Follow-up of High Risk Neonates
|
|
|
- Jocelin Floyd
- 8 years ago
- Views:
Transcription
1 Follow-up of High Risk Neonates Pradeep Kumar, M.Jeeva Sankar, Savita Sapra, Ramesh Agarwal, Ashok Deorari and Vinod Paul Division of Neonatology, Department of Pediatrics All India Institute of Medical Sciences Ansari Nagar, New Delhi Address for correspondence: Dr Ramesh Agarwal Assistant Professor Department of Pediatrics All India Institute of Medical Sciences Ansari Nagar, New Delhi Downloaded from 1
2 Abstract The improvement in perinatal care has led to increase in survival as well as morbidity in sick newborns. These babies need to be followed up regularly to assess growth and neurodevelopmental outcome and for early stimulation and rehabilitation. We present a protocol describing the various components of a follow up program including setting up of follow up services, procedures and timings of follow up. Key words: Follow up; neurodevelopmental outcome; early stimulation Downloaded from 2
3 Introduction Improving perinatal and neonatal care has led to increased survival of infants who are at-risk for long-term morbidities such as developmental delay and visual/hearing problems 1, 2 Moreover, many of these neonates (e.g. extremely low birth weight infants) tend to have higher incidence of growth failure and ongoing medical illnesses A proper and appropriate follow-up program would help in early detection of these problems thus paving way for early intervention. Importance of follow-up care Numerous studies have shown that despite substantial improvements in the neonatal mortality, the incidence of chronic morbidities and adverse outcomes among survivors has not declined much. 3 This highlights the need for a follow-up care service that would ensure systematic monitoring of the general health and neurodevelopmental outcomes after discharge from the hospital. The monitoring would help the infants and their families (early identification of problems and hence early rehabilitation services) as well as the physicians involved in their care (to improve the quality of care provided and for research purposes). There is a common perception that high risk follow-up mainly concerns with detection and management of neurosensory disability. Infact growth failure and ongoing illnesses are equally, if not more important issues in high risk followup. Adequate emphasis must be placed on these. However, a rigorous follow-up of all the neonates discharged from a particular health facility would neither be practical nor feasible. Therefore, it is important to select a cohort of neonates who are at a higher risk of developing these adverse outcomes at-risk infants. Surprisingly, there are no standardized guidelines for follow up of high risk infants even in tertiary care centers 4. We have devised a follow up protocol which identifies the subset of neonates to be followed up and outlines the optimal time for follow-up visits and the appropriate assessment measures to be adopted. Downloaded from 3
4 Setting up of follow up services High risk infants follow-up requires a multidisciplinary approach involving a team of pediatricians, child psychologist, pediatric neurologist, ophthalmologist, otorhinolaryngologist, physiotherapist, occupational therapist, medical social worker, and a dietician. The respective role of each team member is summarized in Table 1. Table 1: Personnel required for follow-up program and their individual roles S. No Team member Role(s) 1. Pediatricians / neonatologists Serves as the nodal person of the team To assess growth and screen for developmental delay To manage intercurrent illnesses 2. Child psychologist(s) For formal neurodevelopmental assessment Screening for behavioral problems and their management 3. Pediatric neurologist Long-term management of neurological illnesses such as seizures 4. Ophthalmologist Follow-up of ROP screening/treatment Assessment of visual acuity and screening for problems such as strabismus, nystagmus, refractory errors, etc. 5. Otorhinolaryngologist Hearing assessment (BERA, OAE, etc.) Management of hearing impairment, if any 6. Dietician Dietary advice regarding complementary feeding Management of infants with failure to thrive and those with special needs (e.g. galactosemia) 7. Medical social worker To take care of the social issues to help improve follow up rates 8. Physiotherapist Assessment and grading of muscle tone and power Plan an appropriate training program for each infant with tone abnormalities To teach the parents for continuing the prescribed exercises at home 9. Speech / occupational Rehabilitation of infants with impairment/disability Downloaded from 4
5 therapist Ideally, all the required personnel should be available under one roof at a place earmarked for follow-up care. If this is not feasible, at least the services of pediatrician, clinical psychologist, dietician, medical social worker, and physiotherapist should be ensured in the follow-up clinic. Medical social worker is an important member of the team liasoning with the family and helps them to keep follow up visits. Infants who need hearing/visual assessment or speech therapy can be referred to the concerned specialist on fixed days. Who needs follow-up care? Selection of high-risk infants should be based on the gestational age, birth weight, occurrence and severity of perinatal/neonatal illnesses, interventions received in the neonatal intensive care unit (NICU), presence of malformations, etc. It can further be modified for each unit based on their admission and outcome profiles. Panel 1 lists the cohort of high risk infants whom we follow-up in our unit. Panel 1: High risk neonates who need follow-up care (customize as per policy) 1. Babies with <1800g birth weight and/or gestation <35 weeks 2. Small for date (<3 rd centile) and large for date (>97 th centile) 3. Perinatal asphyxia - Apgar score 3 or less at 5 min and/or hypoxic ischemic encephalopathy 4. Mechanical ventilation for more than 24 hours 5. Metabolic problems Symptomatic hypoglycemia and hypocalcemia 6. Seizures 7. Infections meningitis and/or culture positive sepsis 8. Shock requiring inotropic/vasopressor support 9. Major morbidities such as chronic lung disease, intraventricular hemorrhage, and periventricular leucomalacia 10. Infants born to HIV-positive mothers 11. Twin with intrauterine death of co-twin 12. Twin to twin transfusion 13. Hyperbilirubinemia > 20mg/dL or requirement of exchange transfusion 14. Rh hemolytic disease of newborn 15. Major malformations Downloaded 16. Inborn from errors of metabolism / other genetic disorders Abnormal neurological examination at discharge
6 The developing brain of premature babies is extremely vulnerable to injury; the risk for neurodevelopmental deficit increases with decreasing gestational age and birth weight resulting in relatively high risk of cerebral palsy, developmental delay, hearing and vision impairment and subnormal academic achievement 5. Similarly, small for date infants (birth weight < 3 rd centile) are also at significant risk of poor long term outcomes. Those who required mechanical ventilation for more than 24hours, babies with metabolic problems symptomatic hypoglycemia as half of them have abnormal neurodevelopmental outcome, symptomatic hypocalcemia, birth asphyxia Apgar score 3 or less at 5 min, abnormal neurological examination at discharge, seizures, hyperbilirubinemia > 20mg/dL or requirement of exchange transfusion, Rh hemolytic disease of newborn as they have anemia presenting till three to six months age, infections culture positive sepsis or meningitis, babies born to HIV infected mothers, twin with intrauterine death of co-twin due to increased incidence of cerebral venous thromboembolic phenomenon, twin to twin transfusion or major malformation. All infants cared for in the NICU should have periodic preventive assessment by their primary care physicians which should include regular assessment of growth, sensory function, behavior and neurodevelopment. Infants with suspect findings should be referred for more comprehensive evaluation to a center with experience in follow up of high risk neonates. Downloaded from 6
7 Pre-requisites for follow-up To ensure proper follow-up of the high risk infants, parents (especially mother) and other family members should be counseled even before discharge from the hospital. Discharge should be planned well in advance so that the mother can be counseled adequately. Discharge planning: Discharge planning should ideally begin as soon as the baby is admitted in the nursery. This gives adequate time for the caretakers to ask questions and practice skills. The following criteria should be fulfilled before discharging a high risk infant: Hemodynamically stable; able to maintain body temperature in open crib On full enteral feeds (either breast feeding or by paladai/spoon) Parents confident enough to take care of the baby at home Has crossed birth weight and showing a stable weight gain for at least three consecutive days; in case of very low birth weight infants, weight should be at least 1400 grams before considering for discharge. Not on any medications (except for vitamins and iron supplementation). Ideally preterm babies on theophylline therapy for apnea of prematurity should be off therapy for at least five days to make sure that there is no recurrence. Received vaccination as per schedule (based on postnatal age). These criteria can be individualized to meet the infant and family needs. Counseling prior to discharge: Counseling plays an important role in the care of these babies at home; regular counseling sessions should be done before discharge. Parents should be given advice regarding: Temperature regulation proper clothing, cap, socks, Kangaroo mother care etc. Feeding type and amount of milk, method of administration, and nutritional supplementation, if any. Prevention of infections hand washing, avoidance of visitors, etc. Follow-up visits where and when (Table I) Danger signs recognition and where to report if signs are present Vaccination schedule, next visit, etc. Downloaded from 7
8 Special needs e.g. next visits for ROP screening. If possible the family should be provided with the telephone number of the health care provider e.g. on-duty doctor in case the family needs to consult for infant s illness. Procedure for follow-up Venue: A specified site should be earmarked for follow up services. The parents should be properly communicated about the venue and it should also be mentioned in the discharge summary. Registration procedure at the follow-up clinic should be simplified to avoid any undue delay. Ongoing illness is common problem among these infants. If the infant develops any illness requiring admission, priority should be given for the same. Record maintenance: There should be a separate but uniform file for each high risk infant. We have separate files for male and female babies. Male babies get blue and female babies get pink files. Addresses and telephone numbers should be entered clearly in the file. If possible, an alternate address and telephone number should also be recorded. It may be good idea to enquire an important landmark for locating the house in case one needs to make a home visit. The family should also be given a booklet containing follow-up information. Schedule: The follow up schedule should be explained to the parents (see below). Timings should be fixed and adhoc visits should be discouraged. Corrected age: Age of the child since the expected date of delivery. The correction for gestational immaturity at birth should be done till 24 months age. All developmental milestones are assessed according to corrected age to compensate for the prematurity. The addition of complementary feeds is also according to corrected age. Postnatal age: Age of the child since birth. Immunization is done according to postnatal age. When to follow up For the purpose of follow-up visits, at-risk infants can be grouped under two major categories: (1) preterm/lbw infants and (2) infants with other conditions. The follow-up Downloaded from 8
9 schedule for both these categories has been summarized in Table II. This schedule represents minimum number of visits of high risk neonates. If the baby has ongoing issues or illness, more frequent visits are recommended. Please note that first contact of the infant with the health providers after discharge is important and helps in identification of adjustment problems at home. Ideally this contact should be achieved by the home visit. Table II: Follow-up schedule of at-risk infants Cohort 1. Infants with <1800g birth weight and/or gestation <35 weeks Schedule for follow-up After 3-7 days of discharge to check if the baby has been adjusted well in the home environment. Every 2 weeks until a weight of 3 kg (immunization schedule until weeks to be covered in these visits) At 3, 6, 9, 12 and 18months of corrected age and then every 6 months until age of 8years 2. All other conditions 2 weeks after discharge At 6, 10, 14 weeks of postnatal age At 3, 6, 9, 12 and 18months of corrected age and then every 6 months until age of 8years Note: If a preterm infant (< 35 weeks) develop any other morbidity covered in other conditions, he should be followed up as per the schedule outlined for the first group of cohort The selection of age of assessment depends on developmental acquisitions available at a given age, availability and applicability of appropriate test instruments at specific ages and the cost and feasibility of long-term tracking in the population in question. The long term follow up of complete cohorts is optimal for determining the outcome of high risk neonates and the safety of antenatal and perinatal interventions. Very low birth weight babies or those born at less than 33 weeks gestation should be followed up for eye check up for retinopathy of prematurity till the postnatal age of 44 weeks. Some neurological abnormalities that are identified in the first year of life are transient or improve whereas findings in other children may worsen over time. 7 By 12 months corrected age the cognitive and language assessment can be done. By months corrected age there is improved prediction to early school age performance. 8, 9, 10 The importance of long term follow up lies in the fact that minor neurological disabilities may not be detected early and become apparent only with increasing age. Standard follow-up for many multicenter networks is currently at months corrected age. Downloaded from 9
10 What should be done at follow up? Table III summarizes the plan for follow up. Table III: Follow up plan for high risk infants Assessment Age in months Downloaded from 10
11 Assessment of feeding and dietary years counseling Growth monitoring All visits Immunization As per schedule (based on postnatal age) Neurological examination Developmental assessment and DQ Hearing (BERA) Ophthalmic evaluation USG/CT brain As indicated if previous test abnormal 1. Assessment of feeding and dietary counseling: Parents should be asked about the infants diet and offered dietary counseling at each visit. Breast feeding frequency and adequacy should be assessed. The amount, dilution and mode of feeding should be noted if supplemental feeding is given. It is a good idea to enquire about source of milk as milk supplied by local vendors is often diluted (dilution has the same impact on the infant whether done by the family or the vendor!). It is also important to record the duration of exclusive breast feeding. If a baby is not gaining adequate weight on exclusive breast feeding take care of any illness, maternal problems which may interfere with feeding and milk output. If poor weight gain persists despite all measures to improve breast milk output, supplementation can be considered. Complementary feeding should be started at 6 months corrected age. Initially, semisolids should be advised in accordance with the local cultural practices. Spend adequate time on explaining what to give and how to give. The common practice of giving too little or too dilute complementary food such as rice-water, dal-water, too much of juice, etc should be discouraged. The recommended meal frequencies assuming a diet with energy density of 0.8 kcal per gram or above and low breast milk intake are: 2 3 meals per day for infants aged 6 8 months; 3 4 meals per day for infants aged 9 11 months and children months; additional nutritious snacks may be offered 1 2 times a day, as desired. Complementary foods should be varied and include adequate quantities of meat, poultry, fish or eggs, as well as vitamin A-rich fruits and vegetables every day. Where this is not possible, the use of fortified complementary foods and vitamin mineral supplements may be necessary to ensure adequacy of particular nutrient intakes. As infants grow, the consistency of complementary foods should change from semisolid to solid foods and the variety of foods offered should increase. By eight months, infants can eat finger foods and by Downloaded from 11
12 12 months, most children can eat the same types of food as the rest of the family. The major problem with the family food is that it is not nutrient-rich Growth monitoring: Growth (including weight, head circumference, mid-arm circumference and length) should be monitored and plotted on an appropriate growth chart at each visit. We use Wright s charts (till 40 weeks PMA) and WHO growth charts (for preterm infants after 40 weeks PMA and for term infants) for growth monitoring. The infant s growth pattern (slope of the curve) is compared with the standard curve; any deviation should be noted and appropriate remedial action taken. Weight should be taken on an electronic weighing scale. Length should be measured with an infantometer. The infant should be held supine and legs fully extended. The feet should be pressed against the movable foot piece with the ankles fixed to 90. Head circumference should be measured with nonstretchable fiberglass tape Developmental assessment: Assessment of developmental milestones should be done according to the corrected age. The milestones should be assessed in four domains- gross motor, fine motor, language, and personal-social (see page 10 with instructions for filling given in page 9 of HRC file). The date of assessment and the infants corrected age should be mentioned against each milestone. Based on the date of achievement of milestones in a particular domain and the expected age of achieving them, the developmental age can be calculated. Infants who lag behind in any domain should undergo a formal developmental evaluation by a clinical psychologist using tests such as Developmental assessment of Indian Infant II (DASII II) 13. This scale consists of 67 items for assessment of motor development and 163 items for assessment of mental development. Motor scale assesses control of gross and fine motor muscle groups. Mental scale assesses cognitive, personal and social skills development. Both mental development index and psychomotor development index can be calculated by DASII. The age placement of the item at the total score rank of the scale is noted as the child developmental age. This converts the child total scores to his motor age (MoA) and Downloaded from 12
13 mental age(mea). The respective ages are used to calculate his motor and mental development quotients respectively by comparing them with his chronological age and multiplying it by 100. (DMoQ = MoA/CA x 100 and DMeQ = MeA/CA x 100). The composite DQ is derived as an average of DMoQ and DMeQ. The Vineland Social Maturity Scale measures social competence, self-help skills, and adaptive behavior from infancy to adulthood. The Vineland scale consists of a 117-item interview with a parent or other primary caregiver. It is emphasized here that developmental stimulation of the child should not be delayed if the above mentioned tests are not available. Age appropriate stimulation should be provided to these babies. Mental development index and Psychomotor development index at 3, 12,18 and 24 months and every 3 months if abnormal. 4. Immunization: Immunization should be ensured according to chronological age. Parents should be offered the option of using additional vaccines such as Hemophilus influenzae B, typhoid and MMR. 5. Ongoing problems: They should be mentioned in the follow up notes. The management of ongoing illnesses is an integral part of any high risk follow up program. The hospital admission of the child should be prioritized, if required. 6. Neurological assessment: Evaluation of muscle tone is an integral part of the neurological examination. A waxing and waning pattern of neuromotor development from 28 weeks of gestation to the end of first year of life was reported by Amiel-Tison. From 28 to 40 weeks gestation, the acquisition of muscle tone and motor function spreads from lower extremities towards the head. After full term, the process is reversed so that relaxation and the motor control proceed downwards for the next 12 to 18 months. So the upper limbs begin to relax and acquire skills before the lower limbs. The axial tone follows a similar pattern. Head control appears first followed by the ability to sit, stand and walk. Hypertonia or hypotonia should be looked for by measuring the following angles: adductor angle, popliteal angle, ankle dorsiflexion, and scarf sign; any Downloaded from 13
14 asymmetry between the extremities should also be recorded. Any history of seizures or involuntary movements should also be recorded. Hypertonia in lower limbs is defined as when either adductor angle is restricted to less than the age specific norms as per Amiel-Tison or if there is scissoring or tight tendo-achilles or restriction of ankle dorsiflexion on extension of knee. Hypertonia in upper limbs is defined as when scarf sign does not cross midline at one year corrected age. Hypertonia of the neck extensors can be inferred by an increased gap between the nape of the neck and examination table with the infant lying in supine position. The following angles should be measured to assess tone as shown in Figure1, Table IV: Table IV: Muscle Tone Norms Age Adductor Popliteal Dorsiflexion Scarf sign (months) angle angle angle Elbow does not cross Truncal extensor hypertonia: there is a tendency of body to go into hyperextension or opisthotonus. Cerebral palsy: Definitely abnormal neurological examination with upper motor neuron signs with motor developmental delay. Spastic hypertonia syndromes: midline Elbow crosses midline Elbow goes beyond axillary line Hemiplegia- only one half of body involved Diplegia- paresis of lower limbs more than upper limbs Downloaded from 14
15 Quadriplegia- Paresis of all four limbs with upper limb involvement equal to or more than lower limbs. Abnormal neurological examination should be defined as definite abnormalities In the form of: a) Brisk reflexes with hypertonia or b) Brisk reflexes with hypotonia or c) Definitely and consistently elicited asymmetrical signs or d) Persistent abnormal posturing or abnormal movements The tone abnormalities should be taken care by regular physiotherapy. This improves mobility of joints and locomotion of the child. The child should be provided with special shoes if required. Orthopedic evaluation should be done and corrective surgery for contractures should be done as required. All possible efforts should be made to improve mobility of these children and make them functionally less dependent and independent if possible. Eye evaluation: The check-up for retinopathy of prematurity starts in the NICU and continues till 44 weeks postconceptional age or till the retinal vessels have matured. Refer to protocol on Retinopathy of prematurity 14. At 9 months corrected age the ophthalmologist should evaluate the baby for vision, squint, cataract and optic atrophy. Subjective visual assessment can be made from clinical clues as inability to fixate eyes, roving eye movements and nystagmus. Objective visual assessment should be done with the Teller Acuity Card. It has seventeen cm cards. Fifteen of these contain cm patches of square-wave gratings( vertical black and white strips) ranging in spatial frequency from 38.0 cycles/cm to 0.32 cycles/cm. The range is in half octave steps. A cycle consists of one black and one white stripe and an octave is a halving or doubling of spatial frequency. In Snellens terms it is an halving or doubling of the denominator e.g. 6/6, 612, 6/24. Half octave steps would be 6/6, 6/9, 6/12, 6/18, 6/24 and so on. Downloaded from 15
16 There is a low vision card containing cm patch of 0.23 cm cycle/cm( 2.2 cm wide black or white stripes). The seventeenth card is a blank grey card with no grating pattern. The gratings have 82 84% contrast and are matched to the surrounding grey card to within 1% in space average luminance. This minimizes the chance of a patient fixating because of brightness difference. Detection of pattern alone determines the fixating preference. Proper illumination without any shadows should be ensured (10 candelas /sqm). Testing distance from patient s eyes to the cards should be maintained constant as it determines the visual acuity. Children from 7m to 3y should be tested at 55 cm and later at 84 cm. Rehabilitation for visual impairment should be early so that the child gets appropriate stimulation. If delayed the restoration of the vision may not be possible because of continuous sensory deprivation of the optic nerve. The child should be provided with glasses or corrective surgery as appropriate. It should be emphasized that a good high risk follow up program does not only pick up handicaps early but also ensures early corrective measures and rehabilitation. This emphasizes the multidisciplinary and well coordinated approach to such babies 7. Hearing evaluation: High risk infants have higher incidence of moderate to profound hearing loss (2.5-5% vs. 1%). Since clinical screening is often unreliable, brainstem auditory evoked responses (BAER/BERA) should be performed between 40 weeks PMA and 3 months postnatal age. A screening BERA is usually done initially. If this is abnormal, a diagnostic BERA should be done within 2 weeks of the initial test. Infants with unilateral abnormal results should have follow-up testing within three months. The test should be carried out in a sound-proof room and the infant should be sedated with oral triclofos 50mg/kg 30 min before the procedure. To measure the electrical pulses, small monitoring electrodes are placed on the scalp. Earphones provide a clicking noise to the ear and the response from the brainstem is measured time-locked to the clicks. The clicks may become louder or softer, faster or slower, to see how the auditory responds to these different stimulus parameters. The other method of assessment for hearing is oto-acoustic emission (OAE). This records acoustic feedback from the cochlea through the ossicles to the tympanic membrane and ear canal following a click stimulus. It is quicker to perform than BERA but is more likely to be affected by debris or fluid in the external and middle ear. It is Downloaded from 16
17 unable to detect some form of sensorineural hearing loss including auditory dyssynchrony. The severity of hearing loss is profound (70 db or more of hearing loss), severe (50 db - 70 db), moderate (30 db - 50 db) and mild (15 db - 30 db). The audiological testing should be done at 3 months of age. Infants with true hearing loss should be referred for early intervention to enhance the child s acquisition of developmentally appropriate language skills. The child should be provided with hearing aids and if severe to profound hearing loss cochlear implants should be considered by 12 months age. Fitting of hearing aids by the age of 6 months has been associated with improved speech outcome. Initiation of early intervention services before three months age has been associated with improved cognitive development at 3years age 15 Early stimulation The high risk baby requires more attention of the family members. Parents and family members need to aid the development process in an age appropriate way spending quality time with children. Such interactions improve parent child relationship and bring about positive parental attitudinal change. Effective parents supervise their children in an age appropriate way, use consistent positive discipline, communicate clearly and supportively, and show warmth, affection, encouragement, and approval. The actions of the child should be appreciated. This makes him happy and encourages doing more activities. 0-2 months: Activities Maintain eye to eye contact Talk and sing to the baby while bathing, dressing and feeding Help the baby to turn his head to sound and light Auditory Downloaded from 17
18 Provide different sounds to the child like rattle, bell, squeezing a toy. Make the child listen to music, high pitched and low pitched human sounds Humming in a soft low voice Visual Keep the baby in a well lighted room Shine mobile, color balls and hang bright clothes Tactile Put the baby on different surfaces like soft clothes, mattresses, rubber mat and mother s lap Change the child s position frequently like putting on his back, sides and tummy Kinesthetic Support the head and gently rock the child avoiding sudden jerky movements 2-4 months General stimulation Hold the baby at the shoulder Place things just out of the reach of the baby. Stimulate him to reach out and grasp the object Auditory Give sound producing toys Talk to the child more frequently Point out the names of objects shown to the child Visual Hang bright objects about 30cm above the crib Maintain eye contact while talking to the child Tactile Give the child paper to crumble and things to bite and suck Place the child on a rubber mat on the ground allowing him to move freely Downloaded from 18
19 4-6 months: General activities: Sit the baby in the mother s lap and ask her to gently bounce her knees singing songs. Place the child flat on the back on the ground over a soft surface. Show him a colorful toy. Slowly turn him by flexing the far away leg. Assist him to turn over the tummy. Show an attractive toy and encourage the child to reach out to it. Put your hands under the child s feet and move his legs up and down like pedaling a cycle. Auditory Shake a bell or a squeaky toy over the head of the baby. Encourage him to turn his head and locate the sound 6-8 months: Call the child by his name Make the child sit as long as possible. Give support to his pelvis. Give him pieces of paper to tear Encourage him to roll over his tummy by showing him colorful toys on one side months: Make the child stand by holding onto the furniture Encourage the child to clap hands Give him a small container and ask to drop small thing into it. Encourage him to produce monosyllables. Show him picture books and assist to turn the pages months: Let the child play with other children Name the body parts while bathing him Take the child on a walk and show him different animals and birds Downloaded from 19
20 Do simple actions like clapping, bye-bye and encourage copying these actions. Encourage him to pull to stand by holding the furniture Make the child sit in front of a mirror so that he can see himself months: Give picture books to the child. Talk about what you see and let him turn the pages Ask him to put cubes one over the other Ask him to put things into the container and then take out things out of the container. Hide a small toy under a cloth. Encourage the baby to find the hidden toy. Ask the child to scribble by drawing a few lines. First demonstrate what he is supposed to do. How to ensure a good follow up rate The importance of follow up should be emphasized frequently to the parents. The permanent and present addresses along with phone numbers should be kept to ensure follow up. If the parents do not turn up for follow up they should be telephoned and letters should be posted to ensure good follow up rates. There should be a dedicated person who can adjust the timing with the parents. If possible home visits should be arranged for those who do not turn up. There should be a comprehensive assessment of the child under one roof to minimize the hassles of roaming from one corner of the hospital to the other. Downloaded from 20
Cerebral palsy, neonatal death and stillbirth rates Victoria, 1973-1999
 Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
Cerebral Palsy. In order to function, the brain needs a continuous supply of oxygen.
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Hearing Tests for Children with Multiple or Developmental Disabilities by Susan Agrawal
 www.complexchild.com Hearing Tests for Children with Multiple or Developmental Disabilities by Susan Agrawal Hearing impairment is a common problem in children with developmental disabilities or who have
www.complexchild.com Hearing Tests for Children with Multiple or Developmental Disabilities by Susan Agrawal Hearing impairment is a common problem in children with developmental disabilities or who have
Cerebral Palsy. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com nr200105 Last reviewed: 06/17/2014 1
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
What is cerebral palsy?
 What is cerebral palsy? This booklet will help you to have a better understanding of the physical and medical aspects of cerebral palsy. We hope it will be a source of information to anyone who wishes
What is cerebral palsy? This booklet will help you to have a better understanding of the physical and medical aspects of cerebral palsy. We hope it will be a source of information to anyone who wishes
Questions and Answers for Parents
 Questions and Answers for Parents There are simple, inexpensive tests available to detect hearing impairment in infants during the first days of life. In the past, most hearing deficits in children were
Questions and Answers for Parents There are simple, inexpensive tests available to detect hearing impairment in infants during the first days of life. In the past, most hearing deficits in children were
Cerebral Palsy: Intervention Methods for Young Children. Emma Zercher. San Francisco State University
 RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
Cerebral Palsy. www.teachinngei.org p. 1
 Cerebral Palsy What is cerebral palsy? Cerebral palsy (CP) is a motor disability caused by a static, non-progressive lesion (encephalopathy) in the brain that occurs in early childhood, usually before
Cerebral Palsy What is cerebral palsy? Cerebral palsy (CP) is a motor disability caused by a static, non-progressive lesion (encephalopathy) in the brain that occurs in early childhood, usually before
1. What is Cerebral Palsy?
 1. What is Cerebral Palsy? Introduction Cerebral palsy refers to a group of disorders that affect movement. It is a permanent, but not unchanging, physical disability caused by an injury to the developing
1. What is Cerebral Palsy? Introduction Cerebral palsy refers to a group of disorders that affect movement. It is a permanent, but not unchanging, physical disability caused by an injury to the developing
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
The National Survey of Children s Health 2011-2012 The Child
 The National Survey of Children s 11-12 The Child The National Survey of Children s measures children s health status, their health care, and their activities in and outside of school. Taken together,
The National Survey of Children s 11-12 The Child The National Survey of Children s measures children s health status, their health care, and their activities in and outside of school. Taken together,
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Title: Routine Screening of Neonates Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6
NEONATAL CLINICAL PRACTICE GUIDELINE Title: Routine Screening of Neonates Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6
Developmental delay and Cerebral palsy. Present the differential diagnosis of developmental delay.
 Developmental delay and Cerebral palsy objectives 1. developmental delay Define developmental delay Etiologies of developmental delay Present the differential diagnosis of developmental delay. 2. cerebral
Developmental delay and Cerebral palsy objectives 1. developmental delay Define developmental delay Etiologies of developmental delay Present the differential diagnosis of developmental delay. 2. cerebral
EXECUTIVE SUMMARY OF JOINT COMMITTEE ON INFANT HEARING YEAR 2007 POSITION STATEMENT. Intervention Programs
 EXECUTIVE SUMMARY OF JOINT COMMITTEE ON INFANT HEARING YEAR 2007 POSITION STATEMENT Principles and Guidelines for Early Hearing Detection and Intervention Programs The Joint Committee on Infant Hearing
EXECUTIVE SUMMARY OF JOINT COMMITTEE ON INFANT HEARING YEAR 2007 POSITION STATEMENT Principles and Guidelines for Early Hearing Detection and Intervention Programs The Joint Committee on Infant Hearing
CEREBRAL PALSY AND MENTAL RETARDATION DEFINITION
 CEREBRAL PALSY AND MENTAL RETARDATION DEFINITION It is a disorder of posture movement and tone due to a static encephalopathy acquired during brain growth in fetal life infancy or early childhood. Though
CEREBRAL PALSY AND MENTAL RETARDATION DEFINITION It is a disorder of posture movement and tone due to a static encephalopathy acquired during brain growth in fetal life infancy or early childhood. Though
HOW YOU CAN HELP YOUR CHILD WITH CEREBRAL PALSY
 HOW YOU CAN HELP YOUR CHILD WITH CEREBRAL PALSY CBM is one of the world s largest international disability and development organisations, committed to improving the quality of life of persons with disabilities
HOW YOU CAN HELP YOUR CHILD WITH CEREBRAL PALSY CBM is one of the world s largest international disability and development organisations, committed to improving the quality of life of persons with disabilities
Cerebral Palsy. Causes
 Cerebral Palsy Cerebral Palsy (sera brul PAUL zee) (CP) is an injury or abnormality of the developing brain that affects movement. This means that something happened to the brain or the brain did not develop
Cerebral Palsy Cerebral Palsy (sera brul PAUL zee) (CP) is an injury or abnormality of the developing brain that affects movement. This means that something happened to the brain or the brain did not develop
Premature Infant Care
 Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
FAILURE TO THRIVE What Is Failure to Thrive?
 FAILURE TO THRIVE The first few years of life are a time when most children gain weight and grow much more rapidly than they will later on. Sometimes, however, babies and children don't meet expected standards
FAILURE TO THRIVE The first few years of life are a time when most children gain weight and grow much more rapidly than they will later on. Sometimes, however, babies and children don't meet expected standards
Medicaid Disability Manual
 Part B The following sections apply to individuals under age 18. If the criteria in Part B do not apply, Part A criteria may be used when those criteria give appropriate consideration to the effects of
Part B The following sections apply to individuals under age 18. If the criteria in Part B do not apply, Part A criteria may be used when those criteria give appropriate consideration to the effects of
CEREBRAL PALSY CLASSIFICATION BY SEVERITY LEVEL
 Patient Name: Today s Date: CAUSE OF CEREBRAL PALSY Hypoxic-Ischemic Encephalopathy (HIE) or Intrapartum Asphyxia - Brain injury Lack of oxygen to the brain or asphyxia. Intracranial Hemorrhage (IVH) Brain
Patient Name: Today s Date: CAUSE OF CEREBRAL PALSY Hypoxic-Ischemic Encephalopathy (HIE) or Intrapartum Asphyxia - Brain injury Lack of oxygen to the brain or asphyxia. Intracranial Hemorrhage (IVH) Brain
EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN
 EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN Our child has a hearing loss. What happens next? What is early intervention? What can we do to
EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN Our child has a hearing loss. What happens next? What is early intervention? What can we do to
Child Development. Caseworker Core Training Module VII: Child Development: Implications for Family-Centered Child Protective Services
 Child Development P R E - T R A I N I N G A S S I G N M E N T Caseworker Core Training Module VII: Child Development: Implications for Family-Centered Child Protective Services Developed by the Institute
Child Development P R E - T R A I N I N G A S S I G N M E N T Caseworker Core Training Module VII: Child Development: Implications for Family-Centered Child Protective Services Developed by the Institute
Cerebral Palsy. 1 - Introduction. An informative Booklet for families in the Children and Teens program
 Cerebral Palsy 1 - Introduction An informative Booklet for families in the Children and Teens program Centre de réadaptation Estrie, 2008 Preface Dear parents, It is with great pleasure that we present
Cerebral Palsy 1 - Introduction An informative Booklet for families in the Children and Teens program Centre de réadaptation Estrie, 2008 Preface Dear parents, It is with great pleasure that we present
How babies' senses develop
 B2 There is much growth and change that must occur in your baby s body. For babies born full-term (37-40 weeks), this growth and change occurred within the warm, dark, watery womb. For the premature baby,
B2 There is much growth and change that must occur in your baby s body. For babies born full-term (37-40 weeks), this growth and change occurred within the warm, dark, watery womb. For the premature baby,
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease.
 Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: info@childmuscleweakness.org Surveillance and Referral
Learn the steps to identify pediatric muscle weakness and signs of neuromuscular disease. Guide for therapists/specialists Questions and comments to: info@childmuscleweakness.org Surveillance and Referral
If baby was born 3 or more weeks prematurely, # of weeks premature: Last name: State/ Province: Home telephone number:
 Ages & Stages Questionnaires 12 11 months 0 days through 12 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this
Ages & Stages Questionnaires 12 11 months 0 days through 12 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this
If baby was born 3 or more weeks prematurely, # of weeks premature: Last name: State/ Province: Home telephone number:
 Ages & Stages Questionnaires 8 7 months 0 days through 8 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
Ages & Stages Questionnaires 8 7 months 0 days through 8 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
Purpose: To develop physical and motor skills and promote health and well-being
 Purpose: To develop physical and motor skills and promote health and well-being The physical and motor development domain includes the physical and motor skills and abilities that emerge during the infant
Purpose: To develop physical and motor skills and promote health and well-being The physical and motor development domain includes the physical and motor skills and abilities that emerge during the infant
Standard of Care: Neonatal Intensive Care Unit (NICU) Physical and Occupational Therapy Management of the high risk infant.
 BRIGHAM & WOMEN S HOSPITAL Department of Rehabilitation Services Standard of Care: Neonatal Intensive Care Unit (NICU) Case Type / Diagnosis: The high-risk infant is defined as the baby with any event
BRIGHAM & WOMEN S HOSPITAL Department of Rehabilitation Services Standard of Care: Neonatal Intensive Care Unit (NICU) Case Type / Diagnosis: The high-risk infant is defined as the baby with any event
Specialist Children s Service
 Specialist Children s Service Information and Guidelines for Referrers March 2009, Version 3.0 Contents CONTENTS... 2 INTRODUCTION... 3 TEAMS BASED AT THE WOOD STREET HEALTH CENTRE:... 3 TEAMS BASED ELSEWHERE
Specialist Children s Service Information and Guidelines for Referrers March 2009, Version 3.0 Contents CONTENTS... 2 INTRODUCTION... 3 TEAMS BASED AT THE WOOD STREET HEALTH CENTRE:... 3 TEAMS BASED ELSEWHERE
REQUIREMENTS FOR REGIONAL CENTER ELIGIBILITY HAVE CHANGED
 REQUIREMENTS FOR REGIONAL CENTER ELIGIBILITY HAVE CHANGED As a result of a Trailer Bill AB 1762, which amended The Lanterman Developmental Disabilities Act, regional centers across the state are required
REQUIREMENTS FOR REGIONAL CENTER ELIGIBILITY HAVE CHANGED As a result of a Trailer Bill AB 1762, which amended The Lanterman Developmental Disabilities Act, regional centers across the state are required
Webinar title: Know Your Options for Treating Severe Spasticity
 Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
CALIFORNIA SPECIAL EDUCATION MANAGEMENT INFORMATION SYSTEM (CASEMIS) SERVICE DESCRIPTIONS. San Diego Unified SELPA
 210 Family training, counseling, and home visits(ages 0-2 only): This service includes: services provided by social workers, psychologists, or other qualified personnel to assist the family in understanding
210 Family training, counseling, and home visits(ages 0-2 only): This service includes: services provided by social workers, psychologists, or other qualified personnel to assist the family in understanding
Criteria for Determining Disability in Infants and Children: Low Birth Weight
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Number 70 Criteria for Determining Disability in Infants and Children: Low Birth Weight Summary Overview The Social Security
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Number 70 Criteria for Determining Disability in Infants and Children: Low Birth Weight Summary Overview The Social Security
Early Intervention Service Procedure Codes, Limits and Rates
 BABIES INFORMATION AND BILLING SYSTEM Early Intervention Service Procedure Codes, Limits and Rates Georgia Department of Public Health Office of Maternal and Child Health Children and Youth with Special
BABIES INFORMATION AND BILLING SYSTEM Early Intervention Service Procedure Codes, Limits and Rates Georgia Department of Public Health Office of Maternal and Child Health Children and Youth with Special
Neonatal Reflexes. By Courtney Plaster
 Neonatal Reflexes By Courtney Plaster Neonatal Reflexes Neonatal reflexes are inborn reflexes which are present at birth and occur in a predictable fashion. A normally developing newborn should respond
Neonatal Reflexes By Courtney Plaster Neonatal Reflexes Neonatal reflexes are inborn reflexes which are present at birth and occur in a predictable fashion. A normally developing newborn should respond
Understanding Hearing Loss 404.591.1884. www.childrensent.com
 Understanding Hearing Loss 404.591.1884 www.childrensent.com You just found out your child has a hearing loss. You know what the Audiologist explained to you, but it is hard to keep track of all the new
Understanding Hearing Loss 404.591.1884 www.childrensent.com You just found out your child has a hearing loss. You know what the Audiologist explained to you, but it is hard to keep track of all the new
If baby was born 3 or more weeks prematurely, # of weeks premature: Last name: State/ Province: Home telephone number:
 Ages & Stages Questionnaires 4 3 months 0 days through 4 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
Ages & Stages Questionnaires 4 3 months 0 days through 4 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
If baby was born 3 or more weeks prematurely, # of weeks premature: Last name: State/ Province: Home telephone number:
 Ages & Stages Questionnaires 10 9 months 0 days through 10 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this
Ages & Stages Questionnaires 10 9 months 0 days through 10 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this
WHAT IS CEREBRAL PALSY?
 WHAT IS CEREBRAL PALSY? Cerebral Palsy is a dysfunction in movement resulting from injury to or poor development of the brain prior to birth or in early childhood. Generally speaking, any injury or disease
WHAT IS CEREBRAL PALSY? Cerebral Palsy is a dysfunction in movement resulting from injury to or poor development of the brain prior to birth or in early childhood. Generally speaking, any injury or disease
IDAHO EARLY LEARNING EGUJDELINES
 IDAHO EARLY LEARNING EGUJDELINES Sus-DOMAIN: MOTOR DEVELOPMENT Goal 17: Goal 18: Goal19: Children demonstrate strength and coordination of large motor muscles. Children demonstrate strength and coordination
IDAHO EARLY LEARNING EGUJDELINES Sus-DOMAIN: MOTOR DEVELOPMENT Goal 17: Goal 18: Goal19: Children demonstrate strength and coordination of large motor muscles. Children demonstrate strength and coordination
A Note to Physical, Occupational and Speech Therapists
 D Page 1 of 5 A Note to Physical, Occupational and Speech Therapists Treating Children with Hurler Syndrome Because Hurler syndrome is such a rare disease, we have provided some basic information to assist
D Page 1 of 5 A Note to Physical, Occupational and Speech Therapists Treating Children with Hurler Syndrome Because Hurler syndrome is such a rare disease, we have provided some basic information to assist
Normal and Abnormal Development in the Infant and Pre-School Child
 Normal and Abnormal Development in the Infant and Pre-School Child Steven Bachrach, M.D. Co-Director, Cerebral Palsy Program A.I. dupont Hospital for Children Development in the Infant and Child A newborn
Normal and Abnormal Development in the Infant and Pre-School Child Steven Bachrach, M.D. Co-Director, Cerebral Palsy Program A.I. dupont Hospital for Children Development in the Infant and Child A newborn
 THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
The Child With Cerebral Palsy
 The Child With Cerebral Palsy Lisa Thornton, MD Medical Director, KidsRehab LaRabida Children's Hospital Schwab Rehabilitation Hospital University of Chicago Pritzker School of Medicine Cerebral Palsy
The Child With Cerebral Palsy Lisa Thornton, MD Medical Director, KidsRehab LaRabida Children's Hospital Schwab Rehabilitation Hospital University of Chicago Pritzker School of Medicine Cerebral Palsy
Clinical Medical Policy Outpatient Rehab Therapies (PT & OT) for Members With Special Needs
 Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
If baby was born 3 or more weeks prematurely, # of weeks premature: Last name: State/ Province: Home telephone number:
 Ages & Stages Questionnaires 2 1 month 0 days through 2 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
Ages & Stages Questionnaires 2 1 month 0 days through 2 months 30 days Month Questionnaire Please provide the following information. Use black or blue ink only and print legibly when completing this form.
CAROLINE S STORY. A real case demonstrating the unfairness of damage caps.
 CAROLINE S STORY A real case demonstrating the unfairness of damage caps. Caroline s Story Little Caroline was born pre-term and was at an increased risk of developing high levels of bilirubin. Her medical
CAROLINE S STORY A real case demonstrating the unfairness of damage caps. Caroline s Story Little Caroline was born pre-term and was at an increased risk of developing high levels of bilirubin. Her medical
Infant hearing screening will not hurt your baby, and will only take between 5 and 20 minutes. Ideally it is done whilst baby is asleep or settled.
 Early diagnosis of hearing loss will make a difference to your baby s life. Significant hearing loss is the most common condition present at birth. In the private sector, 3 in every 1000 babies are born
Early diagnosis of hearing loss will make a difference to your baby s life. Significant hearing loss is the most common condition present at birth. In the private sector, 3 in every 1000 babies are born
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
Hearing Tests And Your Child
 How Early Can A Child s Hearing Be Tested? Most parents can remember the moment they first realized that their child could not hear. Louise Tracy has often told other parents of the time she went onto
How Early Can A Child s Hearing Be Tested? Most parents can remember the moment they first realized that their child could not hear. Louise Tracy has often told other parents of the time she went onto
Facts on. Mental Retardation NATIONAL ASSOCIATION FOR RETARDED. 2709 Avenue E East P.O. Box 6109 Arlington, Texas 76011
 Facts on Mental Retardation NATIONAL ASSOCIATION FOR RETARDED CHILDREN 2709 Avenue E East P.O. Box 6109 Arlington, Texas 76011 This booklet was revised and updated in August, 1973 as part of an ongoing
Facts on Mental Retardation NATIONAL ASSOCIATION FOR RETARDED CHILDREN 2709 Avenue E East P.O. Box 6109 Arlington, Texas 76011 This booklet was revised and updated in August, 1973 as part of an ongoing
Related Services: How Do Special Needs Education Relate to Your Child?
 Related Services: How Do Special Needs Education Relate to Your Child? Family Driven Non-Profit 501(c)3 What makes FND unique is that the majority of our Board of Directors, all of our Management Staff
Related Services: How Do Special Needs Education Relate to Your Child? Family Driven Non-Profit 501(c)3 What makes FND unique is that the majority of our Board of Directors, all of our Management Staff
C CS. California Children Services Alameda County
 C CS California Children Services Alameda County The California Children Services (CCS) Program strives to assure access to medical services essential to the health and well-being of children with catastrophic
C CS California Children Services Alameda County The California Children Services (CCS) Program strives to assure access to medical services essential to the health and well-being of children with catastrophic
UNILATERAL SPATIAL NEGLECT Information for Patients and Families
 UNILATERAL SPATIAL NEGLECT Information for Patients and Families What is unilateral spatial neglect? Unilateral spatial neglect (USN) is the inability to pay attention to things on the side that is affected
UNILATERAL SPATIAL NEGLECT Information for Patients and Families What is unilateral spatial neglect? Unilateral spatial neglect (USN) is the inability to pay attention to things on the side that is affected
Physical Activity Developmental Chapters
 Physical Activity Developmental Chapters Infancy 0 11 Months INFANCY 0 11 MONTHS The first year of life is marked by dramatic changes in the amount and type of physical activity displayed. Infants spend
Physical Activity Developmental Chapters Infancy 0 11 Months INFANCY 0 11 MONTHS The first year of life is marked by dramatic changes in the amount and type of physical activity displayed. Infants spend
An Hour a Day to Play. Infant Activities
 An Hour a Day to Play Infant Activities #Good4Growth good4growth.com Fun & Engaging Activities for Kids of All Ages Presented is a list to help kids of all ages through the following: Physical Well Being
An Hour a Day to Play Infant Activities #Good4Growth good4growth.com Fun & Engaging Activities for Kids of All Ages Presented is a list to help kids of all ages through the following: Physical Well Being
Seeing, Thinking, and Doing in Infancy
 Seeing, Thinking, and Doing in Infancy How Children Develop Chapter 5 Infant Development Perception Action Learning Cognition Motor Development Reflexes Motor Milestones Current Views of Motor Development
Seeing, Thinking, and Doing in Infancy How Children Develop Chapter 5 Infant Development Perception Action Learning Cognition Motor Development Reflexes Motor Milestones Current Views of Motor Development
PUBLIC HEALTH IMPROVEMENT PARTNERSHIP
 PUBLIC HEALTH IMPROVEMENT PARTNERSHIP PUBLIC HEALTH ACTIVITIES & SERVICES INVENTORY TECHNICAL NOTES HEALTHY FAMILY DEVELOPMENT Nurse-Family Partnership Nurse-Family Partnership is a voluntary program of
PUBLIC HEALTH IMPROVEMENT PARTNERSHIP PUBLIC HEALTH ACTIVITIES & SERVICES INVENTORY TECHNICAL NOTES HEALTHY FAMILY DEVELOPMENT Nurse-Family Partnership Nurse-Family Partnership is a voluntary program of
Esotropia (Crossed Eye(s))
 Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
SPECIAL EDUCATION AND RELATED SERVICES
 i SPECIAL EDUCATION AND RELATED SERVICES Updated May 2008 i It is the policy of the South Dakota Department of Education, Office of Educational Services and Supports to provide services to all persons
i SPECIAL EDUCATION AND RELATED SERVICES Updated May 2008 i It is the policy of the South Dakota Department of Education, Office of Educational Services and Supports to provide services to all persons
Hearing Tests And Your Child
 HOW EARLY CAN A CHILD S HEARING BE TESTED? Most parents can remember the moment they first realized that their child could not hear. Louise Tracy has often told other parents of the time she went onto
HOW EARLY CAN A CHILD S HEARING BE TESTED? Most parents can remember the moment they first realized that their child could not hear. Louise Tracy has often told other parents of the time she went onto
Four Areas of Development: Infancy to Toddler
 Four Areas of Development: Infancy to Toddler Copyright Copyright Texas Education Agency, 2012. These Materials are copyrighted and trademarked as the property of the Texas Education Agency (TEA) and may
Four Areas of Development: Infancy to Toddler Copyright Copyright Texas Education Agency, 2012. These Materials are copyrighted and trademarked as the property of the Texas Education Agency (TEA) and may
UNIVERSAL NEWBORN HEARING SCREENING. 1 step. Newborn Hearing Screening. What every parent Should Know PROMOTE. PREVENT. PROTECT.
 UNIVERSAL NEWBORN HEARING SCREENING 1 step Newborn Hearing Screening What every parent Should Know PROMOTE. PREVENT. PROTECT. 1 step What is Newborn Infant Hearing Screening? A newborn hearing screening
UNIVERSAL NEWBORN HEARING SCREENING 1 step Newborn Hearing Screening What every parent Should Know PROMOTE. PREVENT. PROTECT. 1 step What is Newborn Infant Hearing Screening? A newborn hearing screening
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Brachial Plexus Palsy
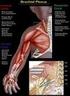 Patient and Family Education Brachial Plexus Palsy A Therapy Guide for Your Baby Brachial Plexus Palsy is caused by trauma to the nerves of the arm. This trauma may have caused muscle weakness, lack of
Patient and Family Education Brachial Plexus Palsy A Therapy Guide for Your Baby Brachial Plexus Palsy is caused by trauma to the nerves of the arm. This trauma may have caused muscle weakness, lack of
Chapter 7 Physical Development of the Infant
 Chapter 7 Physical Development of the Infant Mason is 10 months old. Although he is large for his age, his motor skills lag far behind those of other children his age. For example, Mason has trouble sitting
Chapter 7 Physical Development of the Infant Mason is 10 months old. Although he is large for his age, his motor skills lag far behind those of other children his age. For example, Mason has trouble sitting
a guide to understanding moebius syndrome a publication of children s craniofacial association
 a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
Ambulatory Outcome in Children with Developmental Delay. Rehab Al-Marzooq, MRCP, Arab Board, DCH*
 Bahrain Medical Bulletin, Vol 29, No. 2, June 2007 Ambulatory Outcome in Children with Developmental Delay Rehab Al-Marzooq, MRCP, Arab Board, DCH* Objective: To identify early predictors of walking in
Bahrain Medical Bulletin, Vol 29, No. 2, June 2007 Ambulatory Outcome in Children with Developmental Delay Rehab Al-Marzooq, MRCP, Arab Board, DCH* Objective: To identify early predictors of walking in
School Age Services INTERVENTION SERVICES FOR CHILDREN WITH DEVELOPMENTAL DELAYS
 INTERVENTION SERVICES FOR CHILDREN WITH DEVELOPMENTAL DELAYS Feel Good About Giving School Age Services EASTER SEALS SUPERIOR CALIFORNIA 3205 Hurley Way Sacramento, CA 95864 (916) 679-3155 www.myeasterseals.org
INTERVENTION SERVICES FOR CHILDREN WITH DEVELOPMENTAL DELAYS Feel Good About Giving School Age Services EASTER SEALS SUPERIOR CALIFORNIA 3205 Hurley Way Sacramento, CA 95864 (916) 679-3155 www.myeasterseals.org
Comprehensive Special Education Plan. Programs and Services for Students with Disabilities
 Comprehensive Special Education Plan Programs and Services for Students with Disabilities The Pupil Personnel Services of the Corning-Painted Post Area School District is dedicated to work collaboratively
Comprehensive Special Education Plan Programs and Services for Students with Disabilities The Pupil Personnel Services of the Corning-Painted Post Area School District is dedicated to work collaboratively
Epidemiology 521. Epidemiology of Maternal and Child Health Problems. Winter / Spring, 2010
 Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
So, how do we hear? outer middle ear inner ear
 The ability to hear is critical to understanding the world around us. The human ear is a fully developed part of our bodies at birth and responds to sounds that are very faint as well as sounds that are
The ability to hear is critical to understanding the world around us. The human ear is a fully developed part of our bodies at birth and responds to sounds that are very faint as well as sounds that are
ATLANTA SPEECH SCHOOL 3160 NORTHSIDE PARKWAY, NW ATLANTA, GA 30327 404-233-5332 APPLICATION AND CASE HISTORY QUESTIONNAIRE SUMMER PROGRAMS
 ATLANTA SPEECH SCHOOL 3160 RTHSIDE PARKWAY, NW ATLANTA, GA 30327 404-233-5332 APPLICATION AND CASE HISTORY QUESTIONNAIRE SUMMER PROGRAMS DATE: CHILD S NAME: BIRTH DATE: S. S. # PARENTS: ADDRESS: TELEPHONE:
ATLANTA SPEECH SCHOOL 3160 RTHSIDE PARKWAY, NW ATLANTA, GA 30327 404-233-5332 APPLICATION AND CASE HISTORY QUESTIONNAIRE SUMMER PROGRAMS DATE: CHILD S NAME: BIRTH DATE: S. S. # PARENTS: ADDRESS: TELEPHONE:
Aase Frostad Fasting, Specialist clinical psychology/neuropsychology, Huseby resource centre for the visual impaired
 Aase Frostad Fasting, Specialist clinical psychology/neuropsychology, Huseby resource centre for the visual impaired Assessing the potentialities of children with disabilities. Presentation at the Conference
Aase Frostad Fasting, Specialist clinical psychology/neuropsychology, Huseby resource centre for the visual impaired Assessing the potentialities of children with disabilities. Presentation at the Conference
CHAPTER 7: PHYSICAL ACTIVITY IN INFANCY
 CHAPTER 7: PHYSICAL ACTIVITY IN INFANCY Physical activity, defined as any bodily movement produced by skeletal muscles resulting in energy expenditure, is an important part of overall health and maintenance
CHAPTER 7: PHYSICAL ACTIVITY IN INFANCY Physical activity, defined as any bodily movement produced by skeletal muscles resulting in energy expenditure, is an important part of overall health and maintenance
SCHREIBER PEDIATRIC REHAB CENTER OF LANCASTER COUNTY SCOPE OF CARE. Characteristics of Persons Served
 SCHREIBER PEDIATRIC REHAB CENTER OF LANCASTER COUNTY SCOPE OF CARE Ages: Children ages birth to 21 years of age may be served. Characteristics of Persons Served Cultural: Medical Status: Diagnosis(es):
SCHREIBER PEDIATRIC REHAB CENTER OF LANCASTER COUNTY SCOPE OF CARE Ages: Children ages birth to 21 years of age may be served. Characteristics of Persons Served Cultural: Medical Status: Diagnosis(es):
Your Baby s Care Team
 UW MEDICINE PATIENT EDUCATION Your Baby s Care Team For parents of NICU infants Parents and Family You and your baby are the center of the NICU care team. As parents, you will give input and take part
UW MEDICINE PATIENT EDUCATION Your Baby s Care Team For parents of NICU infants Parents and Family You and your baby are the center of the NICU care team. As parents, you will give input and take part
Static Encephalopathy A Basis Explanation for Parents
 Static Encephalopathy A Basis Explanation for Parents Nancy J. Hitzfelder, M.D. Medical Director July 1999 This article may not be copied without the express written permission of Easter Seals of Greater
Static Encephalopathy A Basis Explanation for Parents Nancy J. Hitzfelder, M.D. Medical Director July 1999 This article may not be copied without the express written permission of Easter Seals of Greater
THE INFANT FOLLOW-UP PROJECT MANUAL OF OPERATIONS THE VERMONT OXFORD NETWORK
 THE INFANT FOLLOW-UP PROJECT Extremely-Low-Birth-Weight Infant Birth Year 2013 Cohort for infants born between January 1, 2013 and December 31, 2013 MANUAL OF OPERATIONS THE VERMONT OXFORD NETWORK July
THE INFANT FOLLOW-UP PROJECT Extremely-Low-Birth-Weight Infant Birth Year 2013 Cohort for infants born between January 1, 2013 and December 31, 2013 MANUAL OF OPERATIONS THE VERMONT OXFORD NETWORK July
Why does my child have a hearing loss?
 Introduction This factsheet will tell you about the range of tests that can be carried out to try to find the cause of your child s hearing loss. The process to find out why a child is deaf is sometimes
Introduction This factsheet will tell you about the range of tests that can be carried out to try to find the cause of your child s hearing loss. The process to find out why a child is deaf is sometimes
The Role of Occupational Therapy for Children with ACC
 These articles were originally published in The Callosal Connection, Fall 2007. The Callosal Connection is a publication of the ACC Network The Role of Occupational Therapy for Children with ACC By Erin
These articles were originally published in The Callosal Connection, Fall 2007. The Callosal Connection is a publication of the ACC Network The Role of Occupational Therapy for Children with ACC By Erin
Documentation Requirements ADHD
 Documentation Requirements ADHD Attention Deficit Hyperactivity Disorder (ADHD) is considered a neurobiological disability that interferes with a person s ability to sustain attention, focus on a task
Documentation Requirements ADHD Attention Deficit Hyperactivity Disorder (ADHD) is considered a neurobiological disability that interferes with a person s ability to sustain attention, focus on a task
Infant reflexes and stereotypies are very important in the process of development
 Infant Reflexes and Stereotypies Infant reflexes and stereotypies are very important in the process of development 2007 McGraw-Hill Higher Education. All rights reserved. Importance of Infant Reflexes
Infant Reflexes and Stereotypies Infant reflexes and stereotypies are very important in the process of development 2007 McGraw-Hill Higher Education. All rights reserved. Importance of Infant Reflexes
Edited by P Larking ACC Date report completed 18 January 2010
 Brief report Hart Walker Reviewer Adrian Purins AHTA Edited by P Larking ACC Date report completed 18 January 2010 1. Background Cerebral Palsy (CP) is a group of disorders that arise from brain damage
Brief report Hart Walker Reviewer Adrian Purins AHTA Edited by P Larking ACC Date report completed 18 January 2010 1. Background Cerebral Palsy (CP) is a group of disorders that arise from brain damage
Once your baby has good head control and can turn towards something interesting, a more advanced behavioural procedure can be used.
 How do we test the hearing of babies and children? An audiologist will select from a range of different tests to evaluate your child s hearing. The choice of test depends on the information that is needed
How do we test the hearing of babies and children? An audiologist will select from a range of different tests to evaluate your child s hearing. The choice of test depends on the information that is needed
Multiple Sclerosis (MS)
 Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
BABIES BORN TO ADDICTED MOTHERS
 BABIES BORN TO ADDICTED MOTHERS PATRICA M. MESSERLE LICENSED CLINICAL PSYCHOLOGIST, M.A., ABSNP LICENSED SCHOOL PSYCHOLOGIST DIPLOMATE OF THE AMERICAN BOARD OF SCHOOL- NEUROPSYCHOLOGY 1 Signs and Symptoms
BABIES BORN TO ADDICTED MOTHERS PATRICA M. MESSERLE LICENSED CLINICAL PSYCHOLOGIST, M.A., ABSNP LICENSED SCHOOL PSYCHOLOGIST DIPLOMATE OF THE AMERICAN BOARD OF SCHOOL- NEUROPSYCHOLOGY 1 Signs and Symptoms
SHAKEN BABY SYNDROME:
 SHAKEN BABY SYNDROME: A SAFETY MANUAL FOR HAND IN HAND CHILD CARE SHAKEN BABY SYNDROME BACKGROUND: The dangers of shaking a baby are becoming more and more apparent, often with disastrous results. The
SHAKEN BABY SYNDROME: A SAFETY MANUAL FOR HAND IN HAND CHILD CARE SHAKEN BABY SYNDROME BACKGROUND: The dangers of shaking a baby are becoming more and more apparent, often with disastrous results. The
What is the Spasticity Clinic?
 The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
Pediatric Hearing Assessment
 Pediatric Hearing Assessment Stanton Jones Key Points This chapter outlines the methods of hearing assessment that are appropriate for children from birth to adolescence. The importance of timely referral
Pediatric Hearing Assessment Stanton Jones Key Points This chapter outlines the methods of hearing assessment that are appropriate for children from birth to adolescence. The importance of timely referral
Technology in Music Therapy and Special Education. What is Special Education?
 Technology in Music Therapy and Special Education What is Special Education? Disabilities are categorized into the following areas: o Autism, visual impairment, hearing impairment, deaf- blindness, multiple
Technology in Music Therapy and Special Education What is Special Education? Disabilities are categorized into the following areas: o Autism, visual impairment, hearing impairment, deaf- blindness, multiple
The Arbor School of Central Florida Medical/Emergency Information Please Print
 Student's Name: Student s Date of Birth: Student's Address: Student's Home Phone: Primary Medical Diagnosis: The Arbor School of Central Florida Medical/Emergency Information Please Print Mothers Name:
Student's Name: Student s Date of Birth: Student's Address: Student's Home Phone: Primary Medical Diagnosis: The Arbor School of Central Florida Medical/Emergency Information Please Print Mothers Name:
0 3 Months Sensory Motor Checklist
 0 3 Months Sensory Motor Checklist Enjoys playful face-to-face interaction with people Coos in response to playful interaction Notices and responds to sounds Moves legs and arms off of surface when excited
0 3 Months Sensory Motor Checklist Enjoys playful face-to-face interaction with people Coos in response to playful interaction Notices and responds to sounds Moves legs and arms off of surface when excited
Cerebral Palsy Information
 Cerebral Palsy Information The following information was extracted from the Mayo Clinic s website Definition: "Cerebral palsy" is a general term for a group of disorders that appear during the first few
Cerebral Palsy Information The following information was extracted from the Mayo Clinic s website Definition: "Cerebral palsy" is a general term for a group of disorders that appear during the first few
Stronger together. We work with individuals, therapists and carers to design products with both a clinical and an emotional focus.
 Stronger together. We work with individuals, therapists and carers to design products with both a clinical and an emotional focus. Using the latest research and clinical understanding, we create practical
Stronger together. We work with individuals, therapists and carers to design products with both a clinical and an emotional focus. Using the latest research and clinical understanding, we create practical
Allied, Therapeutic and Psychology Extender Benefit
 Allied, Therapeutic and Psychology Extender Benefit 2013 The Allied, Therapeutic and Psychology Extender Benefit is available on the Enhanced Option only. Overview This document tells you about the Allied,
Allied, Therapeutic and Psychology Extender Benefit 2013 The Allied, Therapeutic and Psychology Extender Benefit is available on the Enhanced Option only. Overview This document tells you about the Allied,
Making the Connections District 75 NYCDOE
 Medical Syndromes and Their Effect on Learning Making the Connections District 75 NYCDOE Cerebral Palsy The most frequent medical condition in 12:1:4 classes Associated with other disabilities including
Medical Syndromes and Their Effect on Learning Making the Connections District 75 NYCDOE Cerebral Palsy The most frequent medical condition in 12:1:4 classes Associated with other disabilities including
