Chpter 2 Nonoperative Management of Non-displaced Acute Scaphoid Fracture
|
|
|
- Lorena Richardson
- 7 years ago
- Views:
Transcription
1 Chpter 2 Nonoperative Management of Non-displaced Acute Scaphoid Fracture Megan Tomaino and Thomas B. Hughes Case Presentation The patient is a 15-year-old male with a history of left wrist pain following a football-related injury. He described the initial injury as hyperextension of his left wrist during football practice. He was seen at an urgent care center and initially diagnosed with a left wrist sprain. At that time, he was given a cock-up wrist splint. The patient continued to play football and re-aggravated his wrist 1 month later. He presented to a primary care sports medicine physician with left wrist pain. He reported that the pain had never resolved from a month earlier. New X-rays were obtained at that visit, an MRI was ordered, and the patient was removed from sports. The MRI was obtained about 1 week later and the patient was placed in a long arm cast and was referred to a hand surgeon for definitive care. He had no prior medical or surgical history, and he had no previous history of trauma to the left wrist. He denied tobacco use. T. B. Hughes ( ) M. Tomaino Department of Orthopaedic Surgery, University of Pittsburgh School of Medicine, Pittsburgh, PA, USA thughes424@aol.com Springer International Publishing Switzerland 2015 J. Yao (ed.), Scaphoid Fractures and Nonunions, DOI / _2 9
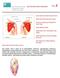
2 10 M. Tomaino and T. B. Hughes Fig. 2.1 An oblique radiograph a and lateral radiograph b obtained a day after the patient s injury. No true AP view was obtained. It is difficult to definitively identify a fracture line on these radiographs. (Published with kind permission of Megan Tomaino and Thomas B. Hughes, All rights reserved) Physical Assessment In the urgent care center on the day of the injury, the patient had point tenderness to the lateral side of the thumb, decreased grip strength, and mild wrist swelling at the radiocarpal joint. One month after the injury, the left wrist was mildly edematous with decreased wrist extension, focal tenderness in the anatomical snuffbox, and diminished grip strength of the left hand. Diagnostic Studies Radiographs of the left wrist on the day after the injury were interpreted as normal. These radiographs were subsequently reviewed by the upper extremity specialist and the scaphoid fracture could not be appreciated (Fig. 2.1). Repeat radiographs were obtained a month after the initial injury which are shown in Fig These demonstrated a minimally displaced scaphoid fracture. An MRI of the left wrist obtained 1 week later (5 weeks after the initial injury) revealed a non-displaced scaphoid waist fracture and intense
3 2 Nonoperative Management of Non-displaced 11 Fig. 2.2 An AP radiograph obtained 1 month after the injury clearly demonstrates an abnormality at the waist of the scaphoid (arrow). This, combined with persistent radial wrist pain, is enough to make the diagnosis. (Published with kind permission of Megan Tomaino and Thomas B. Hughes, All rights reserved) Fig. 2.3 Select coronal MRI demonstrating the fracture of the waist of the scaphoid. (Published with kind permission of Megan Tomaino and Thomas B. Hughes, All rights reserved) edema of both the scaphoid and lunate. No fracture was identified in the lunate (Fig. 2.3). Management Chosen The patient was initially diagnosed with a left wrist strain and treated with a splint for 4 weeks. Initial recommendations for splinting and activities for the patient were nonspecific. It is clear
4 12 M. Tomaino and T. B. Hughes that either the patient was noncompliant or the urgent care clinic was not explicit enough in their recommendations that the patient be immobilized, avoid wrist activities, and seek follow-up care. When the non-displaced scaphoid fracture was suspected at 4 weeks, the patient was removed from sports, placed in a splint, and sent for an MRI. It was appropriate for the patient to be immobilized at this point (although some may recommend inclusion of the thumb in the splint, which was not done) and removed from football. It is unclear what specific advantage the MRI provided in diagnosis, treatment, or stratification of risks for this patient. After the non-displaced scaphoid waist fracture was discovered on MRI, he was immobilized in a cast for 7 weeks. Clinical Course and Outcome The cast was removed when there was radiographic evidence of scaphoid healing (11 weeks post-injury), and the patient had some wrist stiffness but no snuffbox tenderness. He was given a removable thumb spica splint and range of motion exercises for the wrist, but no formal physical therapy and he was not allowed to return to sport. The patient was encouraged to increase his activity as tolerated, but he continued to be restricted from participating in heavy lifting, football, or any sports. Fifteen weeks after the injury, X-rays demonstrated good healing of the fracture and the splint was recommended for comfort only. He was released to return to activities as tolerated, including football. At 15 weeks post-injury, X-rays revealed progressive healing of the mid-body fracture with good consolidation (Fig. 2.4). He had full range of motion of the left wrist, no pain, and he was able to return to normal activities. Clinical Pearls/Pitfalls The key to identifying scaphoid fractures is to suspect them. The practitioner must be aggressive in the diagnosis of scaphoid fractures.
5 2 Nonoperative Management of Non-displaced 13 Fig. 2.4 AP radiographs obtained at 7 a, 11 b, and 15 c weeks after the injury demonstrate progressive healing of the fracture. (Published with kind permission of Megan Tomaino and Thomas B. Hughes, All rights reserved) Education of nonspecialists must continue as there is still a significant percentage of missed occult scaphoid fractures that have been seen by a practitioner that do not receive appropriate treatment or counseling. As more practice extenders are utilized in our health delivery system, this issue will continue to be significant. Patients with radial wrist pain need to be given specific instructions and limitations, including immobilization, in order to prevent scaphoid nonunions. Repeat imaging and close follow-up are critical for the successful treatment of the occult scaphoid fracture. When noncompliance is anticipated, advanced imaging may help establishing a diagnosis and lead to appropriate treatment. Complete bony union for scaphoid fractures takes several months. Even with occult fractures not visible on initial radiographs, healing can take three months or more. The results of nonoperative treatment are excellent with very few risks of complications. This approach to treatment should be considered for all non-displaced fractures and the risks of surgical intervention carefully weighed.
6 14 M. Tomaino and T. B. Hughes Literature Review and Discussion The 15-year-old patient with a football injury in this case study represents a classic presentation of a scaphoid fracture. These fractures are most commonly seen in young adult males (age years) after sports-related injuries or a fall on an outstretched hand. In recent decades, an increasing percentage of scaphoid fractures are occurring in young women, possibly because of increased participation in athletics [1, 2]. A typical description of the injury is a traumatic hyperextension of the wrist with radial deviation, such as described by the current patient during football practice. Patients often complain of generalized wrist or thumb pain and may not have pain over the scaphoid. Common physical exam findings include point tenderness over the anatomic snuffbox or thumb, decreased wrist range of motion, and weakened grip [1]. The current patient suffered from severe point tenderness over the thumb and weak grip of the left hand though radiographs interpreted as normal. The sensitivity of radiographs for scaphoid fractures can be as low as 70 % and highly subject to the experience of the reader, resulting in easily missed fractures on initial testing [3]. Missed or untreated scaphoid fractures are at increased risk of nonunion, carpal collapse, and degenerative arthritis. Therefore, physicians should have a high degree of clinical suspicion for these injuries. In patients with vague symptoms about the radial wrist and thumb, the diagnosis must be excluded definitively prior to discharging the patient. Patients who are at risk for a scaphoid fracture should be placed in full-time immobilization, including the thumb, until the diagnosis is confirmed or eliminated. Further testing with serial radiographs, a computed tomography (CT) or magnetic resonance imaging (MRI) scan is recommended. Serial radiographs may be effective. However, since several weeks of immobilization and activity modification are required between X-rays, there is a significant opportunity cost to this method of treatment. In order to return patients to sport and work faster, early advanced imaging can be helpful. While CT scans are faster, widely available, and expensive, they are less reliable for identifying non-displaced scaphoid fractures.
7 2 Nonoperative Management of Non-displaced 15 CT scans do provide a better resolution of the anatomy of the fracture, in particular if the fracture is displaced and requires reduction. While some studies have shown CT scans to have poor sensitivity to displacement, it remains the best test available to assess displacement. In cases where initial radiographs are normal, it is very unlikely that displacement has occurred, and CT scans are probably unnecessary. However, in cases where there is an obvious fracture at initial presentation, CT scanning should be considered to assess displacement. MRI is the most sensitive test to identify non-displaced fractures, and could have been helpful in this case had it been ordered after his initial evaluation at the urgent care clinic [1]. As it was not ordered until after the fracture was identified on the plain films, it did not aid in the diagnosis in this case. MRI can be useful to identify avascular necrosis, although this waist fracture was at limited risk for this problem [4]. Once the diagnosis of an acute non-displaced scaphoid fracture is confirmed, there are two main approaches to treatment: (1) nonsurgical immobilization and (2) surgical fixation. Both types of management ultimately aim to heal the fracture and avoid delayed union, nonunion, and avascular necrosis. Scaphoid fractures are at higher risk for these issues due to easily disrupted blood supply to the proximal pole. Branches from the radial artery supply the waist and distal tubercle; however, the proximal pole of the scaphoid relies exclusively on intraosseous blood flow, which can become disrupted with a fracture [1]. General considerations when evaluating the role of surgical and nonsurgical management include time to union, risk of nonunion, time to return to work or activities, functionality of the wrist, complications, overall cost, and patient satisfaction. Some studies have shown faster time to union, return to work, and return of range of motion with surgical fixation over casting, but others have found no evidence to support faster fracture union with surgical fixation [5 8]. In one randomized study, no statistically significant difference in time to union or rate of union was found in 53 patients with acute, non-displaced scaphoid waist fractures treated with either percutaneous screw fixation or immobilization for 10 weeks [8]. While patients managed nonoperatively cannot mobilize the wrist
8 16 M. Tomaino and T. B. Hughes as quickly as surgical patients, the benefits of earlier mobilization after surgery may be transient. Follow-up from 12 months to 10 years after fracture has shown no statistically significant difference in fracture union, ROM, or patient satisfaction [7, 9 11]. Surgical treatment may be considered over immobilization in cases where the patient needs to return to work without a cast sooner. While it may seem that laborers are likely to gain the most from operative treatment, it may be those that do lighter tasks that can actually return to work sooner. Occupation is a significant factor in the consideration of surgery versus conservative treatment as self-employed and patients in nonmanual labor positions generally return to work faster than those in manual jobs, regardless of treatment [7, 12]. Surgical fixation may favored when the patient is employed in a job that is precluded by cast treatment because they are able to return to work sooner without a cast [8, 11, 13]. It should be noted that attitudes of the patient, employer, insurance company, and socioeconomic status of the patient are also significant factors in time to return to work [9, 12]. An additional consideration in developing treatment plans are complications. The literature has demonstrated a higher rate of complication with surgical treatment over conservative treatment [9, 14]. Short-term complications of surgery include prominent hardware, technical difficulties, infection, complex regional pain syndrome, and scar-related problems, whereas long-term complications include scaphotrapezial and scaphotrapeziotrapezoid joint osteoarthritis. The higher rate of arthritis with surgical treatment is thought to be from disruption of the scaphoid cartilage with screw fixation, although scaphotrapezial osteoarthritis is found in a small percentage of patients managed nonoperatively as well [10, 13, 15]. Additional complications noted in a small population of nonsurgical patients included intercalated segment instability discovered at 7-year follow-up. It has been suggested the instability in these cases may also be associated with a ligamentous injury at the time of fracture [11]. While there has been recent literature to support operative treatment of non-displaced fractures, there are certainly significant risks to surgical treatment that cannot be ignored. Based on these risks, some authors, such as Dias et al., developed an aggressive
9 2 Nonoperative Management of Non-displaced 17 conservative treatment approach [9, 11]. Other authors have adopted a variation of this treatment approach which generally includes aggressive early diagnosis of the fracture and immobilizing all patients unless they have immediate cause for surgical fixation [15 17]. Early diagnosis and immobilization is important in preventing nonunion, and therefore, any patient suspected of having a scaphoid injury should be evaluated carefully with radiographs and possibly a CT or MRI. The optimal cast for immobilizing an established scaphoid fracture has been studied; however, no significant differences in union rate have been noted with long arm, short arm, or thumb spica casts [17, 18]. A short arm thumb spica cast is generally accepted [14]; however, some institutions use a short arm cast with 20 wrist dorsiflexion and leaving the thumb free for scaphoid fractures [9, 11, 19]. A recent study has even demonstrated that in patients where the thumb is not included, there is a greater extent of healing compared to those in whom the thumb is immobilized [18]. The following algorithm compromises between both practices. If the scaphoid fracture is diagnosed via radiographs, and is non-displaced, a thumb spica cast should be applied initially. These fractures are less stable than more subtle injuries and fear of further displacement is warranted. At 6 weeks, if there is no displacement, or early signs of healing, it can be converted to a short arm cast without the inclusion of the thumb. If the initial radiographs are normal, and the diagnosis is made through serial radiographs or advanced imaging, this fracture is inherently stable and a short arm cast leaving the thumb free for 6 8 weeks can be applied. Regardless of the cast type, all patients should be re-evaluated with radiographs after 6 8 weeks. If radiographs show significant healing, a cast does not need to be reapplied. If radiographs do not clearly demonstrate healing at 6 8 weeks, a CT scan may be needed to assess healing at that point. Once 50 % of the fracture has bridging bone, the patient can be given a removable splint for comfort and return to activities of daily living as tolerated. All patients should be re-evaluated with radiographs again to ensure fracture healing between 12 and 16 weeks postfracture. Patients with clear signs of nonunion, such as fracture motion and vacuolization, are recommended for surgical fixation.
10 18 M. Tomaino and T. B. Hughes In deciding to manage an acute non-displaced scaphoid fracture with an aggressive conservative treatment plan or surgical fixation, having a discussion with the patient regarding the potential risks and benefits of both surgical and nonsurgical treatment is essential. Besides the potential complications of surgery or immobilization, a significant concern for the patient is return to work and activity. These needs for return to activity must be carefully weighed against the higher risk of surgical complications seen with operative management. Both surgical and conservative treatment plans show no significant difference in union, rate of nonunion, or range of motion, and the conservative approach avoids the increased risk of complication associated with surgical fixation. References 1. Kawamura K, Chung KC. Treatment of scaphoid fractures and nonunions. J Hand Surg. 2008;33A: Van Tassel DC, Owens BD, Moriatis J. Incidence estimates and demographics of scaphoid fracture in the U.S. population. J Hand Surg. 2010;35A: Galer C, Kuka C, Breitenseher MJ, Trattnig S, Vecsei V. Diagnosis of occult scaphoid fractures and other wrist injuries. Are repeated clinical examinations and plain radiographs still state of the art? Langenbecks Arch Sug. 2001;120:73e 89e. 4. Lutsky K. Preoperative magnetic resonance imaging for evaluating scaphoid nonunion. J Hand Surg. 2012;37A; MCQueen MM, Gelbke MK, Wakefield A, Will EM, Gaebler C. Percutaneous screw fixation versus conservative treatment for fractures of the waist of the scaphoid. J Bone Jt Surg. 2008;90B: Bond CD, Shin AY, McBride MT, Dao KD. Percutaneous screw fixation or cast immobilization for nondisplaced scaphoid fractures. J Bone Jt Surg. 2001;83A:4: Buijze GA, Doornberg JN, Ham JS, Ring D, Bhandari M, Poolman RW. Surgical compared with conservative treatment acute nondisplaced or minimally displaced scaphoid fractures: a systemic review and meta-analysis of randomized controlled trials. J Bone Jt Surg Am. 2010;92: Adolfson L, Lindau T, Arner M. Acutrak screw fixation versus cast immobilization for undisplaced scaphoid waist fractures. J Hand Surg. 2001;26B:3:192 5.
11
DIAGNOSING SCAPHOID FRACTURES. Anthony Hewitt
 DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
Scaphoid Fracture of the Wrist
 Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
RADIOGRAPHIC EVALUATION
 Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Scaphoid Fractures- Anatomy And Diagnosis: A Systemic Review Of Literature
 Article ID: WMC001268 ISSN 2046-1690 Scaphoid Fractures- Anatomy And Diagnosis: A Systemic Review Of Literature Corresponding Author: Dr. Dharm Meena, junior resident, orthopaedics, PGIMER, E 402, MDH,PGIMER,CHANDIGARH,
Article ID: WMC001268 ISSN 2046-1690 Scaphoid Fractures- Anatomy And Diagnosis: A Systemic Review Of Literature Corresponding Author: Dr. Dharm Meena, junior resident, orthopaedics, PGIMER, E 402, MDH,PGIMER,CHANDIGARH,
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
Wrist Fractures. Wrist Defined: Carpal Bones Distal Radius Distal Ulna
 Wrist Fractures Wrist Fractures Wrist Defined: Carpal Bones Distal Radius Distal Ulna Wrist Fractures Wrist Joints: CMC Intercarpal Radiocarpal DRUJ drudge Wrist Fractures Wrist Fractures: (that we are
Wrist Fractures Wrist Fractures Wrist Defined: Carpal Bones Distal Radius Distal Ulna Wrist Fractures Wrist Joints: CMC Intercarpal Radiocarpal DRUJ drudge Wrist Fractures Wrist Fractures: (that we are
ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329
 ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329 Consultant Orthopaedic Surgeon London Bridge Hospital Medico-Legal Secretary:
ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329 Consultant Orthopaedic Surgeon London Bridge Hospital Medico-Legal Secretary:
NERVE COMPRESSION DISORDERS
 Common Disorders of the Hand and Wrist Ryan Klinefelter, MD Associate Professor of Orthopaedics Department of Orthopaedics The Ohio State University Medical Center NERVE COMPRESSION DISORDERS 1 Carpal
Common Disorders of the Hand and Wrist Ryan Klinefelter, MD Associate Professor of Orthopaedics Department of Orthopaedics The Ohio State University Medical Center NERVE COMPRESSION DISORDERS 1 Carpal
We compared the long-term outcome in 61
 Fracture of the carpal scaphoid A PROSPECTIVE, RANDOMISED 12-YEAR FOLLOW-UP COMPARING OPERATIVE AND CONSERVATIVE TREATMENT B. Saedén, H. Törnkvist, S. Ponzer, M. Höglund From Stockholm Söder Hospital,
Fracture of the carpal scaphoid A PROSPECTIVE, RANDOMISED 12-YEAR FOLLOW-UP COMPARING OPERATIVE AND CONSERVATIVE TREATMENT B. Saedén, H. Törnkvist, S. Ponzer, M. Höglund From Stockholm Söder Hospital,
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Commonly Missed Fractures in the Emergency Department
 Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Fractures around wrist
 Fractures around wrist Colles Fracture Smiths fracture Barton s fracture Chauffer s fracture Scaphoid fracture Lunate dislocation Vivek Pandey Colles fracture Definition: Fracture of the distal end radius
Fractures around wrist Colles Fracture Smiths fracture Barton s fracture Chauffer s fracture Scaphoid fracture Lunate dislocation Vivek Pandey Colles fracture Definition: Fracture of the distal end radius
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Scaphoid Fractures 1
 1 Scaphoid Fractures Scaphoid Fractures Introduction Anatomy Biomechanics History Clinical examination Radiographic evaluation DDx Classification Treatment Complications 2 Scaphoid fractures Introduction
1 Scaphoid Fractures Scaphoid Fractures Introduction Anatomy Biomechanics History Clinical examination Radiographic evaluation DDx Classification Treatment Complications 2 Scaphoid fractures Introduction
Imaging of Lisfranc Injury
 November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
Ankle Fractures - OrthoInfo - AAOS. Copyright 2007 American Academy of Orthopaedic Surgeons. Ankle Fractures
 Copyright 2007 American Academy of Orthopaedic Surgeons Ankle Fractures "I broke my ankle." A broken ankle is also known as an ankle "fracture." This means that one or more of the bones that make up the
Copyright 2007 American Academy of Orthopaedic Surgeons Ankle Fractures "I broke my ankle." A broken ankle is also known as an ankle "fracture." This means that one or more of the bones that make up the
Distal Radius Fractures. Lee W Hash, MD Affinity Orthopedics and Sports Medicine
 Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Musculoskeletal Trauma of the Wrist
 September 2000 Musculoskeletal Trauma of the Wrist Murat Akalin, Harvard Medical School, Year- IV Gillian Lieberman, MD The Wrist Most common site of injury in entire skeleton Distal radius and ulna fractures
September 2000 Musculoskeletal Trauma of the Wrist Murat Akalin, Harvard Medical School, Year- IV Gillian Lieberman, MD The Wrist Most common site of injury in entire skeleton Distal radius and ulna fractures
Scaphoid Non-union. Dr. Mandel Dr. Gyomorey. May 3 rd 2006
 Scaphoid Non-union Dr. Mandel Dr. Gyomorey May 3 rd 2006 Introduction Scaphoid fracture incidence: 8-38/100,000 Non-union 5% (0-22%) Adams and Leonard (1928) first described operative treatment of the
Scaphoid Non-union Dr. Mandel Dr. Gyomorey May 3 rd 2006 Introduction Scaphoid fracture incidence: 8-38/100,000 Non-union 5% (0-22%) Adams and Leonard (1928) first described operative treatment of the
Comparison Of Ct And Plain Film For The Postoperative Assessment Of Scaphoid Fracture Healing
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2011 Comparison Of Ct And Plain Film For The Postoperative
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2011 Comparison Of Ct And Plain Film For The Postoperative
Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma. Magee, 2008. pg.
 PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013
 Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Integra. MCP Joint Replacement PATIENT INFORMATION
 Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Diagnosis of Acromioclavicular Joint Injuries
 PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 Chiroeducation@aol.com www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 Chiroeducation@aol.com www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
Forearm Fractures 09/18/2013. Mechanism: Usually a fall on an outstretched arm. Incidence. Mechansim
 September 20, 2013 Amanda Taylor PA-C Children s Orthopaedics of Louisville Forearm Fractures Incidence 40-50% of all pediatric fractures Mechansim Wide range of mechanism Mechanism: Usually a fall on
September 20, 2013 Amanda Taylor PA-C Children s Orthopaedics of Louisville Forearm Fractures Incidence 40-50% of all pediatric fractures Mechansim Wide range of mechanism Mechanism: Usually a fall on
Scaphoid and Other Wrist Injuries in the Emergency Department
 CLINICAL PRACTICE GUIDELINE Scaphoid and Other Wrist Injuries in the Emergency Department SCOPE (Area): SCOPE (Staff): Emergency Department and Fracture Clinic Medical, Nursing, Patient Service Assistants
CLINICAL PRACTICE GUIDELINE Scaphoid and Other Wrist Injuries in the Emergency Department SCOPE (Area): SCOPE (Staff): Emergency Department and Fracture Clinic Medical, Nursing, Patient Service Assistants
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
.org. Clavicle Fracture (Broken Collarbone) Anatomy. Description. Cause. Symptoms
 Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans
 AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans Summary of Recommendations The following is a summary of the recommendations in the AAOS clinical practice guideline, The Diagnosis
AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans Summary of Recommendations The following is a summary of the recommendations in the AAOS clinical practice guideline, The Diagnosis
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Common wrist injuries in sport. Chris Milne Sports Physician Hamilton,NZ
 Common wrist injuries in sport Chris Milne Sports Physician Hamilton,NZ Overview / Classification Acute injuries Simple - wrist sprain Not so simple 1 - Fracture of distal radius/ulna 2 - Scaphoid fracture
Common wrist injuries in sport Chris Milne Sports Physician Hamilton,NZ Overview / Classification Acute injuries Simple - wrist sprain Not so simple 1 - Fracture of distal radius/ulna 2 - Scaphoid fracture
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Radial Head Fracture Repair and Rehabilitation
 1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
.org. Tennis Elbow (Lateral Epicondylitis) Anatomy. Cause
 Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath
 Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath Difficult Balance Many hand conditions can be managed non-operatively / simply Missed injury or delayed diagnosis not uncommon Common Problems
Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath Difficult Balance Many hand conditions can be managed non-operatively / simply Missed injury or delayed diagnosis not uncommon Common Problems
August 1st, 2006. Scaphoid Fractures. Dr. Christine Walton, PGY 2 Orthopedics
 August 1st, 2006 Scaphoid Fractures Dr. Christine Walton, PGY 2 Orthopedics Injury Patterns to the Carpal Bones 1) Perilunate pattern injuries 2) Axial pattern injuries 3) Local impaction/avulsion injuries
August 1st, 2006 Scaphoid Fractures Dr. Christine Walton, PGY 2 Orthopedics Injury Patterns to the Carpal Bones 1) Perilunate pattern injuries 2) Axial pattern injuries 3) Local impaction/avulsion injuries
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
.org. Distal Radius Fracture (Broken Wrist) Description. Cause
 Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Basal Joint Arthritis
 Basal Joint Arthritis What Is Basal Joint Arthritis? Arthritis is a disease that causes inflammation and stiffness in the joints. It often affects the joint at the base of the thumb, called the basal joint.
Basal Joint Arthritis What Is Basal Joint Arthritis? Arthritis is a disease that causes inflammation and stiffness in the joints. It often affects the joint at the base of the thumb, called the basal joint.
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
ESSENTIALPRINCIPLES. Wrist Pain. Radial and Ulnar Collateral Ligament Injuries. By Ben Benjamin
 ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA
 Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Youth Thrower s Elbow
 Youth Thrower s Elbow Description Youth Thrower s elbow is an inflammatory condition involving the growth plate of the humerus, near the inner elbow at the medial epicondyle.(figure 1) This condition is
Youth Thrower s Elbow Description Youth Thrower s elbow is an inflammatory condition involving the growth plate of the humerus, near the inner elbow at the medial epicondyle.(figure 1) This condition is
We studied 45 patients with 46 fractures of the
 Patterns of healing of scaphoid fractures THE IMPORTANCE OF VASCULARITY R. W. Kulkarni, R. Wollstein, R. Tayar, N. Citron From the St Helier Hospital, Carshalton, England We studied 45 patients with 46
Patterns of healing of scaphoid fractures THE IMPORTANCE OF VASCULARITY R. W. Kulkarni, R. Wollstein, R. Tayar, N. Citron From the St Helier Hospital, Carshalton, England We studied 45 patients with 46
Wrist and Hand Injuries Keep Your Edge: Hockey Sports Medicine 2015 Toronto, Canada August 28-30
 Wrist and Hand Injuries Keep Your Edge: Hockey Sports Medicine 2015 Toronto, Canada August 28-30 Steven E. Rokito, MD Division Chief, Sports Medicine, NSLIJ Associate team orthopedist NY Islanders Wrist
Wrist and Hand Injuries Keep Your Edge: Hockey Sports Medicine 2015 Toronto, Canada August 28-30 Steven E. Rokito, MD Division Chief, Sports Medicine, NSLIJ Associate team orthopedist NY Islanders Wrist
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Treatment Guide Understanding Elbow Pain. Using this Guide. Choosing Your Care. Table of Contents:
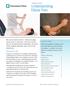 Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Sports Related Fractures of the Foot and Ankle
 Sports Related Fractures of the Foot and Ankle Patrick Ebeling, MD Orthopedic Foot and Ankle Surgeon Twin Cities Orthopedics Burnsville, MN No disclosures Sports Related Fractures of 5 th Metatarsal Fractures
Sports Related Fractures of the Foot and Ankle Patrick Ebeling, MD Orthopedic Foot and Ankle Surgeon Twin Cities Orthopedics Burnsville, MN No disclosures Sports Related Fractures of 5 th Metatarsal Fractures
.org. Metastatic Bone Disease. Description
 Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Hand Injuries and Disorders
 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Ulnar sided Wrist Pain
 Ulnar sided Wrist Pain 1 Susan Cross, 1 Anshul Rastogi, 2 Brian Cohen, 1 Rosy Jalan 1 Dept of Radiology, Barts Health NHS Trust, London, UK 2 London Orthopaedic Centre Contact: susan.cross@bartshealth.nhs.uk
Ulnar sided Wrist Pain 1 Susan Cross, 1 Anshul Rastogi, 2 Brian Cohen, 1 Rosy Jalan 1 Dept of Radiology, Barts Health NHS Trust, London, UK 2 London Orthopaedic Centre Contact: susan.cross@bartshealth.nhs.uk
Treatment Guide Understanding Hand and Wrist Pain. Using this Guide. Choosing Your Care
 Treatment Guide Understanding Hand and Wrist Pain With how much we rely on our hands, there s no wonder hand and wrist pain can be so disabling and frustrating. When this pain interferes with typing on
Treatment Guide Understanding Hand and Wrist Pain With how much we rely on our hands, there s no wonder hand and wrist pain can be so disabling and frustrating. When this pain interferes with typing on
A Patient's Guide to Arthritis of the Finger Joints
 Introduction A Patient's Guide to Arthritis of the Finger Joints When you stop to think about how much you use your hands, it's easy to see why the joints of the fingers are so important. Arthritis of
Introduction A Patient's Guide to Arthritis of the Finger Joints When you stop to think about how much you use your hands, it's easy to see why the joints of the fingers are so important. Arthritis of
Volar percutaneous transtrapezial fixation of scaphoid waist fractures : surgical technique
 Acta Orthop. Belg., 2012, 78, 121-125 TECHNICAL NOTE Volar percutaneous transtrapezial fixation of scaphoid waist fractures : surgical technique Ghislain F. A. E. GEuRtS, Roger P. VAn RiEt, Geert MEERMAnS,
Acta Orthop. Belg., 2012, 78, 121-125 TECHNICAL NOTE Volar percutaneous transtrapezial fixation of scaphoid waist fractures : surgical technique Ghislain F. A. E. GEuRtS, Roger P. VAn RiEt, Geert MEERMAnS,
PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE
 PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE I. DIGITAL FRACTURES A. Background Digital fractures commonly occur in the workplace and are usually the result of a crush injury from a falling object, or
PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE I. DIGITAL FRACTURES A. Background Digital fractures commonly occur in the workplace and are usually the result of a crush injury from a falling object, or
PERILUNATE AND LUNATE DISLOCATIONS
 PERILUNATE AND LUNATE DISLOCATIONS Rebecca Morris Advanced Practitioner Plain Film Reporting March 2011 Perilunate and Lunate dislocations Introduction Definition Anatomy Clinical presentation Mechanism
PERILUNATE AND LUNATE DISLOCATIONS Rebecca Morris Advanced Practitioner Plain Film Reporting March 2011 Perilunate and Lunate dislocations Introduction Definition Anatomy Clinical presentation Mechanism
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a
A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ACUTE HAND INJURY PROTOCOLS
 ACUTE HAND INJURY PROTOCOLS I. FRACTURES OF THE HAND AND DIGITS Digital and hand fractures are seen in workers who use their hands, due to the exposed nature of the hand (in most functions) at work. Most
ACUTE HAND INJURY PROTOCOLS I. FRACTURES OF THE HAND AND DIGITS Digital and hand fractures are seen in workers who use their hands, due to the exposed nature of the hand (in most functions) at work. Most
Sports Related Injuries of the Hand, Wrist and Elbow. Melissa Nayak, M.D. Department of Orthopaedics Division of Sports Medicine
 Sports Related Injuries of the Hand, Wrist and Elbow Melissa Nayak, M.D. Department of Orthopaedics Division of Sports Medicine Injury triage History, mechanism of injury (MOI) Assess extent of swelling,
Sports Related Injuries of the Hand, Wrist and Elbow Melissa Nayak, M.D. Department of Orthopaedics Division of Sports Medicine Injury triage History, mechanism of injury (MOI) Assess extent of swelling,
3.1. Presenting signs and symptoms; may include some of the following;
 Title: Clinical Protocol for the management of Forearm and Wrist injuries. Document Owner: Deirdre Molloy Document Author: Deirdre Molloy Presented to: Care & Clinical Policies Date: August 2015 Ratified
Title: Clinical Protocol for the management of Forearm and Wrist injuries. Document Owner: Deirdre Molloy Document Author: Deirdre Molloy Presented to: Care & Clinical Policies Date: August 2015 Ratified
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Shoulder Impingement/Rotator Cuff Tendinitis
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints
Osteoarthritis progresses slowly and the pain and stiffness it causes worsens over time.
 Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Sports Health. Dedicated to building champions
 Sports Health Dedicated to building champions Dedicated to Building Focus The Competitive Edge All athletes deserve the very best sports-related care and treatment that s one-on-one and state-of-the-art.
Sports Health Dedicated to building champions Dedicated to Building Focus The Competitive Edge All athletes deserve the very best sports-related care and treatment that s one-on-one and state-of-the-art.
WRIST EXAMINATION. Look. Feel. Move. Special Tests
 WRIST EXAMINATION Look o Dorsum, side, palmar- palmar flex wrist to exacerbate dorsal swellings o Deformity e.g. radial deviation after colles, prominent ulna o Swellings e.g. ganglion o Scars, muscle
WRIST EXAMINATION Look o Dorsum, side, palmar- palmar flex wrist to exacerbate dorsal swellings o Deformity e.g. radial deviation after colles, prominent ulna o Swellings e.g. ganglion o Scars, muscle
ISOLATED FRACTURE OF THE CAPITATE : THE VALUE OF MRI IN DIAGNOSIS AND FOLLOW UP
 CASE REPORT ISOLATED FRACTURE OF THE CAPITATE : THE VALUE OF MRI IN DIAGNOSIS AND FOLLOW UP F. DE SCHRIJVER 1, L. DE SMET 1 We report 2 new cases of isolated fracture of the capitate. The diagnosis and
CASE REPORT ISOLATED FRACTURE OF THE CAPITATE : THE VALUE OF MRI IN DIAGNOSIS AND FOLLOW UP F. DE SCHRIJVER 1, L. DE SMET 1 We report 2 new cases of isolated fracture of the capitate. The diagnosis and
Toe fractures are one of the most
 Evaluation and Management of Toe Fractures ROBERT L. HATCH, M.D., M.P.H., and SCOTT HACKING, M.D., University of Florida College of Medicine, Gainesville, Florida Fractures of the toe are one of the most
Evaluation and Management of Toe Fractures ROBERT L. HATCH, M.D., M.P.H., and SCOTT HACKING, M.D., University of Florida College of Medicine, Gainesville, Florida Fractures of the toe are one of the most
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
ICD-10-CM Injury Coding for Orthopedics
 ICD-10-CM Injury Coding for Orthopedics Shelly Cronin, Director ICD-10 Training No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
ICD-10-CM Injury Coding for Orthopedics Shelly Cronin, Director ICD-10 Training No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
3. Be able to perform a detailed clinical examination of the forearm and wrist.
 Patient Care: 1. Demonstrate appropriate evaluation and treatment of patients with hand/wrist surgery problems in the emergency room and as part of the inpatient consultation service, including application
Patient Care: 1. Demonstrate appropriate evaluation and treatment of patients with hand/wrist surgery problems in the emergency room and as part of the inpatient consultation service, including application
Running Head: Salter Harris Fractures 1
 Running Head: Salter Harris Fractures 1 Salter Harris Classification of Growth Plate Fractures November 15 th, 2011 Salter Harris Fractures 2 Abstract Salter-Harris Classifications are a straightforward
Running Head: Salter Harris Fractures 1 Salter Harris Classification of Growth Plate Fractures November 15 th, 2011 Salter Harris Fractures 2 Abstract Salter-Harris Classifications are a straightforward
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
IFSSH Scientific Committee on. Wrist Biomechanics and Instability
 IFSSH Scientific Committee on Wrist Biomechanics and Instability Chair: Hisao Moritomo (Japan) Committee: Emmanuel Apergis (Greece) Guillaume Herzberg (France) Scott Wolfe (USA) Jose Maria Rotella (Argentina)
IFSSH Scientific Committee on Wrist Biomechanics and Instability Chair: Hisao Moritomo (Japan) Committee: Emmanuel Apergis (Greece) Guillaume Herzberg (France) Scott Wolfe (USA) Jose Maria Rotella (Argentina)
Minimal Invasive Treatment for Scaphoid Fractures Using the Cannulated Herbert Screw System
 Techniques in Hand and Upper Extremity Surgery 7(4):141 146, 2003 T E C H N I Q U E 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Minimal Invasive Treatment for Scaphoid Fractures Using the Cannulated
Techniques in Hand and Upper Extremity Surgery 7(4):141 146, 2003 T E C H N I Q U E 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Minimal Invasive Treatment for Scaphoid Fractures Using the Cannulated
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
.org. Osteochondroma. Solitary Osteochondroma
 Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
The 10 Most Common Hand Pathologies In Adults. 1. Carpal Tunnel and Cubital Tunnel
 The 10 Most Common Hand Pathologies In Adults Bobbi Jacobsen PA C 1. Carpal Tunnel and Cubital Tunnel CARPAL TUNNEL (median nerve) ( ) Pain and numbness Distal, proximal radiating Sensory disturbance Distribution
The 10 Most Common Hand Pathologies In Adults Bobbi Jacobsen PA C 1. Carpal Tunnel and Cubital Tunnel CARPAL TUNNEL (median nerve) ( ) Pain and numbness Distal, proximal radiating Sensory disturbance Distribution
Legg-Calve'-Perthes Disease The National Osteonecrosis Foundation
 Home Osteonecrosis Osteonecrosis of the Jaw Mission Statement More About Us Related Sites Questions & Answers NONF Brochure Legg-Calve'-Perthes Disease Brochure Membership Form NONF Newsletter Volunteers
Home Osteonecrosis Osteonecrosis of the Jaw Mission Statement More About Us Related Sites Questions & Answers NONF Brochure Legg-Calve'-Perthes Disease Brochure Membership Form NONF Newsletter Volunteers
X-Plain Temporomandibular Joint Disorders Reference Summary
 X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Non Operative Management of Common Fractures
 Non Operative Management of Common Fractures Mr Duy Thai Orthopaedic Surgeon MBBS, FRACS (Ortho), Dip Surg Anat NOT ALL FRACTURES NEED TO BE FIXED FRACTURE CLINIC EMERGENCY DEPARTMENTS GENERAL PRACTITIONERS
Non Operative Management of Common Fractures Mr Duy Thai Orthopaedic Surgeon MBBS, FRACS (Ortho), Dip Surg Anat NOT ALL FRACTURES NEED TO BE FIXED FRACTURE CLINIC EMERGENCY DEPARTMENTS GENERAL PRACTITIONERS
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
