Early Neonatal Research at Wilford Hall US Air Force Medical Center
|
|
|
- Wilfred McBride
- 8 years ago
- Views:
Transcription
1 Early Neonatal Research at Wilford Hall US Air Force Medical Center The beginning of the many contributions to the field of neonatology originating from Wilford Hall Air Force Medical Center began when Robert delemos, MD (Col, retired US Air Force [USAF]), was assigned to Lackland Air Force Base (AFB) in the summer of When Dr delemos came to Texas, he was the first and only fully trained Air Force neonatologist at a time when neonatal medicine was still just in its infancy. Although surfactant deficiency had been described as the cause of hyaline membrane disease by Dr Avery in her landmark article published in 1959, surfactant replacement therapy in premature infants did not begin until the 1980s after the work of Dr Fujiwara et al was reported in Lancet. 1,2 Morbidity and mortality remained high in premature infants, especially in those under 1500 g with respiratory distress syndrome (RDS). Reports published in the 1960s and 1970s described early attempts at the use of mechanical ventilation to rescue neonates with respiratory failure, but ventilator options were limited and devices were not widely available, resulting in minimal success. 3,4 Given this backdrop, the story of the accomplishments of a relatively small group of military neonatologists led by Dr delemos takes on added historical significance. Some of the most important initial work completed by Dr delemos and his colleagues centered on their efforts to improve respiratory support and cardiovascular monitoring in the critically ill neonate. In the late 1960s and early 1970s, physiologic monitoring of the neonate was very difficult. Blood pressure could only be accurately obtained by using indwelling arterial lines. Ventilators in this time period only provided flow during the inspiratory cycle. If patients breathed between ventilator breaths, they were rebreathing their own exhaled gas contributing to impaired ventilation and oxygenation. In neonates this required mechanical ventilation at rapid rates imposing a greater risk of lung trauma and cardiac and central nervous system complications. Additionally, positive end-expiratory pressure (PEEP) was not a feature of available neonatal ventilator systems. The end result was that assisted ventilation of the preterm infant with surfactant deficiency was of little to no benefit in improving outcome. In an effort to come up with a better solution, Dr delemos, along with Bob Kirby, MD (Col, retired USAF), an anesthesiologist, and Jimmy Schultz, RRT, embarked on a course of developing an effective pediatric/neonatal ventilator. The initial device was built by Jimmy Schultz by using spare parts from predominantly a Mark II ventilator. The original request from Drs Kirby and delemos of Jimmy Schultz was to build a ventilator that allowed for a continuous flow of fresh gas through all phases of the respiratory cycle, thus allowing for a consistent level of oxygen and humidification as well as rapid removal of exhaled CO 2. Additionally, they wanted a device capable of providing continuous PEEP during the AUTHORS: Donald M. Null, MD, FAAP, a Bradley A. Yoder, MD, FAAP, a and Robert J. DiGeronimo, MD b a Division of Neonatology, Department of Pediatrics, University of Utah Health Sciences Center, Salt Lake City, Utah; and b Division of Neonatology, Department of Pediatrics, Wilford Hall US Air Force Medical Center, Lackland Air Force Base, Texas ABBREVIATIONS AFB Air Force Base ECMO extracorporeal membrane oxygenation HFOV high-frequency oscillatory ventilation HFV high frequency ventilation IMV intermittent mandatory ventilation PEEP positive end-expiratory pressure RDS respiratory distress syndrome USAF US Air Force The views and opinions expressed in this article are those of the authors and do not reflect the official policy or position of the Air Force Medical Department, Department of the Air Force, the Department of Defense, or the US Government. doi: /peds e Accepted for publication Oct 7, 2011 Address correspondence to Robert J. DiGeronimo, MD (Col, retired US Air Force), 295 Chipeta Way, Salt Lake City, UT robert.digeronimo@hsc.utah.edu PEDIATRICS (ISSN Numbers: Print, ; Online, ). Copyright 2012 by the American Academy of Pediatrics FINANCIAL DISCLOSURE: The authors have indicated they have no financial relationships relevant to this article to disclose. S20
2 SUPPLEMENT ARTICLE expiratory phase. They also requested that the ventilator be able to provide a peak pressure up to 80 cm H 2 O, PEEP up to 20 cm H 2 O, and rate up to 130 breaths per minute to support small children weighing up to 25 kg in addition to premature infants weighing as little as 800 g. Because patients supported with this device were able to breathe fresh (not expired) gas with spontaneous respirations between machine breaths, this meant that fewer mechanical breaths could be used. With the development of this prototype neonatal ventilator, intermittent mandatory ventilation (IMV) for the neonate was born. Using their prototype ventilator, Kirby et al 5 went on to demonstrate that neonates with respiratory failure could be kept in a physiologic ph range without the need of paralytic agents or complex triggering devices. This allowed for ease of weaning the ventilator rate and better determination of when a patient could be extubated. In 1970 Kirby et al 6 mechanically ventilated 90 infants with their new device, including 60 infants given a diagnosis of RDS for periods ranging from,24 hours to 31 days. No infant was ventilated unless the combined pediatric and anesthesia staffs felt they would not survive without support. Criteria for intubation were a PaO 2 of,40 mm Hg on 100% oxygen, a PaCO 2 of 70 mm Hg and rising, and/or repeated apneic episodes of a life threatening nature. These extreme criteria for intubation were used as assisted ventilation was thought to contribute little to the survival of the preterm infant. At a time when survival was typically,30% for infants with severe RDS, Wilford Hall was surviving 60% of mechanically ventilated infants with RDS with birth weights as low as 750 g and up to 80% of infants 1600 g or greater. 6 After the early success of the prototype ventilator, individuals from Bourns (a leading manufacturer of mechanical ventilators during this era) were contacted to see if they were interested in helping to further develop the Wilford Hall device; however, as Dr delemos later related, they were uninterested given their belief that there was only a limited need for neonatal ventilators in the United States ( 100), and Bourns had close to this number of LS 104 devices already built. Shortly thereafter, Dr Forrest Bird paid a visit to Wilford Hall. Impressed with the success that Drs delemos and Kirby had in ventilating ill premature infants, he became interested in their device. This encounter subsequently led to Dr Bird further refining the Wilford Hall prototype ventilator and eventually marketing it as the Baby Bird ventilator. From the early 1970s into the 1980s, the Baby Bird proved to be the work horse mechanical ventilator used for the management of neonates and infants with RDS and other causes of respiratory failure. During this time, IMV remained the predominant form of ventilatory support until the development of synchronous IMV over the last 15 to 20 years. Nonetheless, to this day,theuseofbothcontinuousgasflow during expiration and the inclusion of PEEP remain standard in the design of neonatal ventilatory support. The ventilator initially developed by the military team of delemos, Kirby, and Schultz proved to be an exceptional device that revolutionized mechanical ventilation of the neonate and small child. A photograph of Dr delemos is pictured in Fig 1, the prototype ventilator built by Jimmy Schulz in Fig 2, and the original Baby Bird device built by Dr Bird in Fig 3. During the early days of experimentation with assisted ventilation of the neonate at Wilford Hall, additional novel work was reported by Dr delemos and colleagues. Among their many contributions, one of the most important was their landmark article published in 1973 describing the beneficial effects of continuous positive airway pressure combined with mechanical ventilation, what we now call PEEP. 7 In this report of 25 mechanically ventilated neonates, delemos et al analyzed the effects of PEEP by increasing support from 0 to 20 cm H 2 O in 5-cm increments. They FIGURE 1 Dr Robert delemos, MD (Col, retired USAF) served as the first fully trained USAF neonatologist at Wilford Hall Medical Center, Lackland AFB, Texas. FIGURE 2 Prototype neonatal and pediatric ventilator built by Jimmy Schulz, RRT. PEDIATRICS Volume 129, Supplement S1, February 2012 S21
3 FIGURE 4 Doppler blood pressure device designed by Gary McLaughlan, MD. FIGURE 3 Original Baby Bird neonatal ventilator built by Dr Forrest Bird. were able to demonstrate improved oxygenation in 80% of patients with increasing PEEP. Of particular importance, they also described in this study the adverse effects of high levels of PEEP (decreased blood pressure and increased PaCO 2 generally occurring above 10 cm H 2 O), noting the principle that just because some is good, more is not always better. The authors recommended that the level of PEEP selected must therefore be individualized for each patient by careful monitoring of blood pressure, chest radiographs, and blood gas measurements. In the 1970s noninvasive blood pressure measurement with a stethoscope and sphygmomanometer was ineffective in the neonate because newborn arteries do not generate an adequate sound for auscultation. Systolic blood pressure was typically estimated by determining when the arm pinked up as pressure was released via the sphygmomanometer. This was a very poor technique for the preterm or ill term infant whose extremities often looked dusky to begin with. Among larger patients indwelling catheters were used to monitor blood pressure; however, umbilical arterial lines could not be placed in many seriously ill newborns, and angiocaths small enough for an infant s peripheral artery did not exist. In an effort to improve existing technology to measure blood pressure, Dr Gary McLaughlan, a fellow at the time under Dr delemos, devised a novel device that used Doppler ultrasound to indirectly measure blood pressure in neonates. In 1971, Dr McLaughlan published the Wilford Hall experience with this device in 15 ill newborns demonstrating its accuracy in comparison with blood pressures measured from indwelling umbilical catheters. 8 Similar to the Baby Bird ventilator, this early prototype developed at Wilford Hall subsequently led to the marketing of a commercially available device that greatly advanced the standard of care available at the time for monitoring critically ill infants. Figure 4 shows the Doppler pressure device used in Dr McLaughlan s original study. Transport has always played a vital role in the military pediatric mission, with many technological advances in this arena originating early on in San Antonio through the collaborative efforts of military personnel atwilford Hall, Brooke Army Medical Center and Brooks AFB. Interest in reliable and safe pediatric transport grew out of the need to support local, regional, and intercontinental movement of critically ill infants from outlying military bases to Wilford Hall and Brooke Army Medical Center often fordefinitive life-saving care. Specifically, in the area of neonatal transport, military physicians were instrumental in developing, testing, and modifying neonatal equipment ensuring that it performed safely while not interfering with aircraft electromechanical operations. 9 Howard Heiman, MD (COL, retired US Army), in conjunction with Airborne Life Support and the testing laboratory at Brooks AFB, developed the first fully contained neonatal transport unit that continues to be the model for systems routinely used today. These systems have been effectively used in the military neonatal care system for several decades, supporting both regional and long distance transports from as far away as Asia and Europe. Over the years, there has remained a strong interest at Wilford Hall in advancing the management of neonates with respiratory failure in an effort to reduce acute and chronic lung injury. In the early 1980s Drs Null, delemos, Yoder (Col, retired USAF), and Clark began working with high frequency ventilation (HFV) aiming to improve survival and reduce bronchopulmonary dysplasia in newborns. These investigators were instrumental in establishing a term and preterm baboon model along with their colleagues at the Southwest Foundation for Biomedical Research in San Antonio that proved to be invaluable for studying HFV. By using the baboon model coupled with clinical experience S22
4 SUPPLEMENT ARTICLE FIGURE 5 Sensormedics 3100A frequency oscillator ventilator. generated from the Wilford Hall NICU, Dr Null and his colleagues were able to develop an appropriate HFV strategy for the management of RDS and other causes of respiratory failure in the newborn. Numerous publications were generated from the Wilford Hall experience with HFV, where the clinical use of HFV dates back to late Of note, HFV research was conducted by using both the Bird volumetric diffusive ventilation flow interrupter and Texas Research high frequency oscillator, the latter of which served as the prototype for the Sensormedics 3100A. One of the first HFV randomized controlled clinical trials conducted at Wilford Hall was led by Dr Reese Clark in the mid 1980s involving very low and extremely low birth weight premature infants. 27 The findings from this trial were extremely important at the time in that they demonstrated that HFV could be safely used in premature infants to significantly decrease bronchopulmonary dysplasia without adverse complications, findings quite disparate from earlier reported studies involving other centers. The many studies and publications from the San Antonio military neonatal community such as the Clark study were integral to the further development of HFV and ultimate Food and Drug Administration approval in the early 1990s, particularly highfrequency oscillatory ventilation (HFOV). Today, HFOV devices are nearly universally present in newborn and pediatric intensive care units not only in the United States but throughout the world. It is important to recognize that an understanding of the utility of HFV was only made possible by the dedication of many Wilford Hall neonatology staff and fellows who spent countless hours at the bedside of critically ill patients, using trial and error to gain insight into different HFV devices and their effect on treating varying underlying lung pathophysiology. 28 A present day Sensormedics HFOV 3100A is pictured in Fig 5. In continuation of the tradition of excellence established early on at Wilford FIGURE 6 Critically ill neonate placed on ECMO by Dr delemos in Hall in managing critically ill newborns, especially those with cardiopulmonary problems, Devin Cornish, MD, also a fellow under Dr delemos, in late 1984 initiated steps to start an extracorporeal membrane oxygenation (ECMO) program. At this time, ECMO was considered largely an experimental therapy and was only being offered at a few centers within the United States. A story that very few people know even today, however, is that in 1972 a neonate dying of respiratory failure was successfully placed on extracorporeal bypass with a membrane oxygenator in the NICU at Wilford Hall by Dr delemos (see Fig 6). Even though this patient eventually died, this case is remarkable in that Dr delemos was even able to offer this therapy several years before the first successful published use of ECMO in a neonate in Dr Cornish, along with Drs Null and delemos, did go on to establish the military s first and only ECMO program at Wilford Hall in Wilford Hall was the 12th center to open in the United States and the first to open in Texas. Given Wilford Hall s large catchment area and the existence of relatively few centers offering ECMO, candidates referred for ECMO were often moribund and too sick to safely transport by conventional means. This resulted in PEDIATRICS Volume 129, Supplement S1, February 2012 S23
5 considerable morbidity and mortality during the referral process to include children dying either before or during attempted transport to ECMO centers. In an effort to address this problem, especially with regards to military dependents stationed with their families at bases where ECMO was not readily available, Drs Cornish, Null, and Neal Ackerman undertook studies to develop an ECMO transport system. 30 During this process, they worked closely with the aeromedical research groups at Brooks AFB and spent many hours doing in-flight testing to ensure safety for the patient, equipment, crew, and aircraft. Their hard work led to the remarkably quick development of a safe and reliable ECMO transport system, resulting in the first ECMO transport being done by Wilford Hall shortly after the ECMO program opened. Figure 7 shows a picture of Dr Null with the original ECMO transport system. Wilford Hall remains at present as one of the world leaders in ECMO transport capability, being 1 of only 3 centers in the United States that routinely performs regional ECMO transport and the only one with the technology and resources to routinely perform longdistance missions. The early Wilford Hall ECMO transport experience was initially described by Dr Cornish in Several updates of this experience have been additionally reported, with the most recent publication noting an average distance of 1380 miles per transport, including several transports from Okinawa, Japan, involving distances of.7500 miles (see Fig 8). 32,33 To date, Wilford Hall has performed over 70 ECMO transports, including missions involving military dependents as well as civilian children requiring humanitarian rescue. All of these transports have been performed successfully and safely without the occurrence of a major complication. Given the high risk FIGURE 7 Dr Don Null (Col, retired USAF) with neonatal patient supported on the original ECMO transport system developed at Wilford Hall. FIGURE 8 Distribution map of ECMO transport missions done by Wilford Hall. Black lines represent course of transport. Average distance for all transports was 1380 miles (2220 km). nature of ECMO transport, especially over extremely long distances often requiring multiple air and ground transfers, this accomplishment is truly remarkable. The success of the Wilford Hall ECMO transport program is a testament to the dedicated efforts of the many military neonatal nurses, respiratory therapists, and physicians who have been involved over the years, as well to the S24
6 SUPPLEMENT ARTICLE commitment by the USAF Aeromedical System and Surgeon s GeneralOffice to make these missions happen. Uniformed physicians stationed at Wilford Hall Air Force Medical Center and affiliated military institutions in San Antonio have provided many significant contributions to the field of neonatology. A test of the success of one s research is often the impact it has on its clinical outcomes and longevity. Continuous flow ventilation is present in all neonatal ventilators today having been initiated by Drs Kirby and delemos along with Jimmy Schultz. Doppler type blood pressure remains a mainstay in all newborn intensive care units. High frequency ventilation, thought by many to be a passing fancy, continues to be used for the very sickest patients from the smallest premature neonate to the largest adult. Wilford Hall remains as an innovator in ECMO research and extracorporeal support technology and continues to be one of the few centers in the world capable of providing ECMO transport to critically ill children. REFERENCES 1. Avery ME, Mead J. Surface properties in relation to atelectasis and hyaline membrane disease. AMA J Dis Child. 1959;97(5 pt 1): Fujiwara T, Maeta H, Chida S, Morita T, Watabe Y, Abe T. Artificial surfactant therapy in hyaline-membrane disease. Lancet. 1980;1(8159): Gregory GA, Kitterman JA, Phibbs RH, Tooley WH, Hamilton WK. Treatment of the idiopathic respiratory-distress syndrome with continuous positive airway pressure. NEngl JMed. 1971;284(24): Delivoria-Papadopoulos M, Levison H, Swyer PR. Intermittent positive pressure respiration as a treatment in severe respiratory distress syndrome. Arch Dis Child. 1965;40 (213): Kirby RR, Robison EJ, Schulz J, DeLemos RA. A new pediatric volume ventilator. Anesth Analg. 1971;50(4): Kirby RR, Robison EJ, Schulz J, DeLemos RA. Continuous-flow ventilation as an alternative to assisted or controlled ventilation in infants. Anesth Analg. 1972;51(6): DeLemos RA, McLaughlin GW, Robison EJ, Schulz J, Kirby RR. Continuous positive airway pressure as an adjunct to mechanical ventilation in the newborn with respiratory distress syndrome. Anesth Analg. 1973;52 (3): McLaughlin GW, Kirby RR, Kemmerer WT, DeLemos RA. Indirect measurement of blood pressure in infants utilizing Doppler ultrasound. J Pediatr. 1971;79(2): Bell RE, Yoder BA, Ackerman NB, Jr, Null DM, Jr, delemos RA. Military neonatal transport and intensive care effective and cost effective. Mil Med. 1984;149(3): Escobedo MB, Hilliard JL, Smith F, et al A baboon model of bronchopulmonary dysplasia. I. Clinical features. Exp Mol Pathol. 1982; 37(3): Ackerman NB Jr, Coalson JJ, Kuehl TJ, et al. Pulmonary interstitial emphysema in the premature baboon with hyaline membrane disease. Crit Care Med. 1984;12(6): Bell RE, Kuehl TJ, Coalson JJ, et al. Highfrequency ventilation compared to conventional positive-pressure ventilation in the treatment of hyaline membrane disease in primates. Crit Care Med. 1984;12(9): Bell RE, Coalson JJ, Ackerman NB Jr;et al. A nonpulmonary complication of highfrequency oscillation. Crit Care Med. 1986; 14(3): Clark RH, Gerstmann DR, Null DM, et al. Pulmonary interstitial emphysema treated by high-frequency oscillatory ventilation. Crit Care Med. 1986;14(11): Yoder BA, Kuehl TJ, de Lemos RA, Null DM Jr, Ackerman NB Jr. Patent ductus arteriosus during high-frequency ventilation for hyaline membrane disease. Crit Care Med. 1987;15(6): Clark RH, Wiswell TE, Null DM, delemos RA, Coalson JJ. Tracheal and bronchial injury in high-frequency oscillatory ventilation compared with conventional positive pressure ventilation. J Pediatr. 1987;111(1): Delemos RA, Coalson JJ, Gerstmann DR, et al. Ventilatory management of infant baboons with hyaline membrane disease: the use of high frequency ventilation. Pediatr Res. 1987;21(6): delemos RA, Gerstmann DR, Clark RH, Guajardo A, Null DM Jr. High frequency ventilation the relationship between ventilator design and clinical strategy in the treatment of hyaline membrane disease and its complications: a brief review. Pediatr Pulmonol. 1987;3(5): Gerstmann DR, delemos RA, Coalson JJ, et al. Influence of ventilatory technique on pulmonary baroinjury in baboons with hyaline membrane disease. Pediatr Pulmonol. 1988;5(2): delemos RA, Coalson JJ, Meredith KS, Gerstmann DR, Null DM Jr;. A comparison of ventilation strategies for the use of high-frequency oscillatory ventilation in the treatment of hyaline membrane disease. Acta Anaesthesiol Scand Suppl. 1989;90: Meredith KS, delemos RA, Coalson JJ, et al. Role of lung injury in the pathogenesis of hyaline membrane disease in premature baboons. J Appl Physiol. 1989;66(5): Carter JM, Gerstmann DR, Clark RH, et al. High-frequency oscillatory ventilation and extracorporeal membrane oxygenation for the treatment of acute neonatal respiratory failure. Pediatrics. 1990;85(2): Kinsella JP, Gerstmann DR, Clark RH, et al. High-frequency oscillatory ventilation versus intermittent mandatory ventilation: early hemodynamic effects in the premature baboon with hyaline membrane disease. Pediatr Res. 1991;29(2): Schwendeman CA, Clark RH, Yoder BA, Null DM, Jr, Gerstmann DR, Delemos RA. Frequency of chronic lung disease in infants with severe respiratory failure treated with high-frequency ventilation and/or extracorporeal membrane oxygenation. Crit Care Med. 1992;20(3): delemos RA, Yoder BA, McCurnin DC, Kinsella J, Clark R, Null D. The use of highfrequency oscillatory ventilation (HFOV) and extracorporeal membrane oxygenation (ECMO) in the management of the term/ near term infant with respiratory failure. Early Hum Dev. 1992;29(1 3): Paranka MS, Clark RH, Yoder BA, Null DM Jr. Predictors of failure of high-frequency oscillatory ventilation in term infants with severe respiratory failure. Pediatrics. 1995; 95(3): Clark RH, Gerstmann DR, Null DM Jr, delemos RA. Prospective randomized comparison of high-frequency oscillatory and conventional ventilation in respiratory distress syndrome. Pediatrics. 1992;89(1): 5 12 PEDIATRICS Volume 129, Supplement S1, February 2012 S25
7 28. Clark RH, Null DM. High frequency oscillatory ventilation. In: Pomerance JJ, Richardson CJ, eds. Neonatology for the Clinician. Norwalk, CT: Appleton and Lange; 1993: Bartlett RH, Gazzaniga AB, Jefferies R, Huxtable RF, Haiduc N, Fong SW. Extracorporeal membrane oxygenation (ECMO) cardiopulmonary support in infancy. Trans Am Soc Artif lntern Organ. 1976;22: Cornish JD, Gerstmann DR, Begnaud MJ, Null DM, Ackerman NB. In flight use of extracorporeal membrane oxygenation for severe respiratory failure. Perfusion. 1986;1: Cornish JD, Carter JM, Gerstmann DR, Null DM Jr. Extracorporeal membrane oxygenation as a means of stabilizing and transporting high risk neonates. ASAIO Trans. 1991;37(4): Wilson BJ Jr, Heiman HS, Butler TJ, Negaard KA, DiGeronimo RJ. A 16-year neonatal/ pediatric extracorporeal membrane oxygenation transport experience. Pediatrics. 2002;109(2): Coppola C, Tyree M, Larry K, DiGeronimo R. A 22-year experience in global transport extracorporeal membrane oxygenation. J Pediatr Surg. 2008;43(1):46 52 S26
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model
 Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model Kurt Gillette, MD, San Antonio Military Medical Center Background: High
Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model Kurt Gillette, MD, San Antonio Military Medical Center Background: High
ELSO GUIDELINES FOR ECMO CENTERS
 ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
University of Kansas. Respiratory Care Education
 University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
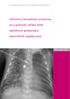 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Respiratory Care. A Life and Breath Career for You!
 Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
MECHANICAL VENTILATION IN THE NEONATE
 Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Mechanical Ventilators
 University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
Neurally Adjusted Ventilatory Assist: NAVA for Neonates
 Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
Respiratory Distress Syndrome of the Newborn
 19 Respiratory Distress Syndrome of the Newborn Respiratory distress syndrome (RDS) of the newborn, also known as hyaline membrane disease, is a breathing disorder of premature babies. In healthy infants,
19 Respiratory Distress Syndrome of the Newborn Respiratory distress syndrome (RDS) of the newborn, also known as hyaline membrane disease, is a breathing disorder of premature babies. In healthy infants,
How To Determine The Difference Between Long Versus Short Inspiratory Times In Neonates
 Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Brenda Neff MSN, RN, NE BC
 Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
Brenda Neff MSN, RN, NE BC 1400 s newborns have a soul 1600 s estimated that only 10% of the abandoned infants reached the age of 5 years. 1857 first incubator documented in western lit 1857 first incubator
What You Need to Know About Respiratory Care
 Loma Linda University 2015-2016 1 Respiratory Care B.S., M.S.R.C. Respiratory care is an allied health profession that promotes health and improvement in the cardiopulmonary function of people with heart
Loma Linda University 2015-2016 1 Respiratory Care B.S., M.S.R.C. Respiratory care is an allied health profession that promotes health and improvement in the cardiopulmonary function of people with heart
CURRICULUM VITAE. Richard L. Trader Sr. MMsc RRT. PA-C. FCCM. Personal. Present Title
 CURRICULUM VITAE Richard L. Trader Sr. MMsc RRT. PA-C. FCCM Personal Present Title Director RLT Medical Associates, Inc. Center for Telemedicine 1300 York Road Timonium, Maryland 21093 (410) 821-9620 Home
CURRICULUM VITAE Richard L. Trader Sr. MMsc RRT. PA-C. FCCM Personal Present Title Director RLT Medical Associates, Inc. Center for Telemedicine 1300 York Road Timonium, Maryland 21093 (410) 821-9620 Home
CURRICULUM VITAE. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.
 CURRICULUM VITAE Date: April 3, 2014 Name: Brian P. Lane, M.D. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.org Place of Birth: Greene
CURRICULUM VITAE Date: April 3, 2014 Name: Brian P. Lane, M.D. Business Address: 3020 Children s Way, RCHSD MC 5008, San Diego, CA 92123 Phone: 858 966-5818 email: blane@rchsd.org Place of Birth: Greene
06/05/2014. Respiratory Medicine Professor Colin Sullivan
 1 Respiratory Medicine Professor Colin Sullivan 2 3 Modalidade utilizada em 90% dos casos. Thorax 1998 53: 416-18 Lancet 1999 353:2100-05 AJRCCM 2004 169:156-62 AJRCCM 161:857-5-859, 2000 Chest 2005; 128:1304-1309
1 Respiratory Medicine Professor Colin Sullivan 2 3 Modalidade utilizada em 90% dos casos. Thorax 1998 53: 416-18 Lancet 1999 353:2100-05 AJRCCM 2004 169:156-62 AJRCCM 161:857-5-859, 2000 Chest 2005; 128:1304-1309
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
Accuracy and reliability of pulse oximetry in
 Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
CPT Pediatric Coding Updates 2009. The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009.
 CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
Mechanical Ventilation
 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
From AARC Protocol Committee; Subcommittee Adult Critical Care Version 1.0a (Sept., 2003), Subcommittee Chair, Susan P. Pilbeam
 AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
2008 Coding Questions and Answers
 2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
Management of Infants with BPD: Evidence-Based or Eminence-Based?
 Management of Infants with BPD: Evidence-Based or Eminence-Based? Steven M. Donn, MD, FAAP Professor of Pediatrics Division of Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan
Management of Infants with BPD: Evidence-Based or Eminence-Based? Steven M. Donn, MD, FAAP Professor of Pediatrics Division of Neonatal-Perinatal Medicine C.S. Mott Children s Hospital University of Michigan
Respiratory Therapist Program Description
 Program Description Respiratory Therapy is a health profession that specializes in the evaluation, treatment, education and rehabilitation of patients with lung and heart disease, under the direction of
Program Description Respiratory Therapy is a health profession that specializes in the evaluation, treatment, education and rehabilitation of patients with lung and heart disease, under the direction of
CONTENTS. Note to the Reader 00. Acknowledgments 00. About the Author 00. Preface 00. Introduction 00
 Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS
 ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
Colorado Cardiac Conference: 2 nd teaching workshop. Proactive Respiratory Therapy in postoperative Cardiac Patients
 Colorado Cardiac Conference: 2 nd teaching workshop Proactive Respiratory Therapy in postoperative Financial Disclosures Donald Fritz, RT Jerrold Judd, RT No relevant financial relationships with any commercial
Colorado Cardiac Conference: 2 nd teaching workshop Proactive Respiratory Therapy in postoperative Financial Disclosures Donald Fritz, RT Jerrold Judd, RT No relevant financial relationships with any commercial
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide
 Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
Overall Goals/Objectives - Surgical Critical Care Residency Program The goal of the Pediatric Surgical Critical Care Residency program is to provide advanced proficiency in the care and management of critically
Respiratory Therapy Program Technical Standards
 Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support
 Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
SAMPLE. Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management ICD-10
 Coding and Payment Guide www.optumcoding.com Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2017 a ICD10 A full suite of resources including
Coding and Payment Guide www.optumcoding.com Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2017 a ICD10 A full suite of resources including
10/2/2012. D04: Help Nurses Help the Smallest Patients: How Infant Care is Reorganized Tuesday, October 2, 2012 3:30 PM - 4:30 PM
 D04: Help Nurses Help the Smallest Patients: How Infant Care is Reorganized Tuesday, October 2, 2012 3:30 PM - 4:30 PM Presenters Richard M. Katz M.D., MBA, Vice-President, Medical Affairs, Mount Washington
D04: Help Nurses Help the Smallest Patients: How Infant Care is Reorganized Tuesday, October 2, 2012 3:30 PM - 4:30 PM Presenters Richard M. Katz M.D., MBA, Vice-President, Medical Affairs, Mount Washington
NICU Level of Care Criteria
 Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
How To Be A Medical Flight Specialist
 Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Outside Patient Transfers. National Pediatric Nighttime Curriculum Written by Erin Augustine, MD Lucile Packard Children s Hospital at Stanford
 Outside Patient Transfers National Pediatric Nighttime Curriculum Written by Erin Augustine, MD Lucile Packard Children s Hospital at Stanford Case 1 A 5 year old male is being transferred from an outside
Outside Patient Transfers National Pediatric Nighttime Curriculum Written by Erin Augustine, MD Lucile Packard Children s Hospital at Stanford Case 1 A 5 year old male is being transferred from an outside
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
TRANSPORT OF CRITICALLY ILL PATIENTS
 TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
Respiratory Care Technology (RC)
 Cincinnati State 1 Cincinnati State offers a comprehensive program in Respiratory Technology. Students develop a wide range of clinical skills in traditional and nontraditional roles and gain proficiency
Cincinnati State 1 Cincinnati State offers a comprehensive program in Respiratory Technology. Students develop a wide range of clinical skills in traditional and nontraditional roles and gain proficiency
Neonatal Intensive Care Unit (NICU)
 Neonatal Intensive Care Unit (NICU) Integrated Care for Newborns with Critical or Special Needs startstrongbaby.org A World Leader in Neonatal Research and Care Innovation As a birthplace of modern neonatology
Neonatal Intensive Care Unit (NICU) Integrated Care for Newborns with Critical or Special Needs startstrongbaby.org A World Leader in Neonatal Research and Care Innovation As a birthplace of modern neonatology
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT
 2012 STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT Department of Health and Human Services Division of Public Health Licensure Unit 301 Centennial Mall South, Third Floor PO Box
2012 STATE OF NEBRASKA STATUTES RELATING TO RESPIRATORY CARE PRACTICE ACT Department of Health and Human Services Division of Public Health Licensure Unit 301 Centennial Mall South, Third Floor PO Box
The Turkish Journal of Pediatrics 2008; 50: 354-358
 The Turkish Journal of Pediatrics 2008; 50: 354-358 Original Comparing body temperature measurements by mothers and physicians using mercury-in-glass, digital mercury and infrared tympanic membrane thermometers
The Turkish Journal of Pediatrics 2008; 50: 354-358 Original Comparing body temperature measurements by mothers and physicians using mercury-in-glass, digital mercury and infrared tympanic membrane thermometers
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii
 Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
The Heart Center Neonatology. Congenital Heart Disease Screening Program
 The Heart Center Neonatology Congenital Heart Disease Screening Program Our goal is simple. We want all infants with critical congenital heart disease to be identified before leaving the nursery. Together,
The Heart Center Neonatology Congenital Heart Disease Screening Program Our goal is simple. We want all infants with critical congenital heart disease to be identified before leaving the nursery. Together,
National Learning Objectives for COPD Educators
 National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
The aero-medical transfer of neonates and children
 The aero-medical transfer of neonates and children Andrew C Argent Red Cross War Memorial Children s Hospital and University of Cape Town introduction context why transfer neonates and children? are children
The aero-medical transfer of neonates and children Andrew C Argent Red Cross War Memorial Children s Hospital and University of Cape Town introduction context why transfer neonates and children? are children
COURSE SYLLABUS RC 223 CLINICAL-3
 COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Title 32: PROFESSIONS AND OCCUPATIONS
 Title 32: PROFESSIONS AND OCCUPATIONS Chapter 97: RESPIRATORY CARE PRACTITIONERS Table of Contents Section 9701. DECLARATION OF PURPOSE... 3 Section 9702. DEFINITIONS... 3 Section 9703. BOARD OF RESPIRATORY
Title 32: PROFESSIONS AND OCCUPATIONS Chapter 97: RESPIRATORY CARE PRACTITIONERS Table of Contents Section 9701. DECLARATION OF PURPOSE... 3 Section 9702. DEFINITIONS... 3 Section 9703. BOARD OF RESPIRATORY
2006-2007 CATALOG ADDENDUM
 Page 11 2006-2007 CATALOG ADDENDUM Credit by Examination for Introduction to Computer Concepts Credit by examination will be granted to students, who successfully complete a computerized true/false, multiple
Page 11 2006-2007 CATALOG ADDENDUM Credit by Examination for Introduction to Computer Concepts Credit by examination will be granted to students, who successfully complete a computerized true/false, multiple
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Year in review: mechanical ventilation
 Year in review: mechanical ventilation Leo Heunks, MD, PhD Pulmonary and Critical Care Physician Dept of Critical Care Intensivisten dagen 2013 Disclosures Maquet (NAVA catheters, travel fee, speakers
Year in review: mechanical ventilation Leo Heunks, MD, PhD Pulmonary and Critical Care Physician Dept of Critical Care Intensivisten dagen 2013 Disclosures Maquet (NAVA catheters, travel fee, speakers
Acknowledgements. PAH in Children: Natural History. The Sildenafil Saga
 The Sildenafil Saga David L. Wessel, MD Executive Vice President Chief Medical Officer Ikaria Distinguished Professor of Critical Care Children s National Medical Center Washington, DC, USA Acknowledgements
The Sildenafil Saga David L. Wessel, MD Executive Vice President Chief Medical Officer Ikaria Distinguished Professor of Critical Care Children s National Medical Center Washington, DC, USA Acknowledgements
Protocols for Early Extubation After Cardiothoracic Surgery
 Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
Sample Consent. Transfusion of Prematures (TOP)
 Final: October 8. 2012 Revised: February 8. 2013 Appendix A: Sample Consent ~ Penn Medicine,~. Informed Consent Form and HIPAA Authorization Protocol Title: Short Title: Principal Investigator: Emergency
Final: October 8. 2012 Revised: February 8. 2013 Appendix A: Sample Consent ~ Penn Medicine,~. Informed Consent Form and HIPAA Authorization Protocol Title: Short Title: Principal Investigator: Emergency
Charles Samuel Cox, Jr.
 February 2014 Charles Samuel Cox, Jr. Present Position: in Neurosciences, Professor of Pediatric Surgery, Pediatrics and Biomedical Engineering, at Houston Director for Molecular Medicine Co-Director,
February 2014 Charles Samuel Cox, Jr. Present Position: in Neurosciences, Professor of Pediatric Surgery, Pediatrics and Biomedical Engineering, at Houston Director for Molecular Medicine Co-Director,
HLTEN609B Practise in the respiratory nursing environment
 HLTEN609B Practise in the respiratory nursing environment Release: 1 HLTEN609B Practise in the respiratory nursing environment Modification History Not Applicable Unit Descriptor Descriptor This unit addresses
HLTEN609B Practise in the respiratory nursing environment Release: 1 HLTEN609B Practise in the respiratory nursing environment Modification History Not Applicable Unit Descriptor Descriptor This unit addresses
Active Rehabilitation and Physical Therapy During Extracorporeal Membrane Oxygenation While Awaiting Lung Transplantation
 Active Rehabilitation and Physical Therapy During Extracorporeal Membrane Oxygenation While Awaiting Lung Transplantation David A Turner MD 1, David Zaas MD MBA 2, Kyle J Rehder MD 1, W Lee Williford RRT
Active Rehabilitation and Physical Therapy During Extracorporeal Membrane Oxygenation While Awaiting Lung Transplantation David A Turner MD 1, David Zaas MD MBA 2, Kyle J Rehder MD 1, W Lee Williford RRT
9/12/2011 OBJECTIVES BREATH OF LIFE. Review the role that Potentially Better Practices (PBP s) play in clinical practice
 Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse
 Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
Pediatrix Medical Group BabySteps and the Clinical Data Warehouse Pediatrix Medical Group Reese H Clark MD Dan Ellsbury MD Alan Spitzer MD Duke Clinical Research Institute Brian Smith MD MPH MHS Danny
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Coding Guidelines for Certain Respiratory Care Services July 2014
 Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Objective of This Lecture
 Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.
 BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 info@bpsweb.org www.bpsweb.org Content Outline for the CRITICAL PHARMACY SPECIALTY CERTIFICATION
Critical Care Paramedic Position Statement
 July 2009 I n t e r n a t i o n a l A s s o c i a t i o n o f F l i g h t P a r a m e d i c s Critical Care Paramedic Position Statement BACKGROUND Historically, to practice as a paramedic in the United
July 2009 I n t e r n a t i o n a l A s s o c i a t i o n o f F l i g h t P a r a m e d i c s Critical Care Paramedic Position Statement BACKGROUND Historically, to practice as a paramedic in the United
High Frequency Ventilation Introductory Information
 High-Frequency Oscillatory Ventilation Learning Objectives: Explain the indications, rationale and monitoring for HFOV. Explain the effects of adjusting HFOV ventilator controls. Arthur Jones EdD, RRT
High-Frequency Oscillatory Ventilation Learning Objectives: Explain the indications, rationale and monitoring for HFOV. Explain the effects of adjusting HFOV ventilator controls. Arthur Jones EdD, RRT
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
USE OF BUSINESS PROCESS MANAGEMENT TECHNOLOGY AND LEAN TO IMPROVE CARE
 USE OF BUSINESS PROCESS MANAGEMENT TECHNOLOGY AND LEAN TO IMPROVE CARE Andrew Steele, MD, MPH, MSc Director of Medical Informatics Denver Health ehealth Services 660 Bannock St. Denver, CO 80204 Deborah
USE OF BUSINESS PROCESS MANAGEMENT TECHNOLOGY AND LEAN TO IMPROVE CARE Andrew Steele, MD, MPH, MSc Director of Medical Informatics Denver Health ehealth Services 660 Bannock St. Denver, CO 80204 Deborah
RESPIRATORY THERAPIST CLASSIFICATION SERIES
 STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 I. INTRODUCTION
STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 I. INTRODUCTION
PULMONARY PHYSIOLOGY
 I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Understanding Stroke Volume Variation and Its Clinical Application
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Hospital Coding Making the Rounds
 Hospital Coding Making the Rounds Initial & Subsequent Care, Consults, Discharges, Observation and Critical Care Objectives Participants will be educated on the documentation requirements for Initial and
Hospital Coding Making the Rounds Initial & Subsequent Care, Consults, Discharges, Observation and Critical Care Objectives Participants will be educated on the documentation requirements for Initial and
British Association of Perinatal Medicine. The Management of Babies born Extremely Preterm at less than 26 weeks of gestation
 Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
