Fast track surgery for biliodigestive derivation: Initial experience
|
|
|
- Pierce Hudson
- 8 years ago
- Views:
Transcription
1 Rios-Cruz et al. 9 case Original report Article peer Reviewed open OPEN ACCESS Fast track surgery for biliodigestive derivation: Initial experience Daniel Rios-Cruz, Joaquin Valerio-Ureña, Julio Abraham Hernández- Ascencio, Patricia Galindo-López, Veronica Torres-Medina Abstract Aims: Talk about Fast Track Surgery is referring to a series of measures implemented to accelerate postoperative recovery of the patient. This has been well demonstrated for colorectal surgery with good results. There is very little experience on its application to biliary surgery. The aim of this study is to describe the initial experience of the application of Fast Track Surgery protocol to biliodigestive surgery at high speciality hospital of Veracruz. Methods: Descriptive, transversal, prospective study. Patients undergoing some kind of biliodigestive derivation, from January 2012 to December 2013 in our hospital under the protocol of Fast Track Surgery, were included. Results: 12 patients were treated. Nine underwent Hepp-Couinaud type derivation; three, common bile duct-duodedum anastomosis was performed. No patient remained with probes or drains after surgery. The time to start orally was 7.27 ± 2.68 hours; time to start mobilization out of bed was 5.39 ± 2.50 hours. Patients were discharged at ± hours post-surgical event. Two patients had surgical site infection. No re-admissions were presented. Conclusion: Application of Fast Track Surgery protocol appears to be safe and feasible. However, it is necessary to expand the sample of patients. Keywords: Biliary tract, Biliodigestive derivation, Enhanced recovery after surgery, Fast track surgery How to cite this article Rios-Cruz D, Valerio-Ureña J, Hernández- Ascencio JA, Galindo-López P, Torres-Medina V. Fast track surgery for biliodigestive derivation: Initial experience. Int J Hepatobiliary Pancreat Dis 2015;5:9 16. Article ID: IJHPDDC2015 Daniel Rios-Cruz 1, Joaquin Valerio-Ureña 1, Julio Abraham Hernández-Ascencio 1, Patricia Galindo-López 2, Veronica Torres-Medina 3 Affiliations: 1 Department of Surgery, High Speciality Hospital of Veracruz. Avenida 20 de noviembre S/N Centro. CP Veracruz, Veracruz, México; 2 School of Medicine University of Veracruz, México; 3 Department of Anesthesiology, High Speciality Hospital of Veracruz. Avenida 20 de noviembre S/N Centro. CP Veracruz, Veracruz, México. Corresponding Author: Dr. Daniel Rios Cruz, JF Oca # 43 interior 4 entre Amado Nervo y Hernández y Hernández, Colonia Flores Magón, Veracruz, Veracruz,México, C.P ; Ph: (52) , Fax: (52) ; jobzon@hotmail.com Received: 01 October 204 Accepted: 19 November 2014 Published: 17 March 2015 ********* doi: /ijhpd oa-3 introduction In the last years the pre, trans and postoperative traditional cares of general surgery have been questioned and even more regarding to gastrointestinal tract [1]. From nutritional support preoperatively to postoperative fasting time through the incision size, if open surgery, have discussed their role in patient recovery. Traditionally, total fasting of eight hours before sugery, intestinal preparation if resection and anastomosis is programed, big incisions, rest in bed for long periods, were part of a common denominator of patients who underwent gastrointestinal surgery.
2 These concepts have been modified in the last decades. Kehlet et al. [2] were the first to establish a specific protocol called Fast-Track; based in the best scientific evidence seeks to minimize the surgical stress response, accelerate recovery, decrease complications and consequently, shorten hospital stay without compromising, therefore, patient safety. The enhanced recovery programs have been subject of numerous systematic reviews in colorectal surgery and most of them have demonstrated a shortened in hospital stay after surgery, lower rate of complications and decreased hospital costs [3 6]. There are also reports about its use in vascular and urological surgery with good results [7 10]. However, there is a little evidence of its use in hepatobiliary surgery. A recent systematic review suggests that the application of Fast Track Surgery protocol appears to be safe and feasible [11]. In our hospital, we have implemented a enhanced recovery protocol in patients undergoing biliodigestive derivation. The aim of this paper is to present our initial experience with this protocol. MATERIALS AND METHODS All patients who underwent some form of biliodigestive derivation, higher than 18 years, both sexs, under the Fast Track Surgery protocol from January 2012 to December 2013 were included. The protocol consists in to inform the patient what is going to happen during his/her hospital stay, what to expect and what is his/her role in the recovery, allow patient s fluid intake 250 ml up to two hours before the surgical event and, if the patient desired, a water jelly 150 ml. During surgery, either foley catheter or nasogastric tube is used if so required, which are removed before patient reversal from anesthesia; at the discretion of the surgical team judicious use of abdominal drains is performed only used if deemed necessary. All anastomoses were performed in a single layer with absorbable stitches 4-0. All the surgeries were performed under general anesthesia and high lumbar regional blockage. The site chosen for the incision is 2 cm below the right costal margin extending it to two or three inches beyond the left midline by following a hockey stick. Intravenous analgesia starts just finishing to intubate the patient and at the end of surgery is complemented. Then continue oral analgesia with tramadol + paracetamol tablets (325 mg and 37.5 mg, respectively) every 8 hours starting from two hours after having extubated (after verifying the proper state of consciousness of the patient) and ketorolac 30 mg IV every 6 hours. Taking adequate analgesia, patients are asked to begin mobilizing out of bed as soon as possible, first sitting in a chair and then walking. Once initiated mobilization out of bed, feeding by mouth starts just with liquids which progresses as the patient will tolerate and usually within the first 12 hours after surgery. Patient is discharged having adequate analgesia orally, tolerating Rios-Cruz et al. 10 diet, walking without presenting a contraindication for hospital discharge as systemic inflammatory response, uncontrolled pain or intolerance to the oral route. The specific protocol is given in Table 1. Descriptive statistics were used to express the data. RESULTS During the period, 12 patients underwent some form of biliodigestive derivation under the established protocol; 10 women and two men. Age was ± years. Nine patients underwent Hepp-Couinaud secondary to a biliary tract injury who were referred to our hospital. Three patients underwent common bile ductduodenum anastomosis for palliation of advanced head pancreatic cancer. Surgery time was 5.24 ± 2.70 hr. All patients undergoing Hepp-Couinaud were placed urinary catheter which was removed before patient reversed from anesthesia. Six patients had nasogastric tube placed during surgery to remove the air passing into the gastric chamber during anesthetic induction and was removed before patient was extubated in all cases. By positioning the tube was obtained 10 ml average of residual liquids ingested before surgery. Careful control of hemostasis was performed in all cases. No intra-abdominal drains were used. Respiratory exercises began in the room with the patient awake, this about 4 hours after surgery. The mobilization out of bed was given to 5.39 ± 2.50 hrs after surgery. The start time of the oral route was presented to 7.27 ± 2.68 hrs after surgery. Three patients had cholangitis with piobilia documented and of these three, two patients had surgical site infection that was treated with cures. The hospital stay after surgery was ± hr. Being higher in the three patient with biliary tract sepsis and inflammatory response and / or surgical wound infections. No re-admissions occurred during the first 30 days after discharge. During the follow-up 9.04 ± 6.85 months only one patient died due to pancreatic cancer for which he was carrying; the remaining patients continue under close monitoring at the office without complications due to the surgical procedure (Table 2). Infected wounds were closed in a delayed manner. One of these two patients with severe cholangitis studied by computed tomography showed multiple colangiolares abscesses and one of them was broken and sealed with the diaphragm; pus from biliary tract during surgery was obtained and culture was positive for E. coli. This patient had a hospital stay of 8 days after surgery because of the need for close monitoring and the use of intravenous antibiotics. DISCUSSION The protocols of accelerated recovery have come to break paradigms around the perioperative environment of the patient. While it has been documented that general
3 Rios-Cruz et al. 11 Table 1: Fast Track Protocol followed in patients with biliodigestive derivation surgery Patient preparation Preoperative oral route Preparation of the digestive tract Initial interview Initial training Breathing exercises Preoperative physical activity Normal diet to 8 hrs. previous; water free demand until 3 hours before surgery. Not required in any case It seeks to the total empathy between patient, family and medical team and is explained in detail in the protocol that is such that they would be clear. It teaches the patient how to get out of bed with some help on the day of surgery and explain the advantages of wandering within hours of surgery; Will be explains to the patient the importance of not be afraid to breathe deeply despite the surgery being performed and is taught to the familiar as an adjunct in pulmonary physiotherapy for the patient. They are emphasizing the importance of nutrition as fast as possible and avoid prolonged preoperative fasting especially because they are patients with previous iatrogenic lesions or cancer that already if they have been depleted. 15 repetitions every 3 hrs. respecting nocturnal sleep, with respiratory exerciser or at least blow party balloons for previous inhales 48 hr before surgery. Frequent ambulation before surgery and exercises muscle tone of arms and legs is encouraged. 2 to 3 hours prior to surgery, 250 cc of fluid in any of the following ways: chamomile tea, coffee (both sweetened to taste) orange juice or apple and optionally 1 water jelly to 150 cc, whether oral medication requires up to 30 min before surgery with 30 cc of water. Trichotomy No required Exceptionally only withdraw if clogged villi at the site of the incision just washing the patient Anesthesia General balanced + Mixed regional block + Fentanyl + propofol + sevorane Heavy Bupivacaine 5% 12 to 15 mg at the onset of subarachnoid anesthesia and ropivacaine 7.5% 2 ml or 150 mg epidural when closing fascia. Analgesia Catheters and probes Drains Postoperative rest Preincisional Local anesthesia Trans-operative intravenous Postoperative (oral and intravenous) Central venous catheter Peripheral vascular Access Foley Nasogastric Penrose 3/4 or drenovack 1/4 In bed In reposet Ropivacaine 7.5% diluted in 40 cc of saline solution to infiltrate incision site and infiltration of intercostal nerve points 6,7 and 8 Before impact, ketorolac 30 mg intravenous and fentanyl 3 mg/kg/hr and at the end of surgery is complemented by ketorolac mg depending on the patient s weight. Tramadol tablets + paracetamol (37.5 mg and 325 mg respectively) every 8 hr.starting from the two hours after having extubated after verifying the proper state of consciousness of the patient and ketorolac 30 mg IV every 6 hr. or ketoprofen 100 mg IV every 12 hours until the withdrawal of the IV solutions after verifying good pain control with oral analgesics. Oral analgesia with ibuprofen 400 mg every 8hrs replacing the endovenous. The patient was discharged with oral analgesics mentioned both by 3-5 days as required with interleaved schedules to always have a good analgesic effect but prevents the patient wakes up during the night to take drugs. It is placed only either if is required to apply damaging drugs to the vessels or is a priority determining central venous pressure. One or two routes of short and thick venous access with catheters and usually at the end of surgery the patient leave the operating room with a single vascular access pathway. During the transoperative if is expected a surgery more than 3 hr and removed at the end of surgery unless the patient pass to intensive therapy or requires detailed monitoring of liquids. It is placed at the beginning of surgery only when the stomach is distended and removed before the patient emerges from anesthesia. In cases where is placed, is tapped and the stomach contents aspirated is measured. No drains are placed unless the possibility of an anastomotic leak is suspected and always prefer to redo an anastomosis at the time if it is necessary instead put a drain. When a drain is placed, a closed one is preferred. On leaving the recovery room, starts in semifowler position in hospitalization bed: passive or active mobilization of limbs inside the bed. It passes the patient to a reposet or chair, 8 16 hrs after surgery unless there is a contraindication for this. After the first 4 hours in semifowler positions the patients begins to repositioning going from sitting up in bed to sitting with feet out of bed and finally sitting out of bed except to be night time in which case starts the next morning. We encourage the patient to urinate out of bed and go to the bathroom to evacuate.
4 Rios-Cruz et al. 12 Post-operative (POP) Ambulation Start of oral route Respiratory therapy Antithrombotic measures Bandages and girdles Day 0 POP Day 1 POP Day 2 POP Medicaments Water Food Breathing exercises Pulmonary percussion Pharmacological Mechanical abdominal Starts 4-16 hr after surgery; Assisted short walks around the bed and near the stall where it is located. The day after the surgery, are made in an average of 3 walks of 50, 100 and 200m and go the bathroom to bathe and perform their stools. The second day at least 3 walks 200m each. The oral medication can initiate even 2 hrs. after waking from anesthesia with ml of water. Water intake is allowed to tolerance from the first 6 hrs. of completed the surgery Clear liquids 6 hours after surgery. The next day normal diet low in fats is allowed and empowers the patient to eat only what he/she wants except that the patient is distended or is vomiting. 15 repetitions every 3 hrs. with inspiratory device respecting nocturnal sleep and if not have this device, at least with balloon inflation with deep breaths before each insufflation. Percussions on the back with the palm of the hand provided by the family every 3 hrs. during the day, respecting the patient s sleep. Enoxaparin 40 mg SC every 24 hrs.from admission except that have altered times and for 1 week after surgery if the daily mobility is inadequate. Graduated compression stockings to upper third of thighs until the patient wanders at least 5 times a day or more than 600m per day for two consecutive days. Are not used. Their use is avoided and we explain to the patient before surgery its exceptional use. Use of stair Use them once the patient goes home as if asleep upstairs, down to the dining room to eat each time corresponds intake is encouraged. Table 2: Specific characteristics of patients Patient Gender Age* Urinary catheter NGT Gastric residual volume** Surgery Performed Surgical Time Mobilization out of bed Starting oral route Follow up HS post surgery 1 F 28 Yes Yes 8 Hepp-Couinaud F 35 Yes No - Hepp-Couinaud F 45 Yes No - Hepp-Couinaud M 55 No No - Common bile duct-duodeno F 48 Yes Yes 10 Hepp-Couinaud F 45 Yes Yes 13 Hepp-Couinaud F 65 No No - Common bile duct-duodeno F 40 Yes Yes 8 Hepp-Couinaud F 63 No Yes 9 Common bile duct-duodeno F 38 Yes No - Hepp-Couinaud F 29 Yes Yes 12 Hepp-Couinaud M 47 Yes No - Hepp-Couinaud Abbreviations: NGT: Nasogastric tube. HS: Hospital stay. *Quantity expressed in years. ** Quantity expressed in milliliters. Quantity expressed in months. Quantity expressed in hours. anesthesia reduces the protective laryngeal reflex and increases the risk of aspiration, has also been shown that subsequent to ingest a volume of 100 ml of solid or liquid food, the stomach only has about 10 ml of liquid material after an hour and about 30 ml of solid material after three hours. For a passive regurgitation and aspiration during anesthesia, some gastric volume must be present and this is estimated to be around 200 ml. Preoperative fluid intake has been associated with better well-being, less thirst and dryness of the mouth and lower postoperative anxiety. Allow habitual coffee intake to coffee drinkers in the morning, can even reduce postoperative headache due to caffeine deprivation [12]. Other authors consider that fasting can be reduced safely up to two to three hours before the surgery [13].
5 Soreide et al. have shown that four hours of fasting are sufficient for a complete gastric emptying [14]. After open abdominal surgery, patients who were treated with an infusion of glucose during the night before surgery, presented a reduction in insulin resistance of 50% compared with patients who fasted the previous night [15]. Why give so much importance to insulin resistance in a patient undergoing any type of surgery? The insulin resistance is an important phenomenon that lasts up to three weeks after uncomplicated open abdominal surgery [16] and the degree of insulin resistance is an independent predictor of in-hospital stay [17]. The main objective of carbohydrate intake before surgery is to produce the change in metabolism that normally takes place when the patient eats breakfast. Based on the previous, we can say that allowing fluid intake two hours before anesthesia for elective surgery is safe and improves subjective well-being of the patient. Furthermore, oral carbohydrate intake before surgery reduces surgical stress [12]. For this reason we allow our patients the intake of carbohydrate rich drinks or coffee and none of them developed reflux event during tracheal intubation and in patients in which nasogastric tube was used, the average output of such liquids through the same was 10 ml. The principal factors to keep an inpatient after uncomplicated major abdominal surgery is the need for intravenous analgesia (aching), intravenous fluids (persistent bowel dysfunction) and bed rest (lack of mobility of the patient). These factors interact with each other and retard the patient reintegration to normal activities. Part of the protocol of Fast Track Surgery is to combat these factors with the aim of accelerating postoperative recovery of the patient and with it, decrease the time in which he/she can be incorporated into daily life. The fact that the patient has probes and catheters, prevent free movement either by fear of those devices or discomfort they generate. There are studies which show that the routine use of the nasogastric tube is not justified because there are no advantages over its use after intestinal surgery [18]. Studies have shown that the use of drains in the peritoneal cavity after intestinal resection and anastomosis do not reduce the incidence or severity of an anastomotic leak and its complications [19, 20]. Therefore, in patients submitted to surgery on the Fast Track protocol Surgery, abdominal drains are not used routinely [21]. Likewise with the urinary catheter; if the surgery was performed without complications, its permanence may limit early mobility of the patient. All our patients left the operating room without nasogastric tubes, urinary catheters or drains into the abdominal cavity. The main foundation of early postoperative mobilization of the patient depends on the pain control. A Cochrane review states that the optimal analgesia that allows early mobilization of the postoperative patient is the continuous epidural analgesia or local anesthesia based on opioids [22]. The employment of intravenous Rios-Cruz et al. 13 opioids does not produce the same effect as epidural analgesia. NSAIDs can provide additional analgesia and the combination of paracetamol and NSAIDs provide superior analgesia. Our patients were managed with epidural analgesia with 150 mg of 7.5% ropivacaine before reverting to general anesthesia, subsequently administered intravenously a dose of paracetamol and NSAIDs for later change the route of administration to the oral route. A meta-analysis concludes that there are no advantages to keep a patient fasting after gastrointestinal resection [23]. Early feeding reduces the risk of infection and length of hospital stay. Also, early feeding was not associated with increased risk of distal anastomotic dehiscence feeding site. Therefore, the patient should be encouraged to start orally four hours after the surgical event. Bed rest only increases insulin resistance and the loss of muscle mass but decreases muscle strength, lung function and tissue oxygenation [24]. Therefore, the patient should be moved out of bed at least two hours on the day of surgery and the remaining days six hours until hospital discharge. On the basis of these principles, patients showed adequate analgesia, which allowed early mobilization out of bed and consequently allowed oral intake. Another objective of the program is to reduce hospital stay. Usually, the biliodigestives surgeries are characterized by longer hospital stays for underlying pathology that is mostly a result of biliary injury. The traditional postoperative behavior is based on prolonged fasting due to anastomosis performed under the argument of intestinal healing. Most of our patients were discharged between 48 hr and 72 hr after the surgical event (common bile duct-duodenum and Hepp-Couinaud respectively) but three of our patients, subjected to Hepp-Couinaud, presented sepsis syndrome associated with cholangitis and piobilia and two of them also had surgical site infections a positive culture for E. coli, so, despite having started early mobilization and orally, their hospital stay was prolonged due to the discomfort it caused their infection to the patient. We can not attribute the surgical site infection to the Fast Track Protocol, as these patients had an identified site of infection (bile duct) that caused contamination to the surgical site. This is one of the first works that seek to implement an accelerated recovery for biliary surgery. An important limitation of our study is the small number of patients that we collect throughout the study period. In our hospital it has been difficult to break traditional paradigms on perioperative care of patients and few surgeons and anesthesiologists who are open to new knowledge and the possibility to change these paradigms and this is reflected in the small sample that we collect. Another limitation of our study is its way of being descriptive. We do not have a control group with which to compare our results and give more validity and this is partly due to this type of surgery is performed mostly by the group of surgeons who carried out the study. It is important to mention, in this protocol, the patient plays an important role in their recovery so it
6 is required to be well informed about what will happen before and after the surgical event, this includes their collaboration to get out of bed and start walking the day of surgery has been performed. CONCLUSION In summary the application of Fast Track Surgery protocol appears to be safe and feasible. However, it is necessary to expand the sample of patients. ********* Author Contributions Daniel Rios-Cruz Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Joaquin Valerio-Ureña Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Julio Abraham Hernández-Ascencio Conception and design, Acquisition of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Patricia Galindo-López Conception and design, Acquisition of data, Drafting the article, Critical revision of the article, Final approval of the version to be published. Veronica Torres-Medina Conception and design, Acquisition of data, Drafting the article, Critical revision of the article, Final approval of the version to be published. Guarantor The corresponding author is the guarantor of submission. Conflict of Interest Authors declare no conflict of interest. Copyright 2015 Daniel Rios-Cruz et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. REFERENCES 1. Esteban Collazo F, Garcia Alonso M, Sanz Lopez R, et al. Results of applying a fast-track protocol in a colorectal surgery unit: comparative study. Cir Esp 2012 Aug-Sep;90(7): [Article in Spanish]. 2. Kehlet H, Mogensen T. Hospital stay of two days after open sigmoidectomy with a multimodal rehabilitation programme. Br J Surg 1999 Feb;86(2): Rios-Cruz et al Lassen K, Soop M, Nygren J, et al. Consensus review of optimal perioperative care in colorectal surgery: Enhanced Recovery After Surgery (ERAS) Group recommendations. Arch Surg 2009 Oct;144(10): Stephen AE, Berger DL. Shortened length of stay and hospital cost reduction with implementation of an accelerated clinical care pathway after elective colon resection. Surgery 2003 Mar;133(3): Adamina M, Kehlet H, Tomlinson GA, Senagore AJ, Delaney CP. Enhanced recovery pathways optimize health outcomes and resource utilization: A metaanalysis of randomized controlled trials in colorectal surgery. Surgery 2011 Jun;149(6): Spanjersberg WR, Reurings J, Keus F, Van Laarhoven CJ. Fast Track Surgery versus conventional recovery strategies for colorectal surgery. Cochrane Database Syst Rev 2011 Feb 16;(2):CD Huber TS, Carlton LM, Harward TR, et al. Impact of clinical pathway for elective infrarrenal aortic reconstructions. Ann Surg 1998 May;227(5): Niino T, Hata M, Sezai A, et al. Optimal clinical pathway for the patient with type B cute aortic dissection. Circ J 2009 Feb;73(2): Koch MO, Smith JA Jr. Influence of patient age and comorbidity on outcome of a collaborative care pathway after radical prostatectomy and cystoprostatectomy. J Urol 1996 May;155(5): Leibman BD, Dillioglugil O, Abbas F, Tanli S, Kattan MW, Scardino PT. Impact of a clinical pathway for radical retropubic prostatectomy. Urology 1998 Jul;52(1): Hall TC, Denninson AR, Bilku DK, Metcalfe MS, Garcea G. Enhanced recovery programmes in hepatobiliary and pancreatic surgery: A systematic review. Ann R Coll Surg Engl 2012 Jul;94(5): Ljungqvist O, Soreide E. Preoperative fasting. Br J Surg 2003 Apr;90(4): Miller M, Wishart HY, Nimmo WS. Gastric content at induction of anesthesia. Is a 4-hour fast necessary? Br J Anaesth 1983 Dec;55(12): Soreide E, Hausken T, Soreide JA, Steen PA. Gastric emptying of a light hospital breakfast. A study using real time ultrasonography. Acta Anaesthesiol Scand 1996 May;40(5): Ljungqvist O, Thorell A, Guntiak M, Haggmark T, Efendic S. Glucose infusion instead of preoperative fasting reduces postoperative insulin resistance. J Am Coll Surg 1994 Apr;178(4): Thorell A, Efendic S, Gutniak M, Häggmark T, Ljungqvist O. Insulin resistance after abdominal surgery. Br J Surg 1994 Jan;81(1): Thorell A, Nygren J, Ljungqvist O. Insuline resistance: A marker of surgical stress. Curr Opin Clin Nutr Metab Care 1999 Jan;2(1): Cheatham ML, Chapman WC, Key SP, Sawyers JL. A meta-analysis of selective versus routine nasogastric decompression after elective laparotomy. Ann Surg 1995 May;221(5): Urbach DR, Kennedy ED, Cohen MM. Colon and rectal anastomoses do not require routine drainage: A systematic review and meta-analysis. Ann Surg 1999 Feb;229(2):
7 20. Jesus EC, Karliczek A, Matos D, Castro AA, Atallah AN. Prophylactic anastomotic drainage for colorectal surgery. Cochrane Database Syst Rev 2004 Oct 18;(4):CD Fearon KC, Ljungqvist O, Von Meyenfeldt M, et al. Enhanced recovery after surgery: A consensus review of clinical care for patients undergoing colonic resection. Clin Nutr 2005 Jun;24(3): Jorgense H, Wetterslev J, Moiniche S, Dahl JB. Epidural local anaesthetics versus opioid-based analgesic regimens on postoperative gastrointestinal Rios-Cruz et al. 15 paralysis, PONV and pain after abdominal surgery. Cochrane Database Syst Rev 2000;(4):CD Lewis SJ, Egger M, Sylvester PA, Thomas S. Early enteral feeding versus nyl by mouth after gastrointestinal surgery: Systematic review and meta-analysis of controlled trials. BMJ 2001 Oct 6;323(7316): Kehlet H, Wilmore DW. Multimodal strategies to improve surgical outcome. Am J Surg 2002 Jun;183(6): About the Authors Article citation: Rios-Cruz D, Valerio-Ureña J, Hernández-Ascencio JA, Galindo-López P, Torres-Medina V. Fast track surgery for biliodigestive derivation: Initial experience. Int J Hepatobiliary Pancreat Dis 2015;5:9 16. Daniel Rios Cruz is Surgeon at Hospital de Alta Especialidad de Veracruz. He earned undergraduate degree of General Medicine from Facultad de Medicina de la Universidad Autonoma de Yucatán, México and postgraduate degree as General Surgeon from Universidad Veracruzana in Veracruz, Veracruz, Mexico. He has a high speciality course in bariatric surgery and laparoscopic gastrointestinal advanced surgery. He has published many research papers in national and international academic journals and authored an electronic book Topicos selectos de gastroenterologia wich will be available very soon. His research interests include obesity surgery, hepatopancreatobiliary surgery and fast track surgery. jobzon@hotmail.com Joaquin Valerio Ureña is Chief of the division of surgery at Hospital de Alta Especialidad de Veracruz in Mexico. He earned undergraduate degree General Medicine from Universidad Veracruzana and postgraduate degree from General Surgeon from Centro Medico Nacional Siglo XXI del IMSS. He has a highly specialized course in gastrointestinal endoscopy and digestive physiology and motility at Instituto Nacional de Nutricion y Ciencias Médicas Salvador Zubiran in Mexico. He has published many research papers in national and international academic journals and authored chapters in books. His search interests include fast track sugery, gastrointestinal physiology and hepatopancreatobiliary surgery. drjvalerio@hotmail.com Julio Abraham Hernández Ascencio is General Surgeon at Hospital General de Boca del Rio Veracruz, México. He earned undergraduate degree Medico General from Facultad de Medicina de la Universidad Autónoma de Yucatán en Mérida, Yucatán, México and postgraduate degree form Cirujano General from Hospital de Alta Especialidad de Veracruz; Universidad Veracruzana. Veracruz, Veracruz, México. His research interests include gastrointestinal surgery. jahascencio@hotmail.com Dra. Patricia Galindo López is a medicine student at Facultad de Medicina, Universidad Veracruzana. Her research interest includes gastrointestinal physiology. pattygalindo91@hotmail.com Dra Veronica Torres Medina is Anesthesiologist at highly specialized hospital of Veracruz. She studied General Medicine at Universidad Michoacana de San Nicolas de Hidalgo. Morelia, Michoacan, México and Specialty in Anesthesiology in Hospital de Especialidades del Centro Médico Nacional SIGLO XXI, IMSS, México. verotom272@yahoo.com.mx
8 Rios-Cruz et al. 16 Access full text article on other devices Access PDF of article on other devices
Enhanced Recovery Initiative
 Enhanced Recovery Initiative On February 14, 2012, the Colon and Rectal Surgery Service at St Joseph Mercy Hospital, Ann Arbor, launched the Enhanced Recovery Initiative, a collection of evidence-based
Enhanced Recovery Initiative On February 14, 2012, the Colon and Rectal Surgery Service at St Joseph Mercy Hospital, Ann Arbor, launched the Enhanced Recovery Initiative, a collection of evidence-based
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy)
 Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Patient Information and Daily Programme for Patients Having Whipple s Surgery (Pancreatico duodenectomy) Date of admission Date of surgery Expected Length of Stay in hospital We will aim to discharge you
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Laparoscopic Cholecystectomy
 National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Consultant Surgeon DRAFT VERSION 0.5 090415 Table of Contents 1.0 Purpose... 3 2.0 Scope... 3 3.0 Responsibility...
National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Consultant Surgeon DRAFT VERSION 0.5 090415 Table of Contents 1.0 Purpose... 3 2.0 Scope... 3 3.0 Responsibility...
The Patient s Guide. Pancreaticoduodenectomy (Whipple) Surgery. Where life shines bright.
 Pancreaticoduodenectomy (Whipple) Surgery The Patient s Guide Where life shines bright. SM Methodist Dallas Medical Center 1441 N. Beckley Ave. Dallas, TX 75203 214-947-8181 MethodistHealthSystem.org Find
Pancreaticoduodenectomy (Whipple) Surgery The Patient s Guide Where life shines bright. SM Methodist Dallas Medical Center 1441 N. Beckley Ave. Dallas, TX 75203 214-947-8181 MethodistHealthSystem.org Find
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
GIANT HERNIA REPAIR MY EXPERIENCE
 GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
Bowel Preparation for Colon Resection. Eric Klein, M.D. SUNY Downstate Department of Surgery
 Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Preparing for your Surgery:
 Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Understanding Laparoscopic Colorectal Surgery
 Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Laparoscopic Sleeve Gastrectomy. Patient information leaflet. www.londonbariatricgroup.co.uk
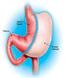 Laparoscopic Sleeve Gastrectomy Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Laparoscopic Sleeve Gastrectomy Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Laparoscopic Cholecystectomy (Removal of the Gallbladder)
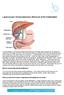 Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Oxford University Hospitals
 Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Rapid Mobilization Decreases Length-of-Stay in Joint Replacement Patients
 222 Rapid Mobilization Decreases Length-of-Stay in Joint Replacement Patients Gregory Tayrose, M.D., Debbie Newman, B.S., James Slover, M.D., M.S., Fredrick Jaffe, M.D., Tracey Hunter, B.S., and Joseph
222 Rapid Mobilization Decreases Length-of-Stay in Joint Replacement Patients Gregory Tayrose, M.D., Debbie Newman, B.S., James Slover, M.D., M.S., Fredrick Jaffe, M.D., Tracey Hunter, B.S., and Joseph
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Beverly Morningstar MD, FRCP(C) Elaine Avila RN, BScN
 Beverly Morningstar MD, FRCP(C) Elaine Avila RN, BScN Outline The University of Toronto ERAS guideline introduction to ERAS how we created the guideline specific elements of guideline with evidence Implementation
Beverly Morningstar MD, FRCP(C) Elaine Avila RN, BScN Outline The University of Toronto ERAS guideline introduction to ERAS how we created the guideline specific elements of guideline with evidence Implementation
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Laparoscopic Gastric Bypass. Patient information leaflet. www.londonbariatricgroup.co.uk
 Laparoscopic Gastric Bypass Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Laparoscopic Gastric Bypass Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS
 YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Endovascular Abdominal Aortic Aneurysm Repair Surgery
 Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
What is the Sleeve Gastrectomy?
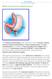 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
restricted to certain centers and certain patients, preferably in some sort of experimental trial format.
 Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Inguinal hernia repair
 Inguinal hernia repair A hernia is an abnormal protrusion on an organ through a weakness in the abdominal wall. The abdominal muscles are usually strong enough to keep your internal organs in place, when
Inguinal hernia repair A hernia is an abnormal protrusion on an organ through a weakness in the abdominal wall. The abdominal muscles are usually strong enough to keep your internal organs in place, when
Percutaneous Abdominal or Pelvic Drain What to expect
 Patient Education Percutaneous Abdominal or Pelvic Drain What to expect This handout explains what percutaneous abdominal or pelvic drain is and what to expect when you have one. What is a percutaneous
Patient Education Percutaneous Abdominal or Pelvic Drain What to expect This handout explains what percutaneous abdominal or pelvic drain is and what to expect when you have one. What is a percutaneous
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson
 The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Endoscopic Management of Strictures and Leaks. Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center
 Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Feeding in Infants with Complex Congenital Heart Disease. Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014
 Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
University College Hospital. Laparoscopic gastric bypass. Centre for Weight Loss, Metabolic and Endocrine Surgery
 University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Whipple Procedure: A guide for patients and families UHN
 Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH)
 GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
The Patient s Guide. Distal Pancreatectomy with Splenectomy Surgery. Where life shines bright.
 Distal Pancreatectomy with Splenectomy Surgery The Patient s Guide Where life shines bright. SM Methodist Dallas Medical Center 1441 N. Beckley Ave. Dallas, TX 75203 214-947-8181 MethodistHealthSystem.org
Distal Pancreatectomy with Splenectomy Surgery The Patient s Guide Where life shines bright. SM Methodist Dallas Medical Center 1441 N. Beckley Ave. Dallas, TX 75203 214-947-8181 MethodistHealthSystem.org
INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE
 INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE Hughes MS, Matava MJ, et al. Interscalene Brachial Plexus Block for Arthroscopic Shoulder Surgery.
INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE Hughes MS, Matava MJ, et al. Interscalene Brachial Plexus Block for Arthroscopic Shoulder Surgery.
Elective Laparoscopic Cholecystectomy
 General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
REPAIR OF A URINARY VAGINAL FISTULA
 Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
Procedure Specific Information What is the evidence base for this information? This publication includes advice from consensus panels, the British Association of Urological Surgeons, the Department of
PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY
 PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY University Colon & Rectal Surgery Removal of a portion of the small bowel, colon, or rectum is a major operation. After a period of hospitalization
PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY University Colon & Rectal Surgery Removal of a portion of the small bowel, colon, or rectum is a major operation. After a period of hospitalization
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE
 VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
Having a Gastric Band
 Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Biliary Stone Disease
 Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
LAPAROSCOPIC GASTRIC BANDING
 LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
Preoperative Education: LUMBAR SPINE SURGERY
 Preoperative Education: LUMBAR SPINE SURGERY 1 Dear Patient, In order to make your hospital stay as comfortable as possible, we have prepared this informational packet for you designed to outline and explain
Preoperative Education: LUMBAR SPINE SURGERY 1 Dear Patient, In order to make your hospital stay as comfortable as possible, we have prepared this informational packet for you designed to outline and explain
