Educational Objectives
|
|
|
- Letitia Bryant
- 7 years ago
- Views:
Transcription
1 1mon.qxd 2/2/04 10:26 AM Page 73 Current Overview of Neurovascular Structures in Hip Arthroplasty: Anatomy, Preoperative Evaluation, Approaches, and Operative Techniques to Avoid Complications John-Paul H. Rue, MD* Nozomu Inoue, MD, PhD* Michael A. Mont, MD A major neurovascular injury during total hip arthroplasty (THA) is uncommon. Nevertheless, these are worrisome due to their devastating consequences. As more THAs are performed each year, the chances of this potentially life- or limb-threatening injury increase. 1 It is crucial for the orthopedic surgeon to have a thorough understanding of the anatomy of the region and the potential complications. This article reviews the exposures to the acetabulum for simple and complex primary THA, as well as revision cases, with particular attention to the neurovascular anatomy of the region. ANATOMY Bone The three-dimensional pelvic anatomy is complex and often hard to understand. Several vital vascular and visceral structures are contained within and immediately around the bony pelvis. The bony pelvis is formed by the ilium, From the *Department of Orthopedic Surgery, The Johns Hopkins Medical Institutions, and Sinai Hospital of Baltimore, Center for Joint Preservation & Reconstruction, Baltimore, Md. Drs Rue, Inoue, and Mont have not declared any industry relationships. Reprint requests: Michael A. Mont, MD, Sinai Hospital of Baltimore, Center for Joint Preservation & Reconstruction, 2401 W Belvedere Ave, Baltimore, MD Educational Objectives As a result of reading this article, physicians should be able to: 1. Identify the bony, vascular, and neural anatomy that is relevant to the surgeon performing total hip arthroplasty. 2. Describe the common approaches to avoid neurovascular complications. 3. Discuss the appropriate clinical work-up of these patients. 4. Describe the various neurovascular complications and how to handle them. ischium, and pubis (Figure 1). The acetabulum is located at the junction of these three bones. These bones unite anteriorly at the pubic symphysis and posteriorly to the sacrum to form a ring of bone, which connects the torso to the lower limbs. Vascular Structures The proximity of the major vessels to bone, and therefore their risk for injury during acetabular surgery, varies. Knowledge of vessel location is important because extensive exposure of the acetabulum may be required for complex revision THA. The major vascular structures located within and around the pelvis are the internal and external iliac, femoral, internal pudendal, obturator, and superior and inferior gluteal vessels. Damage to any of these vessels by retraction, drilling, reaming, or dissection can cause massive hemorrhage, which can lead to exsanguination within minutes. The common iliac artery divides at the L5-S1 vertebral disk. The anterior division, the external iliac artery, continues distally to become the common femoral artery, whereas the posterior division becomes the internal iliac artery. The internal iliac artery branches again into a posterior division, which gives rise to the superior gluteal artery, and an anterior division, which gives off the obturator artery before dividing into the inferior gluteal artery and internal pudendal artery. The external iliac artery and vein are immobile and lie close to the pelvis, and thus are at highest risk for injury in 73
2 1mon.qxd 2/2/04 10:26 AM Page 74 ORTHOPEDICS JANUARY 2004 VOL 27 NO Figure 1: Schematic showing the intrapelvic bony anatomy of the acetabular region. Abbreviation: ASIS=anterior superior iliac spine. Figure 2: Schematic showing the excessively long screws on the quadrilateral intrapelvic surface relative to the iliac arterial system. (Reprinted with permission from Wasielewski RC et al. Acetabular anatomy and the transacetabular fixation of screws in total hip arthroplasty. J Bone Joint Surg Am. 1990; 72: Copyright The Journal of Bone and Joint Surgery Inc.) THA (Figure 2). The external iliac vein has been shown to lie within 7 mm of the anterior column of the pelvis at the anterior inferior iliac spine and within 4 mm at the acetabular dome. The external iliac artery is at less risk due to its thicker intima and increased distance from the bone. It lies within 10 mm of the bone at the anterior inferior iliac spine and within 7 mm at the acetabular dome. The common femoral artery lies anterior and medial to the hip capsule. Only the iliopsoas lies between the vessel and capsule at this point. The femoral vein lies medial to the artery and is thus less likely to be injured. The obturator vessels also are at risk, lying fixed within 1 mm of the bony surface at the quadrilateral surface, with their only protection being the interposition of the obturator internus muscle. At the sciatic notch, the superior gluteal vessels are at greatest risk, lying an average of 5 mm from the notch. Injury to the superior gluteal artery as a complication of THA is rare, but has been reported. 2 At the ischial spine, the inferior gluteal vessels lie an average of 6 mm and the pudendal vessels an average of 12 mm from the posterior column. Both, however, are mobile and well protected by a layer of fat. 3,4 The medial and lateral femoral circumflex arteries arise from the deep femoral artery and are vulnerable to retractors placed near the femoral neck. Neuroanatomy The primary nerves of the region are the sciatic, femoral, inferior and superior gluteal, and obturator. The most common nerve injury during THA is to the peroneal division of the sciatic nerve, followed by superior gluteal, obturator, and femoral nerves. Injury to these structures can lead to loss of function and poor outcomes. The femoral nerve is the most lateral structure within the femoral triangle. It lies on the psoas muscle belly at the approximate midpoint between the anterior superior iliac spine and pubic tubercle. Its relationship to the acetabulum is anterior, thus it is primarily at risk during capsule dissection rather than during reaming or drilling. The superior gluteal nerve traverses the interval between the gluteus medius and minimus muscles. It is generally well protected as long as the dissection does not extend 5 cm above the greater trochanter. 5 The inferior gluteal nerve is rarely injured because it inserts into the gluteus maximus proximal and medial to the area, which is split during the posterior approach to the acetabulum. The obturator nerve runs with the obturator vessels. 6 The most common nerve injury during THA is to the sciatic nerve. 7 Several reasons exist, some of which remain conjectural. It has been postulated that these are common because of the sciatic nerve anatomic location. In a review of normal computed tomography (CT), the sciatic nerve was found to lie closest to the posterior column of the pelvis at the acetabular dome, at an average of 9 mm. It also was shown to be more protected at the ischial spine, as the short external rotator muscles are interposed between the nerve and bone at this point; the nerve was an average 15 mm away from the ischial spine
3 1mon.qxd 2/2/04 10:26 AM Page 75 RUE ET AL 3 4 Figure 3: The acetabular quadrant system. The quadrants are formed by the intersection of lines A and B. Line A extends from the anterior superior iliac spine through the center of the acetabulum to the posterior aspect of the fovea, dividing the acetabulum in half. Line B is drawn perpendicular to line A at the mid-point of the acetabulum, dividing it into four quadrants: anterior-superior, anterior-inferior, posteriorsuperior, and posterior-inferior. Abbreviation: ASIS=anterior superior iliac spine. (Reprinted with permission from Wasielewski RC et al. Acetabular anatomy and the transacetabular fixation of screws in total hip arthroplasty. J Bone Joint Surg Am. 1990; 72: Copyright The Journal of Bone and Joint Surgery Inc.) Figure 4: External view of intrapelvic vessels in the quadrilateral region with superimposed acetabular quadrant system as described by Wasielewski RC et al. 3 Quadrant System The acetabular quadrant system described by Wasielewski et al 3 is useful for determining the location of planned acetabular screw fixation in THA to avoid neurovascular complications. The quadrants are formed by drawing a line from the anterior superior iliac spine through the center of the acetabulum and bisecting that line at the center of the acetabulum to form four equal quadrants. The line from the anterior superior iliac spine to the center of the acetabulum serves as the dividing line between anterior and posterior, and the bisecting line as the division between superior and inferior (Figure 3). In cadaver studies, the posteriorsuperior and posterior-inferior quadrants were shown to have the thickest bone and best potential for obtaining secure fixation with the least risk for injury to vessels. The anterior-superior quadrant (the quadrant of death) and the anterior-inferior quadrant were shown to be the most dangerous quadrants for screw fixation due to the thin bone and close proximity of the vessels to bone in that region (Figure 4). APPROACHES The anterolateral and posterior approaches are the most common surgical approaches to the acetabulum during THA. Both approaches offer excellent visualization of the acetabulum. Comparing lateral- and posteriororiented approaches, lateral approaches offer better exposure, although posterior approaches are more popular. The ilioinguinal and anterior (extended iliofemoral) approach are described as these approaches are often used for more extended exposures. 5 In general, the surgical approach chosen for acetabular revision is likely to be the same as that used for the primary surgery unless other factors are involved, such as the need for increased exposure. Posterior Approach The posterior approach to the acetabulum is the least technically demanding approach for THA and offers good visualization of the acetabulum, especially of the posterior wall. It is the most commonly used approach for THA in the United States. The patient is placed in the lateral position. Because the approach involves splitting of the gluteus maximus in line with its fibers, no internervous plane is present. The sciatic nerve is protected by the short external rotators after they are detached from their insertions on the femur and reflected medially (Figure 5). Damage to the inferior gluteal artery is the main vascular risk of the posterior approach. This vessel has many intramuscular branches, which often are cut when the gluteus maximus is split, and they must be identified and cauterized during dissection. For the trauma surgeon dealing with complex pelvic fractures involving the greater sciatic notch, the inferior gluteal artery also is at risk as it exits the pelvis just below the lower border of the piriformis. The most common nerve injury occurring during the posterior approach is contusion to the sciatic nerve. This can be minimized by avoiding excessive 75
4 1mon.qxd 2/2/04 10:26 AM Page 76 ORTHOPEDICS JANUARY 2004 VOL 27 NO 1 A B Figure 5: Diagram showing exposure of the hip through a posterior approach. Note that the sciatic nerve exits below the piriformis muscle (A). The insertions of the short external rotators have been detached and retracted to protect the sciatic nerve (B). The piriformis insertion is left attached. It is normally detached and retracted as well, but does not protect the sciatic nerve such as the short external rotators. traction and ensuring that the nerve is well protected by the short external rotators. Maintaining the hip in an extended position may also decrease the risk of injury by keeping the nerve out of the operative field. Unless specifically indicated, no attempt to dissect the nerve from its surrounding perineural fat should be made. Anterolateral Approach and Modifications The anterolateral approach is a common approach for THA. It offers excellent exposure to the acetabulum. The patient is placed in the lateral position, and the dissection is carried through the intermuscular plane of the tensor fascia lata and gluteus medius. Some surgeons prefer to perform a trochanteric osteotomy, whereas others prefer to detach the anterior two-thirds of the gluteus medius from its insertion on the greater trochanter. A modification of this approach is the Hardinge, which detaches the anterior two-thirds of the gluteus medius and continues in continuity with a softtissue sleeve incorporating a split in the proximal vastus lateralis. 6 The main risks associated with the anterolateral approach are femoral artery and vein laceration, which are vulnerable to retractors placed too far anteriorly. The anterior retractor should be placed at the 1-o clock position for the right hip and the 11-o clock position for the left hip. Care should be taken to ensure that the tip of the retractor is placed directly on bone and does not pierce the psoas muscle, the only barrier between the acetabulum and femoral vessels. Another reasonable alternative is to pass a blunt curved retractor (eg, a blunt Homan) into the pelvis at the anterior acetabulum. Because the femoral nerve is the most lateral structure in the femoral triangle, it also is vulnerable to retractors and excessive retraction. Any modification of this approach that splits the gluteus medius puts the superior gluteal nerve at risk 6 (Figure 6). The transverse branch of the lateral femoral circumflex artery may be encountered when splitting the vastus lateralis during this approach and must be cauterized or ligated. Anterior Approach and Modifications This approach is primarily used for open reduction of developmental hip dislocations, but offers access to the anterior column and anterior lip of the acetabulum. The patient is in the supine position. The superficial dissection exploits the internervous plane between the sartorius (femoral nerve) and tensor fascia latae (superior gluteal nerve). The lateral femoral cutaneous nerve can usually be identified and protected as it emerges over the sartorius, approximately 2.5 cm inferior to the anterior superior iliac spine. The deep dissection is carried out through the plane between the rectus femoris (femoral nerve) and gluteus medius (superior gluteal nerve). The femoral nerve and vessels, because of their anterior relationship to the hip, are at risk during dissection. The femoral structures are protected provided the dissection does not stray out of the plane of the sartorius and tensor fascia latae superficially and the gluteus medius and rectus femoris more deeply. The ascending branch of the lateral femoral circumflex artery crosses the operative field at the proximal interval between the sartorius and tensor fascia latae and must be ligated or coagulated. More extensive exposure of the medial wall and anterior column can be provided by incising the origin of the sartorius at the anterior superior iliac spine, as well as the direct head of the rectus at the anterior superior iliac spine. Smith-Petersen et al 8 modified this approach by cutting the tensor fascia latae distal to the myofascial portion to allow access to the femoral neck and trochanteric area. A further modification of the anterior approach has been described by Light and Keggi, 9 which involves a lateral dissection splitting the medial fibers of the tensor fascia latae medially to provide a mus- 76
5 1mon.qxd 2/2/04 10:26 AM Page 77 RUE ET AL cle cuff to protect the lateral femoral cutaneous nerve and to minimize nerve complications for THA. Ilioinguinal Approach The ilioinguinal approach provides improved visualization of the pelvic inner surface and anterior column and medial wall of the acetabulum. This approach is effective for acetabular fractures involving the anterior wall, anterior column, and associated anterior and posterior hemitransverse fractures, both column, and transverse fractures. Advantages of this approach include excellent cosmesis, rapid recovery, and reduced heterotopic bone formation compared with other extensile approaches. The patient is placed supine or in a lazy lateral decubitus position. The principle of this approach is to dissect closely along the inner wall of the pelvis and lift each muscular and neurovascular structure off of the bone without avulsing or tearing it. Three windows are present in this approach, each providing access to different structures. The first window allows access to the anterior sacroiliac joint, internal iliac fossa, and upper anterior column. The second window, which lies between the iliopsoas with accompanying femoral nerve and iliac vessels, allows access to the pelvic brim, quadrilateral surface, and superior pubic ramus. The third window allows access to the pubic symphysis, superior ramus, quadrilateral surface, and the retropubic space. Nerves at risk during this approach include the femoral nerve, which lies under the inguinal canal on the anterior surface of the iliopsoas muscle. It may be injured by retraction or lacerated during dissection. The lateral femoral cutaneous nerve often is divided at the anterior superior iliac spine unless it can be easily retracted without tension. The femoral vessels run medial to the iliopectineal fascia and are at risk as previously described. The inferior epigastic artery lies medial to the deep inguinal ring and must be ligated. Figure 6: Diagram showing the relationship of the anterior retractor to the femoral nerve, artery, and vein. The retractor tip should be placed directly on bone. Other structures at risk include the bowel, bladder, and spermatic cord. PREOPERATIVE PLANNING History Complex acetabular revision surgery is challenging. As with all preoperative evaluations, a detailed history is paramount. Relevant questions include the indications for the index procedure and any subsequent procedures, as well as the implant type, if known. Other relevant questions include history of infection and prior neurovascular complications. Physical Examination The physical examination should document sensation and motor function of the entire lower extremity, as well as a thorough vascular examination, including bruits or any other abnormalities that might alert the surgeon to a possible vascular injury. If a neurologic deficit exists, electromyogram nerve conduction studies may be useful as part of the preoperative assessment for complete documentation. Examination should document range of motion of both hips and knees, as well as contractures or limb-length discrepancies. Imaging Plain radiographs are essential for bone stock assessment. Significant bony defects may exist in the acetabulum secondary to osteolysis. These defects may preclude screw placement in the optimal quadrants. Additionally, bone loss can lead to improper revision component placement unless care is taken to ensure its correct anatomic positioning. If extensive osteolysis is suspected, CT is recommended as plain radiographs underestimate the extent of lysis. Helical CT with metal artifact minimization is the most sensitive method for identifying and quantifying the extent of lysis. 10 In revision situations, medial migration of the acetabular component may exist. Preoperatively, it is important to determine the location of any intrapelvic cement or hardware in relation to major vascular and visceral structures. In these cases, angiography or CT may assist the 77
6 1mon.qxd 2/2/04 10:26 AM Page 78 ORTHOPEDICS JANUARY 2004 VOL 27 NO 1 surgeon by demonstrating the vascular anatomy of the pelvic region in relation to the proposed operative field. 11 Several case reports have described vascular pseudoaneurysms developing after unrecognized vascular injury during primary THA, and proper visualization of these potential hazards is critical in avoiding damage to these structures during dissection A radiograph can also ascertain various deformities of the acetabulum and femur. For example, in developmental hip dysplasia, the following bony abnormalities may be found and should be given consideration for exposure: increased femoral anteversion; small, osteoporotic femur; shallow or dysplastic acetabulum; and a subluxated or dislocated femur. OPERATIVE TECHNIQUE As with all surgery, the key to successful acetabular surgery is careful and meticulous dissection. Often, the tissue planes are disrupted and the normal anatomy is distorted. Anatomic landmarks may be present, depending on the degree of bone loss. Careful identification of remaining normal landmarks is vital. Knowledge of the acetabular quadrant system and its landmarks is essential. Component Removal The goal of the surgeon when removing existing components is to preserve as much bone stock as possible and minimize the risk of neurovascular injury. Care should be taken to interrupt the interface between the bone and cement when removing cemented acetabular components. The most important thing to remember is not to create a segmental defect. Rim fracture should be avoided to further preserve the structural integrity of the acetabulum and thus reduce the risk of neurovascular injury. Intrapelvic cement extruded through screw holes can snag the external iliac vessels when the component is removed. In these cases, preoperative imaging with either contrast enhanced CT or angiography offers the surgeon options and a roadmap to the vascular anatomy. Some surgeons perform a two-stage procedure for extruded, intrapelvic cement. When removing press-fit porous ingrowth components, similar care should be taken to disrupt the interface between the bone and component before removing the component. Curved and straight osteotomes of varying sizes can be used to disrupt this interface and to gently lever the component free from the bone. Finally, any soft-tissue adhesions should be properly ligated or coagulated, rather than torn free. A similar technique has been described using a punch, inserted through a separate stab incision in the posterior-lateral acetabulum, to disrupt the boneimplant interface. 18 Avoiding Arterial and Venous Injuries The etiology of vascular injuries may be direct or indirect damage. Indirect damage can be due to stretching, tearing, or compression. Direct damage can be caused by excessive reaming or misplacement of retractors. Oftentimes, these indirect or direct injuries cannot be distinguished. A previous review of the vascular injuries sustained during THA revealed the most common etiology of vascular injury as thromboembolic, followed by laceration, pseudoaneurysm, and arteriovenous fistula. The left side was more commonly involved than the right, and the overall mortality was 7%, with a 15% incidence of major and 4% incidence of minor amputations. 11 Damage to the external iliac artery is more common than to the external iliac vein. 19 Both structures are in close proximity to the acetabular dome and need to be avoided. The mechanism of injury usually is due to retractors placed too far medially in the region proximal to the transverse acetabular ligament. To minimize this risk, anterior retractors should be placed directly on the anterior column. Excessive reaming of the acetabulum can cause injury to the external iliac vein. Inadvertent laceration from transacetabular screw fixation and acetabular component migration can lead to damage of this fragile vessel. 14,20 Avoidance of the anterior quadrants can decrease these risks. The anteroinferior quadrant is especially at risk for cement impingement leading to damage to either the obturator nerve, vein, or external iliac vein or artery. The risk of external iliac artery and vein damage from cement extrusion and the heat of polymerization can be avoided by careful cementing technique, including the liberal use of bone graft to fill any defects. Damage to the femoral vessels is most commonly due to aberrant retractor placement. 17,21 Care should be taken to ensure that the retractor tip is placed directly on bone, and that the iliopsoas is not interposed between the retractor tip and bone. Extruded cement, 22 acetabular cup migration, 16 and capsule dissection 23 have also been implicated in damage to the femoral vessels. The inferior and superior gluteal arteries can be injured by poor placement of transacetabular screws, or by pin retractors placed near the sciatic notch. 2 Proper drilling technique, including direct palpation guidance, can decrease this risk. Although rare, laceration of the obturator vessels can occur from indirect contact by osteophytes or pieces of cement, or by direct violation by a retractor placed into the superior-lateral corner of the obturator foramen. Retroperitoneal Approach for Uncontrolled Bleeding When facing a complex acetabular revision or uncontrollable bleeding, the orthopedic surgeon should also be familiar with the retroperitoneal approach to the acetabulum. This approach has been described as a two-stage procedure for revision total THA and as an emergency procedure for intrapelvic control of a major vascular injury. 24,25 This approach can be used when the surgeon is concerned during complex acetabular revisions in the following situations: intrapelvic dislocation, protrusion with 78
7 1mon.qxd 2/2/04 10:26 AM Page 79 RUE ET AL no bony barrier, intrapelvic cement or implants, and anomalous vessels or path detected on preoperative angiography. This approach lowers the risk of damaging intrapelvic vessels, which may be inaccessible through standard approaches to the hip. For two-stage revisions, the patient is placed in the lateral decubitus position, and the posterior pad is removed to allow the patient to assume a slightly more supine lazy lateral position. The retroperitoneal approach is performed to remove any intrapelvic cement and mobilize the vessels. The posterior pad is then replaced and the patient returned to the lateral position, and the second stage revision of the joint through either a lateral or posterior approach is performed. The advantage of this technique is that it allows for a combined anterior and lateral or posterior approach to the acetabulum during a single operation. A similar technique can be used in an emergency without repositioning the patient, should immediate intrapelvic vascular control be required. The curvilinear incision for the retroperitoneal approach is made starting approximately 3 cm medial to the anterior superior iliac spine and ending at the inguinal ligament, over the femoral artery (Figure 7). The subcutaneous tissue, external and internal obliques, and the transversus abdominus muscles are divided to enter the retroperitoneum. At this level, the external iliac vein lies posterior to the artery. For emergency control of severe bleeding, a vessel loop can be used to temporarily ligate the external iliac vessels until the bleeding vessel can be cauterized or ligated. For two-stage revisions, these vessel loops can be loosely brought out of the wound, and the wound packed and skin temporarily closed in the event that intrapelvic proximal vascular control is needed during the joint revision stage. 26 Ideally, the orthopedic surgeon should be comfortable with the initial retroperitoneal exposure and clamping of the large feeder vessels of the pelvis until a vascular surgeon performs the definitive vascular procedure. It should be noted that ligation as a damage control procedure for major vascular injury is a valid option, provided the consequences are understood. In most patients, ligation of the iliac, common femoral, and superficial femoral arteries results in critical limb ischemia and should be followed by open fasciotomy of all thigh and lower leg compartments, as compartment syndrome is common postoperatively and often difficult to diagnose in these patients. Conversely, all limb veins can be ligated without severe complications. 26 If hemorrhage continues, but the patient is stable, selective arterial embolization may be another option. This procedure has been used in pelvic fractures for control of bleeding. In large centers where emergency angiography is readily available, it offers a less invasive, perhaps more precise method for identifying and embolizing select vessels without extensive surgical dissection, which could cause worsening hemorrhage. Halpern et al 27 reported a case of delayed massive bleeding from the inferior gluteal artery, which was selectively embolized using angiography. Postoperative Care Several postoperative considerations exist for patients after severe bleeding complications. The patient should be closely monitored and aggressively resuscitated. Drain output should be followed closely. Laboratory studies should include serial hematocrits and coagulation panels. The surgeon should have a low threshold for re-exploration of the wound if high drain outputs persist or signs of active bleeding such as tachycardia, hypotension, or a falling hematocrit are present. Figure 7: Diagram showing the skin incisions for the two-incision retroperitoneal approach. Avoiding Nerve Injury Following primary THA, the incidence of nerve palsy has been reported to be approximately 1.3%, but may be as high as 5.2% for primary THA performed for developmental dysplasia or dislocation. 7 For revision surgery, the incidence may be as high as 7.6%. 19 Sciatic nerve palsy is the most common nerve injury following THA, with estimates ranging from 0.5%-2%. 28,29 Clinically, patients with a sciatic nerve palsy complain of weakness or inability to dorsiflex the foot. Approximately 50% of these injuries have been related to lengthening and increasing lateral displacement of the leg, 22% from direct injury, 20% from bleeding complications, and 10% from postoperative dislocations. Leg lengthening should be minimized to 6% of the limb length. Thus, small individuals will be at increased risk, as well as females due to size and less muscle mass. Improved outcome may be expected from patients who have full or returning motor function postoperatively. During surgery, the surgeon should minimize the tension on the sciatic nerve by maintaining the knee in a flexed position as much as possible, and femoral shortening osteotomy in the dislocated dysplastic hip should be considered to reduce the risk of nerve palsy. 19 Femoral nerve palsies are most often caused by retractor placement. Clinically, patients with femoral nerve palsies have weakness or loss of quadriceps function. In general, femoral nerve palsies occur in combination with sciatic nerve palsies; however, they may occur independently. The incidence of 79
8 1mon.qxd 2/2/04 10:26 AM Page 80 ORTHOPEDICS JANUARY 2004 VOL 27 NO 1 femoral nerve palsy is approximately 2%. Injury to the obturator nerve is rare. The use of somatosensory evoked potentials has been studied in patients undergoing THA. Its use was not indicated for primary procedures, although it may play a role in revision surgery, especially in cases where limb lengthening is expected. 7,30 Hematomas The formation of a hematoma can produce immediate or delayed onset nerve palsy subsequent to THA. When it involves the gluteal compartment, the sciatic nerve is at risk. 31 The same is true for a hematoma around the iliacus, which can cause femoral nerve palsy, especially after perforation of the medial wall in complex or revision THA. Symptoms associated with the formation or secondary nerve palsy include excessive pain exacerbated by passive stretch of the involved compartment. Aneurysm/Pseudoaneurysm Unrecognized injury to vascular structures during THA may not result in immediate hemorrhage because of vasoconstriction temporarily occluding the arterial lumen. The manifestation of these injuries may include arteriovenous fistula between the common femoral artery and vein, false aneurysm of the common femoral artery, and hip dislocation from a false aneurysm of the medial femoral circumflex. 32,33 Avoiding Other Surgery-Related Complications Deep venous thrombosis (DVT) is estimated to occur in up to 70% of patients after THA without prophylaxis, with fatal pulmonary embolism occurring in 2%. With appropriate prophylaxis, either mechanical or pharmacologic, the incidence of DVT and pulmonary embolism decreases significantly. Mobilization of the femoral vessels during dissection and kinking during dislocation of the femoral head has been implicated in the etiology of DVT. During revision THA, care must be taken to minimize the insult to all neurovascular structures during surgery to lessen the chance of developing DVT and subsequent complications. Postoperative limb ischemia can result from THA. In patients with preexisting atherosclerosis, various intraoperative maneuvers required for positioning and dislocating the hip have been implicated. 11 Another possible mechanism is occlusion of the external iliac artery by protrusio of the acetabular component. 34 Preoperative vascular consultation is helpful for patients with atherosclerosis undergoing elective THA. SUMMARY Total hip arthroplasty is a common and relatively safe procedure with consistently good results. Despite its popularity and excellent results, THA is a major operation with several major neurovascular structures within reach of retractors, scalpel blades, drills, screws, and reamers. A thorough knowledge of their anatomic location and proximity to the operative field, along with a basic understanding of the principles of vascular surgery can help avoid potentially devastating consequences. Specifically, the surgeon should avoid placement of screws in the anterior-superior quadrant, be vigilant when placing retractors, and avoid excessive tension on the sciatic nerve. REFERENCES 1. Ratliff AH. Editorial: arterial injuries after total hip replacement. J Bone Joint Surg Br. 1985; 67: Lozman H, Robbins H. Injury to the superior gluteal artery as a complication of total hipreplacement arthroplasty. A case report. J Bone Joint Surg Am. 1983; 65: Wasielewski RC, Cooperstein LA, Kruger MP, Rubash HE. Acetabular anatomy and the transacetabular fixation of screws in total hip arthroplasty. J Bone Joint Surg Am. 1990; 72: Keating EM, Ritter MA, Faris PM. Structures at risk from medially placed acetabular screws. J Bone Joint Surg Am. 1990; 72: Ramesh M, O Byrne JM, McCarthy N, Jarvis A, Mahalingham K, Cashman WF. Damage to the superior gluteal nerve after the Hardinge approach to the hip. J Bone Joint Surg Br. 1996; 78: Hoppenfeld S, deboer P. In: Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, Pa: Lippincott Williams and Wilkins; 1994: Schmalzried TP, Amstutz HC, Dorey FJ. Nerve palsy associated with total hip replacement. Risk factors and prognosis. J Bone Joint Surg Am. 1991; 73: Smith-Petersen MN, Cave E, VanGorder G. Intracapsular fractures of the neck of the femur: treatment by internal fixation. Arch Surg. 1931; 23: Light TR, Keggi KJ. Anterior approach to hip arthroplasty. Clin Orthop. 1980; 152: Puri L, Wixson RL, Stern SH, Kohli J, Hendrix RW, Stulberg SD. Use of helical computed tomography for the assessment of acetabular osteolysis after total hip arthroplasty. J Bone Joint Surg Am. 2002; 84: Shoenfeld N, Stuchin SA, Pearl R, Harveson S. The management of vascular injuries associated with total hip arthroplasty. J Vasc Surg. 1990; 11: Gruen GS, Mears DC, Cooperstein LA. Three-dimensional angio-computed tomography. New technique for imaging the acetabulum and adjacent vessels in a patient with acetabular protrusio. J Arthroplasty. 1989; 4: Scullin JP, Nelson CL, Beven EG. False aneurysm of the left external iliac artery following total hip arthroplasty. Clin Orthop. 1975; 113: Ryan JA, Johnson ML, Boettcher WG, Kirkpatrick JN. Mycotic aneurysm of the external iliac artery caused by migration of a total hip prosthesis. Clin Orthop. 1984; 186: Hopkins NF, Vanhegan JA, Jamieson CW. Iliac aneurysm after total hip arthroplasty. Surgical management. J Bone Joint Surg Am. 1983; 65: Giacchetto J, Gallagher J. False aneurysm of the common femoral artery secondary to migration of a threaded acetabular component. A case report and review of the literature. Clin Orthop. 1988; 231: Nachbur B, Meyer RP, Verkkala K, Zurcher R. The mechanisms of severe arterial injury in surgery of the hip joint. Clin Orthop. 1979; 141: Markovich GD, Banks SA, Hodge WA. A new technique for removing noncemented acetabular components in revision total hip arthroplasty. Am J Orthop. 1999; 28: Wasielewski RC, Crossett LS, Rubash HE. Neural and vascular injury in total hip arthroplasty. Orthop Clin North Am. 1992; 23: Mallory TH. Rupture of the common iliac vein from reaming the acetabulum during total hip replacement. A case report. J Bone Joint Surg Am. 1972; 54: Salama R, Stavorovsky M, Iellin A, Weissman SL. Femoral artery injury complicating total hip replacement. Clin Orthop. 1972; 89: Dorr LD, Conaty JP, Kohl R, Harvey JP Jr. False aneurysm of the femoral artery following total hip surgery. J Bone Joint Surg Am. 1974; 56: Brismar B, Veress B, Svensson O. Injury of the femoral artery in total hip replacement causing abdominal pain and hypovolemic shock. A case report. J Bone Joint Surg Am. 1992; 74:
9 1mon.qxd 2/2/04 10:26 AM Page 81 RUE ET AL 24. Petrera P, Trakru S, Mehta S, Steed D, Towers JD, Rubash HE. Revision total hip arthroplasty with a retroperitoneal approach to the iliac vessels. J Arthroplasty. 1996; 11: Rorabeck CH, Partington PF. Retroperitoneal exposure in revision total hip arthroplasty. Instruct Course Lect. 1999; 48: Aucar JA, Hirshberg A. Damage control for vascular injuries. Surg Clin North Am. 1997; 77: Halpern AA, Rinsky LJ, Burton DS. Selective arterial embolization for hemorrhage following hip arthroplasty. Clin Orthop. 1977; 124: Edwards BN, Tullos HS, Noble PC. Contributory factors and etiology of sciatic nerve palsy in total hip arthroplasty. Clin Orthop. 1987; 218: Lewallen DG. Neurovascular injury associated with hip arthroplasty. Instr Course Lect. 1998; 47: DeHart MM, Riley LH Jr. Nerve injuries in total hip arthroplasty. J Am Acad Orthop Surg. 1999; 7: Fleming RE Jr, Michelsen CB, Stinchfield FE. Sciatic paralysis. A complication of bleeding following hip surgery. J Bone Joint Surg Am. 1979; 61: Aust JC, Bredenberg CE, Murray DG. Mechanisms of arterial injuries associated with total hip replacement. Arch Surg. 1981; 116: Mariconda M, Chello M, Lotti G, Mastroroberto P, Milano C. Dislocation of total hip prosthesis by false aneurysm of the medial circumflex femoral artery. Orthopedics. 2000; 23: Reiley MA, Bond D, Branick RI, Wilson EH. Vascular complications following total hip arthroplasty. A review of the literature and a report of two cases. Clin Orthop. 1984; 186:
Surgical Approaches to Total Hip Arthroplasty
 Surgical Approaches to Total Hip Arthroplasty Daniel Kelmanovich, 1 Michael L. Parks, MD, 2 Raj Sinha, MD, PhD, 3 and William Macaulay, MD 4 Surgical exposure of the hip for trauma, infection, or reconstruction
Surgical Approaches to Total Hip Arthroplasty Daniel Kelmanovich, 1 Michael L. Parks, MD, 2 Raj Sinha, MD, PhD, 3 and William Macaulay, MD 4 Surgical exposure of the hip for trauma, infection, or reconstruction
Total hip arthroplasty (THA) through the anterior approach
 Primary Total Hip Arthroplasty with a Minimally Invasive Anterior Approach Jonathan G. Yerasimides, MD, and Joel M. Matta, MD Total hip arthroplasty (THA) through the anterior approach is a minimally invasive
Primary Total Hip Arthroplasty with a Minimally Invasive Anterior Approach Jonathan G. Yerasimides, MD, and Joel M. Matta, MD Total hip arthroplasty (THA) through the anterior approach is a minimally invasive
Chapter 9 The Hip Joint and Pelvic Girdle
 Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. The Hip Joint and Pelvic Girdle Chapter 9 The Hip Joint and Pelvic Girdle Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Hip joint
Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. The Hip Joint and Pelvic Girdle Chapter 9 The Hip Joint and Pelvic Girdle Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Hip joint
13 Adductor Muscle Group Excision
 Malawer Chapter 13 21/02/2001 15:36 Page 243 13 Adductor Muscle Group Excision Martin Malawer and Paul Sugarbaker OVERVIEW The adductor muscle group is the second most common site for high- and low-grade
Malawer Chapter 13 21/02/2001 15:36 Page 243 13 Adductor Muscle Group Excision Martin Malawer and Paul Sugarbaker OVERVIEW The adductor muscle group is the second most common site for high- and low-grade
MIS Direct Anterior Approach Surgical Protocol
 Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Anatomy and Pathomechanics of the Sacrum and Pelvis. Charles R. Thompson Head Athletic Trainer Princeton University
 Anatomy and Pathomechanics of the Sacrum and Pelvis Charles R. Thompson Head Athletic Trainer Princeton University Simplify Everything There are actually only three bones: Two innominates, one sacrum.
Anatomy and Pathomechanics of the Sacrum and Pelvis Charles R. Thompson Head Athletic Trainer Princeton University Simplify Everything There are actually only three bones: Two innominates, one sacrum.
Musculoskeletal Ultrasound Technical Guidelines. IV. Hip
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines IV. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines IV. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
Anterior Superior Iliac Spine. Anterior Inferior Iliac Spine. head neck greater trochanter intertrochanteric line lesser trochanter
 Ilium Bones The Skeleton Ischium Pubis Sacro-iliac Joint Iliac Crest Anterior Superior Superior Pubic Ramus Anterior Inferior Acetabulum Obturator Foramen Ischio-pubic ramus Ischial tuberosity Pubic Crest
Ilium Bones The Skeleton Ischium Pubis Sacro-iliac Joint Iliac Crest Anterior Superior Superior Pubic Ramus Anterior Inferior Acetabulum Obturator Foramen Ischio-pubic ramus Ischial tuberosity Pubic Crest
An overview of the anatomy of the canine hindlimb
 An overview of the anatomy of the canine hindlimb Darren Kelly Artwork by Paddy Lennon Original photos courtesy of Mary Ferguson Students at University College Dublin, School of Veterinary Medicine. Video
An overview of the anatomy of the canine hindlimb Darren Kelly Artwork by Paddy Lennon Original photos courtesy of Mary Ferguson Students at University College Dublin, School of Veterinary Medicine. Video
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral head and neck ostectomy (FHO) is a commonly
 P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
The Abdominal Wall And Hernias. Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK
 The Abdominal Wall And Hernias Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK The Abdominal Wall The structure of the abdominal wall is similar in principle to the thoracic wall. There are
The Abdominal Wall And Hernias Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK The Abdominal Wall The structure of the abdominal wall is similar in principle to the thoracic wall. There are
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
The Anterior Approach for Total Hip Replacement. Background and Operative Technique
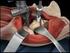 The Anterior Approach for Total Hip Replacement Background and Operative Technique Joel M. Matta, MD Hip and Pelvis Institute at Saint John s Health Center, Director Santa Monica, California RECOVERY FUNCTION
The Anterior Approach for Total Hip Replacement Background and Operative Technique Joel M. Matta, MD Hip and Pelvis Institute at Saint John s Health Center, Director Santa Monica, California RECOVERY FUNCTION
Laparoscopic Anatomy of the Pelvis
 2 Laparoscopic Anatomy of the Pelvis Intra-Abdominal Anatomy of the Male Pelvic Region Bladder Medial Umbilical Ligaments Lateral Umbilical Ligaments Spermatic Cords Iliac Vessels Ureters Seminal Vesicular
2 Laparoscopic Anatomy of the Pelvis Intra-Abdominal Anatomy of the Male Pelvic Region Bladder Medial Umbilical Ligaments Lateral Umbilical Ligaments Spermatic Cords Iliac Vessels Ureters Seminal Vesicular
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
MET: Posterior (backward) Rotation of the Innominate Bone.
 MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
PELVIS. 2007 Lippincott Williams & Wilkins S59 BONE: PELVIS (6) Location: Pelvic ring (61)
 PELVIS BONE: PELVIS (6) Location: Pelvic ring (61) Types: A. Lesion sparing (or with no displacement of) posterior arch (61-A) B. Incomplete disruption of posterior arch, partially stable (61-B) C. Complete
PELVIS BONE: PELVIS (6) Location: Pelvic ring (61) Types: A. Lesion sparing (or with no displacement of) posterior arch (61-A) B. Incomplete disruption of posterior arch, partially stable (61-B) C. Complete
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Lower Extremity Orthopedic Surgery in Cerebral Palsy. Hank Chambers, MD Rady Children s Hospital - San Diego
 Lower Extremity Orthopedic Surgery in Cerebral Palsy Hank Chambers, MD Rady Children s Hospital - San Diego Indications Fixed contracture Joint dislocations Shoe wear problems Pain Perineal hygiene problems
Lower Extremity Orthopedic Surgery in Cerebral Palsy Hank Chambers, MD Rady Children s Hospital - San Diego Indications Fixed contracture Joint dislocations Shoe wear problems Pain Perineal hygiene problems
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284
 ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284 15 TH APRIL 2013 Dr Suresh Kumar Jeyaraj, Specialty Doctor Dr Tim Pepall, Consultant Anaesthetist Frimley Park Hospital NHS foundation
ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284 15 TH APRIL 2013 Dr Suresh Kumar Jeyaraj, Specialty Doctor Dr Tim Pepall, Consultant Anaesthetist Frimley Park Hospital NHS foundation
MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient
 C H A P T E R 4 5 MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient M. Jay Groves, IV, DPM Gastrosoleal equinus is a common deforming force on the foot and ankle.
C H A P T E R 4 5 MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient M. Jay Groves, IV, DPM Gastrosoleal equinus is a common deforming force on the foot and ankle.
Versa-Fx II Femoral Fixation System Surgical Techniques
 Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Converge CSTi Porous Acetabular Cup System. Surgical Technique
 Converge CSTi Porous Acetabular Cup System Surgical Technique 2 Converge CSTi Porous Acetabular Cup System Surgical Technique Converge CSTi Porous Acetabular Cup System Surgical Technique 3 CONVERGE CSTI
Converge CSTi Porous Acetabular Cup System Surgical Technique 2 Converge CSTi Porous Acetabular Cup System Surgical Technique Converge CSTi Porous Acetabular Cup System Surgical Technique 3 CONVERGE CSTI
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Zimmer M/L Taper Hip Prosthesis. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Lower limb nerve blocks
 Lower limb nerve blocks Barry Nicholls is Consultant in Anaesthesia and Pain Management at Musgrove Hospital, Taunton, UK. He qualified from Liverpool University and trained in Newcastle, UK, and Seattle,
Lower limb nerve blocks Barry Nicholls is Consultant in Anaesthesia and Pain Management at Musgrove Hospital, Taunton, UK. He qualified from Liverpool University and trained in Newcastle, UK, and Seattle,
Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D.
 Hip Series Technique Guide Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D. As described by: J.W. Thomas Byrd, M.D. Southern Sports Medicine and Orthopaedic Center Nashville, TN Introduction
Hip Series Technique Guide Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D. As described by: J.W. Thomas Byrd, M.D. Southern Sports Medicine and Orthopaedic Center Nashville, TN Introduction
P REPLACEMENT SURGERY
 P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
ONSTEP Technique. Technique Guide * Anterior Approach to a Part Preperitoneal, Part Intramuscular Inguinal Hernia Repair
 ONSTEP Technique Technical Aspects of the ONSTEP Inguinal Hernia Repair Technique Using the PolySoft Hernia Patch with Interrupted Memory Recoil Ring Technique Guide * Anterior Approach to a Part Preperitoneal,
ONSTEP Technique Technical Aspects of the ONSTEP Inguinal Hernia Repair Technique Using the PolySoft Hernia Patch with Interrupted Memory Recoil Ring Technique Guide * Anterior Approach to a Part Preperitoneal,
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
NETWORK FITNESS FACTS THE HIP
 NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Chapter 7. Expose the Injured Area
 Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
PINNACLE. Polyethylene Surgical Technique. Surgical Technique
 PINNACLE Hip Solutions Polyethylene Surgical Technique Surgical Technique Table of Contents Surgical technique Introduction 4 Templating and Pre-Operative Planning 6 Surgical Approach Anterolateral 8
PINNACLE Hip Solutions Polyethylene Surgical Technique Surgical Technique Table of Contents Surgical technique Introduction 4 Templating and Pre-Operative Planning 6 Surgical Approach Anterolateral 8
FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT
 1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Chapter 9 The Hip Joint and Pelvic Girdle
 Chapter 9 The Hip Joint and Pelvic Girdle Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Hip relatively joint (acetabularfemoral) functions bony strong large stable due to The enhanced architecture
Chapter 9 The Hip Joint and Pelvic Girdle Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Hip relatively joint (acetabularfemoral) functions bony strong large stable due to The enhanced architecture
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica
 Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
Bard * PerFix * Plug. Technique Guide. A Modified Technique with the. Open Inguinal Hernia Repair
 A Modified Technique with the Bard * PerFix * Plug A quick and simple preperitoneal underlay Modified Technique for the repair of groin hernias Technique Guide Open Inguinal Hernia Repair This technique,
A Modified Technique with the Bard * PerFix * Plug A quick and simple preperitoneal underlay Modified Technique for the repair of groin hernias Technique Guide Open Inguinal Hernia Repair This technique,
Anatomy and Physiology 121: Muscles of the Human Body
 Epicranius Anatomy and Physiology 121: Muscles of the Human Body Covers upper cranium Raises eyebrows, surprise, headaches Parts Frontalis Occipitalis Epicranial aponeurosis Orbicularis oculi Ring (sphincter)
Epicranius Anatomy and Physiology 121: Muscles of the Human Body Covers upper cranium Raises eyebrows, surprise, headaches Parts Frontalis Occipitalis Epicranial aponeurosis Orbicularis oculi Ring (sphincter)
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
The Essential Lower Back Exam
 STFM National Convention 2011 New Orleans The Essential Lower Back Exam Judith A. Furlong, M.D., Cathee McGonigle, D.O. & Rob Rutherford, MD Objectives Brief review of the anatomy of the back, (hip and
STFM National Convention 2011 New Orleans The Essential Lower Back Exam Judith A. Furlong, M.D., Cathee McGonigle, D.O. & Rob Rutherford, MD Objectives Brief review of the anatomy of the back, (hip and
Exeter X3 RimFit. Acetabular Cup Surgical Protocol
 Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Surgical Technique. Struan H Coleman MD, PhD
 Surgical Technique Guide Struan H Coleman MD, PhD the Author Struan H. Coleman MD, PhD, specializes in Sports Medicine at Hospital for Special Surgery where he treats orthopedic conditions of the shoulder,
Surgical Technique Guide Struan H Coleman MD, PhD the Author Struan H. Coleman MD, PhD, specializes in Sports Medicine at Hospital for Special Surgery where he treats orthopedic conditions of the shoulder,
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP
 TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so that
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so that
Stretching the Major Muscle Groups of the Lower Limb
 2 Stretching the Major Muscle Groups of the Lower Limb In this chapter, we present appropriate stretching exercises for the major muscle groups of the lower limb. All four methods (3S, yoga, slow/static,
2 Stretching the Major Muscle Groups of the Lower Limb In this chapter, we present appropriate stretching exercises for the major muscle groups of the lower limb. All four methods (3S, yoga, slow/static,
Titanium Wire with Barb and Needle. For canthal tendon procedures.
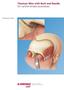 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information
 Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Introduction to the Bertram Hip Spacer
 Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Extremity Trauma. William Schecter, MD
 Extremity Trauma William Schecter, MD Approach to the Evaluation of the Patient with an Extremity Injury Blood Supply Skeleton Neurologic Function Risk for Compartment Syndrome? Coverage (Skin and Soft
Extremity Trauma William Schecter, MD Approach to the Evaluation of the Patient with an Extremity Injury Blood Supply Skeleton Neurologic Function Risk for Compartment Syndrome? Coverage (Skin and Soft
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
Treatment of hip dysplasia in children with. Terje Terjesen Department of Orthopaedic Surgery Oslo University Hospital, Rikshospitalet
 Treatment of hip dysplasia in children with cerebral palsy Terje Terjesen Department of Orthopaedic Surgery Oslo University Hospital, Rikshospitalet Oslo, Norway Why do CP children have problems in the
Treatment of hip dysplasia in children with cerebral palsy Terje Terjesen Department of Orthopaedic Surgery Oslo University Hospital, Rikshospitalet Oslo, Norway Why do CP children have problems in the
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Arthroscopy of the Hip
 Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation
 1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
Wagner SL Revision Hip Stem
 Wagner SL Revision Hip Stem Surgical Technique Femoral Revision Prosthesis for Extensive Bone Loss Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
Wagner SL Revision Hip Stem Surgical Technique Femoral Revision Prosthesis for Extensive Bone Loss Disclaimer This document is intended exclusively for experts in the field, i.e. physicians in particular,
Risks of Spinal Surgery
 Risks of Spinal Surgery Infection One of the more common potential complications of any surgery is a wound infection. In spinal surgery this can be a very severe problem. It occurs in 1.5 percent to 3
Risks of Spinal Surgery Infection One of the more common potential complications of any surgery is a wound infection. In spinal surgery this can be a very severe problem. It occurs in 1.5 percent to 3
SCAPULAR FRACTURES. Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading.
 SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
SECTION II General Osteopathic Techniques
 SECTION II General Osteopathic Techniques Chapter Four The Lower Extremities 40 Ligamentous Articular Strain The lower extremities are among the most important structures of the body and yet are often
SECTION II General Osteopathic Techniques Chapter Four The Lower Extremities 40 Ligamentous Articular Strain The lower extremities are among the most important structures of the body and yet are often
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE
 ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation
 What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
Muscular System. Student Learning Objectives: Identify the major muscles of the body Identify the action of major muscles of the body
 Muscular System Student Learning Objectives: Identify the major muscles of the body Identify the action of major muscles of the body Structures to be identified: Muscle actions: Extension Flexion Abduction
Muscular System Student Learning Objectives: Identify the major muscles of the body Identify the action of major muscles of the body Structures to be identified: Muscle actions: Extension Flexion Abduction
SPINE. Postural Malalignments 4/9/2015. Cervical Spine Evaluation. Thoracic Spine Evaluation. Observations. Assess position of head and neck
 SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
ADVANCEMENTS IN PLANTAR FASCIA SURGERY
 C H A P T E R 3 3 ADVANCEMENTS IN PLANTAR FASCIA SURGERY James L. Bouchard, DPM Andrea Cass, DPM INTRODUCTION It has been estimated that 90% of patients with plantar fasciitis and heel spur syndrome get
C H A P T E R 3 3 ADVANCEMENTS IN PLANTAR FASCIA SURGERY James L. Bouchard, DPM Andrea Cass, DPM INTRODUCTION It has been estimated that 90% of patients with plantar fasciitis and heel spur syndrome get
PRACTICE GUIDELINE TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL
 PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
The Pilates Studio of Los Angeles / PilatesCertificationOnline.com
 Anatomy Review Part I Anatomical Terminology and Review Questions (through pg. 80) Define the following: 1. Sagittal Plane 2. Frontal or Coronal Plane 3. Horizontal Plane 4. Superior 5. Inferior 6. Anterior
Anatomy Review Part I Anatomical Terminology and Review Questions (through pg. 80) Define the following: 1. Sagittal Plane 2. Frontal or Coronal Plane 3. Horizontal Plane 4. Superior 5. Inferior 6. Anterior
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Product overview and surgical technique
 Product overview and surgical technique Overview Every patient moves differently 1 and their total hip replacement should be optimised to account for this. The orientation of the acetabular cup is one
Product overview and surgical technique Overview Every patient moves differently 1 and their total hip replacement should be optimised to account for this. The orientation of the acetabular cup is one
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011
 Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
.org. Clavicle Fracture (Broken Collarbone) Anatomy. Description. Cause. Symptoms
 Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds
 Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Surgical dislocation of the hip for reduction of acetabular fracture and evaluation of chondral damage
 Journal of Orthopaedic Surgery 2014;22(1):18-23 Surgical dislocation of the hip for reduction of acetabular fracture and evaluation of chondral damage Lalit Maini, Sahil Batra, Sumit Arora, Shailendra
Journal of Orthopaedic Surgery 2014;22(1):18-23 Surgical dislocation of the hip for reduction of acetabular fracture and evaluation of chondral damage Lalit Maini, Sahil Batra, Sumit Arora, Shailendra
Diagnostic MSK Case Submission Requirements
 Diagnostic MSK Case Submission Requirements Note: MSK Ultrasound-Guided Interventional Procedures (USGIP) is considered a separate specialty. Corresponds with 4/21/16 Accred Newsletter* From the main site:
Diagnostic MSK Case Submission Requirements Note: MSK Ultrasound-Guided Interventional Procedures (USGIP) is considered a separate specialty. Corresponds with 4/21/16 Accred Newsletter* From the main site:
