Bariatric Surgery. Overview of Procedural Options
|
|
|
- Kristian Henry
- 8 years ago
- Views:
Transcription
1 Bariatric Surgery Overview of Procedural Options
2 The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above 25% 1 Eight states have obesity rates above 30%: Alabama, Arkansas, Kentucky, Louisiana, Mississippi, Oklahoma, Tennessee and West Virginia 1 1 Source: F as in Fat: How Obesity Threatens America s Future
3 How is Obesity Calculated? The standard indicator of level of overweight is the Body Mass Index (BMI), a number calculated from a person s weight and height. BMI is expressed metrically as kg/m 2 and is calculated by: ( ) Weight in Pounds BMI = x 703 (Height in Inches) 2 A BMI of 30 or more is considered to represent obesity. A BMI of 40 or more, or a BMI of 35 or more in the presence of significant obesity related comorbidities is considered to represent morbid obesity. 1 An automatic BMI calculator is also available online at: 1 Source: Abu-Jaish and Rosenthal, Sleeve Gastrectomy: a New Surgical Approach for Morbid Obesity, Expert Rev. Gastroenterol. Hepatol. 4(1), (2010)
4 Prevalence of Obesity for Adults BMI Among Adults Aged 20 Years or Older 68.3% BMI > 25 (Overweight) 33.9% BMI > 30 (Obese) Source: Flegal, K. M. et al. Prevalence and Trends in Obesity among US Adults, JAMA 2010;303:
5 Prevalence of Obesity for Adults BMI >35 Among Adults Aged 20 Years or Older 14.3% BMI > 35 (Obese) 5.7% BMI > 40 (Severely Obese) Source: Flegal, K. M. et al. Prevalence and Trends in Obesity among US Adults, JAMA 2010;303:
6 Obesity-Associated Comorbididites Research has shown that as weight increases to reach the levels referred to as "overweight" and "obesity," the risks for the following conditions also increases: 1 Coronary heart disease Type 2 diabetes Cancers (endometrial, breast, and colon) Hypertension (high blood pressure) Dyslipidemia (for example, high total cholesterol or high levels of triglycerides) Stroke Liver and gallbladder disease Sleep apnea and respiratory problems Osteoarthritis (a degeneration of cartilage and its underlying bone within a joint) Gynecological problems (abnormal menses, infertility) 1 NIH, NHLBI Obesity Education Initiative. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. Available online:
7 How is Obesity Treated? Non-Surgical Treatment Medication Diet and exercise Behavior modification Surgical Treatment Due to the high failure rate in maintaining weight loss after medically supervised diets, surgery has proven to be the most effective and only durable treatment for morbidly obese patients. It delivers long-term weight loss, with minimal morbidity and mortality, and also improves or achieves complete remission for several of the comorbidities associated with the disease. 1 Only surgery has proven effective over the long term for most patients with clinically severe obesity. --The National Institutes of Health Consensus Conference Statement, Source: Abu-Jaish and Rosenthal, Sleeve Gastrectomy: a New Surgical Approach for Morbid Obesity, Expert Rev. Gastroenterol. Hepatol. 4(1), (2010)
8 Bariatric Surgery Overview What is Bariatric Surgery? Bariatric surgery is a medical procedure that produces weight loss by limiting how much the stomach can hold, and by limiting absorption of calories. What is the Goal of Bariatric Surgery? The goal of bariatric surgery is for the patient to lose over half his/her excess weight in order to help reduce or prevent obesity-related health problems What are the Procedural Options? Bariatric Procedures can be classified into three main categories: 1) Restrictive - Laparoscopic Sleeve Gastrectomy, Laparoscopic Adjustable Gastric Banding 2) Malabsorptive - Biliopancreatic Diversion and Duodenal Switch 3) Combination of Restrictive and Malabsorptive - Roux-en-Y Gastric Bypass Is Success Guaranteed? Bariatric surgery is a tool to help patients lose weight, but must be combined with lifelong commitment to diet, activity, and support to increase the chances of success.
9 American Society of Metabolic and Bariatric Surgery Statement Treatment for Metabolic Diseases and Conditions: Bariatric surgery is known to be the most effective and long lasting treatment for morbid obesity and many related conditions, but now mounting evidence suggests it may be among the most effective treatments for metabolic diseases and conditions, including type 2 diabetes, hypertension, high cholesterol, non-alcoholic fatty liver disease and obstructive sleep apnea. Improved Safety: According to a recent study from the Agency for Healthcare Research and Quality (AHRQ), the mortality rate associated with bariatric surgery dropped by a staggering 78.7%, from 0.89% in 1998 to 0.19% in Meanwhile, the mortality rate from morbid obesity was reduced by 89% after bariatric or metabolic surgery, according to a study published in the Annals of Surgery in ASMBS Statement, August 22,
10 American Diabetes Association Statement Surgery for Weight Loss: Gastric reduction surgery can be an effective weight loss treatment for obesity and may be considered in people with diabetes who have BMI 35 kg/m 2. Surgery for Type 2 Diabetes Resolution: A meta-analysis of studies of bariatric surgery reported that 77% of individuals with type 2 diabetes had complete resolution of diabetes (normalization of blood glucose levels in the absence of medications), and diabetes was resolved or improved in 86%. -- Nutrition Recommendations and Interventions for Diabetes: A Position Statement of the American Diabetes Association
11 Review of the Normal Digestive System Esophagus The muscular tube that carries solid foods and liquids from the mouth to the stomach Stomach The storage pouch of the gastro-intestinal tract. After food is swallowed, it arrives in the stomach, where it is processed before passing to the small intestine. Small Intestine (Duodenum, Jejunum, Ileum) A foot tube where the vast majority of nutrients and calories from food are absorbed. Large Intestine The final part of the digestive tract where water is re-absorbed into the body from the leftover liquid from digested food. Normally, as food moves along the digestive tract, appropriate digestive juices and enzymes arrive at the right place at the right time to digest and absorb calories and nutrients. After chewing and swallowing the food, it moves down the esophagus to the stomach, where a strong acid continues the digestive process. When the stomach contents move through the pylorus to the duodenum, bile and pancreatic juice speed up the digestion. Most of the calcium and iron in the foods we eat is absorbed in the duodenum. The jejunum and ileum complete the absorption of almost all calories and nutrients. The food particles that cannot be digested in the small intestine are stored in the large intestine and eliminated.
12 Normal Digestive Process Animation Animations available on
13 Three Types of Most Commonly Performed Bariatric Surgery Procedures Restrictive Malabsorptive Combination Sleeve Gastrectomy Adjustable Gastric Banding Biliopancreatic Diversion with Duodenal Switch Roux-en-Y Gastric Bypass
14 Open and Laparoscopic Techniques Most bariatric surgeries today use laparoscopy, in which a small incision is made in the abdomen and a small camera, or scope, enables the surgeon to view internal organs on a video monitor. Other small incisions are made to insert surgical instruments. Laparoscopic surgery is less invasive than open abdominal procedures, resulting in less postoperative pain, fewer wound complications, shorter hospital stays and quicker returns to work. Through recent technological advances, some minimally invasive procedures are now being performed through the SILS procedure, an advanced technique that requires only one small incision (typically through the belly button), rather than multiple small incisions.
15 Sleeve Gastrectomy Procedure This procedure involves surgery only on the stomach and does not involved any surgery on the intestine. It basically consists of making a stomach that (before surgery) looks like a pouch into a long tube, or sleeve. The sleeve gastrectomy procedure removes approximately 2/3 of the stomach, which provides for quicker satiety (sense of fullness) and decreased appetite. The smaller stomach sleeve restricts food intake by allowing only a small amount of food to be eaten at one time.
16 Sleeve Gastrectomy Procedure 1. A small sleeve (or narrow tube) is created with a surgical stapler along the inside curve of the stomach, from the pylorus of the stomach up to the esophagus. 2. After the separation of the stomach into a smaller tube is completed, the remainder of the stomach is removed. 3. The valve at the outlet of the stomach remains, which provides for the normal process of stomach-emptying to continue, which allows for the feeling of fullness. 4. The muscle defects underneath the skin are often closed with suture that is absorbable. The skin incisions are then closed with suture, steri-strips or staples, depending on the surgeon s preference.
17 Sleeve Gastrectomy Animation Animations available on
18 Laparoscopic Sleeve Gastrectomy (LSG) PATIENT Benefits More effective EWL and T2D resolution than LAGB 1 No need for additional visits for band fills (as with adjustable gastric banding No foreign body Less or absent nutritional deficiencies than LRYGB 2 Greater appetite suppression than LRYGB 3 Can be performed laparoscopically on high BMI patients 3 HOSPITAL Benefits Less resource allocation (potentially shorter LOS than LRYGB) Increased opportunity for SILS technique when compared to LRYGB When combined with LRYGB and LAGB more comprehensive/ competitive patient offering SURGEON Benefits Minimal follow-up required when compared to LRYGB and LAGB 3 (resource strain) Can be performed laparoscopically on high BMI patients 3 Technically simpler 3 and increased opportunity for SILS technique when compared to LRYGB No re-routing of anatomy; no anastomosis Relatively new procedure marketing cache/image/buzz 1 Birkmeyer et al. Hospital Complication Rates with Bariatric Surgery in Michigan 2 Gehrer et al. Fewer Nutrient Deficiencies After LSG than After LRYGB A Prospective Study 3
19 Roux-en-Y Gastric Bypass Procedure This procedure involves surgery on both the stomach and the intestine. As gastric bypass implies, following this surgical procedure, food is now routed past most of the stomach and the first part of the small intestine. In addition to restricting food intake, a Roux-en-Y Gastric Bypass reduces nutrient absorption.
20 Roux-en-Y Gastric Bypass Procedure 1. A small stomach pouch is (about the size of your thumb) is created using a surgical stapler. a. The small stomach pouch restricts food intake. 2. The small bowel is divided, using a surgical stapler, about two feet from the stomach. 3. One end of the small intestine is brought up and attached to the stomach pouch (gastrojejunostomy). 4. The other end of the small intestine, still connected to the non-functional stomach remnant, is reconnected to the intestinal tract (jejunojejunostomy). 5. The surgeon usually places a plastic drainage tube near the gastro-jejunal anastomosis to serve as a sentinel for a leak in this area. 6. The muscle defects underneath the skin are often closed with suture that is absorbable. The skin incisions are then closed with suture, steri-strips or staples, depending on the surgeon s preference.
21 Roux-en-Y Gastric Bypass Animation Animations available on
22 Laparoscopic Roux-en-Y Gastric Bypass (LRYGB) PATIENT Benefits HOSPITAL Benefits SURGEON Benefits Robust long-term data available No need for additional visits for band fills (as with adjustable gastric banding) More effective EWL and T2D resolution than LAGB and LSG 1,2 No foreign body Widely accepted by insurance Established care pathways known body of evidence on what to do Less resource strain than LAGB (no routine maintenance/fills required) Widely accepted by insurance More effective EWL and T2D resolution than LAGB and LSG 1,2 1 Birkmeyer et al. Hospital Complication Rates with Bariatric Surgery in Michigan 2 Lee et al. Gastric Bypass vs Sleeve Gastrectomy for Type 2 Diabetes Mellitus
23 Adjustable Gastric Banding Procedure This procedure utilizes an adjustable band that restricts the opening to the remainder of the stomach, attempting to create anatomy that provides a sensation of satiety after a very small meal. A band is placed at the top of the stomach, creating a pouch. The opening to the rest of the digestive tract is adjustable through an epidermal port. Appropriate aftercare and routine band adjustments are critical to the long-term success of this procedure.
24 Adjustable Gastric Banding Procedure 1. A band is placed around the top of the stomach, creating a small pouch that limits food intake. 2. A small port is affixed inside the body that allows the band to be adjusted later to make the pouch smaller or larger. 3. The muscle defects underneath the skin are often closed with suture that is absorbable. The skin incisions are then closed with suture, steri-strips or staples, depending on the surgeon s preference.
25 Adjustable Gastric Banding Animation Animations available on
26 Laparoscopic Adjustable Gastric Banding (LAGB) PATIENT Benefits HOSPITAL Benefits SURGEON Benefits Lowest rate of complications when compared to LRYGB and LSG 1 No re-routing of the anatomy; no stapling of stomach; no anastomosis Lowest rate of readmission and emergency department visits when compared to LRYGB and LSG 1 Shorter Length of Stay than LRYGB and LSG Potential opportunity for increased cash pay patients Increased opportunity for SILS technique when compared to LRYGB On average, less operative time required can stack more cases each day Increased opportunity for SILS technique when compared to LRYGB 1 Birkmeyer et al. Hospital Complication Rates with Bariatric Surgery in Michigan 2 Abu-Jaish et al. Sleeve Gastrectomy: a New Surgical Approach for Morbid Obesity
27 Who is Eligible for Bariatric Surgery? Through its Obesity Education Initiative, the National Institutes of Health issued the following recommendation: Surgical intervention is an option for carefully selected obesity (a BMI > 40 or > 35 with comorbid conditions) when less invasive methods of weight loss have failed and the patient is at high risk for obesity-associated morbidity and mortality. 1 For patients interested in learning more about their surgical options, a Surgery Eligibility Tool is available at Bariatrics4Diabetes.com. diabetes/bariatric-surgery-eligibility 1 Source: Clinical Guidelines on the Identification, Evaluation and Treatment of Overweight and Obesity in Adults: The Evidence Report,
28 Who is NOT Eligible for Bariatric Surgery? Bariatric Surgery is NOT recommended for patients with*: Untreated major depression or psychosis Binge eating disorders Current drug or alcohol abuse Severe heart disease that makes anesthesia prohibitively risky Severe inability of blood to clot normally Patients unable or unwilling to quit smoking BMI < 35 Currently pregnant Some previous surgery and chronic condition restrictions may prevent eligibility * Note: additional restrictions may apply; please consult your physician for additional information
29 Possible Side Effects and Complications Potential side effects of bariatric surgery include, but are not limited to: Nausea and vomiting Gas and bloating Lactose intolerance Temporary hair thinning Depression and psychological distress Changes in bowel habits Potential complications of bariatric surgery include, but are not limited to: Infection, bleeding or leakage at suture/staple lines Blockage of intestines or stomach pouch Dehydration Blood clots in legs or lungs Vitamin and/or mineral deficiency Protein malnutrition Incisional hernia Irreversibility, or difficulty reversing some procedures Revision procedure(s) sometimes needed Death
30 Typical Patient Care Pathway Initial Contact Informational Seminar Pre-Op Information Exchange Preoperative Evaluation Surgery Post-Op Follow-Up and Support Success!
31 What Patients Can Expect After Surgery In the Weeks Following the Procedure No strenuous activities for three weeks after surgery Patients may walk and perform light household duties as tolerated Most patient return to work 2-4 weeks after surgery Individual circumstances may vary Patient s Lifetime Commitment is Critical to Success Eat healthy foods Take vitamins, minerals and protein supplements Maintain an active lifestyle Attend support group meetings Follow-up with surgical team Avoid alcohol for at least one year post-surgery Avoid tobacco products
32 Questions?
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Understanding Obesity
 Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS
 GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Roux-en-Y Gastric Bypass
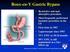 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Catholic Medical Center & Androscoggin Valley Hospital. Surgical Weight Loss Options For a Healthier Tomorrow
 Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
Metabolic and Bariatric Surgery Center
 Metabolic and Bariatric Surgery Center www.bannerhealth.com/universitytucsonsurgicalweightloss 1 Welcome to Banner University Medical Center s Metabolic and Bariatric Surgery Center Thank you for choosing
Metabolic and Bariatric Surgery Center www.bannerhealth.com/universitytucsonsurgicalweightloss 1 Welcome to Banner University Medical Center s Metabolic and Bariatric Surgery Center Thank you for choosing
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
BARIATRIC SURGERY. Prerequisites. Authorization, Notification and Referral
 BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY. Personalized Weight Loss Program
 BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
Weight Loss Surgery. Malabsorptive: Your intestines are rearranged to reduce the amount of food absorbed into the system
 The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
Surgical Weight Loss Program SURG CAL WEIGHT LOSS. at University Medical Center
 Surgical Weight Loss Program 1 SURG CAL WEIGHT LOSS at University Medical Center Welcome to the University Medical Center Surgical Weight Loss Program Thank you for choosing UMC for your weight loss surgery.
Surgical Weight Loss Program 1 SURG CAL WEIGHT LOSS at University Medical Center Welcome to the University Medical Center Surgical Weight Loss Program Thank you for choosing UMC for your weight loss surgery.
Weight Loss Surgery. Our Surgeons. A Patient s Guide
 Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Weight Loss Surgery Information Session. WFBH Bariatric Surgery Program
 Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Roux-en-Y Gastric Bypass. A Surgical Treatment for Weight Loss
 Roux-en-Y Gastric Bypass A Surgical Treatment for Weight Loss When Weight Becomes a Problem Is excess weight affecting your life and your health? A surgery called roux-en-y gastric bypass may help you
Roux-en-Y Gastric Bypass A Surgical Treatment for Weight Loss When Weight Becomes a Problem Is excess weight affecting your life and your health? A surgery called roux-en-y gastric bypass may help you
Bariatric Surgery Guide
 One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Weight Loss Surgery A Patient s Guide
 Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Bariatric Surgery Guide Dr. Stewart s Weight Loss Specialists of North Texas
 Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary?
 White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
What is the Sleeve Gastrectomy?
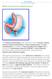 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Weight Loss Surgery Program
 Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
really help your physical, social and emotional wellbeing helping you do more of the things you want and feel more confident and relaxed.
 Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Introduction to obesity surgery
 Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
HOUSTON METHODIST SURGICAL WEIGHT LOSS
 HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
Weight Loss Surgery Information Session
 Welcome to the University Medical Center Surgical Weight Loss Program. Thank you for choosing UMC for your weight loss surgery. Our goal is to provide you with a successful surgery, giving each person
Welcome to the University Medical Center Surgical Weight Loss Program. Thank you for choosing UMC for your weight loss surgery. Our goal is to provide you with a successful surgery, giving each person
Bariatric and Metabolic Surgery
 Bariatric and Metabolic Surgery It may reduce more than just your weight. It may reduce certain risk factors. The information in this brochure is intended as Before Cholesterol 250 Blood pressure 149/95
Bariatric and Metabolic Surgery It may reduce more than just your weight. It may reduce certain risk factors. The information in this brochure is intended as Before Cholesterol 250 Blood pressure 149/95
Bariatric Surgery. Beth A. Ryder, MD FACS. Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University
 Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY
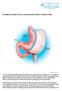 INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
Metabolic & Bariatric Surgery
 Metabolic & Bariatric Surgery Are you...tired of struggling with your weight? aware those extra pounds are putting your health at risk? ready to start a new path to take charge of your life again? If so,
Metabolic & Bariatric Surgery Are you...tired of struggling with your weight? aware those extra pounds are putting your health at risk? ready to start a new path to take charge of your life again? If so,
Choices Around Bariatric Surgery
 Choices Around Bariatric Surgery What should you know? Richard Stubbs MD FRCS FRACS Wakefield Obesity Clinic, Wellington 152 kg / BMI 59 74 kg / BMI 29 Indications (NIH Consensus Statement 1991) BMI >
Choices Around Bariatric Surgery What should you know? Richard Stubbs MD FRCS FRACS Wakefield Obesity Clinic, Wellington 152 kg / BMI 59 74 kg / BMI 29 Indications (NIH Consensus Statement 1991) BMI >
Surgical Associates of Ithaca Guide to Weight-loss Surgery
 Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY)
 BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY) WHAT IS OBESITY? Obesity is the condition whereby the individual sustains the body weight that is significantly higher than ideal body weight for
BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY) WHAT IS OBESITY? Obesity is the condition whereby the individual sustains the body weight that is significantly higher than ideal body weight for
Lose the Weight, Find your Life
 Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Sudbury Bariatric Regional Assessment & Treatment Centre
 Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Gastric Surgery for Clinically Severe (Morbid) Obesity
 Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Gastric Bypass Surgery
 Gastric Bypass Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Bypass Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Transmittal 54 Date: APRIL 28, 2006. SUBJECT: Bariatric Surgery for Treatment of Morbid Obesity
 CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 54 Date: APRIL 28, 2006 Change
CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 54 Date: APRIL 28, 2006 Change
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types:
 INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
BARIATRIC SURGERY PATIENT GUIDE
 You the patient play a critical role in the long term success of surgery. You will need to: Commit to improving your health. Discuss your health history with your surgeon. Discuss any questions or concerns
You the patient play a critical role in the long term success of surgery. You will need to: Commit to improving your health. Discuss your health history with your surgeon. Discuss any questions or concerns
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
5/9/2012. What is Morbid Obesity? Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person)
 Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS Prime Surgicare Morbid Obesity and Treatment Options Qualifying for Bariatric Surgery Co-morbid Conditions Coping with Concerns Life After Surgery Morbid Obesity and Treatment
FREQUENTLY ASKED QUESTIONS Prime Surgicare Morbid Obesity and Treatment Options Qualifying for Bariatric Surgery Co-morbid Conditions Coping with Concerns Life After Surgery Morbid Obesity and Treatment
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
SlEEvE GASTRECTomY SURGERY What is a sleeve gastrectomy operation? BARIATRIC SURGERY
 Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
Sleeve Gastrectomy Weight Loss Surgery General Information
 Sleeve Gastrectomy Weight Loss Surgery General Information What is obesity? How can weight loss surgery (WLS) help? In recent years, we have slowly begun to understand obesity as a disease a chronic disease
Sleeve Gastrectomy Weight Loss Surgery General Information What is obesity? How can weight loss surgery (WLS) help? In recent years, we have slowly begun to understand obesity as a disease a chronic disease
Treatment for Severely Obese Patients
 Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS. Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence
 PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE
 INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
The Role of Obesity in Bariatric Surgery - Part 1
 MORBID OBESITY: The Role of Bariatric Surgery Rajan V. Nair, MD Medical Director Salem Hospital Bariatric Surgery Program ICL Willamette University Tuesday November 27, 2012 DISCLOSURES Medical Director,
MORBID OBESITY: The Role of Bariatric Surgery Rajan V. Nair, MD Medical Director Salem Hospital Bariatric Surgery Program ICL Willamette University Tuesday November 27, 2012 DISCLOSURES Medical Director,
Weight Loss Surgery Program
 Weight Loss Surgery Program Weight loss surgery helped me loose 112 pounds. - Jennifer Weaver Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When Jennifer Weaver s husband was diagnosed
Weight Loss Surgery Program Weight loss surgery helped me loose 112 pounds. - Jennifer Weaver Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When Jennifer Weaver s husband was diagnosed
Weight Loss Surgery Advisory
 PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
The weight of the world.
 The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Consent Document for Bariatric Surgery
 Consent Document for Bariatric Surgery I,, have read and understand the following document completely. In addition, my surgeon has discussed with me at length and I completely understand the risks, benefits,
Consent Document for Bariatric Surgery I,, have read and understand the following document completely. In addition, my surgeon has discussed with me at length and I completely understand the risks, benefits,
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Weight Loss Surgery Educational Seminar
 Weight Loss Surgery Educational Seminar Attendee Handout Obesity Overview Obesity is on the rise in the US Body Mass Index (BMI) (see chart in this handout, page 9) o 18.5-24.9: Ideal Less than 1/3 of
Weight Loss Surgery Educational Seminar Attendee Handout Obesity Overview Obesity is on the rise in the US Body Mass Index (BMI) (see chart in this handout, page 9) o 18.5-24.9: Ideal Less than 1/3 of
BILIOPANCREATIC DIVERSION WITH DUODENAL SWITCH SURGERY
 WITH DUODENAL SWITCH SURGERY Disclaimer This movie is an educational resource only and should not be used to manage Obesity. All decisions about surgical management of Obesity must be made in conjunction
WITH DUODENAL SWITCH SURGERY Disclaimer This movie is an educational resource only and should not be used to manage Obesity. All decisions about surgical management of Obesity must be made in conjunction
Southcoast Center for Weight Loss
 Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Advancing the Field of Bariatric Surgery at University Hospitals
 Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS
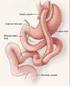 INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS You are considering undergoing a laparoscopic Roux-en-Y gastric bypass for weight loss. The purpose of this information sheet is to provide you
INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS You are considering undergoing a laparoscopic Roux-en-Y gastric bypass for weight loss. The purpose of this information sheet is to provide you
Hypnotic. Gastric Band. Paul McKenna
 Hypnotic Gastric Band Paul McKenna Hypnotic Gastric Band The Amazing Truth About A Hypnotic Gastric Band A Gastric Band is a radical, surgical operation that reduces the available space in your stomach
Hypnotic Gastric Band Paul McKenna Hypnotic Gastric Band The Amazing Truth About A Hypnotic Gastric Band A Gastric Band is a radical, surgical operation that reduces the available space in your stomach
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Weight Loss Surgery and Bariatric Nutrition. Jeanine Giordano, MS, RD, CDN
 Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
The Evolution of Bariatric Surgery. History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics
 The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
Bariatric Surgery Education Syllabus
 Bariatric Surgery Education Syllabus Texas Health Fort Worth Bariatric Services (located in the Klabzuba Tower) 1300 West Terrell Ave, Suite 220 Fort Worth, TX 76104 (817) 250-4933 Revised January 2015
Bariatric Surgery Education Syllabus Texas Health Fort Worth Bariatric Services (located in the Klabzuba Tower) 1300 West Terrell Ave, Suite 220 Fort Worth, TX 76104 (817) 250-4933 Revised January 2015
Laparoscopic Gastric Bypass Informa8on
 (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery (weight loss surgery), is a surgical procedure that alters the process of diges8on. Bariatric
(Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery (weight loss surgery), is a surgical procedure that alters the process of diges8on. Bariatric
Top Ten Things You Need to Know About Bariatric Surgery Patients. Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN
 Top Ten Things You Need to Know About Bariatric Surgery Patients Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN Top Ten Things You Need to Know About Bariatric Surgery
Top Ten Things You Need to Know About Bariatric Surgery Patients Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN Top Ten Things You Need to Know About Bariatric Surgery
12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16
 HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Bariatric Surgery Program. Report on Bariatric Surgery
 Bariatric Surgery Program Report on Bariatric Surgery Mike Ambrosio lost 153 pounds in 11 months and considered the surgery the best decision of his life. Table of Contents Highlights of Care...2 Nationally
Bariatric Surgery Program Report on Bariatric Surgery Mike Ambrosio lost 153 pounds in 11 months and considered the surgery the best decision of his life. Table of Contents Highlights of Care...2 Nationally
