Nikos Kouris a, *, Ignatios Ikonomidis b, Dimitra Kontogianni a, Peter Smith b, Petros Nihoyannopoulos b
|
|
|
- Dulcie Carr
- 7 years ago
- Views:
Transcription
1 Eur J Echocardiography (2005) 6, 435e442 Mitral valve repair versus replacement for isolated non-ischemic mitral regurgitation in patients with preoperative left ventricular dysfunction. A long-term follow-up echocardiography study Nikos Kouris a, *, Ignatios Ikonomidis b, Dimitra Kontogianni a, Peter Smith b, Petros Nihoyannopoulos b a Western Attica General Hospital, Athens, Greece b Hammersmith Hospital, Imperial College, London, UK Received 12 October 2004; received in revised form 15 January 2005; accepted 21 January 2005 Available online 2 April 2005 KEYWORDS Mitral regurgitation; Depressed LV function; Mitral valve repair Abstract The aim of this study was to evaluate LV function, by means of echocardiography, after mitral valve repair () or mitral valve replacement () in patients (pts) with chronic degenerative mitral regurgitation (MR) and depressed LV systolic function during a 6-years follow-up (FU) period. Patients and methods: Forty-five pts with moderately severe or severe MR and preoperative EF % 50% were divided into 2 groups: group (27 pts, 19 mene8 women, aged 62 G 10 years) and group (18 pts, 8 mene10 women, aged 60 G 12 years). The cause of MR was myxomatous mitral valve disease (/: 16/8), endocarditis (0/4) and degenerative mitral valves with ruptured chordae tendineae (11/6). All pts underwent transthoracic echocardiography preoperatively, postoperatively and annually during the FU period (6 G 3 years). Results: In group, 5 pts died, 5 were lost to FU and 2 pts underwent due to failure. In group, 6 pts died, 3 were lost to FU and 1 was re-operated due to prosthetic valve endocarditis. Atrial fibrillation was similar between the 2 groups. pts demonstrated significant LVEDD decrease postoperatively which was persistent during FU (p! 0.05). LVESD also decreased (p! 0.05), VTI improved (p! 0.05), while FS and EF showed a trend to improve. In pts, LVEDD was decreased * Corresponding author. 4, Agiou Georgiou Street, 15236, N. Penteli, Athens, Greece. Tel.: C ; fax: C address: nikoskou@otenet.gr (N. Kouris) /$30 ª 2005 The European Society of Cardiology. Published by Elsevier Ltd. All rights reserved. doi: /j.euje
2 436 N. Kouris et al. (p! 0.05) but increased during FU (p! 0.05) and LVESD remained high, resulting in a decrease of FS and EF (p! 0.05). VTI remained unchanged (p Z NS). Conclusion: in pts with non-ischemic MR and preoperative LV dysfunction achieves better preservation of LV systolic indices than, probably due to preservation of the subvalvular apparatus and LV geometry. ª 2005 The European Society of Cardiology. Published by Elsevier Ltd. All rights reserved. Mitral valve repair (), when feasible, has become the procedure of choice for surgical treatment of chronic mitral regurgitation (MR) because it provides better postoperative clinical outcome than mitral valve replacement (). 1e5 Poor preoperative left ventricular (LV) function has been associated with an adverse clinical outcome 6 in patients with MR, while preoperative LV ejection fraction (EF) may be a powerful predictor of postoperative heart failure and death, 5 regardless of the type of surgery used for correction of chronic MR. This is generally attributed to the postoperative increase in LV afterload and abolition of the pop-off valve effect of the regurgitant leak, further decreasing the EF and cardiac output. 6 The better clinical outcome after is directly related to the preservation of the subvalvular apparatus resulting in preservation of LV geometry. Patients with a significant degree of LV systolic dysfunction (EF! 50%) should undergo surgical correction of MR because: (a) surgical correction, compared to medical treatment, improves prognosis and (b) reduces the incidence of congestive heart failure. 7,8 The purpose of this study was to evaluate the recovery of the preoperative LV function after mitral valve repair or replacement in patients with impaired systolic LV function due to chronic degenerative MR. We also tested the hypothesis that these patients may present a greater improvement of LV function after than after. Patients and methods Study population The study group consisted of 45 patients with isolated moderately severe or severe MR and impaired LV function, without other significant associated valvular or coronary artery disease, documented by preoperative echocardiographic and cardiac catheterization studies. All patients had preoperative ejection fraction!50% (46 G 5%, range 31e50%), determined by echocardiography. The selection of LVEF % 50% as the cut-off point between normal and depressed LV function was based on Veterans Administration Co-operative Study on valvular heart disease. 9 The underlying cause of MR was myxomatous mitral valve disease (floppy mitral valve) in 24 patients, endocarditis in 4 and degenerative valves with ruptured chordae tendineae in 17. Twenty-seven patients (19 mene8 women, aged 62 G 10 years) ( group) underwent (according to the Carpentier type reconstruction 10,11 ) and a rigid Carpentier annular ring was inserted in 16 of them (Table 2). Eighteen patients (8 mene10 women, aged 60 G 12 years) ( group) underwent a conventional without preservation of papillary muscles and a low profile mechanical disc valve was implanted in all of them (Bjork-Shiley in 15 patients and St. Jude in 3). Patients in the 2 groups had similar age and degree of preoperative MR assessed by echocardiography and cardiac catheterization (Table 1). The decision to replace or to repair the valve was made on the table by the surgeon based on the valve anatomy. All patients were operated at the same center (Hammersmith Hospital, London, UK) by the same group of surgeons. Table 1 Preoperative patient characteristics Group A () Group B () No Age (years) 62 G G 12 Sex 19 mene8 women 8 mene10 women MR severity(median) 3/4 3/4 Moderate 2/4 8 4 Mod. severe 3/4 8 9 Severe 4/ Underlying disease Floppy MV 16 8 Flail MV 11 6 Endocarditis 0 4 Leaflets involved Posterior 21 9 Anterior 2 3 Both 4 6 SR/AF/paced 16/10/1 11/7/0, mitral valve repair;, mitral valve replacement; MR, mitral regurgitation; MV, mitral valve; SR, sinus rhythm; AF, atrial fibrillation.
3 vs in depressed LV function 437 Table 2 Group A patients characteristics regarding ring insertion Age (years) Leaflets involved Degree of MR AF Ring (N Z 16) 61 G 8 Posterior: 13 Moderate 2/4: 5 6 Anterior: 1 Mod. severe 3/4: 6 Both: 2 Severe 4/4:5 No ring (N Z 11) 63 G 12 Posterior: 8 Moderate 2/4: 3 10 Anterior: 1 Mod. severe 3/4: 2 Both: 2 Severe 4/4: 6 Follow-up The mean follow-up period was 6 G 3 years in all patients and was divided in 3 consecutive time periods: 6e18 months after surgery (FU1), 18e36 months (FU2) and O36 months (FU3). All patients were evaluated at the outpatient clinic yearly. Echocardiography All patients were evaluated with transthoracic and transoesophageal echocardiography, within 5 months before surgery. Transthoracic echocardiography was repeated within 3 months after surgery and on an annual base during the follow-up (FU) period. Examinations were performed in the left lateral decubitus position. LV systolic function was estimated from LV end-diastolic and end-systolic diameters (LVEDD, LVESD), fractional shortening (FS), ejection fraction (EF) and velocity time integral of LV outflow track (VTI) with Pulse wave Doppler. EF was calculated using the modified Simpson s method. The size of the left atrium (LA) was also measured and pulmonary artery systolic pressure (PASP) was estimated from tricuspid regurgitation. Mitral regurgitation was evaluated semi-quantitatively by color Doppler imaging at transthoracic and transoesophageal echocardiography and was graded as follows: 1 Z mild, 2 Z moderate, 3 Z moderately severe, 4 Z severe. Table 3 Postoperative patients characteristics p FU time (years) 6 G 3 6G 4 NS Deaths 5 6 NS Re-operation 2 1 NS MR increase a 2 1 NS New AF 3 4 NS a MR increase is defined as an increase of MR degree from 1/4 to 2/4. Statistics Statistical analysis was performed using the Statistical Package for the Social Sciences (SPSS) software. 12 Results were expressed as mean values G SD. Normal distribution of the echocardiographic indices was checked with Kolmogorove Smirnov test. Due to the fact that some measured data were skewed, analysis of the overall differences between subgroups was performed using the non-parametric ManneWhitney test or Kruskalle Wallis test for multiple comparisons. Paired analysis of each variable within the 2 groups was performed using the non-parametric Wilcoxon test or Friedman test for multiple comparisons. A p value!0.05 was considered significant. Results Clinical characteristics of the study population Patients clinical characteristics are presented in Table 1. No patient had any residual mitral regurgitation of any clinical significance at the first postoperative study. In the group, 5 patients were lost within the first year of FU and they were not included in the analysis of the data during FU period. In the group, 2 patients died 2 and 3 months, respectively, following surgery and 3 other were lost within the first year of FU and so the data of all 5 patients in this group were not included in the analysis of the data during FU period. Thus, of the 45 patients studied pre- and immediately postoperatively, 35 patients completed the FU3 period (O36 months) (22 in the group and 13 in the group). In-group analysis Overall changes of the echocardiographic indices postoperatively and during FU are presented in Table 4.
4 438 N. Kouris et al. Table 4 Changes of the echocardiographic indices postoperatively and during follow-up Pre-op Post-op FU1 FU2 FU3 Pre-op Post-op FU1 FU2 FU3 LVEDD (mm) 61 G 6 53G 6* 52 G 6 50G 7 51G 9 59G 7 55G 8* 55 G 8 57G 8 59G 9x LVESD (mm) 43 G 4 39G 5* 38 G 7 35G 6 37G 8 42G 5 41G 8 41G 8 43G 9 44G 10 FS (%) 28 G 4 27G 5 29G 6 30G 5 29G 8 28G 4 25G 5x 25 G 6 25G 6 24G 9 EF (%) 48 G 6 46G 7 48G G 9 48G G 6 42G 9{ 43 G G G 14 VTI (cm) 13 G 3 15G 2* 15 G 2 15G 2 16G 2 13G 3 14G 2 14G 3 13G 4 14G 3 LA (mm) 56 G G 9* 49 G G 9 52G 9 53G G G G G 13 PASP (mmhg) 26 G 5 26G 6 28G 7 28G 6 31G G 7 30G 7 32G 9 35G 9U 40 G 10U Values are expressed as mean G SD. FU1: follow-up 6e18 months, FU2: 18e36 months, FU3: O36 months. LVEDD, left ventricular end-diastolic diameter; LVESD, left ventricular end-systolic diameter; FS, fractional shortening; EF, ejection fraction; VTI, velocity time integral at left ventricular outflow tract; LA, left atrium; PASP, pulmonary artery systolic pressure. *p! 0.05 between pre- and postoperative values. xp! 0.02 between pre- and postoperative values and between post- and FU3 values. {p! 0.03 between pre- and postoperative values. Up! 0.05 between post- and FU2 and FU3 values. Values not indicated were NS (see text). Patients in group demonstrated a decrease of LVEDD from 61 G 6 mm preoperatively to 53 G 6 mm early postoperatively (p! 0.001), approaching normal values. The improvement of LVEDD remained unchanged throughout FU (Fig. 1). LVESD was also reduced from 43 G 4mm preoperatively to 39 G 5 mm early postoperatively (p Z 0.002), which was preserved during FU showing a trend for a further decrease (Fig. 2). FS and EF showed a mild deterioration from pre- to postoperative value (28 G 4% / 27 G 5%, p Z 0.2; 48 G 6% / 46 G 7%, p Z 0.25, respectively), but during FU, both indices showed a trend to improve (Fig. 3). Conversely, VTI showed an improvement from 13 G 3 cm preoperatively to 15 G 2 cm early postoperatively, (p! 0.05), which was preserved during FU (Fig. 4). The LA size was reduced after surgery (56 G 10 mm / 50 G 9mm,p Z 0.001) and remained unchanged during FU. Finally, PASP was similar preoperatively, postoperatively and during FU (26 G 5mmHg/ 26 G 6mmHg/ 31 G 10 mmhg, p Z NS). In the subgroup of patients there were no differences in LV diameters and EF during FU between patients with or without an annular ring after surgical repair of the mitral valve. However, a borderline increase in FS and EF (p Z and p Z 0.05, respectively) was noted at FU1, in patients without an annular ring, compared to those 65 Left Ventricular End-Diastolic Diameter 50 Left Ventricular End-Systolic Diameter LVEDD (mm) pre-op post-op FU 1 Time FU 2 FU 3 OPER Figure 1 Changes in left ventricular end-diastolic diameter from preoperative value through follow-up time. p 1 : difference between pre- and postoperative value in each group (in-group analysis), p 2 : difference between postoperative and FU3 value in group B (ingroup analysis), p 3 : difference in FU2 and FU3 values between the 2 groups (between-groups analysis). LVESD (mm) pre-op post-op FU 1 Time FU 2 FU 3 OPER Figure 2 Changes in left ventricular end-systolic diameter from preoperative value through follow-up time. p 1, p 2 : differences between pre- and postoperative value in and group, respectively (in-group analysis) p 3 : difference in FU2 and FU3 values between the 2 groups (between-groups analysis).
5 vs in depressed LV function 439 EF (%) with an annular ring implanted, but this difference was not evident in FU2 and FU3. In the group, LVEDD showed an early postoperative decrease, compared to its preoperative value (59 G 7 mm versus 55 G 8mm, p! 0.05). Conversely, LVEDD increased at 36 months of FU (post-op versus FU3 value: 55 G 8 mm versus 59 G 9mm,p Z 0.016, Fig. 1). LVESD remained high early postoperatively (Fig. 2), resulting in a significant decrease of FS and EF (pre-op / post-op value: 28 G 4% / 25 G 5%, p! 0.02, 47 G 6% / 42 G 9%, p! 0.03, respectively). The reduction in VTI (cm) pre-op pre-op post-op Velocity Time Integral post-op Ejection Fraction FU 1 Time FU 1 Time FU 2 FU 2 FU 3 FU 3 OPER OPER Figure 4 Changes in velocity time integral from preoperative value through follow-up time. p: difference between pre- and postoperative value in group (in-group analysis). All other differences were NS. Figure 3 Changes in left ventricular ejection fraction from preoperative value through follow-up time. p 1, p 2 : differences between pre- and postoperative value in and group, respectively (in-group analysis) p 3 : difference in FU2 and FU3 values between the 2 groups (between-groups analysis). FS and EF further increased at 36 months of FU (Fig. 3). VTI and LA size remained practically unchanged. PASP did not change significantly after surgery (28 G 7 mmhg / 30 G 7 mmhg, p Z NS), but at FU3 it increased from the postoperative value (30 G 7 mmhg / 40 G 10 mmhg, p Z 0.005). Finally, a modest correlation was found in both groups, between preoperative and postoperative LVEF (r Z 0.40). Between-groups analysis Patients in the 2 groups did not show any difference in any echocardiographic parameter preoperatively, as well as postoperatively. During FU1, no difference was found in any parameter, but at FU2 patients in group compared to patients in group demonstrated lower LVEDD (50 G 7 mm versus 59 G 8 mm, p! 0.05), lower LVESD (35 G 6 mm versus 43 G 9mm, p! 0.05), higher FS (30 G 5 mm versus 25 G 6 mm, p Z 0.07) and EF (50 G 9 mm versus 42 G 11 mm, p Z 0.07), smaller LA (51 G 9 mm versus 61 G 11 mm, p! 0.05), lower PASP (28 G 6 mmhg versus 35 G 9 mmhg, p! 0.05) and similar VTI (15 G 2 mm versus 13 G 4 mm, p Z 0.3). Finally, similar differences were observed between patients in the and patients in the group during FU3 (Figs. 1e4). Follow-up In group, five patients died at 5 G 1 years after surgery. All patients who died had completed the FU3 period, so their data were included in the analysis. Two other patients underwent due to failure (1 and 2 years after surgery, respectively). Two more patients demonstrated a progressive increase of mitral regurgitation during the FU period, not requiring surgical intervention. In the remaining 18 patients with, the mild residual MR observed early postoperatively, remained unchanged throughout FU period. Three patients developed atrial fibrillation (AF) during FU. None of the patients developed clinical or echocardiographic signs suggestive of coronary artery disease (akinesis or scar). Also, no perioperative myocardial infarction was found in the group. In the group, 2 patients died during early postoperative period (!3 months) and their data were not included in the analysis. Four other patients died at 7 G 4 years having completed the FU3 period, so their data were analyzed. Additionally, 1 patient was re-operated due to prosthetic valve endocarditis and four patients
6 440 N. Kouris et al. developed AF (2 permanent, 2 paroxysmal) (Group A versus Group B p Z NS, Table 3). Occurrence of AF did not differ between the 2 groups. Furthermore, in the group the mitral prosthesis remained well functioning with the pressure half time remaining unchanged throughout the FU period (PHT post-op: 94 G 35 ms, FU1: 105 G 30 ms, FU2: 88 G 32 ms, FU3: 82 G 27 ms, p Z NS). Finally, only 1 patient demonstrated increase of MR during FU period, not requiring surgical intervention, while in the rest of patients the mild residual MR remained unchanged. Thus, there was no significant difference between the 2 groups in the number of patients with deterioration of MR during FU (Table 3). Discussion Degenerative mitral valve disease is currently the most common cause of mitral regurgitation in Europe. 3 Mitral regurgitation leads to chronic volume overload of the left ventricle, progressively leading to LV dysfunction. 6 The regurgitant volume, ejected into the low-resistance left atrial chamber during systole, increases the total stroke volume and the EF. Since the LVEF, in the presence of severe MR, is often supranormal, the slightest reduction in EF is synonymous to significant LV dysfunction. Myocardial failure is also an important postoperative complication and it is responsible for the majority of postoperative cardiac related mortality and morbidity. 8 Many reports have shown that is superior to, as far as preservation of LV function is concerned. 1e4,13 To our knowledge, there have been no reports on the effects of mitral valve replacement versus repair on an already impaired LV function prior to valve surgery for isolated MR. In our study, LVEDD was significantly reduced in both groups postoperatively. This was an expected finding, since the cause of LV volume overload was eliminated. 14 During FU however, while in patients LVEDD remained within normal limits, in the group it increased again, 3 years after surgery, reaching the preoperative values, without any significant residual MR. This finding could be explained by the fact that in without chordal preservation, LV remodeling alters the shape of the left ventricle toward a spherical geometry (decreased eccentricity index), whether in the LV shape is not affected. Previous reports support this finding, although FU period was shorter. 5,15 It should be also noted that during FU, no perioperative acute myocardial infarction, which develops more frequently during, 16 was found in our group. Consequently, at 6 years FU, patients with demonstrated a lower FS and EF than patients with, compared to the early postoperative study. A possible explanation for these alterations is based upon the aforementioned changes in LV geometry. It has been proposed that, despite expected increase in LV afterload caused by the competent mitral valve, in as well as in with chordal preservation, LV afterload decreases after mitral surgery. 17 Preservation of the subvalvular apparatus in these techniques maintains LV geometry and allows a reduction of LV radius, leading to a reduction in wall stress (LV afterload), according to the Laplace equation. This LV afterload reduction is even more beneficial in patients with preoperatively reduced LV contractility. 6 Conversely, endsystolic wall stress is increased after without chordal preservation due to the loss of chordal support and LV end-systolic volume fails to decrease. 18 Ren and colleagues 15 suggest that preservation of LVEF in and in with chordal preservation is not caused by a decrease in endsystolic volume; the decrease in end-systolic volume is the result of a preserved EF (due to the maintenance of the functional components of the subvalvular apparatus), even though there is a decrease in end-diastolic volume. 15 Our results are in agreement with other reports that showed preservation (not improvement) of LVEF after 1,6,15 and deterioration after 1,13,15 and this preservation is maintained during a long period of time postoperatively after, while it further deteriorates after. The decrease in FS and EF that was noted in both groups at the early postoperative period, is consistent with the reports of Enriquez-Sarano et al., who reported this finding almost 10 years ago, in patients with preoperatively normal systolic function. 2 The weak correlation that was also found in both groups, between preoperative and postoperative LVEF (r Z 0.40), is consistent with previous reports. 19 The data of this cohort demonstrate that patients with MR, who have developed LV dysfunction because they were not operated early enough during the natural history of their valve disease, can benefit from valve reconstruction. However, neither with nor with a normalization of LVEF with mean values O55% could be obtained. Incidence of atrial fibrillation Incidence of AF did not differ between the 2 groups neither preoperatively, nor postoperatively or during FU. Because of the small number of patients, we could not demonstrate whether AF played any role in LV remodeling, although such
7 vs in depressed LV function 441 a role seems inexplicit to influence the results of one surgical technique over the other. This is supported by Lim et al., 20 who suggested that AF did not affect early outcome of. Ring versus no ring Patients who underwent with concomitant annular ring insertion did not show any significant difference in postoperative LV function, compared to those without ring implantation. The decision whether a ring should be inserted was based upon the surgeon s choice for best anatomical correction of the responsible leaflet, since the 2 subgroups with and without ring were identical, concerning the affected leaflet and the degree of MR preoperatively. The use of annular ring during is controversial and not all surgeons do recommend its implantation, since it improves the results of but, on the other hand, it increases the frequency of systolic anterior motion (SAM). 21 Moreover, the effects of rigid or flexible rings on LV function are also controversial. David et al. 22 reported better LV function after insertion of flexible ring, while Castro et al. did not show any significant difference between the 2 rings. 23 Study limitations It is possible that due to the relatively small number of patients involved, some of our results might have been affected, particularly in the subgroup analysis. The patient s surgical procedure was not randomized preoperatively and was determined by the surgeon at the time of the operation. However, since a randomized trial will probably never be performed, the only acceptable method of comparison of the 2 surgical procedures is to adjust the baseline preoperative parameters. We reported a significant increase of LVEDD in group during 6 years FU. However, subclinical coronary artery disease may not be excluded, as coronary angiography was not performed in any patient postoperatively. The paradoxic septal motion associated with cardiac surgery might raise concern about the use of echocardiography for postoperative assessment of LVEF. This, however, has been attributed to a translational movement rather than a regional wall motion abnormality and it does not impair the ability to assess LV function by echocardiography. 24 Finally, we did not perform any formal quantitation of MR due to the absence of any standardized criteria at the time of the study. Conclusion In this study we report that during a 6-year followup, patients with chronic degenerative MR and LV dysfunction show further deterioration of LV function after. Conversely, appear to better preserve the overall LV function. Mitral valve repair should therefore be the surgical procedure of choice, not only for the lower mortality during the operation itself, but also for the better preservation of LV function in the long term and the level of ejection fraction should not be a reason for denying the benefits of repair to patients with MR. Nevertheless, although seems to preserve LV function, it rarely achieves complete normalization of LVEF and therefore early surgery should be performed before these patients develop LV dysfunction. References 1. Goldman ME, Mora F, Guarino T, Fuster V, Mindich BP. Mitral valvuloplasty is superior to valve replacement for preservation of left ventricular function: an intraoperative twodimensional echocardiographic study. J Am Coll Cardiol 1987;10:568e Enriquez-Sarano M, Schaff HV, Orszulak TA, Tajik AJ, Bailey KR, Frye RL. Valve repair improves the outcome of surgery for mitral regurgitation. A multivariate analysis. Circulation 1995;91:1022e8. 3. Lee EM, Shapiro LM, Wells FC. Superiority of mitral valve repair in surgery for degenerative mitral regurgitation. Eur Heart J 1997;18:655e Tischler MD, Cooper KA, Rowen M, LeWinter MM. Mitral valve replacement versus mitral valve repair. A Doppler and quantitative stress echocardiographic study. Circulation 1994;89:132e7. 5. Enriquez-Sarano M, Tajik AJ, Schaff HV, Orszulak TA, McGoon MD, Bailey KR, et al. Echocardiographic prediction of left ventricular function after correction of mitral regurgitation: results and clinical implications. J Am Coll Cardiol 1994;24:1536e de Varennes B, Haichin R. Impact of preoperative left ventricular ejection fraction on postoperative left ventricular remodeling after mitral valve repair for degenerative disease. J Heart Valve Dis 2000;9:313e Enriquez-Sarano M, Tajik AJ, Schaff HV, Orszulak TA, Bailey KR, Frye RL. Echocardiographic prediction of survival after surgical correction of organic mitral regurgitation. Circulation 1994;90:830e7. 8. Enriquez-Sarano M, Schaff HV, Orszulak TA, Tajik AJ, Bailey KR, Frye RL. Congestive heart failure after surgical correction of mitral regurgitation. A long term study. Circulation 1995;92:2496e Crawford MH, Souchek J, Oprian CA, Miller DC, Rahimtoola S, Giacomini JC, et al. Determinants of survival and left ventricular performance after mitral valve replacement: Department of Veterans Affairs Cooperative Study on Valvular Heart Disease. Circulation 1990;81: 1173e81.
8 442 N. Kouris et al. 10. Carpentier A, Relland J, Deloche A, Fabiani JN, D Allaines C, Blondeau P, et al. Conservative management of the prolapsed mitral valve. Ann Thorac Surg 1978;26: 294e Carpentier A. Cardiac valve surgery e the French Correction. J Thorac Cardiovasc Surg 1983;86:323e SPSS. Statistical Package for the Social Sciences. Windows version, release Chicago: SPSS Inc; Huikuri H. Effect of mitral valve replacement on left ventricular function in mitral regurgitation. Br Heart J 1983;49: Tischler MD, Cooper KA, Battle RW, Leavitt BJ. Effect of mitral valve repair for mitral valve prolapse on regression of left ventricular mass. Am J Cardiol 1992;70:1216e Ren J, Aksut S, Lighty GW, Vigilante GJ, Sink JD, Segal BL, et al. Mitral valve repair is superior to valve replacement for the early preservation of cardiac function: relation of ventricular geometry to function. Am Heart J 1996;131: 974e Obarski TP, Loop FD, Cosgrove DM, Lytle BW, Stewart WJ. Frequency of acute myocardial infarction in valve repairs versus valve replacement for pure mitral regurgitation. Am J Cardiol 1990;65:887e Okita Y, Miki S, Veda Y, Tahata T, Sakai T, Matsuyama K. Comparative evaluation of left ventricular performance after mitral valve repair or valve replacement with or without chordal preservation. J Heart Valve Dis 1993;99: 228e Rozich TD, Carabello BA, Usher BW, Kratz JM, Bell AE, Zile MR. Mitral valve replacement with or without chordal preservation in patients with chronic mitral regurgitation. Circulation 1992;86:1718e Matsumura T, Ohtaki E, Tanaka K, Misu K, Tobaru T, Asano R, et al. Echocardiographic prediction of left ventricular dysfunction after mitral valve repair for mitral regurgitation as an indicator to decide the optimal timing of repair. JAm Coll Cardiol 2003;42:464e Lim E, Barlow CW, Hosseinpour AR, Wisbey C, Wilson K, Pidgeon W, et al. Influence of atrial fibrillation on outcome following mitral valve repair. Circulation 2001;104 (12 Suppl.1):I59e Bisbos AD, Spanos PK. Surgical correction of mitral valve regurgitation. Hell J Cardiol 2003;44:469e David TE, Komeda M, Pollick C, Burns RJ. Mitral valve annuloplasty: the effect of the type on left ventricular function. Ann Thorac Surg 1989;47: Castro LJ, Moon MR, Rayhill SC, Niczypornk MA, Ingels Jr NB, Daughters 3rd GT, et al. Annuloplasty with flexible or rigid ring does not alter left ventricular systolic performance, energetics or ventricularearterial coupling in conscious, closed-chest dogs. J Thorac Cardiovasc Surg 1993;105: Lehmann KG, Lee FA, McKenzie WB, Barash PG, Prokop EK, Durkin MA, et al. Onset of altered interventricular septal motion during cardiac surgery: assessment by continuous intraoperative transesophageal echocardiography. Circulation 1990;82:1325e34.
Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease
 Keynote Lecture Series Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease Tirone E. David Division of Cardiovascular Surgery, Peter Munk Cardiac Centre,
Keynote Lecture Series Durability of mitral valve repair for mitral regurgitation due to degenerative mitral valve disease Tirone E. David Division of Cardiovascular Surgery, Peter Munk Cardiac Centre,
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular
 Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation. Michael Acker, MD For the CTSN Investigators AHA November 2013
 Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
5. Management of rheumatic heart disease
 5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Real-Time 3-Dimensional Transesophageal Echocardiography in the Evaluation of Post-Operative Mitral Annuloplasty Ring and Prosthetic Valve Dehiscence
 Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
Mitral valve repair current Status and the modern Sternotomy
 Mitral valve repair current Status and the modern Sternotomy David L Saint MD, FACS Tallahassee Memorial Hospital Clinical Assistant Professor Florida State University School of Medicine History of Mitral
Mitral valve repair current Status and the modern Sternotomy David L Saint MD, FACS Tallahassee Memorial Hospital Clinical Assistant Professor Florida State University School of Medicine History of Mitral
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity
 Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
The road to mitral valve repair with live 3D transesophageal echocardiography (TEE)
 Clinical applications The road to mitral valve repair with live 3D transesophageal echocardiography (T) R.M. Lang I.S. Salgo A.C. Anyanwu D.H. Adams Professor of Medicine; Director, Noninvasive Cardiac
Clinical applications The road to mitral valve repair with live 3D transesophageal echocardiography (T) R.M. Lang I.S. Salgo A.C. Anyanwu D.H. Adams Professor of Medicine; Director, Noninvasive Cardiac
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
How should we treat atrial fibrillation in heart failure
 Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Dysfunction of aortic valve prostheses
 Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway No
Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway Dysfunction of aortic valve prostheses Kai Andersen Oslo University Hospital Rikshospitalet, Norway No
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS
 65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
Transcatheter Mitral Valve-in-Valve and Valve-in-Ring Implantations. Danny Dvir, MD On behalf of VIVID registry investigators
 Transcatheter Mitral Valve-in-Valve and Valve-in-Ring Implantations Danny Dvir, MD On behalf of VIVID registry investigators Introduction Bioprosthetic valves are increasingly implanted in open-heart surgeries.
Transcatheter Mitral Valve-in-Valve and Valve-in-Ring Implantations Danny Dvir, MD On behalf of VIVID registry investigators Introduction Bioprosthetic valves are increasingly implanted in open-heart surgeries.
Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography
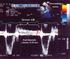 AMERICAN SOCIETY OF ECHOCARDIOGRAPHY REPORT Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography A report from the American
AMERICAN SOCIETY OF ECHOCARDIOGRAPHY REPORT Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography A report from the American
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Ottavio Alfieri S. Raffaele University Hospital, Milano
 The future of mitral surgery: revolution versus involution Ottavio Alfieri S. Raffaele University Hospital, Milano Future The trouble with the future is that it s so much less knowable than the past. John
The future of mitral surgery: revolution versus involution Ottavio Alfieri S. Raffaele University Hospital, Milano Future The trouble with the future is that it s so much less knowable than the past. John
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013. Reference: NHSCB/A09/PS/b
 Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation
 The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation Abdullah A. Alghamdi, MD, MSc, FRCSC King Abdulaziz Cardiac Center, National Guard Riyadh, Saudi Arabia Outlines Not
The Difficult Mitral Valve Repair in Children, Leave with Stenosis or Regurgitation Abdullah A. Alghamdi, MD, MSc, FRCSC King Abdulaziz Cardiac Center, National Guard Riyadh, Saudi Arabia Outlines Not
Medical Policy Manual. Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015. Section: Surgery Last Reviewed Date: November 2015
 Medical Policy Manual Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015 Section: Surgery Last Reviewed Date: November 2015 Policy No: 199 Effective Date: January 1, 2016 IMPORTANT
Medical Policy Manual Topic: Transcatheter Mitral Valve Repair Date of Origin: November 2015 Section: Surgery Last Reviewed Date: November 2015 Policy No: 199 Effective Date: January 1, 2016 IMPORTANT
Mitral Valve Repair. A. Marc Gillinov and Delos M. Cosgrove
 Mitral Valve Repair A. Marc Gillinov and Delos M. Cosgrove Surgical repair of the dysfunctional mitral valve dates back to the early twentieth century when several surgeons developed techniques to try
Mitral Valve Repair A. Marc Gillinov and Delos M. Cosgrove Surgical repair of the dysfunctional mitral valve dates back to the early twentieth century when several surgeons developed techniques to try
5. Diagnosis and management of rheumatic heart disease
 5. Diagnosis and management of rheumatic heart disease Introduction Chronic rheumatic valvular heart disease is the long-term result of ARF. It is a disease of poverty and disadvantage. In Australia, the
5. Diagnosis and management of rheumatic heart disease Introduction Chronic rheumatic valvular heart disease is the long-term result of ARF. It is a disease of poverty and disadvantage. In Australia, the
Carcinoid Hjärtsjukdom
 Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Contemporary Results of Mitral Valve Repair for Infective Endocarditis
 Journal of the American College of Cardiology Vol. 43, No. 3, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.09.034
Journal of the American College of Cardiology Vol. 43, No. 3, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.09.034
Surgeons Role in Atrial Fibrillation
 Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Imaging. Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction
 Imaging Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction Wael AlJaroudi, MD; M. Chadi Alraies, MD; Carmel Halley, MD; Leonardo Rodriguez, MD; Richard
Imaging Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction Wael AlJaroudi, MD; M. Chadi Alraies, MD; Carmel Halley, MD; Leonardo Rodriguez, MD; Richard
Current Strategies of Mitral Valve Repair
 Dan Spiegelstein MD, Probal Ghosh MD, Leonid Sternik MD, Salis Tager MD, Amihai Shinfeld MD and Ehud Raanani MD Department of Cardiothoracic Surgery, Sheba Medical Center, Tel Hashomer, Israel Affiliated
Dan Spiegelstein MD, Probal Ghosh MD, Leonid Sternik MD, Salis Tager MD, Amihai Shinfeld MD and Ehud Raanani MD Department of Cardiothoracic Surgery, Sheba Medical Center, Tel Hashomer, Israel Affiliated
Press conference: Rheumatic Heart Disease a forgotten but devastating disease
 www.worldcardiocongress.org Chairpersons: Bongani M. Mayosi Jonathan Carapetis Press conference: Rheumatic Heart Disease a forgotten but devastating disease www.worldcardiocongress.org www.worldcardiocongress.org
www.worldcardiocongress.org Chairpersons: Bongani M. Mayosi Jonathan Carapetis Press conference: Rheumatic Heart Disease a forgotten but devastating disease www.worldcardiocongress.org www.worldcardiocongress.org
one of the most prevalent cardiac in almost 2.4 percent of the population. 1 Although the incidence of infective
 Case Report Hellenic J Cardiol 2011; 52: 177-181 Successful Surgical Repair of Mitral Valve Prolapse Endocarditis: Case Report and Review of the Current Literature Pavlos N. Stougiannos 1, Dimitrios Z.
Case Report Hellenic J Cardiol 2011; 52: 177-181 Successful Surgical Repair of Mitral Valve Prolapse Endocarditis: Case Report and Review of the Current Literature Pavlos N. Stougiannos 1, Dimitrios Z.
A bs tr ac t. n engl j med 364;15 nejm.org april 14, 2011 1395
 The new england journal of medicine established in 1812 april 14, 2011 vol. 364 no. 15 Percutaneous Repair or Surgery for Mitral Regurgitation Ted Feldman, M.D., Elyse Foster, M.D., Donald D. Glower, M.D.,
The new england journal of medicine established in 1812 april 14, 2011 vol. 364 no. 15 Percutaneous Repair or Surgery for Mitral Regurgitation Ted Feldman, M.D., Elyse Foster, M.D., Donald D. Glower, M.D.,
Chapter 10. Mitral Valve Repair and Redo Repair for Mitral Regurgitation in a Heart Transplant Recipient
 Chapter 10 Mitral Valve Repair and Redo Repair for Mitral Regurgitation in a Heart Transplant Recipient Journal of Cardiothoracic Surgery 2012; 7: 100 Wobbe Bouma a Johan Brügemann b Inez J. Wijdh den
Chapter 10 Mitral Valve Repair and Redo Repair for Mitral Regurgitation in a Heart Transplant Recipient Journal of Cardiothoracic Surgery 2012; 7: 100 Wobbe Bouma a Johan Brügemann b Inez J. Wijdh den
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES.
 PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension
 Ideal risk prognosticator Easy to acquire Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension Safe -- Non-invasive Robust Gerhard-Paul Diller Astrid Lammers Division of Adult Congenital
Ideal risk prognosticator Easy to acquire Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension Safe -- Non-invasive Robust Gerhard-Paul Diller Astrid Lammers Division of Adult Congenital
Surgical repair of a diseased mitral valve has
 Mitral Valve Repair Using the MitraClip: From Concept to Reality Early experience with the MitraClip device suggests that it may be a viable therapeutic option in selected patients with MR. BY SAIBAL KAR,
Mitral Valve Repair Using the MitraClip: From Concept to Reality Early experience with the MitraClip device suggests that it may be a viable therapeutic option in selected patients with MR. BY SAIBAL KAR,
Transcatheter Mitral Valve Repair
 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Transcatheter Mitral Valve Repair Number 2.02.30 Effective Date
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Transcatheter Mitral Valve Repair Number 2.02.30 Effective Date
How do you decide on rate versus rhythm control?
 Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart valve repair and replacement
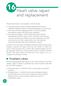 16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Repair of a regurgitant mitral valve is superior to mitral valve
 EDITORIAL ACD GTS ACD ET CSP TX The double-orifice technique in mitral valve repair: A simple solution for complex problems Ottavio Alfieri, MD Francesco Maisano, MD Michele De Bonis, MD Pier Luigi Stefano,
EDITORIAL ACD GTS ACD ET CSP TX The double-orifice technique in mitral valve repair: A simple solution for complex problems Ottavio Alfieri, MD Francesco Maisano, MD Michele De Bonis, MD Pier Luigi Stefano,
Steven J. Yakubov, MD FACC For the CoreValve US Clinical Investigators
 Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
To Bridge or Not to Bridge. Periop Anticoagulation Management. Don Weinshenker, MD Ambulatory Care Denver VAMC
 To Bridge or Not to Bridge Periop Anticoagulation Management Don Weinshenker, MD Ambulatory Care Denver VAMC Financial Disclosure Information Nothing to report Periop AC Management Chronically anti-coagulated
To Bridge or Not to Bridge Periop Anticoagulation Management Don Weinshenker, MD Ambulatory Care Denver VAMC Financial Disclosure Information Nothing to report Periop AC Management Chronically anti-coagulated
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Read It, Code It, See It
 Read It, Code It, See It Richard L. Prager, M.D. University of Michigan Ann Arbor, Michigan Dorothy Latham, R.N. Port Huron Hospital Port Huron, Michigan Nothing to Disclose Disclosure Preoperative diagnosis:
Read It, Code It, See It Richard L. Prager, M.D. University of Michigan Ann Arbor, Michigan Dorothy Latham, R.N. Port Huron Hospital Port Huron, Michigan Nothing to Disclose Disclosure Preoperative diagnosis:
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Fellow TEE Review Workshop Hemodynamic Calculations 2013. Director, Intraoperative TEE Program. Johns Hopkins School of Medicine
 Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Heart Murmurs. Outline. Basic Pathophysiology
 Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Vs. K. Farsalinos, D. Tsiapras, S. Kyrzopoulos, M. Savvopoulou, E. Avramidou, D. Vassilopoulou, V. Voudris
 Vs. Acute effects of using an electronic nicotine-delivery device (e-cigarette) on myocardial function: comparison with the effects of regular cigarettes K. Farsalinos, D. Tsiapras, S. Kyrzopoulos, M.
Vs. Acute effects of using an electronic nicotine-delivery device (e-cigarette) on myocardial function: comparison with the effects of regular cigarettes K. Farsalinos, D. Tsiapras, S. Kyrzopoulos, M.
Mitral Valve Repair: the Multimodal Approach and the Role of Minimally Invasive Procedures
 Cardiovascular Surgery SURGICAL TECHNOLOGY INTERNATIONAL IX Mitral Valve Repair: the Multimodal Approach and the Role of Minimally Invasive Procedures GERALD M. LAWRIE, M.D., F.A.C.S. CLINICAL PROFESSOR
Cardiovascular Surgery SURGICAL TECHNOLOGY INTERNATIONAL IX Mitral Valve Repair: the Multimodal Approach and the Role of Minimally Invasive Procedures GERALD M. LAWRIE, M.D., F.A.C.S. CLINICAL PROFESSOR
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Provider Checklist-Outpatient Imaging. Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469)
 Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Symptomatic Atrial Fibrillation
 Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
2/20/2015. Cardiac Evaluation of Potential Solid Organ Transplant Recipients. Issues Specific to Transplantation. Kidney Transplantation.
 DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
Introduction. Mitral regurgitation
 European Journal of Echocardiography (2010) 11, 307 332 doi:10.1093/ejechocard/jeq031 RECOMMENDATIONS European Association of Echocardiography recommendations for the assessment of valvular regurgitation.
European Journal of Echocardiography (2010) 11, 307 332 doi:10.1093/ejechocard/jeq031 RECOMMENDATIONS European Association of Echocardiography recommendations for the assessment of valvular regurgitation.
Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease
 Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Mitral regurgitation (MR) arises commonly from
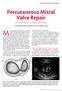 Percutaneous Mitral Valve Repair An overview of the current devices and techniques. BY RAYMOND LEUNG, MDCM, AND TED FELDMAN, MD A Mitral regurgitation (MR) arises commonly from the failure of mitral leaflet
Percutaneous Mitral Valve Repair An overview of the current devices and techniques. BY RAYMOND LEUNG, MDCM, AND TED FELDMAN, MD A Mitral regurgitation (MR) arises commonly from the failure of mitral leaflet
Analysis of Mitral Valve Replacement Outcomes is Enhanced by Meaningful Clinical Use of Electronic Health Records
 credits available for this article see page 88. Original RESEARCH & CONTRIBUTIONS Analysis of Mitral Valve Replacement Outcomes is Enhanced by Meaningful Clinical Use of Electronic Health Records John
credits available for this article see page 88. Original RESEARCH & CONTRIBUTIONS Analysis of Mitral Valve Replacement Outcomes is Enhanced by Meaningful Clinical Use of Electronic Health Records John
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
HISTORY. Questions: 1. What diagnosis is suggested by this history? 2. How do you explain her symptoms during pregnancy?
 HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
ECHOCARDIOGRAPHY PROPERTY OF ELSEVIER SAMPLE CONTENT - NOT FINAL CHAPTER 6. Hisham Dokainish, MD, FACC, FASE
 CHAPTER 6 ECHOCARDIOGRAPHY Hisham Dokainish, MD, FACC, FASE 1. How does echocardiography work? Echocardiography uses transthoracic and transesohageal probes that emit ultrasound directed at cardiac structures.
CHAPTER 6 ECHOCARDIOGRAPHY Hisham Dokainish, MD, FACC, FASE 1. How does echocardiography work? Echocardiography uses transthoracic and transesohageal probes that emit ultrasound directed at cardiac structures.
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
New insights in the assessment of right ventricular function: an echocardiographic study. Avin Calcutteea
 New insights in the assessment of right ventricular function: an echocardiographic study Avin Calcutteea Department of Public Health and Clinical Medicine Umeå University, 2013 New insights in the assessment
New insights in the assessment of right ventricular function: an echocardiographic study Avin Calcutteea Department of Public Health and Clinical Medicine Umeå University, 2013 New insights in the assessment
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014
 ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
on behalf of the AUGMENT-HF Investigators
 One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
Magnetic Resonance Quantitative Analysis. MRV MR Flow. Reliable analysis of heart and peripheral arteries in the clinical workflow
 Magnetic Resonance Quantitative Analysis MRV MR Flow Reliable analysis of heart and peripheral arteries in the clinical workflow CAAS MRV Functional Workflow Designed for imaging specialists, CAAS MRV
Magnetic Resonance Quantitative Analysis MRV MR Flow Reliable analysis of heart and peripheral arteries in the clinical workflow CAAS MRV Functional Workflow Designed for imaging specialists, CAAS MRV
Dynamic Auscultation of Heart Sounds and Murmurs. Acknowledgement. Disclosures Real or Potential Conflicts of Interest
 Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Centennial Medical Center, Nashville, TN, Vanderbilt University, Nashville, TN, Duke University Medical Center, Durham, NC, USA
 Several New Considerations in Mitral Valve Repair J. Scott Rankin, Ricardo E. Orozco, Theodore R. Addai, Tracey L. Rodgers, Robert H. Tuttle, Linda K. Shaw, Donald D. Glower Centennial Medical Center,
Several New Considerations in Mitral Valve Repair J. Scott Rankin, Ricardo E. Orozco, Theodore R. Addai, Tracey L. Rodgers, Robert H. Tuttle, Linda K. Shaw, Donald D. Glower Centennial Medical Center,
CARDIAC RISKS OF NON CARDIAC SURGERY
 CARDIAC RISKS OF NON CARDIAC SURGERY N E W S T U D I E S & N E W G U I D E L I N E S W. B. C A L H O U N, M D, F A C C 2014 ACC/AHA Guideline on perioperative cardiovascular evaluation and management
CARDIAC RISKS OF NON CARDIAC SURGERY N E W S T U D I E S & N E W G U I D E L I N E S W. B. C A L H O U N, M D, F A C C 2014 ACC/AHA Guideline on perioperative cardiovascular evaluation and management
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
The STS Mitral Repair/Replacement Composite Score: A Report of the STS Quality Measurement Task Force
 The STS Mitral Repair/Replacement Composite Score: A Report of the STS Quality Measurement Task Force 1 Vinay Badhwar, MD, 2 J. Scott Rankin, MD, 3 Xia He, MS, 4 Jeffrey P. Jacobs, MD, 5 James S. Gammie,
The STS Mitral Repair/Replacement Composite Score: A Report of the STS Quality Measurement Task Force 1 Vinay Badhwar, MD, 2 J. Scott Rankin, MD, 3 Xia He, MS, 4 Jeffrey P. Jacobs, MD, 5 James S. Gammie,
Disclosure. All the authors have no conflict of interest to disclose in this study.
 Assessment of Left Atrial Deformation and Dyssynchrony by Three-dimensional Speckle Tracking Imaging: Comparative Studies in Healthy Subjects and Patients with Atrial Fibrillation Atsushi Mochizuki, MD*;
Assessment of Left Atrial Deformation and Dyssynchrony by Three-dimensional Speckle Tracking Imaging: Comparative Studies in Healthy Subjects and Patients with Atrial Fibrillation Atsushi Mochizuki, MD*;
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
Posterior mitral annuloplasty for enhancing mitral leaflet coaptation: using a strip designed for placement in the posterior annulus
 Kim et al. Journal of Cardiothoracic Surgery (2015) 10:164 DOI 10.1186/s13019-015-0350-6 RESEARCH ARTICLE Open Access Posterior mitral annuloplasty for enhancing mitral leaflet coaptation: using a strip
Kim et al. Journal of Cardiothoracic Surgery (2015) 10:164 DOI 10.1186/s13019-015-0350-6 RESEARCH ARTICLE Open Access Posterior mitral annuloplasty for enhancing mitral leaflet coaptation: using a strip
Disclosures. Anesthesia and Lead Extractions. Lead Extractions: Objectives. Lead Removal Techniques. None
 Anesthesia and Lead Extractions Disclosures None Bryan Ahlgren DO Assistant Professor University of Colorado Dept of Anesthesiology Objectives Define lead extraction procedures and why Anesthesiologists
Anesthesia and Lead Extractions Disclosures None Bryan Ahlgren DO Assistant Professor University of Colorado Dept of Anesthesiology Objectives Define lead extraction procedures and why Anesthesiologists
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
J of Evidence Based Med & Hlthcare, pissn- 2349-2562, eissn- 2349-2570/ Vol. 2/Issue 42/Oct. 19, 2015 Page 7214
 ORGANIC TRICUSPID VALVE REPAIR WITH AUTOLOGOUS GLUTARALDEHYDE FIXED PERICARDIAL PATCH: A SINGLE CENTER RESULTS Murtaza A Chishti 1, Ajay Meena 2, Gaurav Goyal 3, Premraj Nagarwal 4, Varun Chhabra 5, Aashish
ORGANIC TRICUSPID VALVE REPAIR WITH AUTOLOGOUS GLUTARALDEHYDE FIXED PERICARDIAL PATCH: A SINGLE CENTER RESULTS Murtaza A Chishti 1, Ajay Meena 2, Gaurav Goyal 3, Premraj Nagarwal 4, Varun Chhabra 5, Aashish
Journal of the American College of Cardiology Vol. 33, No. 7, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 7, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00112-6 The Natural
Journal of the American College of Cardiology Vol. 33, No. 7, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00112-6 The Natural
17 Endocarditis. Infective endocarditis
 17 Endocarditis 234 Endocarditis refers to inflammation of the endocardium, the inner layer of the heart (including the heart valves). Endocarditis can be: infective (e.g. bacterial, fungal) non-infective
17 Endocarditis 234 Endocarditis refers to inflammation of the endocardium, the inner layer of the heart (including the heart valves). Endocarditis can be: infective (e.g. bacterial, fungal) non-infective
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
INHERIT. The Lancet Diabetes & Endocrinology In press
 INHibition of the renin angiotensin system in hypertrophic cardiomyopathy and the Effect on hypertrophy a Randomized Intervention Trial with losartan Anna Axelsson, Kasper Iversen, Niels Vejlstrup, Carolyn
INHibition of the renin angiotensin system in hypertrophic cardiomyopathy and the Effect on hypertrophy a Randomized Intervention Trial with losartan Anna Axelsson, Kasper Iversen, Niels Vejlstrup, Carolyn
May 1 6, 2016 Loews Atlanta Hotel Atlanta, GA PRELIMINARY PROGRAM AT A GLANCE
 Sunday, May 1 7:00-8:30 pm Image Optimization Workshop: 2D Echocardiography Moderators: Fabio De Vasconelos Papa, MD; Mark A. Taylor, MD : Annemarie Thompson, MD Speakers: Gregg S. Hartman, MD Lori B.
Sunday, May 1 7:00-8:30 pm Image Optimization Workshop: 2D Echocardiography Moderators: Fabio De Vasconelos Papa, MD; Mark A. Taylor, MD : Annemarie Thompson, MD Speakers: Gregg S. Hartman, MD Lori B.
Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis. Michael A. Blazing
 Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis Michael A. Blazing Outline The coming crush A practical approach to clinical risk assessment Classic approach to
Perioperative Risk Stratification for Noncardiac Surgical Patients with Cardiac Diagnosis Michael A. Blazing Outline The coming crush A practical approach to clinical risk assessment Classic approach to
Workshop B: Essentials of Neonatal Cardiology and CHD Anthony C. Chang, MD, MBA, MPH CARDIAC INTENSIVE CARE
 SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
Updated Cardiac Resynchronization Therapy Guidelines
 The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Current concepts for minimally invasive mitral valve repair
 Endorsed by proceedings in Intensive Care Cardiovascular Anesthesia Review article HSR Proc Intensive Care Cardiovasc Anesth. In press. Current concepts for minimally invasive mitral valve repair 1 B.
Endorsed by proceedings in Intensive Care Cardiovascular Anesthesia Review article HSR Proc Intensive Care Cardiovasc Anesth. In press. Current concepts for minimally invasive mitral valve repair 1 B.
Cardiology Fellowship Manual. Goals & Objectives -Cardiac Imaging- 1 Page
 Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 Page 2015-2016 UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION
Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 Page 2015-2016 UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
CTA OF THE EXTRACORONARY HEART
 CTA OF THE EXTRACORONARY HEART Charles White MD Director of Thoracic Imaging Department of Radiology University of Maryland NO DISCLOSURES CWHITE@UMM.EDU CARDIAC CASE DISTRIBUTION Coronary CTA 30% ED chest
CTA OF THE EXTRACORONARY HEART Charles White MD Director of Thoracic Imaging Department of Radiology University of Maryland NO DISCLOSURES CWHITE@UMM.EDU CARDIAC CASE DISTRIBUTION Coronary CTA 30% ED chest
Valvular Heart Disease in the Patient Undergoing Noncardiac Surgery
 Valvular Heart Disease in the Patient Undergoing Noncardiac Surgery Nancy A. Nussmeier, MD Chair, Department of Anesthesiology SUNY Upstate Medical University, Syracuse, NY Valvular heart disease is becoming
Valvular Heart Disease in the Patient Undergoing Noncardiac Surgery Nancy A. Nussmeier, MD Chair, Department of Anesthesiology SUNY Upstate Medical University, Syracuse, NY Valvular heart disease is becoming
Ole Dyg Pedersen a, T, Henning Bagger b, Lars Kbber c, Christian Torp-Pedersen a FACC, on behalf of the TRACE Study Group
 International Journal of Cardiology 100 (2005) 65 71 www.elsevier.com/locate/ijcard Impact of congestive heart failure and left ventricular systolic function on the prognostic significance of atrial fibrillation
International Journal of Cardiology 100 (2005) 65 71 www.elsevier.com/locate/ijcard Impact of congestive heart failure and left ventricular systolic function on the prognostic significance of atrial fibrillation
