The Growing Role of Bariatric Surgery in the Management of Type 2 Diabetes: Evidences and Open Questions
|
|
|
- Augustus Lester
- 8 years ago
- Views:
Transcription
1 DOI /s REVIEW The Growing Role of Bariatric Surgery in the Management of Type 2 Diabetes: Evidences and Open Questions Luca Busetto & Paolo Sbraccia & Lucia Frittitta & Antonio E. Pontiroli # Springer Science+Business Media, LLC 2011 L. Busetto Unità Bariatrica, Dipartimento di Scienze Mediche e Chirurgiche, Università degli Studi di Padova, Padova, Italy P. Sbraccia Dipartimento di Medicina Interna, Università di Roma Tor Vergata, Rome, Italy L. Frittitta Unità di Endocrinologia, Dipartimento di Biomedicina Clinica e Molecolare, Università di Catania, Ospedale Garibaldi, Catania, Italy A. E. Pontiroli Dipartimento di Medicina, Chirurgia e Odontoiatria, Università degli Studi di Milano, Ospedale San Paolo, Milan, Italy L. Busetto (*) Clinica Medica I, Policlinico Universitario, Via Giustiniani 2, Padova, Italy luca.busetto@unipd.it Abstract The use of bariatric surgery in the clinical management of type 2 diabetes has been recently endorsed in the clinical practice recommendations released by the most influential diabetologic associations. However, authoritative critic voices about the application of metabolic surgery in type 2 diabetes continue to appear in diabetologic literature. In this review, we will try therefore to understand what the reasons for this apparent dichotomy. In this paper, we revised what we believe are now clear evidences about the role of bariatric surgery in the treatment of type 2 diabetes in patients with morbid obesity: the efficacy of bariatric surgery in metabolic control, the existence of plausible weight-independent metabolic mechanisms at least in some bariatric procedure, and the importance of the early referral to surgery in patients with firm indications. However, we stressed also the lack of clear high-quality long-term data about the effects of bariatric surgery in the prevention of both macro- and microvascular hard endpoints in patients with type 2 diabetes. The accrual of these results will be critical to completely clarify the risk/benefit ratio of bariatric surgery in diabetes, as compared to current pharmacologic therapies. This may be particularly important in patients in which data on longterm efficacy are still not completed, such as in patients with lower BMI levels. Keywords Bariatric surgery. Metabolic surgery. Type 2 diabetes Introduction Since the pioneering reports of the last decade of twentieth century [1, 2], the efficacy of bariatric procedures in improving and even normalizing glucose levels in obese patients with type 2 diabetes has been confirmed by a large number of observational studies [3]. Prospective controlled observations [4, 5] and one small randomized controlled trial [6] more recently provided higher level scientific evidences about the beneficial effects of bariatric surgery on the long-term metabolic control in type 2 diabetic obese patients. The availability of these evidences ultimately convinced the most influential scientific associations in the field to introduce for the first time the use of bariatric surgery in the mainstream of the clinical management of type 2 diabetes [7]. A wider application of these recommendations in the general clinical practice now depends on several factors: availability of technical and economic
2 resources, health care systems organization, and, least but not last, the willingness of diabetologists and general practitioners to ask bariatric surgeons to treat their obese patients with diabetes. How we can increase this willingness? What steps forward are needed to further convince the general medical community and health care policy makers of the usefulness of bariatric surgery in type 2 diabetes management? In this review, we will briefly review the evidences that now we have about the effectiveness and mechanism of actions of bariatric surgery in morbid obese patients with type 2 diabetes. A more detailed discussion will be dedicated to the still open clinical questions that we consider critical in determining the complete acceptation of bariatric surgery by the diabetologic and general medical community. Finally, a brief session will be reserved to the possible use of metabolic surgery in non-morbid obese patients. Bariatric Surgery in Morbid Obese Diabetic Patients: The Evidences Numerous clinical studies showed the benefits of bariatric surgery on diabetes. A systematic review and meta-analysis of these studies has been recently provided by Buchwald et al. [3]. The objective of the review was to specifically determine the impact of bariatric surgery on body weight and type 2 diabetes. The dataset included 621 studies with 888 treatment arms and 135,246 patients. Meta-analysis of weight loss overall was 38.5 kg or 55.9% excess body weight loss. Overall, 78.1% of diabetic patients had complete resolution, and diabetes was improved or resolved in 86.6% of patients. Weight and diabetes parameters showed little differences in studies with less than 2 years or more than 2 years of follow-up [3]. The robustness of these estimations may be reduced by the acknowledgment that the large majority of the studies included in the review are observational retrospective not randomized studies without appropriate control groups [8]. However, the results of the few published long-term controlled trials seem to confirm this favorable picture. The Swedish Obese Subjects (SOS) Study was launched in the early 1990s with the aim of to prospectively evaluate total and cause-specific 10-years mortality in a large group of morbid obese patients treated by several types of bariatric procedures [4]. A well-matched group of highly comparable morbid obese patients participating in a national obese registry and not willing to undergo surgery was used as a control group. Weight loss observed in the surgical arm of the SOS study was 23.4% of baseline body weight 2 years after surgery and 16.3% 10 years after surgery. In the same time, the control group of morbid obese patients treated by conventional medical treatment remained substantially weight stable [4]. In the first 2 years of SOS study, 72% of 342 diabetic surgically treated obese patients had a complete resolution of type 2 diabetes, while only 21% of 248 diabetic obese controls did so. The odds ratio for being free from type 2 diabetes 2 years after surgery was 8.42 (95% CI, ) in the surgically treated as compared with the medically treated controls [4]. In the long-term, some of the benefits observed in the first years after surgery tend to vanish, maybe because of the slight tendency to weight regain observed in the surgical group as a whole and of the aging of the study population. Anyway, the proportion of patients with type 2 diabetes at baseline still normoglycemic without pharmacologic treatment 10 years after surgery was higher in the surgically treated group (36%) than in the control group (13%). The probability of being free from diabetes 10 years after surgery was still 3.45 (95% CI, ) times higher in the surgical group [4]. The sustained weight loss observed in the surgical arm of the SOS study was not only associated to an improvement of the diabetic state, but also to the prevention of new cases of type 2 diabetes in those morbid obese patients free from the disease at baseline. Indeed, the incidence of new cases of type 2 diabetes was 1% in the surgically treated patients and 8% in the control group at 2 years (odds ratio (OR), 0.14; 95% CI, ), and it was 7% and 24%, respectively, at 10 years (OR, 0.25; 95% CI, ) [4]. The surgical induced weight loss seems thus to be able to prevent about 75% of new type 2 diabetes cases over a 10-years follow-up. The results of the SOS study have been confirmed by a smaller prospective study evaluating the outcome of diabetes in 73 morbid obese patients treated by laparoscopic adjustable gastric banding and in 43 eligible morbid obese patients who refused surgery for personal reasons [5]. Form baseline to the end of the 4-year follow-up, BMI decreased from 45±0.89 to 37.7±0.71 kg/m 2 in the gastric banding group and remained steady in the non-surgical group. In patients without type 2 diabetes at baseline, the primary intervention study, 17.2% of the subjects in the control group and none of the gastric banding patients (P= ) progressed to type 2 diabetes. In patients with type 2 diabetes at baseline, the secondary intervention study, type 2 diabetes remitted in 4.0% of the patients in the control group and in 45.0% of the surgically treated patients (P=0.0052) [5]. The first randomized clinical trial comparing bariatric surgery and conventional-therapy in the management of obese patients with type 2 diabetes has been published in 2008 [6]. Dixon et al. randomized 60 patients with BMI ranging from 30 to 40 kg/m 2 and recent type 2 diabetes (less than 2 years from diagnosis) to laparoscopic adjust-
3 able gastric banding or to a program of conventional therapy with a specific focus on weight loss. After a 2- year follow-up, weight loss was 21.1±10.3 kg in the surgical group and 1.5±5.4 kg in the conventional-therapy group (P<0.001). Remission of type 2 diabetes was achieved by 73% of the patients in the surgical group and 13% in the conventional-therapy group. Relative risk of remission for the surgical group was 5.5 (95% CI, ) [6]. Efficacy of bariatric surgery was therefore supported now by high-quality research data. The meta-analysis of Buchwald et al. [3] showed substantial differences in the efficacy of different bariatric procedures in metabolic control. Diabetes resolution was greatest for patients undergoing biliopancreatic diversion/ duodenal switch (95.1% resolved), followed by gastric bypass (80.3%), gastroplasty (79.7%), and then laparoscopic adjustable gastric banding (56.7%). These differences in metabolic efficacy were paralleled by differences in weight loss efficacy. By simply putting in a simple correlation, the percentage of excess weight loss and the percentage of diabetes resolution reported by Buchwald et al. for the different procedures (Fig. 1), we may obtain a linear regression line with a R 2 of 0.949, thus implying that 95% of the variability in diabetes resolution may be explained by variations in weight loss. However, even a strong statistical association does not imply automatically a direct causal relationship: the association may be well explained by the existence of other factors having an independent effect on both metabolic control and weight loss. Potential mechanisms underlying the direct antidiabetic impact of metabolic procedures, gastric bypass in particular, have been recently reviewed [8] and their detailed description is beyond the scopes of this paper. Briefly, the existence of procedure-related factors that are able to have a weight loss-independent effect on the Fig. 1 Linear regression analysis between percentage of excess weight loss and the percentage of diabetes resolution after bariatric surgery. The data reported in the meta-analysis of Buchwald et al. [3] are used. LAGB laparoscopic gastric banding, VBG vertical banded gastroplasty, RYGB gastric bypass, BPD-DS biliopancreatic diversion/ duodenal switch control of diabetes is supported by at least three lines of evidence [9]: 1. Glycemic control often occurs within days after gastric bypass, long before significant weight loss was achieved [1, 10, 11]. 2. Glucose control improves more after gastric bypass than with equivalent weight loss obtained by dietary intervention [12] or pure restrictive bariatric procedures [13, 14]. 3. The occurrence of cases of hyperinsulinemic hypoglycemia related to pancreatic islets hyperplasia or nesidioblastosis long term after gastric bypass [15], but not after pure restrictive surgery. Several plausible hypotheses have been articulated to explain the weight-independent effects of metabolic procedures [9]. The two most popular ones were both related to changes in the secretion of intestinal peptides involved in glucose homeostasis and energy balance regulation [16]. The hindgut or lower intestinal hypothesis holds that diabetes control results from the expedited delivery of nutrients to the distal intestine, enhancing the secretion of physiologic mediators able to improve glucose metabolism. Potential candidates are glucagon-like peptide 1 and peptide YY. Both of these hormones have been found to be substantially and durably increased after gastric bypass, but not after gastric banding [14]. According to the foregut or higher intestinal hypothesis, the effect of selected bariatric procedures on glucose metabolism depends on the exclusion of the duodenum and proximal jejunum from the transit of nutrients, possibly preventing the secretion of some yet unknown molecule promoting glucose intolerance [16]. Besides hindgut and foregut hypotheses, several other intestinal mechanisms may play a role: suppression of ghrelin secretion [17], alterations of intestinal nutrient sensing [9], and perturbations of gut microbiota [18]. Furthermore, plausible explanations may be found also out of gastrointestinal tract: in biliopancreatic diversion, the malabsorption of fat is typically associated to a highly significant reduction of the plasma triglycerides levels both in the fasting and in the postprandial states [19]. Reduction in lipid overload has been found to be associated to a reduced fat deposition in skeletal muscle. Intra-myocellular fat deposition is associated to a reduced glucose uptake and utilization, a clear metabolic marker of insulin-resistance. Indeed, in patients treated with biliopancreatic diversion the improvement of insulin sensitivity after surgery was more strictly associated to the reduction of the muscle lipid content than to the fat mass loss [19]. In summary, several hypotheses remain in the field and probably others will appear in the future. Neither of them is mutually exclusive and probably they may have a different importance in different clinical situations or after different surgical techniques.
4 Even by using the most metabolically effective procedure, still some diabetic patients remain to not achieve diabetes remission or improvement after surgery. Several factors have been proposed as positive or negative predictors of diabetes remission, but the more consistent one was diabetes duration. A shorter history of diabetes has been found to be associated to a greater chance of diabetes remission after any type of bariatric procedure [20, 21]. This latter observation may be expected, given that progressive deterioration of β-cell function driven the progression from glucose intolerance to overt hyperglycemia. If the bariatric procedure is performed before irreversible β-cell failure has occurred, then a higher likelihood of long-term remission may be expected. The importance of considering bariatric surgery early in the course of the disease in morbid obese patients with type 2 diabetes has been recently endorsed in a recent position statement on bariatric surgical and procedural interventions in the treatment of obese patients with type 2 diabetes from the International Diabetes Federation Taskforce on Epidemiology and Prevention [22]. Open Question About the Use of Bariatric Surgery in Morbid Obese Diabetic Patients In the first part of this manuscript, we revised what we believe are now clear evidences about the role of bariatric surgery in the treatment of type 2 diabetes in patients with morbid obesity: the efficacy of bariatric surgery in metabolic control, the existence of plausible weightindependent metabolic mechanisms at least in some bariatric procedure, and the importance of the early referral to surgery in patients with firm indications. However, authoritative critic voices about the application of metabolic surgery in type 2 diabetes continue to appear in diabetologic literature [23, 24]. In this second paper of our review, we will try therefore to understand what the reasons for this apparent dichotomy. Bariatric literature usually presents results in terms of rate of diabetes cure or remission, usually defined as the normalization of glucose levels in the absence of active anti-diabetic therapy [3]. This definition has been recently endorsed by a consensus group comprising experts in pediatric and adult endocrinology, diabetes education, transplantation, metabolism, and bariatric/metabolic surgery [25]. In analogy to the oncologic literature, where cure is defined as complete remission of cancer of sufficient duration that the future risk of recurrence is felt to be very low, experts agreed that it may make sense, on a practical ground, to consider prolonged (arbitrarily 5 years) remission of diabetes essentially equivalent to cure. Since the definition of complete diabetes remission required the absence of active pharmacologic therapy, prolonged remission may not be achieved by pharmacology therapy itself [25]. On the other hand, diabetologists and the medical community are used to compare anti-diabetic therapy in terms of metabolic control: how many patients reach therapeutic target with a specific treatment? For how many months I may be able to maintain my patients in metabolic control by using a specific drug or combination of several drugs? It may be difficult to compare these two very different outcomes. In practical terms, it is better for my patient to be in metabolic control for some years by taking three or four pills per day or it is better to be in complete remission without any anti-diabetic drugs, but facing the risks and side effects of a given bariatric procedure? An evidence-based answer probably relies on the appreciation of the number of hard diabetes-related endpoints that may be prevented by each of the two strategies (macro and micro-vascular complications and deaths). However, we lack at this moment comparable data on this crucial point. Bariatric surgeons usually focused the presentation of their results in patients with type 2 diabetes on normalization of glucose levels, without a specific attention to other cardiovascular risk factors and rates of macro and microvascular events [3]. Classic data from the UK Prospective Diabetes Study (UKPDS) demonstrated that the rates of both cardiovascular events (myocardial infarctions) and micro-vascular complications (diabetic retinopathy and nephropathy) are directly related to glycemic control (glycated hemoglobin or HbA1c levels) [26]. However, the strength of the association is not equal for the two groups of diabetes-related outcomes. By classifying patients according to their exposure to increasingly higher glycemic levels, UKPDS investigators calculated that a 1% reduction in HbA1c levels should be associated to a 37% decrease in the incidence of micro-vascular endpoints and to only a 14% decrease in the incidence of fatal and non-fatal myocardial infarction [26]. This estimation was confirmed by the results of the UKPDS prospective randomized trial [27]. Over a 10-year follow-up, patients in the intensive blood glucose control group (HbA1c levels 7.0%) as compared to patients in the conventional treatment group (HbA1c levels 7.9%) had a significant 25% risk reduction in micro-vascular endpoints (RR, 0.75; 95% CI, ) and a non-significant 16% risk reduction in myocardial infarction (RR, 0.84; 95% CI, )[27]; an additional 10-years follow-up was needed in order to reach statistical significance in the risk reduction for myocardial infarction [28]. A recent meta-analysis of five randomized clinical trials aimed at the assessment of the efficacy of lowering blood glucose [28 32] confirmed a significant but moderate effect of intensive glucose control on myocardial infarction rate (overall odds ratio, 0.849; 95% CI, ) [33]. On the other hand, one small randomized trial tested the
5 efficacy of a broader, targeted, intensified, multi-factorial intervention in patients with type 2 diabetes [34]. In the Steno-2 trial, 160 patients were randomly assigned to receive either conventional treatment in accordance with standard guidelines or intensive treatment, with a multifactorial stepwise implementation of behavior modification and pharmacologic therapy that targeted at the same time hyperglycemia, hypertension, dyslipidemia, and microalbuminuria, along with secondary prevention of cardiovascular disease with aspirin. The decline in glycosylated hemoglobin values, systolic and diastolic blood pressure, serum cholesterol and triglyceride levels, and urinary albumin excretion rate were all significantly greater in the intensivetherapy group than in the conventional-therapy group. At the end of a 4-year follow-up, patients receiving intensive therapy had an impressive 50% reduction in cardiovascular events (OR, 0.47; 95% CI, ), along with large reduction in the rates of nephropathy (OR, 0.39; 95% CI, ), retinopathy (OR, 0.42; 95% CI, ), and autonomic neuropathy (OR, 0.37; 95% CI, ) [34]. A reduction in total mortality (OR, 0.54; 95% CI, ) and mortality from cardiovascular causes (OR, 0.43; 95% CI, ) was observed after a prolonged follow-up period [35]. Sustained weight loss produced by bariatric surgery in patients with type 2 diabetes may probably induce an improvement in cardiovascular risk factors well beyond pure glycemic control and therefore may enable a reduction of micro- and particularly macrovascular endpoints more similar to those achieved by multifactorial intervention than by simple intensive glucose control. However, reduction of global cardiovascular risk was seldom appreciable in bariatric reports and no data about the reduction of micro- and macro-vascular events after bariatric procedures in patients with type 2 diabetes are as yet available. Intensive glycemic control is not without risks. In the Action to Control Cardiovascular Risk in Diabetes (AC- CORD) trial, patients in the intensive control group achieved and maintained a 6.4% HbA1c levels whereas patients in the standard therapy group had a mean 7.5% HbA1c level [29]. Intensive glucose control was associated with a small reduction in non-fatal myocardial infarction rates (OR, 0.76; 95% CI, ). However, both deaths for any cause (OR, 1.22; 95% CI, ) and cardiovascular deaths (OR, 1.35; 95% CI, ) were more frequent in the intensive control group than in the standard therapy group [29]. A recent retrospective analysis of a large cohort of type 2 diabetics confirmed the existence of a U-shaped association between HbA1c levels and total mortality [36]. Both in patients treated with oral hypoglycemic agents and in insulin-treated patients, the lowest mortality risk was observed in patients with 7.5% HbA1c levels, and increase mortality rates were observed both at higher than lower HbA1c values [36]. The increase in total mortality observed in the ACCORD trial has been related to the higher frequency of severe episodes of hypoglycemia observed in the intensive control group [33]. Hypoglycemia seldom represents a problem after some of the bariatric procedures [15] and we do not intend to suggest that hypoglycemic events after surgery may per se reduce substantially the benefits of bariatric surgery in patients with type 2 diabetes. However, the key message coming from the ACCORD study was that, beyond certain limits, the benefits of tight metabolic control on cardiovascular risk are so small that they may be overcome by unexpected and also unrelated side effects. This message should be taken into account when we propose the use of bariatric surgery in patients with type 2 diabetes, particularly in patients with not so bad glucose control and at a lower BMI level. Are we sure that the benefits will not be overcome by the side effects induced by the procedures? Still again, more data about hard endpoints are needed. Bariatric Surgery in Non-Morbid Obese Diabetic Patients: The First Steps The recognition that several bariatric procedures may exert some weight loss-independent metabolic effects suggests that metabolic surgery may be beneficial also in diabetic patients with less severe degree of obesity, or even in simply overweight type 2 diabetics. This new frontier of metabolic surgery includes the application of conventional bariatric procedures to patients with lower BMI levels (BMI or kg/m 2 ) and the introduction of new procedures, like ileal interposition and duodenal jejunum exclusion, designed with the specific aim of having metabolic effects irrespective of causing massive weight loss. The results of metabolic surgery in patients with type 2 diabetes and BMI <35 kg/m 2 has been recently reviewed [37]. The dataset included 16 studies and 343 patients with type 2 diabetes treated with restrictive (three studies), malabsorptive/restrictive (five studies), and primarily malabsorptive procedures (eight studies). In the whole sample, 85.3% of patients experienced diabetes resolution, defined as the number of patients not taking any anti-diabetic medications, in a relatively short follow-up (mean followup 23 months, range months). Similarly to what was observed in morbid obese patients, the rate of diabetes resolution was graded according to the type of procedure (72.2% in restrictive, 97.7 in malabsorptive/restrictive, and 72.9 in malabsorptive procedures). When patients were divided according to baseline BMI levels in obese (BMI kg/m 2 ) and overweight (BMI kg/m 2 ) groups, a tendency to a lower effect of metabolic surgery at lower
6 BMI levels was observed. Rates of remission were 89.1% in the obese group and 81.8% in the overweight group [37]. This tendency has been recently confirmed by Scopinaro et al. [38] in a prospective study conducted with DBP in 15 obese (BMI kg/m 2 ) and 15 overweight (BMI kg/m 2 ) patients. The lower efficacy of metabolic surgery in patients with lower BMI has been attributed to the presence of a more advanced, severe, and less responsive disease [38] or to the unrecognized inclusion of patients with late onset type 1 diabetes (LADA) [37]. In summary, the results of metabolic surgery published so far seem to be promising in non-morbid obese patients and less brilliant in overweight patients with type 2 diabetes. Any definitive conclusion is tempered by the fact that we still have very few studies conducted in small numbers of patients and sometimes in patients with peculiar ethnic backgrounds (Chinese and Indian patients in particular) [37]. Moreover, the general considerations about longterm risk/benefit ratio that we exposed for morbid obese patients are obviously applicable, and even reinforced, in patients with lower BMI levels. In this particular group of patients, an additional problem may be represented by the excessive and harmful weight loss that may be produced by the application of some of the bariatric procedures in patients with less severe obesity. In the 2009 Standards of medical care in diabetes, experts from the American Diabetes Association concluded that although small trials have shown glycemic benefit of bariatric surgery in patients with type 2 diabetes and BMI kg/m 2, current evidence was insufficient to generally recommend surgery in patients with BMI<35 kg/m 2 outside of a research protocol [7]. An initial opening to a wider application of bariatric surgery at lower BMI levels has been recently endorsed by the International Diabetes Federation Taskforce on Epidemiology and Prevention [22]. Position statement from IDF suggests that patients with kg/m 2 and type 2 diabetes may be conditionally considered eligible for surgery in case of HbA1c levels>7.5 despite fully optimized conventional-therapy, especially if weight is increasing, or other weight responsive comorbidities not achieving targets on conventional therapies (for example blood pressure, dyslipidemia, and obstructive sleep apnoea) [22]. The sue of metabolic surgery in simply overweight patients remains in our opinion purely experimental and should be performed only in an adequately designed trial under strict institutional monitoring. Conclusion In conclusion, bariatric surgery has been accepted as a reasonable option for the treatment of patients with type 2 diabetes and obesity. The acceptance of and the willingness to use this possibility among diabetologic and internal medicine community needs to be bolstered. Research is now focused on the pathophysiologic mechanisms that may explain the effects of bariatric procedures, on the clinical factors that may predict diabetes remission after surgery, on the development of new procedures specifically tailored for type 2 diabetes control, and on the possible effects of metabolic surgery in type 2 non-obese diabetics. All these studies are certainly interesting and will hopefully open new and exciting therapeutic possibilities. However, we believe that a key point still missing remains: the production of high-level controlled trials evaluating the net benefit of bariatric surgery in the prevention of both macro- and micro-vascular hard endpoints specifically in patients with type 2 diabetes. References 1. Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult onset diabetes mellitus. Ann Surg. 1995;222: MacDonald KG, Long SD, Swanson MS, et al. The gastric bypass operation reduces the progression and mortality of non-insulindependent diabetes mellitus. J Gastrointest Surg. 1997;1: Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and metaanalysis. Am J Med. 2009;122: Sjöström L, Lindroos A-K, Peltonen M, et al. Lifestyle, diabetes and cardiovascular risk factors 10 years after bariatric surgery. N Eng J Med. 2004;351: Pontiroli AE, Folli F, Paganelli M, et al. Laparoscopic gastric banding prevents type 2 diabetes and arterial hypertension and induces their remission in morbid obesity. A 4-year casecontrolled study. Diabetes Care. 2005;28: Dixon JB, O'Brien PE, Playfair J, et al. Adjustable gastric banding and conventional therapy for type 2 diabetes. A randomized controlled trial. JAMA. 2008;299: Executive Summary: Standards of medical care in diabetes Diabetes Care 2009;32:S Chipkin SR, Goldberg RJ. Obesity surgery and diabetes: does a chance to cut mean a chance to cure? Am J Med. 2009;122: Thaler JP, Cummings DE. Minireview: hormonal and metabolic mechanism of diabetes remission after gastrointestinal surgery. Endocrinol. 2009;150: Shauer PR, Burguera B, Ikramuddin S, et al. Effect of laparoscopic Roux-en Y gastric bypass on type 2 diabetes mellitus. Ann Surg. 2003;238: Rubino F, Gagner M, Gentileschi P, et al. The early effect of the Roux-en-Y gastric bypass on hormones involved in body weight regulations and glucose metabolism. Ann Surg. 2004;240: Laferrere B, Teixeira J, McGinty J, et al. Effect of weight loss by gastric bypass surgery versus hypocaloric diet in glucose and incretin levels in patients with type 2 diabetes. J Clin Endocrinol Metab. 2008;93: Pattou F, Beraud G, Arnalsteen L, et al. Restoration of β-cell function after bariatric surgery in type 2 diabetics: a prospective controlled study comparing gastric banding and gastric bypass. Obes Surg. 2007;17: le Roux CW, Aylwin SJ, Batterham RL, et al. Gut hormone profiles following bariatric surgery favour an anorectic state,
7 facilitate weight loss, and improve metabolic parameters. Ann Surg. 2006;243: Service GJ, Thompson GB, Service FJ, et al. Hyperinsulinemic hypoglycemia with nesidioblastosis after gastric bypass surgery. N Engl J Med. 2005;353: Rubino F, Forgione A, Cummings DE, et al. The mechanism of diabetes control after gastrointestinal bypass surgery reveals a role of the proximal small intestine in the pathophysiology of type 2 diabetes. Ann Surg. 2006;244: Cummings DE, Weigle DS, Frayo RS, et al. Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med. 2002;346: Furet JP, Kong LC, Tap J. Differential adaptation of human gut microbiota to bariatric surgery-induced weight loss: links with metabolic and low-grade inflammation markers. Diabetes. 2010;59: Greco AV, Mingrone G, Giancaterini A, et al. Insulin resistance in morbid obesity. Reversal with intramyocellular fat depletion. Diabetes. 2002;51: Dixon JB, Dixon AF, O'Brien P. Improvements in insulin sensitivity and beta-cell function (HOMA) with weight loss in the severely obese. Diabet Med. 2003;20: Hall TC, Pellen MG, Sedman PC, et al. Preoperative factors predicting remission of type 2 diabetes mellitus after Roux-en-Y gastric bypass surgery for obesity. Obes Surg. 2010;20: IDF. Bariatric surgical and procedural interventions in the treatment of obese patients with type 2 diabetes. A position statement from the International Diabetes Federation Taskforce on Epidemiology and Prevention; Schernthaner G, Kopp H-P, Brix JM, et al. Cure of type 2 diabetes by metabolic surgery? A critical analysis of the evidence in Diabetes Care. 2011;34:S Pinkney JH, Johnson AB, Gale EA. The big fat bariatric bandwagon. Diabetologia. 2010;53: Buse JB, Caprio S, Cefalu WT, et al. How do we define cure of diabetes? Diabetes Care. 2009;32: Stratton IM, Adler AI, Neil AW, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321: UK Prospective Diabetes Study (UKPDS) Group. Intensive blood glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352: Holman RR, Paul SK, Bethel MA, et al. 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med. 2008;359: The Action to Control Cardiovascular Risk in Diabetes Study Group. Effects of intensive glucose lowering in type 2 diabetes. N Eng J Med. 2008;358: The ADVANCE Collaborative Group. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Eng J Med. 2008;358: Dormandy JA, Charbonnel B, Eckland DJA, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive study (PROspectivepioglitAzone Clinical Trial In macrovascular Events): a randomized control trial. Lancet. 2005;366: Duckworth W, Abraira C, Moritz T, et al. Glucose control and vascular complications in veterans with type 2 diabetes. N Eng J Med. 2009;360: Mannucci E, Monami M, Lamanna C, et al. Prevention of cardiovascular disease through glycemic control in type 2 diabetes: a meta-analysis of randomized clinical trials. Nutr Metab Cardiovasc Dis. 2009;19: Gaede P, Vedel P, Larsen N, et al. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Eng J Med. 2003;348: Gaede P, Lund-Andersen H, Parving HH, et al. Effect of multifactorial intervention on mortality in type 2 diabetes. N Engl J Med. 2008;358: Currie CJ, Peters JR, Tynan A, et al. Survival as a function of HbA1c in people with type 2 diabetes: a retrospective cohort study. Lancet. 2010;375: Fried M, Ribaric G, Buchwald JN, et al. Metabolic surgery for the treatment of type 2 diabetes in patients with BMI <35 kg/m 2 : an integrative review of early studies. Obes Surg. 2010;20: Scopinaro N, Adami GF, Papadia FS, et al. The effects of biliopancreatic diversion on type 2 diabetes mellitus in patients with mild obesity (BMI kg/m2) and simple overweight (BMI kg/m2): a prospective controlled study. Obes Surg. 2011;21:880 8.
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery
 The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
Is surgery better? Jordan Kautz, MS IV A b atory are C erence, an 08 08 UNC-CH School of Medicine
 Is surgery better? Bariatric surgery versus medical management in type 2 diabetes mellitus Jordan Kautz, MS IV Ambulatory Care Conference, Jan 08 UNC-CH School of Medicine For the soon-to-be medical resident
Is surgery better? Bariatric surgery versus medical management in type 2 diabetes mellitus Jordan Kautz, MS IV Ambulatory Care Conference, Jan 08 UNC-CH School of Medicine For the soon-to-be medical resident
3 WORKSHOP CONGIUNTO SICOb SID SIO 7 MARZO 2014 L integrazione tra terapia medica e chirurgica nel trattamento del paziente obeso diabetico
 3 WORKSHOP CONGIUNTO SICOb SID SIO 7 MARZO 2014 L integrazione tra terapia medica e chirurgica nel trattamento del paziente obeso diabetico Recidive del diabete dopo terapia chirurgica La quantificazione
3 WORKSHOP CONGIUNTO SICOb SID SIO 7 MARZO 2014 L integrazione tra terapia medica e chirurgica nel trattamento del paziente obeso diabetico Recidive del diabete dopo terapia chirurgica La quantificazione
Bariatric Surgery. OHTAC Recommendation. Bariatric Surgery
 OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx:
 James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
Treatment for Severely Obese Patients
 Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Understanding diabetes Do the recent trials help?
 Understanding diabetes Do the recent trials help? Dr Geoffrey Robb Consultant Physician and Diabetologist CMO RGA UK Services and Partnership Assurance AMUS 25 th March 2010 The security of experience.
Understanding diabetes Do the recent trials help? Dr Geoffrey Robb Consultant Physician and Diabetologist CMO RGA UK Services and Partnership Assurance AMUS 25 th March 2010 The security of experience.
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Roux-en-Y Gastric Bypass
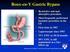 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Cardiovascular Disease in Diabetes
 Cardiovascular Disease in Diabetes Where Do We Stand in 2012? David M. Kendall, MD Distinguished Medical Fellow Lilly Diabetes Associate Professor of Medicine University of MInnesota Disclosure - Duality
Cardiovascular Disease in Diabetes Where Do We Stand in 2012? David M. Kendall, MD Distinguished Medical Fellow Lilly Diabetes Associate Professor of Medicine University of MInnesota Disclosure - Duality
ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Effects of a fixed combination of the ACE inhibitor, perindopril,
ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Effects of a fixed combination of the ACE inhibitor, perindopril,
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes
 Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
EFFICACY OF BARIATRIC SURGERY IN OBESE INDIAN WITH TYPE 2 DIABETES MELLITUS
 EFFICACY OF BARIATRIC SURGERY IN OBESE INDIAN WITH TYPE 2 DIABETES MELLITUS Subodh Banzal, Abhishek Singhai, Mohit Bhandari, Padmnabh Sharma, Rajesh Kumar Jha, Piyush Manoria 1. Associate Professor, DM,
EFFICACY OF BARIATRIC SURGERY IN OBESE INDIAN WITH TYPE 2 DIABETES MELLITUS Subodh Banzal, Abhishek Singhai, Mohit Bhandari, Padmnabh Sharma, Rajesh Kumar Jha, Piyush Manoria 1. Associate Professor, DM,
Diabetes Mellitus. Melissa Meredith M.D. Diabetes Mellitus
 Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
The weight of the world.
 The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
Bariatric Surgery versus Conventional Medical Therapy for Type 2 Diabetes
 original article Bariatric Surgery versus Conventional Medical Therapy for Type 2 Diabetes Geltrude Mingrone, M.D., Simona Panunzi, Ph.D., Andrea De Gaetano, M.D., Ph.D., Caterina Guidone, M.D., Amerigo
original article Bariatric Surgery versus Conventional Medical Therapy for Type 2 Diabetes Geltrude Mingrone, M.D., Simona Panunzi, Ph.D., Andrea De Gaetano, M.D., Ph.D., Caterina Guidone, M.D., Amerigo
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
. 2000 : 2.9 million WORLDWIDE deaths. Diabetes Mortality COST 2007 * Types II Diabetes (T2DM) Type II Diabetes Mellitus: medical or surgical disease?
 Type II Diabetes Mellitus: medical or surgical disease? Conference presented at 4-th National Congress of Romanian Association for Endoscopic Surgery, October 30-th, 2008, Iaşi, Romania Gianfranco Silecchia
Type II Diabetes Mellitus: medical or surgical disease? Conference presented at 4-th National Congress of Romanian Association for Endoscopic Surgery, October 30-th, 2008, Iaşi, Romania Gianfranco Silecchia
嘉 義 長 庚 醫 院 藥 劑 科 Speaker : 翁 玟 雯
 The Clinical Efficacy and Safety of Sodium Glucose Cotransporter-2 (SGLT2) Inhibitors in Adults with Type 2 Diabetes Mellitus 嘉 義 長 庚 醫 院 藥 劑 科 Speaker : 翁 玟 雯 Diabetes Mellitus : A group of diseases characterized
The Clinical Efficacy and Safety of Sodium Glucose Cotransporter-2 (SGLT2) Inhibitors in Adults with Type 2 Diabetes Mellitus 嘉 義 長 庚 醫 院 藥 劑 科 Speaker : 翁 玟 雯 Diabetes Mellitus : A group of diseases characterized
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach
 Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Comparative Studies and Metabolic Effects of Sleeve Gastrectomy
 Comparative Studies and Metabolic Effects of Sleeve Gastrectomy Alfonso Torquati MD, MSCI Associate Professor of Surgery Discosures NIH-NIDDK: grant support Covidien: consulting agreement, grant support
Comparative Studies and Metabolic Effects of Sleeve Gastrectomy Alfonso Torquati MD, MSCI Associate Professor of Surgery Discosures NIH-NIDDK: grant support Covidien: consulting agreement, grant support
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
CASE B1. Newly Diagnosed T2DM in Patient with Prior MI
 Newly Diagnosed T2DM in Patient with Prior MI 1 Our case involves a gentleman with acute myocardial infarction who is newly discovered to have type 2 diabetes. 2 One question is whether anti-hyperglycemic
Newly Diagnosed T2DM in Patient with Prior MI 1 Our case involves a gentleman with acute myocardial infarction who is newly discovered to have type 2 diabetes. 2 One question is whether anti-hyperglycemic
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Weight loss surgery more than just a gastric band
 Weight loss surgery more than just a gastric band Presented by Ms Beth Murgatroyd Honorary Bariatric Nurse Practitioner Mr Ameet G Patel Consultant Surgeon Director of Bariatric Surgery at King s College
Weight loss surgery more than just a gastric band Presented by Ms Beth Murgatroyd Honorary Bariatric Nurse Practitioner Mr Ameet G Patel Consultant Surgeon Director of Bariatric Surgery at King s College
Systematic Literature Review on the Impact of Weight Loss from Adjustable Gastric Banding on Diabetes, Hypertension, and Dyslipidemia
 Systematic Literature Review on the Impact of Weight Loss from Adjustable Gastric Banding on Diabetes, Hypertension, and Dyslipidemia I. Introduction Laparoscopic adjustable gastric banding (LAGB) surgery
Systematic Literature Review on the Impact of Weight Loss from Adjustable Gastric Banding on Diabetes, Hypertension, and Dyslipidemia I. Introduction Laparoscopic adjustable gastric banding (LAGB) surgery
Insulin degludec (Tresiba) for the Management of Diabetes: Effectiveness, Value, and Value-Based Price Benchmarks
 Background: Insulin degludec (Tresiba) for the Management of Diabetes: Effectiveness, Value, and Value-Based Price Benchmarks Final Background and Scope November 19, 2015 The Centers for Disease Control
Background: Insulin degludec (Tresiba) for the Management of Diabetes: Effectiveness, Value, and Value-Based Price Benchmarks Final Background and Scope November 19, 2015 The Centers for Disease Control
The Holy Grail of Bariatric Surgery: Which Patient Should Get What Procedure?
 Jane N. Buchwald Viewpoint Editor The Holy Grail of Bariatric Surgery: Which Patient Should Get What Procedure? Robin Blackstone, MD Scottsdale Bariatric Center, Scottsdale, AZ Patients are looking to
Jane N. Buchwald Viewpoint Editor The Holy Grail of Bariatric Surgery: Which Patient Should Get What Procedure? Robin Blackstone, MD Scottsdale Bariatric Center, Scottsdale, AZ Patients are looking to
Glycemic Control of Type 2 Diabetes Mellitus
 Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Glycemic Control of Type 2 Diabetes Mellitus Majeda Fikree* Baderuldeen Hanafi** Zahra Ali Hussain** Emad M Masuadi*** Objective: To determine the
Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Glycemic Control of Type 2 Diabetes Mellitus Majeda Fikree* Baderuldeen Hanafi** Zahra Ali Hussain** Emad M Masuadi*** Objective: To determine the
Guidelines for the management of hypertension in patients with diabetes mellitus
 Guidelines for the management of hypertension in patients with diabetes mellitus Quick reference guide In the Eastern Mediterranean Region, there has been a rapid increase in the incidence of diabetes
Guidelines for the management of hypertension in patients with diabetes mellitus Quick reference guide In the Eastern Mediterranean Region, there has been a rapid increase in the incidence of diabetes
Sponsor. Novartis Generic Drug Name. Vildagliptin. Therapeutic Area of Trial. Type 2 diabetes. Approved Indication. Investigational.
 Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Vildagliptin Therapeutic Area of Trial Type 2 diabetes Approved Indication Investigational Study Number CLAF237A2386 Title A single-center,
Clinical Trial Results Database Page 1 Sponsor Novartis Generic Drug Name Vildagliptin Therapeutic Area of Trial Type 2 diabetes Approved Indication Investigational Study Number CLAF237A2386 Title A single-center,
Diabetes Complications
 Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
1. PATHOPHYSIOLOGY OF METABOLIC SYNDROME
 1. PATHOPHYSIOLOGY OF METABOLIC SYNDROME Izet Aganović, Tina Dušek Department of Internal Medicine, Division of Endocrinology, University Hospital Center Zagreb, Croatia 1 Introduction The metabolic syndrome
1. PATHOPHYSIOLOGY OF METABOLIC SYNDROME Izet Aganović, Tina Dušek Department of Internal Medicine, Division of Endocrinology, University Hospital Center Zagreb, Croatia 1 Introduction The metabolic syndrome
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Sudbury Bariatric Regional Assessment & Treatment Centre
 Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION. Robert Dobbins, M.D. Ph.D.
 TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study
 DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
Choices Around Bariatric Surgery
 Choices Around Bariatric Surgery What should you know? Richard Stubbs MD FRCS FRACS Wakefield Obesity Clinic, Wellington 152 kg / BMI 59 74 kg / BMI 29 Indications (NIH Consensus Statement 1991) BMI >
Choices Around Bariatric Surgery What should you know? Richard Stubbs MD FRCS FRACS Wakefield Obesity Clinic, Wellington 152 kg / BMI 59 74 kg / BMI 29 Indications (NIH Consensus Statement 1991) BMI >
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
MORTALITY RISK FACTORS IN PATIENTS UNDERGOING GASTRIC BYPASS SURGERY
 Where Do We Stand? Alan M. Brader, MD Lancaster General Bariatrics Introduction The management of a patient with extreme obesity is a challenging task for most health care givers. Unfortunately, there
Where Do We Stand? Alan M. Brader, MD Lancaster General Bariatrics Introduction The management of a patient with extreme obesity is a challenging task for most health care givers. Unfortunately, there
11/2/2015 BARIATRIC SURGERY. When and Why. Morbid Obesity. Body Mass Index (BMI) of 35 or higher
 BARIATRIC SURGERY When and Why Joseph A Johnson, MD Chief of Surgery, Highland Hospital Chief, Division GI and Bariatric Surgery, University of Rochester There is no reliable method of treatment to produce
BARIATRIC SURGERY When and Why Joseph A Johnson, MD Chief of Surgery, Highland Hospital Chief, Division GI and Bariatric Surgery, University of Rochester There is no reliable method of treatment to produce
David Shu, MD, FRCPC Endocrinology, Royal Columbian Hospital October 8 th, 2010
 David Shu, MD, FRCPC Endocrinology, Royal Columbian Hospital October 8 th, 2010 Objectives At the end of the talk, the participants will be able to: 1. Identify the increasing prevalence of type 2 diabetes
David Shu, MD, FRCPC Endocrinology, Royal Columbian Hospital October 8 th, 2010 Objectives At the end of the talk, the participants will be able to: 1. Identify the increasing prevalence of type 2 diabetes
Diabetes, hypertension and a lot more `in the elderly` JORIS SCHAKEL INTERNIST- CLINICAL GERIATRICIAN JGSCHAKEL@SEHOS.CW
 Diabetes, hypertension and a lot more `in the elderly` JORIS SCHAKEL INTERNIST- CLINICAL GERIATRICIAN JGSCHAKEL@SEHOS.CW IT`S HARD TO GIVE GENERAL ADVICE! ``The Elderly`` Heterogeneous group ;widely varying
Diabetes, hypertension and a lot more `in the elderly` JORIS SCHAKEL INTERNIST- CLINICAL GERIATRICIAN JGSCHAKEL@SEHOS.CW IT`S HARD TO GIVE GENERAL ADVICE! ``The Elderly`` Heterogeneous group ;widely varying
Reversing type 2 diabetes: pancreas composition and function during return to normal glucose tolerance
 Reversing type 2 diabetes: pancreas composition and function during return to normal glucose tolerance Dr Sarah Steven Clinical Research Fellow to Professor Roy Taylor Observations from bariatric surgery
Reversing type 2 diabetes: pancreas composition and function during return to normal glucose tolerance Dr Sarah Steven Clinical Research Fellow to Professor Roy Taylor Observations from bariatric surgery
The first endoscopically-delivered device therapy for obese patients with type 2 diabetes
 DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY. Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU
 TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD
 Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD Date written: July 2012 Author: Kate Wiggins, Graeme Turner, David Johnson GUIDELINES We
Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD Date written: July 2012 Author: Kate Wiggins, Graeme Turner, David Johnson GUIDELINES We
Type 2 Diabetes workshop notes
 Group 1 notes Abi / Nicole Type 2 Diabetes workshop notes 4.1 Population The group discussed the following sub groups that may need addressing: Men-as they tend to die earlier compared with women, their
Group 1 notes Abi / Nicole Type 2 Diabetes workshop notes 4.1 Population The group discussed the following sub groups that may need addressing: Men-as they tend to die earlier compared with women, their
Therapeutic Approach in Patients with Diabetes and Coronary Artery Disease
 Home SVCC Area: English - Español - Português Therapeutic Approach in Patients with Diabetes and Coronary Artery Disease Martial G. Bourassa, MD Research Center, Montreal Heart Institute, Montreal, Quebec,
Home SVCC Area: English - Español - Português Therapeutic Approach in Patients with Diabetes and Coronary Artery Disease Martial G. Bourassa, MD Research Center, Montreal Heart Institute, Montreal, Quebec,
GUIDELINES FOR THE TREATMENT OF DIABETIC NEPHROPATHY*
 71 GUIDELINES FOR THE TREATMENT OF DIABETIC NEPHROPATHY* Ryuichi KIKKAWA** Asian Med. J. 44(2): 71 75, 2001 Abstract: Diabetic nephropathy is the most devastating complication of diabetes and is now the
71 GUIDELINES FOR THE TREATMENT OF DIABETIC NEPHROPATHY* Ryuichi KIKKAWA** Asian Med. J. 44(2): 71 75, 2001 Abstract: Diabetic nephropathy is the most devastating complication of diabetes and is now the
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Bariatric Surgery. Beth A. Ryder, MD FACS. Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University
 Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Cardiovascular Effects of Drugs to Treat Diabetes
 Cardiovascular Effects of Drugs to Treat Diabetes Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies Clinical Trials:
Cardiovascular Effects of Drugs to Treat Diabetes Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies Clinical Trials:
Surgical Treatment. Type II Diabetes in. Obesity. for. Mathew Rawlins, MD FACS Rockwood Bariatric Specialists
 Surgical Treatment for Type II Diabetes in Obesity Mathew Rawlins, MD FACS Rockwood Bariatric Specialists Co-Morbidities of Obesity Coronary Disease Hypertension Dyslipidemias Pulmonary insufficiency
Surgical Treatment for Type II Diabetes in Obesity Mathew Rawlins, MD FACS Rockwood Bariatric Specialists Co-Morbidities of Obesity Coronary Disease Hypertension Dyslipidemias Pulmonary insufficiency
Pathophysiology of Type 2 Diabetes and Its Treatment Policy
 Research and Reviews Pathophysiology of Type 2 Diabetes and Its Treatment Policy JMAJ 53(1): 41 46, 2010 Kohei KAKU* 1 Abstract Impaired insulin secretion and increased insulin resistance, the main pathophysiological
Research and Reviews Pathophysiology of Type 2 Diabetes and Its Treatment Policy JMAJ 53(1): 41 46, 2010 Kohei KAKU* 1 Abstract Impaired insulin secretion and increased insulin resistance, the main pathophysiological
Type 2 Diabetes and Prediabetes: A New Understanding of Cause and Treatment. Bruce Latham, M.D. Endocrine Specialists Greenville Health System
 Type 2 Diabetes and Prediabetes: A New Understanding of Cause and Treatment Bruce Latham, M.D. Endocrine Specialists Greenville Health System Objectives for this presentation - Understand the thrifty genotype
Type 2 Diabetes and Prediabetes: A New Understanding of Cause and Treatment Bruce Latham, M.D. Endocrine Specialists Greenville Health System Objectives for this presentation - Understand the thrifty genotype
Gastric Bypass and Other Bariatric Surgical Procedures*
 Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
CHAPTER V DISCUSSION. normal life provided they keep their diabetes under control. Life style modifications
 CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
Weight-loss surgery has been shown to reduce comorbidities
 RESEARCH Review Obesity Surgery: Evidence for Diabetes Prevention/Management SUE CUMMINGS, MS, RD; CAROLINE M. APOVIAN, MD, FACP; LALITA KHAODHIAR, MD ABSTRACT Obesity is associated with an increased risk
RESEARCH Review Obesity Surgery: Evidence for Diabetes Prevention/Management SUE CUMMINGS, MS, RD; CAROLINE M. APOVIAN, MD, FACP; LALITA KHAODHIAR, MD ABSTRACT Obesity is associated with an increased risk
IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL
 464 IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL PRACTICE STEPHAN A SCHREIBER AND ANIKA RUßMAN ABSTRACT
464 IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL PRACTICE STEPHAN A SCHREIBER AND ANIKA RUßMAN ABSTRACT
Bariatric Surgical and Procedural Interventions in the Treatment of Obese Patients with Type 2 Diabetes
 Bariatric Surgical and Procedural Interventions in the Treatment of Obese Patients with Type 2 Diabetes A position statement from the International Diabetes Federation Taskforce on Epidemiology and Prevention
Bariatric Surgical and Procedural Interventions in the Treatment of Obese Patients with Type 2 Diabetes A position statement from the International Diabetes Federation Taskforce on Epidemiology and Prevention
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Using a Flow Sheet to Improve Performance in Treatment of Elderly Patients With Type 2 Diabetes
 Special Series: AAFP Award-winning Research Papers Vol. 31, No. 5 331 Using a Flow Sheet to Improve Performance in Treatment of Elderly Patients With Type 2 Diabetes Gary Ruoff, MD; Lynn S. Gray, MD, MPH
Special Series: AAFP Award-winning Research Papers Vol. 31, No. 5 331 Using a Flow Sheet to Improve Performance in Treatment of Elderly Patients With Type 2 Diabetes Gary Ruoff, MD; Lynn S. Gray, MD, MPH
Statins and Risk for Diabetes Mellitus. Background
 Statins and Risk for Diabetes Mellitus Kevin C. Maki, PhD, FNLA Midwest Center for Metabolic & Cardiovascular Research and DePaul University, Chicago, IL 1 Background In 2012 the US Food and Drug Administration
Statins and Risk for Diabetes Mellitus Kevin C. Maki, PhD, FNLA Midwest Center for Metabolic & Cardiovascular Research and DePaul University, Chicago, IL 1 Background In 2012 the US Food and Drug Administration
Effect of liraglutide on body weight in overweight or obese subjects with type 2 diabetes: SCALE - Diabetes
 Effect of liraglutide on body weight in overweight or obese subjects with type 2 diabetes: SCALE - Diabetes This trial is conducted in Africa, Asia, Europe and the United States of America (USA). The aim
Effect of liraglutide on body weight in overweight or obese subjects with type 2 diabetes: SCALE - Diabetes This trial is conducted in Africa, Asia, Europe and the United States of America (USA). The aim
Managing diabetes in the post-guideline world. Dr Helen Snell Nurse Practitioner PhD, FCNA(NZ)
 Managing diabetes in the post-guideline world Dr Helen Snell Nurse Practitioner PhD, FCNA(NZ) Overview Pathogenesis of T2DM Aims of treatment The place of glycaemic control Strategies to improve glycaemic
Managing diabetes in the post-guideline world Dr Helen Snell Nurse Practitioner PhD, FCNA(NZ) Overview Pathogenesis of T2DM Aims of treatment The place of glycaemic control Strategies to improve glycaemic
Type 2 diabetes mellitus current therapies and the emergence of surgical options
 Type 2 diabetes mellitus current therapies and the emergence of surgical options Harold E. Lebovitz Abstract Patients with type 2 diabetes mellitus (T2DM) are usually treated with pharmacologic agents
Type 2 diabetes mellitus current therapies and the emergence of surgical options Harold E. Lebovitz Abstract Patients with type 2 diabetes mellitus (T2DM) are usually treated with pharmacologic agents
Use of Glycated Hemoglobin and Microalbuminuria in the Monitoring of Diabetes Mellitus
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Number 84 Use of Glycated Hemoglobin and Microalbuminuria in the Monitoring of Diabetes Mellitus Summary Overview Clinical
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Number 84 Use of Glycated Hemoglobin and Microalbuminuria in the Monitoring of Diabetes Mellitus Summary Overview Clinical
Weight Loss After Bariatric Surgery
 BENEFITS OF BARIATRIC SURGERY AND PERIOPERATIVE SURGICAL SAFETY Ji Chung Tham, 1 *Carel W. le Roux 2,3 1. General and Vascular Surgery Department, Musgrove Park Hospital, Taunton, UK 2. Diabetes Complications
BENEFITS OF BARIATRIC SURGERY AND PERIOPERATIVE SURGICAL SAFETY Ji Chung Tham, 1 *Carel W. le Roux 2,3 1. General and Vascular Surgery Department, Musgrove Park Hospital, Taunton, UK 2. Diabetes Complications
Short-term Effects of Sleeve Gastrectomy on Type 2 Diabetes Mellitus in Severely Obese Subjects
 Obesity Surgery, 17, 1069-1074 Research Articles Short-term Effects of Sleeve Gastrectomy on Type 2 Diabetes Mellitus in Severely Obese Subjects J. Vidal, MD, PhD; A. Ibarzabal, MD; J. Nicolau, MD; M.
Obesity Surgery, 17, 1069-1074 Research Articles Short-term Effects of Sleeve Gastrectomy on Type 2 Diabetes Mellitus in Severely Obese Subjects J. Vidal, MD, PhD; A. Ibarzabal, MD; J. Nicolau, MD; M.
Improving drug prescription in elderly diabetic patients. FRANCESC FORMIGA Hospital Universitari de Bellvitge
 Improving drug prescription in elderly diabetic patients FRANCESC FORMIGA Hospital Universitari de Bellvitge High prevalence, but also increases the incidence. The older the patients, the higher the percentages
Improving drug prescription in elderly diabetic patients FRANCESC FORMIGA Hospital Universitari de Bellvitge High prevalence, but also increases the incidence. The older the patients, the higher the percentages
DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE
 DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE 40 yo woman, BMI 36. Motivated to begin diet therapy. Which of the following is contraindicated: Robert B. Baron MD MS Professor and
DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE 40 yo woman, BMI 36. Motivated to begin diet therapy. Which of the following is contraindicated: Robert B. Baron MD MS Professor and
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides.
 Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Measure #1 (NQF 0059): Diabetes: Hemoglobin A1c Poor Control National Quality Strategy Domain: Effective Clinical Care
 Measure #1 (NQF 0059): Diabetes: Hemoglobin A1c Poor Control National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Measure #1 (NQF 0059): Diabetes: Hemoglobin A1c Poor Control National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary?
 White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
Morbid obesity is defined as a body mass index (BMI) >40 kg/m2 (normal BMI range: 19-25 kg/m2)
 Medical Policy Manual Topic: Bariatric Surgery Date of Origin: January 1996 Section: Surgery Last Reviewed Date: January 2014 Policy No: 58 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Bariatric Surgery Date of Origin: January 1996 Section: Surgery Last Reviewed Date: January 2014 Policy No: 58 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
BARIATRIC SURGERY. Prerequisites. Authorization, Notification and Referral
 BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
Ileal transposition provides insight into the effectiveness of gastric bypass surgery
 Physiology & Behavior 88 (2006) 277 282 Ileal transposition provides insight into the effectiveness of gastric bypass surgery April D. Strader Southern Illinois University School of Medicine, Department
Physiology & Behavior 88 (2006) 277 282 Ileal transposition provides insight into the effectiveness of gastric bypass surgery April D. Strader Southern Illinois University School of Medicine, Department
Weight and Type 2 Diabetes after Bariatric Surgery: Systematic Review and Meta-analysis
 CLINICAL RESEARCH STUDY Weight and Type 2 Diabetes after Bariatric Surgery: Systematic Review and Meta-analysis Henry Buchwald, MD, PhD, a Rhonda Estok, RN, BSN, b Kyle Fahrbach, PhD, b Deirdre Banel,
CLINICAL RESEARCH STUDY Weight and Type 2 Diabetes after Bariatric Surgery: Systematic Review and Meta-analysis Henry Buchwald, MD, PhD, a Rhonda Estok, RN, BSN, b Kyle Fahrbach, PhD, b Deirdre Banel,
Subject: Weight Loss Surgery Policy. Effective Date: 1/00 Revision Date: 10/15
 Subject: Weight Loss Surgery Policy Effective Date: 1/00 Revision Date: 10/15 DESCRIPTION OSU Health Plans supports covered members with a spectrum of service for obesity and weight loss attempts. The
Subject: Weight Loss Surgery Policy Effective Date: 1/00 Revision Date: 10/15 DESCRIPTION OSU Health Plans supports covered members with a spectrum of service for obesity and weight loss attempts. The
Potential of Surgery for Curing Type 2 Diabetes Mellitus
 REVIEW ANNALS OF SURGERY Vol. 236, No. 5, 554 559 2002 Lippincott Williams & Wilkins, Inc. Potential of Surgery for Curing Type 2 Diabetes Mellitus Francesco Rubino, MD,* and Michel Gagner, MD, FACS, FRCSC
REVIEW ANNALS OF SURGERY Vol. 236, No. 5, 554 559 2002 Lippincott Williams & Wilkins, Inc. Potential of Surgery for Curing Type 2 Diabetes Mellitus Francesco Rubino, MD,* and Michel Gagner, MD, FACS, FRCSC
Safety & Effectiveness of Drug Therapies for Type 2 Diabetes: Are pharmacoepi studies part of the problem, or part of the solution?
 Safety & Effectiveness of Drug Therapies for Type 2 Diabetes: Are pharmacoepi studies part of the problem, or part of the solution? IDEG Training Workshop Melbourne, Australia November 29, 2013 Jeffrey
Safety & Effectiveness of Drug Therapies for Type 2 Diabetes: Are pharmacoepi studies part of the problem, or part of the solution? IDEG Training Workshop Melbourne, Australia November 29, 2013 Jeffrey
Psoriasis Co-morbidities: Changing Clinical Practice. Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology. Psoriatic Arthritis
 Psoriasis Co-morbidities: Changing Clinical Practice Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology Psoriatic Arthritis Psoriatic Arthritis! 11-31% of patients with psoriasis have psoriatic
Psoriasis Co-morbidities: Changing Clinical Practice Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology Psoriatic Arthritis Psoriatic Arthritis! 11-31% of patients with psoriasis have psoriatic
Jahnavi Srinivasan, MD Assistant Professor of General Surgery Emory University
 Jahnavi Srinivasan, MD Assistant Professor of General Surgery Emory University Definition & Demographics The branch of medicine dealing with the diagnosis and treatment of obesity. BMI NIH Classification
Jahnavi Srinivasan, MD Assistant Professor of General Surgery Emory University Definition & Demographics The branch of medicine dealing with the diagnosis and treatment of obesity. BMI NIH Classification
ORIGINAL ARTICLE. A Prospective Cohort Study of Laparoscopic Sleeve Gastrectomy vs Medical Treatment
 ONLINE FIRST ORIGINAL ARTICLE Obesity, Type 2 Diabetes Mellitus, and Other Comorbidities A Prospective Cohort Study of Laparoscopic Sleeve Gastrectomy vs Medical Treatment Frida Leonetti, MD, PhD; Danila
ONLINE FIRST ORIGINAL ARTICLE Obesity, Type 2 Diabetes Mellitus, and Other Comorbidities A Prospective Cohort Study of Laparoscopic Sleeve Gastrectomy vs Medical Treatment Frida Leonetti, MD, PhD; Danila
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Introduction. Pathogenesis of type 2 diabetes
 Introduction Type 2 diabetes mellitus (t2dm) is the most prevalent form of diabetes worldwide. It is characterised by high fasting and high postprandial blood glucose concentrations (hyperglycemia). Chronic
Introduction Type 2 diabetes mellitus (t2dm) is the most prevalent form of diabetes worldwide. It is characterised by high fasting and high postprandial blood glucose concentrations (hyperglycemia). Chronic
MECHANISMS OF IMPROVED GLYCEMIC CONTROL FOR TYPE 2 DIABETES PATIENTS AFTER BYPASS SURGERY BEYOND THE WEIGHT LOSS
 THE PUBLISHING HOUSE MEDICINE OF THE ROMANIAN ACADEMY Review article MECHANISMS OF IMPROVED GLYCEMIC CONTROL FOR TYPE 2 DIABETES PATIENTS AFTER BYPASS SURGERY BEYOND THE WEIGHT LOSS CORNELIA ZETU 1,3,
THE PUBLISHING HOUSE MEDICINE OF THE ROMANIAN ACADEMY Review article MECHANISMS OF IMPROVED GLYCEMIC CONTROL FOR TYPE 2 DIABETES PATIENTS AFTER BYPASS SURGERY BEYOND THE WEIGHT LOSS CORNELIA ZETU 1,3,
Surgery for Obesity and Related Diseases 7 (2011) 433 447. IDF statement
 Surgery for Obesity and Related Diseases 7 (2011) 433 447 IDF statement Bariatric surgery: an IDF statement for obese Type 2 diabetes J. B. Dixon a, P. Zimmet a, *, K. G. Alberti b, F. Rubino c, on behalf
Surgery for Obesity and Related Diseases 7 (2011) 433 447 IDF statement Bariatric surgery: an IDF statement for obese Type 2 diabetes J. B. Dixon a, P. Zimmet a, *, K. G. Alberti b, F. Rubino c, on behalf
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16
 HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
How To Determine The Prevalence Of Microalbuminuria
 Research Journal of Pharmaceutical, Biological and Chemical Sciences Prevalence of Microalbuminuria in relation to HbA1c among known Type2 Diabetic Patients in Puducherry population Muraliswaran P 1 *,
Research Journal of Pharmaceutical, Biological and Chemical Sciences Prevalence of Microalbuminuria in relation to HbA1c among known Type2 Diabetic Patients in Puducherry population Muraliswaran P 1 *,
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
With an estimated over 300 million
 S E C T I O N I I I Is Type 2 Diabetes an Operable Intestinal Disease? A provocative yet reasonable hypothesis FRANCESCO RUBINO, MD Type 2 diabetes, which accounts for 90 95% of all cases of diabetes,
S E C T I O N I I I Is Type 2 Diabetes an Operable Intestinal Disease? A provocative yet reasonable hypothesis FRANCESCO RUBINO, MD Type 2 diabetes, which accounts for 90 95% of all cases of diabetes,
Bariatric surgery: an IDF statement for obese Type 2 diabetes
 Article: Clinical Practice DOI: 10.1111/j.1464-5491.2011.03306.x Bariatric surgery: an IDF statement for obese Type 2 diabetes J. B. Dixon*, P. Zimmet*, K. G. Alberti and F. Rubino, on behalf of the International
Article: Clinical Practice DOI: 10.1111/j.1464-5491.2011.03306.x Bariatric surgery: an IDF statement for obese Type 2 diabetes J. B. Dixon*, P. Zimmet*, K. G. Alberti and F. Rubino, on behalf of the International
Roux-en-Y gastric bypass (RYGB) is a well-accepted
 RESEARCH Review Meets Learning Need Codes 5000, 5370, and 5390. To take the Continuing Professional Education quiz for this article, log in to ADA s Online Business Center at www.eatright.org/obc, click
RESEARCH Review Meets Learning Need Codes 5000, 5370, and 5390. To take the Continuing Professional Education quiz for this article, log in to ADA s Online Business Center at www.eatright.org/obc, click
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Bariatric surgery in patients with late-stage type 2 diabetes: expected beneficial effects on risk ratio and outcomes
 Diabetes & Metabolism 35 (2009) 564 568 Bariatric surgery in patients with late-stage type 2 diabetes: expected beneficial effects on risk ratio and outcomes E. Renard Endocrinology Department, Centre
Diabetes & Metabolism 35 (2009) 564 568 Bariatric surgery in patients with late-stage type 2 diabetes: expected beneficial effects on risk ratio and outcomes E. Renard Endocrinology Department, Centre
