The Psoriatic Foot. A positive approach. to psoriasis and. psoriatic arthritis
|
|
|
- Arline Harmon
- 7 years ago
- Views:
Transcription
1 The Psoriatic Foot A positive approach to psoriasis and psoriatic arthritis
2 What are the aims of this leaflet? This leaflet is written to help you understand what can happen to the feet when affected by psoriasis or psoriatic arthritis. About psoriasis and psoriatic arthritis Psoriasis (sor-i ah-sis) is a long-term (chronic) scaling disease of the skin that affects about 2% of the UK population. It usually appears as red, raised, scaly patches known as plaques. Any part of the skin surface may be involved b u t t h e p l a q u e s m o s t commonly appear on the elbows, knees and scalp. It can be itchy but is not usually painful. It is not contagious; you cannot catch it from another person. Nail changes, including p i t t i ng a nd ri d g i ng, a re Plaque psoriasis present in 40-50% of people with psoriasis % of people with psoriasis will develop psoriatic arthritis. See our leaflet Nail Psoriasis. There does not seem to be any link between the severity of the psoriasis affecting the skin and the severity of psoriatic arthritis. For more detailed information on psoriasis and psoriatic arthritis see our leaflets What is Psoriasis? and What is Psoriatic Arthritis? About the foot The feet are an important part of the human anatomy; each foot has 26 bones, 33 joints and is controlled by muscles, tendons, and ligaments. The skin on the sole of the foot is different to that on the rest of the body, with a particularly large number of sweat pores. 2
3 To cope with the weight that is continually placed on them, the soles of the feet have the thickest layers of skin on the human body. They are, however, very sensitive and act as sensors when walking or standing. Therefore, anything that interferes or affects the feet can have a profound impact on function and general wellbeing. Psoriasis on the foot Most commonly, psoriasis on the foot looks similar to plaque psoriasis in other locations on the body and is called palmoplantar psoriasis. Often the plaques are thick and scaly, which can be painful and bleed if cracks appear. It is important to distinguish psoriasis from other conditions that affect the foot. Apart from plaque, there are other types of psoriasis which affect the foot and have a different appearance. Localised pustular psoriasis also known as palmoplantar pustular psoriasis (PPP) affects about 5% of people with psoriasis. It occurs most commonly between the ages of 20 and 60. It can be painful and is more common in women than men. About 10-25% of people with PPP have a family history of psoriasis but the precise reason why some people develop it is not known. PPP causes pustules on the palms and soles. As in all types of psoriasis, infection and stress are suspected trigger factors. PPP is normally recognisable by yellow/ white pustules approximately 2-3mm in diameter, appearing on fleshy areas of hands and feet, such as the base of the thumb and the sides of the heels. These pustules are sterile, which means they a r e n o t t h e r e s u l t o f infection. Antibiotics do not affect them. After a time, the pustules dry up and resolve, leaving brown stains on the skin surface. The natural Pustular psoriasis 3
4 history of the disease is usually cyclical (occurring often or repeatedly), with the appearance of new crops of pustules followed by periods of low activity in which the pustules resolve. See our leaflet Pustular Psoriasis. Acrodermatitis continua of Hallopeau is a very rare form of localised pustular psoriasis. This looks similar to palmoplantar pustular psoriasis, but is localised to the ends of the fingers and, less commonly still, the toes (acropustulosis). It usually starts after some trauma to the skin. It tends to be painful and frequently affects the nails. It may lead to loss of the nails. Bone changes can be seen in severe cases. It is difficult to treat and many therapies have been tried. Topical treatments are usually not very successful but occasionally systemic medications may help to clear the lesions and restore the nails. Nail involvement Given they are part of the skin, it is perhaps not surprising that nails can be affected by a skin disease such as psoriasis. Nail psoriasis is very common, yet no one knows why some people get nail involvement and others do not. Nails grow from the nail plate, which is just under the cuticle. In people who develop psoriasis of the nails, it is involvement of the nail plate that causes pitting, ridging, thickening, lifting and discolouration of the nail due to abnormalities in the growth of tissue in the nail bed. The nail is made of modified skin and, once it has grown, it can only be altered by filing or clipping. Treatments are usually directed at the nail bed or the nail folds that tuck around t h e e d g e s. Tr e a t e d inflammation in these tissues can result in better nail growth with fewer features of psoriasis, but treatment of nail psoriasis can be difficult. Nail psoriasis 4
5 Triggers of psoriasis It is not fully understood what causes psoriasis, but it is an inherited inflammatory disease. It can be triggered by events, illness or injury to the skin. A particular process known as Koebner's phenomenon or Koebnerisation is named after the German dermatologist Heinrich Koebner. Koebner found that people with psoriasis whose skin became traumatised following an injury, often developed a psoriatic lesion in the area, but where psoriasis had not previously be seen; such sites include cuts, bruises, burns, bumps, vaccinations, tattoos and other skin conditions. Diagnosis If you think you may have psoriasis on your foot or feet, it is best to get a diagnosis. Visiting your GP or asking your pharmacist is a good place to start. Alternatively, you may wish to see a local chiropodist (sometimes known as a podiatrist), particularly if your nails have become thickened and difficult to manage. Psoriasis on a foot or both feet may be diagnosed by simple examination, but if there is any doubt then referral to a specialist (dermatologist) may be required. It is unlikely that any specific test will be performed unless there is a suspicion of a fungal infection, when some samples may be taken for laboratory analysis. Treatments For plaque psoriasis on the foot, treatment will generally be similar to those recommended for other areas of the body, with the use of topical (applied to the skin) creams, ointment and gels. See our leaflet Treatments for Psoriasis: An overview. The use of phototherapy (ultraviolet light) may be considered, but availability and access to appropriate centres can sometimes be limited. It may be possible to 5
6 treat psoriasis affecting the hands and feet with localised p ho t o t he ra p y. Se e o ur l e a f l e t Psoriasis and Phototherapy. Palmoplantar pustular psoriasis is often difficult to treat, although some people do benefit from potent topical steroids combined with tar preparations. However, in most cases treatment with acitretin (a vitamin A derivative) tablets is the most effective. Treating nails can be problematic, as once the nail changes appear the damage has already occurred. It is important to check that other conditions that affect the nail, such as fungal infection, are not present, as these can often look similar to nail psoriasis. It is advisable to keep nails short and clean. See our leaflet Nail Psoriasis. Psoriatic arthritis in the foot The ankle is a hinge joint between the talus bone of the foot and the two bones of the lower leg, the tibia and fibula. The ankle joint lets you move your foot up and down. Other movements, such as tilting and rotation, occur at other joints in the foot itself. Each foot contains 26 bones which form joints where they meet. These joints are all lined with a synovial membrane that produces a lubricating oil. Many tendons pass around the ankle to connect the bones with the muscles that move them. These are also covered in synovial membrane and oiled with synovial fluid. In psoriatic arthritis, any part of the foot can be affected and become inflamed and painful, which in turn may lead to permanent disability. What happens? The synovial membranes that line joints, tendons and connective tissue become thickened and inflamed (tendonitis and enthesitis). This releases more fluid than normal so the joints and tendons become tender and swollen, which may result in: 6
7 pain tenderness swelling stiffness difficulty walking deformity (such as sausage-shaped toes) decreased range of movement locked joints joints feeling hot. The pattern of joints that may be involved can vary from person to person, and may just affect a small number of joints (oligoarthritis) or many joints (polyarthritis). Most commonly, psoriatic arthritis is asymmetric in pattern (not identical on both sides) unlike rheumatoid arthritis, which is symmetrical. In terms of symptoms, psoriatic arthritis can cause stiffness in the joints, particularly after a period of inactivity such as after waking up in the morning. Psoriatic arthritis Bones of the foot 7
8 can also cause swelling of an individual toe so it looks like a sausage, called dactylitis. S o m e p e o p l e a l s o experience heel pain because the Achilles tendon, which connects the calf muscles to the heel bone, has become inflamed. Swelling around the ankle is Dactylitis common in psoriatic arthritis affecting the foot. Psoriatic arthritis can lead to shortening or clawing of the toes, hyperextension of the big toe and some in-rolling of the ankle with flattening of the metatarsal arch. Stiffness of the joints, rather than instability, also happens quickly and can become irreversible within a few months. The occurrence of calluses and ulcers on the soles of the foot is less common than in rheumatoid arthritis (RA) but corns over the interphalangeal joints can be very painful. Symptoms tend to flare up and then die down again. If the inflammation is persistent and left untreated, toe joints can fuse together, with the space between the individual joints being lost. You should always seek medical advice if you experience stiffness in your joints especially after inactivity, severe pain, redness or swelling in one or both feet, whether this is mild or severe. It is essential to minimise the inflammation to avoid permanent joint deformity. Causes and triggers As with skin psoriasis, the cause of psoriatic arthritis is unknown, with an event or illness often considered a trigger. There is also a theory (hypothesis) of a 'deep Koebner phenomenon' which might initiate psoriatic arthritis, although this is yet to be proven. 8
9 Getting a diagnosis of psoriatic arthritis The presence of psoriasis may provide an indication of psoriatic arthritis when someone develops joint symptoms. Psoriatic arthritis can develop in people with a lot or a little of psoriasis, and may be more common in people with nail psoriasis. As well as joint symptoms, psoriatic arthritis can lead to feeling tired. Many people become frustrated by a lack of diagnosis; psoriatic arthritis tends to have periods of improvement and worsening, which may also be attributed to mechanical joint problems and not inflammatory arthritis. If you have the symptoms of inflammatory arthritis, such as psoriatic arthritis, your doctor will often refer you to a rheumatologist. In some cases, further tests (blood) and imagery (X-ray, ultrasound, MRI) may be sought, although this will depend on the individual circumstances and level of confidence in the initial diagnosis. Treatment In most instances, specific treatment to the foot is necessary to some degree. Treating psoriatic arthritis in the foot will include many of the therapies used in managing arthritis elsewhere. The aim of therapy is to reduce inflammation, pain and avoid permanent disability. Initial treatment is likely to include analgesia (pain relief), often the anti-inflammatory painkillers recommended such as ibuprofen, are those that can be supplied over the counter (OTC). To treat the inflammation and swelling a prescription-only medicine (POM) may be required and would only be available from your doctor. Treatments may include corticosteroid injections to the worst involved areas (painful, but effective for up to 6 months), oral (tablet) corticosteroids, anti-inflammatory gels and disease-modifying drugs such as methotrexate. Sometimes, in large joints, a procedure called arthrocentesis is carried out. This involves drawing out 9
10 (aspirating) the fluid for investigation for infection and the diagnosis of inflammatory conditions. The treatments listed above may only be prescribed if you have seen a rheumatologist. See our leaflet Treatments for Psoriatic Arthritis: An overview. Surgery and the psoriatic foot Orthopaedic surgery to correct deformed joints is only justified in the presence of long-standing deformity where pain is preventing adequate mobility and all alternative medical treatments have failed. The advancement of newer techniques in recent years has seen better results in small joint replacement, but such procedures still need careful consideration and discussion with advice from an appropriate surgeon. Physiotherapy It is always advisable to rest severely inflamed joints, but physiotherapy and exercise can help to maintain mobility of your joints so they are less likely to become stiff and seize up. See our leaflet Physiotherapy and Exercise: Psoriatic Arthritis. How successful are the treatments? Anti-inflammatory drugs can help to reduce pain, swelling and stiffness. Unfortunately, however, they can make skin symptoms worse in some people. Steroid injections to joints may give relief. Disease-modifying drugs such as methotrexate can damp down both skin and joint symptoms, as can targeted biologic agents. In some cases, surgery to remove a thickened synovial membrane (synovectomy), realign a joint (osteotomy) or to fuse a joint (arthrodesis) may stop pain which results from movement. Sometimes it is possible to remove the painful end of a bone (excision arthroplasty). 10
11 Remember: All treatments may have unwanted side effects or require special precautions (eg during pregnancy). Always make sure you have all the information before embarking on any course of therapy; this includes reading the patient information leaflets (PILs) provided with your medicines. Other common conditions If you develop problems with your foot, such as sores, rashes, nail deformities or painful swollen joints, do remember that they may not be caused by psoriasis or psoriatic arthritis. Some common skin conditions that affect the feet include: athlete s foot (tinea pedis) - caused by fungal infections plantar warts (verruccas) - generally appear on the soles of the foot with a callus appearance but are caused by the human papollomavirus (HPV) calluses - often the result of an ill-fitting shoe that rubs, causing the skin to harden corns - similar to calluses, but often found on the top of a toe pitted keratolysis - usually on the soles and caused by bacteria dyshidrotic eczema (dyshidrotic dermatitis) - an itchy rash, the cause of which is unknown, but which worsens in warm weather ingrown toenails - due to poor nail care, where the nail is cut too short and grows into the skin, causing pain and swelling diabetic ulcers - due to decreased blood flow and poor circulation in someone with diabetes. Some common joint conditions that affect the feet include: gout - where crystals of uric acid are deposited in the joints, tendons and skin 11
12 bunions - swellings and tenderness when the joints in your big toe no longer fit together as they should, often caused by ill-fitting shoes heel spurs (plantar fasciitis or fasciosis) - inflammation at the site where the fascia attaches under the heel heel bursitis (subcalcaneal bursitis) - inflammation of the fluid-filled sac (bursa) located between the skin of the back of the heel and the Achilles tendon Achilles tendinosis - the Achilles tendon is placed under more pressure than it can cope with and small tears develop, along with inflammation and, in some cases, leading to tendon rupture chronic inflammation of the heel pad - caused by a heavy heel strike giving rise to a dull ache in the heel, which increases during the day. What can I do to help my feet? The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist. For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait. If you are diagnosed with psoriasis, develop a treatment regime that works for you; often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier. If you have nail involvement, keep nails trimmed and 12
13 clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS. If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you. Useful contacts: For information about health matters in general and how to access services in the UK, the following websites provide national and local information. NHS Choices (England): NHS 24 (Scotland): Health in Wales: HSCNI Services (Northern Ireland): These sites are the official sites for the National Health Service and provide links and signposting services to recognised organisations and charities. References: problems-podiatrist.aspx - accessed 20/1/16 Gelfand JM, Weinstein R, Porter SB, Neimann AL, Berlin JA, Margolis DJ. Prevalence and treatment of psoriasis in the United Kingdom: a population-based study. Arch Dermatol 2005;141: Cohen MR, Reda DJ, Clegg DO. Baseline relationships between psoriasis and psoriatic arthritis: analysis of 221 patients with active psoriatic arthritis. Department of Veterans Affairs cooperative study group on seronegative spondyloarthropathies. J Rheumatol 1999;26: Alamanos Y, Voulgari PV, Drosos AA. Incidence and prevalence of psoriatic arthritis: a systematic review. J 13
14 Rheumatol 2008;35: Ibrahim G, Waxman R, Helliwell PS. The prevalence of psoriatic arthritis in people with psoriasis. Arthritis Rheum 2009;61: Krueger JG, Bowcock A. Psoriasis pathophysiology: current concepts of pathogenesis. Ann Rheum Dis 2005;64 Suppl 2:ii30-6. Gladman DD, Shuckett R, Russell ML, Thorne JC, Schachter RK. Psoriatic arthritis (PsA) - an analysis of 220 patients. Q J Med 1987;62: Gladman DD, Antoni C, Mease P, Clegg DO, Nash P. Psoriatic arthritis: epidemiology, clinical features, course, and outcome. Ann Rheum Dis 2005;64 Suppl 2:ii14-7. Stoll ML, Punaro M. Psoriatic juvenile idiopathic arthritis: a tale of two subgroups. Curr Opin Rheumatol Alamino RP, Maldonado Cocco JA, Citera G, et al. Differential features between primary ankylosing spondylitis and spondylitis associated with psoriasis and inflammatory bowel disease. J Rheumatol McHugh NJ, Balachrishnan C, Jones SM. Progression of peripheral joint disease in psoriatic arthritis: a 5-yr prospective study. Rheumatology (Oxford) 2003;42: Ritchlin CT, Kavanaugh A, Gladman DD, et al. Treatment recommendations for psoriatic arthritis. Ann Rheum Dis 2009;68: Gelfand JM, Gladman DD, Mease PJ, et al. Epidemiology of psoriatic arthritis in the population of the United States. J Am Acad Dermatol 2005;53:573. About this information This material was produced by PAPAA. Please be aware that research and development of treatments is ongoing. For the latest information or any amendments to this material, please contact us or visit our website. The site contains information on treatments and includes patient experiences and case histories. 14
15 Original text written by PAPAA January This edition reviewed and revised by Dr Ruth Murphy, consultant adult and paediatric dermatology consultant, Sheffield Teaching Hospitals NHS Foundation Trust, Dr Esther Burden-Teh, dermatology registrar and clinical research fellow, The Centre of Evidence Based Dermatology, University of Nottingham and Dr Satyapal Rangaraj, consultant paediatric and adolescent rheumatologist, Nottingham University Hospitals NHS Trust in April A lay and peer review panel has provided key feedback on this leaflet. The panel includes people with or affected by psoriasis and/or psoriatic arthritis. Published: May 2016 Review date: November 2018 PAPAA The Information Standard scheme was developed by the Department of Health to help the public identify trustworthy health and social care information easily. At the heart of the scheme is the standard itself a set of criteria that defines good quality health or social care information and the methods needed to produce it. To achieve the standard, organisations have to show that their processes and systems produce information that is: accurate evidence-based impartial accessible balanced well-written. The assessment of information producers is provided by independent certification bodies accredited by The United Kingdom Accreditation Service (UKAS). Organisations that meet The Standard can place the quality mark on their information materials and their website - a reliable symbol of quality and assurance. 15
16 The charity for people with psoriasis and psoriatic arthritis PAPAA, the single identity of the Psoriatic Arthropathy Alliance and the Psoriasis Support Trust. The organisation is independently funded and is a principal source of information and educational material for people with psoriasis and psoriatic arthritis in the UK. PAPAA supports both patients and professionals by providing material that can be trusted (evidencebased), which has been approved and contains no bias or agendas. PAPAA provides positive advice that enables people to be involved, as they move through their healthcare journey, in an informed way which is appropriate for their needs and any changing circumstances. Contact: PAPAA 3 Horseshoe Business Park, Lye Lane, Bricket Wood, St Albans, Herts. AL2 3TA Tel: Fax: info@papaa.org ISBN PF/05/16 Psoriasis and Psoriatic Arthritis Alliance is a company limited by guarantee registered in England and Wales No Registered Charity No Registered office: Acre House, William Road, London, NW1 3ER
Nail Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand what nail psoriasis is, what changes can
Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand what nail psoriasis is, what changes can
Nail Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand what nail psoriasis is, what changes can
Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand what nail psoriasis is, what changes can
Nail Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
A Guide to Heel Pain
 The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
Psoriatic arthritis FACTSHEET
 1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
Psoriatic Arthritis. What is psoriatic arthritis? Understanding joints. Who gets psoriatic arthritis? Page 1 of 5
 Page 1 of 5 Psoriatic Arthritis Psoriatic arthritis causes inflammation, pain, and swelling of joints in some people who have psoriasis. Other parts of the body may also be affected. For example, in many
Page 1 of 5 Psoriatic Arthritis Psoriatic arthritis causes inflammation, pain, and swelling of joints in some people who have psoriasis. Other parts of the body may also be affected. For example, in many
Scalp Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 10672 SCALP0913 Scalp Psoriasis 12pp final_layout 1 11/10/2013 18:13 Page 2 Scalp Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has
10672 SCALP0913 Scalp Psoriasis 12pp final_layout 1 11/10/2013 18:13 Page 2 Scalp Psoriasis A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has
It is worth noting that people with psoriasis can also develop other forms of arthritis such as rheumatoid arthritis and osteoarthritis.
 Psoriatic Arthritis Main Colour - pantone 2597u Research - pantone 206u Children - pantone 123 4 What is psoriatic arthritis? Psoriatic arthritis is an inflammatory joint disease associated with psoriasis.
Psoriatic Arthritis Main Colour - pantone 2597u Research - pantone 206u Children - pantone 123 4 What is psoriatic arthritis? Psoriatic arthritis is an inflammatory joint disease associated with psoriasis.
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Plantar Fasciitis. Plantar Fascia
 Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Psoriatic Arthritis www.arthritis.org.nz
 Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Heel pain and Plantar fasciitis
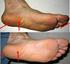 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
Psoriasis and Sensitive Areas
 Psoriasis and Sensitive Areas A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet is written to help you understand the most sensitive areas of the
Psoriasis and Sensitive Areas A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet is written to help you understand the most sensitive areas of the
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
Psoriatic Arthritis. Psoriatic Arthritis 3/05
 Psoriatic Arthritis 3/05 Psoriatic Arthritis Arthritis Ireland, 1 Clanwilliam Square, Grand Canal Quay, Dublin 2 T: (01) 661 8188 F: (01) 661 8261 www.arthritisireland.ie What is in this booklet? This
Psoriatic Arthritis 3/05 Psoriatic Arthritis Arthritis Ireland, 1 Clanwilliam Square, Grand Canal Quay, Dublin 2 T: (01) 661 8188 F: (01) 661 8261 www.arthritisireland.ie What is in this booklet? This
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
FEET and PSORIATIC ARTHRITIS. Louise Skipp Podiatrist, Sirona Care and Health, Bath
 FEET and PSORIATIC ARTHRITIS Louise Skipp Podiatrist, Sirona Care and Health, Bath What would you like to know? Common problems Practical tips What you can do to help yourself When to seek help and from
FEET and PSORIATIC ARTHRITIS Louise Skipp Podiatrist, Sirona Care and Health, Bath What would you like to know? Common problems Practical tips What you can do to help yourself When to seek help and from
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Arthritis www.patientedu.org
 written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
X-Plain Rheumatoid Arthritis Reference Summary
 X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? Rheumatoid arthritis (RA) is the third most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most
Rheumatoid Arthritis www.arthritis.org.nz Did you know? Rheumatoid arthritis (RA) is the third most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most
Rheumatoid Arthritis: Symptoms, Causes, and Treatments of Rheumatoid Foot and Ankle
 Rheumatoid arthritis is the most common form of inflammatory arthritis, affecting about two to three million Americans. Rheumatoid arthritis is a symmetric disease, meaning that it will usually involve
Rheumatoid arthritis is the most common form of inflammatory arthritis, affecting about two to three million Americans. Rheumatoid arthritis is a symmetric disease, meaning that it will usually involve
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Helpline No: 0861 30 30 30
 ARTHRITIS FOUNDATION Registered Nonprofit Organisation - No. 002-847 NPO Helpline No: 0861 30 30 30 PSORIATIC ARTHRITIS This information leaflet is published by the Arthritis Foundation as part of our
ARTHRITIS FOUNDATION Registered Nonprofit Organisation - No. 002-847 NPO Helpline No: 0861 30 30 30 PSORIATIC ARTHRITIS This information leaflet is published by the Arthritis Foundation as part of our
Rheumatoid Arthritis of the Foot and Ankle
 Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Treatments for Psoriatic Arthritis:
 Treatments for Psoriatic Arthritis: An overview A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand the treatments
Treatments for Psoriatic Arthritis: An overview A positive approach to psoriasis and psoriatic arthritis What are the aims of this leaflet? This leaflet has been written to help you understand the treatments
FUNGAL INFECTIONS OF THE NAILS
 FUNGAL INFECTIONS OF THE NAILS What are the aims of this leaflet? This leaflet has been written to help you understand more about fungal infections of the nails. It tells you what they are, what causes
FUNGAL INFECTIONS OF THE NAILS What are the aims of this leaflet? This leaflet has been written to help you understand more about fungal infections of the nails. It tells you what they are, what causes
How can DIABETES affect my FEET? Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
TOPICAL TREATMENTS FOR PSORIASIS
 TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Your psoriasis story. Print this out, answer the questions, then share it with your doctor
 Your psoriasis story Print this out, answer the questions, then share it with your doctor 1 SYMPTOMS Surface Area Your doctor will use a variety of different factors to measure the severity of your disease,
Your psoriasis story Print this out, answer the questions, then share it with your doctor 1 SYMPTOMS Surface Area Your doctor will use a variety of different factors to measure the severity of your disease,
Osteoarthritis progresses slowly and the pain and stiffness it causes worsens over time.
 Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
For more information, please contact the National Psoriasis Foundation at 800-723-9166 or
 For more information, please contact the National Psoriasis Foundation at 800-723-9166 or www.psoriasis.org. PSORIASIS 101: LEARNING TO LIVE IN THE SKIN YOU RE IN is part of an awareness program to educate
For more information, please contact the National Psoriasis Foundation at 800-723-9166 or www.psoriasis.org. PSORIASIS 101: LEARNING TO LIVE IN THE SKIN YOU RE IN is part of an awareness program to educate
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
How To Treat Psoriatic Arthritis
 Taking control of your Psoriatic Arthritis A practical guide to treatments, services and lifestyle choices Taking control of your psoriatic arthritis 1 How can this booklet help you? This booklet is designed
Taking control of your Psoriatic Arthritis A practical guide to treatments, services and lifestyle choices Taking control of your psoriatic arthritis 1 How can this booklet help you? This booklet is designed
How To Treat Heel Pain
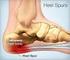 Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
What is Psoriasis? Common Areas Affected. Type Who Does it Affect Characteristics
 What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
GET A HANDLE ON YOUR HEEL PAIN GUIDE
 GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
Treat Your Feet: Foot care for people with diabetes
 Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Recognise, Respond, Relieve, Rheumatoid Arthritis
 Recognise, Respond, Relieve, Rheumatoid Arthritis Anybody can develop rheumatoid arthritis. It can develop at any age in adults but is more common in people in their 40s and 50s. It is two to three times
Recognise, Respond, Relieve, Rheumatoid Arthritis Anybody can develop rheumatoid arthritis. It can develop at any age in adults but is more common in people in their 40s and 50s. It is two to three times
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
NURS 821 Alterations in the Musculoskeletal System. Rheumatoid Arthritis. Type III Hypersensitivity Response
 NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN
 PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN What is Plantar Fasciitis? Plantar fasciitis is pain in the heel and arch area of the foot. The plantar fascia is a strong
PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN What is Plantar Fasciitis? Plantar fasciitis is pain in the heel and arch area of the foot. The plantar fascia is a strong
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
GENETIC ANALYSIS OF PSORIASIS AND PSORIATIC ARTHRITIS Department of Dermatology, University of Michigan
 GENETIC ANALYSIS OF PSORIASIS AND PSORIATIC ARTHRITIS Department of Dermatology, University of Michigan SELF ASSESSMENT FORM FOR STUDY SUBJECTS AND CONTROLS Accession Number (will be filled in by lab)
GENETIC ANALYSIS OF PSORIASIS AND PSORIATIC ARTHRITIS Department of Dermatology, University of Michigan SELF ASSESSMENT FORM FOR STUDY SUBJECTS AND CONTROLS Accession Number (will be filled in by lab)
Forefoot deformity correction
 Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
PRACTICAL HELP FROM THE ARTHRITIS FOUNDATION. www.arthritis.org 800-283-7800. Psoriatic Arthritis
 Psoriatic Arthritis WHAT IS PSORIATIC ARTHRITIS? Psoriatic (sore-ee-aah-tick) arthritis is a condition that causes pain and swelling in joints and scaly patches on the skin. Psoriatic arthritis occurs
Psoriatic Arthritis WHAT IS PSORIATIC ARTHRITIS? Psoriatic (sore-ee-aah-tick) arthritis is a condition that causes pain and swelling in joints and scaly patches on the skin. Psoriatic arthritis occurs
Plantar Fascia Release
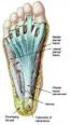 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Raynaud s phenomenon, Scleroderma and associated disorders
 Patient information Raynaud s phenomenon, Scleroderma and associated disorders Vascular Surgery Surgical Division PIF 202/V5 What is Raynaud s phenomenon? Raynaud s phenomenon is a condition where the
Patient information Raynaud s phenomenon, Scleroderma and associated disorders Vascular Surgery Surgical Division PIF 202/V5 What is Raynaud s phenomenon? Raynaud s phenomenon is a condition where the
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Page 2 of 6 plantar fascia. This is called the windlass mechanism. Later, we'll discuss how this mechanism is used to treat plantar fasciitis with str
 Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
Podiatric Medicine. What is a Podiatrist?
 Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
LUPUS. and the Feet LUPUSUK 2015
 16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris. Copyright
 Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris The patient: a 57 year-old man, with a history of psoriatic nail dystrophy for 10 years Past
Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris The patient: a 57 year-old man, with a history of psoriatic nail dystrophy for 10 years Past
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Rheumatology. Rheumatoid Arthritis
 Rheumatology Rheumatoid Arthritis The Rheumatology service specialises in the diagnosis and treatment of diseases affecting the musculoskeletal system. Other than providing inpatient and outpatient consultation,
Rheumatology Rheumatoid Arthritis The Rheumatology service specialises in the diagnosis and treatment of diseases affecting the musculoskeletal system. Other than providing inpatient and outpatient consultation,
Rheumatoid Arthritis
 Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
PSORIASIS AND ITS. Learn how vitamin D medications play an important role in managing plaque psoriasis
 PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
Condition Psoriatic arthritis. Psoriatic arthritis. This booklet provides information and answers to your questions about this condition.
 Condition Psoriatic arthritis Psoriatic arthritis This booklet provides information and answers to your questions about this condition. What is psoriatic arthritis? Psoriatic arthritis is a condition that
Condition Psoriatic arthritis Psoriatic arthritis This booklet provides information and answers to your questions about this condition. What is psoriatic arthritis? Psoriatic arthritis is a condition that
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Information on Rheumatoid Arthritis
 Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Excision or Open Biopsy of a Breast Lump Your Operation Explained
 Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Trochanteric Bursitis Self Management for Patients
 Trochanteric Bursitis Self Management for Patients Updated May 2010 What is the Trochanteric Bursa? The trochanteric bursa is a fluid-filled sac that functions as a gliding surface to reduce friction between
Trochanteric Bursitis Self Management for Patients Updated May 2010 What is the Trochanteric Bursa? The trochanteric bursa is a fluid-filled sac that functions as a gliding surface to reduce friction between
PATIENT RESOURCES: PSORIASIS
 PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
Polymyalgia Rheumatica www.arthritis.org.nz
 Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Osteoarthritis of the ankle
 1 What is osteoarthritis of the ankle? The ankle joint is formed by the upper bone at the front of the foot (the talus) and the leg bones (the tibia and fibula). The ankle is made up of a hinge joint which
1 What is osteoarthritis of the ankle? The ankle joint is formed by the upper bone at the front of the foot (the talus) and the leg bones (the tibia and fibula). The ankle is made up of a hinge joint which
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
Development and Validation of a Screening Questionnaire for Psoriatic Arthritis
 Development and Validation of a Screening Questionnaire for Psoriatic Arthritis Dafna D. Gladman 1, Catherine T. Schentag 1, Brian D. Tom 2, Vinod Chandran 1, Cheryl F. Rosen 1 Vernon T. Farewell 2 1 University
Development and Validation of a Screening Questionnaire for Psoriatic Arthritis Dafna D. Gladman 1, Catherine T. Schentag 1, Brian D. Tom 2, Vinod Chandran 1, Cheryl F. Rosen 1 Vernon T. Farewell 2 1 University
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES
 DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
Psoriatic Arthritis. Ewa Olech, MD Division of Rheumatology University of Nevada School of Medicine Las Vegas
 Psoriatic Arthritis Ewa Olech, MD Division of Rheumatology University of Nevada School of Medicine Las Vegas The Spectrum of Spondyloarthritis Characteristics of the Spondyloarthritis Sacroiliac & spinal
Psoriatic Arthritis Ewa Olech, MD Division of Rheumatology University of Nevada School of Medicine Las Vegas The Spectrum of Spondyloarthritis Characteristics of the Spondyloarthritis Sacroiliac & spinal
Elbow arthroscopy. Key points
 Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Am I likely to develop. rheumatoid Arthritis? A guide for people with joint symptoms
 Am I likely to develop Rheumatoid rheumatoid Arthritis? arthritis? A guide for people with joint symptoms At a glance Rheumatoid arthritis (RA) is a common disease that causes painful and swollen joints,
Am I likely to develop Rheumatoid rheumatoid Arthritis? arthritis? A guide for people with joint symptoms At a glance Rheumatoid arthritis (RA) is a common disease that causes painful and swollen joints,
Case Scenarios. Case Scenario 1 Group A
 Case Scenarios Prior to the workshop please work through the following scenario and be prepared to present this to the rest of the group. You can work in groups of 3-4. Specialist nurses, phototherapy
Case Scenarios Prior to the workshop please work through the following scenario and be prepared to present this to the rest of the group. You can work in groups of 3-4. Specialist nurses, phototherapy
Rheumatoid Arthritis. Disease RA Final.indd 2 15. 6. 10. 11:23
 Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
This is caused by muscle strain to the Achilles tendon in the heel of the foot.
 Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Profile of Psoriatic Arthritis: What to expect as a typical patient Dr Deepak Jadon
 Profile of Psoriatic Arthritis: What to expect as a typical patient Dr Deepak Jadon Rheumatology Specialist Registrar & PhD Research Fellow 2 Overview Back ground on psoriatic arthritis (PsA) Epidemiology
Profile of Psoriatic Arthritis: What to expect as a typical patient Dr Deepak Jadon Rheumatology Specialist Registrar & PhD Research Fellow 2 Overview Back ground on psoriatic arthritis (PsA) Epidemiology
The Many Causes of Joint Pain
 I n t r o d u c t i o n The Many Causes of Joint Pain there are about a hundred different forms of arthritis, an umbrella term for diseases with symptoms that include joint and musculoskeletal pain. And
I n t r o d u c t i o n The Many Causes of Joint Pain there are about a hundred different forms of arthritis, an umbrella term for diseases with symptoms that include joint and musculoskeletal pain. And
Taking control of your Psoriatic Arthritis
 Taking control of your Psoriatic Arthritis A practical guide to treatments, services and lifestyle choices How can this booklet help you This booklet is designed for people who have psoriatic arthritis.
Taking control of your Psoriatic Arthritis A practical guide to treatments, services and lifestyle choices How can this booklet help you This booklet is designed for people who have psoriatic arthritis.
Psoriatic Arthritis. having psoriatic arthritis.
 Psoriatic Arthritis having psoriatic arthritis. Psoriatic arthritis is a chronic disease characterized by a form of inflammation of the skin (psoriasis) and joints (inflammatory arthritis). Psoriasis is
Psoriatic Arthritis having psoriatic arthritis. Psoriatic arthritis is a chronic disease characterized by a form of inflammation of the skin (psoriasis) and joints (inflammatory arthritis). Psoriasis is
A Patient s Guide to Plantar Fasciitis. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Plantar Fasciitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Plantar Fasciitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Outline. The Agony of the Foot: Disclosure. Plantar Fasciitis. Top 5 Foot and Ankle Problems in Primary Care. Daniel Thuillier, M.D.
 The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
www.noc.nhs.uk Achilles Tendinopathy: Advice and Management Delivering Excellence oxsport@noc Department of Sport and Exercise Medicine
 www.noc.nhs.uk Achilles Tendinopathy: Advice and Management Delivering Excellence oxsport@noc Department of Sport and Exercise Medicine Are we speaking your language? If you would like information in another
www.noc.nhs.uk Achilles Tendinopathy: Advice and Management Delivering Excellence oxsport@noc Department of Sport and Exercise Medicine Are we speaking your language? If you would like information in another
Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Local steroid injections
 Drug information Local steroid injections Local steroid injections This leaflet provides information on local steroid injections and will answer any questions you have about the treatment. Arthritis Research
Drug information Local steroid injections Local steroid injections This leaflet provides information on local steroid injections and will answer any questions you have about the treatment. Arthritis Research
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Studies tell us the pain will be gone or improved significantly in ¾ of patients in 4 weeks and 9/10ths of patients in 6 weeks.
 Back pain is common and ranges from mild to severe pain. Most episodes soon ease within 4 weeks and are not due to serious illness. Keeping active is the most important message along with painkillers if
Back pain is common and ranges from mild to severe pain. Most episodes soon ease within 4 weeks and are not due to serious illness. Keeping active is the most important message along with painkillers if
Arthritis: An Overview. Michael McKee, MD, MPH February 23, 2012
 Arthritis: An Overview Michael McKee, MD, MPH February 23, 2012 Supporters Deaf Health Talks is possible through the support of: Rochester Recreation Club for the Deaf ( REAP ) Deaf Health Community Committee
Arthritis: An Overview Michael McKee, MD, MPH February 23, 2012 Supporters Deaf Health Talks is possible through the support of: Rochester Recreation Club for the Deaf ( REAP ) Deaf Health Community Committee
Treating psoriasis and psoriatic arthritis. A booklet for patients and carers
 Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Diabetes and your feet
 The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
