Femorofemoral crossover bypass graft
|
|
|
- Jeffrey Marshall
- 9 years ago
- Views:
Transcription
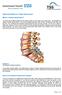
1 Femorofemoral crossover bypass graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as femorofemoral crossover bypass graft; it explains what is involved before, during, and after the operation. It also explains what possible risks there are and how you can help to make your operation a success. We would particularly ask you to read the sections headed Is the treatment safe?, What do I do if I feel unwell at home? and What should I do before I come into hospital?. This leaflet is not meant to replace the information discussed between you and your Doctor but can act as the starting point for this or as a useful reminder of the key points. What is a femorofemoral crossover bypass graft? This is the insertion of a synthetic artificial artery between the femoral arteries in each groin. The graft is placed via incisions in both groins and is passed from side to side buried beneath the skin in the lower abdomen (tummy). Aorta Diseased artery Femoral artery Cross over graft How will this operation help? The aim is to improve the blood supply to your leg and to relieve your symptoms. By doing this it is hoped to prevent and save a foot from progressive ulcers, gangrene, or amputation and to increase the distance that you walk before experiencing a feeling of cramp to the muscles of your legs. Are there alternatives? The blood supply to your leg has become compromised by a blockage of the main artery and needs to be corrected to maintain the health of your leg and foot and to help you walk more comfortably. You could carry on as you are or have the leg amputated. There are sometimes alternative bypass operations (such as, aortobifemoral, iliofemoral, or axillofemoral) that you could have but these will depend on the extent and position of the blockage in your leg artery and your Surgeon feels that this is the best option. 1
2 Is the treatment safe? Although this is a major operation, better than 19 out of 20 people will survive this type of surgery. The risk to you as an individual will depend on: your age your general fitness; and whether you have any medical problems (especially heart disease). As with any major operation such as this, there is a risk of you having complications such as: deep vein thrombosis (blood clots in the leg veins) heart attack (one in 20) stroke kidney failure (one in 40) chest problems with clots (embolism) or infection. None of these is common, but overall it does mean that some patients may have a fatal complication from their operation. For most this risk is about 2%, in other words 98 in every 100 patients will survive the operation. The Doctors and Nurses will try to prevent these complications and to deal with them rapidly if they do occur. The other important surgical complications that you should have discussed with your Consultant are: Infection of the artificial artery - this is rare (about one in 100) but is a serious complication, and its treatment usually involves removal of the graft. To try to prevent this happening you are given antibiotics during your operation. Bleeding, infection, or swelling of the groin wounds. Blockage of the bypass graft where the blood clots within the bypass graft causing it to block. If this occurs it may be necessary and possible to perform another operation to clear the bypass though not always. Limb loss (amputation) - when the bypass blocks and the circulation cannot be restored, and if the circulation to the foot is so badly affected, then an amputation may be required to save or improve the quality of life. The circulation to your good leg may be reduced and cause similar symptoms to those in your bad leg, this is called a steal syndrome. Discomfort from the wound area is normal for several weeks after the operation. You may have patches of numbness around the wound or lower down the leg which is due to the unavoidable cutting of nerves in the skin. It is quite common for the feet to swell due to the improved blood supply, raising the legs when sitting or resting will help this. Before you come into hospital How do I decide whether to have the operation? Everyone varies in the risks they are willing to take. The Doctors will explain about what they think the risks of the operation are for you and what the risks are of not having the operation. Only you can decide whether you go ahead and have the operation. Nothing will happen to you until you understand and agree what has been planned for you. You have the right to refuse if you do not want the operation. 2
3 What should I do before I come into hospital? You will be invited to an Anaesthetic Pre-assessment Clinic before your operation, where you will be seen by one of the Vascular Nurse Specialists to confirm your fitness for surgery and to give you further information about the procedure and your stay in hospital. Your Consultant may also arrange for you to be assessed by the Anaesthetist at this clinic if they have concerns about your health following the special tests that you have undergone as part of your work-up for this operation or because of any problems that you may have had with previous anaesthetics. It is important to prepare well for the operation. There is a lot that you can do to improve your fitness. Smoking - if you smoke, you should try to give up. The longer you can give up for the better. Your arteries and your bypass graft are more likely to stop working if you continue to smoke: if you can stop smoking for a day or two your blood cells can carry more oxygen around your body; if you can stop smoking for about six weeks before you come into hospital you are less likely to get a chest infection after the operation. Gum: please note any patients about to undergo an operative procedure must not chew gum/ nicotine gum prior to surgery. Alcohol: if you are used to drinking a lot of alcohol, it is helpful to reduce the amount that you drink. Alcohol can reduce the function of your heart and it may also cause dehydration and confusion or delerium. Losing weight: if you are overweight, some of the risks of the anaesthetic and the operation are increased. Losing weight will reduce these risks. You should consider a change to your diet by reducing the amount of fat that you eat. If you require any advice about this an appointment can be made to see the Hospital Dietician. Exercise: regular exercise will increase your strength and fitness. There is no need to push yourself a regular walk at your own pace will boost your stamina and get you fitter for the operation. Other medical problems: if you have a long-standing medical problem, such as diabetes, asthma, chronic bronchitis, high blood pressure, or epilepsy, it is helpful to have a check up from your own GP. In particular, so that your blood pressure and these other conditions are as wellcontrolled as possible. Coming into hospital What will happen when I arrive at hospital? On admission you will be greeted by a member of the Kent Ward team and introduced to your named Nurse. They will discuss with you the care that you will receive while you are in hospital. You will also be seen by your Consultant or one of their team to explain anything you may be unsure about before you sign a consent form for your operation. Final preparations will be completed on your admission to the ward. These may include having blood tests, a chest x-ray, and/or tracing of your heart (ECG). Please do not shave any hair from your stomach or legs as this will be done for you in Theatre. Your agreement to having the operation will need yours and the Surgeon s signature on a special legal Consent Form. 3
4 You will meet an Anaesthetist, who is a Doctor with specialist training in Anaesthesia, the treatment of pain, and the care of patients in Intensive Care. They visit you before your operation to discuss the anaesthetic and methods of pain relief, taking into consideration any other medical conditions that you have and also any previous anaesthetics you may have had. They may ask about your health, look at all your test results, listen to your heart and breathing, and look at your neck, jaw, mouth, and teeth. They will be happy to answer your questions and discuss any anaesthetic worries that you have. You will be given clear instructions about when to stop food and drink. It is important to follow this advice. If there is food or liquid in your stomach during the anaesthetic, it can get into and damage your lungs. Usually, you should have no food for six hours but non-milky drinks are allowed until two hours before your operation. You should continue to take all your regular medications even on the morning of the operation, except, if you are taking clopidrogel in combination with aspirin, you would have been advised to stop this if and when you attended the Pre-assessment Clinic. You must also temporarily stop anticoagulants, for example Warfarin. A Physiotherapist may see you before your operation. They will advise you of exercises to perform after the operation that will aid your circulation whilst lying in bed and of deep breathing exercises that will help keep your lungs clear, together with the movements of your legs and feet to prevent blood clots in your leg veins (DVT). It is very important that you can breathe deeply and cough effectively, to help you avoid a chest infection or pneumonia. The operation will take place in the Main Theatre Suite at Kent and Canterbury Hospital. Will I have an anaesthetic? The operation is performed under a general or spinal anaesthetic. You will usually have an epidural anaesthetic as well to provide pain relief after your surgery. This is where a small tube is inserted into your back through which painkillers can be given to numb the lower half of your body during the operation and for several days after. The Anaesthetist will explain these further. What happens in the Anaesthetic Room? There is a period of preparation before your anaesthetic begins. In this period the Anaesthetist s assistant will attach monitoring machines which measure your heart rate (sticky pads on your chest), blood pressure (an inflatable cuff on your arm), and oxygen levels (small peg on your finger or ear lobe). The Anaesthetist will numb your skin with local anaesthetic before using larger needles to insert thin plastic tubes (cannulas) into a vein on the back of your hand or forearm (usually known as a drip and used to keep you well-hydrated and to give anaesthetic drugs) and into the artery at your wrist (arterial line used to monitor blood pressure). These are attached to a bag of fluid The spinal or epidural is usually inserted after all these have been done. For a general anaesthetic you will be asked to breathe oxygen through a mask whilst the Anaesthetist injects drugs into your drip. You will not be aware of anything else until after the operation is finished. Whilst you are anaesthetised, you will have a breathing tube placed in your mouth. A catheter tube will also be passed into your bladder which is used to measure the amount of urine that your kidneys produce and to relieve you of the need to pass urine. As part of your care whilst in hospital, every effort is made to ensure you are seen by the same Doctors who will be part of the Vascular and Interventional Radiology team. 4
5 After the operation How will I feel afterwards? Following your operation you may be transferred to the High Dependency Unit (HDU) for close monitoring overnight or you will be returned to the ward if you are well enough and free of pain. You will still have a drip (tube) into one of your veins which is used to give you fluids until you are able to eat and drink normally. You will also still have the catheter tube in your bladder with a bag on the end of it to collect your urine. This is removed once the epidural is removed and you are more mobile and able to move around more easily. You may need to use a bed pan or commode at first. You will experience varying degrees of pain but you will receive regular painkillers to help make you feel more comfortable. Please alert the staff if and when you have pain. The Anaesthetist will discuss alternative ways in which pain relief can be administered. One way is in the form of patient controlled analgesia. This is by a machine called a PCA that you are able to control yourself by pressing a button to aid pain relief. You may also experience some nausea or sickness. Once again, please alert the staff and they can give you treatment to help this. The position of the groin wounds will make moving uncomfortable at first. You will be encouraged to get up for a short while on the first day after your operation, the Nurses and Physiotherapists will assist you with this. If your feet are healthy and strength good, you will progress to walking two to three days after your operation. This will encourage blood flow and aid healing of your wounds, and reduce some complications in your recovery. As a safety measure, you will receive daily injections of a blood-thinning substance (Clexane) to prevent blood clots from forming. When sitting out in a chair you will be encouraged to elevate your legs. When lying in bed or sitting out, it is advisable to continue doing the leg and deep breathing exercises shown to you by the Physiotherapist. The wounds are usually closed with dissolvable buried sutures that do not need to be removed. You usually have a simple adhesive dressing on the wounds. You may also have a plastic tube to drain fluid from the wounds; these are usually removed after a day or two. It is quite common to feel a bit low after having an operation; this can be caused by a number of factors such as pain, feeling tired, or not sleeping well. The Nurses can help you with this; please do not hesitate to let them know how you are feeling. It may be as simple as changing your painkillers or having a light sleeping tablet that may help you feel better. How long will I be in hospital? You can expect to be in hospital for around three days or more after your operation. The Surgeon and the Nursing team will advise when you are ready to go home. Please do not leave until you have been given instructions, your medication, and discharge letter for your GP. What should I do when I go home? A period of convalescence of two to three weeks is suggested after leaving hospital. This time is spent resting more that usual, such as having a sleep in the afternoon. After this period you can gradually return to normal activities taking care not to put too much strain on your operation wounds to begin with. It is advisable to gradually increase the amounts of exercise that you undertake, lengthening the distance that you walk. Mobility is dictated in part by the severity of your leg problem and your response to the operation and therefore it will vary from patient to patient. Driving: you will be safe to drive when you are able to perform an emergency stop comfortably, this will normally be four weeks after your surgery. If in doubt, please check with your Doctor. Driving too soon after an operation may affect your insurance so we advise you to check your policy details or contact your insurance company. 5
6 It is important you keep your wound areas clean. This can be done with a daily bath or shower, gently patting the areas dry with a clean towel and replacing the dressings. If a wound becomes red and there is a discharge, you should seek advice from your GP as you may need antibiotics. You will be sent home on a small dose of aspirin if you were not already taking it. This is to make the blood less sticky. If you are unable to tolerate aspirin, an alternative drug will be prescribed. In some cases you will be asked to take warfarin, a blood-thinning drug instead. Also, you should be taking a statin, a drug to lower cholesterol, together with any other of your normal medications. What do I do if I feel unwell at home? In general call your GP or the Out-of-Hours Doctors service. If you develop sudden pain or numbness in the leg that does not get better within a couple of hours, then contact the Vascular team immediately. Likewise, if you experience any pain or swelling in your calves, any shortness of breath or pains in your chest, you must seek medical attention. Will I have to come back to hospital? The Vascular team usually review you two to six weeks after discharge in Outpatients to observe your progress, this is not always necessary if you are completely well. You can contact the Vascular team if you have a problem. When can I return to work? You should be able to return to light work or jobs at home after two weeks and heavier jobs after a month. If in doubt, please ask your Surgeon or GP. Finally. Most or all of your questions should have been answered by this leaflet, but remember that this is only a starting point for discussion about your treatment with the Doctors looking after you. Make sure you are satisfied that you have received enough information about the operation before you sign the Consent Form agreeing to the procedure. Source of information The information within this leaflet is based on current practice undertaken by your Consultant and national guidelines. If you have any comments regarding this leaflet we would appreciate your feedback. Where can I get more information? Further information can be obtained from your Consultant s secretary - Mr Insall, Kent and Canterbury Hospital, Canterbury Mr Rix and Mr Senaratne, Kent and Canterbury Hospital, Canterbury Mr Wilson, Kent and Canterbury Hospital, Canterbury or, the Vascular Nurse Specialists - Kent and Canterbury Hospital, Canterbury William Harvey Hospital, Ashford extension You may like to look at the following websites for further information. However, as we are not responsible for these websites we cannot endorse them. Vascular Society of Great Britain and Ireland The Circulation Foundation 6
7 Any complaints, comments, concerns, or compliments If you have other concerns please talk to your doctor or nurse. Alternatively please contact our Patient Advice and Liaison Service (PALS) on or , or Further patient information leaflets In addition to this leaflet, East Kent Hospitals has a wide range of other patient information leaflets covering conditions, services, and clinical procedures carried out by the Trust. For a full listing please go to or contact a member of staff. After reading this information, do you have any further questions or comments? If so, please list below and bring to the attention of your nurse or consultant. Would you like the information in this leaflet in another format or language? We value equality of access to our information and services and are therefore happy to provide the information in this leaflet in Braille, large print, or audio - upon request. If you would like a copy of this document in your language, please contact the ward or department responsible for your care. Pacjenci chcący uzyskać kopię tego dokumentu w swoim języku ojczystym powinni skontaktować się z oddziałem lub działem odpowiedzialnym za opiekę nad nimi. Ak by ste chceli kópiu tohto dokumentu vo vašom jazyku, prosím skontaktujte nemocničné pracovisko, alebo oddelenie zodpovedné za starostlivosť o vás. Pokud byste měli zájem o kopii tohoto dokumentu ve svém jazyce, kontaktujte prosím oddělení odpovídající za Vaši péči. Чтобы получить копию этого документа на вашем родном языке, пожалуйста обратитесь в отделение, ответственное за ваше лечение. We have allocated parking spaces for disabled people, automatic doors, induction loops, and can provide interpretation. For assistance, please contact a member of staff. This leaflet has been produced with and for patients Information produced by the Vascular Surgery Service Date reviewed: June 2015 Next review date: June 2017 Web 026 7
Aortobifemoral Bypass Graft
 Aortobifemoral Bypass Graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as Aortobifemoral Bypass; it explains what is involved before, during,
Aortobifemoral Bypass Graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as Aortobifemoral Bypass; it explains what is involved before, during,
Patients undergoing a CT examination
 Patients undergoing a CT examination Information for patients attending the departments within the Directorate of Radiological Sciences What is a CT scan? A CT (Computed Tomography) scan is an x-ray test
Patients undergoing a CT examination Information for patients attending the departments within the Directorate of Radiological Sciences What is a CT scan? A CT (Computed Tomography) scan is an x-ray test
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Vision imbalance following cataract surgery (anisometropia)
 Vision imbalance following cataract surgery (anisometropia) Information for patients from Ophthalmology This leaflet is not meant to replace the information discussed between you and your doctor, but can
Vision imbalance following cataract surgery (anisometropia) Information for patients from Ophthalmology This leaflet is not meant to replace the information discussed between you and your doctor, but can
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Overactive bladder. Information for patients from Urogynaecology
 Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
How to pay for a funeral
 How to pay for a funeral Information for patients from the Patient Experience Team This leaflet provides advice to people who have just lost a family member or a friend, and who have concerns about how
How to pay for a funeral Information for patients from the Patient Experience Team This leaflet provides advice to people who have just lost a family member or a friend, and who have concerns about how
Cataracts and their treatment
 Cataracts and their treatment Information for patients from Head and Neck Now that you have been told that you may have a cataract, you will be wondering what happens next. This leaflet explains what cataracts
Cataracts and their treatment Information for patients from Head and Neck Now that you have been told that you may have a cataract, you will be wondering what happens next. This leaflet explains what cataracts
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
YOU AND YOUR ANAESTHETIC
 YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
YOU AND YOUR ANAESTHETIC Information Leaflet Your Health. Our Priority. Page 2 of 8 This leaflet aims to answer some of the questions you may have about your anaesthetic and contains fasting instructions.
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Elective Laparoscopic Cholecystectomy
 General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy)
 Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients
 Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Having a Trans-Arterial Embolisation
 Having a Trans-Arterial Embolisation Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a Trans-Arterial Embolisation Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Patient Information. Patient Diary for Gynaecological Laparoscopic Surgery on the Enhanced Recovery Programme. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Vaginal hysterectomy and vaginal repair
 Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Inguinal (Groin) Hernia Repair
 Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What should I expect before the procedure?
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
Hernia- Open Inguinal Hernia Repair PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
LASER TREATMENT FOR VARICOSE VEINS
 LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
Mesenteric Angiography
 Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Tunnelled haemodialysis catheter
 Liver, Renal & Surgery Tunnelled haemodialysis catheter Information for patients and carers This leaflet explains what a tunnelled haemodialysis catheter is and how it is put in. It also covers the risks
Liver, Renal & Surgery Tunnelled haemodialysis catheter Information for patients and carers This leaflet explains what a tunnelled haemodialysis catheter is and how it is put in. It also covers the risks
Headache after an epidural or spinal injection What you need to know. Patient information Leaflet
 Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT)
 ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet
Name of procedure: Laparoscopic (key-hole) ovarian surgery. Left/ Right unilateral salpingo-oophorectomy* (removal of one fallopian tube and ovary)
 For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
For staff use only: Patient Details: Surname: First names: Date of birth: Hospital no: Female: (Use hospital identification label) Gynaecology Patient agreement to treatment Name of procedure: Laparoscopic
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
Spigelian Hernia Repair
 Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Epigastric Hernia Repair
 Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Liver Resection. Patient Information Booklet. Delivering the best in care. UHB is a no smoking Trust
 Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Liver Resection Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
Local anaesthesia for your eye operation A short guide for patients and families. This is for anyone expecting to have an eye operation with a local anaesthetic. It does not give detailed information about
SUPRAPUBIC CATHETER INSERTION INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
VATS Lobectomy. Information for patients
 VATS Lobectomy Information for patients VATS stands for video-assisted thoracoscopic surgery. This is the equipment used for minimal access surgery or keyhole surgery. This leaflet will explain about the
VATS Lobectomy Information for patients VATS stands for video-assisted thoracoscopic surgery. This is the equipment used for minimal access surgery or keyhole surgery. This leaflet will explain about the
Stapedectomy / Stapedotomy / Surgery for Otosclerosis
 Patient information Stapedectomy / Stapedotomy / Surgery for Otosclerosis Ear, Nose and Throat Directorate PIF 230 V6 Your Consultant / Doctor has advised you to have a Stapedectomy / Stapedotomy / Surgery
Patient information Stapedectomy / Stapedotomy / Surgery for Otosclerosis Ear, Nose and Throat Directorate PIF 230 V6 Your Consultant / Doctor has advised you to have a Stapedectomy / Stapedotomy / Surgery
Having a circumcision information for men
 Having a circumcision information for men This leaflet aims to answer your questions about having a circumcision. It explains the benefits, risks and alternatives, as well as what you can expect when you
Having a circumcision information for men This leaflet aims to answer your questions about having a circumcision. It explains the benefits, risks and alternatives, as well as what you can expect when you
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
An operation for prolapse Colpocleisis
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Having a kidney biopsy
 Having a kidney biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Having a kidney biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Having a RIG tube inserted
 Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Venefit treatment for varicose veins
 Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION. Under the Care of Mr M Paterson - 11 -
 ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
A Guide. To Revision Total Knee Replacement. Patient Information Leaflet
 A Guide This leaflet is available in large print, Braille and on tape. Please contact Geoff Pennock on 0151 604 7289. To Revision Total Knee Replacement Wirral University Teaching Hospital NHS Foundation
A Guide This leaflet is available in large print, Braille and on tape. Please contact Geoff Pennock on 0151 604 7289. To Revision Total Knee Replacement Wirral University Teaching Hospital NHS Foundation
Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast. Information for patients Pharmacy
 Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast Information for patients Pharmacy Your doctor has prescribed a tablet called rivaroxaban. This leaflet tells you about
Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast Information for patients Pharmacy Your doctor has prescribed a tablet called rivaroxaban. This leaflet tells you about
Deep Vein Thrombosis (DVT) in pregnancy
 Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
V03 Varicose Veins Surgery
 V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery
 Ambulatory Care & Local Networks Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone
Ambulatory Care & Local Networks Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Transcatheter Aortic Valve Implantation (TAVI) A patient s guide
 Transcatheter Aortic Valve Implantation (TAVI) A patient s guide Valvular heart disease The heart is a muscle which pumps blood to your lungs and around the body. There are four valves within the heart.
Transcatheter Aortic Valve Implantation (TAVI) A patient s guide Valvular heart disease The heart is a muscle which pumps blood to your lungs and around the body. There are four valves within the heart.
University College Hospital. Laparoscopic gastric bypass. Centre for Weight Loss, Metabolic and Endocrine Surgery
 University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
Primary and revision lumbar discectomy. (nerve root decompression)
 Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
