight and gestation of the infant, the condition being treated and the existing unit policy. Those who fail conventional ventilation may require high frequency ventilation. Inhaled nitric oxide therapy Infants with features suggestive of PPHN will require inhaled ino if they meet the criteria. Monitoring and management of complications Infants with respiratory distress need to be monitored for worsening of the distress, hemodynamic instability, features of PPHN, acute kidney injury due to hypoxia and complications due to mechanical ventilation etc. If any such complications develop they should be managed appropriately.
12 Specific therapy Specific treatment strategies include surfactant replacement therapy for RDS, antibiotics for EOS/pneumonia, surgical resection for lung malformations etc.
13 References 1. Mathai SS, Raju U, Kanitkar M et al. Management of respiratory distress in the newborn. MJAFI 2007; 63 : Rubaltelli FF, Dani C, Reali MF, et al: Acute neonatal respiratory distress in Italy: a one- year prospective study, Acta Paediatr 87: , NNPD working definitions.nnpd report NNPD network, ICMR; p Hany Aly. Respiratory Disorders in the Newborn: Identification and Diagnosis. Pediatrics in Review 2004;25; Bonafe` L, Rubaltelli F. The incidence of acute neonatal respiratory disorders in Padova county: an epidemiological survey. Acta Paediatr 1996; 85: Jackson JC. Respiratory distress in the preterm infant. In: Avery s diseases of the newborn 9 th edition. Eds; Gleason CA, Devaskar S, Elsevier Philadelphia 2012.p Kinsella JP. Inhale nitric oxide in the term newborn. Early Human Development 84 (20 08) Silverman WA, Andersen DH. A controlled clinical trial of effects of water mist on obstructive respiratory signs, death rate and necropsy findings among premature infants. Pediatrics:1956:17; Downes JJ, Vidyasagar D, Boggs TR Jr, Morrow GM 3rd. Respiratory distress syndrome of newborn infants. I. New clinical scoring system (RDS score) with acid- - base and blood- gas correlations. Clin Pediatr (Phila) Jun;9(6): Anita Rusmawati, Ekawati L. Haksari, Roni Naning. Downes score as a clinical assessment for hypoxemia in neonates with respiratory distress. Paediatr Indones. 2008;48: Warren JB, Anderson JM. Core Concepts : Respiratory Distress Syndrome. Neoreviews 2009;10;e Kopelman AE, Matthew OP. Common respiratory disorders of the newborn. Pediatr Rev.1995;16: Avery ME, Gatewood OB, Brumly G. Transient tachypnea of the newborn. Am J Dis Child. 1966;111: Haliday H, McClure G, Reid M. Transient tachypnoea of the newborn: two distinct clinical entities? Arch Dis Child. 1981;56: Morrison JJ, Rennie JM, Milton PJ: Neonatal respiratory morbidity and mode of delivery at term: influence of timing of elective caesarean section. Br J Obstet Gynaecol 102: , Jain L, Eaton DC. Physiology of fetal lung fluid clearance and the effect of labor. Semin Perinatol 2006; 30: O Brodovich H, Canessa C, Ueda J, et al: Expression of the epithelial Na+ channel in the developing rat lung. Am J Physiol 265:C491- C496, Dargaville PA, Copnell B. The epidemiology of meconium aspiration syndrome: Incidence, Risk Factors, Therapies, and Outcome. Pediatrics 2006;117: Vain NE, Szyld EG, Prudent LM, Wiswell TE, Aguilar AM, Vivas NI. Oropharyngeal and nasopharyngeal suctioning of meconium- stained neonates before delivery of their shoulders: multicentre, randomised controlled trial.lancet. 2004;364:
14 20. Flidel- Rimon O, Shinwell ES. Respiratory Distress in the term and near- term Infant. Neoreviews 2005;6;e Parker TA, Kinsella JP. Respiratory Failure in the Term Newborn. In: Avery s diseases of the newborn 9 th edition. Eds; Gleason CA, Devaskar S, Elsevier, Philadelphia 2012.p Weschler SB, Wernovsky G. Cardiac disorders. In: Cloherty JP, Eichenwald EC, Stark AR Eds. Manual of Neonatal Care 6 th edition. Lippincott William& Wilkins USA 2011.p Sankar MJ, Sankar J, Agarwal R, Paul VK, Deorari AK. Protocol for administering continuous positive airway pressure in neonates. Indian J Pediatr 2008; 75:
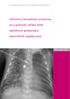
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Fetal Acid Base Status and Umbilical Cord Sampling. David Acker, MD
 Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
General Thoracic Surgery ICD9 to ICD10 Crosswalks. C34.11 Malignant neoplasm of upper lobe, right bronchus or lung
 ICD-9 Code ICD-9 Description ICD-10 Code ICD-10 Description 150.3 Malignant neoplasm of upper third of esophagus C15.3 Malignant neoplasm of upper third of esophagus 150.4 Malignant neoplasm of middle
ICD-9 Code ICD-9 Description ICD-10 Code ICD-10 Description 150.3 Malignant neoplasm of upper third of esophagus C15.3 Malignant neoplasm of upper third of esophagus 150.4 Malignant neoplasm of middle
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships. Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh
 Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh Jan 2006 Respiratory Failure inadequate blood oxygenation
Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh Jan 2006 Respiratory Failure inadequate blood oxygenation
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
Milliman Guidelines NICU Levels*
 Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Accuracy and reliability of pulse oximetry in
 Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
Cardiovascular Pathophysiology:
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology What is Cyanosis? Bluish discoloration of skin that occurs when
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology What is Cyanosis? Bluish discoloration of skin that occurs when
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Physiologic Basis for Fetal Heart Rate Monitoring
 Physiologic Basis for Fetal Heart Rate Monitoring Physiologic Basis for Fetal Heart Rate Monitoring The objective of intrapartum fetal heart rate (FHR) monitoring is to prevent fetal injury that might
Physiologic Basis for Fetal Heart Rate Monitoring Physiologic Basis for Fetal Heart Rate Monitoring The objective of intrapartum fetal heart rate (FHR) monitoring is to prevent fetal injury that might
Respiratory Concerns in Children with Down Syndrome
 Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): 7/1/2002 Most Recent Review Date (Revised): 3/24/2015 Effective Date: 6/1/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Original Issue Date (Created): 7/1/2002 Most Recent Review Date (Revised): 3/24/2015 Effective Date: 6/1/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
The Newborn With a Congenital Disorder. Chapter 14. Copyright 2008 Wolters Kluwer Health Lippincott Williams & Wilkins
 The Newborn With a Congenital Disorder Chapter 14 Congenital Anomalies or Malformations May be caused by genetic or environmental factors Approximately 2% to 3% of all infants born have a major malformation
The Newborn With a Congenital Disorder Chapter 14 Congenital Anomalies or Malformations May be caused by genetic or environmental factors Approximately 2% to 3% of all infants born have a major malformation
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Pulmonary Patterns VMA 976
 Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
The clinical presentation of respiratory
 Respiratory Distress in the Newborn CHRISTIAN L. HERMANSEN, MD, and KEVIN N. LORAH, MD Lancaster General Hospital, Lancaster, Pennsylvania The most common etiology of neonatal respiratory distress is transient
Respiratory Distress in the Newborn CHRISTIAN L. HERMANSEN, MD, and KEVIN N. LORAH, MD Lancaster General Hospital, Lancaster, Pennsylvania The most common etiology of neonatal respiratory distress is transient
Lecture one lung pathology 4 th year MBBS. Dr Asgher Khan Demonstrator of pathology Rawalpindi Medical College Rwp.
 Lecture one lung pathology 4 th year MBBS Dr Asgher Khan Demonstrator of pathology Rawalpindi Medical College Rwp. Expectation at end of lecture Brief review of anatomy and physiology related to lungs
Lecture one lung pathology 4 th year MBBS Dr Asgher Khan Demonstrator of pathology Rawalpindi Medical College Rwp. Expectation at end of lecture Brief review of anatomy and physiology related to lungs
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
Influenza (Flu) Influenza is a viral infection that may affect both the upper and lower respiratory tracts. There are three types of flu virus:
 Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
Quality of Birth Certificate Data. Daniela Nitcheva, PhD Division of Biostatistics PHSIS
 Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
NRP Study Guide. This packet is intended for review only. Requirements to successfully complete NRP:
 This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
Respiratory Emergencies. TEREM-APLS Course
 Respiratory Emergencies TEREM-APLS Course Case Study 1 Mother of 13-month-old boy found him choking and gagging next to container of spilled nuts. On arrival to register at TEREM, the following is noted:
Respiratory Emergencies TEREM-APLS Course Case Study 1 Mother of 13-month-old boy found him choking and gagging next to container of spilled nuts. On arrival to register at TEREM, the following is noted:
Update on Neonatal Resuscitation
 Update on Neonatal Resuscitation Ola Didrik Saugstad MD, PhD, FRCPE Professor of Pediatrics Director Department of Pediatric Research Rikshospitalet, Faculty of Medicine University of Oslo NORWAY 1st.
Update on Neonatal Resuscitation Ola Didrik Saugstad MD, PhD, FRCPE Professor of Pediatrics Director Department of Pediatric Research Rikshospitalet, Faculty of Medicine University of Oslo NORWAY 1st.
Using the ICD-10-CM. The Alphabetic Index helps you determine which section to refer to in the Tabular List. It does not always provide the full code.
 Using the ICD-10-CM Selecting the Correct Code To determine the correct International Classification of Diseases, 10 Edition, Clinical Modification (ICD-10-CM) code, follow these two steps: Step 1: Look
Using the ICD-10-CM Selecting the Correct Code To determine the correct International Classification of Diseases, 10 Edition, Clinical Modification (ICD-10-CM) code, follow these two steps: Step 1: Look
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
The Fetal Treatment Program
 CONGENITAL LUNG LESIONS* The Fetal Treatment Program *This information is intended to supplement your consultation with members of the Fetal Treatment Program regarding your unborn child with a suspected
CONGENITAL LUNG LESIONS* The Fetal Treatment Program *This information is intended to supplement your consultation with members of the Fetal Treatment Program regarding your unborn child with a suspected
11 Newborn Life Support
 11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
NEONATAL ABSTINENCE SYNDROME AND SCORING SYSTEM
 VIDANT MEDICAL CENTER PATIENT CARE _ SUBJECT: Abstinence Scoring NUMBER: A-1 PAGE: 1 OF: 5 _ NEONATAL ABSTINENCE SYNDROME AND SCORING SYSTEM POLICY: A thorough evaluation of the infant is required in order
VIDANT MEDICAL CENTER PATIENT CARE _ SUBJECT: Abstinence Scoring NUMBER: A-1 PAGE: 1 OF: 5 _ NEONATAL ABSTINENCE SYNDROME AND SCORING SYSTEM POLICY: A thorough evaluation of the infant is required in order
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Post - resuscitation management of an asphyxiated neonate
 Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
AHE: NRP AAP/AHA COURSE COMPONENTS
 ADVANCED HEALTHCARE EDUCATION 2011 6 TH EDITION - KEY POINT STUDY GUIDE IMPORTANT INFORMATION FOR STUDENTS REGISTERING FOR CLASSES AFTER 01/011/2012. AAP HAS RESTRUCTURED NRP TO NOW REQUIRE COMPLETION
ADVANCED HEALTHCARE EDUCATION 2011 6 TH EDITION - KEY POINT STUDY GUIDE IMPORTANT INFORMATION FOR STUDENTS REGISTERING FOR CLASSES AFTER 01/011/2012. AAP HAS RESTRUCTURED NRP TO NOW REQUIRE COMPLETION
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN
 MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
SAMPLE. UK Obstetric Surveillance System. Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery.
 ID Number: UK Obstetric Surveillance System Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery Case Definition: Study 04/11 Data Collection Form - Please report any woman delivering
ID Number: UK Obstetric Surveillance System Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery Case Definition: Study 04/11 Data Collection Form - Please report any woman delivering
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and
 What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography
 Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 ABSTRACT The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography Hussain Al Khawahur, MD* Hussain Al Sowaiket, MD** Thuria
Bahrain Medical Bulletin, Vol. 36, No. 2, June 2014 ABSTRACT The Pattern of Congenital Heart Disease among Neonates Referred for Echocardiography Hussain Al Khawahur, MD* Hussain Al Sowaiket, MD** Thuria
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Common Conditions, Concerns, and Equipment in the NICU
 Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
SAMPLE. Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management ICD-10
 Coding and Payment Guide www.optumcoding.com Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2017 a ICD10 A full suite of resources including
Coding and Payment Guide www.optumcoding.com Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2017 a ICD10 A full suite of resources including
ASSISTED VENTILATION IN NEONATES
 ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
Objectives COPD. Chronic Obstructive Pulmonary Disease (COPD) 4/19/2011
 Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES. Appendix 5 166
 APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Respiratory failure and Oxygen Therapy
 Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Neonatal Nurse Practitioner
 Neonatal Nurse Practitioner Your CE and NCC Maintenance Requirements TABLE OF CONTENTS 2 Your CE and the NCC Maintenance Process 3-4 Your NCC Education Plan 5 Common Coding Questions 6-9 Determining What
Neonatal Nurse Practitioner Your CE and NCC Maintenance Requirements TABLE OF CONTENTS 2 Your CE and the NCC Maintenance Process 3-4 Your NCC Education Plan 5 Common Coding Questions 6-9 Determining What
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Pregnancy and Substance Abuse
 Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
How To Determine The Difference Between Long Versus Short Inspiratory Times In Neonates
 Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Mechanical Ventilation
 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
The EMT Instructional Guidelines in this section include all the topics and material at the EMR level PLUS the following material:
 Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse
 Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
2008 Coding Questions and Answers
 2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
CPT Pediatric Coding Updates 2009. The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009.
 CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August 9, 2013
 Stony Brook Medicine Severe Sepsis/Septic Shock Recognition and Treatment Protocols Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August
Stony Brook Medicine Severe Sepsis/Septic Shock Recognition and Treatment Protocols Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August
Pulmonary interstitium. Interstitial Lung Disease. Interstitial lung disease. Interstitial lung disease. Causes.
 Pulmonary interstitium Interstitial Lung Disease Alveolar lining cells (types 1 and 2) Thin elastin-rich connective component containing capillary blood vessels Interstitial lung disease Increase in interstitial
Pulmonary interstitium Interstitial Lung Disease Alveolar lining cells (types 1 and 2) Thin elastin-rich connective component containing capillary blood vessels Interstitial lung disease Increase in interstitial
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Chapter 2 - Anatomy & Physiology of the Respiratory System
 Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Hospital-based SNF Coding Tip Sheet: Top 25 codes and ICD-10 Chapter Overview
 Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Priya Rajan, MD Northwestern University September 13, 2013
 Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Documenting & Coding. Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC
 Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Hyperbaric Oxygen Therapy WWW.RN.ORG
 Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
