The overactive bladder
|
|
|
- Laurence Nichols
- 9 years ago
- Views:
Transcription
1 BJU International (2001), 88, 135±140 The overactive bladder J.J. WYNDAELE Department of Urology, Faculty of Medical and Pharmaceutical Sciences, University Antwerpen, Antwerpen, Belgium Introduction The term `overactive bladder' has been used sporadically for many years; according to the original de nition of the ICS, the overactive bladder refers to the storage phase of the bladder and is diagnosed by urodynamics [1]. The overactivity is caused by involuntary detrusor muscle contractions that occur while the patient is trying to inhibit voiding. If caused by a neurological disease the overactive bladder was referred to as hyper-re exic, and if by a non-neurogenic or unknown cause, as unstable. A different terminology will probably be proposed in the near future as it has become clear that the current nomenclature is unsuitable for many patients and does not correspond with the clinical reality [2]. Abrams and Wein [2] suggested the following de nition: `the overactive bladder is a medical condition referring to the symptoms of frequency and urgency, with or without urge incontinence, when appearing in the absence of local pathology or metabolic factors that would account for these symptoms'. Incontinence is not a necessary condition for diagnosis, because about half of those with an overactive bladder are not incontinent. This proposal starts from a very different perspective from the original de nition; it would seem to accept that the involuntary bladder contractions can be symptomatic or not, the symptomatic form being termed overactivity. This is common knowledge to many physicians involved in urodynamic studies. For the overactive bladder to be symptomatic, an overactivity of the bladder muscle must occur at volumes below the patient's functional bladder capacity and should occur under circumstances of normal daily activity. Moreover, the proposal accepts that the involuntary detrusor contractions should be felt by the patient. The exact relationship between the sensation of urgency and muscle activity of the bladder is not clear. There is some doubt about the relationship of urgency and detrusor pressure increase, because many patients with complaints of urgency do not have motor overactivity. Turner-Warwick once called unstable detrusor contractions a `variant of normality' and this might be the case in some patients [3]. Thus there seems currently to be a transitional period of developing a de nition of what is generally to be accepted as a true overactive bladder. However, whatever de nition is nally adopted, symptomatic bladder overactivity is a very bothersome problem that can signi cantly reduce the quality of life of affected individuals. Current aetiological concepts Ideas for the cause of the overactive bladder are based on increasing knowledge about lower urinary tract physiology. There is ample evidence that micturition and bladder lling are independently organized in the brain; the pontine micturition centre and the pontine storage centre (PSC) in the cat do not seem to be interconnected at the level of the brainstem [4]. The group of neurones in the pons involved in the storage of urine is known as the PSC group or L-region, and projects to the motor neurones of the urethral sphincter in the nucleus of Onuf [5]. Bilateral lesions in the PSC cause an inability to store urine; bladder capacity is reduced and urine is expelled prematurely by excessive detrusor activity, accompanied by urethral relaxation. There is also a PSC in humans [6]. Most of the time bladder control is modulated in an inhibitory fashion by the diencephalic and cerebral cortex functions, the cerebral cortex being responsible for the timing of the control. Neurological de cits in these regions are known to be possible causes of bladder overactivity [7]. Lesions between the pontine and sacral micturition centre may cause neurological detrusor overactivity. Pathological afferent pathways might be important, as shown by the bene cial effect of electrical stimulation on these nerves in inhibiting detrusor function [8]. Abnormalities of bladder smooth muscle have been related to the occurrence of bladder overactivity. Prolonged obstruction could have an in uence through structural deformation of the bladder smooth muscle, an increased production of nerve growth factor and induced neuronal enlargement [9]. Urethral resistance in women with an overactive bladder was much higher than that in women with no abnormality on urodynamic studies [10]. However, obstruction could lead to partial denervation, inducing denervation supersensitivity [11]; it could also # 2001 BJU International 135
2 136 J.J. WYNDAELE have metabolic effects through the generation of free radicals and lipid peroxidases [12]. Little has been published so far on a possible dysfunction in the sensory nervous system, although clinical data are in favour of such a cause of overactivity [13]. The possible role of urinary potassium on bladder overactivity through the A-delta and C- bres corresponds with a similar pathogenesis [14]. Symptomatology of the overactive bladder The clinical relationship between incontinence and the overactive bladder can be very variable. In patients with bladder overactivity there may be several groups with a different clinical picture, i.e. with frequency and urgency, with frequency, urgency and urge incontinence, with mixed incontinence (stress and urge), or with no apparent symptoms, where motor overactivity is discovered during urodynamic investigations undertaken for another reason. This last group probably needs no further diagnosis or treatment if the bladder contractions are really asymptomatic and unrelated to what caused the patients to initially consult their physician. Epidemiology of the overactive bladder Prevalence studies of the overactive bladder differ widely in the methods applied, survey populations and results; there is no conformity in their de nition of the symptomatology, survey methods and validation. The prevalence of the overactive bladder has also probably been underestimated because many studies have been limited to patients with incontinence. This overlooks many people, mostly men, who are signi cantly troubled by frequency and urgency as a consequence of an overactive bladder. The condition is probably more common in women than in men. The results of a Gallup study in six European countries give an overall incidence of 17% of adults having one or more symptoms of an overactive bladder. That survey also showed that the incidence consistently increased with advancing age [2]. Diagnostic assessment of the overactive bladder From the de nitions given above it can be assumed that a detailed history is the key to diagnosing bladder overactivity in most cases. Frequency, urgency and urge incontinence alone or in combination form the basic group of symptoms of possible bladder overactivity. Anatomical, neurological and infectious causes should be excluded rst, with a preliminary clinical examination and urine analysis. Primary-care physicians and many urologists will probably proceed no further with a diagnostic evaluation if these tests reveal no obvious pathology, but will initiate some form of treatment. Urodynamic tests are needed when the probable diagnosis is unclear, if a neuropathy is suspected or if therapy has been unsuccessful. Conventional laboratory urodynamics failed to detect any abnormality in >35% of patients in the study by van Waalwijk van Doorn [15]. Ambulatory urodynamic monitoring would seem to be better than conventional lling cystometry, as motor overactivity of the detrusor is more frequently detected [16]. However, again it would seem appropriate to accept that only if pressure rises correspond with the signs and symptoms do they have any diagnostic value for the overactive bladder, as changes in detrusor pressure can also be detected in many asymptomatic subjects [17]. Overactive bladder and quality of life An overactive bladder has a detrimental effect on quality of life; in most domains (physical functioning, social functioning, vitality, role limitations) affected patients score signi cantly worse than do age-matched controls. Compared with the quality of life of patients with diabetes, hypertension and depression, only depression has a greater effect [18]. Treatment The medical management of the overactive bladder has been a major concern for those involved in treatment during the last few decades. Several different aspects have been studied and methods of treatment evaluated; these are behavioural therapy, pelvic oor therapy, muscarinic receptor antagonists and other drugs, and intravesical treatment. Behavioural therapy is one of the best single-treatment options as it has no risk and gives very acceptable results. The therapy should start with education and an explanation of normal lower urinary tract function, and the dynamic and clinical aspects of overactivity. When the patient understands what actually happens, he/she can better interpret the signs and symptoms after unstable bladder contractions. More information can be obtained from voiding charts and diaries; by completing these and by discussing them, the symptoms can be related to daily living. When this knowledge has been acquired, training can start with timed voiding and bladder training regimens (`bladder drill'). This includes training to perceive the early signs of an overactive contraction (the `warning'), urge inhibition, delayed voiding and reinforcement of these steps when successful. Fluid management is another important part of managing overactivity. A voiding diary is often the basis for evaluating and
3 THE OVERACTIVE BLADDER 137 setting goals, aiming for a better control of the bladder with a reasonable voiding interval and no incontinence. Training for good micturition habits can be useful. Behavioural therapy can be combined with other forms of treatment, e.g. drugs and pelvic oor exercises. This also facilitates the treatment of patients with mixed incontinence, a functional problem or pelvic oor disorders. Reassurance of the patient is always helpful and speci c psychological help might be needed in some cases [19]. Behavioural therapy is effective, with published success rates of >50%, although the long-term results seem to be lower [20]. Most clinicians would agree that every patient with bladder overactivity should be provided with at least the basics of behavioural therapy. Pelvic oor physiotherapy consists of several different techniques applied to treat the overactive bladder. Pelvic oor muscle exercises have been used to try to stop the developing autonomic contractions by squeezing the pelvic oor muscles. To date, published data do not allow a rm conclusion that this method is clinically successful, especially in the long term, although theoretically the method should work. Contraction of the pelvic oor muscles, electrically stimulated or voluntary, provides re ex inhibition of the detrusor muscle [21,22]; this provides the rationale to further explore its therapeutic value. Electrical stimulation is an effective and well-tolerated treatment for the overactive bladder; it is considered to be a neuromodulating therapy which affects the neural signalling that controls continence. There is also an effect in striated muscles, causing hypertrophy of the muscles by recruiting fast-twitch bres which would not be affected by exercise alone. Studies show that the use of vaginal electrical stimulators can reduce the occurrence of symptoms of an overactive bladder in about half of the patients treated [23]. However, the objective ndings do not seem to correlate well with the subjective improvement. Biofeedback is a type of learning or re-education which helps to retrain the patient. Information about one or more of the patient's physiological processes is presented to the patient as a visual, auditory or tactile signal. For bladder overactivity, biofeedback has been used to relate immediately the changes in intravesical pressure (bladder or cystometric biofeedback) and as a method of pelvic oor training. As with all training programmes, biofeedback needs considerable effort from the patient and the training physiotherapist; patients also need to be well motivated and intelligent enough to understand what is expected of them. Those who guide the training must be motivated, skilful and maintain good contact with the patients. Biofeedback has few side-effects and can be used as an adjunct with other forms of treatment. The original technique for biofeedback in managing idiopathic detrusor instability was described in 1978 [24]. Bladder biofeedback gave very acceptable results in two studies by the present author, one in adults and one in children [25,26]. As patients are able to visualise directly the development of intravesical pressure during bladder lling, they can learn to feel the sensory signals that accompany the unstable contractions, and can thus try to stop them with active contractions of the sphincter and pelvic oor. We noted that the problem could be controlled more effectively but that the unstable contractions continued in most of those treated with this technique. This could explain why some patients who were initially cured relapsed in the long term, but the training can be repeated successfully. Cystometric biofeedback is invasive and should therefore be used mostly in refractory cases. Complications such as urinary infection are very rare. Pelvic oor biofeedback has been assessed by several groups, with variable results; the technique has the best chance of success as part of a comprehensive treatment programme [27]. Such biofeedback can use the electromyographic activity of the urethral or anal sphincter or of the pelvic oor; it can also be used to follow pressure changes in the anal canal or in the vagina, measured through balloon catheters. Published results are few and not always easy to interpret because of a possible bias in patient selection, variations in methodology or in the combinations of treatment given. There is a need for randomized controlled trials to determine its optimum place in treatment programmes. The technique causes almost no complications or sideeffects. Muscarinic receptor antagonists These drugs still form the mainstay of treatment for the overactive bladder and there is ample clinical evidence that they are effective. However, the side-effects limit their use, especially those of dry mouth, constipation and blurred vision. Oxybutynin has been used for many years and has good clinical ef cacy [28]. To limit its side-effects, alternative routes of administration have been used [29]; extended-release oral formulations and stimulation of salivation were assessed to improve this bothersome symptom. There have been advances in the understanding of muscarinic receptors and bladder function which have lead to the search for tissue- or subtypeselective antimuscarinic agents with improved tolerability. Tolterodine and darifenacin are being increasingly used in clinical practice; the side-effects from these drugs appear to be less and the drugs more speci c [30,31]. Several questions remain, e.g. about the effect of longterm treatment, and whether adaptation occurs after
4 138 J.J. WYNDAELE prolonged periods of use, so that drugs might need to be changed at regular intervals. Other drugs Imipramine, duloxetine, drugs affecting noradrenaline, dopamine or cxaminobutyric acid receptors, and a1-adrenoceptor antagonists, have all been assessed, with some success. Potassium-channel openers, prostaglandins, selective or nonselective inhibitors of cyclooxygenase, and drugs that reduce afferent activity are possible ways of pharmacological treatment that have been explored. Intravesical treatment has attracted some interest; this route of administration tends to reduce the parasympathetic efferent activity or to cause de-afferentiation of the bladder. Intravesical oxybutynin has been used mainly in patients with a neuropathic bladder who also use intermittent self-catheterization [29]. Capsaicin and resiniferatoxin are under study [32]. The injection of botulin toxin into the detrusor muscle to treat bladder hyper-re exia has been assessed in patients with neurological bladder overactivity and seems to give promising results [33]. Thus the medical management of the overactive bladder is constantly developing; however, for several other methods a proper evaluation is not yet possible because there are few controlled studies, but their use can still be advocated as most have no side-effects, are harmless and based on plausible hypotheses. The best approach is to initiate the treatment of idiopathic bladder overactivity with behavioural training, physiotherapy and drugs. Surgical management Denervation techniques were popular for some time but have been gradually abandoned. Bladder transection by open surgery, endoscopic or transvesical phenolization, hyperbaric bladder distension and peripheral denervation of the bladder provided promising early results but the long-term outcome was poor. Currently sacral de-afferentiation by dorsal root rhizotomy of S2±S5 is successful in patients with a complete supraspinal cord lesion [34]. Sacral neuromodulation has become popular, probably because it bridges the gap between conservative treatment and highly invasive options. Sacral neuromodulation comprises three main stages; the percutaneous location of the sacral spinal nerves with a needle electrode, percutaneous test stimulation with wire electrodes to assess the therapeutic potential in each patient over a period of a few days, and implantation of a stimulation system if the second stage was successful. At present there are no clinical variables that can reliably predict the ef cacy of neuromodulation in an individual patient. All patients must have a test stimulation before having an implant, but success with the test does not always mean certain success with the implant. Some centres report a close match between those responding in the subchronic and chronic effects of sacral neuromodulation; in contrast, others report therapeutic failure rates in up to half of patients during chronic sacral neuromodulation, despite good responses to the shorter test trials. Several clinical studies reported signi cant therapeutic success for neuromodulation in patients with bladder overactivity, especially if detrusor overactivity could be detected [35,36]. The complication rate for neuromodulation is low, but the technique is expensive and should preferably be offered to those with symptoms refractory to conservative treatment. There are arguments that the stimulation operates through the afferent nerves [37] but the exact mode of action remains to be elucidated. Bladder augmentation Gastrointestinal segments are commonly used for bladder replacement and augmentation. These techniques are needed infrequently in patients with an overactive bladder but the rare refractory patient with substantial symptoms may bene t from them. However, contact between gastrointestinal tissue and urine can induce several complications. Autoaugmentation has been successful in several series and many new techniques are being developed after experimental assessment and will soon appear in clinical practice if the clinical results are good. De-epithelialized bowel segments have been used and a system of progressive dilatation for ureters and bladders described. There is a new interest in the use of acellular collagen-based matrices as scaffolds for bladder regeneration. Recently, bladder tissue has been engineered using selective cell transplantation techniques, such that the tissue can be used in children and adults. Tissue is taken from the host, the cells are dissociated and expanded in vitro, re-attached to a matrix and implanted in the same host. The prospects are good but the results of the clinical applications are awaited [38]. Summary The overactive bladder causes frequency, urgency and/or urge incontinence, and may have a signi cant effect on quality of life. The de nition of the overactive bladder needs clari cation and this should help to overcome the current confusion. Possible neurological, muscular and metabolic causes have been proposed but in many cases
5 THE OVERACTIVE BLADDER 139 the exact cause remains unclear. The diagnosis depends greatly on a detailed history, clinical examination and urine analysis. Urodynamic investigations are indicated when neuropathy is suspected, the treatment remains unsuccessful or if there is doubt about the exact situation. The overactive bladder can be treated conservatively, by training, physiotherapy and drugs. For refractory cases neuromodulation, denervation techniques and bladder augmentation may be indicated. References 1 Abrams PH, Blaivas JG, Stanton SL, Andersen JT. Standardization of terminology of lower urinary tract function. Neurourol Urodyn 1988; 7: 403±7 2 Abrams P, Wein AJ. Introduction: overactive bladder and its treatments. Urology 2000; 55 (Suppl 5A): 1±2 3 Wyndaele JJ. The normal pattern of perception of bladder lling during cystometry studied in 38 young healthy volunteers. J Urol 1998; 160: 479±81 4 Blok BFM, Holstege G. The two pontine micturition centers in the cat are not interconnected: implications for the central organization of micturition. J Comp Neurol 1999; 403: 209±18 5 Holstege G, Grif ths D, De Wall H, Dalm E. Anatomical and physiological observations on supraspinal control of bladder and urethral sphincter muscles in the cat. J Comp Neurol 1986; 250: 449±61 6 Blok BFM, Willemsen ATM, Holstege G. A PET study on brain control of micturition in humans. Brain 1997; 120: 111±21 7 Blaivas JG. The neurophysiology of micturition: a clinical study of 550 patients. J Urol 1982; 127: 958±63 8 Vodusek DB, Plevnik S, Janez J, Vrtacnik P. Detrusor inhibition on selective pudendal nerve stimulation in the perineum. Neurourol Urodyn 1988; 6: 389±93 9 Steers WD, de Groat WC. Effect of bladder outlet obstruction on micturition re ex pathways in the rat. J Urol 1988; 140: 864±71 10 Bosch R, Groen J. Urethral resistance is related to type of incontinence: changing etiologic concepts in female incontinence. Neurourol Urodyn 1998; 17: 386±8 11 Brading AF, Turner WH. The unstable bladder: towards a common mechanism. Br J Urol 1994; 73: 3±8 12 Levin RM. Potential future pharmacological approaches. Urology 1997; 50 (Suppl. 6A): 87±8 13 Wyndaele JJ. La sensation du bas appareil urinaire est-elle diffeârente chez des patients ayant une instabiliteâ veâsicale? ProgreÁs En Urologie 1992; 2: 220±5 14 Hohlbrugger G. Urinary potassium and the overactive bladder. BJU Int 1999; 83 (Suppl. 2): 22±8 15 Van Waalwijk van Doorn ESC. Ambulatory urodynamics: from physiological research to daily practice. Thesis. University of Maastricht, The Netherlands Porru D, Usai E. Standard and extramural ambulatory investigation for the diagnosis of detrusor instabilitycorrelated incontinence and micturition disorders. Neurourol Urodyn 1994; 13: 237±42 17 Wyndaele JJ. Normality of urodynamics studied in healthy volunteers. J Urol 1999; 161: 899± Kobelt-Nguyen G, Johannesson M, Mattiasson A, Abrams P. Correlations between symptoms of urge incontinence and scores of a generic quality of life instrument (SF36) and health status measurements (EuroQol) and between changes in symptoms and QoL scores. Abstract 195. Presented at the 27th Annual meeting of ICS, Yokohama, Japan, September 23± :165±6 19 Frewen WK. The management of urgency and frequency of micturition. Br J Urol 1980; 52: 367±9 20 Payne CK. Behavioral therapy for overactive bladder. Urology 2000; 55 (Suppl. 5A): 3±6 21 Godec C, Cass AS, Ayala GF. Bladder inhibition with functional electrical stimulation. Urology 1975; 6: 663±6 22 Bo K, Berghmans LCM. Nonpharmacologic treatments for overactive bladder - pelvic oor exercises. Urology 2000; 55 (Suppl. 5A): 7±11 23 Brubacker L. Electrical stimulation in overactive bladder. Urology 2000; 55 (Suppl. 5A): 17±23 24 Cardozo L. Biofeedback in overactive bladder. Urology 2000; 55 (Suppl. 5A): 24±8 25 Wyndaele JJ, Hoekx L, Vermandel A. Bladder biofeedback for the treatment of refractory sensory urgency in adults. Eur Urol 1997; 32: 429±32 26 Hoekx L, Wyndaele JJ, Vermandel A. The role of bladder biofeedback in the treatment of children with refractory nocturnal enuresis associated with idiopathic detrusor instability and small bladder capacity. J Urol 1998; 160: 858±60 27 Fall M. Discussion: reactivation of bladder inhibitory re exes ± an underestimated asset in the treatment of overactive bladder. Urology 2000; 55 (Suppl. 5A): 29±30 28 Diokno A, Lapides J. Oxybutynin: a new drug with analgesic and anticholinergic properties. J Urol 1972; 108: 307±9 29 Madersbacher H, Jilg G. Control of detrusor hyperre exia by intravesical instillation of oxybutynin hydrochloride. Paraplegia 1991; 29: 84±90 30 Larsson G, HalleÂn B, Nilverbrant L. Tolterodine in the treatment of overactive bladder: analysis of the pooled phase II ef cacy and safety data. Urology 1999; 53: 990±8 31 Rosario D, Cutinha P, Chapple C, Milroy E. The effects of single dose darfenacin on cystometric parameters and salivary ow in patients with urge incontinence secondary to detrusor instability. Eur Urol 1996; 30 (Suppl. 2): 240A Fowler CJ, Beck RO, Gerrard S, Betts CD, Fowler CG. Intravesical capsaicin for treatment of detrusor hyperre- exia. J Neurol Neurosurg Psychiatry 1994; 57: 169±73 33 StoÈhrer M, Schurch B, Kramer G, Schmid D, Gaul G, Haun D. Botulinum A-toxin in the treatment of detrusor hyperre exia in spinal cord injured patients: a new alternative to medical and surgical procedures? Neurourol Urodyn 1999; 18: 401±2 A Madersbacher H. Denervation techniques. BJU Int 2000; 85 (Suppl. 3): 1±6 35 Hassouna MM, Siegel SW, Nyeholt AA et al. Sacral neuromodulation in the treatment of urgency-frequency
6 140 J.J. WYNDAELE symptoms: a multicenter study on ef cacy and safety. J Urol 2000; 163: 1849±54 36 Everaert K, De Ridder D, Baert L, Oosterlinck W, Wyndaele JJ. Patient satisfaction and complications following sacral nerve stimulation for urinary retention, urge incontinence and perineal pain: a multicenter evaluation. Int Urogynecol J 2000; 11: 231±6 37 Wyndaele JJ, Michielsen D, Van Dromme S. In uence of neuromodulation on electrosensation in the lower urinary tract. J Urol 2000; 163: 221±4 38 Atala A. New methods of bladder augmentation. BJU Int 2000; 85 (Suppl. 3): 24±34 Author J.J. Wyndaele, MD, DSc, PhD, FEAU, Department of Urology, University Hospital Antwerpen, 10 Wilrijkstraat, B-2650, Edegem, Belgium. [email protected]
Overactive Bladder (OAB) Content of the lecture
 Overactive bladder (OAB) : Introduction and Medical Management R.J. Opsomer Cliniques St Luc, labo d urodynamique, UCL - Bruxelles Overactive Bladder (OAB) Content of the lecture The syndrome of Overactive
Overactive bladder (OAB) : Introduction and Medical Management R.J. Opsomer Cliniques St Luc, labo d urodynamique, UCL - Bruxelles Overactive Bladder (OAB) Content of the lecture The syndrome of Overactive
Urinary Continence. Second edition FAST FACTS. by Julian Shah and Gary Leach. Anatomy and physiology 7. Investigations and diagnosis 11
 FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE
 in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
Urinary Incontinence in Women. Susan Hingle, M.D. Department of Medicine
 Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL
 GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Overactive bladder syndrome (OAB)
 Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
Classification of Mixed Incontinence
 european urology supplements 5 (2006) 837 841 available at www.sciencedirect.com journal homepage: www.europeanurology.com Classification of Mixed Incontinence Christopher Chapple * Sheffield Hallam University,
european urology supplements 5 (2006) 837 841 available at www.sciencedirect.com journal homepage: www.europeanurology.com Classification of Mixed Incontinence Christopher Chapple * Sheffield Hallam University,
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
It usually presents with a sudden urge to urinate that is very difficult to delay and may be associated with leakage. Other features include:
 visited on Page 1 of 5 View this article online at http://patient.info/doctor/overactive-bladder Overactive Bladder This PatientPlus article is written for healthcare professionals so the language may
visited on Page 1 of 5 View this article online at http://patient.info/doctor/overactive-bladder Overactive Bladder This PatientPlus article is written for healthcare professionals so the language may
URINARY INCONTINENCE
 URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
Urinary Incontinence: an overview!! Neil Harris Consultant Urological Surgeon, Leeds
 Urinary Incontinence: an overview!! Neil Harris Consultant Urological Surgeon, Leeds Content 1. Epidemiology of pelvic floor dysfunction Urinary incontinence Bowel dysfunction Sexual dysfunction 2. Treatment
Urinary Incontinence: an overview!! Neil Harris Consultant Urological Surgeon, Leeds Content 1. Epidemiology of pelvic floor dysfunction Urinary incontinence Bowel dysfunction Sexual dysfunction 2. Treatment
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
TIBIAL NERVE STIMULATION: ONE OF SEVERAL NEW OPTIONS FOR THE MANAGEMENT OF OVERACTIVE BLADDER IN WOMEN
 TIBIAL NERVE STIMULATION: ONE OF SEVERAL NEW OPTIONS FOR THE MANAGEMENT OF OVERACTIVE BLADDER IN WOMEN Scott A Farrell MD Professor Dept of Obstetrics and Gynaecology Dalhousie University Declaration of
TIBIAL NERVE STIMULATION: ONE OF SEVERAL NEW OPTIONS FOR THE MANAGEMENT OF OVERACTIVE BLADDER IN WOMEN Scott A Farrell MD Professor Dept of Obstetrics and Gynaecology Dalhousie University Declaration of
Overactive bladder and urgency incontinence
 Overactive bladder and urgency incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing
Overactive bladder and urgency incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing
THE ROLE OF OVERACTIVE BLADDER TREATMENT
 THE ROLE OF OVERACTIVE BLADDER TREATMENT Prof. Junizaf, SpOG(K) Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
THE ROLE OF OVERACTIVE BLADDER TREATMENT Prof. Junizaf, SpOG(K) Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
Mixed urinary incontinence - sling or not sling
 Mixed urinary incontinence - sling or not sling 吳 銘 斌 Ming-Ping Wu, M.D.,Ph.D. Director, Div. Urogynecology & Pelvic Floor Reconstruction, Chi Mei Foundation Hospital, Tainan, Taiwan Assistant Professor,
Mixed urinary incontinence - sling or not sling 吳 銘 斌 Ming-Ping Wu, M.D.,Ph.D. Director, Div. Urogynecology & Pelvic Floor Reconstruction, Chi Mei Foundation Hospital, Tainan, Taiwan Assistant Professor,
FEMALE INCONTINENCE REVIEW
 200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
Lower Urinary Tract Symptoms (LUTS) in Middle-Aged and Elderly Men
 Prostatic Diseases Lower Urinary Tract Symptoms (LUTS) in Middle-Aged and Elderly Men JMAJ 47(12): 543 548, 2004 Tomonori YAMANISHI Associate Professor, Department of Urology, Dokkyo University School
Prostatic Diseases Lower Urinary Tract Symptoms (LUTS) in Middle-Aged and Elderly Men JMAJ 47(12): 543 548, 2004 Tomonori YAMANISHI Associate Professor, Department of Urology, Dokkyo University School
Female Urinary Incontinence
 Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
Management of Urinary Incontinence. Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine)
 Management of Urinary Incontinence Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine) Managing Urinary Incontinence Urinary incontinence is very prevalent among older animals. In this group
Management of Urinary Incontinence Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine) Managing Urinary Incontinence Urinary incontinence is very prevalent among older animals. In this group
Urinary Incontinence Dr. Leffler
 Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 18 December 2002 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON THE
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 18 December 2002 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON THE
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Overactive bladder is a common condition thought to. women, and is a serious condition that can lead to. significant lifestyle changes.
 Overactive bladder is a common condition thought to FADE UP TO WIDE SHOT OF FEMALE MODEL WITH TRANSPARENT SKIN. URINARY BLADDER VISIBLE IN PELVIC REGION affect over 16 percent of adults. It affects men
Overactive bladder is a common condition thought to FADE UP TO WIDE SHOT OF FEMALE MODEL WITH TRANSPARENT SKIN. URINARY BLADDER VISIBLE IN PELVIC REGION affect over 16 percent of adults. It affects men
Women suffer in silence
 Women suffer in silence Stress urinary incontinence is the involuntary loss of urine resulting from increased intra-abdominal pressure. In people who suffer with this condition, forms of exertion such
Women suffer in silence Stress urinary incontinence is the involuntary loss of urine resulting from increased intra-abdominal pressure. In people who suffer with this condition, forms of exertion such
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
OVERACTIVE BLADDER DIAGNOSIS AND TREATMENT OF OVERACTIVE BLADDER IN ADULTS:
 2014 OVERACTIVE BLADDER DIAGNOSIS AND TREATMENT OF OVERACTIVE BLADDER IN ADULTS: AUA/SUFU Guideline (2012); Amended (2014) For Primary Care Providers OVERACTIVE BLADDER Diagnosis and Treatment of Overactive
2014 OVERACTIVE BLADDER DIAGNOSIS AND TREATMENT OF OVERACTIVE BLADDER IN ADULTS: AUA/SUFU Guideline (2012); Amended (2014) For Primary Care Providers OVERACTIVE BLADDER Diagnosis and Treatment of Overactive
Bladder and Bowel Assessment Ann Yates Director of Continence Services. 18/07/2008 Cardiff and Vale NHS Trust
 Bladder and Bowel Assessment Ann Yates Director of Continence Services Types of continence problems Bladder Stress incontinence Urgency and urge Incontinence Mixed incontinence Obstructive incontinence
Bladder and Bowel Assessment Ann Yates Director of Continence Services Types of continence problems Bladder Stress incontinence Urgency and urge Incontinence Mixed incontinence Obstructive incontinence
Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly. Prapa Pattrapornpisut 7 June 2012
 1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
Management of Neurogenic Bladder Disorders
 Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
Electroneuromyographic studies
 Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
URINARY INCONTINENCE CASE PRESENTATION #1. Urinary Incontinence - History 2014/10/07. Structure of the Female Lower Urinary Tract
 Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Learning Resource Guide. Understanding Incontinence. 2000 Prism Innovations, Inc. All Rights Reserved
 Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
OAB (Overactive Bladder)
 OAB (Overactive Bladder) PharmCon is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education. This webcast has been supported by an educational grant
OAB (Overactive Bladder) PharmCon is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education. This webcast has been supported by an educational grant
Urinary incontinence and Prolapse. Dr Zeelha Abdool Consultant OBGYN Steve Biko Academic Hospital
 Urinary incontinence and Prolapse Dr Zeelha Abdool Consultant OBGYN Steve Biko Academic Hospital Definitions: IUGA/ICS standardized terminology Urinary incontinence (symptom): complaint of involuntary
Urinary incontinence and Prolapse Dr Zeelha Abdool Consultant OBGYN Steve Biko Academic Hospital Definitions: IUGA/ICS standardized terminology Urinary incontinence (symptom): complaint of involuntary
Overview of Urinary Incontinence in the Long Term Care Setting
 Overview of Urinary Incontinence in the Long Term Care Setting Management Strategies for the Nursing Assistant Ann M. Spenard RN, C, MSN Courtney Lyder ND, GNP Learning Objectives Describe common types
Overview of Urinary Incontinence in the Long Term Care Setting Management Strategies for the Nursing Assistant Ann M. Spenard RN, C, MSN Courtney Lyder ND, GNP Learning Objectives Describe common types
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse
 Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Urinary Incontinence
 Urinary Incontinence (Involuntary Passage of Urine) Basics OVERVIEW Loss of voluntary control of urination, usually observed as involuntary urine leakage while resting SIGNALMENT/DESCRIPTION OF PET Species
Urinary Incontinence (Involuntary Passage of Urine) Basics OVERVIEW Loss of voluntary control of urination, usually observed as involuntary urine leakage while resting SIGNALMENT/DESCRIPTION OF PET Species
PROCEDURE FOR THE ASSESSMENT OF ADULTS AND CHILDREN WITH BLADDER OR BOWEL DYSFUNCTION
 PROCEDURE FOR THE ASSESSMENT OF ADULTS AND CHILDREN WITH BLADDER OR BOWEL DYSFUNCTION First Issued Issue Version One Purpose of Issue/Description of Change Planned Review Date Procedure for the effective
PROCEDURE FOR THE ASSESSMENT OF ADULTS AND CHILDREN WITH BLADDER OR BOWEL DYSFUNCTION First Issued Issue Version One Purpose of Issue/Description of Change Planned Review Date Procedure for the effective
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
Bowel and Bladder Dysfunction in MS. Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center. Bladder Dysfunction
 Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Treatments for Urinary Incontinence in Women
 Treatments for Urinary Incontinence in Women National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH
Treatments for Urinary Incontinence in Women National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH
Urodynamics in Neuro-Urology
 Urodynamics in Neuro-Urology R Hamid MD (Res), FRCS (Urol) Consultant Urologist London Spinal Injuries Unit, Stanmore & University College London Hospitals Micturition Micturition can be visualized as
Urodynamics in Neuro-Urology R Hamid MD (Res), FRCS (Urol) Consultant Urologist London Spinal Injuries Unit, Stanmore & University College London Hospitals Micturition Micturition can be visualized as
Guidelines on Urinary Incontinence
 Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2007 TABLE OF CONTENTS
Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2007 TABLE OF CONTENTS
Female Urinary Incontinence
 Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. Objectives Which is most true? Review the problem
Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. Objectives Which is most true? Review the problem
Lifestyle changes. Pelvic floor muscle training
 Incontinence, urinary - Treatment Treating urinary incontinence The treatment you receive for urinary incontinence will depend on the type of incontinence you have and the severity of your symptoms. If
Incontinence, urinary - Treatment Treating urinary incontinence The treatment you receive for urinary incontinence will depend on the type of incontinence you have and the severity of your symptoms. If
Urinary Incontinence Definitions
 (AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
(AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
Saint Mary s Hospital. Gynaecology Service Warrell Unit. Overactive Bladder. Information for Patients
 Saint Mary s Hospital Gynaecology Service Warrell Unit Overactive Bladder Information for Patients What is Overactive Bladder (OAB)? OAB is a condition that causes you to need to pass urine more often
Saint Mary s Hospital Gynaecology Service Warrell Unit Overactive Bladder Information for Patients What is Overactive Bladder (OAB)? OAB is a condition that causes you to need to pass urine more often
Gwen Griffith Clinical Nurse Specialist Bolton NHS foundation Trust
 Gwen Griffith Clinical Nurse Specialist Bolton NHS foundation Trust Overview Setting the Scene Beginning of the journey & specialist nurse role Why people with MS experience bladder problems MS and the
Gwen Griffith Clinical Nurse Specialist Bolton NHS foundation Trust Overview Setting the Scene Beginning of the journey & specialist nurse role Why people with MS experience bladder problems MS and the
A Physical Therapist s Perspective
 You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
Liberty Pelvic Floor Stimulation
 Liberty Pelvic Floor Stimulation A logical first choice for treatment of urinary incontinence Liberty s simplified design exercises the correct muscles and is easy to use, therefore helping increase patient
Liberty Pelvic Floor Stimulation A logical first choice for treatment of urinary incontinence Liberty s simplified design exercises the correct muscles and is easy to use, therefore helping increase patient
URINARY INCONTINENCE IN WOMEN
 URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
Posterior Tibial Nerve Stimulation for Voiding Dysfunction. Original Policy Date
 MP 7.01.86 Posterior Tibial Nerve Stimulation for Voiding Dysfunction Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
MP 7.01.86 Posterior Tibial Nerve Stimulation for Voiding Dysfunction Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Canine Urinary Incontinence
 Urinary Incontinence in the Bitch Laurie Edge-Hughes, BScPT, MAnimSt, CAFCI, CCRT Urinary Incontinence = Involuntary leakage of urine during storage Micturation disorders (non-neurologic): 61% = Urethral
Urinary Incontinence in the Bitch Laurie Edge-Hughes, BScPT, MAnimSt, CAFCI, CCRT Urinary Incontinence = Involuntary leakage of urine during storage Micturation disorders (non-neurologic): 61% = Urethral
Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom
 British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
Urinary incontinence poses major medical
 ONE SIZE DOES NOT FIT ALL: MANAGEMENT OF THE DIFFICULT PATIENT * Karl J. Kreder, Jr, MD ABSTRACT Although the prevalence of urinary incontinence varies greatly depending on the criteria used to define
ONE SIZE DOES NOT FIT ALL: MANAGEMENT OF THE DIFFICULT PATIENT * Karl J. Kreder, Jr, MD ABSTRACT Although the prevalence of urinary incontinence varies greatly depending on the criteria used to define
Primary Care management of Overactive Bladder (OAB)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
Fecal incontinence (Encopresis) It is the fecal incontinence condition observed in children with chronic constipation over 1-2 years.
 WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
Painful Bladder Syndrome and Interstitial Cystitis
 Painful Bladder Syndrome and Interstitial Cystitis PAINFUL BLADDER AND INTERSTITIAL CYSTITIS OVERVIEW Painful bladder syndrome/interstitial cystitis (PBS/IC) is a disorder with symptoms of mild to severe
Painful Bladder Syndrome and Interstitial Cystitis PAINFUL BLADDER AND INTERSTITIAL CYSTITIS OVERVIEW Painful bladder syndrome/interstitial cystitis (PBS/IC) is a disorder with symptoms of mild to severe
Primary Care Management Guidelines Female Urinary Incontinence. Overview of Lecture
 Primary Care Management Guidelines Female Urinary Incontinence Professor Don Wilson Department of Women s and Children s Health Dunedin School of Medicine University of Otago GP Teaching for Roy Morris,
Primary Care Management Guidelines Female Urinary Incontinence Professor Don Wilson Department of Women s and Children s Health Dunedin School of Medicine University of Otago GP Teaching for Roy Morris,
Dr Eva Fong. Urologist Auckland
 Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use.
 Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
Enuresis BOWEL AND BLADDER CONTROL. Voiding disorders. Involuntary voiding at an inappropriate time or in a socially unacceptable setting
 Enuresis Why does my child have damp pants? Douglas E. Coplen Involuntary voiding at an inappropriate time or in a socially unacceptable setting Division of Pediatric Urology Washington University School
Enuresis Why does my child have damp pants? Douglas E. Coplen Involuntary voiding at an inappropriate time or in a socially unacceptable setting Division of Pediatric Urology Washington University School
Prospective Study of Transcutaneous Parasacral Electrical Stimulation for Overactive Bladder in Children: Long-Term Results
 Prospective Study of Transcutaneous Parasacral Electrical Stimulation for Overactive Bladder in Children: Long-Term Results Patrícia Lordêlo, Paulo Vitor Lima Soares, Iza MacIel, Antonio Macedo, Jr. and
Prospective Study of Transcutaneous Parasacral Electrical Stimulation for Overactive Bladder in Children: Long-Term Results Patrícia Lordêlo, Paulo Vitor Lima Soares, Iza MacIel, Antonio Macedo, Jr. and
1 in 3 women experience Stress Urinary Incontinence.
 A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
botulinum toxin type A 50, 100, 200 Allergan units/vial (Botox ) SMC No. (916/13) Allergan Ltd
 botulinum toxin type A 50, 100, 200 Allergan units/vial (Botox ) SMC No. (916/13) Allergan Ltd 06 September 2013 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
botulinum toxin type A 50, 100, 200 Allergan units/vial (Botox ) SMC No. (916/13) Allergan Ltd 06 September 2013 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015
 Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
Spine Care Centre (SCC) protocols for Multiple Sclerosis Update 1 August 2015 Introduction Multiple sclerosis (MS) affects nerves in the brain and spinal cord, causing a wide range of symptoms including
GLOSSARY of research terms
 GLOSSARY of research terms JLA Urinary Incontinence Working Partnership Workshop to set research priorities in Urinary Incontinence November 2008 Terms in bold are commonly used clinical/research terms.
GLOSSARY of research terms JLA Urinary Incontinence Working Partnership Workshop to set research priorities in Urinary Incontinence November 2008 Terms in bold are commonly used clinical/research terms.
Urinary Continence Management after a. Stroke. Liz Mackey, CNC Stroke Clinical Coordinator Western Health
 Urinary Continence Management after a Stroke Liz Mackey, CNC Stroke Clinical Coordinator Western Health Royal Women s Hospital Innervation of the Bladder Neuromuscular coordination for control of both
Urinary Continence Management after a Stroke Liz Mackey, CNC Stroke Clinical Coordinator Western Health Royal Women s Hospital Innervation of the Bladder Neuromuscular coordination for control of both
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
PROCEEDINGS INCIDENCE AND PREVALENCE OF STRESS URINARY INCONTINENCE * Ananias C. Diokno, MD ABSTRACT
 INCIDENCE AND PREVALENCE OF STRESS URINARY INCONTINENCE * Ananias C. Diokno, MD ABSTRACT Urinary incontinence is a worldwide problem that affects millions of women, although the magnitude of the problem
INCIDENCE AND PREVALENCE OF STRESS URINARY INCONTINENCE * Ananias C. Diokno, MD ABSTRACT Urinary incontinence is a worldwide problem that affects millions of women, although the magnitude of the problem
Bladder and Bowel Control
 Bladder and Bowel Control Dr Sue Woodward Lecturer, Florence Nightingale School of Nursing and Midwifery 2 Why do we need to understand anatomy? Normal physiology Normal adult bladder capacity = 450-500mls
Bladder and Bowel Control Dr Sue Woodward Lecturer, Florence Nightingale School of Nursing and Midwifery 2 Why do we need to understand anatomy? Normal physiology Normal adult bladder capacity = 450-500mls
SOGC Recommendations for Urinary Incontinence
 The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
Acupuncture for the treatment of overactive bladder
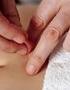 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 53 58 CASE REPORT Acupuncture for the treatment of overactive bladder P. Graham & T. Cook Physiotherapy Department,
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 53 58 CASE REPORT Acupuncture for the treatment of overactive bladder P. Graham & T. Cook Physiotherapy Department,
Case Study on the use of Electro acupuncture for Overactive Bladder. Siu Cheetham Physiotherapist Kwong Wah Hospital
 Case Study on the use of Electro acupuncture for Overactive Bladder Siu Cheetham Physiotherapist Kwong Wah Hospital Overactive bladder Approximately 34 million adults in the United States The International
Case Study on the use of Electro acupuncture for Overactive Bladder Siu Cheetham Physiotherapist Kwong Wah Hospital Overactive bladder Approximately 34 million adults in the United States The International
Sacral Nerve Neuromodulation/Stimulation
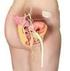 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
