Painful bladder syndrome/ interstitial cystitis (PBS/IC)
|
|
|
- Brianna Miles
- 7 years ago
- Views:
Transcription
1 Painful bladder syndrome/ interstitial cystitis (PBS/IC) Painful bladder syndrome/interstitial cystitis (PBS/IC) is a condition characterised by pelvic pain and urinary storage symptoms (eg, urinary urgency or the strong desire to pass urine and frequency, or going to the toilet often). It is very important to realise that PBS/IC is a condition or group of conditions that are still poorly defined, and inflammation is an important feature in only a small number (<20%) of patients. This group is considered to have interstitial cystitis (IC) or a special type of chronic inflammation of the bladder, whereas PBS refers to pain felt in the bladder region. IC, as opposed to PBS is a chronic bladder problem with associated inflammation. People with IC have a bladder wall that is inflamed and irritated (red and sore). This inflammation can scar the bladder or make it stiff. A stiff bladder can't expand as urine fills it. There may be pinpoint bleeding from the walls of the bladder. A few people get sores in the bladder lining. American Urological Association guidelines recently provided a modified definition for the diagnosis and treatment of PBS/ IC: An unpleasant sensation (pain, pressure, discomfort) perceived to be related to the urinary bladder, associated with lower urinary tract symptom(s) of more than 6 weeks duration, in the absence of infection or other identifiable causes What causes PBS/IC? There is no general agreement about the cause of PBS/IC and many theories have been proposed including involvement of inflammatory cells or mast cells that release histamine or having a lining of the bladder which allows some of the urine to permeate or leak into the surface as normally the lining protects the bladder wall from the toxic effects of urine. In about 70 percent of people with IC, the protective layer of the bladder is "leaky." This may let urine irritate the bladder wall, causing IC. There may be problems with function of the local nerves, pelvic floor muscle function and tension, an autoimmune condition (when antibodies are made that act against a part of the body) or the possibility of an as yet unidentified infective cause. The lack of clear reason for PBS/IC to develop and the troublesome symptoms it causes make it a very frustrating condition for patients to understand and manage. Treatment and management approaches vary widely because the condition is complex, we don t have a definite way to diagnose it and the cause is not understood. What are the features of PBS/IC? The condition for most patients has a relatively quick onset, which is unusual in for a chronic condition. Many patients can tell you the day symptoms began. Symptoms will not usually progress but will often reach their final stage rapidly and continue without significant change in
2 the future. The commonest age of onset is around 40 years old but 30% are less than 30 years old. About half of patients will experience spontaneous remission for anywhere between a short period of a month and much longer, even up to years. Patients with PBS/IC are times more likely to have had childhood bladder problems than the unaffected population and are twice as likely to report a history of urinary tract infection. There are many associations with PBS/IC, these include allergies, irritable bowel syndrome, fibromyalgia, some autoimmune conditions, migraine and chronic fatigue. Symptoms in PBS/IC may include an urgent need to urinate, both in the daytime and during the night, a frequent need to urinate; women with severe cases of IC may urinate as many as 60 times a day. Pressure, pain and tenderness around the bladder, pelvis and perineum (the area between the anus and vagina or back of the scrotum) may be a feature. This pain and pressure may increase as the bladder fills and decrease as it empties in urination. A bladder that won't hold as much urine as it did before and pain during sexual intercourse or orgasm may be symptoms. The symptoms of IC vary from case to case and even in the same individual. Stress may also make the symptoms worse, but it doesn't cause them. How is PBS/IC diagnosed? How do I know I have it? You may have PBS/IC if you have symptoms of urinating often or urgently, pelvic or bladder pain, finding bladder wall inflammation, pinpoint bleeding or ulcers during an exam with a special scope (called a cystoscope) that looks inside your bladder. Your doctor has had to also rule out other diseases such as urinary tract infections, vaginal infections, bladder cancer or sexually transmitted diseases. Diagnostic tests that help identify other conditions include urinalysis, urine culture, cystoscopy, biopsy of the bladder wall, distension of the bladder under anaesthesia and urine cytology. How is PBS/IC treated? There are many different types of behavioural, dietary, pharmacologic (drug), and surgical treatments that have been used. The Interstitial Cystitis Data Base study reported on more than 180 different treatment modalities which is why if you search using the internet there can be both a baffling quantity and very varying quality of unfiltered information available. Hopefully this document will give you a good starting point and cover most of the information you will need to manage you condition better. If you use the internet, be sure to question what you are reading and where it came from before reaching conclusions about your diagnosis or treatment. 2
3 Because the causes of PBS/IC are unknown, current treatments are aimed at relieving symptoms. One or a combination of treatments helps most people for variable periods. As researchers learn more about PBS/IC, the list of potential treatments will change, so patients should discuss their options with a doctor. Most people feel better after trying one or more of the following treatments: 1. Diet: Your doctor may tell you to change what you eat. You may need to avoid alcohol, acidic foods and tobacco. 2. Physiotherapy Many patients with PBS/IC have tight and tender muscles and connective tissue in the pelvis, lower abdomen, thighs, groin, and buttocks. Tight muscles and connective tissue can be diagnosed during a physical examination. Physiotherapy may be recommended to decrease tightness in these muscles. Physio can decrease bladder or pelvic pain as well as urinary urgency and frequency. This type of physio is quite different from that intended to treat a knee injury or back pain, which usually works to increase muscle strength. With pelvic floor physiotherapy, you lie flat as the physio works on your body to manually "release" the tightness, tender points, trigger points, and restricted movement of the connective tissues and muscles. This includes the muscles and tissues of the vagina or rectum, abdomen, hips, thighs, and lower back. Physiotherapists perform this type of treatment must be specially trained in pelvic soft tissue manipulation and rehabilitation. Several small studies have demonstrated the benefit of physiotherapy for tight and tender pelvic muscles associated with painful bladder syndrome/interstitial cystitis. One study reported that 70 percent of interstitial cystitis patients who were treated with manual physical therapy to the pelvic floor tissues for 12 to 15 visits experienced moderate to marked improvement. 3. Bladder distension: Sometimes people feel better after having a bladder distension or hydrodilatation. Under anaesthesia, a doctor overfills your bladder with fluid. This stretches the walls of the bladder. Doctors don't know why distension helps. It may make your bladder be able to hold more urine. It may also interfere with pain signals sent by nerves in the bladder. Often as a part of the diagnostic process this is done at the cystoscopy to ensure there are no other pathologies present. 3
4 4. Medication: Your doctor may have you take an oral medicine called pentosan polysulfate (brand name: Elmiron). This medicine helps to protect the lining of the bladder wall from the toxic parts of urine. Elmiron is not on the PBS and is expensive. It helps about 40% of patients. Another medicine that may help is amitriptyline (brand name: Endep). It blocks pain and reduces bladder spasms. This medicine can make you sleepy, so it's usually taken at bedtime. Some patients find antihistamines (such as Zyrtec) helpful. Each medication should be treid for a period on its own to assess its true effect. Sometimes referral to a Pain Specialist is advised to access more complex medicines which are aimed at the nerve aspects of pain more directly. 5. Bladder instillation: During a bladder instillation, a catheter (a thin tube) is used to fill your bladder with a liquid medicine. You hold the medicine inside your bladder for a few seconds to 15 minutes. Then the liquid drains out through the catheter. Treatments are given every one to two weeks for six to eight weeks. The treatment can be repeated as needed. The substances used include a mixture of local anaesthetic, steroids and heparin that reduce inflammation and may help the lining of the bladder and Dimethyl sulfoxide or DMSO (Rimso-50), a chemical solvent from wood pulp which has several uses in medicine. It is known to reduce inflammation and block pain in about a third of IC patients. A further agent, Clorpactin can be given under anaesthesia as an instillation for pain. For instillations to be effective you generally need to have a reduced capacity to store urine and some inflammatory changes on inspection or cystoscopy. Difficult Cases An extremely small minority of patients are not helped with regular treatments and require surgery. Many approaches and techniques are used, each of which have their own advantages and complications that should be discussed with a surgeon. Surgery should be considered only if all available treatments have failed and the pain is disabling. Most doctors are reluctant to operate because the outcome is unpredictable and some people still have symptoms after surgery. 4
5 What else can I do to help my symptoms? 1. Diet - Alcohol, tomatoes, spices, chocolate, caffeine, citrus drinks, artificial sweeteners and acidic foods may irritate your bladder. That makes your symptoms worse. Try removing these foods from your diet for a couple of weeks. Then try eating one food at a time to see if it makes your symptoms worse. 2. Smoking - Many people with PBS/IC find that smoking makes their symptoms worse. Because smoking is also a main cause of bladder cancer, people with interstitial cystitis have another good reason to quit smoking. 3. Bladder training - Many people can train their bladder to urinate less often. You can train your bladder by going to the bathroom at scheduled times and using relaxation techniques. After a while, you try to make the time you can wait longer. Your physiotherapist can help you with bladder training and relaxation techniques. 4. Physical therapy and biofeedback - People with PBS/IC may have painful spasms of the pelvic floor muscles. If you have muscle spasms, you can learn exercises to help strengthen and relax your pelvic floor muscles. 5. TENS (this stands for "transcutaneous electrical nerve stimulation"). You can use a TENS machine to put mild electrical pulses into your body through special wires. You would do this at least two times a day. You might do it for a few minutes, or you might do it for a longer time. Some doctors think that electric pulses increase blood flow to the bladder. The increased blood flow strengthens the muscles that help control the bladder. It also releases hormones that block pain. TENS is not expensive. 6. Supportive therapy and psychology Whist stress is not know to cause PBS/IC, it can be worsened by stress, anxiety, depression, and other psychological factors. In addition, living with pain can cause difficulties in relationships, at work or school, and with general day to day living. Psychosocial support can be helpful in dealing with these issues. Psychosocial support is not recommended because a person with painful bladder syndrome/interstitial cystitis is "crazy" or "difficult". Rather, it is recommended to address the stress, anger, or frustration that can develop as a result of frequent or chronic pain. Depression is common in people with chronic pain, and can interfere with the success of any treatment regimen. Therefore, evaluation and treatment of depression is recommended, if needed. Relaxation techniques can also relieve musculoskeletal tension, and may include meditation, progressive muscle relaxation, self-hypnosis, or biofeedback. 5
6 I work with particular psychologists who I recommend and are experienced in seeing these types of issues. Where can I get more information about PBS/IC? The support of family, friends and other people with PBS/IC is very important to help you cope with this problem. People who learn about PBS/IC and participate in their own care do better than people who don't. Support groups exist in Australia and can be accessed via most large hospital urology or urogynaecology departments. Please discuss this with the urology nurses if you would like more information. Please remember that only a minority of patients will have true interstitial cystitis and most with PBS respond well to physiotherapy and lifestyle changes, occasionally requiring a bladder stretch or medication. Websites for further information: (including some of the information contained in this document) Interstitial Cystitis Network (Australia) Interstitial Cystitis Association Up to Date and request EAU guidelines on Chronic Pelvic Pain 6
Painful Bladder Syndrome and Interstitial Cystitis
 Painful Bladder Syndrome and Interstitial Cystitis PAINFUL BLADDER AND INTERSTITIAL CYSTITIS OVERVIEW Painful bladder syndrome/interstitial cystitis (PBS/IC) is a disorder with symptoms of mild to severe
Painful Bladder Syndrome and Interstitial Cystitis PAINFUL BLADDER AND INTERSTITIAL CYSTITIS OVERVIEW Painful bladder syndrome/interstitial cystitis (PBS/IC) is a disorder with symptoms of mild to severe
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
URINARY INCONTINENCE
 URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
I can t empty my rectum without pressing my fingers in or near my vagina
 Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
The Well Woman Centre. Adult Urinary Incontinence
 The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
How to Improve Bladder After Bowler Cancer
 Bladder changes after bowel cancer treatment This information is from the booklet Managing the late effects of bowel cancer treatment. You may find the full booklet helpful. We can send you a free copy
Bladder changes after bowel cancer treatment This information is from the booklet Managing the late effects of bowel cancer treatment. You may find the full booklet helpful. We can send you a free copy
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
Urinary Incontinence. Patient Information Sheet
 Urinary Incontinence Patient Information Sheet What is urinary incontinence (UI)? UI happens when you are not able to control when you urinate and you wet yourself. How common is urinary incontinence?
Urinary Incontinence Patient Information Sheet What is urinary incontinence (UI)? UI happens when you are not able to control when you urinate and you wet yourself. How common is urinary incontinence?
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Overview of Urinary Incontinence in the Long Term Care Setting
 Overview of Urinary Incontinence in the Long Term Care Setting Management Strategies for the Nursing Assistant Ann M. Spenard RN, C, MSN Courtney Lyder ND, GNP Learning Objectives Describe common types
Overview of Urinary Incontinence in the Long Term Care Setting Management Strategies for the Nursing Assistant Ann M. Spenard RN, C, MSN Courtney Lyder ND, GNP Learning Objectives Describe common types
Urinary Incontinence
 Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Learning Resource Guide. Understanding Incontinence. 2000 Prism Innovations, Inc. All Rights Reserved
 Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
es of Urinary Incontinence:
 Reversible Cause Urinary incontinence is a loss of control over the passing of urine. Urine loss can occur in very small amounts (enough only to dampen underwear) to very large amounts (requiring a change
Reversible Cause Urinary incontinence is a loss of control over the passing of urine. Urine loss can occur in very small amounts (enough only to dampen underwear) to very large amounts (requiring a change
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Bladder Control Does Matter
 Bladder Control Does Matter Y0028_2726_0 File&Use 04092012 If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Bladder Control Does Matter Y0028_2726_0 File&Use 04092012 If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
International Painful Bladder Foundation IPBF. Interstitial Cystitis/Bladder Pain Syndrome, Hypersensitive Bladder, Hunner Lesion
 IPBF Interstitial Cystitis/Bladder Pain Syndrome, Hypersensitive Bladder, Hunner Lesion What is it? How is it diagnosed? How is it treated? How do you cope with it? www.painful-bladder.org March 2016 1
IPBF Interstitial Cystitis/Bladder Pain Syndrome, Hypersensitive Bladder, Hunner Lesion What is it? How is it diagnosed? How is it treated? How do you cope with it? www.painful-bladder.org March 2016 1
FUNCTIONAL BOWEL DISORDERS
 FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Patient Questionnaire for Men
 Patient Questionnaire for Men Please fill out the following questionnaire to the best of your ability prior to your first appointment. Your physical therapist will review your responses during your initial
Patient Questionnaire for Men Please fill out the following questionnaire to the best of your ability prior to your first appointment. Your physical therapist will review your responses during your initial
Managing Changes in Your Bladder Function After Cancer Treatment
 Managing Changes in Your Bladder Function After Cancer Treatment Information for cancer survivors UHN Read this resource to learn: What a urinary problem is What causes it What you can do to improve your
Managing Changes in Your Bladder Function After Cancer Treatment Information for cancer survivors UHN Read this resource to learn: What a urinary problem is What causes it What you can do to improve your
Drinking fluids and how they affect your bladder
 Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS. Ask a member of
Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS. Ask a member of
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
Endometriosis: An Overview
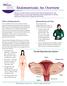 Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Endometriosis
 Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Tone Up Your Pelvic Floor. A regular pelvic floor exercise ( Kegel ) routine can prevent symptoms before, during, and after childbirth.
 Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Urinary Incontinence Definitions
 (AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
(AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
Saint Mary s Hospital. Gynaecology Service Warrell Unit. Overactive Bladder. Information for Patients
 Saint Mary s Hospital Gynaecology Service Warrell Unit Overactive Bladder Information for Patients What is Overactive Bladder (OAB)? OAB is a condition that causes you to need to pass urine more often
Saint Mary s Hospital Gynaecology Service Warrell Unit Overactive Bladder Information for Patients What is Overactive Bladder (OAB)? OAB is a condition that causes you to need to pass urine more often
Acute pelvic inflammatory disease: tests and treatment
 Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Urinary Incontinence. Types
 Urinary Incontinence Leakage of urine is called urinary incontinence. It is a common problem in women. Some women occasionally leak small amounts of urine. At other times, leakage of urine is frequent
Urinary Incontinence Leakage of urine is called urinary incontinence. It is a common problem in women. Some women occasionally leak small amounts of urine. At other times, leakage of urine is frequent
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Empower Physical Therapy
 PAYMENT AND COLLECTION POLICY Payment is expected at the time of service. Unpaid balances left by your insurance companies will be your responsibility. In the event you are unable to pay the balance in
PAYMENT AND COLLECTION POLICY Payment is expected at the time of service. Unpaid balances left by your insurance companies will be your responsibility. In the event you are unable to pay the balance in
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Overactive bladder syndrome (OAB)
 Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form
 Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
Dr. Kenneth A. Giraldo, MD, P.A. Patient Controlled Substance Agreement Informed Consent Form The following agreement relates to my use of controlled substance for chronic pain prescribed by Dr. Kenneth
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY
 BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use.
 Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE
 VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Managing Acute Side Effects of Colorectal & Anal Radiation Therapy
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Colorectal & Anal Radiation Therapy In this booklet you will learn about: Common side effects when you receive radiation therapy to your
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Colorectal & Anal Radiation Therapy In this booklet you will learn about: Common side effects when you receive radiation therapy to your
Urinary Incontinence. Causes of Incontinence. What s Happening?
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
Patient Information Incontinence & Prolapse Self Help
 Patient Information Incontinence & Prolapse Self Help Urogynaecology Introduction This leaflet is produced as a self help guide for women of East and North Herts that are experiencing issues with continence.
Patient Information Incontinence & Prolapse Self Help Urogynaecology Introduction This leaflet is produced as a self help guide for women of East and North Herts that are experiencing issues with continence.
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH)
 GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Treatment for Stress Incontinence Patient Decision Aid
 Treatment for Stress Incontinence Patient Decision Aid Patient Information Author ID: JD/NS Leaflet Number: Gyn 056 Version: 1 Name of Leaflet: Treatment for stress incontinence - Patient decision aid
Treatment for Stress Incontinence Patient Decision Aid Patient Information Author ID: JD/NS Leaflet Number: Gyn 056 Version: 1 Name of Leaflet: Treatment for stress incontinence - Patient decision aid
After pelvic radiotherapy
 After pelvic radiotherapy in women 1 After pelvic radiotherapy in women This information is from the booklet Pelvic radiotherapy in women managing side effects during treatment. You may find the full booklet
After pelvic radiotherapy in women 1 After pelvic radiotherapy in women This information is from the booklet Pelvic radiotherapy in women managing side effects during treatment. You may find the full booklet
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Erectile Dysfunction (ED)
 Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
A Physical Therapist s Perspective
 You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
Abdominal Wall Pain. What is Abdominal Wall Pain?
 Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant
 Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant Goal of the Procedure Brachytherapy, or internal radiation therapy, is a way of giving a higher dose of radiation to the tumor area while
Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant Goal of the Procedure Brachytherapy, or internal radiation therapy, is a way of giving a higher dose of radiation to the tumor area while
Why is radiation therapy used to treat prostate cancer? Is there anything that I have to do before my treatment planning appointment?
 2015 Information for Patients Receiving Radiation Therapy: External Beam Treatment for Prostate Cancer Why is radiation therapy used to treat prostate cancer? Prostate cancer may be treated with a combination
2015 Information for Patients Receiving Radiation Therapy: External Beam Treatment for Prostate Cancer Why is radiation therapy used to treat prostate cancer? Prostate cancer may be treated with a combination
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear
 Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
Endometriosis. Information and advice. Page 12 Patient Information
 Endometriosis Information and advice Page 12 Patient Information Contents page What is Endometriosis?... page 3 Symptoms page 5 Treatments.. page 7 Further information and support.. page 9 Contact us page
Endometriosis Information and advice Page 12 Patient Information Contents page What is Endometriosis?... page 3 Symptoms page 5 Treatments.. page 7 Further information and support.. page 9 Contact us page
Radiotherapy for vulval cancer
 This information is an extract from the booklet Understanding cancer of the vulva. You may find the full booklet helpful. We can send you a copy free see page 6. Contents External radiotherapy Internal
This information is an extract from the booklet Understanding cancer of the vulva. You may find the full booklet helpful. We can send you a copy free see page 6. Contents External radiotherapy Internal
Patient Guide. Sacroiliac Joint Pain
 Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Stress Urinary Incontinence
 Saint Mary s Hospital Gynaecology Service Warrell Unit Stress Urinary Incontinence Information for patients What is Stress Incontinence? Stress incontinence is a leakage of urine occurring on physical
Saint Mary s Hospital Gynaecology Service Warrell Unit Stress Urinary Incontinence Information for patients What is Stress Incontinence? Stress incontinence is a leakage of urine occurring on physical
FROZEN SHOULDER OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU. Frozen Shoulder FROZEN SHOULDER
 OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Uterine fibroids (Leiomyoma)
 Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate)
 Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
GreenLight laser prostatectomy
 Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Spinal cord stimulation
 Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Information for Patients
 Notes Information for Patients Sling procedure for urinary stress incontinence Aysha Qureshi Version 1, June 2010 Review date June 2013 Date of publication: June 2010 Ref: RUH GYN/002 Royal United Hospital
Notes Information for Patients Sling procedure for urinary stress incontinence Aysha Qureshi Version 1, June 2010 Review date June 2013 Date of publication: June 2010 Ref: RUH GYN/002 Royal United Hospital
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Botox (Botulinum Toxin) injections into the bladder
 York Teaching Hospital NHS Foundation Trust Botox (Botulinum Toxin) injections into the bladder Information for patients, relatives and carers Department of Urology York Teaching Hospital NHS Foundation
York Teaching Hospital NHS Foundation Trust Botox (Botulinum Toxin) injections into the bladder Information for patients, relatives and carers Department of Urology York Teaching Hospital NHS Foundation
Problems of the Digestive System
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
Concentrated Oral Aloe Vera for Alleviating IC Symptoms A White Paper
 Concentrated Oral Aloe Vera for Alleviating IC Symptoms A White Paper A survey was sent to approximately 20,000 individuals who have taken Aloe Vera, primarily for interstitial cystitis (IC). A total of
Concentrated Oral Aloe Vera for Alleviating IC Symptoms A White Paper A survey was sent to approximately 20,000 individuals who have taken Aloe Vera, primarily for interstitial cystitis (IC). A total of
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Vesico-Vaginal Fistula
 Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system.
 Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Bladder and Pelvic Health
 A Woman s Guide to Bladder and Pelvic Health Symptoms Tests Conditions Treatments 937-277-8988 1-888-808-1016 Dayton Center Englewood Center Huber Heights Center Trotwood Satellite Table of Contents About
A Woman s Guide to Bladder and Pelvic Health Symptoms Tests Conditions Treatments 937-277-8988 1-888-808-1016 Dayton Center Englewood Center Huber Heights Center Trotwood Satellite Table of Contents About
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Please read these instructions carefully before using Poise* Bladder Supports
 For the Temporary Management of Stress Urinary Incontinence in Women INSTRUCTIONS FOR USE Please read these instructions carefully before using Poise* Bladder Supports 500000023088 For the Temporary Management
For the Temporary Management of Stress Urinary Incontinence in Women INSTRUCTIONS FOR USE Please read these instructions carefully before using Poise* Bladder Supports 500000023088 For the Temporary Management
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Managing Acute Side Effects of Prostate Radiation Therapy
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Prostate Radiation Therapy In this booklet you will learn about: Common side effects when you receive radiation therapy to your prostate
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Prostate Radiation Therapy In this booklet you will learn about: Common side effects when you receive radiation therapy to your prostate
Stress incontinence in Women
 Stress incontinence in Women Exceptional healthcare, personally delivered Operations for Stress Incontinence Introduction Stress incontinence is a medical word used to describe the type of leakage that
Stress incontinence in Women Exceptional healthcare, personally delivered Operations for Stress Incontinence Introduction Stress incontinence is a medical word used to describe the type of leakage that
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact

 Full version is >>> HERE
Full version is >>> HERE