The Long Journey to Interatrial Block Discovery
|
|
|
- Joy Cole
- 8 years ago
- Views:
Transcription
1 The Long Journey to Interatrial Block Discovery A. Bayés de Luna Fundació Investigació Cardiovascular, ICCC, Barcelona, Spain 1. Introduction To begin, I feel it is important to point out that before our publications on interatrial block starting in the mid-1970s, a number of papers had already discussed, with isolated cases or short series, different aspects of so-called blocks at atrial levels and specifically of interatrial or intraatrial block (IAB) [1-8], that is the topic that we will comment in this paper. Although there is some discrepancy in different papers [1-4] about the significance of the concept of interatrial or intraatrial block, usually this represents an impaired propagation of the stimulus between two portions of the atria, with enlarged P waves greater than or equal to ms, and normally accompanied by left atrial enlargement. In a few articles [5-8] written in Latin languages, also was considered that if the stimulus was completely blocked at the upper part of the Bachmann zone, the activation of the left atrium would take place retrogradely, originating a long P wave ( 120ms) together with a ± morphology in II, III and VF. However, there are many aspects that are not well explained or discussed in these publications, as outlined below. 1. In no publication did it state that these ECG patterns of interatrial (intraatrial) block (IAB) are in fact a pattern of block based on the presence of the following 3 conditions: a) the pattern may appear suddenly and may be transient, b) the pattern may exist without associated enlargement of involved chambers. In fact, the term left atrial abnormality was coined and widely used to encompass both atrial enlargement and interatrial block [9, 10] and c) the ECG pattern may be reproduced experimentally. 2. Furthermore, no paper discussed at any time any possible clinical implications of these ECG patterns. We, therefore, cannot know if these cases were associated with supraventricular tachyarrhythmias, mortality or other problems. 3. There was no clear definition and classification of block at the atrial level, specifically of interatrial block (IAB) this means block between two atria. There was no mention that IAB may be, as other types of block, of partial (first-degree block), transient (second-degree block) or advanced (third-degree block) types. 4. There were no data about the prevalence of these blocks, and its etiological aspects. 5. There were no clear ECG-VCG criteria for advanced IAB, based on long series of patients. 6. The concept of IAB is not frequently used in cardiology. The P wave still remains The Cinderella of the ECG. In a review of 76 books on ECG in English, Spanish, French and Italian languages, from the beginning of ECG study (Lewis books) to present day, we have only found a clear reference to interatrial block in our books since the first edition [11] and in Piccolo and Oreto s book [12, 13]. For example, Te-Chuan Chou [14] states that in P-wave changes, conduction defects may be present. A less specific term such as atrial abnormality is found in other books. Macfarlane [15], while discussing the concept of intra-atrial block, only defines it following the criteria of WHO/ISFC [16] that corresponds to partial interatrial block (IAB). In terms of general cardiology, the textbook by Braunwald [17] includes all anomalies of P wave under the term atrial abnormalities, which is also the case in the chapter on ECG of the previous editions of the textbook The heart, by Fuster et al [18], except the last edition written by our group. 31
2 2. Our studies on interatrial block Our dedication to the study of blocks at the atrial level, and especially to interatrial blocks (IAB), has been one of our favourite topics throughout the last 40 years. The following is a summary of the most important successive studies performed by our group. Identification and classification of blocks at atrial level We classified blocks at atrial level [19-22] in interatrial and other types of atrial blocks that includes right atrial block and atrial aberrancy. For the remainder of this paper we will focus on interatrial block (IAB). This is the block between the right and left atria in the zone of the Bachmann bundle and may be of first-degree (partial), when the stimulus pass through the Bachmann bundle but with delay the ECG criterion of which is P wave 120ms ( 110 for others); third-degree (advanced), when the stimulus is blocked in the zone of Bachmann bundle, and left atrium is retrogradely conducted to left atrium (RCLA) (Fig.1-3); the ECG criteria of which are P wave 120ms and ± morphology in II, III and VF. Second-degree, IAB is a transient pattern of partial or advanced IAB, a form of atrial aberrancy (Fig.4). Fig. 1. Left: Scheme of atrial activation in a normal case (A), in presence of partial IAB (B), and of IAB with LARA (C). Right: Characteristics of the P loop and P wave in each case. Fig. 2. Left: Characteristics of the P wave in the three bipolar limb leads. Note the existence of an open angle between the vector of the 1 st part and of the 2 nd. Right: Electrophysiological study that demonstrates the retrograde activation of the left atrium. HE: High esophageal lead. HRA: High right atrium. LRA: Low right atrium. In HE the morphology is -+ because the electrode first face the tale of activation and later the head of the vector. The way of activation is HRA-LRA-Second part (positive) in HE. 32
3 Although we published this classification already in the 70 s [19-22] and in all editions of our ECG books published since the mid 1970s, this concept has not become popular. Very recently, we published a consensus paper on IAB under the auspices of ISHNE in the Journal of Electrocardiology [23] and a new edition of my book [30], and we hope this will help to further disseminate all these concepts. Fig. 3. A. Typical morphology of advanced interatrial conduction block and retrograde activation of the left atrium, in sinus rhythm. B. The polarity of the flutter wave indicates that the flutter is an atypical flutter. These patterns may correspond to block. Evidence consisted of the following: a) we found cases of partial and advanced IAB without LAE [21, 22]; b) we found cases of intermittent and progressive partial and advanced IAB [22]; and c) in the 1970s Waldo and others demonstrated that the pattern of advanced IAB may be reproduced experimentally [24] (Fig.5). Definition of ECG-VCG diagnostic criteria In 1976 and 1978 we published, our first abstract and paper on advanced interatrial block (19,20). Later, a larger series was published in 1985 (22) (Figs. 1-3) (Table 1). X X Fig. 4. Two cases of atrial aberrancy. The first one A is a case of second degree interatrial block. This is a case of a patient with basal advanced interatrial block (P± with first part isoelectric that mimics AV junction rhythm) that presents aberrant atrial conduction, ectopically induced by premature atrial complex, with a pattern, in this case, of first degree interatrial block (x). B. A patient with aberrant atrial conduction also ectopically induced by a premature atrial complex. After this premature complex, a transitory P wave with a different morphology, but not with a pattern of first or third interatrial block appear (x). The PR interval is equal to previous PR intervals. Other explanations to this change (atrial escape, artifact, etc.) are unlikely (see Bayés de Luna 2014 [30]). 33
4 Fig. 5. Adapted from experimental Bachmann s bundle block (Waldo et al. 1971). (A) Control P wave recorded in ECG lead II when the atria were paced from the right atrium. See the change of morphology after Bachmann s bundle lesion in the right side. (B) P wave recorded in lead II after the creation of a lesion in the left atrial (LA) portion of Bachmann s bundle (BB). In both cases the changes in conduction time and morphology after block are shown. Fig. 6. Examples of the P loops in presence of advanced IAB. A) Closed loop. B) Open loop with a left final part. C) Open loop with a right final part. Of the ECGs, we collected, 83 cases that fulfilled the criteria of advanced IAB (P ± in II, III and VF with P width 120 ms.). We presented a detailed study of 35 cases with surface ECG and VCG and 29 cases with orthogonal ECG leads (Table I and fig. 2, 3, 6, 7). The results were then compared against 2 control groups: patients with heart disease (30 cases) and those without heart disease (25 cases). The prevalence of advanced IAB was nearly 1% in the global population, and 2% among patients with valvular heart disease. The diagnostic criteria for advanced IAB included (Fig.6, 7 and Table I); 1) ECG: P ± in II, III and VF and P 120 ms, with an open angle (usually >90 ) between the first and second parts of the P wave; 2) orthogonal ECG: P ± in the Y lead with a negative mode > 40 ms; 3) VCG: more than 50 ms above the X or Z axis, duration of the P loop 110 ms, with an open angle between the 2 parts of the P loop in both frontal (131.3 ± 32.3 ) and right saggital planes (171.2 ± 15.1 ), and the presence of notches and slurrings in the last part of the P loop. 34
5 Fig. 7. Direction of the vectors of the first and second parts of the P wave in presence of advanced IAB in the three groups studied. We have found that the pattern of interatrial block, not only may be transient (second degree) (Fig. 4A) but also may appear progressively (Fig. 8). In these papers [22, 23] we had already emphasized that the diagnosis of advanced IAB is not only of academic interest but may also have clinical implications due to the following: a) This is a very specific sign of LAE that is present in 90% of cases. b) In the absence of preventive treatment there is a high incidence of supraventricular paroxysmal arrhythmia (96 %) (flutter and fibrillation) within 1 year. Incidence is 100 % in valvular disease and cardiomyopathic groups. c) Paroxysmal arrhythmia appears to be due to IACD-LARA rather than atrial enlargement; in the control groups of valvular disease and cardiomyopathies with similar LAE the incidence of paroxysmal tachyarrhythmia is much lower (20 % vs 100 %). 35
6 Fig. 8. Progressive interatrial block: P wave patterns in VF from a patient with mitro-aortic valve disease. (A) P wave with normal atrial duration (P = 105ms), (B) An intermediate morphology that corresponds to a first-degree interatrial block (P = 135ms). (C) Advanced interatrial block appearing after 5 years with P ± morphology in II, III, and VF (P = 145ms). Identification of the syndrome [25] We proceeded to study a series of patients with a long-term follow-up to better determine the true incidence of supraventricular arrhythmias in these groups of patients when compared with patients of the same clinical and echocardiographic characteristics. We studied 16 patients with electrocardiographic evidence of advanced IAB and retrograde activation of the left atrium (P 0.12 s and dysphasic (±) P waves in leads II, III and VF). Eight patients had valvular heart disease, 4 had dilated cardiomyopathy and 4 had other forms of heart disease. Patients were compared with a control group of 22 patients with similar clinical and echocardiographic characteristics but who presented partial instead of advanced IAB. Fig. 9. Life table analysis of the probability of remaining free of supraventricular tachyarrhythmias in patients with advanced interatrial block (IAB) and controls. Taken from [26]. Patients with advanced IAB and retrograde activation of the left atrium had a much higher incidence of paroxysmal supraventricular tachyarrhythmias (93.7 %) during follow-up when compared to the control group with partial IAB, (27.7 %) (P < 0.001) (Fig.9). Eleven of the 16 patients (68.7 %) with advanced IAB and retrograde activation of left atrium had atrial flutter (atypical in 7 cases, typical in 2 cases, and with 2 or more morphologies in 2 cases). Six patients from the control group (27.7 %) had sustained atrial tachyarrhythmias (5 with atrial fibrillation and 1 with typical atrial flutter) (Fig.3 and Table II). The atrial tachyarrhythmias were due more to advanced IAB and retrograde activation of the left atrium with frequent atrial extrasystoles than to left atrial enlargement, because the control group of patients with a left atrium of the same size, but with partial IAB instead of advanced IAB and less incidence of atrial extrasystoles, had a much lower incidence of paroxysmal tachycardia. 36
7 Prevention of the syndrome and recurrences [26] Having found a strong relationship between the presence of advanced IAB and the incidence of atrial flutter or atrial fibrillation when compared with a control group (93.7 % vs %), along with a high incidence of an uncommon type of atrial flutter (4), we decided to study the role of preventive antiarrhythmic treatment for this disorder. Fifteen of the 16 consecutive patients we studied, who did not have preventive antiarrhythmic treatment (93.75 %), presented at least 1 crisis of paroxysmal supraventricular tachyarrhythmia requiring emergency treatment over a follow-up of 10 ± 6.1 months. In view of the confirmation of high incidence of paroxysmal supraventricular tachyarrhythmias in this type of patient, and especially in valvular disease and cardiomyopathic patients, we decided to institute preventive antiarrhythmic treatment in subsequent patients. With the use of preventive antiarrhythmic treatment in our 16 subsequent patients, once diagnosed of advanced IAB, the incidence of paroxysmal supraventricular tachyarrhythmia was greatly lowered (25 %) even with longer follow-up (18 ± 10.2 months) (Fig.10). Because of the high risk of embolism in valvular and cardiomyopathic disease, we now consider it advisable to start preventive antiarrhythmic treatment in such patients, prior to the onset of tachyarrhythmia. It is extremely important to corroborate these results in a greater series of patients. We are therefore preparing a larger trial for this purpose. Fig. 10. Follow-up of 32 patients with advanced interatrial block with retrograde activation of left atrium with and without antiarrhythmic treatment 37
8 Table II. Characteristics of the sustained paroxysmal tachyarrhythmias Group with interatrial block (16 patients; 15 with tachyarrhythmia during the follow-up) (93,7%) Atrial flutter Atrial fibrillation Atrial flutter with fibrillation MRV 133 ± 42 beats min -1 Characteristics of the atrial flutter (11 cases) Typical form (AR 276 ± 21 min -1) Atypical form (AR 252 ± 36 min -1) Two or more morphologies Control group (22 patients; 6 with tachyarrhythmia at follow-up) (27,7%) Typical atrial flutter (AR 270 min -1) Atrial fibrillation MRV 127 ± 28 beats min-1 7 / 15 cases 4 / 15 cases 4 / 15 cases 2 cases 7 cases 2 cases 1 case 5 cases AR, atrial rate; MVR, mean ventricular rate during crises. 3. Our most recent papers In 1999 we published [27] a review paper in Europace commenting The syndrome of advanced interatrial block and supraventricular arrhythmia in which we summarized all previous research by our group and confirmed our view that this association most certainly constituted a syndrome. We also published a review paper on block at atrial level [21], including the possible diagnosis of right atrial block in case of clockwise rotation of P loop in FP. Also we publish several papers on atrial aberrancy [28, 29], concept that, if the change of P wave is a pattern of partial or advanced IAB, corresponds to a second degree IAB [30] (Fig.4). We emphasized as we stated in papers and books on ECG [11, 22, 30] and in the latest consensus paper on IAB [23] that these ECG patterns described as patterns of partial and advanced IAB are due to a block, not to atrial enlargement because a) it may be transient and progressive (Fig.7), b) it may exist without associated left atrial enlargement and c) it may be reproduced experimentally [24] (Fig.12). 4. Conclusion a) We have defined the ECG-VCG criteria of advanced IAB and its etiological aspects and prevalence. b) We have observed that supraventricular arrhythmias appear very often in a short follow-up in patients with ECG pattern of advanced IAB, if left untreated, and that when are in front of a patient with atypical flutter we can be nearly certain that in sinus rhythm the patient will have the ECG pattern of advanced IAB. c) We have demonstrated that if we treat with antiarrhythmic drugs the patients with advanced IAB, the incidence of supraventricular tachyarrhythmic in the future is much lower. d) Therefore, we may conclude that this association should be considered a syndrome. 38
9 5. The recognition and the future Thanks to all this information, a select group of cardiologists have manifested their agreement by writing with our view and are convinced that the association of advanced IAB together with supraventricular arrhythmias is a syndrome. This includes Braunwald [31], Daubert [32], and Brugada [33]. Furthermore some groups especially the ones of Daubert [34], Spodick [35, 36], Platonov [37, 38] Garcia-Cossio [39] and Baranchuk and Conde [40-43] have also published different and important aspects on this topic. However, in all these decades it has never occurred to me that one might consider the name Bayés syndrome. Therefore, it was with great surprise that I learned of the generosity of Adrian Baranchuk, seconded by Diego Conde, and many other colleagues when I received the first paper on the proposed name for this syndrome, which appeared recently in Revista Instituto de México [40], and later other articles in Revista Argentina Cardiología [12], the American Journal of Cardiology [42], ANE [43], among others. What is truly important, however, is that the physicians have to be awarded that the association of advanced IAB plus supraventricular arrhythmias is a syndrome. Really the ECG pattern of advanced IAB is an extremely strong marker of supraventricular tachyarrhythmias in a short period of time, much more so than the presence of partial IAB (only P 120 msec), which already presents a high incidence of arrhythmia [26, 28], although to a lesser degree when compared with advanced IAB pattern, as we have already shown. The other speakers of this symposium will explain other very important aspects of the electrophysiology of the atria, and Adrian Baranchuk, the father of this symposium will outline the many possibilities for research that still exist with this syndrome, whatever its name may be in the future. I would like to express my gratitude to Dr. L. Bacharova President of the meeting (ICE- 2014), and International Society of Electrocardiology (ISE) President Dr.C.Pastore, for giving to me the opportunity to explain this story to so many friends. It was extremely generous of her. My special thanks go to all other members of this round table for your friendship and for attending this symposium. I also have to thank the support and intellectual challenge provided by several cardiologists working in this field in different aspects, who have been exchanging ideas with me from the beginning: P. Puech, JC. Daubert, D. Spodick, P. Platonov, A. Waldo, F. Garcia-Cossio, A. Baranchuk, D. Conde and the friendly support of B. Olson, E. Braunwald, P. Chiale, M. Elizari, A. Perez-Riera, R. Barbosa, C. Pastore, Hnos. Brugada, X. Viñolas, W. Zareba, I. Cygankiewicz, R. Baranowski, R. Villuendas, A. Bayés Genís, and of course each and every member of my team. Thank you all so very much. References [1] Bachmann G. The significance of splitting of the P-wave in the ECG. Am.Int.Med.1941;14:1707. [2] Cohen J, Scharf D. Complete interatrial and intraatrial block (atrial demonstration). American Heart Journal 1965;70:24 [3] Legato MJ, Ferrer MI. Intermitent intra-atrial block: its diagnosis, incidence, and implications. Chest 1974;65:243 [4] Zoneraich O, Zoneraich S. Atrial tachycardia with high degree intraatrial block. J.Electricardiol. 1971;4:369. [5] Puech P. L activite electrique auriculaire normal et pathologique. Maron 1956 p.206. [6] Castillo A, Vernant P. Troubes de la conduction interauriculaire par bloc du fascion de Bachmann. Estude de 3 cas per ECG endoauriculaire. Arch. Mal. Coeur 1973;4:31 [7] D.Biase M, Rizzon P. Blocco interatriale con activatione retrograde dell atrio sinistro. Giornale Italiano Card. 1975;5:323. [8] Garcia Civera R, Llinus A, Benages A, et al. Estúdio de la activación auricular y de la conducción AV en el bloqueo del Haz de Bachmann en el corazón humano. Rev.Esp. Card. 1972;24:341 [9] Lee K, Appleton C, Lester S, et al. Relation of ECG criteria for LAE in two-dimensional echocardiographic left atrial volume measurements. American Journal Card. 2007;99:113. [10] Tsao CW, Josepson ME, Hauser TH. Accuraces of ECG criteria for LAE. J. Cardio. Mag. Resonance 2002;10:7. 39
10 [11] Bayés de Luna A, et al. Curso de Electrocardiografia y vectorcardiografia. Edit. Cientifico Médica [12] Piccolo E. Electrocardiografic e veto cardiografic. Edit. Piccin 1981 p.88. [13] Oreto G. L elletrocardiogramma: a mosaico a 12 tessere. Centro Scientifico Editore [14] T-Chuan Chou. Electrocardiography in clinical practice. Grune-Stratton 1979 [15] Marfarlane P, et al. Editors. Comprehensive Electrocardiology. Springer [16] Willems JL, Robles de Medina EO, Bernard R, et al. Criteri for intraventricular conduction disturbances and pre-excittion: WHO/ISFC Task Force Ad Hoc. J Am Coll Cardiol 1985;5:1261. [17] Mirivis D, Gordberger. Electrocardiography Chapter V.Braunwald textbook.heart disease. Saunders [18] Fuster V, et al, Editors. The heart 13th Edition. Mc-Graw Hill [19] Bayés de Luna A, Ferrer S, Vilaplana J, et al. Interatrial block with left atrial retrograde activation. Abstract in Eu.Con.Card. Book II p [20] Bayés de Luna A. Bloqueo a nivel auricular. Rev.Esp.Cardiol.1979;39:5. [21] Bayés de Luna A, Bailén JL, Guindo, et al. Blocks at the atrial level. New Trends in Arrhythmias 1987;3:219. [22] Bayés de Luna A, Fort de Ribot R, Trilla E, et al. Electrocrdiographic and vectorcardiographic study of interatrial conduction disturbances with left atrial retrograde activation. J Electrocardiology 1985;18:1. [23] Bayés de Luna A, Platonov P, Cossio FG, et al. Interatrial blocks. A separate entity from left atrial enlargement: a consensus report. Journal of Electrocardilogy 2012;45: [24] Waldo A, Harry L, Bush Jr, et al. Effects on the canine P wave of descrete lesions in the specialized atrial tracts. Circulation Res 1971;29:452. [25] Bayés de Luna A, Cladellas R, Oter P, et al. Interatrial conduction block and retrograde activation of the lerf atrium and paroxysmal supraventricular tachyarrhythmia. European Heart Journal 1988;9:1112. [26] Interatrial conduction block with retrograde activation of the left atrium and paroxysmal supraventricular tachyarrhythmias: influence of preventive antiarrhythmic treatment. International Journal of Cardiol.1989;22: [27] Bayés de Luna A, Guindo J, Viñolas X, et al. Third-degree inter-atrial block and supraventricular tachyarrhythmias.europace 1999;1:43. [28] Bayés de Luna A, Julià J, Lopez J. ECG-VCG study of atrial aberrancy. Book V International Congress in ECG. Glasgow [29] Julià J, Bayés de Luna A, Candell J, et al. Aberrancia auricular. A proposito de 21 casos. Rev. Esp. Cardiologia 1978;31:207. [30] Bayés de Luna A. The ECG for beginners. Wiley-Blackwell [31] Braunwald E. Foreword. In: Bayés de Luna A, Clinical Electrocardiography: a textbook. Chichester, West Sussex, UK: Wiley-Blackwell;2012. [32] Daubert JC. Atrial flutter and interatrial conduction block. In: Waldo A, Touboul P, editors. Atrial Flutter. Armonk, NY: Futura Publisihing; p.33. [33] Brugada P, Brugada J, Brugada R. Sindromes arritmologicos en Cardiologia clinica. Bayés de Luna et al, editors.p.478. Masson [34] Daubert JC, Pavin D, Jauvert G, et al. Intra and interatrial conduction delay: implications for cardiac pacing. Pacing Clin Electrophysiol 2004;27:507. [35] Spodick DH, Ariyarah V. Interatrial block. The pandemic remains poorly perceived. Pacing Clin Electrophisiol 2009;32:662. [36] Spodick DH, Ariyarah V. Interatrial block; a prevalent, widely neglected and portentous anormality. J Electrocardiol 2008;41:61. [37] Platonov P. Atrial conduction and atrial fibrillation. What can we learn form ECG? Cardiol J 2008;15:402. [38] Platonov P, Mitrofanova L, Ivanov V, et al. Substrates for intra-atrial and interatrial conduction in the atrial septum: anatomical study on 84 humans hearts. Heart Rhythm 2008;5:1189. [39] Cosio FG, Martín-Peñato A, Pastor A, et al. Atrial activation zapping in sinus rhythm in the clinical electrophysiology laboratory. Observations in Bachmann s bundle block. J Cardiovasc Electrophysiol 2004;15:524. [40] Conde D, Baranchuk A. Bloqueo interauricular como sustrato anatómico-eléctrico de arritmias supraventriculares: syndrome de Bayés.Archivos de Cardiología de México [41] Conde D, Baranchuk A. Síndrome de Bayés: lo que un cardiologo no debe dejar de saber. Revista Argentina de Cardiologia in press. [42] Enriquez A, Conde D, Baranchuk A, et al. Relation of interatrial block to new-onset atrial fibrillation in patients with chagas cardiomyopathy and implantable cardioverter-defibrillators. AJC impress. DOI: /j.amjcard [43] Baranchuk A, Conde D, Enriquez A, et al. P-wave duration or Pwave morphology? Interatrial block: seeking for the holy grail to predict AF recurrence. Ann Noninvasive Electrocardiol 2014;00:
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS
 65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Electrocardiographic Issues in Williams Syndrome
 Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
How should we treat atrial fibrillation in heart failure
 Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ
 «Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
Objectives. The ECG in Pulmonary and Congenital Heart Disease. Lead II P-Wave Amplitude during COPD Exacerbation and after Treatment (50 pts.
 The ECG in Pulmonary and Congenital Heart Disease Gabriel Gregoratos, MD Objectives Review the pathophysiology and ECG signs of pulmonary dysfunction Review the ECG findings in patients with: COPD (chronic
The ECG in Pulmonary and Congenital Heart Disease Gabriel Gregoratos, MD Objectives Review the pathophysiology and ECG signs of pulmonary dysfunction Review the ECG findings in patients with: COPD (chronic
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
How to read the ECG in athletes: distinguishing normal form abnormal
 How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
The abbreviation EKG, for electrocardiogram,
 CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Il loop recorder esterno. Roberto Maggi
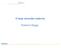 Il loop recorder esterno Roberto Maggi ECG monitoring and syncope In-hospital monitoring Holter Monitoring Event recorder External loop recorder Remote (at home) telemetry Implantable loop recorder External
Il loop recorder esterno Roberto Maggi ECG monitoring and syncope In-hospital monitoring Holter Monitoring Event recorder External loop recorder Remote (at home) telemetry Implantable loop recorder External
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
510(k) Summary May 7, 2012
 510(k) Summary Medicalgorithmics 510(k) Premarket Notification 510(k) Summary May 7, 2012 1. Submitter Name and Address Medicalgorithmics LLC 245 West 107th St., Suite 11A New York, NY 10025, USA Contact
510(k) Summary Medicalgorithmics 510(k) Premarket Notification 510(k) Summary May 7, 2012 1. Submitter Name and Address Medicalgorithmics LLC 245 West 107th St., Suite 11A New York, NY 10025, USA Contact
Lead avr: The Neglected Lead
 Chapter 22 Lead avr: The Neglected Lead M Chenniappan INTRODUCTION Lead avr, one of the 12 electrocardiographic leads, is frequently ignored in clinical medicine. In fact, many clinicians refer to the
Chapter 22 Lead avr: The Neglected Lead M Chenniappan INTRODUCTION Lead avr, one of the 12 electrocardiographic leads, is frequently ignored in clinical medicine. In fact, many clinicians refer to the
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
VCA Veterinary Specialty Center of Seattle
 An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
22 Arrhythmias. C. Scharf and F. Duru. Siegenthaler, Differential Diagnosis in Internal Medicine (ISBN9783131421418), 2007 Georg Thieme Verlag
 22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects
 Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects Halon Alternatives Technical Working Conference 1993 Reva Rubenstein, Ph.D. U.S.Environmenta1 Protection Agency
Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects Halon Alternatives Technical Working Conference 1993 Reva Rubenstein, Ph.D. U.S.Environmenta1 Protection Agency
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Detection of Heart Diseases by Mathematical Artificial Intelligence Algorithm Using Phonocardiogram Signals
 International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 3 No. 1 May 2013, pp. 145-150 2013 Innovative Space of Scientific Research Journals http://www.issr-journals.org/ijias/ Detection
International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 3 No. 1 May 2013, pp. 145-150 2013 Innovative Space of Scientific Research Journals http://www.issr-journals.org/ijias/ Detection
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
The choice for quality ECG arrhythmia monitoring
 GE Healthcare EK-Pro The choice for quality ECG arrhythmia monitoring David A. Sitzman, MSEE. Mikko Kaski, MSAM. Ian Rowlandson, MSBE. Tarja Sivonen, RN. Olli Väisänen, MD, PhD. Clinical care environments
GE Healthcare EK-Pro The choice for quality ECG arrhythmia monitoring David A. Sitzman, MSEE. Mikko Kaski, MSAM. Ian Rowlandson, MSBE. Tarja Sivonen, RN. Olli Väisänen, MD, PhD. Clinical care environments
Signal-averaged electrocardiography late potentials
 SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Surgeons Role in Atrial Fibrillation
 Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
How do you decide on rate versus rhythm control?
 Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Feature Vector Selection for Automatic Classification of ECG Arrhythmias
 Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
Corporate Medical Policy
 Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
Management of Symptomatic Atrial Fibrillation
 Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
ATRIAL FIBRILLATION: Scope of the Problem. October 2015
 ATRIAL FIBRILLATION: Scope of the Problem October 2015 Purpose of the Presentation Review the worldwide incidence and prognosis associated with atrial fibrillation (AF) Identify the types of AF, clinical
ATRIAL FIBRILLATION: Scope of the Problem October 2015 Purpose of the Presentation Review the worldwide incidence and prognosis associated with atrial fibrillation (AF) Identify the types of AF, clinical
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
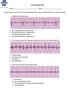 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
TOP 5. The term cardiac arrhythmia encompasses all cardiac. Arrhythmias in Dogs & Cats. Sinus Arrhythmia. TOP 5 Arrhythmias Seen in Dogs & Cats
 Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Evaluation of a direct access cardiac arrhythmia monitoring service
 ORIGINAL ARTICLE Cardiology Journal 2012, Vol. 19, No. 1, pp. 70 75 10.5603/CJ.2012.0010 Copyright 2012 Via Medica ISSN 1897 5593 Evaluation of a direct access cardiac arrhythmia monitoring service David
ORIGINAL ARTICLE Cardiology Journal 2012, Vol. 19, No. 1, pp. 70 75 10.5603/CJ.2012.0010 Copyright 2012 Via Medica ISSN 1897 5593 Evaluation of a direct access cardiac arrhythmia monitoring service David
Electrocardiogram (ECG) as a diagnostic tool for the assessment of Cardiovascular status in alcoholics
 Biomedical Research 2011; 22 (3): 333-337 Electrocardiogram (ECG) as a diagnostic tool for the assessment of Cardiovascular status in alcoholics Venkatesh G Department of Physiology, Sri Siddhartha Medical
Biomedical Research 2011; 22 (3): 333-337 Electrocardiogram (ECG) as a diagnostic tool for the assessment of Cardiovascular status in alcoholics Venkatesh G Department of Physiology, Sri Siddhartha Medical
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Electrophysiology Introduction, Basics. The Myocardial Cell. Chapter 1- Thaler
 Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients
 Premio al mejor Tema Libre Realizado por Médicos Residentes Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients Olivares-Reyes Alexander; Al-Kamme Ahmad; Gonzalez Javier Cardiology Department
Premio al mejor Tema Libre Realizado por Médicos Residentes Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients Olivares-Reyes Alexander; Al-Kamme Ahmad; Gonzalez Javier Cardiology Department
Michael Hartman, CRNA, DNP, MSN, BSN, BA
 Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
Evaluation and Initial Treatment of Supraventricular Tachycardia
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Atrial Fibrillation in the Wolff-Parkinson-White Syndrome. John Whitaker, Conn Sugihara and Michael Cooklin (Guy s and St Thomas NHS Foundation Trust)
 Atrial Fibrillation in the Wolff-Parkinson-White Syndrome John Whitaker, Conn Sugihara and Michael Cooklin (Guy s and St Thomas NHS Foundation Trust) A 38 year old paramedic was admitted with symptoms
Atrial Fibrillation in the Wolff-Parkinson-White Syndrome John Whitaker, Conn Sugihara and Michael Cooklin (Guy s and St Thomas NHS Foundation Trust) A 38 year old paramedic was admitted with symptoms
Basics of Pacing. Ruth Hickling, RN-BSN Tasha Conley, RN-BSN
 Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Rome, Italy December 4-7, 2012 Rome Cavalieri TIMETABLE
 Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Implantable Cardioverter Defibrillator Treatment: Benefits and Pitfalls in the Currently Indicated Population. Carel Jan Willem Borleffs
 Implantable Cardioverter Defibrillator Treatment: Benefits and Pitfalls in the Currently Indicated Population Carel Jan Willem Borleffs The studies described in this thesis were performed at the Department
Implantable Cardioverter Defibrillator Treatment: Benefits and Pitfalls in the Currently Indicated Population Carel Jan Willem Borleffs The studies described in this thesis were performed at the Department
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
The new generation in ECG interpretation
 The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
Surgically Induced Right Bundle-Branch Block with Left Anterior Hemiblock
 Surgically Induced Right Bundle-Branch Block with Left Anterior Hemiblock An Ominous Sign in Postoperative Tetralogy of Fallot By GRACE S. WOLFF, M.D., THOMAS W. ROWLAND, M.D., AND R. CURTIS ELLISON, M.D.
Surgically Induced Right Bundle-Branch Block with Left Anterior Hemiblock An Ominous Sign in Postoperative Tetralogy of Fallot By GRACE S. WOLFF, M.D., THOMAS W. ROWLAND, M.D., AND R. CURTIS ELLISON, M.D.
QT analysis: A guide for statistical programmers. Prabhakar Munkampalli Statistical Analyst II Hyderabad, 7 th September 2012
 QT analysis: A guide for statistical programmers Prabhakar Munkampalli Statistical Analyst II Hyderabad, 7 th September 2012 Agenda ECG ICH E14 Thorough QT/QTc study Role of Statistical Programmer References
QT analysis: A guide for statistical programmers Prabhakar Munkampalli Statistical Analyst II Hyderabad, 7 th September 2012 Agenda ECG ICH E14 Thorough QT/QTc study Role of Statistical Programmer References
Electrophysiology Heart Study - EPS -
 Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
TABLE 1 Clinical Classification of AF. New onset AF (first detected) Paroxysmal (<7 days, mostly < 24 hours)
 Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them?
 2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them? Gaetano Senatore DIVISION OF CARDIOLOGY HOSPITAL OF CIRIE
2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them? Gaetano Senatore DIVISION OF CARDIOLOGY HOSPITAL OF CIRIE
Tips and Tricks to Demystify 12 Lead ECG Interpretation
 Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Comparison of bipolar and unipolar programmed electrical stimulation for the initiation of ventricular arrhythmias: significance of anodal excitation
 DIAGNOSTIC METHODS ELECTROPHYSIOLOGY Comparison of bipolar and unipolar programmed electrical stimulation for the initiation of ventricular arrhythmias: significance of anodal excitation during bipolar
DIAGNOSTIC METHODS ELECTROPHYSIOLOGY Comparison of bipolar and unipolar programmed electrical stimulation for the initiation of ventricular arrhythmias: significance of anodal excitation during bipolar
ECG Measurement and Interpretation
 ECG Measurement and Interpretation Statement of accuracy for analysing ECG units *2.530036* Physicians Guide Sales and Service Information The SCHILLER sales and service centre network is world-wide. For
ECG Measurement and Interpretation Statement of accuracy for analysing ECG units *2.530036* Physicians Guide Sales and Service Information The SCHILLER sales and service centre network is world-wide. For
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being
 Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. danjcohen@optonline.net
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. danjcohen@optonline.net
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D.
 HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D. INTRODUCTION Heart rhythm disorders, called arrhythmias, pose one of the paradoxes of medicine. Almost anyone s heart will
HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D. INTRODUCTION Heart rhythm disorders, called arrhythmias, pose one of the paradoxes of medicine. Almost anyone s heart will
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
Doc, I Am Fine, But I Have A Cardiac Condition
 Doc, I Am Fine, But I Have A Cardiac Condition Nevine Mahmoud, MD John Ludtke, MD Maj, USAFR, MC, FS RAM Class 2014 Wright State University Boonshoft School of Medicine Division of Aerospace Medicine Dayton,
Doc, I Am Fine, But I Have A Cardiac Condition Nevine Mahmoud, MD John Ludtke, MD Maj, USAFR, MC, FS RAM Class 2014 Wright State University Boonshoft School of Medicine Division of Aerospace Medicine Dayton,
Cardiac Arrhythmias. Introduction. Sinus Rhythms. Premature Beats. Secondary article. John A Kastor, University of Maryland, Baltimore, Maryland, USA
 John A Kastor, University of Maryland, Baltimore, Maryland, USA Cardiac arrhythmias are disturbances in the rhythm of the heart manifested by irregularity or by abnormally fast rates ( tachycardias ) or
John A Kastor, University of Maryland, Baltimore, Maryland, USA Cardiac arrhythmias are disturbances in the rhythm of the heart manifested by irregularity or by abnormally fast rates ( tachycardias ) or
