How To Diagnose Thyroid Problems During Pregnancy
|
|
|
- Shanon Webster
- 3 years ago
- Views:
Transcription
1 Thyroid Disease in Pregnancy and Postpartum 9 INTRODUCTION This chapter discusses cases of pregnancy complicated by thyroid disease and thyroid test abnormalities, as well as thyroid problems after delivery. Thyroid diagnosis and treatment during pregnancy is more complex because there are two patients with whom to be concerned the mother and the fetus. Diagnosis is more difficult because thyroid tests may be harder to interpret in this setting. Also, tests using radiation, such as the thyroid uptake and scan, cannot be safely performed on pregnant women. Treatment is more difficult because of concern about the effect of thyroid disease and medication on the fetus. Radioactive iodine (RAI) treatment is contraindicated during pregnancy. Thyroid problems are also common in the months after delivery, and they are often missed. Following delivery, women may develop nonspecific symptoms, such as fatigue, depression, nervousness, and palpitations. These complaints may be the result of the stress of caring for a new infant and the major lifestyle changes that result. However, they may also result from thyroid dysfunction. Postpartum hypothyroidism or hyperthyroidism occurs in up to 20% of women. It is often transient, but awareness and possible treatment may make a big difference to the patient. Often, the physician will feel that the complaints are the result of emotional problems, and the patient will either reject this diagnosis or feel unhappy about it. The diagnosis of an underlying and probably temporary thyroid disorder will relieve a lot of the patient s stress even if treatment is not indicated. This chapter discusses several cases that demonstrate the types of thyroid problems that are seen in pregnancy and the postpartum period. CASE 1 A 32-year-old woman was referred because of abnormal thyroid function tests. Her thyroid-stimulating hormone (TSH) was less than 0.03, total thyroxine (T 4 ) was 20 (4 12), and total triiodothyronine (T 3 ) was 274 (70 180). She was 16 weeks pregnant and had severe hyperemesis gravidarum with a 19-lb weight loss. She had noted shakiness and intermittent palpitations. From: Current Clinical Practice: Thyroid Disease: A Case-Based and Practical Guide for Primary Care By: E. O. Brams Humana Press Inc., Totowa, NJ 79
2 80 Thyroid Disease Physical examination revealed an acutely ill young woman who was weak and shaky. Pulse was 100 and blood pressure (BP) was 80/44. Her buccal mucosa was dry and her eyes were sunken. The thyroid was enlarged to about 1.5 times the normal size. She had no thyroid eye signs. The following laboratory results were obtained: Free thyroxine (FT 4 ):1.48 ( ). Free triiodothyronine (FT 3 ): 515 ( ). Antithyroid peroxidase antibody was negative. Thyroid-stimulating immunoglobulin (TSI) was normal. What Is Your Diagnosis? The patient is clearly thyrotoxic. The differential diagnosis includes Graves disease and thyrotoxicosis of hyperemesis gravidarum. This is often a very difficult differential to make (see Case Discussion section). In this case, my working diagnosis was Graves disease. How Would You Manage This Patient? The patient was started on 100 mg of propylthiouracil (PTU) every 8 hours, and given parenteral hyperalimentation. One week later, she was seen by her obstetrician for jaundice and referred to a gastroenterologist. I was concerned that the jaundice might be a side effect of the PTU. Fortunately, she had not started the PTU yet because it was pending approval by Medicaid. The gastrointestinal consultant diagnosed fatty liver of pregnancy. The Medicaid approval came through and she started the PTU. Clinical Course The patient gained weight, her pulse slowed to 70 to 80, and the tremor cleared. Follow-up FT 3 and FT 4 were normal, although the TSH remained low. The PTU dose was gradually decreased to 50 mg twice daily. A TSI at 8 months of pregnancy was normal. She delivered a normal full-term infant. Postpartum The baby s total T 4 at 1 d was 24.1 (upper-normal for that age). At 1 week, the baby s total T 4 was 13.6, TSH was 1. The mother became clinically hyperthyroid and required an increase in PTU to 150 mg every 8 hours. She was continued on PTU for several months while awaiting Medicaid approval for RAI therapy. Eventually, she was treated with RAI and developed the usual post-rai hypothyroidism. She is now euthyroid on replacement T 4. The baby is doing well. Case Discussion This challenging case demonstrates the difficulty in diagnosis of the etiology of hyperthyroidism in a pregnant woman. Making the correct diagnosis is obvi-
3 Chapter 9/Pregnancy and Postpartum Thyroid Disease 81 ously critical to appropriate treatment. The differential diagnosis is usually between transient hyperthyroidism of hyperemesis gravidarum (THHG) and Graves disease. THHG is caused by inappropriate secretion of human chorionic gonadotropin (HCG). HCG and TSH have the same α-subunit and different β-subunits. HCG is a mild thyroid stimulator, and high levels may produce hyperthyroidism. Graves disease is, of course, an autoimmune disease and is caused by immunoglobulins that stimulate the TSH receptors on thyroid cells. Hyperthyroidism is the second most common endocrine disease in pregnancy (diabetes is the first) and occurs in 1 in 500 pregnancies. Graves disease is the more serious problem, and requires aggressive therapy to avoid complications in mother and child. THHG is usually a self-limited disease and may only require symptomatic therapy or observation. In the absence of Graves disease ophthalmopathy, the differential diagnosis is often difficult. Some clinical clues that point to Graves disease include a history of hyperthyroid symptoms prior to pregnancy, the presence of goiter, and exophthalmos and positive antibodies. In THHG, the severity of the hyperthyroidism is usually related to the severity of the vomiting, and the hyperthyroidism will usually spontaneously clear by the fourth or fifth month of pregnancy. A suppressed TSH may also be seen in normal pregnancy without thyroid disease, but in this case the patient will not have hyperthyroid symptoms, and the T 3 and T 4 will be normal. This patient had severe hyperemesis and could well have had THHG. However, she had a goiter, and I made a working diagnosis of Graves disease. Antithyroid drugs (ATDs) are the treatment of choice in the pregnant Graves patient. She was started on PTU in a moderate dose, and the dose was tapered as she improved. It is important not to over treat and cause hypothyroidism, because hypothyroidism in the mother may produce goiter and hypothyroidism in the fetus. The ATD dose should be adjusted to keep the FT 4 in the upper normal range. Graves disease, like other autoimmune diseases, tends to improve during pregnancy, and the ATD can often be decreased and even discontinued in the latter part of pregnancy. This patient delivered a normal infant. The baby was euthyroid and had no goiter. A TSI at 8 months of pregnancy was normal. The TSI should be measured in the last trimester. A significantly elevated TSI should alert the physician to the possibility of neonatal hyperthyroidism in the newborn. This is a serious problem that requires expert help from the endocrinologist and pediatrician. My working diagnosis of Graves disease in the mother proved correct in this patient. The Graves disease persisted through pregnancy and became more severe after delivery. She required definitive therapy with RAI and has done well on replacement T 4. If she becomes pregnant again, a TSI should be done in early pregnancy. A significantly elevated TSI will alert the physician to the pos-
4 82 Thyroid Disease sibility of neonatal hyperthyroidism. The mother s thyroid function should be monitored during pregnancy and the T 4 dosage adjusted to maintain a euthyroid state. What Can We Learn From This Case? Consider hyperthyroidism in pregnancy, especially if the patient has a resting pulse over 100 and fails to gain weight despite good intake. Obtain FT 4 and TSH. Try to make differential diagnosis between Graves disease and the less serious THHG. Be aware that a suppressed TSH alone without symptoms and other findings of hyperthyroidism is common in normal pregnancies and requires no medication. Look for thyroid ophthalmopathy and goiter as signs that may point to Graves disease. In difficult cases, thyroid peroxidase (TPO) antibody and TSI testing may be helpful. If Graves disease is diagnosed, treatment with PTU or methimazole may be needed. Close monitoring is required to prevent maternal hypothyroidism from medication, which can result in fetal goiter and fetal hypothyroidism. In pregnant women with Graves disease, a TSI should be obtained in the last trimester. A signifigantly elevated TSI indicates that fetal or neonatal hyperthyroidism may occur. If treatment with an ATD is needed, keep FT 4 in upper third of the normal range, and try to decrease the dosage as pregnancy progresses. It may be possible to discontinue the drug in the last trimester. Be aware that autoimmune diseases, such as Graves disease, tend to improve in the last half of pregnancy and may flare up after delivery. Flare-ups can also occur in the first trimester. TSI should be monitored in the last trimester in all Graves disease patients, even those who have been treated prior to pregnancy and are euthyroid. TSI crosses the placental barrier and may cause fetal or neonatal hyperthyroidism. Think of hyperthyroidism in the fetus of a Graves disease mother if fetal tachycardia, growth retardation, or goiter on ultrasound are seen. CASE 2 A 30-year-old woman was referred for thyroid evaluation. She was 12 weeks pregnant with her second child. She had noted fatigue, moodiness, and heat intolerance over the previous 2 months. She had constant nausea from morning sickness, but no vomiting. She had lost 5 lb over the previous 2 weeks and complained of headaches. She denied palpitations or tremor. She noted no change in the appearance of her eyes or in her vision. She had one child age 7 years and had no thyroid problems with that pregnancy or postpartum. However, she was found to have a goiter 4 years previously and was treated with T 4 for 3 months. The past several days she had felt better, less tired, but still moody. There was no family history of thyroid disease.
5 Chapter 9/Pregnancy and Postpartum Thyroid Disease 83 Physical examination revealed a pulse of 72 and BP of 110/70. The eyes showed bilateral stare without proptosis or lid lag and the extraocular movements appeared normal. The thyroid was bilaterally enlarged to about twice the normal size, firm, and without nodules. The examination was otherwise normal. The following test results were obtained: TSH less than 0.03; FT ( ); sedimentation rate, 18. TPO antibody, FT 3, and TSI were normal. What Is Your Differential Diagnosis? The differential diagnosis includes Graves disease, THHG, and low TSH of pregnancy. This patient could have THHG, however, the goiter and previous history of thyroid disease make Graves disease a more likely diagnosis. Suppressed TSH with normal T 4 is also a common finding in normal pregnancies, but these patients do not usually have a goiter or other evidence of thyroid disease. I saw this patient on a short locum assignment and was not able to follow her further. She probably had Graves disease. CASE 3 A 26-year-old woman was referred because of a TSH of 0.14, total T 4 of 9.7 (4.5 12), and thyroid microsomal antibody elevated to 15 (<1). She was 6 months postpartum and had complained to her doctor that she could not lose the weight she had gained during pregnancy. She reported that she has been warmer than others at work. She felt otherwise well. Her only medication was a birth control pill. On physical examination, the pulse was 68, BP was 124/72. There were no thyroid eye signs. The thyroid gland was diffusely enlarged to twice the normal size and rubbery in consistency. Examination was otherwise normal. What Is Your Diagnosis? The most likely diagnosis is postpartum thyroiditis (PPT) with mild or subclinical hyperthyroidism. Early Graves disease should be considered in the differential diagnosis. Additional Testing? Treatment? No additional testing or treatment is indicated at this point. Close follow-up is important. Clinical Course The patient returned 1 month later. She was no longer hot and felt well. Physical examination revealed that her thyroid had decreased in size to about 1.5 times the normal size. The TSH was now elevated to 46, FT 4 was 0.24 (0.75 2).
6 84 Thyroid Disease What s Going On? The patient has switched from borderline hyperthyroid to biochemically hypothyroid. In view of the degree of TSH and FT 4 abnormality, she was started on T 4. She returned 2 months later and reported a 6-lb weight loss. Her TSH was Final Diagnosis? Treatment Plan? The final diagnosis is PPT. Treatment Plan Options for treatment include continuing T 4 or discontinuing T 4 with close follow-up to see if her thyroid has recovered. The majority of patients with PPT recover, whereas some go on to permanent hypothyroidism. Because she planned another pregnancy, I elected to continue therapy rather than risk hypothyroidism during pregnancy. Case Summary This 26-year-old woman presented 6 mo postpartum with mild heat intolerance and an enlarged thyroid gland. Her TSH was low with a normal T 4 and thyroid microsomal antibody was positive. The diagnosis was subclinical hyperthyroidism due to PPT. She then converted to hypothyroidism and was treated with T 4. Because she planned another pregnancy, the T 4 was continued to ensure a euthyroid state. What Can We Learn From This Case? Consider thyroid disease in the postpartum period when the patient has vague complaints. Once the physician thinks about thyroid disease in this setting, the diagnosis can be easily ruled in or out with a TSH and FT 4. Postpartum thyroid dysfunction can present as either hyperthyroidism or hypothyroidism and can progress from one to the other. PPT is an autoimmune disease. The patient will return to a euthyroid state spontaneously in the majority of cases. Short-term treatment may be needed to relieve symptoms in some patients, whereas others can be followed without treatment. Whereas the majority of patients will return spontaneously to a euthyroid state, about 25% of patients will become permanently hypothyroid. Look for thyroid dysfunction in subsequent pregnancies. CASE 4 A 28-year-old woman was referred because of heat intolerance and abnormal thyroid function tests. She had delivered twins 10 wk previously. Thyroid testing at 6 weeks postpartum revealed a TSH of 0.05, FT 4 of 2.45 ( ), and FT 3 of
7 Chapter 9/Pregnancy and Postpartum Thyroid Disease ( ). The patient developed PPT after the birth of her first child approx 2 years previously. Approximately 5 months after her first delivery, she noted palpitations, nervousness, insomnia, and fatigue. Her thyroid was noted to be enlarged. Thyroid studies at that time revealed a TSH of less than 0.06 and total T 4 of 10 (4.5 12). Over the next several weeks, these symptoms cleared and she noted the onset of severe fatigue. Repeat studies showed a TSH of 98, FT 4 of 0.39, and radioactive iodine uptake (RAIU) of 2% (7 24). She was started on T 4 and the dose was adjusted over the next several months to normalize her TSH. She was maintained on mg of T 4 daily until the present time. Family history was positive for thyroid disease in the patient s mother. Physical examination currently revealed an enlarged thyroid gland and was otherwise negative. What Is Your Diagnosis? Recurrent PPT with probable hyperthyroidism Treatment T 4 was discontinued. The patient was given a β-blocker as symptomatic therapy for her hyperthyroidism and asked to return with repeat studies off T 4 in 1 month. Case Summary This young woman developed PPT with her previous pregnancy and again after delivering twins. Because she had been maintained on T 4 after her first pregnancy, the thyroid tests were more difficult to evaluate. However, she was clinically hyperthyroid. The history of hyperthyroidism progressing to hypothyroidism with her previous pregnancy and a very low RAIU was compatible with PPT. It seemed likely that she had recurrent PPT with her second pregnancy, although an RAIU would be needed to rule out Graves disease. The appropriate course was to discontinue her T 4, treat her hyperthyroidism symptomatically, and see her again in 1 2 months. What Can We Learn From This Case? When PPT occurs after a pregnancy, it frequently recurs after subsequent pregnancies and the patient should be alerted to look for it. PPT can cause hyperthyroidism alone, hypothyroidism alone or, as in this case, progress from one to the other. The differential diagnosis is Graves disease and the correct test to make the diagnosis is the RAIU. The RAIU will usually be elevated in Graves disease and low in PPT. The hyperthyroidism of PPT may be treated symptomatically and followed because it tends to be self-limited, and the patient will usually either return to a euthyroid state or progress to hypothyroidism. PPT is an autoimmune disease and the TPO or microsomal antibody will often be positive.
8 86 Thyroid Disease CASE 5 A 27-year-old woman was referred to me because of abnormal thyroid function tests. She had delivered her third child about 8 months previously and there was no history of thyroid problems with her previous pregnancies. After her last delivery, she noted mood swings, fatigue, and heat intolerance along with a 15-lb weight gain. She was having regular menses. There was no family history of thyroid disease. Physical examination revealed a pulse of 76 and BP of 114/72. No thyroid eye signs were noted. The thyroid gland was mildly enlarged. The remainder of the examination was normal. The following laboratory studies were reviewed: The initial thyroid studies at 6 months postpartum showed a TSH of less than and FT 4 of 1.7 ( ). Repeat studies 1 mo prior to this visit revealed a TSH of 2.84, FT 4 of 0.8, and total T 3 was normal. RAIU was 2.4% at 24 hours (7 24). Thyroid ultrasound had been reported as normal. What Is Your Diagnosis? The diagnosis is PPT with borderline or subclinical hyperthyroidism that had resolved and might be progressing toward hypothyroidism in view of the recent borderline low-normal FT 4 with normal TSH. Treatment At the time of my evaluation, the patient was clinically euthyroid. She required no thyroid treatment but careful follow-up was required. Case Summary This 27-year-old woman had clinical and laboratory evidence of mild PPT disease. Her thyroid tests at 6 months postpartum were compatible with subclinical hyperthyroidism and the very low RAIU confirmed PPT as the etiology rather than Graves disease. Her TSH then normalized and the FT 4 dropped to the lower edge of normal with low-normal total T 3. She will require careful follow-up to see if she progresses to hypothyroidism or becomes euthyroid. I discussed all of this at length with her and her husband and told them what to look for. They were reassured that the thyroid problem was mild and likely would resolve over time. What Can We Learn From This Case? This case of PPT was much milder than those discussed previously and might have been overlooked if the patient had not developed several nonspecific complaints.
9 Chapter 9/Pregnancy and Postpartum Thyroid Disease 87 The test results included a low TSH and upper-normal FT 4 initially, which were compatible with subclinical or borderline hyperthyroidism. The very low RAIU confirmed the diagnosis of PPT rather than Graves disease. The follow-up tests showed a normal TSH and borderline low FT 4 suggesting that she might be edging toward hypothyroidism. The important point is that, when thyroid status is changing, the FT 4 will change faster than the TSH and may be a more valid reflection of current thyroid status. The TSH may take several weeks to equilibrate and reflect thyroid status. When thyroid status is relatively stable over time, the TSH is a more accurate guide to thyroid status. The patient will probably eventually become euthyroid, although the possibility of permanent hypothyroidism was discussed with her. She was also advised that thyroid disease may recur with future pregnancies. SUMMARY The cases discussed in this chapter demonstrate different clinical presentations of thyroid disease during pregnancy and in the postpartum period. Case 1 is a pregnant woman who was acutely ill. She presented with severe hyperemesis with dehydration and thyroid function tests compatible with hyperthyroidism. She required urgent treatment while the underlying cause of her hyperthyroidism was being determined. The difficulty in making the differential diagnosis between THHG and Graves disease is discussed. The diagnosis of Graves disease was eventually established and she was successfully treated. The second patient presented with vague symptoms, an enlarged thyroid, and biochemical findings of subclinical hyperthyroidism. She was followed without treatment and subsequently developed clinical hypothyroidism that required treatment with T 4. The third patient presented with overt hyperthyroidism several weeks after delivering twins. She had a history of PPT disease after her previous pregnancy. She was treated symptomatically and followed. The last patient presented with nonspecific symptoms, an enlarged thyroid, and laboratory findings of subclinical hyperthyroidism. Her TSH normalized without treatment, but she requires follow-up. These cases demonstrate the importance of thinking about thyroid disease in pregnancy and the postpartum period, and checking thyroid tests in patients with nonspecific complaints. SELECTED SOURCES Brent GA. Maternal thyroid function: interpretation of thyroid function tests in pregnancy. Clin Obstet Gynecol 1997;40: Ecker JL, Musci TJ. Treatment of thyroid disease in pregnancy. Obstet Gynecol Clin North Am 1997;24: ACOG practice bulletin. Thyroid disease in pregancy. Int J Gynaecol Obstet 2002; 79:
10 88 Thyroid Disease Neale D, Burrow G. Thyroid disease in pregnancy. Obstet Gynecol Clin North Am 2004;31: Muller AF, Berghout A. Consequences of autoimmune thyroiditis before, during and after pregnancy. Minerva Endocrinol 2003;28:
Ordering and interpreting thyroid tests in children. Paul Kaplowitz, MD, PhD Children s National Medical Center, Washington, DC
 Ordering and interpreting thyroid tests in children Paul Kaplowitz, MD, PhD Children s National Medical Center, Washington, DC Objectives To review indications for thyroid testing To discuss which tests
Ordering and interpreting thyroid tests in children Paul Kaplowitz, MD, PhD Children s National Medical Center, Washington, DC Objectives To review indications for thyroid testing To discuss which tests
Guidance for Preconception Care of Women with Thyroid Disease
 Before, Between & Beyond Pregnancy The National Preconception Curriculum and Resources Guide for Clinicians Guidance for Preconception Care of Women with Thyroid Disease Avi Alkalay, MD Department of Obstetrics
Before, Between & Beyond Pregnancy The National Preconception Curriculum and Resources Guide for Clinicians Guidance for Preconception Care of Women with Thyroid Disease Avi Alkalay, MD Department of Obstetrics
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy.
 Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy. Early diagnosis and good management of maternal thyroid dysfunction is essential to ensure minimal adverse effects on
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy. Early diagnosis and good management of maternal thyroid dysfunction is essential to ensure minimal adverse effects on
Patient Guide to Radioiodine Treatment For Thyrotoxicosis (Overactive Thyroid Gland or Hyperthyroidism)
 Patient Guide to Radioiodine Treatment For Thyrotoxicosis (Overactive Thyroid Gland or Hyperthyroidism) Your doctor has referred you to Nuclear Medicine for treatment of your overactive thyroid gland.
Patient Guide to Radioiodine Treatment For Thyrotoxicosis (Overactive Thyroid Gland or Hyperthyroidism) Your doctor has referred you to Nuclear Medicine for treatment of your overactive thyroid gland.
THYROID DISEASE IN CHILDREN
 THYROID DISEASE IN CHILDREN Douglas G. Rogers, M.D. Center for Pediatric and Adolescent Endocrinology Cleveland Clinic Foundation Unfortunately neither I nor any immediate family members have any financial
THYROID DISEASE IN CHILDREN Douglas G. Rogers, M.D. Center for Pediatric and Adolescent Endocrinology Cleveland Clinic Foundation Unfortunately neither I nor any immediate family members have any financial
Thyroid Disease in Pregnancy
 Thyroid Disease in Pregnancy The following section is entitled Thyroid Disease in Pregnancy. This section deals with some of the basic concepts important to the diagnosis, management and investigation
Thyroid Disease in Pregnancy The following section is entitled Thyroid Disease in Pregnancy. This section deals with some of the basic concepts important to the diagnosis, management and investigation
Autoimmune Thyroid Disorders. Register at www.srlknowledgeforum.com
 Autoimmune Thyroid Disorders Register at www.srlknowledgeforum.com 1 What is AITD? Autoimmune thyroid disease (AITD) is a common organ specific autoimmune disorder seen mostly in women between 30-50 yrs
Autoimmune Thyroid Disorders Register at www.srlknowledgeforum.com 1 What is AITD? Autoimmune thyroid disease (AITD) is a common organ specific autoimmune disorder seen mostly in women between 30-50 yrs
THYROID FUNCTION TESTS
 Thyroid Stimulating Hormone (TSH): THYROID FUNCTION TESTS The thyroid stimulating hormone (TSH) assay measures the concentration of thyroid stimulating hormone in the serum. TSH assays have been classified
Thyroid Stimulating Hormone (TSH): THYROID FUNCTION TESTS The thyroid stimulating hormone (TSH) assay measures the concentration of thyroid stimulating hormone in the serum. TSH assays have been classified
Thyroid Disorders. Hypothyroidism
 1 There are a number of problems associated with the thyroid gland. Hypothyroidism, hyperthyroidism, and thyroid nodules will be presented here. The thyroid gland is located in the middle of the neck,
1 There are a number of problems associated with the thyroid gland. Hypothyroidism, hyperthyroidism, and thyroid nodules will be presented here. The thyroid gland is located in the middle of the neck,
loving life YOUR GUIDE TO YOUR THYROID
 loving life YOUR GUIDE TO YOUR THYROID one THE THYROID two HYPOTHYROIDISM three HYPERTHYROIDISM four TREATING HYPERTHYROIDISM five THYROID NODULES AND GOITRES one THE THYROID What is the thyroid? The thyroid
loving life YOUR GUIDE TO YOUR THYROID one THE THYROID two HYPOTHYROIDISM three HYPERTHYROIDISM four TREATING HYPERTHYROIDISM five THYROID NODULES AND GOITRES one THE THYROID What is the thyroid? The thyroid
Thyroid Gland Disease. Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc
 Thyroid Gland Disease Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc t 1/2 = 5-7d t 1/2 = < 24 hrs Normal Daily Thyroid Secretion Rate:
Thyroid Gland Disease Zdeněk Fryšák 3rd Clinic of Internal Medicine Nephrology-Rheumatology-Endocrinology Faculty Hospital Olomouc t 1/2 = 5-7d t 1/2 = < 24 hrs Normal Daily Thyroid Secretion Rate:
RECOMMENDATIONS. INVESTIGATION AND MANAGEMENT OF PRIMARY THYROID DYSFUNCTION Clinical Practice Guideline April 2014
 INVESTIGATION AND MANAGEMENT OF PRIMARY THYROID DYSFUNCTION Clinical Practice Guideline April 2014 OBJECTIVE Alberta clinicians optimize laboratory testing for the investigation and management of primary
INVESTIGATION AND MANAGEMENT OF PRIMARY THYROID DYSFUNCTION Clinical Practice Guideline April 2014 OBJECTIVE Alberta clinicians optimize laboratory testing for the investigation and management of primary
GUIDELINES & PROTOCOLS
 GUIDELINES & PROTOCOLS ADVISORY COMMITTEE Effective Date: January 1, 2010 Scope This guideline applies to: the detection of thyroid dysfunction in adults (individuals 19 years of age and over) monitoring
GUIDELINES & PROTOCOLS ADVISORY COMMITTEE Effective Date: January 1, 2010 Scope This guideline applies to: the detection of thyroid dysfunction in adults (individuals 19 years of age and over) monitoring
Everything You Ever Wanted to Know About the Thyroid
 Everything You Ever Wanted to Know About the Thyroid (but were afraid to ask ) Caroline Messer, MD Board Certified Internist, Endocrinologist, and Physician Nutrition Specialist Topics Thyroid Nodules
Everything You Ever Wanted to Know About the Thyroid (but were afraid to ask ) Caroline Messer, MD Board Certified Internist, Endocrinologist, and Physician Nutrition Specialist Topics Thyroid Nodules
UK Guidelines for the Use of Thyroid Function Tests (July 2006)
 Adapted Summary of UK Guidelines for the Use of Thyroid Function Tests (July 2006) Introduction The Use of Thyroid Function Tests Guidelines Development Group was formed in 2002 under the auspices of the
Adapted Summary of UK Guidelines for the Use of Thyroid Function Tests (July 2006) Introduction The Use of Thyroid Function Tests Guidelines Development Group was formed in 2002 under the auspices of the
Guidelines for the Use of Thyroid Function Tests. Grey s Hospital Laboratory. Pietermartizburg Complex. Compiled and adapted by
 Guidelines for the Use of Thyroid Function Tests Grey s Hospital Laboratory Pietermartizburg Complex Compiled and adapted by Dr. R. Sirkar Chemical Pathologist UKZN August 2006 Compiled and Adapted by
Guidelines for the Use of Thyroid Function Tests Grey s Hospital Laboratory Pietermartizburg Complex Compiled and adapted by Dr. R. Sirkar Chemical Pathologist UKZN August 2006 Compiled and Adapted by
Pregnancy and hypothyroidism
 Pregnancy and hypothyroidism Departments of Endocrinology & Obstetrics Patient Information What What is hypothyroidism? is hypothyroidism? Hypothyroidism means an underactive thyroid gland, which does
Pregnancy and hypothyroidism Departments of Endocrinology & Obstetrics Patient Information What What is hypothyroidism? is hypothyroidism? Hypothyroidism means an underactive thyroid gland, which does
Thyroid Tests. National Endocrine and Metabolic Diseases Information Service
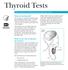 Thyroid Tests National Endocrine and Metabolic Diseases Information Service What is the thyroid? The thyroid is a 2-inch-long, butterfly-shaped gland weighing less than 1 ounce. Located in the front of
Thyroid Tests National Endocrine and Metabolic Diseases Information Service What is the thyroid? The thyroid is a 2-inch-long, butterfly-shaped gland weighing less than 1 ounce. Located in the front of
Hyperthyroidism INTRODUCTION. Overview. Introduction cont. Signs and Symptoms. Signs and Symptoms cont. Marisol Amaral Mona Ruiz Ulises Gonzalez
 INTRODUCTION Hyperthyroidism Marisol Amaral Mona Ruiz Ulises Gonzalez What is Hyperthyroidism? It is the 2 nd most prevalent endocrine disorder. Grave s disease is the most common type of hyperthyroidism,
INTRODUCTION Hyperthyroidism Marisol Amaral Mona Ruiz Ulises Gonzalez What is Hyperthyroidism? It is the 2 nd most prevalent endocrine disorder. Grave s disease is the most common type of hyperthyroidism,
"Women's Health" is also available at www.squarepharma.com.bd
 "Women's Health" is also available at www.squarepharma.com.bd Volume : 8, No. : 1 April - June 2015 Editorial Board Dr. Omar Akramur Rab MBBS, FCGP, FIAGP Ahmed Kamrul Alam M. Pharm, MBA Imran Hassan M.
"Women's Health" is also available at www.squarepharma.com.bd Volume : 8, No. : 1 April - June 2015 Editorial Board Dr. Omar Akramur Rab MBBS, FCGP, FIAGP Ahmed Kamrul Alam M. Pharm, MBA Imran Hassan M.
Thyroid-Stimulating Hormone (TSH)
 Thyroid-Stimulating Hormone (TSH) Table of Contents Test Overview Why It Is Done How To Prepare How It Is Done How It Feels Risks Results What Affects the Test What To Think About References Credits Test
Thyroid-Stimulating Hormone (TSH) Table of Contents Test Overview Why It Is Done How To Prepare How It Is Done How It Feels Risks Results What Affects the Test What To Think About References Credits Test
Thyroid Problems after Childhood Cancer
 Thyroid Problems after Childhood Cancer Some people who were treated for cancer during childhood may develop endocrine (hormone) problems as a result of changes in the function of a complex system of glands
Thyroid Problems after Childhood Cancer Some people who were treated for cancer during childhood may develop endocrine (hormone) problems as a result of changes in the function of a complex system of glands
Graves disease in childhood Antithyroid drug therapy
 83rd Annual Meeting of the ATA October 620, 203 Duration of antithyroid drugs treatment Disclosure Nothing to disclose Pr Juliane Léger Paediatric Endocrinology Department Paris Diderot University Hôpital
83rd Annual Meeting of the ATA October 620, 203 Duration of antithyroid drugs treatment Disclosure Nothing to disclose Pr Juliane Léger Paediatric Endocrinology Department Paris Diderot University Hôpital
optimal use of thyroid function tests (TFTs) to diagnose and monitor thyroid disease.
 Guidance for Thyroid Function Testing in Primary Care in Lothian In July 2006 following a lengthy consultation process, a joint working group comprising representatives from the Association of Clinical
Guidance for Thyroid Function Testing in Primary Care in Lothian In July 2006 following a lengthy consultation process, a joint working group comprising representatives from the Association of Clinical
Laboratory evaluation of thyroid function
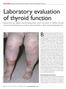 FEATURE: LAURA M. GUNDER, DHSC, MHE, PA-C, AND SARA HADDOW, MSA, PA-C Laboratory evaluation of thyroid function Blood tests can detect thyroid dysfunction, which can result in cardiac, GI, and menstrual
FEATURE: LAURA M. GUNDER, DHSC, MHE, PA-C, AND SARA HADDOW, MSA, PA-C Laboratory evaluation of thyroid function Blood tests can detect thyroid dysfunction, which can result in cardiac, GI, and menstrual
CLINICAL GUIDELINE FOR THE NEONATAL MANAGEMENT OF INFANTS BORN TO MOTHERS WITH THYROID DISEASE 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR THE NEONATAL MANAGEMENT OF INFANTS BORN TO MOTHERS WITH THYROID DISEASE 1. Aim/Purpose of this Guideline 1.1. This guideline applies to Neonatal/Paediatric and Midwifery/Obstetric
CLINICAL GUIDELINE FOR THE NEONATAL MANAGEMENT OF INFANTS BORN TO MOTHERS WITH THYROID DISEASE 1. Aim/Purpose of this Guideline 1.1. This guideline applies to Neonatal/Paediatric and Midwifery/Obstetric
TSH. TSH is an integral part of a thyroid panel useful for the determination and potential differentiation of hypothyroidism.
 TSH Background Thyroid hormone synthesis and secretion is regulated via a negative feed-back control system, which involves the hypothalamus, anterior pituitary, and the thyroid gland. Thyrotrophin-releasing
TSH Background Thyroid hormone synthesis and secretion is regulated via a negative feed-back control system, which involves the hypothalamus, anterior pituitary, and the thyroid gland. Thyrotrophin-releasing
Thyroid disease is second only to
 This is a corrected version of the article that appeared in print. Thyroid Disease in Pregnancy LEO A. CARNEY, DO, Naval Hospital Pensacola Family Medicine Residency Program, Pensacola, Florida JEFF D.
This is a corrected version of the article that appeared in print. Thyroid Disease in Pregnancy LEO A. CARNEY, DO, Naval Hospital Pensacola Family Medicine Residency Program, Pensacola, Florida JEFF D.
Hypothyroidism. Written by Donald Yung Edited by Dianna Louie. Basic Embryology and Anatomy
 Hypothyroidism Written by Donald Yung Basic Embryology and Anatomy The thyroid gland consists of two lobes connected by an isthmus and is located anterior to the trachea at the base of the neck. During
Hypothyroidism Written by Donald Yung Basic Embryology and Anatomy The thyroid gland consists of two lobes connected by an isthmus and is located anterior to the trachea at the base of the neck. During
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
A Parent s Guide to Understanding Congenital Hypothyroidism. Children s of Alabama Department of Pediatric Endocrinology
 A Parent s Guide to Understanding Congenital Hypothyroidism Children s of Alabama Department of Pediatric Endocrinology How did you get here? Every baby born in the state of Alabama is required by law
A Parent s Guide to Understanding Congenital Hypothyroidism Children s of Alabama Department of Pediatric Endocrinology How did you get here? Every baby born in the state of Alabama is required by law
Adrenal Insufficiency. Adrenal cortex secretions. Adrenal Insufficiency. Adrenal Insufficiency. Acute Adrenal Insufficiency
 Adrenal cortex secretions Cortisol secretion Diurnal pattern 24 hour secretion = Stress = demands 30 mg 300 mg to meet physiological Adrenal Insufficiency PRIMARY ADDISON S DISEASE Autoimmune Infection
Adrenal cortex secretions Cortisol secretion Diurnal pattern 24 hour secretion = Stress = demands 30 mg 300 mg to meet physiological Adrenal Insufficiency PRIMARY ADDISON S DISEASE Autoimmune Infection
Parents Guide To Primary Congenital Hypothyroidism
 Parents Guide To Primary Congenital Hypothyroidism California Department of Health Services Genetic Disease Branch www.dhs.ca.gov/gdb To Parents: California State Law requires that all babies have the
Parents Guide To Primary Congenital Hypothyroidism California Department of Health Services Genetic Disease Branch www.dhs.ca.gov/gdb To Parents: California State Law requires that all babies have the
Hypothyroidism clinical features and treatment. 1. The causes of hypothyroidism
 Hypothyroidism clinical features and treatment 1. The causes of hypothyroidism The thyroid is a gland in the neck which makes two thyroid hormones, thyroxine (T4) and tri-iodothyronine (T3). Thyroxine
Hypothyroidism clinical features and treatment 1. The causes of hypothyroidism The thyroid is a gland in the neck which makes two thyroid hormones, thyroxine (T4) and tri-iodothyronine (T3). Thyroxine
Thyroid pathology in the Presence of antiviral treatment of chronic hepatitis C. Professor Nikitin Igor G Russian State Medical University MOSCOW
 Thyroid pathology in the Presence of antiviral treatment of chronic hepatitis C Professor Nikitin Igor G Russian State Medical University MOSCOW The structure of the side effects associated with antiviral
Thyroid pathology in the Presence of antiviral treatment of chronic hepatitis C Professor Nikitin Igor G Russian State Medical University MOSCOW The structure of the side effects associated with antiviral
Congenital hypothyroidism and your child
 Screening Programmes Congenital hypothyroidism and your child What is congenital hypothyroidism (CHT)? About 1 in 3000 babies born in the UK has CHT. Congenital means the baby is born with the condition.
Screening Programmes Congenital hypothyroidism and your child What is congenital hypothyroidism (CHT)? About 1 in 3000 babies born in the UK has CHT. Congenital means the baby is born with the condition.
Goiter. This reference summary explains goiters. It covers symptoms and causes of the condition, as well as treatment options.
 Goiter Introduction The thyroid gland is located at the base of your neck. If the gland becomes abnormally enlarged, it is called a goiter. Goiters usually do not cause pain. But a large goiter could cause
Goiter Introduction The thyroid gland is located at the base of your neck. If the gland becomes abnormally enlarged, it is called a goiter. Goiters usually do not cause pain. But a large goiter could cause
Blood Pressure Management and Your Pregnancy
 Patient Education Blood Pressure Management and Your Pregnancy This handout explains: How your blood pressure is checked during pregnancy. What preeclampsia is, including risk factors, treatments, and
Patient Education Blood Pressure Management and Your Pregnancy This handout explains: How your blood pressure is checked during pregnancy. What preeclampsia is, including risk factors, treatments, and
NHS FORTH VALLEY Thyroid Storm
 NHS FORTH VALLEY Thyroid Storm Date of First Issue 01 August 2006 Approved 01 August 2006 Current Issue Date 1 st July 2016 Review Date 1 st July 2018 Version EQIA Yes 01/08/2010 Author / Contact Group
NHS FORTH VALLEY Thyroid Storm Date of First Issue 01 August 2006 Approved 01 August 2006 Current Issue Date 1 st July 2016 Review Date 1 st July 2018 Version EQIA Yes 01/08/2010 Author / Contact Group
Down s Syndrome Association Medical Series. Notes for parents & carers
 An updated version of one of a series of leaflets available from the Down s Syndrome Association Down s Syndrome Association Medical Series 1. THYROID DISORDER AMONG PEOPLE WITH DOWN S SYNDROME Notes for
An updated version of one of a series of leaflets available from the Down s Syndrome Association Down s Syndrome Association Medical Series 1. THYROID DISORDER AMONG PEOPLE WITH DOWN S SYNDROME Notes for
Thyroid Dysfunction in the Elderly. Rund Tahboub, MD University Hospitals Case Western Reserve University
 Thyroid Dysfunction in the Elderly Rund Tahboub, MD University Hospitals Case Western Reserve University Outline Normal thyroid physiology, regulation and action Changes in thyroid function with aging
Thyroid Dysfunction in the Elderly Rund Tahboub, MD University Hospitals Case Western Reserve University Outline Normal thyroid physiology, regulation and action Changes in thyroid function with aging
Oxford Centre for Head and Neck Oncology The Thyroid Gland and Thyroid Cancer Information for patients
 Oxford University Hospitals NHS Trust Oxford Centre for Head and Neck Oncology The Thyroid Gland and Thyroid Cancer Information for patients What is the thyroid gland? The thyroid gland is an endocrine
Oxford University Hospitals NHS Trust Oxford Centre for Head and Neck Oncology The Thyroid Gland and Thyroid Cancer Information for patients What is the thyroid gland? The thyroid gland is an endocrine
Thyroid disease, which is actually
 Toxicology Thyroid Storm During Pregnancy A Medical Emergency Patricia A. Waltman, RN, EdD, CNNP Joyce M. Brewer, RN, MSN, CS, CNM, CFNP Sharon Lobert, RN, PhD Thyroid disease, which is actually several
Toxicology Thyroid Storm During Pregnancy A Medical Emergency Patricia A. Waltman, RN, EdD, CNNP Joyce M. Brewer, RN, MSN, CS, CNM, CFNP Sharon Lobert, RN, PhD Thyroid disease, which is actually several
Chickenpox in pregnancy: what you need to know
 Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Thyroid Cancer Finding It and Treating It Using Radioiodine
 Thyroid Cancer Finding It and Treating It Using Radioiodine Your doctor has referred you to Nuclear Medicine to learn more about the extent of your thyroid cancer, and perhaps even for treatment of the
Thyroid Cancer Finding It and Treating It Using Radioiodine Your doctor has referred you to Nuclear Medicine to learn more about the extent of your thyroid cancer, and perhaps even for treatment of the
Neuroendocrine Evaluation
 Neuroendocrine Evaluation When women have health concerns they usually prefer to discuss them with another woman. Dr. Vliet is a national expert on hormone-related problems and specializes in neuroendocrine
Neuroendocrine Evaluation When women have health concerns they usually prefer to discuss them with another woman. Dr. Vliet is a national expert on hormone-related problems and specializes in neuroendocrine
PATIENT HISTORY FORM
 PATIENT HISTORY FORM If you are new to the office, have not been seen in over one (1) year, or are returning for a new problem, please complete this form in full. If there have been any changes since your
PATIENT HISTORY FORM If you are new to the office, have not been seen in over one (1) year, or are returning for a new problem, please complete this form in full. If there have been any changes since your
Zika Virus. Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases
 Zika Virus Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases What is the incubation period for Zika virus infection? Unknown but likely to be several
Zika Virus Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases What is the incubation period for Zika virus infection? Unknown but likely to be several
BCCA Protocol Summary for Palliative Treatment of Advanced Pancreatic Neuroendocrine Tumours using SUNItinib (SUTENT )
 BCCA Protocol Summary for Palliative Treatment of Advanced Pancreatic Neuroendocrine Tumours using SUNItinib (SUTENT ) Protocol Code Tumour Group Contact Physician UGIPNSUNI Gastrointestinal Dr. Hagen
BCCA Protocol Summary for Palliative Treatment of Advanced Pancreatic Neuroendocrine Tumours using SUNItinib (SUTENT ) Protocol Code Tumour Group Contact Physician UGIPNSUNI Gastrointestinal Dr. Hagen
Endocrine Module (PYPP 5260), Thyroid Section, Spring 2002 THYROID HORMONE TUTORIAL: THYROID PATHOLOGY. Jack DeRuiter
 I. INTRODUCTION Endocrine Module (PYPP 5260), Thyroid Section, Spring 2002 THYROID HORMONE TUTORIAL: THYROID PATHOLOGY Jack DeRuiter Thyroid disorder is a general term representing several different diseases
I. INTRODUCTION Endocrine Module (PYPP 5260), Thyroid Section, Spring 2002 THYROID HORMONE TUTORIAL: THYROID PATHOLOGY Jack DeRuiter Thyroid disorder is a general term representing several different diseases
2. What Should Advocates Know About Diabetes? O
 2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
Institute of Ophthalmology. Thyroid Eye Disease. aka Thyroid Associated Ophthalmopathy
 Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Management of Clients with Thyroid and Parathyroid Disorders
 Management of Clients with Thyroid and Parathyroid Disorders Black, J.M. & Hawks, J.H. (2005) Chapters 45, (pp 1191-1216) 1216) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey,
Management of Clients with Thyroid and Parathyroid Disorders Black, J.M. & Hawks, J.H. (2005) Chapters 45, (pp 1191-1216) 1216) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey,
The Development and Treatment of Hypothyroidism
 The Development and Treatment of Hypothyroidism Release Date: 04/05/2012 Expiration Date: 04/05/2015 FACULTY: Meg Brannagan, RN FACULTY AND ACCREDITOR DISCLOSURE STATEMENTS: Meg Brannagan has no actual
The Development and Treatment of Hypothyroidism Release Date: 04/05/2012 Expiration Date: 04/05/2015 FACULTY: Meg Brannagan, RN FACULTY AND ACCREDITOR DISCLOSURE STATEMENTS: Meg Brannagan has no actual
MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families
 MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lee S. Cohen, MD, and Lori L. Altshuler, MD www.womensmentalhealth.org
MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lee S. Cohen, MD, and Lori L. Altshuler, MD www.womensmentalhealth.org
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
GESTATIONAL DIABETES. Diabete Gestazionale (Lingua Inglese)
 GESTATIONAL DIABETES Diabete Gestazionale (Lingua Inglese) CONTENTS DEFINITION 03 WHAT CAUSES AND HOW TO MANAGE GESTATIONAL DIABETES 04 HOW TO CONTROL DIABETES 06 CORRECT LIFESTYLE 08 DURING AND AFTER
GESTATIONAL DIABETES Diabete Gestazionale (Lingua Inglese) CONTENTS DEFINITION 03 WHAT CAUSES AND HOW TO MANAGE GESTATIONAL DIABETES 04 HOW TO CONTROL DIABETES 06 CORRECT LIFESTYLE 08 DURING AND AFTER
Parvovirus B19 Infection in Pregnancy
 Parvovirus B19 Infection in Pregnancy Information Pack Parvovirus B19 Infection in Pregnancy Information Booklet CONTENTS: THE VIRUS page 3 CLINICAL MANIFESTATIONS page 6 DIAGNOSIS page 8 PATIENT MANAGEMENT
Parvovirus B19 Infection in Pregnancy Information Pack Parvovirus B19 Infection in Pregnancy Information Booklet CONTENTS: THE VIRUS page 3 CLINICAL MANIFESTATIONS page 6 DIAGNOSIS page 8 PATIENT MANAGEMENT
Thyroid Hormone Replacement
 Thyroid Hormone Replacement Name: Levothyroxine is the generic name for all thyroid hormone that replaces T4. Recommended Brand names are Synthroid and Levoxyl What is levothyroxine? Levothyroxine is synthetic
Thyroid Hormone Replacement Name: Levothyroxine is the generic name for all thyroid hormone that replaces T4. Recommended Brand names are Synthroid and Levoxyl What is levothyroxine? Levothyroxine is synthetic
Screening for Thyroid Disease
 This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or a basis for reimbursement and coverage policies. AHRQ
This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or a basis for reimbursement and coverage policies. AHRQ
Recovering with T3 - by Paul Robinson. Introduction
 Recovering with T3 - by Paul Robinson Introduction I am not a professional writer. Neither am I a doctor, a medical researcher or a biochemist. I am simply a man who has had his life derailed by thyroid
Recovering with T3 - by Paul Robinson Introduction I am not a professional writer. Neither am I a doctor, a medical researcher or a biochemist. I am simply a man who has had his life derailed by thyroid
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Lakeview Endocrinology and Diabetes Consultants. 2719 N Halsted St C-1. Chicago IL 60614 P: 773 388 5685 F: 773 388 5687. www.lakeviewendocrinolgy.
 Lakeview Endocrinology and Diabetes Consultants 2719 N Halsted St C-1 Chicago IL 60614 P: 773 388 5685 F: 773 388 5687 www.lakeviewendocrinolgy.com Patient information: Early menopause (premature ovarian
Lakeview Endocrinology and Diabetes Consultants 2719 N Halsted St C-1 Chicago IL 60614 P: 773 388 5685 F: 773 388 5687 www.lakeviewendocrinolgy.com Patient information: Early menopause (premature ovarian
Hypothyroidism and Depression: Use of TSH as a Diagnostic Tool and the Role of Thyroid Supplement Therapy in Psychiatric Practice
 Hypothyroidism and Depression: Use of TSH as a Diagnostic Tool and the Role of Thyroid Supplement Therapy in Psychiatric Practice By Scott McDonald, DO PGY1 Hypothyroidism General medicine texts always
Hypothyroidism and Depression: Use of TSH as a Diagnostic Tool and the Role of Thyroid Supplement Therapy in Psychiatric Practice By Scott McDonald, DO PGY1 Hypothyroidism General medicine texts always
DEPRESSION DURING THE TRANSITION TO MENOPAUSE: A Guide for Patients and Families
 DEPRESSION DURING THE TRANSITION TO MENOPAUSE: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lori L. Altshuler, MD, and Lee S. Cohen, MD www.womensmentalhealth.org
DEPRESSION DURING THE TRANSITION TO MENOPAUSE: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lori L. Altshuler, MD, and Lee S. Cohen, MD www.womensmentalhealth.org
Paxil/Paxil-CR (paroxetine)
 Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
First Trimester Screening for Down Syndrome
 First Trimester Screening for Down Syndrome What is first trimester risk assessment for Down syndrome? First trimester screening for Down syndrome, also known as nuchal translucency screening, is a test
First Trimester Screening for Down Syndrome What is first trimester risk assessment for Down syndrome? First trimester screening for Down syndrome, also known as nuchal translucency screening, is a test
A publication of the American Thyroid Association (ATA) www.thyroid.org
 HYPOTHYROIDISM A BOOKLET FOR PATIENTS AND THEIR FAMILIES A publication of the American Thyroid Association (ATA) www.thyroid.org COPYRIGHT 2013 AMERICAN THYROID ASSOCIATION THE AMERICAN THYROID ASSOCIATION
HYPOTHYROIDISM A BOOKLET FOR PATIENTS AND THEIR FAMILIES A publication of the American Thyroid Association (ATA) www.thyroid.org COPYRIGHT 2013 AMERICAN THYROID ASSOCIATION THE AMERICAN THYROID ASSOCIATION
Neural Tube Defects - NTDs
 Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
TSH assay is used as the primary newborn screening test for congenital hypothyroidism (CH).
 Guidelines for Management of Congenital Hypothyroidism Summary Please refer to the full Guidelines below for details. 1. Diagnosis TSH assay is used as the primary newborn screening test for congenital
Guidelines for Management of Congenital Hypothyroidism Summary Please refer to the full Guidelines below for details. 1. Diagnosis TSH assay is used as the primary newborn screening test for congenital
Crohn's disease and pregnancy.
 Gut, 1984, 25, 52-56 Crohn's disease and pregnancy. R KHOSLA, C P WILLOUGHBY, AND D P JEWELL From the Gastroenterology Unit, Radcliffe Infirmary, Oxford SUMMARY Infertility and the outcome of pregnancy
Gut, 1984, 25, 52-56 Crohn's disease and pregnancy. R KHOSLA, C P WILLOUGHBY, AND D P JEWELL From the Gastroenterology Unit, Radcliffe Infirmary, Oxford SUMMARY Infertility and the outcome of pregnancy
The clinical spectrum of thyroid disease varies
 R e v i e w o f C l i n i c a l S i g n s Series Editor: Bernard M. Karnath, MD Signs and Symptoms of Thyroid Dysfunction Bernard M. Karnath, MD Nasir Hussain, MD The clinical spectrum of thyroid disease
R e v i e w o f C l i n i c a l S i g n s Series Editor: Bernard M. Karnath, MD Signs and Symptoms of Thyroid Dysfunction Bernard M. Karnath, MD Nasir Hussain, MD The clinical spectrum of thyroid disease
Polycystic ovary syndrome: what it means for your long-term health
 Polycystic ovary syndrome: what it means for your long-term health Information for you Published in February 2005, minor amendments in June 2005 Revised 2009 What is polycystic ovary syndrome? Polycystic
Polycystic ovary syndrome: what it means for your long-term health Information for you Published in February 2005, minor amendments in June 2005 Revised 2009 What is polycystic ovary syndrome? Polycystic
Hyperthyroidism & Hypothyroidism
 Hyperthyroidism & Hypothyroidism TSH: 7,1 mu/l (?) Overview 1. Thyroid physiology 2. Hypothyroidism 3. Hyperthyroidism 4. Tumors 5. Case History 1-6 The Thyroid gland and its downward migration Failure
Hyperthyroidism & Hypothyroidism TSH: 7,1 mu/l (?) Overview 1. Thyroid physiology 2. Hypothyroidism 3. Hyperthyroidism 4. Tumors 5. Case History 1-6 The Thyroid gland and its downward migration Failure
Steroids. What are steroids?
 Steroids What are steroids? Also known as corticosteroids and glucocorticoids, steroids are hormones that are normally produced by the adrenal glands. They are mainly used in multiple sclerosis (MS) because
Steroids What are steroids? Also known as corticosteroids and glucocorticoids, steroids are hormones that are normally produced by the adrenal glands. They are mainly used in multiple sclerosis (MS) because
New Estimates of the Economic Benefits of Newborn Screening for Congenital Hypothyroidism in the US
 The findings and conclusions in this presentation have not been formally disseminated by the Centers for Disease Control and Prevention and should not be construed to represent any agency determination
The findings and conclusions in this presentation have not been formally disseminated by the Centers for Disease Control and Prevention and should not be construed to represent any agency determination
Patient Guide. Important information for patients starting therapy with LEMTRADA (alemtuzumab)
 Patient Guide Important information for patients starting therapy with LEMTRADA (alemtuzumab) This medicinal product is subject to additional monitoring. This will allow quick identification of new safety
Patient Guide Important information for patients starting therapy with LEMTRADA (alemtuzumab) This medicinal product is subject to additional monitoring. This will allow quick identification of new safety
Benign Pituitary Tumor
 PATIENT EDUCATION patienteducation.osumc.edu The pituitary gland is a small, pea-sized endocrine gland in the center of the brain. Also known as the master gland, the pituitary gland helps control the
PATIENT EDUCATION patienteducation.osumc.edu The pituitary gland is a small, pea-sized endocrine gland in the center of the brain. Also known as the master gland, the pituitary gland helps control the
X-Plain Low Testosterone Reference Summary
 X-Plain Low Testosterone Reference Summary Introduction Testosterone is the most important male sex hormone. It helps the body produce and maintain adult male features. Low levels of testosterone affect
X-Plain Low Testosterone Reference Summary Introduction Testosterone is the most important male sex hormone. It helps the body produce and maintain adult male features. Low levels of testosterone affect
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
www.healthoracle.org 1
 How does hair grow and should it recycle? A single hair follicle grows its hair strand over a period of four to six years (the anagen phase). It then rests for two to four months (the telogen phase), after
How does hair grow and should it recycle? A single hair follicle grows its hair strand over a period of four to six years (the anagen phase). It then rests for two to four months (the telogen phase), after
I will be having surgery and radiation treatment for breast cancer. Do I need drug treatment too?
 What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
What is node-positive breast cancer? Node-positive breast cancer means that cancer cells from the tumour in the breast have been found in the lymph nodes (sometimes called glands ) in the armpit area.
Cancer of the Thyroid Explained
 Cancer of the Thyroid Explained Patient Information Introduction This leaflet tells you about the condition known as thyroid cancer. We hope it will answer some of the questions that you or those who care
Cancer of the Thyroid Explained Patient Information Introduction This leaflet tells you about the condition known as thyroid cancer. We hope it will answer some of the questions that you or those who care
Abnormal Uterine Bleeding
 Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Preconception Clinical Care for Women Medical Conditions
 Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Darren Lackan, MD Chris Bajaj, DO Anjanette Tan, MD Christopher Hudak, MD
 Darren Lackan, MD Chris Bajaj, DO Anjanette Tan, MD Christopher Hudak, MD I-131 (Radioactive Iodine) Treatment Patient Name: : Out of courtesy, our office expects 24 hour notice for the cancellation of
Darren Lackan, MD Chris Bajaj, DO Anjanette Tan, MD Christopher Hudak, MD I-131 (Radioactive Iodine) Treatment Patient Name: : Out of courtesy, our office expects 24 hour notice for the cancellation of
HCSP GUIDES A GUIDE TO: PREPARING FOR TREATMENT. A publication of the Hepatitis C Support Project
 HCSP GUIDES T R E AT M E N T I S S U E S A publication of the Hepatitis C Support Project The information in this guide is designed to help you understand and manage HCV and is not intended as medical
HCSP GUIDES T R E AT M E N T I S S U E S A publication of the Hepatitis C Support Project The information in this guide is designed to help you understand and manage HCV and is not intended as medical
Patient & Family Guide Pre-Existing Diabetes and Pregnancy
 Patient & Family Guide Pre-Existing Diabetes and Pregnancy Center for Perinatal Care Meriter Hospital 202 S. Park Street Madison, WI 53715 608.417.6667 meriter.com 09/12/1000 A Meriter Hospital and University
Patient & Family Guide Pre-Existing Diabetes and Pregnancy Center for Perinatal Care Meriter Hospital 202 S. Park Street Madison, WI 53715 608.417.6667 meriter.com 09/12/1000 A Meriter Hospital and University
AACE Thyroid Task Force. Chairman H. Jack Baskin, MD, MACE
 AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS MEDICAL GUIDELINES FOR CLINICAL PRACTICE FOR THE EVALUATION AND TREATMENT OF HYPERTHYROIDISM AND HYPOTHYROIDISM AACE Thyroid Task Force Chairman H. Jack
AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS MEDICAL GUIDELINES FOR CLINICAL PRACTICE FOR THE EVALUATION AND TREATMENT OF HYPERTHYROIDISM AND HYPOTHYROIDISM AACE Thyroid Task Force Chairman H. Jack
About Postpartum Depression and other Perinatal Mood Disorders
 About Postpartum Depression and other Perinatal Mood Disorders The entire period of pregnancy up to one year after delivery is described as the perinatal period. Many physical and emotional changes occur
About Postpartum Depression and other Perinatal Mood Disorders The entire period of pregnancy up to one year after delivery is described as the perinatal period. Many physical and emotional changes occur
THYROGEN-STIMULATED RADIOACTIVE IODINE (I-131) THERAPY FOR THYROID CANCER FOLLOWED BY WHOLE BODY SCAN
 MANFRED BLUM, M.D. F.A.C.P. NYU School of Medicine 530 First Avenue New York, N.Y. 10016 OFFICE:Phone (212) 263-7444 Fax (212) 263-0401 LAB: Phone (212) 263-7410 Fax: (212) 263-7519 Rev.7/1/09 FORM 4B
MANFRED BLUM, M.D. F.A.C.P. NYU School of Medicine 530 First Avenue New York, N.Y. 10016 OFFICE:Phone (212) 263-7444 Fax (212) 263-0401 LAB: Phone (212) 263-7410 Fax: (212) 263-7519 Rev.7/1/09 FORM 4B
Healing Depression Naturally
 Healing Depression Naturally By Peter Bongiorno ND, LAc and Pina LoGiudice ND, LAc Directors of Inner Source Health (www.innersourcehealth.com) While everyone experiences the blues from time to time, depression
Healing Depression Naturally By Peter Bongiorno ND, LAc and Pina LoGiudice ND, LAc Directors of Inner Source Health (www.innersourcehealth.com) While everyone experiences the blues from time to time, depression
Associates in Pediatric & Adult Urology, PA A division of Garden State Urology 282 Route 46 PO Box 1160 Denville, NJ 07834
 Associates in Pediatric & Adult Urology, PA A division of Garden State Urology 282 Route 46 PO Box 1160 Denville, NJ 07834 Dear New Patient: Welcome to Associates in Pediatric and Adult Urology, PA, a
Associates in Pediatric & Adult Urology, PA A division of Garden State Urology 282 Route 46 PO Box 1160 Denville, NJ 07834 Dear New Patient: Welcome to Associates in Pediatric and Adult Urology, PA, a
Post-Coital Hormonal Contraception Instructions for Use of Plan B, Plan B One-Step, Next Choice One Dose, My Way, Generic Levonorgestrel and Ella
 Post-Coital Hormonal Contraception Instructions for Use of Plan B, Plan B One-Step, Next Choice One Dose, My Way, Generic Levonorgestrel and Ella Several options for emergency birth control exist for women
Post-Coital Hormonal Contraception Instructions for Use of Plan B, Plan B One-Step, Next Choice One Dose, My Way, Generic Levonorgestrel and Ella Several options for emergency birth control exist for women
Polymyalgia Rheumatica www.arthritis.org.nz
 Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
How is Your Brain Working Now? A Questionnaire for Hypothyroid Patients
 How is Your Brain Working Now? A Questionnaire for Hypothyroid Patients In the Volume XIII, Number 1 issue of The Bridge, we asked patients who had formerly been hyperthyroid how they felt. Most thyroidologists
How is Your Brain Working Now? A Questionnaire for Hypothyroid Patients In the Volume XIII, Number 1 issue of The Bridge, we asked patients who had formerly been hyperthyroid how they felt. Most thyroidologists
SCRIPT NUMBER 88 FOOD POISONING (ONE SPEAKER)
 SCRIPT NUMBER 88 FOOD POISONING (ONE SPEAKER) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: FOOD POISONING PROGRAM NUMBER: 88 SUBJECT: CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF FOOD POISONING KEY WORDS:
SCRIPT NUMBER 88 FOOD POISONING (ONE SPEAKER) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: FOOD POISONING PROGRAM NUMBER: 88 SUBJECT: CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF FOOD POISONING KEY WORDS:
