Steven M. Falowski, Amanda Celii, Anthony K. Sestokas, Daniel M. Schwartz, Craig Matsumoto, Ashwini Sharan
|
|
|
- Egbert Hodge
- 7 years ago
- Views:
Transcription
1 As submitted to: Neuromodulation And later published: Awake versus Asleep Placement of Spinal Cord Stimulators: A Cohort Analysis of Complications Associated with Placement Volume 14, Issue 2, pages , March/April 2011 DOI: /j x Steven M. Falowski, Amanda Celii, Anthony K. Sestokas, Daniel M. Schwartz, Craig Matsumoto, Ashwini Sharan Abstract: Introduction: Patients will typically undergo awake surgery for permanent implantation of SCS in an attempt to optimize electrode placement using patient feedback about the distribution of stimulation-induced paresthesia. The present study compared efficacy of first-time electrode placement under awake conditions with that of neurophysiologicallyguided placement under general anesthesia. Methods: A retrospective review was performed of 387 SCS surgeries among 259 patients which included 167 new stimulator implantation to determine whether first time awake surgery for placement of spinal cord stimulators is preferable to non-awake placement. Results: The incidence of device failure for patients implanted using neurophysiologically-guided placement under general anesthesia was one-half that for patients implanted awake (14.94% vs 29.7%). Conclusion: Non-awake surgery is associated with fewer failure rates and therefore fewer re-operations, making it a viable alternative. Any benefits of awake implantation should carefully be considered in the future. Introduction: Spinal cord stimulation (SCS) is an adjustable, non-destructive, therapy which delivers doses of electrical current to the spinal cord for the management of neuropathic pain. The most common indications include post-laminectomy syndrome, complex regional pain syndrome (CRPS), ischemic limb pain, and angina. (Reference 6) The success of the therapy relies on the ability to create an overlap between the pain areas and the device induced paresthesia. (Reference 6) Extensive work has been done
2 previously in describing the mapping of the spinal structure and the relationship between the spinal level of stimulation and the somatotopy of paresthesia. (Reference 1) A patient typically will undergo implantation of the device in an awake operation to permit testing of the distribution of the induced paresthesia and assessment of the discomfort thresholds. It is commonly believed that intra-operative testing in the awake patient is likely to optimize placement of the electrode, although this method has not been formally compared with other methods of guided placement. Electrode implantation can be performed either under a version of profound anesthesia (local anesthetic and intravenous sedation) which allows for awake intraoperative testing of the implant or under general anesthesia which precludes patient interaction during surgery. The original practice at our institution was to perform the permanent implant under profound anesthesia. Observation and changes in the technique and evolution of the electrode technology allowed for a reassessment and a change in the implant technique. Over the last two years, the majority of the operations have shifted to general anesthesia. The following study is designed to compare two implant techniques for a single surgeon by assessing differences in complications rates in the two cohort groups- awake versus non awake placement. Methods: An IRB approved retrospective review of 387 SCS surgeries with 167 first time internalization operations was undertaken to determine whether there are differences in the surgical complication rates between first time awake surgery for placement of spinal cord stimulators compared to non-awake placement. Patients implanted between by a single surgeon at a single center were included in the review. All patients were implanted with either one or two dual column plate electrode(s). Patients included those requiring follow up despite having been implanted previously by a different surgeon; however, these patients were not included in the analysis of first time implantations. Failure revision surgery was also included for multiple operations or revisions on the same patient. All patients underwent spinal imaging via MRI as surgeon preference prior to implantation. The most common post surgical events included repositioning of the battery, repositioning of the electrode, device failures, and infection. A device failure was defined as any re-operation secondary to a traumatic break in the SCS system, a device malfunction requiring re-exploration, or a device removal secondary to lack of efficacy. Infections were only included if they were associated with a draining wound which resulted in explantation of the entire system. Description of the surgical procedures. Awake Surgery: The awake insertion has been previously described. (Reference 6) The key differences in the techniques used for the two cohorts (awake, non- awake) are described. In the awake group, all patients were positioned in the lateral decubitus position. The majority
3 of the dissection and laminotomy exposure was performed with a laryngeal mask airway under propofol for sedation (Diprivan, Stuart Pharmaceuticals, Wilmington, DE). Identification of the surgical level was confirmed with intra-operative X-ray. Once the electrode was positioned in the epidural space, anesthetics were decreased until the patient was lucid. The device was tested to assess distribution of the paresthesia and then re-positioned, as necessary. Closure was performed under additional sedation and local anesthetics. Non-Awake Surgery: General anesthesia was achieved utilizing a total intravenous anesthesia regimen (propofol, narcotics and benzodiazepines). The patient was intubated endotracheally and positioned on chest rolls in the prone position. The use of neuromuscular blocking agents was avoided following patient intubation. Sterile, 1.3cm, 27 gauge conventional subdermal needle electrode pairs (Sunspots Disposable Electrodes, Axon Systems, Hauppauge, New York) were placed into selected extremity muscle groups along the distributional path of the patient's pain. For T9-T10 thoracic stimulator electrode placements, monitoring electrodes were also placed in the periumbilical rectus abdominis muscles to achieve sensitivity in the T8-T12 spinal nerve root distributions. Symmetrical placement of the monitoring leads is critical since response amplitude comparisons are the basis for the neurophysiologic mapping of the dual strip electrode placement. All neuromonitoring was performed by a single group of board-certified professional surgical neurophysiologists capable of interpreting the data directly in the operating room. Intra-operative fluoroscopy was utilized prior to making incision. The rostral-caudal level of the planned electrode insertion was determined based on the percutaneous trial experience and the active cathode position used at that time. Dissection was performed as previously described to allow exposure of the epidural space. The electrode was connected to testing cables which were passed off the sterile field and connected to a portable stimulator. Intraoperative test stimulation was delivered between select pairs of electrodes at frequencies between 3-5Hz using a pulse-width (PW) between milliseconds (ms) and intensities up to 12 milliamperes (ma). Stimulation intensity was increased gradually from 0 ma until compound muscle action potentials (CMAPS) were elicited from one or more monitored myotomes. These stimulus-evoked electromyographic (EMG) responses were used together with surgeon perception of placement and fluoroscopyto determine the physiological midline, as well as laterality and orientation of the electrode. Spinal cord and spinal nerve root function was monitored on all non-awake procedures to minimize the risk of iatrogenic injury during laminotomies and manipulation of epidural electrodes. This monitoring included somatosensory evoked potentials (SSEP), transcranial electric motor evoked potentials (tcemep) and EMG. Additionally, electroencephalography (EEG) and train-of-four (TOF) testing was performed to aid in the assessment of depth of anesthesia and neuromuscular blockade clearing. Assessment
4 of these modalities assured the safety of the spinal cord and optimal testing conditions for placement of epidural stimulator electrodes. Results: During the period of the review 387 surgical procedures were performed of which 167 were first time internalization of a spinal cord stimulation paddle style electrode. This included 76 with the patient awake and 91 occurring under general anesthesia.. FIGURE 1 shows a graph of the number of cases per year and change in methodology to non- awake surgery. The number of awake procedures peaked in 2004 and then declined as the number of procedures performed under general anesthesia increased. # cases Y e a r Y # Non- Awake # Awake Figure 1: Number of cases per year performed awake versus number performed under general anesthesia Figure 2 demonstrates the operations divided into five categories based on why the surgery was performed. The most common was for new implantation, or an additional implantation. Equipment failure was the second most common including multiple revisions on the same patient if needed. The least common indication for surgery was for infection requiring wound debridement or equipment removal.
5 NEW STIMULATOR FAILURE REPOSITION BATTERY EOL INFECTION Type Count NEW STIMULATOR 167 FAILURE 117 REPOSITION 47 BATTERY EOL 39 INFECTION 17 Total 387 Figure 2: Operations based on indication for surgery A typical example of compound muscle action potentials recorded during neurophysiological mapping is shown for one patient in Figure 3. This patient presented preoperatively with a diagnosis of reflex sympathetic dystrophy and medically intractable pain in both legs. The stimulation electrode was positioned via a T9/10 laminotomy to trigger test responses from bilateral lower extremity myotomes whose distribution overlapped the somatotopic distribution of the patient s symptoms. Subsequent postoperative activation and programming of the stimulator was effective in facilitating management of the patient s pain in this distribution without disruptive motor side effects.
6 Figure 3: Example of EMG responses elicited intraoperatively from bilateral quadriceps and tibialis anterior muscles during test activation of a spinal cord stimulator implanted at the T9/10 spinal level. Position of the implanted electrode was adjusted until clear responses were recorded from both lower extremities, overlapping the distribution of the patient s preoperative pain. Arrows indicate test stimulus delivery times. Muscle Abbreviations: RA- rectus abdominis, QD- quadriceps, TA- tibialis anterior, AHabductor hallucis Awake surgeries versus non awake surgeries were then divided into subcategories of failure versus non-failure within each. Figure 4 demonstrates that using wakeup at first surgery is associated with a higher chance of seeing one or more failures. The incidence of device failure for patients implanted under general anesthesia was one-half that for patients implanted awake (14.94% vs 29.7%, p<.03). This failure rate included those patients requiring multiple surgeries and was over a greater than 5 year follow up period. The overall failure rate for new stimulator implants placed by the primary surgeon was 16%. The rate of infection was analyzed. There was not a statistically significant difference when comparing awake (4.48%) to non- awake (5.7%) placement for rate of infection
7 and therefore the occurrence of infection is not explained by whether wakeup was used at the first surgery. (Figure 4) Additionally, the rate of electrode repositioning for patients originally implanted under general anesthesia was 14.9%, and 17.9% for patients implanted awake. This difference did not reach statistical significance (Figure 4), therefore demonstrating no difference between these two groups. 40% 35% 30% 25% 20% 15% 10% 5% 0% Failure, no wakeup Failure, wakeup 1st Infection, no wakeup Infection, wakeup 1st Reposition, no wakeup Reposition, wakeup 1st Figure 4: Comparison between Awake and Non- Awake placement of SCS Discussion: In the present series, the incidence of device failure following spinal cord implantation performed under general anesthesia using neurophysiologically guided electrode placement was significantly lower than that following implantation in the awake patient. This may be due in part to greater control of the patient under general anesthesia and an associated reduction in spontaneous movements which might otherwise dislodge electrodes and their connections. Surgeon experience and improved technology may also be factors in the observed reduction of device failures implanted under general anesthesia. Surgeon experience increased from 2 years of practice to 7 years of practice during the observed time period. Awake
8 implantations predominated early in the series, while those performed under general anesthesia were phased in later in time. The incidence of other major complications, including infections and poorly placed electrodes that required repositioning in a second operation, did not differ significantly between the two cohorts. These latter results suggest that the neurophysiological mapping technique used to help guide electrode placement under general anesthesia was at least as effective as patient feedback during awake placement. The limitation in the interpretation of the data lies in the lack of two comparable groups done simultaneously. The ideal way to compare these two cohorts would be to have the patients randomized to either Awake or non- awake placement and performed over a set period of time. Surgeon experience and improved technology would then be held constant. This study however is an observation of these two cohorts and the change in surgeon preference overtime. The initial conception for use of EMG/SSEP during implantation was devised in 1998 allowing a stimulation lead to be positioned relative to a physiological midline and/or positioned along the dorsal column in a longitudinal direction (Reference 7). This has been followed up with descriptions and clinical application in placement of surgical leads via a laminotomy (reference 8) as well as by clinical evaluation of this monitoring (reference 9). Throughout the study period patients were implanted with either single or dual column electrodes. The analysis did not account for potential differences between these two patient groups. Manufacturer of the product was not maintained consistent throughout the study period and can also be a confounding factor. Although this study points out a change between placement in awake and non- awake patients it is important to realize that the critical change may not have been appreciated. It is because of these factors that are not accounted for, which are inherent in any study of this type, that the hope is to demonstrate equal efficacy between these two surgical techniques. Device failure requiring revision is a soft and difficult endpoint to characterize. In the analysis some patients may have required one surgery to revise both a device malfunction, as well as a traumatic break. This may have also overlapped with the need for repositioning. The need for the revision of a malfunctioned 4 contact electrode is not equal to that of a 16 contact electrode. Therefore breakdown in each group for a sub analysis is beyond the scope of our study, but opens interest for looking at specific device failure as a future endpoint to study. Historically, spinal cord stimulator implantation has been performed in the awake patient because it provides immediate feedback to the surgeon regarding stimulationinduced paresthesia. Two options for implantation include percutaneous electrodes and laminectomy electrode placement. Lind et al. performed the implantation with a spinal anesthetic and examined whether stimulation-induced paresthesiae could still be evoked to guide the positioning of the electrode. In all patients, it was possible to evoke paresthesiae, the distribution of which could be reproduced postoperatively. The
9 paresthesia thresholds during surgery were only moderately higher than those recorded after implantation (reference 5). Garcia-Perez et al evaluated the safety and efficacy of laminectomy lead placement under epidural anesthesia concluding that it was a feasible alternative (reference 2). Minimally invasive techniques have recently come into favor and are now used in the placement of spinal cord stimulators. Vangeneugden (2007) compared postoperative outcomes following electrode placement using the classical midline laminotomy technique with those following use of a minimally invasive unilateral technique in awake patients. He concluded that a minimally invasive unilateral technique has some advantages over midline laminotomy, based on reduced postoperative pain and length of hospital stay (reference 3). Beems at al. used a modified implantation technique to implant under awake surgery. Using a tubular retractor system, originally developed for minimally invasive degenerative disc surgery, they introduced the plate electrode with a small approach under local anesthesia both allowing trial stimulation and avoiding severe postoperative backache related to the approach in these patients (reference 4). Despite the advantages inherent in the use of different minimally invasive techniques and various methods of focused anesthesia under awake placement, there remain a number of reasons why implantation under general anesthesia may be desirable. The awake operation is often performed while the patient is under local anesthesia, which is very stressful for the patient, and predisposes them to movement. This can lead to decreased patient satisfaction, equipment migration, undesired stimulation effects and treatment failure. These factors lead to the implanting surgeon having a preference for non- awake placement. Additionally, personal experience for most implanting physician s reveals that intraoperative wake up is not always desirable. Some patients are severely disoriented, and others are agitated, which interferes with reliable communication with the surgeon. Further the pre- operative narcotic medication doses frequently required for these patients with chronic severe pain often makes pain control during the wake up very difficult even with generous local anesthetic. Finally, X-ray identification of the midline is often times not possible in the lateral decubitus position. The results of the present study show that when the procedure is performed under general anesthesia, it is possible to rely on radiographic information about electrode position and on the results of neurophysiological mapping to assure proper electrode placement. In our experience, this combination has proved effective for reliable electrode placement after a percutaneous trial. A multi- array electrode can be placed at the same location as the trial electrode, and the orientation and laterality of the lead can be confirmed and adjusted based on neurophysiologic surveillance and guidance. The availability of multiple channel arrays and implantable pulse generators that can function with multiple electrodes now allows for generous implantation of extra electrodes. This advance in technology permits greater flexibility in generating appropriate paresthesia coverage postoperatively via programming of the device. Previously, with 4 or 8 contact electrodes, much more extensive intraoperative testing of the awake patient was required for accurate placement of the electrode. Conclusion:
10 The treatment of chronic pain remains challenging. Spinal cord stimulation has been performed for over 30 years, and slow but steady progress with this technology has been made. Experience in the technique and the equipment has made SCS a much more reliable and safe modality. Careful follow-up of the patients is necessary for successful long-term satisfaction. Equipment related problems can arise at any time after implantation, such as electrode(s) breakage or migration, infection, etc., and an open dialogue with the patients is vital for the continuing successful implementation of the modality. In the present series, implantation under general anesthesia was associated with a lower device failure rate than awake implantation, did not compromise therapeutic efficacy or result in additional complications, therefore leading to fewer re-operations, making it a viable alternative. Any benefits of awake implantation should carefully be considered in the future. References: 1) Barolat G, Fulvio M, He J, Seme S, Ketcik B. Mapping of sensory resposens to epidural stimulation of the intraspinal neural structures in man. J Neurosug 78: , )García-Pérez ML, Badenes R, García-March G, Bordes V, Belda FJ. Epidural anesthesia for laminectomy lead placement in spinal cord stimulation. Anesth Analg Nov;105(5): ) Vangeneugden J. Implantation of surgical electrodes for spinal cord stimulation: classical midline laminotomy technique versus minimal invasive unilateral technique combined with spinal anaesthesia. Acta Neurochir Suppl. 2007;97(Pt 1): ) Beems T, van Dongen RT. Minimally invasive placement of epidural plate electrodes under local anaesthesia in spinal cord stimulation. Acta Neurochir Suppl. 2007;97 (Pt 1): ) Lind G, Meyerson BA, Winter J, Linderoth B. Implantation of laminotomy electrodes for spinal cord stimulation in spinal anesthesia with intraoperative dorsal column activation. Neurosurgery Nov;53(5): ) Falowski S. Celii A, Sharan A. Spinal cord stimulation: an update. Neurotherapeutics Jan;5(1): ) Feler C. Apparatus and method for positioning spinal cord stimulation leads. United States Patent February 2000.
11 8) Alo KM. EMG/SSEP During SCS Implant Surgery. In Book Chapter: Kumar K, et al. Spinal Cord Stimulation: Placement of Surgical Leads Via Laminotomy- Techniques and Benefits. Neuromodulation editors Krames, Peckham, Rezai; 2009:pgs ) North R, et al. page 174 Re: SSEP observations/clinical correlations from the NANS meeting - abstract from December 2009
Electroneuromyographic studies
 Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Contractor Number 11302. Oversight Region Region IV
 Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Economic aspects of Spinal Cord Stimulation (SCS)
 Economic aspects of Spinal Cord Stimulation (SCS) Burden of Chronic Pain Chronic pain affects one in five adults in Europe 1. Up to 10 per cent of chronic pain cases are neuropathic in origin. 2 Chronic
Economic aspects of Spinal Cord Stimulation (SCS) Burden of Chronic Pain Chronic pain affects one in five adults in Europe 1. Up to 10 per cent of chronic pain cases are neuropathic in origin. 2 Chronic
David Logé, MD*, Sven Vanneste, MS, MA, PhD, Tim Vancamp, PT, MBA, Dirk Rijckaert, MD* OBJECTIVE. Neuromodulation: Technology at the Neural Interface
 Neuromodulation: Technology at the Neural Interface Received: April 26, 2012 Revised: October 18, 2012 Accepted: October 25, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12012 Long-Term Outcomes of
Neuromodulation: Technology at the Neural Interface Received: April 26, 2012 Revised: October 18, 2012 Accepted: October 25, 2012 (onlinelibrary.wiley.com) DOI: 10.1111/ner.12012 Long-Term Outcomes of
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet
 Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION
 NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION Introduction: Spinal cord stimulation (SCS) is an established treatment for chronic neuropathic pain, which can
NEUROMODULATION THERAPY ACCESS COALITION POSITION STATEMENT ON SPINAL CORD NEUROSTIMULATION Introduction: Spinal cord stimulation (SCS) is an established treatment for chronic neuropathic pain, which can
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705)
 Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients
 Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
Oxford University Hospitals NHS Trust Department of Neurosciences Dorsal Root Ganglion (DRG) Stimulation Information for patients We have recently seen you in clinic as you have had pain for a long period
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Intraoperative Nerve Monitoring Coding Guide. March 1, 2010
 Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Ms. Jackson is the Manager of Health Finance and Reimbursement, Division of Health Policy and Practice Services, Washington, DC.
 Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
GE Healthcare. Quick Guide PDF PROOF. Neuromuscular Transmission (NMT)
 GE Healthcare Quick Guide Neuromuscular Transmission (NMT) WHAT is Neuromuscular Transmission (NMT)? Neuromuscular Transmission (NMT) is the transfer of an impulse between a nerve and a muscle in the neuromuscular
GE Healthcare Quick Guide Neuromuscular Transmission (NMT) WHAT is Neuromuscular Transmission (NMT)? Neuromuscular Transmission (NMT) is the transfer of an impulse between a nerve and a muscle in the neuromuscular
Pain Management. Practical Applications in Electrotherapy
 Pain Management Practical Applications in Electrotherapy The TENS Advantage Deliver Immediate Pain Relief using a unique waveform designed to help prevent nerve accommodation. Manage Dynamic Pain by adjusting
Pain Management Practical Applications in Electrotherapy The TENS Advantage Deliver Immediate Pain Relief using a unique waveform designed to help prevent nerve accommodation. Manage Dynamic Pain by adjusting
Neurostimulation: Orthopaedic Institute of Ohio 801 Medical Drive Lima, Ohio 45804 419-222-6622
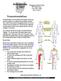 801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
Spinal Cord Stimulation Business Case for
 Spinal Cord Stimulation Business Case for Failed Back Surgery Syndrome Understanding How Various Stakeholders Gauge Success in Treating Chronic Pain FBSS is a subset of chronic low back pain, which is
Spinal Cord Stimulation Business Case for Failed Back Surgery Syndrome Understanding How Various Stakeholders Gauge Success in Treating Chronic Pain FBSS is a subset of chronic low back pain, which is
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
CLINICAL NEUROPHYSIOLOGY
 CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
Assessment of spinal anaesthetic block
 Assessment of spinal anaesthetic block Dr Graham Hocking Consultant in Anaesthesia and Pain Medicine John Radcliffe Hospital Oxford UK Email: ghocking@btinternet.com Spinal anaesthesia has the advantage
Assessment of spinal anaesthetic block Dr Graham Hocking Consultant in Anaesthesia and Pain Medicine John Radcliffe Hospital Oxford UK Email: ghocking@btinternet.com Spinal anaesthesia has the advantage
FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE
 FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE The following describes the open surgical preparation and implantation technique for the Freedom Inguinal Hernia Repair System. 1) Anesthesia can be
FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE The following describes the open surgical preparation and implantation technique for the Freedom Inguinal Hernia Repair System. 1) Anesthesia can be
A New Spinal Cord Stimulation System. Effectively Relieves Chronic, Intractable Pain: A Multicenter Prospective Clinical Study
 NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 10 Number 3 2007 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE A New Spinal Cord Stimulation System Blackwell Publishing Inc Effectively
NEUROMODULATION: TECHNOLOGY AT THE NEURAL INTERFACE Volume 10 Number 3 2007 http://www.blackwell-synergy.com/loi/ner ORIGINAL ARTICLE A New Spinal Cord Stimulation System Blackwell Publishing Inc Effectively
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
 Epimed Would Like To Congratulate The 20th Annual Budapest Conference The New Shape of Pain Relief SmalleST. ThiNNeST. CoNTouRed design. Precision Novi is the world s smallest, thinnest 16 contact primary
Epimed Would Like To Congratulate The 20th Annual Budapest Conference The New Shape of Pain Relief SmalleST. ThiNNeST. CoNTouRed design. Precision Novi is the world s smallest, thinnest 16 contact primary
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Physician Coding and Payment Guide 2015
 Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
LAW ANESTHESIA. the. Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients
 ANESTHESIA & the LAW A RISK MANAGEMENT NEWSLETTER DON T SETTLE. OWN. ISSUE 28 Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients W hether regional blocks should be placed in adult
ANESTHESIA & the LAW A RISK MANAGEMENT NEWSLETTER DON T SETTLE. OWN. ISSUE 28 Nerve Damage from Regional Blocks Placed In Anesthetized/Sedated Patients W hether regional blocks should be placed in adult
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Pain Management in the Critically ill Patient
 Pain Management in the Critically ill Patient Jim Ducharme MD CM, FRCP President-Elect, IFEM Clinical Professor of Medicine, McMaster University Adjunct Professor of Family Medicine, Queens University
Pain Management in the Critically ill Patient Jim Ducharme MD CM, FRCP President-Elect, IFEM Clinical Professor of Medicine, McMaster University Adjunct Professor of Family Medicine, Queens University
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Your anaesthetist may suggest that you have a spinal or epidural injection. These
 Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Effectiveness of spinal cord stimulation for the management of neuropathic pain
 Effectiveness of spinal cord stimulation for the management of neuropathic pain August 2009 Author: Peter Larking PhD Important Note This evidence-based review summarises information on spinal cord stimulation
Effectiveness of spinal cord stimulation for the management of neuropathic pain August 2009 Author: Peter Larking PhD Important Note This evidence-based review summarises information on spinal cord stimulation
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
EMG and the Electrodiagnostic Consultation for the Family Physician
 EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Ambulatory Surgery Center Coding and Payment Guide 2015
 Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
TABLE OF CONTENTS CPT
 TABLE OF CONTENTS CPT Coding Basics...1 National Correct Coding Initiative Edits...1 How to Use NCCI Edits...2 Evaluation and Management...3 Integumentary System... 20 Debridement... 20 Surgery/Musculoskeletal...
TABLE OF CONTENTS CPT Coding Basics...1 National Correct Coding Initiative Edits...1 How to Use NCCI Edits...2 Evaluation and Management...3 Integumentary System... 20 Debridement... 20 Surgery/Musculoskeletal...
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy
 Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Electrodiagnostic Testing
 Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Percutaneous Abscess Drainage
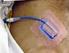 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Handbook of Neurodiagnostic Job Descriptions and Competencies
 Handbook of Neurodiagnostic Job Descriptions and Competencies Table of Contents Introduction Page 6 Acknowledgements. Page 7 Scope of Practice for Neurodiagnostic Technology Page 8 National Competency
Handbook of Neurodiagnostic Job Descriptions and Competencies Table of Contents Introduction Page 6 Acknowledgements. Page 7 Scope of Practice for Neurodiagnostic Technology Page 8 National Competency
www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862
 Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Failed back spine surgery
 Failed back spine surgery Presentation Definition Etiology Prevalence Evaluation Treatment Case study FBSS: Definition A constellation of conditions that describes persistent or recurring low back pain,
Failed back spine surgery Presentation Definition Etiology Prevalence Evaluation Treatment Case study FBSS: Definition A constellation of conditions that describes persistent or recurring low back pain,
Significant nerve damage is uncommonly associated with a general anaesthetic
 Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Intra-operative Nerve Monitoring Coding Guide. March 1, 2011
 Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
NIM EMG Endotracheal Tube
 NIM EMG Endotracheal Tube Product Information and Instructions REF I.D. (mm) O.D. (mm) FR# 9450060 6.0 8.8 27 9450061 7.0 10.2 31 9450062 8.0 11.3 34 Rx Only INTENDED USE AND DEVICE DESCRIPTION The NIM
NIM EMG Endotracheal Tube Product Information and Instructions REF I.D. (mm) O.D. (mm) FR# 9450060 6.0 8.8 27 9450061 7.0 10.2 31 9450062 8.0 11.3 34 Rx Only INTENDED USE AND DEVICE DESCRIPTION The NIM
Spinal Discectomy & Decompression Surgery
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Sacrodyny- Pain in the iliosacral jointcauses and therapy procedure
 Sacrodyny- Pain in the iliosacral jointcauses and therapy procedure The problem Perhaps, you have heard about the following clinical history: A patient, who had got a slipped disc and was treated successfully
Sacrodyny- Pain in the iliosacral jointcauses and therapy procedure The problem Perhaps, you have heard about the following clinical history: A patient, who had got a slipped disc and was treated successfully
MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER
 MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER This case is decided pursuant to Chapter 410 of the Texas Workers Compensation Act and Rules of the Division of Workers Compensation
MEDICAL CONTESTED CASE HEARING NO 12090 M6-12-38043-01 DECISION AND ORDER This case is decided pursuant to Chapter 410 of the Texas Workers Compensation Act and Rules of the Division of Workers Compensation
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
THYMECTOMY. Thymectomy. Common questions patients ask about thymectomies. www.myasthenia.org
 THYMECTOMY Thymectomy Common questions patients ask about thymectomies. www.myasthenia.org The following are some of the most common questions asked when a thymectomy is being considered for adult and
THYMECTOMY Thymectomy Common questions patients ask about thymectomies. www.myasthenia.org The following are some of the most common questions asked when a thymectomy is being considered for adult and
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Fall 2011. Pain Consult A physician newsletter from the Department of Pain Management
 Fall 2011 Pain Consult A physician newsletter from the Department of Pain Management Dear Colleague, Cooled Radiofrequency Ablation New treatment shows promise for long-term relief of certain chronic back
Fall 2011 Pain Consult A physician newsletter from the Department of Pain Management Dear Colleague, Cooled Radiofrequency Ablation New treatment shows promise for long-term relief of certain chronic back
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis
 Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Cervical Spine Radiculopathy: Convervative Treatment. Christos K. Yiannakopoulos, MD Orthopaedic Surgeon
 Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg
 Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg Pain after Lumbar Surgery A Prospective Study to Describe Costs, Complications, and Patient Outcomes: Final Report September
Spinal Cord Stimulators (SCS) for Injured Workers with Chronic Back and Leg Pain after Lumbar Surgery A Prospective Study to Describe Costs, Complications, and Patient Outcomes: Final Report September
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California.
 Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY
 CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY ANESTHESIA BILLING: MUST BE DOCUMENTED AS: Personally performed: you perform the case without a resident or a CRNA
CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY ANESTHESIA BILLING: MUST BE DOCUMENTED AS: Personally performed: you perform the case without a resident or a CRNA
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
OU Medical System Safe Procedural and Surgical Verification
 OU Medical System Safe Procedural and Surgical Verification I hereby attest that I am aware of OUMS Safe Procedural and Surgical Verification process. I have received a copy of the OUMS Policy on Safe
OU Medical System Safe Procedural and Surgical Verification I hereby attest that I am aware of OUMS Safe Procedural and Surgical Verification process. I have received a copy of the OUMS Policy on Safe
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
PAIN MANAGEMENT AT UM/SYLVESTER
 PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions
 Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions Q: What is the thyroid gland? A: The thyroid is a butterfly-shaped gland located in the front of the neck. It is one of the
Thyroid Surgery at Massachusetts General Hospital Frequently Asked Questions Q: What is the thyroid gland? A: The thyroid is a butterfly-shaped gland located in the front of the neck. It is one of the
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
3M Steri-Strip S Surgical Skin Closure. Commonly Asked Questions
 3M Steri-Strip S Surgical Skin Closure Commonly Asked Questions What are the indications for use of 3M Steri-Strip S Surgical Skin Closure? Steri-Strip S Surgical Skin Closures are indicated as a primary
3M Steri-Strip S Surgical Skin Closure Commonly Asked Questions What are the indications for use of 3M Steri-Strip S Surgical Skin Closure? Steri-Strip S Surgical Skin Closures are indicated as a primary
New Paradigms in Spinal Cord Stimulation. Steven Falowski MD
 New Paradigms in Spinal Cord Stimulation Steven Falowski MD Objectives Background of SCS Mechanisms of Action Indications Equipment Placement Introduction Spinal cord stimulation (SCS) delivers electrical
New Paradigms in Spinal Cord Stimulation Steven Falowski MD Objectives Background of SCS Mechanisms of Action Indications Equipment Placement Introduction Spinal cord stimulation (SCS) delivers electrical
Spinal cord stimulation
 Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Spinal cord stimulation This leaflet aims to answer your questions about having spinal cord stimulation. It explains the benefits, risks and alternatives, as well as what you can expect when you come to
Coding and Payment Guide for Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management
 Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
THE BULLETIN. MEDICAL COSTS AND HOW THEY ARE INCREASING THE COSTS OF YOUR CLAIMS page 1. COMING ATTRACTIONS page 5
 October 2010 THE BULLETIN Contents: MEDICAL COSTS AND HOW THEY ARE INCREASING THE COSTS OF YOUR CLAIMS page 1 COMING ATTRACTIONS page 5 Editor: JONATHAN S. WEBER Medical Costs and How They Are Increasing
October 2010 THE BULLETIN Contents: MEDICAL COSTS AND HOW THEY ARE INCREASING THE COSTS OF YOUR CLAIMS page 1 COMING ATTRACTIONS page 5 Editor: JONATHAN S. WEBER Medical Costs and How They Are Increasing
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
