Percutaneous lumbar and thoracic pedicle screws: a trauma experience 1
|
|
|
- Regina Simpson
- 7 years ago
- Views:
Transcription
1 Percutaneous lumbar and thoracic pedicle screws: a trauma experience 1 Authors: Daniel K. Park MD 1, Anil Thomas MD 2, Selvon St. Clair, MD PhD 3, Maneesh Bawa, MD 4 Affiliations: 1 Attending Spine Surgeon William Beaumont Hospital Royal Oak, MI 2 Resident Emory University Atlanta, GA 3 Attending Spine Surgeon Orthopaedic Institute of Ohio Lima, OH 4 Attending Spine Surgeon San Diego, CA Corresponding-Author: Daniel K. Park, MD danparkmd@gmail.com 1 This study has been given approval by the Emory University IRB
2 Introduction Minimally invasive spine surgical techniques have been growing in popularity. A critical component of the armamentarium is percutaneous pedicle screw instrumentation into the spine. Regardless of technique, pedicle screw fixation has allowed for more stable constructs, earlier mobilization, and better deformity correction through the use of three column spinal fixation. However, with usage of minimal invasive percutaneous techniques, pedicle screws can be placed in the spine without the traditional large posterior skin incisions, extensive striping and retraction of the paraspinal musculature, significant postoperative pain, and long recovery times 4. Standard exposure has also been shown to cause muscle denervation, increased intramuscular pressure, ischemia, and revascularization injury 4,20. The end results of the collateral soft tissue damage are paraspinal muscle atrophy, scarring, and decreased strength and endurance. Percutaneous fixation is not without its attendant disadvantages. This minimal technique requires use of fluoroscopy or various types of specialized radiological guidance. Furthermore, because percutaneous techniques do not allow gross visualization and tactile feel, the technique is very demanding and the incidence of erroneous placement of pedicle screws may be high. Even in traditional open techniques the rate of screw misplacement has been as high as 40%, but only 5.7% severe medial penetrations 2. Erroneous placement, particularly medial and inferior, can lead to neurological deficits since the nerve root passes medial and inferior to the pedicle. Lateral malposition on the other hand can affect stability and can cause loosening of the fixation. Previous cadaveric study has reported an overall perforation rate of 10% using percutaneous techniques 21. Using CT imaging to verify placement, the same authors found a rate of 6.6% (mainly affecting S1 level) in another study 22. A wide range of pedicle malpositioning exists in the literature primarily due to variation in assessment methods including the definition of
3 misplacement. To minimize these malpositions, various surgical techniques have been developed for safe percutaneous placement of pedicle screws which require modification of implants or the need for additional or customized instruments and navigation. Despite its wide use in traditional degenerative spine conditions, percutaneous screw fixation in trauma is novel 1,10,11,15,19,23. Furthermore, the purported benefits of minimally invasive surgery stated previously may be even more advantageous in the trauma setting as Verlann et al found trauma patients may be more susceptible to increased operative blood loss and infection. Therefore incorporating minimally invasive techniques would ultimately, minimize morbidity in patients with multitrauma. The first aim of the present study is to define/describe a technique of placing percutanous screw fixation with only 2D fluoroscopy in trauma patients and verify its the clinical accuracy. The second aim of the study is to validate the technique by a morphometric study of the spine in patients without spinal fracture. Methods Patients who underwent percutaneous pedicle screw placement by one surgeon (MB) at a Level I trauma center were included in this study for clinical review. Exclusion criteria included patients who did not have a postoperative computerized tomography (CT) scan to review the accuracy of pedicle screw placement. Inclusion criteria included patients who underwent percutaneous pedicle screw placement with at least 3 month follow-up and with pre and postoperative CT scan available for review. Surgical Technique
4 Patients were placed in the prone position on the Jackson table in the standard fashion. Fluoroscopy was used to confirm and mark the midline on the skin. C-arm again was used to locate the position of the pedicles once each level s endplates were parallel to the image intensifier s beam. A Jamshidi needle was then advanced through skin at the 3 o clock or 9 o clock position at each pedicle to be included in the instrumentation. The Jamshidi needles were docked such that they were in the lateral halves of each pedicle. The Jamshidi needles were slightly placed into the pedicle to stabilize the position. Then using only an AP image, guidewires were placed 20 mm into the pedicle making sure that the wire tip was lateral to the medial border of the pedicle on the AP image Figure 1a. Once all guidewires were placed on the AP image, a lateral image was then obtained to verify the sagittal alignment figure 1b. Any adjustments were then made then utilizing the lateral view. The appropriate screw length was then determined Figure 1c. Pedicle strew instrumentation was either the Depuy Viper 2 (Depuy Orthopaedics, Warsaw, IN) or Stryker MANTIS (Stryker, Kalamazoo, MI) minimally invasive systems. In situations requiring fusion, decortications and grafting with autologous cancellous graft chips and with bone morphogenetic protein was accomplished in the facet joints through the percutaneous pedicle screw skin incision. Postoperatively, CT scans of instrumented levels were obtained to evaluate screw placement. Grading of CT Accuracy of pedicle screw placement was as follows: grade I when the screw is within the pedicle, II if less than 2 mm is outside the pedicle, III if 2-4 mm is outside the pedicle, and IV > 4 mm is outside the pedicle. Screw positioning was assessed in axial, sagittal, and coronal
5 images to assess if breaches occurred medially, laterally, inferiorly, or superiorly. Three orthopedic surgeons assessed the grading of the screw. Final grading was assigned when at least two of the three graders had agreement. Any major postoperative complications were recorded. Reoperations were also recorded. Morphometric Study Forty consecutive patients who received standard CT scans of the spine (thoracic and lumbar) as part of the standard trauma protocol at a level 1 hospital were reviewed. Inclusion criteria were ages of years old to minimize abnormal measurements due to facet arthropathy and no spinal fractures. Pedicle length was defined as the length of the pedicle at mid axis of the pedicle in both the cephalad-caudad and medial-lateral dimension. In this mid axis point, the length from the dorsal cortex to the junction of the pedicle and the posterior vertebral body was measured. Using Philips isite PACS Suite (Koninklijke Philips Electronics; Amsterdam, Netherlands) for multiplanar reconstruction of CTs, mid-axis pedicle lengths were measured in the axial, coronal, and sagittal planes. Figure 2 demonstrates the usage of multiplanar reconstruction for accurate measurement of pedicle lengths. Two reviewers measured the length of the pedicle. Inter-observer reliability of the values obtained for the morphometric portion of the study was determined with Pearson correlation coefficient. Least squares of the mean were applied to pedicle lengths for the morphometric portion of the study to assess if the pedicle lengths across the thoracic and lumbar spine were different. Results Clinical analysis
6 Overall, 26 patients that had undergone percutaneous spinal instrumentation were included in the clinical review portion of this study. Age distribution of this group ranged from 20 to 69 years old. Mechanisms of injury were predominately motor vehicle accidents, but also included fractures due to falls from heights and insufficiency fractures. A total of 172 pedicle screws were placed. Of these, there were 20 grade II (less than 2mm) medial perforations (11.6%). There were two grade III (2-4mm) medial perforations (1.2%), and no grade IV (>4mm) medial perforations. There were five grade II lateral perforations (2.9%), one grade III lateral perforation (0.6%) and two grade IV lateral perforations (1.2%). There was also one grade II inferior perforation (0.6%). Overall there were 31 grade II-IV perforations (18.0%), with only five (2.9%) being significant perforations (grade III or IV). (Figures 3-5) Levels were also subdivided into thoracic, thoracolumbar, and lower lumbar segments. The thoracic level (T1-T9) had a perforation rate about 28% (14 of 50 screws). The thoracolumbar levels (T10-L2) had a perforation rate of about 16.9% (14 of 83 screws). The lower lumbar levels (L3-L5) had a perforation rate of 10% (3 of 30 screws). The sacroiliac levels had no perforations. In terms of inter-observer reliability, the majority of screws (156 screws) had complete agreement (90.7%), and no screw had complete disagreement. Of the 26 patients that underwent percutaneous posterior spinal fusion, there were no cases of postoperative infections. No patient reported new onset postoperative weakness, paresthesias, or any other new neurological deficits on follow up visits. Three patients required subsequent hardware removal. One patient following a L4-ilium fixation for a comminuted sacral fracture required removal of instrumentation once healed due to loosening of the rods out of the pedicle screw tulip. Another patient who underwent instrumentation at L1-S1 with a L1-3 fusion required removal of hardware once healed due to loosening of the distal L5 and S1 pedicle
7 screws. The third patient underwent removal of T7-12 posterior instrumentation after his thoracic level injuries showed adequate healing. Morphometric analysis The morphometric analysis of pedicle lengths of 40 patients from T1-L5 levels reveals a range of pedicle length from 14mm to 22mm, with the smaller values in the upper thoracic levels. The pedicles in the thoracolumbar junction were the longest as the pedicle length decreased at lower lumbar levels (Figure 6). There was no statistical difference between right and left pedicles at each level (Table 1) (p>0.2). The pedicle lengths were not significant for T2 compared to T3; T4 to T5; T5 to T6, 8, 9; T6 to T7, 8, 9, 10, L5; T7 to T8, 9, 10, L5; T8 to T9, 10, L5; T9 to T10, L5; T10 to L5; T12 to L3; L1 to L2; L2 to L3. The other pairings were statistically significant using the least squares of the means (Table 2). The inter-observer reliability was high (r=0.96). Discussion Various studies have demonstrated the feasibility of percutaneous pedicle screw instrumentation. Each study utilizes a slightly different technique or instrumentation such as fluoroscopic navigation 13, CT navigation 6, or robotics 12. Few published reports rely solely on fluoroscopy. This study is one of the largest published studies on use of percutaneous screw fixation using only fluoroscopy especially in the setting of trauma. Furthermore, the morphometric study analyzing the length of the pedicle confirms and validates the technique. In this study, 172 screws were placed in 26 patients. The rate of cortical breach was 18.0%, but only 2.9% were greater than grade II breach. Therefore, our rate compares favorably to the previous literature utilizing only fluoroscopy as well as to screws placed via navigation.
8 Furthermore, we utilized CT scans to assess cortical breaches which is much more accurate compared to conventional radiographs 7. We also evaluated medial/lateral perforations and cephalad/caudal perforations. If one considers potential dangerous breaches as malpositions greater than grade II breaches, our success rate was 97.2%. Grade II and less is considered safe in many instances because CT has artifact from metal; 1 to 2 mm of error may occur due to artifact 13. Furthermore, frank perforations of the cortex do not correlate with neurological damage. Lien et al showed the distance between the pedicle wall and nerve root vary, but usually 2.4 mm of space is present 9. We believe our rate of perforation is low due to the tenet that as long as the guide-wire remains lateral to the border of the medial wall of the pedicle throughout the length of the pedicle, the trajectory should be safe. The distance necessary to trespass the pedicle is confirmed via the morphometric study, which demonstrated the pedicle length to range from 14.4 to 22.1 mm. The longest being at L1-2 and the shortest in the upper thoracic spine. Because of this fact, a short length may suffice in the upper thoracic spine. We believe this is the one of the first study analyzing the lengths of the pedicles in the general population. The only other published finding is by Li et al who found pedicle length to range from 18 to 25 mm on CT scan in 41 Chinese patients 8. Because of our low breach rate, we did not have any patients who had to be revised due to screw malpositioning. Two complications related to hardware however did arise. In one patient, the rods had slipped out of the pedicle screw tulips at the most cephalad level postoperatively. Patient remains asymptomatic however. In another patient, there was evidence of screw loosening prior to hardware removal at the cephalad level. This patient however underwent a fusion at L3-S1 and only instrumentation at L1-3. In addition, one patient
9 underwent a concomitant miniopen exposure to help reduce a T11-T12 fracture dislocation. The miniopen approach was not used for screw insertion however. Overall, no neurological complications occurred. There are previous studies in the literature that have relied solely on fluoroscopy. Schizas reported 60 screws in 15 patients using fluoroscopy only and found 80% of patients with some perforation while an overall rate of screw perforation of 23%. Only one patient needed revision due to screw placement. There was no association of breached pedicles with the specific spinal level instrumented 16. In this technique, surgeons placed guide wires until the K wire reached the posterior vertebral wall level on the lateral fluoroscopic image. The exact distance was not measured. In another study, re-operation rate due to screw misplacement, presumably with neurological symptoms was 4% 17. Another larger study using fluoroscopy found in 104 patients (115 pedicle screws), the postoperative CT scans demonstrated 87% good screw placement, 10% acceptable, 11 revisions necessary (9 for screw placement and 2 for loosening bolts), and 2 patients with new radicular pain because of screw placement. Screw was rated good if < 2 mm of violation, acceptable > 2 mm but still sufficient bone purchase, and unacceptable if >2 mm and poor bone purchase or new screw associated symptoms 14. Another technique using fluoroscopic guidance found overall misplacement ranging from 8-13% depending on the traditional Magerl technique or a modified version technique. Thirty of 37 violations were less than 3.0 mm 21. Previously, a similar technique used by the senior author has been described with good clinical outcomes however a radiological evaluation of screw placement was not reported 3. Although technology has advanced and there is a trend toward navigation techniques, the advantages of fluoroscopic guidance only is that navigation techniques such as fluoro-navigation require lengthy set up time while CT-dependent navigation utilize pre-procedure CT which may
10 differ after decompression or positioning on bed. In addition, CT based navigation is surgeon dependent; it requires the surgeon to register landmarks on preoperative CT with corresponding anatomy intraoperatively. The advantage of navigation however is potential decreased screw malpositioning. In FluoroNav (2D virtual navigation), 161 screws were placed, 83.8% where grade II or less 13. CT navigation depends on preoperatively obtained data to provide 3-D views intraoperative. Kosmopoulos and Schizas found in a meta-analysis of 130 studies, 96.1% accuracy in navigated group compared to 79% in non navigation 5. We believe this report differs from the others for multiple reasons. This technique relies only on the AP image for the majority of the case and utilizes the lateral image as a confirmatory image. Second, this study is a report on use in the trauma setting. Third, a morphogenetic study is included to justify the amount of guide wire that is inserted before checking a lateral image. Last, clinical data is presented for 172 screws placed in 26 patients. Disadvantages of this study mainly reside in the follow-up. Long-term follow is incomplete in this study cohort. Because of the trauma setting, patient follow up is unpredictably difficult. It would be interesting to see whether there are other instrumentation related complications such as loosening. Notably, the major complications associated with neurologic compromise or instrumentation catastrophes are unlikely after the immediate postoperative state. Lastly, the ideal evaluation of screw accuracy may be best evaluated doing CT scans after pedicle screw removal to eliminate artifact from the instrumentation. In summary, this paper reports a comprehensive overview of a technique utilizing only fluoroscopic guidance for the placement of pedicle screws percutaneously. The applicability in
11 the spinal trauma patients is viable while the rate of cortical breaches compares favorably with the published literature. Additionally, morphometric studies validate the technique. Reference 1. Beringer W, Potts E, Khairi S, et al. Percutaneous pedicle screw instrumentation for temporary internal bracing of nondisplaced bony Chance fractures. J Spinal Disord Tech 2007;20: Castro WH, Halm H, Jerosch J, et al. Accuracy of pedicle screw placement in lumbar vertebrae. Spine (Phila Pa 1976) 1996;21: Harris EB, Massey P, Lawrence J, et al. Percutaneous techniques for minimally invasive posterior lumbar fusion. Neurosurg Focus 2008;25:E Kim DY, Lee SH, Chung SK, et al. Comparison of multifidus muscle atrophy and trunk extension muscle strength: percutaneous versus open pedicle screw fixation. Spine (Phila Pa 1976) 2005;30: Kosmopoulos V, Schizas C. Pedicle screw placement accuracy: a meta-analysis. Spine (Phila Pa 1976) 2007;32:E Laine T, Lund T, Ylikoski M, et al. Accuracy of pedicle screw insertion with and without computer assistance: a randomised controlled clinical study in 100 consecutive patients. Eur Spine J 2000;9: Learch TJ, Massie JB, Pathria MN, et al. Assessment of pedicle screw placement utilizing conventional radiography and computed tomography: a proposed systematic approach to improve accuracy of interpretation. Spine (Phila Pa 1976) 2004;29: Li B, Jiang B, Fu Z, et al. Accurate determination of isthmus of lumbar pedicle: a morphometric study using reformatted computed tomographic images. Spine (Phila Pa 1976) 2004;29: Lien SB, Liou NH, Wu SS. Analysis of anatomic morphometry of the pedicles and the safe zone for through-pedicle procedures in the thoracic and lumbar spine. Eur Spine J 2007;16: Logroscino CA, Proietti L, Tamburrelli FC. Minimally invasive spine stabilisation with long implants. Eur Spine J 2009;18 Suppl 1: Palmisani M, Gasbarrini A, Brodano GB, et al. Minimally invasive percutaneous fixation in the treatment of thoracic and lumbar spine fractures. Eur Spine J 2009;18 Suppl 1: Pechlivanis I, Kiriyanthan G, Engelhardt M, et al. Percutaneous placement of pedicle screws in the lumbar spine using a bone mounted miniature robotic system: first experiences and accuracy of screw placement. Spine (Phila Pa 1976) 2009;34: Ravi B, Zahrai A, Rampersaud R. Clinical accuracy of computer-assisted twodimensional fluoroscopy for the percutaneous placement of lumbosacral pedicle screws. Spine (Phila Pa 1976) 2011;36: Ringel F, Stoffel M, Stuer C, et al. Minimally invasive transmuscular pedicle screw fixation of the thoracic and lumbar spine. Neurosurgery 2006;59:ONS361-6; discussion ONS6-7.
12 15. Schizas C, Kosmopoulos V. Percutaneous surgical treatment of chance fractures using cannulated pedicle screws. Report of two cases. J Neurosurg Spine 2007;7: Schizas C, Michel J, Kosmopoulos V, et al. Computer tomography assessment of pedicle screw insertion in percutaneous posterior transpedicular stabilization. Eur Spine J 2007;16: Schwender JD, Holly LT, Rouben DP, et al. Minimally invasive transforaminal lumbar interbody fusion (TLIF): technical feasibility and initial results. J Spinal Disord Tech 2005;18 Suppl:S Verlaan JJ, Diekerhof CH, Buskens E, et al. Surgical treatment of traumatic fractures of the thoracic and lumbar spine: a systematic review of the literature on techniques, complications, and outcome. Spine (Phila Pa 1976) 2004;29: Wang MY, Ludwig SC, Anderson DG, et al. Percutaneous iliac screw placement: description of a new minimally invasive technique. Neurosurg Focus 2008;25:E Weber BR, Grob D, Dvorak J, et al. Posterior surgical approach to the lumbar spine and its effect on the multifidus muscle. Spine (Phila Pa 1976) 1997;22: Wiesner L, Kothe R, Ruther W. Anatomic evaluation of two different techniques for the percutaneous insertion of pedicle screws in the lumbar spine. Spine (Phila Pa 1976) 1999;24: Wiesner L, Kothe R, Schulitz KP, et al. Clinical evaluation and computed tomography scan analysis of screw tracts after percutaneous insertion of pedicle screws in the lumbar spine. Spine (Phila Pa 1976) 2000;25: Wild MH, Glees M, Plieschnegger C, et al. Five-year follow-up examination after purely minimally invasive posterior stabilization of thoracolumbar fractures: a comparison of minimally invasive percutaneously and conventionally open treated patients. Arch Orthop Trauma Surg 2007;127:
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
The goals of modern spinal surgery are to maximize
 SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
-Increases the safety, accuracy and efficiency of certain spine procedures
 Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Value Analysis Brief MIS Lateral Approach to Interbody Fusion
 Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Robotics. Neil Badlani MD, MBA The Orthopedic Sports Clinic Nobilis Health Corp. Houston, TX. The Orthopedic Sports Clinic
 Robotics Neil Badlani MD, MBA The Orthopedic Sports Clinic Nobilis Health Corp. Houston, TX The Orthopedic Sports Clinic Disclosure Consulting/Speaking Medtronic Amendia Nutech Mazor * MIS Device Outline
Robotics Neil Badlani MD, MBA The Orthopedic Sports Clinic Nobilis Health Corp. Houston, TX The Orthopedic Sports Clinic Disclosure Consulting/Speaking Medtronic Amendia Nutech Mazor * MIS Device Outline
A MORPHOMETRIC STUDY OF THE PEDICLES IN DRY HUMAN TYPICAL THORACIC VERTEBRAE
 IJCRR Research Article A MORPHOMETRIC STUDY OF THE PEDICLES IN DRY HUMAN TYPICAL THORACIC VERTEBRAE Dhaval K. Patil, Pritha S. Bhuiyan Department of Anatomy, Seth G S Medical College, Parel, Mumbai-12,
IJCRR Research Article A MORPHOMETRIC STUDY OF THE PEDICLES IN DRY HUMAN TYPICAL THORACIC VERTEBRAE Dhaval K. Patil, Pritha S. Bhuiyan Department of Anatomy, Seth G S Medical College, Parel, Mumbai-12,
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Abstract. Introduction. Case Report. imedpub Journals http://www.imedpub.com/
 Case Report imedpub Journals http://www.imedpub.com/ Unusual 2-Stages Posterior Approach Surgical Treatment for Complete Fracture Dislocation of the Upper Thoracic Spine without Neurologic Deficit: A Case
Case Report imedpub Journals http://www.imedpub.com/ Unusual 2-Stages Posterior Approach Surgical Treatment for Complete Fracture Dislocation of the Upper Thoracic Spine without Neurologic Deficit: A Case
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
HOW TO CITE THIS ARTICLE:
 POST TRAUMATIC INSTABILITY OF SUB-AXIAL CERVICAL SPINE - REDUCTION AND INTERNAL FIXATION BY LATERAL MASS SCREWS A LONG TERM FOLLOW-UP STUDY Godagu Bhaskar 1, Ambarapu Mastan Reddy 2, Akyam Lakshman Rao
POST TRAUMATIC INSTABILITY OF SUB-AXIAL CERVICAL SPINE - REDUCTION AND INTERNAL FIXATION BY LATERAL MASS SCREWS A LONG TERM FOLLOW-UP STUDY Godagu Bhaskar 1, Ambarapu Mastan Reddy 2, Akyam Lakshman Rao
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013
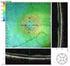 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
R/F. Applications and Present Issues of Tomosynthesis in Spine Surgery. 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4
 R/F Applications and Present Issues of Tomosynthesis in Spine Surgery 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4 Professor and Chairman Department of Orthopaedic Surgery
R/F Applications and Present Issues of Tomosynthesis in Spine Surgery 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4 Professor and Chairman Department of Orthopaedic Surgery
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
MINIMAL ACCESS SPINE SURGERY
 MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Planning and Achieving Lumbar Spinal Balance
 Planning and Achieving Lumbar Spinal Balance December 12, 2014 New York, NY W New York Hotel Course Chairmen: Dom Coric, MD Paul C. McAfee, MD, MBA Course Dom Coric, MD Co-Chairman Paul C. McAfee, MD,
Planning and Achieving Lumbar Spinal Balance December 12, 2014 New York, NY W New York Hotel Course Chairmen: Dom Coric, MD Paul C. McAfee, MD, MBA Course Dom Coric, MD Co-Chairman Paul C. McAfee, MD,
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Biomechanics of the Lumbar Spine
 Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Hybrid Technique for Posterior Lumbar Interbody Fusion: A Combination of Open Decompression and Percutaneous Pedicle Screw Fixation
 135 2013 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd SURGICAL TECHNIQUE Hybrid Technique for Posterior Lumbar Interbody Fusion: A Combination of Open Decompression and Percutaneous
135 2013 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd SURGICAL TECHNIQUE Hybrid Technique for Posterior Lumbar Interbody Fusion: A Combination of Open Decompression and Percutaneous
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Planning and Achieving Lumbar Spinal Balance. November 7, 2015 New York, NY. Course Chairmen: Dom Coric, MD Paul McAfee, MD, MBA EW YORK
 Planning and Achieving Lumbar Spinal Balance November 7, 2015 New York, NY Course Chairmen: Dom Coric, MD Paul McAfee, MD, MBA EW YORK Course Dom Coric, MD Co-Chairman Paul McAfee, MD, MBA Co-Chairman
Planning and Achieving Lumbar Spinal Balance November 7, 2015 New York, NY Course Chairmen: Dom Coric, MD Paul McAfee, MD, MBA EW YORK Course Dom Coric, MD Co-Chairman Paul McAfee, MD, MBA Co-Chairman
(Dynamic Surgical Guidance) Hear what you cannot see. Challenges in pedicle screw placement. Pedicle screw misplacement
 Innovation in Spine Surgery Safety DSG TM Technology (Dynamic Surgical Guidance) Hear what you cannot see Accuracy of pedicle screw placement remains a critical issue in spine surgery. A number of patients
Innovation in Spine Surgery Safety DSG TM Technology (Dynamic Surgical Guidance) Hear what you cannot see Accuracy of pedicle screw placement remains a critical issue in spine surgery. A number of patients
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
SALVATION. Fusion Bolts and Beams SURGICAL TECHNIQUE
 SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults
 Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
(Dynamic Surgical Guidance) Hear what you cannot see. Challenges in pedicle screw placement. Pedicle screw misplacement
 Innovation in Spine Surgery Safety DSG TM Technology (Dynamic Surgical Guidance) Hear what you cannot see Accuracy of pedicle screw placement remains a critical issue in spine surgery. A number of patients
Innovation in Spine Surgery Safety DSG TM Technology (Dynamic Surgical Guidance) Hear what you cannot see Accuracy of pedicle screw placement remains a critical issue in spine surgery. A number of patients
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY
 ORIGINAL RESEARCH ARTICLE http://www.eternalpublication.com InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY IJAPB: Volume: 1; Issue: 1; October 2014 ISSN(Online):2394-3440 A Morphometric Study
ORIGINAL RESEARCH ARTICLE http://www.eternalpublication.com InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY IJAPB: Volume: 1; Issue: 1; October 2014 ISSN(Online):2394-3440 A Morphometric Study
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
PAUL PARK, M.D., 1 AND KEVIN T. FOLEY, M.D. 2. Methods
 Neurosurg Focus 25 (2):E16, 2008 Minimally invasive transforaminal lumbar interbody fusion with reduction of spondylolisthesis: technique and outcomes after a minimum of 2 years follow-up PAUL PARK, M.D.,
Neurosurg Focus 25 (2):E16, 2008 Minimally invasive transforaminal lumbar interbody fusion with reduction of spondylolisthesis: technique and outcomes after a minimum of 2 years follow-up PAUL PARK, M.D.,
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach
 Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
2013 North American SSL Certificate
 2013 2014 INSERT COMPANY LOGO HERE 2014 North American 2013 North American SSL Certificate Minimally Invasive Spinal Surgical Solutions Product Product Line Leadership Strategy Leadership Award Award Background
2013 2014 INSERT COMPANY LOGO HERE 2014 North American 2013 North American SSL Certificate Minimally Invasive Spinal Surgical Solutions Product Product Line Leadership Strategy Leadership Award Award Background
The field of spinal surgery has advanced. Spinal Robotics: Current Applications and Future Perspectives SUPERVISORY-CONTROLLED SYSTEMS TOPIC
 TOPIC SUPERVISORY-CONTROLLED SYSTEMS SUPERVISORY-CONTROLLED SYSTEMS Spinal Robotics: Current Applications and Future Perspectives Florian Roser, MD, PhD Marcos Tatagiba, MD, PhD Gottlieb Maier, MD From
TOPIC SUPERVISORY-CONTROLLED SYSTEMS SUPERVISORY-CONTROLLED SYSTEMS Spinal Robotics: Current Applications and Future Perspectives Florian Roser, MD, PhD Marcos Tatagiba, MD, PhD Gottlieb Maier, MD From
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Compression Fractures
 September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
Objectives. Spinal Fractures: Classification Diagnosis and Treatment. Level of Fracture. Neuro exam Muscle Grading
 Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Vivian Gonzalez Gillian Lieberman, MD. January 2002. Lumbar Spine Trauma. Vivian Gonzalez, Harvard Medical School Year III Gillian Lieberman, MD
 January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
Imaging of Lisfranc Injury
 November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular bone grafting
 Eur Spine J (2002) 11 :435 440 DOI 10.1007/s00586-002-0390-1 ORIGINAL ARTICLE A. Kaminski E. J. Müller G. Muhr Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular
Eur Spine J (2002) 11 :435 440 DOI 10.1007/s00586-002-0390-1 ORIGINAL ARTICLE A. Kaminski E. J. Müller G. Muhr Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular
Cervical Spine Imaging
 March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
APSS YANGON OPERATIVE SPINE COURSE. Local Organizing Chairman: Prof Myint Thaung. Venue: Yangon Orthopaedic Hospital
 5 th - 8 th Feb 2015 Pls insert Hospital Logo here Local Organizing Chairman: Prof Myint Thaung Venue: Yangon Orthopaedic Hospital Invited International and Local Faculties Arvind Jayaswal (India) Chung-Chek
5 th - 8 th Feb 2015 Pls insert Hospital Logo here Local Organizing Chairman: Prof Myint Thaung Venue: Yangon Orthopaedic Hospital Invited International and Local Faculties Arvind Jayaswal (India) Chung-Chek
Thoracolumbar Spine Fractures. Outline. Outline. Holmes Criteria. Disclosure:
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
(English) NEXUS SPINE SPACER SYSTEM
 (English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
(English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
coligne treatment technology
 coligne treatment technology coligne a strategy in spine Leadership begins before the patient enters the surgical theater, among the spine care professionals forming the coalliance. This may be a small
coligne treatment technology coligne a strategy in spine Leadership begins before the patient enters the surgical theater, among the spine care professionals forming the coalliance. This may be a small
ICD-10-PCS Documentation and Coding for Spinal Procedures October 22, 2015
 Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Her past medical history was non significant. She never had surgery, had no history or family history of cancer and was a nonsmoker.
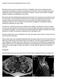 Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
TABLE OF CONTENTS. Indications and Contraindications 3. Features and Benefits 4. Ease of connection 4 Stable fixation concept 5
 Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS
 ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
BODY BODY PEDICLE PEDICLE TRANSVERSE TRANSVERSE PROCESS PROCESS
 Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
DRAFT. EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques. Leiden The Netherlands 5 November 8 November 2012
 EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques DRAFT Leiden The Netherlands 5 November 8 November 2012 Provisional Course Programme Monday 5 th November Trauma
EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques DRAFT Leiden The Netherlands 5 November 8 November 2012 Provisional Course Programme Monday 5 th November Trauma
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. CP57 Version: V3
 GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
Spinal fusion for degenerative disease of the lumbar
 ORIGINAL ARTICLE Minimally Invasive Lumbar Transfacet Screw Fixation in the Lateral Decubitus Position After Extreme Lateral Interbody Fusion A Technique and Feasibility Study Jean-Marc Voyadzis, MD and
ORIGINAL ARTICLE Minimally Invasive Lumbar Transfacet Screw Fixation in the Lateral Decubitus Position After Extreme Lateral Interbody Fusion A Technique and Feasibility Study Jean-Marc Voyadzis, MD and
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated And Fenestrated Pedicle
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Simplified surgery. Personalized performance.
 Simplified surgery. Personalized performance. VISIONAIRE Patient Matched Technology Accuracy Advanced surgical precision, resulting in reproducible outcomes Efficiency Simplifying surgery, reducing costs,
Simplified surgery. Personalized performance. VISIONAIRE Patient Matched Technology Accuracy Advanced surgical precision, resulting in reproducible outcomes Efficiency Simplifying surgery, reducing costs,
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Instability concept. Symposium- Cervical Spine. Barcelona, February 2014
 Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Titanium Wire with Barb and Needle. For canthal tendon procedures.
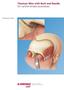 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
CURRCULUM VITAE. 1. PERSONAL DATA Citizenship Status: Citizen, Republic of Korea
 CURRCULUM VITAE NAME: JUN-YEONG SEO, M.D. AFFILIATION: Jeju National University Hospital MOBILE: +82 10 3384 2267 E-MAIL: jys@jejunu.ac.kr FAX: +82 64 717 1131 1. PERSONAL DATA Citizenship Status: Citizen,
CURRCULUM VITAE NAME: JUN-YEONG SEO, M.D. AFFILIATION: Jeju National University Hospital MOBILE: +82 10 3384 2267 E-MAIL: jys@jejunu.ac.kr FAX: +82 64 717 1131 1. PERSONAL DATA Citizenship Status: Citizen,
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Case Report Reconstructive Osteotomy for Ankle Malunion Improves Patient Satisfaction and Function
 Case Reports in Orthopedics Volume 2015, Article ID 549109, 5 pages http://dx.doi.org/10.1155/2015/549109 Case Report Reconstructive Osteotomy for Ankle Malunion Improves Patient Satisfaction and Function
Case Reports in Orthopedics Volume 2015, Article ID 549109, 5 pages http://dx.doi.org/10.1155/2015/549109 Case Report Reconstructive Osteotomy for Ankle Malunion Improves Patient Satisfaction and Function
Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic Procedures
 Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: computer_assisted_surgical_navigational_orthopedic_procedures
Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: computer_assisted_surgical_navigational_orthopedic_procedures
Orthopaedic Approach to Back Pain. Seth Cheatham, MD
 Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Spinal Fractures Classification System
 Spinal Fractures Classification System an AOSpine Knowledge Forum initiative Cervical Spine Fractures Thoracolumbar Spine Fractures Sacral Spine Fractures AOSpine the leading global academic community
Spinal Fractures Classification System an AOSpine Knowledge Forum initiative Cervical Spine Fractures Thoracolumbar Spine Fractures Sacral Spine Fractures AOSpine the leading global academic community
