Guillain-Barré Syndrome, CIDP and Variants Guidelines for Physical and Occupational Therapy
|
|
|
- Shanon Parker
- 8 years ago
- Views:
Transcription
1 Guillain-Barré Syndrome, CIDP and Variants Guidelines for Physical and Occupational Therapy A publication of the GBS/CIDP Foundation International
2 Guidelines for Physical and Occupational Therapy Provided through an educational grant from CSL Behring
3 Dear Therapist/Therapist Assistant, Thank you for taking a few moments to learn more about what your patient with Guillain-Barré syndrome (GBS), chronic inflammatory demyelinating neuropathy (CIDP) or a variant has been experiencing and how you better can help them on their road to recovery. Perhaps they already are well along on their journey, or they just may be getting started, but their experience to this point undoubtedly has been a frightening and stressful one. Some of a patient s greatest fears regarding therapy are that their therapist will not know what to do with them and/or will not understand their limitations, or that therapy will be so painful and/ or hard that they will not be able to move the next day. We know that therapists and therapist assistants have a solid base of academic and clinical knowledge from which to work, but many have not encountered GBS or CIDP directly during their careers. Accordingly, the GBS/CIDP Foundation International (the Foundation ) has published this booklet and encourages patients to share it with their physical and occupational therapists. Regardless of your familiarity with GBS or CIDP, your taking the time to review this information will offer your patient peace of mind in knowing that you are interested in their care and sensitive to issues that are unique to their condition. What are GBS, CIDP and related disorders? GBS and CIDP are acquired immune-mediated inflammatory disorders of the peripheral nervous system. Their etiology is not completely understood, and neither disorder is contagious. Most GBS cases appear to be precipitated by an infectious respiratory or gastrointestinal illness with diarrhea. In the U.S. and Europe, 60 to 80 percent of GBS cases occur within four weeks of a preceding infection. For an as yet unknown reason, the body s response to the infection goes awry and the immune system attacks the myelin and sometimes the axons of the peripheral nerves. As a consequence, neurological signals are slowed, altered or blocked
4 altogether, resulting in paresthesias (e.g. numbness, tingling, crawling skin ), loss of sensation and deep tendon reflexes, progressive muscle weakness, often general fatigue, sometimes pain and a number of other possible secondary complications. Motor and sensory involvement is symmetrical in proximal and distal muscles with symptoms progressing in an ascending fashion, the lower limbs usually being affected first. In severe cases, autonomic nervous system dysfunction also can occur, the presence of which is suggested by orthostatic dizziness, bowel and bladder function complications and/or cardiac symptoms. Unlike multiple sclerosis and amyotrophic lateral sclerosis (a.k.a. Lou Gehrig s disease), GBS and CIDP generally do not cause damage to the central nervous system, although GBS patients may experience difficulty with swallowing (dysphagia), facial drooping and other deficits of the lower cranial nerves. Neither condition affects a patient s cognition. Guillain-Barré Syndrome Guillain-Barré syndrome, also called acute inflammatory demyelinating polyneuropathy (AIDP), affects one to two new persons per 100,000 population each year. It can strike anyone without warning regardless of gender, age or ethnic background. About 50 percent of patients initially develop abnormal sensations such as tingling of the feet or fingers; twenty-five percent initially develop muscle weakness (e.g. difficulty climbing stairs, getting up from a chair and/or cramping) and 25 percent begin with a combination of abnormal sensations and weakness. Pain is also a common symptom, sometimes experienced as deep aching or cramping in the buttocks, thighs or between the shoulders. Disability caused by GBS generally progresses over the course of a few days to four weeks, with weakness starting distally and ascending in a matter of hours to days. At the peak of the condition s progress, many patients experience flaccid paralysis of nearly all skeletal muscles, with talking, swallowing and breathing frequently being affected. Seventy percent of patients lose some strength in respiratory muscles that can lead to shortness 2
5 of breath; in about one third of patients, intubation and a ventilator temporarily become required. Consequently, most newly diagnosed patients are placed in an intensive care unit for monitoring. Plasma exchange (PE) or a high dose of intravenous immune globulins (IVIG) often hasten recovery. Corticosteroids are not helpful for GBS, but frequently are used to treat CIDP. Fortunately, GBS typically is self-limiting with improvement usually beginning spontaneously after weakness maximizes. The death rate is approximately three percent, and the recurrence rate less than five percent. Most patients eventually reach a full or nearly full recovery. Many patients will walk without aid after three months and experience only minor residual symptoms by the end of the first year following onset. Nevertheless, recovery can be extremely slow (stretching over the course of six months to two years or longer) and five to twenty percent of patients are left with significant residual symptoms that lead to long-term disability and prevent a successful return to their prior lifestyle or occupation. Acute Motor Axonal Neuropathy This variant of GBS initially was recognized by westerners as epidemics of paralysis in children in rural northern China and first was named the Chinese paralytic syndrome. It often follows diarrhea from Campylobacter jejuni, does occur occasionally in the western world, but unlike classic GBS does not affect sensory nerves, and more often progresses sufficiently to require ventilator support. Medical management and occupational and physical therapy methods (see below) are the same as for GBS. Miller Fisher Syndrome Miller Fisher syndrome (MFS), named after C. Miller Fisher, MD, who described the disorder, is an uncommon variant of GBS. It consists of the triad of areflexia, external ophthalmoplegia, that is, weak eye muscles that cause diplopia, and ataxia. Both the double vision and ataxic gait can contribute to impaired activities of daily
6 living. Clinical features of MFS often accompany GBS. Principles of care for GBS also are applicable to MFS. Chronic Inflammatory Demyelinating Polyneuropathy CIDP is a chronic counterpart to Guillain-Barré syndrome, and also is characterized by symmetrical weakness and sensory changes. New cases of the condition are rare compared to GBS 1.5 to 3.6 new patients per 1,000,000 population each year but because CIDP can persist for years, there are estimated to be as many as eight cases per 100,000 population, or five to nine thousand people in the U.S. at any one time. In contrast to GBS, CIDP develops slowly, often over the course of two months or longer. It can manifest in a variety of patterns; however, the most common is a series of recurrent relapses and remissions of ascending weakness over the course of years. Occasionally, the disorder may run a slowly progressive deteriorating course without improvement. Because of its typically slowly progressive nature, CIDP can present symptoms for months or longer before activities of daily living are impaired and the disorder is diagnosed. Once it is determined that a patient has CIDP, first line treatment choices are corticosteroids, plasmapheresis (plasma exchange) or intravenous immunoglobulin (IVIG). In contrast to GBS, breathing, swallowing and speaking are rarely affected, though it is still important to establish a diagnosis and set a course of treatment as soon as possible. If left untreated, or if treatment is significantly delayed, CIDP can lead to severe nerve damage that may not be entirely recoverable. In fact, reinnervation and long-term disability rates are worse for patients with CIDP than for those with GBS, with the likelihood of progression and recurrence being much higher. Multifocal Motor Neuropathy Multifocal motor neuropathy (MMN) is a rare chronic inflammatory neuropathy characterized by episodes of right and/or left-sided, i.e., asymmetric, distal limb weakness, of the upper more often than the lower limbs. Thus weakness may occur at the wrist, fingers and/or ankles and reflects inflammation
7 of their motor nerves with slowed conduction. The disorder can extend over two to as long as 20 years or more. Nerve conduction tests with selective nerve mapping aids the diagnosis. Because of its slow and variable presentation, MMN may not be recognized readily. Over time, ongoing weakness may lead to muscle atrophy. Fasciculations may occur. Treatment with IVIG is usually beneficial but not PE or corticosteroids. Various immunosuppressive drugs have been tried with variable benefit. The principles of OT and PT care for GBS and CIDP as described below apply to MMN. The Plan of Care should be customized to the individual patient s disability. Orthotics may be indicated to compensate for distal weakness. What is your patient feeling? In order to maximize the impact of your Plan of Care on your patient s prognosis, it is important to understand that their emotions frequently will override reason. When you first meet, the patient likely will have thoughts such as: Will I ever walk again? and When will I get back to normal, or will I? Even when it is time to be discharged from services, they likely will be asking themselves, Will this ever happen to me again? The therapist always should be encouraging and hopeful regarding the patient s recovery without making promises about the degree of recovery or the time frame. It can, however, be said with confidence that the vast majority of patients return to some level of independence. The following is a list of concerns that should be recognized as you work with your patient: Fear and Anxiety Your patient went from being completely independent to experiencing at least some level of dependence on others for no apparent reason and in a short amount of time. If they are still in the acute stage of the condition, they and their caregivers are looking desperately for answers and may be thinking the worst. Once stabilized, your patient probably will continue to experience some anxiety during quiet times alone or 5
8 during treatment. Because GBS and CIDP are rare, often not diagnosed immediately, and the reason for their having developed the condition uncertain, patients and caregivers often wonder whether their condition may worsen. Pain Pain can be significant with GBS, occurs less often with CIDP and contributes significantly to patient anxiety. As sensory nerves begin to heal and grow back, the sensitive regenerating axons impulsively generate abnormal signals that can be exacerbated by weight bearing and exercise. Abnormal sensations, which usually occur distally in the feet and hands, can be difficult for the patient to describe but often interfere with daily activity. Many GBS survivors report increased sensitivity to light touch. It is not uncommon to hear comments such as, I can feel my fingerprints, or The wrinkle in the bed sheet is excruciating. CIDP patients can experience lightning bolts of pain shooting from their lower and upper extremities. Always ask a patient for permission before touching them, and think of how their Plan of Care may affect their sensory system. Depression and Guilt Patients almost certainly wonder if they ever will be able to contribute physically or financially to their family, friends or community again. Medical bills quickly accumulate at the same time that income and benefits diminish. Many patients also demonstrate at least a period of low motivation toward participating in their Plan of Care (especially home programs) as they realize that their recovery is not always directly related to their personal efforts. This understanding is discouraging and can lead to apathy and/or depression. Your greatest tool is the active involvement of your patient in their Plan of Care. Unless they can get past their feelings of fear, anxiety and guilt, it will be very difficult to move forward. The best way to help your patient conquer these challenges is to let them know that they are not alone. 6
9 The GBS/CIDP Foundation has many support groups groups for CIDP patients, children, pregnant patients with GBS, etc. with whom individuals may share experiences and learn from each other. (Patients may contact the Foundation for information.) Evaluation Because the clinical features of GBS or CIDP can differ dramatically from one person to the next, a thorough physical therapy (PT) and occupational therapy (OT) evaluation is imperative to understanding the patient s particular needs. The evaluation will vary somewhat based on the setting in which a patient is being seen, as well as their current status in the pathology process. Patients with GBS frequently begin care in the intensive care unit of a hospital, then progress to a sub-acute setting in a rehabilitation department or outside nursing/rehab facility and eventually to home-based or outpatient therapy. Patients with CIDP, on the other hand, usually begin with outpatient or home-based therapy, and only visit a hospital or rehabilitation department if they experience severe symptoms associated with a relapse or if long-term dependent care is required. It is not uncommon for OT to address primarily the upper body and activities of daily living (e.g. dressing, grooming and feeding) while PT focuses on the lower body and mobility; however, this is certainly not universal and may depend on a given site s policies and the specific state s practice acts. Regardless of who ultimately is responsible for each aspect of an initial evaluation, therapists should be sure to include the following components in their assessment: Patient/Caregiver Interview The most important part of any evaluation is the patient interview. Only the patient can tell you how they are feeling, what they have experienced and where they want to be after therapy. Be conscious and respective of their emotions. The interview is also a good time to assess the caregiver and environmental support that the patient has at home and what their needs may be after discharge.
10 Sensory Assessment Ask the patient if they are sensitive to touch, and if so, where and what types of touch are aggravating or painful, before placing a finger on them. There is no quicker way to lose a patient s confidence and set a negative precedence for the evaluation and future treatment than to begin by causing pain. Of the most commonly used tests to evaluate sensation, touch and pressure and touch localization are the most important to assess during the initial evaluation (use of a filament test kit or other acceptable means as tolerated). Sensation should be re-assessed frequently to track progress of reinnervation, monitor muscle soreness and avoid causing undue pain during therapy. Skin Inspection After asking the patient for consent and explaining what you will be doing, check their skin for lesions or pressure spots. The skin over boney prominences (e.g. heels, sacrum and hips) is particularly susceptible to break down. If a patient is independently mobile, sufficiently cognizant, and has already been performing skin inspections, their report alone may be sufficient. Joint Range of Motion Pay particular attention to the ankles, knees and hips, especially if the patient has spent a lot of time sitting or confined to a wheelchair. Foot and wrist drop are not uncommon and may require bracing or splinting to prevent contractures. If joint contracture is suspected, measure passive range of motion with a goniometer to guide stretching exercises. Muscle Testing Manual Muscle Testing (MMT) grades of zero to five commonly are used to assess muscle strength (as tolerated). If a patient is unable to move a defined body part independently against gravity (grade 3/5), gravity reduced or eliminated positions may be used. If a patient exhibits at least a grade 3/5, the therapist can apply manual resistance to determine higher grades. Consider assessing grip and pinch strength via a dynamometer or pinch gauge, respectively, or through functional testing. 8
11 Functional Testing Depending on the findings from the previous measures, mat mobility, transfers, self-care tasks (e.g. grooming, feeding and dressing) and other functional tasks related to the patient s work and/or leisure activities may be assessed during the initial evaluation. Mobility If a patient is functionally mobile, a brief gait and/or wheelchair assessment/observation may be performed; however, take care to assure that the patient is not already exhausted from the previous activities. If this is the case, the mobility assessment may be postponed until the beginning of the next session. Other In addition to the preceding assessments, and in accordance with the client s current status, the following areas also may be evaluated: o o o o Respiration Test with a hand-held-monitor or spirometer. Vital capacity and inspiratory force or effort are measures of diaphragm strength frequently used to gauge breathing status of the GBS patient. Deep-Vein-Thrombosis (DVT) A firm, tender, warm or swollen calf raises suspicion of DVT. Use the patient s history or a venous duplex ultrasound study to guide the differential diagnosis of DVT. Autonomic Dysfunction If the patient reports dizziness, consider obtaining a blood pressure and heart rate while supine and then standing to identify orthostatic hypotension. Endurance Patients should not be tested to exhaustion since recovery from fatigue can take some time and will delay the rehabilitation process. Note when the patient begins to show early signs of fatigue during the assessment and adjust or discontinue the activity accordingly.
12 Treatment The principal goals of therapy are to: Help the patient to achieve optimal muscle use at a tolerable pain level as nerve supply returns; and Use supportive equipment and other functional adaptations to help patients with residual impairments to resume an activity level that is as close to their previous lifestyle as possible. Therapy does not facilitate nerve repair; however, it does help the recovering patient to learn optimal use of muscles as the nerves heal and innervation improves. Every person with GBS, CIDP or variants responds differently to the physical manifestations of his or her condition as well as pharmaceutical and therapeutic/ rehabilitation interventions. Consequently, it is essential to keep in mind that the body only will do what it is capable physically of doing, regardless of the expectations of the patient or therapy staff. Use a safety first approach by teaching your patient to perform only activities he or she can do safely. Acute Stage During the acute phase of GBS or an exacerbation of CIDP, a patient may not tolerate, or be unable to participate in active movement. Although the condition still may be worsening at this point and care may be more medical than rehabilitative, physical and occupational therapy still play an important role. Initially, your Plan of Care likely will be more consultative in nature, with patient participation being mostly passive during direct treatment. Include the following in this consultation process: Provide patient and caregiver with education and training for the prevention of contractures, DVT and bedsores, as well as proper positioning and the expected course of future rehabilitation. To this end, advise the patient and their caregivers of the following: o Avoid prolonged hip and knee flexion; 0
13 o o Change position at least every two hours in bed and perform regular pressure reliefs when sitting; and Support weak upper extremities with armrests, a wheelchair tray and/or pillows to prevent stretching of shoulder muscles and joint tissues. Educate yourself about the patient s home life, work demands, recreational interests and support system in order to customize your Plan of Care to their needs. Anticipate the need for assistive devices and other adaptive equipment/technology and be prepared to train the patient and caregivers in their use. Use gentle passive range-of-motion to reduce the risk of contractures and DVT. Introduce breathing and coughing exercises to maintain good airway exchange. Communicate clearly with the patient before and during any physical interaction. Recovery As the patient begins to recover sensation and motor control, exercises may be progressed from passive to active-assisted range-of-motion. Initially, active movement should be performed at low repetitions and resistance with frequent rest breaks. A powder board (a smooth surface designed to enable gravity reduced active sliding of a limb), slings and even hydrotherapy, with exercise performed in a pool or large tub (as appropriate), can facilitate the active movement of muscle groups that are not yet able to move independently against gravity. It is essential to help the patient move on their own as soon as possible, without exercising to fatigue, in order to help reduce the progression of disuse atrophy and other complications. The No pain, no gain philosophy should not be applied. Exercising to exhaustion will delay recovery without benefitting the patient.
14 Rather, approach your Plan of Care in this manner: Expand activities gradually. Increase repetitions before resistance in order to avoid injury to muscles, tendons and joints. Use of proprioceptive neuromuscular facilitation (PNF) techniques may be helpful. Teach energy conservation (e.g. pacing and breaking tasks into steps). Train caregivers in proper body mechanics for transfers, positioning, etc. to decrease the risk of injuries to themselves and the patient. Once sufficient active movement has returned, therapy sessions should begin to focus on the patient s ability to perform daily activities. Whenever possible, practiced activities should be real world. Working on cones and peg boards with an OT does not approximate the realistic demands of a patient who needs to bring a spoon to his or her mouth without spilling, nor does performing 10 repetitions of knee extension with a PT represent the patient s ability to get up from the chair in which they are sitting. Several possible functional activities include bed mobility, transfers, gait and/or wheelchair mobility, sitting and standing balance while reaching, dressing, feeding, bathing/toileting, writing/typing, leisure activities and/or reintegration into the work environment. Remember that pain can be a prominent factor during the entire course of recovery. Most problems with sensation resolve over time; however, persistent pain may require treatment via various therapeutic modalities (e.g. TENS, moist heat pack, or sensory desensitization techniques). It is important to note that what may be comforting to one patient may cause discomfort or pain to another. To this end, you should: Customize exercises to strengthen weak muscles and watch for muscle substitution. For example, a patient may demonstrate hip-hiking and a circumduction gait pattern as a consequence of substitution for weak hip flexors. 2
15 Plan multiple rest breaks during therapy if fatigue occurs. Exercising to exhaustion will require recovery time that can delay resumption of therapy. If complaints of increased fatigue last more than 12 to 24 hours, then the patient probably has worked too hard. Establish a home program that fits the patient s current activity level as soon as they and/or their caregivers have demonstrated a thorough understanding of the exercises. Assure that they are aware of the increased risk of falling as a result of their decreased strength. Provide a variety of additional activities that promote gross and fine motor skills and sensory stimulation and/or desensitization outside of therapy. Consider adding aerobic training at a moderate Rate of Perceived Exertion on the Borg scale as soon as the patient s doctor indicates that it is safe to do so. Provide your patient with adaptive/compensatory strategies and equipment as needed. Continue to perform follow-up assessments so that the Plan of Care may be altered to reflect new abilities. In Conclusion Physical and occupational therapy are integral parts of the recovery and management of GBS, CIDP and variants. Their proper utilization can help a patient minimize pain, increase strength and endurance and prevent secondary complications and overuse damage to muscles and joints while improving balance and mobility and restoring functional activity at home, work and play. If you or your patient has additional questions regarding GBS, CIDP or variants, please contact the Foundation directly or visit our website at In many instances, one of our local contacts will be available to visit personally with your patient and provide support to them and their caregivers.
16 Again, thank you for your advocacy! Matthew Hansen, Doctor of Physical Therapy; Santo Garcia, MOTR/L For the: GBS/CIDP Foundation International The Holly Building 104 1/2 Forrest Avenue Narberth, PA Tel: ; Fax: Toll Free: About the authors: Dr. Hansen is a practicing physical therapist, President of SOMA Healthcare Staffing & Consulting and a contributing writer for I.G.Living magazine as well as the GBS/ CIDP Foundation International s newsletter, the Communicator. Santo Garcia, Master s in Occupational Therapy, provides homebased OT. He teaches health care professionals as Adjunct Professor at Hodges University School of Allied Health as well as through his national educational programs. His personal experience with CIDP provides added expertise.
17 For more information, please contact: GBS/CIDP Foundation International The Holly Building 104 1/2 Forrest Avenue Narberth, PA tel tel fax Non-profit 501(c)(3)
Multifocal Motor Neuropathy. Jonathan Katz, MD Richard Lewis, MD
 Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
How To Cover Occupational Therapy
 Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
A Note to Physical, Occupational and Speech Therapists
 D Page 1 of 5 A Note to Physical, Occupational and Speech Therapists Treating Children with Hurler Syndrome Because Hurler syndrome is such a rare disease, we have provided some basic information to assist
D Page 1 of 5 A Note to Physical, Occupational and Speech Therapists Treating Children with Hurler Syndrome Because Hurler syndrome is such a rare disease, we have provided some basic information to assist
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Once the immune system is triggered, cells migrate from the blood into the joints and produce substances that cause inflammation.
 HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
Multiple Sclerosis (MS)
 Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015
 Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
A Definition of Multiple Sclerosis
 English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Understanding. Multiple Sclerosis. Tim, diagnosed in 2004.
 Understanding Multiple Sclerosis Tim, diagnosed in 2004. What Is Multiple Sclerosis? Multiple sclerosis (MS) is a neurologic disorder that affects the central nervous system (CNS). The CNS includes the
Understanding Multiple Sclerosis Tim, diagnosed in 2004. What Is Multiple Sclerosis? Multiple sclerosis (MS) is a neurologic disorder that affects the central nervous system (CNS). The CNS includes the
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Therapeutic Canine Massage
 Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Fact Sheet: Occupational Overuse Syndrome (OOS)
 Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
WORKERS COMPENSATION INTAKE FORM
 WORKERS COMPENSATION INTAKE FORM related injury? No Yes INSURANCE INFORMATION RELEASE By clicking this box,i hereby authorize ABA Physical Therapy Associates to release to my Insurance company/attorney,
WORKERS COMPENSATION INTAKE FORM related injury? No Yes INSURANCE INFORMATION RELEASE By clicking this box,i hereby authorize ABA Physical Therapy Associates to release to my Insurance company/attorney,
Physiotherapy in Rheumatoid Arthritis. Information for patients Gina Wall Senior Physiotherapist
 Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
EMG and the Electrodiagnostic Consultation for the Family Physician
 EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
IMGPT: Exercise After a Heart Attack 610 944 8140 805 N. RICHMOND ST (Located next to Fleetwood HS) Why is exercise important following a heart
 Why is exercise important following a heart attack? Slow progression back into daily activity is important to strengthen the heart muscle and return blood flow to normal. By adding aerobic exercises, your
Why is exercise important following a heart attack? Slow progression back into daily activity is important to strengthen the heart muscle and return blood flow to normal. By adding aerobic exercises, your
Muscular Dystrophy and Multiple Sclerosis. ultimately lead to the crippling of the muscular system, there are many differences between these
 Battles 1 Becky Battles Instructor s Name English 1013 21 November 2006 Muscular Dystrophy and Multiple Sclerosis Although muscular dystrophy and multiple sclerosis are both progressive diseases that ultimately
Battles 1 Becky Battles Instructor s Name English 1013 21 November 2006 Muscular Dystrophy and Multiple Sclerosis Although muscular dystrophy and multiple sclerosis are both progressive diseases that ultimately
Managing the Symptoms of Multiple Sclerosis. Yolanda Harris, MSN, CRNP-AC CPODD Nurse Practitioner
 Managing the Symptoms of Multiple Sclerosis Yolanda Harris, MSN, CRNP-AC CPODD Nurse Practitioner What is Multiple Sclerosis An autoimmune disease that affects the central nervous system (CNS) The immune
Managing the Symptoms of Multiple Sclerosis Yolanda Harris, MSN, CRNP-AC CPODD Nurse Practitioner What is Multiple Sclerosis An autoimmune disease that affects the central nervous system (CNS) The immune
Coding and Documentation in Practice
 Coding and Documentation in Practice Great Exam Documentation By: Kathy Mills Chang Kathy Mills Chang is a Certified Medical Compliance Expert, Reimbursement Consultant, Medicare Specialist, and a Documentation
Coding and Documentation in Practice Great Exam Documentation By: Kathy Mills Chang Kathy Mills Chang is a Certified Medical Compliance Expert, Reimbursement Consultant, Medicare Specialist, and a Documentation
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B
 1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
PLANTAR FASCITIS (Heel Spur Syndrome)
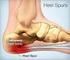 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Fact Sheet. Queensland Spinal Cord Injuries Service. Pain Management Following Spinal Cord Injury for Health Professionals
 Pain Management Following Injury for Health Professionals and Introduction Pain is a common problem following SCI. In the case where a person with SCI does have pain, there are treatments available that
Pain Management Following Injury for Health Professionals and Introduction Pain is a common problem following SCI. In the case where a person with SCI does have pain, there are treatments available that
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
What is Multiple Sclerosis? Gener al information
 What is Multiple Sclerosis? Gener al information Kim, diagnosed in 1986 What is MS? Multiple sclerosis (or MS) is a chronic, often disabling disease that attacks the central nervous system (brain and spinal
What is Multiple Sclerosis? Gener al information Kim, diagnosed in 1986 What is MS? Multiple sclerosis (or MS) is a chronic, often disabling disease that attacks the central nervous system (brain and spinal
Updating the Vaccine Injury Table: Guillain-Barré Syndrome (GBS) and Seasonal Influenza Vaccines
 Updating the Vaccine Injury Table: Guillain-Barré Syndrome (GBS) and Seasonal Influenza Vaccines Ahmed Calvo, M.D., M.P.H. Medical Officer, National Vaccine Injury Compensation Program (VICP) Advisory
Updating the Vaccine Injury Table: Guillain-Barré Syndrome (GBS) and Seasonal Influenza Vaccines Ahmed Calvo, M.D., M.P.H. Medical Officer, National Vaccine Injury Compensation Program (VICP) Advisory
Clinical Medical Policy Outpatient Rehab Therapies (PT & OT) for Members With Special Needs
 Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Spine University s Guide to Transient Osteoporosis
 Spine University s Guide to Transient Osteoporosis 2 Introduction The word osteoporosis scares many people because they ve heard about brittle bone disease. They may know someone who has had it or seen
Spine University s Guide to Transient Osteoporosis 2 Introduction The word osteoporosis scares many people because they ve heard about brittle bone disease. They may know someone who has had it or seen
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES
 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Transmittal 55 Date: MAY 5, 2006. SUBJECT: Changes Conforming to CR3648 for Therapy Services
 CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
PAIN MANAGEMENT During Your Hospital Stay
 PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
1. Describe the causes of pain experienced by people with multiple sclerosis.
 1. Describe the causes of pain experienced by people with multiple sclerosis. Pain experienced by people with MS can be either neuropathic (arising directly from nervous system dysfunction) or may be musculoskeletal,
1. Describe the causes of pain experienced by people with multiple sclerosis. Pain experienced by people with MS can be either neuropathic (arising directly from nervous system dysfunction) or may be musculoskeletal,
Multiple Sclerosis: What You Need To Know. For Professionals
 Multiple Sclerosis: What You Need To Know For Professionals What will I learn today? The Basics: What is MS? Living with MS: A Family Affair We Can Help: The National MS Society What MS Is: MS is thought
Multiple Sclerosis: What You Need To Know For Professionals What will I learn today? The Basics: What is MS? Living with MS: A Family Affair We Can Help: The National MS Society What MS Is: MS is thought
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY / PROCEDURE:
 PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
Whiplash Associated Disorder
 Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Intravenous Immunoglobulin in Neurological disorders
 Intravenous Immunoglobulin in Neurological disorders Exceptional healthcare, personally delivered What is Intravenous Immunoglobulin (IVIg)? Intravenous immunoglobulin (IVIg) is a blood product that combines
Intravenous Immunoglobulin in Neurological disorders Exceptional healthcare, personally delivered What is Intravenous Immunoglobulin (IVIg)? Intravenous immunoglobulin (IVIg) is a blood product that combines
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
Clinical Care Program
 Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
OCCUPATIONAL THERAPY
 OCCUPATIONAL THERAPY This document is subject to change. Please check our web site for updates. This provider manual outlines policy and claims submission guidelines for claims submitted to the North Dakota
OCCUPATIONAL THERAPY This document is subject to change. Please check our web site for updates. This provider manual outlines policy and claims submission guidelines for claims submitted to the North Dakota
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
INFORMATION FOR YOU. Lower Back Pain
 INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
Schiffert Health Center www.healthcenter.vt.edu. Neck Pain (Cervical Strain) COMMON CAUSES: QUICK TREATMENT : NECK PAIN TREATING NECK PAIN:
 Schiffert Health Center www.healthcenter.vt.edu Patient Information: Neck Pain (Cervical Strain) COMMON CAUSES: Neck pain may be triggered by a specific event, such a sport injury or motor vehicle accident.
Schiffert Health Center www.healthcenter.vt.edu Patient Information: Neck Pain (Cervical Strain) COMMON CAUSES: Neck pain may be triggered by a specific event, such a sport injury or motor vehicle accident.
12. Physical Therapy (PT)
 1 2. P H Y S I C A L T H E R A P Y ( P T ) 12. Physical Therapy (PT) Clinical presentation Interventions Precautions Activity guidelines Swimming Generally, physical therapy (PT) promotes health with a
1 2. P H Y S I C A L T H E R A P Y ( P T ) 12. Physical Therapy (PT) Clinical presentation Interventions Precautions Activity guidelines Swimming Generally, physical therapy (PT) promotes health with a
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
CIDP Chronic Inflammatory Demyelinating Polyneuropathy. A publication of the GBS/CIDP Foundation International
 CIDP Chronic Inflammatory Demyelinating Polyneuropathy A publication of the GBS/CIDP Foundation International A special acknowledgement to Dr. Carol Lee Koski, member of the GBS/CIDP Medical Advisory Board
CIDP Chronic Inflammatory Demyelinating Polyneuropathy A publication of the GBS/CIDP Foundation International A special acknowledgement to Dr. Carol Lee Koski, member of the GBS/CIDP Medical Advisory Board
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people)
 Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people) California Animal Rehabilitation (CARE) www.calanimalrehab.com Heather Oxford, DVM, MPH, CVA, CCRT Jessica H. Waldman,
Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people) California Animal Rehabilitation (CARE) www.calanimalrehab.com Heather Oxford, DVM, MPH, CVA, CCRT Jessica H. Waldman,
Premier patient information. Whiplash. Whiplash Exercises
 Premier patient information Whiplash Whiplash Exercises Keep moving! It may be painful but you ll get back to normal much quicker. Moving forward (in fact - moving in any direction!) Movement is the key
Premier patient information Whiplash Whiplash Exercises Keep moving! It may be painful but you ll get back to normal much quicker. Moving forward (in fact - moving in any direction!) Movement is the key
Occupational Therapy
 Occupational Therapy I. Policy University Health Alliance (UHA) will reimburse for occupational therapy when it is determined to be medically necessary and when it meets the medical criteria guidelines
Occupational Therapy I. Policy University Health Alliance (UHA) will reimburse for occupational therapy when it is determined to be medically necessary and when it meets the medical criteria guidelines
Muscular Dystrophy. By. Tina Strauss
 Muscular Dystrophy By. Tina Strauss Story Outline for Presentation on Muscular Dystrophy What is Muscular Dystrophy? Signs & Symptoms Types When to seek medical attention? Screening and Diagnosis Treatment
Muscular Dystrophy By. Tina Strauss Story Outline for Presentation on Muscular Dystrophy What is Muscular Dystrophy? Signs & Symptoms Types When to seek medical attention? Screening and Diagnosis Treatment
let s talk bleeds a bleed checklist for haemophilia patients
 let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Voting for your top research questions Survey
 MS Priority Setting Partnership Voting for your top research questions Survey Prioritising important research questions for multiple sclerosis a partnership between people affected by MS and healthcare
MS Priority Setting Partnership Voting for your top research questions Survey Prioritising important research questions for multiple sclerosis a partnership between people affected by MS and healthcare
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
Rheumatoid Arthritis
 Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
CONTENTS. Note to the Reader 00. Acknowledgments 00. About the Author 00. Preface 00. Introduction 00
 Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
The type of cancer Your specific treatment Your pre training levels before diagnose (your current strength and fitness levels)
 Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
How To Treat Musculoskeletal Injury In Sonographers
 MUSCULOSKELETAL DISORDERS IN SONOGRAPHERS: ARE WE DOING ENOUGH? Many terms are used to refer to work related injuries among sonographers. Musculosketetal injury (MSI) Repetitive motion injury (RMI) Repetitive
MUSCULOSKELETAL DISORDERS IN SONOGRAPHERS: ARE WE DOING ENOUGH? Many terms are used to refer to work related injuries among sonographers. Musculosketetal injury (MSI) Repetitive motion injury (RMI) Repetitive
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
ALL ABOUT SPASTICITY. www.almirall.com. Solutions with you in mind
 ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
DENVER CHIROPRACTIC CENTER GLENN D. HYMAN, DC, CSCS
 DENVER CHIROPRACTIC CENTER GLENN D. HYMAN, DC, CSCS Are you in the right place? Please read this before proceeding with paperwork: At Denver Chiropractic Center, we specialize in treating muscles with
DENVER CHIROPRACTIC CENTER GLENN D. HYMAN, DC, CSCS Are you in the right place? Please read this before proceeding with paperwork: At Denver Chiropractic Center, we specialize in treating muscles with
Physical Therapy. Physical Therapy Payment Policy Policy number M.RTH.02.120301 effective 10/01/2015. Page 1
 Physical Therapy I. Policy University Health Alliance (UHA) will reimburse for physical therapy when it is determined to be medically necessary and when it meets the medical criteria guidelines (subject
Physical Therapy I. Policy University Health Alliance (UHA) will reimburse for physical therapy when it is determined to be medically necessary and when it meets the medical criteria guidelines (subject
Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU
 FOR MS RELAPSES Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU As a person with multiple sclerosis (MS), you know firsthand the profound impact MS relapses can have on your
FOR MS RELAPSES Stepping toward a different treatment option LEARN WHAT ACTHAR CAN DO FOR YOU As a person with multiple sclerosis (MS), you know firsthand the profound impact MS relapses can have on your
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Healing the Invisible Wound. Recovery and Rehabilitation from a Post Traumatic. Stress Injury. By Dr. Amy Menna
 Healing the Invisible Wound Recovery and Rehabilitation from a Post Traumatic Stress Injury By Dr. Amy Menna Post Traumatic Stress Disorder can affect anyone. It is a term used to describe a reaction to
Healing the Invisible Wound Recovery and Rehabilitation from a Post Traumatic Stress Injury By Dr. Amy Menna Post Traumatic Stress Disorder can affect anyone. It is a term used to describe a reaction to
Plantar Fascia Release
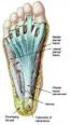 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders
 Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders INTRODUCTION: Health and well being are the result of many factors: Physical activity is one of these factors.
Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders INTRODUCTION: Health and well being are the result of many factors: Physical activity is one of these factors.
Occupational Therapy
 Occupational Therapy Policy Number: Original Effective Date: MM.09.003 07/15/2003 Line(s) of Business: Current Effective Date: HMO; PPO; EUTF; HSTA; QUEST; Federal Plan 87 02/01/2012 Line(s) of Business
Occupational Therapy Policy Number: Original Effective Date: MM.09.003 07/15/2003 Line(s) of Business: Current Effective Date: HMO; PPO; EUTF; HSTA; QUEST; Federal Plan 87 02/01/2012 Line(s) of Business
Stem cell transplant, you and your rehabilitation Information for patients and their carers
 Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds
 Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
CHIROPRACTIC WELLNESS AWARENESS ONE FREE MASSAGE SESSION
 CHIROPRACTIC WELLNESS AWARENESS Do you want to have a healthy body? Do you like to maintain your high energy level? Do you want to be stress-less? Do you like to be pain free? Please call Conrad Nieh D.C.
CHIROPRACTIC WELLNESS AWARENESS Do you want to have a healthy body? Do you like to maintain your high energy level? Do you want to be stress-less? Do you like to be pain free? Please call Conrad Nieh D.C.
REHABILITATION. begins right here
 REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Understanding Relapse in Multiple Sclerosis. A guide for people with MS and their families
 Understanding Relapse in Multiple Sclerosis A guide for people with MS and their families Introduction You have been given this booklet because you have been diagnosed with Multiple Sclerosis (MS) and
Understanding Relapse in Multiple Sclerosis A guide for people with MS and their families Introduction You have been given this booklet because you have been diagnosed with Multiple Sclerosis (MS) and
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
BOTOX Treatment. for Chronic Migraine. Information for patients and their families. Botulinum Toxin Type A
 BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
PHYSICAL THERAPY INTERVENTION WITH ALS
 PHYSICAL THERAPY INTERVENTION WITH ALS Richard W. Briggs MA, PT Chair, APTA Hospice and Palliative Care SIG Amyotrophic Lateral Sclerosis (ALS) provides a challenge to those physical therapists charged
PHYSICAL THERAPY INTERVENTION WITH ALS Richard W. Briggs MA, PT Chair, APTA Hospice and Palliative Care SIG Amyotrophic Lateral Sclerosis (ALS) provides a challenge to those physical therapists charged
