How To Have A Gallbladder Removed
|
|
|
- Lewis Stuart Jefferson
- 3 years ago
- Views:
Transcription
1 Laparoscopic removal of your gallbladder General Surgery Patient Information Leaflet Introduction This leaflet is about laparoscopic (keyhole) removal of the gallbladder for those who are considering this operation. It gives information on the operation, its benefits, risks and how people feel afterwards. What is the gallbladder? The gallbladder lies behind your right ribs at the front, below the liver and above the duodenum. The duodenum is the first part of the intestine immediately after the stomach. The gallbladder is a pouch that stores bile. Bile is the digestive fluid produced by the liver that helps to break down fatty foods. Bile is carried from the liver to the gallbladder and from there to the gut by tubing called bile ducts.
2 Bile is made from cholesterol, bile salts and waste products. When these substances are out of balance, small, hard stones called gallstones can form. The stones form in the gallbladder and often cause pain. Occasionally the stones can cause the gallbladder to become irritated and inflamed. If stones escape from the gallbladder, they can block the bile ducts, causing pain, fever and yellow jaundice. Why remove the gallbladder? If your gallbladder is diseased and inflamed, it will continue to cause problems unless it is removed. If only the stones are removed, new ones are likely to form. What does the operation consist of? We take out your gallbladder and the stones in it. We have already checked that there are no stones, as far as we can tell, in your bile ducts. Some patients have already had their bile ducts cleared of stones. In your case, we should be able to do the operation using keyhole surgery. This means making three cuts about a centimetre long in front of your tummy, plus another in your navel (belly button). We pass a very long narrow telescope called a laparoscope through one of the cuts. Using this, we can see what is going on inside your tummy on a television screen. We pass special narrow instruments through the other cuts. We free the gallbladder and draw it out through one of the cuts. The medical name of this removal is a cholecystectomy. Then we close the cuts with stitches under the skin. The operation is carried out using a general anaesthetic which means that you will be asleep. Most patients can go home either the same day or the next day after this operation. Rarely after starting the operation, we find that we cannot safely take out the gallbladder this way. Then we need to make a bigger cut to do the job. We can only tell at the time of the operation. This will usually mean being in hospital for two to three days. 2
3 What are the benefits of the operation? Removing a diseased and inflamed gallbladder will stop the pain you have been experiencing. What are the risks? As with any operation, there are some risks. These may relate to any operation, or specifically to this operation. Risks relating to any operation You may develop an infection at the site of the cuts. We will give you antibiotics to reduce this risk. You may develop a chest infection after the operation. To help prevent this, we will encourage you to get moving as soon as possible after the operation. A physiotherapist will advise you about breathing exercises. If you smoke, it is a good idea to give up at least a week before the operation. You may develop a blood clot (thrombosis) in the veins of your legs. Rarely, part of the clot may break off and travel to your lungs. This is known as pulmonary embolism and can be very dangerous. To reduce this risk, we may give you anti-embolism stockings. Some patients are given an injection of a blood-thinning drug called enoxaparin once a day while they are in hospital. Moving around after your operation will also help prevent blood clots from forming. Although we carry out heart checks before an operation, very rarely unforeseen problems can occur, such as a heart attack or heart failure. You will have a needle inserted into your hand or arm to give you fluids and drugs during the operation. The site of the needle entry can become inflamed and painful. Rarely an ulcer can develop. 3
4 During the operation, an electrical instrument called a diathermy will be used to stop any bleeding from small vessels. To use this, we have to put a pad directly onto the skin, usually on the leg. We may need to shave this area. Very rarely, some people experience a reaction under this pad, which may cause a burn. Some people have bleeding after the operation. If this happens, you may need another operation to stop it. Risks relating specifically to this operation In some cases, the operation is too difficult to perform using keyhole surgery and the surgeon has to carry out open surgery. This can mean you have a longer recovery time. The keyhole instruments used to remove the gallbladder can injure surrounding structures, such as the intestine, bowel and blood vessels. The risk is increased if the gallbladder is inflamed. This type of injury is rare and can usually be repaired at the time of the operation. Sometimes injuries are noticed afterwards and a further operation is needed. Damage to the bile ducts can occur which would require a bigger operation to repair the damage. A stone may escape from the gallbladder and get stuck in the duct. Usually, the stone can be removed at a later date using a telescope passed through the mouth and into the stomach. When the gallbladder is removed, special clips are used to seal the tube that connects the gallbladder to the main bile duct that drains the liver. The clips may come off and this may result in a leakage of bile into the abdomen. This can be controlled using a telescope passed through the mouth, or a second operation may be advised. Complications are unusual but are rapidly recognised and dealt with by the nursing and surgical staff. If you think that all is not well, please ask the nurses or doctors. 4
5 You may feel aches and twinges in the wounds for up to six months after the operation. Occasionally, some people have numb patches in the skin around the wound. This may take about two to three months to get better. Complications of anaesthetics You may react to any of the anaesthetic drugs. These reactions are recognised and anticipated by the anaesthetist and usually cause no permanent damage. Feeling or being sick is one of the most common problems after an operation. If you feel sick, please speak to a nurse as we can give you anti-sickness medicine. Chest infections are more common after surgery in patients who smoke or who have chest problems. The anaesthetic gases can affect secretions in the lungs and it is harder to cough them up after the operation, when it hurts to do so. If you have a smoker s cough, this may be worse. The physiotherapists will help you to cough and clear your chest. During the operation, you will have a tube inserted into your throat. For this reason you may have a sore throat for a while afterwards. Occasionally, there may be difficulty introducing a tube for breathing into your windpipe. You may receive a letter about this from the anaesthetist after your operation. The importance of this is to highlight the problem so that if in the future you need another operation, you can warn the anaesthetist by showing them this letter. There are other unusual complications that are not listed in this brief overview. However, if you ask the anaesthetist who visits you before the operation, he or she will be happy to go into as much detail as you wish. If you have any particular worry, write it down so that you do not forget to ask about it. 5
6 Modern anaesthetics are very safe and the complications are very rare. Remember there are over three million patients having anaesthetics every year in this country, and only very few have any sort of problem, if they are fit and well before the operation. Are there any alternatives? If you leave things as they are, you are likely to have more of the same symptoms. This may be more episodes of pain from the gallbladder, which are unpleasant although not dangerous. If you have had only one attack of pain, you may like to wait and see. If you feel you could not cope with the operation, and especially if you are over seventy years old, this is worth thinking about. However, if you have had yellow jaundice, or pancreatitis, you can get seriously ill if you have another attack. Research has shown that dissolving the stones away by drug treatment has been disappointing. It takes many months of treatment. Often the drug cannot get into the gallbladder. The stones may not dissolve away if they are big or chalky. The stones come back after the treatment has stopped. Shock wave treatment has been tried but with very disappointing results. At the present time, it just makes the results from drug treatment a little better. What happens before the operation? We will give you a date to come to the pre-admission unit. Here you will have a health assessment with a nurse. This will determine whether there are any reasons why you should not have surgery. During this health assessment we will: Check your suitability for anaesthetic. Give you information about the surgery and recovery process. It is important that you know what to do to help your recovery. Carry out investigations to ensure that you are fit and well to have the surgery. 6
7 A range of investigations will be carried out such as: A blood test, if you take certain medications. You may have an ECG a heart trace test. This is nothing to be alarmed about, just a routine test to check your heart. Your blood pressure, pulse and weight will be recorded. You will be screened for MRSA a nasal and groin swab will be taken to see if you have any evidence of infection. A finger prick test to check your blood glucose levels. You will have the opportunity to ask any questions or discuss any problems you may have. At this assessment, please tell us if: You are diabetic. You have a cold, cough or any type of infection. You take any medications and what these are. You may need to stop taking some of these for a short period of time before you have the operation. For women who are on the pill or HRT, please tell your surgeon. We may discuss the option of stopping these four weeks before surgery. Another option may be to go ahead with the surgery, with or without additional measures to reduce the risks associated with the pill and HRT. This will be discussed with you in more detail. Eating and drinking before the operation We will give you instructions about when you need to stop eating and drinking before your operation. Usually, you can eat normally until about six to 12 hours before the operation. After this, you will not be able to eat or drink anything until after your operation. This will let your stomach empty to make sure you are not sick during your operation. 7
8 What if I become ill before my operation? It is important that you tell us if you are not well enough to come in for the operation. Please ring the following number: Surgical Assessment Unit (SAU) on ext. 3359, ext or ext Also, please ring us if you have any type of infection such as: a chesty cough, cold or throat infection skin problems such as a rash, cut or skin infection, especially if it is on the area that is to be operated on diarrhoea and sickness in the last 48 hours If you are not sure and want to ask about this, please ring for advice. What do I need to bring for my operation? Please bring a dressing gown, slippers and any medication you are currently taking. About half of the patients having this operation will only be in hospital for the day but in case you need to stay overnight, please bring an overnight bag with nightwear, toiletries etc. Please do not wear or bring any jewellery. However, you can wear your wedding ring. Please do not wear any make up; or nail varnish or gel nails on your fingers or toes. Personal property The Dudley Group NHS Foundation Trust and its staff cannot be held responsible for the personal property of patients or visitors. You are advised not to bring valuable items with you. Where this is unavoidable, please note that the hospital cannot accept responsibility for your property unless it is handed to a staff member for safekeeping and an official receipt is obtained. 8
9 What happens when I come for my operation? You will need to go to the Admissions Lounge where all your notes and the results of your tests will be ready. You will then be taken to a ward. The surgeon will see you first. They will check the results of your tests and explain the operation to you. If you are happy to go ahead with the operation, they will ask you to sign a consent form. If you are not clear about any part of the operation, ask for more details from the doctors or the nurses. They are never too busy to do this. One or more anaesthetists who will be giving your anaesthetic will talk to you and examine you. They will be especially interested in any chest troubles, dental treatment and any previous anaesthetics you have had. Tell them about any anaesthetic problems in the family. A nurse will check your blood pressure, temperature and pulse. They will talk through what will happen and check for your understanding of this. They will give you an approximate time for your operation. Unfortunately, you may sometimes have to wait for a number of hours for your surgery. We do appreciate how difficult and inconvenient this might be and we try to minimise delays for all patients as much as possible. The nurse will ask you to undress and put on a theatre gown shortly before your surgery. A nurse will take you to the operating theatre. A member of the theatre team will check your personal details with you. You will then be given the anaesthetic. What happens after the operation? Coming round after the anaesthetic Although you will be conscious a minute or two after the operation ends, you are unlikely to remember anything until you are back in your bed on the ward. 9
10 Some patients feel a bit sick for up to twelve hours after operation but this passes. We will give you some treatment for sickness if necessary. You will have a plastic intravenous tube (a drip) in an arm vein to give you fluids and drugs. You may be given oxygen from a facemask for a few hours. Recovering after a general anaesthetic The majority of patients recover very smoothly. You may be able to have a drink or a cup of tea once you are fully awake. After four to six hours, if you are feeling well, you may be able to eat a small amount of food. You may be able to sit out and walk about on the same day. During surgery, we give local anaesthetic injections along the cuts in your skin so that you feel comfortable after surgery. We will also give you painkiller tablets. It is important to make sure that you have passed water and empty your bladder a few hours after the procedure. You will be able to go home when you are comfortable and have recovered from the anaesthetic. We will give you an adequate supply of painkillers to take home and a supply of dressings, if necessary. With modern anaesthetics combined with safe techniques of surgery, usually we would expect a smooth recovery. At the moment, nearly 50 per cent of our patients having this operation are able to go home on the same day as surgery. If we have to leave a drain in your wound, or have had to convert to open surgery during the procedure, you may have to stay a bit longer in the hospital, until we feel that you are safe to go home. This is usually about two to three days. What happens when I go home? If you go home the same day as the operation, you will need to have someone to care for you for at least the first 24 hours. You must not drive yourself home. You will not be able to go home on public transport on your own. Therefore, you will need to arrange for someone to collect you and take you home. 10
11 When you leave hospital, the nurse will give you a letter for your GP, a sick note if you need it and any medication that has been prescribed for you. We will also give you a separate information leaflet about how to care for yourself after your operation. We will give you instructions on caring for your wound. You will need to keep your wound clean and dry. If you have any problems with your dressing, or any other queries, please contact: Surgical Assessment Unit (SAU) on ext. 3359, ext or ext Opening bowels It is quite normal for the bowels not to open for a day or so after the operation. If you have not opened your bowels after two days and you feel uncomfortable, take a mild laxative such as senna. Living without a gallbladder You can live without a gallbladder as although it is useful, it is not essential. Your liver will still produce bile to help digest food. However, some people who have had their gallbladder removed have symptoms of bloating and diarrhoea after eating certain foods, such as fatty or spicy food. If you find that certain foods do trigger symptoms, you may wish to avoid them in the future. Driving Some insurance companies do not insure drivers for a number of weeks after surgery so it is best to check what your policy says before starting to drive. You can start driving again when you can do an emergency stop without any discomfort. Do not drive if you have any pain that will distract you. Getting back to normal Most people are back to normal within a week or two of leaving hospital after keyhole surgery, and can get back to work and do gentle exercise. You can usually resume strenuous exercise or work after a month but your consultant will discuss this with you. Please note that recovery often takes longer after open surgery. 11
12 Can I find out more? You can find out more from the following weblinks: NHS Choices ntroduction.aspx The Royal College of Anaesthetists 12
13 If you have any questions, or if there is anything you do not understand about this leaflet, please contact: Surgical Assessment Unit (SAU) on ext. 3359, ext or ext Russells Hall Hospital switchboard number: This leaflet can be downloaded or printed from: If you have any feedback on this patient information leaflet, please Originator: H Ward, M Deeley, S Garratt. Date reviewed: December Next review due: December Version: 3. DGH ref: DGH/PIL/
Elective Laparoscopic Cholecystectomy
 General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
Biliary Stone Disease
 Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Name of procedure: Laparoscopic (key-hole) ovarian surgery. Left/ Right unilateral salpingo-oophorectomy* (removal of one fallopian tube and ovary)
 For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
Laparoscopic cholecystectomy. Golden Jubilee National Hospital NHS National Waiting Times Centre. Patient information guide
 Golden Jubilee National Hospital NHS National Waiting Times Centre Laparoscopic cholecystectomy Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Golden Jubilee National Hospital NHS National Waiting Times Centre Laparoscopic cholecystectomy Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
YOU AND YOUR ANAESTHETIC
 YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
An operation for prolapse Colpocleisis
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Umbilical or Paraumbilical Hernia Adults
 Umbilical or Paraumbilical Hernia Adults WHAT IS AN UMBILICAL OR PARAUMBILICAL HERNIA? 2 THE OPERATION? 2 ANY ALTERNATIVES 3 BEFORE THE OPERATION 3 AFTER YOUR SURGERY - IN HOSPITAL 4 POSSIBLE COMPLICATIONS?
Umbilical or Paraumbilical Hernia Adults WHAT IS AN UMBILICAL OR PARAUMBILICAL HERNIA? 2 THE OPERATION? 2 ANY ALTERNATIVES 3 BEFORE THE OPERATION 3 AFTER YOUR SURGERY - IN HOSPITAL 4 POSSIBLE COMPLICATIONS?
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Vaginal hysterectomy and vaginal repair
 Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
LAPAROSCOPIC GASTRIC BANDING
 LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
SlEEvE GASTRECTomY SURGERY What is a sleeve gastrectomy operation? BARIATRIC SURGERY
 Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy.
 Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients
 Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Inguinal (Groin) Hernia Repair
 Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy)
 Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
However, each person may be managed in a different way as bowel pattern is different in each person.
 Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
An operation for prolapse Laparoscopic Sacrohysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Laparoscopic Sacrohysteropexy Information for Patients What is a prolapse? Uterine prolapse is a bulge or lump in the vagina
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Laparoscopic Sacrohysteropexy Information for Patients What is a prolapse? Uterine prolapse is a bulge or lump in the vagina
Laparoscopic Cholecystectomy (Removal of the Gallbladder)
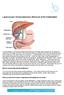 Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Stapedectomy / Stapedotomy / Surgery for Otosclerosis
 Patient information Stapedectomy / Stapedotomy / Surgery for Otosclerosis Ear, Nose and Throat Directorate PIF 230 V6 Your Consultant / Doctor has advised you to have a Stapedectomy / Stapedotomy / Surgery
Patient information Stapedectomy / Stapedotomy / Surgery for Otosclerosis Ear, Nose and Throat Directorate PIF 230 V6 Your Consultant / Doctor has advised you to have a Stapedectomy / Stapedotomy / Surgery
Epigastric Hernia Repair
 Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Cholangiocarcinoma (Bile Duct Cancer) Patient Information Booklet
 Cholangiocarcinoma (Bile Duct Cancer) Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Cholangiocarcinoma (Bile Duct Cancer) Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Spigelian Hernia Repair
 Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
LASER TREATMENT FOR VARICOSE VEINS
 LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Liver Resection. Patient Information Booklet. Delivering the best in care. UHB is a no smoking Trust
 Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Percutaneous Endoscopic Gastrostomy (PEG) removal
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Sigmoid Colectomy Your Operation Explained
 Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Keyhole (Laparoscopic) Surgery
 Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
Having a laparoscopic sterilisation
 Having a laparoscopic sterilisation This booklet has been written to provide information about your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions
Having a laparoscopic sterilisation This booklet has been written to provide information about your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Removal of the Submandibular Salivary Gland
 Department of Oral and Maxillofacial Surgery Removal of the Submandibular Salivary Gland Information for patients This leaflet will help you understand your treatment and should answer many of the questions
Department of Oral and Maxillofacial Surgery Removal of the Submandibular Salivary Gland Information for patients This leaflet will help you understand your treatment and should answer many of the questions
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Having a Trans-Arterial Embolisation
 Having a Trans-Arterial Embolisation Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a Trans-Arterial Embolisation Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk PROCEDURE-
Cardiac Catheter Lab Information for patients having a Coronary Angiogram
 Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Hysteroscopy (Out Patient, Day Case or In Patient)
 Hysteroscopy (Out Patient, Day Case or In Patient) Exceptional healthcare, personally delivered Introduction This leaflet explains the procedure of hysteroscopy. If you have any other questions do not
Hysteroscopy (Out Patient, Day Case or In Patient) Exceptional healthcare, personally delivered Introduction This leaflet explains the procedure of hysteroscopy. If you have any other questions do not
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Name of procedure: Squint Surgery (Child)
 Eye Surgery Surgical procedure information leaflet Name of procedure: Squint Surgery (Child) This leaflet is for parents whose child has a squint that may be helped by an operation. In this leaflet we
Eye Surgery Surgical procedure information leaflet Name of procedure: Squint Surgery (Child) This leaflet is for parents whose child has a squint that may be helped by an operation. In this leaflet we
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Vesico-Vaginal Fistula
 Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Undergoing an Oesophageal Endoscopic Resection (ER)
 Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Having a RIG tube inserted
 Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
UNDERGOING OESOPHAGEAL STENT INSERTION
 UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis)
 Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Headache after an epidural or spinal injection What you need to know. Patient information Leaflet
 Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Blood Transfusion. There are three types of blood cells: Red blood cells. White blood cells. Platelets.
 Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Procedure Name: Day Case - Laparoscopic Inguinal Hernia Repair (TEP)
 Dr Philip Lockie MB BCh MPhil FRCSI FRACS PO Box 1275, Kenmore 4069 Tel: 07 3834 7080 Fax: 07 3834 6148 E-mail: info@drphillockie.com.au Provider No: 248127EW Brochure Code: DC GS13 Procedure Name: Day
Dr Philip Lockie MB BCh MPhil FRCSI FRACS PO Box 1275, Kenmore 4069 Tel: 07 3834 7080 Fax: 07 3834 6148 E-mail: info@drphillockie.com.au Provider No: 248127EW Brochure Code: DC GS13 Procedure Name: Day
Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients
 Oxford University Hospitals NHS Trust Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients What are the parathyroid glands? There are four parathyroid glands
Oxford University Hospitals NHS Trust Parathyroidectomy An operation to remove overactive parathyroid glands Information for patients What are the parathyroid glands? There are four parathyroid glands
Having a PEG tube inserted?
 Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Ulnar Nerve Decompression/Transposition
 Department of Neurosurgery Ulnar Nerve Decompression/Transposition What happens when you are in hospital page 2 Ulnar Nerve Decompression/Transposition This leaflet explains what to expect when you are
Department of Neurosurgery Ulnar Nerve Decompression/Transposition What happens when you are in hospital page 2 Ulnar Nerve Decompression/Transposition This leaflet explains what to expect when you are
Mesenteric Angiography
 Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
ENDOSCOPY UNIT. Duodenum Stomach. Having an oesophageal stent. Patient information leaflet
 Trafford Hospitals ENDOSCOPY UNIT Gastroscope Oesophagus Lungs Duodenum Stomach Having an oesophageal stent Patient information leaflet If you are unable to keep your appointment, please telephone the
Trafford Hospitals ENDOSCOPY UNIT Gastroscope Oesophagus Lungs Duodenum Stomach Having an oesophageal stent Patient information leaflet If you are unable to keep your appointment, please telephone the
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Deep Vein Thrombosis (DVT) in pregnancy
 Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Meatoplasty/Canalplasty
 Meatoplasty/Canalplasty What is a meatoplasty/canalplasty and why do I need this operation? This operation is performed to widen your ear canals so that they do not get blocked with wax and debris. It
Meatoplasty/Canalplasty What is a meatoplasty/canalplasty and why do I need this operation? This operation is performed to widen your ear canals so that they do not get blocked with wax and debris. It
Excision or Open Biopsy of a Breast Lump Your Operation Explained
 Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
