Computer-Aided Diagnosis of Lumbar Stenosis Conditions
|
|
|
- Jessica Bates
- 8 years ago
- Views:
Transcription
1 Computer-Aided Diagnosis of Lumbar Stenosis Conditions Soontharee Koompairojn 1 Kathleen Hua 2 Kien A. Hua 1 Jintavaree Srisomboon 3 1 University of Central Florida, Orlando FL 32816, U.S.A. [soonthar, kienhua]@eecs.ucf.edu 2 Emory University, Atlanta, GA 30332, U.S.A., khua@learnlink.emory.edu 3 BMA General Hospital, Pomprab, Bangkok 10110, Thailand, J_tavare@bma.go.th ABSTRACT Computer-aided diagnosis (CAD) systems are indispensable tools for patients healthcare in modern medicine. Nevertheless, the only fully automatic CAD system available for lumbar stenosis today is for X-ray images. Its performance is limited due to the limitations intrinsic to X-ray images. In this paper, we present a system for magnetic resonance images. It employs a machine learning classification technique to automatically recognize lumbar spine components. Features can then be extracted from these spinal components. Finally, diagnosis is done by applying a Multilayer Perceptron. This classification framework can learn the features of different spinal conditions from the training images. The trained Perceptron can then be applied to diagnose new cases for various spinal conditions. Our experimental studies based on 62 subjects indicate that the proposed system is reliable and significantly better than our older system for X-ray images. Keywords: Feature extraction, Machine Learning, Computer-aided diagnosis, Lumbar spine, Spinal stenosis, MR images, Multilayer perceptron 1. INTRODUCTION Global prevalence of lower back pain could be as high as 42% according to the World Health Organization. It is the second most common neurological ailment in the United States, only headache is more common. Such pain, interfering with work and routine daily activities, is the most common cause of job-related disability and a leading contributor to missed work. Approximately 2% of workers injure their back each year; and this is considered the most expensive ailments inflicted on industrial societies [2][4]. The National Institute of Neurological Disorders and Stroke estimates Americans spend at least $50 billion each year due to low back pain [11]. It is a chief cause of visits to primary care physicians. A common cause of low back pain is lumbar spinal stenosis. The spinal cord and the spinal nerve roots are surrounded by bone structures. Wear-and-tear effects of aging can lead to narrowing of the space around the spinal cord or the nerve roots. This condition is called spinal stenosis. When this condition occurs in the lower back, it is called lumbar spinal stenosis. Lumbar spinal stenosis which compresses on the nerves may cause pain, numbness, or weakness in the legs. Currently, the prevalent systems for lumbar spinal stenosis diagnosis are PACS (Picture Archiving and communication system) and other viewing tools such as Syngo fastview [13]. Radiologists use them to manually draw lines to measure various canal distances. The effectiveness of these tools depends on the knowledge and experience of the user. A system capable of suggesting a diagnosis plan based on data obtained from the history, physical examination, and diagnostic studies in the patient suspected of having a herniated lumbar disc is presented in [7]. To the best of our knowledge, we introduced the only image-based CAD system for LSS in [10]. This system can detect various spinal conditions from X-ray images. First we applied the Active Appearance Modeling [15] technique to automatically label the boundary points of the vertebrae. Then, we adapted the vertebral morphology technique [8] to extract features from the labeling points. With this framework, we built a CAD system with two environments one for managing training images and building the classifiers, and the other environment for diagnosis use in practice. The experiment studies for this system, based on the X-ray image database NHANES II available from the National Library of Medicine, indicate that the system is effective for screening purposes. However, its performance is constrained to the lateral view of lumbar spine X-ray images. In this paper, we introduce a new CAD system that leverages magnetic resonance (MR) images to achieve substantially better
2 diagnosis quality. In recent years, magnetic resonance imaging (MRI) has become the preferred modality since it scans large areas of the spine without ionizing radiation. Moreover, MRI provides exquisite soft tissue details, is multiplanar and reveals more details of lumbar spine stenosis. The remainder of this paper is organized as follows. In Section 2, we provide background information on the anatomy of the lumbar spine and lumbar spine stenosis. We present our visual features for the characterization of various lumbar spinal conditions, and discuss the proposed automatic feature extraction technique in Section 3. Our method for building the classifier for stenosis diagnosis is introduced in Section 4. The experimental results of the system are given in Section 5. Finally, we give our concluding remarks and discuss our future work in Section BACKGROUND - LUMBAR SPINAL STENOSIS To make the paper self-contained, we give a brief introduction to the anatomy of the lumbar spine and discuss the two types of lumbar spinal stenosis in this section. The normal spine is composed of 24 bony structures called vertebrae. The lumbar spine is the lower portion of the spine structure. It normally consists of five vertebrae; designated L1 through L5, starting at the top. Each vertebra (Figure 1) comprises a vertebral body, lamina, and pedicles, which surround a ring-like space, the spinal canal. Each vertebra has two sets of facet joints - one pair faces upward and one downward. They are hinge-like and connect the adjacent vertebrae together (Figure 2). Between two vertebrae is a gel-like cushion called an intervertebral disc [1][3]. These discs help to absorb pressure and keep the vertebrae from grinding against each other. Facet joints and discs allow the spine to bend and twist. The vertebrae and discs are held together by groups of ligaments (Figure 2). Also illustrated in Figure 2 is the spinal canal. It is the vertical space within the spinal column which contains the spinal cord. Nerves branching from the spinal cord travel to different parts of the body through small openings on the sides of the canal, called intervertebral foramina (lateral canals). Each foramen is formed by the pedicles of adjacent vertebrae above, the vertebral bodies in front, and the articular processes behind (Figure 2). This foramen allows for the passage of the spinal nerve root. Figure 1. Anatomy of a spinal vertebrae Figure 2. Spinal canal and an intervertebral disc between two adjacent vertebrae (image courtesy of St. Joseph s Hospital Health Center).
3 Lumbar spinal stenosis (LSS) is defined as a focal narrowing of the spinal canal. The symptoms are nerve root pain and/or back pain due to compression of the nerves. As an example, one scenario is as follows. Degenerative disc due to tears can weaken the disc wall. Disc center becomes damaged and loses part of its water content. Unable to act as a cushion, the disc flattens causing facet joints to misalign. This condition may encourage bone spurs. If the spurs grow into the spinal canal, they cause spinal stenosis, and may compress the spinal cord and nerves. In general, spinal stenosis can be applied to any combination of the following root compression mechanisms: Posterior osteophytes - Abnormal bony outgrowth protrude toward the front of the spinal canal. Hypertrophy of ligament and facet - Ligaments and facet joint grow abnormally large and reduce the diameter of the foramen. Disc space narrowing - A damaged disc may lose some of its water content and become thinner. Disc herniation/bulging - Tear in the disc wall may allow the soft central portion of the disc to bulge out. Spondylolisthesis - A forward dislocation of one vertebra over the one beneath can produce pressure on spinal nerves Lumbar spinal stenosis conditions can be grouped into two categories. Stenosis occurring in the central spinal canal where the spinal cord is located (Figure 3) is referred to as central stenosis. More often, stenosis may also occur due to the entrapment and compression of the nerve root in its pathway through the foramen (Figure 3). This is called lateral stenosis [5]. The challenging problem for LSS is that there is little or no evidence to investigate the nerve root compression that occurs. Figure 3. Types of lumbar spinal stenosis (left - image courtesy of Lordex Spine Institute at Lincoln Health Center.) and vertical view of nerve root canal (right) 3. AUTOMATIC FEATURE EXTRACTION The input to our CAD system is a series of T2-weighted MR images of lumbar spine in transverse (axial) views as shown in Figures 4(A). We leave the investigation of the sagittal (side) view (Figure 4(B)) to a future study. Our technique has three major steps: (1) Spinal components segmentation: This task performs image segmentation to recognize the components of spine. (2) Spinal features extraction: This task measures and calculates to extract spinal characteristics such as the diameters and length of the spinal components. (3) Spinal stenosis classification: This task applies a multilayer Perceptron framework to classify new cases according to the spinal features. We discuss the details of the first two steps and a briefly introduce the third step in this section. The details of the third step are given in Section 3.
4 (A) Transverse view Figure 4. Sagittal view and transverse view of lumbar spine (B) Sagittal view 2.1 Spinal components recognition We applied the Multilayer Perceptron (MLP) framework to develop a fully automatic segmentation technique for the transverse views of lumbar spine. The objective is to segment the image (at its reduced pixel resolution) into spinal components, each can be examined later to detect a certain spinal condition. First, the system searches around the center of the image for the area of the spinal canal, which is the brightest region of the image. As an example, the intensity histograms of the spinal canal area and the right superior articular facet area are shown in the right and left of Figure 5, respectively. The two histograms look very different. They show that most pixels in the right superior articular facet are dark (i.e., data skew to the left), whereas the spinal canal consists of mostly very bright pixels (i.e., data skew to the right). By exploiting this property, the area of the spinal canal can be recognized by first finding a very bright pixel and then performing image segmentation using region growing. This bright canal area is represented by its minimum bounding rectangle, our first region of interest (ROI) as shown in Figure 6. Based on this ROI, the system derives two additional rectangular regions of interest, the right hand side of the spinal canal (labeled 3) and the left hand side of the spinal canal (labeled 4), as illustrated in Figure 6. Similarly, the ROI corresponding to the bottom of the intervertebral disc (labeled 2) is obtained based on the 3 rd and 4 th ROI s as depicted in Figure 6. These four ROI s are also shown in Figure 7 for a real image. Figure 5. Grayscale histogram show spinal canal (right histogram) has mostly bright pixels and the right superior articular facet (left histogram) has mostly dark pixels.
5 Figure 6. Four regions of interest Figure 7. Four regions of interest of a real image. Next, the system performs segmentation by examining each pixel of the four regions of interest and assign it to one of the six segmented areas, each corresponds to one of the six spinal components as shown in Figure 8, namely (1) spinal canal, (2.1) bottom of intervertebral disc, (2.2) right superior articular facet (including both the superior articular process and the facet joint), (2.3) left superior articular facet, (3) right ligamentum flavum, and (4) left ligamentum flavum. This is achieved by using three MLP s (Figure 9), one for each of the ROI s 2, 3, and 4. The input to each MLP is the feature vector of the pixel being labeled. This feature vector consists of the following values: the x-coordinate and y-coordinate of the pixel being labeled; 13 intensity values, one for the pixel being labeled and one for each of its 12 neighboring pixels as illustrated in Figure 9; and the intervertebral disc level. Figure 8. Boundaries of spinal components
6 The intervertebral disc level is included in the feature vector because we use a single MLP for all intervertebral disc levels. Given a larger training set, one can consider training an MLP for each disc level to achieve better performance. Figure 9. Spinal component segmentation using multilayer perceptron The output of the MLP indicates the type of the pixel. The MLP for ROI 2 recognizes pixels of the intervertebral disc, vertebral body, and superior articular facet; the MLP for ROI 3 recognizes pixels of the right ligamentum flavum; and the MLP for ROI 4 recognizes pixels of the left ligamentum flavum. We note that the segmentation of the spinal canal has already been done by region growing as described in Section 2.1. An example of the segmentation result is given in Figure 8. It shows the boundaries of the six spinal components. 2.2 Spinal Feature Extraction After spinal components have been identified, we can measure the spinal features to facilitate spinal stenosis diagnosis. We first determine the five boundary points that outline the posterior border of the vertebra (vertebral body or intervertebrtal disc) as shown in Figures 10 and 11. To facilitate our discussion, we refer to these boundary points from right to left as BP 1 to BP 5, respectively. The 1 st ROI is equally divided into equal partitions by five vertical lines (V 1, V 2, V 3, V 4, and V 5 ), and three horizontal lines H 1, H 2, and H 3, as depicted in Figure 10. BP 2, BP 3, and BP 4, are the intersections between the posterior border of the vertebra and the vertical lines V 1, V 3, and V 5, respectively. The boundary point BP 1 is 14 pixels away from BP 2 along the posterior border. Similarly, the boundary point BP 5 is 14 pixels away from BP 4 along the posterior border. Figure 10. The five boundary points and six spinal canal features The spinal features are measured from the six spinal components as follows: Anteroposterior diameter: This is the distance between BP 3 (i.e., the middle boundary point) and the bottom of the spinal canal along the vertical line V 3 (Figure 10).
7 Right (Left) canal height: This is the distance between BP 2 (BP 4 ) and the bottom of the spinal canal along the vertical line V 1 (V 2 ) (Figure 10). Transverse diameter: This is the width of the spinal canal along the horizontal line H 2 (Figure 10). Upper (Lower) canal widths: This is the width of the spinal canal along the horizontal line H 1 (H 3 ) (Figure 10) Right (Left) lateral canal diameter: This is the vertical distance between the boundary point BP1 (BP5) at the posterior border of the vertebra and the superior articular facet (Figure 11). This feature measures the diameter of the lateral recess, a region located between the central canal and the intervertebral foramen (Figure 3). Ligamentum flavum thickness: The thickness of this soft tissue can be measured at the facet joint level. There are left and right ligamentum flavum thickness measurements(figure 11). They are the thickest area of the corresponding ligamentum flavum measured along a 40 angel with the anteroposterior diameter. Figure 11. Spinal features used in stenosis diagnosis The aforementioned features are designed to measure the various conditions of both central stenosis and lateral stenosis. The relationship between our spinal features, the types of compression mechanism, and the stenosis categories these features are designed to detect is summarized in Table 1. As an example, the second row of the table indicates that a herniated disc can affect the height of the anteroposterior diameter; and as a consequence, central stenosis can be detected using this feature. Table 1. Spinal features related to Spinal conditions Compression Mechanisms Stenosis Categories Spinal Features Disc Herniation Hypertrophy of Ligaments or Facet Central Lateral Left & Right Canal Heights Anteroposterior Diameter Transverse Diameter Upper Canal Width Lower Canal Width Lateral Canal Diameter Ligamentum Flavum Thickness
8 2.3 Spinal Stenosis Classification After extracting spinal features from the training MR images, this information is verified by the radiologists and used to train one Multilayer Perceptron (MLP) classifier, as shown in Figure 12, for each of the four stenosis conditions (Table 1). The input to this MLP is the set of spinal features, and its output indicates the positive or negative result of the diagnosis. We shall discuss this MLP in greater detail in the next section. 4. BUILDING THE CLASSIFIER MLP is a feedforward network of artificial neurons, which maps the input data onto a set of desired output [6][14[16]. Our MLP consists of a layer of input neurons, a layer of output neurons, and a hidden layer. The neurons of any two consecutive layers are connected together as a bipartite graph as illustrated in Figure 12. Similar to many other supervised learning techniques, an MLP can deduct a function from training data. The goal of the learning process is to predict the value of the function for any valid input object (i.e., a feature vector in our context) after having seen a number of training examples. This is achieved by finding the set of weight values for the links that will cause the output from the neural network to match the desired target values as closely as possible. This process is based on a gradient descent (an error minimization) technique we shall describe shortly. Figure 12. A Multilayer Perceptron for spinal stenosis classification. 3.1 MLP learning process The basic MLP learning procedure is as follows. 1. All weights of the links between nodes are set to random numbers. 2. The network learns from the training data instance to calculate the output values. 3. These output values are compared to the target values (from the training set). 4. The difference between the output values and the target values are propagated backwards, and all the weights are adjusted accordingly. 5. Repeat Steps 2-4 for each data instance in the training set to complete the training. The adjustment performed in Step 4 is based on a gradient descent technique. Consider an error surface with respect to all the weights. This surface shows the amount of error that would result for each combination of weights. The bottom of this error surface gives the optimal set of weights. The learning challenge is to find the set of weights that produce the minimum error for the whole training set. The gradient descent technique uses the error gradient to descend this error surface. This gradient is the slope of the error surface which indicates the sensitivity of the error to changes in the weights. This sensitivity can be exploited to incrementally guide the changes in the weights towards the optimum.
9 3.2 MLP parameters In our performance evaluation, we used the MLP in WEKA data mining software [12]. There are several parameters that we needed to set up. We discuss these parameters below; and their values used in our experiments will be given in Section Learning rate: This is the amount the weights are updated. The weight is updated as follows: W mk t + 1 = W mk t + αe k where W mk is the weight of the link from node m to node k of two consecutive layers, t is the time at that moment, α is the learning rate, and E k is the error function of node k. 2. Momentum: This factor is applied to the weights during updating. It is used to avoid oscillating weight changes. Therefore, the weight would not stay the same. 3. Training time: This is the number of iterations of the training session. 4. The validation threshold: This threshold is used to terminate validation testing for over fitting. It dictates how many times in the row the validation set error can get worse before training is terminated. 5. The number of nodes in the hidden layer (N H ): For our experiment, Where N H is the number of hidden nodes, N I is the number of input nodes, and N o is the number of the output nodes. N H = N I + N o 2 5. EXPERIMENTAL RESULTS We evaluated our system on the lumbar spine MR images in transverse view of 50 subjects. The contrast of the MR image can be controlled through the pulse sequence parameters. There are two common pulse sequences, T1- weighted sequence and T2-weighted spin-echo sequences. Our MR images were generated using T2-weighted sequence with a long TR (1000ms TR 2500ms, mostly 1290) and a short TE (25ms TE 30ms, mostly 26). The 50 clinical MRI volumes include both normal and abnormal vertebrae. The clinical diagnosis reports are obtained from Bangkok Metropolitan Medical Center, Prasat Neurological Institute, Rajavithi Hospital, all in Bangkok, Thailand. These reports were generated by agreement between at least one radiologist and one orthopedist. Without loss of generality, we consider only female patients in this study. Male patients typically have larger spinal structures and the same technique can be applied to them separately. The ages of our patients range between 18 and 74, with a mean of 48. In our experiments, we focused on the four conditions that could be examined in the transverse view of the spine, namely (1) hypertrophy of ligamentum flavum and facet, (2) disc herniation, (3) central spinal stenosis, and (4) lateral spinal stenosis. We investigated the four intervertebral discs between vertebra L2 and the first sacral vertebra S1 (Figure 13). These intervertebral discs are called L2-L3, L3-L4, L4-5, and L5-S1, respectively. The number of verified positive cases for each spinal condition in the experimental data set is given in Table 2. These clinical diagnosis data are generated under the collaboration between radiologists and orthopedists. We present the performance of the segmentation technique and the quality of the diagnosis in the following two subsections.
10 Figure 13. The four intervertebral discs considered in the experiments (image courtesy of Taiwan Spine Center). Table 2. Number of positive cases for each spinal condition at differenct disc levels in the data set Intervertebral disc level Spinal conditions L2-L3 L3-L4 L4-L5 L5-S1 Hypertrophy of ligamentum flavum & facet Disc space narrowing Disc Herniation Central spinal stenosis Lateral spinal stenosis Performance Metrics We evaluate the correctness of the segmentation results (extract the spinal components) in order to gain insight into the overall performance of the proposed CAD system. We consider the following three parameters: (1) TP (true positive) is the overlap between the region segmented by the algorithm and the ground truth; (2) FN (false negative) is the ground truth region which is not included by the region segmented by the algorithm.; and (3) FP (false positive) is the region segmented by the algorithm but is not found in the ground truth. The correlation between the three regions is illustrated in Figure 14. Based on these parameters, we can define the performance metric, Quality of the segmentation result, as: (1) Similarly, Diagnosis Correctness is computed as the percentage of correct diagnosis. In our experiments, we performed a ten-fold cross validation [9] for each performance metric as follows. The data set of 50 subjects is randomly split into ten approximately equal partitions. Each partition is used in turn for testing while the remaining partitions are used for training. This process is repeated ten times; and the overall performance is the average over the ten rounds. This assessment strategy reduces the variability and gives more accurate performance results.
11 Figure 14. Performance parameters. 4.2 Correctness of the Segmentation In our experiment, the MLP for image segmentation, as illustrated in Figure 9, was implemented with a learning rate of 0.3, momentum of 0.2, training time of 500, validation threshold of 20, and 16 nodes in the hidden layer. The performance results of the spinal component segmentation as described in Section 2.1 are given in Table 3. Overall, the accuracy consistently ranges above 91%, which is adequate for our diagnosis purposes. Table 3. The average percentage of correct segmentation of spinal components Spinal Components Segmentation Quality (1) Spinal canal (2.1) Intervertebral disc (2.2) Right superior articular facet (2.3) Left superior articular facet (3) Right ligamentum flavum & facet (4) Left ligamentum flavum & facet Quality of the Spinal stenosis classification After the spinal components are segmented, spinal features such as the anteroposterior diameter, lateral canal distance, and ligamentum flavum thickness in each image are calculated and extracted. These features are input into the Multilayer Perceptrons, as illustrated in Figure 12, to predict the stenosis conditions. The MLP s for diagnosis was implemented with a learning rate of 0.3, momentum of 0.2, training time of 500, validation threshold of 20, and 10 nodes in the hidden layer. Again, the ten-fold cross validation is applied in this study. The results are shown in Table 4. Table 4. The average percentage of correct diagnosis Spinal conditions Diagnosis Correctness Hypertrophy of ligament flavum & facet Disc Herniation Central Spinal stenosis Lateral Spinal stenosis 96.29
12 In this study, we do not include intervertebral disc level L5-S1 in computing the correctness of disc herniation diagnosis since L5-S1 looks quite different from the other disc levels. The results in Table 4 indicate that MRI is significantly more effective in facilitating spinal stenosis diagnosis, compared to our own older X-ray CAD system whose correctness averages 74.5%. This can be attributed to the fact that MR images can reveal more important spinal features and enhance boundaries of spinal components allowing the segmentation and diagnosis classification to be more accurate. 6. CONCLUSIONS AND FUTURE RESEARCH We have developed a fully automatic computer-aided diagnosis system for lumbar spine stenosis. The system accepts a series of T2-weighted axial views as input, and detects the following stenosis conditions: hypertrophy of ligament flavum and facet, disc herniation, central spinal stenosis, and lateral spinal stenosis. The average accuracy ranges from about 92% to 97%. The performance can be further improved by considering also the sagittal views (Figure 3(B)) of lumbar spine. There are several spinal conditions, related to spinal stenosis, such as posterior osteophyte, disc space narrowing, and spondylolisthesis that were not considered directly in this study. These spinal conditions could be recognized from the sagittal views. We will extend our CAD system with these new capabilities in our future research. REFERENCES [1] Abrahams, P., [The atlas of the human body], Bright Star Publishing plc.,london, (2008). [2] Agency of Healthcare Research and Quality, Treatment of Degenerative Lumbar Spinal Stenosis, AHRQ Publication, (2001). [3] Bogduk, N., [Clinical anatomy of the lumbar spine and sacrum], Churchill Livingstone Publishers, London, Third edition, (2005). [4] Furman, M. B. and Puttlitz, K. M., Spinal Stenosis and Neurogenic Claudication, EMedicine (2009). ( [5] Gunzburg, S.M. and Hagerstown, R., Lumbar spinal stenosis. Lippincott Williams & Wilkins [6] Haykin, S. Neural Networks: A Comprehensive Foundation (2 ed.). Prentice Hall, (1998). [7] Hudgins, W.R., Computer-aided diagnosis of lumbar disk herniation, Spine 8, (1983). [8] Hedlund, L. R. and Gallagher, J. C., Vetebral morphometry in diagnosis of spinal fractures, Bone Miner, (1988). [9] Kohavi, R., A study of cross validation and bootstrap for accuracy and model selection, Proc. AI 2(12), (1995). [10] Koompairojn, S., Hua, K. A. and Bhadrakom, C., Automatic classification system for lumbar spine X-ray images, Proc. CBMS 1(1), (2006). [11] National Institute of Neurological Disorders and Stroke (NINDS), Low back pain fact,, NINDS Publication, (2008).( [12] Seewald, A., Introduction to Weka, (2009). ( [13] Sennst, D.A., Kachelriess, M., Leidecker, C., Schmidt, B., Watzke, O. and Kalender,W.A., An extensible software-based platform for reconstruction and evaluation of CT images, RadioGraphics 24, (2004). [14] Seung, S., Multilayer perceptrons and backpropagation learning, Lecture Notes (2002). [15] Stegmann, M. B., Active Appearance Model, theory extensions and cases, Master Thesis,Technical University of Denmark (2000). [16] Wasserman, P.D.; Schwartz, T., Neural networks. II. What are they and why is everybody so interested in them now?, IEEE Expert 3(1),10-15; (1988).
Thoracic Spine Anatomy
 A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Spine University s Guide to Kinetic MRIs Detect Disc Herniations
 Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Lumbar Spine Anatomy. eorthopod.com 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.
 A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Anatomy and Terminology of the Spine. Bones of the Spine (Vertebrae)
 Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Compression Fractures
 September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
BODY BODY PEDICLE PEDICLE TRANSVERSE TRANSVERSE PROCESS PROCESS
 Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Vertebral anatomy study guide. Human Structure Summer 2015. Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey.
 Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Spinal Anatomy. * MedX research contends that the lumbar region really starts at T-11, based upon the attributes of the vertebra.
 Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Lower Back Pain. Introduction. Anatomy
 Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
SPINE SURGERY - LUMBAR DECOMPRESSION
 SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Vivian Gonzalez Gillian Lieberman, MD. January 2002. Lumbar Spine Trauma. Vivian Gonzalez, Harvard Medical School Year III Gillian Lieberman, MD
 January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
There are four main regions of the back; the cervical (C), thoracic (T), lumbar (L), and sacral (S) regions
 Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Options for Cervical Disc Degeneration A Guide to the M6-C. clinical study
 Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Magnetic Resonance Imaging
 Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, The Cervical Spine. What is the Cervical Spine?
 Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Problems. Knowing. back of the
 Introduction Welcome to BodyZone Physiotherapy patient resource about Cervical Spine Problems. Knowing the main parts of your neck and how these parts work is important as you learn to care for your neck
Introduction Welcome to BodyZone Physiotherapy patient resource about Cervical Spine Problems. Knowing the main parts of your neck and how these parts work is important as you learn to care for your neck
Lectures of Human Anatomy
 Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Imaging degenerative disk disease in the lumbar spine. Elaine Besancon MS III Dr. Gillian Lieberman
 Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
Lumbar Spinal Stenosis CAD from Clinical MRM and MRI Based on Inter- and Intra-Context Features with a Two-Level Classifier
 Lumbar Spinal Stenosis CAD from Clinical MRM and MRI Based on Inter- and Intra-Context Features with a Two-Level Classifier Jaehan Koh, Raja S Alomari, Vipin Chaudhary a and Gurmeet Dhillon, MD b a Department
Lumbar Spinal Stenosis CAD from Clinical MRM and MRI Based on Inter- and Intra-Context Features with a Two-Level Classifier Jaehan Koh, Raja S Alomari, Vipin Chaudhary a and Gurmeet Dhillon, MD b a Department
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
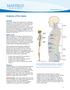 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
Lumbar Nerve Root Block
 Lumbar Nerve Root Block Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Imaging techniques, such as an MRI scan, can reveal small disc bulges and / or wear and tear in the spine with possible
Lumbar Nerve Root Block Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Imaging techniques, such as an MRI scan, can reveal small disc bulges and / or wear and tear in the spine with possible
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs
 Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs Doug Dean ENGN 2500: Medical Image Analysis Final Project Outline Introduction to the problem Based on paper:
Quantitative Comparison of Conventional and Oblique MRI for Detection of Herniated Spinal Discs Doug Dean ENGN 2500: Medical Image Analysis Final Project Outline Introduction to the problem Based on paper:
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Biomechanical Basis of Lumbar Pain. Prepared by S. Pollak. Introduction:
 Biomechanical Basis of Lumbar Pain Prepared by S. Pollak Introduction: The lumbar area of the back is made up of five movable L1-L5 vertebrae which have intervertebral discs in between them 1. The intervertebral
Biomechanical Basis of Lumbar Pain Prepared by S. Pollak Introduction: The lumbar area of the back is made up of five movable L1-L5 vertebrae which have intervertebral discs in between them 1. The intervertebral
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
What are Core Muscles?... 2. A Healthy Lumbar Spine...3. What is Low Back Pain?...4. Rehabilitation...6. Stages of Rehabilitation...
 Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
IP'Lumbar Spinal Stenosis
 A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
Skeletal System. Axial Skeleton: Vertebral Column and Ribs
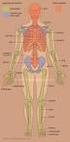 Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
Degenerative Changes of the Cervical Spine
 Anatomical Demonstration of Cervical Degeneration 1 Anatomical Demonstration: Degenerative Changes of the Cervical Spine 20 Slides of anatomical specimens, Xrays and MRIs By: William J. Ruch, D.C. Copyright
Anatomical Demonstration of Cervical Degeneration 1 Anatomical Demonstration: Degenerative Changes of the Cervical Spine 20 Slides of anatomical specimens, Xrays and MRIs By: William J. Ruch, D.C. Copyright
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
But My Back Hurts Only When I m Standing!
 But My Back Hurts Only When I m Standing! Axial Loading for Spinal Canal Stenosis Matthew Cham, MD; Akio Hiwatashi, MD; Per-Lennart Westesson, MD, PhD, DDS Division of Diagnostic and Interventional Neuroradiology,
But My Back Hurts Only When I m Standing! Axial Loading for Spinal Canal Stenosis Matthew Cham, MD; Akio Hiwatashi, MD; Per-Lennart Westesson, MD, PhD, DDS Division of Diagnostic and Interventional Neuroradiology,
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
The Anatomy of Spinal Cord Injury (SCI)
 The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
CERVICAL SPONDYLOSIS
 CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
Spine DJD Nomenclature. Sonia K Ghei, MD
 Spine DJD Nomenclature Sonia K Ghei, MD Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology http://www.asnr.org/spine_nomenclature/
Spine DJD Nomenclature Sonia K Ghei, MD Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology http://www.asnr.org/spine_nomenclature/
Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE
 Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE IN PARTIAL FULFILLMENT OF THE REGULATIONS FOR THE AWARD
Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE IN PARTIAL FULFILLMENT OF THE REGULATIONS FOR THE AWARD
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN
 Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
FRAUD DETECTION IN ELECTRIC POWER DISTRIBUTION NETWORKS USING AN ANN-BASED KNOWLEDGE-DISCOVERY PROCESS
 FRAUD DETECTION IN ELECTRIC POWER DISTRIBUTION NETWORKS USING AN ANN-BASED KNOWLEDGE-DISCOVERY PROCESS Breno C. Costa, Bruno. L. A. Alberto, André M. Portela, W. Maduro, Esdras O. Eler PDITec, Belo Horizonte,
FRAUD DETECTION IN ELECTRIC POWER DISTRIBUTION NETWORKS USING AN ANN-BASED KNOWLEDGE-DISCOVERY PROCESS Breno C. Costa, Bruno. L. A. Alberto, André M. Portela, W. Maduro, Esdras O. Eler PDITec, Belo Horizonte,
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Introduction: Anatomy of the spine and lower back:
 Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Do you have Back Pain? Associated with:
 Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Cervical Spondylosis. Understanding the neck
 Page 1 of 5 Cervical Spondylosis This leaflet is aimed at people who have been told they have cervical spondylosis as a cause of their neck symptoms. Cervical spondylosis is a 'wear and tear' of the vertebrae
Page 1 of 5 Cervical Spondylosis This leaflet is aimed at people who have been told they have cervical spondylosis as a cause of their neck symptoms. Cervical spondylosis is a 'wear and tear' of the vertebrae
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
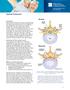 Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Cervical Spine Imaging
 March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
ARTICLES. Prevalence of Herniated Intervertebral Discs of the Cervical Spine in Asymptomatic Subjects Using MRI Scans: A Qualitative Systematic Review
 Please note that this electronic prepublication galley may contain typographical errors and may be missing artwork, such as charts, photographs, etc. Pagination in this version will differ from the published
Please note that this electronic prepublication galley may contain typographical errors and may be missing artwork, such as charts, photographs, etc. Pagination in this version will differ from the published
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Herniated Disk in the Lower Back
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Degenerative Lumbar Spine Disease
 Beth Israel Deaconess Medical Center A Member of Caregroup Harvard Medical School Degenerative Lumbar Spine Disease Michael Barnett, HMS III Core Radiology Clerkship BIDMC PCE Overview Patient Presentation:
Beth Israel Deaconess Medical Center A Member of Caregroup Harvard Medical School Degenerative Lumbar Spine Disease Michael Barnett, HMS III Core Radiology Clerkship BIDMC PCE Overview Patient Presentation:
Report #9. Human Anatomy and Soft Tissue Injuries:
 Report #9 Human Anatomy and Soft Tissue Injuries: The most common injury occurs from the bouncing around of a body in a vehicle. Often, a car occupant s neck whips back and forth, giving rise to what is
Report #9 Human Anatomy and Soft Tissue Injuries: The most common injury occurs from the bouncing around of a body in a vehicle. Often, a car occupant s neck whips back and forth, giving rise to what is
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro
 Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 healtheephan@yahoo.com ABSTRACT
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 healtheephan@yahoo.com ABSTRACT
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
MD 2016. Back Muscles & Movements Applied Anatomy. A/Prof Chris Briggs Anatomy & Neuroscience
 MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
