The American Society of Colon and Rectal Surgeons
|
|
|
- Joseph Golden
- 7 years ago
- Views:
Transcription
1 PRACTICE PARAMETERS Practice Parameters for the Management of Perianal Abscess and Fistula-in-Ano Scott R. Steele, M.D. Ravin Kumar, M.D. Daniel L. Feingold, M.D. Janice L. Rafferty, M.D. W. Donald Buie, M.D. Prepared by the Standards Practice Task Force of the American Society of Colon and Rectal Surgeons The American Society of Colon and Rectal Surgeons is dedicated to ensuring high-quality patient care by advancing the science, prevention, and management of disorders and diseases of the colon, rectum, and anus. The Standards Committee is composed of Society members who are chosen because they have demonstrated expertise in the specialty of colon and rectal surgery. This Committee was created to lead international efforts in defining quality care for conditions related to the colon, rectum, and anus. This is accompanied by developing Clinical Practice Guidelines based on the best available evidence. These guidelines are inclusive, and not prescriptive. Their purpose is to provide information on which decisions can be made, rather than dictate a specific form of treatment. These guidelines are intended for the use of all practitioners, health care workers, and patients who desire information about the management of the conditions addressed by the topics covered in these guidelines. It should be recognized that these guidelines should not be deemed inclusive of all proper methods of care or exclusive of methods of care reasonably directed to obtaining the same results. The ultimate judgment regarding the propriety of any specific procedure must be made by the physician in light of all the circumstances presented by the individual patient. STATEMENT OF THE PROBLEM Key Words: Perianal abscess; Fistula-in-ano; Seton; Rectovaginal fistula. Dis Colon Rectum 2011; 54: DOI: /DCR.0b013e b3 The ASCRS 2011 Anorectal abscess is a potentially debilitating condition most often originating from a cryptoglandular infection in the anal canal, 1 and remains one of the more common anorectal conditions encountered in practice. Although the underlying pathogenesis is the same in the majority of patients, these abscesses are classified into perianal, ischiorectal, intersphincteric, and supralevator based on location. 2 As such, patients may present with a variety of signs and symptoms ranging from fever, pain, tenderness, erythema, and a fluctuant mass to relatively normal external findings and deep-seated rectal pain. 2 In approximately 30% to 50% of patients with an anorectal abscess, a persistent tract, or fistula-in-ano, develops, extending from the anal canal to the perineal skin. 3,4 Unfortunately, there is no definitive way to predict who will develop one, or how to prevent one. Patients often report persistent purulent drainage or intermittent perianal swelling and tenderness followed by spontaneous discharge. Fistulas are categorized based on their anatomical course relative to the sphincter complex: intersphincteric, transsphincteric, suprasphincteric, and extrasphincteric. 4 Fistulas can also be classified as simple or complex, with simple fistulas including low transsphincteric and intersphincteric fistulas that cross 30% of the external sphincter. 5 Complex fistulas include high transsphincteric fistulas with or without a high blind tract, suprasphincteric and extrasphincteric fistulas, horseshoe fistulas, and those associated with inflammatory bowel disease, radiation, malignancy, preexisting incontinence, or chronic diarrhea, as well. 6 8 Given the attenuated nature of the anterior sphincter complex in women, fistulas in this location deserve special consideration and may be considered complex as well. This practice parameter will focus on the evaluation and management of both perianal abscess and fistula-in-ano. METHODOLOGY These guidelines are built on the last set of the American Society of Colon and Rectal Surgeons Practice Parameters for treatment of perianal abscess and fistula-in-ano published in An organized search of MEDLINE, PubMed, EMBASE, and the Cochrane Database of Collected Reviews was performed through February Key word combinations included abscess, fistula, fistula-in-ano, anal, rectal, perianal, perineal, rectovaginal, anovaginal, seton, fistula plug, fibrin glue, advancement flap, and DISEASES OF THE COLON &RECTUM VOLUME 54: 12 (2011) 1465
2 1466 STEELE ET AL:PRACTICE PARAMETERS FOR PERIANAL ABSCESS AND FISTULA-IN-ANO TABLE 1. The GRADE system: Grading recommendations a 1A 1B 1C 2A 2B 2C Description Strong recommendation, high-quality evidence Strong recommendation, moderate-quality evidence Strong recommendation, low or very low quality evidence Weak recommendation, highquality evidence Weak recommendations, moderate-quality evidence Weak recommendation, low or very low quality evidence Benefit vs. risk and burdens Benefits clearly outweigh risk and burdens or vice versa Benefits clearly outweigh risk and burdens or vice versa Benefits clearly outweigh risk and burdens or vice versa Benefits closely balanced with risks and burdens Benefits closely balanced with risks and burdens Uncertainty in the estimates of benefits, risks and burden; benefits, risks, and burden may be closely balanced Methodologic quality of supporting evidence RCTs without important limitations or overwhelming evidence from observational studies RCTs with important limitations (inconsistent results, methodologic flaws, indirect or imprecise) or exceptionally strong evidence from observational studies Observational studies or case series RCTs without important limitations or overwhelming evidence from observational studies RCTs with important limitations (inconsistent results, methodologic flaws, indirect or imprecise) or exceptionally strong evidence from observational studies Observational studies or case series GRADE Grades of Recommendation, Assessment, Development, and Evaluation; RCT randomized controlled trial. a Adapted from Guyatt et al. 10 Table 2. Used with permission. Implications Strong recommendation, can apply to most patients in most circumstances without reservation Strong recommendation, can apply to most patients in most circumstances without reservation Strong recommendation but may change when higherquality evidence becomes available Weak recommendation, best action may differ depending on circumstances or patients or societal values Weak recommendation, best action may differ depending on circumstances or patients or societal values Very weak recommendations; other alternatives may be equally reasonable Crohn s disease. Directed searches of the embedded references from the primary articles were also performed in selected circumstances. Primary authors reviewed all English language manuscripts and studies of adults. Recommendations were formulated by the primary authors and reviewed by the entire Committee. The final grade of recommendation was performed using the Grades of Recommendation, Assessment, Development, and Evaluation (GRADE) system 10 and reviewed by the entire Standards Committee (Table 1). 11 RECOMMENDATIONS Initial Evaluation of Perianal Abscess and Fistula-in-Ano 1. A disease-specific history and physical examination should be performed, emphasizing symptoms, risk factors, location, and presence of secondary cellulitis or fistula-in-ano. Grade of Recommendation: Strong recommendation based on low-quality evidence 1C The diagnosis of anorectal abscess is usually made based on the patient s history and physical examination. It is important to distinguish anorectal abscess from other perianal suppurative processes such as hidradenitis suppurativa, infected skin furuncles, and infectious processes including herpes simplex virus, HIV, tuberculosis, syphilis, and actinomycosis. 12 In addition, features suggestive of Crohn s disease, including large skin tags or multiple fistulas, require a more detailed workup and potentially additional medical therapy. 13 On examination, a tender, fluctuant mass is almost always present with perianal and ischiorectal abscesses. Patients with intersphincteric or supralevator abscesses may have a paucity of external findings, with only pelvic or rectal tenderness or fluctuance on digital rectal examination. Careful inspection may detect the presence of other anorectal pathology or an external opening suggestive of a fistula-in-ano. 14,15 Palpation of the perianal area, digital rectal examination, and careful probing of the tract(s) often aids in defining the presence and anatomy of the fistula. Anoscopy and sigmoidoscopy may be performed to try to visualize the internal opening of a fistula and other mucosal abnormalities such as proctitis secondary to Crohn s disease. In general, laboratory evaluation is not necessary, with the exception of patients with systemic symptoms such as fever, serious underlying medical problems, or an unclear diagnosis. 2. Studies such as fistulography, endoanal ultrasound, CT scan, and MRI may be considered in selected
3 DISEASES OF THE COLON &RECTUM VOLUME 54: 12 (2011) 1467 patients to help define the anatomy of an anorectal abscess or fistula-in-ano and to guide management. Grade of Recommendation: Strong recommendation based on low-quality evidence 1C Although anorectal abscess and fistula-in-ano are most commonly diagnosed and managed on the basis of clinical findings alone, adjunctive radiological studies can occasionally provide valuable information in complex tracts or recurrent disease. The vast majority of fistulas, however, do not require any imaging. Traditionally, fistulography was the method of choice. 16 Reported accuracy rates as low as 16% have largely led to this test falling out of favor. 17 Endoanal ultrasound is very effective for characterizing anorectal abscess and fistulas with accuracy rates as high as 80% to 89% for delineating fistula tracts, and is especially effective in identifying horseshoe abscess extensions Three-dimensional ultrasound techniques provide even better imaging, especially in patients with complex perianal sepsis or high-riding tracts. 21 Combining 3-dimensional ultrasound with hydrogen peroxide injection through the external opening has demonstrated accuracy rates comparable to MRI, with close to 90% concordance CT scan can be useful for patients with complex suppurative anorectal conditions, and is especially helpful in identifying supralevator abscesses, or for those patients who would otherwise be difficult to examine without anesthesia. 25 In patients with Crohn s disease who have perianal pathology, CT has proven reliable in helping to delineate fistulas and abscesses from isolated rectal inflammation. 26 MRI with or without endoanal coils has reported accuracy rates of more than 90% for mapping fistula tracts and identifying the internal opening. 27,28 The majority of studies comparing pelvic MRI with endoanal ultrasound have shown slightly higher 20,22,29,30 rather than lower 31,32 rates of sensitivity and accuracy depending, in part, on operator experience (ultrasound) and patient population (ie, recurrent disease, abscess/fistula location, Crohn s disease). Perianal Abscess 1. Patients with acute anorectal abscess should be treated in a timely fashion with incision and drainage. Grade of Recommendation: Strong recommendation based on lowquality evidence 1C The primary treatment of anorectal abscesses remains surgical drainage. In general, the incision should be kept as close as possible to the anal verge to minimize the length of a potential fistula, while still providing adequate drainage. With an adequately sized elliptical incision, postoperative wound packing is usually not necessary. A variation of incision and drainage uses a small latex catheter (eg, 10 14F Pezzer catheter) placed into the abscess cavity with the use of local anesthesia and a small stab incision. The catheter is removed when the abscess drainage stops and the cavity has closed down around the catheter (usually 3 10 days). 33,34 After simple incision and drainage, the overall recurrence rate ranges from 3% to 44%, depending on the abscess location and the length of follow-up. 35,36 Additional factors associated with recurrence and the need for early repeat drainage include incomplete initial drainage, failure to break up loculations within the abscess, missed abscess, and undiagnosed fistula. 37 Horseshoe abscesses have been associated with especially high rates of persistence and recurrence ranging between 18% and 50%, 37,38 and often require multiple operations before definitive healing Antibiotics have a limited role in the treatment of uncomplicated anorectal abscess. Grade of Recommendation: Strong recommendation based on moderatequality evidence 1B 3. Antibiotics may be considered in patients with significant cellulitis, underlying immunosuppression, or concomitant systemic illness. Grade of Recommendation: Weak recommendation based on low-quality evidence 2C In general, the addition of antibiotics to routine incision and drainage of uncomplicated anorectal abscess does not improve healing time or reduce recurrences, and it is therefore not indicated However, limited data suggest that antibiotics be considered for use in patients with extensive cellulitis, systemic symptoms, or failure to improve with drainage alone. 43 In patients with underlying immunosuppression, the data also suggest that antibiotics may play a role. Although patients with a higher absolute neutrophil count ( 1000/mm 3 ) and fluctuance on examination demonstrate higher resolution rates with incision and drainage, patients with lower neutrophil counts (ANC /mm 3 ) and/or lack of fluctuance on examination have been successfully treated with antibiotics alone in 30% to 88% The emergence of community-acquired methicillinresistant Staphylococcus aureus in otherwise routine anorectal abscesses 47 raises the question whether wound culture is indicated after incision and drainage. Although wound culture is rarely helpful, it may be considered in cases of recurrent infection or nonhealing wounds. Patients with underlying HIV infection with either concomitant infections or atypical microbes, including tuberculosis 48 may benefit from wound culture and targeted antibiotic treatment. Finally, recent guidelines from the American Heart Association recommend preoperative antibiotics before incision and drainage of infected tissue in patients with prosthetic valves, previous bacterial endocarditis, congenital heart disease, and heart transplant recipients with valve pathology. Unlike prior guidelines, antibiotic prophylaxis is no longer recommended in patients with routine mitral valve prolapse. 49
4 1468 STEELE ET AL:PRACTICE PARAMETERS FOR PERIANAL ABSCESS AND FISTULA-IN-ANO Fistula-in-Ano The goal in the treatment of fistula-in-ano is to obliterate the internal fistulous opening and any associated epithelialized tracks with minimal sphincter division. Thus, it is imperative to identify the internal opening and the course of all tracts relative to the sphincter muscles. Goodsall s rule attempts to predict the location of the internal opening in relation to its external (secondary) opening. External openings posterior to a transverse line through the anal verge will open into the anal canal in the midline. Conversely, anterior placed openings will run in a radial direction, analogous to spokes on a wheel. Although Goodsall s rule accurately predicts the location of the internal opening in 49% to 81% of patients, the location of the external opening can be a poor predictor of the location of a fistula, in particular, in patients with long fistula tracts, recurrent fistulas, or Crohn s disease. 14,50 52 In addition to direct visualization and palpation, the surgeon must be familiar with adjunctive intraoperative measures, including hydrogen peroxide/methylene blue injection of the external opening, to assist in the identification of tract origin, with reported success rates greater than 90% and 80%. 50,51 In addition, the etiology should be determined. Approximately 80% of fistulas are secondary to cryptoglandular infection, but other diagnoses such as Crohn s, trauma, radiation, malignancy, or infection must be considered in fistulas with an unusual appearance or location. Because no single technique is appropriate for the treatment of all fistulas-in-ano, treatment must be directed by the etiology and anatomy of the fistula, degree of symptoms, patient comorbidities, and the surgeon s experience. One should keep in mind the progressive tradeoff between the extent of operative sphincter division, postoperative healing rates, and functional compromise. Treatment of a Simple Fistula-in-Ano 1. Simple anal fistulas may be treated by fistulotomy. The addition of marsupialization may improve the rate of wound healing. Grade of Recommendation: Strong recommendation based on moderate-quality evidence 1B There is no universal answer to the question of how much muscle can be safely divided. Nevertheless, with proper patient selection, fistulotomy has been associated with success rates of 92% to 97%. 53,54 Higher recurrence rates have been associated with complex fistulas, failure to identify the internal opening, and Crohn s disease. 53,55,56 Postoperative alterations in continence are reported in 0% to 73% of patients. This wide range is due to differences in the definition of incontinence, variable follow-up, and the degree of disturbance. Risk factors include preoperative incontinence, recurrent disease, female sex, complex fistulas, and prior fistula surgery. 53,56 58 The addition of marsupialization has also been associated with less postoperative bleeding and accelerated wound healing by approximately 4 weeks. 59,60 Limited data have shown that fistulectomy, in which the tract is resected, is associated with longer healing times, larger defects, and a higher risk of incontinence, although recurrence rates are similar when compared with fistulotomy. 61,62 2. Concomitant fistulotomy with incision and drainage may be considered in select patients with anorectal abscess and fistula. Grade of Recommendation: Weak recommendation based on moderate-quality evidence 2B One of the more controversial topics in dealing with anorectal abscess is the role of primary fistulotomy at the time of initial incision and drainage. Proponents of this practice cite the infected crypt as the origin of the problem and believe that failure to address this leads to higher recurrence rates. 35 Opponents counter with the higher rate of continence disturbances in patients undergoing concomitant fistulotomy and the potential for unnecessary fistulotomy. 3,63 Quah and colleagues performed a metaanalysis including 5 trials of 405 patients and demonstrated that sphincter division (via fistulotomy or fistulectomy) at the time of incision and drainage was associated with a significant decrease in recurrence (relative risk (RR) 0.17, 95% CI , P.001), but higher levels of continence disorders (RR 2.46, 95% CI , P.140). 64 Thus, the utility of fistulotomy in conjunction with incision and drainage of an anorectal abscess remains controversial. The surgeon should weigh the possible decreased recurrence rate in light of the potential increased risk of continence disturbances. 3. Simple anal fistulas may be treated with debridement and fibrin glue injection. Grade of Recommendation: Weak recommendation based on low-quality evidence 2C Fibrin glue has a number of advantages, including its ease of use, repeatability, and avoidance of sphincter division, especially in patients with a high risk of incontinence following fistulotomy. However, this must be weighed against the high failure rate. Retrospective and prospective cohort data for fibrin glue use in simple fistulas has demonstrated healing rates of 40% to 78% Simple low fistulas have a decreased rate of healing with fibrin glue compared with fistulotomy (50% (3/6) vs 100% (7/7), P.06) with low rates of incontinence in both groups. Treatment of Complex Fistula-in-Ano In select patients, radiographic evaluation may be beneficial to identify an occult internal opening and secondary tracts or abscesses, or to help delineate the fistula s relationship to the sphincter complex. 1. Complex anal fistulas may be treated with debridement and fibrin glue injection. Grade of Recommendation: Weak recommendation based on low-quality evidence 2C In the randomized controlled trial by Lindsey et al, 69 the authors compared fibrin glue with loose setons
5 DISEASES OF THE COLON &RECTUM VOLUME 54: 12 (2011) 1469 followed by flap repair for complex fistulas (n 29). Fibrin glue was associated with higher healing rates (69% (9/13) vs 13% (2/16), P.003), whereas incontinence rates were similar between the 2 groups (0/13 vs 2/16). Overall healing rates in nonrandomized series using fibrin glue for complex disease has ranged from 10% to 67%. Although fibrin glue therapy has a relatively low success rate in complex disease, for those that eventually heal, it does appear to be a durable repair. Furthermore, given the low morbidity associated with the procedure, it may be considered for initial therapy. 2. Anal fistula plug may be used for treatment of complex anal fistula disease. Grade of Recommendation: Weak recommendation based on moderate-quality evidence 2C The bioprosthetic anal fistula plug is used to close the primary internal anal opening and serves as a matrix for the obliteration of the fistula tract. Although limited data have demonstrated success with the plug in up to 70% to 100% of low-lying fistulas, outcomes in complex disease have been less promising In patients with Crohn s disease, initial reports demonstrated closure rates of 80%, 76 with the same group demonstrating persistent closure in 83% of all types of complex fistulas at a median of 12 months. 77 Unfortunately, most other studies have not been able to replicate those results, with the majority of studies reporting 50%. 72,73,78 80 Lower success rates are associated with longer follow-up periods. The low morbidity, repeatability, and lack of other options warrant consideration of this therapy in patients with complex fistulas. 3. Endoanal advancement flaps may be used for treatment of complex anal fistula disease. Grade of Recommendation: Strong recommendation based on moderate-quality evidence 1C Endoanal advancement flap is another sphincter-sparing technique that consists of curettage of the tract, and mobilizing a segment of proximal healthy anorectal mucosa, submucosa, and muscle to cover the site of the sutured internal opening. In general, recurrence rates range from 13% to 56% The addition of fibrin glue to obliterate the tract has failed to improve success rates. 81,84 Factors associated with failed repair include radiation, underlying Crohn s disease, active proctitis, rectovaginal fistula, malignancy, and number of prior attempted repairs. 53,82,85 88 Although the sphincter is not divided with endoanal advancement flaps, mild or moderate incontinence is still reported in up to 7% 38% of patients, with associated decreases reported in both resting and squeeze 85,89 91 pressures on postoperative manometry. 4. Complex anal fistulas may be treated by the use of a seton and/or staged fistulotomy. Grade of Recommendation: Strong recommendation based on moderatequality evidence 1B The seton (ie, suture, rubber band, Silastic vessel loop) is passed through the fistula tract to convert an inflammatory process to a foreign body reaction causing perisphincteric fibrosis. Setons may be of the cutting type, for which progressive tightening will produce a gradual fistulotomy with scarring of the tract, over the course of weeks. Alternatively, a loose seton may be placed to promote drainage and avoidance of recurrent perineal sepsis, and may be left in place long-term or removed with ultimate cure. There remains a lack of high-quality data with regard to setons, with only 4 randomized controlled trials to date, all with varying results. 69,92 94 In the setting of complex anal fistulas, setons are commonly used in a staged fashion, with initial seton placement to control sepsis followed by a secondary procedure (ie, endoanal advancement flap, fibrin glue, anal plug) weeks later to avoid division of the sphincter muscle. 95 Success rates in this setting have ranged from 62% to 100%, depending on the type of secondary procedure Changes in continence range from 0% to 54% with patients undergoing 2-staged procedures or cutting setons. Incontinence to flatus is seen more often than liquid or solid stool incontinence Finally, in sepsis secondary to fistula disease that is recalcitrant to other methods, diversion and appropriate drainage may be required. 5. Complex fistulas may be treated with ligation of the intersphincteric fistula tract (LIFT). Grade of Recommendation: No recommendation A relatively new technique called the LIFT procedure involves ligation and division of the fistula tract in the intersphincteric space The procedure typically involves placement of a seton for 8 or more weeks to allow fibrosis of the tract. Using an intersphincteric approach, the tract can be identified, ligated, and divided, with possible closure of the internal opening and widening of the external opening for drainage. Using this approach, there is no sphincter muscle divided and, theoretically, continence is preserved. Although there are only a few small series to date in the literature, successful closure has been reported in 57% to 94% at a mean follow-up of 3 to 8 months, with a recurrence rate of 6% to 18% In the 3 major series to date, there have been no major changes in continence or morbidity. Unfortunately, data are too preliminary to make a formal recommendation as to their ultimate expected outcomes and place in the treatment algorithm. This parameter will be updated as more evidence becomes available. Treatment of Perianal Fistula Associated With Crohn s Disease Perianal pathology occurs in 40% to 80% of patients with Crohn s disease with perianal fistula presenting a particular challenge. 105 The primary treatment for perianal Crohn s fistulas is medical; surgery is reserved for the control of
6 1470 STEELE ET AL:PRACTICE PARAMETERS FOR PERIANAL ABSCESS AND FISTULA-IN-ANO sepsis and occasionally as an adjunct for cure. Antibiotics are effective, especially in fistulizing disease, with metronidazole and fluoroquinolones demonstrating improved perianal symptoms (at least temporarily) in over 90% of patients. 106 Limited data for azathioprine, 6-mercaptopurine, cyclosporine, and tacrolimus have also reported some success for fistulizing Crohn s disease Finally, infliximab, a monoclonal antibody against tumor necrosis factor, has been shown to increase the healing rate of perianal fistulas, with complete closure in up to 46% of patients. 110 The decision to embark on surgical treatment for perianal Crohn s disease must be individualized and based on the extent of disease and the severity of symptoms. Unfortunately, despite all efforts, disease may result in proctectomy or permanent diversion in patients with severe perianal fistulizing disease Asymptomatic fistulas in patients with Crohn s disease do not require surgical treatment. Grade of Recommendation: Strong recommendation based on lowquality evidence 1C Anal fistulas in patients with perianal Crohn s disease may be secondary to either Crohn s disease or cryptoglandular origin. Irrespective of etiology, patients with asymptomatic fistulas and no signs of local sepsis require no surgical intervention. 115,116 These fistulas may remain dormant for an extended period of time; therefore, patients need not be subjected to the morbidity of operative intervention. 2. Symptomatic simple low Crohn s fistulas may be treated by fistulotomy. Grade of Recommendation: Strong recommendation based on low-quality evidence 1C Fistulotomy is safe and effective in low-lying simple fistulas involving no or minimal external anal sphincter. 106,117 Given the chronicity of the disease and high frequency of disease relapse, maximum preservation of sphincter function is essential. Thus, before embarking on any fistulotomy, surgeons should consider all relevant patient factors, in particular, the extent of anorectal disease, sphincter status and continence, rectal compliance, presence of active proctitis, previous anorectal operations, and stool consistency. With proper patient selection, healing rates following fistulotomy are reported in 56% to 100% of patients, with mild incontinence rates of 6% to 12%. 54,96, This may be, in part, secondary to repeated fistulotomy in patients with recurrent low fistulas. Wound healing in this patient population may be delayed by 3 to 6 months. 3. Complex Crohn s fistulas may be well palliated with long-term draining setons. Grade of Recommendation: Strong recommendation based on low-quality evidence 1C For complex fistulas associated with Crohn s disease, long-term ( 6 wk) placement of loose setons, such as vessel loops or Silastic catheters, can successfully control drainage and allow inflammation to resolve by providing continuous drainage and preventing closure of the external skin opening. 105,106,117 Despite this technique, recurrent sepsis occurs in 20% to 40%, with approximately 8% to 13% of patients experiencing some degree of fecal soilage. 8,99,120 Recent data on the use of concurrent seton drainage and infliximab therapy have reported fistula closure in 24% to 78% of patients following induction therapy, with 25% to 100% of these patients responding to subsequent courses of infliximab therapy Complex Crohn s fistulas may be treated with advancement flap closure if the rectal mucosa is grossly normal. Grade of Recommendation: Weak recommendation based on low-quality evidence 2C Endorectal and anodermal advancement flaps may also be used in complex Crohn s fistulas in select patients without active proctitis. Short-term success is reported to range between 64% and 75%. 82,88,124,125 Recurrence rates increase over time with extended follow-up. 113,126 Rectovaginal fistulas associated with Crohn s have a short-term success rates of 40% to 50% when treated with a flap. 124,127 Treatment with biologics to cause remission of active proctitis may permit the use of an anal flap at a later date. 5. Complex Crohn s fistulas may require permanent diversion or proctectomy for uncontrollable symptoms. Grade of Recommendation: Strong recommendation based on low-quality evidence 1C A small percentage of patients with extensive and aggressive disease that is uncontrolled by medical management and long-term seton placement may require diversion or proctectomy to control perianal sepsis. 123 For patients with complex perianal Crohn s disease, diversion rates range from 31% to 49%. Concomitant colonic disease, persistent anal sepsis, prior temporary diversion, fecal incontinence, and anal canal stenosis are reported as predictive factors. 112,128 Despite optimal medical and minimally invasive therapy, 8% to 40% will require proctectomy to control recalcitrant symptoms. 106,113,123,129 The practice parameters set forth in this document have been developed from sources believed to be reliable. The American Society of Colon and Rectal Surgeons makes no warranty, guarantee, or representation whatsoever as to the absolute validity or sufficiency of any parameter included in this document, and the Society assumes no responsibility for the use of the material contained. APPENDIX A: CONTRIBUTING MEMBERS OF THE ASCRS STANDARDS COMMITTEE W. Donald Buie, M.D., Chair; Janice Rafferty, M.D., Cochair; Farshid Araghizadeh, M.D.; Robin Boushey, M.D.; Srihdhar Chalasani, M.D.; George Chang, M.D.; Robert Cima, M.D.; Gary Dunn, M.D.; Daniel Feingold, M.D.; Phillip Fleshner, M.D.; Daniel Geisler, M.D.; Jill Jenua, M.D.; Sharon Gregorcyk, M.D.; Daniel Herzig, M.D.; Andreas Kaiser, M.D.; Ravin Kumar, M.D.; David Larson,
7 DISEASES OF THE COLON &RECTUM VOLUME 54: 12 (2011) 1471 M.D.; Stephen Mills, M.D.; John Monson, M.D.; W. Brian Perry, M.D.; P. Terry Phang, M.D.; David Rivadeneira, M.D.; Howard Ross, M.D.; Peter Senatore, M.D.; Elin Sigurdson, M.D.; Thomas Stahl, M.D.; Scott Steele, M.D.; Scott Strong, M.D.; Charles Ternent, M.D.; Judith Trudel, M.D.; Madhulika Varma, M.D.; Martin Weiser, M.D. REFERENCES 1. Parks AG. Pathogenesis and treatment of fistula-in-ano. Br Med J. 1961;5224: Read DR, Abcarian H. A prospective survey of 474 patients with anorectal abscess. Dis Colon Rectum. 1979;22: Hämäläinen KP, Sainio AP. Incidence of fistulas after drainage of acute anorectal abscesses. Dis Colon Rectum. 1998;41: Parks AG, Gordon PH, Hardcastle JD. A classification of fistula-in-ano. Br J Surg. 1976;63: Parks AG, Stitz RW. The treatment of high fistula-in-ano. Dis Colon Rectum. 1976;19: Sangwan YP, Rosen L, Riether RD, Stasik JJ, Sheets JA, Khubchandani IT. Is simple fistula-in-ano simple? Dis Colon Rectum. 1994;37: Kondylis PD, Shalabi A, Kondylis LA, Reilly JC. Male cryptoglandular fistula surgery outcomes: a retrospective analysis. Am J Surg. 2009;197: Galis-Rozen E, Tulchinsky H, Rosen A, et al. Long-term outcome of loose-seton for complex anal fistula: a two-centre study of patients with and without Crohn s disease [published online ahead of print February 7, 2009]. Colorectal Dis. doi: /j x. 9. Whiteford MH, Kilkenny J III, Hyman N, et al.; The Standards Practice Task Force; The American Society of Colon and Rectal Surgeons. Practice parameters for the treatment of perianal abscess and fistula-in-ano (revised). Dis Colon Rectum. 2005; 48: Schunemann HJ, Jaeschke R, Cook DJ, et al. An official ATS statement: grading the quality of evidence and strength of recommendations in the ATS guidelines and recommendations. Am J Respir Crit Care Med. 2006;174: Guyatt G, Gutermen D, Baumann MH, et al. Grading strength of recommendations and quality of evidence in clinical guidelines: report from an American College of Chest Physicians Task Force. Chest. 2006;129: Nelson J, Billingham R. Pilonidal disease and hidradenitis suppurativa. In: Wolff BG, Fleshman JW, Beck DE, Pemberton JH, Wexner SD, eds. The ASCRS Textbook of Colon and Rectal Surgery. New York: Springer; 2007: Buchmann P, Keighley MR, Allan RN, Thompson H, Alexander-Williams J. Natural history of perianal Crohn s disease. Ten year follow-up: a plea for conservatism. Am J Surg. 1980; 140: Cirocco WC, Reilly JC. Challenging the predictive accuracy of Goodsall s rule for anal fistulas. Dis Colon Rectum. 1992;35: Chinn BT. Outpatient management of pilonidal disease. Semin Colon Rectal Surg. 2003;14: Weisman RI, Orsay CP, Pearl RK, Abcarian H. The role of fistulography in fistula-in-ano: report of five cases. Dis Colon Rectum. 1991;34: Kuijpers HC, Schulpen T. Fistulography for fistula-in-ano: is it useful? Dis Colon Rectum. 1985;28: Toyonaga T, Matsushima M, Tanaka Y, et al. Microbiological analysis and endoanal ultrasonography for diagnosis of anal fistula in acute anorectal sepsis. Int J Colorectal Dis. 2007;22: Toyonaga T, Tanaka Y, Song JF, et al. Comparison of accuracy of physical examination and endoanal ultrasonography for preoperative assessment in patients with acute and chronic anal fistula. Tech Coloproctol. 2008;12: Buchanan GN, Halligan S, Bartram CI, Williams AB, Tarroni D, Cohen CR. Clinical examination, endosonography, and MR imaging in preoperative assessment of fistula in ano: comparison with outcome-based reference standard. Radiology. 2004; 233: Santoro GA, Fortling B. The advantages of volume rendering in three-dimensional endosonography of the anorectum. Dis Colon Rectum. 2007;50: West RL, Zimmerman DD, Dwarkasing S, et al. Prospective comparison of hydrogen peroxide-enhanced three-dimensional endoanal ultrasonography and endoanal magnetic resonance imaging of perianal fistulas. Dis Colon Rectum. 2003;46: Buchanan GN, Bartram CI, Williams AB, Halligan S, Cohen CR. Value of hydrogen peroxide enhancement of three-dimensional endoanal ultrasound in fistula-in-ano. Dis Colon Rectum. 2005;48: West RL, Dwarkasing S, Felt-Bersma RJ, et al. Hydrogen peroxide-enhanced three-dimensional endoanal ultrasonography and endoanal magnetic resonance imaging in evaluating perianal fistulas: agreement and patient preference. Eur J Gastroenterol Hepatol. 2004;16: Guillaumin E, Jeffrey RB Jr, Shea WJ, Asling CW, Goldberg HI. Perirectal inflammatory disease: CT findings. Radiology. 1986; 161: Yousem DM, Fishman EK, Jones B. Crohn disease: perianal and perirectal findings at CT. Radiology. 1988;167: Schaefer O, Lohrmann C, Langer M. Assessment of anal fistulas with high-resolution subtraction MR-fistulography: comparison with surgical findings. J Magn Reson Imaging. 2004;19: Maccioni F, Colaiacomo MC, Stasolla A, Manganaro L, Izzo L, Marini M. Value of MRI performed with phased-array coil in the diagnosis and pre-operative classification of perianal and anal fistulas. Radiol Med. 2002;104: Maier AG, Funovics MA, Kreuzer SH, et al. Evaluation of perianal sepsis: comparison of anal endosonography and magnetic resonance imaging. J Magn Reson Imaging. 2001;14: Sahni VA, Ahmad R, Burling D. Which method is best for imaging of perianal fistula? Abdom Imaging. 2008;33: Orsoni P, Barthet M, Portier F, Panuel M, Desjeux A, Grimaud JC. Prospective comparison of endosonography, magnetic resonance imaging and surgical findings in anorectal fistula and abscess complicating Crohn s disease. Br J Surg. 1999;86: Gustafsson UM, Kahvecioglu B, Aström G, Ahlström H, Graf W. Endoanal ultrasound or magnetic resonance imaging for
8 1472 STEELE ET AL:PRACTICE PARAMETERS FOR PERIANAL ABSCESS AND FISTULA-IN-ANO preoperative assessment of anal fistula: a comparative study. Colorectal Dis. 2001;3: Beck DE, Fazio VW, Jagelman DG, Lavery IL, Weakley FL. Catheter drainage of ischiorectal abscesses. South Med J. 1988; 81: Vasilveski CA. Anorectal abscesses and fistulas. In: Wolff BG, Fleshman JW, Beck DE, Pemberton JH, Wexner SD, eds. The ASCRS Textbook of Colorectal Surgery. New York: Springer; 2007: Cox SW, Senagore AJ, Luchtefeld MA, Mazier WP. Outcome after incision and drainage with fistulotomy for ischiorectal abscess. Am Surg. 1997;63: Ramanujam PS, Prasad ML, Abcarian H, Tan AB. Perianal abscesses and fistulas: a study of 1023 patients. Dis Colon Rectum. 1984;27: Onaca N, Hirshberg A, Adar R. Early reoperation for perirectal abscess: a preventable complication. Dis Colon Rectum. 2001; 44: Held D, Khubchandani I, Sheets J, Stasik J, Rosen L, Riether R. Management of anorectal horseshoe abscess and fistula. Dis Colon Rectum. 1986;29: Rosen SA, Colquhoun P, Efron J, et al. Horseshoe abscesses and fistulas: how are we doing? Surg Innov. 2006;13: Llera JL, Levy RC. Treatment of cutaneous abscess: a doubleblind clinical study. Ann Emerg Med. 1985;14: Stewart MP, Laing MR, Krukowski ZH. Treatment of acute abscesses by incision, curettage and primary suture without antibiotics: a controlled clinical trial. Br J Surg. 1985;72: Macfie J, Harvey J. The treatment of acute superficial abscesses: a prospective clinical trial. Br J Surg. 1977;64: North JH Jr, Weber TK, Rodriguez-Bigas MA, Meropol NJ, Petrelli NJ. The management of infectious and noninfectious anorectal complications in patients with leukemia. J Am Coll Surg. 1996;183: Büyükaşik Y, Ozcebe OI, Sayinalp N, et al. Perianal infections in patients with leukemia: importance of the course of neutrophil count. Dis Colon Rectum. 1998;41: Cohen JS, Paz IB, O Donnell MR, Ellenhorn JD. Treatment of perianal infection following bone marrow transplantation. Dis Colon Rectum. 1996;39: Grewal H, Guillem JG, Quan SH, Enker WE, Cohen AM. Anorectal disease in neutropenic leukemic patients: operative vs nonoperative management. Dis Colon Rectum. 1994;37: Albright JB, Pidala MJ, Cali JR, Snyder MJ, Voloyiannis T, Bailey HR. MRSA-related perianal abscesses: an underrecognized disease entity. Dis Colon Rectum. 2007;50: Goldberg GS, Orkin BA, Smith LE. Microbiology of human immunodeficiency virus anorectal disease. Dis Colon Rectum. 1994;37: Wilson W, Taubert KA, Gewitz T, et al. Prevention of Infective Endocarditis. Guidelines From the American Heart Association: A Guideline From the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation. 2007; 116: Gonzalez-Ruiz C, Kaiser AM, Vukasin P, Beart RW Jr, Ortega AE. Intraoperative physical diagnosis in the management of anal fistula. Am Surg. 2006;72: Gunawardhana PA, Deen KI. Comparison of hydrogen peroxide instillation with Goodsall s rule for fistula-in-ano. ANZ J Surg. 2001;71: Coremans G, Dockx S, Wyndaele J, Hendrickx A. Do anal fistulas in Crohn s disease behave differently and defy Goodsall s rule more frequently than fistulas that are cryptoglandular in origin? Am J Gastroenterol. 2003;98: Garcia-Aguilar J, Belmonte C, Wong WD, Goldberg SM, Madoff RD. Anal fistula surgery: factors associated with recurrence and incontinence. Dis Colon Rectum. 1996;39: Davies M, Harris D, Lohana P, et al. The surgical management of fistula-in-ano in a specialist colorectal unit. Int J Colorectal Dis. 2008;23: Nwaejike N, Gilliland R. Surgery for fistula-in-ano: an audit of practice of colorectal and general surgeons. Colorectal Dis. 2007;9: Jordán J, Roig JV, García-Armengol J, García-Granero E, Solana A, Lledó S. Risk factors for recurrence and incontinence after anal fistula surgery [published online ahead of print February 7, 2009]. Colorectal Dis. doi: /j x. 57. van Koperen PJ, Wind J, Bemelman WA, Bakx R, Reitsma JB, Slors JF. Long-term functional outcome and risk factors for recurrence after surgical treatment for low and high perianal fistulas of cryptoglandular origin. Dis Colon Rectum. 2008;51: van Tets WF, Kuijpers HC. Continence disorders after anal fistulotomy. Dis Colon Rectum. 1994;37: Pescatori M, Ayabaca SM, Cafaro D, Iannello A, Magrini S. Marsupialization of fistulotomy and fistulectomy wounds improves healing and decreases bleeding: a randomized controlled trial. Colorectal Dis. 2006;8: Ho YH, Tan M, Leong AF, Seow-Choen F. Marsupialization of fistulotomy wounds improves healing: a randomized controlled trial. Br J Surg. 1998;85: Kronborg O. To lay open or excise a fistula-in-ano: a randomized trial. Br J Surg. 1985;72: Belmonte Montes C, Ruiz Galindo GH, Montes Villalobos JL, Decanini Terán C. Fistulotomy vs fistulectomy: ultrasonographic evaluation of lesion of the anal sphincter function [in Spanish]. Rev Gastroenterol Mex. 1999;64: Schouten WR, van Vroonhoven TJ. Treatment of anorectal abscess with or without primary fistulectomy: results of a prospective randomized trial. Dis Colon Rectum. 1991;34: Quah HM, Tang CL, Eu KW, Chan SY, Samuel M. Meta-analysis of randomized clinical trials comparing drainage alone vs primary sphincter-cutting procedures for anorectal abscessfistula. Int J Colorectal Dis. 2006;21: Adams T, Yang J, Kondylis LA, Kondylis PD. Long-term outlook after successful fibrin glue ablation of cryptoglandular transsphincteric fistula-in-ano. Dis Colon Rectum. 200;51: Sentovich SM. Fibrin glue for anal fistulas: long-term results. Dis Colon Rectum. 2003;46: Swinscoe MT, Ventakasubramaniam AK, Jayne DG. Fibrin glue for fistula-in-ano: the evidence reviewed. Tech Coloproctol. 2005;9:89 94.
9 DISEASES OF THE COLON &RECTUM VOLUME 54: 12 (2011) Yeung JM, Simpson JA, Tang SW, Armitage NC, Maxwell- Armstrong C. Fibrin glue for the treatment of fistulae-in-ano: a method worth sticking to? [published online ahead of print February 7, 2009] Colorectal Dis. doi: /j x. 69. Lindsey I, Smilgin-Humphreys MM, Cunningham C, Mortensen NJ, George BD. A randomized, controlled trial of fibrin glue vs conventional treatment for anal fistula. Dis Colon Rectum. 2002; 45: Loungnarath R, Dietz DW, Mutch MG, Birnbaum EH, Kodner IJ, Fleshman JW. Fibrin glue treatment of complex anal fistulas has low success rate. Dis Colon Rectum. 2004;47: de Parades V, Far HS, Etienney I, Zeitoun JD, Atienza P, Bauer P. Seton drainage and fibrin glue injection for complex anal fistulas[published online ahead of print February 7, 2009]. Colorectal Dis. doi: /j x 72. Song WL, Wang ZJ, Zheng Y, Yang XQ, Peng YP. An anorectal fistula treatment with acellular extracellular matrix: a new technique. World J Gastroenterol. 2008;14: Ky AJ, Sylla P, Steinhagen R, Steinhagen E, Khaitov S, Ly EK. Collagen fistula plug for the treatment of anal fistulas. Dis Colon Rectum. 2008;51: Ellis CN, Rostas JW, Greiner FG. Long-term outcomes with the use of bioprosthetic plugs for the management of complex anal fistulas. Dis Colon Rectum. 2010;53: Zubaidi A, AL-Obeed O. Anal fistula plug in high fistula-inano: an early Saudi experience. Dis Colon Rectum. 2009;52: O Connor L, Champagne BJ, Ferguson MA, Orangio GR, Schertzer ME, Armstrong DN. Efficacy of anal fistula plug in closure of Crohn s anorectal fistulas. Dis Colon Rectum. 2006; 49: Champagne BJ, O Connor LM, Ferguson M, Orangio GR, Schertzer ME, Armstrong DN. Efficacy of anal fistula plug in closure of cryptoglandular fistulas: long-term follow-up. Dis Colon Rectum. 2006;49: Schwandner O, Stadler F, Dietl O, Wirsching RP, Fuerst A. Initial experience on efficacy in closure of cryptoglandular and Crohn s transsphincteric fistulas by the use of the anal fistula plug. Int J Colorectal Dis. 2008;23: Safar B, Jobanputra S, Sands D, Weiss EG, Nogueras JJ, Wexner SD. Anal fistula plug: initial experience and outcomes. Dis Colon Rectum. 2009;52: Christoforidis D, Etzioni DA, Goldberg SM, Madoff RD, Mellgren A. Treatment of complex anal fistulas with the collagen fistula plug. Dis Colon Rectum. 2008;51: van Koperen PJ, Wind J, Bemelman WA, Slors JF. Fibrin glue and transanal rectal advancement flap for high transsphincteric perianal fistulas: is there any advantage? Int J Colorectal Dis. 2008;23: Mizrahi N, Wexner SD, Zmora O, et al. Endorectal advancement flap: are there predictors of failure? Dis Colon Rectum. 2002;45: Mitalas LE, Gosselink MP, Zimmerman DD, Schouten WR. Repeat transanal advancement flap repair: impact on the overall healing rate of high transsphincteric fistulas and on fecal continence. Dis Colon Rectum. 2007;50: Ellis CN, Clark S. Fibrin glue as an adjunct to flap repair of anal fistulas: a randomized, controlled study. Dis Colon Rectum. 2006;49: Schouten WR, Zimmerman DD, Briel JW. Transanal advancement flap repair of transsphincteric fistulas. Dis Colon Rectum. 1999;42: Zimmerman DD, Briel JW, Gosselink MP, Schouten WR. Anocutaneous advancement flap repair of transsphincteric fistulas. Dis Colon Rectum. 2001;44: Jones IT, Fazio VW, Jagelman DG. The use of transanal rectal advancement flaps in the management of fistulas involving the anorectum. Dis Colon Rectum. 1987;30: Sonoda T, Hull T, Piedmonte MR, Fazio VW. Outcomes of primary repair of anorectal and rectovaginal fistulas using the endorectal advancement flap. Dis Colon Rectum. 2002;45: Athanasiadis S, Helmes C, Yazigi R, Köhler A. The direct closure of the internal fistula opening without advancement flap for transsphincteric fistulas-in-ano. Dis Colon Rectum. 2004; 47: Perez F, Arroyo A, Serrano P, Sánchez A, et al. Randomized clinical and manometric study of advancement flap versus fistulotomy with sphincter reconstruction in the management of complex fistula-in-ano. Am J Surg. 2006;192: Uribe N, Millán M, Minguez M, et al. Clinical and manometric results of endorectal advancement flaps for complex anal fistula. Int J Colorectal Dis. 2007;22: Zbar AP, Ramesh J, Beer-Gabel M, Salazar R, Pescatori M. Conventional cutting vs. internal anal sphincter-preserving seton for high trans-sphincteric fistula: a prospective randomized manometric and clinical trial. Tech Coloproctol. 2003;7: Shukla N. Multicentric randomized controlled clinical trial of Kshaarasootra (Ayurvedic medicated thread) in the management of fistula-in-ano. Indian Council of Medical Research. Indian J Med Res. 1991;94: Ho KS, Tsang C, Seow-Choen F, et al. Prospective randomised trial comparing ayurvedic cutting seton and fistulotomy for low fistula-in-ano. Tech Coloproctol. 2001;5: Tyler KM, Aarons CB, Sentovich SM. Successful sphinctersparing surgery for all anal fistulas. Dis Colon Rectum. 2007;50: Williams JG, MacLeod CA, Rothenberger DA, Goldberg SM. Seton treatment of high anal fistulae. Br J Surg. 1991;78: Isbister WH, Al Sanea N. The cutting seton: an experience at King Faisal Specialist Hospital. Dis Colon Rectum. 2001;44: Mentes BB, Oktemer S, Tezcaner T, Azili C, Leventoğlu S, Oğuz M. Elastic one-stage cutting seton for the treatment of high anal fistulas: preliminary results. Tech Coloproctol. 2004;8: Eitan A, Koliada M, Bickel A. The use of the loose seton technique as a definitive treatment for recurrent and persistent high trans-sphincteric anal fistulas: a long-term outcome [published online ahead of print February 24, 2009]. J Gastrointest Surg. doi: /s Theerapol A, So BY, Ngoi SS. Routine use of setons for the treatment of anal fistulae. Singapore Med J. 2002;43: Chuang-Wei C, Chang-Chieh W, Cheng-Wen H, Tsai-Yu L, Chun-Che F, Shu-Wen J. Cutting seton for complex anal fistulas. Surgeon. 2008;6:
Perianal Abscess and Fistula-in-ano. Background
 Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Treatment of Fistula in Ano. Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012
 Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract
 LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract Charles TSANG Division of Colorectal Surgery, National University Health System drcharlestsang@gmail.com Evolution in the
LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract Charles TSANG Division of Colorectal Surgery, National University Health System drcharlestsang@gmail.com Evolution in the
The enigma of the transsphincteric anal fistula. Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden
 The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
Original Policy Date
 MP 7.01.103 Plugs for Fistula Repair Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.01.103 Plugs for Fistula Repair Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies
 DOI 10.1007/s10151-015-1282-9 ORIGINAL ARTICLE Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies P. Giamundo L. Esercizio M. Geraci L. Tibaldi M. Valente Received:
DOI 10.1007/s10151-015-1282-9 ORIGINAL ARTICLE Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies P. Giamundo L. Esercizio M. Geraci L. Tibaldi M. Valente Received:
Anal Surgery. Colon and Rectal Surgery. Surgery of the Anus. Hemorrhoids Fistula Fissure Abscess
 Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial
 Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
Anorectal Abscess and Fistula
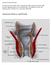 Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Transanal Radiofrequency Treatment of Fecal Incontinence
 Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Closure of fistula-in-ano with laser FiLaC TM : an effective novel sphincter-saving procedure for complex disease
 Original article doi:10.1111/codi.12440 Closure of fistula-in-ano with laser FiLaC TM : an effective novel sphincter-saving procedure for complex disease P. Giamundo, M. Geraci, L. Tibaldi and M. Valente
Original article doi:10.1111/codi.12440 Closure of fistula-in-ano with laser FiLaC TM : an effective novel sphincter-saving procedure for complex disease P. Giamundo, M. Geraci, L. Tibaldi and M. Valente
2.01.58. Description. Section: Medicine Effective Date: January 15, 2015 Subsection: Medicine Original Policy Date: June 7, 2012 Subject: Page: 1 of 6
 Page: 1 of 6 Last Review Status/Date: December 2014 Description Radiofrequency (RF) energy has been investigated as a minimally invasive treatment of fecal incontinence, referred to as the Secca procedure.
Page: 1 of 6 Last Review Status/Date: December 2014 Description Radiofrequency (RF) energy has been investigated as a minimally invasive treatment of fecal incontinence, referred to as the Secca procedure.
Section: Surgery Last Reviewed Date: December 2013. Policy No: 129 Effective Date: March 1, 2014
 Medical Policy Manual Topic: Transanal Radiofrequency Treatment of Fecal Incontinence Date of Origin: December 2003 Section: Surgery Last Reviewed Date: December 2013 Policy No: 129 Effective Date: March
Medical Policy Manual Topic: Transanal Radiofrequency Treatment of Fecal Incontinence Date of Origin: December 2003 Section: Surgery Last Reviewed Date: December 2013 Policy No: 129 Effective Date: March
Current management of anal fistulas in Crohn s disease
 Review paper Current management of anal fistulas in Crohn s disease Jacek Hermann 1, Piotr Eder 2, Tomasz Banasiewicz 1, Konrad Matysiak 1, Liliana Łykowska-Szuber 2 1 Chair and Department of General and
Review paper Current management of anal fistulas in Crohn s disease Jacek Hermann 1, Piotr Eder 2, Tomasz Banasiewicz 1, Konrad Matysiak 1, Liliana Łykowska-Szuber 2 1 Chair and Department of General and
Victims Compensation Claim Status of All Pending Claims and Claims Decided Within the Last Three Years
 Claim#:021914-174 Initials: J.T. Last4SSN: 6996 DOB: 5/3/1970 Crime Date: 4/30/2013 Status: Claim is currently under review. Decision expected within 7 days Claim#:041715-334 Initials: M.S. Last4SSN: 2957
Claim#:021914-174 Initials: J.T. Last4SSN: 6996 DOB: 5/3/1970 Crime Date: 4/30/2013 Status: Claim is currently under review. Decision expected within 7 days Claim#:041715-334 Initials: M.S. Last4SSN: 2957
EVIDENCE BASED TREATMENT OF CROHN S DISEASE. Dr E Ndabaneze
 EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Patient information regarding care and surgery associated with ULCERATIVE COLITIS
 Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
MANAGEMENT OF COMPLEX POSTERIOR HORSESHOE ANAL FISTULA BY A MODIFIED HANLEY PROCEDURE: CLINICAL EXPERIENCE AND REVIEW OF 28 PATIENTS
 Basrah Journal Of Surgery MANAGEMENT OF COMPLEX POSTERIOR HORSESHOE ANAL FISTULA BY A MODIFIED HANLEY PROCEDURE: CLINICAL EXPERIENCE AND REVIEW OF 28 PATIENTS Ibrahim Falih Noori MBChB, CABS, FICS, DS,
Basrah Journal Of Surgery MANAGEMENT OF COMPLEX POSTERIOR HORSESHOE ANAL FISTULA BY A MODIFIED HANLEY PROCEDURE: CLINICAL EXPERIENCE AND REVIEW OF 28 PATIENTS Ibrahim Falih Noori MBChB, CABS, FICS, DS,
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY
 YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606
 October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
Treatment of non-ibd anal fistula
 CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Treatment of non-ibd anal fistula Lilli Lundby, Kikke Hagen, Peter Christensen, Steen Buntzen, Ole Thorlacius-Ussing, Jens Andersen, Marek Krupa & Niels Qvist
CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Treatment of non-ibd anal fistula Lilli Lundby, Kikke Hagen, Peter Christensen, Steen Buntzen, Ole Thorlacius-Ussing, Jens Andersen, Marek Krupa & Niels Qvist
Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement
 CLINICAL REPORT Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement Edwin F. de Zoeten, z Brad A. Pasternak, Peter Mattei, Robert E. Kramer, and y Howard
CLINICAL REPORT Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement Edwin F. de Zoeten, z Brad A. Pasternak, Peter Mattei, Robert E. Kramer, and y Howard
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures
 Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Wound Care on the Field. Objectives
 Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
GIANT HERNIA REPAIR MY EXPERIENCE
 GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
What to Expect from Intestinal Ultrasonography
 261) What to Expect from Intestinal Ultrasonography Červenková J., Steyerová P. Charles University in Prague, First Faculty of Medicine and General Teaching Hospital, Department of Radiology, Prague, Czech
261) What to Expect from Intestinal Ultrasonography Červenková J., Steyerová P. Charles University in Prague, First Faculty of Medicine and General Teaching Hospital, Department of Radiology, Prague, Czech
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Topic: Plugs for Enteric and Anorectal Fistula Repair Date of Origin: August 2010. Section: Surgery Last Reviewed Date: May 2016
 Medical Policy Manual Topic: Plugs for Enteric and Anorectal Fistula Repair Date of Origin: August 2010 Section: Surgery Last Reviewed Date: May 2016 Policy No: 175 Effective Date: July 1, 2016 IMPORTANT
Medical Policy Manual Topic: Plugs for Enteric and Anorectal Fistula Repair Date of Origin: August 2010 Section: Surgery Last Reviewed Date: May 2016 Policy No: 175 Effective Date: July 1, 2016 IMPORTANT
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Effects of Pregnancy & Delivery on Pelvic Floor
 Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Cancer of the Cervix
 Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
COMPLICATIONS OF FISTULA REPAIR SURGERY. Sherif Mourad
 COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
Complications that may occur with ulcerative colitis:
 Ulcerative Colitis What is ulcerative colitis? Ulcerative colitis is one of the major forms of inflammatory bowel disease. The other major form is Crohn s disease. Ulcerative colitis is felt to be due
Ulcerative Colitis What is ulcerative colitis? Ulcerative colitis is one of the major forms of inflammatory bowel disease. The other major form is Crohn s disease. Ulcerative colitis is felt to be due
(Anorectum Anorectum)
 Surgical anatomy (Anorectum Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD Associate Professor Surgical anatomy (Anorectum Anorectum) Surgical anatomy
Surgical anatomy (Anorectum Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD Associate Professor Surgical anatomy (Anorectum Anorectum) Surgical anatomy
Gallstone Ileus. Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005
 Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
2/21/2016. Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape. Disclosures. Objectives. No Relevant Disclosures
 Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape David R. Ellington, MD, FACOG Assistant Professor Division of Urogynecology and Pelvic Reconstructive Surgery Disclosures No Relevant Disclosures
Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape David R. Ellington, MD, FACOG Assistant Professor Division of Urogynecology and Pelvic Reconstructive Surgery Disclosures No Relevant Disclosures
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
BIOGRAPHICAL SKETCH. Assistant Professor of Clinical Surgery Georgetown University School of Medicine
 BIOGRAPHICAL SKETCH NAME Stahl, Thomas J. era COMMONS USER NAME (credential, e.g., agency login) POSITION TITLE Interim Chair, Department of Surgery MedStar Washington Hospital Center Assistant Professor
BIOGRAPHICAL SKETCH NAME Stahl, Thomas J. era COMMONS USER NAME (credential, e.g., agency login) POSITION TITLE Interim Chair, Department of Surgery MedStar Washington Hospital Center Assistant Professor
Bridging Techniques. What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS
 Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
M O V I N G F R E E LY. HerniaCenter. The Columbia Hernia Center at ColumbiaDoctors Midtown
 M O V I N G F R E E LY HerniaCenter The Columbia Hernia Center at ColumbiaDoctors Midtown Director, Dr. Peter L. Geller The Columbia Hernia Center brings together a group of surgeons adept in using the
M O V I N G F R E E LY HerniaCenter The Columbia Hernia Center at ColumbiaDoctors Midtown Director, Dr. Peter L. Geller The Columbia Hernia Center brings together a group of surgeons adept in using the
Tone Up Your Pelvic Floor. A regular pelvic floor exercise ( Kegel ) routine can prevent symptoms before, during, and after childbirth.
 Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
INFLAMMATORY BOWEL DISEASE: A PRACTICAL APPROACH, SERIES #40. New Advances in Surgical Treatment of Crohn s Disease
 Seymour Katz, M.D., Series Editor New Advances in Surgical Treatment of Crohn s Disease Sharon L. Stein Fabrizio Michelassi Despite many advances in medical treatment of Crohn s disease, the majority of
Seymour Katz, M.D., Series Editor New Advances in Surgical Treatment of Crohn s Disease Sharon L. Stein Fabrizio Michelassi Despite many advances in medical treatment of Crohn s disease, the majority of
INFORMED CONSENT DERMABRASION
 INFORMED CONSENT DERMABRASION INSTRUCTION This is an informed-consent document which has been prepared to help your plastic surgeon inform you about dermabrasion, its risks, and alternative treatments.
INFORMED CONSENT DERMABRASION INSTRUCTION This is an informed-consent document which has been prepared to help your plastic surgeon inform you about dermabrasion, its risks, and alternative treatments.
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Stadards in Abdominoperineal Resection
 Stadards in Abdominoperineal Resection Manuel Francisco T. Roxas, MD, FPCS, FPSCRS, FACS Clinical Associate Professor, University of the Philippines Chief, Section of Colorectal Surgery, Department of
Stadards in Abdominoperineal Resection Manuel Francisco T. Roxas, MD, FPCS, FPSCRS, FACS Clinical Associate Professor, University of the Philippines Chief, Section of Colorectal Surgery, Department of
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy
 Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
Bile Leaks After Laparoscopic Cholecystectomy. Kings County Hospital Center Eliana A. Soto, MD
 Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Evaluation and Management of the Breast Mass. Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003
 Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES
 Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
Mesh Erosion and What to do
 Disclosures Mesh Erosion and What to do None Michelle Y. Morrill, MD Chief of Urogynecology, TPMG Director of Urogynecology, Kaiser San Francisco Assistant Professor, Volunteer Faculty Dept of Ob/Gyn,
Disclosures Mesh Erosion and What to do None Michelle Y. Morrill, MD Chief of Urogynecology, TPMG Director of Urogynecology, Kaiser San Francisco Assistant Professor, Volunteer Faculty Dept of Ob/Gyn,
Using the COLO and HYST Surgical Site Infection (SSI) Medical Record Abstraction Tools
 Using the COLO and HYST Surgical Site Infection (SSI) Medical Record Abstraction Tools Janet Brooks RN, BSN, CIC Nurse Consultant State HAI Grantee Meeting November 14, 2013 National Center for Emerging
Using the COLO and HYST Surgical Site Infection (SSI) Medical Record Abstraction Tools Janet Brooks RN, BSN, CIC Nurse Consultant State HAI Grantee Meeting November 14, 2013 National Center for Emerging
Open the Flood Gates Urinary Obstruction and Kidney Stones. Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke
 Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY
 UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY Robert Fridman DPM, Jarrett Cain DPM, Lowell Weil Jr. DPM,
UNILATERAL VS. BILATERAL FIRST RAY SURGERY: A PROSPECTIVE STUDY OF 186 CONSECUTIVE CASES COMPLICATIONS, PATIENT SATISFACTION, AND COST TO SOCIETY Robert Fridman DPM, Jarrett Cain DPM, Lowell Weil Jr. DPM,
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Definition(s) of Diverticular Disease
 Falk-Symposium 148 "Divertikelkrankheit: Neue Erkenntnisse einer Volkskrankheit" München; 17.-18. Juni 2005; Session II 11:15-12:20 Definition(s) of Diverticular Disease Prof. Edmund Neugebauer, Dr. J.
Falk-Symposium 148 "Divertikelkrankheit: Neue Erkenntnisse einer Volkskrankheit" München; 17.-18. Juni 2005; Session II 11:15-12:20 Definition(s) of Diverticular Disease Prof. Edmund Neugebauer, Dr. J.
IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology
 IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology This performance feedback document and the accompanying spreadsheet include
IV Contrast Extravasation PQI Project Feed-Back Document from the Society of Abdominal Radiology & American College of Radiology This performance feedback document and the accompanying spreadsheet include
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Comparative analysis of summary scoring systems in measuring fecal incontinence
 J Korean Surg Soc 2011;81:326-331 http://dx.doi.org/10.4174/jkss.2011.81.5.326 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903ㆍeISSN 2093-0488 Comparative analysis of summary
J Korean Surg Soc 2011;81:326-331 http://dx.doi.org/10.4174/jkss.2011.81.5.326 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903ㆍeISSN 2093-0488 Comparative analysis of summary
Yu-Li Lin 1, Tien-Jye Chang 2
 Formos J Surg 009;4:6-67 6 Original Articles Effect of a Pediatric Surgeon on Pediatric Inguinal Hernia Repair --- Evaluation of the Importance of Surgeons with Subspecialty Training by a Single-Hospital
Formos J Surg 009;4:6-67 6 Original Articles Effect of a Pediatric Surgeon on Pediatric Inguinal Hernia Repair --- Evaluation of the Importance of Surgeons with Subspecialty Training by a Single-Hospital
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Surgical Site Infection. Kings County Hospital Center Audrey C. Durrant 6/10/2005
 Surgical Site Infection Kings County Hospital Center Audrey C. Durrant 6/10/2005 Case Presentation HPI patient xx year old presented with approximately xx days periumbillical pain 10/10 on pain scale,
Surgical Site Infection Kings County Hospital Center Audrey C. Durrant 6/10/2005 Case Presentation HPI patient xx year old presented with approximately xx days periumbillical pain 10/10 on pain scale,
Surgical Site Infection Prevention
 Surgical Site Infection Prevention 1 Objectives 1. Discuss risk factors for SSI 2. Describe evidence-based best practices for SSI prevention 3. State principles of antibiotic prophylaxis 4. Discuss novel
Surgical Site Infection Prevention 1 Objectives 1. Discuss risk factors for SSI 2. Describe evidence-based best practices for SSI prevention 3. State principles of antibiotic prophylaxis 4. Discuss novel
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
CERVICAL MEDIASTINOSCOPY WITH BIOPSY
 INFORMED CONSENT INFORMATION ADDRESSOGRAPH DATA CERVICAL MEDIASTINOSCOPY WITH BIOPSY You have decided to have an important procedure and we appreciate your selection of UCLA Healthcare to meet your needs.
INFORMED CONSENT INFORMATION ADDRESSOGRAPH DATA CERVICAL MEDIASTINOSCOPY WITH BIOPSY You have decided to have an important procedure and we appreciate your selection of UCLA Healthcare to meet your needs.
Original Policy Date
 MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
PROPERTY OF ELSEVIER SAMPLE CONTENT - NOT FINAL
 Oncoplastic breast conservation surgery Melvin J Silverstein C H A P T E R 5 Introduction Oncoplastic breast conservation surgery combines oncologic principles with plastic surgical techniques. But it
Oncoplastic breast conservation surgery Melvin J Silverstein C H A P T E R 5 Introduction Oncoplastic breast conservation surgery combines oncologic principles with plastic surgical techniques. But it
Acticon. Neosphincter. Getting Back to Life. Information Guide treatment for fecal incontinence
 Acticon Neosphincter Information Guide treatment for fecal incontinence Getting Back to Life Introduction If you suffer from loss of bowel control, you are not alone. Did you know that over 2% of the worldwide
Acticon Neosphincter Information Guide treatment for fecal incontinence Getting Back to Life Introduction If you suffer from loss of bowel control, you are not alone. Did you know that over 2% of the worldwide
A PATIENT S GUIDE TO ABLATION THERAPY
 A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
