MANAGEMENT OF HEAD INJURY & INTRACRANIAL PRESSURE D. Franzon, MD, S. Kache, MD
|
|
|
- Iris Fox
- 7 years ago
- Views:
Transcription
1 MANAGEMENT OF HEAD INJURY & INTRACRANIAL PRESSURE D. Franzon, MD, S. Kache, MD Etiologies of elevated ICP: Increased ICP can occur with any CNS pathology that results in a space occupying mass lesion, edema (osmotic, vasogenic, cytotoxic), or obstruction to CSF flow. Some common etiologies include: Trauma: epidural, subdural bleeds, contusion, hematomas, diffuse axonal injury, intraventricular hemorrhage Infection: meningitis, encephalitis, cerebritis VP shunt malfunction Mass lesion: tumors, AVM Metabolic: hepatic encephalopathy, DKA Vascular or embolic disease, stroke with subsequent edema or mass effect Hypoxic/ischemic disease resulting in cytoxic edema from cell death Physiology of Intracranial Vault Components of intracranial vault The intracranial vault is comprised of brain (80%), cerebrospinal fluid CSF (10%), cerebral blood volume (10%). The Monroe-Kellie Doctrine states that any individual component of the intra-cranial vault may undergo alterations but the total volume remains fixed since the space within the skull is fixed. The following is a formula of this doctrine with V standing for volume. V (intracranial vault)= V (CSF) + V (brain) + V (blood) + V (other, i.e. mass) The brain has certain normal compensatory mechanisms in place to maintain this equilibrium and in turn maintains normal intra-cranial pressure (ICP). For example displacement of CSF or blood will occur to maintain normal ICP. Eventually, the compensatory mechanisms are exhausted and a sharp rise in ICP will occur. The brain has an elastance that is best demonstrated by a pressurevolume curve (see Figure 1). A normal ICP does not indicate where in the pressure volume curve the patient is at and if any compensatory mechanisms are still in tact. Figure 1 Good Poor Deranged Compensatory Reserve Cerebrovascular Reserve Reactivity ICP Volume Head Injury & ICP 1
2 3 types of cerebral edema Vasogenic: Increased permeability of brain capillary endothelium leads to edema and is usually seen around tumors, abscesses, intracerebral hematomas, encephalitis & meningitis. Neurons are not primarily injured. Reduction of this type of edema can minimize secondary injury Cytotoxic: Neuronal swelling occurs secondary to cell injury caused by failure of the ATPase dependent pump as occurs in diffuse axonal injury. This type of injury is often irreversible. Interstitial: Edema results from increased CSF hydrostatic pressure and is usually seen in hydrocephalus or decreased CSF absorption by arachnoid villi, e.g. intraventricular hemorrhage. Regulation of cerebral blood flow (CBF) The brain maintains CBF via auto-regulation over a wide range of mean arterial pressure (MAP) by altering resistance of cerebral blood vessels. By maintaining a constant CBF, the supply of oxygen and metabolic substrates to the neurons are unaltered. A constant CBF is maintained between MAP of 60mmHg-150mmHg. At a MAP of 60mmHg, the cerebral vessels are maximally dilated; below this MAP, cerebral ischemia will occur. MAP above 150mmHg can lead to ischemia, disruption of the blood-brain barrier, and increased ICP. Cerebral Blood Flow 50 (ml/100g/min) Mean Arterial Pressure (mmhg) Loss of auto-regulation may occur with certain pathologies; i.e. the CBF changes in direct correlation to the blood pressure and is not maintained in a constant range. As blood pressure rises, the CBF rises and as blood pressure falls CBF falls. Cerebral perfusion pressure (CPP), as determined by the formula below, is directly related to CBF. Head Injury & ICP 2
3 CPP = MAP ICP or CVP (which ever of the two pressures is higher) A minimum CPP needs to be maintained to prevent cerebral insult. The minimal CPP is age variant and is as follows: Infants - 50mmHg, Children - 60mmHg, Adults - 70mmHg. CBF is very sensitive to oxygen and carbon dioxide. Hypoxia results in vasodilation therefore increasing CBF and potentially worsening ICP. Hypercarbia likewise results in vasodilation and can alter ICP via effects on CSF ph and increases in CBF. Intracranial pressure monitoring Maintaining adequate CPP is an important factor in survival for patients with elevated ICP. Several forms of ICP monitors exist. Intraventricular monitor is the gold standard. It is accurate and can be re-zeroed. Most importantly, it can withdraw CSF for ICP management. Risks include infection, hemorrhage at time of insertion or removal, and obstruction of the catheter. Insertion of the catheter becomes difficult if the ventricles are small or displaced from shift or mass effect. It is usually positioned at 15cm H2O above the ear. Excessive drainage should be avoided to prevent ventricular collapse. Intraparenchymal monitors are generally fiber optic, and are placed directly into brain parenchyma. They can be easily inserted. Although they are fairly accurate initially, they cannot be re-zeroed and will develop drift over time (6mmHg in 5 days). They can t be used for CSF removal. Evaluation of Elevated ICP: Physical exam should be done with special attention to vital signs, pupillary response, reflexes, fontanelle, focal deficit, and baseline level of consciousness. Signs and symptoms of concern include: Headache Vomiting or poor feeding Altered level of consciousness: drowsy, combative, agitated, irritable, lethargic Full anterior fontanelle in infants Focal neurologic deficit Posturing, seizures Nuchal rigidity (typically with meningitis, encephalitis) Respiratory symptoms: distress, stridor, hyperventilation, Cheyne-Stokes respiration particularly seen if brainstem involved and can be mistaken for a pulmonary source of respiration distress Head Injury & ICP 3
4 Cushing s Triad: hypertension, bradycardia, and abnormal respiration; it is a late and ominous sign of brainstem compression and suggests impending herniation. Pupils: unequal, unreactive, sluggishly reactive, pinpoint, or dilated. Sun-setting : bilateral downward gaze of eyes sometimes seen with shunt malfunction and impending herniation Papilledema Retinal hemorrhages: seen in non-accidental trauma Glasgow Coma Scale (GCS) is an objective measurement, readily available, and is not dependent on the history of illness. The score is a sum of the best eye, verbal and motor response as listed in the table below. Motor Response Verbal Response Eye Opening 6 Follows Commands 5 Oriented 4 Spontaneous 5 Localizes 4 Confused 3 To Speech 4 Withdraws 3 Inappropriate words 2 To Pain 3 Abnormal flexion 2 Incomprehensible 1 No response 2 Extensor response 1 No response 1 No response Laboratory studies that may be helpful. CBC w/diff (trauma, bleed, infection) Coagulation panel (trauma, bleeding) Na+, Ca+, Mg+, glucose ABG - assess oxygenation and ventilation if patient significantly altered BUN/Creatinine (uremia) LFTs, ammonia Tox screen, Salicylate, tylenol levels Thyroid function CSF studies if LP is done Neuroimaging & other modalities of evaluating ICP CT scan is ideal for urgent imaging, and quickly assesses mass effect, shift, edema, and changes in gray/white matter differentiation. It rapidly identifies abnormalities amenable to intervention such as post-traumatic injuries, hemorrhage, tumor, fracture, & hydrocephalus. In trauma patients, the presence of pneumocephalus can be evaluated and bone windows can delineate the location of any skull fractures. A contrast CT is helpful to assess areas of inflammation such as meningitis, vasculitis, encephalitis, and areas surrounding tumors or other lesions (abscess). Decreased enhancement with contrast may indicate infarction, edema or non-enhancing tumors. Acute blood attenuates and is bright, but CSF is Head Injury & ICP 4
5 dark. An indirect assessment of ICP and presence of cerebral edema can be accomplished by evaluating the ventricles and the basal cistern. MRI displays in much greater detail lesions of soft tissue and brain matter. It is the mode of choice for delineating tumors. MRA/MRV are the optimal studies to visualize cerebral blood flow and evaluate for vascular anomalies. It may be used to clarify initial findings seen on CT or that escaped detection on CT, i.e. diffuse axonal injury. Limitations of the MRI include a strong magnetic field making use of equipment more challenging, and longer imaging time. Also, any bony abnormalities are not well visualized on MRI. Lumbar puncture should also be done if the CT and the patient s condition do not preclude it. Always obtain an opening pressure (OP), and a closing pressure if fluid is removed; this allows for evaluation of the brain on the pressure-volume curve. Convert cmh2o on manometer to mmhg by dividing by 1.2. For example, an OP of 28 cmh2o is 23 mmhg. The CSF should be sent for usual studies to rule out infectious sources. Treatment of intracranial hypertension: Patients with a CNS insult have two components: the primary injury, and the secondary injuries that ensue. Once the initial insult has occurred, e.g. head injury or encephalitis, it cannot be reversed. Treatment must therefore focus on either controlling or minimizing the causes of secondary injury. In evaluating the list of secondary injury etiologies, it becomes self evident that if adequate metabolites for recovery are not provided, the pre-existing injury is amplified. The factors associated with secondary CNS injury are hypoxia, hypotension, intracranial hypertension, seizures, fever, and hyperglycemia. General principles: Recall Monroe-Kellie doctrine volume of rigid skull is fixed; therefore therapy for intracranial hypertension should be directed at reducing space occupied by brain, blood CSF, or new pathology. Reduce brain size: osmolar therapy (mannitol, hypertonic saline) Reduce CSF: drainage (EVD) Reduce blood volume (hyperventilation, avoid hypercarbia, hypoxia) Surgical removal of pathology (bleed, tumor) Alternatively can expand skull by decompressive craniectomy 1) ABCs: AVOID HYPOXIA AND HYPOTENSION!! In traumatic brain injury hypoxia and hypotension have been strongly shown to be associated with increased morbidity and mortality amplifies secondary insult. Monitor oxygenation and apply supplemental O2 as required. If the patient has inadequate respiratory effort, GCS <8, rapid clinical Head Injury & ICP 5
6 deterioration (signs of herniation, unequal pupils), or status epilepticus unresponsive to medications, then s/he should be intubated. Support blood pressure by fluid resuscitating the patient as required. Always use at least NS for resuscitative efforts and consider 5-10 cc/kg bolus of hypertonic 3%NS in acutely hypotensive head injury patients. PRBCs may be indicated in trauma with ongoing bleeding. Maintain normal blood pressure in order to maintain adequate cerebral perfusion pressure to the injured brain (CPP=MAP-ICP). If signs of elevated ICP are present, but an ICP monitor hasn t placed, one can assume an ICP of at least 20mmHg. Efforts should be made to maintain a MAP that supports the ideal CPP for age. Patients should be monitored with an arterial line and may need a CVP as well for infusion of vasoactive drips and other medications. 2) General measures Temperature: Avoid fever since it increases cerebral metabolic demand and affects ICP. Head position: Maintain head in midline position at 30 degrees to improve cerebral venous drainage; lower cerebral blood volume (CBV) will lower ICP. In trauma patients, C-spine immobilization must be maintained if concerns until the patient is alert enough for an appropriate exam (even if radiographs and CT of neck are negative). Seizure control & prophylaxis: Seizures worsen secondary CNS injury by increasing the metabolic requirement and potentially increasing ICP. The incidence of post-traumatic seizures is about 10%. Seizures should be controlled with appropriate therapy. Ativan of mg/kg is the initial treatment. A fosphenytoin load of 20mg/kg should also be considered; phenytoin is less likely to interfere with the neuro exam as compared with phenobarbital. The need for seizure prophylaxis should be evaluated on an individual basis and discussed with neurosurgery. Fluid management: Goal is euvolemia. Maintain adequate cardiac output and filling pressures (CVP 4-10) in order to maintain adequate cerebral perfusion. Use isotonic fluids (NS), never hypotonic solutions, for patients with elevated ICP. Avoid hyperglycemia since worse neurologic outcomes have been noted with elevated blood sugars. Hyperglycemia appears to amplify secondary injury through ischemic acidosis. Start enteral nutrition early since head injured patients have increased energy requirements. Stress ulcer prophylaxis should also be initiated immediately. Sepsis is common, particularly 3-7days after head injury; don t delay appropriate antibiotic therapy and consider empiric anti-fungal therapy early. Head Injury & ICP 6
7 3) Ventilator management: Avoid hypercarbia and hypoxia. The brain is very sensitive to PaCO 2 ; a 1mmHg decrease in PaCO 2 could decrease ICP 2-5 mmhg depending on brain compliance. Ventilate to normal PaCO 2 of 35mmHg-40mmHg. Patients with refractory elevated ICP can be hyperventilated to PaCO 2 of 28-32mmHg. However, hyperventilation should not be used as a long-term treatment modality since it results in risk of cerebral ischemia to injured areas and its effects of decreasing ICP are only short lived. 4) Sedation: Agitation, pain, and muscular activity increase ICP. Ideally select a drug that provides analgesia, anxiolysis, avoids hypotension, and allows some examination (particularly if ICP not being monitored). Fentanyl: safe if patient intubated, may develop hypercarbia if oversedated and not intubated (Dosing 1-4 mcg/kg/hr) Propofol: good sedative, short acting, may actually lower ICP, and has the advantage of allowing periodic assessment of neurologic function. Carries risk of hypotension and fatal acidosis; generally safe at modest doses and not for prolonged periods (i.e. <72hrs). (Dosing mcg/kg/min) Versed: sedative, anxiolytic, may cause hypotension (Dosing mg/kg/hr) Ketamine: not recommended since it may increase ICP. Muscle relaxants: Vecuronium or Rocuronium are best for intubation; avoid Succinylcholine since fasciculations may increase ICP. Use paralytics judiciously while the patient is intubated to maintain a physical exam, but also avoid sudden spikes in ICP with sudden cough or valsalva. 5) Osmotic therapy: Hypertonic saline (3%NS approx 500meq/L) has osmotic, hemodynamic, vasoregulatory and immunomodulatory effects. 3% NS reduces osmolar swelling by decreasing both intra-cellular and interstitial fluid volume. It also improves and maintains intravascular volume and blood pressure. Other effects may include decreased vascular resistance with improved cerebral blood flow by decreasing vascular endothelial edema. Inhibition of posttraumatic activation of leukocytes also decreases the degree of inflammation. 3%NS has the added advantage over mannitol of maintaining hemodynamic stability by maintaining intra-vascular volume status. A minimum serum sodium of 145 meq/l should be maintained. Higher sodium levels can be achieved as needed to maintain ICP control either by intermittent boluses or by a continuous infusion of 3% NS. A hypothetical risk of central pontine myelinolysis by rapid increase of serum sodium levels also exists, but has not been reported in trials for traumatic brain injury. Head Injury & ICP 7
8 o Dosing: 5-10cc/kg boluses over 1hr, not to exceed 500 ml or continuous infusion cc/kg/hr, not to exceed 30ml/hr Mannitol is an osmotic diuretic that increases serum osmolality. Effects include decreased blood viscosity, maintaining CBF, decreasing CBV and thereby decreasing ICP if cerebral autoregulation is intact. Maximal effect is within 10 minutes, duration of action is 75 minutes, and it is most effective when given in bolus form. Use the minimum amount needed to maintain a goal serum osmolarity generally of 320 mosm/kg. At high levels, >340 mosm/kg, a risk of renal insufficiency exists. o Dosing gm/kg bolus q 4-6hrs 6) Barbiturates: Barbiturates decrease cerebral metabolic rate and thereby lower CBV and ICP. Free-radical mediated cell injury may also be limited. Side effects include hypotension and myocardial depression; the use of inotropes (Norepi) is often required to maintain MAP and CPP. Barbiturates may also increase the risk of infections by suppressing neutrophil function. 7) Cooling: Induced hypothermia of Celsius may be neuro-protective by decreasing excitatory amino acid levels, and have anti-oxidant plus antiinflammatory effects. Studies have shown active cooling to be effective in both adult and neonatal patients with hypoxic / ischemic insults. Pediatric trials in traumatic brain injury, however, have not demonstrated any improvements in outcomes with active cooling. 8) CSF removal: A surgically placed intraventricular catheter can be used to drain CSF. It improves elevated ICP in patients with decreased intracranial compliance, i.e. small change in intra-cranial volume dramatically reduces intra-cranial pressure. The drain can either be positioned at 10-15cm H2O above the level of ear and left open to drain, or it may be used to monitor ICP and only drained when ICP >20mmHg. 9) Surgical decompression is indicated for clear-cut mass lesions amenable to removal, i.e. tumor, epidural bleed, large contusion. For refractory elevated ICP without a surgical lesion, there may be a role for a decompressive craniectomy. Especially if done early after the initial insult, it may improve functional outcomes of patients. 10) Corticosteroids: Steroids maybe effective in decreasing vasogenic edema as seen with CNS tumors and abscesses. Stepwise approach to ICP Management/Algorithm 1) Avoid hypoxia/hypotension Supplemental O2 or intubate Head Injury & ICP 8
9 Achieve euvolemia Support BP to maintain CPP 2) Avoid Fever 3) Intubate/sedate 4) Mild hyperventilation/avoid hypercapnia Keep PaCO 2 normal 35mmHg-40mmHg 5) Ventricular Drainage 6) Osmolar therapy to achieve serum Osm 320 Mannitol (0.25 to 0.5 g/kg) Hypertonic saline (5 ml/kg of 3%NS) may be given as bolus or continuous 3% infusion checking sodium frequently (q4-6hr) 7) More aggressive hyperventilation - PaCO 2 (28-32 mmhg) Refractory ICP acute short term therapy 8) Barbiturates (Thiopental/Pentobarbital) Thiopental: initial infusion of 10mg/kg/hr for 4 hours followed by infusion at 4mg/kg/hr Pentobarbital: initial infusion of 10mg/kg over 30 minutes, then 5mg/kg/hr for 3 hours, then 1-2mg/kg/hr Drug levels must be monitored Continuous bedside EEG required for patients on barbiturate infusion; monitor for burst suppression 9) Consider cooling particularly in patients with hypoxic-ischemic injury 10) Decompressive craniectomy has shown promising results for some patients with refractory intracranial hypertension Any acute change in ICP during any step of therapy should warrant consideration for re-imaging (head CT) and notifying neurosurgery. Head Injury & ICP 9
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
The Clinical Evaluation of the Comatose Patient in the Emergency Department
 The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Types of Brain Injury
 Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
THERAPY INTENSITY LEVEL
 THERAPY INTENSITY LEVEL TILBasic = TIL Basic. CDE Variable TILBasic = TIL Basic; Global summary measure of Therapy Intensity Level for control of Intracranial Pressure (ICP).. CDE Definition This summary
THERAPY INTENSITY LEVEL TILBasic = TIL Basic. CDE Variable TILBasic = TIL Basic; Global summary measure of Therapy Intensity Level for control of Intracranial Pressure (ICP).. CDE Definition This summary
Traumatic Head Injuries
 Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
TRAUMATIC BRAIN INJURY (TBI)
 Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
Cerebral blood flow (CBF) is dependent on a number of factors that can broadly be divided into:
 Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Using the Pupillometer in Clinical Practice
 Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. chmephill@sfgh.ucsf.edu Kathy Johnson RN, MSN KJOHNSON@queens.org Mary Kay Bader RN, MSN, CCNS Badermk@aol.com Pupillometry: How It
Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. chmephill@sfgh.ucsf.edu Kathy Johnson RN, MSN KJOHNSON@queens.org Mary Kay Bader RN, MSN, CCNS Badermk@aol.com Pupillometry: How It
Traumatic Brain Injury (1.2.3) Management of severe TBI (1.2.3.1) Learning Objectives
 Traumatic Brain Injury (1.2.3) 1.2.3.1 Management of severe TBI 1.2.3.2 Management of concussions 1.2.3.3 Sideline management for team medics/physicians 1.4.2.3.10 Controlled hyperventilation for management
Traumatic Brain Injury (1.2.3) 1.2.3.1 Management of severe TBI 1.2.3.2 Management of concussions 1.2.3.3 Sideline management for team medics/physicians 1.4.2.3.10 Controlled hyperventilation for management
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
LECTURE 16 NEUROPATHOPHYSIOLOGY (HEAD INJURY)
 LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Adult CCRN/CCRN E/CCRN K Certification Review Course: Endocrine 12/2015. Endocrine 1. Disclosures. Nothing to disclose
 Adult CCRN/CCRN E/CCRN K Certification Review Course: Carol Rauen RN BC, MS, PCCN, CCRN, CEN Disclosures Nothing to disclose 1 Body Harmony disorders and emergencies Body Harmony (cont) Introduction Disorders
Adult CCRN/CCRN E/CCRN K Certification Review Course: Carol Rauen RN BC, MS, PCCN, CCRN, CEN Disclosures Nothing to disclose 1 Body Harmony disorders and emergencies Body Harmony (cont) Introduction Disorders
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
Diabetic Emergencies. David Hill, D.O.
 Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 One Children s Plaza Dayton, OH 45404-1815 www.childrensdayton.org DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended
One Children s Plaza Dayton, OH 45404-1815 www.childrensdayton.org DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Cerebral Resusitation and Increased Intracranial Pressure Laura Ibsen, M.D.
 Cerebral Resusitation and Increased Intracranial Pressure Laura Ibsen, M.D. I. Introduction There is a delicate balance between the volume of the intracranial vault (closed compartment) and the volume
Cerebral Resusitation and Increased Intracranial Pressure Laura Ibsen, M.D. I. Introduction There is a delicate balance between the volume of the intracranial vault (closed compartment) and the volume
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Lothian Diabetes Handbook MANAGEMENT OF DIABETIC KETOACIDOSIS
 MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Headache: Differential diagnosis and Evaluation. Raymond Rios PGY-1 Pediatrics
 Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Dehydration & Overhydration. Waseem Jerjes
 Dehydration & Overhydration Waseem Jerjes Dehydration 3 Major Types Isotonic - Fluid has the same osmolarity as plasma Hypotonic -Fluid has fewer solutes than plasma Hypertonic-Fluid has more solutes than
Dehydration & Overhydration Waseem Jerjes Dehydration 3 Major Types Isotonic - Fluid has the same osmolarity as plasma Hypotonic -Fluid has fewer solutes than plasma Hypertonic-Fluid has more solutes than
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
Ischemia and Infarction
 Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Constituents within the skull include the brain (80%/1400ml), blood (10%/150ml) and cerebrospinal fluid (CSF 10%/150ml)
 Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. Part
Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. Part
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Hyperbaric Oxygen Therapy WWW.RN.ORG
 Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
DIAGNOSTIC CRITERIA OF STROKE
 DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
 Approximately 70-80% of all strokes are ischemic and 20-30% are hemorrhagic Hemorrhagic stroke is defined as an acute neurologic injury resulting from bleeding in the brain There are two distinct types
Approximately 70-80% of all strokes are ischemic and 20-30% are hemorrhagic Hemorrhagic stroke is defined as an acute neurologic injury resulting from bleeding in the brain There are two distinct types
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Mind the Gap: Navigating the Underground World of DKA. Objectives. Back That Train Up! 9/26/2014
 Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August 9, 2013
 Stony Brook Medicine Severe Sepsis/Septic Shock Recognition and Treatment Protocols Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August
Stony Brook Medicine Severe Sepsis/Septic Shock Recognition and Treatment Protocols Subject: Severe Sepsis/Septic Shock Published Date: August 9, 2013 Scope: Hospital Wide Original Creation Date: August
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Therapeutic Hypothermia after Cardiac Arrest General Guideline
 Therapeutic Hypothermia after Cardiac Arrest General Guideline I. Associated Guidelines and Appendices 1. Neurological Prognosis after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm 3. Effect
Therapeutic Hypothermia after Cardiac Arrest General Guideline I. Associated Guidelines and Appendices 1. Neurological Prognosis after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm 3. Effect
Is this pt s brain dysfunction due to ischemia? Onset & progression of sx; location of deficit
 CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
Paediatric Clinical Guidelines: Status Epilepticus
 Paediatric Clinical Guidelines: Status Epilepticus Consultant: Dr Alastair Sutcliffe, Dr Christina Petrololous, Dr Tom Bailey Pharmacist: Simon Keady/Neil Tickner To be reviewed: Autumn 2010 The following
Paediatric Clinical Guidelines: Status Epilepticus Consultant: Dr Alastair Sutcliffe, Dr Christina Petrololous, Dr Tom Bailey Pharmacist: Simon Keady/Neil Tickner To be reviewed: Autumn 2010 The following
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
20. Cerebral Compartmental Compliances
 20. Cerebral Compartmental Compliances CBF a (t) Cerebral arterial inflow Cerebral arterial blood volume (C a BV) mean CBF a 0 CBF v (t) Cerebral venous outflow CBV(t) mean CBV + - t t ΔCBV (CBF (t) CBF
20. Cerebral Compartmental Compliances CBF a (t) Cerebral arterial inflow Cerebral arterial blood volume (C a BV) mean CBF a 0 CBF v (t) Cerebral venous outflow CBV(t) mean CBV + - t t ΔCBV (CBF (t) CBF
Objectives. Important Principles
 Management of the Intubated Patient Christopher J. Edwards, PharmD, BCPS Clinical Pharmacist - Emergency Medicine March 19 th, 2013 REPS EC SAG 2 Objectives Describe the rationale for post intubation analgesia
Management of the Intubated Patient Christopher J. Edwards, PharmD, BCPS Clinical Pharmacist - Emergency Medicine March 19 th, 2013 REPS EC SAG 2 Objectives Describe the rationale for post intubation analgesia
Advanced Practice Provider Academy
 (+)Corey M. Slovis, MD, FACEP Professor, Emergency Medicine and Medicine; Chairman, Department of Emergency Medicine, Vanderbilt University Medical Center, Nashville, Tennessee; Medical Director, Metro
(+)Corey M. Slovis, MD, FACEP Professor, Emergency Medicine and Medicine; Chairman, Department of Emergency Medicine, Vanderbilt University Medical Center, Nashville, Tennessee; Medical Director, Metro
Status Epilepticus and Epilepsy
 Status Epilepticus and Epilepsy Chapter 25 Status Epilepticus and Epilepsy Status Epilepticus Defined as protracted or recurrent seizures causing prolonged changes in sensorium and other neurological impairment
Status Epilepticus and Epilepsy Chapter 25 Status Epilepticus and Epilepsy Status Epilepticus Defined as protracted or recurrent seizures causing prolonged changes in sensorium and other neurological impairment
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
HYPOTHERMIA / NORMOTHERMIA: ARCTIC SUN TEMPERATURE MANAGEMENT SYSTEM PROTOCOL AND PROCEDURE
 Page 1 of 7 TOPIC: MANAGEMENT SYSTEM PROTOCOL AND PROCEDURE PURPOSE: To outline the nursing management of a patient receiving hypothermia or normothermia therapy via Arctic Sun Temperature Management System
Page 1 of 7 TOPIC: MANAGEMENT SYSTEM PROTOCOL AND PROCEDURE PURPOSE: To outline the nursing management of a patient receiving hypothermia or normothermia therapy via Arctic Sun Temperature Management System
Diabetic Ketoacidosis
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Post - resuscitation management of an asphyxiated neonate
 Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
+Severe Sepsis EMS Spearheads the Attack against a Devastating Syndrome
 + +Severe Sepsis EMS Spearheads the Attack against a Devastating Syndrome By Andrew Garlisi MD MPH MBA VAQSF CASE PRESENTATION You are called to the residence of a 74 year-old female who has experienced
+ +Severe Sepsis EMS Spearheads the Attack against a Devastating Syndrome By Andrew Garlisi MD MPH MBA VAQSF CASE PRESENTATION You are called to the residence of a 74 year-old female who has experienced
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Emergency Fluid Therapy in Companion Animals
 Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
Emergency Fluid Therapy in Companion Animals Paul Pitney BVSc paul.pitney@tafensw.edu.au The administration of appropriate types and quantities of intravenous fluids is the cornerstone of emergency therapy
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
Emergency Neurological Life Support. Spinal Cord Compression. Version: 1.0 Last Updated: 8/3/2014. Checklist & Communication
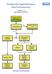 Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Promising Treatments for SCI: What s on The Horizon. SCI: A Devastating Injury. Case: Mr. MC 9/21/2015. Epidemiology: Costs:
 Promising Treatments for SCI: What s on The Horizon Shawn Song, MD SCI Fellow University of Washington/VA Puget Sound Healthcare System SCI: A Devastating Injury Epidemiology: Incidence of ~12,000 patients/year.
Promising Treatments for SCI: What s on The Horizon Shawn Song, MD SCI Fellow University of Washington/VA Puget Sound Healthcare System SCI: A Devastating Injury Epidemiology: Incidence of ~12,000 patients/year.
NORTH WALES CRITICAL CARE NETWORK
 NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
NORTH WALES CRITICAL CARE NETWORK LEVELS OF CRITICAL CARE FOR ADULT PATIENTS Throughout the work of the North Wales Critical Care Network reference to Levels of Care for the critically ill are frequently
Revised 10-4-10 Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes
 Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes If the Certified Athletic Trainer of Bethel Park School District has a concern that a student-athlete
Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes If the Certified Athletic Trainer of Bethel Park School District has a concern that a student-athlete
Seizures (Convulsions, Status Epilepticus) in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Seizures (Convulsions, Status Epilepticus) in Dogs Basics OVERVIEW Seizures are
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Seizures (Convulsions, Status Epilepticus) in Dogs Basics OVERVIEW Seizures are
Inpatient Heart Failure Management: Risks & Benefits
 Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
Management of Acute Traumatic Brain Injury
 Management of Acute Traumatic Brain Injury By G. Christopher Wood, Pharm.D., FCCP, BCPS (AQ Infectious Diseases); and Bradley A. Boucher, Pharm.D., FCCP, FCCM, BCPS Reviewed by Teresa A. Allison, Pharm.D.,
Management of Acute Traumatic Brain Injury By G. Christopher Wood, Pharm.D., FCCP, BCPS (AQ Infectious Diseases); and Bradley A. Boucher, Pharm.D., FCCP, FCCM, BCPS Reviewed by Teresa A. Allison, Pharm.D.,
Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center. April 2007. Revised September 2007
 Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center April 2007 Revised September 2007 Reviewed March 2012 2 The Queen s Medical Center (QMC) is the only trauma
Guidelines for the Triage and Transfer of Patients with Brain Injury to The Queen s Medical Center April 2007 Revised September 2007 Reviewed March 2012 2 The Queen s Medical Center (QMC) is the only trauma
Paediatric fluids 13/06/05
 Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Sepsis: Identification and Treatment
 Sepsis: Identification and Treatment Daniel Z. Uslan, MD Associate Clinical Professor Division of Infectious Diseases Medical Director, UCLA Sepsis Task Force Severe Sepsis: A Significant Healthcare Challenge
Sepsis: Identification and Treatment Daniel Z. Uslan, MD Associate Clinical Professor Division of Infectious Diseases Medical Director, UCLA Sepsis Task Force Severe Sepsis: A Significant Healthcare Challenge
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Both clinical condition and treatment criteria must be met to qualify for critical care coding.
 Yale Compliance Department CRITICAL CARE FACT SHEET 99291 - Critical care, evaluation and management; first 30-74 minutes + 99292 - Critical care, evaluation and management, each additional 30 minutes
Yale Compliance Department CRITICAL CARE FACT SHEET 99291 - Critical care, evaluation and management; first 30-74 minutes + 99292 - Critical care, evaluation and management, each additional 30 minutes
Eileen Whitehead 2010 East Lancashire HC NHS Trust
 Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
The patient s response to therapy within the first hour in the Emergency Room is one of the most reliable ways to predict need for hospitalization.
 Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
sound or ringing in the ears.
 (Idiopathic Intracranial Hypertension) Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis Symptoms The symptoms of include: Headaches
(Idiopathic Intracranial Hypertension) Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis Symptoms The symptoms of include: Headaches
Guidelines and Protocols
 TITLE: HEAD TRAUMA PURPOSE: To provide guidelines for rapid, accurate assessment of the head and intracranial structures for traumatic injury and to plan and implement appropriate interventions for identified
TITLE: HEAD TRAUMA PURPOSE: To provide guidelines for rapid, accurate assessment of the head and intracranial structures for traumatic injury and to plan and implement appropriate interventions for identified
traumatic brain injuries:
 Caring for patients with traumatic brain injuries: Are you up to the challenge? Help your patients survive the immediate and long-term effects of these life-changing injuries. By Debra L. Ryan, MN, RN,
Caring for patients with traumatic brain injuries: Are you up to the challenge? Help your patients survive the immediate and long-term effects of these life-changing injuries. By Debra L. Ryan, MN, RN,
ACID-BASE DISORDER. Presenter: NURUL ATIQAH AWANG LAH Preceptor: PN. KHAIRUL BARIAH JOHAN
 ACID-BASE DISORDER Presenter: NURUL ATIQAH AWANG LAH Preceptor: PN. KHAIRUL BARIAH JOHAN OBJECTIVES OF PRESENTATION 1. To refresh knowledge of acid-base disorders 2. To evaluate acid-base disorders using
ACID-BASE DISORDER Presenter: NURUL ATIQAH AWANG LAH Preceptor: PN. KHAIRUL BARIAH JOHAN OBJECTIVES OF PRESENTATION 1. To refresh knowledge of acid-base disorders 2. To evaluate acid-base disorders using
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
INTRAVENOUS FLUIDS. Acknowledgement. Background. Starship Children s Health Clinical Guideline
 Acknowledgements Background Well child with normal hydration Unwell children (+/- abnormal hydration Maintenance Deficit Ongoing losses (e.g. from drains) Which fluid? Monitoring Special Fluids Post-operative
Acknowledgements Background Well child with normal hydration Unwell children (+/- abnormal hydration Maintenance Deficit Ongoing losses (e.g. from drains) Which fluid? Monitoring Special Fluids Post-operative
THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES
 THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES Guidelines for Inclusion: (check all that apply) Cardiac arrest patients with any of the following: Ventricular fibrillation Pulseless Ventricular tachycardia
THERAPEUTIC INDUCED HYPOTHERMIA GUIDELINES Guidelines for Inclusion: (check all that apply) Cardiac arrest patients with any of the following: Ventricular fibrillation Pulseless Ventricular tachycardia
Hummi Micro Draw Blood Transfer Device. The Next Generation System for Closed Micro Blood Sampling in the Neonate
 Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Hummi Micro Draw Blood Transfer Device The Next Generation System for Closed Micro Blood Sampling in the Neonate Current Methods for Umbilical Blood Sampling Current Methods for Umbilical Blood Sampling
Mary Case, MD Professor of Pathology St. Louis University USA. 2015 MO Juvenile Justice Association Conference Lake Ozark, MO
 Mary Case, MD Professor of Pathology St. Louis University USA 2015 MO Juvenile Justice Association Conference Lake Ozark, MO I have nothing to disclose 75 80% of child abuse deaths are due to head trauma
Mary Case, MD Professor of Pathology St. Louis University USA 2015 MO Juvenile Justice Association Conference Lake Ozark, MO I have nothing to disclose 75 80% of child abuse deaths are due to head trauma
Do We Need a New Definition of Stroke & TIA as Proposed by the AHA? Stroke & TIA need to Remain Clinical Diagnoses: to Change Would be Bonkers!
 Do We Need a New Definition of Stroke & TIA as Proposed by the AHA? No Stroke & TIA need to Remain Clinical Diagnoses: to Change Would be Bonkers! A/Prof Anne L. Abbott Neurologist School of Public Health
Do We Need a New Definition of Stroke & TIA as Proposed by the AHA? No Stroke & TIA need to Remain Clinical Diagnoses: to Change Would be Bonkers! A/Prof Anne L. Abbott Neurologist School of Public Health
Imaging of Acute Stroke. Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group
 Imaging of Acute Stroke Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group Modalities Non Contrast CT (NCCT) Contrast CT Angiography MRI MR Angiography Perfusion
Imaging of Acute Stroke Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group Modalities Non Contrast CT (NCCT) Contrast CT Angiography MRI MR Angiography Perfusion
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
SERVICE: Neurosurgery - Sinai, PGY 1
 SERVICE: Neurosurgery - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Neurosurgery at Sinai Hospital during their intern year. The duration of this rotation
SERVICE: Neurosurgery - Sinai, PGY 1 General description: The Sinai surgical residents will rotate in the Department of Neurosurgery at Sinai Hospital during their intern year. The duration of this rotation
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Common Surgical Procedures in the Elderly
 Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT
 LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT I. GENERAL GUIDELINES Many patients who require transport to centers with specialized or tertiary level resources are appropriate for transport by
LIFEFLIGHT OF MAINE GUIDELINES FOR HELICOPTER TRANSPORT I. GENERAL GUIDELINES Many patients who require transport to centers with specialized or tertiary level resources are appropriate for transport by
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.
 BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
 University of Kentucky / UK HealthCare Policy and Procedure Policy # CH02-02 Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
University of Kentucky / UK HealthCare Policy and Procedure Policy # CH02-02 Title/Description: Admission Criteria, Discharge Criteria, and Standards of Operation of the Pediatric Intensive Care Unit.
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
PHYSICIAN ORDERS / PROGRESS NOTES
 PHYSICIAN / PROGRESS NOTES Drs Joseph Thibodeau and Louis Violi Created: 4/10 - Next Review: 4/10 Page 1 of 5 Initiation Phase: Emergency Department Notify Interventional Cardiology and Cath Lab immediately
PHYSICIAN / PROGRESS NOTES Drs Joseph Thibodeau and Louis Violi Created: 4/10 - Next Review: 4/10 Page 1 of 5 Initiation Phase: Emergency Department Notify Interventional Cardiology and Cath Lab immediately
