RADICAL PROSTATECTOMY USING DAVINCI ROBOTIC SYSTEM HARTFORD HOSPITAL, HARTFORD, CT Broadcast May 17, 2004
|
|
|
- Stephanie Fisher
- 7 years ago
- Views:
Transcription
1 RADICAL PROSTATECTOMY USING DAVINCI ROBOTIC SYSTEM HARTFORD HOSPITAL, HARTFORD, CT Broadcast May 17, 2004 NARRATOR Prostate cancer is the most common type of cancer, excluding skin cancer, among American men. At Hartford Hospital in Hartford, CT, a revolutionary new surgical technique is bringing hope to prostate cancer patients. Hospital surgeons are performing radical prostatectomy using the DaVinci laparoscopic robotic system. The DaVinci has a three-dimensional camera so when I m sitting at the console, I m getting two different images through the telescope, to each of my eyes, so that threedimensional image means I m not struggling to determine how far away something is. That s advantage #1. Advantage #2 is that the instruments have all the range of motion of my hands. NARRATOR Until recently, surgeons performed prostatectomies in traditional open surgery, but today, advances in minimally invasive procedures are making prostate cancer treatment easier for surgeons and patients. You are about to see a radical prostatectomy by robotic surgery at Hartford Hospital in Hartford, CT. During today s presentation, you may send questions to the faculty at any time by clicking the button below. Hello and welcome. I m Dr. Vincent Laudone, urologic surgeon at Hartford Hospital. It is my privilege today to welcome you to Hartford, where we are going to witness a live video webcast of a surgical procedure utilizing the DaVinci surgical robot. The procedure we will be seeing involves the removal of a prostate in a man with prostate cancer. The operation will be performed by my partners, Dr. Joseph Wagner and Dr. Steven Schichman. We will now go to the operating room to talk with Dr. Wagner. Thanks, Vin. The first thing I d like to do is I d like to thank our patient and his family for graciously allowing us to webcast this procedure. I d also like to now take the
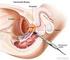
2 opportunity to introduce our operating room staff. We have Beth and Sue as the circulating and scrub nurses, Dr. Raman and Dr. Parsh as our anesthesia team, and next I d like to turn the microphone over to Dr. Schichman, who is assisting me on the patient s side. Good evening and welcome to Hartford Hospital. We hope you will enjoy viewing this surgery. Please contact us by if you have any questions regarding the procedure. We re going to try to explain step by step what you re seeing and we hope you enjoy yourself. Vin, back to you. Thank you, Dr. Schichman. I d like to tell you a little bit about the patient we re operating on tonight. This is a 54-year-old gentleman who was found to have an elevation in a blood test called the PSA, which stands for prostate-specific antigen. The PSA is a blood test that we utilize now as the primary method for detecting the presence of prostate cancer. This patient s PSA was slightly elevated at 5.8, with normal being anywhere from 0 to 4. As a result of this, he underwent a transrectal ultrasound of the prostate with biopsy of the prostate. The biopsies on pathologic examination revealed a Gleason grade 6 prostate cancer involving two out of eight biopsy specimens. Now, perhaps we ll go back to the operating room and Dr. Wagner can fill us in on where he is in the procedure. This procedure did begin a while ago and he is partway through it. Dr. Wagner. Right now we re doing the posterior dissection, so we re still early on in the procedure. We started minutes ago. This patient had some adhesions of his sigmoid colon to his abdominal wall, which had to be taken down first, and then we ve incised his peritoneum posteriorly to expose his seminal vesicles and vasa. These are one of the seminal vesicles here that I m dissecting off. I m holding the tip in this area. What we can see here is Dr. Wagner is at the surgical console and is manipulating the robot. Now we re seeing a live picture from inside the patient. This is the view that Dr. Wagner gets, as well as Dr. Schichman, who is the first assistant. Down here, this very white shiny area is called Denonvilliers fascia. Below that is the rectum and perirectal fat. To the side here are some blood vessels that are coming into the prostate. Probably in this area is what are termed the neurovascular bundles. Those are the blood vessels that go down to the penis to cause erections, so I m being very careful
3 now, as I dissect, to stay on the seminal vesicle and away from this outer area, where the blood vessels lie. What we re actually doing here is working behind the bladder. We re lifting the bladder up and going behind the bladder and on top of the rectum to dissect out the seminal vesicles. As Dr. Wagner said, this is the posterior portion of the dissection. Once we finish this part of the dissection, we re going to drop the bladder back down and get to the prostate from an anterior approach. Perhaps I can explain a little bit of this using a model that I have up front. This is a model of a male pelvis. What we see here is the urinary bladder, cut open, and right below the urinary bladder is the prostate gland. When a man urinates, the bladder here contracts and the urine is forced through the middle of the prostate and then into the urethra and out the penis. This here is the prostate gland and this is what Drs. Wagner and Schichman will be removing tonight. In addition, there are two structures that are attached to the back of the prostate, called the seminal vesicles, and these structures will be removed along with the prostate gland. Now, the approach that you were just looking at is coming in from this direction, behind the bladder, between the bladder, which is here, and the rectum, here. They are dissecting down in this direction, having just exposed the seminal vesicle here, behind the bladder, and are now working their way down here, along, on top of the rectum, underneath the prostate, in order to separate the seminal vesicle and prostate from the rectum. What I ve done now, Vin, is I ve gotten a layer. This is Denonvilliers fascia. This is the perirectal fat down below. What I ve done is I ve incised sort of in between the two layers of Denonvilliers fascia. I m in between those two layers. One of the thing you might want to explain a little bit more, Vin, as we watch the instruments work, if you see the instrument coming in from the right side of the screen, you ll see a nice reticulating wrist where the end of the instrument can twist and turn at the same time. That s really what we call reticulation. That allows Dr. Wagner to move the tip of the instrument just as he would move his hands or fingers. The same thing applies for the left instrument, which you ll see working right now. Now, that s a great advantage compared to what you see me controlling right here, the suction apparatus in the middle of the screen, where the tip of it doesn t twist or turn. You can have the tip of the laparoscopic instrument with a mechanism at the end which can open or close or cut, but we typically weren t able to twist and turn, as we can do with the DaVinci robot.
4 Perhaps this would be a good time to take a look at some slides which explain exactly the different components to the robot. The robot is comprised of three main components. The first one is what s termed the surgical cart, which is actually what we refer to as the robot itself. It is a multi-armed instrument. It can have two or three arms holding instruments and a third arm or fourth arm that will control the camera. The surgeon himself sits in what is called the surgical console and we re seeing the hands of Dr. Wagner within that surgical console, manipulating a couple of mechanical arms which are directly linked to the robot. Any movement that he makes is translated exactly to the robot. The robot does not act independently. It only does what Dr. Wagner has it do. The third component is the visual system. This is a complex three-dimensional visual system which allows Dr. Wagner to have a magnified, close-up view of the operating field that we see here, and it s in three dimensions, which differs from laparoscopic surgery. The reason it s in three dimensions is because there s actually two cameras within the robotic arm that s holding the camera. They re separated similar to how two eyes would be separated, allowing for the stereoscopic vision to occur. We just want to show you what we re doing now, before we move to the next step. What we ve done is, these are the seminal vesicles and vasa raised up. Again, you can see rectum down low with fat. This is Denonvilliers fascia. We found a plane in between the two layers of Denonvilliers and then I ve spread all the way down to the apex of the prostate. That afterwards, when we cut the bladder neck, will give us a good plane between the prostate and the posterior leaf of Denonvilliers. Letting this drop, these are the two vasa that carry the sperm from the testicles to the prostate. On either side are the two seminal vesicles that make a lot of the fluid that comes out when men ejaculate or orgasm. So the next step of the operation is that I m going to back up my telescope and we re going to look anteriorly and start to do what we call the anterior dissection. Vin, if you can explain the two-dimensional view that everyone has as compared to the three-dimensional view that Dr. Wagner is seeing. Actually, the image that we re watching on the TV screen is a two-dimensional image, as opposed to what Dr. Wagner is actually seeing within the surround type video console that he is sitting. Because he has a three-dimensional image, he is able to pick up depth perception much better than we can with the two-dimensional image that we re seeing on the standard TV screen. That is one of the major advantages of the robot over laparoscopic surgery, which still uses a two-dimensional visual image system.
5 So what I m doing right now is I m cutting the peritoneum on either side of what s called the medial umbilical ligament, which are the obliterated umbilical arteries. I m doing that all the way down. This is very good anatomy because he is a thin patient. This is his vas deferens, which is going down toward his groin. This is his external iliac artery. You see the vas deferens crossing that. Then his ureter is somewhere probably back in here, crossing his vessels and going down to the bladder, well out of harm s way. So now I m just doing to cut his peritoneum straight across and what we re looking for is this fluffy tissue, in this area, is exactly what we want to see. That tells me I m in the correct plane. Perhaps I could show a few more slides of the robot itself. This is a closer view of the actual robot, with its multiple arms. This gets wheeled up to the patient and the instruments are inserted through small openings which are called ports. If we look at the surgical picture now, we can see one of the ports in the upper corner, the plastic tube cut at an angle. Through that port is where the instruments that the robot is holding are inserted. Again, please feel free to any questions that you might have. We look forward to trying to answer them. Now I m on the left hand side. I m cutting the peritoneum The second component to the robot is this console which we ve seen Dr. Wagner working in. It is both a media console and also a control console for the robotic arms. The arms are controlled by hand controls and also foot controls, so it s a lot like playing an organ, where you re using both your hands and feet to create the music. The third and final component of the robot is this three-dimensional video system, which has two cameras allowing for a three-dimensional natural but magnified, highly magnified, image. That s one of the main advantages to robotic surgery, the ability to magnify the image. That camera can be zoomed in and out and moved left to right by the foot and hand controls that Dr. Wagner is manipulating. One of the questions that patients commonly ask is can you see as well what you re working on when you re performing laparoscopic surgery as you can when you re performing open surgery? Just to reinforce what Dr. Laudone was just speaking about, we can actually see the tissues much better when we perform laparoscopic surgery,
6 especially robotic surgery, due to both the magnification and the three dimensions. One of the questions people always ask is how can you see with all that blood there? You can also see quite plainly here that if you re in the right dissection plane, where you want to separate tissues in their natural dissection plane, there really isn t that much bleeding, if any at all. What Dr. Wagner s right hand is controlling is a little electrocautery blade that cauterizes the tissues as he pulls through it. There s a foot control that sends an electrical current to the tip of that instrument you see just to the right of center, going through the tissue right now, so that cautery will help stop any small bleeding vessels or cauterize these vessels, instead of just cutting through them with a sharp object. Steve, perhaps you could elaborate a little bit as to what the role of the first assistant is. Well, if you have a good surgeon, not much, right Dr. Wagner? No, it depends on the surgical case. I m going to be responsible for changing any instruments on the surgical arms. You ll see that we will change the instruments that Dr. Wagner is working with. Also I have to just hold the tissues in the proper orientation so he can dissect through them in the correct planes. I m operating with two instruments. One is a grasper, which you see to the right here that I m wiggling around, and one you can t see, which is a suction I m just bringing in for a second, that I push and pull tissue with. Also I m sucking smoke or any little blood that comes up. And then I m another pair of eyes. A good first assistant helps guide the surgeon. Dr. Wagner is very focused on the tissue that he s cutting through and I help look at the big picture and make sure there s nothing going astray or he s not going astray or some other areas or issues we should be working on. Anatomy-wise, this is the pubic bone. There s a little tubercle on here that sore of marks the center, so I know I m in the middle. Now I m going to take down some of this fat that s on either side of the prostate. Perhaps we can take a look at the model that I have and explain where we are in the surgical procedure. Initially we were dissecting behind the bladder to get the vas deferens and the seminal vesicles, between the bladder and the rectum. Now Dr. Wagner has switched to the other side of the prostate and is coming in in front of the bladder, behind the pubic bone, and is trying to develop this plane of dissection that will bring him between the bladder and the pubic bone, right down on top of the prostate, in the front. So the idea is to free the prostate up from the back, free it up from the front, and then next work around each side until eventually the entire prostate is freed.
7 So here, Vin, I ve isolated the endopelvic fascia on the left hand side. This bulge in the middle is the catheter balloon. I still have a little bit of extra fat in here that I m going to have to take care of eventually, but I d like to see the anatomy on the other side first. Again I remind everyone to . I have a couple of s already. One has to do with the cost of the procedure relative to doing the surgery by other techniques, such as the traditional open, or a laparoscopic approach. That question is a bit complicated because costs of surgical procedures have many factors, not only costs due to the instruments that are involved, costs due to the time in the operating room, and then the time that the patient spends in the hospital. Clearly the robot is not an inexpensive instrument and there are certain disposable pieces that are used for every case. That increases costs. If the time of the operation with the robot is a little longer than perhaps doing it by the standard technique, that also can increase costs. However, if the patient can get out of the hospital a day earlier or use less medication in the postoperative period, that decreases costs, so there are pluses and minuses when we look at it from an economic perspective. From a patient s perspective, in terms of the economics, if he can get back to work sooner, that obviously has a positive benefit for him. Real detailed cost analyses have suggested that the costs of the robot procedure can be brought down to be quite similar to that of a traditional open surgical prostatectomy. One of the most important costs is of the lost time from work and time of convalescence. In some very good prospective studies, they have shown that there s no question that the initial capital cost of minimally invasive surgery is higher with regard to the instrumentation, but once you get the operative times down to their equivalent open procedures, the savings are dramatic once you factor in the decreased time of convalescence. So right now what I m going is taking down what we term the periprostatic fat. You can see I ve sort of slowed down a bit, compared to the pace I was operating before. There are some veins in here called the superficial dorsal veins. What I m doing is dissecting those off carefully and cauterizing using electrical current to stop the bleeding as I cut through these. These can be sort of pesky, annoying bleeding if you don t control them early. Can you comment on the degree of magnification that your image affords?
8 Sure. The camera itself has 10 times the magnification of my naked eye. In addition, I can put it a few mm away from what I m operating on, so right now my estimate would be that my camera is probably on the order of 3-4 cm or a couple of inches away from what I m operating on. Obviously I can t do that with open surgery, just because of sterility. I can t stick my head inside the wound, right up against what I m operating on, so this really does give an unparalleled view, I think, surgically. Let s take one moment and just zoom in on that tissue as far as you can, just go in so people can appreciate. You can see how close he can get in. Actually, right here you see two veins. Those are the dorsal veins of the prostate. That s the main blood return from the penis. I m going to refocus now. You can see the tip of that instrument, with that little hook, that s about 5 mm in size, so when he was zoomed in all the way, it was occupying the majority of the screen. Just to give you some appreciation of the magnification. What I m doing, now that I ve taken down those superficial dorsal veins, I m taking back the periprostatic fat, back toward what we term the bladder neck. The bladder neck is where the prostate and the bladder meet. Another question we have is, is this procedure supported by most insurance companies? We have to realize that the procedure we re doing today is a standard radical prostatectomy that s been done for many years for the treatment of localized prostate cancer. The insurance companies view it as just that, an operation to remove the prostate for prostate cancer. This is just one more technique by which that operation can be done. Clearly we think it offers certain advantages and that s what we hope to demonstrate tonight. Right now Dr. Wagner is operating on top of the prostate, up toward the bladder. He s trying to identify the junction between the prostate and the bladder because eventually the prostate has to be separated from the bladder. It just so happens there s a lot of fatty tissue on top of the bladder. The yellow tissue we see in the screen is that fatty tissue that
9 he s removing to get a clearer view of the junction between the prostate and the bladder. He can actually remove that tissue and take it out through one of the ports. I d like to comment a little bit about the movement of the instruments. The slide in front of us shows a laparoscopic instrument, which is traditional for laparoscopic surgery. When we talk about the degrees of freedom of motion with an instrument like that, basically how much movement can you get out of an instrument? With a traditional laparoscopic instrument, there are four degrees of freedom. You can move in and out. You can rotate the instrument. It has pitch, which is up and down, and there s yaw, which is side to side. The robot goes a step further than this, getting closer to what the human hand can do in that there s at least 6 and actually 7 degrees of freedom of motion with the robot. The reason for the additional degrees of freedom is that the robot is not a completely rigid instrument. It actually has not only an arm, but a wrist as well, and by adding movement at the wrist, we ve picked up an additional 2-3 degrees of motion. We can show that with a little video clip that we have. As you can see, the instrument can rotate and go from side to side. It s moving not only the black arm, but the wrists and fingers of the instrument. Here is a surgical demonstration showing the surgeon operating the controls and the robot performing corresponding motions on a small blood vessel. That suture is about the size of a human hair, which gives you a better idea of the degree of magnification that can be achieved with the robot. So basically whatever the surgeon is doing with his arm, wrists, and fingers, the robot is replicating. We re back to a live video of Dr. Wagner s hands in the console, operating those very same mechanical arms. We can now see the endopelvic fascia. So we ve made it around the back of the prostate. We ve made it on top of the prostate, made the dissection. Now we re working on the sides of the prostate. The sides of the prostate have a band of tissue called the endopelvic fascia, which has to be opened in order to free the lateral edges of the prostate. That s what Dr. Wagner has just opened and is now enlarging the opening. Dr. Schichman, what s your role at this point in the operation? Not much. Everything s going nice and smoothly. I m just giving a little counter-traction on the tissues, sucking some smoke, keeping the tissues spread out so the dissection planes are well visualized, and just getting ready to perform the suturing of the dorsal venous complex. At that time I m going to put a sound in the urethra to help move the prostate around, but we ll describe that as soon as we come to that. You can notice as I suck out the pneumoperitoneum...what the pneumoperitoneum is is we re insufflating, blowing up the abdominal cavity with carbon dioxide gas. This gives up a nice big working space as we blow up that space, but it also increases the pressure in the abdominal cavity. Excuse me one second while we change the instruments.
10 If you could take the Foley catheter out and the sound in, please. There are a variety of instruments that are currently available for the robot and many more in development. You will see us periodically switching instruments in and out of the procedure. It takes on the order of seconds to change from one instrument to another. The slide on the screen gives you an idea of some of the different instruments that are currently available. They include graspers, like the one being used by Dr. Wagner in his left hand, and a hook that has electrocautery in his right hand. At some point during the operation, we ll also introduce needle drivers to hold sutures, scissors to help in the dissection, and a variety of grasping instruments to hold various types of tissue. This procedure is utilized for a variety of other operations as well, so there are different instruments that are available, depending on the exact type of operation that s being performed. So now, Vin, we have a sound, a piece of metal inside the urethra to spread out the apex. What I m doing here is spreading beside the puboprostatic ligament, which is some fascia that attaches up to the pubic bone and supports the apex of the prostate. In this area here, exiting out this way, is the neurovascular bundle. These are the nerves that I m going to try to spare later on during the procedure to maintain the patient s erectile function. So I m going to spread in this area a little bit. I m going to do this on the other side and then we ve going to cut these puboprostatic ligaments. Again, on this side, you can see here the same sort of tissue exiting out toward the pelvic side wall, into the muscle. I m going to spread just beyond that. Then we re going to throw our stitches to control the dorsal venous complex, somewhere down in there. We ll see, once we drop these ligaments, where it is. If we could return to the model for a minute, I ll show you where Dr. Wagner is operating. He s coming down from above, between the prostate and the public bone, and is trying to separate the tissues at what we call the apex of the prostate. That is where the prostate joins with the urethra tube. On top of the urethra is a large complex of blood vessels called the dorsal venous complex. He will be suture ligating these vessels to try to prevent them from bleeding when he cuts through them to get down to the urethra because eventually the urethra and prostate have to be separated. He s developing the space on either side of these blood vessels, preparing it so that he will have room to then throw that suture, necessary to control that dorsal venous complex. Dr. Schichman, a question for you from one of your fans. It says Dr. Schichman is a very good laparoscopic surgeon. Can this procedure be done without another well trained laparoscopic assistant? What about a surgical PA, for example?
11 Absolutely. We commonly perform this procedure with one skilled laparoscopic surgeon and we have a first assistant who may or may not be a skilled laparoscopic surgeon, but they may be very experienced in performing this procedure with a skilled laparoscopic surgeon. So, to answer your question, yes it can be performed without two experienced laparoscopic surgeons. What about doing the procedure totally laparoscopically? Yes. The procedure was actually first described totally laparoscopically and yes it can be performed. We have performed many laparoscopic prostatectomies without the DaVinci robot. Again, the advantages have been demonstrated with regard to the visualization. It s easier for also a non-laparoscopic surgeon or standard urologic surgeon or a general surgeon to reproduce the procedures laparoscopically if they have the DaVinci robot available. You ll be able to perform the procedure much better if you do not have the laparoscopic experience behind you. A couple more questions. How much blood is lost during this procedure with and without the DaVinci robot? Not much blood is lost. Hopefully not much. I know that s a very subjective answer, but typically we like to think it s less than 3-4 oz. of blood is lost, sometimes just 1-2 ounces. Obviously it varies and it may be more. You can see right now that we really haven t lost any blood up to this point in the operation. Excuse me one second while I change out some of our instruments. Again, one of the advantages is that pneumoperitoneum that Dr. Schichman was discussing before, it creates a certain degree of pressure within the body cavity that will actually put pressure on all the small blood vessels so they don t ooze as you dissect through the tissues. That s a significant advantage in terms of reducing blood loss. In general, blood loss probably runs about half with using the DaVinci robot, as opposed to doing it by the open procedure. Fortunately, doing it either way, most surgeons nowadays have gotten to the point where it s unusual to have to transfuse the patient to undergo this operation, whether it be done open, laparoscopically, or by the DaVinci system.
12 What we re going to see next is Dr. Wagner actually passing a suture around the dorsal venous complex on top of the urethra and then he will tie this suture to try to prevent subsequent bleeding when he has to cut through that vascular complex. The robot allows him to turn the needle as if he were holding it with a standard needle driver in an open operation. He has come in from the right and passed it over to the left. This is where one of the beauties of the robot comes in. The true advantage is when we re performing suturing maneuvers and we have to tie sutures, the ends that reticulate are very useful in helping us tie down these knots. This is one area where the DaVinci is clearly advantageous over straight laparoscopic procedures. Any knots that can be tied with an open approach can also be tied with a robotic approach. The slide on the screen gives us a little bit of an idea of the scale of the instruments compared to the human hand. We ve tied the knot, put two throws, and we ll now cut the suture and remove it. He s bringing a second suture to doubly ligate this. One of the questions is who is an ideal candidate for this type of surgery? First off, this operation is done only in men with prostate cancer and then in men whose prostate cancer is localized to their prostate. Once the prostate cancer has spread beyond the prostate, then typically we do not remove the prostate, but treat the patient with other forms of therapy. Almost any patient who is a candidate for open surgery would also be a candidate for robotic surgery, although there are some exceptions. Patients whose body habitus is extremely large and might prevent the instrument from being able to be used effectively might not be candidates for robotic surgery. Also, because the patient is put in a head-down position, any patient that has significant lung problems may also not be a candidate for robotic prostatectomy, given the pressure that occurs to the lungs when the patient is tilted head down. Here we re watching the knot being tied. Dr. Wagner is using visual clues to determine how tight that knot is. That s a little different than open surgery, where you can actually feel the tension in the knot. This is one part of robotic surgery which clearly takes some getting used to. There is a lack of tactile feedback, so we have to rely on visual clues to determine such things as knot tightness. Another question is how widespread is the DaVinci robot? Worldwide, there s more than 130 systems currently functioning in hospitals throughout the world. A little over 100 of those are here in the United States, so it s becoming an increasingly popular and widespread technology.
13 Now we ve controlled the dorsal venous complex, which is a notoriously bloody portion of the procedure. We ve probably lost less than people lose when they give a blood specimen at the lab. Dr. Schichman is using an irritating instrument there. He s squirting water in each of the operative fields in order to clear away the little bit of blood that is currently present. You can also see, if we go back to those stitches, these are where the nerves are exiting, somewhere out this way. The apex or where the prostate ends is about here, but we ve gotten these stitches well below the pubic bone, which is way up here, probably on the order of 2 cm or so below. This is a tough area to get to at times, again depending on a patient s size and build. One of the questions is how long does a patient keep a Foley catheter in post-op? This does vary somewhat with the surgeon. On average, approximately one week, somewhere in the 7-9 day range. Someone asked how many of these operations has Dr. Wagner performed. I think right now on the order of, either performing or teaching people to do them, on the order of 200. At Hartford Hospital, this is approximately our 50 th or so case, 45 or 50, since January. Currently we re doing 2-3 a week. Alright, so this is a little break now in the procedure. What we re going to do now is take out both needle drivers and we re going to replace our 0 o lens, which gives us a straight ahead view, with a 30 o down lens, which will allow us to sort of look back on ourselves a little bit and give us a better view of the bladder neck. If we can give the patient 1 amp of indigo carmine, please. The indigo carmine is a medication that we re going to give through the IV, which will turn the patient s urine blue. What I m going to do next is I m going to cut in between the prostate and the bladder. Take out the suction, please. What that will do is allow us to identify the ureteral orifices, where the urine is coming down from the kidneys into the bladder. Right now they re changing the camera. As Dr. Wagner was just mentioning, there are a variety of camera lens combinations that can be used, the difference being the angle at
14 which the camera looks. It can look straight ahead. It can look down. It can look up and at various angles. During certain parts of the operation, it s advantageous to have the camera looking in a particular orientation. One of the other advantages of the robot is that any tremor that the surgeon might have is completely eliminated by the robot. In addition, the robot can actually scale down the movements of the surgeon. So, for example, Dr. Wagner makes a 1 movement with the controls. The robot can scale that down to 1/2 movement or even 1/5 movement, so it allows for much more precise movement of the actual instrument. A couple more questions. Do you think that the fourth arm of the robot will replace the assistant surgeon? Right now, Dr. Wagner is using a three-armed robot, two for instruments and one for the camera. There is a fourth arm available, which can be utilized to hold tissue. Largely the role of the first assistant, as Dr. Schichman elaborated earlier, is to hold tissue out of the way to allow the primary surgeon a clear field. The fourth arm could eliminate the need for an actual surgical assistant, although there are some advantages to having a surgical assistant who can move rather than just hold tissue. How about the size of the incision? There are 5 or 6 port incisions that are used to do this operation. Each one is under 1 cm in size or approximately 1 cm in size, so the total length, combined is approximately somewhere around 5 cm. However, they are separate and, being so small, heal quite quickly. That was a question originally presented to all laparoscopic surgeons over a decade ago. The additive length of the trochar incisions has been shown that it s definitely not equivalent to making a similar length incision at one site, so if you have 5 trochar sites of 1 cm each, how does that patient compare to a patient who has a 5 cm incision made in their abdominal wall? It is clear that the patient with 5 separate 1 cm incisions is much more comfortable, heals much quicker, and has less postoperative pain than the patient with one larger incision. Right now, Dr. Wagner is trying to open the space between the prostate and the bladder. He s using the hook electrode to actually make an incision at the bladder neck, between the bladder and the prostate. Eventually he ll take this incision all the way around the bladder neck. We can just see the Foley catheter that we inserted earlier, coming through the prostate and into the bladder neck and out through the incision that we have made in the anterior bladder neck. We ll pull this up and now work on separating the posterior bladder neck from the prostate. We re now looking right into the prostatic urethra, right at the bladder neck. I can show this on the model here again. This is the bladder. This is the bladder neck and the prostate. We ve separated the prostate in front. We ve separated in back and worked on
15 the sides as well. Now he s coming between the prostate and the bladder, separating the bladder neck from the prostate. He s coming from an anterior approach. We ve made an incision here, in the anterior bladder neck, and then brought the catheter, which is traveling through the urethra and the prostate, out through that incision and now is looking at the posterior bladder neck. He s going to make an incision down through the posterior bladder neck, eventually separating the prostate completely from the bladder. Here he is making the incision in the posterior bladder. A fellow wrote in that he had a vasectomy 30 years ago and was wondering if that would make a difference. The difference I think he s asking is whether that might increase his risk of developing prostate cancer. There was several years ago a study that suggested that having a vasectomy could perhaps have some influence on one s risk of developing prostate cancer, but most of the subsequent studies that have looked at that particular question have not found that to be the case. In general, it is not felt that vasectomy plays a significant role in the risk of prostate cancer. Having a vasectomy itself would not in any way interfere with having a prostatectomy performed, regardless of the approach that might be utilized. There is a question about how long the procedure typically takes. We started with the robot at 5:45. What time is it now? Around 7:00? So typically the robot time for a case like this is about 2 hours and 40 minutes, 3 hours, with 20 minutes setup and 20 minutes on the other end, taking the specimen out and closing the holes, so the totals are just under four hours in my hands. There are some surgeons who are a little faster and some a little slower. In general, it s probably fair to say that robotic prostatectomy takes longer than the open procedure, but as experience grows with the robotic procedure, it is likely that those time intervals will decrease. Another question is does the robot give any force feedback? Again, this is the issue of tactile feedback. One of the disadvantages of the robot is that you do not get the same kind of tactile feedback that you get when you actually have your hands in the operative field. You can get a very general sense of force, but the robot is strong and can easily move tissue. What I m doing now is Steve is holding up the seminal vesicles, so we went straight through the bladder. These are the seminal vesicles that we dissected out before. He s lifting that up in the air and then this, under here, is that space that we cleared out earlier
16 to show me the plane in between the prostate and the rectum. You can let go of that now, Steve. I m going to swing this over and get the other one. Dr. Schichman, what happens if we had a complication and we had to get the robot out of the way? Well, it s pretty easy to disengage the instruments. As you can see, the instruments slide out quite easily and unhook. Once the camera slides out, I just have to snap off the connection where the camera trochar or little tube where the camera slides in is connected to the robot. Then the other two tubes with those two laparoscopic instruments that Dr. Wagner is operating with are also just connected to the robot with two little thumb screws which we can just disengage. So the total time involved to move the robot out of the way? Couple minutes. And of course that would only be done if it was necessary to open the patient to complete the surgery. Please continue to your questions. I think what we ll do, Vin, is I think we re pretty close to 7:00 and this is a major break point. These are the prostatic pedicles, the main blood supply that I m taking down to the prostate now. Once we do this, we re going to switch to two different instruments. One is called the bipolar forcep. The advantage of it is it s a little grasper and I ll demonstrate it once it s inside the abdomen, but the electrical current goes from one hand to the other, so it only cauterizes what s in between it and it has less arc effect. What we re going to do now is be very precise and particular about the blood vessels we re cauterizing as we dissect off the neurovascular bundles, the blood vessels and nerves that go down to the penis and cause erections, so we re going to use that very precise cautery and also scissors to cut the neurovascular bundle off the prostate, so we ll show a little bit of that and then I think we ll just move on with the procedure but end the webcast.
17 One of the main concerns in terms of the long-term complications with prostate removal is interference with erectile function. The reason that erectile function can be disrupted by prostate removal is that the nerves that supply the penis with the ability to get an erection happen to be the same nerves that supply the penis with erectile ability and those nerves are actually attached to the prostate before they go out to the penis. What we re going to see here is Dr. Wagner actually trying to separate the tissue that contains the nerves, called the neurovascular bundle, away from the prostate. Again, we re going to start to accept a little bit of oozing at this point that we wouldn t have accepted before. Now what I m doing is I m cutting the prostatic fascia on either side of the prostate, just like surgeons do during open surgery, in order to drop those bundles down. These nerves are on either side of the prostate, so whatever is done on one side will also be done on the other. How much dissection gets done to try to save these nerves has to do a little bit with the cancer itself. If the patient has an extensive cancer on the edge of the prostate, near where these neurovascular bundles are, then the surgeon will purposefully go wider in that area, taking some of the neurovascular bundles in order to obtain a clear surgical margin, that is to get around the cancer cleanly without getting too close to it. Not all patients are candidates for nerve-sparing. Clearly that would affect the chances of potential potency. So here we see Dr. Wagner separating the neurovascular bundle below from the prostate above. He s purposely not using a lot of electrocautery here in order to prevent any damage to the neurovascular bundle. Since we re not going to be able to see the entire procedure tonight, I d like to show a short video clip of another important aspect of the procedure itself. That s the anastomosis of the bladder back to the urethra, once the prostate has been completely removed. This is important because it affects the return of continence or control of urinary function. Here we see a video clip of the actual anastomosis being performed. The urethra is at the top of the screen, the bladder at the lower portion of the screen. Dr. Wagner in this case has passed the suture first through the urethra, then through the bladder, and is now tying the suture down, which will bring the bladder down to meet the urethra, so the gap that gets created by removal of the prostate is made up by simply moving the bladder down to join the cut end of the urethra. In this particular case, Dr. Wagner is doing an interrupted anastomosis, where he will place several interrupted sutures, but it can also be done in a continuous fashion, where a single suture is used and simply spun around the entire anastomosis. Currently that is the preferred method that Dr. Wagner is employing.
18 One of the other questions is whether or not a lymph node dissection to check to see whether or not cancer has spread to the lymph nodes can be done by the DaVinci approach. It certainly can. It adds approximately 40 minutes to the time of the surgery, but one can do as thorough a lymph node dissection using the DaVinci as can be done with an open surgical approach. One of the important questions is can we truly get a negative surgical margin doing this operation? That s something we strive for, since this is a cancer operation first and foremost. Currently, Dr. Wagner, would you like to comment on what the positive surgical margin rate is? I actually just happened to look at our positive surgical margin rate here after our first 45 cases. Our current rate, and this is all comers, so it s very dependent on Gleason score before the operation, PSA, etc., etc., but our number was 23%, which is very comparable to open series. Any hospitals where they ve compared open surgery to robotic surgery have shown fairly equal rates between robotic and open surgery. So we re back again, watching Dr. Wagner trim away the neurovascular bundles from the side of the prostate on the left side. He will do this all the way down to the prostatic apex, where the urethra and prostate join. He ll do a similar process on the other side and then he will cut across the urethra right at the junction of the prostate and urethra. Once he has done that, the prostate will be completely free and can be removed from the patient. It is removed by enlarging one of the instrument ports just enough to be able to fit the specimen through. The specimen is then taken to the pathologist, where they will look at the amount of cancer that is present and look at such things as the surgical margins to see whether or not the cancer extended to the margins or perhaps beyond, into the tissues around the prostate. In cases like that, some patients will then require additional therapy after their surgery, such as radiation. One question for the OR staff is how do you clean and sterilize the robot? The only thing that s in contact with the patient are the surgical arms...excuse me, not the surgical arms, but the actual instruments that you see. Each one of these instruments goes through a sterilization process which has been well tested to make sure that there is no residual tissue or any bacteria or any live cells present. The rest of the instrument is not in contact with the patient. You can see from the external views, the surgical arms are actually covered with sterile surgical drapes, clear plastic drapes, where they re not in contact with, in fact, anything on the patient.
19 I have been asked to expand a little bit on my comments about who would not be a good candidate for nerve-sparing surgery. I think I consider taking the nerves as part of the specimen in patients that have a very high Gleason score on that side with multiple biopsies positive. So, for instance, I might be much more inclined to take the nerves on someone who had multiple biopsies, 4 out of 4 on the left hand side, let s say, with Gleason 8 and perhaps a lot of perineural involvement on the biopsies. How about if you can feel the cancer on a rectal examination? Will that influence your decision? It does somewhat. I m a little bit more concerned when we feel disease. That s called T2 prostate cancer and then I get a little bit even more concerned, but it s not a definite. I certainly don t, in all patients that I feel something, end up taking the nerves on that side. If you can see right now, we re in the exact right plane that I want to be in, so this is the plane initially that I m poking at right now with my scissors. That s Denonvilliers fascia that was straight underneath the prostate. I use that to sort of guide me as I come up and that rolls very nicely into the smooth, shiny surface underneath the prostate. Then I m just sort of cutting in between those two to drop down the neurovascular bundles of the prostate, so this is exactly where we want to be. You can see how it starts to tease off once we get a little further toward the tip of the prostate, toward the apex. I think we ve just about run out of time for this video webcast. We hope that we ve given you a glimpse of robotic surgery and what it s all about and what the future of robotic surgery may hold. We think there s enormous potential here. As technology improves, so will the robot. As we get more experience, so will the skill of the surgeon utilizing the robot. I d like to thank everyone for joining us tonight. We will try to respond to your questions that come in after we go off the air. There will be an archive of this webcast available at the website shortly, so check back to the website and you ll be able to view the entire webcast through the archive system. Thank you and good night. NARRATOR
20 This has been a radical prostatectomy by robotic surgery, performed live at Hartford Hospital in Hartford, CT. For more information, to make a referral or make an appointment, click on the buttons below.
da Vinci Prostatectomy Information Guide (Robotically-Assisted Radical Prostatectomy)
 da Vinci Prostatectomy Information Guide (Robotically-Assisted Radical Prostatectomy) Prostate Cancer Overview Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the
da Vinci Prostatectomy Information Guide (Robotically-Assisted Radical Prostatectomy) Prostate Cancer Overview Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
RADICAL HYSTERECTOMY IN ROBOTIC SURGERY
 RADICAL HYSTERECTOMY IN ROBOTIC SURGERY FLORENCE BOCHU CENTRE OSCAR LAMBRET LILLE PATRICIA VARUMBEKE CENTRE OSCAR LAMBRET LILLE MELANIE FLAMENT CENTRE OSCAR LAMBRET LILLE More and more centers across the
RADICAL HYSTERECTOMY IN ROBOTIC SURGERY FLORENCE BOCHU CENTRE OSCAR LAMBRET LILLE PATRICIA VARUMBEKE CENTRE OSCAR LAMBRET LILLE MELANIE FLAMENT CENTRE OSCAR LAMBRET LILLE More and more centers across the
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Introduction
 Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Types of surgery for kidney cancer
 Useful information for cancer patients Contents This information is about the different operations that you may have for kidney cancer. Surgery can be used to treat almost any stage of kidney cancer. There
Useful information for cancer patients Contents This information is about the different operations that you may have for kidney cancer. Surgery can be used to treat almost any stage of kidney cancer. There
DISCUSSION ABOUT OPEN, LAPAROSCOPIC, AND ROBOTIC PROSTATECTOMIES MOUNT SINAI MEDICAL CENTER NEW YORK CITY, NEW YORK August 13, 2008
 DISCUSSION ABOUT OPEN, LAPAROSCOPIC, AND ROBOTIC PROSTATECTOMIES MOUNT SINAI MEDICAL CENTER NEW YORK CITY, NEW YORK August 13, 2008 00:00:08 ANNOUNCER: Today, Mount Sinai Medical Center s leading urological
DISCUSSION ABOUT OPEN, LAPAROSCOPIC, AND ROBOTIC PROSTATECTOMIES MOUNT SINAI MEDICAL CENTER NEW YORK CITY, NEW YORK August 13, 2008 00:00:08 ANNOUNCER: Today, Mount Sinai Medical Center s leading urological
male sexual dysfunction
 male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
CONTENTS: WHAT S IN THIS BOOKLET
 Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner
 Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner The following information is based on the general experiences of many prostate cancer patients. Your
Dealing with Erectile Dysfunction During and After Prostate Cancer Treatment For You and Your Partner The following information is based on the general experiences of many prostate cancer patients. Your
Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy
 6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
That being said, consider the following as you decide whether or not a vasectomy is your best option for birth control.
 Since you re reading this, you are probably strongly considering a vasectomy as a way to enjoy sex without the risk of pregnancy. You may feel nervous or hesitant to get one or have questions and concerns
Since you re reading this, you are probably strongly considering a vasectomy as a way to enjoy sex without the risk of pregnancy. You may feel nervous or hesitant to get one or have questions and concerns
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
UROLOGY GROUP of PRINCETON
 UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Lymph Node Dissection for Penile Cancer
 Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
Achieving Independence
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Intraperitoneal Chemotherapy
 Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
INFORMATION FOR PATIENTS CONSIDERING LAPAROSCOPIC INGUINAL HERNIA REPAIR
 INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Laparoscopic Anatomy of the Pelvis
 2 Laparoscopic Anatomy of the Pelvis Intra-Abdominal Anatomy of the Male Pelvic Region Bladder Medial Umbilical Ligaments Lateral Umbilical Ligaments Spermatic Cords Iliac Vessels Ureters Seminal Vesicular
2 Laparoscopic Anatomy of the Pelvis Intra-Abdominal Anatomy of the Male Pelvic Region Bladder Medial Umbilical Ligaments Lateral Umbilical Ligaments Spermatic Cords Iliac Vessels Ureters Seminal Vesicular
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Prostate Cancer. Understanding your diagnosis
 Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
After Diagnosis: Prostate Cancer. Understanding Your Treatment Options
 After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
MANAGEMENT OF PROSTATE ENLARGEMENT/BPH
 MANAGEMENT OF PROSTATE ENLARGEMENT/BPH J E S S I C A E. P A O N E S S A, M. D. A S S I S T A N T P R O F E S S O R D E P A R T M E N T O F U R O L O G Y S U N Y U P S T A T E M E D I C A L U N I V E R
MANAGEMENT OF PROSTATE ENLARGEMENT/BPH J E S S I C A E. P A O N E S S A, M. D. A S S I S T A N T P R O F E S S O R D E P A R T M E N T O F U R O L O G Y S U N Y U P S T A T E M E D I C A L U N I V E R
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Questions to Ask My Doctor About Prostate Cancer
 Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Surgery for breast cancer in men
 Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
How do I know if I need to have surgery?
 How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
The Take-Apart Human Body
 The Take-Apart Human Body As any teacher knows, children are naturally curious about their bodies. Their questions are endless, and present a tremendous educational opportunity: How do my ears work? Where
The Take-Apart Human Body As any teacher knows, children are naturally curious about their bodies. Their questions are endless, and present a tremendous educational opportunity: How do my ears work? Where
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary
 X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
Surgical scissors and forceps Product List
 Surgical scissors and forceps Product List Sr. No Items Picture of Product Product specification 1 Grasping forceps-- 5 MM Grasping forceps are used to remove stones and retrieve foreign objects under
Surgical scissors and forceps Product List Sr. No Items Picture of Product Product specification 1 Grasping forceps-- 5 MM Grasping forceps are used to remove stones and retrieve foreign objects under
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
How prostate cancer is diagnosed
 How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery
 Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION
 A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Therapies for Prostate Cancer and Treatment Selection
 Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
A start to help you understand prostate cancer
 A start to help you understand prostate cancer If you are reading this because you have worries or concerns about yourself or someone you know then the best thing to do is make an appointment with your
A start to help you understand prostate cancer If you are reading this because you have worries or concerns about yourself or someone you know then the best thing to do is make an appointment with your
Vasectomy What happens under normal conditions? What is a vasectomy? How is a vasectomy performed?
 Vasectomy The decision to proceed with a vasectomy is a very personal one. It is important that you have a clear understanding of what a vasectomy is and what it is not. Most patients can expect to recover
Vasectomy The decision to proceed with a vasectomy is a very personal one. It is important that you have a clear understanding of what a vasectomy is and what it is not. Most patients can expect to recover
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
SHEEP EYE DISSECTION PROCEDURES
 SHEEP EYE DISSECTION PROCEDURES The anatomy of the human eye can be better shown and understood by the actual dissection of an eye. One eye of choice for dissection, that closely resembles the human eye,
SHEEP EYE DISSECTION PROCEDURES The anatomy of the human eye can be better shown and understood by the actual dissection of an eye. One eye of choice for dissection, that closely resembles the human eye,
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Testing for Prostate Cancer
 Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Testing for Prostate Cancer Should I be tested? Is it the right choice for me? Prostate cancer affects many men. There are tests to find it early. There may be benefits and risks with testing. Research
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis)
 Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Talking about Prostate Cancer
 Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
Talking about Prostate Cancer Talking about Prostate Cancer If I can avoid going to a doctor, I will but not when we re talking about prostate cancer. Why take chances with a condition that might be serious?
INSULIN INJECTION KNOW-HOW
 0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
Abdominal Aortic Aneurysm (AAA) General Information. Patient information Leaflet
 Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 1 st July 2016 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the heart
Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 1 st July 2016 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the heart
Building A Computer: A Beginners Guide
 Building A Computer: A Beginners Guide Mr. Marty Brandl The following was written to help an individual setup a Pentium 133 system using an ASUS P/I- P55T2P4 motherboard. The tutorial includes the installation
Building A Computer: A Beginners Guide Mr. Marty Brandl The following was written to help an individual setup a Pentium 133 system using an ASUS P/I- P55T2P4 motherboard. The tutorial includes the installation
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
VASECTOMY What is Vasectomy? How is the procedure performed? What is the no-scalpel method of doing vasectomy? When can I go back to work?
 VASECTOMY What is Vasectomy? Every man has a basic right to a vasectomy, a valuable medical procedure. Before you actually have a vasectomy, you should think about it carefully, because a vasectomy is
VASECTOMY What is Vasectomy? Every man has a basic right to a vasectomy, a valuable medical procedure. Before you actually have a vasectomy, you should think about it carefully, because a vasectomy is
How common is bowel cancer?
 information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
restricted to certain centers and certain patients, preferably in some sort of experimental trial format.
 Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
GreenLight laser prostatectomy
 Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
LIvING WITH Prostate Cancer
 Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
The temporary haemodialysis catheter
 The temporary haemodialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information in this booklet is for: People have renal failure and who require urgent haemodialysis.
The temporary haemodialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information in this booklet is for: People have renal failure and who require urgent haemodialysis.
Laparoscopic Assisted Vaginal Hysterectomy
 Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Placement of an indwelling urinary catheter in female dogs
 Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
PROSTATE CANCER. Diagnosis and Treatment
 Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer
 Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
ACTION PLAN. Choosing the treatment that s right for you. Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology
 Prostate Cancer ACTION PLAN Choosing the treatment that s right for you Video Series Guidebook View videos at kpactionplans.org Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology 2015 Kaiser
Prostate Cancer ACTION PLAN Choosing the treatment that s right for you Video Series Guidebook View videos at kpactionplans.org Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology 2015 Kaiser
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
PHaSES: Practical Hands-on Surgical Education System
 U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
Women s Health Laparoscopy Information for patients
 Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Caring for Your PleurX Pleural Catheter
 Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Exercises after breast or upper body lymph node surgery
 Exercises after breast or upper body lymph node surgery Surgery may limit the strength and movement of your arm. These exercises are helpful if you have had: breast surgery with or without lymph node removal
Exercises after breast or upper body lymph node surgery Surgery may limit the strength and movement of your arm. These exercises are helpful if you have had: breast surgery with or without lymph node removal
CATHETER for Hemodialysis
 CATHETER for Hemodialysis What You Need to Know to Stay Healthy with a Catheter One treatment choice for kidney failure is hemodialysis (HD). HD removes wastes and excess fluid from your blood. Your lifeline
CATHETER for Hemodialysis What You Need to Know to Stay Healthy with a Catheter One treatment choice for kidney failure is hemodialysis (HD). HD removes wastes and excess fluid from your blood. Your lifeline
Recovery of Erectile Function After Radical Prostatectomy Vanderbilt University Department of Urologic Surgery
 Recovery of Erectile Function After Radical Prostatectomy Vanderbilt University Department of Urologic Surgery Postoperative erectile dysfunction is a potential risk of surgery for prostate cancer, whether
Recovery of Erectile Function After Radical Prostatectomy Vanderbilt University Department of Urologic Surgery Postoperative erectile dysfunction is a potential risk of surgery for prostate cancer, whether
Prostate Specific Antigen (PSA) Blood Test
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
Male Infertility. Penis. Epididymis
 Male Infertility Introduction Infertility is a term used when a man is unable to get a woman pregnant. But the term is only used after at least one year of trying. Infertility is a common problem. About
Male Infertility Introduction Infertility is a term used when a man is unable to get a woman pregnant. But the term is only used after at least one year of trying. Infertility is a common problem. About
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH)
 GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
Possible Side Effects of Radiation Therapy on the Prostate Gland
 Possible Side Effects of Radiation Therapy on the Prostate Gland Information compiled by Daniel J. Faber, Coordinator of the Warriors+one, a Breakout Group of the Prostate Cancer Canada Network- Ottawa,
Possible Side Effects of Radiation Therapy on the Prostate Gland Information compiled by Daniel J. Faber, Coordinator of the Warriors+one, a Breakout Group of the Prostate Cancer Canada Network- Ottawa,
