How To Help People In Detention Centre
|
|
|
- Damon Wade
- 3 years ago
- Views:
Transcription
1 Beyond Comprehension and Decency An introduction to the work of Medical Justice July
2 Contents 00. Foreword What is Medical Justice? Facts about immigration detention What problems does Medical Justice address? Medical Justice Study of 56 Detainees Medical Justice case studies Other Medical Justice work How can I help Medical Justice? 18 Contact Medical Justice Phone: info@medicaljustice.org.uk Web: Post: Medical Justice, 86 Durham Road, London N7 7DU Bank : Nationwide Building Society (sort code / account number 0230/ ) Cheques payable to: Medical Justice Network For Medical Justice Oxford or Medical Justice Kent contact us as above and we will put you in touch. 2
3 00. Foreword "The strength of a liberal democracy is measured not by how it treats the majority but by how it cares for minorities and those at the margins of society. The best tests for humanity and decency are conducted in its dark places: in prisons, psychiatric hospitals, and in institutions for failed asylum-seekers and other migrants" Stephen Shaw, Prison Ombudsman Medical Justice has been in existence for almost two years and has grown faster than anyone envisaged. It owes its existence entirely to the extraordinary generosity of everyone involved in working with it. It is an organisation built on people s kindness to others and on a shared belief in human dignity and freedom. Medical Justice s work relies on a unique and exciting collaboration between asylum seekers, exdetainees, solicitors, barristers, doctors, nurses, campaigners, detention centre visitors and other volunteers. In my work with Medical Justice as a barrister, my experience has been that a culture has evolved in which people held in detention centres are perceived as having less value than those with legal rights to be in this country. Many detainees describe a feeling of being treated like nothing or like dirt. Such a perception is hurtful to those involved and it violates their dignity as human beings. But the problem is not only that people in detention are perceived as being of less value, it is that they also come to be treated as such. All of those who work with detainees share experiences of neglect, discrimination and abuse on a scale that is saddening and frightening. I see Medical Justice s work as reminding ourselves that we must treat all people with equal value, not just for those people s sakes, but for the sake of our society. We have now assisted over 500 individuals held in detention. We have had numerous successes in changing policy and practice in detention centres. We have a number of publications to our name. We have managed to raise awareness of the problems in detention centres through our work and media activities. I hope that this booklet may give some insight into the scale of the problems we have encountered and why we are working so hard to bring them to an end. We believe that the harm being caused by these institutions is so widespread that the only solution is to close them down. In time we will succeed in that aim. In the interim, we work to reform the institutions and to stand up for the rights of those held within them. I sincerely hope you will support the work of Medical Justice. Alexander Goodman Chair of Medical Justice 3
4 01. What is Medical Justice? Medical Justice facilitates the provision of independent medical advice and independent legal advice and representation to asylum seekers detained in immigration removal centres. We also seek to negotiate changes to policy and practice within detention centres and publish our findings on the treatment of detainees. We have had some notable successes in those respects (see Chapter 6 for further details). Medical Justice was established in October 2005 and its membership comprises highly skilled medical professionals, solicitors, barristers, ex-detainees and detention centre visitors. The national office for Medical Justice is located in London in addition to two regional branches in Oxford and Dover/Canterbury. Core Work Volunteers working for Medical Justice visit detainees in Immigration Removal Centres (also referred to as detention centres) and identify whether that person has any medical issues which need to be addressed by an independent doctor, particularly those relevant to that person s claim for asylum or for humanitarian protection. For example, a Medical Justice volunteer may, on visiting a detainee, learn that that person is claiming to have been tortured in their home country and that the person bears physical scars from those experiences. If that appears to be the case, the volunteer may then decide to refer the person s case to Medical Justice. Medical Justice requires the volunteer to take on the administrative responsibilities of coordinating the case and to provide sufficient background information about the detainee by filling out a referral form. We always welcome more volunteers who are willing to actively take on cases. Medical Justice periodically holds training events to facilitate volunteers wishing to handle cases. Medical Justice s administrator will then send one of our doctors specialising in wound healing and scarring to visit the detainee. Our doctor will produce a medical report, or medico-legal report employing their expertise. Medical Justice will also seek to obtain the services of a solicitor and barrister from our network where appropriate. If the case is taken on by legal representatives, they will often seek to employ the medical evidence in a claim for asylum on behalf of the detainee or in applying for the person s release from detention. The medical evidence is often crucial in corroborating an account of ill-treatment as part of the asylum claim where otherwise there is no supporting evidence. Victims of rape or torture, for example, often have difficulty in recounting their experiences and frequently find that their accounts are not believed in the absence of medical evidence. 4
5 Origins of Medical Justice Medical Justice was founded following a mass hunger-strike by a group of over 100 Zimbabweans held in detention in Harmondsworth Immigration Removal Centre in July After three weeks, one of the hunger-strikers, Harris Nyatsanza had became too weak to walk. Harmondsworth detention centre management refused to send him to hospital and Harris came to the brink of dying. It was only after detention centre visitors managed to obtain the services of Dr Frank Arnold (an independent doctor now working for Medical Justice) that it was possible ensure that Harris be transferred to hospital. That was on the 28 th day of the hunger-strike. On arrival at hospital, Harris was so dehydrated that medical staff had trouble finding a vein in which to insert a drip. Harris was guarded by detention custody officers at his bedside. During the subsequent weeks that Harris spent in hospital it was discovered that the Home Office has no guidance on the care for and re-feeding of hungerstriking immigration detainees. A number of fellow hunger-strikers suffered permanent damage as a consequence of the medical neglect experienced in detention. Partly as a result of the hunger strike, the UK government has since suspended removals to Zimbabwe. Harris Nyatsanza and many of his companions have now been recognised as refugees. When Harris was well enough to walk, he and Dr Arnold got a group of lawyers and doctors together to form Medical Justice, an organisation to address the medical needs of immigration detainees. From the sixteen who attended the first meeting, Medical Justice now has over 300 members. Medical Justice has since managed to make a real difference to many hundreds of detainees by providing this service. Largely through the generosity of doctors, solicitors and barristers working pro bono we offer a vital service to detainees. Owing to the restricted availability of legal aid, and the inability of detainees to pay for medical reports and examinations privately, our services are not provided by any other organisations. 5
6 Asylum claims 02. Facts about immigration detention The number of people claiming asylum In the UK has dropped from a high point of 84,000 per year in 2002 to around 25,000 per year at present. That is lower than 1993 levels. The majority of asylum claims, (according to the most recent figures, relating to 2005) are from Somalia, Iran, Afghanistan China, Eritrea and Iraq. Detention Detainees are either held on arrival to this country while their asylum claims are being processed or pending removal to their home country (in 75% of cases after being refused asylum). The number of asylum seekers held in detention has steadily grown over the last 14 years since detention was first employed on a large scale. According to the latest snapshot figures from the Home Office some 2,220 men, women and children who had claimed asylum were detained in 10 removal centres around the UK (including 170 in criminal prisons but not those held in police cells and short-term holding centres). Official figures state that about 30,000 people are detained each year. There is no limit on how long a person may be held in detention and in some cases detention can be for years at a time. Around 2000 of those detained each year are children. The UK is the only European country to hold children in detention indefinitely. A new detention centre is being built at Gatwick and another is planned in Norfolk. Legal and medical services A large proportion of those held in detention do not have legal representation, and are not entitled to legal aid. Further cuts in legal aid are likely in autumn Medical services for those in detention are very restricted; they lack the range of expertise required for the medical conditions detainees suffer and in Medical Justice s experience are frequently inadequate, neglectful and even abusive. The Home Office, with whom ultimate responsibility lies, did not employ any doctor to advise it on healthcare in immigration detention until our intervention. Operation of seven out of the ten removal centres are sub-contracted by the Home Office to private profit-making companies such as Global Solutions Ltd (GSL) which was formerly known as Group4. They in turn may sub-contract health care to a second private profit making company. The other three removal centres are converted criminal prisons, run by the Prison Service and healthcare responsibility lies with the NHS. 6
7 7
8 03. What problems does Medical Justice address? Lack of adequate legal representation for detainees "the recent cuts in immigration & asylum legal aid are leaving many detained without representation people are languishing in unsafe detention centres because of the inefficiencies and chaos of the Home Office". Her Majesty s Inspector of Prisons In many cases detainees who are not entitled to legal aid have to present their asylum claims on their own. They may not necessarily have the services of an interpreter in so doing and will rarely be aware that medical evidence can be an important part of making an asylum claim. Medical Justice s experience is that there are many cases in which the lack of adequate access to lawyers and medical services means that detainees claims for asylum are not being properly or fairly determined and that there is little opportunity for detainees to redress injustices. We have encountered many cases in which there is strong medical evidence supporting accounts of rape or torture which was never considered in determining an asylum claim. Our experience is that Home Office procedures for dealing with asylum claims are often not properly followed and asylum decisions often lack the degree of rigour to be expected. Our experiences are shared by most other organisations working with detainees. Lack of adequate legal representation also results in unlawful and unnecessary detention of vulnerable persons. One HMIP report found that even Immigration Officers themselves thought there was little or no consistency or logic in who gets detained. There are reports of asylum seekers arriving in the UK and given Temporary Admission with instructions to report back in 48 hours. On reporting back the person may then be detained on the basis of being a potential absconder, even though they have just demonstrated otherwise. Amnesty International reported in June 2005 that immigration detention in the UK is in many cases protracted, inappropriate, disproportionate and unlawful, and the organisation called on the Government to justify the lawfulness of detention in each and every case: Seeking asylum is not a crime, it is a right. Thousands of people who have done nothing wrong are being locked up in the UK. We found that in many cases there was no apparent reason to detain people. One of the most disturbing elements of the UK s policy of detention is the length of time for which children are being detained. Anne Owers, Her Majesty s Inspector Prisons expressed the view in her report into Dungavel detention centre that the welfare and development of children is likely to be compromised by detention, however humane the provisions, and that will increase the longer detention is maintained." The supposed safeguard of ministerial review of detention of children every 28 days is, in practice, ineffective. 8
9 Welfare of asylum seekers in detention "lack of supervision [in the Home Office] can result in arbitrary or sloppy decision-making... in one case a detainee literally lost in the system, three months into what was supposed to be an overnight stay in prison". Her Majesty s Inspector of Prisons Medical Justice is also concerned with the care of people whilst in detention. The United Nations High Commission for Refugees advises that those seeking asylum should not be held in detention because the psychological and physical effects of detention can be particularly difficult for those fleeing persecution and traumatic experiences. The Home Office does not follow the United Nations guidance, but it does have a policy that the most vulnerable groups (children, pregnant women, victims of torture, the elderly and those with mental illness or serious physical illness) should only be detained in very exceptional circumstances and then only for the shortest period necessary. There are many cases where that policy is not observed. Many of Medical Justice s patients are people from those vulnerable groups who have been held in detention for months and, in some cases, for years. Around 200 individuals referred to Medical Justice have subsequently been released. Many of those have been young children. Applications are made in the first instance to the Home Office, and if refused, applications are made to the Asylum and Immigration Tribunal for bail, or to the High Court for habeas corpus. In making those applications our solicitors and barristers often rely on medical evidence from our doctors demonstrating that a person is mentally ill, seriously physically ill, or has been a victim of torture, and setting out the effects of detention on the physical or mental health of the person detained. Such medical evidence, and the legal submissions accompanying it, can often result in a detainee being released. Medical Justice doctors are frequently involved in diagnosing the medical needs of detainees, which have often not been identified. At present the medical services in detention centres rarely have the capacity or expertise to deal with the wide range of serious mental and physical conditions presented by detainees. The consequences for those individuals can be grave. Detainees are commonly suffering from anxiety, depression, post traumatic stress disorder, and serious mental illnesses which can be perpetuated or exacerbated by detention. In some cases infectious Tuberculosis has gone undiagnosed until Medical Justice Doctors have intervened. Many detainees from sub-saharan Africa suffer from HIV/AIDS and are in dire need of anti-retroviral treatment. Again, that need is often not identified until a Medical Justice Doctor intervenes. We have also, for example, successfully encouraged the Home Office to adopt a policy of providing vaccinations and prophylaxis against malaria to young children prior to removing them to Sub-Saharan Africa and other risk areas. 9
10 Abuse of people in detention A young woman was held in the holding room who had miscarried a few days previously. She had been collected from a hospital following psychiatric referral, had not eaten for three days and had to be helped to and from the van. She was subject to a live F2052SH self-harm monitoring form because she kept asking for her baby and said she wanted to die. Having been delivered to the holding room in the morning, she was not due to be collected by another vehicle until more than six hours later. Apart from staff who had received first aid training, there was no on-site healthcare Her Majesty s Inspector of Prisons The lack of adequate legal assistance for detainees leads to abuses of detainees rights. A report into Short Term Residential Holding Centres referred to: "recent evidence of abuse under escort and at the point of removal" Her Majesty s Inspector of Prisons HMIP also reported that a holding centre: "operates out of the sight of the community but unlike other custodial environments, with no regular independent monitoring" Her Majesty s Inspector of Prisons Lawyers working on cases referred by Medical Justice have brought numerous claims in the Courts, usually employing medical evidence for detainees seeking to obtain redress for unlawful detention, or for abuse while in detention. Such abuses include assaults, inappropriate use of handcuffs, unlawful use of solitary confinement and the withholding of medication from detainees. 10
11 11
12 04. Medical Justice study of 56 detainees Of the 500 detainees now seen, Medical Justice doctors recorded their findings on examining the first 56 consecutive "failed" asylum seekers treated in a six month period in four UK detention centres, before, or shortly after, their release. Torture Victims 20 of the 56 detainees seen by highly respected experts in torture and scarring working for Medical Justice gave a history of torture and had physical signs "consistent with", highly consistent with or "typical of" torture (using the definitions established by the Istanbul Protocol on the Reporting of Torture). In no case had the Home Office investigated the allegations of torture or offered medical assistance, even when it had been appropriately reported to Home Office officials and doctors. Those failures were in breach of the statutory duties imposed by the Detention Centre Rules 2001, in particular rules 33, 34, and 35. In a recent High Court case (D & K EWHC [2006] 980) Mr. Justice Davis described the Home Office s failures to carry out proper investigation of the allegations of torture in these terms: It was not a rare and regrettable lapse in the circumstances of these two cases. Rather it reflected the cross-the-board failure to give effect to the requirements of Rule 34 (and applicable Standards): the [Home Office] regarding compliance as neither necessary nor appropriate. I repeat what I have said earlier: that is not acceptable. Mr Justice Davis HIV Three of four women who had been receiving anti-retroviral drugs in the community had disruptions to their treatment (this can have the potentially disastrous consequence that the Virus establishes immunity to the treatment). Other detainees were not given the results of their positive HIV test until taken to the airport for deportation. Some rape survivors were denied an HIV test. Tuberculosis Three patients were found to have tuberculosis. In one case diagnosis was delayed. He also suffered side effects which were not adequately explained to him. Another, who is believed to have had multi-drug resistance, had treatment disrupted during his detention for over one month. He was also prevented from keeping hospital appointments for specialist management of his TB and three other medical conditions. Malaria Six patients who were removed developed laboratory-confirmed falciparum malaria following their forced return to sub-saharan Africa. None had been offered prophylaxis or bed-nets to mitigate the loss of immunity from being in the UK. 12
13 Hunger-strikers Eleven patients were first seen during or shortly after being on hunger strike. Six were in imminent danger of organ failure. According to the medical notes, four had not been examined by a doctor for extended periods. Despite the frequency of hunger strikes in detention, the Home Office had no policy or guidance for detention centre staff dealing with well documented dangers of recommencing food intake after prolonged starvation. Depression and suicide attempts At least 33 patients fulfilled ICD10 criteria for Post-Traumatic Stress Disorder or depression. Many had either harmed themselves or made determined attempts at suicide. Medical Justice s findings and experience are supported by data on the treatment of mentally ill and suicidal persons in detention. There were 176 attempts of selfharm that required medical treatment in 10 months up to January 2007, and 1,643 detainees were on formal suicide-watch. There have been 8 suicides in immigration detention since An HMIP report on Harmondsworth Removal Centre noted "The centre's suicide awareness team was unaware that there had been 11 incidents in the month before the inspection". Amnesty reported in 2005: "The human cost of this [detention] policy is frighteningly high. We found that languishing in detention with no end in sight had led to mental illness, self-harm and even to people trying to take their own life". Medical Justice conclusions Unmet health needs are a major problem among immigration detainees. Moreover, detention itself is frequently damaging to the health of detainees, sometimes profoundly so. Detention of torture survivors, children and those with physical or mental ill health is unjustifiable, contrary to the Home Office s own policy, and should cease. Our findings agree with those reported by Médicins Sans Frontières and the British Medical Journal: detainees, particularly those held for long periods, suffer from profound hopelessness, despair, and suicidal urges. In many of these patients, both medical and psychiatric needs were frequently not adequately addressed. Such neglect violates the European Convention on Human Rights and other agreed international obligations with respect to medical care Médicins Sans Frontières and the British Medical Journal 13
14 05. Medical Justice case studies The following are supplied by three Medical Justice doctors: an expert in wound healing; a psychiatrist and a GP. Consent to be included has been obtained from the individuals concerned. A gay man from a Muslim country was repeatedly tortured with cigarette burns and beatings and suffered other significant injuries. He fled to the UK and was detained at Colnbrook Detention Centre on arrival for an extended period. The detention centre nurses and doctors are required to ask him whether he had been tortured, so that they can inform the Home Office, who can then attempt to comply with their duty only to detain such people only in very exceptional circumstances. Until my arrival the Detention Centre had failed to ask him or record the answer as to whether he had been a victim of torture. After this, a nurse recorded his blatant cigarette burns as shrapnel wounds. (It is hard to describe to anyone who is not a clinician how difficult it is to confuse the two.) On the basis of a medico-legal report he has been freed and is pursuing a fresh claim for asylum. Dr Frank Arnold MB FRCS (Surgeon and expert in wound healing) C is 30 years old and was born in Uganda. After leaving university he became a tourist guide. Five years ago, while escorting a tourist group he was the victim of an attack by a group of soldiers who killed several of the tourists and his fellow guides. He was able to escape and suffered transient sleep disturbance and nightmares which resolved over several months. In 2004 he was arrested by soldiers whom he recognised as involved in the original attack. He was detained, interrogated, kicked and beaten and forced to bury the bodies of dead soldiers. After escaping he fled to the UK where he claimed asylum and was immediately detained. Within 3 months he was given a removal date. He tried to hang himself in detention because it would be better to take my life in a simple way than to be tortured. He continued to have nightmares of seeing dead soldiers in detention. He was bailed and while on bail formed a long term relationship with an Englishwoman by whom he had a daughter. On Christmas Eve 2006 he was again detained. A week later he took a serious overdose in detention. When I saw him his symptoms fulfilled the criteria both for depression and for post-traumatic stress disorder. Following a fresh bail application invoking my psychiatric report he was released, shortly after which he and his partner were married. His asylum appeal is outstanding. Professor Cornelius Katona (Dean of Kent Institute of Medicine & Health Sciences and Psychiatrist) A is a 30 year old woman who fled a West African country after being repeatedly raped and tortured by soldiers. She claimed asylum on arrival in the UK in mid-2005, but her story was disbelieved by the immigration service and she was detained on Fast Track at Yarl s Wood IRC for three and a half months. A had a number of serious health problems which were severely neglected by Yarl s Wood healthcare. She was never seen by a gynaecologist nor screened for sexually-transmitted infections during her time in detention. A had raised blood pressure: this too was not investigated or treated. A suffered diabetes, which was also not treated, and she developed a painful and longstanding complication of damage to the nerves in her feet. 14
15 A also suffered severe depression and post-traumatic stress disorder and was placed on suicide watch for several weeks after harming herself. She was given counselling treatment but still held in detention in contravention of the Home Office s own rules. Attempts were made to remove her while she was on continuous 24 hour suicide watch. Although her asylum claim was ruled not credible, A was threatened by an immigration officer during a failed removal attempt that the army in her home country would be informed about her arrival unless she co-operated with her removal. After being seen by a doctor working with Medical Justice, and efforts by her solicitors, A was released from detention and is pursuing a claim for damages against the Home Office. Dr Jonathan Fluxman (GP registered under section 12 of the Mental Health Act, Harrow Road Health Centre) A woman was detained at Yarl s Wood DC while pregnant and with a history of insulin dependent diabetes and high blood pressure. The nurses refused to believe she was pregnant until she presented them with the results of a miscarriage in a bucket. She was not allowed to test her blood sugar four times daily as she had been advised to do by her GP, but only twice and the control of her diabetes deteriorated. She vomited blood, but even after this was proved to be coming from her stomach (by gastroscopy) the nurses tried to continue feeding her Brufen, a drug which commonly causes gastric bleeding. She next developed chest pain and was referred to hospital for a cardiograph, which was indeterminate. The cardiologist requested an isotope scan to be done at a second hospital. The Detention Centre, for what it says were security reasons refused to tell her about this appointment in advance, and she drank tea shortly before being taken to hospital. As a result, she developed chest pain during the test of such degree that the crash team had to be called and the scan terminated. In the following month she was not re-referred by the detention centre for another appointment. The consultant wrote to the Detention Centre to complain. She was released on bail following a medical report from a Medical Justice doctor. Following release, the Detention Centre failed to provide her or her new GP with her medical notes, despite repeated requests from her and the Medical Justice doctor. (This is important, because her diabetes and blood pressure are likely to be contributing to her increasing blindness.) After a final protest to the Home Office about this, she was detained the following day, but suffered a further attack of chest pain and was hospitalised for 10 days. She is pursuing an asylum case on fresh medical evidence of serious abuse in her country of origin and she is considering a civil case for damages against the detention centre and Home Office. Dr Frank Arnold B fled from a Caribbean country in 2002 after her home was attacked during which her 6 year old daughter was killed in front of her and she herself was shot and injured. She was detained for 6 months in 2002 and then re-detained in mid When seen by a doctor working with Medical Justice she had been at Yarl s Wood Immigration Removal Centre for 7 months and had become severely depressed with marked suicidal risk. Healthcare at Yarl s Wood were completely unaware of this, but B was placed on 24 hour suicide watch straight away once they were informed. B also suffers asthma and has marked stress-induced high blood pressure. Three removal attempts had to be abandoned because B became too ill during each of them. B was not facing imminent removal at the time she was seen. She had become suicidally depressed at the prospect of her ongoing and indefinite detention. B also had a previous history of trying to take her own life after her daughter was killed and during her previous period in detention. 15
16 B was assessed by a psychiatrist who works at the local mental health unit and who regularly provides psychiatric assessments of detainees at Yarl s Wood. Despite her traumatic history, her previous suicidal behaviour, the findings of two other doctors and that B was on continuous 24 hour suicide watch, the psychiatrist found after a cursory examination B was not depressed and recommended she receive no treatment. She remained on suicide watch after this but her depression and suicide risk was not treated. Fortunately B was released on bail soon afterwards and her depression was treated in the community. Dr Jonathan Fluxman D is in his mid 30s and was born in a small predominantly Muslim republic within the Russian Federation. After university he worked as a TV documentary maker. He was imprisoned and repeatedly beaten after making documentary about a detention camp in neighbouring republic. During this time his flat was broken into and he was outed as a homosexual in a state in which homosexuality is not tolerated despite its theoretical legality throughout Russia. He fled to the UK and sought asylum. While living in NASS accommodation he became depressed and started drinking heavily and received treatment for this within his local psychiatric service. He was detained in While in detention he was raped by a fellow detainee. His depression worsened and he became determined that he would kill himself if removed. He was seen by a consultant psychiatrist who recommended admission to hospital. Despite this he was given removal directions. These were cancelled following intervention by a Member of Parliament and an article in national press and he was admitted to psychiatric hospital as a detained patient. He was found to be HIV positive. He remained in hospital for a year, with minimal improvement in his mood and episodes of heavy drinking and aggressive behaviour before being discharged into NASS accommodation. Following an Immigration Tribunal ruling he was given discretionary leave to remain in UK where he remains depressed and in close psychiatric follow-up. His HIV related illness has deteriorated and he is currently about to start antiretroviral treatment. He is pursuing a civil claim for inappropriate detention. Professor Cornelius Katona A 30 year old man from Nigeria was referred to Medical Justice by detention centre visitors. He said that he had been assaulted by guards at Haslar detention centre during a protest by detainees about the death of Bereket Johannes in Harmondsworth. DC. He had suffered injuries to the nerves to both hands, and to his left leg, on which he could not bear weight. He had been rendered unconscious. He was transferred in this state - not to hospital as good practice dictates for unconscious patients - but to Colnbrook Detention Centre. Here no doctor s examination was recorded until the following day; nor was he allowed a wheel chair during my visit. In protest, he refused food and water, and went into early renal failure. At his request, and with help from MJ lawyers, I compelled his admission to hospital and he was rehydrated by drip. The detention centre have not complied with a court order to deliver crucial charts (which I have seen) which show a concerning lack of competence in measuring his fluid balance. Following continued hunger strike (to 29 days) he was readmitted to hospital and safely refed. Medical reports about his injuries and inadequate subsequent management at Colnbrook were held to play a significant part in his being granted bail. He is pursuing a claim for asylum, supported by a medico-legal report concerning scars consistent with his account of torture in his country of origin. Dr Frank Arnold 16
17 06. Other Medical Justice work Policy work As a result of our negotiations with the Home Office and detention centre authorities the following have been adopted: A Home Office policy on the provision of anti-malarial drugs and vaccinations to children and pregnant women before removal to their home countries where they will be at risk; Changes in Home Office policy on access for detainees to independent medics; An end to the routine handcuffing of detainees when being escorted to hospital for medical treatment; A Home Office agreement to audit management of detainees claims to be torture victims; A Home Office agreement to consider medical evidence direct from independent doctors Yarl s Wood detention centre agreement not to obstruct detainees from obtaining hospital test results Publications We have published two leaflets, Know your Medical Rights and Advice to Hunger Strikers available to detainees in detention centres. A number of articles concerning our work have been published by Medical Justice doctors in the British Medical Journal. Parliamentary work We successfully encouraged Her Majesty s Inspector of Prisons to carry out the first ever inquiry into healthcare at Yarl's Wood Removal Centre. We have met with, and made submissions to, the Parliamentary Joint Committee on Human Rights. Medical Justice has succeeded in helping parliamentarians to include immigration detainee healthcare in debates, parliamentary questions, and committee inquiries, and to challenge misleading statements by Home Office representatives. Medical Justice has arranged for MPs to visit patients in detention centres and frequently gets parliamentarians involved in individuals cases. Medical Justice has been supported in its work by MPs, Peers and MEPs from the Conservative Party, the Green Party, the Labour Party, and the Liberal Democrats. We have had ardent and effective support from a small number of politicians from all the major political parties for which we are grateful. 17
18 HMIP Inquiry into Healthcare at Yarl s Wood Following a series of suicides and a number of instances of alleged mistreatment of detainees, Medical Justice and the local MP Alistari Burt requested an inquiry into healthcare at Yarl's Wood Removal Centre and specifically into the medical treatment of a Ugandan woman held in detention for seven months. The Inquiry was conducted by Anne Owers, Her Majesty s Inspector of Prisons and sought to establish whether the suspected brain damage suffered by the detainee was caused by mistreatment while she was held in detention and by aborted attempts to return her to Uganda. The detainee was eventually released from detention into a psychiatric hospital for 6 months. The inquiry s findings lead Alistair Burt, the MP for the Bedfordshire area in which Yarl s Wood is located, to say [The inquiry] was appalling in what it revealed and should be a source of shame to those involved. I am not totally surprised at the results, though shocked and genuinely appalled at the depth of failures revealed and inadequacies of those with care and responsibility for detainees... [IND's] repeated attempts to removed sick detainees went beyond comprehension and decency". Alistair Burt MP The inquiry was the first of its kind and recommended three major changes, in line with Medical Justice s key demands Transfer of detention centre healthcare responsibility from private companies to NHS Proper enforcement of Home Office policy not to detain vulnerable people An end to obstruction to appropriate healthcare for detainees Diagram above: Control & Restraint as described by Ms J, a detainee at Yarl s Wood Removal Centre who later won a civil action case regarding her treatment there. 18
19 07. How can I help Medical Justice? Volunteer for Medical Justice At present all our work is done by volunteers. We accept offers of help from all quarters for all administrative and organisational tasks. The easiest way to find out about us is to come to one of the open meetings held in London every 6 weeks. Open meetings are held in Canterbury and Oxford at similar intervals. We particularly welcome asylum seekers and refugees. Your first-hand experience of the asylum determination process is vital to the work of Medical Justice. Doctors - We need qualified doctors to volunteer to give advice to detainees over the phone and conduct medical visits in places of detention where necessary. Social workers working with children, nurses, midwives, and mental health nurses - your clinical experience and knowledge of NHS and Social Services standards of care is a valuable resource for supporting adults and children in detention. Visits, phone contact or writing a report can be very helpful. Solicitors, barristers and qualified immigration case-workers to advise Medical Justice patients and to take on cases where possible. Also to inform Medical Justice of legal and policy developments for the benefit of volunteers. Researchers, students, journalists - to volunteer to do research, media work, documentation, administration, organisational development tasks, website management and fundraising. Visitors and case co-ordinators - to volunteer to visit detainees and co-ordinate Medical Justice resources around individual cases no qualifications other than patience and determination needed; we hold training sessions and provide support where we can. Donate to Medical Justice Medical Justice presently has no funding we rely entirely on donations. Make a donation, take out a Standing Order, solicit a donation or affiliation fee from your organisation or trade union. See details below. Join Medical Justice Membership for asylum seekers and ex-detainees is free. Membership for waged members is 10 for each 3,000 of your salary (e.g. 50 for 15,000 salary, 100 for 30,000 salary). Tell us your contact details, your skills and make a donation direct to the bank, or send us a cheque. See details below. Phone: info@medicaljustice.org.uk Web: Post: Medical Justice, 86 Durham Road, London N7 7DU Bank : Nationwide Building Society (sort code / account number 0230/ ) Cheques payable to: Medical Justice Network 19
20 20
ILPA response to Inquiry into Asylum Support for Children and Young People
 ILPA response to Inquiry into Asylum Support for Children and Young People Annexe 1 Caselist The cases below are drawn from ILPA s February 2010 response evidence to the Ministry of Justice consultation
ILPA response to Inquiry into Asylum Support for Children and Young People Annexe 1 Caselist The cases below are drawn from ILPA s February 2010 response evidence to the Ministry of Justice consultation
Access to HIV Treatment and Care in the UK
 Access to HIV Treatment and Care in the UK Cases Related to Charging 1. A was a Somalian national who claimed asylum in 1999 and was supported under the Immigration and Asylum Act 1999 Interim Regulations.
Access to HIV Treatment and Care in the UK Cases Related to Charging 1. A was a Somalian national who claimed asylum in 1999 and was supported under the Immigration and Asylum Act 1999 Interim Regulations.
GETTING PROBATION APPROVAL FOR YOUR IMMIGRATION BAIL ADDRESS
 Factsheet 2 GETTING PROBATION APPROVAL FOR YOUR IMMIGRATION BAIL ADDRESS I m a foreign national ex-offender, I m still on Licence, and I want to apply for immigration bail. What do I need to do? September
Factsheet 2 GETTING PROBATION APPROVAL FOR YOUR IMMIGRATION BAIL ADDRESS I m a foreign national ex-offender, I m still on Licence, and I want to apply for immigration bail. What do I need to do? September
It is important that you apply for asylum as soon as you enter the UK and that you seek legal advice as soon as possible.
 March 2012 English When you apply for asylum in the United Kingdom (UK), you are asking the Home Office to recognise you as a refugee. The definition of a refugee comes from a piece of international law
March 2012 English When you apply for asylum in the United Kingdom (UK), you are asking the Home Office to recognise you as a refugee. The definition of a refugee comes from a piece of international law
REPORT TO THE UNITED KINGDOM BORDER AGENCY ON OUTSOURCING ABUSE BARONESS NUALA O LOAN DBE MARCH 2010
 REPORT TO THE UNITED KINGDOM BORDER AGENCY ON OUTSOURCING ABUSE by BARONESS NUALA O LOAN DBE MARCH 2010 FOREWORD At various stages in 2007-2008 the Agency faced criticism in some elements of the press
REPORT TO THE UNITED KINGDOM BORDER AGENCY ON OUTSOURCING ABUSE by BARONESS NUALA O LOAN DBE MARCH 2010 FOREWORD At various stages in 2007-2008 the Agency faced criticism in some elements of the press
CRIMINAL LAW & YOUR RIGHTS MARCH 2008
 CRIMINAL LAW & YOUR RIGHTS MARCH 2008 1 What are your rights? As a human being and as a citizen you automatically have certain rights. These rights are not a gift from anyone, including the state. In fact,
CRIMINAL LAW & YOUR RIGHTS MARCH 2008 1 What are your rights? As a human being and as a citizen you automatically have certain rights. These rights are not a gift from anyone, including the state. In fact,
Investigation into the death of Mr George Joseph, a prisoner at HMP Belmarsh, in April 2015
 Investigation into the death of Mr George Joseph, a prisoner at HMP Belmarsh, in April 2015 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence v3.0 except
Investigation into the death of Mr George Joseph, a prisoner at HMP Belmarsh, in April 2015 Crown copyright 2015 This publication is licensed under the terms of the Open Government Licence v3.0 except
How to Prevent and Cope With Police Casualities
 1 INDEPENDENT POLICE COMPLAINTS COMMISSION Preventing Deaths in Police Care Speech to Criminal Justice Management Conference 2015 Commissioner Carl Gumsley Criminal Justice Management Conference 2015.
1 INDEPENDENT POLICE COMPLAINTS COMMISSION Preventing Deaths in Police Care Speech to Criminal Justice Management Conference 2015 Commissioner Carl Gumsley Criminal Justice Management Conference 2015.
A GUIDE TO CRIMINAL INJURIES COMPENSATION
 A GUIDE TO CRIMINAL INJURIES COMPENSATION Being a victim of crime such as physical or sexual assault can have significant and long-term consequences for a woman s health and wellbeing. If you have experienced
A GUIDE TO CRIMINAL INJURIES COMPENSATION Being a victim of crime such as physical or sexual assault can have significant and long-term consequences for a woman s health and wellbeing. If you have experienced
Prison Law Team. Leading prison lawyers. We re and we believe everyone has the right to justice and for their voice to be heard.
 We re and we believe everyone has the right to justice and for their voice to be heard. Prison Law Team Leading prison lawyers The firm has a burgeoning prison practice and has been handling an increasing
We re and we believe everyone has the right to justice and for their voice to be heard. Prison Law Team Leading prison lawyers The firm has a burgeoning prison practice and has been handling an increasing
Response by Bristol Refugee Rights to the Home Office consultation on "Reforming support for failed asylum seekers and other illegal migrants"
 Response by Bristol Refugee Rights to the Home Office consultation on "Reforming support for failed asylum seekers and other illegal migrants" Bristol Refugee Rights views the Home Office proposals to
Response by Bristol Refugee Rights to the Home Office consultation on "Reforming support for failed asylum seekers and other illegal migrants" Bristol Refugee Rights views the Home Office proposals to
Self-Help Guide for a Prosecutorial Discretion Request
 Self-Help Guide for a Prosecutorial Discretion Request In June 2011, Immigration and Customs Enforcement ( ICE ) announced it would not use its resources to deport people it considers low priority and
Self-Help Guide for a Prosecutorial Discretion Request In June 2011, Immigration and Customs Enforcement ( ICE ) announced it would not use its resources to deport people it considers low priority and
Submission to the Parliamentary inquiry into the use of immigration detention in the UK, hosted by the APPG on Refugees and the APPG on Migration
 Submission to the Parliamentary inquiry into the use of immigration detention in the UK, hosted by the APPG on Refugees and the APPG on Migration by Her Majesty s Chief Inspector of Prisons Introduction
Submission to the Parliamentary inquiry into the use of immigration detention in the UK, hosted by the APPG on Refugees and the APPG on Migration by Her Majesty s Chief Inspector of Prisons Introduction
Section 4 Support for Refused Somali Asylum Seekers
 Section 4 Support for Refused Somali Asylum Seekers This advice sheet provides advice on Section 4 support for Somali nationals who have been refused asylum in the UK and who are destitute. Over the past
Section 4 Support for Refused Somali Asylum Seekers This advice sheet provides advice on Section 4 support for Somali nationals who have been refused asylum in the UK and who are destitute. Over the past
7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ
 7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ 7.1 Victim of a crime What are my rights if I have been the victim of a crime? As a victim of crime, you have the right to report that crime to
7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ 7.1 Victim of a crime What are my rights if I have been the victim of a crime? As a victim of crime, you have the right to report that crime to
Resident Rights in Nursing Homes
 Resident Rights in Nursing Homes Nursing home residents have patient rights and certain protections under the law. The nursing home must list and give all new residents a copy of these rights. Resident
Resident Rights in Nursing Homes Nursing home residents have patient rights and certain protections under the law. The nursing home must list and give all new residents a copy of these rights. Resident
Detention under the Mental Health Act
 Detention under the Mental Health Act This factsheet gives information about detention under the Mental Health Act. This is also known as being sectioned. It explains what the Mental Health Act is, why
Detention under the Mental Health Act This factsheet gives information about detention under the Mental Health Act. This is also known as being sectioned. It explains what the Mental Health Act is, why
Guidance to support the Levels of Need poster
 Guidance to support the Levels of Need poster V.1 Approved by Cheshire East Safeguarding Children Board 24 th January 2014 1 Introduction This Framework aims to provide all professionals working with children
Guidance to support the Levels of Need poster V.1 Approved by Cheshire East Safeguarding Children Board 24 th January 2014 1 Introduction This Framework aims to provide all professionals working with children
Going to a Mental Health Tribunal hearing
 June 2015 Going to a Mental Health Tribunal hearing Includes: information about compulsory treatment and treatment orders information about Mental Health Tribunal hearings worksheets to help you represent
June 2015 Going to a Mental Health Tribunal hearing Includes: information about compulsory treatment and treatment orders information about Mental Health Tribunal hearings worksheets to help you represent
To ensure compliance with State and Federal mandated reporting requirements. To ensure appropriate documentation of significant events.
 Vermont State Hospital Policy Mandatory Reporting Policy Replaces version dated: 1/20/10 Updated X Effective Date: 3/04/10 Approved by the Commissioner of the Department of Mental Health: Date: 1/20/10
Vermont State Hospital Policy Mandatory Reporting Policy Replaces version dated: 1/20/10 Updated X Effective Date: 3/04/10 Approved by the Commissioner of the Department of Mental Health: Date: 1/20/10
Duty of public authorities (and contractors) not to act in ways incompatible with a Convention Right.
 Appendix F The Legal Framework This section lists some of the key legislation that may be relevant in the management of individual Adult Safeguarding cases. In any situation where the Adult Safeguarding
Appendix F The Legal Framework This section lists some of the key legislation that may be relevant in the management of individual Adult Safeguarding cases. In any situation where the Adult Safeguarding
Health (Compulsory Assessment and Treatment) Act 1992
 2 Mental Health (Compulsory Assessment and Treatment) Act 1992 PART 1 Terms and definitions 27 PART 2 Compulsory Assessment and Treatment 38 PART 3 Your rights under the Mental Health Act 60 PART 4 Young
2 Mental Health (Compulsory Assessment and Treatment) Act 1992 PART 1 Terms and definitions 27 PART 2 Compulsory Assessment and Treatment 38 PART 3 Your rights under the Mental Health Act 60 PART 4 Young
BASIC IMMIGRATION LAW
 BASIC IMMIGRATION LAW Introduction Under immigration law, anyone not having a right of abode in the UK is subject to immigration control and can only live, work and settle in the UK by permission (Section
BASIC IMMIGRATION LAW Introduction Under immigration law, anyone not having a right of abode in the UK is subject to immigration control and can only live, work and settle in the UK by permission (Section
CURE THE NHS Campaigning for better NHS care www.curethenhs.co.uk
 CURE THE NHS Campaigning for better NHS care www.curethenhs.co.uk LONDON CURE THE NHS INTERNET WEBSITE RESOURCES LIST Please note that LCNHS has no responsibility for the content of these sites and does
CURE THE NHS Campaigning for better NHS care www.curethenhs.co.uk LONDON CURE THE NHS INTERNET WEBSITE RESOURCES LIST Please note that LCNHS has no responsibility for the content of these sites and does
PARENT GUIDE TO THE JUVENILE COURT CHIPS PROCESS
 PARENT GUIDE TO THE JUVENILE COURT CHIPS PROCESS INTRODUCTION This booklet has been prepared to help parents gain a better understanding of what to expect in Juvenile Court CHIPS proceedings (Chapter 48
PARENT GUIDE TO THE JUVENILE COURT CHIPS PROCESS INTRODUCTION This booklet has been prepared to help parents gain a better understanding of what to expect in Juvenile Court CHIPS proceedings (Chapter 48
Effectiveness, efficiency and equity principle- this refers to the most appropriate use of resources to meet the needs of patients.
 Introduction Where medicine meets the law, there is a fascinating and often complex interaction. One the one hand, as a doctor you are expected to work with your patient to help them to make informed choices
Introduction Where medicine meets the law, there is a fascinating and often complex interaction. One the one hand, as a doctor you are expected to work with your patient to help them to make informed choices
GOVERNMENT PROPOSALS FOR REFORM OF LEGAL CLAIMS AGAINST THE NHS A BRIEFING FROM THE ASSOCIATION OF PERSONAL INJURY LAWYERS (APIL)
 Association of Personal Injury Lawyers GOVERNMENT PROPOSALS FOR REFORM OF LEGAL CLAIMS AGAINST THE NHS A BRIEFING FROM THE ASSOCIATION OF PERSONAL INJURY LAWYERS (APIL) CONTENTS Introduction 3 5 ways for
Association of Personal Injury Lawyers GOVERNMENT PROPOSALS FOR REFORM OF LEGAL CLAIMS AGAINST THE NHS A BRIEFING FROM THE ASSOCIATION OF PERSONAL INJURY LAWYERS (APIL) CONTENTS Introduction 3 5 ways for
Loss of. focus. Report from our investigation into the care and treatment of Ms Z
 A Loss of focus Report from our investigation into the care and treatment of Ms Z Contents Who we are 1 What we do 1 Introduction 1 How we conducted the investigation 3 Summary of Ms Z s Circumstances
A Loss of focus Report from our investigation into the care and treatment of Ms Z Contents Who we are 1 What we do 1 Introduction 1 How we conducted the investigation 3 Summary of Ms Z s Circumstances
UNITED NATIONS OFFICE OF THE UNITED NATIONS HIGH COMMISSIONER FOR HUMAN RIGHTS NATIONS UNIES HAUT COMMISSARIAT DES NATIONS UNIES AUX DROITS DE L HOMME
 NATIONS UNIES HAUT COMMISSARIAT DES NATIONS UNIES AUX DROITS DE L HOMME PROCEDURES SPECIALES DU CONSEIL DES DROITS DE L HOMME UNITED NATIONS OFFICE OF THE UNITED NATIONS HIGH COMMISSIONER FOR HUMAN RIGHTS
NATIONS UNIES HAUT COMMISSARIAT DES NATIONS UNIES AUX DROITS DE L HOMME PROCEDURES SPECIALES DU CONSEIL DES DROITS DE L HOMME UNITED NATIONS OFFICE OF THE UNITED NATIONS HIGH COMMISSIONER FOR HUMAN RIGHTS
Inquiry into the quality of healthcare at Yarl s Wood immigration removal centre. 20 24 February 2006 by HM Chief Inspector of Prisons
 Inquiry into the quality of healthcare at Yarl s Wood immigration removal centre 20 24 February 2006 by HM Chief Inspector of Prisons 1 ISBN: 1-84726-083-7 978-1-84276-083-3 Published by: HM Inspectorate
Inquiry into the quality of healthcare at Yarl s Wood immigration removal centre 20 24 February 2006 by HM Chief Inspector of Prisons 1 ISBN: 1-84726-083-7 978-1-84276-083-3 Published by: HM Inspectorate
Tuberculosis Management of People Knowingly Placing Others at Risk of Infection
 Policy Directive Ministry of Health, NSW 73 Miller Street North Sydney NSW 2060 Locked Mail Bag 961 North Sydney NSW 2059 Telephone (02) 9391 9000 Fax (02) 9391 9101 http://www.health.nsw.gov.au/policies/
Policy Directive Ministry of Health, NSW 73 Miller Street North Sydney NSW 2060 Locked Mail Bag 961 North Sydney NSW 2059 Telephone (02) 9391 9000 Fax (02) 9391 9101 http://www.health.nsw.gov.au/policies/
This document is classified as OFFICIAL in accordance with the IPCC s protective marking scheme
 Case 4 Bulletin 23 Man with a head injury who was also intoxicated Published 26 March 2015 For archived bulletins, learning reports and related background documents please visit www.ipcc.gov.uk/learning-the-lessons
Case 4 Bulletin 23 Man with a head injury who was also intoxicated Published 26 March 2015 For archived bulletins, learning reports and related background documents please visit www.ipcc.gov.uk/learning-the-lessons
International Transfer of Prisoners (South Australia) Act 1998
 Version: 2.4.2000 South Australia International Transfer of Prisoners (South Australia) Act 1998 An Act relating to the transfer of prisoners to and from Australia. Contents Part 1 Preliminary 1 Short
Version: 2.4.2000 South Australia International Transfer of Prisoners (South Australia) Act 1998 An Act relating to the transfer of prisoners to and from Australia. Contents Part 1 Preliminary 1 Short
NOTICE OF PRIVACY PRACTICES. The University of North Carolina at Chapel Hill. UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates
 NOTICE OF PRIVACY PRACTICES The University of North Carolina at Chapel Hill UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU
NOTICE OF PRIVACY PRACTICES The University of North Carolina at Chapel Hill UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU
Problems in Medical Report Writing for Asylum Seekers
 Problems in Medical Report Writing for Asylum Seekers Michael Peel Ashgate Publishing Limited 1998 Reproduced with the kind permission of the Ashgate Publishing Limited This paper first appeared in the
Problems in Medical Report Writing for Asylum Seekers Michael Peel Ashgate Publishing Limited 1998 Reproduced with the kind permission of the Ashgate Publishing Limited This paper first appeared in the
Taking Care of Yourself and Your Family After Self-Harm or Suicidal Thoughts A Family Guide
 It is devastating to have a suicidal family member and to live with the feelings that go with this kind of traumatic anxiety. That is why this guide is developed for you. It will give you some important
It is devastating to have a suicidal family member and to live with the feelings that go with this kind of traumatic anxiety. That is why this guide is developed for you. It will give you some important
Rights and Entitlements
 Rights and Entitlements How you should be treated if you are taken in by the police. Please keep this information and read it as soon as possible. It will help you to make choices while you are at the
Rights and Entitlements How you should be treated if you are taken in by the police. Please keep this information and read it as soon as possible. It will help you to make choices while you are at the
DISCIPLINARY, DISMISSAL AND GRIEVANCE PROCEDURES. Guidance for employers
 DISCIPLINARY, DISMISSAL AND GRIEVANCE PROCEDURES Guidance for employers Contents Foreword...1 Chapter 1: Disciplinary and dismissal procedures...2 Communicating your disciplinary and grievance procedures...2
DISCIPLINARY, DISMISSAL AND GRIEVANCE PROCEDURES Guidance for employers Contents Foreword...1 Chapter 1: Disciplinary and dismissal procedures...2 Communicating your disciplinary and grievance procedures...2
PRISONERS INTERNATIONAL TRANSFER (QUEENSLAND) ACT 1997
 Queensland PRISONERS INTERNATIONAL TRANSFER (QUEENSLAND) ACT 1997 Reprinted as in force on 1 April 1999 (Act not amended up to this date) Reprint No. 1 This reprint is prepared by the Office of the Queensland
Queensland PRISONERS INTERNATIONAL TRANSFER (QUEENSLAND) ACT 1997 Reprinted as in force on 1 April 1999 (Act not amended up to this date) Reprint No. 1 This reprint is prepared by the Office of the Queensland
Clinical negligence. Grounds
 Clinical negligence Clinical negligence occurs when the care or treatment the Claimant received from a health service provider was below the standard that is expected. This test was established in the
Clinical negligence Clinical negligence occurs when the care or treatment the Claimant received from a health service provider was below the standard that is expected. This test was established in the
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Vision MH - Cornerstone House Barnet Lane, Elstree, WD6 3QU
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Vision MH - Cornerstone House Barnet Lane, Elstree, WD6 3QU
A Guide for Larimer County Parents
 Services Child Protection A Guide for Larimer County Parents This booklet was prepared by the Program Committee of the Larimer County Child Advocacy Center in consultation with the Larimer County Department
Services Child Protection A Guide for Larimer County Parents This booklet was prepared by the Program Committee of the Larimer County Child Advocacy Center in consultation with the Larimer County Department
Justice denied. A summary of our investigation into the care and treatment of Ms A
 Justice denied A summary of our investigation into the care and treatment of Ms A Contents Introduction 1 Summary of our key findings 2 Key recommendations 5 1 Introduction Ms A is a 67 year old woman
Justice denied A summary of our investigation into the care and treatment of Ms A Contents Introduction 1 Summary of our key findings 2 Key recommendations 5 1 Introduction Ms A is a 67 year old woman
CHILDREN AND YOUNG PEOPLE SERVICE ALCOHOL, DRUG OR OTHER SUBSTANCE MISUSE OR ABUSE POLICY
 CHILDREN AND YOUNG PEOPLE SERVICE ALCOHOL, DRUG OR OTHER SUBSTANCE MISUSE OR ABUSE POLICY KirkleesEdnet/Management/HumanResources APRIL 2008 Prepared by: Human Resources Strategy Unit Revised: November
CHILDREN AND YOUNG PEOPLE SERVICE ALCOHOL, DRUG OR OTHER SUBSTANCE MISUSE OR ABUSE POLICY KirkleesEdnet/Management/HumanResources APRIL 2008 Prepared by: Human Resources Strategy Unit Revised: November
Independent investigation into the care and treatment of Ms M. Case 13. Commissioned by NHS London
 Independent investigation into the care and treatment of Ms M Case 13 Commissioned by NHS London Contents Page No 1. Introduction to the Incident 3 2. Condolences 3 3. Trust Internal Investigation 3 4.
Independent investigation into the care and treatment of Ms M Case 13 Commissioned by NHS London Contents Page No 1. Introduction to the Incident 3 2. Condolences 3 3. Trust Internal Investigation 3 4.
SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION. Assaults on Clients: Suspected or Reported
 SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION DATE: March 22, 2001 MENTAL HEALTH POLICY: MH 01-03 SUBJECT: Assaults on Clients: Suspected or Reported AUTHORITY: California Welfare and Institution Codes
SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION DATE: March 22, 2001 MENTAL HEALTH POLICY: MH 01-03 SUBJECT: Assaults on Clients: Suspected or Reported AUTHORITY: California Welfare and Institution Codes
Witness Protection Act 1995 No 87
 New South Wales Witness Protection Act 1995 No 87 Status information Currency of version Current version for 5 October 2012 to date (generated 10 October 2012 at 19:15). Legislation on the NSW legislation
New South Wales Witness Protection Act 1995 No 87 Status information Currency of version Current version for 5 October 2012 to date (generated 10 October 2012 at 19:15). Legislation on the NSW legislation
Best Practices in Mental Health at Corrections Facilities
 POLICY BRIEF November 2011 Best Practices in Mental Health at Corrections Facilities Sahil Jain Introduction Police, court personnel, and correctional staff interact with, stabilize, and treat more persons
POLICY BRIEF November 2011 Best Practices in Mental Health at Corrections Facilities Sahil Jain Introduction Police, court personnel, and correctional staff interact with, stabilize, and treat more persons
Criminal Injuries Compensation: Your rights
 Criminal Injuries Compensation: Your rights A brief leaflet summarising the 2012 Scheme. Includes information about how LSA can help. www.lsa.org.uk Freephone: 0800 315 8450 About this leaflet If you
Criminal Injuries Compensation: Your rights A brief leaflet summarising the 2012 Scheme. Includes information about how LSA can help. www.lsa.org.uk Freephone: 0800 315 8450 About this leaflet If you
Personal beliefs and medical practice
 You can find the latest version of this guidance on our website at www.gmc-uk.org/guidance. Published 25 March 2013 Comes into effect 22 April 2013 Personal beliefs and medical practice 1 In Good medical
You can find the latest version of this guidance on our website at www.gmc-uk.org/guidance. Published 25 March 2013 Comes into effect 22 April 2013 Personal beliefs and medical practice 1 In Good medical
1. Tell the police if you want a solicitor to help you while you are at the police station. It is free.
 The following rights and entitlements are guaranteed to you under the law in England and Wales and comply with the European Convention on Human Rights. Remember your rights 1. Tell the police if you want
The following rights and entitlements are guaranteed to you under the law in England and Wales and comply with the European Convention on Human Rights. Remember your rights 1. Tell the police if you want
JUSTICE FOR MESOTHELIOMA VICTIMS
 JUSTICE FOR MESOTHELIOMA VICTIMS Fact, fiction and ideas for change A briefing from The Association of Personal Injury Lawyers (APIL) November 2013 The Association of Personal Injury Lawyers (APIL) is
JUSTICE FOR MESOTHELIOMA VICTIMS Fact, fiction and ideas for change A briefing from The Association of Personal Injury Lawyers (APIL) November 2013 The Association of Personal Injury Lawyers (APIL) is
Guide to compensation claims against the police
 Tel: 020 8492 2290 I N C O R P O R A T I N G D O N A L D G A L B R A I T H & C O Guide to compensation claims against the police This guide is designed to provide a general overview to bringing compensation
Tel: 020 8492 2290 I N C O R P O R A T I N G D O N A L D G A L B R A I T H & C O Guide to compensation claims against the police This guide is designed to provide a general overview to bringing compensation
B e f o r e: SECRETARY OF STATE FOR THE HOME DEPARTMENT
 Neutral Citation Number: [2009] EWHC 1888 (Admin) IN THE HIGH COURT OF JUSTICE QUEEN'S BENCH DIVISION THE ADMINISTRATIVE COURT Case No. CO/653/2007 Royal Courts of Justice Strand London WC2A 2LL Date:
Neutral Citation Number: [2009] EWHC 1888 (Admin) IN THE HIGH COURT OF JUSTICE QUEEN'S BENCH DIVISION THE ADMINISTRATIVE COURT Case No. CO/653/2007 Royal Courts of Justice Strand London WC2A 2LL Date:
Traumatic Stress. and Substance Use Problems
 Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
Traumatic Stress and Substance Use Problems The relation between substance use and trauma Research demonstrates a strong link between exposure to traumatic events and substance use problems. Many people
The Code. Professional standards of practice and behaviour for nurses and midwives
 The Code Professional standards of practice and behaviour for nurses and midwives Introduction The Code contains the professional standards that registered nurses and midwives must uphold. UK nurses and
The Code Professional standards of practice and behaviour for nurses and midwives Introduction The Code contains the professional standards that registered nurses and midwives must uphold. UK nurses and
HOW TO GET OUT OF DETENTION
 HOW TO GET OUT OF DETENTION a free guide for detainees BiDBail for Immigration Detainees This handbook tells you how you can get released from detention. This handbook is updated regularly. Bail for Immigration
HOW TO GET OUT OF DETENTION a free guide for detainees BiDBail for Immigration Detainees This handbook tells you how you can get released from detention. This handbook is updated regularly. Bail for Immigration
Independent Advisory Panel on Non-Compliance Management (IAPNCM): comments from the Prisons and Probation Ombudsman
 Stephen Shaw CBE Chair, Independent Advisory Panel on Non-Compliance Management c/o Emma Ross Home Office 2 nd Floor, Bedford Point 35 Dingwall Road Croydon CR9 2EF 31 May 2013 Dear Stephen, Independent
Stephen Shaw CBE Chair, Independent Advisory Panel on Non-Compliance Management c/o Emma Ross Home Office 2 nd Floor, Bedford Point 35 Dingwall Road Croydon CR9 2EF 31 May 2013 Dear Stephen, Independent
A GUIDE TO FAMILY LAW LEGAL AID
 A GUIDE TO FAMILY LAW LEGAL AID Important new rules in relation to legal aid were introduced on 1 April 2013 by the Legal Aid, Sentencing and Punishment of Offenders Act 2012 (LASPO). This legal guide
A GUIDE TO FAMILY LAW LEGAL AID Important new rules in relation to legal aid were introduced on 1 April 2013 by the Legal Aid, Sentencing and Punishment of Offenders Act 2012 (LASPO). This legal guide
Rights for Individuals in Mental Health Facilities
 HANDBOOK Rights for Individuals in Mental Health Facilities Admitted Under the Lanterman-Petris-Short Act C A L I F O R N I A D E P A R T M E N T O F Mental Health How to Reach Your Patients Rights Advocate
HANDBOOK Rights for Individuals in Mental Health Facilities Admitted Under the Lanterman-Petris-Short Act C A L I F O R N I A D E P A R T M E N T O F Mental Health How to Reach Your Patients Rights Advocate
Legal Support Service South West. Support for life after childhood brain and other serious injuries. www.childbraininjurytrust.org.
 Legal Support Service South West Support for life after childhood brain and other serious injuries www.childbraininjurytrust.org.uk Hello and welcome to the Legal Support Services booklet for the South
Legal Support Service South West Support for life after childhood brain and other serious injuries www.childbraininjurytrust.org.uk Hello and welcome to the Legal Support Services booklet for the South
Alcohol and drugs prevention, treatment and recovery: why invest?
 Alcohol and drugs prevention, treatment and recovery: why invest? 1 Alcohol problems are widespread 9 million adults drink at levels that increase the risk of harm to their health 1.6 million adults show
Alcohol and drugs prevention, treatment and recovery: why invest? 1 Alcohol problems are widespread 9 million adults drink at levels that increase the risk of harm to their health 1.6 million adults show
HOSPITAL POLICY AND INFORMATION MANUAL Date Issued: Date Last Revised: Next Review Date: Approved By:
 Page 1 of 12 Policy Applies to: All Mercy Hospital staff. Compliance by Credentialed Specialists or Allied Health Professionals, contractors, visitors and patients will be facilitated by Mercy Hospital
Page 1 of 12 Policy Applies to: All Mercy Hospital staff. Compliance by Credentialed Specialists or Allied Health Professionals, contractors, visitors and patients will be facilitated by Mercy Hospital
NHS Constitution The NHS belongs to the people. This Constitution principles values rights pledges responsibilities
 for England 21 January 2009 2 NHS Constitution The NHS belongs to the people. It is there to improve our health and well-being, supporting us to keep mentally and physically well, to get better when we
for England 21 January 2009 2 NHS Constitution The NHS belongs to the people. It is there to improve our health and well-being, supporting us to keep mentally and physically well, to get better when we
U.C. Riverside Police Department Policy Manual Use of Force
 300.1 PURPOSE AND SCOPE This policy provides guidelines on the reasonable use of force. While there is no way to specify the exact amount or type of reasonable force to be applied in any situation, every
300.1 PURPOSE AND SCOPE This policy provides guidelines on the reasonable use of force. While there is no way to specify the exact amount or type of reasonable force to be applied in any situation, every
Walking a Tightrope. Alcohol and other drug use and violence: A guide for families. Alcohol- and Other Drug-related Violence
 Walking a Tightrope Alcohol and other drug use and violence: A guide for families Alcohol- and Other Drug-related Violence Alcohol and other drug use and family violence often occur together. Families
Walking a Tightrope Alcohol and other drug use and violence: A guide for families Alcohol- and Other Drug-related Violence Alcohol and other drug use and family violence often occur together. Families
Get in on the Act: Children and Families Act 2014. Corporate
 Get in on the Act: Children and Families Act 2014 Corporate Get in on the Act: Children and Families Act 2014 Background The Children and Families Bill was introduced in the House of Commons on 4 February
Get in on the Act: Children and Families Act 2014 Corporate Get in on the Act: Children and Families Act 2014 Background The Children and Families Bill was introduced in the House of Commons on 4 February
Protecting Vulnerable Adults from Abuse and Neglect: a U.S. Experience. Page Ulrey January 15, 2015
 Protecting Vulnerable Adults from Abuse and Neglect: a U.S. Experience Page Ulrey January 15, 2015 Question. Report. Collaborate. My Position Senior Deputy Prosecuting Attorney Elder Abuse Project King
Protecting Vulnerable Adults from Abuse and Neglect: a U.S. Experience Page Ulrey January 15, 2015 Question. Report. Collaborate. My Position Senior Deputy Prosecuting Attorney Elder Abuse Project King
Improving the Performance of Doctors. Complaints Investigations and Remediation
 Improving the Performance of Doctors Complaints Investigations and Remediation SHARING INFORMATION WITH PATIENTS AND CARERS HAPIA GOOD PRACTICE GUIDE 2014 HEALTHWATCH AND PUBLIC INVOLVEMENT ASSOCIATION
Improving the Performance of Doctors Complaints Investigations and Remediation SHARING INFORMATION WITH PATIENTS AND CARERS HAPIA GOOD PRACTICE GUIDE 2014 HEALTHWATCH AND PUBLIC INVOLVEMENT ASSOCIATION
Southwest Regional Office, 110 Broadway, Ste. 300, San Antonio, Texas 78205
 Southwest Regional Office, 110 Broadway, Ste. 300, San Antonio, Texas 78205 Testimony of Marisa Bono, MALDEF Staff Attorney PREA and Complaints of Sexual Abuse at ICE Karnes Facility U.S. Commission on
Southwest Regional Office, 110 Broadway, Ste. 300, San Antonio, Texas 78205 Testimony of Marisa Bono, MALDEF Staff Attorney PREA and Complaints of Sexual Abuse at ICE Karnes Facility U.S. Commission on
A response by the Association of Personal Injury Lawyers
 Northern Ireland Office Proposed Northern Ireland Criminal Injuries Compensation Scheme 2009 A response by the Association of Personal Injury Lawyers June 2008 The Association of Personal Injury Lawyers
Northern Ireland Office Proposed Northern Ireland Criminal Injuries Compensation Scheme 2009 A response by the Association of Personal Injury Lawyers June 2008 The Association of Personal Injury Lawyers
FEEDBACK ON REPORTS BY DR. K.J.B. RIX IN CIVIL CASES
 FEEDBACK ON REPORTS BY DR. K.J.B. RIX IN CIVIL CASES I would be grateful if you would accept instructions to see xxxx and to prepare your report. I have no doubt that this will be with the same degree
FEEDBACK ON REPORTS BY DR. K.J.B. RIX IN CIVIL CASES I would be grateful if you would accept instructions to see xxxx and to prepare your report. I have no doubt that this will be with the same degree
Adviceguide Advice that makes a difference
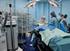 Health in prison Getting medical treatment in prison If you re in prison, you should get the same health services as you'd get from the NHS. This includes mental health services. Qualified doctors, dentists,
Health in prison Getting medical treatment in prison If you re in prison, you should get the same health services as you'd get from the NHS. This includes mental health services. Qualified doctors, dentists,
THE CHARTERED INSTITUTE OF LEGAL EXECUTIVES UNIT 8 IMMIGRATION LAW *
 14 January 2014 Level 6 IMMIGRATION LAW Subject Code L6-8 THE CHARTERED INSTITUTE OF LEGAL EXECUTIVES UNIT 8 IMMIGRATION LAW * Time allowed: 3 hours plus 15 minutes reading time Instructions to Candidates
14 January 2014 Level 6 IMMIGRATION LAW Subject Code L6-8 THE CHARTERED INSTITUTE OF LEGAL EXECUTIVES UNIT 8 IMMIGRATION LAW * Time allowed: 3 hours plus 15 minutes reading time Instructions to Candidates
The Arrest Pocketbook
 British Columbia British Columbia Civil Liberties Association Civil Liberties Association The Arrest Pocketbook A Guide to Your Rights by David Eby B.C. Civil Liberties Association, 2008 No commercial
British Columbia British Columbia Civil Liberties Association Civil Liberties Association The Arrest Pocketbook A Guide to Your Rights by David Eby B.C. Civil Liberties Association, 2008 No commercial
Journeys through the Criminal Justice System for Suspects, Accused and Offenders with Learning Disabilities. A Graphic Representation
 Journeys through the Criminal Justice System for Suspects, Accused and Offenders with Learning Disabilities A Graphic Representation 0 Contents Introduction page 2 Methodology page 4 Stage One Getting
Journeys through the Criminal Justice System for Suspects, Accused and Offenders with Learning Disabilities A Graphic Representation 0 Contents Introduction page 2 Methodology page 4 Stage One Getting
ILPA RESPONSE TO CONSULTATION: REFUSING ENTRY OR STAY TO NHS DEBTORS
 ILPA RESPONSE TO CONSULTATION: REFUSING ENTRY OR STAY TO NHS DEBTORS A PUBLIC CONSULTATION AROUND PROPOSED CHANGES TO THE IMMIGRATION RULES, UKBA (February 2010) ILPA The Immigration Law Practitioners
ILPA RESPONSE TO CONSULTATION: REFUSING ENTRY OR STAY TO NHS DEBTORS A PUBLIC CONSULTATION AROUND PROPOSED CHANGES TO THE IMMIGRATION RULES, UKBA (February 2010) ILPA The Immigration Law Practitioners
Borderline personality disorder
 Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
BOURNEMOUTH & POOLE SAFEGUARDING ADULT BOARD
 BOURNEMOUTH & POOLE SAFEGUARDING ADULT BOARD EXECUTIVE SUMMARY Regarding the Serious Case Review In respect of Mrs. A Author: Elizabeth Whatley Date: 4 November 2010 1. INTRODUCTION 1 1.1 MRS. A was an
BOURNEMOUTH & POOLE SAFEGUARDING ADULT BOARD EXECUTIVE SUMMARY Regarding the Serious Case Review In respect of Mrs. A Author: Elizabeth Whatley Date: 4 November 2010 1. INTRODUCTION 1 1.1 MRS. A was an
LEGAL SCHEME REGULATIONS
 LEGAL SCHEME REGULATIONS These Regulations came into force on 1 July 2014. 1 Introduction 1.1 These Regulations govern the Union s legal Scheme. The Rules of the Union set out your other rights and entitlements.
LEGAL SCHEME REGULATIONS These Regulations came into force on 1 July 2014. 1 Introduction 1.1 These Regulations govern the Union s legal Scheme. The Rules of the Union set out your other rights and entitlements.
ADVANCE HEALTH DIRECTIVE
 Form 4 Queensland Powers of Attorney Act 1998 (Section 44(2)) ADVANCE HEALTH DIRECTIVE This form deals with your future health care. The time may come when you cannot speak for yourself. By completing
Form 4 Queensland Powers of Attorney Act 1998 (Section 44(2)) ADVANCE HEALTH DIRECTIVE This form deals with your future health care. The time may come when you cannot speak for yourself. By completing
Ministry of Social Affairs and Health, Finland N.B. Unofficial translation. Legally binding only in Finnish and Swedish
 Ministry of Social Affairs and Health, Finland N.B. Unofficial translation. Legally binding only in Finnish and Swedish No. 1116/1990 Mental Health Act Issued in Helsinki on 14 December 1990 Chapter 1
Ministry of Social Affairs and Health, Finland N.B. Unofficial translation. Legally binding only in Finnish and Swedish No. 1116/1990 Mental Health Act Issued in Helsinki on 14 December 1990 Chapter 1
VISIT AND MONITORING REPORT
 VISIT AND MONITORING REPORT An Analysis of emergency detention certificates revoked by approved medical practitioners Report compiled for the Mental Welfare Commission by Mira Thomas and Karthik Bommu,
VISIT AND MONITORING REPORT An Analysis of emergency detention certificates revoked by approved medical practitioners Report compiled for the Mental Welfare Commission by Mira Thomas and Karthik Bommu,
Rome Workshop Cooperation between state officials and NGOs
 Rome Workshop Cooperation between state officials and NGOs I understand that participants are expecting to engage in this workshop, so I do not intend to speak initially for very long. l will briefly introduce
Rome Workshop Cooperation between state officials and NGOs I understand that participants are expecting to engage in this workshop, so I do not intend to speak initially for very long. l will briefly introduce
Clinical Negligence: A guide to making a claim
 : A guide to making a claim 2 Our guide to making a clinical negligence claim At Kingsley Napley, our guiding principle is to provide you with a dedicated client service and we aim to make the claims process
: A guide to making a claim 2 Our guide to making a clinical negligence claim At Kingsley Napley, our guiding principle is to provide you with a dedicated client service and we aim to make the claims process
Vicarious liability of a charity or its trustees
 1 of 7 Guidance Vicarious liability of a charity or its trustees Contents In general, for what are trustees liable? Liability for the actions or omissions of others What does the law cover in this area?
1 of 7 Guidance Vicarious liability of a charity or its trustees Contents In general, for what are trustees liable? Liability for the actions or omissions of others What does the law cover in this area?
How To Protect Yourself From Violence
 FAMILY VIOLENCE Violence takes many forms. It is unacceptable whenever it happens. Violence by a family member who is loved and trusted can be particularly devastating. Family violence happens where the
FAMILY VIOLENCE Violence takes many forms. It is unacceptable whenever it happens. Violence by a family member who is loved and trusted can be particularly devastating. Family violence happens where the
Criminal Justice (Scotland) Bill [AS INTRODUCED]
![Criminal Justice (Scotland) Bill [AS INTRODUCED] Criminal Justice (Scotland) Bill [AS INTRODUCED]](/thumbs/26/8940436.jpg) Criminal Justice (Scotland) Bill [AS INTRODUCED] CONTENTS Section PART 1 ARREST AND CUSTODY CHAPTER 1 ARREST BY POLICE 1 Power of a constable 2 Exercise of the power Arrest without warrant Procedure following
Criminal Justice (Scotland) Bill [AS INTRODUCED] CONTENTS Section PART 1 ARREST AND CUSTODY CHAPTER 1 ARREST BY POLICE 1 Power of a constable 2 Exercise of the power Arrest without warrant Procedure following
NOTICE OF PRIVACY PRACTICES UNIVERSITY OF CALIFORNIA DAVIS HEALTH SYSTEM
 NOTICE OF PRIVACY PRACTICES Effective Date: April 14, 2003 UNIVERSITY OF CALIFORNIA DAVIS HEALTH SYSTEM THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN
NOTICE OF PRIVACY PRACTICES Effective Date: April 14, 2003 UNIVERSITY OF CALIFORNIA DAVIS HEALTH SYSTEM THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN
ALLERDALE BOROUGH COUNCIL SECTION. FOOD HYGIENE POLICY & PROCEDURES
 ALLERDALE BOROUGH COUNCIL SECTION. FOOD HYGIENE POLICY & PROCEDURES PAGE Food Safety Enforcement Policy Revision No: 0 Date: January 2002 Authorised Signature: FHP... 1. Purpose This document establishes
ALLERDALE BOROUGH COUNCIL SECTION. FOOD HYGIENE POLICY & PROCEDURES PAGE Food Safety Enforcement Policy Revision No: 0 Date: January 2002 Authorised Signature: FHP... 1. Purpose This document establishes
Health Committee information
 Health Committee information This leaflet is for nurses and midwives who have been referred to our Health Committee because an allegation has been made against them and, after initial investigation, we
Health Committee information This leaflet is for nurses and midwives who have been referred to our Health Committee because an allegation has been made against them and, after initial investigation, we
FROM CHARGE TO TRIAL: A GUIDE TO CRIMINAL PROCEEDINGS
 FROM CHARGE TO TRIAL: A GUIDE TO CRIMINAL PROCEEDINGS If you are experiencing, or have experienced, domestic violence and/or sexual violence there are a number of ways the law can protect you. This includes
FROM CHARGE TO TRIAL: A GUIDE TO CRIMINAL PROCEEDINGS If you are experiencing, or have experienced, domestic violence and/or sexual violence there are a number of ways the law can protect you. This includes
Statutory Rape: What You Should Know
 Statutory Rape: What You Should Know 2013 Why Do You Need To Read This? Many teens are concerned about the laws regarding something commonly called statutory rape. This brochure will explain what statutory
Statutory Rape: What You Should Know 2013 Why Do You Need To Read This? Many teens are concerned about the laws regarding something commonly called statutory rape. This brochure will explain what statutory
Key Legal terms: Family Law Issues for Immigrant, Refugee and Non Status Women
 Key Legal terms: Family Law Issues for Immigrant, Refugee and Non Status Women Permanent Resident A permanent resident is an immigrant or refugee who has been given the right to live in Canada permanently.
Key Legal terms: Family Law Issues for Immigrant, Refugee and Non Status Women Permanent Resident A permanent resident is an immigrant or refugee who has been given the right to live in Canada permanently.
Child Abuse, Child Neglect. What Parents Should Know If They Are Investigated
 Child Abuse, Child Neglect What Parents Should Know If They Are Investigated Written by South Carolina Appleseed Legal Justice Center with editing and assistance from the Children s Law Center and the
Child Abuse, Child Neglect What Parents Should Know If They Are Investigated Written by South Carolina Appleseed Legal Justice Center with editing and assistance from the Children s Law Center and the
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Appletree Care Home 158 Burnt Oak Broadway, Burnt Oak, Edgware,
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Appletree Care Home 158 Burnt Oak Broadway, Burnt Oak, Edgware,
COMPLAINTS IN RETIREMENT HOMES
 COMPLAINTS IN RETIREMENT HOMES This article was originally published in ACE s Spring/Summer 2013 Newsletter which is available at www.acelaw.ca Conflicts may arise in any type of housing. Retirement homes
COMPLAINTS IN RETIREMENT HOMES This article was originally published in ACE s Spring/Summer 2013 Newsletter which is available at www.acelaw.ca Conflicts may arise in any type of housing. Retirement homes
I WAS ARRESTED BY THE POLICE AND I BELIEVE THEY WILL TURN ME OVER TO IMMIGRATION. I WAS ARRESTED BY IMMIGRATION.
 I AM IN IMMIGRATION DETENTION W HAT I WAS ARRESTED BY THE POLICE AND I BELIEVE THEY WILL TURN ME OVER TO IMMIGRATION. ARE MY RIGHTS? I WAS ARRESTED BY IMMIGRATION. You have a right NOT to sign any statements
I AM IN IMMIGRATION DETENTION W HAT I WAS ARRESTED BY THE POLICE AND I BELIEVE THEY WILL TURN ME OVER TO IMMIGRATION. ARE MY RIGHTS? I WAS ARRESTED BY IMMIGRATION. You have a right NOT to sign any statements
Understanding the Civil Involuntary Commitment Process
 Understanding the Civil Involuntary Commitment Process About the Author By D. Renée Hildebrant http://www.okbar.org/obj/articles_05/021205.htm Oklahoma Bar Journal D. Renée Hildebrant is the trial court
Understanding the Civil Involuntary Commitment Process About the Author By D. Renée Hildebrant http://www.okbar.org/obj/articles_05/021205.htm Oklahoma Bar Journal D. Renée Hildebrant is the trial court
Contents. Section/Paragraph Description Page Number
 - NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICA CLINICAL NON CLINICAL - CLINICAL CLINICAL Complaints Policy Incorporating Compliments, Comments,
- NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICAL NON CLINICA CLINICAL NON CLINICAL - CLINICAL CLINICAL Complaints Policy Incorporating Compliments, Comments,
