T lymphocyte engineering ex vivo for cancer and infectious disease
|
|
|
- Gwendoline McDaniel
- 7 years ago
- Views:
Transcription
1 Review General T lymphocyte engineering ex vivo for cancer and infectious disease 1. Introduction 2. T lymphocyte subsets 3. Ex vivo culture methods for T-cell therapy 4. Clinical-scale culture of co-stimulated T lymphocytes for cell therapy 5. Clinical trials of co-stimulated T lymphocytes 6. Expert opinion Bruce L Levine The University of Pennsylvania School of Medicine, Hospital of the University of Pennsylvania, Department of Pathology and Laboratory Medicine, Philadelphia, PA , USA Background : Basic research contributions towards the molecular and cellular understanding of immune mediated control of cancer and infectious diseases have created opportunities to develop new forms of T-cell-based vaccination for cancer and chronic infections like HIV. In the past two decades, there has been a dramatic increase in the number of cell therapy clinical trials around the world aimed at enhancing antitumor immunity, restoring immune function to infectious diseases and augmenting vaccine efficacy. Objective : To provide a review of new and emerging methods of T lymphocyte engineering, gene transfer to T cells and clinical trials. Methods : A review of recent clinical trials, along with a brief historical perspective, with a focus on challenges and recent advances in the field and requirements for successful T-cell therapies. Conclusion : Advances in the technological approaches and methods for ex vivo manipulation have led to T lymphocytes endowed with enhanced potency and unique functions, with promise as the new generation of infused therapeutics. Keywords: adoptive immunotherapy, clinical trials, gene therapy, T lymphocytes, vaccines Expert Opin. Biol. Ther. (2008) 8(4): Introduction Cell therapy laboratories have developed from their roots in blood banking and blood and bone marrow transplantation into what can now be described as cellular engineering laboratories, where cells can be isolated, enriched, transduced, activated, expanded and manipulated in ways that change or enhance their function, prior to reinfusion. Together with evidence for the role of the immune response in controlling cancer and infectious disease, technological advances have facilitated a paradigm shift from the use of cells and tissues only for homologous function to the engineering of cells for non-homologous or improved function. An ideal cell therapy would have the following properties: i) demonstrated potency against tumor or infectious organism; ii) efficient engraftment, enabling a high effector to target ratio; iii) long-term persistence and memory; and iv) being easily obtained and efficiently manufactured. Adoptive T-cell therapies that would meet the above criteria depend on the ability to optimally select, genetically engineer or induce cells with targeted antigen specificity while preserving their effector function and engraftment and homing abilities. 2. T lymphocyte subsets 2.1 Activation, differentiation and memory Naive CD4 + and CD8 + T cells undergo unique developmental programs after antigen activation, resulting in the generation of effector memory and long-lived central memory T cells, TEM cells and TCM cells, respectively. Naive T cells, because of their higher threshold for activation and their inability to react to most / Informa UK Ltd ISSN
2 T lymphocyte engineering ex vivo for cancer and infectious disease tumors and pathogens in rapid fashion, are not thought to be useful for adoptive transfer unless first primed in vivo and/or activated and expanded in vitro. Models for the development and maintenance of T-cell memory include those based on linear differentiation [1], signal strength [2], and memory stem cells [3]. Some studies indicate that naive T cells first differentiate into effector T cells, a proportion of which then differentiate into TCM cells [4]. Other studies suggest that parallel differentiation occurs, with naive T cells directly differentiating into TCM and effector cells simultaneously through asymmetric division [5]. The recent demonstration of asymmetric division of T lymphocytes following antigenic stimulus [6] lends further credence to the parallel differentiation model. However, it may still be true that some TCM are derived from TEM that do not undergo apoptosis when antigen is no longer abundant. Understanding the mechanism of TEM and TCM generation is important so that culture systems can be devised to optimally derive populations of TEM and TCM cells. TCM cells retain the capacity for marked clonal expansion [7]. It has also been shown that naive T cells have a longer chromosomal telomere length compared with memory T cells and that telomere length correlates with lymphocyte replicative history and residual replicative potential [8]. With regard to memory T cells, the demonstration that TCM and TEM cell subsets have discrete trafficking and functional properties [9] has important implications for adoptive T-cell therapy. For example, CCR7 and CD62L, both important for homing to lymph nodes, are not expressed or are expressed at lower levels in TEM cells. In retrospect, previous clinical trials have primarily tested adoptively transferred populations of CD8 + TEM cells [10]. This was due to the available tissue culture technologies at the time, which resulted in rapid differentiation of T cells to late-stage effector cells which are CD28-negative, express CD57 and have poor replicative capacity [11,12]. In vitro, TEM cells are superior to TCM cells at tumor cytotoxicity. However, in vivo, TCM cells exhibit superior therapeutic effects when compared with TEM cells on a per cell basis [10,13]. Therefore, in principle, adoptive T-cell transfer strategies to generate long-lived populations of TCM cells capable of immune surveillance as well as tumor eradication would be an attractive approach. 2.2 CD8 + and CD4 + T lymphocytes for adoptive transfer Many studies show that the generation and/or maintenance of CD8 + T-cell memory requires CD4 + T-cell help [14,15] and that immunity specific for tumors lacking expression of MHC class II molecules is enhanced with CD4 + T-cell help [16]. It may be counterintuitive that CD4 + T cells enhance antitumor effects in hosts bearing tumors that lack MHC class II. However, adoptively transferred CD4 + T cells have the potential to augment tumor immunity by several mechanisms that might enhance the survival and function of CD8 + T cells, including the secretion of cytokines and the expression of CD40L [17]. Besides their intimate involvement in priming tumor-specific cytotoxic T lymphocytes (CTLs), CD4 + cells participate in additional effector functions. Clinical adoptive transfer studies also show that the persistence of adoptively transferred cytotoxic CD8 + effector T cells is enhanced with the concomitant administration of IL-2 [18] or CD4 + T cells [19]. Recent studies in patients with myeloma show that the adoptive transfer of mixed populations of pathogen-specific CD4 + and CD8 + T cells promoted the establishment of immunity with a robust central memory component [20]. However, it is not yet known if this approach enhances the establishment of immunity to self antigens in cancer patients. At present, one of the most important issues facing the field is the complexity of CD4 + -lineage T cells. Until recently, CD4 + T helper (T H ) cells were separated into two different subsets named T H 1 and T H 2 cells, based on the pattern of cytokines that they produce when stimulated. Additionally, several types of CD4 + regulatory/suppressor T cells (Tregs) have now been described in humans [21], and it is probably important to remove Tregs from adoptively transferred T-cell populations because they suppress antitumor immunity [22]. Tregs are CD25 + CD127 - [23] and could be removed by flow cytometry sorting, though at present the technical hurdles, as described in section 3.1 below, for tetramer sorting would need to be overcome. An alternative approach that has been tested in a clinical trial is to remove Tregs from an apheresis product via anti-cd25 antibody conjugated to magnetic beads [24]. Since Tregs are often enriched in tumor-infiltrating lymphocytes and the peripheral blood in cancer patients [25], it is possible that the outcomes of previous adoptive T cell therapy clinical trials were compromised because the adoptively transferred T-cell populations inadvertently contained Tregs. 3. Ex vivo culture methods for T-cell therapy 3.1 Source of T cells and initial processing The only forms of adoptive cellular therapy routinely employed in the practice of medicine are allogeneic bone marrow and peripheral blood stem cell transplantation. In this setting, donor leukocyte infusions mediate various potent antitumor effects [26]. The adoptive transfer of activated donor (allogeneic) T cells shows promise of augmenting this effect [27,28]. Ex vivo culture approaches to altering the ratio of effector T cells to Tregs have the potential of decreasing the risk of graft-versus-host disease (GVHD) while preserving antitumor effects [29]. Engineered adoptive T-cell therapy approaches to date have used peripheral blood, tumors, malignant effusions and draining lymph nodes as the anatomical sources of input T cells for adoptive transfer [30-33]. Given that the bone marrow from patients with breast cancer, pancreatic cancer and myeloma has recently been shown to be enriched in tumor-reactive 476 Expert Opin. Biol. Ther. (2008) 8(4)
3 Levine Starting T cell repertoire Polyclonal stimulation Time Time TILs or PBMCs Antigen-specific stimulation 7 10 d Antigen and APC Ctclic stimulation with CD3-and CD28-specific antibodies Antigen and APC 6w Functional development Treg cell depletion Genetic modification T cell selection and/or expansion in the host Figure 1. Polyclonal and antigen-specific T-cell propagation. Left: Antigen-specific T-cell culture, particularly without prior selection or enrichment, requires several rounds of stimulation with antigen-pulsed antigen presenting cells or feeder cells. Right: Polyclonal stimulation via CD3/CD28 stimulation maintains the T-cell receptor repertoire of the starting population. PBMC: Peripheral blood mononuclear cell; TILs: Tumour-infiltrating lymphocyte; Treg: Regulatory T cell. CD8+ T cells [34-37], it is important to determine whether improved antitumor effects are observed when bone marrow resident T cells are used for adoptive transfer. Preclinical data demonstrating that activated marrowinfiltrating lymphocytes show enhanced tumor-specific activity compared with peripheral blood lymphocytes has led to a clinical trial testing this approach [37]. With leukapheresis, mononuclear cells or more may be obtained as starting material with small modifications of established protocols [38,39]. With the other sources of T cells, such as bone marrow and tumors, the number of cells obtained as starting material is usually much less and may vary widely among patients and with disease status, which indicates the critical importance of validation studies prior to the initiation of clinical trials. Two basic approaches are being tested for clinical adoptive T-cell therapy (Figure 1). The first approach is to isolate and activate antigen-specific T cells from peripheral blood, bone marrow, or tumor specimens in vitro and then to use repetitive stimulation to clonally expand the antigenspecific T cells in vitro by various approaches. In the second approach, polyclonal ex vivo activation of the T cells is performed based on three assumptions: first, that antigenspecific T cells are present in the patient; second, that antigen-specific T cells are primed in the patient; and third, that the in vivo function of the antigen-specific T cells in the patient is impaired. In this second approach, the cells are activated in vitro by various means that preserve the polyclonal repertoire and are then reinfused into the patient with the expectation that they will respond directly to antigens presented by antigen-presenting cells (APCs) or on virally infected cells. The first approach guarantees antigen specificity but is costly in materials, labor and time needed for the expansion. The second approach is technically more rapid, feasible and in general less expensive. In practical terms, the second approach has been efficient and robust enough to support randomized clinical trials [20], and therefore, only this approach has the potential for regulatory approval. The rationale for the second approach has been substantially strengthened by the realization that many patients are already primed to their tumors [40,41]. A combination approach, whereby patients are first vaccinated and then primed T cells are collected for polyclonal expansion may also be taken [20,42,43]. As vaccination approaches with defined tumor or infectious disease antigens may cover only a proportion of patients or may induce a narrow range of antigenic T-cell specificities, vaccination with a broad range of antigens, antigen matched to the patient or tumor lysate, may generate more antigen-specific T cells that could be expanded in vitro for adoptive transfer. In a research setting, MHC tetramers may be used to sort for antigen-specific T cells by flow cytometry. This approach faces several hurdles prior to testing in clinical trials. First, clinical grade tetramers must be generated and tested at Expert Opin. Biol. Ther. (2008) 8(4) 477
4 T lymphocyte engineering ex vivo for cancer and infectious disease significant cost. HLA-A2 tetramers would cover less than 50% of most patient populations; thus additional tetramers would need to be manufactured to cover many more patients. Each tetramer would isolate T cells specific for only one peptide and would thus complicate generation of a multimeric cellular therapy. Additionally, current flow cytometry sorter rates are such that sort times of several hours are usually required to isolate enough antigen-specific T cells sufficient for clinical scale expansion. Clinical flow sorters pose challenges for sterility of the sorted cells and containment due to the generation of aerosols, although new designs and technological advances may address these concerns. An alternate approach for the isolation of antigenspecific T cells that has been evaluated in clinical trials is the magnetic capture of IFN- γ secreting cells [44]. Polyclonal cells isolated from peripheral blood, bone marrow or tumors are first stimulated with antigen in vitro. T cells secreting interferon- γ are then isolated with clinical-grade commercially available antibody-conjugated magnetic particles. The advantages of this method are that the antigen need not be defined or limited to a particular peptide or protein and that T cells of multiple antigenic specificities can be generated and isolated. With either of the above positive selection approaches, Tregs could be effectively removed. For donor lymphocyte infusions, alloreactive cells may be depleted in vitro using the cytokine capture system and host cells as stimulators, and thus reducing the risk of GVHD. 3.2 Presenting antigen to T cells ex vivo The most appropriate methods of ex vivo T-cell culture mimic the physiological processes whereby dendritic cells (DCs) generate a constellation of antigen-specific and costimulatory signals in the T cells. However, although useful for therapeutic vaccination, due to practical considerations such as substantial manufacturing costs and the logistics of maintaining independent culture systems for each type of cell, DCs are not useful as APCs for large-scale adoptive T-cell therapy trials. In addition, for ex vivo expansion of autologous T cells, it is desirable to have APCs with extensive replicative potential to facilitate both the scaling up of the process and multiple rounds of T-cell stimulation. The rapid expansion method developed by Riddell and co-workers uses irradiated allogeneic peripheral blood mononuclear cells as APCs (also known as feeder cells) to expand CTLs for adoptive transfer [18]. The main limitation of this approach is in clinical scale-up, because conforming to FDA-mandated requirements for the validation and qualification of allogeneic feeder cells can be tedious and expensive. Schultze and co-workers have shown that CD40-stimulated B cells, which have an extensive replicative potential, are an efficient means of propagating antigen-specific T cells [45]. Therefore, although currently available tissue culture approaches have provided proof of concept for adoptive T-cell therapy, a current priority is to develop alternative approaches, such as artificial antigen-presenting cells, that can support the randomized large-scale trials required for FDA approval. 3.3 Cytotoxic T lymphocyte therapy At present, there is a plethora of suitable CTL targets for many tumors and viruses. In melanoma, CTLs derived from peripheral blood lymphocytes were used to treat patients with refractory, metastatic melanoma, and 8 out of 20 patients had minor, mixed or stable antitumor immune responses [18]. Furthermore, the infusion of autologous Melanoma-associated Antigen Recognized by T cells-1 (MART-1)-specific CD8 + T cells into a patient with metastatic melanoma resulted in T-cell infiltration into both the skin and tumor tissue [46]. These results were confirmed in a recent study in which engraftment of the CTLs, as measured by an elevated frequency of circulating T cells able to bind tetramers loaded with MART-1 peptides, was detectable up to 2 weeks after T-cell transfer in all patients, with a maximal frequency of 2% of the total CD8 + T cells [47]. Despite this high level of engraftment in all patients, only 3 out of 11 patients had clinical antitumor responses, and a selective loss of MART-1 expression was observed. Therefore, perhaps the most worrisome issue revealed with CTL transfers is the emergence of antigen escape variants. It is possible that this problem can be addressed by cell isolation and culture methods that facilitate a broad tumor-antigen-specific T-cell repertoire. Immunotherapy of human viral infection using adoptively transferred antigen-specific T cells has been studied in the setting of cytomegalovirus (CMV), Epstein Barr virus (EBV) and HIV infection. Riddell et al. have explored this strategy using T-cell clones with HLA restricted antigenic specificity for CMV [48,49]. Recovery of CMV-specific CTL activity was observed and adoptively transferred CTL persisted in vivo for up to 12 weeks. In a similar study, Brenner, Heslop and coworkers administered donor-derived EBVspecific CD8 + and CD4 + T cells, genetically marked with the neomycin resistance gene, to six recipients of T-celldepleted allogeneic bone marrow allografts that persisted for as long as 18 months [50,51]. Autologous EBV-specific T cells can also be generated [52-54], however, culture of a sufficient number of EBV-specific cells may require months, and this amount of time may not be practical and may result in a population of cells that is near replicative senescence. While the generation of EBV-specific cell lines could be attempted for each patient with the goal of infusing the cells if posttransplant lymphoproliferative disorder (PTLD) develops, if the incidence of PTLD is < 10% this would require a substantial investment in time and resources for each treated patient. A novel combination strategy to generate CTL specific for multiple viruses was reported recently [55]. In this study, a chimeric adenovirus-cmv vector was used to modify EBV-expressing B cells lines to serve as APC. Multi-virus-specific T cells were then generated and infused into 11 patients where they could be detected in vivo. In the 478 Expert Opin. Biol. Ther. (2008) 8(4)
5 Levine setting of HIV, the infusion of HIV-specific CTL s has been less encouraging. While infused HIV-specific CTL have been shown to be present in peripheral blood and to traffic to lymph nodes following infusion, persistence was limited to only days or weeks [56,57], and no significant clinical benefit was noted. This may have been due to the severe defects in the CD4 helper response resulting from HIV infection. 3.4 Tumor-infiltrating lymphocyte therapy Adoptive transfer therapy with tumor-infiltrating lymphocytes (TILs) requires the isolation of T cells from fresh patient biopsy specimens and the progressive selection of tumor-specific T cells ex vivo using high levels of IL-2. The adoptive transfer of these cells, with perhaps one exception [30], has been almost uniformly disappointing [58-60]. However, recent studies suggest that prior host conditioning with chemotherapy increases the response to adoptive immunotherapy with TILs [31,61]. An objective response rate of 50% was confirmed in a subsequent report from the same group [61]. Importantly, the TILs showed prolonged engraftment compared with TILs transfused to patients without prior treatment with these chemotherapeutics, and the levels of engraftment correlated with the clinical responses. However, the ability to successfully generate TILs for therapy could in itself be predictive of a more favorable clinical outcome [40,62]. In the absence of a randomized clinical trial it is not possible to determine how much lymphoablative chemotherapy, highdose IL-2 administration and TIL therapy contributed to the promising results of these recent trials. This indicates the importance of the measurement of cell yield, expression of homing receptors, potency and immune assessment assays in developing improved methods of cell processing. Technical issues with producing tumor-specific T cells currently present a formidable barrier to conducting randomized clinical trials using TILs. Only 30 40% of biopsy specimens yield satisfactory T-cell populations, and the process is labor- and time-intensive, requiring about 6 weeks to produce the T cells for infusion [63]. Therefore, randomized trials based on rigorous intent-to-treat analysis design (in which all data from all patients are included in the data analysis and any patients who are discontinued or otherwise non-evaluable are considered to be treatment failures) cannot be performed using currently available tissue culture technologies, and the trials reported to date have been performed based on an ad hoc, as-treated analysis plan. Should technical limitations of current tissue culture approaches be overcome, TILs harvested from other commonly encountered epithelial cancers, in addition to melanoma, could be expanded to clinically relevant numbers. 3.5 Genetic engineering of T-cell function In patients with congenital and acquired immunodeficiency, genetically modified T cells have been shown to persist for years following adoptive transfer [51,64-66], which indicates that the general approach is feasible. Persistence with conditions such as adenosine deaminase deficiency, where there is a strong selective advantage for the corrected genetically modified cells, have shown the most durable persistence. A potential safety concern when infusing individuals with engineered T cells is one that arose with genetically engineered hematopoietic stem cells (HSCs) for severe combined immunodeficiency in four patients in one study [67], and recently one patient [68] in a second similar study [69], when viral insertional mutagenesis was shown to cause cellular transformation [70]. Although there is little clinical experience with engineered T cells for cancer therapy, it is notable that clinical trials to date using cells engineered to express suicide molecules have indicated that the approach is safe. It may be that terminally differentiated cells, such as T lymphocytes pose less of a risk for transformation than hematopoietic stem cells. Unlike HSCs, currently available retroviral vectors provide high-level expression of transgenes in T cells in vitro. The advent of lentiviral vectors has greatly increased the efficiency of human T-cell engineering, and a recent pilot study with lentivirus-engineered T cells that expressed an antisense HIV vector showed promise in patients infected with HIV [71]. As mentioned above, insertional mutagenesis is a safety concern with any integrating viral vector. It is reassuring that the natural history of HIV does not include an increased incidence of T-cell leukemia; this provides empirical data that lentiviral vectors might be safer in this respect than oncoretroviral vectors. Furthermore, side-by-side tests in preclinical models indicate that lentiviral vectors are less prone to insertional mutagenesis [72]. Nevertheless, longterm observational studies with large patient safety data sets are required to determine the ultimate safety of this approach. A novel targeted gene correction technique employs chimeric zinc-finger proteins coupled to endonucleases [73]. With these zinc-finger nucleases, genes can be corrected or disabled in T cells in a specific fashion without the need for integrating vectors, an approach that could be applied to a number of monogenic congenital and acquired diseases such as HIV [74]. Ex vivo gene delivery to T cells, has advantages over in vivo delivery of gene vectors in terms of efficiency and persistence, and may be a safer approach that reduces the risk of off-target genetic modification and adverse events T cells engineered to express tumor-antigen-specific receptors One genetic engineering approach has been to endow T cells with novel receptors by introduction of T bodies, chimeric receptors that have an antibody-based external receptor linked to cytosolic domains that encode signal transduction modules of the T-cell receptor [75]. These constructs can function to retarget T cells in an MHC-unrestricted manner to attack the tumor or virally Expert Opin. Biol. Ther. (2008) 8(4) 479
6 T lymphocyte engineering ex vivo for cancer and infectious disease infected cell while retaining MHC-restricted specificity of their endogenous TCR. An additional benefit is that a population of antigen-specific T cells can be generated without extensive T-cell expansion and differentiation to a TEM population. One trial that tested T cells expressing a T body receptor specific for a folate-binding protein present on ovarian carcinoma cells indicated that the approach was safe but poor expression and persistence of the transgene encoding the T body receptor were observed in vivo [76]. Similarly, a pilot test in children with neuroblastoma treated with autologous T cells retargeted for a tumor-associated adhesion molecule indicated that the approach was safe but limited by poor persistence of the T cells [77]. Lamers and colleagues recently tested T cells expressing a T body receptor specific for carbonic anhydrase IX (CAIX), an antigen present on the surface of clear-cell renal cell carcinoma [78]. They observed an unexpected serious hepatic toxicity in several patients within a week of T-cell infusion that seemed to be due to CAIX expression in the biliary tract. If confirmed, this would indicate that engineered T cells can traffic to and exert effector function at sites of antigen expression in vivo. However, this study indicates that the targets of chimeric antigen receptors must be carefully chosen to avoid unwanted autoimmune and other adverse effects, or that additional safety features, such as suicide switches (see below), should be incorporated. In several of the patients in the studies described above, the engineered cells persisted for several days to weeks before elimination by host immune responses [76-78], indicating that a technical challenge for this approach is to prevent a host immune response from eliminating the adoptively transferred cells. Optimizing the ligand-binding domain and incorporating costimulatory signaling domains [79,80], may ensure better long-term survival of the T cells so that the proper costimulatory signals can be delivered upon target recognition [79,81]. T cells are also being transduced to express natural TCR specific for MART-1 in a study where lymphodepleted patients with melanoma were given a single infusion of engineered T cells followed by IL-2 [82]. A concern with transgenic TCR has been that additional, novel receptor specificities might be generated by pairing of the transgenes with the endogenous TCR chains [83]. A general limitation of inserting TCR as opposed to antibody/tcr chimeric receptors for humans is that each TCR is specific for a given peptide-mhc complex, such that each TCR vector would only be useful for patients that shared both MHC alleles and tumor antigens. Engineering enhanced specificity of T cells through receptor modification has recently been reviewed in further detail [84,85] Engineering enhanced T-cell survival or death A limitation of adoptive transfer of expanded CTLs discussed above is that they have short-term persistence in the host in the absence of antigen-specific Th cells and/or exogenous cytokine infusions. In some settings, where passenger lymphocytes or HSC will eventually reconstitute the lymphoid compartment, this may be acceptable. In chronic infections or residual disease where immediate and sustained immune augmentation is required, other strategies are being pursued. Greenberg and co-workers have transduced human CTLs with chimeric GM-CSF IL-2 receptors that deliver an IL-2 signal when they bind GM-CSF [86]. Stimulation of the CTLs with antigen caused GM-CSF secretion and resulted in an autocrine growth loop such that the CTL clones proliferated in the absence of exogenous cytokines. This type of genetic modification has the potential to increase the circulating half-life of the CTLs and, by extension, the efficacy of these ex vivo-expanded cells. A related strategy to rejuvenate T-cell function is to engineer T cells to ectopically express CD28 [87] or the catalytic subunit of telomerase [88]. Severe and potentially lethal GVHD represents a frequent complication of allogeneic immunotherapy and donor lymphocyte infusion (DLI). The promising results with DLI have created increased interest in developing T cells with an inducible suicide phenotype. Expression of herpes simplex virus thymidine kinase (HSV-TK) in T cells provides a means of ablating transduced T cells in vivo by the administration of acyclovir or ganciclovir. Using this strategy, Bordignon and colleagues infused allogeneic donor lymphocytes engineered to express HSV-TK into patients with refractory hematologic malignancies who had suffered complications following allogeneic bone marrow transplants and donor lymphocytes [89]. The HSV-TK lymphocytes survived for up to a year, and complete or partial tumor remission in five of eight patients was achieved. Tumor regression coincided with onset of GVHD, and in most cases, GVHD was abrogated when ganciclovir was administered. A recent Phase II clinical trial has confirmed and extended these results [90]. It is possible that the first form of adoptive therapy with engineered T cells to enter clinical practice will be the use of allogeneic T cells with a conditional suicide switch, as a Phase III clinical trial is planned to test this approach in the setting of haploidentical HSC transplantation. The principal concern with the HSV-TK approach has been that it would generate potent HSV-TK specific immune responses as others have found that humans efficiently reject cells engineered to express HSV-TK or similar constructs [91,92]. Therefore, HSV-TK might confer immunogenicity to the transfused cells, leading to their impaired survival and the inability to retreat a patient with a DLI of cells engineered to express HSV-TK should the tumor recur. In patients who are immunosuppressed, this may not be the case. Development of vectors that encode less immunogenic suicide proteins will be required to extend this approach to immunocompetent hosts. Recently, investigators have developed suicide systems comprised of fusion proteins containing a human FAS or caspase death domain and a modified FK506-binding protein (FKBP) [93,94]. T cells expressing these modified 480 Expert Opin. Biol. Ther. (2008) 8(4)
7 Levine Figure 2. First generation artificial antigen presenting cells. Magnetic beads 4.5 µm in diameter are coupled to monoclonal antibodies directed against CD3 and CD28 on T lymphocytes. Beads are added to T lymphocytes at a 3:1 ratio enabling efficient activation and expansion [96]. chimeric proteins are induced to undergo apoptosis when exposed to a drug that dimerizes the modified FKBP. These approaches have the advantage that the suicide switches are expected to be non-immunogenic because they are based on endogenous proteins. 3.6 Tuning up T lymphocytes with artificial antigen presenting cells In recent years, a greater understanding has emerged of the receptor signaling pathways for T-cell activation, particularly the recognition that both a primary specificity signal via the T-cell receptor (TCR) (Signal 1) and a costimulatory/regulatory signal via the CD28 receptor (Signal 2) are simultaneously required for the generation of full T-cell effector function and a long-lasting immune response [81]. In cancer or infectious disease, antigen-specific T cells may have been deleted or tolerized due to suboptimal T-cell activation. With this knowledge, we have developed efficient and reproducible methods of mimicking the signal provided to T cells by dendritic cells but without delivering a negative costimulatory signal. With consistent lots of artificial antigen presenting cells (aapc), appropriate signals can reproducibly be delivered to T cells to improve on the function, activation/expansion and length of T-cell survival in vivo. These aapc methods allow for T cells to be grown rapidly ex vivo to clinical scale for therapeutic applications. The technology enables direct T-cell activation, instead of indirect activation via vaccines, which can be modulated by the nature of cell dose as necessary to achieve a clinical response [95,96]. The first generation of off-the-shelf aapc was developed by covalently linking clinical grade anti-human CD3 and anti-cd28 monoclonal antibodies to magnetic beads, which serves to crosslink the endogenous CD3 and CD28 receptors on the T cell ( Figure 2 ). This bead-based aapc enables the most efficient growth of human polyclonal naive and memory CD4 + T cells reported [96]. In terms of cell function, the expanded cells retain a highly diverse TCR repertoire and, by varying the culture conditions, can be induced to secrete cytokines characteristic of Th1 or Th2 cells [27]. One important advantage of this bead-based system is that it does not crossreact with CTL antigen 4 (CTLA4) and therefore provides unopposed CD28 stimulation for more efficient expansion of T cells. Another, unanticipated discovery was that crosslinking of CD3 and CD28 with bead-immobilized antibody renders CD4 + T lymphocytes highly resistant to HIV infection. This is due to the downregulation of the chemokine receptor CCR5, a necessary co-receptor for the internalization of HIV, and the induction of high levels of β -chemokines, the natural ligands for CCR5 [97,98], and allows for the efficient culture of CD4 + T cells from HIV-infected study subjects. Ex vivo expansion may also indirectly enhance T-cell activity by removing T cells from a tumor-induced immunosuppressive milieu [99,100]. Other key features are that exogenous growth factors or accessory cells are not needed to enable T-cell stimulation and expansion, as with previous methods. 3.7 Cell-based artificial antigen presenting cells Recently, aapc lines derived from the chronic myelogenous leukemia line K562 have been described [ ]. K562 cells do not express MHC) or T costimulatory ligands, and these cells may represent DC precursors that retain many other attributes that make DCs such effective APCs, such as cytokine production, adhesion molecule expression and macropinocytosis. These cells have been transduced with a library of lentiviral vectors that allows for the customized expression of stimulatory and costimulatory molecules that can be used to activate and expand different subset of T cells, and can be further modified to amplify antigen specific T cells in culture. These aapcs offer the advantage of expression of molecules additional to CD3 and CD28 on their surface. The K562 aapcs have been transduced with vector to express the antibody Fc-binding receptor and the costimulatory molecule 4-1BB. The expression of CD64, the high affinity Fc receptor, on K562 aapc s allows the flexibility of loading antibodies directed against T-cell surface receptors. CD3 and CD28 antibodies are added to the cells and are bound by the Fc receptor to yield a cell that expresses anti-cd3 mab, anti-cd28 mab and 4-1BB. These cell-based aapc s have proved to be more efficient at Expert Opin. Biol. Ther. (2008) 8(4) 481
8 T lymphocyte engineering ex vivo for cancer and infectious disease LV-aAPC T cell Figure 3. Second-generation artificial antigen presenting cells optimized for CD8 T lymphocytes and antigen-specific T lymphocyte activation. K562 cell lentivirally transduced to express CD64 and CD137L and loaded with anti-cd3 and anti-cd28 antibodies stimulates a CD8 + T lymphocyte [103]. activating and expanding T cells, especially CD8 +, CD28 - TEM, and antigen-specific T cells ( Figure 3 ), than the magnetic bead-based aapc [103]. In addition, the cells are capable of stimulating CD4 cells efficiently. Thus, K562 cells may represent ideal scaffolds to which the desired MHC molecules, costimulatory ligands, and cytokines can be introduced in order to establish a DC-like aapc that has the advantages of DCs (e.g., high levels of MHC expression, a wide array of costimulatory ligands and the ability to engage in cytokine crosstalk with the T cell) without any of the disadvantages (i.e., the need to derive natural DCs from either G-CSF mobilized CD34 + cells or monocytes using cytokines that are not currently available as good manufacturing practice reagents, patient-specific expansion, limited lifespan and limited replicative capacity). Moreover, these cells have been injected into humans as part of a tumor vaccine [104], signifying that these cells can be used in a good manufacturing practice manner. Additionally, this lab and its colaborators have now developed either bead- or cell-based aapcs optimized for Th2 cells [27,105], and for T regulatory cells [106]. 4. Clinical-scale culture of co-stimulated T lymphocytes for cell therapy 2 µm One challenge in translating research findings to clinical scale is technical, there may be differences in cell yield and function due to changes in nutrient and metabolite exchange, gas transfer, shear stress, or other conditions at large scale that are not apparent at small scales. A second challenge is the availability of clinical-grade reagents, materials and equipment to enable cellular engineering at the clinical scale that mimics as closely as possible the methods developed at the research scale. The use of either the bead-based or cell-based aapc s described above serves as an efficient GMP-compatible method for robust production of engineered T lymphocytes. In the case of bead-based aapc, a cohort of clinical trials (described in the next section) has demonstrated safety and feasibility of co-stimulated T lymphocytes, and the potential for efficacy in malignancies and HIV infection. Independent of which of the aapcs is used, the manufacturing procedure remains similar, starting with an apheresis product and depleting monocytes either by adherence to magnetic beads or via an Elutra counterflow centrifugal elutriator. If a CD8 + or CD4 + T-cell product is desired, the depletion of CD4 + or CD8 + T cells can be accomplished via large-scale magnetic cell selection in a closed and sterile system. T cells can then be cultured in a nutrient media and stimulated to divide and grow via the addition of either antibody-coated magnetic beads or the irradiated and antibody preloaded K562 aapc s described above. With either method, gene transduction with either retroviral or lentiviral vectors is very efficient [65,71,107]. T cells may be cultured either in static gas-permeable bags [108] or in a dynamic wave action bioreactor at high concentrations. Measurement of nutrients and metabolites in the cell culture media can provide invaluable assistance in optimizing conditions beyond what can be gleaned from simply counting and phenotyping cells. After completion of cell culture, antibody coated beads are removed by passing the cells over a magnet using a closed system of bags and tubing [108]. Prior to infusion, engineered T cells must be tested to ensure that they meet release criteria such as T-cell phenotype, cell viability, pyrogenicity, sterility and demonstration of the removal of residuals such as beads used in manufacturing to address regulatory requirements regarding purity, potency and sterility [109,110]. 5. Clinical trials of co-stimulated T lymphocytes To date, several hundred infusions of co-stimulated beadexpanded T cells have been safely administered to treat several types of malignancies with both autologous and allogeneic T cells and HIV with autologous T cells. In patients with high risk lymphoma, expanded co-stimulated T cells were infused on day 14 post CD34-selected hematopoietic stem cell transplantation (HCT), and immune reconstitution was assessed following post-transplant T-cell reconstitution. Of the 16 subjects, 5 had an unexpected lymphocytosis following T-cell infusion and the frequency of interferon- γ secreting cells also increased markedly in some patients. This trial indicated for the first time that it is possible to accelerate immune reconstitution in patients with advanced lymphoma who are given high dose therapy and autologous stem cell transplantation. In a subsequent trial 482 Expert Opin. Biol. Ther. (2008) 8(4)
9 Levine for chronic myelogenous leukemia, a second objective was to determine the frequency of hematologic, cytogenetic and molecular remissions from the treatment approach of autologous transplants followed by T-cell infusions. Of the four subjects who proceeded through the trial regimen, all had rapid recovery of lymphocyte counts following T-cell infusion and had complete cytogenetic remissions early after transplantation, three also became PCR negative for the bcr/abl fusion mrna [111]. A randomized Phase I/II study in subjects with advanced myeloma was designed to examine the relative benefits of pre- and post-transplant vaccine immunizations in combination with adoptive T-cell transfer. Post-stem-cell-transplant lymphocyte reconstitution and the pneumococcal vaccine (Prevnar) response were evaluated in 42 subjects. As in the lymphoma trial, the infusion of activated autologous T cells by day 14 post-transplant resulted in the induction of what appeared to be homeostatic T-cell proliferation in the first few weeks following transplantation. In addition, only those subjects that received antigen-experienced T cells showed robust antibody responses. This in vivo prime-and-boost with ex vivo -expanded and co-stimulated T cells would be a hybrid of the two approaches shown in Figure 1 and may prove to be a useful way to generate and/or enhance protective antitumor immunity [20,42] and in infectious diseases where effective vaccines are not yet available. A follow-on trial is now open in which the potency of a putative myeloma-specific peptide vaccine is being tested to evaluate the induction of T-cell-mediated graft versus myeloma effect. In an allogeneic setting, activated donor leukocyte infusions (adli) were administered in a trial to treat relapsed advanced hematologic malignancies after allogeneic bone marrow transplantation and standard DLI [28]. Of the 17 subjects evaluable for response, 8 achieved a complete remission with 6 still alive in complete remission a median of 17 months after adli. This trial suggests that adoptive transfer of activated allogeneic T cells is associated with durable complete remission in a subset of subjects without excessive GVHD or other toxicity. In general, these trials demonstrate that infusion of activated and expanded T cells, in combination with other therapies such as stem cell transplantation, chemotherapy and alkylating agent therapy (i.e., melphalan-containing regimens) has been associated with complete and partial responses in the treated subjects. In follicular lymphoma, regulatory-t-cell-depleted and co-stimulated T-cell infusion results in significant CD4 + and CD8 + numerical and functional lymphocyte recovery after cyclophosphamide-fludarabine chemotherapy [24,112]. In HIV, adoptive transfer of co-stimulated autologous CD4 + T cells resulted in a dose-dependent increase in CD4 counts and in the CD4:CD8 ratio following infusions. Sustained increases in CD4 + T-cell numbers and decreases in the percentage of CD4 + CCR5 + cells in patients were also found, suggesting augmentation of natural immunity to HIV infection [113]. More recently, co-stimulated T cells genetically modified using vectors that express proteins or antisense RNAs that target specific HIV genes have been generated and the safety and feasibility of this gene transduction and expansion method has beenassessed in the first clinical trial of a lentiviral vector [71,114]. In HIV+ study subjects who had failed at least two prior combinationantiviral drug regimens, following T-cell infusion, viral loads were stable or decreased in all five subjects. One subject has had a prolonged 2-log decrease in viral load for at least 2 years. CD4 counts remained stable in all patients and circulating genetically modified cells were detected in all patients for at least 6 months. Sustained lentiviral gene transfer was demonstrated in all subjects, and has persisted for more than 2 years in three of the patients. Promising results in heavily pretreated patients, from these early trials for various cancers and HIV, have led to a second series of randomized trials to address the efficacy of engineered T-cell therapies. 6. Expert opinion Cell therapies created through ex vivo manipulation may entail the isolation and/or propagation of T lymphocytes with a greater specificity for tumor antigens or pathogens along with enhanced function, or engineered with novel functions. Considerations of the best method to produce a large population of functional antigen-specific T cells ex vivo have centered on the source of T cells followed by repetitive stimulations in extended ex vivo culture. This requirement may be surmountable by redirection of T-cell specificity through gene transfer of chimeric receptor or engineered TCR constructs. Alternatively, the ex vivo manipulation may serve to activate, reeducate or endow T cells with enhanced or novel functions in a way that was not possible in vivo, perhaps due to masking of antigens or disease-induced immunosuppression. Central to the success of future clinical trials of engineered T lymphocytes is the determination of whether one approach or a combination of approaches should be employed and how to engineer and manufacture the respective T lymphocytes for human testing in a variety of disease settings. It may be that a combination approach, where patients are first vaccinated with peptides, proteins, DNA or peptide pulsed DCs, followed by collection of the primed T cells, expansion and reinfusion may be the best approach in settings of immune deficiency or tumor tolerance [20,42,43]. Box 1 lists some points to consider in engineering effective T lymphocyte therapies in the light of our current understanding of T lymphocyte biology and homeostasis. Unfortunately, until recently many trials were carried out before the complexity of T-cell biology and costimulation was understood. As a result, cells were propagated under what are now understood to be suboptimal conditions that impair the essential functions and long-term engraftment of T cells. Similarly, in vitro Expert Opin. Biol. Ther. (2008) 8(4) 483
10 T lymphocyte engineering ex vivo for cancer and infectious disease Box 1. Points to consider in ex vivo engineering of an effective T lymphocyte therapy. The infused T-cell population should retain properties that permit persistence and homing to tumor or lymph node Engraftment and persistence of adoptively transferred CTLs may well depend on adequate CD4 T-cell help or exogenous cytokine support Transduced gene product of transferred cells should not be immunogenic T-cell manufacturing process should avoid induction of replicative senescence Effector to target ratio: host tumor burden should not exceed killing capacity of adoptively transferred cells Tumor- or HIV-antigen-specific T cells may have been deleted or tolerized in the donor by previous chemotherapy or by the tumor itself Lack of costimulation may induce anergy or apoptosis of adoptively transferred cells activity observed in preclinical experiments may not translate to in vivo activity due to a lack of costimulation in the local tumor environment or any of several other reasons listed in Box 1. There is now a more detailed understanding of the regulation of T-cell activation and signaling, the process of immunosenescence, and a greater appreciation of the heterogeneity of T-cell memory, effector and regulatory/suppressor (Tregs) cell subsets. The implications of these findings need to be incorporated into the translation of therapeutic approaches from animal models to clinical settings. In addition, the ideal ex vivo culture process in a research setting must be adapted to clinical scale and clinically compatible reagents to achieve regulatory compliance and yet still be robust enough to support large scale trials of potent cells [109]. With improved methods of T lymphocyte engineering, a remaining barrier is widespread access and application of new technologies consistent with optimum and durable T-cell function. Frequently, reagents or materials that serve the research market are either not available in clinical grades or are prohibitively expensive. There are limited options for equipment for large-scale cell isolation, washing and concentration with sterile fluid paths. Should cell therapies be viewed as a traditional vaccine manufactured in central plants or processing facilities or more like surgery or stem cell transplantation? What federal, philanthropic and industry-funded mechanisms will ensure the clinical development, manufacturing and conduct of definitive clinical trials? These major challenges facing the field at present must be met to expand upon the promise of early successful trials. Demonstrated clinical benefit in randomized clinical trials will then justify the regulatory approval for licensure of customized T lymphocyte therapies. Acknowledgements The author would like to acknowledge helpful discussions and assistance from C June, J Riley, R Carroll, A Chew, G Binder and D Powell. Declaration of interest BL Levine is a consultant for GE Healthcare. 484 Expert Opin. Biol. Ther. (2008) 8(4)
11 Levine Bibliography Papers of special note have been highlighted as either of interest ( ) or of considerable interest ( ) to readers. 1. Kaech SM, Ahmed R. Memory CD8 + T cell differentiation: initial antigen encounter triggers a developmental program in naive cells. Nat Immunol 2001 ;2(5): Sallusto F, Geginat J, Lanzavecchia A. Central memory and effector memory T cell subsets: function, generation, and maintenance. Ann Rev Immunol 2004 ;22: Fearon DT, Manders P, Wagner SD. Arrested differentiation, the self-renewing memory lymphocyte, and vaccination. Science 2001 ;293(5528): Opferman JT, Ober BT, Shton-Rickardt PG. Linear differentiation of cytotoxic effectors into memory T lymphocytes. Science 1999 ;283(5408): Bouneaud C, Garcia Z, Kourilsky P, Pannetier C. Lineage relationships, homeostasis, and recall capacities of central- and effector-memory CD8 T cells in vivo. J Exp Med 2005 ;201(4): Chang JT, Palanivel VR, Kinjyo I, et al. Asymmetric T lymphocyte division in the initiation of adaptive immune responses. Science 2007 ;315(5819): Maus MV, Kovacs B, Kwok WW, et al. Extensive replicative capacity of human central memory T cells. J Immunol 2004 ;172(11): Weng NP, Palmer LD, Levine BL, et al. Tales of tails: regulation of telomere length and telomerase activity during lymphocyte development, differentiation, activation, and aging. Immunol Rev 1997 ;160: Sallusto F, Lenig D, Forster R, et al. Two subsets of memory T lymphocytes with distinct homing potentials and effector functions. Nature 1999 ;401(6754): Klebanoff CA, Gattinoni L, Torabi-Parizi P, et al. Central memory self/tumor-reactive CD8 + T cells confer superior antitumor immunity compared with effector memory T cells. Proc Natl Acad Sci USA 2005 ;102(27): Monteiro J, Batliwalla F, Ostrer H, Gregersen PK. Shortened telomeres in clonally expanded CD28-CD8 + T cells imply a replicative history that is distinct from their CD28 + CD8 + counterparts. J Immunol 1996 ;156(10): Van den Hove LE, Van Gool SW, Vandenberghe P, et al. CD57 + /CD28 - T cells in untreated hemato-oncological patients are expanded and display a Th1-type cytokine secretion profile, ex vivo cytolytic activity and enhanced tendency to apoptosis. Leukemia 1998 ;12(10): Barber DL, Wherry EJ, Ahmed R. Cutting edge: rapid in vivo killing by memory CD8 T cells. J Immunol 2003 ;171(1): Sprent J, Surh CD. T cell memory. Ann Rev Immunol 2002 ;20: Bevan MJ. Helping the CD8(+) T-cell response. Nat Rev Immunol 2004 ;4(8): Ossendorp F, Mengede E, Camps M, et al. Specific T helper cell requirement for optimal induction of cytotoxic T lymphocytes against major histocompatibility complex class II negative tumors. J Exp Med 1998 ;187(5): Schoenberger SP, Toes RE, van d V, et al. T-cell help for cytotoxic T lymphocytes is mediated by CD40-CD40L interactions. Nature 1998 ;393(6684): Yee C, Thompson JA, Byrd D, et al. Adoptive T cell therapy using antigen-specific CD8 + T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc Natl Acad Sci USA 2002 ;99(25): A clinical trial demonstrating that CD8 + clones persist at higher levels in peripheral blood when IL-2 is also infused. 19. Einsele H, Roosnek E, Rufer N, et al. Infusion of cytomegalovirus (CMV)-specific T cells for the treatment of CMV infection not responding to antiviral chemotherapy. Blood 2002 ;99(11): Rapoport AP, Stadtmauer EA, Aqui N, et al. Restoration of immunity in lymphopenic individuals with cancer by vaccination and adoptive T-cell transfer. Nat Med 2005 ;11(11): A randomized clinical trial showing the early reconstitution of lymphocytes and early induction of functional immunity to pneumococcus post stem cell transplantation following in vivo vaccine priming followed by the early infusion of primed and expanded T lymphocytes. 21. Jiang H, Chess L. An integrated view of suppressor T cell subsets in immunoregulation. J Clin Invest 2004 ;114(9): Shimizu J, Yamazaki S, Sakaguchi S. Induction of tumor immunity by removing CD25 + CD4 + T cells: a common basis between tumor immunity and autoimmunity. J Immunol 1999 ;163(10): A demonstration that in mice, the depletion of CD4 + CD25 + cells or administration of anti-cd25 antibody can augment anti-tumor immunity. 23. Liu W, Putnam AL, Xu-Yu Z, et al. CD127 expression inversely correlates with FoxP3 and suppressive function of human CD4 + T reg cells. J Exp Med 2006 ;203(7): Schuster SJ, Levine BL, Nasta S, et al. Adoptive immunotherapy with autologous CD25-depleted and CD3/CD28-costimulated T-cells (ACTC) enhances numeric and functional lymphocyte recovery after cyclophosphamide fludarabine chemotherapy in patients with low-grade follicular lymphoma. Blood 2007 ;110(11): Woo EY, Chu CS, Goletz TJ, et al. Regulatory CD4(+)CD25(+) T cells in tumors from patients with early-stage non-small cell lung cancer and late-stage ovarian cancer. Cancer Res 2001 ;61(12): Evidence is presented that costimulation provided by triggering the CD28 receptor is able to increase CD25 expression and cytokine secretion in tumor-associated T cells. 26. Loren AW, Bunin GR, Boudreau C, et al. Impact of donor and recipient sex and parity on outcomes of HLA-identical sibling allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2006 ;12(7): Fowler DH, Odom J, Steinberg SM, et al. Phase I clinical trial of costimulated, IL-4 polarized donor CD4 + T cells as augmentation of allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant 2006 ;12(11): Porter DL, Levine BL, Bunin N, et al. A phase 1 trial of donor lymphocyte infusions expanded and activated ex vivo via CD3/CD28 costimulation. Blood 2006 ;107(4): Expert Opin. Biol. Ther. (2008) 8(4) 485
12 T lymphocyte engineering ex vivo for cancer and infectious disease 29. June CH, Blazar BR. Clinical application of expanded CD cells. Semin Immunol 2006 ;18(2): Kono K, Takahashi A, Ichihara F, et al. Prognostic significance of adoptive immunotherapy with tumor-associated lymphocytes in patients with advanced gastric cancer: a randomized trial. Clin Cancer Res 2002 ;8(6): Dudley ME, Wunderlich JR, Robbins PF, et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 2002 ;298(5594):850-4 Evidence is presented that the addition of a non-myeloblative, but lymphodepleting conditioning regimen, showed, in contrast to previous studies, a robust engraftment of ex vivo -expanded tumor infiltrating lymphocytes. In 6 of 13 patients regression of metastatic melanoma was observed. 32. Chang AE, Aruga A, Cameron MJ, et al. Adoptive immunotherapy with vaccine-primed lymph node cells secondarily activated with anti-cd3 and interleukin-2. J Clin Oncol 1997 ;15(2): Takayama T, Sekine T, Makuuchi M, et al. Adoptive immunotherapy to lower postsurgical recurrence rates of hepatocellular carcinoma: a randomised trial. Lancet 2000 ;356(9232): Feuerer M, Beckhove P, Bai L, et al. Therapy of human tumors in NOD/SCID mice with patient-derived reactivated memory T cells from bone marrow. Nat Med 2001 ;7(4): Choi C, Witzens M, Bucur M, et al. Enrichment of functional CD8 memory T cells specific for MUC1 in bone marrow of patients with multiple myeloma. Blood 2005 ;105(5): Schmitz-Winnenthal FH, Volk C, Z graggen K, et al. High frequencies of functional tumor-reactive T cells in bone marrow and blood of pancreatic cancer patients. Cancer Res 2005 ;65(21): Noonan K, Matsui W, Serafini P, et al. Activated marrow-infiltrating lymphocytes effectively target plasma cells and their clonogenic precursors. Cancer Res 2005 ;65(5): Trickett A, Dwyer J, Tedla N, Lam-Po-Tang R. Safety and feasibility of harvesting cells for adoptive immunotherapy from patients with asymptomatic HIV infection. J Acquir Immune Defic Syndr Hum Retrovirol 1996 ;12(5): Korbling M, Giralt S, Khouri I, et al. Donor lymphocyte apheresis for adoptive immunotherapy compared with blood stem cell apheresis. J Clin Apher 2001 ;16(2): Zhang L, Conejo-Garcia JR, Katsaros D, et al. Intratumoral T cells, recurrence, and survival in epithelial ovarian cancer. N Engl J Med 2003 ;348(3): Germeau C, Ma W, Schiavetti F, et al. High frequency of antitumor T cells in the blood of melanoma patients before and after vaccination with tumor antigens. J Exp Med 2005 ;201(2): Molldrem JJ. Vaccinating transplant recipients. Nat Med 2005 ;11(11): Powell DJ Jr, Dudley ME, Hogan KA, et al. Adoptive transfer of vaccine-induced peripheral blood mononuclear cells to patients with metastatic melanoma following lymphodepletion. J Immunol 2006 ;177(9): Feuchtinger T, Matthes-Martin S, Richard C, et al. Safe adoptive transfer of virus-specific T-cell immunity for the treatment of systemic adenovirus infection after allogeneic stem cell transplantation. Br J Haematol 2006 ;134(1): Schultze JL, Michalak S, Seamon MJ, et al. CD40-activated human B cells: an alternative source of highly efficient antigen presenting cells to generate autologous antigen-specific T cells for adoptive immunotherapy. J Clin Invest 1997 ;100(11): Yee C, Thompson JA, Roche P, et al. Melanocyte destruction after antigen-specific immunotherapy of melanoma: direct evidence of T cell-mediated vitiligo. J Exp Med 2000 ;192(11): Mackensen A, Meidenbauer N, Vogl S, et al. Phase I study of adoptive T-cell therapy using antigen-specific CD8 + T cells for the treatment of patients with metastatic melanoma. J Clin Oncol 2006 ;24(31): Walter EA, Greenberg PD, Gilbert MJ, et al. Reconstitution of cellular immunity against cytomegalovirus in recipients of allogeneic bone marrow by transfer of T-cell clones from the donor. N Engl J Med 1995 ;333(16): Riddell SR, Watanabe KS, Goodrich JM, et al. Restoration of viral immunity in immunodeficient humans by the adoptive transfer of T cell clones. Science 1992 ;257: A clinical trial showing that adoptive transfer of Cytomegalovirus-specific CD8 + cytotoxic T cell clones could establish anti-viral immunity in vivo. 50. Rooney CM, Smith CA, Ng CY, et al. Use of gene-modified virus-specific T lymphocytes to control Epstein-Barr-virus-related lymphoproliferation. Lancet 1995 ;345(8941):9-13 Ex vivo -expanded and genetically marked EBV-specific donor derived CTL were shown to engraft and persist and were associated with clinical benefit in patients with EBV lymphoproliferative disease. 51. Heslop HE, Ng CY, Li C, et al. Long-term restoration of immunity against Epstein-Barr virus infection by adoptive transfer of gene-modified virus-specific T lymphocytes. Nat Med 1996 ;2(5): Bollard CM, Savoldo B, Rooney CM, Heslop HE. Adoptive T-cell therapy for EBV-associated post-transplant lymphoproliferative disease. Acta Haematol 2003 ;110(2-3): Khanna R, Bell S, Sherritt M, et al. Activation and adoptive transfer of Epstein-Barr virus-specific cytotoxic T cells in solid organ transplant patients with posttransplant lymphoproliferative disease. Proc Natl Acad Sci USA 1999 ;96(18): Gottschalk S, Heslop HE, Roon CM. Treatment of Epstein-Barr virus-associated malignancies with specific T cells. Adv Cancer Res 2002 ;84: Leen AM, Myers GD, Sili U, et al. Monoculture-derived T lymphocytes specific for multiple viruses expand and produce clinically relevant effects in immunocompromised individuals. Nat Med 2006 ;12(10): This paper describes a novel strategy for the simultaneous expansion of T cells specific for CMV, EBV and adenovirus. EBV-transformed antigen presenting cell lines were genetically modified with chimeric adenoviral vectors encoding CMV antigen. 56. Brodie SJ, Patterson BK, Lewinsohn DA, et al. HIV-specific cytotoxic T lymphocytes traffic to lymph nodes and localize at 486 Expert Opin. Biol. Ther. (2008) 8(4)
13 Levine sites of HIV replication and cell death. J Clin Invest 2000 ;105(10): Tan R, Xu X, Ogg GS, et al. Rapid death of adoptively transferred T cells in acquired immunodeficiency syndrome. Blood 1999 ;93(5): Rosenberg SA, Yannelli JR, Yang JC, et al. Treatment of patients with metastatic melanoma with autologous tumorinfiltrating lymphocytes and interleukin 2. J Natl Cancer Inst 1994 ;86: Figlin RA, Thompson JA, Bukowski RM, et al. Multicenter, randomized, Phase III trial of CD8(+) tumor-infiltrating lymphocytes in combination with recombinant interleukin-2 in metastatic renal cell carcinoma. J Clin Oncol 1999 ;17(8): Dreno B, Nguyen JM, Khammari A, et al. Randomized trial of adoptive transfer of melanoma tumor-infiltrating lymphocytes as adjuvant therapy for stage III melanoma. Cancer Immunol Immunother 2002 ;51(10): Dudley ME, Wunderlich JR, Yang JC, et al. Adoptive cell transfer therapy following non-myeloablative but lymphodepleting chemotherapy for the treatment of patients with refractory metastatic melanoma. J Clin Oncol 2005 ;23(10): Extension of the results first reported in reference 31 to a total of 35 patients with refractory metastatic melanoma using selected and expanded TIL cultures. 62. Sato E, Olson SH, Ahn J, et al. Intraepithelial CD8 + tumor-infiltrating lymphocytes and a high CD8 + /regulatory T cell ratio are associated with favorable prognosis in ovarian cancer. Proc Natl Acad Sci USA 2005 ;102(51): Dudley ME, Wunderlich JR, Shelton TE, et al. Generation of tumor-infiltrating lymphocyte cultures for use in adoptive transfer therapy for melanoma patients. J Immunother 2003 ;26(4): (1997) 64. Muul LM, Tuschong LM, Soenen SL, et al. Persistence and expression of the adenosine deaminase gene for 12 years and immune reaction to gene transfer components: long-term results of the first clinical gene therapy trial. Blood 2003 ;101(7): This follow up report on the first clinical trial of gene modified T cells shows the persistence of these cells for 12 years in a highly selective in vivo environment of congenital adenosine deaminase deficiency. Currently, genetically modified cells can be detected in each patient 16 years after infusion (L. Muul, pers. commun.). 65. Mitsuyasu RT, Anton PA, Deeks SG, et al. Prolonged survival and tissue trafficking following adoptive transfer of CD4 ζ gene-modified autologous CD4(+) and CD8(+) T cells in human immunodeficiency virus-infected subjects. Blood 2000 ;96(3): van Lunzen J, Glaunsinger T, Stahmer I, et al. Transfer of autologous gene-modified T cells in HIV-infected patients with advanced immunodeficiency and drug-resistant virus. Mol Ther 2007 ;15(5): Cavazzana-Calvo M, Hacein-Bey S, de Saint BG, et al. Gene therapy of human severe combined immunodeficiency (SCID)-X1 disease. Science 2000 ;288(5466): Available from: X-SCID_statement_AT.pdf 69. Thrasher AJ, Gaspar HB, Baum C, et al. Gene therapy: X-SCID transgene leukaemogenicity. Nature 2006 ;443(7109):E Hacein-Bey-Abina S, von Kalle C, Schmidt M, et al. LMO2-associated clonal T cell proliferation in two patients after gene therapy for SCID-X1. Science 2003 ;302(5644):415-9 Following the development of leukemia in patients with severe combined immunodeficiency who had received retrovirally transduced hematopoietic stem cells, clonal proliferation of T cells was detected by TCR V β analysis. Tracking TCR V β clonality and integration site analysis is an important part of long-term follow up in gene transfer studies. 71. Levine BL, Humeau LM, Boyer J, et al. Gene transfer in humans using a conditionally replicating lentiviral vector. Proc Natl Acad Sci USA 2006 ;103(46): The first clinical use of a lentiviral vector. 72. Montini E, Cesana D, Schmidt M, et al. Hematopoietic stem cell gene transfer in a tumor-prone mouse model uncovers low genotoxicity of lentiviral vector integration. Nat Biotechnol 2006 ;24(6): Urnov FD, Miller JC, Lee YL, et al. Highly efficient endogenous human gene correction using designed zinc-finger nucleases. Nature 2005 ;435(7042): Perez E, Jouvenot Y, Miller JC, et al. Towards gene knock out therapy for AIDS/HIV: targeted disruption of CCR5 using engineered Zinc Finger Protein Nucleases (ZFNs). Mol Ther 2007 ;13:S Eshhar Z, Waks T, Bendavid A, Schindler DG. Functional expression of chimeric receptor genes in human T cells. J Immunol Methods 2001 ;248(1-2): Kershaw MH, Westwood JA, Parker LL, et al. A Phase I study on adoptive immunotherapy using gene-modified T cells for ovarian cancer. Clin Cancer Res 2006 ;12(20 Pt 1): Park JR, DiGiusto DL, Slovak M, et al. Adoptive transfer of chimeric antigen receptor re-directed cytolytic T lymphocyte clones in patients with neuroblastoma. Mol Ther 2007 ;15(4): Lamers CH, Sleijfer S, Vulto AG, et al. Treatment of metastatic renal cell carcinoma with autologous T-lymphocytes genetically retargeted against carbonic anhydrase IX: first clinical experience. J Clin Oncol 2006 ;24(13):e Loskog A, Giandomenico V, Rossig C, et al. Addition of the CD28 signaling domain to chimeric T-cell receptors enhances chimeric T-cell resistance to T regulatory cells. Leukemia 2006 ;20(10): Evidence is presented that the incorporation of the intracellular portion of the CD28 molecule fused to the CD3 ζ -chain and CD19 single-chain Fv chimeric receptor shows that suppression induced by T regulatory cells can be overcome compared with chimeric receptor with CD3 ζ alone in the intracellular portion. 80. Sadelain M, Riviere I, Brentjens R. Targeting tumours with genetically enhanced T lymphocytes. Nat Rev Cancer 2003 ;3(1): Riley JL, June CH. The CD28 family: a T-cell rheostat for therapeutic control of T-cell activation. Blood 2005 ;105(1): Morgan RA, Dudley ME, Wunderlich JR, et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 2006 ;314(5796):126-9 A clinical trial of redirected TCR gene-modified T cells shows engraftment and persistence of the Expert Opin. Biol. Ther. (2008) 8(4) 487
14 T lymphocyte engineering ex vivo for cancer and infectious disease modified cells, although only 2 of 17 patients demonstrated a sustained objective regression. 83. Heemskerk MH, Hagedoorn RS, van der Hoorn MA, et al. Efficiency of T-cell receptor expression in dual-specific T cells is controlled by the intrinsic qualities of the TCR chains within the TCR-CD3 complex. Blood 2007 ;109(1): Thomas S, Hart DP, Xue SA, et al. T-cell receptor gene therapy for cancer: the progress to date and future objectives. Expert Opin Biol Ther 2007 ;7(8): Berger C, Berger M, Feng J, Riddell SR. Genetic modification of T cells for immunotherapy. Expert Opin Biol Ther 2007 ;7(8): Evans LS, Witte PR, Feldhaus AL, et al. Expression of chimeric granulocyte-macrophage colony-stimulating factor/interleukin 2 receptors in human cytotoxic T lymphocyte clones results in granulocyte-macrophage colony-stimulating factor-dependent growth. Hum Gene Ther 1999 ;10(12): Chimeric GM-CSFR/IL-2R receptors that deliver an IL-2 signal on binding GM-CSF, a novel design to address the issue of long-term survival of adoptively transferred CTLs, are described. 87. Topp MS, Riddell SR, Akatsuka Y, et al. Restoration of CD28 expression in CD28- CD8 + memory effector T cells reconstitutes antigen-induced IL-2 production. J Exp Med 2003 ;198(6): Rufer N, Migliaccio M, Antonchuk J, et al. Transfer of the human telomerase reverse transcriptase (TERT) gene into T lymphocytes results in extension of replicative potential. Blood 2001 ;98(3): Bonini C, Ferrari G, Verzeletti S, et al. HSV-TK gene transfer into donor lymphocytes for control of allogeneic graft-versus-leukemia. Science 1997 ;276(5319): Ciceri F, Bonini C, Marktel S, et al. Antitumor effects of HSV-TK-engineered donor lymphocytes after allogeneic stem-cell transplantation. Blood 2007 ;109(11): A clinical demonstration that immune suppression of the patient and kinetics of graft versus tumor effect mediated by thymidine kinase-transduced donor lymphocytes in the setting of stem cell transplantation may allow the full exploitation of TK-DLI. 91. Riddell SR, Elliott M, Lewinsohn DA, et al. T-cell mediated rejection of gene-modified HIV-specific cytotoxic T lymphocytes in HIV-infected patients. Nat Med 1996 ;2(2): Berger C, Flowers ME, Warren EH, Riddell SR. Analysis of transgene-specific immune responses that limit the in vivo persistence of adoptively transferred HSV-TK-modified donor T cells after allogeneic hematopoietic cell transplantation. Blood 2006 ;107(6): Clackson T, Yang W, Rozamus LW, et al. Redesigning an FKBP-ligand interface to generate chemical dimerizers with novel specificity. Proc Natl Acad Sci USA 1998 ;95(18): Straathof KC, Spencer DM, Sutton RE, Rooney CM. Suicide genes as safety switches in T lymphocytes. Cytotherapy 2003 ;5(3): Levine BL, Ueda Y, Craighead N, et al. CD28 ligands CD80 (B7-1) and CD86 (B7-2) induce long-term autocrine growth of CD4 + T cells and induce similar patterns of cytokine secretion in vitro. Int Immunol 1995 ;7(6): Levine BL, Bernstein WB, Connors M, et al. Effects of CD28 costimulation on long-term proliferation of CD4 + T cells in the absence of exogenous feeder cells. J Immunol 1997 ;159(12): Levine BL, Mosca JD, Riley JL, et al. Antiviral effect and ex vivo CD4 + T cell proliferation in HIV- positive patients as a result of CD28 costimulation. Science 1996 ;272(5270): Carroll RG, Riley JL, Levine BL, et al. Differential regulation of HIV-1 fusion cofactor expression by CD28 costimulation of CD4 + T cells. Science 1997 ;276(5310): Renner C, Ohnesorge S, Held G, et al. T cells from patients with Hodgkin s disease have a defective T-cell receptor zeta chain expression that is reversible by T-cell stimulation with CD3 and CD28. Blood 1996 ;88(1): Bonyhadi M, Frohlich M, Rasmussen A, et al. In vitro engagement of CD3 and CD28 corrects T cell defects in chronic lymphocytic leukemia. J Immunol 2005 ;174(4): Maus MV, Thomas AK, Leonard DG, et al. Ex vivo expansion of polyclonal and antigen-specific cytotoxic T lymphocytes by artificial APCs expressing ligands for the T-cell receptor, CD28 and 4-1BB. Nat Biotechnol 2002 ;20(2): Thomas AK, Maus MV, Shalaby WS, et al. A cell-based artificial antigen-presenting cell coated with anti-cd3 and CD28 antibodies enables rapid expansion and long-term growth of CD4 T lymphocytes. Clin Immunol 2002 ;105(3): Suhoski MM, Golovina TN, Aqui NA, et al. Engineering artificial antigen-presenting cells to express a diverse array of co-stimulatory molecules. Mol Ther 2007 ;15(5):981-8 Lentivirally transduced universal aapcs for the activation and expansion of antigen-speficic and polyclonal T lymphocytes are described Smith B, Kasamon YL, Miller CB, et al. K562/GM-CSF vaccination reduces tumor burden, including achieving molecular remissions, in chronic myeloid leukemia (CML) patients (PTS) with residual disease on imatinib mesylate (IM). J Clin Oncol 2006 ;24(18S): Broeren CP, Gray GS, Carreno BM, June CH. Costimulation light: activation of CD4 + T cells with CD80 or CD86 rather than anti-cd28 leads to a Th2 cytokine profile. J Immunol 2000 ;165(12): Godfrey WR, Ge YG, Spoden DJ, et al. In vitro-expanded human CD4(+)CD25(+) T-regulatory cells can markedly inhibit allogeneic dendritic cell-stimulated MLR cultures. Blood 2004 ;104(2): Walker RE, Bechtel CM, Natarajan V, et al. Long-term in vivo survival of receptor-modified syngeneic T cells in patients with human immunodeficiency virus infection. Blood 2000 ;96(2): Levine BL, Cotte J, Small CC, et al. Large scale production of CD4 + T cells from HIV-1 infected donors following CD3/CD28 costimulation. J Hematotherapy 1998 ;7: Burger SR. Current regulatory issues in cell and tissue therapy. Cytotherapy 2003 ;5(4): Cross P, Levine BL. Assays for the release of cellular gene therapy products. In: Concepts in Genetic Medicine. 488 Expert Opin. Biol. Ther. (2008) 8(4)
15 Levine Dropulic B, Carter B, editors. Hoboken, NJ, John Wiley & Sons; Rapoport AP, Levine BL, Badros A, et al. Molecular remission of CML after autotransplantation followed by adoptive transfer of costimulated autologous T cells. Bone Marrow Transplant 2004 ;33(1): Andreadis C, Levine BL, Nasta SD, et al. Adaptive immunotherapy with autologous CD25-depleted and CD3/CD28-costimulated T-cells enhances lymphocyte recovery after cyclophosphamide fludarabine chemotherapy in patients with low-grade follicular lymphoma. Blood 2006 ;108(11): Levine BL, Bernstein WB, Aronson NE, et al. Adoptive transfer of costimulated CD4(+) T cells induces expansion of peripheral T cells and decreased CCR5 expression in HIV infection. Nat Med 2002 ;8(1): Kohn DB. Lentiviral vectors ready for prime-time. Nat Biotechnol 2007 ;25(1):65-6 Affiliation Bruce L Levine PhD The University of Pennsylvania School of Medicine, Hospital of the University of Pennsylvania, Department of Pathology and Laboratory Medicine, M6.40 Maloney, 3400 Spruce Street, Philadelphia, PA , USA Tel: ; Fax: ; LevineBL@mail.med.upenn.edu Expert Opin. Biol. Ther. (2008) 8(4) 489
16
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
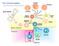 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Dendritic Cells: A Basic Review *last updated May 2003
 *last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
*last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY. Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds
 NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
Hematopoietic Stem Cell Transplantation. Imad A. Tabbara, M.D. Professor of Medicine
 Hematopoietic Stem Cell Transplantation Imad A. Tabbara, M.D. Professor of Medicine Hematopoietic Stem Cells Harvested from blood, bone marrow, umbilical cord blood Positive selection of CD34 (+) cells
Hematopoietic Stem Cell Transplantation Imad A. Tabbara, M.D. Professor of Medicine Hematopoietic Stem Cells Harvested from blood, bone marrow, umbilical cord blood Positive selection of CD34 (+) cells
2) Macrophages function to engulf and present antigen to other immune cells.
 Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials
 LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials OUR FOCUS ABOUT emerging treatments Presentation for: Judith E. Karp, MD Advancements for Acute Myelogenous Leukemia Supported by an unrestricted educational
LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials OUR FOCUS ABOUT emerging treatments Presentation for: Judith E. Karp, MD Advancements for Acute Myelogenous Leukemia Supported by an unrestricted educational
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
Making the switch to a safer CAR-T cell therapy
 Making the switch to a safer CAR-T cell therapy HaemaLogiX 2015 Technical Journal Club May 24 th 2016 Christina Müller - chimeric antigen receptor = CAR - CAR T cells are generated by lentiviral transduction
Making the switch to a safer CAR-T cell therapy HaemaLogiX 2015 Technical Journal Club May 24 th 2016 Christina Müller - chimeric antigen receptor = CAR - CAR T cells are generated by lentiviral transduction
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
2011 Update on the ECIL-3 guidelines for EBV management in patients with leukemia and other hematological disorders
 UPDATE ECIL-4 2011 2011 Update on the ECIL-3 guidelines for EBV management in patients with leukemia and other hematological disorders Jan Styczynski, Hermann Einsele, Rafael de la Camara, Catherine Cordonnier,
UPDATE ECIL-4 2011 2011 Update on the ECIL-3 guidelines for EBV management in patients with leukemia and other hematological disorders Jan Styczynski, Hermann Einsele, Rafael de la Camara, Catherine Cordonnier,
Challenges of Hematopoietic Stem Cell Transplantation. Robert J. Soiffer, MD Dana Farber Cancer Institute
 Challenges of Hematopoietic Stem Cell Transplantation Robert J. Soiffer, MD Dana Farber Cancer Institute Hematopoietic Stem Cell Transplantation Objectives Deliver sufficient chemo-radio therapy to destroy
Challenges of Hematopoietic Stem Cell Transplantation Robert J. Soiffer, MD Dana Farber Cancer Institute Hematopoietic Stem Cell Transplantation Objectives Deliver sufficient chemo-radio therapy to destroy
INFORMATION ON STEM CELLS/BONE MARROW AND REINFUSION/TRANSPLANTATION SUR703.002
 INFORMATION ON STEM CELLS/BONE MARROW AND REINFUSION/TRANSPLANTATION SUR703.002 COVERAGE: SPECIAL COMMENT ON POLICY REVIEW: Due to the complexity of the Peripheral and Bone Marrow Stem Cell Transplantation
INFORMATION ON STEM CELLS/BONE MARROW AND REINFUSION/TRANSPLANTATION SUR703.002 COVERAGE: SPECIAL COMMENT ON POLICY REVIEW: Due to the complexity of the Peripheral and Bone Marrow Stem Cell Transplantation
Blood & Marrow Transplant Glossary. Pediatric Blood and Marrow Transplant Program Patient Guide
 Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Presenter Disclosure: Renier J. Brentjens, MD, PhD. Nothing to disclose
 Presenter Disclosure: Renier J. Brentjens, MD, PhD Nothing to disclose Adoptive Therapy of Cancer with T cells Genetically Targeted to Tumor Associated Antigens through the Introduction of Chimeric Antigen
Presenter Disclosure: Renier J. Brentjens, MD, PhD Nothing to disclose Adoptive Therapy of Cancer with T cells Genetically Targeted to Tumor Associated Antigens through the Introduction of Chimeric Antigen
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
Activation and effector functions of HMI
 Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
A Genetic Analysis of Rheumatoid Arthritis
 A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_epithelial_ovarian_cancer 2/2001 11/2015 11/2016 11/2015 Description
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_epithelial_ovarian_cancer 2/2001 11/2015 11/2016 11/2015 Description
Chimeric Antigen Receptor T Cell Therapy
 Chimeric Antigen Receptor T Cell Therapy Yi Lin, MD, PhD Mayo Clinic, Rochester, MN Alliance Spring Group Meeting - May 13, 2016 Presentation Objectives l Scientific overview of chimeric antigen receptor
Chimeric Antigen Receptor T Cell Therapy Yi Lin, MD, PhD Mayo Clinic, Rochester, MN Alliance Spring Group Meeting - May 13, 2016 Presentation Objectives l Scientific overview of chimeric antigen receptor
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
B cell activation and Humoral Immunity
 B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center
 Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Chapter 43: The Immune System
 Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Update in Hematology Oncology Targeted Therapies. Mark Holguin
 Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
Oncos Therapeutics: ONCOS THERAPEUTICS Personalized Cancer Immunotherapy. March 2015. Antti Vuolanto, COO and co-founder
 Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation
 Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation Dr Ros Ganderton, Ms Kate Parratt, Dr Debbie Richardson, Dr Kim Orchard and Dr Liz Hodges Departments of Molecular Pathology
Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation Dr Ros Ganderton, Ms Kate Parratt, Dr Debbie Richardson, Dr Kim Orchard and Dr Liz Hodges Departments of Molecular Pathology
Human CD4+T Cell Care Manual
 Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
The Four Pillars of Cancer Therapy
 Improving the Overall Understanding of Immunotherapy in Multiple Myeloma Webinar 2, August 19, 2015 Myeloma Vaccines: A New Use of a Time-Tested Treatment The Four Pillars of Cancer Therapy Surgery Radiation
Improving the Overall Understanding of Immunotherapy in Multiple Myeloma Webinar 2, August 19, 2015 Myeloma Vaccines: A New Use of a Time-Tested Treatment The Four Pillars of Cancer Therapy Surgery Radiation
B Cell Generation, Activation & Differentiation. B cell maturation
 B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
Stem Cell Transplantation
 Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Disclosure. Gene Therapy. Transfer of genes into cells Expression of transferred genes
 Disclosure Equity interest in Genetix Pharm. Inc. Exclusive license of retroviral cell lines from Columbia No direct participation in MDR clinical trials Columbia U. annual reporting FDA Gene Therapy Transfer
Disclosure Equity interest in Genetix Pharm. Inc. Exclusive license of retroviral cell lines from Columbia No direct participation in MDR clinical trials Columbia U. annual reporting FDA Gene Therapy Transfer
HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES JASON CYSTER SECTION 13
 SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
Bottle-neck Problems of Current Human Cancer Therapy
 International Conference on Human Cell, Tissue-based Products and Tissue Banks, Oct. 13-14,Taipei, Taiwan Autologous Dendritic Cell-based Immunotherapy of Glioblastoma Multiforme: Post-Phase-I Clinical
International Conference on Human Cell, Tissue-based Products and Tissue Banks, Oct. 13-14,Taipei, Taiwan Autologous Dendritic Cell-based Immunotherapy of Glioblastoma Multiforme: Post-Phase-I Clinical
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Bone Marrow Transplantation and Peripheral Blood Stem Cell Transplantation: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Bone Marrow Transplantation
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Bone Marrow Transplantation
This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking
 Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
DEPARTMENT OF BONE MARROW AND STEM CELL TRANSPLANT
 www.narayanahealth.org DEPARTMENT OF BONE MARROW AND STEM CELL TRANSPLANT About Narayana Health City Narayana Health, one of India's largest and the world's most economical healthcare service providers
www.narayanahealth.org DEPARTMENT OF BONE MARROW AND STEM CELL TRANSPLANT About Narayana Health City Narayana Health, one of India's largest and the world's most economical healthcare service providers
Blood-Forming Stem Cell Transplants
 Blood-Forming Stem Cell Transplants What are bone marrow and hematopoietic stem cells? Bone marrow is the soft, sponge-like material found inside bones. It contains immature cells known as hematopoietic
Blood-Forming Stem Cell Transplants What are bone marrow and hematopoietic stem cells? Bone marrow is the soft, sponge-like material found inside bones. It contains immature cells known as hematopoietic
Autologous Cellular Therapies. Adrian Gee Center for Cell & Gene Therapy Baylor College of Medicine Production Assistance for Cellular Therapy (PACT)
 Autologous Cellular Therapies Adrian Gee Center for Cell & Gene Therapy Baylor College of Medicine Production Assistance for Cellular Therapy (PACT) Autologous Cellular Therapies Definition Advantages
Autologous Cellular Therapies Adrian Gee Center for Cell & Gene Therapy Baylor College of Medicine Production Assistance for Cellular Therapy (PACT) Autologous Cellular Therapies Definition Advantages
One of the most important recent developments in cancer treatment has been the ability to harvest stem
 BIOTECHNOLOGY A Patient-Friendly Approach to Human Cell Transplantation One of the most important recent developments in cancer treatment has been the ability to harvest stem cells from bone marrow or
BIOTECHNOLOGY A Patient-Friendly Approach to Human Cell Transplantation One of the most important recent developments in cancer treatment has been the ability to harvest stem cells from bone marrow or
What is a Stem Cell Transplantation?
 What is a Stem Cell Transplantation? Guest Expert: Stuart, MD Associate Professor, Medical Oncology www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with Drs. Ed and Ken. I am
What is a Stem Cell Transplantation? Guest Expert: Stuart, MD Associate Professor, Medical Oncology www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with Drs. Ed and Ken. I am
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Evaluation of Medicines for Human Use London, 10 October 2007 Doc. Ref. COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON POTENCY TESTING OF CELL BASED IMMUNOTHERAPY
European Medicines Agency Evaluation of Medicines for Human Use London, 10 October 2007 Doc. Ref. COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON POTENCY TESTING OF CELL BASED IMMUNOTHERAPY
The Body s Defenses CHAPTER 24
 CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
Cytoreductive Therapy for Autologous Cell Therapy in HIV
 Cytoreductive Therapy for Autologous Cell Therapy in HIV Ronald Mitsuyasu, MD Professor of Medicine UCLA Center for Clinical AIDS Research and Education (CARE Center) HSC Transfer from CCR5-delta 32 Donor
Cytoreductive Therapy for Autologous Cell Therapy in HIV Ronald Mitsuyasu, MD Professor of Medicine UCLA Center for Clinical AIDS Research and Education (CARE Center) HSC Transfer from CCR5-delta 32 Donor
An overview of CLL care and treatment. Dr Dean Smith Haematology Consultant City Hospital Nottingham
 An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
THE INFLUENCE OF TISSUE (IN)COMPATIBILITY IN UMBILICAL CORD BLOOD TRANSPLANTATION
 THE INFLUENCE OF TISSUE (IN)COMPATIBILITY IN UMBILICAL CORD BLOOD TRANSPLANTATION Matjaž Jeras Blood Transfusion Centre of Slovenia Tissue Typing Center Šlajmerjeva 6, 1000 Ljubljana, Slovenia matjaz.jeras@ztm.si
THE INFLUENCE OF TISSUE (IN)COMPATIBILITY IN UMBILICAL CORD BLOOD TRANSPLANTATION Matjaž Jeras Blood Transfusion Centre of Slovenia Tissue Typing Center Šlajmerjeva 6, 1000 Ljubljana, Slovenia matjaz.jeras@ztm.si
How To Follow Up After Treatment With Gene Therapy
 European Medicines Agency London, 30 May 2008 Doc. Ref. EMEA/CHMP/GTWP/60436/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) DRAFT GUIDELINE ON FOLLOW-UP OF PATIENTS ADMINISTERED WITH GENE THERAPY
European Medicines Agency London, 30 May 2008 Doc. Ref. EMEA/CHMP/GTWP/60436/2007 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) DRAFT GUIDELINE ON FOLLOW-UP OF PATIENTS ADMINISTERED WITH GENE THERAPY
Uses of Flow Cytometry
 Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
STEM CELL TRANSPLANTS
 UAMS Information on STEM CELL TRANSPLANTS What is a Stem Cell Transplant? A stem cell transplant is an infusion of stem cells following high-dose chemotherapy. The infused cells effectively rescue the
UAMS Information on STEM CELL TRANSPLANTS What is a Stem Cell Transplant? A stem cell transplant is an infusion of stem cells following high-dose chemotherapy. The infused cells effectively rescue the
Pros and Cons of Stem Cell Sources and their availability in Africa. Dr Jaimendra Singh Inkosi Albert Luthuli Central Hospital Durban, South Africa
 Pros and Cons of Stem Cell Sources and their availability in Africa Dr Jaimendra Singh Inkosi Albert Luthuli Central Hospital Durban, South Africa Introduction The ability to perform a haematopoietic stem
Pros and Cons of Stem Cell Sources and their availability in Africa Dr Jaimendra Singh Inkosi Albert Luthuli Central Hospital Durban, South Africa Introduction The ability to perform a haematopoietic stem
MAB Solut. MABSolys Génopole Campus 1 5 rue Henri Desbruères 91030 Evry Cedex. www.mabsolut.com. is involved at each stage of your project
 Mabsolus-2015-UK:Mise en page 1 03/07/15 14:13 Page1 Services provider Department of MABSolys from conception to validation MAB Solut is involved at each stage of your project Creation of antibodies Production
Mabsolus-2015-UK:Mise en page 1 03/07/15 14:13 Page1 Services provider Department of MABSolys from conception to validation MAB Solut is involved at each stage of your project Creation of antibodies Production
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: immune_cell_function_assay 11/2009 3/2016 3/2017 3/2016 Description of Procedure or Service Careful monitoring
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: immune_cell_function_assay 11/2009 3/2016 3/2017 3/2016 Description of Procedure or Service Careful monitoring
FDA Perspective on the Regulation of TCR/CAR T-cell Products
 FDA Perspective on the Regulation of TCR/CAR T-cell Products Raj K. Puri, M.D., Ph.D. Director, Division of Cellular and Gene Therapies, FDA, CBER CIMT2014 Talk (by Phone) Date: May 8, 2014 Time: 12:30
FDA Perspective on the Regulation of TCR/CAR T-cell Products Raj K. Puri, M.D., Ph.D. Director, Division of Cellular and Gene Therapies, FDA, CBER CIMT2014 Talk (by Phone) Date: May 8, 2014 Time: 12:30
Modelling and analysis of T-cell epitope screening data.
 Modelling and analysis of T-cell epitope screening data. Tim Beißbarth 2, Jason A. Tye-Din 1, Gordon K. Smyth 1, Robert P. Anderson 1 and Terence P. Speed 1 1 WEHI, 1G Royal Parade, Parkville, VIC 3050,
Modelling and analysis of T-cell epitope screening data. Tim Beißbarth 2, Jason A. Tye-Din 1, Gordon K. Smyth 1, Robert P. Anderson 1 and Terence P. Speed 1 1 WEHI, 1G Royal Parade, Parkville, VIC 3050,
Project Lead: Stephen Forman, M.D. PI: Elizabeth Budde, M.D., Ph.D
 Phase I study using T cells expressing a CD123-specific chimeric antigen receptor and truncated EGFR for patients with relapsed or refractory acute myeloid leukemia Project Lead: Stephen Forman, M.D. PI:
Phase I study using T cells expressing a CD123-specific chimeric antigen receptor and truncated EGFR for patients with relapsed or refractory acute myeloid leukemia Project Lead: Stephen Forman, M.D. PI:
Immune Checkpoint Blockade in Acute Myeloid Leukemia. Kinsey McCormick Hematology Fellow s Conference January 10, 2014
 Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
Overview of Phase 1 Oncology Trials of Biologic Therapeutics
 Overview of Phase 1 Oncology Trials of Biologic Therapeutics Susan Jerian, MD ONCORD, Inc. February 28, 2008 February 28, 2008 Phase 1 1 Assumptions and Ground Rules The goal is regulatory approval of
Overview of Phase 1 Oncology Trials of Biologic Therapeutics Susan Jerian, MD ONCORD, Inc. February 28, 2008 February 28, 2008 Phase 1 1 Assumptions and Ground Rules The goal is regulatory approval of
Chapter 3. Immunity and how vaccines work
 Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma
 On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma
 Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
CPT Codes for Bone Marrow Transplant January 2015 James L. Gajewski, MD
 The blood and marrow transplant field has 15 dedicated CPT codes. These CPT codes can be categorized into three groups: 1. Collection Codes 2. Cell Processing Codes 3. Cell Infusion Codes Collection Codes
The blood and marrow transplant field has 15 dedicated CPT codes. These CPT codes can be categorized into three groups: 1. Collection Codes 2. Cell Processing Codes 3. Cell Infusion Codes Collection Codes
Adoptive cell transfer: a clinical path to effective cancer immunotherapy
 Adoptive cell transfer: a clinical path to effective cancer immunotherapy Steven A. Rosenberg, Nicholas P. Restifo, James C. Yang, Richard A. Morgan and Mark E. Dudley Abstract Adoptive cell therapy (ACT)
Adoptive cell transfer: a clinical path to effective cancer immunotherapy Steven A. Rosenberg, Nicholas P. Restifo, James C. Yang, Richard A. Morgan and Mark E. Dudley Abstract Adoptive cell therapy (ACT)
Lymphomas after organ transplantation
 Produced 21.03.2011 Revision due 21.03.2011 Lymphomas after organ transplantation People who have undergone an organ transplant are more at risk of developing lymphoma known as post-transplant lymphoproliferative
Produced 21.03.2011 Revision due 21.03.2011 Lymphomas after organ transplantation People who have undergone an organ transplant are more at risk of developing lymphoma known as post-transplant lymphoproliferative
A Letter from MabVax Therapeutics President and Chief Executive Officer
 A Letter from MabVax Therapeutics President and Chief Executive Officer Dear Fellow Stockholder: You have invested in MabVax Therapeutics because you share our passion for finding new therapies for the
A Letter from MabVax Therapeutics President and Chief Executive Officer Dear Fellow Stockholder: You have invested in MabVax Therapeutics because you share our passion for finding new therapies for the
Core Topic 2. The immune system and how vaccines work
 Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
OKT3. ~ The first mouse monoclonal antibody. used in clinical practice in the field of transplantation ~
 g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
LESSON 3.5 WORKBOOK. How do cancer cells evolve? Workbook Lesson 3.5
 LESSON 3.5 WORKBOOK How do cancer cells evolve? In this unit we have learned how normal cells can be transformed so that they stop behaving as part of a tissue community and become unresponsive to regulation.
LESSON 3.5 WORKBOOK How do cancer cells evolve? In this unit we have learned how normal cells can be transformed so that they stop behaving as part of a tissue community and become unresponsive to regulation.
Infosheet. Allogeneic stem cell transplantation in myeloma. What is the principle behind stem cell transplantation?
 Infosheet Allogeneic stem cell transplantation in myeloma High-dose therapy and autologous stem cell transplantation is currently the first-line treatment standard of care for younger/fitter myeloma patients.
Infosheet Allogeneic stem cell transplantation in myeloma High-dose therapy and autologous stem cell transplantation is currently the first-line treatment standard of care for younger/fitter myeloma patients.
Introduction. About 10,500 new cases of acute myelogenous leukemia are diagnosed each
 Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
Pr Eliane Gluckman, MD, FRCP, Disclosure of Interest: Nothing to Disclose
 Pr Eliane Gluckman, MD, FRCP, Hospital Saint Louis, University Paris- Diderot, France Should Haplo-identical transplantation be preferred to cord blood in patients without a matched donor? Disclosure of
Pr Eliane Gluckman, MD, FRCP, Hospital Saint Louis, University Paris- Diderot, France Should Haplo-identical transplantation be preferred to cord blood in patients without a matched donor? Disclosure of
Outline of thesis and future perspectives.
 Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
T Cell Immunotherapy for Cancer
 T Cell Immunotherapy for Cancer Chimeric Antigen Receptors Targeting Tag-72 Glycoprotein for Colorectal Cancer Mitchell H. Finer Ph.D Genetix Pharmaceuticals Inc Work Completed at Cell Genesys Inc T Cell
T Cell Immunotherapy for Cancer Chimeric Antigen Receptors Targeting Tag-72 Glycoprotein for Colorectal Cancer Mitchell H. Finer Ph.D Genetix Pharmaceuticals Inc Work Completed at Cell Genesys Inc T Cell
Understanding How Existing and Emerging MS Therapies Work
 Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
MULTIPLE MYELOMA. Dr Malkit S Riyat. MBChB, FRCPath(UK) Consultant Haematologist
 MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
MEDICAL BREAKTHROUGHS RESEARCH SUMMARY
 MEDICAL BREAKTHROUGHS RESEARCH SUMMARY TOPIC: Training the Body to Fight Melanoma REPORT: 3823 BACKGROUND: Melanoma is the most dangerous form of skin cancer that can be hard to treat and fatal if not
MEDICAL BREAKTHROUGHS RESEARCH SUMMARY TOPIC: Training the Body to Fight Melanoma REPORT: 3823 BACKGROUND: Melanoma is the most dangerous form of skin cancer that can be hard to treat and fatal if not
The role of IBV proteins in protection: cellular immune responses. COST meeting WG2 + WG3 Budapest, Hungary, 2015
 The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
BioMmune Technologies Inc. Corporate Presentation 2015
 BioMmune Technologies Inc Corporate Presentation 2015 * Harnessing the body s own immune system to fight cancer & other autoimmune diseases BioMmune Technologies Inc. (IMU) ABOUT A public biopharmaceutical
BioMmune Technologies Inc Corporate Presentation 2015 * Harnessing the body s own immune system to fight cancer & other autoimmune diseases BioMmune Technologies Inc. (IMU) ABOUT A public biopharmaceutical
Stem Cell Quick Guide: Stem Cell Basics
 Stem Cell Quick Guide: Stem Cell Basics What is a Stem Cell? Stem cells are the starting point from which the rest of the body grows. The adult human body is made up of hundreds of millions of different
Stem Cell Quick Guide: Stem Cell Basics What is a Stem Cell? Stem cells are the starting point from which the rest of the body grows. The adult human body is made up of hundreds of millions of different
Potency Assays for an Autologous Active Immunotherapy (Sipuleucel-T) Pocheng Liu, Ph.D. Senior Scientist of Product Development Dendreon Corporation
 Potency Assays for an Autologous Active Immunotherapy (Sipuleucel-T) Pocheng Liu, Ph.D. Senior Scientist of Product Development Dendreon Corporation Sipuleucel-T Manufacturing Process Day 1 Leukapheresis
Potency Assays for an Autologous Active Immunotherapy (Sipuleucel-T) Pocheng Liu, Ph.D. Senior Scientist of Product Development Dendreon Corporation Sipuleucel-T Manufacturing Process Day 1 Leukapheresis
Immuno-Oncology Therapies to Treat Lung Cancer
 Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
4. All cord blood banks should be subject to the same standards, regulations and accreditation requirements.
 WMDA Policy Statement on the Utility of Autologous or Family Cord Blood Unit Storage The WMDA Board adopted this policy on 25 th of May 2006. Policy updated _April 2011 The Cord Blood Working Group and
WMDA Policy Statement on the Utility of Autologous or Family Cord Blood Unit Storage The WMDA Board adopted this policy on 25 th of May 2006. Policy updated _April 2011 The Cord Blood Working Group and
CHAPTER 6: RECOMBINANT DNA TECHNOLOGY YEAR III PHARM.D DR. V. CHITRA
 CHAPTER 6: RECOMBINANT DNA TECHNOLOGY YEAR III PHARM.D DR. V. CHITRA INTRODUCTION DNA : DNA is deoxyribose nucleic acid. It is made up of a base consisting of sugar, phosphate and one nitrogen base.the
CHAPTER 6: RECOMBINANT DNA TECHNOLOGY YEAR III PHARM.D DR. V. CHITRA INTRODUCTION DNA : DNA is deoxyribose nucleic acid. It is made up of a base consisting of sugar, phosphate and one nitrogen base.the
ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES
 ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES DESCRIPTION OF GRANT MECHANISM The Alliance for Lupus Research (ALR) is an independent,
ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES DESCRIPTION OF GRANT MECHANISM The Alliance for Lupus Research (ALR) is an independent,
Drug Development Services
 Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
5 Frequently Asked Questions About Adult Stem Cell Research
 5 Frequently Asked Questions About Adult Stem Cell Research Stem cells are often referred to in the sociopolitical realm with some level of controversy and beyond that, some level of confusion. Many researchers
5 Frequently Asked Questions About Adult Stem Cell Research Stem cells are often referred to in the sociopolitical realm with some level of controversy and beyond that, some level of confusion. Many researchers
Epstein-Barr Virus (EBV) complications following HSCT: from viremia to post transplant lymphoproliferative disease (PTLD) and lymphoma
 Epstein-arr Virus (EV) complications following HSCT: from viremia to post transplant lymphoproliferative p disease (PTLD) and lymphoma Laurie A. Milner, MD Associate Professor, Pediatric Hematology / Oncology
Epstein-arr Virus (EV) complications following HSCT: from viremia to post transplant lymphoproliferative p disease (PTLD) and lymphoma Laurie A. Milner, MD Associate Professor, Pediatric Hematology / Oncology
CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy
 CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy Joseph M. Tuscano, Jason Kato, David Pearson, Chengyi Xiong, Laura Newell, Yunpeng Ma, David R. Gandara,
CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy Joseph M. Tuscano, Jason Kato, David Pearson, Chengyi Xiong, Laura Newell, Yunpeng Ma, David R. Gandara,
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Hemophilia Care. Will there always be new people in the world with hemophilia? Will hemophilia be treated more effectively and safely in the future?
 Future of This chapter provides answers to these questions: Will there always be new people in the world with hemophilia? Will hemophilia be treated more effectively and safely in the future? Will the
Future of This chapter provides answers to these questions: Will there always be new people in the world with hemophilia? Will hemophilia be treated more effectively and safely in the future? Will the
Hematopoietic Stem Cell Transplantation: Evolving Strategies That Have Resulted in Improved Outcomes
 Hematopoietic Stem Cell Transplantation: Evolving Strategies That Have Resulted in Improved Outcomes Asad Bashey, MD, PhD Blood and Marrow Transplantation Program at Northside Hospital Atlanta, Georgia
Hematopoietic Stem Cell Transplantation: Evolving Strategies That Have Resulted in Improved Outcomes Asad Bashey, MD, PhD Blood and Marrow Transplantation Program at Northside Hospital Atlanta, Georgia
Gene Therapy. The use of DNA as a drug. Edited by Gavin Brooks. BPharm, PhD, MRPharmS (PP) Pharmaceutical Press
 Gene Therapy The use of DNA as a drug Edited by Gavin Brooks BPharm, PhD, MRPharmS (PP) Pharmaceutical Press Contents Preface xiii Acknowledgements xv About the editor xvi Contributors xvii An introduction
Gene Therapy The use of DNA as a drug Edited by Gavin Brooks BPharm, PhD, MRPharmS (PP) Pharmaceutical Press Contents Preface xiii Acknowledgements xv About the editor xvi Contributors xvii An introduction
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
CLINICAL TRIALS SHOULD YOU PARTICIPATE? by Gwen L. Nichols, MD
 CLINICAL TRIALS SHOULD YOU PARTICIPATE? by Gwen L. Nichols, MD Gwen L. Nichols, M.D., is currently the Oncology Site Head of the Roche Translational Clinical Research Center at Hoffman- LaRoche. In this
CLINICAL TRIALS SHOULD YOU PARTICIPATE? by Gwen L. Nichols, MD Gwen L. Nichols, M.D., is currently the Oncology Site Head of the Roche Translational Clinical Research Center at Hoffman- LaRoche. In this
HemaCare Corporation Company Overview. Comprehensive Product and Service Solutions for BioResearch and Cellular Therapy
 HemaCare Corporation Company Overview Comprehensive Product and Service Solutions for BioResearch and Cellular Therapy 2015 HemaCare Corporation Leading provider of apheresis products, human blood cells,
HemaCare Corporation Company Overview Comprehensive Product and Service Solutions for BioResearch and Cellular Therapy 2015 HemaCare Corporation Leading provider of apheresis products, human blood cells,
