Standard of Care: Ankylosing Spondylitis
|
|
|
- Deborah James
- 8 years ago
- Views:
Transcription
1 Department of Rehabilitation Services Physical Therapy Diagnosis: Ankylosing Spondylitis also known as Marie-Strumpell disease or Bechterew s disease. (ICD-9: 720.0) Ankylosing Spondylitis (AS) is an inflammatory rheumatic disease, which primarily affects the axial skeleton manifesting in chronic back pain and spinal stiffness 1. The onset of the disease is gradual and characterized by aseptic inflammation at the sacroiliac (SI) joints. As the disease progresses it moves cephalad up the vertebral column. In advanced cases the stiffness progresses into spinal fusion and the normal lumbar lordosis is flattened and the thoracic kyphosis becomes exaggerated. Due to costovertebral involvement chest expansion can also become limited. It is not uncommon to also find peripheral joints that are affected in 25% of the cases primarily involving the hips, knees, and shoulders. Acute anterior uveitis is also a common finding in 20-25% of patients with AS. Acute anterior uveitis may be a precursor to disease onset up to a few years prior. It presents as pain, photophobia, and increased lacrimation in the eye. In 5-10% of AS cases atrioventricular conduction defects, aortic insufficiency, and/or ascending aortitis will occur and is associated with spondylitic heart disease 2,3. AS is prevalent in approximately 0.1% of the general population and affects men greater than women with a 2-3:1 ratio 4,5. AS is found worldwide but is more prevalent in Caucasians. A collection of laboratory findings can assist in the diagnosis of AS. The Erythrocyte sedimentation rate (ESR) will be elevated in 85% of the cases. C-reactive protein (CRP) is often elevated. Both are markers of inflammation. Human leukocyte antigen (HLA)-B27 is correlated with 90% of Caucasian patients and 50% of black patients with AS 2. The earliest radiographic changes will be seen on x-rays of the sacroiliac joints with symmetrical blurring of the cortical margins or postage stamp serrated erosions in the lower third of the SI joints. Magnetic resonance imaging (MRI) and computed tomography (CT) can detect earlier stages of the disease and detect inflammation of the SI joints before plain radiographs 3. Radiographically this appears as squaring off of the vertebrae 6. Eventually, in the late stages of the disease x-rays demonstrating intervertebral fusion are known by the term bamboo spine due to their appearance 6. The etiology of AS is currently unclear, but it appears to be entirely genetic and immune system mediated. The enthesis or site of ligamentous attachment to bone is implicated as the primary site of pathology in the SI joints and the spine in AS. The enthesitis is associated with local bone marrow edema and eventually bone erosions occur. The erosions are replaced by fibrocartilage and eventually ossification occurs. In the spine, syndesmophytes form from the outer annular portion of the intervertebral disc. Eventually these syndesmophytes grow vertically across the 1
2 margin of the vertebral disc and bridge the adjacent vertebrae. This process is repeated up the spine 6. The pain is multifactorial in origin but is likely due to sacroiliitis, spondylitis, the formation of syndesmophytes leading to ankylosis, and is frequently associated with peripheral arthritis, enthesitis, and acute anterior uveitis 1 The diagnosis of AS is made based upon the modified New York Criteria 7 A. Diagnosis 1. Clinical criteria a. Low back pain and stiffness for more than 3 months which improves with exercise, but is not relieved by rest. b. Limitation of motion of the lumbar spine in both the sagital and frontal planes. c. Limitation of chest expansion relative to normal values corrected for age and sex. (<5cm=Abnormal in young adult) 2. Radiologic criterion of sacroiliitis grade greater than or equal to 2 bilaterally or sacroiliitis grade 3-4 unilaterally. Grades are as follows a. 0 = normal b. 1 = suspicious changes c. 2 = minimum abnormality (small localized areas with erosions or sclerosis) d. 3 = unequivocal abnormality (moderate or advanced sacroiliitis with erosions, evidence of sclerosis, widening, narrowing or partial ankylosis) e. 4 = severe abnormality (total ankylosis) B. Grading 1. Definite ankylosing spondylitis diagnosis if the radiologic criterion is associated with at least 1 clinical criterion. 2. Probable ankylosing spondylitis if: a. Three clinical criteria are present. b. The radiologic criterion is present without any signs or symptoms satisfying the clinical criteria. (Other causes of sacroiliitis should be considered.) Indications for Treatment: Patients typically present in physical therapy with impairments of pain, loss of function, weakness and loss of muscle performance, fatigue, loss of flexibility and range of motion (ROM), and a knowledge deficit in self-management of symptoms and the nature of the disease process. 2
3 Contraindications / Precautions for Treatment: A fused osteopenic spine is at great risk for fracture and the practitioner should use extreme caution when attempting to mobilize an AS spine 3. From the 1920 s until the last few decades AS was treated effectively with spinal radiation. These patients carry a higher risk of cancer such as myeloid leukemias and hematologic malignancies. All AS patients should be asked if they have undergone this treatment 3. Examination: Medical History: Patients may report a history of acute anterior uveitis, diffuse pain in the lower back or SI joints described as deep and dull. They may report a history of morning stiffness, which improves with exercise. All results of imaging studies should be reported. History of Present Illness: What symptoms are they having? How long have the symptoms been present? What mitigates or ameliorates symptoms? What worsens symptoms? Most patients complain of pain, stiffness, decreased spinal movement, and reduced energy. Were the symptoms insidious in onset? A careful and detailed history can be quite revealing and may prove useful when coupled with objective clinical information and imaging studies. Social History: Suggested interview questions may include Does patient live alone? Level of activity? Difficulty with ADLs? Frequency of exercise? Does the patient work? What behaviors have already been modified in order to accommodate the level of symptoms? What recreational activities would the patient like to do that currently is intolerable? What is/are the patient s goal(s)? Medications: Non-steroidal anti-inflammatory drugs (NSAIDs) appear to be effective with Indomethacin being the most effective. Sulfasalazine is useful for peripheral arthritis but not axial 2. Anti-tumor necrosis factor (TNF) such as Infliximab or Etanercept has been extremely successful and show a 60% reduction in the Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) 6. In 2005 the ASsessment in AS (ASAS) International Working Group collaborated with the European League Against Rheumatism (EULAR) and compiled a group of evidence based medical recommendations for treatment of AS 8. 3
4 Optimal management of AS requires a combination of non-pharmacological and pharmacological treatments. NSAIDs are recommended as first line drug treatment for patients with AS with pain and stiffness. In those with increased GI risk, non-selective NSAIDs plus a gastroprotective agent, or a selective COX-2 inhibitor could be used. NSAIDS are insufficient, contraindicated, and/or poorly tolerated, however, analgesics, such as acetaminophen and opiods, might be considered for pain control. Corticosteroid injections directed to the local side of musculoskeletal inflammation may be considered. The use of systemic corticosteroids is not supported by evidence. There is no evidence for the efficacy of disease modifying anti-rheumatic drugs (DMARDs), including sulfasalazine and methotrexate, for the treatment of axial disease. Anti-TNF treatment should be given to patients with persistently high disease activity despite conventional treatments according to the ASAS recommendations. There is no evidence to support the obligatory use of DMARDs before, or concomitant with, anti-tnf treatment in patients with axial disease. Examination: (Physical / Cognitive / applicable tests and measures / other) This section is intended to capture the minimum data set and identify specific circumstance(s) that might require additional tests and measures. Pain: Visual Analog Scale (VAS). Locus and nature of complaints, pattern am vs. pm, rest vs. activity. Patients may complain of waking from sleep and having to walk to relieve night pain, which is a rare complaint of mechanical low back pain 3. Muscle Performance: Perform specific manual muscle testing depending upon findings of upper and lower quadrant screening and patient s subjective reports of weakness. Gait: Evaluate gait pattern and independence. Assess stair negotiation. Neurological: Note the findings of deep tendon reflexes, sensory changes and/or muscle weakness. Assess reported numbness and/or paraesthesias. Note the locus of symptoms (dermatomal distribution) and level of severity associated with the defined level of activity. The most common neurological compromise is secondary to spinal fracture and neurological compromise affects one third of these cases. In patients with advanced AS, cauda equina syndrome can develop 3. Inspection/Posture: In cases of advanced disease a marked loss of the normal lumbar lordosis and a marked increase of the normal thoracic kyphosis may be seen. Balance: According to Murray et al 9 poor posture, decreased ROM and pain lead to a significant number of AS patients having impaired balance with eyes open or closed. 4
5 The Berg balance test may be administered for objective measurement of balance impairment. Function: The BASDAI 10, 11 (see appendix A) has established content validity and has been used as an index to evaluate patients on a visual analog scale (0-10) quantifying: Fatigue Axial pain Peripheral pain Stiffness Enthesopathy Palpation: Maneuvers or direct pressure over the SI joints can be used to stress the SI joints 6. ROM: A lack of spinal mobility is the hallmark of AS. All planes should be measured for active and passive ROM of the spine, shoulders, hips, knees and ankles as appropriate. Special Tests: Cervical Rotation (CROT): distance between tip of nose and the acromioclavicular joint in neutral and maximal ipsilateral rotation. The difference between the two positions is calculated for right and left rotation. Smaller differences indicate a more restricted range of motion. Measured with a tape measure 12. Tragus-to-wall distance (TWD): measures the horizontal distance between the right tragus and the wall, standing with the heels and buttocks against the wall, knees extended and chin tucked in. The large the distance indicates worse spinal/upper cervical posture. Measured with a tape measure. This distance has been correlated with radiographic change in the cervical spine 12. Fingertip-to-Floor distance (FFD): measures the distance between the tip of the right middle finger and the floor following maximal lumbar flexion, while maintaining heel contact with the floor and without trunk rotation. A smaller distance indicates greater movement. Measured with a tape measure 12. Modified Schober index (MSI): is a useful measure of lumbar spine flexion. The patient stands erect, with heels together, and marks are made directly over the spine 5 cm below and 10 cm above the lumbosacral junction (identified by a horizontal line between the posterosuperior iliac spines.) The patient then bends forward maximally, and the distance between the two marks is measured. The distance between the two marks increases by greater than or equal to 5 cm in the case of normal mobility and by <4cm in the case of decreased mobility. Measured with a tape measure 12. 5
6 Lumbar Lateral Flexion (LLF): distance between the tip of the ipsilateral middle finger and the floor following maximal LLF maintaining heel contact with the floor and without trunk rotation. Smaller distance indicates greater movement. Measured with a tape measure 12. The literature suggests a strong correlation between the Modified Schober Index and the measurement of Lumbar Lateral Flexion (LLF) and AS specific lumbar spine radiographic changes 12. Chest expansion is measured as the difference between maximal inspiration and maximal forced expiration in the fourth intercostals space in males or just below the breasts in females. Normal chest expansion is greater than or equal to 5 cm and any measurement less indicates impairment. Assess for limitation of motion in the hips or shoulders 6. Due to restriction in the chest wall pulmonary function can suffer minor impairment with slight reduction in vital lung capacity, total lung capacity, and normal diffusion capacity 3. The CROT and/or the FFD are recommended for use in measuring reversible short-term change in spinal mobility. The MSI is recommended for use in measuring long-term irreversible change in spinal mobility. The ASAS recommends that chest expansion, MSI, and occiput (tragus)-to-wall be used to measure change in spinal mobility. After study and structured review of the literature Haywood et al recommends the use of the MSI, CROT and FFD for measurement of spinal mobility in AS 12. Differential Diagnosis: Sacroiliits can be present in the following disease processes 3 Hyperparathyroidism: if prolonged (can be induced by hemodialysis) Familial Mediterranean fever: can create sacroiliac erosions. Whipple disease: can create sacroiliac erosions. Paget s disease: can create sacroiliac erosions. Paraplegia: rarely can create sacroiliac erosions. Bechet disease: debatable. Tuberculosis: has an affinity for settling in the SI joints. Brucellosis: has an affinity for settling in the SI joints. Pyogenic sacroiliitis Malignancy: rare Retinoid treatment Synovitis-acne-pustulosis-hyperostosis-osteitis (SAPHO) syndrome Vertebral hyperostosis can be present in the following disease processes 3 Ankylosing hyperostosis or diffuse idiopathic skeletal hyperostosis (DISH): 6
7 there exists exuberant osteophyte formation but they are more anterior. The SI joints are not affected and they do not have inflammatory back pain 2. Ochronosis SAPHO syndrome Retinoid treatment Enthesopathy can be present in the following disease processes 3 Gout Disseminated gonococcal infection SAPHO syndrome Retinoid treatment Bacillus Calmette-Guerin (BCG)-induced Other related disease processes. Degenerative joint disease Rheumatoid arthritis: primarily affects multiple small peripheral joints. RA spares the SI joints and the majority of the spine except C1-C2. Pt s with RA usually have a positive rheumatoid factor present of lab results 2. Osteitis condensans ilii Chondrocalcinosis Gout Evaluation / Assessment: Establish Diagnosis and Need for Skilled Services Problem List (Identify Impairment(s) and/ or dysfunction(s)) Knowledge deficit re: understanding of diagnosis, relationship of posture and upright activity on symptoms, correct use of joint protection techniques, modification(s) of activity level, proper positioning and stretching techniques, use of assistive device(s) and posture cues, and use of cold/ heat, massage and other comfort measures. Pain - management with conservative measures of positioning, pacing and/ or modification of functional activities, therapeutic exercise, and conditioning activities. Impaired muscle performance Impaired function. Impaired ROM (active and/or passive restrictions) Prognosis Some studies show that onset of the disease in adolescence correlates with a worse prognosis and early severe hip involvement is an indication of progressive disease. The disease in women tends to progress less frequently to total spinal ankylosis, however, there is evidence of isolated 7
8 cervical ankylosis and peripheral arthritis 6. The extent of spinal involvement has a direct correlation with the patients functional status 3. Goals (with measurable parameters and with specific timelines) Independent home program and avoidance of provoking postures and activities; progressive independence in advancing home program over 6-8 treatments. Independent pain management with proper use of joint protection methods including posture, positioning, use of assistive device(s), pacing of activities, modification of activities, body mechanics and, use of comfort measures as needed (heat, ice, massage, relaxation techniques); 4-6 treatments Improve function including safe and proper transfers and ambulation with or without ambulatory device(s) and/or frequency or distance of walking; 2-4 treatments. Improve muscle performance; progressive improvement in quality of performance, number and nature of exercises, MMT and/or number of repetitions tolerated over 6-8 treatments Improve flexibility of identified tight soft tissue structures; measurable decrease per particular measures over 6-8 treatments. E.g. 25% decrease in hip flexor tightness as measured by the Thomas Test. Improve level of fitness; patient to return to conditioning activities or recreational activities. 6-8 treatments To maintain the patient s maximal potential movement, prevent postural deformities, improve muscle strength and fitness, and relieve pain 5. Age Specific Considerations: The average age of diagnosis is 24 and the median age is 23. The most active disease phase occurs between the ages of 20 and 50 years 5. Diagnosis after the age of 40 is uncommon 3. Treatment Planning / Interventions Established Pathway Yes, see attached. X No Established Protocol Yes, see attached. X No Interventions most commonly used for this case type/diagnosis. This section is intended to capture the most commonly used interventions for this case type/diagnosis. It is not intended to be either inclusive or exclusive of appropriate interventions. Joint Protection Techniques: Body mechanics for transfers, lifting and carrying methods, positioning techniques, posture awareness and cues for maintaining pelvis in 8
9 neutral, pacing and planning activities, modifications of activities, use of assistive device(s). Therapeutic exercises: A progressive therapeutic exercise program with extension bias, stretching of identified tight muscles; lumbar and lower extremity stabilization exercise techniques; strengthening of any identified muscle weaknesses; postural reeducation, conditioning activities (recumbent bike, stationary bike, walking program, treadmill use), return to recreational sport activities (for example, swimming with use of modified stokes to avoid trunk extension). Breathing exercises and postural exercises should also be incorporated 2. Transfer and gait training: Balance, safety, pacing of cadence and planning for distance tolerated. Appropriate assessment for and use of any assistive device(s) should be addressed. Consider the use of 1 or 2 canes or a rolling walker for patients who require an assistive device(s). Some patients may benefit from a specialized walker with a seat option. Consider adjusting the height of the assistive device just slightly lower than usual to help patient achieve the postural correction needed for symptom management. Manual therapy: Soft tissue and joint mobilization techniques to improve patient s level of symptoms and/or mobility. It may be inferred general fitness exercises will not isolate specific spinal segments that need to be mobilized. Manual treatments specifically designed to target a portion of the column are required 5. The effects of different hands-on techniques such as manual therapy, electrotherapy, and information on education programs need to be studied further with regard to patients suffering from AS. Exercise Considerations: Studies show that patients with AS had some short term beneficial effects on function from individualized home exercise programs, but supervised group physical therapy programs were better than an individualized home exercise program (HEP). It has also been shown that patients who participated in group exercise (inpatient and outpatient) improved more than individual HEP due to nonphysical factors such as mutual encouragement, increased motivation, and exchange of experiences with fellow sufferers of AS 5. When group exercise is combined with a three week thermal hydrotherapy, or spa treatment the intervention was better than weekly group physical therapy alone 1.. Frequency & Duration: 6-8 treatments to achieve identified short-term goals over an 8 week period. Patients with lower tolerance levels may require more intensive intervention. Patient / family education: It has been found that educating and advising patients about their condition is important because it enables the patients to manage their disease more effectively and know when to seek assistance at the appropriate time. It has been shown 9
10 that education improves motivation and reduces anxiety 1. The patient should understand the diagnosis and related basic anatomy, joint protection techniques including posture awareness, activity modifications, body mechanics, proper positioning and stretching techniques, use of assistive device(s) and heat/cold, relaxation techniques or massage. Recommendations and referrals to other providers: 1. Occupational therapy- especially for ADL and additional training in joint protection methods if pain symptoms, loss of function and health status limit patient s independence and ease of function. Discuss with referring physician and explain your recommendations to the patient. 2. Additional support system/ counseling if patient has difficulty coping with the loss of independence and needs to modify activity level. Discuss with referring physician. 3. A referral will need to be made to an orthopedic surgeon if spinal alignment correction is needed to improve gait or field of vision. Typically this requires a large procedure involving a lumbar osteotomy 3. In 5% of cases, patients with AS will require a hip replacement. These patients have an increased risk of peri-implant heterotopic ossification 3.Referral to an orthopedic surgeon to perform total hip arthroplasty should be considered in patients with refractory pain or disability and radiographic evidence of structural damage, regardless of age 1. If vertebral fracture is suspected the patient should be immediately immobilized and treated with emergency medical management 3. Referrals can be made for inta-articular corticosteroid injections to manage sacroiliitis 8. Re-evaluation / assessment Standard Time Frame: every 30 days. Other Possible Triggers: Worsening symptoms despite adhering to recommendations. Discharge Planning Commonly expected outcomes at discharge: Independence in home program of body mechanics, pain management with conservative measures, a routine stretching and strengthening program and independence in walking with or without an assistive device(s). According to Dr. Annelies Boonen the total cost-of-illness was $6,720 per AS patient per year. Person s older in age at the onset of disease, performing manual jobs, having a lower educational level, or poor coping mechanisms are associated with withdrawal from the work force 13. Patient s discharge instructions: Continue prescribed home program. 10
11 Appendix A The Bath Ankylosing Spondylitis Disease Activity Index. 11
12 References 1. Zochling J, van der Heijde D, Burgos-Vargas R, et al. ASAS/EULAR recommendations for the management of ankylosing spondylitis. Ann Rheum Dis Tierney LM, McPhee, Stephen J., Jr., Papadikis MA, Gonzales R, Zeiger R. Seronegative spondyloarthropathies. In: Current Medical Diagnosis & Treatment Vol Musculoskeletal Disorders. 45th edition ed. United States of America: The McGraw-Hill Companies, Inc; Imboden J, Hellmann DB, Stone JH. Section II rheumatoid arthritis & spondyloarthropathies. In: Current Rheumatology Diagnosis & Treatment. Vol Chapter 18: Spondyloarthropathies. 1st ed. United States of America: The McGraw-Hill Companies, Inc.; Gran JT, Husby G. The epidemiology of ankylosing spondylitis. Semin Arthritis Rheum. 1993;22: Dagfinrud H, Kvien TK, Hagen KB. The Cochrane review of physiotherapy interventions for ankylosing spondylitis. J Rheumatol. 2005;32: Kasper DL, Braunwald E, Fauci AS, et al. Disorders of immune-mediated injury. In: Harrison's Principles of Internal Medicine. Vol Part 13 Disorders of the Immune System, Connective Tissue, and Joints. 16th edition ed. United States of America: The McGraw-Hill Companies, Inc.; : Chapter van der Linden S, Valkenburg HA, Cats A. Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum. 1984;27: Zochling J, van der Heijde D, Dougados M, Braun J. Current evidence for the management of ankylosing spondylitis a systematic literature review for the asas/eular management recommendations in ankylosing spondylitis. Ann Rheum Dis Murray HC, Elliott C, Barton SE, Murray A. Do patients with ankylosing spondylitis have poorer balance than normal subjects? Rheumatology (Oxford). 2000;39: Garrett S, Jenkinson T, Kennedy LG, Whitelock H, Gaisford P, Calin A. A new approach to defining disease status in ankylosing spondylitis: The bath ankylosing spondylitis disease activity index. J Rheumatol. 1994;21: Calin A, Nakache JP, Gueguen A, Zeidler H, Mielants H, Dougados M. Defining disease activity in ankylosing spondylitis: Is a combination of variables (bath ankylosing spondylitis disease activity index) an appropriate instrument? Rheumatology (Oxford). 1999;38:
13 12. Haywood KL, Garratt AM, Jordan K, Dziedzic K, Dawes PT. Spinal mobility in ankylosing spondylitis: Reliability, validity and responsiveness. Rheumatology (Oxford). 2004;43: Boonen A. Socioeconomic consequences of ankylosing spondylitis. Clin Exp Rheumatol. 2002;20:S23-6. Author: Reviewers: Kenneth Shannon 1/06 Ethan Jerome 4/06 Marie Weafer-Hodgins 5/06 Sharon Alzner 6/06 13
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Low Back Pain Protocols
 Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security *14.09 Inflammatory arthritis. As described in 14.00D6. With: A. Persistent inflammation or persistent deformity of: 1. One or more major peripheral weight-bearing
Disability Evaluation Under Social Security *14.09 Inflammatory arthritis. As described in 14.00D6. With: A. Persistent inflammation or persistent deformity of: 1. One or more major peripheral weight-bearing
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
NURS 821 Alterations in the Musculoskeletal System. Rheumatoid Arthritis. Type III Hypersensitivity Response
 NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Response to Public Comments From the Core Leadership Team for the ACR/SPARTAN/SAA Axial SpA Guideline Development Project July 2013
 We thank members of the rheumatology community for their interest in the proposed treatment recommendations for patients with axial spondyloarthritis (axspa) including ankylosing spondylitis (AS). In general,
We thank members of the rheumatology community for their interest in the proposed treatment recommendations for patients with axial spondyloarthritis (axspa) including ankylosing spondylitis (AS). In general,
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis
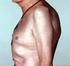 Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Once the immune system is triggered, cells migrate from the blood into the joints and produce substances that cause inflammation.
 HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
DIFFERENTIATING INFLAMMATORY AND MECHANICAL BACK PAIN
 DIFFERENTIATING INFLAMMATORY AND MECHANICAL BACK PAIN CHALLENGE YOUR DECISION MAKING Claire Harris, Senior Physiotherapist, The North West London Hospitals NHS Trust Susan Gurden, Advanced Physiotherapy
DIFFERENTIATING INFLAMMATORY AND MECHANICAL BACK PAIN CHALLENGE YOUR DECISION MAKING Claire Harris, Senior Physiotherapist, The North West London Hospitals NHS Trust Susan Gurden, Advanced Physiotherapy
RECOGNISING INFLAMMATORY BACK PAIN. This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248
 RECOGNISING INFLAMMATORY BACK PAIN This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248 Contents Inflammatory back pain: overview Spondyloarthropathies
RECOGNISING INFLAMMATORY BACK PAIN This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248 Contents Inflammatory back pain: overview Spondyloarthropathies
Practice Guidelines For Low Back Pain
 Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
New York State Workers' Comp Board. Mid and Lower Back Treatment Guidelines. Summary From 1st Edition, June 30, 2010. Effective December 1, 2010
 New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
What s new in clinical assesment of ankylosing spondylitis?
 What s new in clinical assesment of ankylosing spondylitis? Désirée van der Heijde Professor of Rheumatology Leiden University Medical Center, the Netherlands Diakonhjemmet Hospital, Oslo, Norway Content
What s new in clinical assesment of ankylosing spondylitis? Désirée van der Heijde Professor of Rheumatology Leiden University Medical Center, the Netherlands Diakonhjemmet Hospital, Oslo, Norway Content
Stickler Syndrome and Arthritis
 Stickler Syndrome and Arthritis Arthritis Foundation Pacific Region, Nevada Office Presented by: Crystal Schulz, MPH Community Development Manager Arthritis Foundation Improving lives through leadership
Stickler Syndrome and Arthritis Arthritis Foundation Pacific Region, Nevada Office Presented by: Crystal Schulz, MPH Community Development Manager Arthritis Foundation Improving lives through leadership
Psoriatic Arthritis www.arthritis.org.nz
 Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Rheumatoid Arthritis. Nicole Klett,, M.D.
 Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
X-Plain Rheumatoid Arthritis Reference Summary
 X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
BACK PAIN: WHAT YOU SHOULD KNOW
 BACK PAIN: WHAT YOU SHOULD KNOW Diane Metzer LOWER BACK PAIN Nearly everyone at some point has back pain that interferes with work, recreation and routine daily activities. Four out of five adults experience
BACK PAIN: WHAT YOU SHOULD KNOW Diane Metzer LOWER BACK PAIN Nearly everyone at some point has back pain that interferes with work, recreation and routine daily activities. Four out of five adults experience
Injury Prevention for the Back and Neck
 Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Do I need a physician referral? Yes, we see patients on referral from a health care provider.
 FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
Arthritis in Children: Juvenile Rheumatoid Arthritis By Kerry V. Cooke
 Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
How To Choose A Biologic Drug
 North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
Spine University s Guide to Transient Osteoporosis
 Spine University s Guide to Transient Osteoporosis 2 Introduction The word osteoporosis scares many people because they ve heard about brittle bone disease. They may know someone who has had it or seen
Spine University s Guide to Transient Osteoporosis 2 Introduction The word osteoporosis scares many people because they ve heard about brittle bone disease. They may know someone who has had it or seen
Patient Guide. Sacroiliac Joint Pain
 Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
First Year. PT7040- Clinical Skills and Examination II
 First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Arthritis and Rheumatology Clinics of Kansas Patient Education. Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis
 Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Psoriatic Arthritis. Title. Understanding and Managing. in All the Wrong Places. Clinical Features. Etiology of Psoriatic Arthritis
 Focus on CME at Memorial University Understanding and Managing Title Psoriatic Arthritis in All the Wrong Places Proton Rahman MD, MSc, FRCPC Although Baron Jean-Luis Aubert offered the first case description
Focus on CME at Memorial University Understanding and Managing Title Psoriatic Arthritis in All the Wrong Places Proton Rahman MD, MSc, FRCPC Although Baron Jean-Luis Aubert offered the first case description
There are four main regions of the back; the cervical (C), thoracic (T), lumbar (L), and sacral (S) regions
 Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Rheumatoid Arthritis Information
 Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS
 ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
Rheumatoid Arthritis
 Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Information on Rheumatoid Arthritis
 Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Spine University s Guide to Kinetic MRIs Detect Disc Herniations
 Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Osteoporosis and Arthritis: Two Common but Different Conditions
 and : Two Common but Different Conditions National Institutes of Health and Related Bone Diseases ~ National Resource Center 2 AMS Circle Bethesda, MD 20892 3676 Tel: 800 624 BONE or 202 223 0344 Fax:
and : Two Common but Different Conditions National Institutes of Health and Related Bone Diseases ~ National Resource Center 2 AMS Circle Bethesda, MD 20892 3676 Tel: 800 624 BONE or 202 223 0344 Fax:
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B
 1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES
 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
Rehabilitation Documentation and Proper Coding Guidelines
 Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Arthritis of the Spine
 Arthritis of the Spine Runsheng Wang and Michael M. Ward Abstract Arthritis is the common term used to describe pathological changes of joints and adjoining parts of the bone. Several types of arthritis
Arthritis of the Spine Runsheng Wang and Michael M. Ward Abstract Arthritis is the common term used to describe pathological changes of joints and adjoining parts of the bone. Several types of arthritis
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
July 2012 Exercise Away Your Knee Pain It seems counterintuitive, but when it hurts to move
 Exercise Away Your Knee Pain It seems counterintuitive, but when it hurts to move your knee, the best thing you can do is move your knee. A 2009 study in the British Medical Journal found that supervised
Exercise Away Your Knee Pain It seems counterintuitive, but when it hurts to move your knee, the best thing you can do is move your knee. A 2009 study in the British Medical Journal found that supervised
ABOUT RHEUMATOID ARTHRITIS
 MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
Polymyalgia Rheumatica www.arthritis.org.nz
 Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic
 Cox Technic Email Case #77 October 2009 by Dr. Greenwood 1 Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic A case study presented to the Part III Hospital Based Training Course for Cox
Cox Technic Email Case #77 October 2009 by Dr. Greenwood 1 Large L5 S1 Disc Protrusion Treated Successfully With Cox Technic A case study presented to the Part III Hospital Based Training Course for Cox
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Diagnostic Imaging Exams
 Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Body Mechanics for Mammography Technologists
 Body Mechanics for Mammography Technologists Diane Rinella RT(R)(M)(BD)RDMS(BR)CDT Objectives Recognize causes and risk factors for Musculoskeletal Disorders (MSDs) for mammography technologists Understand
Body Mechanics for Mammography Technologists Diane Rinella RT(R)(M)(BD)RDMS(BR)CDT Objectives Recognize causes and risk factors for Musculoskeletal Disorders (MSDs) for mammography technologists Understand
 Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
Therapeutic Canine Massage
 Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
CERVICAL SPONDYLOSIS
 CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
Refer to Specialist. The Diagnosis and Management of Shoulder Pain 1. SLAP lesions, types 1 through 4
 The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency London, 14 December 2006 Doc. Ref. CHMP/EWP/438/04 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL INVESTIGATION OF MEDICINAL PRODUCTS FOR THE TREATMENT
European Medicines Agency London, 14 December 2006 Doc. Ref. CHMP/EWP/438/04 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL INVESTIGATION OF MEDICINAL PRODUCTS FOR THE TREATMENT
Treatment of Young Athletes with Spine Injuries
 Treatment of Young Athletes with Spine Injuries North American Spine Society Public Education Series Treatment of the Young Athlete Although not common, low back injuries can occur in young athletes who
Treatment of Young Athletes with Spine Injuries North American Spine Society Public Education Series Treatment of the Young Athlete Although not common, low back injuries can occur in young athletes who
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
PILATES Fatigue Posture and the Medical Technology Field
 PILATES Fatigue Posture and the Medical Technology Field Marybeth Kane May 2014 Course: 2014, Pacific Palisades, CA 1 ABSTRACT A medical laboratory scientist (MLS) (also referred to as a medical technologist
PILATES Fatigue Posture and the Medical Technology Field Marybeth Kane May 2014 Course: 2014, Pacific Palisades, CA 1 ABSTRACT A medical laboratory scientist (MLS) (also referred to as a medical technologist
RHEUMATOLOGY ICD-10 CROSSWALK
 RHEUMATOLOGY ICD-10 CROSSWALK ICD is revised periodically and is currently in its tenth edition and will be implemented in the United States on October 1, 2015. There is an annual minor update and three-yearly
RHEUMATOLOGY ICD-10 CROSSWALK ICD is revised periodically and is currently in its tenth edition and will be implemented in the United States on October 1, 2015. There is an annual minor update and three-yearly
How to Get and Keep a Healthy Back. Amy Eisenson, B.S. Exercise Physiologist
 How to Get and Keep a Healthy Back Amy Eisenson, B.S. Exercise Physiologist Lesson Objectives Statistics of Back Pain Anatomy of the Spine Causes of Back Pain Four Work Factors Core Muscles Connection
How to Get and Keep a Healthy Back Amy Eisenson, B.S. Exercise Physiologist Lesson Objectives Statistics of Back Pain Anatomy of the Spine Causes of Back Pain Four Work Factors Core Muscles Connection
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Arthritis www.patientedu.org
 written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Pathophysiology of Acute and Chronic Low Back Pain
 Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Rheumatoid Arthritis. Disease RA Final.indd 2 15. 6. 10. 11:23
 Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
Preventing & Treating Low Back Pain
 Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
