Impaired Function of the Levator Ani Muscle in the Grand Multipara and Great Grand Multipara
|
|
|
- Willis Wood
- 8 years ago
- Views:
Transcription
1 Tohoku J. Exp. Med., 2006, Function 210, of the Levator Ani Muscle in the Grand Multipara 365 Impaired Function of the Levator Ani Muscle in the Grand Multipara and Great Grand Multipara EROL KISLI, 1 MESUDE KISLI, 2 HAVVA AGARGUN, 3 FILIZ ALTINOKYIGIT, 3 MANSUR KAMACI, 4 EKREM OZMAN 5 and CETIN KOTAN 1 1 Department of General Surgery, School of Medicine, Yuzuncu Yıl University, Van, Turkey 2 Department of Neurology, State Hospital, Van, Turkey 3 Department of Obstetric and Gynecology, State Hospital, Van, Turkey 4 Department of Obstetric and Gynecology, School of Medicine, Yuzuncu Yıl University, Van, Turkey 5 Department of Urology, School of Medicine, Yuzuncu Yıl University, Van, Turkey KISLI, E., KISLI, M., AGARGUN, H., ALTINOKYIGIT, F., KAMACI, M., OZMAN, E. and KOTAN, C. Impaired Function of the Levator Ani Muscle in the Grand Multipara and Great Grand Multipara. Tohoku J. Exp. Med., 2006, 210 (4), Repeated deliveries might disturb the levator function and increase defecation disorders. In this prospective study, we determined the electric activity of the levator ani muscle (LAM) in nullipara, multipara, grand multipara, and great grand multipara (20 subjects for each group). Multiparity, grand multiparity, and great grand multiparity were defined as women having 2-5, 6-9, and 10 and over deliveries, respectively. The number of deliveries of multipara, grand multipara and great grand multipara were 4.05 ± 1.14 (2-5), 7.55 ± 1.23 (6-9) and 12.2 ± 2.16 (10-17), respectively. All women were asked whether they had experienced constipation, fecal or urinary incontinence, and/or pelvic pain. All women were also evaluated for pelvic organ prolapse. Electromyography (EMG) of the LAM at rest and on contraction was recorded. EMG is an electrical recording of muscle activity. Constipation, incontinence and pelvic organ prolapse were encountered in multipara, grandmultipara and great grand multipara women. The LAM EMG at rest and on contraction in the nullipara was accepted as control. Both the resting and contractile activities of the LAM were as follows: nullipara > multipara > grand multipara > great grand multipara. These findings indicate that levator dysfunction and defecation disorders are increased with repeated deliveries because of pudendal and/or levator ani nerve injury and traumatic injury to the LAM occurred with the mechanical stresses of vaginal deliveries. electric activity; levator ani muscle; multipara; grand multipara; great grand multipara 2006 Tohoku University Medical Press There are several causes of levator ani muscle (LAM) dysfunction, such as conditions of chronic straining and increased intraabdominal pressure, senility, debility and obesity due to fat-laden viscera, which lead to increase in the intraabdominal pressure (Shafik 1983). One of Received May 8, 2006; revision accepted for publication October 20, Correspondence: Dr. Erol Kisli, Tip Fakultesi Araştirma Hastanesi, Genel Cerrahi Anabilim Dalı, Maraş caddesi, Van, Turkey. erolkisli@hotmail.com 365
2 366 E. Kisli et al. the common causes of levator dysfunction seems to be gestation and delivery. The gravid uterus enlarges progressively during gestation. It induces its effect on the LAM probably through: (a) increase of the uterine weight, (b) elevation of the intraabdominal pressure and (c) mechanical interference with its functional activity. These effects might disturb the levator function and also it is postulated that these effects are augmented with repeated pregnancies. The continuously increasing size of the gravid uterus presumably affects the levator function, particularly in women with repeated deliveries (Shafik and El-Sibai 2002). Previous studies have shown that multiparity, forceps delivery, increased duration of the second stage of labour and high birth weight may lead to anal sphincter injury (Beevors et al. 1991; Cornes et al. 1991; Sultan et al. 1993; Ryhammer et al. 1995). While most injuries to the anal sphincter following delivery are recognised and repaired, an injury to the LAM may occur and remain undiagnosed (Shafik and El-Sibai 2002). The LAM is a muscle of evacuation. Its contraction at defecation or urination helps to evacuate the rectum or urinary bladder (Shafik 1991, 1992a). Preceding studies have demonstrated that a derangement of the LAM would lead to a levator dysfunction syndrome which comprises defecation and urinary disorders as well as perineal descent, anorectal intussusception and rectal prolapse (Shafik 1983). Grand multiparity and great grand multiparity are not uncommon in Van, the east of Turkey (Gurel 1999). The aim of the current study is to investigate the electric activity of LAM in nullipara, multipara, grand multipara and great grand multipara and to determine LAM dysfunction in grand multipara and great grand multipara. MATERIALS AND METHODS The study was approved by the ethics committee of Yuzuncu Yıl University and patients had given informed consent to the investigation. Eighty women were included in this prospective study. Twenty nullipara, 20 multipara, 20 grand multipara and 20 great grand multipara women who were come in to the clinic for routine examination were chosen for the study. These women were asked to participate in the study. Women who had accepted to participate were included in the study. The mean age of nullipara women were ± 9.39 S.D. years (range 32-58). They had no history of deliveries or abortions. These women were considered as controls. The mean age of the multipara women were 45.9 ± 9.48 S.D. years (range 33-63). The mean number of full term deliveries was 4.05 ± 1.14 S.D. (range 2-5). The grand multipara women had a mean age of 45.2 ± 7.69 S.D. years (range 33-62). The mean number of full term deliveries was 7.55 ± 1.23 S.D. (range 6-9). The great grand multipara women had a mean age of ± 6.13 S.D. years (range 39-59). The mean number of full term deliveries was 12.2 ± 2.16 S.D. (range 10-17) (Table 1). Multipara, grand multipara and great grand multipara women who had only some prolonged second stage of labour as determined by medical records are included. The second stage was considered prolonged if it lasted more than 1 hr. Woman who had obesity, caesarean section delivery, forceps delivery, history of abortions, chronic cough or smoking was not included. Women who were over 65 years of ages excluding from the study. Parous women, who had detected sphincter injuries and perineal lacerations at the time of delivery, clinically were also excluded from the study. The initial assessment of the patients in our unit is made by anamnesis and physical examination. Urogynecologic histories were taken and physical examinations were performed. All women were asked whether they had experienced constipation, fecal or urinary incontinence, and/or pelvic pain in the form of proctalgia or vulvodynia. Electromyography (EMG) The LAM EMG at rest and on contraction by straining was recorded using the method described previously (Shafik 1998). Briefly, a concentric needle electromyographic electrode (Type 151T, Nihon Kohden, Tokyo) was introduced into the LAM 2 cm lateral to the anal orifice and 2 cm deep. A ground electrode was applied to the thigh and a standard electromyographic apparatus (Type MEP-9104K, Nihon Kohden) was used to amplify and display the potentials recorded. Statistical analysis The results were analysed statistically using ANOVA test. Scheffe test was used for post-hoc comparisons. Pearson correlation analysis was used for correlations. Significance was described to p < 0.05, and values were given as the mean ± S.D.
3 Function of the Levator Ani Muscle in the Grand Multipara 367 RESULTS There was no statistical difference in aspect of ages among groups (p > 0.05). Mean birthweight in multipara, grand multipara and great grand multipara women were 3, ± g, 3, ± g, and 3, ± g, respectively. Mean body mass index (BMI) in nullipara, multipara, grand multipara and great grand multipara women were ± 1.62, ± 1.07, ± 0.91, and ± 0.70, respectively. There are no significant differences in aspect of mean birthweight (other than the nulliparous group) and mean BMI in groups, statistically (p > 0.05) (Table 1). All parous (multipara, grand multipara and great grand multipara) women had episiotomy. Five of nullipara, 6 of multipara, 5 of grand multipara and 5 of great grand multipara women are in menopause. TABLE 1. Clinical features of the studied subjects. Nullipara (n = 20) Multipara (n = 20) Grand multipara (n = 20) Great grand multipara (n = 20) Years of age Number of deliveries Mean ± S.D ± ± ± ± 6.13 Range Mean ± S.D ± ± ± 2.16 Range Mean birthweight (g) 3, ± , ± , ± Mean BMI (kg/m 2 ) ± ± ± ± 0.70 Values were given as the mean ± S.D. BMI, body mass index. TABLE 2. Defecation disorders, pelvic organ prolapse and pelvic pain in the studied subjects. Constipation Incontinence Pelvic pain Pelvic organ prolapse Fecal Urinary Proctalgia Vulvodynia Nullipara Cystocele Rectocele Uterine prolapse Multipara Cystocele 1 Rectocele Uterine prolapse Grand multipara 5 3 (α) 4 (β) 1 Cystocele 2 (α) Rectocele 1 Uterine prolapse 1 (β) Great grand multipara 4 5 (γ, λ) 7 (ω, δ) 2 1 (ε) Cystocele 2 (γ, λ) Rectocele 1 (ω) Uterine prolapse 2 (δ, ε) Each of α, β, γ, λ, ω, δ and ε indicates the same subject.
4 368 E. Kisli et al. Clinical findings Table 2 exhibits the defecation, urinary disorders, pelvic pain as well as the pelvic organ prolapse of the studied groups. Nullipara women had no constipation, fecal or urinary incontinence or pelvic organ prolapse. Constipation, incontinence and pelvic organ prolapse were encountered in multipara, grand multipara and great grand multipara women (Table 2). Constipation took the form of excessive straining at defecation although the stools were soft and bulky. Meanwhile, one woman in grand multipara and 2 women in great grand multipara complained of pelvic pain in the form of proctalgia. One woman (subject ε ) complained of vulvodynia in great grand multipara. None of the nullipara women had pelvic organ prolapse. One of multipara, 2 of grand multipara and 2 of great grand multipara women had cystocele. One of grand multipara and 1 of great grand multipara (subject ω ) had rectocele. One of grand multipara (subject β) and 2 of great grand multipara (subjects δ, ε) had uterine prolapse (Table 2). One woman (subject α) with cystocele had also fecal incontinence, and one woman (β ) with uterine prolapse had also urinary incontinence in grand multipara. Two women (γ, λ) with cystocele had also fecal incontinence, one woman (ω) with rectocele had also urinary incontinence, one woman (δ) with uterine prolapse had also urinary incontinence, and one woman (ε) with uterine prolapse had also vulvodynia in great grand multipara. EMG TABLE 3. The LAM EMG at rest and on contraction in the studied subjects Potentials (mv). At rest ± On contraction Nullipara (control) Multipara Grandmultipara Great grandmultipara Mean ± S.D. Range Mean Range Mean Range Mean Range ± 80.4 Values were given as the mean ± S.D. Post hoc Scheffe test: * p < with respect to control. p < 0.01 with respect to multipara. p < with respect to multipara. Ω p < with respect to grand multipara ± 9.77 * ± ± 5.09 Ω ± * ± ± Ω Fig. 1. EMG of the levator ani muscle in a nulliparous woman. Resting activity (A); on contraction (B).
5 Function of the Levator Ani Muscle in the Grand Multipara 369 EMG findings The LAM EMG at rest and on contraction in the nullipara was accepted as control (Table 3 and Fig. 1). In the multiparous women, resting and contraction EMG of the LAM differed significantly from that of the controls with a mean potential of ± 9.77 mv and ± 43.9 mv, respectively (p < 0.001, p < 0.001) (Table 3 and Fig. 2). In the grand multiparous women, the mean of both the resting and contractile activity of the LAM was significantly lower than that of the multipara with a mean potential of 70.1 ± mv and ± mv, respectively (p < 0.01, p < 0.001) (Table 3 and Fig. 3). In the great grand multipara, the mean of both the resting and contractile activity of the LAM was significantly lower than that of the grand multipara with a mean potential of 45.8 ± 5.09 mv and Fig. 2. EMG of the levator ani muscle in a multiparous woman. Resting activity (A); on contraction (B). Fig. 3. EMG of the levator ani muscle in a grand multiparous woman. Resting activity (A); on contraction (B). Fig. 4. EMG of the levator ani muscle in a great grand multiparous woman. Resting activity (A); on contraction (B).
6 370 E. Kisli et al ± mv, respectively ( p < 0.001, p < 0.001) (Table 3 and Fig. 4). A negative correlation was found among labour number and both resting (r = 0.73, p < 0.001) and contraction potentials (r = 0.85, p < 0.001) (Pearson correlation analysis). DISCUSSION The cause of levator dysfunction in the parous women needs to be discussed. Studies have shown that the gravid uterus, by virtue of its weight and associated increased intraabdominal pressure, might disturb the levator function. It is postulated that this effect is augmented with repeated pregnancies (Shafik and El-Sibai 2002). However, Lien et al. (2005) reported that the pudendal nerve is injured during vaginal delivery but not during pregnancy. Animal models simulating the childbirth trauma with vaginal distension in rat support this hypothesis (Lin et al. 1998; Damaser et al. 2003). Heit et al. (2001) reported that elective cesarean section is the only true primary prevention strategy for childbirth injuries to the pelvic floor. The function of the LAM as a muscle of evacuation for rectum and urinary bladder is disturbed with repeated pregnancies and delivery. The derangement of LAM may lead to fecal and urinary disorders in the form of incontinence or retention (Shafik and El-Sibai 2002). Shafik and El-Sibai (2002) reported that the LAM EMG in multipara women with a prolonged 2nd stage of labour exhibited a lower activity than controls at rest and on contraction. They also reported that primipara women showed diminished activity in both conditions, which was significantly higher than that of multipara. In the present study, it was found that grand multiparous women showed diminished both the resting and contractile activity of the LAM significantly, lower than that of the multipara and nullipara. It was also found that great grand multiparous women showed diminished both the resting and contractile activity of the LAM significantly, lower than that of the grand multipara and multipara. Shafik and El-Sibai (2002) reported that 16.6% of primipara and 31.8% of multipara with prolonged 2nd stage of labour had constipation. Shafik (1988) reported that they experienced excessive straining at stool (strainodynia) although the stools were soft and bulky. They explained that this strainodynia is probably due to the levator sagging, which exposes the anal canal to the direct effect of the increased intra-abdominal pressure. On straining at stool, the anal canal is occluded rather than opened, as would occur under normal physiological conditions (Shafik and El-Sibai 2002). In the present study, 10% of multipara, 25% of grand multipara and 20% of great grand multipara women had constipation. Shafik and El-Sibai (2002) reported that 8.3% of prolonged 2nd stage of labour in the primiparous women and 22.7% of prolonged 2nd stage of labour in the multiparous women occurred fecal incontinence. They also reported that 8.3% of prolonged 2nd stage of labour in the primiparous women and 36.3% of prolonged 2nd stage of labour in the multiparous women occurred stress urinary incontinence. They explained that incontinence whether fecal or urinary is due most probably to pudendal neuropathy because of sagging of the LAM. The type of incontinence would depend on the branch of pudendal nerve most involved: in fecal incontinence it is related to the inferior rectal nerve and in urinary incontinence to the perineal branch (Shafik 1992b, 1994; Shafik and El-Sibai 2002). However, no contribution of the pudendal nerves to levator ani innervation was noted. Additionally, many electrophysiologic studies have demonstrated that the levator ani muscles and the external anal sphincter have physiologically distinct innervations and that the pudendal nerve does not appear to innervate the iliococcygeal, pubococcygeal, or puborectalis muscles (Percy et al. 1981; Swash et al. 1985; Snooks and Swash 1986). Pierce et al. (2005) studied in the female squirrel monkey to characterize the spinal distribution of afferent and efferent pathways that innervate the levator ani muscle and they concluded that the levator ani muscle has a distinct innervation with very little or no contribution from the pudendal nerve. Barber et al. (2002) studied on 12 fresh-frozen female cadavers and reported that the female levator ani muscle is not innervated by the pudendal nerve, but rather
7 Function of the Levator Ani Muscle in the Grand Multipara 371 by innervation that originates from the S3-5 nerve roots that travel on the superior surface of the pelvic floor. They also reported that the distinct innervation of the levator ani muscles by the levator ani nerve and the external anal and urethral sphincters by the pudendal nerve provide a mechanism to explain the varying types of pelvic floor disorders that can occur in women after childbirth. For instance, it may explain the reason that some women experience urinary incontinence or fecal incontinence and that other women experience pelvic organ prolapse. In the current investigation, fecal incontinence occurred in both multiparous, grandmultiparous and great grand multiparous women 5%, 15% and 25%, respectively and urinary incontinence occurred in both multiparous, grandmultiparous and great grand multiparous women 10%, 20% and 35%, respectively. The incidence of incontinence (fecal and urinary) was higher in the great grand multipara than the grand multipara and multipara women, due apparently to a greater extent of traumatisation to the LAM in the great grand multipara than the grand multipara and multipara women. Although constipation, fecal or urinary incontinence occurred with multiparous, grandmultiparous and great grand multiparous women, did not occur with control (nullipara women) groups probably because levator dysfunction did not occur. None of the nullipara women had pelvic organ prolapse. Five percent of multipara, 10% of grand multipara and 10% of great grand multipara women had cystocele. Five percent of grand multipara and 5% of great grand multipara women had rectocele. Five percent of grand multipara and 10% of great grand multipara women had uterine prolapse. Pelvic organ prolapse occured with parous women due probably to levator dysfunction. One woman in grand multipara and 2 women in great grand multipara women studied complain of pelvic pain in the form of proctalgia and one woman complain of vulvodynia in great grand multipara women, due probably to involvement of the sensory fibres of the pudendal nerve and or levator ani nerve. Sometimes even after menopause, when loss of estrogen support to the pelvic floor had led to deterioration in fecal control (Donnelly et al. 1997). Most cases of stress urinary incontinence occur years after menopause. It has been postulated that many women with a slightly weakened urethra and levator from birth injury remain asymptomatic until menopause and aging further impair the continence mechanism (Lin et al. 1998). In our study, one of multipara woman who was in menopause had urinary incontinence. Two of grand multipara women who were in menopause had urinary incontinence. One of grand multipara woman who was in menopause had fecal incontinence. Two of great grand multipara women who were in menopause had urinary incontinence. One of great grand multipara women who were in menopause had fecal incontinence. One of great grand multipara woman who was in menopause had rectocele and urinary incontinence. One of great grand multipara woman who was in menopause had cystocele. For these patients menopause may have a contributory role for the disorders. The present study is the first, to our knowledge, that compares the EMG findings and LAM dysfunction in multipara and grand multipara with great grand multipara. In conclusion, these findings suggest that levator dysfunction may occur in the parous women due to pudendal and/or levator ani nerve injury and traumatic injury to the levator ani muscle occur with the mechanical stresses of vaginal delivery. LAM dysfunction is most common in the great grand multipara. CONCLUSION The EMG findings as well as the clinical manifestations of the population in the current study have shown that repeated deliveries may affect the electric activity of the LAM. The insult to the LAM is maximum in the great grand multipara women. In conclusion, defecation disorders are increased with repeated deliveries. References Barber, M.D., Bremer, R.E., Thor, K.B., Dolber, P.C., Kuehl, T.J. & Coates, K.W. (2002) Innervation of the female levator ani muscles. Am. J. Obstet. Gynecol., 187, Beevors, M.A., Lubowski, D.Z., King, D.W. & Carlton, M.A. (1991) Pudendal nerve function in women with symptom-
8 372 E. Kisli et al. atic uterovaginal prolapse. Int. J. Colorectal. Dis., 6, Cornes, H., Bartolo, D.C.C. & Stirrat, G.M. (1991) Changes in anal canal sensation after childbirth. Br. J. Surg., 78, Damaser, M.S., Broxton-King, C., Ferguson, C., Kim, F.J. & Kerns, J.M. (2003) Functional and neuroanatomical effects of vaginal distention and pudendal nerve crush in the female rat. J. Urol., 170, Donnelly, V.S., O Connell, P.R. & O Herlihy, C. (1997) The influence of oestrogen replacement on fecal incontinence in post-menopausal women. BJOG, 104, Gurel, H., Gurel, S.A. & Kamaci, M. (1999) Obstetric features and fetal outcome in grandgrandmultiparas. J. Clin. Sci. Doc., 2, Heit, M., Mudd, K. & Culligan, P. (2001) Prevention of childbirth injuries to the pelvic floor. Curr. Womens Health Rep., 1, Lin, A.S., Carrier, S., Morgan, D.M. & Lue, T.F. (1998) Effect of simulated birth trauma on the urinary continence mechanism in the rat. Urology, 52, Lien, K.C., Morgan, D.M., Delancey, J.O. & Ashton-Miller, J.A. (2005) Pudendal nerve stretch during vaginal birth: a 3D computer simulation. Am. J. Obstet. Gynecol., 192, Percy, J.P., Neill, M.E., Swash, M. & Parks, A.G. (1981) Electrophysiological study of motor nerve supply of pelvic floor. Lancet, 1, Pierce, L.M., Reyes, M., Thor, K.B., Dolber, P.C., Bremer, R.E., Kuehl, T.J. & Coates, K.W. (2005) Immunohistochemical evidence for the interaction between levator ani and pudendal motor neurons in the coordination of pelvic floor and visceral activity in the squirrel monkey. Am. J. Obstet. Gynecol., 192, Ryhammer, A.M., Bek, K.M. & Lauberg, S. (1995) Multiple vaginal deliveries increase the risk of permanent incontinence of flatus and urine in normal premenopausal women. Dis. Colon Rectum., 38, Shafik, A. (1983) The levator dysfunction syndrome. A new syndrome with report of seven cases. Coloproctology, 5, Shafik, A. (1988) Strainodynia: an etiopathologic study. J. Clin. Gastroenterol., 10, Shafik, A. (1991) Constipation: some provocative thoughts. J. Clin. Gastroenterol., 13, Shafik, A. (1992a) Micturition and urinary continence. New concepts. Int. Urogynecol. J., 3, Shafik, A. (1992b) Pudendal canal decompression in the treatment of idiopathic fecal incontinence. Dig. Surg., 9, Shafik, A. (1994) Pudendal canal decompression in the treatment of urinary stress incontinence. Int. Urogynecol. J., 5, Shafik, A. (1998) A new concept of the anatomy of the anal sphincter mechanism and the physiology of defecation. Mass contraction of the pelvic floor muscles. Int. Urogynecol. J., 9, Shafik, A. & El-Sibai, O. (2002) Study of the levator ani muscle in the multipara: role of levator dysfunction in defecation disorders. J. Obstet. Gynaecol., 22, Snooks, S.J. & Swash, M. (1986) The innervation of the muscles of continence. Ann. R. Coll. Surg. Engl., 68, Sultan, A.H., Kamm, M.A., Hudson, C.N., Thomas, J.M. & Batram, C.I. (1993) Anal sphincter disruption during vaginal delivery. N. Engl. J. Med., 329, Swash, M., Snooks, S.J. & Henry, M.M. (1985) Unifying concept of pelvic floor disorders and incontinence. J. R. Soc. Med., 78,
Effects of Pregnancy & Delivery on Pelvic Floor
 Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
UNREPORTED URINARY AND ANAL INCONTINENCE IN WOMEN
 Original Article UNREPORTED URINARY AND ANAL INCONTINENCE IN WOMEN Humera Ansar, Fauzia Adil and Aftab A. Munir ABSTRACT OBJECTIVE: To know the occurrence of unreported urinary and anal incontinence in
Original Article UNREPORTED URINARY AND ANAL INCONTINENCE IN WOMEN Humera Ansar, Fauzia Adil and Aftab A. Munir ABSTRACT OBJECTIVE: To know the occurrence of unreported urinary and anal incontinence in
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Urinary incontinence symptoms during and after pregnancy in continent and incontinent primiparas
 Int Urogynecol J DOI 10.1007/s00192-006-0124-8 ORIGINAL ARTICLE Angela D. Thomason. Janis M. Miller. John OL DeLancey Urinary incontinence symptoms during and after pregnancy in continent and incontinent
Int Urogynecol J DOI 10.1007/s00192-006-0124-8 ORIGINAL ARTICLE Angela D. Thomason. Janis M. Miller. John OL DeLancey Urinary incontinence symptoms during and after pregnancy in continent and incontinent
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse
 Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Urinary Incontinence. Anatomy and Terminology Overview. Moeen Abu-Sitta, MD, FACOG, FACS
 Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Prolapse Repair Systems. a guide To correcting PELVIC ORGAN PROLAPSE
 Anterior PROLAPSE & Posterior REPAIR SYSTEM Prolapse Repair Systems a guide To correcting PELVIC ORGAN PROLAPSE Restore Your Body Pelvic organ prolapse occurs when pelvic structures, like the bladder or
Anterior PROLAPSE & Posterior REPAIR SYSTEM Prolapse Repair Systems a guide To correcting PELVIC ORGAN PROLAPSE Restore Your Body Pelvic organ prolapse occurs when pelvic structures, like the bladder or
Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA
 Pelvic Floor Relaxation Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA Disclosures Beverly Hashimoto: GE Medical Systems: research support and consultant (all fees given to Virginia
Pelvic Floor Relaxation Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA Disclosures Beverly Hashimoto: GE Medical Systems: research support and consultant (all fees given to Virginia
An advanced diagnostic
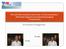 Pelvi-perineal myofascial syndromes: clinical presentation, differential diagnosis and electrophysiological characteristics An advanced diagnostic Dr. Zarza Dr. Itza There's an elephant in this room What
Pelvi-perineal myofascial syndromes: clinical presentation, differential diagnosis and electrophysiological characteristics An advanced diagnostic Dr. Zarza Dr. Itza There's an elephant in this room What
CHAPTER 7. Summary and conclusions
 CHAPTER 7 Summary and conclusions 88 Summary 7.1 SUMMARY 7.1.1 Introduction 7.1.1.1 Incontinence in pregnancy and after childbirth Pelvic floor dysfunction in women is a major health problem. Symptoms
CHAPTER 7 Summary and conclusions 88 Summary 7.1 SUMMARY 7.1.1 Introduction 7.1.1.1 Incontinence in pregnancy and after childbirth Pelvic floor dysfunction in women is a major health problem. Symptoms
Tone Up Your Pelvic Floor. A regular pelvic floor exercise ( Kegel ) routine can prevent symptoms before, during, and after childbirth.
 Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
2 of 6 10/17/2014 9:51 AM
 1 of 6 10/17/2014 9:51 AM 010101 Free 14-Day Trial Tutorial Help Search by keyword or medical code User Name: Password: Directory Print Email Advanced Search Medical Disability Advisor > Cystocele Or Rectocele
1 of 6 10/17/2014 9:51 AM 010101 Free 14-Day Trial Tutorial Help Search by keyword or medical code User Name: Password: Directory Print Email Advanced Search Medical Disability Advisor > Cystocele Or Rectocele
Prevention of Childbirth Injuries to the Pelvic Floor
 Prevention of Childbirth Injuries to the Pelvic Floor Michael Heit, MD, MSPH, Kelly Mudd, MD, and Patrick Culligan, MD Address University of Louisville Health Science Center, Department of Obstetrics and
Prevention of Childbirth Injuries to the Pelvic Floor Michael Heit, MD, MSPH, Kelly Mudd, MD, and Patrick Culligan, MD Address University of Louisville Health Science Center, Department of Obstetrics and
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Does vaginal closure force differ in the supine and standing positions?
 American Journal of Obstetrics and Gynecology (2005) 192, 1722 8 www.ajog.org Does vaginal closure force differ in the supine and standing positions? Daniel M. Morgan, MD, a, * Gurpreet Kaur, BS, a Yvonne
American Journal of Obstetrics and Gynecology (2005) 192, 1722 8 www.ajog.org Does vaginal closure force differ in the supine and standing positions? Daniel M. Morgan, MD, a, * Gurpreet Kaur, BS, a Yvonne
It is well established that parity increases the risk of
 Effect of Mode of Delivery on the Incidence of Urinary Incontinence in Primiparous Women Sarah Hamilton Boyles, MD, MPH, Hong Li, MSPH, Tomi Mori, PhD, Patricia Osterweil, BS, and Jeanne-Marie Guise, MD,
Effect of Mode of Delivery on the Incidence of Urinary Incontinence in Primiparous Women Sarah Hamilton Boyles, MD, MPH, Hong Li, MSPH, Tomi Mori, PhD, Patricia Osterweil, BS, and Jeanne-Marie Guise, MD,
How do I know if I need to have surgery?
 How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
URINARY INCONTINENCE CASE PRESENTATION #1. Urinary Incontinence - History 2014/10/07. Structure of the Female Lower Urinary Tract
 Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Stress Urinary Incontinence & The Pelvis
 Stress Urinary Incontinence & The Pelvis Updated January 2011 by Diane Lee Introduction The research in the last decade has led to a clearer understanding of how load is transferred through the low back
Stress Urinary Incontinence & The Pelvis Updated January 2011 by Diane Lee Introduction The research in the last decade has led to a clearer understanding of how load is transferred through the low back
URINARY INCONTINENCE IN WOMEN
 URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly. Prapa Pattrapornpisut 7 June 2012
 1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
Basics on Bladder and Bowel
 Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Urinary Continence. Second edition FAST FACTS. by Julian Shah and Gary Leach. Anatomy and physiology 7. Investigations and diagnosis 11
 FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
Pelvic Symptoms in Women With Pelvic Organ Prolapse
 Pelvic Symptoms in Women With Pelvic Organ Prolapse Lara J. Burrows, MD, Leslie A. Meyn, MS, Mark D. Walters, MD, and Anne M. Weber, MD, MS From the Department of Obstetrics, Gynecology, and Reproductive
Pelvic Symptoms in Women With Pelvic Organ Prolapse Lara J. Burrows, MD, Leslie A. Meyn, MS, Mark D. Walters, MD, and Anne M. Weber, MD, MS From the Department of Obstetrics, Gynecology, and Reproductive
Quantification of major morphological abnormalities of the levator ani
 Ultrasound Obstet Gynecol 2007; 29: 329 334 Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.3951 Quantification of major morphological abnormalities of the levator
Ultrasound Obstet Gynecol 2007; 29: 329 334 Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.3951 Quantification of major morphological abnormalities of the levator
Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606
 October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
Electroneuromyographic studies
 Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Urinary Incontinence Dr. Leffler
 Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
The Well Woman Centre. Adult Urinary Incontinence
 The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
A Physical Therapist s Perspective
 You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures
 Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Urinary Incontinence in Women. Susan Hingle, M.D. Department of Medicine
 Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
Pelvic Organ Prolapse FAQs
 What is prolapse? Prolapse is a hernia of the vagina that a woman may feel as a bulge or pressure. This is referred to in many different ways, including dropped bladder, dropped uterus, dropped vagina,
What is prolapse? Prolapse is a hernia of the vagina that a woman may feel as a bulge or pressure. This is referred to in many different ways, including dropped bladder, dropped uterus, dropped vagina,
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006
 Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL
 GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
Women suffer in silence
 Women suffer in silence Stress urinary incontinence is the involuntary loss of urine resulting from increased intra-abdominal pressure. In people who suffer with this condition, forms of exertion such
Women suffer in silence Stress urinary incontinence is the involuntary loss of urine resulting from increased intra-abdominal pressure. In people who suffer with this condition, forms of exertion such
Prevention & Treatment of De Novo Stress Incontinence after POP. Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX.
 Prevention & Treatment of De Novo Stress Incontinence after POP Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX Surgery Presenter Disclosure No Conflict of Interest to disclose No Financial
Prevention & Treatment of De Novo Stress Incontinence after POP Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX Surgery Presenter Disclosure No Conflict of Interest to disclose No Financial
Pelvic Anatomy. Robert E. Gutman, MD
 Pelvic Anatomy Robert E. Gutman, MD Objectives Understand pelvic anatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony
Pelvic Anatomy Robert E. Gutman, MD Objectives Understand pelvic anatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony
Preconceptional counseling of women with previous third and fourth degree perineal tears
 20 Preconceptional counseling of women with previous third and fourth degree perineal tears Maria Memtsa and Wai Yoong INTRODUCTION More than 85% of women in the United Kingdom (UK) sustain some form of
20 Preconceptional counseling of women with previous third and fourth degree perineal tears Maria Memtsa and Wai Yoong INTRODUCTION More than 85% of women in the United Kingdom (UK) sustain some form of
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Longitudinal Changes in Overactive Bladder and Stress Incontinence Among Parous Women
 Neurourology and Urodynamics Longitudinal Changes in Overactive Bladder and Stress Incontinence Among Parous Women Victoria L. Handa, 1 * Christopher B. Pierce, 2 Alvaro Mu~noz, 2 and Joan L. Blomquist
Neurourology and Urodynamics Longitudinal Changes in Overactive Bladder and Stress Incontinence Among Parous Women Victoria L. Handa, 1 * Christopher B. Pierce, 2 Alvaro Mu~noz, 2 and Joan L. Blomquist
Fecal incontinence (Encopresis) It is the fecal incontinence condition observed in children with chronic constipation over 1-2 years.
 WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
PROLAPSE WHAT IS A VAGINAL (OR PELVIC ORGAN) PROLAPSE? WHAT ARE THE SIGNS OF PROLAPSE?
 WHAT IS A VAGINAL (OR PELVIC ORGAN)? Your pelvic organs include your bladder, uterus (womb) and rectum (back passage). These organs are held in place by tissues called fascia and ligaments. These tissues
WHAT IS A VAGINAL (OR PELVIC ORGAN)? Your pelvic organs include your bladder, uterus (womb) and rectum (back passage). These organs are held in place by tissues called fascia and ligaments. These tissues
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Intrapartum & Postpartum Bladder Management
 Intrapartum & Postpartum Bladder Management Nothing to disclose Sharon K Knight, MD Overview Intrapartum & Postpartum Bladder Management Literature, available guide lines Fluid status, Avoid injury, UTI
Intrapartum & Postpartum Bladder Management Nothing to disclose Sharon K Knight, MD Overview Intrapartum & Postpartum Bladder Management Literature, available guide lines Fluid status, Avoid injury, UTI
Urinary Incontinence
 Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
in 1996 by the Agency for Health Care Policy and Research, 13 million Americans are
 Seeking Treatment: What? When? Why? Who? How? & Where? In recent membership surveys, the National Association For Continence (NAFC) was distressed to learn that on average people were waiting years before
Seeking Treatment: What? When? Why? Who? How? & Where? In recent membership surveys, the National Association For Continence (NAFC) was distressed to learn that on average people were waiting years before
1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE
 in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
Urinary incontinence during pregnancy
 Urinary incontinence during pregnancy Stian Langeland Wesnes 1,2 MD, Guri Rortveit 2,3 MD PhD, Kari Bø 4 PT PhD, Steinar Hunskaar 2 MD PhD Bergen, Norway From 1 Department of medicine, Haugesund Hospital,
Urinary incontinence during pregnancy Stian Langeland Wesnes 1,2 MD, Guri Rortveit 2,3 MD PhD, Kari Bø 4 PT PhD, Steinar Hunskaar 2 MD PhD Bergen, Norway From 1 Department of medicine, Haugesund Hospital,
Stress Urinary Incontinence Parous Versus Nulliparous Women Ages 18-35
 Grand Valley State University ScholarWorks@GVSU Masters Theses Graduate Research and Creative Practice 2000 Stress Urinary Incontinence Parous Versus Nulliparous Women Ages 18-35 Lisa Stoner Grand Valley
Grand Valley State University ScholarWorks@GVSU Masters Theses Graduate Research and Creative Practice 2000 Stress Urinary Incontinence Parous Versus Nulliparous Women Ages 18-35 Lisa Stoner Grand Valley
Management of Neurogenic Bladder Disorders
 Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear
 Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
FEMALE INCONTINENCE REVIEW
 200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
Female Urinary Incontinence
 Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
Bladder and Pelvic Health
 A Woman s Guide to Bladder and Pelvic Health Symptoms Tests Conditions Treatments 937-277-8988 1-888-808-1016 Dayton Center Englewood Center Huber Heights Center Trotwood Satellite Table of Contents About
A Woman s Guide to Bladder and Pelvic Health Symptoms Tests Conditions Treatments 937-277-8988 1-888-808-1016 Dayton Center Englewood Center Huber Heights Center Trotwood Satellite Table of Contents About
Ask the Expert - Answers
 Ask the Expert - Answers Q. I had a hysterectomy four years ago. Since then, I have been experiencing progressively increasing urgency. I drink one XL cup of coffee per day but when I have to go, I have
Ask the Expert - Answers Q. I had a hysterectomy four years ago. Since then, I have been experiencing progressively increasing urgency. I drink one XL cup of coffee per day but when I have to go, I have
An Operation for Stress Incontinence. Tension Free Vaginal Tape - TVT (Retropubic tape)
 An Operation for Stress Incontinence Tension Free Vaginal Tape - TVT (Retropubic tape) Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together
An Operation for Stress Incontinence Tension Free Vaginal Tape - TVT (Retropubic tape) Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together
SOGC Recommendations for Urinary Incontinence
 The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
EVALUATION OF URINARY INCONTINENCE IN WOMEN
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (2): 165-170, March - April, 2001 EVALUATION OF URINARY INCONTINENCE IN WOMEN STEVEN P. PETROU,
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 27 (2): 165-170, March - April, 2001 EVALUATION OF URINARY INCONTINENCE IN WOMEN STEVEN P. PETROU,
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
I can t empty my rectum without pressing my fingers in or near my vagina
 Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
PHYSICIAN / HEALTH CARE PROVIDER POCKET GUIDE. Stress Urinary Incontinence
 PHYSICIAN / HEALTH CARE PROVIDER POCKET GUIDE Stress Urinary Incontinence 1 in 3 women experience Stress Urinary Incontinence. This pocket guide is intended as a resource for physicians on the complex
PHYSICIAN / HEALTH CARE PROVIDER POCKET GUIDE Stress Urinary Incontinence 1 in 3 women experience Stress Urinary Incontinence. This pocket guide is intended as a resource for physicians on the complex
1 in 3 women experience Stress Urinary Incontinence.
 A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
COMPLICATIONS OF FISTULA REPAIR SURGERY. Sherif Mourad
 COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
FEMALE ANATOMY. the Functions of the Female Organs
 FEMALE ANATOMY the Functions of the Female Organs An educational video for every woman who is told she needs pelvic surgery, including exploratory surgery or removal of the uterus, fallopian tubes, or
FEMALE ANATOMY the Functions of the Female Organs An educational video for every woman who is told she needs pelvic surgery, including exploratory surgery or removal of the uterus, fallopian tubes, or
Antenatal perineal massage. Information for women
 Antenatal perineal massage Information for women Research has shown that antenatal perineal massage from approximately 35 weeks gestation reduces the likelihood of perineal trauma that needs stitching.
Antenatal perineal massage Information for women Research has shown that antenatal perineal massage from approximately 35 weeks gestation reduces the likelihood of perineal trauma that needs stitching.
287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org. 287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org
 Urogynecology Services at the Bladder Control Center 287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org 287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org Table of Contents What is a Urogynecologist?...........................
Urogynecology Services at the Bladder Control Center 287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org 287 Main Street Plaza, Lewiston 207 795-2121 www.cmmc.org Table of Contents What is a Urogynecologist?...........................
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
NHS Professionals. CG8 Guidelines for Continence and Catheter Care. Introduction
 NHS Professionals CG8 Guidelines for Continence and Catheter Care Introduction Continence has been defined as control of bladder and bowel function and continence care is the name given to the total care
NHS Professionals CG8 Guidelines for Continence and Catheter Care Introduction Continence has been defined as control of bladder and bowel function and continence care is the name given to the total care
Information for patients. Sex and Incontinence. Royal Hallamshire Hospital
 Information for patients Sex and Incontinence Royal Hallamshire Hospital Why is sex important? We may choose to be sexual, regardless of our age, physical status or stage of life. Those with health problems
Information for patients Sex and Incontinence Royal Hallamshire Hospital Why is sex important? We may choose to be sexual, regardless of our age, physical status or stage of life. Those with health problems
Understanding Chronic Pelvic Pain : The Role of Physical Therapy in Pelvic Floor Health. Heather Moky P.T., D.P.T
 Understanding Chronic Pelvic Pain : The Role of Physical Therapy in Pelvic Floor Health Heather Moky P.T., D.P.T Disclosures No true disclosures Work for UIC Medical Center- Program Coordinator for the
Understanding Chronic Pelvic Pain : The Role of Physical Therapy in Pelvic Floor Health Heather Moky P.T., D.P.T Disclosures No true disclosures Work for UIC Medical Center- Program Coordinator for the
TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION
 TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION PRESENTED BY: THE PINKERTON LAW FIRM, PLLC The Pinkerton Law Firm is located in Houston, Texas. The firm specializes in mass tort litigation, including
TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION PRESENTED BY: THE PINKERTON LAW FIRM, PLLC The Pinkerton Law Firm is located in Houston, Texas. The firm specializes in mass tort litigation, including
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Prolapse of the Uterus, Bladder, Bowel, or Rectum
 Prolapse of the Uterus, Bladder, Bowel, or Rectum Broad bands of uterine ligaments provide structural support to the uterus and pelvis. The uterine ligaments may weaken, stretch, or spontaneously become
Prolapse of the Uterus, Bladder, Bowel, or Rectum Broad bands of uterine ligaments provide structural support to the uterus and pelvis. The uterine ligaments may weaken, stretch, or spontaneously become
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Many physicians are unaware that fecal incontinence
 Mayo Clin Proc, March 2002, Vol 77 Fecal Incontinence 271 Concise Review for Clinicians A Practical Guide to the Diagnosis and Management of Fecal Incontinence WILLIAM RUDOLPH, MD, AND SUSAN GALANDIUK,
Mayo Clin Proc, March 2002, Vol 77 Fecal Incontinence 271 Concise Review for Clinicians A Practical Guide to the Diagnosis and Management of Fecal Incontinence WILLIAM RUDOLPH, MD, AND SUSAN GALANDIUK,
Stress incontinence. Supported by an unrestricted grant from
 Stress incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing conservative therapies
Stress incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing conservative therapies
Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
Guide to Pregnancy and Birth Injury Claims
 Being pregnant, especially for the first time can be a very daunting experience where you often have to put all of your faith in your midwife or doctor. The majority of pregnancies and births occur without
Being pregnant, especially for the first time can be a very daunting experience where you often have to put all of your faith in your midwife or doctor. The majority of pregnancies and births occur without
Treatment for Stress Incontinence Patient Decision Aid
 Treatment for Stress Incontinence Patient Decision Aid Patient Information Author ID: JD/NS Leaflet Number: Gyn 056 Version: 1 Name of Leaflet: Treatment for stress incontinence - Patient decision aid
Treatment for Stress Incontinence Patient Decision Aid Patient Information Author ID: JD/NS Leaflet Number: Gyn 056 Version: 1 Name of Leaflet: Treatment for stress incontinence - Patient decision aid
Urodynamics in Neuro-Urology
 Urodynamics in Neuro-Urology R Hamid MD (Res), FRCS (Urol) Consultant Urologist London Spinal Injuries Unit, Stanmore & University College London Hospitals Micturition Micturition can be visualized as
Urodynamics in Neuro-Urology R Hamid MD (Res), FRCS (Urol) Consultant Urologist London Spinal Injuries Unit, Stanmore & University College London Hospitals Micturition Micturition can be visualized as
Migration of an intrauterine contraceptive device to the sigmoid colon: a case report
 The European Journal of Contraception and Reproductive Health Care 2003;8:229 232 Case Report Migration of an intrauterine contraceptive device to the sigmoid colon: a case report Ü. S. nceboz, H. T. Özçakir,
The European Journal of Contraception and Reproductive Health Care 2003;8:229 232 Case Report Migration of an intrauterine contraceptive device to the sigmoid colon: a case report Ü. S. nceboz, H. T. Özçakir,
Urinary Incontinence 9/17/2015. Conflict of Interest. Objectives. None
 Urinary Incontinence Karla Reinhart DNP, FNP-C, ARNP October, 2015 Conflict of Interest None Objectives Acquire knowledge of A & P of micturition, as well as pertinent pathologies for male and female incontinence
Urinary Incontinence Karla Reinhart DNP, FNP-C, ARNP October, 2015 Conflict of Interest None Objectives Acquire knowledge of A & P of micturition, as well as pertinent pathologies for male and female incontinence
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence after Vaginal Delivery or Cesarean Section
 The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom
 British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
Prolonged Second Stage of Labor and Levator Ani Muscle Injuries
 Global Journal of Health Science; Vol. 7, No. 1; 2015 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Prolonged Second Stage of Labor and Levator Ani Muscle Injuries
Global Journal of Health Science; Vol. 7, No. 1; 2015 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Prolonged Second Stage of Labor and Levator Ani Muscle Injuries
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
Normal bladder function. Aging of the bladder and urethra
 SECTION 10 Bladder and bowel control (continence) Section overview This section looks at: Normal bladder function Stroke and loss of bladder control (incontinence) Normal bowel function Stroke and bowel
SECTION 10 Bladder and bowel control (continence) Section overview This section looks at: Normal bladder function Stroke and loss of bladder control (incontinence) Normal bowel function Stroke and bowel
An illustrated guide to the management of incontinence.
 An illustrated guide to the management of incontinence. 1 The problem of incontinence The ACA describes incontinence as an involuntary loss of urine and/or bowel motion. The amount can vary from slight
An illustrated guide to the management of incontinence. 1 The problem of incontinence The ACA describes incontinence as an involuntary loss of urine and/or bowel motion. The amount can vary from slight
