Post-traumatic stress disorder (PTSD)
|
|
|
- Suzan Taylor
- 7 years ago
- Views:
Transcription
1 Issue date: March 2005 Quick reference guide Post-traumatic stress disorder (PTSD) The management of PTSD in adults and children in primary and secondary care Clinical Guideline 26 Developed by the National Collaborating Centre for Mental Health
2 Ordering information Copies of this quick reference guide can be obtained from the NICE website at or from the NHS Response Line by telephoning and quoting reference number N0848. Information for the public on the guideline ( Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children ) is also available from the NICE website at or from the NHS Response Line (quote reference number N0849 for a version in English and N0850 for a version in English and Welsh). This guidance is written in the following context This guidance represents the view of the Institute, which was arrived at after careful consideration of the evidence available. Health professionals are expected to take it fully into account when exercising their clinical judgement. The guidance does not, however, override the individual responsibility of health professionals to make decisions appropriate to the circumstances of the individual patient, in consultation with the patient and/or guardian or carer. National Institute for Clinical Excellence MidCity Place 71 High Holborn London WC1V 6NA ISBN: Published by the National Institute for Clinical Excellence March 2005 Artwork by LIMA Graphics Ltd, Frimley, Surrey Printed by Abba Litho Sales Limited, London National Institute for Clinical Excellence, March All rights reserved. This material may be freely reproduced for educational and not-for-profit purposes within the NHS. No reproduction by or for commercial organisations is permitted without the express written permission of the Institute.
3 Contents Patient-centred care 2 Grading of the recommendations 2 Contents Key priorities for implementation 3 Post-traumatic stress disorder (PTSD) 5 Recognition 6 Recognition in primary care and general hospital settings 6 Specific recognition issues for children and young people 7 Screening 8 Screening after a major disaster 8 Screening refugees and asylum seekers 8 Assessment and coordination of care 8 Support to families and carers 9 Practical and social support 9 Language and culture 10 Care across all conditions 10 Comorbidities 11 Depression 11 High risk of suicide or at risk of harming others 11 Drug or alcohol problem 11 Personality disorder 11 Death of a close friend or relative 11 Treatment of PTSD 12 Early interventions 12 Interventions where symptoms have been present for more than 3 months after a trauma 13 Drug treatments 14 Children and young people 15 Disaster planning 16 Implementation 17 Further information Back cover NICE Guideline: quick reference guide Post-traumatic stress disorder 1
4 Grading of the recommendations/patient-centred care Patient-centred care Treatment and care should take into account patients individual needs and preferences. Good communication is essential, supported by evidence-based information, to allow patients to reach informed decisions about their care. Carers and relatives should have the chance to be involved in discussions unless the patient considers it inappropriate. Grading of the recommendations This quick reference guide summarises the recommendations in the NICE clinical guideline Post-traumatic stress disorder (PTSD): the management of PTSD in adults and children in primary and secondary care. The recommendations are based on the best available evidence and are graded A, B, C or good practice point ( GPP ) depending on the type of evidence they are based on. For more information on the grading system, see the NICE guideline ( 2 NICE Guideline: quick reference guide Post-traumatic stress disorder
5 Key priorities for implementation The following recommendations have been identified as priorities for implementation. Initial response to trauma For individuals who have experienced a traumatic event the systematic provision to that individual alone of brief, single-session interventions (often referred to as debriefing) that focus on the traumatic incident should not be routine practice when delivering services. Key priorities for implementation Where symptoms are mild and have been present for less than 4 weeks after the trauma, watchful waiting, as a way of managing the difficulties presented by individual people with post-traumatic stress disorder (PTSD), should be considered. A follow-up contact should be arranged within 1 month. Trauma-focused psychological treatment Trauma-focused cognitive behavioural therapy should be offered to those with severe post-traumatic symptoms or with severe PTSD in the first month after the traumatic event. These treatments should normally be provided on an individual outpatient basis. All people with PTSD should be offered a course of trauma-focused psychological treatment (trauma-focused cognitive behavioural therapy [CBT] or eye movement desensitisation and reprocessing [EMDR]). These treatments should normally be provided on an individual outpatient basis. NICE Guideline: quick reference guide Post-traumatic stress disorder 3
6 Key priorities for implementation Children and young people Trauma-focused CBT should be offered to older children with severe post-traumatic symptoms or with severe PTSD in the first month after the traumatic event. Children and young people with PTSD, including those who have been sexually abused, should be offered a course of trauma-focused CBT adapted as needed to suit their age, circumstances and level of development. Drug treatments for adults Drug treatments for PTSD should not be used as a routine first-line treatment for adults (in general use or by specialist mental health professionals) in preference to a trauma-focused psychological therapy. Drug treatments (paroxetine or mirtazapine for general use, and amitriptyline or phenelzine for initiation only by mental health specialists) should be considered for the treatment of PTSD in adults who express a preference not to engage in trauma-focused psychological treatment 1. Screening for PTSD For individuals at high risk of developing PTSD following a major disaster, consideration should be given (by those responsible for coordination of the disaster plan) to the routine use of a brief screening instrument for PTSD at 1 month after the disaster. 1 Paroxetine is the only drug listed with a current UK product licence for PTSD at the date of publication (March 2005). 4 NICE Guideline: quick reference guide Post-traumatic stress disorder
7 Post-traumatic stress disorder (PTSD) PTSD can develop in people of any age following a stressful event or situation of an exceptionally threatening or catastrophic nature. PTSD does not usually develop following generally upsetting situations such as divorce, loss of job, or failing an exam. Up to Effective treatment of PTSD can only take place if the 30% of people disorder is recognised. In some cases, for example experiencing a following a major disaster, specific arrangements to traumatic event screen people at risk may be considered. may develop PTSD For the vast majority of people with PTSD, opportunities for recognition and identification come as part of routine healthcare interventions, such as treatment following an assault or accident, or when domestic violence or childhood sexual abuse is disclosed. Post-traumatic stress disorder (PTSD) Symptoms often develop immediately after the traumatic Remember event but the onset of symptoms may be delayed in some that PTSD can people (less than 15%). PTSD is treatable even when also develop problems present many years after the traumatic event. in children following a Identification of PTSD in children People traumatic event presents particular problems, but with PTSD may is improved if children are asked not present for directly about their experiences. treatment for months or years Assessment can present significant challenges as after onset of many people avoid talking about their problems. symptoms NICE Guideline: quick reference guide Post-traumatic stress disorder 5
8 Recognition Recognition Recognition in primary care and general hospital settings Symptoms typically associated with PTSD are as follows: re-experiencing flashbacks, nightmares, repetitive and distressing intrusive images or sensory impressions; in children, these symptoms may include: reenacting the experience, repetitive play or frightening dreams without recognisable content avoidance avoiding people, situations or circumstances resembling or associated with the event hyperarousal hypervigilance for threat, exaggerated startle response, sleep problems, irritability and difficulty concentrating emotional numbing lack of ability to experience feelings, feeling detached from other people, giving up previously significant activities, amnesia for significant parts of the event depression drug or alcohol misuse anger unexplained physical symptoms (resulting in repeated attendance). If it is not immediately clear that symptoms relate to a specific traumatic event: ask patients if they have experienced a traumatic event and give examples (such as assault, rape, road traffic accidents, childhood sexual abuse and traumatic childbirth) GPP consider asking adults specifically about re-experiencing (including flashbacks and nightmares) or hyperarousal (including exaggerated startle response or sleep disturbance). GPP 6 NICE Guideline: quick reference guide Post-traumatic stress disorder
9 Specific recognition issues for children and young people Do not rely solely on information from the parent/guardian in any assessment for PTSD ask the child or young person separately and directly about PTSD symptoms. GPP Recognition Consider asking children and/or their parents/guardians about sleep disturbance or significant changes in sleeping patterns. C Children in emergency departments Inform the parents/guardians that PTSD may develop in children who have been involved in traumatic events. GPP Briefly describe the possible symptoms to the parents/guardians (e.g. sleep disturbance, nightmares, difficulty concentrating and irritability). GPP Suggest to parents/guardians they contact the child s GP if the symptoms persist beyond 1 month. GPP NICE Guideline: quick reference guide Post-traumatic stress disorder 7
10 Screening Screening Screening after a major disaster Those coordinating the disaster plan should consider using a brief screening instrument for PTSD 1 month after the event for individuals at high risk of developing PTSD following a major disaster. C Screening refugees and asylum seekers Those managing refugee programmes should consider using a brief screening instrument for PTSD for: programme refugees (people who are brought to the UK from a conflict zone through a programme organised by an agency such as the United Nations High Commission for Refugees) and asylum seekers at high risk of developing PTSD. This should be part of the initial refugee healthcare assessment and of any comprehensive physical and mental health screen. C Assessment and coordination of care Assessment and coordination of care GPs should take responsibility for initial assessment and coordination of care of PTSD sufferers in primary care and determine the need for emergency medical or psychiatric assessment. C Ensure that assessment is comprehensive and includes a risk assessment and assessment of physical, psychological and social needs, and is conducted by a competent individual. GPP Give PTSD sufferers sufficient information about effective treatments and take into account their preference for treatment. C If management is shared between primary and secondary care, establish a written agreement outlining the responsibilities for monitoring individuals. Where appropriate, use the Care Programme Approach (CPA) and share with the sufferer, their family and carers. C 8 NICE Guideline: quick reference guide Post-traumatic stress disorder
11 Support to families and carers Consider and, when appropriate, assess the impact of the traumatic event on all family members and consider providing appropriate support. GPP With the consent of the PTSD sufferer where appropriate, inform their family about common reactions to traumatic events, the symptoms of PTSD, and its course and treatment. GPP Inform families and carers about self-help and support groups and encourage them to participate. GPP Effectively coordinate the treatment of all family members if more than one family member has PTSD. GPP Practical and social support Provide practical advice to enable people with PTSD to access appropriate information and services for the range of emotional responses that may develop. GPP Identify the need for social support and advocate for the meeting of this need. GPP Consider offering help and advice on how continuing threats related to the traumatic event may be alleviated or removed. GPP Support to families and carers Practical and social support NICE Guideline: quick reference guide Post-traumatic stress disorder 9
12 Language and culture Language and culture Familiarise yourself with the cultural and ethnic backgrounds of PTSD sufferers. GPP Consider using interpreters and bicultural therapists if language or cultural differences present challenges for trauma-focused psychological interventions. GPP Pay particular attention to the identification of individuals with PTSD where the culture of the working or living environment is resistant to recognition of the psychological consequences of trauma. GPP Care across all conditions Care across all conditions When developing and agreeing a treatment plan, ensure individuals receive information about common reactions to traumatic events, the symptoms of PTSD, and its course and treatment. GPP Do not withhold or delay treatment because of court proceedings or applications for compensation. C Respond appropriately if a PTSD sufferer is anxious about and may avoid treatment (e.g. by following up those who miss scheduled appointments). C Keep technical language to a minimum and treat patients with respect, trust and understanding. GPP Only consider providing trauma-focused psychological treatment when the patient considers it safe to proceed. GPP Ensure that treatment is delivered by competent individuals who have received appropriate training. C 10 NICE Guideline: quick reference guide Post-traumatic stress disorder
13 Comorbidities Depression Consider treating the PTSD first unless the depression is so severe that it makes psychological treatment very difficult, in which case treat the depression first. C Comorbidities High risk of suicide or at risk of harming others Concentrate first on the management of this risk in PTSD sufferers. C Drug or alcohol problem Treat any significant drug or alcohol problem before treating the PTSD. C Personality disorder For PTSD sufferers with personality disorder, consider extending the duration of trauma-focused psychological interventions. C Death of a close friend or relative For patients who have lost a close friend or relative due to an unnatural or sudden death, assess for PTSD and traumatic grief and consider treating the PTSD first (without avoiding discussion of the grief). C NICE Guideline: quick reference guide Post-traumatic stress disorder 11
14 Treatment of PTSD Treatment of PTSD Early interventions Watchful waiting Consider watchful waiting when symptoms are mild and have been present for less than 4 weeks after the trauma. C Arrange a follow-up contact within 1 month. C Immediate psychological interventions for all Be aware of the psychological impact of traumatic events in the immediate post-incident care of survivors and offer practical, social and emotional support. GPP For individuals who have experienced a traumatic event, do not routinely offer brief, single-session interventions (debriefing) that focus on the traumatic incident to that individual alone. A Interventions where symptoms are present within 3 months of a trauma Offer trauma-focused CBT (usually on an individual outpatient basis) to people: with severe post-traumatic symptoms or with severe PTSD within 1 month after the event B who present with PTSD within 3 months of the event. A Consider offering 8 12 sessions of trauma-focused CBT (or fewer sessions about 5 if the treatment starts in the first month after the event). When the trauma is discussed, longer treatment sessions (90 minutes) are usually necessary. B Ensure that psychological treatment is regular and continuous (usually at least once a week) and is delivered by the same person. B Consider the following drug treatment for sleep disturbance: hypnotic medication for short-term use a suitable antidepressant for longer-term use, introduced at an early stage to reduce later risk of dependence. C Do not routinely offer non-trauma-focused interventions (such as relaxation or non-directive therapy) that do not address traumatic memories. B 12 NICE Guideline: quick reference guide Post-traumatic stress disorder
15 Interventions where symptoms have been present for more than 3 months after a trauma Offer trauma-focused psychological treatment (trauma-focused CBT or EMDR) to all patients, usually on an individual outpatient basis. A Consider offering 8 12 sessions of trauma-focused psychological treatment when the PTSD results from a single event. When the trauma is discussed, longer treatment sessions (90 minutes) are usually necessary. B Ensure that trauma-focused psychological treatment is: offered regardless of the time elapsed since the trauma B regular and continuous (usually at least once a week) B delivered by the same person. B Consider extending trauma-focused psychological treatment beyond 12 sessions and integrating it into an overall care plan if several problems need to be addressed, particularly: after multiple traumatic events after traumatic bereavement where chronic disability results from the trauma when significant comorbid disorders or social problems are present. C If the individual finds it difficult to disclose details of the trauma(s), consider devoting several sessions to establishing a trusting therapeutic relationship and emotional stabilisation before addressing the trauma. C Do not routinely offer non-trauma-focused interventions (such as relaxation or non-directive therapy) that do not address traumatic memories. B For PTSD sufferers with no or limited improvement after a specific traumafocused psychological treatment, consider: an alternative form of trauma-focused psychological treatment pharmacological treatment in addition to trauma-focused psychological treatment. C If PTSD sufferers request other forms of psychological treatment (e.g. supportive therapy, non-directive therapy, hypnotherapy, psychodynamic therapy or systemic psychotherapy), inform them that there is no convincing evidence for a clinically important effect. GPP Treatment of PTSD NICE Guideline: quick reference guide Post-traumatic stress disorder 13
16 Treatment of PTSD Drug treatments Do not offer drugs as routine first-line treatment for adult PTSD sufferers (for general use or by specialist mental health professionals) in preference to trauma-focused psychological therapy. A Consider paroxetine or mirtazapine (for general use) and amitriptyline or phenelzine (under specialist mental health care supervision) in adult PTSD sufferers 2 : if the individual prefers not to engage in a trauma-focused psychological treatment B if the individual cannot start psychological treatment because of serious threat of further trauma C if the individual has gained little or no benefit from a course of trauma-focused psychological treatment C as an adjunct to psychological treatment where there is significant comorbid depression or severe hyperarousal that significantly affects the individual s ability to benefit from psychological treatment. C For sleep disturbance, consider: hypnotic medication for short-term use a suitable antidepressant for longer-term use, introduced at an early stage to reduce later risk of dependence. C When an adult PTSD sufferer responds to drug treatment, continue the treatment for at least 12 months before gradual withdrawal. C When an adult PTSD sufferer does not respond to drug treatment, consider increasing the dose within approved limits. If further drug treatment is considered, it should generally be with a different class of antidepressant or involve the use of adjunctive olanzapine. C Starting drug treatments Inform all adult PTSD sufferers who are prescribed antidepressants of potential side effects and discontinuation/ withdrawal symptoms (particularly with paroxetine) at the time that treatment is initiated. C 2 Paroxetine is the only drug listed with a current UK product licence for PTSD at the date of publication (March 2005). 14 NICE Guideline: quick reference guide Post-traumatic stress disorder
17 See adult PTSD sufferers who are at increased risk of suicide, and all PTSD sufferers aged 18 29, after 1 week of starting antidepressants and frequently thereafter until the risk is not considered significant. GPP Seek out signs of akathisia, suicidal ideation and increased anxiety and agitation, particularly in the initial stages of SSRI treatment. Advise adult PTSD sufferers of the risk of these symptoms and to seek help promptly if these are distressing. GPP Review the use of the drug if the PTSD sufferer develops marked and/or prolonged akathisia. GPP See adult PTSD sufferers who are not considered to be at increased risk of suicide after 2 weeks of starting antidepressants and thereafter on an appropriate and regular basis (e.g. every 2 4 weeks in the first 3 months, and at greater intervals thereafter if response is good). GPP Treatment of PTSD Discontinuation/withdrawal symptoms Gradually reduce the dose of antidepressants over a 4-week period (some people may require longer periods). C If discontinuation/withdrawal symptoms are mild, reassure the PTSD sufferer and arrange for monitoring. C If symptoms are severe, consider re-introducing the original antidepressant (or another with a longer half-life from the same class) and reduce gradually while monitoring symptoms. C Chronic disease management Consider chronic disease management models for people with chronic PTSD who have not benefited from a number of courses of evidence-based treatment. C Children and young people Interventions in the first month after a trauma Offer trauma-focused CBT to older children with severe post-traumatic symptoms or with severe PTSD in the first month after the event. B NICE Guideline: quick reference guide Post-traumatic stress disorder 15
18 Treatment of PTSD Interventions more than 3 months after a trauma Offer children and young people a course of trauma-focused CBT adapted as needed to suit their age, circumstances and level of development. (This should also be offered to those who have experienced sexual abuse.) B For chronic PTSD in children and young people resulting from a single event, consider offering 8 12 sessions of trauma-focused psychological treatment. When the trauma is discussed, longer treatment sessions (90 minutes) are usually necessary. C Psychological treatment should be regular and continuous (usually at least once a week) and delivered by the same person. C Do not routinely prescribe drug treatments for children and young people with PTSD. C Involve families in the treatment of children and young people where appropriate, but remember that treatment consisting of parental involvement alone is unlikely to be of benefit for PTSD symptoms. C Inform parents (and where appropriate, children and young people) that apart from trauma-focused psychological interventions, there is no good evidence for the efficacy of other forms of treatment such as play therapy, art therapy or family therapy. C Disaster planning Disaster planning Ensure disaster plans contain provision for a fully coordinated psychosocial response. GPP Ensure that the psychosocial aspect of the plan contains: provision for immediate practical help means to support the role of the affected communities in caring for those involved in the disaster provision of specialist mental health, evidence-based assessment and treatment services. GPP Ensure that all healthcare workers involved in a disaster plan have clear roles and responsibilities agreed in advance. GPP 16 NICE Guideline: quick reference guide Post-traumatic stress disorder
19 Implementation Local health communities should review their existing practice in the treatment and management of PTSD. The review should consider the resources required to implement the recommendations set out in Section 1 of the NICE guideline, the people and processes involved and the timeline over which full implementation is envisaged. It is in the interests of PTSD sufferers that the implementation timeline is as rapid as possible. Implementation Relevant local clinical guidelines, care pathways and protocols should be reviewed in the light of this guidance and revised accordingly. This guideline should be used in conjunction with the National Service Framework for Mental Health, which is available from NICE Guideline: quick reference guide Post-traumatic stress disorder 17
20 Further information Distribution This quick reference guide to the Institute s guideline on post-traumatic stress disorder contains the key priorities for implementation, summaries of the guidance, and notes on implementation. The distribution list for this quick reference guide is available from NICE guideline The NICE guideline, Post-traumatic stress disorder (PTSD): the management of PTSD in adults and children in primary and secondary care, is available from the NICE website ( The NICE guideline contains the following sections: Key priorities for implementation; 1 Guidance; 2 Notes on the scope of the guidance; 3 Implementation in the NHS; 4 Research recommendations; 5 Other versions of this guideline; 6 Related NICE guidance; 7 Review date. It also gives details of the grading scheme for the evidence and recommendations, the Guideline Development Group and the Guideline Review Panel, and technical detail on the criteria for audit. Full guideline The full guideline includes the evidence on which the recommendations are based, in addition to the information in the NICE guideline. It is published by the National Collaborating Centre for Mental Health. It is available from and the website of the National Library for Health ( Information for the public NICE has produced a version of this guidance for people with PTSD, their advocates and carers, and the public. The information is available, in English and Welsh, from the NICE website ( Printed versions are also available see inside front cover for ordering information. Related guidance For information about NICE guidance that has been issued or is in development, see the website ( Anxiety: management of anxiety (panic disorder, with or without agoraphobia, and generalised anxiety disorder) in adults in primary, secondary and community care. NICE Clinical Guideline No. 22 (December 2004). Available from Depression: management of depression in primary and secondary care. NICE Clinical Guideline No. 23 (December 2004). Available from Self-harm: the short-term physical and psychological management and secondary prevention of self-harm in primary and secondary care. NICE Clinical Guideline No. 16 (July 2004). Available from Depression in children: identification and management of depression in children and young people in primary care and specialist services. NICE Clinical Guideline. (Publication expected August 2005.) Review date The process of reviewing the evidence is expected to begin 4 years after the date of issue of this guideline. Reviewing may begin before this if significant evidence that affects the guideline recommendations is identified. The updated guideline will be available within 2 years of the start of the review process. N0848 1P 80k March 2005 (ABA) National Institute for Clinical Excellence MidCity Place 71 High Holborn London WC1V 6NA
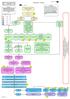
Post-traumatic stress disorder overview
 Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children
 Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Post-traumatic stress disorder (PTSD)
 Post-traumatic stress disorder (PTSD) The management of PTSD in adults and children in primary and secondary care Clinical Guideline 26 March 2005 Developed by the National Collaborating Centre for Mental
Post-traumatic stress disorder (PTSD) The management of PTSD in adults and children in primary and secondary care Clinical Guideline 26 March 2005 Developed by the National Collaborating Centre for Mental
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Rehabilitation after critical illness
 Quick reference guide Issue date: March 2009 Rehabilitation after critical illness NICE clinical guideline 83 Developed by the Centre for Clinical Practice at NICE Patient-centred care This is a quick
Quick reference guide Issue date: March 2009 Rehabilitation after critical illness NICE clinical guideline 83 Developed by the Centre for Clinical Practice at NICE Patient-centred care This is a quick
Depression in children and young people. Quick reference guide. Issue date: September 2005
 Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
Acute Stress Disorder and Posttraumatic Stress Disorder
 Acute Stress Disorder and Posttraumatic Stress Disorder Key Messages Traumatic Events Events that involve actual or threatened death or serious injury (real or perceived) to self or others (e.g., accidents,
Acute Stress Disorder and Posttraumatic Stress Disorder Key Messages Traumatic Events Events that involve actual or threatened death or serious injury (real or perceived) to self or others (e.g., accidents,
Common mental health disorders
 Issue date: May 2011 Common mental health disorders Identification and pathways to care NICE clinical guideline 123 Developed by the National Collaborating Centre for Mental Health NICE clinical guideline
Issue date: May 2011 Common mental health disorders Identification and pathways to care NICE clinical guideline 123 Developed by the National Collaborating Centre for Mental Health NICE clinical guideline
1. What is post-traumatic stress disorder (PTSD)?
 Post-traumatic stress disorder (PTSD) This factsheet has information about the symptoms and causes of posttraumatic stress disorder (PTSD). It says who might get PTSD and what treatment is available. You
Post-traumatic stress disorder (PTSD) This factsheet has information about the symptoms and causes of posttraumatic stress disorder (PTSD). It says who might get PTSD and what treatment is available. You
Borderline personality disorder
 Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Post-Traumatic Stress Disorder (PTSD)
 Post-Traumatic Stress Disorder (PTSD) Post traumatic stress disorder is a condition where you have recurring distressing memories, flashbacks, and other symptoms after suffering a traumatic event. Treatment
Post-Traumatic Stress Disorder (PTSD) Post traumatic stress disorder is a condition where you have recurring distressing memories, flashbacks, and other symptoms after suffering a traumatic event. Treatment
Depression in children and young people. Identification and management in primary, community and secondary care
 NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm
 E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
Sunderland Psychological Wellbeing Service
 Sunderland Psychological Wellbeing Service Information for Referrers Offering a range of psychological therapies across Sunderland. To make a referral call 0191 566 5454 A partnership between Northumberland,
Sunderland Psychological Wellbeing Service Information for Referrers Offering a range of psychological therapies across Sunderland. To make a referral call 0191 566 5454 A partnership between Northumberland,
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
FACT SHEET. What is Trauma? TRAUMA-INFORMED CARE FOR WORKING WITH HOMELESS VETERANS
 FACT SHEET TRAUMA-INFORMED CARE FOR WORKING WITH HOMELESS VETERANS According to SAMHSA 1, trauma-informed care includes having a basic understanding of how trauma affects the life of individuals seeking
FACT SHEET TRAUMA-INFORMED CARE FOR WORKING WITH HOMELESS VETERANS According to SAMHSA 1, trauma-informed care includes having a basic understanding of how trauma affects the life of individuals seeking
WHAT IS PTSD? A HANDOUT FROM THE NATIONAL CENTER FOR PTSD BY JESSICA HAMBLEN, PHD
 WHAT IS PTSD? A HANDOUT FROM THE NATIONAL CENTER FOR PTSD BY JESSICA HAMBLEN, PHD Posttraumatic Stress Disorder (PTSD) is an anxiety disorder that can occur following the experience or witnessing of a
WHAT IS PTSD? A HANDOUT FROM THE NATIONAL CENTER FOR PTSD BY JESSICA HAMBLEN, PHD Posttraumatic Stress Disorder (PTSD) is an anxiety disorder that can occur following the experience or witnessing of a
Understanding post-traumatic stress disorder. understanding. post-traumatic stress disorder
 Understanding post-traumatic stress disorder understanding post-traumatic stress disorder Understanding post-traumatic stress disorder This booklet is for anyone who experiences post-traumatic stress disorder
Understanding post-traumatic stress disorder understanding post-traumatic stress disorder Understanding post-traumatic stress disorder This booklet is for anyone who experiences post-traumatic stress disorder
Antisocial personality disorder
 Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Borderline personality disorder
 Issue date: January 2009 Borderline personality disorder Borderline personality disorder: treatment and management NICE clinical guideline 78 Developed by the National Collaborating Centre for Mental Health
Issue date: January 2009 Borderline personality disorder Borderline personality disorder: treatment and management NICE clinical guideline 78 Developed by the National Collaborating Centre for Mental Health
Acute Stress Disorder and Posttraumatic Stress Disorder
 AUSTRALIAN GUIDELINES FOR THE TREATMENT OF ADULTS WITH Acute Stress Disorder and Posttraumatic Stress Disorder Practitioner Guide Copies of the full set of the Guidelines, this guide and a booklet for
AUSTRALIAN GUIDELINES FOR THE TREATMENT OF ADULTS WITH Acute Stress Disorder and Posttraumatic Stress Disorder Practitioner Guide Copies of the full set of the Guidelines, this guide and a booklet for
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
Post-traumatic stress disorder. Understanding post-traumatic stress disorder
 Post-traumatic stress disorder Understanding post-traumatic stress disorder Understanding post-traumatic stress disorder Post-traumatic stress disorder (PTSD) may emerge months or sometimes years after
Post-traumatic stress disorder Understanding post-traumatic stress disorder Understanding post-traumatic stress disorder Post-traumatic stress disorder (PTSD) may emerge months or sometimes years after
Postpartum Depression and Post-Traumatic Stress Disorder
 Postpartum Depression and Post-Traumatic Stress Disorder Emotional Recovery: Postpartum Depression and Post-Traumatic Stress Disorder By: Lisa Houchins Published: July 23, 2013 Emotions vary widely after
Postpartum Depression and Post-Traumatic Stress Disorder Emotional Recovery: Postpartum Depression and Post-Traumatic Stress Disorder By: Lisa Houchins Published: July 23, 2013 Emotions vary widely after
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78
 Borderline personality disorder: recognition and management Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78 NICE 2009. All rights reserved. Your responsibility The recommendations
Borderline personality disorder: recognition and management Clinical guideline Published: 28 January 2009 nice.org.uk/guidance/cg78 NICE 2009. All rights reserved. Your responsibility The recommendations
Policy on Supporting Staff Involved in a Traumatic/Stressful. Incident, Complaint or Claim Associated with Employment
 Policy on Supporting Staff Involved in a Traumatic/Stressful Incident, Complaint or Claim Associated with Employment DOCUMENT CONTROL: Version: 3 Ratified by: Human Resources and Organisational Development
Policy on Supporting Staff Involved in a Traumatic/Stressful Incident, Complaint or Claim Associated with Employment DOCUMENT CONTROL: Version: 3 Ratified by: Human Resources and Organisational Development
North Pacific Epilepsy Research 2311 NW Northrup Street Suite #202 Portland, Oregon 97210 Tel: 503-291-5300 Fax: 503-291-5303
 North Pacific Epilepsy Research 2311 NW Northrup Street Suite #202 Portland, Oregon 97210 Tel: 503-291-5300 Fax: 503-291-5303 Post-Traumatic Stress Disorder (PTSD) Post-traumatic stress disorder (PTSD)
North Pacific Epilepsy Research 2311 NW Northrup Street Suite #202 Portland, Oregon 97210 Tel: 503-291-5300 Fax: 503-291-5303 Post-Traumatic Stress Disorder (PTSD) Post-traumatic stress disorder (PTSD)
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD
 Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31
 Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
Borderline personality disorder
 Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí
 mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí Plan of the presentation Summary of NICE recommended psychological
mpv`elildf`^i=qob^qjbkqp=ñçê= ^åñáéíó=~åç=aééêéëëáçå h~íó=dê~òéäêççâ `äáåáå~ä=ié~çi=dêééåïáåü=qáãé=qç=q~äâ `çåëìäí~åí=`äáåáå~ä=mëóåüçäçöáëí Plan of the presentation Summary of NICE recommended psychological
TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines
 TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines DATE: 01 December 2009 CONTEXT AND POLICY ISSUES: Post-traumatic stress disorder
TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines DATE: 01 December 2009 CONTEXT AND POLICY ISSUES: Post-traumatic stress disorder
Mental Health Needs Assessment Personality Disorder Prevalence and models of care
 Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Policy for Preventing and Managing Critical Incident Stress
 Policy for Preventing and Managing Critical Incident Stress Document reference number HSAG 2012/3 Document developed by Revision number 1.0 Document approved by Consultation with 14 September 2012 Presented
Policy for Preventing and Managing Critical Incident Stress Document reference number HSAG 2012/3 Document developed by Revision number 1.0 Document approved by Consultation with 14 September 2012 Presented
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
Traumatic Stress. and Substance Use Problems
 Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
Psychiatric Issues and Defense Base Act Claims. Dr. Michael Hilton
 Psychiatric Issues and Defense Base Act Claims Dr. Michael Hilton Criteria for DSM-IVRPosttraumatic Stress Disorder with changes now in effect with DSM5 a. The person has been exposed to a traumatic event
Psychiatric Issues and Defense Base Act Claims Dr. Michael Hilton Criteria for DSM-IVRPosttraumatic Stress Disorder with changes now in effect with DSM5 a. The person has been exposed to a traumatic event
Low back pain. Quick reference guide. Issue date: May 2009. Early management of persistent non-specific low back pain
 Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
When is psychological therapy warranted for patients with mental health problems?
 The Guidelines Advisory Committee (GAC) is empowered by the Ministry of Health and Long-Term Care and the Ontario Medical Association to promote evidence-based health care in Ontario, by encouraging physicians
The Guidelines Advisory Committee (GAC) is empowered by the Ministry of Health and Long-Term Care and the Ontario Medical Association to promote evidence-based health care in Ontario, by encouraging physicians
Depression. The treatment and management of depression in adults. This is a partial update of NICE clinical guideline 23
 Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Treatments for drug misuse
 Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Executive summary. Request for advice
 Executive summary Request for advice Child abuse has always been with us and it takes many different forms. It is estimated that more than 100,000 children are abused in the Netherlands each year. In recent
Executive summary Request for advice Child abuse has always been with us and it takes many different forms. It is estimated that more than 100,000 children are abused in the Netherlands each year. In recent
Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder
 Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder December 2009 Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the
Anxiety Care Pathway Panic Disorder and Generalised Anxiety Disorder December 2009 Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the
Supporting Children s Mental Health Needs in the Aftermath of a Disaster: Pediatric Pearls
 Supporting Children s Mental Health Needs in the Aftermath of a Disaster: Pediatric Pearls Satellite Conference and Live Webcast Thursday, August 25, 2011 5:30 7:00 p.m. Central Time Faculty David J. Schonfeld,
Supporting Children s Mental Health Needs in the Aftermath of a Disaster: Pediatric Pearls Satellite Conference and Live Webcast Thursday, August 25, 2011 5:30 7:00 p.m. Central Time Faculty David J. Schonfeld,
and body dysmorphic disorder (BDD) in adults, children and young people Issue date: November 2005
 Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Supporting children in the aftermath of a crisis
 Supporting children in the aftermath of a crisis David J. Schonfeld, MD Thelma and Jack Rubinstein Professor of Pediatrics Director, National Center for School Crisis and Bereavement Division of Developmental
Supporting children in the aftermath of a crisis David J. Schonfeld, MD Thelma and Jack Rubinstein Professor of Pediatrics Director, National Center for School Crisis and Bereavement Division of Developmental
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Understanding PTSD and the PDS Assessment
 ProFiles PUTTING ASSESSMENTS TO WORK PDS TEST Understanding PTSD and the PDS Assessment Recurring nightmares. Angry outbursts. Easily startled. These are among the many symptoms associated with Post Traumatic
ProFiles PUTTING ASSESSMENTS TO WORK PDS TEST Understanding PTSD and the PDS Assessment Recurring nightmares. Angry outbursts. Easily startled. These are among the many symptoms associated with Post Traumatic
Psychotherapeutic Interventions for Children Suffering from PTSD: Recommendations for School Psychologists
 Psychotherapeutic Interventions for Children Suffering from PTSD: Recommendations for School Psychologists Julie Davis, Laura Lux, Ellie Martinez, & Annie Riffey California Sate University Sacramento Presentation
Psychotherapeutic Interventions for Children Suffering from PTSD: Recommendations for School Psychologists Julie Davis, Laura Lux, Ellie Martinez, & Annie Riffey California Sate University Sacramento Presentation
CHAPTER 6 Diagnosing and Identifying the Need for Trauma Treatment
 CHAPTER 6 Diagnosing and Identifying the Need for Trauma Treatment This chapter offers mental health professionals: information on diagnosing and identifying the need for trauma treatment guidance in determining
CHAPTER 6 Diagnosing and Identifying the Need for Trauma Treatment This chapter offers mental health professionals: information on diagnosing and identifying the need for trauma treatment guidance in determining
Depression Assessment & Treatment
 Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
USVH Disease of the Week #1: Posttraumatic Stress Disorder (PTSD)
 USVH Disease of the Week #1: Posttraumatic Stress Disorder (PTSD) Effects of Traumatic Experiences A National Center for PTSD Fact Sheet By: Eve B. Carlson, Ph.D. and Josef Ruzek, Ph.D. When people find
USVH Disease of the Week #1: Posttraumatic Stress Disorder (PTSD) Effects of Traumatic Experiences A National Center for PTSD Fact Sheet By: Eve B. Carlson, Ph.D. and Josef Ruzek, Ph.D. When people find
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Overcoming the Trauma of Your Motor Vehicle Accident
 Overcoming the Trauma of Your Motor Vehicle Accident Chapter 1 Introductory Information for Therapists Case Study: Mary The day had begun like any other. Mary was on her way to work early in the morning.
Overcoming the Trauma of Your Motor Vehicle Accident Chapter 1 Introductory Information for Therapists Case Study: Mary The day had begun like any other. Mary was on her way to work early in the morning.
Diagnosis and management of ADHD in children, young people and adults
 Issue date: September 2008 Attention deficit hyperactivity disorder Diagnosis and management of ADHD in children, young people and adults NICE clinical guideline 72 Developed by the National Collaborating
Issue date: September 2008 Attention deficit hyperactivity disorder Diagnosis and management of ADHD in children, young people and adults NICE clinical guideline 72 Developed by the National Collaborating
Costing statement: Depression: the treatment and management of depression in adults. (update) and
 Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Cognitive Behavioral Therapy for PTSD. Dr. Edna B. Foa
 Cognitive Behavioral Therapy for PTSD Presented by Dr. Edna B. Foa Center for the Treatment and Study of Anxiety University of Pennsylvania Ref # 3 Diagnosis of PTSD Definition of a Trauma The person has
Cognitive Behavioral Therapy for PTSD Presented by Dr. Edna B. Foa Center for the Treatment and Study of Anxiety University of Pennsylvania Ref # 3 Diagnosis of PTSD Definition of a Trauma The person has
National Defence. Défense nationale A-MD-007-144/JD-004. Preparing for CRITICAL incident. Stress
 National Defence Défense nationale A-MD-007-144/JD-004 Preparing for CRITICAL incident Stress Foreword This publication is presented as a resource for the Department of National Defence (DND) community,
National Defence Défense nationale A-MD-007-144/JD-004 Preparing for CRITICAL incident Stress Foreword This publication is presented as a resource for the Department of National Defence (DND) community,
Care Programme Approach (CPA)
 Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90
 Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Coping with trauma and loss
 Coping with trauma and loss Coping with trauma and loss Someone close to you may have died in sudden and/or traumatic circumstances. You may have witnessed the death, or the deaths and injury of others.
Coping with trauma and loss Coping with trauma and loss Someone close to you may have died in sudden and/or traumatic circumstances. You may have witnessed the death, or the deaths and injury of others.
Post Traumatic Stress Disorder & Substance Misuse
 Post Traumatic Stress Disorder & Substance Misuse Produced and Presented by Dr Derek Lee Consultant Chartered Clinical Psychologist Famous Sufferers. Samuel Pepys following the Great Fire of London:..much
Post Traumatic Stress Disorder & Substance Misuse Produced and Presented by Dr Derek Lee Consultant Chartered Clinical Psychologist Famous Sufferers. Samuel Pepys following the Great Fire of London:..much
Costing report. Drug misuse: psychosocial interventions and opioid detoxification. Implementing NICE guidance. July 2007
 Drug misuse: psychosocial interventions and opioid detoxification Costing report Implementing NICE guidance July 2007 NICE clinical guidelines 51 and 52 National costing report: Drug misuse guidelines
Drug misuse: psychosocial interventions and opioid detoxification Costing report Implementing NICE guidance July 2007 NICE clinical guidelines 51 and 52 National costing report: Drug misuse guidelines
Original Article: http://www.mayoclinic.com/health/post-traumatic-stress-disorder
 1 of 11 6/29/2012 12:17 PM MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution,
1 of 11 6/29/2012 12:17 PM MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution,
Trauma FAQs. Content. 1. What is trauma? 2. What events are traumatic?
 Trauma FAQs Content 1. What is trauma? 2. What events are traumatic? 3. Who experiences trauma? 4. What are symptoms of trauma? 5. How can I help someone who may be experiencing trauma? 6. Where can people
Trauma FAQs Content 1. What is trauma? 2. What events are traumatic? 3. Who experiences trauma? 4. What are symptoms of trauma? 5. How can I help someone who may be experiencing trauma? 6. Where can people
Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults
 Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults Introduction The partial update of the guideline on Generalised anxiety disorder and panic disorder
Costing statement: Generalised anxiety disorder and panic disorder (with or without agoraphobia) in adults Introduction The partial update of the guideline on Generalised anxiety disorder and panic disorder
EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY
 Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
4/25/2015. Traumatized People, Service Delivery Systems, and Learning from 9/11 (NYC)
 Traumatized People, Service Delivery Systems, and Learning from 9/11 (NYC) Ryan Edlind MS, MSW, LISW-S April 29, 2015 Traumatized People, Service Delivery Systems, and Learning from 9/11 (NYC) Ryan Edlind
Traumatized People, Service Delivery Systems, and Learning from 9/11 (NYC) Ryan Edlind MS, MSW, LISW-S April 29, 2015 Traumatized People, Service Delivery Systems, and Learning from 9/11 (NYC) Ryan Edlind
Uncertainty: Was difficulty falling asleep and hypervigilance related to fear of ventricular tachycardia returning, or fear of being shocked again?
 Manuel Tancer, MD Chart Review: PTSD PATIENT INFO 55 Age: Background: Overweight nurse with 6-month history of nightmares, hyperarousal, and flashbacks; symptoms began after implanted defibrillator was
Manuel Tancer, MD Chart Review: PTSD PATIENT INFO 55 Age: Background: Overweight nurse with 6-month history of nightmares, hyperarousal, and flashbacks; symptoms began after implanted defibrillator was
What is Narrative Exposure Therapy (NET)?
 What is Narrative Exposure Therapy (NET)? Overview NET is a culturally universal short-term intervention used for the reduction of traumatic stress symptoms in survivors of organised violence, torture,
What is Narrative Exposure Therapy (NET)? Overview NET is a culturally universal short-term intervention used for the reduction of traumatic stress symptoms in survivors of organised violence, torture,
Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal
 Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal February 2010 NICE clinical guidelines 100 and 115 1 These sample chlordiazepoxide dosing regimens
Alcohol use disorders: sample chlordiazepoxide dosing regimens for use in managing alcohol withdrawal February 2010 NICE clinical guidelines 100 and 115 1 These sample chlordiazepoxide dosing regimens
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression
 Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
A Carer s Guide to Depression in People with a Learning Disability
 A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
Treatment of Rape-related PTSD in the Netherlands: Short intensive cognitivebehavioral
 Treatment of Rape-related PTSD in the Netherlands: Short intensive cognitivebehavioral programs Agnes van Minnen October 2009 University of Nijmegen Clinic of Anxiety Disorders Acknowledgements: We kindly
Treatment of Rape-related PTSD in the Netherlands: Short intensive cognitivebehavioral programs Agnes van Minnen October 2009 University of Nijmegen Clinic of Anxiety Disorders Acknowledgements: We kindly
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Rehabilitation during the patient s critical care stay bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online.
Rehabilitation during the patient s critical care stay bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online.
Care Programme Approach (CPA)
 Care Programme Approach (CPA) The Care Programme Approach (CPA) is the system that is used to organise many people s care from 'secondary mental health services'. This factsheet explains what you should
Care Programme Approach (CPA) The Care Programme Approach (CPA) is the system that is used to organise many people s care from 'secondary mental health services'. This factsheet explains what you should
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Child Welfare Trauma Referral Tool
 Module 4, Activity 4F; Module 4, Activity 4G Child Welfare Trauma Referral Tool This measure is designed to help child welfare workers make more trauma-informed decisions about the need for referral to
Module 4, Activity 4F; Module 4, Activity 4G Child Welfare Trauma Referral Tool This measure is designed to help child welfare workers make more trauma-informed decisions about the need for referral to
Your guide to. anxiety treatment. after a motor vehicle accident
 Your guide to anxiety treatment after a motor vehicle accident November 2003 ISBN 1 876958 16 2 Published by the Motor Accidents Authority of NSW Level 22, 580 George Street, Sydney 2000 Phone: 1300 137
Your guide to anxiety treatment after a motor vehicle accident November 2003 ISBN 1 876958 16 2 Published by the Motor Accidents Authority of NSW Level 22, 580 George Street, Sydney 2000 Phone: 1300 137
Treatment of PTSD in Children
 Treatment of PTSD in Children Why Treat PTSD in Kids? Distress & Disabling Impairs Functioning Development Affected Co- morbid Problems Chronicity Limited research on Child PTSD Treatment Combined approach
Treatment of PTSD in Children Why Treat PTSD in Kids? Distress & Disabling Impairs Functioning Development Affected Co- morbid Problems Chronicity Limited research on Child PTSD Treatment Combined approach
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Depression in Adults
 Depression in Adults A chapter of Croydon s mental health Joint Strategic Needs Assessment 2012/13 Health and Wellbeing Board 5 December 2012 Bernadette Alves, Locum Consultant in Public Health Croydon
Depression in Adults A chapter of Croydon s mental health Joint Strategic Needs Assessment 2012/13 Health and Wellbeing Board 5 December 2012 Bernadette Alves, Locum Consultant in Public Health Croydon
How Emotional/ Psychological Trauma Affects the Body
 How Emotional/ Psychological Trauma Affects the Body Objectives: Define trauma What is the relationship between physical health and PTSD? Identify how trauma is assessed/screened How can family members
How Emotional/ Psychological Trauma Affects the Body Objectives: Define trauma What is the relationship between physical health and PTSD? Identify how trauma is assessed/screened How can family members
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011
 SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
SOMERSET DUAL DIAGNOSIS PROTOCOL OCTOBER 2011 This document is intended to be used with the Somerset Dual Diagnosis Operational Working guide. This document provides principles governing joint working
Suzanne R. Merlis, Psy. D. Georgia-LLC Licensed Psychologist
 Suzanne R. Merlis, Psy. D. Georgia-LLC Licensed Psychologist If going to asylum officer at affirmative stage: ASYLUM OFFICER, ARLINGTON ASYLUM OFFICE In the Matter of Mr. X Respondent If referred to judge:
Suzanne R. Merlis, Psy. D. Georgia-LLC Licensed Psychologist If going to asylum officer at affirmative stage: ASYLUM OFFICER, ARLINGTON ASYLUM OFFICE In the Matter of Mr. X Respondent If referred to judge:
Expert Witness Services for Personal Injury Lawyers
 Advanced Assessments Ltd Expert witnesses and Psychologists A Member of the Strategic Enterprise Group 180 Piccadilly, London, W1J 9HP T: 0845 130 5717 Expert Witness Services for Personal Injury Lawyers
Advanced Assessments Ltd Expert witnesses and Psychologists A Member of the Strategic Enterprise Group 180 Piccadilly, London, W1J 9HP T: 0845 130 5717 Expert Witness Services for Personal Injury Lawyers
SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES
 SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES Psychological therapies are increasingly viewed as an important part of both mental and physical healthcare, and there is a growing demand for
SPECIALIST ARTICLE A BRIEF GUIDE TO PSYCHOLOGICAL THERAPIES Psychological therapies are increasingly viewed as an important part of both mental and physical healthcare, and there is a growing demand for
The Priory Group. What is obsessive-compulsive disorder?
 The Priory Group What is obsessive-compulsive disorder? by Dr David Veale Dr Veale is a Consultant Psychiatrist at the Priory Hospital North London and the coauthor of Overcoming Obsessive Compulsive Disorder
The Priory Group What is obsessive-compulsive disorder? by Dr David Veale Dr Veale is a Consultant Psychiatrist at the Priory Hospital North London and the coauthor of Overcoming Obsessive Compulsive Disorder
Manual for the Administration and Scoring of the PTSD Symptom Scale Interview for DSM-5 (PSS-I-5) Past Month Version. Edna B. Foa and Sandy Capaldi
 Manual for the Administration and Scoring of the PTSD Symptom Scale Interview for DSM-5 (PSS-I-5) Past Month Version Edna B. Foa and Sandy Capaldi 1 Introduction The PTSD Symptom Scale Interview for DSM-5
Manual for the Administration and Scoring of the PTSD Symptom Scale Interview for DSM-5 (PSS-I-5) Past Month Version Edna B. Foa and Sandy Capaldi 1 Introduction The PTSD Symptom Scale Interview for DSM-5
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Drug treatments for neuropathic pain
 Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Post Traumatic Stress Disorder and Substance Abuse. Impacts ALL LEVELS of Leadership
 Post Traumatic Stress Disorder and Substance Abuse Impacts ALL LEVELS of Leadership What IS Post Traumatic Stress Disorder (PTSD) PTSD is an illness which sometimes occurs after a traumatic event such
Post Traumatic Stress Disorder and Substance Abuse Impacts ALL LEVELS of Leadership What IS Post Traumatic Stress Disorder (PTSD) PTSD is an illness which sometimes occurs after a traumatic event such
