Transvaginal repair of anterior and posterior compartment prolapse with Atrium polypropylene mesh
|
|
|
- Ernest Lane
- 8 years ago
- Views:
Transcription
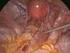
1 BJOG: an International Journal of Obstetrics and Gynaecology August 2004, Vol. 111, pp DOI: /j x Transvaginal repair of anterior and posterior compartment prolapse with Atrium polypropylene mesh Peter L. Dwyer, Barry A. O Reilly Objective To determine the efficacy and safety of a new technique using Atrium polypropylene mesh (Atrium, Hudson, New Hampshire, USA) as an overlay graft for repair of large or recurrent anterior and posterior compartment prolapse. Design A retrospective review of women who had vaginal prolapse surgery with Atrium mesh reinforcement. Setting Tertiary referral urogynaecology unit in Australia. Population Forty-seven women where mesh was placed under the bladder base with lateral extensions onto the pelvic sidewall, 33 women where a Y-shaped mesh was placed from the sacrospinous ligaments to the perineal body and 17 women who had mesh placement in both compartments. Methods Women were assessed by site-specific vaginal examination pre-operatively and post-operatively at six weeks, six months and two years. Main outcome measures All complications. Rate of recurrent prolapse assessed by the Baden Walker halfway classification system. Results Mean follow up was 29 months (range 6 to 52). Four of 64 women with anterior mesh placement (6%) developed a grade 2 asymptomatic cystocele. Five women (5%) required further surgery for recurrent prolapse at a non-mesh site. Erosion occurred in nine women (9%). Three healed after intravaginal oestrogen cream, five after excision of exposed mesh and vaginal closure and one woman also had surgical closure of a rectovaginal fistula. The risk of mesh erosion decreased over the study period. Urinary, coital and bowel symptoms were significantly improved following surgery. Conclusions This technique shows promise in correcting pelvic organ prolapse. Vaginal mesh erosion is the most common complication and is related to surgical experience. INTRODUCTION Genital prolapse is a common cause of surgery in women, which is frequently unsuccessful. In a recent Australian prevalence survey, 1 46% of women aged had symptoms of pelvic floor dysfunction and 23.7% of women had undergone a previous pelvic floor repair. A recent North American Study 2 showed that the lifetime risk of surgery for prolapse or stress incontinence was 11% with one in three patients requiring more than one surgical repair. The pelvic floor musculature is considered to be the most important factor in the maintenance of pelvic organ support with the fascia and ligaments providing secondary support. 3,4 Weakness of the muscular pelvic floor can be caused by disuse, nerve damage or trauma but is generally not amenable to surgical repair. Dissatisfaction after surgery may be caused by recurrence of prolapse but also by Urogynaecology Department, Mercy Hospital for Women, Melbourne, Australia Correspondence: Dr P. L. Dwyer, Mercy Hospital for Women, 126 Clarendon Street, East Melbourne, 3002 Victoria, Australia. D RCOG 2004 BJOG: an International Journal of Obstetrics and Gynaecology the persistence or development of urinary, anorectal symptoms or dyspareunia caused by excessive scarring or vaginal skin excision. Synthetic non-absorbable mesh has been used extensively for the abdominal repair of vaginal prolapse by placing mesh over the anterior and posterior vaginal wall and attaching the mesh to the anterior sacrum, providing good vaginal support. 5 This success has encouraged us to explore the transvaginal use of mesh in order to improve the anatomical and functional results of pelvic floor surgery. In this study, we assessed the efficiency and complications of Atrium polypropylene mesh (Atrium, Hudson, New Hampshire, USA) in the repair of recurrent or large anterior and posterior compartment vaginal prolapse. METHODS Ninety-seven patients had transvaginal surgery with Atrium mesh reinforcement performed for symptomatic vaginal prolapse between February 1999 and May Atrium mesh is a monofilament polypropylene woven of 92 g/m 2 weight with a pore size (interfibre space) of 800 Am. Seventeen women had mesh placed both in the anterior and posterior vaginal mesh repair (APVMR); 47 women only in
2 832 P.L. DWYER & B.A. O REILLY the anterior compartment (AVMR) and in 33 women only in the posterior compartment (PVMR). The indication for mesh usage was recurrent vaginal prolapse or where a large fascial defect was unsuitable for standard repair alone. Anterior and posterior Atrium mesh repairs were combined with a number of other pelvic floor surgeries, namely, vaginal hysterectomy (10), sacrospinous fixation (12), bilateral iliococcygeal fixation (4), abdominal sacrocolpopexy (1) and tension-free vaginal (TVT) sling (24). All patients had a standardised urogynaecological history and examination performed before and after surgery including data on urinary, coital and bowel symptoms. Urodynamic evaluation was performed when indicated for urinary symptoms. All patients were examined vaginally with a Sims speculum in the left lateral and sitting positions with the Valsalva manoeuvre. Vaginal support was graded using the modified Baden Walker halfway system. 6 Prophylactic antibiotics were routinely given intravenously prior to surgery. Data are presented as mean or median and range and as number (%). Differences are presented with their 95% confidence intervals. Approval was obtained for conducting this study from the hospital Ethics and Research Committee. For an anterior compartment mesh repair, a midline incision was made along the anterior vaginal wall suburethrally to the vaginal apex and the bladder was separated from the vagina. This dissection was extended bilaterally to the ischial spines and advanced anteriorly along the arcus tendineus. Midline plication of the fascial layer was performed using interrupted 2/0 polydioxanone (PDS) sutures. Atrium mesh (2 15 cm) with a widened elliptical mid-portion (5 cm) was placed under the bladder base and each lateral extension was positioned onto the iliococcygeal fascia anterior to the ischial spines (Fig. 1A). The mesh was usually unsutured, although in four cases of complete vaginal eversion, a 1 PDS suture was placed into the iliococcygeal fascia using a Miya hook to attach the mesh and vagina as described previously. 7 The mesh overlay was sutured with 2/0 Vicryl sutures at the anterior and posterior margins for stabilisation and to prevent folding. If there was coexistent urodynamic stress incontinence, a TVT sling procedure was performed according to Ulmsten et al. 8 For a posterior compartment mesh repair, a midline incision from the perineum to the vaginal apex was made and the vagina detached from the rectum with sharp dissection, which was extended, laterally to the ischiorectal fossa and superiorly onto the sacrospinous ligament. If an enterocele was present, the sac was dissected out and opened; and then closed by high ligation using 2/0 PDS. Any fascial defect in the rectovaginal septum was repaired using 2/0 PDS suture. Atrium mesh (10 15 cm) was fashioned in a Y shape, the arms of the Y (2 cm wide), and the body (5 cm wide) as shown in Fig. 1B. The arms of the Y were placed onto the sacrospinous ligaments bilaterally with the main body of mesh overlaying the repaired rectovaginal fascia and the perineal body. The mesh was also stabilised with 2/0 Vicryl sutures placed superiorly, laterally and onto the perineal body. Rectal examination was performed routinely to exclude damage or the inadvertent placement of sutures into the rectum. For a combined anterior and posterior compartment mesh repair, a midline vertical incision was made suburethrally extending along the full vaginal length to the perineum with wide lateral sharp dissection in the anterior, apical and posterior compartments. The standard repair was performed as outlined above for each compartment. Atrium mesh was fashioned into a cross shape and laid along the repair with the arms of the mesh extending along the iliococcygeal fascia anterior to the ischial spines and the long stem of the cross extending over the vaginal apex, repaired enterocele and rectovaginal fascia to the perineum (Fig. 1C). In 12 patients with large vaginal eversions or enteroceles, sutures of 1 PDS were placed into the sacrospinous ligament, using a Miya hook, through the arms of the mesh and then through the full thickness of the vaginal epithelium. Following placement of the mesh overlay, the vagina was closed. A cystourethroscopy and rectal examination were performed to exclude any urinary or rectal injury. No financial assistance was received from any company in the design or execution of this study. RESULTS Atrium polypropylene mesh was used in anterior compartment repairs on 64 women, in the posterior compartment on 50 women and in both compartments on 17 women. The median age at the time of surgery was 61 years (range 30 to 86 years); the median parity was 3 (range 0 to 8) with three women being nulliparous. Many women had previous pelvic surgery including one or more vaginal repairs (48), sacrospinous fixation (15), abdominal sacrocolpopexy (3), vaginal (24) and abdominal hysterectomy (37). Fourteen had a previous Burch colposuspension and 2 a pubovaginal sling. There were few serious complications. Two women had secondary post-operative haemorrhages ( >500 ml) and one woman developed a rectovaginal fistula on the fifth day. The mean follow up was 29 months (6 to 52 months). Ninety-seven women were reviewed at 6 weeks, 96 women at 6 months, 91 women at 12 months and 77 women had follow up of >24 months. The pre- and post-operative vaginal findings are shown in Table 1. Of the 64 women who had polypropylene mesh placed in the anterior compartment, four women (6%) developed an asymptomatic grade 2 cystocele by 12 months and one woman (1.5%) a grade 2 cuff prolapse. Of the 17 women who had mesh reinforcement of both anterior and posterior compartments, one woman (6%) required a further anterior repair after 30 months for recurrent cystocele and repair
3 ATRIUM POLYPROPYLENE MESH IN TRANSVAGINAL REPAIR 833 Fig. 1. Mesh placement in the anterior (A) and posterior (B) vaginal compartments. Combined anterior and posterior mesh repair (C). of posterior mesh erosion. Two patients (4%) who had posterior compartment mesh repairs with standard anterior repair developed an asymptomatic grade 2 cystocele. There was no recurrence of posterior compartment prolapse in the 50 women who had mesh reinforcement posteriorly, although four women (6%) who had anterior compartment mesh reinforcement developed significant symptomatic posterior compartment prolapse (grade 2). There were nine mesh erosions (9%) overall: three erosions on the anterior vaginal wall and six on the posterior wall. Seven mesh erosions (78%) were diagnosed within six months. Three women were asymptomatic and the vaginal wall re-epithelised after administration of intravaginal oestrogen for between six weeks and three months. Six patients had symptoms of vaginal discharge, bleeding or dyspareunia and were cured after excision of
4 834 P.L. DWYER & B.A. O REILLY Table 1. Number of patients with significant vaginal prolapse (grade 2 Baden Walker) pre- and post-operatively. Repair with mesh No. with pre-op prolapse 2 (%) Follow up recurrent prolapse 2 (cumulative no. of patients) 6 months (94) 12 months (91) 24 months (77) B C E R B C E R B C E R Anterior (A) 47 (48) * 4* Posterior (P) 33 (34) A and P 17 (18) B ¼ bladder, C ¼ cuff, E ¼ enterocele, R ¼ rectum. * Same patients. the exposed mesh, undermining of the vaginal edges and then suture closure without tension. One woman had a rectovaginal fistula diagnosed one week post-operatively. On proctoscopy, the Atrium mesh was seen protruding through the rectal mucosa. The rectovaginal fistula was repaired transvaginally seven weeks later with partial excision of the Atrium mesh and a layered closure of the fistula with a Martius graft. Follow up over 30 months showed no recurrence of the fistula. Over the study period, the rate of mesh erosion decreased from 19% in 1999 (3 of 16) to 13% in 2000 (4 of 32) and 4% in 2001/ 2002 (2 of 49) (differences not significant). Sixty-seven patients (69%) were sexually active preoperatively and 66 (68%) were sexually active at the 24- month review. Dyspareunia was reported by 25 patients (25.8%) before surgery, 6 (6.3%) at 6 months, 7 (7.7%) at 12 months and 7 (9.1%) at 24 months (each change significant vs pre-op value, data not shown). In three patients, the dyspareunia occurred de novo following surgery (two AVMR and one PVMR). Urinary and bowel functional symptoms pre- and postoperatively are shown in Table 2. Urinary and bowel symptoms were common before surgery and were significantly improved following surgery. At 24 months postoperatively, there were three patients with de novo urgency (two had an APVMR and one AVMR). Three patients had de novo urge incontinence (two had APVMR and one had PVMR). One patient had de novo constipation (AVMR). Table 2. Functional symptoms pre- and post-operatively. Symptom Pre-op (n ¼ 97) 24 months post-op (n ¼ 77) Percent difference (95% CI)* Stress incontinence 37 (38.1) 3 (3.9) 34.2 (21.7, 46.8) Urge 52 (53.6) 12 (15.6) 38.0 (23.6, 52.4) Urge incontinence 40 (41.2) 7 (7.2) 32.1 (18.9, 45.4) Constipation 21 (21.6) 2 (2.6) 19.1 (8.9, 29.2) Dyspareunia 20 (20.6) 7 (7.2) 11.5 (0.7, 22.4) Voiding difficulty 32 (33.0) 1 (1.0) 31.7 (20.0, 43.4) * 95% confidence intervals of percentage difference. Twenty-five women had urodynamically confirmed stress incontinence. Twenty-four women had TVT slings and one had a Burch colposuspension. Three women redeveloped symptoms of stress incontinence after surgery (one PVMR and TVT; one PVMR; one APVMR). One patient had voiding difficulty at 24-month review that occurred de novo following AVMR and sling. DISCUSSION In this study, Atrium polypropylene mesh placed under the bladder base with extensions up the pelvic sidewall provided good medium term support for the anterior compartment with a low recurrence rate (6%) but with a small but significant morbidity. Some pelvic surgeons believe that complete vaginal reconstruction of all compartments is necessary, 9 but our philosophy with regard to reparative vaginal surgery has been to repair only areas where defective support was found. Seven patients (7%) in this series developed de novo prolapse during the follow up period in a compartment that clinically had previously appeared well supported. The prophylactic use of synthetic mesh for prolapse women with no anatomical defects requires further evaluation. The major morbidity was vaginal erosion, which in one case possibly resulted in a rectovaginal fistula. Most cases were diagnosed in the first six months post-operatively and the majority were managed conservatively or with minor surgical intervention. Although fistula formation is a potential risk of mesh, we believe that this is an uncommon complication and we have no further fistulae with subsequent experience in 140 women using Vypro II mesh (Ethicon, Summerville, New Jersey, USA). Synthetic meshes have been used for abdominal wall hernia surgery since the late 1950s. 10,11 Nevertheless, gynaecologists have been reluctant to use synthetic mesh in reconstructive pelvic surgery because of the risk of infection and erosion into the urinary, genital or gastrointestinal tract. The synthetic non-absorbable meshes most commonly used have been polypropylene (Marlex, Prolene, Atrium), polyethylene terephthalate (Mersilene), and
5 ATRIUM POLYPROPYLENE MESH IN TRANSVAGINAL REPAIR 835 expanded polytetrafluoroethylene (PTFE) (Gore-Tex). Polypropylene mesh is monofilament while polyethylene and PTFE are multifilament synthetic meshes. The other important quality of synthetic mesh is their interfibre spaces (pore size), which should be of sufficient size not to harbour bacteria but allow macrophages and leucocytes to penetrate, while also permitting connective tissue ingrowth for permanent support. Bobyn et al. 12 found that the best mechanical anchorage occurs when pore size was between 50 and 200 Am with an average of 90 Am. Currently, polypropylene mesh is the most widely used synthetic prosthesis in general surgery and gynaecology. 13 In 1996, Julian 14 reported a prospective randomised study of synthetic, non-absorbable mesh in 24 women with recurrent anterior wall prolapse. After two years, four women in the control group and none in the mesh group had recurrent anterior wall prolapse. Three women (33%) with mesh repair had erosions. Flood et al. 15 placed a strip of Marlex mesh under the vesicourethral junction extending into the Cave of Retzius and found no anterior wall prolapse recurrences but three mesh erosions after three years. Migliari and Usai 16 placed mixed fibre mesh (60% polyglactin and 40% polyester) under the urethra and bladder base of 15 women. Two patients developed posterior compartment prolapse after a mean follow up of 23 months. Synthetic non-absorbable mesh has been used less frequently in the transvaginal repair of posterior compartment prolapse. Watson et al. 17 placed a strip of polypropylene mesh (Marlex) between the rectum and the vagina for posterior compartment prolapse. After a mean of 29 months, eight of nine patients had improved defecation. One patient had a wound infection and one developed dyspareunia post-operatively. There were no mesh erosions and the incidence of prolapse pre- and post-operatively was not stated. Synthetic absorbable mesh has been used for prolapse in both compartments. Sand et al. 18 reported a prospective randomised study of three strips of polyglactin 910 mesh (Vicryl mesh; Ethicon) placed on the anterior endopelvic fascia. At 12 months follow up, there was a significantly lower recurrence rate in the mesh group compared with the controls (25% vs 43%, P ¼ 0.02). Weber et al. 19 found no significant difference in recurrence of cystocele in their prospective randomised study using the same mesh. The positioning of the mesh as much as the type used influences the anatomical and functional outcome. In this study, the mesh was laid over the fascial repair in both compartments. The use of extensions onto the pelvic sidewall or to the sacrospinous ligaments superiorly provided a strong continuous scaffold for fibrous tissue ingrowth extending from the pelvic floor ligaments and muscles superiorly through the rectovaginal septum onto the perineal body, thus mimicking the normal fascial supports of each compartment. A standard fascial repair was performed but no or little vaginal epithelium was removed. We found that the vagina adheres to the underlying mesh and the vaginal wall remodels to the appropriate site once the underlying pulsion pressures have been relieved, providing a better functional result while avoiding vaginal stenosis caused by excessive vaginal epithelial removal. The functional results of surgery are as important as the anatomical outcome. In our study, the incidence of dyspareunia halved following surgery irrespective of compartment. Salvatore et al. 20 found an increased incidence of dyspareunia following the use of Prolene mesh. In our study, the risk of new functional symptoms was low following vaginal mesh surgery. We believe that lateral dissection and wide placement of synthetic mesh overlay is important in preventing excessive folding and scarring in the anterior and posterior compartments. The risk of mesh erosion varies depending on the type of mesh used and its placement. Other possible factors affecting the incidence of erosion are the use of prophylactic antibiotics, menopausal status and age, the use of pre-operative oestrogens and, post-operatively, pelvic infection. Current evidence would suggest that monofilament polypropylene has the lowest incidence of infection and erosion compared with the other non-absorbable meshes. 13 Recently, lighter meshes of polypropylene and vicryl (Vypro I and II; Ethicon) have been introduced for abdominal hernia repair and a monofilament polypropylene mesh (Gynemesh PS; Ethicon) for pelvic reconstructive surgery. These are lighter (area weight 50 g/m 2 ) compared with Atrium (92 g/m 2 ), Prolene (85 g/m 2 ) and Marlex (95 g/m 2 ), more flexible, softer and easier to handle, and have been shown in animal studies to have less contracture and folding during healing. To date, there are no studies in humans to indicate the rate of erosion of these meshes. This retrospective study described a new approach to the vaginal placement of synthetic mesh with a good anatomical and functional outcome but does not prove that mesh reinforcement provides better long term support than fascial repair alone. This would require a prospective randomised trial similar to a recently published prolapse study 21 comparing the abdominal and vaginal approach. However, our experience is that even the most complicated genital prolapse can be successfully treated transvaginally using mesh while maintaining adequate vaginal size and function. We need to clarify when and where synthetic grafts should be used in the anterior and posterior vaginal compartments, how it should be best placed and the most appropriate type of prosthesis. Acknowledgements The authors would like to thank Dr Judith Goh for her contribution with the early collection of data.
6 836 P.L. DWYER & B.A. O REILLY References 1. Maclennan AH, Taylor AW, Wilson AW, Wilson D. The prevalence of pelvic floor disorders and their relationship to gender, age and mode of delivery. Br J Obstet Gynaecol 2000;107: Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 1997;89: Gosling JA. The structure of the bladder neck, urethra and pelvic floor in relation to female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1996;7: DeLancey JO. Structural anatomy of the posterior pelvic compartment as it relates to rectocele. Am J Obstet Gynecol 1999;180: Fynes M, Goh J, Chong C, et al. Abdominal sacral colpopexy for vaginal vault prolapse. Int Urogynecol J Pelvic Floor Dysfunct 2001;12: Baden W, Walker T. Surgical Repair of Vaginal Defects. Philadelphia: JB Lippincott, Dwyer PL, Schraffordt S. Iliococcygeal fixation middle compartment prolapse. In: Stanton SL, Zimmern PE, editors. Female Pelvic Reconstructive Surgery. London: Springer-Verlag, 2002: Ulmsten U, Henrikson L, Johnson P, Varhos G. An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1996;7: Benson JT, Lucent V, McClellan E. Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects. A prospective randomised study of long-term outcome evaluation. Am J Obstet Gynecol 1996;175: Usher FC, Gannon JR. Marlex mesh, a new plastic mesh for replacing tissue defects. Arch Surg 1959;78: Lichtenstern IL, Shulman AG, Parutz Amid P, Montllor MM. The tension-free hernioplasty. Am J Surg 1989;157: Bobyn JD, Wilson GJ, MacGregor DC, et al. Effect of pore size on the peel strength of attachment of fibrous tissue to porous-surfaced implants. PJ Biomed Mater Res 1982;16: Birch C, Fynes MM. The role of synthetic and urological prosthesis in reconstructive pelvic floor surgery. Curr Opin Obstet Gynecol 2002; 14: Julian TM. Efficacy of Marlex mesh in the repair of severe, recurrent vaginal prolapse of the anterior midvaginal wall. Am J Obstet Gynecol 1996;175: Flood CG, Drutz HP, Waja L. Anterior colporrhaphy reinforced with Marlex Mesh for the treatment of cystoceles. Int Urogynecol J Pelvic Floor Dysfunct 1998;9: Migliari R, Usai E. Treatment results using a mixed fiber mesh in patients with grade IV cystocele. J Urol 1999;161: Watson SJ, Loder PB, Halligan S, Bartram CI, Kamm MA, Phillips RK. Transperineal repair of symptomatic rectocele with Marlex mesh: a clinical, physiological and radiologic assessment of treatment. J Am Coll Surg 1996;183: Sand PK, Koduri S, Lobel RW, et al. Prospective randomized trial of polyglactin 910 mesh to prevent recurrence of cystocele and rectoceles. Am J Obstet Gynecol 2001;184: Weber AM, Walters MD, Piedmonte MR, Ballard LA. Anterior colporrhaphy: a randomized trial of three surgical techniques. Am J Obstet Gynecol 2001;185: Salvatore S, Soligno M, Meschia M, Luppino G, Piffarotti P, Arcari V. Prosthetic surgery for genital prolapse: functional outcome. Neurourol Urodyn 2002;21: Maher CF, Qatawneh AM, Dwyer PL, Carey MP, Cornish A, Schluter P. Abdominal sacral colpopexy or vaginal sacrospinous colpopexy for vaginal vault prolapse: a prospective randomised study. Am J Obstet Gynecol 2004;190: Accepted 5 March 2004
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Mesh Erosion and What to do
 Disclosures Mesh Erosion and What to do None Michelle Y. Morrill, MD Chief of Urogynecology, TPMG Director of Urogynecology, Kaiser San Francisco Assistant Professor, Volunteer Faculty Dept of Ob/Gyn,
Disclosures Mesh Erosion and What to do None Michelle Y. Morrill, MD Chief of Urogynecology, TPMG Director of Urogynecology, Kaiser San Francisco Assistant Professor, Volunteer Faculty Dept of Ob/Gyn,
Urinary Incontinence. Anatomy and Terminology Overview. Moeen Abu-Sitta, MD, FACOG, FACS
 Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Urogynecologic Surgical Mesh: Update on the Safety and Effectiveness of Transvaginal Placement for Pelvic Organ Prolapse
 Urogynecologic Surgical Mesh: Update on the Safety and Effectiveness of Transvaginal Placement for Pelvic Organ Prolapse July 2011 I. EXECUTIVE SUMMARY...3 II. OVERVIEW...3 III. SURGICAL MESH FOR UROGYNECOLOGIC
Urogynecologic Surgical Mesh: Update on the Safety and Effectiveness of Transvaginal Placement for Pelvic Organ Prolapse July 2011 I. EXECUTIVE SUMMARY...3 II. OVERVIEW...3 III. SURGICAL MESH FOR UROGYNECOLOGIC
Vaginal Mesh Kits for Pelvic Organ Prolapse, Friend or Foe: A Comprehensive Review
 Review Special Issue: Update on Lower Urinary Tract Symptoms TheScientificWorldJOURNAL (2009) 9, 163 189 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.19 Vaginal Mesh Kits for Pelvic Organ Prolapse,
Review Special Issue: Update on Lower Urinary Tract Symptoms TheScientificWorldJOURNAL (2009) 9, 163 189 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.19 Vaginal Mesh Kits for Pelvic Organ Prolapse,
2/21/2016. Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape. Disclosures. Objectives. No Relevant Disclosures
 Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape David R. Ellington, MD, FACOG Assistant Professor Division of Urogynecology and Pelvic Reconstructive Surgery Disclosures No Relevant Disclosures
Prolapse Surgery after Transvaginal Mesh: The Evolving Landscape David R. Ellington, MD, FACOG Assistant Professor Division of Urogynecology and Pelvic Reconstructive Surgery Disclosures No Relevant Disclosures
Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA
 Pelvic Floor Relaxation Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA Disclosures Beverly Hashimoto: GE Medical Systems: research support and consultant (all fees given to Virginia
Pelvic Floor Relaxation Beverly E Hashimoto, M.D. Virginia Mason Medical Center, Seattle, WA Disclosures Beverly Hashimoto: GE Medical Systems: research support and consultant (all fees given to Virginia
Vaginal Mesh: The FDA Decision and Repurcussions. Roger Dmochowski MD, FACS Dept of Urology Vanderbilt University Medical Center Nashville, TN
 Vaginal Mesh: The FDA Decision and Repurcussions Roger Dmochowski MD, FACS Dept of Urology Vanderbilt University Medical Center Nashville, TN 1 ANATOMY FUNCTION 2 Mesh vs No Mesh Outcomes Sivaslioglu 2007
Vaginal Mesh: The FDA Decision and Repurcussions Roger Dmochowski MD, FACS Dept of Urology Vanderbilt University Medical Center Nashville, TN 1 ANATOMY FUNCTION 2 Mesh vs No Mesh Outcomes Sivaslioglu 2007
TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION
 TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION PRESENTED BY: THE PINKERTON LAW FIRM, PLLC The Pinkerton Law Firm is located in Houston, Texas. The firm specializes in mass tort litigation, including
TRANSVAGINAL MESH TVM HEALTH CONCERNS AND LITIGATION PRESENTED BY: THE PINKERTON LAW FIRM, PLLC The Pinkerton Law Firm is located in Houston, Texas. The firm specializes in mass tort litigation, including
Clinical audit of the use of tension-free vaginal tape as a surgical treatment for urinary stress incontinence, set against NICE guidelines
 GYNAECOLOGY Clinical audit of the use of tension-free vaginal tape as a surgical treatment for urinary stress incontinence, set against NICE guidelines NATALIA PRICE and SIMON R JACKSON The John Radcliffe
GYNAECOLOGY Clinical audit of the use of tension-free vaginal tape as a surgical treatment for urinary stress incontinence, set against NICE guidelines NATALIA PRICE and SIMON R JACKSON The John Radcliffe
Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
Mesh surgery; rationale and concepts?
 Mesh surgery; rationale and concepts? Jan-Paul Roovers uro-gynaecologist, AMC Amsterdam medical director Alant Vrouw Amsterdam Pelvic floor center Amsterdam Ultimate goals of prolapse surgery Optimal restoration
Mesh surgery; rationale and concepts? Jan-Paul Roovers uro-gynaecologist, AMC Amsterdam medical director Alant Vrouw Amsterdam Pelvic floor center Amsterdam Ultimate goals of prolapse surgery Optimal restoration
Pelvic Organ Prolapse FAQs
 What is prolapse? Prolapse is a hernia of the vagina that a woman may feel as a bulge or pressure. This is referred to in many different ways, including dropped bladder, dropped uterus, dropped vagina,
What is prolapse? Prolapse is a hernia of the vagina that a woman may feel as a bulge or pressure. This is referred to in many different ways, including dropped bladder, dropped uterus, dropped vagina,
Prolapse Repair Systems. a guide To correcting PELVIC ORGAN PROLAPSE
 Anterior PROLAPSE & Posterior REPAIR SYSTEM Prolapse Repair Systems a guide To correcting PELVIC ORGAN PROLAPSE Restore Your Body Pelvic organ prolapse occurs when pelvic structures, like the bladder or
Anterior PROLAPSE & Posterior REPAIR SYSTEM Prolapse Repair Systems a guide To correcting PELVIC ORGAN PROLAPSE Restore Your Body Pelvic organ prolapse occurs when pelvic structures, like the bladder or
Tension-free vaginal tape sling for recurrent stress incontinence after transobturator tape sling failure
 Int Urogynecol J (2007) 18:309 313 DOI 10.1007/s00192-006-0149-z ORIGINAL ARTICLE Tension-free vaginal tape sling for recurrent stress incontinence after transobturator tape sling failure Robert D. Moore
Int Urogynecol J (2007) 18:309 313 DOI 10.1007/s00192-006-0149-z ORIGINAL ARTICLE Tension-free vaginal tape sling for recurrent stress incontinence after transobturator tape sling failure Robert D. Moore
FEMALE UROLOGY Suprapubic sling adjustment: minimally invasive method of curing recurrent stress incontinence after sling surgery
 FEMALE UROLOGY Suprapubic sling adjustment: minimally invasive method of curing recurrent stress incontinence after sling surgery Choe JM Urodynamics and Continence Center, Division of Urology, University
FEMALE UROLOGY Suprapubic sling adjustment: minimally invasive method of curing recurrent stress incontinence after sling surgery Choe JM Urodynamics and Continence Center, Division of Urology, University
VAGINAL MESH WHAT IS THE FUTURE? Ryan R. Stratford, MD, MBA FPMRS
 VAGINAL MESH WHAT IS THE FUTURE? Ryan R. Stratford, MD, MBA FPMRS CONFLICTS OF INTEREST American Urogynecologic Society Board of Directors OBJECTIVES Discuss the cause for the development of transvaginal
VAGINAL MESH WHAT IS THE FUTURE? Ryan R. Stratford, MD, MBA FPMRS CONFLICTS OF INTEREST American Urogynecologic Society Board of Directors OBJECTIVES Discuss the cause for the development of transvaginal
August 25, 2011. Dear Drs. Hamburg and Shuren,
 August 25, 2011 Margaret A. Hamburg, M.D. Commissioner Food and Drug Administration Department of Health and Human Services WO 2200 10903 New Hampshire Avenue Silver Spring, MD 20993-0002 Jeffrey E. Shuren,
August 25, 2011 Margaret A. Hamburg, M.D. Commissioner Food and Drug Administration Department of Health and Human Services WO 2200 10903 New Hampshire Avenue Silver Spring, MD 20993-0002 Jeffrey E. Shuren,
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES. Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida
 MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
Systematic review of the efficacy and safety of using mesh or grafts in surgery for uterine or vaginal vault prolapse
 Systematic review of the efficacy and safety of using mesh or grafts in surgery for uterine or vaginal vault prolapse Xueli Jia, Cathryn Glazener, Graham Mowatt, David Jenkinson, Cynthia Fraser, Jennifer
Systematic review of the efficacy and safety of using mesh or grafts in surgery for uterine or vaginal vault prolapse Xueli Jia, Cathryn Glazener, Graham Mowatt, David Jenkinson, Cynthia Fraser, Jennifer
Vaginal mesh erosion after abdominal sacral colpopexy
 Vaginal mesh erosion after abdominal sacral colpopexy Anthony G. Visco, MD, Alison C. Weidner, MD, Matthew D. Barber, MD, Evan R. Myers, MD, MPH, Geoffrey W. Cundiff, MD, Richard C. Bump, MD, and W. Allen
Vaginal mesh erosion after abdominal sacral colpopexy Anthony G. Visco, MD, Alison C. Weidner, MD, Matthew D. Barber, MD, Evan R. Myers, MD, MPH, Geoffrey W. Cundiff, MD, Richard C. Bump, MD, and W. Allen
Vaginal prolapse repair surgery with mesh
 Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR.
 TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
CONDITIONS REQUIRING IsolveTEM
 CONDITIONS REQUIRING IsolveTEM The IsolveTEM procedure uses a soft elastic synthetic mesh to restore normal anatomy and tissue contour, and corrects symptoms in the case of a Pelvic Organ Prolapse (POP)..
CONDITIONS REQUIRING IsolveTEM The IsolveTEM procedure uses a soft elastic synthetic mesh to restore normal anatomy and tissue contour, and corrects symptoms in the case of a Pelvic Organ Prolapse (POP)..
Should SUI Surgery be Combined with Pelvic Organ Prolapse Surgery?
 Should SUI Surgery be Combined with Pelvic Organ Prolapse Surgery? Geoffrey W. Cundiff, M.D. 36 th National Congress of the South African Society of Obstetricians and Gynaecologists SASOG 2014 Learning
Should SUI Surgery be Combined with Pelvic Organ Prolapse Surgery? Geoffrey W. Cundiff, M.D. 36 th National Congress of the South African Society of Obstetricians and Gynaecologists SASOG 2014 Learning
Science behind it. Life ahead of it. Transabdominal Pelvic Floor Restoration
 Science behind it. Life ahead of it. Transabdominal Pelvic Floor Restoration Our Story Over 10 years ago, a urogynecologist set out to develop a mesh specifically with a woman s anatomy in mind. He created
Science behind it. Life ahead of it. Transabdominal Pelvic Floor Restoration Our Story Over 10 years ago, a urogynecologist set out to develop a mesh specifically with a woman s anatomy in mind. He created
Tension-Free Vaginal Tape: Outcomes Among Women With Primary Versus Recurrent Stress Urinary Incontinence
 Tension-Free Vaginal Tape: Outcomes Among Women With Versus Stress Urinary Incontinence C. R. Rardin, MD, N. Kohli, MD, P. L. Rosenblatt, MD, J. R. Miklos, MD, R. Moore, MD, and W. C. Strohsnitter, MS
Tension-Free Vaginal Tape: Outcomes Among Women With Versus Stress Urinary Incontinence C. R. Rardin, MD, N. Kohli, MD, P. L. Rosenblatt, MD, J. R. Miklos, MD, R. Moore, MD, and W. C. Strohsnitter, MS
capio Sacrospinous Ligament Suspension: Improved Outcomes Using the Capio Suture Capturing Device Suture Capturing Device
 Roger P. Goldberg, MD MPH Assistant Professor of Obstetrics and Gynecology Northwestern University Medical School Director of Research, ENH Urogynecology Evanston, Illinois, USA TECHNIQUE SPOTLIGHT Sacrospinous
Roger P. Goldberg, MD MPH Assistant Professor of Obstetrics and Gynecology Northwestern University Medical School Director of Research, ENH Urogynecology Evanston, Illinois, USA TECHNIQUE SPOTLIGHT Sacrospinous
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006
 Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
Prevention & Treatment of De Novo Stress Incontinence after POP. Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX.
 Prevention & Treatment of De Novo Stress Incontinence after POP Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX Surgery Presenter Disclosure No Conflict of Interest to disclose No Financial
Prevention & Treatment of De Novo Stress Incontinence after POP Andy Vu, DO, FACOG UNT Health Science Center Fort Worth, TX Surgery Presenter Disclosure No Conflict of Interest to disclose No Financial
Position Statement on Mesh Midurethral Slings for Stress Urinary Incontinence
 Position Statement on Mesh Midurethral Slings for Stress Urinary Incontinence The polypropylene mesh midurethral sling is the recognized worldwide standard of care for the surgical treatment of stress
Position Statement on Mesh Midurethral Slings for Stress Urinary Incontinence The polypropylene mesh midurethral sling is the recognized worldwide standard of care for the surgical treatment of stress
INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS
 INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS Analysis of NHS information on surgery for stress urinary incontinence and pelvic organ prolapse in Scotland Contents 1 Introduction 1 Treatment for these
INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS Analysis of NHS information on surgery for stress urinary incontinence and pelvic organ prolapse in Scotland Contents 1 Introduction 1 Treatment for these
Sonographic Evaluation of Anatomic Results After the Pubovaginal Sling Procedure for Stress Urinary Incontinence
 Article Sonographic Evaluation of Anatomic Results After the Pubovaginal Sling Procedure for Stress Urinary Incontinence Hann-Chorng Kuo, MD Objective. To investigate the anatomic changes after the pubovaginal
Article Sonographic Evaluation of Anatomic Results After the Pubovaginal Sling Procedure for Stress Urinary Incontinence Hann-Chorng Kuo, MD Objective. To investigate the anatomic changes after the pubovaginal
SURGICAL MESH FOR TREATMENT OF WOMEN WITH PELVIC ORGAN PROLAPSE AND STRESS URINARY INCONTINENCE FDA EXECUTIVE SUMMARY
 SURGICAL MESH FOR TREATMENT OF WOMEN WITH PELVIC ORGAN PROLAPSE AND STRESS URINARY INCONTINENCE FDA EXECUTIVE SUMMARY OBSTETRICS & GYNECOLOGY DEVICES ADVISORY COMMITTEE MEETING SEPTEMBER 8-9, 2011 TABLE
SURGICAL MESH FOR TREATMENT OF WOMEN WITH PELVIC ORGAN PROLAPSE AND STRESS URINARY INCONTINENCE FDA EXECUTIVE SUMMARY OBSTETRICS & GYNECOLOGY DEVICES ADVISORY COMMITTEE MEETING SEPTEMBER 8-9, 2011 TABLE
SOGC Recommendations for Urinary Incontinence
 The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
Insertion and Removal of Vaginal Mesh for Pelvic Organ Prolapse
 CLINICAL OBSTETRICS AND GYNECOLOGY Volume 53, Number 1, 99 114 r 2010, Lippincott Williams & Wilkins Insertion and Removal of Vaginal Mesh for Pelvic Organ Prolapse TYLER M. MUFFLY, MD and MATTHEW D. BARBER
CLINICAL OBSTETRICS AND GYNECOLOGY Volume 53, Number 1, 99 114 r 2010, Lippincott Williams & Wilkins Insertion and Removal of Vaginal Mesh for Pelvic Organ Prolapse TYLER M. MUFFLY, MD and MATTHEW D. BARBER
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse
 Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
2 of 6 10/17/2014 9:51 AM
 1 of 6 10/17/2014 9:51 AM 010101 Free 14-Day Trial Tutorial Help Search by keyword or medical code User Name: Password: Directory Print Email Advanced Search Medical Disability Advisor > Cystocele Or Rectocele
1 of 6 10/17/2014 9:51 AM 010101 Free 14-Day Trial Tutorial Help Search by keyword or medical code User Name: Password: Directory Print Email Advanced Search Medical Disability Advisor > Cystocele Or Rectocele
OPEN TENSION FREE REPAIR OF INGUINAL HERNIAS; THE LICHTENSTEIN TECHNIQUE
 C:\251 GNA\preperitoneal hernia repair\lichtenstein-english.doc To be considered for publication in BMC-Surgery OPEN TENSION FREE REPAIR OF INGUINAL HERNIAS; THE LICHTENSTEIN TECHNIQUE George H. Sakorafas,
C:\251 GNA\preperitoneal hernia repair\lichtenstein-english.doc To be considered for publication in BMC-Surgery OPEN TENSION FREE REPAIR OF INGUINAL HERNIAS; THE LICHTENSTEIN TECHNIQUE George H. Sakorafas,
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
ROYAL AUSTRALASIAN COLLEGE OF SURGEONS
 ROYAL AUSTRALASIAN COLLEGE OF SURGEONS SUBMISSION TO THE HEALTH SELECT COMMITTEE ON THE PETITION 2011 / 102 CARMEL BERRY AND CHARLOTTE KORTE REGARDING SURGICAL MESH MAY 2015 Introduction The Royal Australasian
ROYAL AUSTRALASIAN COLLEGE OF SURGEONS SUBMISSION TO THE HEALTH SELECT COMMITTEE ON THE PETITION 2011 / 102 CARMEL BERRY AND CHARLOTTE KORTE REGARDING SURGICAL MESH MAY 2015 Introduction The Royal Australasian
Y O R K. Health Economics MEDICINES AND HEALTHCARE PRODUCTS REGULATORY AGENCY
 Y O R K Health Economics C O N S O R T I U M MEDICINES AND HEALTHCARE PRODUCTS REGULATORY AGENCY Summaries of the Safety/Adverse Effects of Vaginal Tapes/Slings/Meshes for Stress Urinary Incontinence and
Y O R K Health Economics C O N S O R T I U M MEDICINES AND HEALTHCARE PRODUCTS REGULATORY AGENCY Summaries of the Safety/Adverse Effects of Vaginal Tapes/Slings/Meshes for Stress Urinary Incontinence and
How do I know if I need to have surgery?
 How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
What you should know about Stress Urinary Incontinence
 Gynecare TVT Stop coping. Start living. What you should know about Stress Urinary Incontinence Have you ever leaked urine when you laughed, coughed or sneezed? You are not alone. Many women suffer from
Gynecare TVT Stop coping. Start living. What you should know about Stress Urinary Incontinence Have you ever leaked urine when you laughed, coughed or sneezed? You are not alone. Many women suffer from
Transobturator mid urethral sling surgery for stress urinary incontinence: our experience
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bettaiah R et al. Int J Reprod Contracept Obstet Gynecol. 2015 Dec;4(6):1831-1835 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Bettaiah R et al. Int J Reprod Contracept Obstet Gynecol. 2015 Dec;4(6):1831-1835 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
Laparoscopic Hernia Repair. Hernia Repair. Laparoscopic Ventral. Several Different Types of Hernia
 Laparoscopic Hernia Repair David B Renton, MD Assistant Professor Department of Surgery The Ohio State University Advantages of Laparoscopic Ventral vs. Open Hernia Repair Lower wound infection rate: 2.6%
Laparoscopic Hernia Repair David B Renton, MD Assistant Professor Department of Surgery The Ohio State University Advantages of Laparoscopic Ventral vs. Open Hernia Repair Lower wound infection rate: 2.6%
Surgical management of mesh-related complications after prior pelvic floor reconstructive surgery with mesh
 DOI 10.1007/s00192-011-1476-2 ORIGINAL ARTICLE Surgical management of mesh-related complications after prior pelvic floor reconstructive surgery with mesh Myrthe M. Tijdink & Mark E. Vierhout & John P.
DOI 10.1007/s00192-011-1476-2 ORIGINAL ARTICLE Surgical management of mesh-related complications after prior pelvic floor reconstructive surgery with mesh Myrthe M. Tijdink & Mark E. Vierhout & John P.
Facial Patch Surgical Technique in Treatment of Stress Urinary Incontinence in Women
 Iranian Red Crescent Medical Journal ORIGINAL ARTICLE Facial Patch Surgical Technique in Treatment of Stress Urinary Incontinence in Women F Khezri 1,2, A Samsami Dehaghani 3, M Ostovan 4, M Bahadorani
Iranian Red Crescent Medical Journal ORIGINAL ARTICLE Facial Patch Surgical Technique in Treatment of Stress Urinary Incontinence in Women F Khezri 1,2, A Samsami Dehaghani 3, M Ostovan 4, M Bahadorani
Surgery for Pelvic Organ Prolapse
 Committee 15 Surgery for Pelvic Organ Prolapse Chairman L. BRUBAKER (USA) Members C. GLAZENER (U.K), B. JACQUETIN (France), C. MAHER (Australia), A. MELGREM (USA), P. NORTON (USA), N. RAJAMAHESWARI (India),
Committee 15 Surgery for Pelvic Organ Prolapse Chairman L. BRUBAKER (USA) Members C. GLAZENER (U.K), B. JACQUETIN (France), C. MAHER (Australia), A. MELGREM (USA), P. NORTON (USA), N. RAJAMAHESWARI (India),
Pelvic Anatomy. Robert E. Gutman, MD
 Pelvic Anatomy Robert E. Gutman, MD Objectives Understand pelvic anatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony
Pelvic Anatomy Robert E. Gutman, MD Objectives Understand pelvic anatomy Organs and structures of the female pelvis Vascular Supply Neurologic supply Pelvic and retroperitoneal contents and spaces Bony
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Patient-Reported Outcomes of Retropubic versus Trans-Obturator Mid-Urethral Slings for Urinary Stress Incontinence: The Malaysian Experience
 Patient-Reported Outcomes of Retropubic versus Trans-Obturator Mid-Urethral Slings for Urinary Stress Incontinence: The Malaysian Experience Zalina N a, Kamal N b, Aruku N b, Jamaluddin AR c a Obstetrics
Patient-Reported Outcomes of Retropubic versus Trans-Obturator Mid-Urethral Slings for Urinary Stress Incontinence: The Malaysian Experience Zalina N a, Kamal N b, Aruku N b, Jamaluddin AR c a Obstetrics
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
PUBOVAGINAL FASCIAL SLING FOR ALL TYPES OF STRESS URINARY INCONTINENCE: LONG-TERM ANALYSIS
 22-5347/9~164-1312$3./ THE JOURNAL OF UROLOGY copyright 8 1998 by AMEmcm URO~ICAL ASS~CUTION, INC. Vol. 16, 1312-1316, October 1998 Printed in U.S.A. PUBOVAGINAL FASCIAL SLING FOR ALL TYPES OF STRESS URINARY
22-5347/9~164-1312$3./ THE JOURNAL OF UROLOGY copyright 8 1998 by AMEmcm URO~ICAL ASS~CUTION, INC. Vol. 16, 1312-1316, October 1998 Printed in U.S.A. PUBOVAGINAL FASCIAL SLING FOR ALL TYPES OF STRESS URINARY
Tissue Reinforcement Solutions
 Tissue Reinforcement Solutions Tissue Reinforcement Solutions Confidence in your hands One source for all your surgical mesh needs. One source for all your surgical mesh needs. Contact your local ETHICON
Tissue Reinforcement Solutions Tissue Reinforcement Solutions Confidence in your hands One source for all your surgical mesh needs. One source for all your surgical mesh needs. Contact your local ETHICON
FUNCTIONAL OUTCOME OF VAGINAL MESH FOR PELVIC ORGAN PROLAPSE IN GELRE HOSPITAL APELDOORN
 UNIVERSITY TWENTE AND GELRE HOSPITAL APELDOORN FUNCTIONAL OUTCOME OF VAGINAL MESH FOR PELVIC ORGAN PROLAPSE IN GELRE HOSPITAL APELDOORN Masterthesis Health Science Milou Scheltes (s0138657) 28-9-2012 UT:
UNIVERSITY TWENTE AND GELRE HOSPITAL APELDOORN FUNCTIONAL OUTCOME OF VAGINAL MESH FOR PELVIC ORGAN PROLAPSE IN GELRE HOSPITAL APELDOORN Masterthesis Health Science Milou Scheltes (s0138657) 28-9-2012 UT:
Apparently, providing an estimate of
 THE CUTTING EDGE Web-enhanced article! Go to www.femalepatient.com for additional Web-only content. The Rapid Evolution of Vaginal Mesh Delivery Systems for the Correction of Pelvic Organ Prolapse, Part
THE CUTTING EDGE Web-enhanced article! Go to www.femalepatient.com for additional Web-only content. The Rapid Evolution of Vaginal Mesh Delivery Systems for the Correction of Pelvic Organ Prolapse, Part
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Recurrence of Pelvicol and Its Effect ofPolystocele
 UNIVERSITÀ DEGLI STUDI DI ROMA "TOR VERGATA" FACOLTA' DI MEDICINA E CHIRUGIA DOTTORATO DI RICERCA IN "TERAPIE AVANZATE IN CHIRURGIA E RIABILITAZIONE DEL PAVIMENTO PELVICO FEMMINILE" XX CICLO DEL CORSO
UNIVERSITÀ DEGLI STUDI DI ROMA "TOR VERGATA" FACOLTA' DI MEDICINA E CHIRUGIA DOTTORATO DI RICERCA IN "TERAPIE AVANZATE IN CHIRURGIA E RIABILITAZIONE DEL PAVIMENTO PELVICO FEMMINILE" XX CICLO DEL CORSO
GIANT HERNIA REPAIR MY EXPERIENCE
 GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
Stress Urinary Incontinence & Sexual Function
 Stress Urinary Incontinence & Sexual Function Lior Lowenstein, MD, MS Associate Professor Deputy Chairman of Obstetrics and Gynecology Department Rambam Health Care Campus Haifa Israel No Disclosures Disclosures
Stress Urinary Incontinence & Sexual Function Lior Lowenstein, MD, MS Associate Professor Deputy Chairman of Obstetrics and Gynecology Department Rambam Health Care Campus Haifa Israel No Disclosures Disclosures
What do I need to know about Mesh Implants in Prolapse Surgery?
 Saint Mary s Hospital Gynaecology Service Warrell Unit What do I need to know about Mesh Implants in Prolapse Surgery? Information for Patients What is a mesh? A mesh is a material used in prolapse surgery.
Saint Mary s Hospital Gynaecology Service Warrell Unit What do I need to know about Mesh Implants in Prolapse Surgery? Information for Patients What is a mesh? A mesh is a material used in prolapse surgery.
Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom
 British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
British Journal of Obstetrics and Gynaecology April 1988, Vol. 95, pp. 77-81 Urinary incontinence during sexual intercourse: a common, but rarely volunteered, symptom PAUL HILTON Summary. A total of 4
In Situ Anterior Vaginal Wall Sling for Treatment of Stress Urinary Incontinence Extended Application and Further Experience
 Female Urology In Situ Anterior Vaginal Wall Sling for Treatment of Stress Urinary Incontinence Extended Application and Further Experience Mahmoud Mustafa, 1 Bassam S Wadie 2 Keywords: stress urinary
Female Urology In Situ Anterior Vaginal Wall Sling for Treatment of Stress Urinary Incontinence Extended Application and Further Experience Mahmoud Mustafa, 1 Bassam S Wadie 2 Keywords: stress urinary
Pelvic Symptoms in Women With Pelvic Organ Prolapse
 Pelvic Symptoms in Women With Pelvic Organ Prolapse Lara J. Burrows, MD, Leslie A. Meyn, MS, Mark D. Walters, MD, and Anne M. Weber, MD, MS From the Department of Obstetrics, Gynecology, and Reproductive
Pelvic Symptoms in Women With Pelvic Organ Prolapse Lara J. Burrows, MD, Leslie A. Meyn, MS, Mark D. Walters, MD, and Anne M. Weber, MD, MS From the Department of Obstetrics, Gynecology, and Reproductive
Review Article The Role of Vaginal Mesh Procedures in Pelvic Organ Prolapse Surgery in View of Complication Risk
 Obstetrics and Gynecology International, Article ID 356960, 7 pages http://dx.doi.org/10.1155/2013/356960 Review Article The Role of Vaginal Mesh Procedures in Pelvic Organ Prolapse Surgery in View of
Obstetrics and Gynecology International, Article ID 356960, 7 pages http://dx.doi.org/10.1155/2013/356960 Review Article The Role of Vaginal Mesh Procedures in Pelvic Organ Prolapse Surgery in View of
Mixed urinary incontinence - sling or not sling
 Mixed urinary incontinence - sling or not sling 吳 銘 斌 Ming-Ping Wu, M.D.,Ph.D. Director, Div. Urogynecology & Pelvic Floor Reconstruction, Chi Mei Foundation Hospital, Tainan, Taiwan Assistant Professor,
Mixed urinary incontinence - sling or not sling 吳 銘 斌 Ming-Ping Wu, M.D.,Ph.D. Director, Div. Urogynecology & Pelvic Floor Reconstruction, Chi Mei Foundation Hospital, Tainan, Taiwan Assistant Professor,
Laparoscopic Ventral Rectopexy
 Laparoscopic Ventral Rectopexy Patient information leaflet What is a laparoscopic ventral rectopexy? It is a keyhole operation, performed whilst you are asleep; the rectum is suspended back into its normal
Laparoscopic Ventral Rectopexy Patient information leaflet What is a laparoscopic ventral rectopexy? It is a keyhole operation, performed whilst you are asleep; the rectum is suspended back into its normal
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you Published February 2005 by the RCOG Contents Page number Key points 1 About this information 2 What is stress incontinence? 2 Do I need an operation?
Surgery for stress incontinence: information for you Published February 2005 by the RCOG Contents Page number Key points 1 About this information 2 What is stress incontinence? 2 Do I need an operation?
Stress incontinence. Supported by an unrestricted grant from
 Stress incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing conservative therapies
Stress incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing conservative therapies
Sacrohysteropexy for Uterine Prolapse
 Sacrohysteropexy for Uterine Prolapse Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG Governance Committee paying
Sacrohysteropexy for Uterine Prolapse Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG Governance Committee paying
Coding & Reimbursement
 2013 Coding & Reimbursement 2013 Coding and Reimbursement MatriStem is a unique extracellular matrix derived from a porcine urinary bladder. It has been shown to be effective in the treatment of acute
2013 Coding & Reimbursement 2013 Coding and Reimbursement MatriStem is a unique extracellular matrix derived from a porcine urinary bladder. It has been shown to be effective in the treatment of acute
PROLAPSE WHAT IS A VAGINAL (OR PELVIC ORGAN) PROLAPSE? WHAT ARE THE SIGNS OF PROLAPSE?
 WHAT IS A VAGINAL (OR PELVIC ORGAN)? Your pelvic organs include your bladder, uterus (womb) and rectum (back passage). These organs are held in place by tissues called fascia and ligaments. These tissues
WHAT IS A VAGINAL (OR PELVIC ORGAN)? Your pelvic organs include your bladder, uterus (womb) and rectum (back passage). These organs are held in place by tissues called fascia and ligaments. These tissues
Macroplastique injection for stress urinary incontinence
 Macroplastique injection for stress urinary incontinence Information for patients This information sheet answers some of the questions you may have about having a Macroplastique injection. It explains
Macroplastique injection for stress urinary incontinence Information for patients This information sheet answers some of the questions you may have about having a Macroplastique injection. It explains
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Complications of the tension-free vaginal tape procedure for stress urinary incontinence
 Int Urogynecol J (2010) 21:1353 1357 DOI 10.1007/s00192-010-1210-5 ORIGINAL ARTICLE Complications of the tension-free vaginal tape procedure for stress urinary incontinence Ingrid Kristensen & Maysoon
Int Urogynecol J (2010) 21:1353 1357 DOI 10.1007/s00192-010-1210-5 ORIGINAL ARTICLE Complications of the tension-free vaginal tape procedure for stress urinary incontinence Ingrid Kristensen & Maysoon
URINARY INCONTINENCE CASE PRESENTATION #1. Urinary Incontinence - History 2014/10/07. Structure of the Female Lower Urinary Tract
 Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Outcomes for Hong Kong Women Following Vaginal Mesh Repair Surgery for Pelvic Organ Prolapse
 Outcome of Vaginal Mesh Repair Outcomes for Hong Kong Women Following Vaginal Mesh Repair Surgery for Pelvic Organ Prolapse Chi-Wai TUNG MBChB, MRCOG, FHKCOG, FHKAM (O&G), DCH (Sydney) Urogynaecology Team,
Outcome of Vaginal Mesh Repair Outcomes for Hong Kong Women Following Vaginal Mesh Repair Surgery for Pelvic Organ Prolapse Chi-Wai TUNG MBChB, MRCOG, FHKCOG, FHKAM (O&G), DCH (Sydney) Urogynaecology Team,
Dr Eva Fong. Urologist Auckland
 Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Preservation of the uterus in vaginal prolapse surgery: the sacrospinous hysteropexy
 Preservation of the uterus in vaginal prolapse surgery: the sacrospinous hysteropexy Viviane Dietz Preservation of the uterus in vaginal prolapse surgery: the sacrospinous hysteropexy Vaginale prolapse
Preservation of the uterus in vaginal prolapse surgery: the sacrospinous hysteropexy Viviane Dietz Preservation of the uterus in vaginal prolapse surgery: the sacrospinous hysteropexy Vaginale prolapse
In the mid-1990s, Ulmsten and Petros 1 introduced the synthetic,
 Surgical Intervention for Stress Urinary Incontinence: Comparison of Midurethral Sling Procedures Joseph M. Novi, DO Beth H.K. Mulvihill, DO Context: The synthetic, tension-free midurethral sling was introduced
Surgical Intervention for Stress Urinary Incontinence: Comparison of Midurethral Sling Procedures Joseph M. Novi, DO Beth H.K. Mulvihill, DO Context: The synthetic, tension-free midurethral sling was introduced
Trocarless system for mesh attachment in pelvic organ prolapse repair 1-year evaluation
 DOI 10.1007/s00192-010-1349-0 ORIGINAL ARTICLE Trocarless system for mesh attachment in pelvic organ prolapse repair 1-year evaluation Menachem Alcalay & Michel Cosson & Miron Livneh & Jean-Philippe Lucot
DOI 10.1007/s00192-010-1349-0 ORIGINAL ARTICLE Trocarless system for mesh attachment in pelvic organ prolapse repair 1-year evaluation Menachem Alcalay & Michel Cosson & Miron Livneh & Jean-Philippe Lucot
previous surgery for incontinence.
 Predictive Title page Authors procedure value for of urinary urethra stress mobility incontinence before sub-urethra in women tape Xavier Khalid Alain Fabien Jean-Louis Pigné, Demaria, Zabak, Fritel, MD
Predictive Title page Authors procedure value for of urinary urethra stress mobility incontinence before sub-urethra in women tape Xavier Khalid Alain Fabien Jean-Louis Pigné, Demaria, Zabak, Fritel, MD
Do I Need to Have Surgery for Urinary Incontinence? What Kinds of Surgery Can Treat Stress Incontinence?
 Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Bard * PerFix * Plug. Technique Guide. A Modified Technique with the. Open Inguinal Hernia Repair
 A Modified Technique with the Bard * PerFix * Plug A quick and simple preperitoneal underlay Modified Technique for the repair of groin hernias Technique Guide Open Inguinal Hernia Repair This technique,
A Modified Technique with the Bard * PerFix * Plug A quick and simple preperitoneal underlay Modified Technique for the repair of groin hernias Technique Guide Open Inguinal Hernia Repair This technique,
AMS Sphincter 800 Urinary Prosthesis
 AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
Surgical Treatment for Female Stress Urinary. Continence. Consumer Education
 Surgical Treatment for Female Stress Urinary Incontinence By: Amy Rosenman, MD Geffen School of Medicine at UCLA Santa Monica, California Promoting Quality Continence Care through Consumer Education Always
Surgical Treatment for Female Stress Urinary Incontinence By: Amy Rosenman, MD Geffen School of Medicine at UCLA Santa Monica, California Promoting Quality Continence Care through Consumer Education Always
Analysis of retropubic colpourethrosuspension results by suburethral sling with REMEEX prosthesis
 European Journal of Obstetrics & Gynecology and Reproductive Biology 106 (2003) 179±183 Analysis of retropubic colpourethrosuspension results by suburethral sling with REMEEX prosthesis A. MartõÂn MartõÂnez
European Journal of Obstetrics & Gynecology and Reproductive Biology 106 (2003) 179±183 Analysis of retropubic colpourethrosuspension results by suburethral sling with REMEEX prosthesis A. MartõÂn MartõÂnez
Contents. 1. Milestones in Hernia Surgery 1. 2. Surgical Anatomy of Hernia Sites 5. 3. Incidence, Prevalence of Hernia 32
 1. Milestones in Hernia Surgery 1 History of the Procedure 3 2. Surgical Anatomy of Hernia Sites 5 Surgical Anatomy of Hernia Sites 5 External Anatomy of Abdominal Wall The Surface Markings 6 The Fascia
1. Milestones in Hernia Surgery 1 History of the Procedure 3 2. Surgical Anatomy of Hernia Sites 5 Surgical Anatomy of Hernia Sites 5 External Anatomy of Abdominal Wall The Surface Markings 6 The Fascia
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Effects of Pregnancy & Delivery on Pelvic Floor
 Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Stress incontinence in Women
 Stress incontinence in Women Exceptional healthcare, personally delivered Operations for Stress Incontinence Introduction Stress incontinence is a medical word used to describe the type of leakage that
Stress incontinence in Women Exceptional healthcare, personally delivered Operations for Stress Incontinence Introduction Stress incontinence is a medical word used to describe the type of leakage that
