Hypodermoclysis (HDC) Administration
|
|
|
- Abraham Bell
- 9 years ago
- Views:
Transcription
1 Approved by: Hypodermoclysis (HDC) Administration Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-315 Date Approved September 15, 2015 Date Effective October 9, 2015 Next Review (3 years from Effective Date) October 2018 Purpose Policy Statement Applicability Principles Procedure Definitions This policy acts as a resource for health care professionals when providing care for patients receiving subcutaneous (SC) infusions when oral or transdermal route is inappropriate or ineffective. Health care professionals shall adhere to the requirements outlined herein when providing care for patients receiving subcutaneous (SC) infusions. This policy and procedure applies to all Covenant Health facilities, staff, members of the medical staff, volunteers, students and any other persons acting on behalf of Covenant Health. Subcutaneous infusions provide continuous long or short-term administration of parenteral drugs or fluids into the loose connective tissue underlying the dermis. Fluid is absorbed into the intravascular compartment by a combination of perfusion, diffusion, hydrostatic pressure and osmotic pressure. A short length of catheter is used for several days, although therapy may last for months. See attached. Hypodermoclysis: The continuous administration of solution, which may or may not contain medication, into subcutaneous tissue. This definition is interchangeable with subcutaneous infusion. Subcutaneous Injection: The intermittent administration of a dose of medication directly into the subcutaneous tissue or into/via the injection site of an indwelling subcutaneous catheter. Health care professional means an individual who is a member of a regulated health discipline, as defined by the Health Disciplines Act or the Health Professions Act, and who practises within scope or role. Related Documents References Appendix A BD Saf-T-Intima Product Codes Appendix B BD Saf-T-Intima Brochure Journal of Infusion Nursing: Infusion Nursing Standards of Practice Jan/Feb supplemental vol. 34, No1S ISSN Oncology Nursing Society. Access Device Guidelines: Recommendations for Nursing Practice and Education. Editor Dawn Camp-Sorrell Third Edition Policy and Procedures for Infusion Nursing, 4 th edition. Infusion nurses society. 2011
2 VII-B-315 Page 2 of 16 Revisions June 25, 2014 Infusion Nursing society: Infusion nursing: an evidence-based approach.. 3rd edition. 2010Editied by Mary Alexander. Lyabarger, Edward H. Hypodermoclysis in the home and long-term care settings, Journal of infusion nursing VOLUME 32 NUMBER 1 JANUARY/FEBRUARY 2009 Dychter, Samual, Gold, David, Haller, Michael F. subcutaneous drug delivery: a route to increased safety, patient satisfaction and reduced costs. Jouranl of infusion nursing. 2012, volume 35, No. 3, May/June Covenant Health Corporate Policy/Procedure #VII-B-110, Full Scope of Practice Coyle, Ness (1986), Continuous Subcutaneous Infusions of Opiates in Cancer Patient with Pain, Oncology Nursing Forum, Vol 13, No. 4, p Bruera, Dr. Eduardo, de Stoutz, Dr. Noemi, Fainsinger, Dr. Robin, Spachynski, Kathy, Suarez-Almazor, Dr. Maria, Hanson, John (1995), Comparison of Two Different Concentrations of Hyaluronidase in Patients Receiving One Hour Infusions of Hypodermoclysis, Journal of Pain and Symptom Management, Vol10, No 7, p Fainsinger, Dr. Robin; MacEachern, Tara; Miller, Dr. Melvin, Bruera, Dr. Eduardo; Spachynski, Kathy; Kuehn, Norma; Hanson, John (1994), The Use of Hypodermoclysis for Rehydration in Terminally Ill Cancer Patients, Journal of Pain and Symptom Management, 9(5), p Fainsinger, Dr. Robin; Bruera, Dr. Eduardo (1994), The Management of Dehydration in Terminally Ill Patients, Journal at Palliative Care, 10(3), p Logan, Marion and Fothergill-Bourbonnais, Continuous Subcutaneous Infusion of Narcotics: Patient Care and Family Support: A Guide to CSCI for Nurses, Knoll Pharmaceuticals Macmillan, Karen; Bruera, Dr. Eduardo; Kuehn, Norma;Selmser, Pat; Macmillan, Andrew (1994), A Prospective Comparison Study Between a Butterfly Catheter and a Teflon Cannula for Subcutaneous Narcotic Administration, Journal of Pain and Symptom Management, 9(2), p
3 Table of Contents VII-B-315 Page 3 of 16 PROCEDURE 1.0 General Information 2.0 Initiating a Subcutaneous Infusion Site / Necessary Equipment 3.0 Procedure 4.0 Solutions Which May be Used in Hypodermoclysis 5.0 Insertion of Indwelling Subcutaneous Catheter for Medication Injection - Procedure 6.0. Care Guidelines 7.0 Removal 8.0 Documentation in the Patient Care Record
4 VII-B-315 Page 4 of GENERAL INFORMATION 1.1 The following types of devices are used: a. Small gauge, short length catheters are recommended because of the longer life and reduced risk of needlestick injury and exposure to blood borne pathogens (to both patient and caregiver). These may be gauge, ½ to ¾ inch intravenous catheters, or commercially available SC infusion devices. b. If possible, do not use gauges, short length metal butterfly catheters as they are more prone to causing catheter-stick injuries to both patients and caregivers. 1.2 Indications for hypodermoclysis: a. oral or transdermal route inappropriate, eg. dysphasia, malabsorption, b. poor or depleted peripheral veins; c. aspiration risk. 1.3 Indication of subcutaneous infusions: a. pain management acute or chronic; b. symptom control for intractable nausea and vomiting; c. sedation d. hypercalcemia treatment; e. immune gamma globulin; f. fluid and electrolyte replacement by administering medications and/or fluids subcutaneously. 1.4 Relative Contraindications: a. generalized edema, poor peripheral circulation, minimal SC tissue b. when rapid control of severe pain or frequent fluid boluses are needed; c. patients with bleeding or coagulation disorders; d. when infusions of more than 3000mL/24 hours are required; e. emergency situations such as severe electrolyte imbalances or circulatory failure; f. emaciated or hypoalbuminemic patients who are edematous.
5 VII-B-315 Page 5 of Advantages and disadvantages: Advantages Simple insertion technique Low maintenance Low cost Less painful than peripheral IV Less likely to cause fluid overload Suitable for home-care and long term care environments Less likely to experience systemic complications (e.g. septicaemia, respiratory depression) Disadvantages Limit volume for rapid fluid resuscitation Small volume limitations Limitations on fluid & medication types Local reactions may occur Volume control pumps for medications or manual flow control devices for continuous infusions are required Not appropriate for emergencies Potential for site abscess or cellulitis formation May not be effective in emaciated of hypoalbuminemic patients who are edematous 1.6 Prescriber will order the type of solution, any medications to be added, and rate of flow. Always check the current order with the solution and concentration presently infusing (rate/dosages may change), expiration date and time. 1.7 Flow rate is dependent on the individual s fluid requirements, absorptive ability of the tissues and/or the desired medication dosages. If the solution bag has medication in it, notify pharmacist of any increase or reduction in rate so that they can prepare the next bag at the appropriate time. Also, notify them if the solution is discontinued. 1.8 More than one infusion site may be used to accommodate high infusion rates Subcutaneous insertion sites used for medication administration should be rotated every 2-7 days and as clinically indicated Subcutaneous insertion sites used for hydration fluids should be rotated every hours or after litres of fluid and as clinically indicated. 1.9 Infusion sites include; a. anterior chest, upper abdomen, anterior or lateral aspects of the thigh, on the back above the scapula, and outer-upper arm; b. ambulatory patients the upper chest area (subclavicular) is recommended because it allows full range of motion; c. patients with little subcutaneous tissue use the upper abdomen away from the waistline. Avoid areas of constriction and areas over large underlying muscles or nerves. Low abdominal sites may cause scrotal edema. Insulin is absorbed most consistently in this site so is preferred for continuous insulin infusion;
6 VII-B-315 Page 6 of 16 d. sites in the thighs may cause scrotal edema; e. confused patients upper back can be useful to prevent accidental removal; f. skin should be intact, site located away from bony prominences and umbilical area to ensure adequate adipose tissue Avoid: a. the waistline; b. areas of constriction from clothing; c. areas of large underlying muscles or nerves; d. bony prominences; e. irritated or infected sites; f. tumors Medications and fluid should be isotonic, non-irritating, non- viscous and water soluble. The parenteral manual should be consulted for administration of medications into the subcutaneous space. 2.0 INITIATING A SUBCUTANEOUS INFUSION SITE / NECESSARY EQUIPMENT Hypodermoclysis solution as ordered, check the expiry date Small gauge catheters (27/25/24/22 gauge), or a subcutaneous safety catheter system (eg BD Saf-T-Intima), are the devices of choice. IV tubing set/infusion set IV pole or infusion pump Sterile securement device - see picture at end of document Injection cap Gloves Transparent dressing
7 VII-B-315 Page 7 of 16 2% chlorhexidine/alcohol swab In case of allergy to chlorhexidine use povidone iodine or alcohol swabs Label Microclave Clear injection cap 3.0 PROCEDURE Use standard precautions and strict aseptic technique 3.1 Explain procedure, purpose of infusion to patient and/or significant other. 3.2 Perform hand hygiene. Assemble and set-up equipment. Spike the HDC solution bag and flush administration set. The drip chamber should be ½ to 2/3 full of solution. 3.3 Verify identity using two patient identifiers. Refer to Covenant Health corporate policy #VII-B-25, Identification of Patient, Resident or Client Using Two Identifiers. 3.4 Priming the subcutaneous extension set before initiation of the site is dependent on the catheter that is used. The catheter is not being inserted into a vascular space; therefore priming is NOT necessary. If using the BD Saf-T-Intima catheter without a Y-port, priming is not possible. If administering only one medication into the Y-site, the tubing may be primed with medication after insertion. See section 6 for priming directions when administering medications 3.5 Choose site. Identify appropriate site based on patient condition, adequate subcutaneous tissue and intact skin. Avoid areas that are scarred, infected, irritated, edematous, bony, highly vascular, near the waistline or breast tissue, affected side of a masectomy with node removal, and avoid arm with PICC insitu. Note: Do not use upper arm for continuous subcutaneous infusion if an alternate site can be used. 3.6 If site is visibly soiled, wash area with soap and water. Cleanse site with 2% chlorhexidine with 70% alcohol swabs by using a back and forth motion with friction for at least 30 seconds. Allow to dry. In case of allergy to alcohol or chlorhexidine, use povidone iodine or alcohol swabs. 3.7 Perform hand hygiene with alcohol-based hand cleanser. Wear protective gloves. 3.8 Choose smallest catheter possible. Insert catheter. Using the thumb and index finger, gently pinch the resident/patient s skin around the injection site, 1.25 to 2.5 cm.
8 VII-B-315 Page 8 of 16 Ask the resident/patient to take a deep breath and insert catheter at a angle into the tissue depending on the amount of subcutaneous fatty tissue. A lower angle is required for patients with minimal subcutaneous tissue. Proper catheter placement is facilitated if the catheter is inserted into the base of the pinch. Check for blood return. There should be no blood return although air bubbles may be seen. NOTE: If blood return is noted, withdraw the catheter. Repeat the procedure using a new catheter and an adjacent site. Make sure the cannula end is sitting well within the subcutaneous layer which is just under the skin 2mm thick1 If no blood is seen attach administration tubing to injection cap. Set rate and administer hydration or medication. Medications may be administered into the y-port. The lower injection port may be used if compatible with the hydration solution. Direction of catheter: In abdomen, direct laterally to prevent pinching or grabbing when person sits or bends. In chest, the catheter may be placed in any direction. Care must be taken to avoid breast tissue as the solution may pool. Also do not insert catheter in the axilla region which may result in decreased absorption and discomfort. Placement of the catheter too low in the abdomen or too high on the thigh may cause scrotal edema.
9 VII-B-315 Page 9 of 16 The catheter should lie in the subcutaneous space, above the underlying fascia. It should move freely in that space (Figure 1). Aspirate to ensure that you are not in the bloodstream. Insertion of the catheter too deep into the tissue will result in the catheter being IM. Problems occur if catheter is too superficial. 3.9 If the solution infuses easily then secure the wings or hub with a sterile securement device to stabilize it. The wings of the catheter should be flush with the skin Apply transparent dressing over catheter wings and insertion site. Replace injection cap on catheter. Coil tubing and secure with sterile securement device and a flat film dressing, i.e. Tegaderm, as appropriate. With pen indicate gauge and today s date as well as the purpose of the site, i.e. whether for hydration or multiple medication administration, or single medication name and concentration. Affix a label to the extension of the subcutaneous catheter/catheter, stating subcutaneous or subcut.
10 VII-B-315 Page 10 of Guidelines for Infusion Rates: a) Rate for fluid replacement/hydration depends upon how quickly the replacement must be achieved, but range from ml/h. Rates up to 300 ml/h can be safely given, but may only be tolerated for 1 or 2 hours. Maximum volume is 3000 ml/24 hours. Observe site frequently for poor absorption. Use an infusion pump or fluid control device. Maximum infusion volume is 1500 ml / 24 hours or 3000 ml / 24 hours with two sites. b) Maximum infusion rate 1000 ml/8 hours during nocturnal infusion. c) Maximum rate no faster than 1000 ml/two hours. d) Rate for Medication infusion is 3-5 ml/hr or much higher, with a maximum rate dependant on absorption. Faster medicated infusion rates may result in tissue irritation and sloughing. If possible the drug dose should be concentrated to ensure a flow rate of 3-5 ml/hr or less, taking bolus dosing into consideration. If required, the rate may be faster, but the site must be monitored frequently for poor absorption. An infusion pump is required for infusions of medications. 4.0 SOLUTIONS WHICH MAY BE USED IN HYPODERMOCLYSIS 0.9% sodium chloride (normal saline) Dextrose 5% and 0.9% sodium chloride (normal saline) Dextrose 3.33% and 0.3% sodium chloride (2/3-1/3) Lactated ringers
11 VII-B-315 Page 11 of 16 Consult parenteral monograph for solutions with electrolyte added. NURSING ALERT: Monitor resident s electrolytes with blood work, per the prescriber s orders. 4.1 Check the Parenteral Blood flow and drug solubility is the major determinants of how fast absorption occurs. 5.0 PROCEDURE INSERTION OF INDWELLING SUBCUTANEOUS CATHETER FOR MEDICATION INJECTION 5.1 Perform catheter insertion procedure as for hypodermoclysis. 5.2 Choose the site and direction of catheter/catheter. 5.3 In upper arm - use for medication administration only. 5.4 Medication Injection: The following are guidelines for medication administration into indwelling subcutaneous sites: If the site will be used for a single medication, prepare the medication according to the prescriber orders; drawing additional medication to prime the tubing set and injection cap for initial dose only (add the priming volume of the tubing and the priming volume of the injection cap for the initial administration: this additional amount of medication will fill the dead space of extension and the cap with fluid). See Appendix A for priming volume of BD Saf-T-Intima. If there is only one medication going into the site, flushing the tubing after medication administration is NOT necessary. The site is identified with the medication name and concentration on the dressing or extension. If one site for each medication/concentration: Label the site with the name of the medication, concentration, and date. Concentration is especially important for narcotics as around the clock medication concentrations/doses may be very different than breakthrough doses/concentrations; i.e. Dilaudid 2 mg/ml vs 10 mg/ml. After administering the medication, do not flush with NS. See Appendix A for BD Saf-T- Intima priming volumes. CAUTION: If site is labelled with a single medication name and concentration DO NOT USE THIS SITE FOR MULTIPLE MEDICATIONS OR CONCENTRATIONS.
12 VII-B-315 Page 12 of 16 If the one site is used for multiple medications/concentration flush with a compatible solution after each medication. The volume of the flush should be equal to the volume of the tubing. a) If one site for multiple medications/concentration: All medications must be compatible. Do not fill extension tubing with medication. Tubing may be left empty or prefilled with NS. Flush (the volume of the tubing dead space) with normal saline or compatible solution between medications and after medication administration. Label site multiple medications. Note: Haldol requires its own designated site as it is not compatible with sodium chloride 9% c) Inject medication VERY slowly - dependent upon patient discomfort. d) Monitor sites pre and post medication administration. e) Remove at the first sign of irritation, non-absorption, infection, leaking pain and dislodgement 5.5 Specific patients, due to individual circumstances, may require changes to these guidelines. 6.0 CARE GUIDELINES 6.1 Observe site every eight hours for local irritation, patient comfort, leaking and infusion rate, and every time anything is administered or the solution changed and as needed for signs of local or systemic complications. Monitor the site every shift if the site is not being used at regular intervals Edema at Site Monitor if it occurs in a small amount consider slowing the infusion rate and monitor for absorption if edema persists for greater than eight hours or increases, discontinue and restart in another site Use two or more sites for infusions up to 3000 ml/24 hours. Monitor patients with poor circulation for medication pockets Redness/erythema Irritation, edema, induration, bruising at site possible allergic reaction to medications or catheter possible causes are prolonged duration of catheter placement, rapid infusion or irritation from solution monitor, if redness does not resolve remove catheter
13 VII-B-315 Page 13 of 16 NURSING ALERT: Slight local redness at insertion site may be present for several minutes (up to one hour) immediately following the establishment of a new site or manipulation of the catheter. If the redness extends beyond the insertion site or persists, remove catheter Pain or discomfort at infusion site Possible causes are catheter migration, prolonged duration of catheter, inadvertent placement into muscle tissue or rapid infusion. Warm compresses after catheter removal may be used for comfort Infection at Site discontinue infusion remove catheter and culture catheter and site restart in new site change administration set that is connected to solution notify physician/np monitor the site every shift until healed Dislodgement of Catheter apply gauze dressing over site restart with new catheter in another site Leakage or pooling of fluid at insertion site Possible cause is poor absorption or too rapid infusion Stop infusion and remove catheter, restart in another site. 6.2 Assess person for systemic complications Fluid Overload observe for increased pulse and blood pressure, systemic edema (specially of pelvis, feet and genitalia), respiratory congestion, USE CAUTION with residents with end stage renal disease. slow infusion rate and notify physician if there is an increase in the resident/patient s pulse or blood pressure and or signs of respiratory congestion, stop the infusion and immediately contact the physician/np monitor person's condition closely
14 VII-B-315 Page 14 of REMOVAL Make patient comfortable in chair or bed. Discontinue all infusions. Perform hand hygiene and don clean gloves. Remove dressing. Stabilize the skin and pull catheter out at the same angle that it was inserted. Apply pressure to exit site if there is bleeding. Cover with bandage or sterile gauze. 8.0 DOCUMENT IN THE PATIENT CARE RECORD / IV THERAPY FLOW SHEET 8.1 Initiation of therapy including type of device inserted the site and rate date and time of the initiation of therapy date and time of new solution bags being hung 8.2 Integrity of site every (shift). 8.3 Any adverse reactions follow facility incident reporting processes. 8.4 Time, dosage and route of all medications (on the MAR). 8.5 Care and maintenance procedures performed - eg. dressing changes, injection cap changes. 8.6 Removal. 8.7 Patient response.
15 VII-B-315 Page 15 of 16 APPENDIX A BD Saf-T-Intima Without Y adapter Priming capacity 0.25 ml With Y adaptor Priming capacity 0.5 ml BD Saf-T-Intima Product codes Description BD Product code 24gx0.75 straight g x 0.75 with Y adapter g x 0.75 straight g x 0.75 with Y adapter
16 VII-B-315 Page 16 of 16
A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS
 SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS
 PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis)
 Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Dehydration and Fluid Therapy Guide
 Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
POSSIBLE NURSING DIAGNOSIS: Pain Potential for Infection / Infection Fluid volume deficit
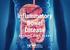 1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol
 Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol Who Division 1 Registered Nursing staff for the purposes of administering and monitoring of infusion Division 2
Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol Who Division 1 Registered Nursing staff for the purposes of administering and monitoring of infusion Division 2
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
BD Saf-T-Intima. Hidden talents of BD Saf-T-Intima. BD SAF-T-Intima and SUBCUTANEOUS THERAPY REHYDRATION PALLIATIVE CARE. POST OPERATIVe PAIN RELIEF
 Hidden talents of BD Saf-T-Intima BD Saf-T-Intima SUBCUTANEOUS INFUSION REHYDRATION PALLIATIVE CARE BD SAF-T-Intima and SUBCUTANEOUS THERAPY PAEDIATRIC CARE POST OPERATIVe PAIN RELIEF BD Saf-T-Intima First
Hidden talents of BD Saf-T-Intima BD Saf-T-Intima SUBCUTANEOUS INFUSION REHYDRATION PALLIATIVE CARE BD SAF-T-Intima and SUBCUTANEOUS THERAPY PAEDIATRIC CARE POST OPERATIVe PAIN RELIEF BD Saf-T-Intima First
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
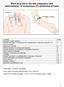 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
An introduction to the principles and practice of safe and effective administration of injections
 An introduction to the principles and practice of safe and effective administration of injections Introduction Giving an injection safely is considered to be a routine nursing activity. However it requires
An introduction to the principles and practice of safe and effective administration of injections Introduction Giving an injection safely is considered to be a routine nursing activity. However it requires
DISTRIBUTION: All Clinical Units JHCH, J1, J2, H1, Oncology Day Stay Unit & J2 Day Stay Unit. JHH Intensive Care Unit and Emergency Department
 13.12 PROCEDURE SUBJECT: (This guideline is relevant to inpatient use only) DOCUMENT NUMBER: 13.12 DATE DEVELOPED: May 2013 LAST REVISED DATE: NEW PLANNED REVIEW DATE: November 2017 DISTRIBUTION: All Clinical
13.12 PROCEDURE SUBJECT: (This guideline is relevant to inpatient use only) DOCUMENT NUMBER: 13.12 DATE DEVELOPED: May 2013 LAST REVISED DATE: NEW PLANNED REVIEW DATE: November 2017 DISTRIBUTION: All Clinical
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC)
 Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Date effective: Jan 2005 Date revised: June 2015
 Section H: Administration of Blood Products Page 1 of 8 I. Introduction... 1 II. Intravenous (IV) Access... 2 Peripheral Line:...2 Central Venous Catheter:...2 III. Compatible Solutions with Blood Products...
Section H: Administration of Blood Products Page 1 of 8 I. Introduction... 1 II. Intravenous (IV) Access... 2 Peripheral Line:...2 Central Venous Catheter:...2 III. Compatible Solutions with Blood Products...
Appendix L: Accessing/Deaccessing Implanted Central Venous Access Port
 Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
Administration of Medications & Fluids via a Peripheral Intravenous Cannula
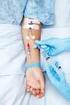 Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Achieving Independence
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter. Peripherally-Inserted Central Catheter (PICC)
 Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Cytotoxic and Biotherapies Credentialing Programme Module 6
 Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
PATIENT INFORMATION. Medicine To Treat: D iabetes. What You Need to Know About. Insulin
 PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
Policies & Procedures. I.D. Number: 1073
 Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
How To Prepare and Give a Prefilled Syringe Injection
 Diablo Valley Onc&Hem Med Grp, Inc Phone Number: (925)6775041 How To Prepare and Give a Prefilled Syringe Injection Patient Education Quick Reference Guide The following are instructions for use of prefilled
Diablo Valley Onc&Hem Med Grp, Inc Phone Number: (925)6775041 How To Prepare and Give a Prefilled Syringe Injection Patient Education Quick Reference Guide The following are instructions for use of prefilled
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Intravenous Therapy. Marjorie Wiltshire, RN
 Intravenous Therapy Marjorie Wiltshire, RN :OBJECTIVES Define key terms related to intravenous therapy. Demonstrate the procedure for IV insertion, conversion to a saline lock, administration of IV fluids,
Intravenous Therapy Marjorie Wiltshire, RN :OBJECTIVES Define key terms related to intravenous therapy. Demonstrate the procedure for IV insertion, conversion to a saline lock, administration of IV fluids,
REMOVAL OF A PICC. Possible Cause Nursing Actions Prevention
 REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Tell your doctor about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements.
 SOMAVERT pegvisomant for injection PATIENT INFORMATION SOMAVERT (SOM-ah-vert) (pegvisomant for injection) Read the patient information that comes with SOMAVERT before you start using it and each time you
SOMAVERT pegvisomant for injection PATIENT INFORMATION SOMAVERT (SOM-ah-vert) (pegvisomant for injection) Read the patient information that comes with SOMAVERT before you start using it and each time you
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and
 Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
Procedure for Inotrope Administration in the home
 Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Beaumont Hospital Department of Nephrology and Renal Nursing. Guideline for administering Ferinject
 Beaumont Hospital Department of Nephrology and Renal Nursing Guideline Name: Guideline for administering Ferinject Guideline Number: 18 Guideline Version: a Developed By: Louise Kelly CNM 1 Renal Day Care
Beaumont Hospital Department of Nephrology and Renal Nursing Guideline Name: Guideline for administering Ferinject Guideline Number: 18 Guideline Version: a Developed By: Louise Kelly CNM 1 Renal Day Care
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm
 Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm Why might my Doctor ask me to inject Methotrexate? Methotrexate comes in two forms:
Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm Why might my Doctor ask me to inject Methotrexate? Methotrexate comes in two forms:
Instructions for Use PROCRIT (PRO KRIT) (epoetin alfa)
 Instructions for Use PROCRIT (PROKRIT) (epoetin alfa) Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless
Instructions for Use PROCRIT (PROKRIT) (epoetin alfa) Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES
 02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
NURSING PRACTICE & SKILL
 NURSING PRACTICE & SKILL ICD-9 99.29 Author Carita Caple, RN, BSN, MSHS Reviewers Eliza Schub, RN, BSN Sara Richards, MSN, RN Nursing Practice Council Glendale Adventist Medical Center, Glendale, CA Editor
NURSING PRACTICE & SKILL ICD-9 99.29 Author Carita Caple, RN, BSN, MSHS Reviewers Eliza Schub, RN, BSN Sara Richards, MSN, RN Nursing Practice Council Glendale Adventist Medical Center, Glendale, CA Editor
V: Infusion Therapy. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 181
 V: Infusion Therapy College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 181 Competency: V-1 Principles of V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability
V: Infusion Therapy College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 181 Competency: V-1 Principles of V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Peripherally Inserted Central Catheter (PICC)
 Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
9.Pediatric Procedures
 9.Pediatric Procedures A. Introduction 1. Pediatric blood collection may be by skin puncture or venipuncture. 2. Skill in pediatric phlebotomy is gained by knowledge of special collection equipment, observation
9.Pediatric Procedures A. Introduction 1. Pediatric blood collection may be by skin puncture or venipuncture. 2. Skill in pediatric phlebotomy is gained by knowledge of special collection equipment, observation
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS
 SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
STANDARDIZED PROCEDURE BONE MARROW ASPIRATION
 I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
INSULIN INJECTION KNOW-HOW
 0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
INJECTION TECHNIQUE. IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole
 IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
Central Venous Catheter (CVC) Sterile Dressing Change - The James
 PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
Intraperitoneal Chemotherapy
 Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
Care of your peripherally inserted central catheter
 Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Gentle and safe injections. Tips and tricks for injecting insulin.
 Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
PHARMACOTHERAPY HOW TO INJECT INSULIN. Living your life as normal as possible. www.lilly-pharma.de www.lilly-diabetes.de
 PHARMACOTHERAPY HOW TO INJECT INSULIN Living your life as normal as possible www.lilly-pharma.de www.lilly-diabetes.de In Germany about 1.9 million people with diabetes are being treated with insulin.
PHARMACOTHERAPY HOW TO INJECT INSULIN Living your life as normal as possible www.lilly-pharma.de www.lilly-diabetes.de In Germany about 1.9 million people with diabetes are being treated with insulin.
BEAUMONT HOSPITAL DEPARTMENT OF NEPHROLOGY RENAL BIOPSY
 1 BEAUMONT HOSPITAL DEPARTMENT OF NEPHROLOGY GUIDELINES ON ADMINISTRATION OF INTRAVENOUS IRON SUCROSE (VENOFER) AS A BOLUS DOSE IN THE RENAL OUTPATIENT SETTING Date Developed: August- October 2007 RENAL
1 BEAUMONT HOSPITAL DEPARTMENT OF NEPHROLOGY GUIDELINES ON ADMINISTRATION OF INTRAVENOUS IRON SUCROSE (VENOFER) AS A BOLUS DOSE IN THE RENAL OUTPATIENT SETTING Date Developed: August- October 2007 RENAL
Central venous catheters. Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95
 4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
INSTRUCTIONS FOR USE HUMIRA 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE
 INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE Do not try to inject HUMIRA yourself until you have been shown the right way
INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE Do not try to inject HUMIRA yourself until you have been shown the right way
Peripherally Inserted Central Catheter
 Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
Chapter 11. Everting skin edges
 Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
HED\ED:NS-BL 037-3rd
 HED\ED:NS-BL 037-3rd Insulin Insulin is produced by the beta cells in the islets of Langerhans in the pancreas. When glucose enters our blood, the pancreas should automatically excrete the right amount
HED\ED:NS-BL 037-3rd Insulin Insulin is produced by the beta cells in the islets of Langerhans in the pancreas. When glucose enters our blood, the pancreas should automatically excrete the right amount
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC
 Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Peripherally Inserted Central Catheter (PICC) Benefits Long-term access - dwell time varies (can be > one year) Decreased length of stay in hospital a
 Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
APPLICATION OF DRY DRESSING
 G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
Percutaneous Abscess Drainage
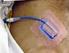 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
PROCEDURE FOR THE ADMINISTRATION OF MEDICATION BY INJECTION VIA THE INTRAMUSCULAR ROUTE OR VIA THE SUBCUTANEOUS ROUTE
 PROCEDURE FOR THE ADMINISTRATION OF MEDICATION BY INJECTION VIA THE INTRAMUSCULAR OR VIA THE SUBCUTANEOUS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date October 2012
PROCEDURE FOR THE ADMINISTRATION OF MEDICATION BY INJECTION VIA THE INTRAMUSCULAR OR VIA THE SUBCUTANEOUS First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date October 2012
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
Management of Catheters Infectious Diseases Working Party/Nurses Group
 Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Medication Guide Rebif (Re-bif) Interferon beta-1a (in-ter-feer-on beta-one-â)
 Medication Guide Rebif (Re-bif) Interferon beta-1a (in-ter-feer-on beta-one-â) Please read this leaflet carefully before you start to use Rebif and each time your prescription is refilled since there may
Medication Guide Rebif (Re-bif) Interferon beta-1a (in-ter-feer-on beta-one-â) Please read this leaflet carefully before you start to use Rebif and each time your prescription is refilled since there may
Intravenous Therapy Principles of Care. Breege Smithers Practice Educator
 Intravenous Therapy Principles of Care Breege Smithers Practice Educator Objectives State indications for intravenous therapy List the advantages and disadvantages of intravenous therapy Identify the principles
Intravenous Therapy Principles of Care Breege Smithers Practice Educator Objectives State indications for intravenous therapy List the advantages and disadvantages of intravenous therapy Identify the principles
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line)
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients with a Peripherally Inserted
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients with a Peripherally Inserted
FRAGMIN Please bring this booklet the day of your surgery.
 FRAGMIN Please bring this booklet the day of your surgery. QHC#72 Fragmin (dalteparin sodium injection); an anticoagulant (blood thinner) is used to help prevent blood clots after surgery. While on Fragmin,
FRAGMIN Please bring this booklet the day of your surgery. QHC#72 Fragmin (dalteparin sodium injection); an anticoagulant (blood thinner) is used to help prevent blood clots after surgery. While on Fragmin,
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
IVF CLASS. IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, nicole.l.sobers.ctr@health.
 IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, [email protected] PLEASE NOTE: If you do not have medications for the next
IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, [email protected] PLEASE NOTE: If you do not have medications for the next
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Why is Insulin so Important?
 Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
