Guidelines and References
|
|
|
- Sybil Carroll
- 7 years ago
- Views:
Transcription
1 ACCF 2013 Appropriate Use Criteria for Peripheral Vascular Ultrasound and Physiological Testing Part II: Testing for Venous Disease and Evaluation of Hemodialysis Access Guidelines and References
2 Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency and Thrombosis Indication Limb Swelling 1. Unilateral acute American College of Radiology. ACR Appropriateness Criteria. Suspected Upper Extremity Deep Vein Thrombosis Clinical condition: Suspected upper-extremity deep vein thrombosis. Rating upper extremity ultrasound with Doppler 9 (highest, usually appropriate) American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised III. The indications for peripheral venous ultrasound examinations include, but are not limited to: 1. Evaluation of possible venous thromboembolic disease or venous obstruction in symptomatic or high-risk asymptomatic individuals. 2. Assessment of venous insufficiency, reflux, and varicosities 3. Assessment of dialysis access. 4. Venous mapping prior to surgical procedures 5. Evaluation of veins prior to venous access. Follow-up of patients with known venous thrombosis near the end of anticoagulation to determine if residual venous thrombosis is present. 2. Unilateral chronic, persistent 3. Bilateral acute
3 Suspected central venous obstruction 4. Bilateral chronic, persistent No alternative diagnosis identified (e.g., no CHF or anasarca from hypoalbuminemia) Suspected central venous obstruction Limb Pain (Without Swelling) 5. Non-articular pain in the upper extremity (no indwelling upper extremity venous catheter) 6. Non-articular pain in the upper extremity with indwelling upper extremity venous catheter 7. Tender, palpable cord in the upper extremity Shortness of Breath 8. Suspected pulmonary embolus (no indwelling upper extremity venous catheter) 9. Suspected pulmonary embolus with indwelling upper extremity venous catheter. 10. Diagnosed pulmonary embolus (no indwelling upper extremity venous catheter) 11. Diagnosed pulmonary embolus with indwelling upper extremity venous catheter. Fever 12. Fever of unknown origin (no indwelling upper extremity venous catheter) 13. Fever with indwelling upper extremity venous catheter Known Upper Extremity Venous Thrombosis 14. New upper extremity pain or swelling while on anticoagulation 15. New upper extremity pain or swelling, not on anticoagulation (i.e., contraindication to anticoagulation)
4 16. Before anticipated discontinuation of anticoagulation treatment 17. Shortness of breath in a patient with known upper extremity DVT 18. Surveillance after diagnosis of upper extremity superficial phlebitis Not on anticoagulation, phlebitis location < 5 cms from deep vein junction 19. Surveillance after diagnosis of upper extremity superficial phlebitis Not on anticoagulation, phlebitis location > 5 cms from deep vein junction Vein Mapping Prior to Bypass Surgery (Coronary or Peripheral) 20. In the absence of adequate leg vein for harvest 21. In the presence of adequate leg vein for harvest Screening Examination for Upper Extremity DVT 22. Prior to pacemaker or implantable cardiac defibrillator placement 23. Prolonged ICU stay (e.g., > 4 days) No indwelling upper extremity venous catheter 24. Prolonged ICU stay (e.g., > 4 days) with indwelling upper extremity venous catheter 25. Monitoring indwelling upper extremity venous catheter that is functional 26. In those with high-risk: acquired, inherited or hypercoagulable state 27. Positive D-dimer test in a hospital inpatient Screening examination performed in the absence of upper extremity pain or swelling References: American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised American College of Radiology. ACR Appropriateness Criteria. Suspected Upper Extremity Deep Vein Thrombosis. Last updated 2011.
5 Bates, Shannon M, Jaeschke R, Stevens SM, et al. Diagnosis of DVT. Antithrombotic Therapy and Prevention of Thrombosis 9 th ED: American College of Chest Physicians. Evidence Based Practice Guidelines Chest 2012;141(2):1412S1. Constans J, Salmi LR, Sevestre-Pietri MA, et al. A clinical prediction score for upper extremity deep venous thrombosis. Thromb Haemost. 2008;99: Lower Extremity Venous Evaluation Table 2. Venous Duplex of the Lower Extremities for Patency and Thrombosis Indication Limb Swelling 28. Unilateral acute American College of Radiology. ACR Appropriateness Criteria on Suspected Lower Extremity Deep Vein Thrombosis. J Am Coll Radiol 2011;8: Clinical condition: Suspected Lower Extremity DVT. Ultrasound, lower extremity with Doppler with compression Rating 9 (highest, usually appropriate) Joint American Academy of Family Physicians/American College of Physicians Panel on Deep Venous Thrombosis/Pulmonary Embolism. Current diagnosis of venous thromboembolism in primary care: a clinical practice guideline from the American Academy of Family Physicians and the American College of Physicians. Ann Intern Med Mar 20;146(6): Recommendation 3: Ultrasound is recommended for patients with intermediate to high pretest probability of DVT in the lower extremities. American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound
6 29. Unilateral chronic, persistent 30. Bilateral acute 31. Bilateral chronic, persistent No alternative diagnosis identified (e.g., no CHF or anasarca from hypoalbuminemia) Limb Pain (Without Swelling) Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised III. The indications for peripheral venous ultrasound examinations include, but are not limited to: 1. Evaluation of possible venous thromboembolic disease or venous obstruction in symptomatic or high-risk asymptomatic individuals. 2. Assessment of venous insufficiencym, reflux, and varicosities 3. Assessment of dialysis access. 4. Venous mapping prior to surgical procedures 5. Evaluation fo veins prior to venous access. 6. Follow-up of patients with known venous thrombosis near the end of anticoagulation to determine if residual venous thrombosis is present. 32. Non-articular pain in the lower extremity (e.g., calf or thigh) 33. Knee pain 34. Tender, palpable cord in the lower extremity Shortness of Breath 35. Suspected pulmonary embolus 36. Diagnosed pulmonary embolus Fever
7 37. Fever of unknown origin (no indwelling lower extremity venous catheter) 38. Fever with indwelling lower extremity venous catheter Known Lower Extremity Venous Thrombosis 39. Surveillance of calf vein thrombosis for proximal propagation in patient with contraindication to anticoagulation (within 2 weeks of diagnosis) 40. New lower extremity pain or swelling while on anticoagulation 41. New lower extremity pain or swelling, not on anticoagulation (i.e., contraindication to anticoagulation) 42. Before anticipated discontinuation of anticoagulation treatment 43. Shortness of breath in a patient with known lower extremity DVT 44. Surveillance after diagnosis of lower extremity superficial phlebitis Not on anticoagulation, phlebitis location < 5 cms from deep vein junction 45. Surveillance after diagnosis of lower extremity superficial phlebitis Not on anticoagulation, phlebitis location > 5 cms from deep vein junction Vein Mapping Prior to Bypass Surgery (Coronary or Peripheral) 46. In the absence of prior lower extremity vein harvest or ablation procedure 47. In the presence of prior lower extremity vein harvest or ablation procedure Screening Examination for Lower Extremity DVT 48. After orthopedic surgery American Academy of Orthopaedic Surgeons Clinical Practice Guideline Summary. Prevention of Sypmtomatic Pulmonary Embolism in Patients Undergoing Total Hip or Knee Arthoplasty. Journal of the American Academic of Orthopaedic Surgeons 2009; 17:183. Recommend against routine post-operative duplex ultrasonography screening of patients who undergo elective hip or knee arthroplasty. (Grade of Recommendation: Strong) American College of Chest Physicians Evidence-Based Clinical
8 Practice Guidelines (8th Edition). Prevention of Venous Thromboembolism. Chest 2008 June;133(6 Suppl):381S-453S For asymptomatic patients following major orthopedic surgery, we recommend against the routine use of DUS screening before hospital discharge (Grade 1A). 49. Prolonged ICU stay (e.g., > 4 days) 50. In those with high-risk: acquired, inherited or hypercoagulable state 51. Positive D-dimer test in a hospital inpatient Post Endovenous (Great or Small) Saphenous Ablation 52. Lower extremity swelling or pain 53. Routine post procedural follow-up, no lower extremity pain or swelling Within 10 days post procedure Other Symptoms or Signs of Vascular Disease 54. Physiologic testing positive for venous obstruction 55. Patent foramen ovale with suspected paradoxical embolism for patient without lower extremity pain or swelling obstruction Screening examination performed in the absence of lower extremity pain or swelling References: AbuRahma AF, Saiedy S, Robinson PA, et al. Role of Venous Duplex Imaging of the Lower Extremities in Patients with Fever of Unknown Origin. Surgery ;121: Bates, Shannon M, Jaeschke R, Stevens SM, et al. Diagnosis of DVT. Antithrombotic Therapy and Prevention of Thrombosis 9 th ED: American College of Chest Physicians. Evidence Based Practice Guidelines Chest 2012;141(2):1412S1 American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised 2010.
9 Geerts WH, Bergqvist D, Pineo GF et al. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008 June;133(6 Suppl):381S-453S. Ho VB, van Geertruyden PH, Yucel EK, et al. American College of Radiology. ACR Appropriateness Criteria on Suspected Lower Extremity Deep Vein Thrombosis. J Am Coll Radiol 2011;8: Johanson NA, Lachiewicz PF, Lieberman JR, et al. American Academy of Orthopaedic Surgeons Clinical Practice Guideline Summary. Prevention of Sypmtomatic Pulmonary Emoblism in Patients Undergoing Total Hip or Knee Arthoplasty. Journal of the American Academic of Orthopaedic Surgeons 2009; 17:183. Kazmers A, Groehn H, Meeker C. Do patients with Acute Deep Vein Thrombosis Have Fever? Am Surg. 2000;66: Mourad O, Palda V, Detsky AS. A Comprehensive Evidence-Based approach to Fever of Unknown Origin. Arch Intern Med. 2003;163: Qaseem A, et al; Joint American Academy of Family Physicians/American College of Physicians Panel on Deep Venous Thrombosis/Pulmonary Embolism. Current diagnosis of venous thromboembolism in primary care: a clinical practice guideline from the American Academy of Family Physicians and the American College of Physicians. Ann Intern Med Mar 20;146(6): Table 3. Duplex Evaluation for Venous Incompetency Indication Venous Insufficiency (Venous Duplex with Provocative Maneuvers for Incompetency) Appropriate Use Rating 56. Active venous ulcer International Union of Phlebology consensus document. Part I. 57. Healed venous ulcer Basic principles. Eur J Vasc Endovasc Surg Jan;31(1): Epub 2005 Oct Spider veins (telangiectasias) 59. Varicose veins, entirely asymptomatic 60. Varicose veins with lower extremity pain or heaviness Primary uncomplicated great saphenous territory varicose veins
10 61. Visible varicose veins with chronic lower extremity swelling or skin changes of chronic venous insufficiency (e.g., hyperpigmentation, lipodermatosclerosis) 62. Skin changes of chronic venous insufficiency without visible varicose veins (e.g., hyperpigmentation, lipodermatosclerosis) 63. Lower extremity pain or heaviness without signs of venous disease 64. Mapping prior to venous ablation procedure 65. Prior endovenous (great or small) saphenous ablation procedure with new or worsening varicose veins in the ipsilateral limb 66. Prior endovenous (great or small) saphenous ablation procedure with no residual symptoms. Whether all patients require scanning is debated. Clinical assessment with or without pocket (continuous wave, CW) Doppler will miss up to 30% of important connections from deep to superficial veins and information on affected veins when compared to duplex scanning Primary uncomplicated small saphenous territory varicose veins Duplex scanning is considered to be essential prior to treatment to determine whether there is a saphenopopliteal junction (SPJ), to record its level, and to show complex anatomy such as a common insertion with the gastrocnemius veins Non-saphenous varicose veins Veins such as those related to pelvic/perineal vein reflux, varices unrelated to the great or small saphenous veins, or isolated lateral thigh varicose veins will be demonstrated to indicate that saphenous ligation or stripping may not be required Recurrent varicose veins Duplex scanning is considered to be essential to establish the complex anatomy and haemodynamics of recurrent varices to show whether surgery or endovenous treatment is appropriate Chronic venous disease with complications Duplex scanning is considered to be essential to assess the relative involvement of the deep and superficial venous systems to predict the likely outcome after treating superficial disease alone and to select patients suitable for consideration of deep venous reconstruction Duplex ultrasound surveillance after treatment This may be used to assess the outcome of therapy and for early detection of recurrence. This is likely to be the only way to obtain level I evidence as to outcome in the future Explanation
11 Duplex ultrasonography can localise and specify the source of the venous problem to provide a map to help select best treatment and evaluate outcome for the venous problems discussed above. The care of patients with varicose veins and associated chronic venous diseases: clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg May;53(5 Suppl):2S-48S. 2.1 We recommend that in patients with chronic venous disease, a complete history and detailed physical examination are complemented by duplex scanning of the deep and superficial veins. The test is safe, noninvasive, cost-effective, and reliable. 1 A 7.3 We recommend duplex scanning for follow-up of patients after venous procedures who have symptoms or recurrence of varicose veins. Multi-disciplinary quality improvement guidelines for the treatment of lower extremity superficial venous insufficiency with ambulatory phlebectomy from the Society of Interventional Radiology, Cardiovascular Interventional Radiological Society of Europe, American College of Phlebology and Canadian Interventional Radiology Association. J Vasc Interv Radiol 2010 January;21(1):1-13. Duplex ultrasound is essential in all patients with CEAP classification of C2 or higher and in patients with clinical symptoms of leg pain, swelling, or night cramps to identify relfux and patency and to establish the pattern of disease. American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound
12 Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised III. The indications for peripheral venous ultrasound examinations include, but are not limited to: Assessment of venous insufficiency, reflux, and varicosities References: American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Peripheral Venous Ultrasound Examination. Revised Coleridge-Smith P, Labropoulos N, Partsch H, et al. Duplex ultrasound investigation of the veins in chronic venous disease of the lower limbs--uip (International Union of Phlebology) consensus document. Part I. Basic principles. Eur J Vasc Endovasc Surg Jan;31(1): Epub 2005 Oct 14. Gloviczki P, Comerota AJ, Dalsing MC, et al. The care of patients with varicose veins and associated chronic venous diseases: clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg May;53(5 Suppl):2S-48S. Kundu S, Grassi CJ, Khilnani NM et al. Multi-disciplinary quality improvement guidelines for the treatment of lower extremity superficial venous insufficiency with ambulatory phlebectomy from the Society of Interventional Radiology, Cardiovascular Interventional Radiological Society of Europe, American College of Phlebology and Canadian Interventional Radiology Association. J Vasc Interv Radiol 2010 January;21(1):1-13. Table 4. Venous Physiological Testing (Plethysmography) With Provocative Maneuvers to Assess for Patency and/or Incompetency Appropriate Use Rating Indication Limb Pain, Swelling or Other Signs of Venous Disease 67. Active venous ulcer The care of patients with varicose veins and associated
13 68. Varicose veins, entirely asymptomatic chronic venous diseases: clinical practice guidelines of the Society for Vascular Surgery and the American Venous 69. Varicose veins with lower extremity pain or heaviness Forum. J Vasc Surg May;53(5 Suppl):2S-48S. 70. Varicose veins with chronic lower extremity swelling or skin changes of chronic venous insufficiency (e.g., hyperpigmentation or lipodermatosclerosis) 71. Skin changes of chronic venous insufficiency without visible varicose veins (e.g., hyperpigmentation or lipodermatosclerosis) 72. Lower extremity pain or heaviness without signs of venous disease 73. Limb swelling: unilateral acute Suspected acute venous thrombosis Shortness of Breath 74. Suspected pulmonary embolus 3.1 We suggest that venous plethysmography be used selectively for the noninvasive evaluation of the venous system in patients with simple varicose veins (CEAP class C2 ). 2 C 3.2 We recommend that venous plethysmography be used for the noninvasive evaluation of the venous system in patients with advanced chronic venous disease if duplex scanning does not provide definitive information on pathophysiology (CEAP class C3 -C6). 1 B References: Gloviczki P, Comerota AJ, Dalsing MC, et al. The care of patients with varicose veins and associated chronic venous diseases: clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg May;53(5 Suppl):2S-48S. Duplex Evaluation of the Inferior Vena Cava (IVC) and Iliac Veins Table 5. Duplex of the IVC and Iliac Veins for Patency and Thrombosis Indication Prior to IVC Filter Placement Appropriate Use Rating
14 75. Prior to IVC filter placement For procedural access planning Evaluation for Suspected Deep Vein Thrombosis 76. Lower extremity swelling - unilateral or bilateral as a stand alone test without a venous duplex of the lower extremities 77. Lower extremity swelling unilateral or bilateral combined routinely with a venous duplex of the lower extremities 78. Lower extremity swelling unilateral or bilateral performed selectively when the lower extremity venous duplex is normal 79. Lower extremity swelling unilateral or bilateral performed selectively when the lower extremity venous duplex is positive for acute proximal DVT 80. Selectively - When the flow pattern in one or both common femoral veins is abnormal Evaluation for Suspected Pulmonary Embolus 81. Pulmonary symptoms (suspected pulmonary embolus) - as a stand alone test without a venous duplex of the lower extremities 82. Pulmonary symptoms (suspected pulmonary embolus) combined routinely with a venous duplex of the lower extremities Evaluation of Other Symptoms or Signs of Abdominal Vascular Disease 83. Abdominal pain 84. Abdominal bruit 85. Fever of unknown origin
15 Hepatoportal and Renal Venous Evaluation Table 6. Duplex of the Hepatoportal System (portal vein, hepatic veins, splenic vein, superior mesenteric vein, inferior vena cava) for patency, thrombosis, and flow direction Indication Evaluation of Hepatic Dysfunction or Portal Hypertension 86. Abnormal liver function tests No alternative diagnosis identified (e.g., medication related or infectious hepatitis) 87. Cirrhosis with or without ascites 88. Jaundice As an initial diagnostic test 89. Jaundice No alternative diagnosis identified after initial evaluation (e.g., no biliary obstruction) 90. Hepatomegaly and/or splenomegaly 91. Portal hypertension Surveillance following Portal Decompression Procedure Appropriate Use Rating 92. Follow-up of a TIPS American Association for the Study of Liver Diseases Practice Guidelines: the role of transjugular intrahepatic portosystemic shunt creation in the management of portal hypertension. J Vasc Interv Radiol May;16(5): Recommendation 9: Each center performing TIPS should have an established program of TIPS surveillance and although there are no established guidelines, Doppler ultrasound should be performed before the patient is
16 Evaluation of Other Symptoms or Signs of Abdominal Vascular Disease 93. Abdominal pain 94. Fever of unknown origin Evaluation of Cardiac and/or Pulmonary Symptoms 95. Pulmonary symptoms (suspected pulmonary embolus) 96. Cor pulmonale discharged from the hospital and at specified intervals following the procedure and the yearly anniversary of the TIPS therafter (evidence: grade II-1). Recommendation11: TIPS stenosis is common, especially in the first year, and Doppler ultrasound lacks the sensitivity and specificity needed to identify many of these patients. Therefore, repeat catheterization of the TIPS or upper endoscopy should be performed at the 1-year anniversary of placement, especially in those patients who bled from varices (evidence: grade II-3). American Association for the Study of Liver Diseases Practice Guidelines: the role of transjugular intrahepatic portosystemic shunt creation in the management of portal hypertension. J Vasc Interv Radiol May;16(5): Recommendation 10: Ultrasonographic findings suggesting TIPS dysfunction or recurrence of the complication of portal hypertension that lead to the initial TIPS should lead to venography and intervention, as indicated. The recurrence of symptoms in the face of a normal ultrasound does not eliminate the need for TIPS venography (evidence: grade II- 2). Testing indications refer to evaluation of native hepatoportal venous system only (i.e. hepatic transplant sites and arterial system excluded).
17 References: Boyer TD, Haskal ZJ. American Association for the Study of Liver Diseases Practice Guidelines: the role of transjugular intrahepatic portosystemic shunt creation in the management of portal hypertension. J Vasc Interv Radiol May;16(5): Table 7. Duplex of the Renal Veins for Patency and Thrombosis Indication Evaluation for Suspected Renal Vein Thrombosis Potential Signs and/or Symptoms 97. Gross hematuria 98. Acute renal failure 99. Acute flank pain Evaluation of Cardiac and/or Pulmonary Symptoms 100. Pulmonary symptoms (suspected pulmonary embolus) Evaluation of Other Symptoms or Signs of Abdominal Vascular Disease 101. Drug-resistant hypertension (suspected renal artery stenosis) 102. Microscopic hematuria (prior to urological evaluation) 103. Fever of unknown origin 104. Epigastric bruit Appropriate Use Rating Testing indications refer to evaluation of native renal veins only for patency (i.e. renal transplant sites and renal arteries excluded).
18 Hemodialysis Vascular Access Duplex Ultrasound Table 8. Preoperative Planning and Postoperative Assessment of a Vascular Access Site* Indication Assessment Prior to Access Site Placement* 105. Preoperative Mapping Study (Upper extremity arterial and venous duplex) 3 months prior to access placement Appropriate Use Rating K/DOQI Clinical Practice Recommendations for Vascular Access; 2001, updated Evaluation that should be performed before placement of a permanent hemodialysis access include: History and physical examination (B) Duplex ultrasound of the upper extremity arteries and veins (B) Central vein evaluation in the appropriate patient known to have a previous catheter or pacemaker (A) 2006 update: 1.4 Alternative imaging studies for the central veins include DDU (sic: duplex ultrasound) and magnetic resonance imaging/mra. American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access. Revised II. Indications for vascular mapping for preoperative planning of dialysis access include planning of vascular access for hemodialysis. There are no absolute
19 106. Preoperative Mapping Study (Upper extremity arterial and venous duplex) <3 months prior to access placement Failure to Mature 107. Failure to Mature on basis of physical examination 0-6 weeks after placement 108. Failure to Mature on basis of physical examination > 6 weeks after placement Symptoms and Signs of Disease 109. Signs of access site malfunction during dialysis (e.g., low blood flows, kt/v, recirculation times or increased venous pressure) contraindications for this examination. K/DOQI Clinical Practice Recommendations for Vascular Access; 2001, updated If a fistula fails to mature by 6 weeks, a fistulogram or other imaging study should be obtained to determine the cause of the problem (B) American College of Radiology/American Institute of Ultrasound in Medicine Practice Guideline for the Performance of Vascular Ultrasound for Postoperative Assessment of Dialysis Access. Published II. Indications for dialysis access ultrasound include, but are not limited to: 1. Patients with decreased flow rates during hemodialysis 2. Patients with development of arm swelling or discomfort after access placement surgery or a hemodialysis session 3. Patients with prolonged immaturity of a surgically created AVF 4. Patients suspected of having a pseduoaneurysm, AVF or graft stenosis, or adjacent fluid collection The Society for Vascular Surgery: clinical practice guidelines for the surgical placement and maintenance of arteriovenous hemodialysis access. J Vasc Surg 2008 November;48(5 Suppl):2S-25S. Recommendation 5.A. We recommend regular clinical
20 monitoring (inspection, palpation, ausculatation, and monitoring for prolonged bleeding after needle withdrawal) to detect access dysfunction (Grade 1, very low-quality evidence). Recommendation 5.B. We suggest access flow monitoring or static dialysis venous pressures for routine surveillance (Grade 2, very low quality evidence). Recommendation 5.C. We suggest performing a Duplex ultrasound (DU) study or contrast imaging study in accesses that display clinical signs of dysfunction or abnormal routine surveillance (Grade 2, very low-quality evidence) K/DOQI Clinical Practice Recommendations for Vascular Access; 2001, updated Techniques, not mutually exclusive, that may be used in surveillance for stenosis in grafts include: Preferred Intra-access flow by using 1 of several methods(a) Directly measured or derived status venous dialysis pressure by 1 of several methods (A) Duplex ultrasound (A) 4.3 Techniques, not mutually exclusive, that may be used in surveillance for stenosis in AVFs include: Preferred Direct flow measurements (A) Physical findings of persistent swelling of the arm, presence of collateral veins, prolonged bleeding after needle withdrawal, or altered characteristics of pulse or thrill in the outflow vein (A)
21 Duplex ultrasound American College of Radiology/American Institute of Ultrasound in Medicine Practice Guideline for the Performance of Vascular Ultrasound for Postoperative Assessment of Dialysis Access. Published II. Indications for dialysis access ultrasound include, but are not limited to: 5. Patients with decreased flow rates during hemodialysis 6. Patients with development of arm swelling or discomfort after access placement surgery or a hemodialysis session 7. Patients with prolonged immaturity of a surgically created AVF 8. Patients suspected of having a pseduoaneurysm, AVF or graft stenosis, or adjacent fluid collection 110. Mass associated with an AVF/AVG 111. Loss of palpable thrill of AVF/AVG 112. Arm swelling 113. Hand pain, pallor, and/or digital ulceration (i.e., evaluation for suspected arterial steal syndrome) 114. Cool extremity Without pain, pallor, or ulceration 115. Difficult cannulation by multiple personnel on multiple attempts Asymptomatic 116. Routine surveillance of a functioning AVF or AVG The Society for Vascular Surgery: clinical practice guidelines for the surgical placement and maintenance of arteriovenous hemodialysis access. J Vasc Surg 2008 November;48(5 Suppl):2S-25S. Recommendation 5.A. We recommend regular clinical monitoring (inspection, palpation, ausculatation, and
22 monitoring for prolonged bleeding after needle withdrawal) to detect access dysfunction (Grade 1, very low-quality evidence). Recommendation 5.B. We suggest access flow monitoring or static dialysis venous pressures for routine surveillance (Grade 2, very low quality evidence). Recommendation 5.C. We suggest performing a Duplex ultrasound (DU) study or contrast imaging study in accesses that display clinical signs of dysfunction or abnormal routine surveillance (Grade 2, very low-quality evidence) K/DOQI Clinical Practice Recommendations for Vascular Access; 2001, updated Techniques, not mutually exclusive, that may be used in surveillance for stenosis in grafts include: Preferred Intra-access flow by using 1 of several methods(a) Directly measured or derived status venous dialysis pressure by 1 of several methods (A) Duplex ultrasound (A) 4.3 Techniques, not mutually exclusive, that may be used in surveillance for stenosis in AVFs include: Preferred Direct flow measurements (A) Physical findings of persistent swelling of the arm, presence of collateral veins, prolonged bleeding after needle withdrawal, or altered characteristics of pulse or thrill in the outflow vein (A) Duplex ultrasound
23 *Ultrasound assessment prior to creation of dialysis access (AVF or AVG) typically includes a combined arterial and venous duplex examination that is performed to determine the adequacy of superficial veins (patency, size, and length of conduit), patency of central venous outflow, and adequacy of adequate arterial inflow. Determination of central venous patency is particularly important for patients with a history of prior central venous catheter(s). In a mature AVF or AVG that is being accessed for hemodialysis References: American College of Radiology/American Institute of Ultrasound in Medicine/Society for Radiologists in Ultrasound Practice Guideline for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access. Revised American College of Radiology/American Institute of Ultrasound in Medicine Practice Guideline for the Performance of Vascular Ultrasound for Postoperative Assessment of Dialysis Access. Published Casey ET, Murad MH, Rizvi AZ, et al. Surveillance of Arteriovenous Hemodialysis Access: a Systematic Review and Meta-analysis. J Vasc Surg Nov;48(5 Suppl):48S-54S. National Kidney Foundation K/DOQI Clinical Practice Recommendations for Vascular Access; 2001, updated Available at: Sidawy AN, Spergel LM, Besarab A et al. The Society for Vascular Surgery: Clinical Practice Guidelines for the Surgical Placement and Maintenance of Arteriovenous Hemodialysis Access. J Vasc Surg 2008 November;48(5 Suppl):2S-25S. Umphrey HR, Lockhart ME, Abts CA, Robbin ML. Dialysis Grafts and Fistulae: Planning and Assessment. Ultrasound Clin 2011;6(4): Robbin ML, Chamberlain NE, Lockhart ME, Gallichio MH, Young CJ, Deierhoi MH, Allon MA. Hemodialysis Arteriovenous Fistula Maturity: US Evaluation. Radiology 2002;225(1): Singh P, Robbin ML, Lockhart ME, Allon M. Clinically Immature Arteriovenous Hemodialysis Fistulas: Effect of US on Salvage. Radiology 2008;246(1):
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Surgical Options for Venous Disease. Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart
 Surgical Options for Venous Disease Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart Chronic Venous Disease Approximately 23% of adults in the US have varicose veins Estimated 22 million women
Surgical Options for Venous Disease Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart Chronic Venous Disease Approximately 23% of adults in the US have varicose veins Estimated 22 million women
Effective Date: March 2, 2016
 Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Catheter Reduction Program: Creating the Ideal Vascular Access Culture. Presented by: Diane Peck, RN, CNN
 Catheter Reduction Program: Creating the Ideal Vascular Access Culture Presented by: Diane Peck, RN, CNN Fistula First Initiative The superiority of an AVF over an AVG is an accepted fact. For this reason
Catheter Reduction Program: Creating the Ideal Vascular Access Culture Presented by: Diane Peck, RN, CNN Fistula First Initiative The superiority of an AVF over an AVG is an accepted fact. For this reason
EFSUMB EUROPEAN FEDERATION OF SOCIETIES FOR ULTRASOUND IN MEDICINE AND BIOLOGY Building a European Ultrasound Community
 MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 8: Vascular Ultrasound Level 1 Training and Practice Practical training should involve at least two half day ultrasound
MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 8: Vascular Ultrasound Level 1 Training and Practice Practical training should involve at least two half day ultrasound
MEDICAL COVERAGE POLICY. SERVICE: Varicose Veins of the Lower Extremities. PRIOR AUTHORIZATION: Required.
 Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
Local Coverage Determination (LCD): Non-Invasive Peripheral Venous Vascular and Hemodialysis Access Studies (L35751)
 Local Coverage Determination (LCD): Non-Invasive Peripheral Venous Vascular and Hemodialysis Access Studies (L35751) Contractor Information Contractor Name Wisconsin Physicians Service Insurance Corporation
Local Coverage Determination (LCD): Non-Invasive Peripheral Venous Vascular and Hemodialysis Access Studies (L35751) Contractor Information Contractor Name Wisconsin Physicians Service Insurance Corporation
Non-surgical treatment of severe varicose veins
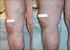 Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
Stenosis Surveillance 2009
 5 Diamond Patient Safety Program Stenosis Surveillance 2009 *This presentation was collaboratively developed by the Mid-Atlantic Renal Coalition (MARC) and the ESRD Network of New England for the 5-Diamond
5 Diamond Patient Safety Program Stenosis Surveillance 2009 *This presentation was collaboratively developed by the Mid-Atlantic Renal Coalition (MARC) and the ESRD Network of New England for the 5-Diamond
LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND:
 LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND: Chronic Venous Insufficiency Phillip J Bendick, PhD William Beaumont Hospital Royal Oak, Michigan Prevalence: Carotid ASO ~ 3M Peripheral Arterial Dz ~ 5M + CAD
LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND: Chronic Venous Insufficiency Phillip J Bendick, PhD William Beaumont Hospital Royal Oak, Michigan Prevalence: Carotid ASO ~ 3M Peripheral Arterial Dz ~ 5M + CAD
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery
 XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery Fast Facts: XARELTO is a novel, once-daily, oral anticoagulant recently approved in the United States for the prevention (prophylaxis)
XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery Fast Facts: XARELTO is a novel, once-daily, oral anticoagulant recently approved in the United States for the prevention (prophylaxis)
Venous Thromboembolic Treatment Guidelines
 Venous Thromboembolic Treatment Guidelines About the NYU Venous Thromboembolic Center (VTEC) The center s mission is to deliver advanced screening, detection, care, and management services for patients
Venous Thromboembolic Treatment Guidelines About the NYU Venous Thromboembolic Center (VTEC) The center s mission is to deliver advanced screening, detection, care, and management services for patients
Upper Extremity Vein Mapping for Placement of a Dialysis Access
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Vein Mapping for Placement of a Dialysis Access This Guideline was prepared by the Professional Guidelines Subcommittee of the Society
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Vein Mapping for Placement of a Dialysis Access This Guideline was prepared by the Professional Guidelines Subcommittee of the Society
Yes when meets criteria below
 Vein Disease Treatment MP9241 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Dean Health Plan covers
Vein Disease Treatment MP9241 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Dean Health Plan covers
Peninsula Commissioning Priorities Group. Commissioning Policy Varicose Vein Referral
 NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
Strategies to Reduce Catheter Use in 2014
 Strategies to Reduce Catheter Use in 2014 Timothy A. Pflederer, MD Chair, Network 10 MRB (I have no commercial affiliations or conflicts of interest to report) Fibrin Sheathing Central Venous Stenosis
Strategies to Reduce Catheter Use in 2014 Timothy A. Pflederer, MD Chair, Network 10 MRB (I have no commercial affiliations or conflicts of interest to report) Fibrin Sheathing Central Venous Stenosis
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis
 Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery
 Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery Position Statement There is currently insufficient data for the (AOFAS) to recommend for or against routine VTED prophylaxis for
Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery Position Statement There is currently insufficient data for the (AOFAS) to recommend for or against routine VTED prophylaxis for
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Spotlight Series: Interventional Radiology. Varicose Veins and Venous Insufficiency
 Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Venous and Lymphatic Disorders
 Venous and Lymphatic Disorders. ก. Venous and Lymphatic Disorders Varicose Veins Deep Vein Thrombosis (DVT) Lymphedema What Is Varicose Veins? Latin: Varicose = Varix = twisted Abnormal venous dilatation
Venous and Lymphatic Disorders. ก. Venous and Lymphatic Disorders Varicose Veins Deep Vein Thrombosis (DVT) Lymphedema What Is Varicose Veins? Latin: Varicose = Varix = twisted Abnormal venous dilatation
Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access
 predialysisaccess.qxp_0616 6/29/16 3:58 PM Page 1 AIUM Practice Parameter for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access Parameter developed in collaboration
predialysisaccess.qxp_0616 6/29/16 3:58 PM Page 1 AIUM Practice Parameter for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access Parameter developed in collaboration
Varicose veins and venous thrombosis: The latest treatment options
 Varicose veins and venous thrombosis: The latest treatment options DR ROBERT McBANE: I'm Rob McBane from the Vascular Center at Mayo Clinic in Rochester. Today we have the pleasure of talking with my esteemed
Varicose veins and venous thrombosis: The latest treatment options DR ROBERT McBANE: I'm Rob McBane from the Vascular Center at Mayo Clinic in Rochester. Today we have the pleasure of talking with my esteemed
Col league. SMMC Vascular Center Opens A PUBLICATION FOR SOUTHERN MAINE PHYSICIANS
 A PUBLICATION FOR SOUTHERN MAINE PHYSICIANS Col league 8 2012 SMMC Vascular Center Opens By Frank Lavoie, MD, Executive Vice President and Chief Operating Officer During the last year, Southern Maine Medical
A PUBLICATION FOR SOUTHERN MAINE PHYSICIANS Col league 8 2012 SMMC Vascular Center Opens By Frank Lavoie, MD, Executive Vice President and Chief Operating Officer During the last year, Southern Maine Medical
Clinical Medical Policy Varicose Vein Treatment
 Benefit Coverage Covered Benefit for lines of business including: Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Benefit Coverage Covered Benefit for lines of business including: Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Medical Affairs Policy
 Service: Varicose Vein Treatments PUM 250-0032 Medical Affairs Policy Implemented 04/04/14, 04/01/15, 4/1/16 Reviewed 12/12/14 Revised 12/12/14, 12/11/15 Developed Arise/WPS Policy 12/12/14, 12/11/15 Committee
Service: Varicose Vein Treatments PUM 250-0032 Medical Affairs Policy Implemented 04/04/14, 04/01/15, 4/1/16 Reviewed 12/12/14 Revised 12/12/14, 12/11/15 Developed Arise/WPS Policy 12/12/14, 12/11/15 Committee
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
Patient Information Understanding Varicose Veins
 Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
Clinical Review Criteria
 Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
Modern Varicose Vein Treatments: What Every Patient Should Know
 The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
Coding Companion for Radiology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Radiology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Diagnostic Radiology Head/Neck...1 Chest...38 Spine/Pelvis...51
Coding Companion for Radiology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Diagnostic Radiology Head/Neck...1 Chest...38 Spine/Pelvis...51
Confirmed Deep Vein Thrombosis (DVT)
 Confirmed Deep Vein Thrombosis (DVT) Information for patients What is deep vein thrombosis? Blood clotting provides us with essential protection against severe loss of blood from an injury to a vein or
Confirmed Deep Vein Thrombosis (DVT) Information for patients What is deep vein thrombosis? Blood clotting provides us with essential protection against severe loss of blood from an injury to a vein or
ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014
 ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014 Thromboembolism epidemiology 5 million DVT s 900,000 PE s 290,000 fatalities Heit J. Blood. 2005;106:910. 10 VTE events Since this talk began DVT
ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014 Thromboembolism epidemiology 5 million DVT s 900,000 PE s 290,000 fatalities Heit J. Blood. 2005;106:910. 10 VTE events Since this talk began DVT
CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE
 Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
treatment of varicose and spider veins patient information SAMPLE a publication by advancing vein care
 treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Vascular Technology (VT) Content Outline Anatomy & physiology 20% Cerebrovascular Cerebrovascular normal anatomy Evaluate the cerebrovascular vessels
 Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
SCREENING COMPRESSION ULTRASOUND FOR LOWER EXTREMITY DVT
 SCREENING COMPRESSION ULTRASOUND FOR LOWER EXTREMITY DVT R. Eugene Zierler, M.D. The D. E. Strandness, Jr. Vascular Laboratory University of Washington Medical Center Division of Vascular Surgery University
SCREENING COMPRESSION ULTRASOUND FOR LOWER EXTREMITY DVT R. Eugene Zierler, M.D. The D. E. Strandness, Jr. Vascular Laboratory University of Washington Medical Center Division of Vascular Surgery University
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
Delineation of Privileges Department of Surgery/Section of Vascular Surgery. Name: Please print or type
 University of Michigan Hospitals and Health Centers Delineation of Privileges Department of Surgery/Section of Vascular Surgery Name: Please print or type CORE PRIVILEGES VASCULAR SURGEON Vascular Surgery
University of Michigan Hospitals and Health Centers Delineation of Privileges Department of Surgery/Section of Vascular Surgery Name: Please print or type CORE PRIVILEGES VASCULAR SURGEON Vascular Surgery
Ultrasound in Vascular Surgery. Torbjørn Dahl
 Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Varicose veins - 1 -
 Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Published 2011 by the American Academy of Orthopaedic Surgeons 6300 North River Road Rosemont, IL 60018. AAOS Clinical Practice Guidelines Unit
 Volume 4. AAOS Clinical Guideline on Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty Comparison with Other Guidelines Disclaimer This clinical guideline
Volume 4. AAOS Clinical Guideline on Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty Comparison with Other Guidelines Disclaimer This clinical guideline
6/19/2012. Update on Venous Thromboembolism Prophylaxis. Disclosure. Learning Objectives. No conflicts of interest to declare
 Update on Venous Thromboembolism Prophylaxis Disclosure No conflicts of interest to declare Learning Objectives After completion of this presentation, participants should be able to: Define venous thromboembolism,
Update on Venous Thromboembolism Prophylaxis Disclosure No conflicts of interest to declare Learning Objectives After completion of this presentation, participants should be able to: Define venous thromboembolism,
MEDICAL COVERAGE POLICY SERVICE: Varicose Veins of the Lower Extremities. SERVICE: Treatment of Varicose Veins of the Lower Extremities
 Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your particular benefit plan. Each benefit
Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your particular benefit plan. Each benefit
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE
 CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
Pediatric Hemodialysis Access
 Pediatric Hemodialysis Access Vincent L. Rowe, M.D., FACS Professor of Surgery Division of Vascular Surgery Keck School of Medicine at University of Southern California NO FINANCIAL DISCLOSURES Outline
Pediatric Hemodialysis Access Vincent L. Rowe, M.D., FACS Professor of Surgery Division of Vascular Surgery Keck School of Medicine at University of Southern California NO FINANCIAL DISCLOSURES Outline
Varicose Veins Backgrounder
 What Are Varicose Veins? Varicose veins are a clinical presentation of superficial venous insufficiency a condition in which veins are inefficient in returning blood to the heart due to venous hypertension.
What Are Varicose Veins? Varicose veins are a clinical presentation of superficial venous insufficiency a condition in which veins are inefficient in returning blood to the heart due to venous hypertension.
Resection, Reduction, and Revision of Aneurysmal AV Fistulas
 Resection, Reduction, and Revision of Aneurysmal AV Fistulas Patrick R. Cook DO, FACS Timothy G. Canty Jr. MD Robert J. Hye MD, FACS Kaiser Permanente San Diego, CA Aneurysmal AVF Over last decade K-DOQI
Resection, Reduction, and Revision of Aneurysmal AV Fistulas Patrick R. Cook DO, FACS Timothy G. Canty Jr. MD Robert J. Hye MD, FACS Kaiser Permanente San Diego, CA Aneurysmal AVF Over last decade K-DOQI
Ultrasound - Vascular
 Scan for mobile link. Ultrasound - Vascular Vascular ultrasound uses sound waves to evaluate the body s circulatory system and help identify blockages and detect blood clots. A Doppler ultrasound study
Scan for mobile link. Ultrasound - Vascular Vascular ultrasound uses sound waves to evaluate the body s circulatory system and help identify blockages and detect blood clots. A Doppler ultrasound study
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796)
 Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L31796 LCD Title Varicose
Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L31796 LCD Title Varicose
Medical Coverage Policy Varicose Vein Treatment sad
 Medical Coverage Policy Varicose Vein Treatment sad EFFECTIVE DATE: 10 28 2001 POLICY LAST UPDATED: 05 07 2013 OVERVIEW Varicose veins are large superficial veins that have become swollen. These veins
Medical Coverage Policy Varicose Vein Treatment sad EFFECTIVE DATE: 10 28 2001 POLICY LAST UPDATED: 05 07 2013 OVERVIEW Varicose veins are large superficial veins that have become swollen. These veins
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH
 Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty
 Round Table: Antithrombotic therapy beyond ACS Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty M. Matsagkas, MD, PhD, EBSQ-Vasc Associate Professor
Round Table: Antithrombotic therapy beyond ACS Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty M. Matsagkas, MD, PhD, EBSQ-Vasc Associate Professor
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment
 Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment Lower Extremity Venous Anatomy Deep, Superficial, Perforating, Reticular veins Located in two separate compartments (deep and
Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment Lower Extremity Venous Anatomy Deep, Superficial, Perforating, Reticular veins Located in two separate compartments (deep and
Complications of Femoral Catheterization. Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005
 Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
Veins. Zapping Varicose. Venous diseases affect many people and represent a major cost to the health-care system.
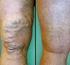 Zapping Varicose Veins Improving the Quality of Life for Sufferers By Jeannette Soriano, MD Venous diseases affect many people and represent a major cost to the health-care system. Hippocrates used compression
Zapping Varicose Veins Improving the Quality of Life for Sufferers By Jeannette Soriano, MD Venous diseases affect many people and represent a major cost to the health-care system. Hippocrates used compression
SEDICO Newsletter Issue 8. Varicose veins
 SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
HEART & VASCULAR SERVICES. Heart & Vascular Services www.mhsystem.org
 HEART & VASCULAR SERVICES Heart & Vascular Services www.mhsystem.org Heart Services Testing Before Your Procedure If you are scheduled for a procedure in the catheterization lab, there will be blood work
HEART & VASCULAR SERVICES Heart & Vascular Services www.mhsystem.org Heart Services Testing Before Your Procedure If you are scheduled for a procedure in the catheterization lab, there will be blood work
Optimal Management of Splenic/Portal Vein Thrombosis. David Mauchley University of Colorado
 Optimal Management of Splenic/Portal Vein Thrombosis David Mauchley University of Colorado Overview Portal Vein Thrombosis (PVT) Etiology Presentation/Clinical Aspects Diagnosis Management Cirrhotic vs.
Optimal Management of Splenic/Portal Vein Thrombosis David Mauchley University of Colorado Overview Portal Vein Thrombosis (PVT) Etiology Presentation/Clinical Aspects Diagnosis Management Cirrhotic vs.
Suffering from varicose veins? Patient Information. ELVeS Radial Minimally invasive laser therapy of venous insufficiency
 Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Health Technology Assessment of Scheduled Surgical Procedures
 HTA of Scheduled Surgical Procedures April 2013 Health Technology Assessment of Scheduled Surgical Procedures Varicose Vein Surgery April 2013 Safer Better Care About the The (HIQA) is the independent
HTA of Scheduled Surgical Procedures April 2013 Health Technology Assessment of Scheduled Surgical Procedures Varicose Vein Surgery April 2013 Safer Better Care About the The (HIQA) is the independent
Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC
 Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC 2015 Edition All Reimbursement Amounts are Listed at National Rates and Do Not Include the 2% Sequestration
Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC 2015 Edition All Reimbursement Amounts are Listed at National Rates and Do Not Include the 2% Sequestration
Recurrent Varicose Veins. Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio
 Recurrent Varicose Veins Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio Disclosures None Possible Causes of Recurrence DNA:
Recurrent Varicose Veins Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio Disclosures None Possible Causes of Recurrence DNA:
Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis
 Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Ch. 138 CARDIAC CATHETERIZATION SERVICES 28 138.1 CHAPTER 138. CARDIAC CATHETERIZATION SERVICES GENERAL PROVISIONS
 Ch. 138 CARDIAC CATHETERIZATION SERVICES 28 138.1 CHAPTER 138. CARDIAC CATHETERIZATION SERVICES Sec. 138.1 Principle. 138.2. Definitions. GENERAL PROVISIONS PROGRAM, SERVICE, PERSONNEL AND AGREEMENT REQUIREMENTS
Ch. 138 CARDIAC CATHETERIZATION SERVICES 28 138.1 CHAPTER 138. CARDIAC CATHETERIZATION SERVICES Sec. 138.1 Principle. 138.2. Definitions. GENERAL PROVISIONS PROGRAM, SERVICE, PERSONNEL AND AGREEMENT REQUIREMENTS
Trust Guideline for Thromboprophylaxis in Trauma and Orthopaedic Inpatients
 A clinical guideline recommended for use In: By: For: Key words: Department of Orthopaedics, NNUHT Medical staff Trauma & Orthopaedic Inpatients Deep vein thrombosis, Thromboprophylaxis, Orthopaedic Surgery
A clinical guideline recommended for use In: By: For: Key words: Department of Orthopaedics, NNUHT Medical staff Trauma & Orthopaedic Inpatients Deep vein thrombosis, Thromboprophylaxis, Orthopaedic Surgery
Preventing Blood Clots in Adult Patients. Information For Patients
 Preventing Blood Clots in Adult Patients Information For Patients 1 This leaflet will give you information on how to reduce the risk of developing blood clots during and after your stay in hospital. If
Preventing Blood Clots in Adult Patients Information For Patients 1 This leaflet will give you information on how to reduce the risk of developing blood clots during and after your stay in hospital. If
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Recanalized Umbilical Vein in the Presence of Cirrhosis-Induced Portal Hypertension
 Recanalized Umbilical Vein in the Presence of Cirrhosis-Induced Portal Hypertension Audrey Galey RDMS, RVT, Mary Grace Renfro RDSM, RVT, Lindsey Simon, RVT March 22, 2013 2 Abstract A recanalized umbilical
Recanalized Umbilical Vein in the Presence of Cirrhosis-Induced Portal Hypertension Audrey Galey RDMS, RVT, Mary Grace Renfro RDSM, RVT, Lindsey Simon, RVT March 22, 2013 2 Abstract A recanalized umbilical
Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal
 ORIGINAL ARTICLE JIACM 2013; 14(3-4): 209-13 Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal Ksh Kala Singh*, A Surjyalal Sharma**, L Sunil Singh***,
ORIGINAL ARTICLE JIACM 2013; 14(3-4): 209-13 Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal Ksh Kala Singh*, A Surjyalal Sharma**, L Sunil Singh***,
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Upper Extremity Arterial Duplex Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Arterial Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Arterial Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE?
 TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
Varicose Veins: Causes, Symptoms and Management. Andrew C. Stanley MD Section of Vascular Surgery
 Varicose Veins: Causes, Symptoms and Management Andrew C. Stanley MD Section of Vascular Surgery Circulation Heart (Pump)-MI, Sudden Death Arteries (Stroke, Aneurysms, Walking dysfunction, Limb loss) Veins
Varicose Veins: Causes, Symptoms and Management Andrew C. Stanley MD Section of Vascular Surgery Circulation Heart (Pump)-MI, Sudden Death Arteries (Stroke, Aneurysms, Walking dysfunction, Limb loss) Veins
Vascular Laboratory Education and Training
 Vascular Laboratory Education and Training David L. Dawson, MD, RVT, RPVI Vascular laboratory professionals technologists and physicians have specific knowledge and expertise in the use of non- invasive
Vascular Laboratory Education and Training David L. Dawson, MD, RVT, RPVI Vascular laboratory professionals technologists and physicians have specific knowledge and expertise in the use of non- invasive
Fort Hamilton Hospital Specialty: Cardiology Department of Medicine Delineation of Privileges
 NAME Fort Hamilton Hospital Specialty: Cardiology Department of Medicine Delineation of Privileges GENERAL CARDIOLOGY Required Qualifications for General Cardiology Education/Training/Experience Must have
NAME Fort Hamilton Hospital Specialty: Cardiology Department of Medicine Delineation of Privileges GENERAL CARDIOLOGY Required Qualifications for General Cardiology Education/Training/Experience Must have
ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS
 ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS 1. VARICOSE VEINS MPC 00727 ICD-9 454 DEFINITION Varicose Veins of the lower extremities are a dilatation, lengthening
ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS 1. VARICOSE VEINS MPC 00727 ICD-9 454 DEFINITION Varicose Veins of the lower extremities are a dilatation, lengthening
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Provided by the American Venous Forum: veinforum.org
 CHAPTER 19 VASCULAR MALFORMATIONS Original authors: David H. Deaton, Byung Boong Lee, James Loredo, Richard F. Neville, William H. Pearce, and Heron E. Rodriguez Abstracted by Raghu Motaganahalli Introduction
CHAPTER 19 VASCULAR MALFORMATIONS Original authors: David H. Deaton, Byung Boong Lee, James Loredo, Richard F. Neville, William H. Pearce, and Heron E. Rodriguez Abstracted by Raghu Motaganahalli Introduction
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Emory Healthcare s model for a PA based vein clinic
 Emory Healthcare s model for a PA based vein clinic Stephen Konigsberg PA-C No relationships to disclose Society for Vascular Surgery 2011 Vascular Annual Meeting Chicago, IL June 17, 2011 Division of
Emory Healthcare s model for a PA based vein clinic Stephen Konigsberg PA-C No relationships to disclose Society for Vascular Surgery 2011 Vascular Annual Meeting Chicago, IL June 17, 2011 Division of
Title Use of rivaroxaban in suspected DVT in the Emergency Department Standard Operating Procedure. Author s job title. Pharmacist.
 Document Control Title Use of rivaroxaban in suspected DVT in the Emergency Department Author Pharmacist Directorate Clinical Support Services Version Date Issued Status 0.1 Oct Draft 2015 1.0 Dec Final
Document Control Title Use of rivaroxaban in suspected DVT in the Emergency Department Author Pharmacist Directorate Clinical Support Services Version Date Issued Status 0.1 Oct Draft 2015 1.0 Dec Final
Modern Management of Varicose Veins
 Modern Management of Varicose Veins GPCME 2008 David Ferrar Vascular and Endovascular Surgeon Vascular Ultrasound Specialist Multimodality treatment Compression stockings Sclerotherapy Ultrasound guided
Modern Management of Varicose Veins GPCME 2008 David Ferrar Vascular and Endovascular Surgeon Vascular Ultrasound Specialist Multimodality treatment Compression stockings Sclerotherapy Ultrasound guided
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Treatment by LASER. Understanding Varicose veins and. Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD)
 Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair
 A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair Table of Contents The AFX Endovascular AAA System............................................ 1 What is an Abdominal Aortic Aneurysm
A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair Table of Contents The AFX Endovascular AAA System............................................ 1 What is an Abdominal Aortic Aneurysm
Varicose Vein Treatment (Endovenous Ablation of Varicose Veins)
 Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info
 TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
DEBATE ON Management of primary Varicose Veins SURGERY. Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University
 DEBATE ON Management of primary Varicose Veins SURGERY Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University Efficacy of treatment alternatives Durability of results Cosmetically acceptable results
DEBATE ON Management of primary Varicose Veins SURGERY Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University Efficacy of treatment alternatives Durability of results Cosmetically acceptable results
