Office/Outpatient Evaluation and Management Services Reference Guide and Clinical Examples
|
|
|
- Alfred Nash
- 3 years ago
- Views:
Transcription
1 Office/Outpatient Evaluation and Management Services Reference Guide and Clinical Examples January 2021 Developed by the IDSA Clinical Affairs Committee E/M Work Group: Drs. Ron Devine (chair), John Fangman, Nilesh Hingarh, Alice Kim, Prashant Malhotra and Matt Shoemaker Section One: Overview and Introduction to Concepts Revisions to E/M Services CPT Codes On Jan. 1, 2021, revised office/outpatient visit E/M CPT codes ( ) and associated documentation went into effect. The revised codes are the culmination of collaboration among the Centers for Medicare & Medicaid Services, American Medical Association and other medical specialty societies, including IDSA. The changes to these codes were the start of a multi-year, multi-phase AMA project to revise nearly all the CPT E/M code set. The revisions are long overdue, as the codes were established nearly 20 years ago and, in that time, patient care along with how to document that care has changed. Reducing provider burden by decreasing charting requirements was also a primary driver for the revision of the codes. Office or Other Outpatient E/M Services CPT Codes The E/M visit CPT codes (new and established patients) were revised to decrease documentation and coding administrative burden and to ensure that E/M payment is resource-based. The revisions remove the history and physical examination as key components in choosing the appropriate E/M level of a visit. Now, code level selection for an E/M service performed is based on medical decision-making (MDM) or total time. Summary of Revisions The revisions to the E/M documentation guidelines are only applicable to the office/outpatient new patient and established patient visit E/M codes ( ). For all other E/M services performed, such as consultations, inpatient E/M, observation E/M and critical care, services will continue to be governed by the existing E/M documentation guidelines and CPT instructions. The history and physical exam elements of a visit are not required when making a code level selection. However, one should still perform and document these elements when medically appropriate. The level of code selection is based on medical decision-making or total time on the date of the encounter. Medical decision-making is based on three elements: o Number and complexity of problems addressed; o Amount or complexity of data to be reviewed and interpreted; o Level of risk of complications and morbidity/mortality. The definition of total time includes face-to-face and non-face-to-face time on the date of encounter spent by the provider, including time reviewing medical records; reviewing tests; reviewing or obtaining a medical history; ordering medications, tests and procedures; documentation in the electronic health record; and communication with the patient, family members and caregivers. Documentation of time spent is only required when time is used to choose the code level. CPT code has been deleted.
2 Section Two: Descriptions, Definitions and Elements of Medical Decision Table Risk of Complications and Morbidity or Mortality of Patient Management Risk of complications and/or morbidity or mortality of patient management decisions made at the visit, associated with the patient s problem(s) and treatment(s): Includes possible management options selected and those considered but not selected; Addresses risks associated with social determinants of health. Two of three elements must be met or exceeded when selecting the code level. For example, if a new patient encounter involves a low level of MDM, a limited review of data and a low level of risk, the code selected should be Table 1 below provides information on these elements for some of the more commonly used CPT codes. Table 1: Abbreviated Table of Code Level Selection CPT Codes Level of MDM Number and/or Complexity of Problems Addressed Amount and/or Complexity of Data Reviewed and Analyzed 99202, Straightforward Minimal Minimal or None Minimal 99203, Limited 99204, , Extensive Medical Decision-Making MDM is composed of three elements: 1. Number and complexity of problems addressed at encounter; 2. Amount and/or complexity of data reviewed/analyzed; 3. Risk of complications, morbidity and/or mortality of patient management decisions. Risk of Complications and/or Morbidity/Mortality There are four types of MDM (Straightforward,,, and ). The level of MDM is chosen based on meeting or exceeding two of the three MDM elements. Table 2 below defines the types of complexity of clinically relevant problems addressed at the encounter. The number and complexity of problems addressed at a patient encounter is a vital component when choosing the code level. Table 2: Medical Decision-Making Complexity Definition Straightforward Self-limited Stable, uncomplicated, single problem Multiple problems or significantly ill Very ill
3 Table 3 highlights categories of data that are reviewed or interpreted during a patient encounter, and Table 4 provides information on which code should be selected based on total time spent on the date of the encounter for new and established patients. Table 3: Amount and Complexity of Data Reviewed and Interpreted Category 1 Tests, Documents, Orders or Independent Historian Category 2 Independent Interpretation of Tests Category 3 Discussion of Management or Test Interpretation Table 4: Total Time Spent on the Date of the Encounter (New and Established Patient) New Patient E/M CPT Code Total Time minutes minutes minutes minutes Established Patient E/M CPT Code Total Time Time component removed minutes minutes minutes minutes For more detail, visit the CPT E/M Office Revisions Level of Decision Making. The table depicts the levels of medical decision-making coupled with the associated complexity and problems addressed, the elements required of medical decision-making for each code level and the level of risk associated with a patient encounter. The table was developed by the American Medical Association CPT Editorial Panel to assist with proper coding of office visit E/M services.
4 Description of Total Time For office/outpatient E/M visits, the element of coding by time has been changed from counting only face-to-face time when counseling and/or coordination of time dominated the visit (greater than 50% of the time to total time on the date of the encounter) to now include non-face-to-face time. The total time includes all activities related to the patient visit on the date of the encounter and includes: Preparing to see patient (e.g., review tests, medical records); Obtaining history; Performing a medically appropriate physical examination; Counseling and education (patient, family member, caregiver); Ordering medications, tests and procedures; Referring and communicating to other health care professionals; Documenting the encounter; Independent interpretation of tests (when not separately reported); Care coordination (when not separately reported). Total time does not include any activities or time spent other than on the date of the encounter. To bill by time, the total time spent on patient care activities on the date of the encounter should be documented as well as activities performed. Time spent with normal activities by clinical staff and time spent on a date other than the date of encounter should not be used to calculate total time. For shared or split visits between a physician and other qualified health care provider, such as advanced practice providers, time spent separately on the date of the encounter may be summed to equal total time, but time spent doing the same task may only be counted by one provider. Refer to Table 4 for time requirements for each level of E/M CPT code when total time is used to make the code level determination. Prolonged Service Time New CPT Code CPT code is used to report additional time beyond the time periods required for office/outpatient E/M visits. Additional time includes face-to-face and non-face-to-face activities. Code may only be used when total time has been used to select the appropriate E/M visit and the highest E/M level has been achieved (i.e., or 99215). CPT code is parsed into 15-minute increments and may be used only when the total time on the date of the encounter exceeds the minimal time for the highest-level E/M visit by 15 minutes. For example, a provider spends a total time of 83 minutes with a new patient. The time limits for a new outpatient visit E/M visit is minutes. The 83 minutes is 23 minutes beyond the minimal time limit of of 60 minutes, and therefore the provider can bill CPT code For each additional 15 minutes, code may be reported. Tables 6 and 7 below provide guidance on which code(s) may be reported for new and established patient E/M services, respectively, based on service time. Table 6: Using Code with New Patient E/M Use with (New Patient) Code(s) Reported Less than 75 minutes Use appropriate E/M code minutes x1 AND x1
5 minutes x1 AND x2 105 minutes or more x1 AND x3 or more for each additional 15 minutes Table 7: Using Code with Established Patient E/M Use with (Established Patient) Less than 55 minutes Code(s) Reported Use appropriate E/M code minutes x1 AND x minutes x1 AND x2 85 minutes or more x1 AND x3 or more for each additional 15 minutes
6 Section Three: Clinical Examples of Code Level Selection The following clinical examples build on a base-level patient who is 65 years old with congestive heart failure, diabetes mellitus and hypertension. Patient presents with a problem in their leg. For each example, the severity of the patient s problem progresses, therefore indicating a higher level of MDM. MDM includes an increase in the number or complexity of problems to be assessed along with review of increasing amounts of complex data and an increase in the level of risk. The notes of the case are presented first, followed by the MDM table highlighting (in red) the elements that were considered when choosing the code level. As noted previously, E/M code level selection is now based on medical decision-making or time. In the clinical examples that follow, for examples 1-4 medical decision-making was used to select the code level and for example 5 time was used to select the code level. Tables adapted from the AMA CPT Table of Medical Decision Making. Copyright of the American Medical Association. All rights reserved.
7 Clinical Example #1: CPT Code Level (New Patient)/99212 (Established Patient) Patient is a 65 yo with CHF, DM and HTN. Patient presents with leg swelling and erythema. There is no tenderness. Exam indicates signs of stasis and but no cellulitis. Advised patient to perform leg elevation and to schedule follow-up visit with primary care physician for possible adjustment of CHF medication. No antimicrobials were prescribed. Follow-up as needed. Medical decision-making for this case is a straightforward review of a single self-limiting problem, with review of minimal data and a minimal level of risk; therefore, code level or is indicated. CPT Code MDM Level Straightforward Problems (Number and Complexity) 1 self-limited problem or minor problem > 2 self-limited/minor problems 1 stable chronic illness 1 acute, uncomplicated illness or injury >1 chronic problem with progression/exacerbation/adverse effects of treatment >2 stable chronic illnesses 1 undiagnosed new problem with uncertain prognosis 1 new problem or acute illness + systemic symptoms 1 acute complicated injury Minimal or none Data Reviewed Limited (must meet requirements of at least 1 of the 2 categories) 2 of 3 of ordering test, review of results or prior external note Assessment requiring an independent historian (must meet the requirements of at least 1 of the 3 categories) Independent historian y Independently review and interpret test/radiology Minimal Level of Risk Examples: Prescription management Decision for minor surgery Decision for elective major surgery without risk factors, diagnosis and treatment limited by social determinants of health >1 chronic illness with severe progression/exacerbation/adverse effects or treatment 1 acute or chronic illness or injury that poses threat to life or body function Extensive (must meet the requirements of at least 2 of the 3 categories) Independent historian Independently review and interpret test/radiology Intensive drug toxicity monitoring Elective surgery with risk factor Emergency surgery Hospitalization Advance care directives
8 Clinical Example #2: CPT Code Level (New Patient)/99213 (Established Patient) Patient is a 65 yo with CHF, DM and HTN. Patient presents with leg swelling and erythema that began four days ago. Patient indicates there is some pain in the leg and is feeling feverish; however, vital signs show no fever. Exam is suggestive of non-purulent cellulitis. Review of prior records from PCP is performed and there is no history of methicillin-resistant Staphylococcus aureus indicated in the patient record or in any cultures performed. The patient indicates no allergies and is prescribed a five-day course of Keflex and asked to follow-up with the ID physician in seven days. Medical decision-making for this case is low-level with review of a single, acute, uncomplicated problem which involved the review of a prior external note and tests. Even though moderate risk level could be met, since two of the three elements are needed, code level or is indicated. CPT Code MDM Level Problems (Number and Complexity) Data Reviewed Straightforward 1 self-limited problem or minor problem Minimal or none Minimal > 2 self-limited/minor problems 1 stable chronic illness 1 acute, uncomplicated illness or injury >1 chronic problem with progression/exacerbation/adverse effects of treatment >2 stable chronic illnesses 1 undiagnosed new problem with uncertain prognosis 1 new problem or acute illness + systemic symptoms 1 acute complicated injury >1 chronic illness with severe progression/exacerbation/adverse effects or treatment 1 acute or chronic illness or injury that poses threat to life or body function Limited (must meet requirements of at least 1 of the 2 categories) 2 of 3 of ordering tests, review of results or prior external note Assessment requiring an independent historian (must meet the requirements of at least 1 of the 3 categories) Independent historian Independently review and interpret test/radiology Extensive (must meet the requirements of at least 2 of the 3 categories) Independent historian Independently review and interpret test/radiology Level of Risk Examples: Prescription management Decision for minor surgery Decision for elective major surgery without risk factors, diagnosis and treatment limited by social determinants of health Intensive drug toxicity monitoring Elective surgery with risk factor Emergency surgery Hospitalization Advance care directives
9 Clinical Example #3: CPT Code Level (New Patient)/99214 (Established Patient) Patient is a 65 yo with CHF, DM and HTN. Patient presents with leg swelling and erythema that began four days ago. Patient indicates there is some pain in the leg and is feeling feverish; however, there is no fever on vital signs. Exam is suggestive of purulent cellulitis. Records from PCP are reviewed and reveal history of MRSA. The patient indicates no allergies. A complete blood count, comprehensive metabolic panel and a wound culture are ordered. The patient is prescribed five days of oral doxycycline. Adverse effects of doxycycline are discussed with the patient. The case and management are also discussed with patient s PCP. Patient is to return to office in one week or sooner if problem worsens. Medical decision-making for this case has now progressed to a moderate level. The problem is now a single new problem that involved discussion with another provider and review of historical records. The risk has now increased to a moderate level given the patient was given a prescription that may often lead to side effects; therefore, code level or is indicated. CPT Code MDM Level Problems (Number and Complexity) Data Reviewed Straightforward 1 self-limited problem or minor problem Minimal or none Minimal > 2 self-limited/minor problems 1 stable chronic illness 1 acute, uncomplicated illness or injury >1 chronic problem with progression/exacerbation/adverse effects of treatment >2 stable chronic illnesses 1 undiagnosed new problem with uncertain prognosis 1 new problem or acute illness + systemic symptoms 1 acute complicated injury >1 chronic illness with severe progression/exacerbation/adverse effects or treatment 1 acute or chronic illness or injury that poses threat to life or body function Limited (must meet requirements of at least 1 of the 2 categories) 2 of 3 of ordering tests, review of results or prior external note Assessment requiring and independent historian (must meet the requirements of at least 1 of the 3 categories) Independent historian Independently review and interpret test/radiology Extensive (must meet the requirements of at least 2 of the 3 categories) Independent historian Independently review and interpret test/radiology Level of Risk Examples: Prescription management Decision for minor surgery Decision for elective major surgery without risk factors, diagnosis and treatment limited by social determinants of health Intensive drug toxicity monitoring Elective surgery with risk factor Emergency surgery Hospitalization Advance care directives
10 Clinical Example #4: CPT Code Level (New Patient)/99215 (Established Patient) Patient is a 65 yo with CHF, DM and HTN. Patient presents with leg swelling and erythema that began four days ago. Patient indicates there is pain in the leg. The patient is feeling very sick and is unable to provide a history. The patient s daughter is called and indicates that patient has had a fever, malaise and severe leg pain. Exam indicates a patient who appears very sick and has leg erythema and severe tenderness. Patient has no allergies. Vital signs reveal hypotension and tachycardia. Decision is made to send patient to the emergency room for hospitalization and emergent surgical evaluation for possible necrotizing fasciitis. CBC, CMP and blood cultures are ordered. It is recommended that patient is started on IV vancomycin and piperacillin-tazobactam with vancomycin level monitoring. The case is discussed with the ER and surgical attending physicians. Patient is transported to the ER for admission. Medical decision-making for this case is at the highest level given that the patient has a very complex problem that could threaten life or body function. The data reviewed is now more complicated in nature and involves speaking with an independent historian (the patient s daughter), ordering tests and discussions with other providers. The risk has now increased to the high level given the patient needs to be hospitalized and started on IV antibiotics, and there is consideration of emergency surgery; therefore, code level or is indicated. CPT Code MDM Level Straightforward Problems (Number and Complexity) 1 self-limited problem or minor problem > 2 self-limited/minor problems 1 stable chronic illness 1 acute, uncomplicated illness or injury >1 chronic problem with progression/exacerbation/adverse effects of treatment >2 stable chronic illnesses 1 undiagnosed new problem with uncertain prognosis 1 new problem or acute illness + systemic symptoms 1 acute complicated injury Minimal or none Data Reviewed Limited (must meet requirements of at least 1 of the 2 categories) of 2 of 3 of ordering tests, review of results or prior external note Assessment requiring and independent historian (must meet the requirements of at least 1 of the 3 categories) Independent historian Independently review and interpret test/radiology Minimal Level of Risk Examples: Prescription management Decision for minor surgery Decision for elective major surgery without risk factors, diagnosis and treatment limited by social determinants of health >1 chronic illness with severe progression/exacerbation/adverse effects or treatment 1 acute or chronic illness or injury that poses threat to life or body function Extensive (must meet the requirements of at least 2 of the 3 categories) Independent historian Independently review and interpret test/radiology Intensive drug toxicity monitoring Elective surgery with risk factor Emergency surgery Hospitalization Advance care directives
11 Clinical Example #5: Using Time to Select Code Level A 58 yo male established patient with venous insufficiency and chronic edema of both legs presents with complaint of redness and pain in the right lower leg. Examination notes cellulitis of the right lower leg without any open wounds or ulcers noted as well as no abscesses or purulence identified. Patient was prescribed cephalexin and instructed to elevate his right leg. Provider also discusses with the patient the importance of elevating his leg to decrease edema to facilitate resolution of the cellulitis. Discussion also included instructions to get compression stockings and proper wear of and care for compression stockings. Total time for patient care on the date of encounter was 34 minutes. As total time of visit on date of encounter is 34 minutes, this meets the time requirement of CPT 99214, which ranges from minutes. The code to report is In this case, while the MDM was low, the actual time devoted to the patient was high, therefore using time to select the code level is a more accurate description and more appropriate way to value the physician s services.
12 Section Four: Additional Resources E/M Coding and Documentation Resources AMA E/M CPT Code Resources AMA is the official source of CPT code information and guidelines. This website provides information on the revised E/M codes and provides a learning module to assist physicians and their staff in navigating those changes. CMS Evaluation and Management Services Guide This guide from the Centers for Medicare & Medicaid Services is a comprehensive guide issued by CMS to educate providers on the appropriate use of E/M codes and the associated documentation. The guide has been updated to include the revisions to the office visit E/M codes. To assist with questions regarding CPT coding or other reimbursement issues, IDSA offers Ask the Coder. This service is available to IDSA members to aid in understanding and resolving medical coding issues. For more information and general inquiries, contact IDSA staff via clinicalaffairs@idsociety.org. Disclaimer: CPT Copyright 2021 American Medical Association. All rights reserved. CPT is a registered trademark of the American Medical Association. Given the inherent subjectivity of choosing the most appropriate CPT code or HCPCS code for services provided to patients, the material provided within this document is for informational and educational purposes only. Readers must use their independent, professional judgment in making coding decisions. IDSA assumes no risk in providing coding information and all risks are assumed by the provider, physician or other qualified health care professional.
Documentation Guidelines for Physicians Interventional Pain Services
 Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
E/M Learning Tips INTRODUCTION TO EVALUATION. Introduction to Evaluation and Management (E/M) Coding for the Child and Adolescent Psychiatrist
 INTRODUCTION TO EVALUATION AND MANAGEMENT (E/M) CODING FOR THE CHILD AND ADOLESCENT PSYCHIATRIST Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy
INTRODUCTION TO EVALUATION AND MANAGEMENT (E/M) CODING FOR THE CHILD AND ADOLESCENT PSYCHIATRIST Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy
Medical Decision Making
 Disclaimer This presentation is intended only for use by Tulane University faculty, staff, and students. No copy or use of this presentation should occur without the permission of Tulane University. Tulane
Disclaimer This presentation is intended only for use by Tulane University faculty, staff, and students. No copy or use of this presentation should occur without the permission of Tulane University. Tulane
Current Procedural Terminology (CPT) Code Changes for 2013
 Current Procedural Terminology (CPT) Code Changes for 2013 For 2013 there have been major changes to the codes in the Psychiatry section of the AMA s Current Procedural Terminology, the codes that must
Current Procedural Terminology (CPT) Code Changes for 2013 For 2013 there have been major changes to the codes in the Psychiatry section of the AMA s Current Procedural Terminology, the codes that must
Billing and Coding Conference
 Billing and Coding Conference February 26 th 2013 Agenda 1. Hospital Medicine Coding Pattern 2. Tips to maximize individual billing 3. Billing audit 4..SPLITSHAREDNPPVISIT 5. Basic Coding Guidelines focus
Billing and Coding Conference February 26 th 2013 Agenda 1. Hospital Medicine Coding Pattern 2. Tips to maximize individual billing 3. Billing audit 4..SPLITSHAREDNPPVISIT 5. Basic Coding Guidelines focus
CPT Coding Changes for 2013
 CPT Coding Changes for 2013 Getting Prepared Presenter Ronald Burd, MD Psychiatrist, Stanford Health, Fargo, ND Chair, APA Committee on Codes, RBRVS and Reimbursements APA Representative, AMA s RBRVS Update
CPT Coding Changes for 2013 Getting Prepared Presenter Ronald Burd, MD Psychiatrist, Stanford Health, Fargo, ND Chair, APA Committee on Codes, RBRVS and Reimbursements APA Representative, AMA s RBRVS Update
Part 1 General Issues in Evaluation and Management (E&M) in Headache
 AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 1 General Issues in Evaluation and Management (E&M) in Headache By better understanding the Evaluation and
AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 1 General Issues in Evaluation and Management (E&M) in Headache By better understanding the Evaluation and
AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding
 AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 3 - Medical Decision Making (MDM) coding in Headache As stated in the CPT codebook, the classification of
AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 3 - Medical Decision Making (MDM) coding in Headache As stated in the CPT codebook, the classification of
Coding for Evaluation and Management Services
 Coding for Evaluation and Management Services Joanne Mehmert, CPC Joanne Mehmert & Associates, LLC fmeh@aol.com 2006 CPT E&M Updates May 2006 2 1 E&M Deleted Codes Deleted codes 99261-99263 Follow-up consultation
Coding for Evaluation and Management Services Joanne Mehmert, CPC Joanne Mehmert & Associates, LLC fmeh@aol.com 2006 CPT E&M Updates May 2006 2 1 E&M Deleted Codes Deleted codes 99261-99263 Follow-up consultation
99213 or 99214 Visit?
 JUST HOW MUCH DOCUMENTATION IS REQUIRED 1 99213 or 99214 Visit? Presented by: Leslie C. Bembry CPC Coding and Compliance Manager Montgomery Hospital Health Systems Fornance Physician Services Inc. Norristown
JUST HOW MUCH DOCUMENTATION IS REQUIRED 1 99213 or 99214 Visit? Presented by: Leslie C. Bembry CPC Coding and Compliance Manager Montgomery Hospital Health Systems Fornance Physician Services Inc. Norristown
KINDRED HEALTHCARE. Billing & Coding for SNF Physician Visits. KINDRED HEALTHCARE Continue the Care
 KINDRED HEALTHCARE Billing & Coding for SNF Physician Visits KINDRED HEALTHCARE Continue the Care 1 SNF CPT Codes Initial Care Services 99304 99305 99306 Subsequent Care Services 99307 99308 99309 99310
KINDRED HEALTHCARE Billing & Coding for SNF Physician Visits KINDRED HEALTHCARE Continue the Care 1 SNF CPT Codes Initial Care Services 99304 99305 99306 Subsequent Care Services 99307 99308 99309 99310
E&M Coding- It s All About The Documentation
 E&M Coding- It s All About The Documentation Presented for Anthem Blue Cross and Blue Shield By: Penny Osmon, BA, CPC Coding & Reimbursement Educator WI Medical Society Wisconsin Medical Society, Copyright
E&M Coding- It s All About The Documentation Presented for Anthem Blue Cross and Blue Shield By: Penny Osmon, BA, CPC Coding & Reimbursement Educator WI Medical Society Wisconsin Medical Society, Copyright
Step 2 Use the Medical Decision-Making Table
 Step 2 Use the Medical Decision-Making Table In Step 1, we determined the patient location and patient type. For most patient encounters, this determines the first 4 digits of the 5-digit CPT code. Three
Step 2 Use the Medical Decision-Making Table In Step 1, we determined the patient location and patient type. For most patient encounters, this determines the first 4 digits of the 5-digit CPT code. Three
Hot Topics in E & M Coding for the ID Practice
 Hot Topics in E & M Coding for the ID Practice IDSA Webinar February, 2010 Barb Pierce, CCS-P, ACS-EM Consulting, LLC barbpiercecoder@aol.com www.barbpiercecodingandconsulting.com Disclaimer This information
Hot Topics in E & M Coding for the ID Practice IDSA Webinar February, 2010 Barb Pierce, CCS-P, ACS-EM Consulting, LLC barbpiercecoder@aol.com www.barbpiercecodingandconsulting.com Disclaimer This information
Evaluation & Management. Guidelines. Presented by: Kristi A. Gutierrez CCS-P, CPC, CEMC
 Evaluation & Management Documentation and Coding Guidelines Presented by: Kristi A. Gutierrez CCS-P, CPC, CEMC Objectives Participants will gain a working knowledge of Medicare s 1995 Evaluation & Management
Evaluation & Management Documentation and Coding Guidelines Presented by: Kristi A. Gutierrez CCS-P, CPC, CEMC Objectives Participants will gain a working knowledge of Medicare s 1995 Evaluation & Management
Payment Policy. Evaluation and Management
 Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Question and Answer Submissions
 AACE Endocrine Coding Webinar Welcome to the Brave New World: Billing for Endocrine E & M Services in 2010 Question and Answer Submissions Q: If a patient returns after a year or so and takes excessive
AACE Endocrine Coding Webinar Welcome to the Brave New World: Billing for Endocrine E & M Services in 2010 Question and Answer Submissions Q: If a patient returns after a year or so and takes excessive
New Patient Visit. UnitedHealthcare Medicare Reimbursement Policy Committee
 New Patient Visit Policy Number NPV04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 12/16/2015 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to
New Patient Visit Policy Number NPV04242013RP Approved By UnitedHealthcare Medicare Committee Current Approval Date 12/16/2015 IMPORTANT NOTE ABOUT THIS REIMBURSEMENT POLICY This policy is applicable to
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Forms designed to collect this information will help staff collect all pertinent information.
 1 CPT AUDIT TOOL INSTRUCTIONS The Nursing Consultants from the Public Health Nursing and Professional Development Unit based on multiple Evaluation & Management audits across the state have developed these
1 CPT AUDIT TOOL INSTRUCTIONS The Nursing Consultants from the Public Health Nursing and Professional Development Unit based on multiple Evaluation & Management audits across the state have developed these
E/M Documentation Auditors Worksheet
 E/M Documentation Auditors Worksheet Patient s ID/MR #: _ Y R Physician s Name and/or ID#: _ Resident yes no Staff Physician s Name and/or ID#(if resident is used): _ Date of Service Billed: Actual Date
E/M Documentation Auditors Worksheet Patient s ID/MR #: _ Y R Physician s Name and/or ID#: _ Resident yes no Staff Physician s Name and/or ID#(if resident is used): _ Date of Service Billed: Actual Date
OBSERVATION CARE EVALUATION AND MANAGEMENT CODES
 REIMBURSEMENT POLICY OBSERVATION CARE EVALUATION AND MANAGEMENT CODES Policy Number: ADMINISTRATIVE 232.8 T0 Effective Date: April, 205 Table of Contents APPLICABLE LINES OF BUSINESS/PRODUCTS... APPLICATION...
REIMBURSEMENT POLICY OBSERVATION CARE EVALUATION AND MANAGEMENT CODES Policy Number: ADMINISTRATIVE 232.8 T0 Effective Date: April, 205 Table of Contents APPLICABLE LINES OF BUSINESS/PRODUCTS... APPLICATION...
Patient Progress Note & Dictation Standard
 Objective: The patient progress note serves as a basis for planning patient care, documenting communication between the health care provider and any other health professional contributing to the patient's
Objective: The patient progress note serves as a basis for planning patient care, documenting communication between the health care provider and any other health professional contributing to the patient's
Observation Care Evaluation and Management Codes Policy
 Policy Number REIMBURSEMENT POLICY Observation Care Evaluation and Management Codes Policy 2016R0115A Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT
Policy Number REIMBURSEMENT POLICY Observation Care Evaluation and Management Codes Policy 2016R0115A Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT
Empire BlueCross BlueShield Professional Reimbursement Policy
 Subject: Documentation and Reporting Guidelines for Evaluation and Management Services NY Policy: 0024 Effective: 12/01/2013-03/31/2014 Coverage is subject to the terms, conditions, and limitations of
Subject: Documentation and Reporting Guidelines for Evaluation and Management Services NY Policy: 0024 Effective: 12/01/2013-03/31/2014 Coverage is subject to the terms, conditions, and limitations of
Modifiers 25 and 59. Modifier 25
 Modifiers 25 and 59 This article discusses the appropriate use of modifier 25, Significant, Separately Identifiable Evaluation and Management Service by the Same Physician on the Same Day of the Procedure
Modifiers 25 and 59 This article discusses the appropriate use of modifier 25, Significant, Separately Identifiable Evaluation and Management Service by the Same Physician on the Same Day of the Procedure
ICD-9 Basics Study Guide
 Board of Medical Specialty Coding ICD-9 Basics Study Guide for the Home Health ICD-9 Basic Competencies Examination Two Washingtonian Center 9737 Washingtonian Blvd., Ste. 100 Gaithersburg, MD 20878-7364
Board of Medical Specialty Coding ICD-9 Basics Study Guide for the Home Health ICD-9 Basic Competencies Examination Two Washingtonian Center 9737 Washingtonian Blvd., Ste. 100 Gaithersburg, MD 20878-7364
Coding for the Internist: The Basics
 Coding for the Internist: The Basics Evaluation and management is the most important part of the practice for an internist and coding for these visits can have an important effect for the bottom line of
Coding for the Internist: The Basics Evaluation and management is the most important part of the practice for an internist and coding for these visits can have an important effect for the bottom line of
Non-Physician Practitioner Services Coding & Reporting. Karla R. Peter, RHIT, CCS, CCS-P, CPC Avera Health September 6, 2013
 Non-Physician Practitioner Services Coding & Reporting Karla R. Peter, RHIT, CCS, CCS-P, CPC Avera Health September 6, 2013 Medical Necessity Overarching Criterion Medicare Claims Processing Manual, Chapter
Non-Physician Practitioner Services Coding & Reporting Karla R. Peter, RHIT, CCS, CCS-P, CPC Avera Health September 6, 2013 Medical Necessity Overarching Criterion Medicare Claims Processing Manual, Chapter
MLN Matters Number: MM5972 Related Change Request (CR) #: 5972. Related CR Transmittal #: R1490CP Implementation Date: July 7, 2008
 The NPI will be Required for all HIPAA Standard Transactions on May 23 rd. As of May 23, 2008, the NPI will be required for all HIPAA standard transactions. This means: - For all primary and secondary
The NPI will be Required for all HIPAA Standard Transactions on May 23 rd. As of May 23, 2008, the NPI will be required for all HIPAA standard transactions. This means: - For all primary and secondary
Determine the Appropriate Level E/M Code Based on the Encounter
 Determine the Appropriate Level E/M Code Based on the Encounter Jeffrey D. Lehrman, DPM, FACFAS, FASPS, FAPWH APMA Coding Committee Expert Panelist, Codingline.com Fellow, American Academy of Podiatric
Determine the Appropriate Level E/M Code Based on the Encounter Jeffrey D. Lehrman, DPM, FACFAS, FASPS, FAPWH APMA Coding Committee Expert Panelist, Codingline.com Fellow, American Academy of Podiatric
E/M and Psychotherapy Coding Algorithm
 Inpatient PHP Outpatient E/M and Psychotherapy Coding Algorithm CPT five-digit codes, descriptions, and other data only are copyright 2012 by the American Medical Association (AMA). All Rights Reserved.
Inpatient PHP Outpatient E/M and Psychotherapy Coding Algorithm CPT five-digit codes, descriptions, and other data only are copyright 2012 by the American Medical Association (AMA). All Rights Reserved.
Coding, billing and documentation tips for effective reimbursement. Beth Milligan, MD, FAAFP, CHCOM, CPE
 Coding, billing and documentation tips for effective reimbursement Beth Milligan, MD, FAAFP, CHCOM, CPE Objectives Explain the importance of clinical documentation Understand the principles of documentation
Coding, billing and documentation tips for effective reimbursement Beth Milligan, MD, FAAFP, CHCOM, CPE Objectives Explain the importance of clinical documentation Understand the principles of documentation
How To Write A Health Insurance Claim Form
 Kim Huey, MJ, CPC, CCS-P, PCS, CPCO President, KGG Coding and Reimbursement Consulting April 16, 2015 Elements of Successful Coding in Your Practice Kim Huey, MJ, CPC, CCS P, PCS, CPCO for Medical Association
Kim Huey, MJ, CPC, CCS-P, PCS, CPCO President, KGG Coding and Reimbursement Consulting April 16, 2015 Elements of Successful Coding in Your Practice Kim Huey, MJ, CPC, CCS P, PCS, CPCO for Medical Association
NEW YORK STATE MEDICAID PROGRAM MIDWIFE PROCEDURE CODES
 NEW YORK STATE MEDICAID PROGRAM MIDWIFE PROCEDURE CODES Table of Contents GENERAL INFORMATION... 3 SERVICES PROVIDED IN ARTICLE 28 FACILITIES... 4 MMIS MODIFIERS... 4 MEDICINE SECTION... 7 GENERAL INFORMATION
NEW YORK STATE MEDICAID PROGRAM MIDWIFE PROCEDURE CODES Table of Contents GENERAL INFORMATION... 3 SERVICES PROVIDED IN ARTICLE 28 FACILITIES... 4 MMIS MODIFIERS... 4 MEDICINE SECTION... 7 GENERAL INFORMATION
Evaluation & Management Coding Category Selection Individual Exercises
 Evaluation & Management Coding Category Selection Individual Exercises Note: Unless otherwise stated, each problem is intended to be independent of the preceding problems. Do not assume that any facts
Evaluation & Management Coding Category Selection Individual Exercises Note: Unless otherwise stated, each problem is intended to be independent of the preceding problems. Do not assume that any facts
HEALTH DEPARTMENT BILLING GUIDELINES
 HEALTH DEPARTMENT BILLING GUIDELINES Acknowledgement: Current Procedural Terminology (CPT ) is copyright 2015 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative
HEALTH DEPARTMENT BILLING GUIDELINES Acknowledgement: Current Procedural Terminology (CPT ) is copyright 2015 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative
Billing an NP's Service Under a Physician's Provider Number
 660 N Central Expressway, Ste 240 Plano, TX 75074 469-246-4500 (Local) 800-880-7900 (Toll-free) FAX: 972-233-1215 info@odellsearch.com Selection from: Billing For Nurse Practitioner Services -- Update
660 N Central Expressway, Ste 240 Plano, TX 75074 469-246-4500 (Local) 800-880-7900 (Toll-free) FAX: 972-233-1215 info@odellsearch.com Selection from: Billing For Nurse Practitioner Services -- Update
Update on New Coordination of Care and Transition of Care Coding
 Update on New Coordination of Care and Transition of Care Coding Michele Olivier ACP Colorado Chapter February 5, 2015 (303) 801-0123 Agenda Introduction Chronic Care Management Coding Advanced Care Planning
Update on New Coordination of Care and Transition of Care Coding Michele Olivier ACP Colorado Chapter February 5, 2015 (303) 801-0123 Agenda Introduction Chronic Care Management Coding Advanced Care Planning
E/M Components EVALUATION AND MANAGEMENT (E/M) CODING FOR CHILD AND ADOLESCENT PSYCHIATRIC OUTPATIENTS OVERVIEW
 EVALUATION AND MANAGEMENT (E/M) CODING FOR CHILD AND ADOLESCENT PSYCHIATRIC OUTPATIENTS Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy of Child
EVALUATION AND MANAGEMENT (E/M) CODING FOR CHILD AND ADOLESCENT PSYCHIATRIC OUTPATIENTS Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy of Child
CODE AUDITING RULES. SAMPLE Medical Policy Rationale
 CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
Evaluation and Management Coding Advisor
 Evaluation and Management Coding Advisor Contents Chapter 1: Introduction...1 High Volume Services...1 Documenting Evaluation and Management Services...1 Documentation and the EHR...3 Summary...3 Knowledge
Evaluation and Management Coding Advisor Contents Chapter 1: Introduction...1 High Volume Services...1 Documenting Evaluation and Management Services...1 Documentation and the EHR...3 Summary...3 Knowledge
ICD-10-CM Training Module for Dental Practitioners. Presented by Workgroup for Electronic Data Interchange
 ICD-10-CM Training Module for Dental Practitioners Presented by Workgroup for Electronic Data Interchange Disclaimer This presentation is for discussion and educational purposes only and is not intended
ICD-10-CM Training Module for Dental Practitioners Presented by Workgroup for Electronic Data Interchange Disclaimer This presentation is for discussion and educational purposes only and is not intended
Implementing Prescribing Guidelines in the Emergency Department. April 16, 2013
 Implementing Prescribing Guidelines in the Emergency Department April 16, 2013 Housekeeping Note: Today s presentation is being recorded and will be provided within 48 hours. Two ways to ask questions
Implementing Prescribing Guidelines in the Emergency Department April 16, 2013 Housekeeping Note: Today s presentation is being recorded and will be provided within 48 hours. Two ways to ask questions
Billing for Non-Physician Practitioners
 Billing for Non-Physician Practitioners Incident to and Shared Services 2007 Betsy Nicoletti 1 Betsy Nicoletti www.mpconsulting.org Author: 2007 Physician Auditing Workbook The Field Guide to Physician
Billing for Non-Physician Practitioners Incident to and Shared Services 2007 Betsy Nicoletti 1 Betsy Nicoletti www.mpconsulting.org Author: 2007 Physician Auditing Workbook The Field Guide to Physician
Modifiers The Key To Proper Reimbursement. Proper use of modifiers (usually) leads to correct payment. Author: Kenneth F. Malkin, D.P.M.
 Modifiers The Key To Proper Reimbursement Proper use of modifiers (usually) leads to correct payment. Author: Kenneth F. Malkin, D.P.M. Dr. Malkin is a diplomate of the American Board of Quality Assurance
Modifiers The Key To Proper Reimbursement Proper use of modifiers (usually) leads to correct payment. Author: Kenneth F. Malkin, D.P.M. Dr. Malkin is a diplomate of the American Board of Quality Assurance
Therefore, a physician should only bill for new patient services when the elements of the definition is met.
 Private Property of Florida Blue. This payment policy is Copyright 2012, Florida Blue. All Rights Reserved. You may not copy or use this document or disclose its contents without the express written permission
Private Property of Florida Blue. This payment policy is Copyright 2012, Florida Blue. All Rights Reserved. You may not copy or use this document or disclose its contents without the express written permission
HealthCare Partners of Nevada. Heart Failure
 HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
HealthCare Partners of Nevada Heart Failure Disease Management Program 2010 HF DISEASE MANAGEMENT PROGRAM The HealthCare Partners of Nevada (HCPNV) offers a Disease Management program for members with
E/M Documentation: Deal or No Deal? Documentation Guidelines. Documentation Elements 3/25/2013
 E/M Documentation: Deal or No Deal? Presented by Maggie Mac, CPC, CEMC, CHC, CMM, ICCE and Dennis Mihale, MD Documentation Guidelines 1995 vs 1997 guidelines 95 for? 97 for? General Multi-System? Specialty
E/M Documentation: Deal or No Deal? Presented by Maggie Mac, CPC, CEMC, CHC, CMM, ICCE and Dennis Mihale, MD Documentation Guidelines 1995 vs 1997 guidelines 95 for? 97 for? General Multi-System? Specialty
PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 2 EVALUATION AND MANAGEMENT (E/M) SERVICES
 PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 2 EVALUATION AND MANAGEMENT (E/M) SERVICES Evaluation and Management (E/M) Documentation E/M Documentation Background: Physician payment for inpatient
PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 2 EVALUATION AND MANAGEMENT (E/M) SERVICES Evaluation and Management (E/M) Documentation E/M Documentation Background: Physician payment for inpatient
School Based Health Care Coding at Your Best
 School Based Health Care Coding at Your Best Presented by Carley Spangler, CPC Account Manager, OCHIN Billing Services October 2011 OCHIN 707 SW Washington Suite 1200 Portland, OR 97205 P 503-943-2500
School Based Health Care Coding at Your Best Presented by Carley Spangler, CPC Account Manager, OCHIN Billing Services October 2011 OCHIN 707 SW Washington Suite 1200 Portland, OR 97205 P 503-943-2500
Disclaimers/Confessions. Best Practices for Eye Care Staff Related to Medical Records. Disclaimers/Confessions, con. National Guidelines for Records
 Disclaimers/Confessions Best Practices for Eye Care Staff Related to Medical Records Presented by. Charles B. Brownlow, O.D., F.A.A.O. Medical Records Consultant PMI, LLC DrBrownlow@PMI EYES.com This presentation
Disclaimers/Confessions Best Practices for Eye Care Staff Related to Medical Records Presented by. Charles B. Brownlow, O.D., F.A.A.O. Medical Records Consultant PMI, LLC DrBrownlow@PMI EYES.com This presentation
Provider Manual. Section 18.0 - Case Management and Disease Management
 Section 18.0 - Case Management and Disease Management 18.1.1 Introduction 18.2.1 Scope 18.3.1 Objectives 18.4.1 Procedures Case Management 18.4.1-A. Referrals 18.4.1-B. Case Management Mercy Maricopa Acute
Section 18.0 - Case Management and Disease Management 18.1.1 Introduction 18.2.1 Scope 18.3.1 Objectives 18.4.1 Procedures Case Management 18.4.1-A. Referrals 18.4.1-B. Case Management Mercy Maricopa Acute
NEW YORK STATE MEDICAID PROGRAM NURSE PRACTITIONER PROCEDURE CODES
 NEW YORK STATE MEDICAID PROGRAM NURSE PRACTITIONER PROCEDURE CODES Table of Contents GENERAL INFORMATION... 3 STATE DEPARTMENT OF HEALTH CONDITIONS FOR PAYMENT... 6 PRACTITIONER SERVICES PROVIDED IN HOSPITALS...
NEW YORK STATE MEDICAID PROGRAM NURSE PRACTITIONER PROCEDURE CODES Table of Contents GENERAL INFORMATION... 3 STATE DEPARTMENT OF HEALTH CONDITIONS FOR PAYMENT... 6 PRACTITIONER SERVICES PROVIDED IN HOSPITALS...
TRANSITIONAL CARE MANAGEMENT CHECKLIST
 _ Name of TCM Qualified Healthcare Professional (QHP) Provider: Discharge Date: TCM End Date (29 days after day of discharge): TCM services are for an established patient whose medical and/or psychosocial
_ Name of TCM Qualified Healthcare Professional (QHP) Provider: Discharge Date: TCM End Date (29 days after day of discharge): TCM services are for an established patient whose medical and/or psychosocial
Sandra Parker, M.D. Chief Medical Officer, AltaPointe Health Systems Vice-Chair, University of South Alabama Department of Psychiatry
 Sandra Parker, M.D. Chief Medical Officer, AltaPointe Health Systems Vice-Chair, University of South Alabama Department of Psychiatry President-Elect, Alabama Psychiatric Physicians Association No Disclosures
Sandra Parker, M.D. Chief Medical Officer, AltaPointe Health Systems Vice-Chair, University of South Alabama Department of Psychiatry President-Elect, Alabama Psychiatric Physicians Association No Disclosures
CRASH COURSE MEDICAL NECESSITY SKILLS FOR NON PROVIDERS
 CRASH COURSE MEDICAL NECESSITY SKILLS FOR NON PROVIDERS PRESENTED BY: MAGGIE MAC CPC, CEMC, CHC, CMM, ICCE, AHIMA APPROVED ICD 10 CM/PCS TRAINER STEPHANIE CECCHINI, CPC, CEMC, CHISP, APPROVED ICD 10 TRAINER
CRASH COURSE MEDICAL NECESSITY SKILLS FOR NON PROVIDERS PRESENTED BY: MAGGIE MAC CPC, CEMC, CHC, CMM, ICCE, AHIMA APPROVED ICD 10 CM/PCS TRAINER STEPHANIE CECCHINI, CPC, CEMC, CHISP, APPROVED ICD 10 TRAINER
GUIDE TO HOME HEALTH DIAGNOSIS CODES
 GUIDE TO HOME HEALTH DIAGNOSIS CODES Proper selection of diagnoses codes for the Medicare OASIS Assessment The process of selecting correct diagnosis codes for the OASIS Start of Care, Re-Certification
GUIDE TO HOME HEALTH DIAGNOSIS CODES Proper selection of diagnoses codes for the Medicare OASIS Assessment The process of selecting correct diagnosis codes for the OASIS Start of Care, Re-Certification
5557 FAQs & Definitions
 5557 FAQs & Definitions These Questions and Answers are intended to present information that has been acquired as part of the discovery process and provides necessary context for the Policy Directives
5557 FAQs & Definitions These Questions and Answers are intended to present information that has been acquired as part of the discovery process and provides necessary context for the Policy Directives
A GUIDE TO EVALUATION & MANAGEMENT CODING AND DOCUMENTATION
 A GUIDE TO EVALUATION & MANAGEMENT CODING AND DOCUMENTATION Produced by ConnectiCare, Inc. in conjunction with its affiliate Group Health Incorporated TABLE OF CONTENTS Summary and Overview...Page 3 Part
A GUIDE TO EVALUATION & MANAGEMENT CODING AND DOCUMENTATION Produced by ConnectiCare, Inc. in conjunction with its affiliate Group Health Incorporated TABLE OF CONTENTS Summary and Overview...Page 3 Part
PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 5 OUTPATIENT OBSERVATION SERVICES
 PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 5 OUTPATIENT OBSERVATION SERVICES Definition of Observation Care Medicare defines observation care* as: a well defined set of specific, clinically
PROFESSIONAL BILLING COMPLIANCE TRAINING PROGRAM MODULE 5 OUTPATIENT OBSERVATION SERVICES Definition of Observation Care Medicare defines observation care* as: a well defined set of specific, clinically
Suggestions for Billing Codes for IBCLCs
 Suggestions for Billing Codes for IBCLCs There are several classifications of CPT or HCPCS Codes which IBCLCs can theoretically use to bill for their services. There are advantages and disadvantages to
Suggestions for Billing Codes for IBCLCs There are several classifications of CPT or HCPCS Codes which IBCLCs can theoretically use to bill for their services. There are advantages and disadvantages to
Introduction to Medical Coding For Lawyers
 American Health Lawyers Association Institute on Medicare and Medicaid Payment Issues March 20-22, 2013 Introduction to Medical Coding for Payment Lawyers Robert A. Pelaia Senior University Counsel for
American Health Lawyers Association Institute on Medicare and Medicaid Payment Issues March 20-22, 2013 Introduction to Medical Coding for Payment Lawyers Robert A. Pelaia Senior University Counsel for
Few non-clinical issues have created as
 How to Get All the 99214s You Deserve It s easier than you might think to get what s coming to you. Emily Hill, PA-C Few non-clinical issues have created as much controversy as the CPT codes for evaluation
How to Get All the 99214s You Deserve It s easier than you might think to get what s coming to you. Emily Hill, PA-C Few non-clinical issues have created as much controversy as the CPT codes for evaluation
E/M coding workshop. The risk of not getting it right. PAMELA PULLY CPC, CPMA BILLING/CLAIMS SUPERVISOR GENESEE HEALTH SYSTEM
 E/M coding workshop. The risk of not getting it right. PAMELA PULLY CPC, CPMA BILLING/CLAIMS SUPERVISOR GENESEE HEALTH SYSTEM Disclaimer This information is accurate as of December 1, 2014 and is designed
E/M coding workshop. The risk of not getting it right. PAMELA PULLY CPC, CPMA BILLING/CLAIMS SUPERVISOR GENESEE HEALTH SYSTEM Disclaimer This information is accurate as of December 1, 2014 and is designed
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infusion_therapy_in_the_home 3/1998 2/2016 2/2017 2/2016 Description of Procedure or Service Home infusion
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infusion_therapy_in_the_home 3/1998 2/2016 2/2017 2/2016 Description of Procedure or Service Home infusion
Care Coordination. The Embedded Care Manager. Presented by Thomas Decker, MD Mary Finnegan, BSN, M.Ed
 Care Coordination The Embedded Care Manager Presented by Thomas Decker, MD Mary Finnegan, BSN, M.Ed Goals of Care Management The goals of care Management are consistent with the Triple Aim: Improve population
Care Coordination The Embedded Care Manager Presented by Thomas Decker, MD Mary Finnegan, BSN, M.Ed Goals of Care Management The goals of care Management are consistent with the Triple Aim: Improve population
Modifier -25 Significant, Separately Identifiable E/M Service
 Manual: Policy Title: Reimbursement Policy Modifier -25 Significant, Separately Identifiable E/M Service Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM028 Last Updated:
Manual: Policy Title: Reimbursement Policy Modifier -25 Significant, Separately Identifiable E/M Service Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM028 Last Updated:
2013 IHCP 2 nd Quarter Provider Workshop Indiana Care Select Program
 2013 IHCP 2 nd Quarter Provider Workshop Indiana Care Select Program This presentation can be downloaded at: www.advantageplan.com/advcareselect http://www.mdwise.org/providers-workshops.html DOC_43_13
2013 IHCP 2 nd Quarter Provider Workshop Indiana Care Select Program This presentation can be downloaded at: www.advantageplan.com/advcareselect http://www.mdwise.org/providers-workshops.html DOC_43_13
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008
 Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Licensed Healthcare Providers Guidelines for Telemedicine Using the MyDocNow Platform
 Contents 1. Scope of These Guidelines... 2 2. What is Telemedicine?... 2 3. Introduction... 3 4. What Are the Benefits of Telemedicine?... 3 5. Frequently Asked Questions Physician Care and Treatment...
Contents 1. Scope of These Guidelines... 2 2. What is Telemedicine?... 2 3. Introduction... 3 4. What Are the Benefits of Telemedicine?... 3 5. Frequently Asked Questions Physician Care and Treatment...
AHLA. HH. Introduction to Medical Coding for Payment Lawyers
 AHLA HH. Introduction to Medical Coding for Payment Lawyers Robert A. Pelaia Senior University Counsel University of Florida Jacksonville Jacksonville, FL Institute on Medicare and Medicaid Payment Issues
AHLA HH. Introduction to Medical Coding for Payment Lawyers Robert A. Pelaia Senior University Counsel University of Florida Jacksonville Jacksonville, FL Institute on Medicare and Medicaid Payment Issues
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
9/15/2015. Learning objectives. Coding and compliance. Coding Compliance for the IDS Environment. Could Your Coding be Costing You Money?
 Coding Compliance for the IDS Environment Could Your Coding be Costing You Money? Nancy Enos, FACMPE, CPC-I, CPMA, CEMC MGMA 2015 Annual Conference Learning objectives 1. Discover how administrators of
Coding Compliance for the IDS Environment Could Your Coding be Costing You Money? Nancy Enos, FACMPE, CPC-I, CPMA, CEMC MGMA 2015 Annual Conference Learning objectives 1. Discover how administrators of
National PPO 1000. PPO Schedule of Payments (Maryland Small Group)
 PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
Medical Management. G.2 At a Glance. G.3 Procedures Requiring Prior Authorization. G.5 How to Contact or Notify Medical Management
 G.2 At a Glance G.3 Procedures Requiring Prior Authorization G.5 How to Contact or Notify Medical Management G.6 When to Notify Medical Management G.9 Case Management Services G.12 Special Needs Services
G.2 At a Glance G.3 Procedures Requiring Prior Authorization G.5 How to Contact or Notify Medical Management G.6 When to Notify Medical Management G.9 Case Management Services G.12 Special Needs Services
July 3, 2001. Helen Blumen, MD Medical Director Aspen Systems Corporation 2277 Research Boulevard Rockville, MD 20850. Dear Dr.
 July 3, 2001 Helen Blumen, MD Medical Director Aspen Systems Corporation 2277 Research Boulevard Rockville, MD 20850 Dear Dr. Blumen: The American College of Physicians American Society of Internal Medicine
July 3, 2001 Helen Blumen, MD Medical Director Aspen Systems Corporation 2277 Research Boulevard Rockville, MD 20850 Dear Dr. Blumen: The American College of Physicians American Society of Internal Medicine
A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser
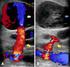 A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser BY MATTHEW L HARRISON Abstract Introduction. Intravenous drug abuse is a global
A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser BY MATTHEW L HARRISON Abstract Introduction. Intravenous drug abuse is a global
Essentials of Coding and Billing in Palliative Care
 Essentials of Coding and Billing in Palliative Care John C. Ely M.D. Martha L. Twaddle M.D. Midwest Palliative and Hospice CareCenter Glenview, IL The following is an excerpt from the 2006 Annual Assembly
Essentials of Coding and Billing in Palliative Care John C. Ely M.D. Martha L. Twaddle M.D. Midwest Palliative and Hospice CareCenter Glenview, IL The following is an excerpt from the 2006 Annual Assembly
Blue Team Teaching Module: Periorbital/Orbital Infections
 Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
High Desert Medical Group Connections for Life Program Description
 High Desert Medical Group Connections for Life Program Description POLICY: High Desert Medical Group ("HDMG") promotes patient health and wellbeing by actively coordinating services for members with multiple
High Desert Medical Group Connections for Life Program Description POLICY: High Desert Medical Group ("HDMG") promotes patient health and wellbeing by actively coordinating services for members with multiple
Billing Code DOS Issue Law Payments Award
 Billing Code DOS Issue Law Payments Award DRG 460 64635 64636 93307 93320 1 1-18-to 01-23- February 11, February 11, February 12, February 12, Implants not separately reimbursed for DRG 460 Denial of the
Billing Code DOS Issue Law Payments Award DRG 460 64635 64636 93307 93320 1 1-18-to 01-23- February 11, February 11, February 12, February 12, Implants not separately reimbursed for DRG 460 Denial of the
OPEN DOOR FAMILY MEDICAL CENTERS, INC. POLICY AND PROCEDURE. Appointment Scheduling RESPONSIBLE DIRECTOR: Chief Operations Officer
 OPEN DOOR FAMILY MEDICAL CENTERS, INC. POLICY AND PROCEDURE TOPIC: RESPONSIBLE DIRECTOR: AFFECTED DEPARTMENTS: AUTHORIZED BY: Appointment Scheduling Chief Operations Officer Patient Services, Nursing,
OPEN DOOR FAMILY MEDICAL CENTERS, INC. POLICY AND PROCEDURE TOPIC: RESPONSIBLE DIRECTOR: AFFECTED DEPARTMENTS: AUTHORIZED BY: Appointment Scheduling Chief Operations Officer Patient Services, Nursing,
We Bring The Pieces Together For You
 Modifier 25 Visit No how-de-do visits in Hematology Oncology MOASC Discussion of Meaningful Information Compliance Education We do it right. We Bring The Pieces Together For You NBC Neltner Billing & Consulting
Modifier 25 Visit No how-de-do visits in Hematology Oncology MOASC Discussion of Meaningful Information Compliance Education We do it right. We Bring The Pieces Together For You NBC Neltner Billing & Consulting
2013 PSYCHIATRY CPT CODES
 2013 PSYCHIATRY CPT CODES Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy of Child and Adolescent Psychiatry OVERVIEW 2 The Old Psychiatry Codes
2013 PSYCHIATRY CPT CODES Benjamin Shain, MD, PhD David Berland, MD Sherry Barron-Seabrook, MD Copyright 2012 by the American Academy of Child and Adolescent Psychiatry OVERVIEW 2 The Old Psychiatry Codes
Let's Play a Game: Emergency Medical Documentation Coding for Emergency PHYSICIANS (not coders) Georgia College of Emergency Physicians June 5, 2012
 Let's Play a Game: Emergency Medical Documentation Coding for Emergency PHYSICIANS (not coders) Georgia College of Emergency Physicians June 5, 2012 Definitions: CPT: Current Procedural Terminology; every
Let's Play a Game: Emergency Medical Documentation Coding for Emergency PHYSICIANS (not coders) Georgia College of Emergency Physicians June 5, 2012 Definitions: CPT: Current Procedural Terminology; every
Streptococcal Infections
 Streptococcal Infections Introduction Streptococcal, or strep, infections cause a variety of health problems. These infections can cause a mild skin infection or sore throat. But they can also cause severe,
Streptococcal Infections Introduction Streptococcal, or strep, infections cause a variety of health problems. These infections can cause a mild skin infection or sore throat. But they can also cause severe,
Meditec.com Free Trial Offer Medical Coding Mini Course. Notice to user:
 Meditec.com Free Trial Offer Medical Coding Mini Course Notice to user: The materials contained in this mini course are copyrighted and may not be reproduced or distributed by any means, or used for any
Meditec.com Free Trial Offer Medical Coding Mini Course Notice to user: The materials contained in this mini course are copyrighted and may not be reproduced or distributed by any means, or used for any
CPT 99213. The Key to E/M Documentation (and Reimbursement)? Rick Horsman DPM Olympia, WA
 CPT 99213 The Key to E/M Documentation (and Reimbursement)? Rick Horsman DPM Olympia, WA CodinglinePRINT www.codingline.com/silver.htm www.apmacodingrc.com COGNITIVE VS. PROCEDURAL SERVICES Cognitive Services
CPT 99213 The Key to E/M Documentation (and Reimbursement)? Rick Horsman DPM Olympia, WA CodinglinePRINT www.codingline.com/silver.htm www.apmacodingrc.com COGNITIVE VS. PROCEDURAL SERVICES Cognitive Services
EPEC. Education for Physicians on End-of-life Care. Trainer s Guide
 EPEC Education for Physicians on End-of-life Care Trainer s Guide Procedure/Diagnosis Coding and Reimbursement Mechanisms for Physician Services in Palliative Care EPEC Project, The Robert Wood Johnson
EPEC Education for Physicians on End-of-life Care Trainer s Guide Procedure/Diagnosis Coding and Reimbursement Mechanisms for Physician Services in Palliative Care EPEC Project, The Robert Wood Johnson
Codes and Documentation for Evaluation and Management Services
 4 Codes and Documentation for Evaluation and Management Services The evaluation and management (E/M) codes were introduced in the 1992 update to the fourth edition of Physicians Current Procedural Terminology
4 Codes and Documentation for Evaluation and Management Services The evaluation and management (E/M) codes were introduced in the 1992 update to the fourth edition of Physicians Current Procedural Terminology
How Physicians Get Paid: It's as Easy as: CMS, RVUs, ICD-9, and CPT
 How Physicians Get Paid: It's as Easy as: CMS, RVUs, ICD-9, and CPT Aaron Michelfelder, M.D. Associate Professor of Family Medicine, and Bioethics & Health Policy Goals Define the Acronyms CMS, RVU, ICD-9,
How Physicians Get Paid: It's as Easy as: CMS, RVUs, ICD-9, and CPT Aaron Michelfelder, M.D. Associate Professor of Family Medicine, and Bioethics & Health Policy Goals Define the Acronyms CMS, RVU, ICD-9,
FAQ for Coding Encounters in ICD 10 CM
 FAQ for Coding Encounters in ICD 10 CM Topics: Encounter for Routine Health Exams Encounter for Vaccines Follow Up Encounters Coding for Injuries Encounter for Suture Removal External Cause Codes Tobacco
FAQ for Coding Encounters in ICD 10 CM Topics: Encounter for Routine Health Exams Encounter for Vaccines Follow Up Encounters Coding for Injuries Encounter for Suture Removal External Cause Codes Tobacco
OBJECTIVES FACTS AND FIGURES CMS CHRONIC CARE MANAGEMENT 10/20/2015. Another Step Towards Care Coordination
 CMS CHRONIC CARE MANAGEMENT Another Step Towards Care Coordination Care Coordination Patient/ Family Community Resources APARNA GUPTA, CRNP, MSN, PGDBA Transitions of Care Chronic Diseases OBJECTIVES AT
CMS CHRONIC CARE MANAGEMENT Another Step Towards Care Coordination Care Coordination Patient/ Family Community Resources APARNA GUPTA, CRNP, MSN, PGDBA Transitions of Care Chronic Diseases OBJECTIVES AT
10/31/2014. Medication Adherence: Development of an EMR tool to monitor oral medication compliance. Conflict of Interest Disclosures.
 Medication Adherence: Development of an EMR tool to monitor oral medication compliance Donna Williams, RN PHN Carol Bell, NP MSN Andrea Linder, RN MS CCRC Clinical Research Nurses Stanford University SOM
Medication Adherence: Development of an EMR tool to monitor oral medication compliance Donna Williams, RN PHN Carol Bell, NP MSN Andrea Linder, RN MS CCRC Clinical Research Nurses Stanford University SOM
Chiropractic Billing Guide
 Chiropractic Billing Guide AmeriHealth HMO Inc., and its affiliates (AmeriHealth) have created this 2006 Chiropractic Billing Guide Supplement in order to provide clear and helpful information about billing
Chiropractic Billing Guide AmeriHealth HMO Inc., and its affiliates (AmeriHealth) have created this 2006 Chiropractic Billing Guide Supplement in order to provide clear and helpful information about billing
ICD-9 CM. ICD-9 9 CM stands for International Classification of Diseases, 9 th revision, clinical modifications
 Ophthalmology Coding ICD-9 9 CM & CPT By Alice Landry, Registered Health Information Administrator and Certified Procedural Coder Harvey & Bernice Jones Eye Institute University of Arkansas for Medical
Ophthalmology Coding ICD-9 9 CM & CPT By Alice Landry, Registered Health Information Administrator and Certified Procedural Coder Harvey & Bernice Jones Eye Institute University of Arkansas for Medical
Critical Care Billing and Coding. Date: February 2015 Presented by: Part B Provider Outreach & Education (POE)
 Critical Care Billing and Coding Date: February 2015 Presented by: Part B Provider Outreach & Education (POE) Workshop Protocol Cannot register with WebEx using mobile device Must use desktop or laptop
Critical Care Billing and Coding Date: February 2015 Presented by: Part B Provider Outreach & Education (POE) Workshop Protocol Cannot register with WebEx using mobile device Must use desktop or laptop
Person Centered Care: Walk the Talk
 Person Centered Care: Walk the Talk Integration of Nurse Practitioner (NP) Role into Extendicare Michener Hill Long Term Care (LTC) Presented by: Sandi Engi MN, NP Michener Hill Extendicare November 25
Person Centered Care: Walk the Talk Integration of Nurse Practitioner (NP) Role into Extendicare Michener Hill Long Term Care (LTC) Presented by: Sandi Engi MN, NP Michener Hill Extendicare November 25
Date: Referring Facility: Phone#: Anticipated Patient Needs (Please check appropriate boxes and include details within referral paperwork)
 Barbara McInnis House Initial Referral Form Please fill form out completely. Include additional forms if prompted. Fax to Admissions Department. Follow up with a phone call. Patient Name: DOB: Gender:
Barbara McInnis House Initial Referral Form Please fill form out completely. Include additional forms if prompted. Fax to Admissions Department. Follow up with a phone call. Patient Name: DOB: Gender:
