Lumbar transforaminal injection is a commonly performed
|
|
|
- Easter Mosley
- 7 years ago
- Views:
Transcription
1 SPINE Volume 37, Number 9, pp , Lippincott Williams & Wilkins TECHNIQUE Ultrasound-Guided Lumbar Transforaminal Injections Feasibility and Validation Study Michael Gofeld, MD, Sandee J. Bristow, MD, Sheila C. Chiu, DO, Carlton K. McQueen, MD, and Laurent Bollag, MD Study Design. Preclinical feasibility study. Objective. Evaluation and validation of ultrasound-guided lumbar transforaminal injections. Summary of Background Data. Lumbar transforaminal injections are routinely implemented in the interventional management of spinal radicular pain. Typically, these injections are administered under fluoroscopy or computed tomography. Although radiological guidance provides anatomical precision and accuracy, it is associated with radiation exposure and cannot be performed during outpatient visits or at bedside. Ultrasound-guided techniques have been previously described; however, the methodological generalizability remained unknown and validation against routine fluoroscopy has never been conducted on multiple spinal levels. Methods. We addressed the procedural accuracy of ultrasoundguided lumbar transforaminal injections and proposed anatomically sound approach. Fluoroscopic validation was performed. Results. Of the 50 planned injections, 46 procedures were performed. L5/S1 foraminal access was impossible in 4 cases (8%). Fluoroscopy confirmed the correct foraminal placement in all 46 injections (100%). The contrast-spread pattern was intraforaminal in 42 cases (91.3%) and extraforaminal (nerve root) in 4 cases (8.7%). When intraforaminal pattern was detected on anteroposterior image, lateral fluoroscopy demonstrated ventral epidural flow in all occasions. In 3 cases, intravascular injection was detected (6.5%). Conclusion. Ultrasound-guided lumbar transforaminal injections are accurate and feasible in the preclinical setting. From the University of Washington, Anesthesiology & Pain Medicine and Neurological Surgery, Seattle. Acknowledgment date: March 22, First revision date: May 31, Second revision date: July 9, Acceptance date: August 5, The manuscript submitted does not contain information about medical device(s)/drug(s). No funds were received in support of this work. Although one or more of the author(s) has/have received or will receive benefits for personal or professional use from a commercial party related directly or indirectly to the subject of this manuscript, benefits will be directed solely to a research fund, foundation, educational institution, or other nonprofit organization which the author(s) has/have been associated. Address correspondence and reprint requests to Michael Gofeld, MD, University of Washington, Anesthesiology & Pain Medicine and Neurological Surgery, 4225 Roosevelt Way NE, Ste 401, Seattle, WA 98105; gofeld@uw.edu Key words: ultrasound, transforaminal injection, feasibility. Spine 2012 ; 37 : Lumbar transforaminal injection is a commonly performed procedure to treat spinal radicular pain. Typically, these injections are administered under fluoroscopy or computed tomography. Although considered relatively safe, several case reports of devastating neurological complications 1 4 have been published. All reported events of permanent neurological damage were linked to the injections of nonsoluble particulate steroids. Current recommendations for safer and more accurate techniques include the adoption of radiopaque real-time and/or digital subtraction contrast injection prior to the instillation of a steroid. 5 Other technical pearls, such as injection of a local anesthetic first 4, 6 and use of a water-soluble steroid, 7 have been suggested. A novel ultrasound-guided lumbar transforaminal approach described recently in the literature 8, 9 appeared in the current procedural terminology 10 and was implemented in clinical practice. The absence of radiation exposure, equipment affordability, and bedside setting 11 favorably compare ultrasound with traditional radiological imaging. However, several concerns should be addressed, such as accuracy, reliability, and patient safety. The method of Galiano et al, 8 for example, outlines so-called posterior foraminal approach when needle was directed toward the nerve root. It may lead to an inadvertent needle placement into the neuroaxial compartment without realization of the mishap. A definite sonographic landmark has yet to be described in published literature. We modified the original in-plane technique 8 and developed a different, anatomically sound approach. MATERIALS AND METHODS The main outcome of the study was to confirm the feasibility of ultrasound-guided lumbar transforaminal injections on multiple levels. Specifically, accuracy of the spinal segment identification, patterns of the radiopaque contrast spread, and visibility of the defined target were evaluated. Three female and 2 male unembalmed cadavers donated to the University of Washington Willed Body program were used. No institutional review board approval was required DOI: /BRS.0b013e April 2012
2 because the personal health data, excluding biometrics, of the deceased were not disclosed to investigators. Five transforaminal injections (L1/L2 L5/S1) were planned to be administered bilaterally on each specimen (10 injections per specimen). We intended to complete 50 injections in total. Specimens were placed in prone position. Towel rolls were placed under the abdomen to alleviate lumbar lordosis. Paramedian sagittal sonography was performed at the level of transverse processes for the orientation purposes. The second scanning was performed in the short axis. The operator announced the level of injection. The injections were administered by using the C5-1 broadband curved array transducer and the CX-50 CompactXtreme ultrasound system (Phillips, Eindhoven, the Netherlands). The ultrasound transducer was positioned at the short axis paramedian view between 2 adjacent transverse processes, so the sonogram reflected the spinous process, lamina, and dorsal part of the vertebral body ( Figure 1 ). If the exiting nerve was seen, the transducer was shifted caudally to avoid trespassing the nerve root. Twentygauge 5-inch Quincke-type spinal needles were inserted by using the in-plane approach, aiming to for the most medially visible shadow of the vertebral body. Once the needle touched the bone surface, 1 ml of iohexol (Omnipaque) 240 mgi/ml was injected. Then anteroposterior and lateral fluoroscopy was performed. In the event of an intravascular contrast spread, the injections were repeated by using 20-gauge Coudé (curved) versions of the blunt nerve block needle (Epimed, Johnstown, NY). The vertebral level of injection, position of the needle tip, contrast flow pattern, and aberrant contrast spread were registered. RESULTS All cadavers had skin-to-vertebra distance of 6 to 9 cm measured on the ultrasound examination. L5/S1 in-plane injections were deemed impossible in 2 specimens, that is, on 4 vertebral levels (8%). In those cases, L5 vertebral body could not be visualized. Therefore, total 46 injections were administered. Fluoroscopy confirmed the foraminal placement in all 46 injections (100%). As expected, the needle tip was located at the ventral part of the intervertebral foramen on the lateral view and under the pedicle (6-o clock position) on the anteroposterior view. The cephalocaudad tip position was varied between the lower part of the cephalad vertebra and the upper part of the caudad vertebra ( Figure 2 ). The contrast spread pattern was intraforaminal in 42 cases (91.3%) and extraforaminal (nerve root) in 4 cases (8.7%). All intraforaminal injections cases demonstrated ventral epidural flow of the injected radiopaque contrast agent on the lateral fluoroscopy ( Figures 3 and 4 ). The correct spinal level was identified in all 46 cases (100%). As stated, in 2 L5/S1 cases, the vertebral body could not be detected. We nevertheless attempted injections and fluoroscopy confirmed erroneous L4/5 or sacral placement, most probably related to a deviation of the needle tip by the L5 transverse process. Therefore, on the basis of predetermined imaging inclusion criteria (lamina and vertebral body must be seen), we decided to exclude those L5/S1 cases from the final analysis. All 4 injections with extraforaminal spread occurred in a 104-year-old female cadaver. Intrathecal contrast injection was administered. The obtained myelographic image detected multilevel severe spinal stenosis, which could explain the aberrant extraforaminal contrast flow. While using a 20-gauge Quinke-type spinal needle, intravascular venous pattern was detected in 3 cases (6.5%) ( Figure 5 ). The intravascular injections occurred at the left L1/2, L2/3, and the right L5/S1 levels. The L2/3 injection resulted in both epidural and intravascular contrast flow. Repeated injection with a 20-gauge Coudé needle revealed no intravascular uptake. DISCUSSION A modified in-plane technique aiming vertebral body as a sonographic landmark has not been previously described. When the needle is resting at the bone, no further advancement into the neuraxial compartment is possible. The injection administered in this position of the needle tip resulted in the transforaminal epidural flow in most cases. The methodology Figure 1. Axial sonogram of lumbar vertebra. S indicates spinous Figure 2. Anteroposterior fluoroscopy with typical distribution of the process; L, lamina; V, vertebral body; arrowhead, target for injection. observed needle positions (white eclipse). Spine 809
3 Figure 3. Anteroposterior (left) and lateral (right) fluoroscopy of the needle position and the contrast flow at L5/S1 level. developed during the experiments was centered on improving success and eliminating potential complications. All needle placements were done at the correct vertebral level, and in 91.7% ensued in a ventral epidural contrast-dye spread confirmed by fluoroscopy. The intravascular injection rate was 6.5%. This is comparable with the incidence reported in a clinical study. 12 Another publication rated occurrence of this event as high as 11.2%. 13 The sample size (n = 761) in the article by Furman et al 13 was substantially larger than that in this study. In any case, the difference may not reflect potential superiority of the ultrasound-guided injections. When no contrast-enhanced fluoroscopy is used, inadvertent intravascular injections cannot be recognized in a procedural setting. Clinical comparative imaging research may be needed to answer this question. Notably, the lumbar nerve root and blood vessel imaging is a function of depth and echogenicity of the surrounding tissues. Therefore, poorly visualized nerve may be traversed by needle. Use of a blunt Coudé needle may prevent nerve root trauma and intravascular injection. It seemed that the vertebral body and the intervertebral disc have different acoustic properties. While the bone has hyperechoic signal, the disc appearance is rather hypoechoic. This phenomenon was previously published. 14 However, the observation was valid only in the younger specimen. Aged, degenerated discs are heavily calcified and cannot be differentiated from bone by the sonographic examination. Ultrasound-guided lumbar transforaminal injections are deemed controversial among interventional pain physicians. According to current beliefs, ultrasonography may not guarantee needle placement at the correct level, accurate spread of the injectate, and prevention of the intravascular injection. Our work at least partially addressed these concerns: precise needle placement was feasible and the correct vertebral levels can clearly be identified. Use of a blunt-tip needle may reduce inadvertent intra-arterial injection, but probably not intravenous injection, which may lead to false-negative results. The procedure, however, can then be repeated under fluoroscopy. Previous publications 8, 9 already confirmed the feasibility of the ultrasound-guided transforaminal injections. However, the approach described by Galiano et al, 8 if applied in the clinical setting, may result in needle advancement into the neuroaxial compartment without notice. Perhaps, in order to prevent such advancement, Galiano et al 8 advised halting needle progress when it reached the dorsal foraminal opening laterally to the superior articular process. It is unlikely that an injectate will extend to the ventral epidural compartment (the recommended location for transforaminal injection) when the needle was placed dorsally and laterally. Most likely, it will spread onto the exiting nerve root. No contrast dye injection was used in the study of Galiano et al 8 to confirm epidural spread. We experimentally tested the possibility of the neuroaxial injection by using the previously described Figure 4. Anteroposterior (left) and lateral (right) fluoroscopy of the needle position and the contrast flow at L4/L5 level April 2012
4 result of the procedure was disappointing, practitioners may consider repeating the injection by using fluoroscopy or computed tomography. Blunt-tip Coudé needle may also be helpful in avoiding direct nerve trauma and intravascular injection. Ultrasound-guided lumbar transforaminal injections were accurate and feasible in the preclinical setting. Clinical correlation was required for dissemination of this novel technique in routine practice. Figure 5. Anteroposterior fluoroscopy demonstrated aberrant (vascular) contrast flow. technique. Once the needle tip approached the level of the articular processes, its further progress was shadowed by bony structures and the needle entered the neuroaxial space ( Figure 6 ). Sato et al 9 used an out-of-plane technique and demonstrated feasibility and accuracy of the L5 nerve root injection. In 3 cases (3.8%), injection was not successful because of L5 articular process protruded laterally. Approach of Sato et al 9 may be considered for the L5/S1 injections, because the technique used in this study showed poor accessibility of the L5/S1 foramen via the in-plane method. At this stage, ultrasound-guided transforaminal injections may be furnished at the practitioner s discretion, when the dorsal vertebral body is visible at the foraminal level. Only water-soluble corticosteroids should be injected, and if the Key Points Previously described ultrasound-guided transforaminal injection technique was modified. A modified in-plane technique aiming vertebral body as a sonographic landmark prevents further advancement into the neuraxial compartment. This method has advantages of a bedside procedural setting and spares patients and personnel from radiation exposure. Ultrasonography provides reliable setup in localizing foramina and performing transforaminal lumbar injections. Water-soluble steroids should be used when practicing this technique. Acknowledgments This work would not be possible without the support of the University of Washington Body Willed program. Philips Healthcare provided necessary equipment. IRB approval was not required. References 1. Houten J, Errico T. Paraplegia after lumbosacral nerve root block: report of three cases. Spine J 2002 ; 2 : Huntoon M, Martin D. Paralysis after transforaminal epidural injection and previous spinal surgery. Reg Anesth Pain Med 2004 ; 29 : Somayaji HM, Saifuddin AM, Casey AF, et al. Spinal cord infarction following therapeutic computed tomography-guided left L2 nerve root injection. Spine 2005 ; 30 : E Kennedy DJ, Dreyfuss P, Aprill CN, et al. Paraplegia following image-guided transforaminal lumbar spine epidural steroid injection: two case reports. Pain Med 2009 ; 10 : Bogduk N, Dreyfuss P, Baker R, et al. Complications of spinal diagnostic and treatment procedures. Pain Med 2008 ; 6 : S Karasek M, Bogduk N. Temporary neurologic deficit after cervical transforaminal injection of local anesthetic. Pain Med 2004 ; 5 : Lee JW, Park KW, Chung SK, et al. Cervical transforaminal epidural steroid injection for the management of cervical radiculopathy: a comparative study of particulate versus non-particulate steroids. Skeletal Radiol 2009 ; 38 : Galiano K, Obwegeser AA, Bodner G, et al. Real-time sonographic imaging for periradicular injections in the lumbar spine: a sonographic anatomic study of a new technique. J Ultrasound Med 2005 ; 24 : Sato M, Simizu S, Kadota R, et al. Ultrasound and nerve stimulation-guided L5 nerve root block. Spine 2009 ; 34 : Figure 6. Anteroposterior fluoroscopy demonstrated potential severe complication inadvertent neuraxial needle placement. Spine 811
5 10. CPT Washington, DC : American Medical Association Press ; Pro edition; October 30, 2010 : Gofeld M. Ultrasonography in pain medicine: a critical review. Pain Pract 2008 ; 8 : Nahm FS, Lee CJ, Lee SH, et al. Risk of intravascular injection in transforaminal epidural injections. Anaesthesia 2010 ; 65 : Furman M, O Brien E, Zgleszewski T. Incidence of intravascular penetration in transforaminal lumbosacral epidural steroid injections. Spine 2000 ; 25 : Tervonen O, Lähde S, Vanharanta H. Ultrasound diagnosis of lumbar disc degeneration. Comparison with computed tomography/ discography. Spine 1991 ; 16 : April 2012
 Ultrasound Evaluation of Low Back Pain Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Ultrasound Evaluation of Low Back Pain Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Report therapeutic hip injection under fluoro with 20610 and 77002
 Report therapeutic hip injection under fluoro with 20610 and 77002 Use the following Q & A to determine how to bill imaging when you provide a hip injection. Question: How do you report an injection of
Report therapeutic hip injection under fluoro with 20610 and 77002 Use the following Q & A to determine how to bill imaging when you provide a hip injection. Question: How do you report an injection of
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
Ultrasound-guided injections in the lumbar spine
 Continuing education Medical Ultrasonography 2011, Vol. 13, no. 1, 54-58 Ultrasound-guided injections in the lumbar spine Alexander Loizides 1, Siegfried Peer 1, Michaela Plaikner 1, Verena Spiss 1, Klaus
Continuing education Medical Ultrasonography 2011, Vol. 13, no. 1, 54-58 Ultrasound-guided injections in the lumbar spine Alexander Loizides 1, Siegfried Peer 1, Michaela Plaikner 1, Verena Spiss 1, Klaus
Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation
 167 Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation Richard F. Costello, DO a, *, Douglas P. Beall, MD a,b MAGNETIC RESONANCE IMAGING CLINICS Magn Reson Imaging Clin N
167 Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation Richard F. Costello, DO a, *, Douglas P. Beall, MD a,b MAGNETIC RESONANCE IMAGING CLINICS Magn Reson Imaging Clin N
-Increases the safety, accuracy and efficiency of certain spine procedures
 Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
BODY BODY PEDICLE PEDICLE TRANSVERSE TRANSVERSE PROCESS PROCESS
 Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
Anatomy and Terminology of the Spine. Bones of the Spine (Vertebrae)
 Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Percutaneous Treatment of Vertebral Compression Fractures
 Percutaneous Treatment of Vertebral Compression Fractures A Meta-analysis of Complications Michael J. Lee, MD, Mark Dumonski, MD, Patrick Cahill, MD, Tom Stanley, MD, Daniel Park, MD, and Kern Singh, MD
Percutaneous Treatment of Vertebral Compression Fractures A Meta-analysis of Complications Michael J. Lee, MD, Mark Dumonski, MD, Patrick Cahill, MD, Tom Stanley, MD, Daniel Park, MD, and Kern Singh, MD
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Procedure. 2 29827 $ 3,560 $ 1,476 Arthroscopy, shoulder, surgical; with rotator cuff repair 5.5% 241.1%
 Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Cervical Transforaminal Epidural injections Pro-view. Richard Kendall, D.O. Associate Professor, PM&R
 Cervical Transforaminal Epidural injections Pro-view Richard Kendall, D.O. Associate Professor, PM&R Disclosures No financial disclosures Overview of procedure Anatomical reasoning Physiological reasoning
Cervical Transforaminal Epidural injections Pro-view Richard Kendall, D.O. Associate Professor, PM&R Disclosures No financial disclosures Overview of procedure Anatomical reasoning Physiological reasoning
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Thoracic Spine Anatomy
 A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Thoracic Epidural Catheterization Using Ultrasound in Obese Patients for Bariatric Surgery
 IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING
 POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
Vertebral anatomy study guide. Human Structure Summer 2015. Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey.
 Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Pain Management. the primary procedure allowable reimbursement; 50% of add-on. Injection/Destruction Procedures
 Pain Management In addition to the General Guidelines, this section applies to the unique guidelines for Pain Management services. I. Reimbursement for Pain Management Services A. Pain Management Base
Pain Management In addition to the General Guidelines, this section applies to the unique guidelines for Pain Management services. I. Reimbursement for Pain Management Services A. Pain Management Base
Problems. Knowing. back of the
 Introduction Welcome to BodyZone Physiotherapy patient resource about Cervical Spine Problems. Knowing the main parts of your neck and how these parts work is important as you learn to care for your neck
Introduction Welcome to BodyZone Physiotherapy patient resource about Cervical Spine Problems. Knowing the main parts of your neck and how these parts work is important as you learn to care for your neck
CPT Changes in Spine 2012
 CPT Changes in Spine 2012 Are you prepared? Presented by Barbara Cataletto, MBA, CPC Disclaimer The following presentations are not to be considered a replacement for the Current Procedural Terminology
CPT Changes in Spine 2012 Are you prepared? Presented by Barbara Cataletto, MBA, CPC Disclaimer The following presentations are not to be considered a replacement for the Current Procedural Terminology
Effects of vertebral axial decompression on intradiscal pressure
 This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
Physician Coding and Payment Guide 2015
 Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
October 3, 2005. RE: Appropriate use of CPT 76003 and 76005. Dear Ms. Kotowicz:
 October 3, 2005 Grace M. Kotowicz, Director CPT Editorial Research and Development American Medical Association 515 North State Street Chicago, IL 60610 RE: Appropriate use of CPT 76003 and 76005 Dear
October 3, 2005 Grace M. Kotowicz, Director CPT Editorial Research and Development American Medical Association 515 North State Street Chicago, IL 60610 RE: Appropriate use of CPT 76003 and 76005 Dear
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
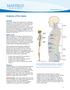 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
Compression Fractures
 September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Lumbar Spine Anatomy. eorthopod.com 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.
 A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
Skeletal System. Axial Skeleton: Vertebral Column and Ribs
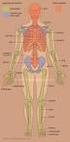 Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Ultrasound, breast, unilateral, real time with image documentation, including axilla when performed; complete 76642 limited
 Radiology CPT Coding Updates for 2015 Note: This article contains coding information from the 2015 Physician's Current Procedural Terminology (CPT ) Manual. CPT is a registered trademark of the American
Radiology CPT Coding Updates for 2015 Note: This article contains coding information from the 2015 Physician's Current Procedural Terminology (CPT ) Manual. CPT is a registered trademark of the American
Sonographically Guided Ilioinguinal Nerve Block
 Technical Advance Sonographically Guided Ilioinguinal Nerve Block Michael Gofeld, MD, Monique Christakis, MD, FRCPC Objective. The aim of this study was to describe a sonographically guided ilioinguinal
Technical Advance Sonographically Guided Ilioinguinal Nerve Block Michael Gofeld, MD, Monique Christakis, MD, FRCPC Objective. The aim of this study was to describe a sonographically guided ilioinguinal
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN
 Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Workers Compensation Insurance
 Workers Compensation Insurance New Hampshire Insurance Department Detailed Medical Cost Comparison The following exhibits compare the cost of Workers Compensation Medical services in New Hampshire to our
Workers Compensation Insurance New Hampshire Insurance Department Detailed Medical Cost Comparison The following exhibits compare the cost of Workers Compensation Medical services in New Hampshire to our
Selective Nerve Root Block
 Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Virtual 3D Model of the Lumbar Spine
 LSNA Virtual 3D Model of the Lumbar Spine Alberto Prats-Galino 1, Miguel Angel Reina 2, Marija Mavar Haramija 1, Anna Puigdellivol-Sánchez 1, Joan San Molina 3 and José Antonio De Andrés 4. 1 Laboratory
LSNA Virtual 3D Model of the Lumbar Spine Alberto Prats-Galino 1, Miguel Angel Reina 2, Marija Mavar Haramija 1, Anna Puigdellivol-Sánchez 1, Joan San Molina 3 and José Antonio De Andrés 4. 1 Laboratory
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY. Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572 CODMAN
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572 CODMAN
Orthopaedics: Low Back Pain
 Technical Guidance for Surgical Specialty Quality Dashboard: Orthopaedics: Low Back Pain V1.1 Contents 1. Introduction... 3 Spell Identification... 3 2. Dashboard Guidance... 4 2.1. Spine Charts... 4 2.2.
Technical Guidance for Surgical Specialty Quality Dashboard: Orthopaedics: Low Back Pain V1.1 Contents 1. Introduction... 3 Spell Identification... 3 2. Dashboard Guidance... 4 2.1. Spine Charts... 4 2.2.
Cervical Spine Imaging
 March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information
 Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
An Algorithmic Approach for Clinical Management of Chronic Spinal Pain
 Pain Physician 2009; 12:E225-E264 ISSN 2150-1149 Evidence-Based Medicine An Algorithmic Approach for Clinical Management of Chronic Spinal Pain Laxmaiah Manchikanti, MD 1, Standiford Helm, MD 2, Vijay
Pain Physician 2009; 12:E225-E264 ISSN 2150-1149 Evidence-Based Medicine An Algorithmic Approach for Clinical Management of Chronic Spinal Pain Laxmaiah Manchikanti, MD 1, Standiford Helm, MD 2, Vijay
Preparation iagnostic Medical Sonographer Overview"
 Diagnostic Medical Sonographer Overview The Field - Preparation - Specialty Areas - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Diagnostic imaging
Diagnostic Medical Sonographer Overview The Field - Preparation - Specialty Areas - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Diagnostic imaging
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO?
 Cox Case Report #59 by Dr. James Cox published 4/08 1 TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO? A 26-year-old, white,
Cox Case Report #59 by Dr. James Cox published 4/08 1 TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO? A 26-year-old, white,
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT. Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: codmanpump@aol.com Fax: 303-703-1572
Workers Compensation Medical Costs in NH Significantly Higher
 EMBARGOED: FOR RELEASE THURSDAY, MAY 22, 10 AM NOT FOR RELEASE UNTIL: May 22, 2014 Contact: Danielle Barrick, director of communications, (603) 271-7973, ext. 336, danielle.barrick@ins.nh.gov; Deb Stone,
EMBARGOED: FOR RELEASE THURSDAY, MAY 22, 10 AM NOT FOR RELEASE UNTIL: May 22, 2014 Contact: Danielle Barrick, director of communications, (603) 271-7973, ext. 336, danielle.barrick@ins.nh.gov; Deb Stone,
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure
 Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Original Contribution
 Original Contribution 266 Pain Physician, Volume 5, Number 3, pp 266-270 2002, American Society of Interventional Pain Physicians ISSN 1533-3159 Effectiveness of Transforaminal Epidural Steroid Injections
Original Contribution 266 Pain Physician, Volume 5, Number 3, pp 266-270 2002, American Society of Interventional Pain Physicians ISSN 1533-3159 Effectiveness of Transforaminal Epidural Steroid Injections
Your anaesthetist may suggest that you have a spinal or epidural injection. These
 Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Electrodiagnostic Testing
 Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management.
 Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management. MAGNITUDE OF THE PROBLEM It is one of the commonest experiences of humankind. It
Non Surgical Management of Back pain. Dr Pankaj Wadhwa MBBS,MD(Anaesth),DNB,Dip.Acu, FIPP, Fellowship in Pain Management. MAGNITUDE OF THE PROBLEM It is one of the commonest experiences of humankind. It
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Research article Basic and applied anatomy Study on incidence of sacralisation of fifth lumbar vertebra in South Indian population
 IJAE Vol. 121, n. 1: 60-65, 2016 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article Basic and applied anatomy Study on incidence of sacralisation of fifth lumbar vertebra in South Indian population
IJAE Vol. 121, n. 1: 60-65, 2016 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article Basic and applied anatomy Study on incidence of sacralisation of fifth lumbar vertebra in South Indian population
RADIOLOGY SERVICES. By Dr Lim Eng Kok 1
 INTRODUCTION RADIOLOGY SERVICES By Dr Lim Eng Kok 1 Radiology is the branch of medicine that deals with the use of ionising (e.g. x- rays and radio-isotopes) and non-ionising radiation (e.g. ultrasound
INTRODUCTION RADIOLOGY SERVICES By Dr Lim Eng Kok 1 Radiology is the branch of medicine that deals with the use of ionising (e.g. x- rays and radio-isotopes) and non-ionising radiation (e.g. ultrasound
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach
 Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy
 Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
MD 2016. Back Muscles & Movements Applied Anatomy. A/Prof Chris Briggs Anatomy & Neuroscience
 MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Lectures of Human Anatomy
 Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Vivian Gonzalez Gillian Lieberman, MD. January 2002. Lumbar Spine Trauma. Vivian Gonzalez, Harvard Medical School Year III Gillian Lieberman, MD
 January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
On Cervical Zygapophysial Joint Pain After Whiplash. Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199
 On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
Coding and Payment Guide for Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management
 Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Efficacy of Epidural Steroid Injections for Lumbar Radiculopathy. Dr Chris Milne Sports Physician Hamilton
 Efficacy of Epidural Steroid Injections for Lumbar Radiculopathy Dr Chris Milne Sports Physician Hamilton Clinical Background 1-Low back pain is common 2-Early resolution is the usual outcome 3-A small
Efficacy of Epidural Steroid Injections for Lumbar Radiculopathy Dr Chris Milne Sports Physician Hamilton Clinical Background 1-Low back pain is common 2-Early resolution is the usual outcome 3-A small
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis
 Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Computer-Aided Diagnosis of Lumbar Stenosis Conditions
 Computer-Aided Diagnosis of Lumbar Stenosis Conditions Soontharee Koompairojn 1 Kathleen Hua 2 Kien A. Hua 1 Jintavaree Srisomboon 3 1 University of Central Florida, Orlando FL 32816, U.S.A. [soonthar,
Computer-Aided Diagnosis of Lumbar Stenosis Conditions Soontharee Koompairojn 1 Kathleen Hua 2 Kien A. Hua 1 Jintavaree Srisomboon 3 1 University of Central Florida, Orlando FL 32816, U.S.A. [soonthar,
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs
 Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs Doug Dean ENGN 2500: Medical Image Analysis Final Project Outline Introduction to the problem Based on paper:
Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs Doug Dean ENGN 2500: Medical Image Analysis Final Project Outline Introduction to the problem Based on paper:
An Anatomical Comparison of the Human and Bovine Thoracolumbar Spine
 Journal of Orthopaedic Research 4:298-303, Raven Press, New York 0 1986 Orthopaedic Research Society An Anatomical Comparison of the Human and Bovine Thoracolumbar Spine Paul C. Cotterill, J. P. Kostuik,
Journal of Orthopaedic Research 4:298-303, Raven Press, New York 0 1986 Orthopaedic Research Society An Anatomical Comparison of the Human and Bovine Thoracolumbar Spine Paul C. Cotterill, J. P. Kostuik,
Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic
 Cox Technic Email Case #77 October 2009 by Dr. Greenwood 1 Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic A case study presented to the Part III Hospital Based Training Course for Cox
Cox Technic Email Case #77 October 2009 by Dr. Greenwood 1 Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic A case study presented to the Part III Hospital Based Training Course for Cox
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
