Dynamic Gait Index (DGI)/Functional Gait Assessment (FGA)
|
|
|
- Lucy Brown
- 9 years ago
- Views:
Transcription
1 DYNAMIC GAIT INDEX (DGI)/FUNCTIONAL GAIT ASSESSMENT (FGA) Type of test: Time to administer: 15 minutes Clinical Comments: Familiarity with the ordinal scoring system prior to administering test as important, as scoring system varies among items. Standardized instructions seem cumbersome. Purpose/population for which tool was developed: The Dynamic Gait Index (DGI) was developed as part of a profile for predicting likelihood of falls in older adults. The tool was presented in 1993 as a way to assess and document a patient s ability to respond to changing task demands during walking. 1, 2 The 8 items vary the walking task by changing walking speeds, adding head turning, turning and stopping, walking over and around obstacles, and ascending / descending stairs. Scoring focuses on changes in balance or changes in gait patterns during the various walking tasks. A shortened DGI was developed based on Rasch analysis of level of item difficulty for 123 persons with diagnosed balance or vestibular problems. It contains 4 items: horizontal head turns, vertical head turns, gait on level surfaces, and changes in gait speed; the shortened version has equivalent or superior psychometric properties compared to the 8 item version. 3 When appropriate to use: This tool has been used with older adults with a history of falls and imbalance, 1-5 patients with bilateral vestibular loss, 6 patients with vestibular dysfunction with & without migraine headaches, 7-10 patients with chronic stroke, 11 Parkinson Disease 12 multiple sclerosis, 13 and essential tremor. 14 Scaling: Each of the 8 items is scored from 0 3, on an ordinal scale, with the best possible total equal to 24 and the worst score equal to zero. The Rasch measurement model, applied to data on 84 community-dwelling male veterans, showed that the 4-point rating scale appeared to distinctly identify subjects at different ability levels. 15 The 4 item version is scored Equipment needed: Scoring form level walking area at least 20 feet in length stopwatch shoe box 2 cones (to serve as obstacles in walking pathway) stairs with railing Directions: Instructions for each item are included on the scoring form (attached). In 84 community dwelling male veterans, Rasch measurement model analysis showed that the most difficult items were gait with horizontal head turns, steps, and gait with vertical head turns ; the easiest items were gait on level surfaces, change in gait speed, and step around obstacles. Clinicians may want to consider changing the order of test administration (from easiest to most difficult) especially in clients with severe impairment. 15 Reliability: Reference N = Sample Description Reliability Statistic Intrarater Reliability: same rater within one session (or one day) Wolf, Adults (over age 75) with impaired balance; physical therapist raters were trained in a ICC=.98 standardized test protocol and practiced this protocol before data collection. McConvey, Patients with multiple sclerosis; 11 Physical ICC=.76 to.986 therapist raters watching videotaped gait Interrater Reliability: Wolf, Adults with impaired balance over age 75; physical therapist raters were trained in a standardized test protocol and practiced this protocol before data collection. ICC=.99 Tests and Measures: Adult; 2012 DGI Page 1
2 Shumway Cook, Community-dwelling older adults with varying balance abilities; 5 physical therapist raters..96 to 1.00 (ratio of subject variability to total variability) ICC =.983 McConvey, Patients with multiple sclerosis; 11 Physical therapist raters watching videotaped gait Marchetti, Adults in tertiary-care setting, test and control; 6.54 to.80 Kappa paired physical therapist raters on 8 item version. Internal Consistency: how items in a scale relate to each other and to the group of items as a whole Marchetti, of the subjects had known balance Chronbach s alpha disorders; 103 subjects were controls without 8 item version: 0.92 balance or vestibular dysfunction. All were 4 item version: 0.89 community dwellers. Chiu, Community-dwelling male veterans (mean age Person separation = 75) reliability.80 Test-Retest Reliabilty Hall, Adults with peripheral vestibular ICC (3,1) =.86 disorders,(same day, same raters). Validity: Construct / Concurrent Validity: It is difficult to always differentiate between these 2 types of validity. Evaluating this property requires a gold standard measure with which to compare the tests results. Such a gold standard is often not available. Population N = Support for Validity Communitydwelling older adults with and without hx of falls Patients with unilateral vestibular dysfunction (retrospective review) 105 DGI is correlated with: the Berg Balance Scale (BBS) (0.67), with a balance self-perceptions test (0.76), with use of an assistive device ( -0.44), and with a history of imbalance (-0.46) DGI scores correlated with: ABC scale for persons with mild moderate vestibular weakness (0.72); ABC scale for persons with severe vestibular weakness (0.48). 17 Multiple sclerosis 10 DGI scores correlated inversely with: time to walk six meters (-0.80) 16 Persons with and 81 (with balance DGI scores correlated inversely with 5-timed-sit-to-stand test scores (- without balance or disorders) 0.68). 18 vestibular disorders (retrospective review) 93 (without balance disorders) Persons with vestibular disorders (Age range 14 88, mean=65) Persons with vestibular dysfunction (Mean age = 64) (retrospective review) Multiple Sclerosis (Mean age = 45) 32 DGI correlates with Gait speed (0.82) measured as time to walk 11 meters, inversely with Four Square Step Test (-0.51), inversely with Timed Up and Go (TUG) (-0.56) DGI correlates with BBS (0.71) DGI correlates with BBS (0.78), ABC (0.54) and inversely with TUG (0.72) Dizziness Handicap Index (DHI) (-0.39), and Deambulation Index (0.8). 13 Tests and Measures: Adult; 2012 DGI Page 2
3 Predictive Validity Population N = Results Communitydwelling older adults, with and without history of falls. Persons with vestibular dysfunction with history of migraines Persons with vestibular disorders Independent communitydwelling older adults (Mean age = 74) Unilateral vestibular hypofunction (Ages years old) Patients with dizziness, with or without selfperceived unsteadiness. Patients with variety of vestibular disorders. (Mean age = 61) (retrospective review) Self-reported fallers with vestibular dysfunction (retrospective review) Persons with essential tremor, with and without head tremor Sensitivity/specificity: Population Identifying fallers vs nonfallers in persons with Parkinson s Disease 44 DGI score was not a significant risk factor in a logistic regression model for falls. The Berg Balance Scale and history of imbalance were significant risk factors in this model for falls The DGI score is included in an overall score of disability, calculated as follows: 100 x / 296; where ABC equals the score on the Activities Specific Balance Confidence; DHI equals the score on the Dizziness Handicap Inventory; and DGI equals the score on the Dynamic Gait Index. The maximum possible score is 100, with the following disability interpretation by the authors: > 91 No impairment Minimal impairment Moderate impairment <40 Severe Impairment Persons with DGI 19 were 2.58 times more likely to report falls in previous 6 months than persons with scores > 19/ DGI scores were not predictive of falls within 1 year following testing Initial DGI scores along with DVA scores (Dynamic Visual Acuity) were significant factors in a regression model for predicting fall risk reduction at discharge (sensitivity of the model = 77%) Average DGI scores were not significantly different between patients with dizziness who perceived themselves to the unsteady vs. those who felt steady Mean DGI scores were significantly different between persons with mild or moderate dizziness handicap scores compared to those with severe handicap scores (p<.05) Persons with DGI score 18 were 2.7 times more likely to have reported a fall in the previous 6 months than those with scores > 18/24 (p =.03) DGI scores significantly different between controls and persons with ET with and without head tremor (Kruskal-Wallis p =.009) and between control group and ET group with head tremor (Mann-Whitney U p =.002) 14 N = Cutoff Score and Description Results 45 Cutoff score < 19 Sensitivity (57%) Specificity (90%) Cutoff score < Sensitivity (89%)Specificity(48%) Tests and Measures: Adult; 2012 DGI Page 3
4 Identifying fallers vs. nonfallers Identifying persons with balance dysfunction Identifying persons with balance or vestibular disorders Persons with balance or vestibular disorder who reported a fall in previous 6 months Identifying fallers vs nonfallers in persons with multiple sclerosis 44 Cutoff score equal or less than 19: (adults over 65) Cutoff score 22 (young and older adults, with or without balance disorders) Cutoff score <12 (on 4 Item DGI ) of adults with mean age 56.7 with or without balance disorders Cutoff score < 19 (on 8 Item) Cutoff score < 9 (4 Item) Adults with mean age Sensitivity (59%); Specificity (64%) BBS was shown to have greater sensitivity and specificity than DGI in the same study. Sensitivity (82%) Specificity (88%) Sensitivity (85%) Specificity (74%) The AUC for 8-item DGI was.89 with cutoff score <24, for 4-item DGI was.87 showing similar sensitivity and specificity. Sensitivity (68%), Specificity (60%) Sensitivity (56%), Specificity (62%) 51 Cutoff score < Sensitivity (45%) Specificity (80%) BBS, using a cutoff score of 44, was shown to have less sensitivity but more specificity than DGI in the same study Responsiveness/Sensitivity to change: Population Descriptor N= Reference and Intervention Responsive Yes/No VESTIBULAR DYSFUNCTIONS Patients with 62 Wrisley, Yes vestibular Hx of Rx: Physical Therapy, mean dysfunction migraines of 4 visits (N=31 ) No hx /migraines Diagnosis of Bilateral vestibular disorder Central vestibular dysfunction Unilateral vestibular hypofunction Patients seen for vestibular and balance rehab Patients with vestibular disorders (chronic dizziness) (N=31) 24 Brown, Rx: customized PT (mean visits = 4.6) 48 Brown, Rx: Customized PT (Mean visits = 5) 47 Hall, Rx: vestibular rehabilitation 20 (mean age = 65) Badke, Rx: customized exercise program; (1-20 visits) 43 Meli, Rx: vestibular rehabilitation, 2 hrs, 12 sessions, plus home exercise program (HEP) 2x/day. Yes Yes Yes Yes Ave. change after intervention Group differences significant? Mean change after Rx: With Migraines = +4 (p<.001) Without Migraines = +4 (p =.001) Mean change after Rx: +4 (p =.005) Mean change after Rx: +3.8 (p<.01) Group showed significant increases in DGI after Rx (p <.001) Mean change after Rx: +4.4 (p<.01) Yes? Mean before Rx = (2.12) Mean after Rx = (1.44) Before Rx: 25% of pts scored 19/24; After Rx:0 scored 19/24 Tests and Measures: Adult; 2012 DGI Page 4
5 Diagnosis of BPPV: Benign paroxysmal positional vertigo Patients with chronic stroke Adults over 75 with impaired balance Physically inactive older adults Adults, inactive, community-living 88 overall 22 tested with DGI Dannenbaum, Rx: Vestibular rehabilitation program, VRP, consisting of modified Epley, Semont, Brandt-Daroff, or log roll repositioning exercises + eye-head and balance exercises + HEP GENERAL BALANCE DYSFUNCTIONS 8 Fritz, Rx: 3 hours CIMT for 10 consecutive workdays, 1:1 with DPT student 94 Experimental Grp: (N=37) Control Group: (N=40) Wolf, Experimental Group: Individualized balance program, x12 Control Group: Individualized extra attention, 12 visits Yes Mean before Rx: 18.4 (3.2) COMMUNITY-LIVING, SEDENTARY Yes After Rx: 256 Li, Length/frequency/Intens ity 60 min sessions, 3x/wk for 6 months Experimental (N=125): Tai Chi Control (N=131): Exercise stretching 256 (mean age = 77) Li, x/week x 6 months w/instructor Control group, n=131 stretching classes Intervention group, n=125 Yang Tai Chi classes Mean after Rx:22.6(1.7) (p<.01, t-test) Yes Mean baseline = 10.3 (3.1) Mean after Rx = 14.3 (4.9) Yes Mean change after Rx: Experimental = +4 Control = Between group differences = (p <.001) Control showed no change in score; Tai Chi grp showed increase (p<.001) 6 mo post intervention follow-up: Tai Chi grp showed less decline (p=.05) Yes Baseline: Control 19.76(2.89) Rx: 19.40(2.48) 6 mos: Control 20.12(3.07) P<.001 Rx: 21.43(2.62) 12 mos follow-up: 19.47(3.24) P<.05 Rx : 21.10(2.68) Significant change with Rx on analyses of repeated measures; no significant change in control group Ceiling or floor effect: Persons need to be able to ambulate at least 20 feet in order to be tested with the DGI, thus it would not be appropriate for very low functioning patients. Ceiling effects of 7.8% - 72% have been reported in 3, 13, 14 combined test and control subjects by several authors. Interpreting results: The score of this Index has been interpreted as a measure of functional balance during walking. Scores equal to or less than 19 (of 24) are associated with an increased risk of falling. 1 The test appears to be responsive to showing change after intervention in persons with vestibular disorders and older adults with impaired balance. Tests and Measures: Adult; 2012 DGI Page 5
6 Reference Data: Young and older adults, with or without balance disorders based on vestibular testing 18 Subjects N DGI Scores Mean (SD) 95% CI Young controls (Mean age = 41; range 23-57) (.3) Older controls (Mean age = 73; range 63-84) (1.7) Young, with balance disorder (Mean age = 48; range 14-59) (4.4) Older, with balance disorder (Mean age = 75, range 61-90) (5.1) Younger adults, with surgical excision of schwannoma or matched healthy controls 31 Mean 14 months after schwannoma removal, no physical therapy (Mean age = 52, range 43-57) (0.8) Difference from control ( ) Controls (Mean age 52, range 43-57) (0.2) Other: To avoid ceiling effect a modified version of the DGI, called the Functional Gait Assessment (FGA) was created 32 and reference data established. 33 The FGA uses 7 of the 8 tasks of the DGI (eliminates walking around the obstacle) plus adds 3 items and specifies a standardized surface (Gait Grid ). Risk for falls is suggested to be < or = to 22/30 in a 6 month prospective cohort study of 35 older adults aged 60 to 90. This score provided a100% sensitivity, 72% specificity, LR+ of 3.6 and LR- of 0 to predict prospective falls. 34 Walker, M.L. (2007). Reference Group Data for the Functional Gait Assessment. Physical Therapy (87)11, References: 1. Shumway Cook A, Baldwin M, Polissar N, Gruber W. Predicting the probability for falls in communitydwelling older adults. Phys Ther 1997;77: Shumway Cook A. Motor control: Theory and practical applications. Baltimore: Williams & Wilkins; Binder Marchetti G, Whitney S. Construction and validations of the 4-item dynamic gait index. Phys Ther 2006;86(12): Shumway Cook A, Gruber W, Baldwin M, Liao S. The effect of multidimensional exercises on balance, mobility, and fall risk in community-dwelling older adults. Phys Ther 1997;77: Wolf B, Feys H, De Weerdt W, van der Meer J, Noom M, Aufdemkampe G. Effect of a physical therapeutic intervention for balance problems in the elderly: a single-blind, randomized, controlled multicentre trial. Clin Rehabil 2001;15: Brown K, Whitney S, Wrisley D, Furman J. Physical therapy outcomes for persons with bilaterial vestibular loss. Laryngoscope 2001;111: Whitney S, Hudak M, Marchetti G. The dynamic gait index relates to self-reported fall history in individuals with vestibular dysfunction. J Vestib Res 2000;10: Wrisley D, Whitney S, Furman J. Vestibular rehabilitation outcomes in patients with a history of migraine. Otol Neurotol 2002;23: Dannenbaum E, Rappaport JM, Paquet N, Visintin M, Fung J, Watt D. 2-year review of a novel vestibular rehabilitation program in Montreal and Laval, Quebec. J Otolaryngol 2004;33:5-9. Tests and Measures: Adult; 2012 DGI Page 6
7 10. Hall C, SJ H. Reliability of clinical measures used to assess patients with peripheral vestibular disorders. J Neurol Phys Ther 2006;30(2): Fritz SL, Pittman AL, Robinson AC, Orton SC, Rivers ED. An intense intervention for improving gait, balance, and mobility for individuals with chronic stroke: a pilot study J Neurol Phys Ther 2007;31: Dibble L, Lange M. Predicting falls in individuals with Parkinson disease: a reconsideration of clinical balance measures J Neurol Phys Ther 2006;30(2): Cattaneo D, Regola A, Meotti M. Validity of six balance disorders scales in persons with multiple sclerosis. Disabil Rehabil 2006;28(12): Parisi S, Heroux M, Gulham E, Norman K. Functional mobility and postural control in essential tremor. Arch Phys Med Rehabil 2006;87: Chiu Y, Fritz S, Light K, Velozo C. Use of item response analysis to investigate measurement properties and clinical validity of data for the dynamic gait index. Phys Ther 2006;86(6): McConvey J, Bennett S. Reliability of the dynamic gait index in individuals with multiple sclerosis. Arch Phys Med Rehabil 2005;86: Legters K, Whitney S, Porter R, Buczek F. The relationship between the activities-specific balance confidence scale and the dynamic gait index in peripheral vestibular dysfunction. Physio Research Inter 2005;10(1): Whitney S, Wrisley D, Marchetti G, Gee M, Redfern M, Furman J. Clinical measurement of sit-to-stand performance in people with balance disorders: validity of data for the five-times-sit-to-stand test. Phys Ther 2005;85(10): Whitney S, G. Marchetti, L. O. Morris, Sparto PJ. The reliability and validity of the four square step test for people with balance deficits secondary to a vestibular disorder. Arch Phys Med Rehabil 2007;88: Whitney S, Wrisley D, Furman J. Concurrent validity of the berg balance scale and the dynamic gait index in people with vestibular dysfunction. Physiother Res Int 2003;8(4): Boulgarides L, McGinty S, Willett J, Barnes C. Use of clinicaland impairment- Based tests to predict falls by community-dwelling older adults. Phys Ther 2003;83(4): Hall C, Shubert M, Herdman S. Prediction of fall risk reduction as measured by dynamic gait index in individuals with unilateral vestibular hypofunction. Otol Neurotol 2004;25: Lin S, Tsai T, Lee I, Wu Y. Perception of unsteadiness in patients with dizziness: Association with handicap and imbalance. J Biomed Sci 2002;9: Whitney S, Wrisley D, Brown K, Furman J. Is perception of handicap related to functional performance in persons with vestibular dysfunction? Otol Neurotol 2004;25: Whitney S, Marchetti G, Schade A, Wrisley D. The sensitivity and specificity of the timed "up and go" and the dynamic gait index for self-reported falls in persons with vestibular disorders. J Vestib Res 2004;14: Brown K, Whitney S, Marchetti G, Wrisley D, Furman J. Physical therapy for central vestibular dysfunction. Arch Phys Med Rehabil 2006;87: Badke M, Shea T, Miedaner J, Grove C. Outcomes after rehabilitation for adults with balance dysfunction. Arch Phys Med Rehabil 2004;85(February): Meli A, Zimatore G, Badaracco C, De Angelis E, Tufarelli D. Vestibular rehabilitation and 6-month follow-up using objective and subjective measures. Acta OtoLaryngologica 2006;126: Li F, Harmer P, Fisher K, Mcauley E. Tai Chi: improving functional balance and predicting subsequent falls in older persons. Med Sci Sports Exerc 2004;36(12): Li F, Harmer P, Fisher KJ, McAuley E, Chaumeton N, Eckstrom E et al. Tai chi and fall reductions in older adults: a randomized controlled trial. J Gerontol A Biol Sci Med Sci 2005;60A(2): Low Choy N, Johnson N, Treleavan J, Jull G, Panizza B, Brown-Rothwell D. Balance, mobility and gaze stability deficits remain following surgical removal of vestibular schwannoma (acustic neuroma): An observational study. Aust J Physiother 2006: Wrisley DM, Marchetti GF, Kuharsky DK, Whitney SL. Reliability, internal consistency, and validity of data obtained with the functional gait assessment. Phys Ther 2004;84(10): Walker ML, Austin AG, Banke GM, Foxx SR, Gaetano L, Gardner LA et al. Reference group data for the functional gait assessment. Phys Ther 2007;87(11): Wrisley, DM, Kumar,NA. Functional gait assessment: Concurrent, discriminative, and predictive validity in community-dwelling older adults. Phys Ther 2010: 90(5): Tests and Measures: Adult; 2012 DGI Page 7
8 Functional Gait Assessment Appendix. Requirements: A marked 6-m (20-ft) walkway that is marked with a cm (12-in) width. 1. GAIT LEVEL SURFACE Instructions: Walk at your normal speed from here to the next mark (6 m[20 ft]). (3) Normal Walks 6 m (20 ft) in less than 5.5 seconds, no assistive devices, good speed, no evidence for imbalance, normal gait pattern, deviates no more than cm (6 in) outside of the cm (12-in) walkway width. (2) Mild impairment Walks 6 m (20 ft) in less than 7 seconds but greater than 5.5 seconds, uses assistive device, slower speed, mild gait deviations, or deviates cm (6 10 in) outside of the cm (12-in) walkway width. (1) Moderate impairment Walks 6 m (20 ft), slow speed, abnormal gait pattern, evidence for imbalance, or deviates cm (10 15 in) outside of the cm (12-in) walkway width. Requires more than 7 seconds to ambulate 6 m (20 ft). (0) Severe impairment Cannot walk 6 m (20 ft) without assistance, severe gait deviations or imbalance, deviates greater than 38.1 cm (15 in) outside of the cm (12-in) walkway width or reaches and touches the wall. 2. CHANGE IN GAIT SPEED Instructions: Begin walking at your normal pace (for 1.5 m [5 ft]). When I tell you go, walk as fast as you can (for 1.5 m [5 ft]). When I tell you slow, walk as slowly as you can (for 1.5 m [5 ft]). (3) Normal Able to smoothly change walking speed without loss of balance or gait deviation. Shows a significant difference in walking speeds between normal, fast, and slow speeds. Deviates no more than cm (6 in) outside of the cm (12-in) walkway width. (2) Mild impairment Is able to change speed but demonstrates mild gait deviations, deviates cm (6 10 in) outside of the cm (12-in) walkway width, or no gait deviations but unable to achieve a significant change in velocity, or uses an assistive device. (1) Moderate impairment Makes only minor adjustments to walking speed, or accomplishes a change in speed with significant gait deviations, deviates cm (10 15 in) outside the cm (12-in) walkway width, or changes speed but loses balance but is able to recover and continue walking. (0) Severe impairment Cannot change speeds, deviates greater than 38.1 cm (15 in) outside cm (12-in) walkway width, or loses balance and has to reach for wall or be caught. 3. GAIT WITH HORIZONTAL HEAD TURNS Instructions: Walk from here to the next mark 6 m (20 ft) away. Begin walking at your normal pace. Keep walking straight; after 3 steps, turn your head to the right and keep walking straight while looking to the right. After 3 more steps, turn your head to the left and keep walking straight while looking left. Continue alternating looking right and left Tests and Measures: Adult; 2012 DGI Page 8
9 every 3 steps until you have completed 2 repetitions in each direction. (3) Normal Performs head turns smoothly with no change in gait. Deviates no more than cm (6 in) outside cm (12-in) walkway width. (2) Mild impairment Performs head turns smoothly with slight change in gait velocity (eg, minor disruption to smooth gait path), deviates cm (6 10 in) outside cm (12-in) walkway width, or uses an assistive device. (1) Moderate impairment Performs head turns with moderate change in gait velocity, slows down, deviates cm (10 15 in) outside cm (12-in) walkway width but recovers, can continue to walk. (0) Severe impairment Performs task with severe disruption of gait (eg, staggers 38.1 cm [15 in] outside cm (12-in) walkway width, loses balance, stops, or reaches for wall). 4. GAIT WITH VERTICAL HEAD TURNS Instructions: Walk from here to the next mark (6 m [20 ft]). Begin walking at your normal pace. Keep walking straight; after 3 steps, tip your head up and keep walking straight while looking up. After 3 more steps, tip your head down, keep walking straight while looking down. Continue alternating looking up and down every 3 steps until you have completed 2 repetitions in each direction. (3) Normal Performs head turns with no change in gait. Deviates no more than cm (6 in) outside cm (12-in) walkway width. (2) Mild impairment Performs task with slight change in gait velocity (eg, minor disruption to smooth gait path), deviates cm (6 10 in) outside cm (12-in) walkway width or uses assistive device. (1) Moderate impairment Performs task with moderate change in gait velocity, slows down, deviates cm (10 15 in) outside cm (12-in) walkway width but recovers, can continue to walk. (0) Severe impairment Performs task with severe disruption of gait (eg, staggers 38.1 cm [15 in] outside cm (12-in) walkway width, loses balance, stops, reaches for wall). 5. GAIT AND PIVOT TURN Instructions: Begin with walking at your normal pace. When I tell you, turn and stop, turn as quickly as you can to face the opposite direction and stop. (3) Normal Pivot turns safely within 3 seconds and stops quickly with no loss of balance. (2) Mild impairment Pivot turns safely in _3 seconds and stops with no loss of balance, or pivot turns safely within 3 seconds and stops with mild imbalance, requires small steps to catch balance. (1) Moderate impairment Turns slowly, requires verbal cueing, or requires several small steps to catch balance following turn and stop. Tests and Measures: Adult; 2012 DGI Page 9
10 (0) Severe impairment Cannot turn safely, requires assistance to turn and stop. 6. STEP OVER OBSTACLE Instructions: Begin walking at your normal speed. When you come to the shoe box, step over it, not around it, and keep walking. (3) Normal Is able to step over 2 stacked shoe boxes taped together (22.86 cm [9 in] total height) without changing gait speed; no evidence of imbalance. (2) Mild impairment Is able to step over one shoe box (11.43 cm [4.5 in] total height) without changing gait speed; no evidence of imbalance. (0) Moderate impairment Is able to step over one shoe box (11.43 cm [4.5 in] total height) but must slow down and adjust steps to clear box safely. May require verbal cueing. (0) Severe impairment Cannot perform without assistance. 7. GAIT WITH NARROW BASE OF SUPPORT Instructions: Walk on the floor with arms folded across the chest, feet aligned heel to toe in tandem for a distance of 3.6 m [12 ft]. The number of steps taken in a straight line are counted for a maximum of 10 steps. (3) Normal Is able to ambulate for 10 steps heel to toe with no staggering. (2) Mild impairment Ambulates 7 9 steps. (1) Moderate impairment Ambulates 4 7 steps. (0) Severe impairment Ambulates less than 4 steps heel to toe or cannot perform without assistance. 8. GAIT WITH EYES CLOSED Instructions: Walk at your normal speed from here to the next mark (6 m [20 ft]) with your eyes closed. (3) Normal Walks 6 m (20 ft), no assistive devices, good speed, no evidence of imbalance, normal gait pattern, deviates no more than cm (6 in) outside cm (12-in) walkway width. Ambulates 6 m (20 ft) in less than 7 seconds. (2) Mild impairment Walks 6 m (20 ft), uses assistive device, slower speed, mild gait deviations, deviates cm (6 10 in) outside cm (12-in) walkway width. Ambulates 6 m (20 ft) in less than 9 seconds but greater than 7 seconds. (1) Moderate impairment Walks 6 m (20 ft), slow speed, abnormal gait pattern, evidence for imbalance, deviates cm (10 15 in) outside cm (12-in) walkway width. Requires more than 9 seconds to ambulate 6 m (20 ft). (0) Severe impairment Cannot walk 6 m (20 ft) without assistance, severe gait deviations or imbalance, deviates greater than 38.1 cm (15 in) outside cm (12-in) walkway width or will not attempt task. 9. AMBULATING BACKWARDS Instructions: Walk backwards until I tell you to stop. (3) Normal Walks 6 m (20 ft), no assistive devices, good speed, no evidence for imbalance, normal gait pattern, deviates no Tests and Measures: Adult; 2012 DGI Page 10
11 more than cm (6 in) outside cm (12-in) walkway width. (2) Mild impairment Walks 6 m (20 ft), uses assistive device, slower speed, mild gait deviations, deviates cm (6 10 in) outside cm (12-in) walkway width. (1) Moderate impairment Walks 6 m (20 ft), slow speed, abnormal gait pattern, evidence for imbalance, deviates cm (10 15 in) outside cm (12-in) walkway width. (0) Severe impairment Cannot walk 6 m (20 ft) without assistance, severe gait deviations or imbalance, deviates greater than 38.1 cm (15 in) outside cm (12-in) walkway width or will not attempt task. 10. STEPS Instructions: Walk up these stairs as you would at home (ie, using the rail if necessary). At the top turn around and walk down. (3) Normal Alternating feet, no rail. (2) Mild impairment Alternating feet, must use rail. (1) Moderate impairment Two feet to a stair; must use rail. (0) Severe impairment Cannot do safely. TOTAL SCORE: MAXIMUM SCORE 30 a Adapted from Dynamic Gait Index.1 Modified and reprinted with permission of authors and Lippincott Williams & Wilkins ( Walker, M.L. (2007). Reference Group Data for the Functional Gait Assessment. Physical Therapy (87)11, Tests and Measures: Adult; 2012 DGI Page 11
ARE THE USE OF MEDICARE G CODES MAKING YOU SPIN?
 1 2 3 4 5 6 7 8 ARE THE USE F MEDICARE G CDES MAKING YU SPIN? HERE ARE SME ANSWERS: VESTIBULAR REHABILITATIN SPECIAL INTEREST GRUP Functional Limitation Reporting Kenda Fuller, PT South Valley Physical
1 2 3 4 5 6 7 8 ARE THE USE F MEDICARE G CDES MAKING YU SPIN? HERE ARE SME ANSWERS: VESTIBULAR REHABILITATIN SPECIAL INTEREST GRUP Functional Limitation Reporting Kenda Fuller, PT South Valley Physical
BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008
 BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008 TEST NUMBER/SUBJECT CODE DATE EXAMINER NAME EXAMINER Instructions for BESTest 1. Subjects should be tested with flat heeled shoes or
BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008 TEST NUMBER/SUBJECT CODE DATE EXAMINER NAME EXAMINER Instructions for BESTest 1. Subjects should be tested with flat heeled shoes or
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling
 Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
Functional Assessments for Geriatric Clients
 Disability Schemes Functional Assessments for Geriatric Clients Ann Medley, PT, PhD Texas Woman s s University School of Physical Therapy International Classification of Functioning, Disability, and Health
Disability Schemes Functional Assessments for Geriatric Clients Ann Medley, PT, PhD Texas Woman s s University School of Physical Therapy International Classification of Functioning, Disability, and Health
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL
 BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
or [email protected]
 INTRODUCTION The consequences of postural dyscontrol are pervasive and have a significant impact on activities of daily living, community mobility and social, work and leisure pursuits. The Community Balance
INTRODUCTION The consequences of postural dyscontrol are pervasive and have a significant impact on activities of daily living, community mobility and social, work and leisure pursuits. The Community Balance
FALLS PREVENTION & RISK ASSESSMENTS
 FALLS PREVENTION & RISK ASSESSMENTS Created With Support From: Buffalo Rehab Group Physical Therapy PC Continuing Care Division of Catholic Health System s Senior Services D Youville College, Occupational
FALLS PREVENTION & RISK ASSESSMENTS Created With Support From: Buffalo Rehab Group Physical Therapy PC Continuing Care Division of Catholic Health System s Senior Services D Youville College, Occupational
Vestibular Rehabilitation for Dizziness and Balance Disorders After Concussion
 ARTICLE Vestibular Rehabilitation for Dizziness and Balance Disorders After Concussion Bara A. Alsalaheen, PT, MS, Anne Mucha, PT, MS, NCS, Laura O. Morris, PT, NCS, Susan L. Whitney, PT, PhD, NCS, FAPTA,
ARTICLE Vestibular Rehabilitation for Dizziness and Balance Disorders After Concussion Bara A. Alsalaheen, PT, MS, Anne Mucha, PT, MS, NCS, Laura O. Morris, PT, NCS, Susan L. Whitney, PT, PhD, NCS, FAPTA,
Vestibular Rehabilitation What s the Spin?
 Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
Vestibular Assessment
 Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
Predicting Fall Risk in Acute Rehabilitation Facilities Stephanie E. Kaplan, PT, DPT, ATP Emily R. Rosario, PhD
 Objectives Predicting Fall Risk in Acute Inpatient Rehabilitation Facilities Director of Rehabilitation and Director of Research Casa Colina Centers for Rehabilitation March 16, 2012 Current Falls Assessment
Objectives Predicting Fall Risk in Acute Inpatient Rehabilitation Facilities Director of Rehabilitation and Director of Research Casa Colina Centers for Rehabilitation March 16, 2012 Current Falls Assessment
Vestibular Rehabilitation Therapy (Rationale) Adaptation Guidelines. Substitution guidelines. Habituation exercise guidelines. Substitution guidelines
 Vestibular Rehabilitation Therapy Outline: Rationale for the effect of exercises Framework for exercise prescription Exercise progression Preferred prescription patterns Case study General treatment guidelines
Vestibular Rehabilitation Therapy Outline: Rationale for the effect of exercises Framework for exercise prescription Exercise progression Preferred prescription patterns Case study General treatment guidelines
A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS
 The Indian Journal of Occupational Therapy : Vol. XXXVI : No. 1 (April - July 04) A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS * Pina
The Indian Journal of Occupational Therapy : Vol. XXXVI : No. 1 (April - July 04) A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS * Pina
Dizziness and Vertigo
 Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
Outcomes After Rehabilitation for Adults With Balance Dysfunction
 227 Outcomes After Rehabilitation for Adults With Balance Dysfunction Mary Beth Badke, PhD, PT, Terry A. Shea, BSc, PT, James A. Miedaner, MS, PT, Colin R. Grove, BSc, PT ABSTRACT. Badke MB, Shea TA, Miedaner
227 Outcomes After Rehabilitation for Adults With Balance Dysfunction Mary Beth Badke, PhD, PT, Terry A. Shea, BSc, PT, James A. Miedaner, MS, PT, Colin R. Grove, BSc, PT ABSTRACT. Badke MB, Shea TA, Miedaner
MEASUREMENT SCALES USED IN ELDERLY CARE FUNCTIONAL INDEPENDENCE MEASURE AND FUNCTIONAL ASSESSMENT MEASURE
 FUNCTIONAL INDEPENDENCE MEASURE AND FUNCTIONAL ASSESSMENT MEASURE Functional Independence Measure The Functional Independence Measure (FIM) scale assesses physical and cognitive disability. This scale
FUNCTIONAL INDEPENDENCE MEASURE AND FUNCTIONAL ASSESSMENT MEASURE Functional Independence Measure The Functional Independence Measure (FIM) scale assesses physical and cognitive disability. This scale
Gait with Assistive Devices
 Gait with Assistive Devices Review Last Lecture Weak dorsiflexors? Vaulting? Hip hiking? Weak hip abductors? Hip circumduction? Ataxic gait? Antalgic gait? Explain the line of gravity Ambulation with Assistive
Gait with Assistive Devices Review Last Lecture Weak dorsiflexors? Vaulting? Hip hiking? Weak hip abductors? Hip circumduction? Ataxic gait? Antalgic gait? Explain the line of gravity Ambulation with Assistive
1/12/2015. Tom Ambury, PT, CHC
 Tom Ambury, PT, CHC Attendees will understand the key components of the initial evaluation Attendees will understand the importance of the initial evaluation in establishing the skilled need for therapy
Tom Ambury, PT, CHC Attendees will understand the key components of the initial evaluation Attendees will understand the importance of the initial evaluation in establishing the skilled need for therapy
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT
 Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
ANKLE STRENGTHENING INTRODUCTION EXERCISES SAFETY
 ANKLE STRENGTHENING INTRODUCTION Welcome to your Ankle Strengthening exercise program. The exercises in the program are designed to improve your ankle strength, fitness, balance and dynamic control. The
ANKLE STRENGTHENING INTRODUCTION Welcome to your Ankle Strengthening exercise program. The exercises in the program are designed to improve your ankle strength, fitness, balance and dynamic control. The
ABOUT THE FUNCTIONAL FITNESS TEST: ABOUT THE AUTHORS:
 The Interactive Health Partner Wellness Program addresses fall prevention with assessments and outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com
The Interactive Health Partner Wellness Program addresses fall prevention with assessments and outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com
Research Report. Key Words: Measurement, Motor recovery, Outcome measure, Psychometrics, Stroke.
 Research Report The Stroke Rehabilitation Assessment of Movement (STREAM): A Comparison With Other Measures Used to Evaluate Effects of Stroke and Rehabilitation Background and Purpose. The Stroke Rehabilitation
Research Report The Stroke Rehabilitation Assessment of Movement (STREAM): A Comparison With Other Measures Used to Evaluate Effects of Stroke and Rehabilitation Background and Purpose. The Stroke Rehabilitation
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic
 Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Stroke Rehabilitation Triage Severe Strokes
 The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
Recovering from a Mild Traumatic Brain Injury (MTBI)
 Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Stand with your feet hip-width apart and your weight equally distributed on both legs (A).
 Introduction to balance exercises Balance exercises can help you maintain your balance and confidence at any age. Balance exercises can also help prevent falls and improve your coordination. For older
Introduction to balance exercises Balance exercises can help you maintain your balance and confidence at any age. Balance exercises can also help prevent falls and improve your coordination. For older
Vestibular Rehabilitation Therapy. Melissa Nelson
 Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
SENIOR/LTC ASSESSMENT TRAINING MODULE
 Welcome to the Superior Mobile Medics Senior/LTC Assessment Training i Module Learning Objectives Gain familiarity with the Senior/LTC Assessment process, including company-specific requirements. Know
Welcome to the Superior Mobile Medics Senior/LTC Assessment Training i Module Learning Objectives Gain familiarity with the Senior/LTC Assessment process, including company-specific requirements. Know
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: [email protected] Surveillance and Referral
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: [email protected] Surveillance and Referral
Follow-up Form B3: Evaluation Form Unified Parkinson s Disease Rating Scale (UPDRS 1 ) Motor Exam
 phone: (206) 543-8637; fax: (206) 616-5927 e-mail: [email protected] website: www.alz.washington.edu NACC Uniform Data Set (UDS) Follow-up Form B3: Evaluation Form Unified Parkinson s Disease Rating
phone: (206) 543-8637; fax: (206) 616-5927 e-mail: [email protected] website: www.alz.washington.edu NACC Uniform Data Set (UDS) Follow-up Form B3: Evaluation Form Unified Parkinson s Disease Rating
Benign Paroxysmal Positional Vertigo. By Mick Benson
 Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
PEOPLE WITH DYSFUNCTION within the vestibular system
 ORIGINAL ARTICLE Short-Term Effects of Vestibular Rehabilitation in Patients With Chronic Unilateral Vestibular Dysfunction: A Randomized Controlled Study Murat Giray, MD, Yesim Kirazli, MD, Hale Karapolat,
ORIGINAL ARTICLE Short-Term Effects of Vestibular Rehabilitation in Patients With Chronic Unilateral Vestibular Dysfunction: A Randomized Controlled Study Murat Giray, MD, Yesim Kirazli, MD, Hale Karapolat,
Ulster GAA Sport Science Services Fitness Testing Procedures 2012 2016. Ulster GAA Fitness Testing Procedures For County Academy Squads 2012-2016
 Ulster GAA Fitness Testing Procedures For County Academy Squads 2012-2016 Introduction This document has been compiled by Kevin McGuigan (Ulster GAA, Sport Science Support Officer) following consultation
Ulster GAA Fitness Testing Procedures For County Academy Squads 2012-2016 Introduction This document has been compiled by Kevin McGuigan (Ulster GAA, Sport Science Support Officer) following consultation
The Role of Physical Therapy in Post Concussion Management. Non Disclosure
 The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
The Human Balance System
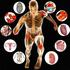 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
Vestibular Rehabilitation
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
The Rehab Professional s Role in Dining for Persons with Dementia. By: Bonnie Saunders PT, MPA, CDP
 The Rehab Professional s Role in Dining for Persons with Dementia By: Bonnie Saunders PT, MPA, CDP There have been many advances that have brought about an increased understanding of the etiologies and
The Rehab Professional s Role in Dining for Persons with Dementia By: Bonnie Saunders PT, MPA, CDP There have been many advances that have brought about an increased understanding of the etiologies and
Knee Pain/OA Physical Therapy Approaches
 Knee Pain/OA Physical Therapy Approaches G. Kelley Fitzgerald, PT, PhD, FAPTA Professor, Department of Physical Therapy, School of Health and Rehabilitation Sciences Director, Physical Therapy Clinical
Knee Pain/OA Physical Therapy Approaches G. Kelley Fitzgerald, PT, PhD, FAPTA Professor, Department of Physical Therapy, School of Health and Rehabilitation Sciences Director, Physical Therapy Clinical
The Morse Fall Scale Training Module Partners HealthCare System Fall Prevention Task Force
 The Morse Fall Scale Training Module Partners HealthCare System Fall Prevention Task Force Based on J. Morse (1997). Preventing Patient Falls. CA: Sage Publishing Co. 1 2 Objectives 1. What is fall risk
The Morse Fall Scale Training Module Partners HealthCare System Fall Prevention Task Force Based on J. Morse (1997). Preventing Patient Falls. CA: Sage Publishing Co. 1 2 Objectives 1. What is fall risk
Physical Therapy Sample Reports 2009
 Sample Reports 2009 Includes: Progress/ Treatment Note Plan of Care from Initial Evaluation Initial Evaluation/ Examination (full-length compliant) Ten (10) Visit Progress Report Discharge Summary Physician
Sample Reports 2009 Includes: Progress/ Treatment Note Plan of Care from Initial Evaluation Initial Evaluation/ Examination (full-length compliant) Ten (10) Visit Progress Report Discharge Summary Physician
Traumatic brain injury (TBI)
 Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
Preparing for the Washington State Criminal Justice Training Commission Physical Ability Test
 Preparing for the Washington State Criminal Justice Training Commission Physical Ability Test Whereas many training routines can be used to improve performance in the Physical Ability Test (PAT), participants
Preparing for the Washington State Criminal Justice Training Commission Physical Ability Test Whereas many training routines can be used to improve performance in the Physical Ability Test (PAT), participants
Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment
 Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment Teresa Leung Therapist Prince of Wales Hospital 7 th May, 2012 Outline of Presentation Introduction Study Objectives,
Prediction of the MoCA and the MMSE in Out-patients with the risks of cognitive impairment Teresa Leung Therapist Prince of Wales Hospital 7 th May, 2012 Outline of Presentation Introduction Study Objectives,
Sue Schuerman, PT, GCS, PhD UNLVPT
 Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Fear of falling in older people
 Fear of falling in older people new findings from recent international research Presentation by Kim Delbaere Falls Prevention Symposium 2012 Catholic University Leuven 1.Fear of falling as a fall risk
Fear of falling in older people new findings from recent international research Presentation by Kim Delbaere Falls Prevention Symposium 2012 Catholic University Leuven 1.Fear of falling as a fall risk
Stair Workouts Get in Shape: Step up!
 Stair Workouts Get in Shape: Step up! Warning: If you feel any knee pains, refrain from continuing that particular exercise. Avoid the no pain, no gain motto and modify with regular walking or any activity
Stair Workouts Get in Shape: Step up! Warning: If you feel any knee pains, refrain from continuing that particular exercise. Avoid the no pain, no gain motto and modify with regular walking or any activity
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Elderly Mobility Scale (EMS)
 Elderly Mobility Scale (EMS) Summary: Measures: Scale of assessment of mobility. Description: The EMS is a 20 point validated assessment tool for the assessment of frail elderly subjects (Smith 1994).
Elderly Mobility Scale (EMS) Summary: Measures: Scale of assessment of mobility. Description: The EMS is a 20 point validated assessment tool for the assessment of frail elderly subjects (Smith 1994).
Environmental modifiers: Prospects for rehabilitation in Huntington s disease
 Environmental modifiers: Prospects for rehabilitation in Huntington s disease Jan Frich Oslo University Hospital / University of Oslo EHDN 8th Plenary Meeting, Sept 19, 2014 Background Growing interest
Environmental modifiers: Prospects for rehabilitation in Huntington s disease Jan Frich Oslo University Hospital / University of Oslo EHDN 8th Plenary Meeting, Sept 19, 2014 Background Growing interest
UCCS Women s Soccer. 2012 Summer Workout Packet. Everything You Need to Succeed. Lifting and Training Schedule
 UCCS Women s Soccer 2012 Summer Workout Packet Everything You Need to Succeed Day to Day Calendar Lifting and Training Schedule Day to Day Record Sheets Fitness Tests Daily Record Sheet Sunday Monday Tuesday
UCCS Women s Soccer 2012 Summer Workout Packet Everything You Need to Succeed Day to Day Calendar Lifting and Training Schedule Day to Day Record Sheets Fitness Tests Daily Record Sheet Sunday Monday Tuesday
adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes
 Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health & Science University, Portland, Oregon
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
Rehabilitation Where You Recover. Inpatient Rehabilitation Services at Albany Medical Center
 Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rationale of The Knee Society Clinical Rating System. John N. Insall, MD, Lawrence D. Dorr, MD, Richard D. Scott, MD, and W.
 Rationale of The Knee Society Clinical Rating System John N. Insall, MD, Lawrence D. Dorr, MD, Richard D. Scott, MD, and W. Norman Scott, MD From the Hospital for Special Surgery, affiliated with The New
Rationale of The Knee Society Clinical Rating System John N. Insall, MD, Lawrence D. Dorr, MD, Richard D. Scott, MD, and W. Norman Scott, MD From the Hospital for Special Surgery, affiliated with The New
Exercises for older people
 Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Updates into Therapeutic Exercise Programs for Patients with LBP. Maximizing Patient Motivation and Outcomes Alice M.
 Updates into Therapeutic Exercise Programs for Patients with LBP Maximizing Patient Motivation and Outcomes Alice M. Davis, PT, DPT Objectives Review Statistics on LBP Discuss current research findings
Updates into Therapeutic Exercise Programs for Patients with LBP Maximizing Patient Motivation and Outcomes Alice M. Davis, PT, DPT Objectives Review Statistics on LBP Discuss current research findings
CAPTURE Collaboration and Proactive Teamwork Used to Reduce. Best Practices in Safe Transfers and Mobility to Decrease Fall Risk
 CAPTURE Collaboration and Proactive Teamwork Used to Reduce Falls Best Practices in Safe Transfers and Mobility to Decrease Fall Risk August 20, 2013 10 a.m. CST Dawn M. Venema, PT, PhD Jill Hassel, DPT
CAPTURE Collaboration and Proactive Teamwork Used to Reduce Falls Best Practices in Safe Transfers and Mobility to Decrease Fall Risk August 20, 2013 10 a.m. CST Dawn M. Venema, PT, PhD Jill Hassel, DPT
Stick with the program!
 Getting Physically Prepared for the Naval Academy Physical education is an important part of the program at the Naval Academy. To ensure that you are physically prepared for Plebe Summer, you are encouraged
Getting Physically Prepared for the Naval Academy Physical education is an important part of the program at the Naval Academy. To ensure that you are physically prepared for Plebe Summer, you are encouraged
Instructions & Forms for Submitting Claims to Medicare
 Instructions & Forms for Submitting Claims to Medicare The Centers for Medicare and Medicaid services have issued a national coverage policy for the WalkAide. CMS will cover patients who have a diagnosis
Instructions & Forms for Submitting Claims to Medicare The Centers for Medicare and Medicaid services have issued a national coverage policy for the WalkAide. CMS will cover patients who have a diagnosis
How To Diagnose Stroke In Acute Vestibular Syndrome
 Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
How To Help Reduce Fall Risk
 C A P T U R E Collaboration and Proactive Teamwork Used to Reduce Falls Best Practices in Mobility Assessment to Decrease Fall Risk July 9, 2013 10:00 11:00 a.m. CST Dawn M. Venema, PT, PhD Jill Hassel,
C A P T U R E Collaboration and Proactive Teamwork Used to Reduce Falls Best Practices in Mobility Assessment to Decrease Fall Risk July 9, 2013 10:00 11:00 a.m. CST Dawn M. Venema, PT, PhD Jill Hassel,
Topic: Passing and Receiving for Possession
 U12 Lesson Plans Topic: Passing and Receiving for Possession Objective: To improve the players ability to pass, receive, and possess the soccer ball when in the attack Dutch Square: Half of the players
U12 Lesson Plans Topic: Passing and Receiving for Possession Objective: To improve the players ability to pass, receive, and possess the soccer ball when in the attack Dutch Square: Half of the players
Perceptual Motor Development
 Perceptual Motor Development Characteristic Involves children during preschool to primary grades; usually ages 21/2 to 6. Combines movement abilities with academics (reading,writing,language, math) Engages
Perceptual Motor Development Characteristic Involves children during preschool to primary grades; usually ages 21/2 to 6. Combines movement abilities with academics (reading,writing,language, math) Engages
Outpatient Neurological Rehabilitation Victoria General Hospital. Pam Loadman BSC.P.T., MSc. Physiotherapist
 Outpatient Neurological Rehabilitation Victoria General Hospital Pam Loadman BSC.P.T., MSc. Physiotherapist OPN - overview Who we see: Inclusion criteria Diagnoses Who we are: Clinicians involved What
Outpatient Neurological Rehabilitation Victoria General Hospital Pam Loadman BSC.P.T., MSc. Physiotherapist OPN - overview Who we see: Inclusion criteria Diagnoses Who we are: Clinicians involved What
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA
 Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Conditioning From Gym To Home To Gym
 Page 1 of 6 Conditioning From Gym To Home To Gym by Vladimir Artemov, Olympic and World Champion and USA Gymnastics Women's National Clinician In the beginning, and throughout the training process, conditioning
Page 1 of 6 Conditioning From Gym To Home To Gym by Vladimir Artemov, Olympic and World Champion and USA Gymnastics Women's National Clinician In the beginning, and throughout the training process, conditioning
WHAT IS A JOURNAL CLUB?
 WHAT IS A JOURNAL CLUB? With its September 2002 issue, the American Journal of Critical Care debuts a new feature, the AJCC Journal Club. Each issue of the journal will now feature an AJCC Journal Club
WHAT IS A JOURNAL CLUB? With its September 2002 issue, the American Journal of Critical Care debuts a new feature, the AJCC Journal Club. Each issue of the journal will now feature an AJCC Journal Club
BEACH VOLLEYBALL TRAINING PROGRAM
 2008 ELITE PERFORMANCE ATHLETE CONDITIONING BEACH VOLLEYBALL TRAINING PROGRAM Team BC 2008 Steve Van Schubert, CAT(C), CSCS Training Schedule General Outline Phase 1 2 Weeks Phase 2 3 Weeks Phase 3 3 Weeks
2008 ELITE PERFORMANCE ATHLETE CONDITIONING BEACH VOLLEYBALL TRAINING PROGRAM Team BC 2008 Steve Van Schubert, CAT(C), CSCS Training Schedule General Outline Phase 1 2 Weeks Phase 2 3 Weeks Phase 3 3 Weeks
Vestibular Rehabilitation: Theory, Evidence and Practical Application
 Vestibular Rehabilitation: Theory, Evidence and Practical Application www.ric.org/education has been ranked Best Rehabilitation Hospital in America" every year since 1991 by U.S. News & World Report. Wesley
Vestibular Rehabilitation: Theory, Evidence and Practical Application www.ric.org/education has been ranked Best Rehabilitation Hospital in America" every year since 1991 by U.S. News & World Report. Wesley
Using FOTO for Reporting Medicare Functional Limitation G-Codes/Severity Modifiers
 Using FOTO for Reporting Medicare Functional Limitation G-Codes/Severity Modifiers FOTO is a very efficient tool to utilize in complying with Medicare Functional Limitation Reporting (FLR) G Codes/Severity
Using FOTO for Reporting Medicare Functional Limitation G-Codes/Severity Modifiers FOTO is a very efficient tool to utilize in complying with Medicare Functional Limitation Reporting (FLR) G Codes/Severity
Vestibular Rehabilitation: Theory, Evidence and Practical Application
 Vestibular Rehabilitation: Theory, Evidence and Practical Application A cademy www.ric.org/education Rehabilitation Institute of Chicago has been ranked Best Rehabilitation Hospital in America" every year
Vestibular Rehabilitation: Theory, Evidence and Practical Application A cademy www.ric.org/education Rehabilitation Institute of Chicago has been ranked Best Rehabilitation Hospital in America" every year
Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University [email protected]
 Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University [email protected] Curtin University is a trademark of Curtin University of Technology CRICOS Provider Code 00301J
Professor Keith Hill, School of Physiotherapy and Exercise Science Curtin University [email protected] Curtin University is a trademark of Curtin University of Technology CRICOS Provider Code 00301J
YMCA Basketball Games and Skill Drills for 3 5 Year Olds
 YMCA Basketball Games and s for 3 5 Year Olds Tips ( s) Variations Page 2 Dribbling Game 10 Players will learn that they must be able to dribble to attack the basket (target) to score in basketball. The
YMCA Basketball Games and s for 3 5 Year Olds Tips ( s) Variations Page 2 Dribbling Game 10 Players will learn that they must be able to dribble to attack the basket (target) to score in basketball. The
Otago Exercise Program
 Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Post-Concussion Syndrome
 Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
2014 Annual Report. HHCRehabNetwork.org. Home Office: 181 Patricia M. Genova Drive Newington, CT 06111 860.696.2500 tel 860.696.
 2014 Annual Report Home Office: 181 Patricia M. Genova Drive Newington, CT 06111 860.696.2500 tel 860.696.2525 fax HHCRehabNetwork.org To the Community: Hartford Hospital Rehabilitation Network (HHRN)
2014 Annual Report Home Office: 181 Patricia M. Genova Drive Newington, CT 06111 860.696.2500 tel 860.696.2525 fax HHCRehabNetwork.org To the Community: Hartford Hospital Rehabilitation Network (HHRN)
CART Community Assessment of Risk Tool
 CART Community Assessment of Risk Tool 0 3-0 7. 2 0 1 2 D E M E N T I A L E A R N I N G E V E N T M U L L I N G A R PA R K H O T E L T U E S D AY 3 R D J U LY 2 0 1 2 D R R Ó N Á N O C A O I M H P R O
CART Community Assessment of Risk Tool 0 3-0 7. 2 0 1 2 D E M E N T I A L E A R N I N G E V E N T M U L L I N G A R PA R K H O T E L T U E S D AY 3 R D J U LY 2 0 1 2 D R R Ó N Á N O C A O I M H P R O
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
This document fully describes the 30 Day Flexibility Challenge and allows you to keep a record of your improvements in flexibility.
 Welcome to the StretchTowel 30 Day Flexibility Challenge! You can Be More Flexible in 30 days by following our stretching program for 10 minutes a day. The best part is that you can stretch using the StretchTowel
Welcome to the StretchTowel 30 Day Flexibility Challenge! You can Be More Flexible in 30 days by following our stretching program for 10 minutes a day. The best part is that you can stretch using the StretchTowel
Clinical Medical Policy Outpatient Rehab Therapies (PT & OT) for Members With Special Needs
 Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Exercises for Low Back Injury Prevention
 DIVISION OF AGRICULTURE RESEARCH & EXTENSION University of Arkansas System Family and Consumer Sciences Increasing Physical Activity as We Age Exercises for Low Back Injury Prevention FSFCS38 Lisa Washburn,
DIVISION OF AGRICULTURE RESEARCH & EXTENSION University of Arkansas System Family and Consumer Sciences Increasing Physical Activity as We Age Exercises for Low Back Injury Prevention FSFCS38 Lisa Washburn,
are you reaching your full potential...
 T h e r e s n o s u c h t h i n g a s b a d e x e r c i s e - j u s t e x e r c i s e d o n e b a d l y FIT for sport are you reaching your full potential... These tests are a series of exercises designed
T h e r e s n o s u c h t h i n g a s b a d e x e r c i s e - j u s t e x e r c i s e d o n e b a d l y FIT for sport are you reaching your full potential... These tests are a series of exercises designed
Agility. Agility Evaluation Tests
 55 2 Agility The multi dimensional movement demands of field and court games dictate a revaluation of the traditional approach to the development of agility. This demands a systematic multi factored approach
55 2 Agility The multi dimensional movement demands of field and court games dictate a revaluation of the traditional approach to the development of agility. This demands a systematic multi factored approach
Spine Vol. 30 No. 16; August 15, 2005, pp 1799-1807
 A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Therapy Functional Reassessment: It s a good thing. Objectives. Oasis-not just a requirement 3/19/2012. Vicki D. Gines PT DPT CEEAA
 Therapy Functional Reassessment: It s a good thing Missouri Alliance For Home Care Annual Conference 2012 Vicki D. Gines PT DPT CEEAA Objectives State how Oasis ties to Therapy evaluations State key components
Therapy Functional Reassessment: It s a good thing Missouri Alliance For Home Care Annual Conference 2012 Vicki D. Gines PT DPT CEEAA Objectives State how Oasis ties to Therapy evaluations State key components
PT and Physician Perspectives
 PT and Physician Perspectives Specialists in evaluating and treating movement disorders Restore, maintain, and promote optimal physical function, as well as, optimal wellness and fitness and optimal quality
PT and Physician Perspectives Specialists in evaluating and treating movement disorders Restore, maintain, and promote optimal physical function, as well as, optimal wellness and fitness and optimal quality
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Edited by P Larking ACC Date report completed 18 January 2010
 Brief report Hart Walker Reviewer Adrian Purins AHTA Edited by P Larking ACC Date report completed 18 January 2010 1. Background Cerebral Palsy (CP) is a group of disorders that arise from brain damage
Brief report Hart Walker Reviewer Adrian Purins AHTA Edited by P Larking ACC Date report completed 18 January 2010 1. Background Cerebral Palsy (CP) is a group of disorders that arise from brain damage
The Human Balance System
 5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
