Hip dislocations occur infrequently and almost always. Asymmetric Bilateral Hip Dislocation after Motor Vehicle Accident
|
|
|
- Leslie Benson
- 8 years ago
- Views:
Transcription
1 320 Asymmetric Bilateral Hip Dislocation after Motor Vehicle Accident A Case Study and Review of the Literature Samuel Sanders, M.D., and Nirmal C. Tejwani, M.D. Abstract Bilateral asymmetric dislocations of the hip are rare compared to unilateral dislocations. This case study describes a female restrained passenger involved in a motor vehicle accident who sustained asymmetric bilateral hip dislocations. The patient underwent successful closed reduction of both hips. The clinical course and follow-up assessment of the patient was otherwise uneventful. Computed tomography scans, essential for diagnosing intra-articular loose bodies and subtle s, were performed after reduction and revealed in the right hip a nondisplaced acetabular rim of the posterior wall on the side of the posterior dislocation. Hip dislocations are an injury requiring careful trauma evaluation to rule out concomitant injuries. Time to presentation and, more importantly, reduction of a hip dislocation, is essential in treating this injury and preventing long-term complications, such as avascular necrosis and posttraumatic arthritis. The incidence, anatomy, mechanism of injury, treatment options, and long-term sequelae of hip dislocation, with literature review, are discussed. Samuel Sanders, M.D., was a Chief Resident in the Department of Orthopaedic Surgery, NYU Hospital for Joint Diseases. Nirmal C. Tejwani, M.D., is Associate Professor, New York University School of Medicine, and from the Division of Orthopaedic Trauma, Department of Orthopaedic Surgery, NYU Hospital for Joint Diseases, NYU Langone Medical Center, New York, New York. Correspondence: Nirmal Tejwani, M.D., Suite1402, Department of Orthopaedic Surgery, NYU Hospital for Joint Diseases, 301 E 17th Street, New York, New York 10003; nirmal.tejwani@med. nyu.edu. Hip dislocations occur infrequently and almost always after traumatic injury; 85% to 90% of these are posterior dislocations. 1 Bilateral hip dislocations are rare and asymmetric are even more rare, with only 14 reported cases in the literature. A Medline search was performed for articles, using the key words traumatic bilateral hip dislocation. The search resulted in 14 cases of asymmetric bilateral hip, all of which occurred in male patients and the majority of which resulted from a motor vehicle accident. To the best of our knowledge, this case report is the first to describe this injury pattern in a female patient. All of the cases reviewed had varying times of reduction of the femoral heads, but all resulted in positive outcomes. Associated injuries that were described included femur 2 and acetabular. 3 Case Description A 31-year-old female restrained passenger in a motor vehicle accident was brought by ambulance to the trauma bay after the automobile in which she was traveling collided with a brick wall at approximately 30 mph. Upon arrival, she was found to be hemodynamically stable, with a Glasgow Coma Scale (GCS) score of 15. During the initial evaluation, it was found that there was no loss of consciousness (LOC) or internal injuries sustained during the accident. The patient arrived at the trauma bay within 2 hours of the accident and had obvious deformities of both lower extremities. On physical examination, the right hip was shortened, adducted, and internally rotated. The patient had limited external rotation, with passive and active range of motion, and had greater than 45 passive internal rotation. The left hip was shortened, flexed, abducted, and externally rotated. There was limited internal rotation, with passive and active range of motion, and greater than 45 of passive external rotation. The lower extremities had palpable pulses, with sensation and motor function intact bilaterally. Initial imaging included anteroposterior radiographs of the pelvis that revealed a right posterior hip dislocation and left anterior-inferior hip dislocation (Fig. 1A). Using conscious sedation (100 mg of IV fentanyl and 4 mg of IV Versed ), the right posterior hip dislocation was reduced first Sanders S, Tejwani NC. Asymmetric bilateral hip dislocation after motor vehicle accident: a case study and review of the literature. Bull NYU Hosp Jt Dis. 2008;66(4):320-6.
2 A 321 B Figure 1 A, Right posterior hip dislocation and left anterior-inferior hip dislocation injury. B, Post-reduction radiograph of the pelvis, demonstrating reduced hips without any obvious s. A B Figure 2 CT scans showing a small right-sided acetabular rim of the posterior wall. with gentle traction and countertraction with both the hip and knee in 90 of flexion. This maneuver was accompanied by gentle internal rotation to clear the posterior acetabular rim, followed by external rotation to position the femoral head within the acetabulum. Once the right hip was reduced, traction and countertraction was applied to the left hip in 45 of flexion and the knee in 90 of flexion. With traction being held, the hip was gently externally rotated to clear the anterior acetabular rim and then internally rotated to seat the femoral head within the acetabulum. A post-reduction radiograph of the pelvis demonstrated reduced hips without any obvious s (Fig. 1B). A post-reduction computed tomography (CT) scan showed a small right-sided acetabular rim of the posterior wall (Fig. 2). Radiographs of the wrist and hand showed a fifth metacarpal, treated by delayed operative fixation. At 6 months, the patient was jogging 15 miles per week and complained of an occasional dull aching right hip pain (side of posterior dislocation) only during sudden changes in weather. Discussion Anatomy The hip joint is a true ball-and-socket joint in which the head is incompletely covered. Because of the depth of the acetabulum, enhanced by the labrum, and its thick capsule and strong muscular support, the hip joint is less likely to dislocate than any other joint in the body. The ligamentous support is provided by strong capsular ligaments that run from the acetabulum to the femoral neck and the intertrochanteric region. The iliofemoral, or Y ligament, is located anteriorly. The ischiofemoral ligament is located posteriorly. The short external rotators adhere to the capsule posteriorly, providing additional stability. The blood supply to the femoral head has been well described.1 In adults, the main arterial supply is derived from the cervical arteries, which originate from an extracapsular ring at the base of the femoral neck. This ring is formed by contributions from the medial femoral circumflex artery posteriorly and the lateral femoral circumflex artery anteriorly. The capital branches pass through the
3 322 Table 1 Reported Asymmetric Hip Dislocations Time (Hrs) Traction X PWB FWB AVN F/U Case Age/Sex Mechanism Treatment P Injury Injuries (wks) at (wks) at (wks) Y/N (mos) 1 36/M MVA Anterior Closed N 20 Posterior Closed Acetabular 6 10 N (ORIF) Open patella (incision and drainage 2 26/M Trapped Anterior Open N 60 between Posterior Closed 2 4 N auto & wall 3 28/M MVA Anterior Closed N 24 Posterior Open Acetabular 6 Y at 8 M /M Thrown from Anterior Closed N motorcycle Posterior Closed N 5 18/M MVA Anterior Closed Posterior Closed /M Ped struck Anterior Closed N 36 Posterior Closed Acetabular 6 12 N 7 50/M MVA Anterior Closed N 12 Posterior Closed Femoral shaft 4 N (ORIF) 8 18/M MVA Anterior Open 6 12 N 24 Posterior Closed 6 12 N /M MVA Anterior Closed 12 Posterior Closed Acetabular 10 28/M MVA Anterior Closed 6 Posterior Closed /M Fall from Anterior Closed Femoral head a height (Open treatment) Posterior Closed 12 38M Plane crash Anterior Closed 6 Posterior Closed SI joint diastasis 13 21M MVA Anterior Closed N 44 Posterior Closed Lisfranc N /dislocation 14* 31F MVA Anterior Closed 2 1 Posterior Closed 1 15 Anterior Posterior 16 Anterior Posterior 17 Anterior Posterior *Current Case; PWB, Partial weightbearing; FWB, Full weightbearing capsule close to its insertion to lie on the femoral neck. They then ascend the neck and enter the femoral head just below the articular surface. The superior and posterior cervical arteries are derived primarily from the medial circumflex artery. They are larger and outnumber the anterior vessels. A lesser contribution to the femoral head comes from the foveal artery via the ligamentum teres. With a hip dislocation, whether anterior and posterior, the tenuous blood supply will be compromised, which can lead to an increased risk of avascular necrosis (AVN). 4 Mechanism of Injury In multiple case studies, the mechanism of bilateral asymmetric dislocation of the hips has been shown to be
4 323 Table 2 Systems for Classifying Hip Dislocation Stewart-Milford System Type I Simple dislocation without Type II Dislocation with one or more rim fragments but with sufficient socket to endure stability after reduction Type III Dislocation with of the rim, producing gross instability Type IV Dislocation with of the head or neck of the femur Thompson-Epstein System Type I Dislocation with or without minor Type II Dislocation with single large of the posterior rim of the acetabulum Type III Dislocation with a comminuted of the rim with or without a large major fragment Type IV Dislocation with of the acetabular floor Type V Dislocation with of the femoral head dashboard injuries. 2,3,5,6-8 The direction of the dislocation is dependent on the position of the hip and the direction of the force vector applied, as well as the anatomy of the femur. 9 Asymmetric dislocation in a patient is due to the differing positions of the lower extremity during impact. 1 The impact on the knee with the hip in an adducted position leads to a backward force, causing a posterior dislocation. In contrast, an anterior dislocation occurs with the hip in abduction and external rotation. Associated Injuries and Pathoanatomy Associated injuries include those directly related to the hip dislocation and those due to the traumatic incident itself. Ipsilateral injuries include femoral head, neck, and shaft s; acetabular s; pelvic s; sciatic nerve injury; knee injuries; and foot and ankle injuries Knee injuries, including patellar s, ligament rupture, and knee dislocation, are associated with posterior dislocations due to direct trauma to the knee. Intra-abdominal, head, and chest trauma have also been widely reported. A high index of suspicion must be maintained and careful trauma evaluation is necessary for all patients with a hip dislocation. It should also be noted that the frequency of severe associated injuries often causes delay in the diagnosis of dislocation. 4 With hip dislocations, the capsule and the ligamentum are usually disrupted. Labral tears and muscular injury can occur as well. In anterior dislocations, the psoas is a fulcrum for the hip, and the capsule is disrupted anteriorly and inferiorly. Posterior dislocations tear through the capsule either inferoposterior or directly posteriorly, depending on the amount of flexion present. The Y ligament is usually intact, and the capsule is stripped from its acetabular attachment posterior to it. In some cases, however, the Y ligament may be avulsed from the acetabulum with a fragment of bone. 13 Fractures of the femoral head are common and may be the result of impaction injuries, avulsions, or shear s. Impaction injuries commonly occur in anterior dislocations. 1 Avulsed fragments of bone are frequently found attached to the ligamentum teres and lying in the fovea. Posterior dislocations may be associated with acetabular s, similar to our patient who sustained a posterior wall. Classification System The first part of the description is the specification of whether the direction of dislocation is anterior or posterior. Those of Stewart and Milford, and Thompson and Epstein are the most commonly used. These classification systems have been found to have prognostic significance, as s associated with operative acetabular or femoral head s have a worse prognosis than others In our patient, the classification was SM 2 for the right hip and SM 1 for the left hip (Table 1). 4 Diagnosis In the absence of femoral shaft or neck s, the position of the leg is the key to diagnosis. For the posterior dislocation, the leg is flexed, adducted, and internally rotated. With an anterior dislocation, the leg is externally rotated with varying amounts of flexion and abduction. A detailed examination of the entire lower extremity is required to rule out concomitant injury. A single AP radiograph as part of the standard Advanced Trauma Life Support (ATLS) protocol is usually sufficient to confirm the diagnosis. The head will not be congruent in the acetabulum. In posterior dislocations, the head will appear small and will lie superiorly and overlap the acetabular roof. In anterior dislocations, it will appear larger and will either lie inferiorly near the obturator foramen or overlap the medial acetabulum. Treatment The treatment of hip dislocations is aimed at the avoidance of complications. This begins with an emergent reduction. The incidence of AVN increases if reduction is delayed. 15,17 A closed reduction should always be attempted unless there is an associated hip or femoral neck. There are several described techniques in the reduction of both anterior and posterior hip dislocations. Regardless of the direction of the dislocation, the reduction can be attempted using in-line traction with the patient lying supine, with countertraction exerted by an assistant holding the pelvis, and with the reversal force of the injury. The preferred method is to perform a closed reduction under general anesthesia; if this is not feasible, reduction under intravenous sedation is possible. Regardless of the direction
5 324 of the dislocation, traction should be applied in a steady manner to overcome muscular spasms and elastic restraints. Femoral neck s may be caused by overly enthusiastic reduction maneuvers. 18 Three popular methods for achieving closed reduction of the hip are: 1. Allis method: Traction is applied in line with the deformity. The patient is placed supine, with the surgeon standing above the patient on the stretcher. Initially, the surgeon applies in-line traction, while the assistant applies countertraction by stabilizing the patient s pelvis. While increasing the traction force, the surgeon should slowly increase the degree of flexion to approximately 70. Gentle rotational motions of the hip and slight adduction will often help the femoral head clear the lip of the acetabulum. A lateral force to the proximal thigh may assist in reduction. An audible clunk is a sign of a successful closed reduction Stimson gravity technique: The patient is placed prone on the stretcher, with the affected leg hanging off the side of the stretcher. This brings the extremity into a position of both hip and knee flexion of 90 each. In this position, the assistant immobilizes the pelvis and the surgeon applies an anteriorly directed force on the proximal calf. Gentle rotation of the limb may assist in reduction Bigelow and reverse Bigelow maneuvers: These have been associated with iatrogenic femoral neck s and are not as frequently used as reduction techniques. In the Bigelow maneuver, the patient is supine, and the surgeon applies longitudinal traction on the limb. The adducted and internally rotated thigh is then flexed to at least 90. The femoral head is levered into the acetabulum by abduction, external rotation, and extension of the hip. In the reverse Bigelow maneuver, used for anterior dislocations, traction is again applied in the line of the deformity. The hip is then adducted, sharply internally rotated, and extended. 1 Approximately 2% to 15% of hip dislocations are irreducible. 4 In anterior dislocations, this may be due to buttonholing through the capsule or interposition of the rectus, capsule, labrum, or psoas. In posterior dislocations, the piriformis, gluteus maximus, capsule, ligamentum teres, or the labrum or a bone fragment may prevent reduction. 19 If the hip is irreducible, urgent, open reduction is recommended. If possible, Judet views, inlet and outlet views of the pelvis, and a CT study should precede the procedure to identify coincident bone injury and possible obstructions to reduction. Following closed reduction, radiographs should be obtained to confirm adequate reduction. The hip should be examined for stability while the patient is still sedated or under anesthesia. If an obvious large, displaced acetabular is found, the stability examination need not be performed. Stability is checked by flexing the hip to 90 in neutral position. A posteriorly directed force is then applied. If any subluxation is detected, the patient will require additional diagnostic studies and possibly surgical exploration or traction. After successful closed reduction and completion of the stability examination, the patient should undergo a CT scan to assess for any acetabular femoral head pathology and to evaluate possible loose bodies within the hip joints. If the hip is unstable, then skeletal traction is used. Operative Management The absolute indications for surgery include irreducible dislocations and nonconcentric reductions with intra-articular fragments of bone or cartilage. Irreducible dislocations should be treated as surgical emergencies. Open reduction should be performed from the direction that the hip dislocated. Posterior dislocations are addressed via a Kocher-Langenbach approach. The sciatic nerve is protected, and direct access to impediments to reduction is provided. The capsular disruption may require extension, and interposed soft tissue must be removed from the joint. The acetabulum should be examined for loose bodies before the hip is reduced. After the joint has been cleaned out, the hip is reduced. If an associated posterior wall exists, stability testing is required. After confirmation of the reduction, the bony, capsular and soft tissue injuries are repaired. 4 Irreducible anterior dislocations are addressed through an anterior or an anterolateral approach. The direct anterior approach will allow better visualization of the anterior joint and femoral head s, if present; the anterolateral approach allows access to the posterior hip through the same skin incision, if needed. The approach used depends on the associated lesions. 4 Removal of intra-articular fragments of bone or cartilage, especially if the reduction is not concentric, is another indication for surgery. 15,16,20 Small fragments that are seen in the fovea and which do not impinge on the head need not be removed. 21 This is a common finding and usually represents a small piece of bone avulsed from the femoral head by the ligamentum teres. The fragments that require removal are interposed between the articular surfaces of the head and the acetabulum. For small intra-articular fragments that will not require fixation, arthroscopic removal may be performed. 22 Using this technique, redislocation of the hip joint is not needed to debride the joint, and additional vascular insult to the head can be avoided. It may also be used to diagnose labral tears. 23 Regardless of the type of surgery, a concentric reduction of the hip should be confirmed before wound closure. The final indication for surgery is an unstable dislocation and requires surgical fixation of an acetabular. Often, stability testing under general anesthesia is required to determine stability. The definitive test for stability is a stress test. Since clinical instability leads to repeated subluxation and arthritis, the most conservative estimate must be used to determining stability. If more than 20%
6 325 of the posterior wall of the acetabulum is d, stress testing should be performed. 24 If an open reduction is being performed, direct examination of the hip should be done at the same time. If the hip is being reduced in a closed manner, the use of fluoroscopy will be helpful in assessing stability. The patient is positioned supine. The hip is flexed to 90, internally rotated slightly, and a posterior force is applied. 4 Post-Reduction Treatment Strict immobilization leads to intra-articular adhesions and arthritis, and therefore should be avoided. Some recommend a temporary period of traction or balance suspension until the patient s initial pain has subsided. 4 After this, controlled passive range of motion exercises with a continuous passive motion (CPM) machine and early mobilization are thought to benefit the patient s overall condition. Extremes of motion should be avoided for 4 to 6 weeks, to allow for capsular and soft tissue healing. At our institution, the patients with hip dislocations are mobilized as soon as pain permits, with no traction used. The patients are allowed to weightbear, as tolerated. Although early weightbearing has not been shown to add to the initial ischemic insult, it is believed that the amount of collapse in patients who develop AVN may be diminished if weightbearing is delayed. 24 Rehabilitation should include strengthening exercises for the musculature about the hip. Proprioceptive training, such as that with the use of a tilt board can be helpful. Return to high demand activities and sports should be delayed until hip strength is near normal. Outcome In general, anterior dislocations without femoral head injury have a better long-term prognosis than posterior dislocations. 1 Other variables have also been associated with poorer outcomes, although these may have their effect by inducing AVN or arthritis. Associated injuries have a negative prognostic effect on the clinical result. The most important prognostic factor is probably time to reduction. 14,15,17,25 AVN of the femoral head has also been found to occur in dislocations and is a poor prognostic indicator of clinical outcomes. AVN in previous studies was seen in 4.8% of those patients who received hip reduction in less than 6 hours; however, a 52.9% rate was seen in those whose hips were reduced after 6 hours. Weightbearing was not shown to have a significant effect on AVN in this study. 25 The dislocated hips of the patient being reported here were reduced within the first 3 hours and at last follow-up there was no radiological evidence of AVN. Long-term follow-up using imaging to monitor would benefit patients. AVN usually appears within 2 years, but has been seen to occur as long as 5 years after injury. None of the patients in the literature had developed AVN after 6 months of bilateral hip dislocation. Arthritis is the most common complication in those patients with dislocations from traumatic injuries. It has been shown to occur in up to 24% of patients, with those who have a sedentary lifestyle having lower rates after 14 years of follow-up. In those involved in the highest levels of manual work, up to 37.5% were shown to develop arthritis after traumatic accidents. 9 The damage to the chondrocytes at the time of the injury is probably responsible for the incidence of late arthritis seen after dislocation. It is important to counsel patients about the long-term impact of these injuries. Sciatic nerve injury is more common after -dislocation than after pure dislocation. If it occurs, it is usually partial and most often affects the peroneal distribution. Resolution after reduction of the dislocation is the rule, and exploration is not required unless nerve function was intact before the reduction and then lost afterward. Conclusion Hip dislocations are uncommon injuries that result from high energy trauma and require careful trauma evaluation to rule out concomitant injuries. Bilateral asymmetric dislocations are rare. This is the first report of such an injury in a female patient. Early reduction, within 6 hours, and close radiological follow-up, including CT scans, is recommended. It is also essential to educate and follow the patient for evidence of AVN and posttraumatic arthritis. Disclosure Statement None of the authors have a financial or proprietary interest in the subject matter or materials discussed, including, but not limited to, employment, consultancies, stock ownership, honoraria, and paid expert testimony. References 1. DeLee JC. Fractures and dislocations of the hip. In: Rockwood CA Jr, Green DP, Bucholz R (eds): Fractures in Adults (4th ed). Philadelphia: Lippincott-Raven, 1996, Vol 2, pp Kundu ZS, Mittal R, Sangwan SS, Sharma A. Simultaneous asymmetric bilateral hip dislocation with unilateral of the femur-peculiar mode of trauma in a case. Eur J Orthop Surg Traumatol. 2003;13: Martinez AA, Gracia F, Rodrigo J. Asymmetrical bilateral traumatic hip dislocation with ipsilateral acetabular. J Orthop Sci. 2000;5(3): Tornetta P, Mostafavi H. Hip Dislocation: current treatment regimens. J Am Acad Orthop Surg Jan;5(1): Dudkiewicz I, Salai M, Horowitz S, Chechik A. Bilateral asymmetric traumatic dislocation of the hip joints. J Trauma Aug;49(2): Kaleli T, Alyuz N. Bilateral traumatic dislocation of the hip: simultaneously one hip anterior and the other posterior. Arch Orthop Trauma Surg. 1998;117(8): Lam F, Walczak J, Franklin A. Traumatic asymmetrical bilateral hip dislocation in an adult. Emerg Med J Nov;18(6): Maqsood M, Walker AP. Asymmetrical bilateral traumatic hip dislocation with ipsilateral of the femoral shaft. Injury Sep;27(7): Upadhyay SS, Moulton A, Srikrishnamurthy K. An analysis
7 326 of the late effects of traumatic posterior dislocation of the hip without s. J Bone Joint Surg Br Mar;65(2): Gillespie WJ. The incidence and pattern of knee injury associated with dislocation of the hip. J Bone Joint Surg Br Aug;57(3): Suraci AL. Distribution and severity of injuries associated with hip dislocations secondary to motor vehicle accidents. J Trauma May;26(5): Wu CC, Shih CH, Chen LH. Femoral shaft s complicated by -dislocations of the ipsilateral hip. J Trauma Jan;34(1): Bucholz RW, Wheeless G. Irreducible posterior dislocations of the hip. The role of the iliofemoral ligament and the rectus femoris muscle. Clin Orthop Relat Res Jul;(167): Paus B. Traumatic dislocations of the hip; late results in 76 cases. Acta Orthop Scand. 1951;21(2): Stewart MJ, Milford MW. Fracture-dislocation of the hip; an end-result study. J Bone Joint Surg Am Apr;36(A:2): Thompson RC. A new physical test in dislocation of the hip. J Bone Joint Surg Am Sep;54(6): Brav EA. Traumatic dislocation of the hip: army experience and results over a twelve-year period. J Bone Joint Surg Am. 1962;44: Polesky RE, Polesky FA. Intrapelvic dislocation of the femoral head following anterior dislocation of the hip. A case report. J Bone Joint Surg Am Jul;54(5): Canale SF, Manugian AH. Irreducible traumatic dislocations of the hip. J Bone Joint Surg Am Jan;61(1): Levine RG, Kauffman CP, Reilly MC, Behrens FF. Floating pelvis. A combination of bilateral hip dislocation with a lumbar ligamentous disruption. J Bone Joint Surg Br Mar;81(2): Rosenthal RE, Coker WL. Posterior -dislocation of the hip: an epidemiologic review. J Trauma Aug;19(8): Keene GS, Villar RN. Arthroscopic loose body retrieval following traumatic hip dislocation. Injury Oct;25(8): Fitzgerald RH. Acetabular labrum tears. Diagnosis and treatment. Clin Orthop Relat Res Feb;(311): Stuck WG, Vaughan WH. Prevention of disability after traumatic dislocation of the hip. South Surg. 1949;15: Hougaard K, Thompson PB. Traumatic posterior dislocation of the hip prognostic factors influencing the incidence of avascular necrosis of the femoral head. Arch Orthop Trauma Surg. 1986;106(1):32-5.
Imaging of Lisfranc Injury
 November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
DISLOCATION AND FRACTURE-DISLOCATION OF THE HIP R. A. JASKULKA, G. FISCHER, 0. FENZL. From the Second Clinic of Trauma Surgery, University of Vienna
 DISLOCATION AND FRACTURE-DISLOCATION OF THE HIP R. A. JASKULKA, G. FISCHER,. FENZL From the Second Clinic of Trauma Surgery, University of Vienna of patients with posterior dislocations of the hip of type
DISLOCATION AND FRACTURE-DISLOCATION OF THE HIP R. A. JASKULKA, G. FISCHER,. FENZL From the Second Clinic of Trauma Surgery, University of Vienna of patients with posterior dislocations of the hip of type
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE
 ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation
 1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
Arthroscopy of the Hip
 Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
Arthroscopy of the Hip Professor Ernest Schilders FRCS, FFSEM Consultant Orthopaedic Surgeon Specialist in Shoulder and Hip Arthroscopy, Groin and Sports Injuries Private consulting rooms The London Hip
Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS
 Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS Steadman Hawkins Clinic Denver at Lone Tree 10103 RidgeGate Pkwy, Aspen Bldg#110 Lone Tree, CO 80124 Phone: 303-586-9500
Femoral Acetabular Impingement And Labral Tears of the Hip James Genuario, MD MS Steadman Hawkins Clinic Denver at Lone Tree 10103 RidgeGate Pkwy, Aspen Bldg#110 Lone Tree, CO 80124 Phone: 303-586-9500
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
PELVIS. 2007 Lippincott Williams & Wilkins S59 BONE: PELVIS (6) Location: Pelvic ring (61)
 PELVIS BONE: PELVIS (6) Location: Pelvic ring (61) Types: A. Lesion sparing (or with no displacement of) posterior arch (61-A) B. Incomplete disruption of posterior arch, partially stable (61-B) C. Complete
PELVIS BONE: PELVIS (6) Location: Pelvic ring (61) Types: A. Lesion sparing (or with no displacement of) posterior arch (61-A) B. Incomplete disruption of posterior arch, partially stable (61-B) C. Complete
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D.
 Hip Series Technique Guide Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D. As described by: J.W. Thomas Byrd, M.D. Southern Sports Medicine and Orthopaedic Center Nashville, TN Introduction
Hip Series Technique Guide Hip Arthroscopy Principles and Application J.W. Thomas Byrd, M.D. As described by: J.W. Thomas Byrd, M.D. Southern Sports Medicine and Orthopaedic Center Nashville, TN Introduction
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
Hamstring Apophyseal Injuries in Adolescent Athletes
 Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY
 George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Chapter 9 The Hip Joint and Pelvic Girdle
 Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. The Hip Joint and Pelvic Girdle Chapter 9 The Hip Joint and Pelvic Girdle Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Hip joint
Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. The Hip Joint and Pelvic Girdle Chapter 9 The Hip Joint and Pelvic Girdle Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Hip joint
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation
 What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
What Is Femoral Acetabular Impingement? Patient Guide into Joint Preservation Normal Hip Joint The hip joint, also known as a ball and socket joint is located where the femur (the thigh bone) meets the
A patient s s guide to: Arthroscopy of the Hip
 A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
Syndesmosis Injuries
 Syndesmosis Injuries Dr. Alex Rabinovich Outline Anatomy Injury types and classification Treatment options Nonoperative vs. Operative Indications for operative Operative technique Postoperative management
Syndesmosis Injuries Dr. Alex Rabinovich Outline Anatomy Injury types and classification Treatment options Nonoperative vs. Operative Indications for operative Operative technique Postoperative management
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Arthroscopic Shoulder Procedures. David C. Neuschwander MD. Shoulder Instability. Allegheny Health Network Orthopedic Associates of Pittsburgh
 Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
HIP ARTHROSCOPY : PATIENT INFORMATION
 !! HIP ARTHROSCOPY : PATIENT INFORMATION Contents Diagram of a labral tear 2 Operative technique 4 Operating time 6 Complications 6 After hip arthroscopy 7 Further reading : Femoro-Acetabular Impingement
!! HIP ARTHROSCOPY : PATIENT INFORMATION Contents Diagram of a labral tear 2 Operative technique 4 Operating time 6 Complications 6 After hip arthroscopy 7 Further reading : Femoro-Acetabular Impingement
NETWORK FITNESS FACTS THE HIP
 NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
ULTRASONOGRAPHIC EVALUATION OF HIP DYSPLASIA: review. L. Breysem, MD DEPARTMENT OF RADIOLOGY
 ULTRASONOGRAPHIC EVALUATION OF HIP DYSPLASIA: review L. Breysem, MD DEPARTMENT OF RADIOLOGY INTRODUCTION Clinical hip examination is part of the first routine examination of every newborn. An abnormal
ULTRASONOGRAPHIC EVALUATION OF HIP DYSPLASIA: review L. Breysem, MD DEPARTMENT OF RADIOLOGY INTRODUCTION Clinical hip examination is part of the first routine examination of every newborn. An abnormal
Goals of Post-operative operative Rehab. Surgical Procedures. Phase 1 Maximum protection and Mobility (1-4 weeks)
 Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
The Ankle Sprain That Won t Get Better. By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the
 The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
POSTERIOR LABRAL (BANKART) REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Thoracolumbar Spine Fractures. Outline. Outline. Holmes Criteria. Disclosure:
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Semmelweis University Department of Traumatology Dr. Gál Tamás
 Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
Slipped Capital Femoral Epiphysis, Emergency? Scott Ferry, MD Rockford Orthopedic Associates November 10 th, 2012
 Slipped Capital Femoral Epiphysis, Emergency? Scott Ferry, MD Rockford Orthopedic Associates November 10 th, 2012 AAOS-POSNA 2011 Course AAOS/POSNA Five Pediatric Orthopaedic Problems that Should Get You
Slipped Capital Femoral Epiphysis, Emergency? Scott Ferry, MD Rockford Orthopedic Associates November 10 th, 2012 AAOS-POSNA 2011 Course AAOS/POSNA Five Pediatric Orthopaedic Problems that Should Get You
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
SCIENTIFIC PAPER Anterior Dislocation Following Primary Total Hip Replacement by the Posterior Approach Aetiology and Treatment
 Hong HKJOS Kong Journal of Orthopaedic Surgery 2003;7(1):14-18. SCIENTIFIC PAPER Anterior Dislocation Following Primary Total Hip Replacement by the Posterior Approach Aetiology and Treatment Ng TP, Yau
Hong HKJOS Kong Journal of Orthopaedic Surgery 2003;7(1):14-18. SCIENTIFIC PAPER Anterior Dislocation Following Primary Total Hip Replacement by the Posterior Approach Aetiology and Treatment Ng TP, Yau
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Objectives. Spinal Fractures: Classification Diagnosis and Treatment. Level of Fracture. Neuro exam Muscle Grading
 Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital
 By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
Standard of Care: Tibial Plateau Fracture
 Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: ICD-9: 823.00 - fracture of proximal tibia Tibial plateau fractures can occur as a result of high-energy trauma or in low-energy
Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: ICD-9: 823.00 - fracture of proximal tibia Tibial plateau fractures can occur as a result of high-energy trauma or in low-energy
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the
 Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Distal Radius Fractures. Lee W Hash, MD Affinity Orthopedics and Sports Medicine
 Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
SCAPULAR FRACTURES. Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading.
 SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Surgical Technique. Struan H Coleman MD, PhD
 Surgical Technique Guide Struan H Coleman MD, PhD the Author Struan H. Coleman MD, PhD, specializes in Sports Medicine at Hospital for Special Surgery where he treats orthopedic conditions of the shoulder,
Surgical Technique Guide Struan H Coleman MD, PhD the Author Struan H. Coleman MD, PhD, specializes in Sports Medicine at Hospital for Special Surgery where he treats orthopedic conditions of the shoulder,
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT
 1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Common Pediatric Fractures. Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014
 Common Pediatric Fractures Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014 Pediatric fractures 20% of injured kids found to have fracture on evaluation Between birth and
Common Pediatric Fractures Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014 Pediatric fractures 20% of injured kids found to have fracture on evaluation Between birth and
DIAGNOSING SCAPHOID FRACTURES. Anthony Hewitt
 DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
Rehabilitation Guidelines For SLAP Lesion Repair
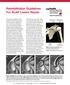 Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Hip Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
MET: Posterior (backward) Rotation of the Innominate Bone.
 MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
Instability concept. Symposium- Cervical Spine. Barcelona, February 2014
 Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Commonly Missed Fractures in the Emergency Department
 Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
(in: Skeletal Radiology - Vol. 30, n. 3 - March 2001)
 ACUTE AVULSION FRACTURES OF THE PELVIS IN ADOLESCENT COMPETITIVE ATHLETES: PREVALENCE, LOCATION AND SPORTS DISTRIBUTION OF 203 CASES COLLECTED Folco Rossi - Stefano Dragoni (in: Skeletal Radiology - Vol.
ACUTE AVULSION FRACTURES OF THE PELVIS IN ADOLESCENT COMPETITIVE ATHLETES: PREVALENCE, LOCATION AND SPORTS DISTRIBUTION OF 203 CASES COLLECTED Folco Rossi - Stefano Dragoni (in: Skeletal Radiology - Vol.
Rehabilitation of Hip Injuries in Athletes
 Rehabilitation of Hip Injuries in Athletes Kevin E Wilk, PT, DPT Hip injuries are somewhat common in sports & daily activities Hip injuries less common than other joints More difficult to identify than
Rehabilitation of Hip Injuries in Athletes Kevin E Wilk, PT, DPT Hip injuries are somewhat common in sports & daily activities Hip injuries less common than other joints More difficult to identify than
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior
 Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Dr. Benjamin Hewitt. Shoulder Stabilisation
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Patellofemoral Joint: Superior Glide of the Patella
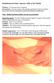 Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
How To Treat A Patella Dislocation
 Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior
 Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Toe fractures are one of the most
 Evaluation and Management of Toe Fractures ROBERT L. HATCH, M.D., M.P.H., and SCOTT HACKING, M.D., University of Florida College of Medicine, Gainesville, Florida Fractures of the toe are one of the most
Evaluation and Management of Toe Fractures ROBERT L. HATCH, M.D., M.P.H., and SCOTT HACKING, M.D., University of Florida College of Medicine, Gainesville, Florida Fractures of the toe are one of the most
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
On Cervical Zygapophysial Joint Pain After Whiplash. Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199
 On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Chapter 9 The Hip Joint and Pelvic Girdle
 Chapter 9 The Hip Joint and Pelvic Girdle Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Hip relatively joint (acetabularfemoral) functions bony strong large stable due to The enhanced architecture
Chapter 9 The Hip Joint and Pelvic Girdle Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Hip relatively joint (acetabularfemoral) functions bony strong large stable due to The enhanced architecture
