Alterations of Immune Functions in Heroin Addicts and Heroin Withdrawal Subjects 1
|
|
|
- Rosamond McKenzie
- 8 years ago
- Views:
Transcription
1 /98/ $03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 286, No. 2 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in U.S.A. JPET 286: , 1998 Alterations of Immune Functions in Heroin Addicts and Heroin Withdrawal Subjects 1 PIYARAT GOVITRAPONG, TUNDA SUTTITUM, NAIPHINICH KOTCHABHAKDI and THONGCHAI UNEKLABH Neuro-Behavioural Biology Center (P.G., T.S., N.K.), Institute of Science and Technology for Research and Development, Mahidol University at Salaya, Nakornpathom 73170, Thailand and Thanyarak Hospital (T.U.), Department of Medical Services, Ministry of Public Health, Thunyaburi, Pathumthani 12130, Thailand Accepted for publication April 8, 1998 This paper is available online at ABSTRACT Conflicting results, both decreased and increased, have been reported concerning the function of T-lymphocytes in heroin addicts. We investigated the alterations of T-lymphocyte proliferative responses and immunophenotypic markers on lymphoid cells in heroin addicts and during different periods of heroin withdrawal in addicted subjects. This study has demonstrated a decrease in the response of T-lymphocytes to 1.2, 2.5, 5 and 10 g/ml of phytohemagglutinin stimuli in heroin addicts and 1- to 5-day heroin withdrawal subjects compared with controls. Similarly, in an in vitro study, 10 4,10 6 and 10 8 M concentrations of morphine were shown to suppress 0.6 and 2.5 g/ml of PHA-stimulated T-lymphocyte obtained from naive subjects. This inhibitory effect of morphine on PHA stimulation was completely abolished by 100 M naloxone. The immunological parameters of total T-lymphocytes (CD3), T- helper cells (CD4), cytotoxic T-cells (CD8), B-cells and natural killer cells that are the immunophenotypic markers studied by flow cytometric analysis were altered in heroin addicts, 15- to 21-day and 6- to 24-month heroin withdrawal subjects, when compared with controls. These results suggest that heroin addicts and short period (15 to 21 days and 6 to 24 months) of heroin withdrawal have decreases in their immune system functioning and that the heroin withdrawal subjects seem to gradually reverse their immunological parameters to normal levels when withdrawal was sustained 2 years. This is the first report examining immune function in heroin withdrawal subjects using the cold turkey method. The results are beneficial for further study of the mechanism responsible for the opioid-induced changes in immune function. Received for publication December 12, This work was supported by a Mahidol University Research Grant (P.G.) and a Thanyarak Hospital Research Fund (T.U.). Because of the AIDS epidemic, interest in studying the effects of drugs of abuse, especially opiates, on the immune system has increased greatly. This issue is now of paramount importance because of the association of AIDS with intravenous drug abuse. Heroin abusers are a high-risk group for the development of AIDS and HIV infection. Intravenous drug abusers account for 7.3% of the total AIDS cases in Thailand (Wongkhomthong et al., 1995). Indeed, the HIVseropositivity rate among intravenous drug abusers can be even greater, ranging from 5% in certain areas to 75% in others (Curran et al., 1984), and this group is generally regarded as posing the most substantial risk of furthering spread of the disease. Even in the absence of AIDS, increasing evidence indicates that chronic use of opioid drugs can affect the functioning of the immune system. Heroin addicts have an increased susceptibility to a variety of infectious diseases (Louria et al., 1967), and alterations in a wide variety of immune parameters also have been reported among them (for reviews, see Rouveix, 1992; Sibinga and Goldstein, 1988; Carr et al., 1996). A variety of changes in the immune system have been observed, indicative of both decreased and increased functioning in heroin addicts. The absolute number and percentage of total and active T lymphocytes in the peripheral blood of opiate addicts and T-cell rosette formation were significantly depressed (McDonough et al., 1980). In contrast, an increase in the absolute number of T-cells in the blood of heroin addicts who were not malnourished was reported in another study (Heathcote et al., 1981). Similar conflicting results have been reported concerning the functional activity of T lymphocytes from heroin addicts. Brown et al. (1974) found impaired in vitro responsiveness of lymphocytes to each of the three mitogens (PHA, concavanalin A, pokeweed mitogen) in heroin addicts relative to control values. Similarly, a suppressed PHA response in methadone patients was reported (Quagliata et al., 1977); but Reddy et al. (1987) found normal T-proliferative responses to both concavanalin ABBREVIATIONS: PHA, phytohemagglutinin; NK, natural killer; HIV, human immunodeficiency virus; AIDS, acquired immune deficiency syndrome; HPA, hypothalamus-pituitary-adrenal; IL-1, interleukin-1; RPMI, Roswell Park Memorial Institute; DAMGO, [D-Ala 2,MePhe 4, Gly-ol 5 ]enkephalin; HBsAg, hepatitis B antigens. 883
2 884 Govitrapong et al. Vol. 286 A and tetanus toxoid antigen in another group of healthy addicts. Immunophenotypic markers on lymphoid cells in human addicts have been studied using flow cytometric analysis. There was a profound decrease in the T-helper/cytotoxic T- cell (CD4/CD8) ratio in heroin addicts (Donahoe et al., 1987). Shine et al. (1987) found a normal pattern of T-cell subsets and a normal CD4/CD8 ratio in another group of healthy intravenous drug abusers and methadone patients. Most of the data have suggested that opiates are involved in the cell-mediated immune responses in heroin addicts. However, data of immune responses in heroin-withdrawal subjects during various withdrawal periods are not available at this moment. Thus, the evidence for the immunomodulatory, and even the immunocompromising potential of opioids is compelling. Still, our understanding of the effects of opioids on the immune system is incomplete. Controversial results, in part, may be due to the specific mechanisms responsible for morphine-induced changes in the immune system being undefined. In addition, most of the heroin addicts are polydrug users. It is necessary to better understand the way in which heroin modulates immune responses, as well as the relationship between these effects, and to investigate whether this results in increased susceptibility to infections. We focused our attention on studies of the heroin-addicted and heroin withdrawal subjects by considering the lymphocyte proliferative responses, the expression of total T lymphocytes (CD3), T-helper cells (CD4), cytotoxic T-cell (CD8) antigenic markers of T-cells, B cells and NK cells. We conducted studies in humans because humans are significantly different from even the closest primates, and certainly profoundly different from rodents, with respect to certain specific immune indices and the pharmacokinetics of many drugs, as well as neuroendocrine functions. This is the first study of the immune function in heroin withdrawal subjects who used the cold turkey method, with no supplement of methadone or other drugs in the withdrawal period. Methods Subject selection. Subjects consisted of parenteral heroin abusers and heroin withdrawal subjects from Thanyarak Hospital, which is one of the biggest hospitals in Thailand, with 100 to 200 cases of outpatient drug abusers daily. All subjects were men, aged 20 to 40 years, and none had recent infections, active inflammatory disease or a positive HIV or HBsAg test. They were free of drugs affecting the immune system and had no history of neuropsychiatric disorders. Subjects participating in this study gave written informed consent. All of the parenteral heroin abusers were selected from those who had a history of intravenous injection of heroin for 1 year, with a daily heroin dosage of not less than 600 mg. They absolutely did not abuse other drugs. The heroin withdrawal subjects used the cold turkey method for withdrawal from heroin, after which they experienced craving with some withdrawal symptoms, such as rhinorrhea, lacrimation, piloerection, restlessness, irritability, insomnia, abdominal cramps, muscle bone aches and so on. They were free of drugs for suppressing the withdrawal symptoms. Serum and urine analyses. Blood and urine from volunteers in all groups of this study were obtained between 9:00 to 11:30 a.m. Blood was collected into polyethylene tubes containing 1000 U/ml heparin. Routine medical and immunological histories were obtained from all subjects. Routine urine analysis was performed, emphasizing the measurement of type and quantity of substances abused. Urine morphine was reported positive by a cutoff limit at 5.50 g/ml. Sera from all subjects were tested for HIV antibodies using a particle-agglutination test for screening of antibodies to HIV (Serodia-HIV, Tokyo, Japan) at Thanyarak hospital and double-checked by using MICRO RED kit (BioRad, Hercules, CA) for screening of HIV-1/HIV-2 antibodies in our laboratory. Blood chemistry studies to assess hepatitic function were determined in all subjects. Lymphocyte cultures. Freshly drawn venous blood (10 ml) from subjects was diluted 1:1 with Hanks balanced salt solution. The cell suspension (20 ml) was layered on 4 ml of Ficoll-paque solution (Pharmacia, Uppsala, Sweden) (specific gravity, 1.083) for separation of lymphocytes according to the method of Sacerdote et al. (1991). After centrifugation at 600 g for 20 min, the layer containing lymphocytes was transferred to another centrifuge tube, washed twice in 10 ml of Hanks balanced salt solution and then centrifuged at 1200 g for 10 min. The cells were resuspended again with RPMI media containing 10% heat-inactivated fetal calf serum, 100 IU/ml penicillin, 100 mg/ml streptomysin, 1% L-glutamine (Sigma Chemical, St. Louis, MO) and 1 mm HEPES (Sigma). Then, the suspension was centrifuged at 1200 g for 10 min. The pellets were lymphocytes that were brought to culture for studying proliferation. Lymphocyte cells were counted with the viable dye, 0.1% trypan blue (Sigma) and adjusted to a final concentration of cells/ml in RPMI media. Triplicate cultures containing cells in 200 l of RPMI media/well were seeded onto 96-microwell plates and treated with a mitogen, PHA (Seromed, Berlin, Germany), in concentrations of 1.2, 2.5, 5 and 10 g/ml. Lymphocyte cultures were incubated for 48 hr at 37 C in 5% CO 2 and aired in a humidified incubator. After incubation, cells were pulsed for an additional 18 hr with 1 Ci of [ 3 H]thymidine (2.0 Ci/mmol) (New England Nuclear, Boston, MA). Cell proliferation was determined by the incorporation of [ 3 H]thymidine into cellular DNA. A semiautomated cell harvesting apparatus (Nunc, Naperville, CT) was then used to lyse the cells with distilled water and precipitate the labeled DNA on glass filter paper (Whatman, Clifton, NJ). The filter pads were dried, 1 ml of scintillation fluid was added and then the radioactive material trapped on filter paper was counted as cpm by a Beckman Instruments (Columbia, MD) LS5000CE Scintillation Spectrometer. The counting efficiency for tritium was 45%. Cell preparation for immunofluorescent staining in flow cytometric studies. Peripheral blood samples were collected into EDTA anticoagulant tubes and processed within 2 hr of collection. All samples were prepared using lysed whole blood and stained with the following panel of two-color antibody conjugates: LeucoGATE (CD45FITC/CD14PE) [CD45/CD14], isotype control (IgG 1 FITC/ IgG 1 PE)[ 1 / 2 ], CD3FITC/CD16 56PE(Leu4/11C 19), CD3FITC/ CD19PE(Leu-4/12), CD3FITC/CD8PE(CD3/CD8)[Leu-4/2] and CD3FITC/CD4PE (CD3/CD4) [Leu-4/3]. After a 15-min room temperature incubation period, the red blood cells were lysed with FACS- Lysing Solution (Becton Dickinson, San Jose, CA). Samples were then fixed in a 1.0% paraformaldehyde solution before flow cytometric analysis. Flow cytometric analysis. Flow cytometric studies were performed on a FACScan Analyzer (Becton Dickinson, San Jose, CA). The FACScan used an air-cooled argon ion laser with emission at 488 nm. The FACScan was calibrated using an automatic software, AutoCOMP and CaliBRITE beads. SimulSET software was used for data acquisition and analysis, and LeucoGATE defined the lymphocyte gate, which included 95% of the total lymphocyte population. Isotype controls defined autofluorescence and positioned the quadrant markers to calculate the percent positive cells for a given antibody. Statistical analysis. Results were expressed as mean S.E.M. Student s t tests were performed on continuous variables. For studies involving multiple comparisons, data were analyzed by Tukey- Kramer multiple comparison test.
3 1998 Immune Functions in Heroin Abusers 885 Results PHA-stimulated T lymphocyte proliferation in heroin-addicted and heroin withdrawal subjects. The baseline characteristics of all subjects; normal (N; n 17), heroin addicts (H; n 19) and heroin withdrawal subjects (HW; n 17) in the T-lymphocyte proliferation study are shown in table 1. The ages of the subjects ranged from 22 to 28 years. The dosage range of heroin that was used by heroin addicts and heroin withdrawal subjects was 600 to 1200 mg/day. The durations of heroin abuse were and years in heroin addicts and heroin withdrawal groups, respectively. Urine morphine of 5.50 g/ml was detected in the heroin-addicted group.the duration of withdrawal periods ranged from 1 to 5 days. They all were negative in HIV and HBsAg tests. T-lymphocyte function was determined by the incorporation of [ 3 H]thymidine into the intracellular DNA of the cells stimulated by PHA, a specific T-cell mitogen. The percentage of T-lymphocyte proliferation compared with those of B-lymphocyte was 99%. T-lymphocytes obtained from normal, heroin-addicted and heroin withdrawal subjects were proliferated as a dose-dependent manner in the present of various concentrations (1.2, 2.5, 5 and 10 g/ml) of PHA (fig. 1). The data represent the percentage of the control (unstimulated cells of each group expressed as 100%). The proliferative responses of the cells from heroin addicts in the presence of 1.2, 2.5, 5 and 10 g/ml PHA in culture were suppressed significantly compared with normal subjects. In the heroin withdrawal (HW) group, significant immunosuppression (P.01) was also found in cells stimulated by every concentration of PHA. However, the [ 3 H]thymidine incorporation into DNA of the cells obtained from heroin withdrawal subjects was significantly increased (P.01) compared with those from the heroin-addicted (H) group. To determine the possibly direct effect of morphine on lymphocyte function, various concentrations of morphine were included in the T-lymphocyte cultured cells from normal subjects. Morphine concentrations ranging from 0.01 to 100 M induced a significant reduction (P.05 and P.01) in lymphocyte [ 3 H]thymidine incorporation in cultures stimulated with PHA 0.6 (fig. 2A) and 2.5 (fig. 2B) g/ml, respectively. To determine whether the inhibition of T-lymphocyte proliferation by morphine was abolished by naloxone, an opioid receptor antagonist, cells were cultured with 0.01, 1 and 100 M morphine in the presence of 100 M naloxone. The morphine-induced inhibition on 2.5 g/ml PHA-stimulated T- TABLE 1 Base-line characteristics (mean S.E.) of normal, heroin addicts and heroin withdrawal subjects in T-lymphocyte proliferation study. Normal Heroin addicts Heroin withdrawal Sex Male Male Male Number of subjects Age (yr) Urine morphine ( g/ml) Negative 5.50 Negative Dosage of heroin abuse (mg/day) Duration of heroin abuse (yr) HIV test Negative Negative Negative HBsAg test Negative Negative Negative Withdrawal period 1 5 days Fig. 1. Effect of 1.2, 2.5, 5 and 10 g/ml of PHA on proliferation of T-lymphocytes in normal (n 17), heroin-addicted (n 19) and heroin withdrawal subjects (n 17). Cell proliferation of T-lymphocytes extracted from three different groups of subjects were assayed as described in Materials and Methods. T-lymphocyte proliferation responses were expressed as mean S.E. of [ 3 H]thymidine incorporation into DNA compared with each unstimulated cell group (as percent control). a, Significant difference between heroin-addicted and normal subjects (P.05). b, Significant difference between heroin-addicted and normal subjects (P.01). c, Significant difference between heroin-withdrawal and normal subjects (P.01). d, Significant difference between heroin-withdrawal and heroin-addicted subjects (P.01). Fig. 2. Concentration-response effect of morphine on 0.6 (A) and 2.5 (B) g/ml PHA stimulated T-lymphocyte proliferation in normal subjects. Cell proliferation was assayed using cells/ml of lymphocyte cells in 96-microwell plate containing varying concentrations of morphine ( M) and PHA as indicated in a final volume of 200 l. After incubation (48 hr, 37 C 5% CO 2 ), all cells were pulsed for an additional 18 hr with 1 Ci [ 3 H]thymidine, and the radioactivity associated with the cells was determined. Data presented as mean S.E. of triplicate determinations from seven normal subjects. a, Significant difference from without morphine group (P.05). b, Significant difference from without morphine group (P.01). lymphocyte proliferation was totally reversed by 100 M naloxone (fig. 3). A significant difference (P.05) in T- lymphocyte proliferations was shown when compared between each concentration of morphine group, with and without naloxone, except those from the without-morphine-added group (fig. 3). Comparison of lymphocyte subsets among normal, heroin-addicted and heroin withdrawal subjects. To further evaluate the immunosuppressive responses in heroin
4 886 Govitrapong et al. Vol. 286 Fig. 3. Concentration-response effect of morphine on 2.5 g/ml PHAstimulated T-lymphocyte proliferation in normal subjects is shown in a black bar with naloxone and in a white bar without naloxone. Cell proliferation was assayed using cells/ml of lymphocyte cells in 96 microwell plate containing naloxone (100 M) 45 min before adding morphine ( M). After incubation (48 hr, 37 C, 5% CO 2 ), all cells were pulsed for an additional 18 hr with 1 Ci of [ 3 H]thymidine, and the radioactivity associated with the cells was determined. Data presented as mean S.E. of triplicate determinations from 10 normal subjects. a, Significant difference from without morphine group (P.05). b, Significant difference from 0.01 M morphine without naloxone group (P.05). c, Significant difference from 1 M morphine without naloxone group (P.05). d, Significant difference from 100 M morphine without naloxone group (P.05). abusers and heroin withdrawal subjects during various periods of time, flow cytometric analysis was performed and subjects were selected accordingly. The base-line characteristics of all subjects: normal (N; n 17), heroin addicts (H; n 15), 15- to 21-day heroin withdrawal (HW1; n 15), 6- to 24-month heroin withdrawal (HW2; n 16) and 3- to 5-year heroin withdrawal (HW3; n 15), are shown in table 2. The average age was between 21 to 31 years, with the same daily doses of heroin use (range, mg/day). The average durations of heroin abuse were , , and years in heroin addicts and in 15- to 21-day (HW1), 6- to 24-month (HW2) and 3- to 5-year (HW3) withdrawal groups, respectively. They all were free from HIV and HBs infections. The mean S.E.M. values of percent and absolute numbers of lymphocyte and total T- lymphocyte (CD3) obtained from various groups of subjects are shown in figure 4, A D. There was no significant difference in the percentages of lymphocytes and total T-lymphocytes among different groups compared with controls. However, the absolute numbers of lymphocytes (fig. 4B) and total Fig. 4. Comparison of percentage of lymphocytes (A), absolute lymphocyte count (B), percentage of total T-lymphocytes [CD3] (C) and absolute CD3 count (D) among normal (N; n 17), heroin addicts (H; n 15), 15- to 21-day heroin withdrawal (HW1; n 15), 6- to 24-month heroin withdrawal (HW2; n 16) and 3- to 5-year heroin withdrawal (HW3; n 15) subjects. The data were obtained by using a highly sensitive FACScan flow cytometer. Each group presented as mean S.E. a, Significant difference from normal group (P.05). T-lymphocytes (CD3) (fig. 4D) were both significantly increased in heroin addicts, gradually declining to normal levels as heroin withdrawal progressed. The percentages of T- helper cells (CD4) obtained from heroin addicts and short period heroin withdrawal groups were significantly decreased, reverting to normal levels when heroin withdrawal had continued for a longer period of time (6 months to 5 years) (fig. 5A). In contrast, the percentages of cytotoxic T-cell (CD8) obtained from heroin addicts and short period heroin withdrawal groups were significantly increased (P.001), reverting to normal levels when heroin withdrawal had continued for a longer period of time (fig. 5C). The absolute TABLE 2 Base-line characteristics (mean S.E.) of normal, heroin addicts and heroin withdrawal subjects in flow cytometric analysis Heroin withdrawal subjects Normal Heroin addicts HW1 HW2 HW3 Number of subjects Sex Male Male Male Male Male Age (yr) Urine morphine ( g/ml) Negative 5.50 Negative Negative Negative Dosage of heroin abuse (mg/day) Duration of heroin abuse (yr) HIV test Negative Negative Negative Negative Negative HBsAg test Negative Negative Negative Negative Negative Withdrawal period days 6 24 mo 3 5 yr
5 1998 Immune Functions in Heroin Abusers 887 Fig. 5. Comparison of percentage of T-helper [CD4](A), absolute CD4 count (B), percentage of T-suppressor [CD8] (C), absolute CD8 count (D) and the T-helper/T-suppressor [CD4/CD8] ratio (E) among normal (N; n 17), heroin addicts (H; n 15), 15- to 21-day heroin withdrawal (HW1; n 15), 6- to 24-month heroin withdrawal (HW2; n 16) and 3- to 5-year heroin withdrawal (HW3; n 15) subjects. The data were obtained by using a highly sensitive FACScan flow cytometer. Each group presented as mean S.E. a, Significant difference from normal group (P.05). b, Significant difference from normal group (P.01). c, Highly significant difference from heroin-addicted group (P.001). d, Significant difference from heroin-addicted group (P.01). Fig. 6. Comparison of percentage of B-cell (A), NK cell (B), absolute B-cell count (C) and absolute NK-cell count (D) among normal (N; n 17), heroin addicts (H; n 15), 15- to 21-day heroin withdrawal (HW1; n 15), 6- to 24-month heroin withdrawal (HW2; n 16) and 3- to 5-year heroin withdrawal (HW3; n 15) subjects. The data were obtained by using a highly sensitive FACScan flow cytometer. Each group presented as mean S.E. a, Significant difference from normal group (P.05). b, Significant difference from normal group (P.01). c, Significant difference from heroin-addicted group (P.05). numbers of CD8 in different groups of subjects were altered in the same manner as the percents of CD8 (fig. 5D), whereas the absolute numbers of CD4 in all cases did not show any significant difference among groups (fig. 5B). The ratios of T-helper/cytotoxic T-cell (CD4/CD8) were shown to be significantly decreased in heroin addicts (P.001), in 15- to 21-day heroin withdrawal (P.001) and in 6- to 24-month heroin withdrawal (P.05) compared with normal subjects, whereas this ratio reversed to normal values in 3- to 5-year heroin withdrawal subjects (fig. 5E). Both the percentage (fig. 6A) and absolute numbers of B-cells (fig. 6B) obtained from heroin addicts and 15- to 21-day heroin withdrawal subjects were significantly increased (P.01) compared with those obtained from normal subjects, whereas the numbers obtained from subjects during longer periods of heroin withdrawal were comparable to those of normal subjects. The percentage of NK cells (fig. 6C) obtained from heroin addicts and the 15- to 21-day heroin withdrawal group were significantly decreased (P.05 and P.01, respectively) compared with normal subjects, whereas the absolute numbers of NK cells (fig. 6D) from all groups of subjects were not significantly different. However, the percentage (fig. 6C) and absolute number of NK cells (fig. 6D) in the 6- to 24-month heroin withdrawal group were increased significantly (P.05) compared with heroin-addicted subjects. Discussion Alteration of immune function in heroin addicts. Opiates have been shown to produce effects on immune function in vivo (Weber and Pert, 1989), and clinical observations that opiate addicts have increased susceptibility to infections (Louria et al., 1967) were subsequently shown to be related to deficits in immune function (Brown et al., 1974). Our study has demonstrated a decrease in the response of T lymphocytes to a wide range of concentrations of mitogenic (PHA) stimuli in heroin-addicted subjects. This data supports the result from Roy et al. (1995), who demonstrated that chronic morphine treatment in vivo inhibited PHA-IL1-activated thymocyte proliferation. It has been proposed that the effects of opioids on lymphocyte proliferation may operate via a direct interaction with opioid receptors (Sibinga and Goldstein, 1988). To test the above hypothesis, the effect of morphine in vitro has therefore been studied. Morphine attenuated the mitogen-induced lymphocyte proliferation in a dosedependent manner. Roy et al. (1991) showed a suppressive effect of chronic morphine treatment on macrophage colony formation in bone marrow. In addition, morphine inhibited
6 888 Govitrapong et al. Vol. 286 proliferation of PHA-IL-1 activation of naive mice thymocytes in a dose-dependent manner could be demontrated in vitro (Roy et al., 1995). Our data also indicate that this inhibitory effect was abolished by naloxone. However, our unpublished observation showed that neither morphine nor naloxone could significantly alter the background (without PHA) proliferation of lymphocyte. Roy et al. (1996) and Wick et al. (1996) demonstrated that morphine-mediated inhibition of Bac1.2 F5 macrophage in culture was partially reversible by naloxone, and their previous experiment showed that activation of thymocyte with PHA-IL1 in vitro resulted in a dramatic increase in ( 3 H)-morphine specific binding (Roy et al., 1992). Collectively, we suggest that PHA might induce proliferation of different population of lymphocytes containing different affinities of opioid receptors that are more or less sensitive to morphine. Immunophenotypic markers on lymphoid cells have been determined using flow cytometric analysis in heroin addicts. There was a profound decrease in the proportion of CD4/CD8 and the percentage of CD4, with an increase in both the percentage and absolute numbers of CD8 and the absolute numbers of cell expressing CD3. The data obtained here are parallel with the proliferative responses. However, Shine et al. (1987) found a normal pattern of T-cell subsets in a group of healthy intravenous drug abusers and methadone patients, whereas Sei et al. (1991) and Novick et al. (1989) found that parenteral heroin abusers had higher absolute numbers of CD4 cells in the peripheral blood. NK cell activity mediated predominantly by large granular lymphocytes is also regulated by opioid compounds. In vitro, -endorphin and met-enkephalin augmented NK activity in a dose-dependent and naloxone-reversible fashion (Matthews et al., 1983; Kay et al., 1984). Morphine was slightly suppressive (Matthews et al., 1983), and DAMGO suppressed NK activity (Weber et al., 1989). Shavit et al. (1986) have previously shown that opiates interacting with opiate receptors in the brain are implicated in the suppression of NK activity. Those authors suggested novel central nervous system mechanisms through which the immune response might be regulated. In the present study, the percentage of NK cells was suppressed in heroin addicts. This was supported by a previous study showing that parenteral heroin addicts had significantly reduced NK activity while the absolute numbers of NK cells in peripheral blood were unchanged (Novick et al., 1989). The similar findings had previously been reported by Reddy et al. (1987) and DePaoli et al. (1986), who observed reduced NK cell activity in HIV-seronegative parenteral drug addicts and a further reduction in HIV-seropositive patients. The present study in heroin addicts has shown an increase in both the number and the percentage of B cells by immunofluorescence staining. Johnson et al. (1982) reported that -endorphin in vivo significantly depressed primary antibody production to sheep red blood cells. Both met-enkephalin and leu-enkephalin are modulate inhibitors, whereas - and -endorphin are not effective. Morphine seems to have no effect on antibody production where animals are immunized with a T-independent antigen. However, in vivo administration of -endorphin inhibited the primary antibody response to keyhole limpet hemocyanin but enhanced the secondary response (Munn et al., 1989). Immune status in heroin-withdrawal subjects. The immune function in heroin withdrawal subjects also was a focus of the present study. In most previous studies of heroin addiction, the data were obtained from patients who were not only polydrug abuses but also in the withdrawal state; most patients were either treated with drugs to suppress withdrawal symptoms, in methadone maintenance therapy or both. The patients in our study not only were single-drug abusers but, in the withdrawal state, also were free of any drug, as heroin withdrawal was carried out cold turkey. This would make our results extremely beneficial for the better understanding of heroin withdrawal mechanisms. In a previous study (Novick et al., 1989) of long-term stabilized methadone-maintenanced patients, NK cell activity and absolute B- and T-cell subset numbers were not significantly different from those of normal control subjects. Kind (1988) performed a study in unselected groups of former narcotic addicts in methadone maintenance treatment for varying periods of time, including patients both with and without continuing polydrug and alcohol abuse. He found that 53% of subjects had normal NK cell cytotoxicity. However, methadone itself has been shown to have immunomodulatory effects, and these effects are dose dependent. At doses below 75 mg/kg, it was possible to reverse the immunodepressive effect of heroin (Novick et al., 1989). In contrast, in an in vitro study, Kind (1988) showed that neither opioid antagonist (naloxone) nor opioid agonist (methadone) altered NK cytotoxicity until drug concentrations pf 10 4 M above pharmacological levels were reached, at which point both compounds reduced NK activity in parallel responses. In the present study, the suppression of lymphocyte proliferation responses was partially reversed in the heroin withdrawal subjects. All parameters, assessed by flow cytometric analysis, were altered in heroin addicts but gradually returned to normal levels, with the exception of the short period of withdrawal (15 to 21 days), where they seemed to get worse. However, the total recovery in almost all immunological parameters obtained here would not occur before 3 to 5 years after drug withdrawal. Our studies supported the notion that the time course of the development of tolerance following initial drug exposure and the persistence of tolerance following sudden removal of the drug was found to parallel the development and decline of immune reactions (Cochin and Kornetsky, 1964). Our result clearly demonstrates that the immunological deficits evidenced during drug consumption are reversible slowly after heroin is withdrawn, without taking methadone and concomitantly in parallel with the decline of the withdrawal signs and other neurobehavioral effects. A considerable amount of evidence suggests that opioids administrated in vivo modify the immune system indirectly. The HPA axis has been implicated in the morphine-mediated suppression of primary humoral immune responses (Pruett et al., 1992). Other recent studies also suggest that morphine-mediated effects on the immune system operates through central processes (Hernandez et al., 1993; Fecho et al., 1993). However, there was an indication that the HPA axis was not necessarily involved in all opioid-mediated immunosuppressive effects because injection of opioid compounds into specific sites of the brain that resulted in a suppressive effect on immune function (e.g., lymphocyte proliferation on splenic NK activity) did not change the circulating levels of corticosterone (Band et al., 1992; Hernandez et al., 1993). Collectively, these results provide convincing evidence for the local and systemic activity of opioids on immu-
7 1998 Immune Functions in Heroin Abusers 889 nocompetence and immune homeostasis. Attempts to definitively prove of the existence of opioid receptors on cells of the immune system have been unsucessful in various laboratories, including our own by using radioligand binding. However, recently, molecular techniques have provided data (Sedqi et al., 1995; Chuang et al., 1995; Wick et al., 1996; Roy et al., 1996) indicating the existence of opioid receptors on cells of the immune system. In conclusion, the results from our study indicate a depression in PHA-stimulated T lymphocyte proliferation, both as an in vitro effect of morphine and in heroin addicts, including the modulation of surface markers observed on T cells. The alteration of the T lymphocyte proliferative responses and surface markers seems to gradually reverse to normal levels when heroin is withdrawn. The mechanisms responsible for the opioid-induced changes in immune function are still unclear. They may be mediated directly via opioid receptors present on lymphocytes (Wick et al., 1996; Roy et al., 1996) and/or indirectly via opioid receptors in the central nervous system. Molecular biological and biochemical characterizations suggest that immune cell differentially express classic opioid receptors. In addition, the presence of a novel class of opioid receptor in immune cells has been suggested, and it is believed that the antiproliferative effect is mediated via this receptor type (Roy and Loh, 1996). However, multifactorial elements might be involved in such alteration. Efforts should be continued and expanded to facilitate an interchange of new ideas that will accelerate research and lead to the more rapid development of new and more effective treatments for substance abuse. Acknowledgments We express their appreciation to the staff of Thanyarak Hospital for their support, helpful cooperation and suggestions. References Band LC, Pert A, Williams W, DeCosta BR, Rice KC and Weber R (1992) Central -opioid receptors mediate suppression of natural killer activity in vivo. Prog Neuroendocrinimmunol 5: Brown SM, Stimmel B and Taub RN (1974) Immunologic dysfunction in heroin addicts. Arch Intern Med 134: Carr DJJ, Rogers TJ and Weber RJ (1996) The relevance of opioids and opioid receptors on immunocompetence and immune homeostasis. Proc Soc Exp Biol Med 213: Chuang LF, Chuang TK, Killam KF, Qui JQ, Wang XR, Lin JJ, Kung HF, Sheng W, Chao C, Yu L and Chuang RY (1995) Expression of kappa opioid receptors in human and monkey lymphocytes. Biochem Biophys Res Commun 209: Cochin J and Kornetsky C (1964) Development and loss of tolerance to morphine in the rat after single and multiple injections. J Pharmacol Exp Ther 145:1 10. Curran JW, Lawrence DN, Jaffe H, Kaplan JE, Zyla LD, Chamberland M, Weinstein R, Lui KJ, Schonberger LB and Spira TJ (1984) Acquired immunodeficiency syndrome (AIDS) associated with transfusion. N Engl J Med 310: DePaoli P, Reitano M and Battlinstin S (1986) Immunological abnormalities in intravenous drug abuser and relationship to generalized lymphadenopathy in Italy. Clin Exp Immunol 64: Donahoe RM, Bueso-Ramos C, Donahoe F, Madden JJ, Falek A, Nicholson JKA and Bokos P (1987) Mechanistic implications of the findings that opiates and other drugs of abuse moderate T-cell surface receptors and antigenic markers. Ann NY Acad Sci 496: Fecho K, Dykstra LA and Lysle DT (1993) Evidence for beta adrenergic receptor involvement in the immunomodulatory effects of morphine J Pharmacol Exp Ther 265: Heathcote J and Taylor KB (1981) Immunity and nutrition in heroin addicts. Drug Alcohol Depend 8: Hernandez MC, Flores LR and Bayer BM (1993) Immunosuppression by morphine is mediated by central pathways. J Pharmacol Exp Ther 267: Johnson HM, Smith EM, Torres BA and Blalock JE (1982) Regulation of the in vitro antibody response by neuroendocrine hormones. Proc Natl Acad Sci USA 79: Kay N, Allen J and Morley JE (1984) Endorphins stimulate normal human peripheral blood lymphocyte natural killer activity. Life Sci 35: Kind P (1988) Basic immunology issues in drug abuse. NIDA Res Monogr 90: Louria DB, Hensle T and Rose J (1967) The major medical complications of heroin addiction. Ann Intern Med 67:1 22. Matthews PM, Froelich CJ, Sibbit WJ and Bankhurst AD (1983) Enhancement of natural cytotoxicity by beta-endophin. J Immunol 130: McDonough RJ, Madden JJ, Falek A, Shafer DA, Pline M, Dordon D, Gokos P, Kuehnle JC and Mendelson J (1980) Alteration of T and null lymphocyte frequencies in the peripheral blood of human opiate addicts: In vivo evidence for opiate receptor sites on T lymphocytes. J Immunol 125: Munn NA and Lum LG (1989) Immunoregulatory effects of alpha-endorphin, betaendorphin, methionine-enkephalin adrenocorticotropic hormone on anti-tetanus toxiod antibody synthesis by human lymphocytes. Clin Immunol Immunopathol 52: Novick DM, Ochshornn M and Ghali V (1989) Natural killer cell and lymphocyte subsets in parenteral heroin abuser and long term methadone maintenance patients. J Pharmacol Exp Ther 250: Pruett SB, Han YC and Fuchs BA (1992) Morphine suppresses primary humoral immune responses by a predominantly indirect mechanism. J Pharmacol Exp Ther 262: Quagliata F, Melton R and Soika I (1977) Decrease response to mitogens and impaired capping ability of lymphocytes in narcotic addiction. Clin Res 25:513A. Reddy MM, Englard A, Brown D, Buimovici-Klien E and Grieco MH (1987) Lymphoproliferative responses to human immunodeficiency virus in asymptomatic intravenous drug abusers and in patients with lymphodenopathy or AIDS. J Infect Dis 156: Rouveix B (1992) Opiates and immune function. Therapie 47: Roy S, Ge BL, Loh HH and Lee NM (1992) Characterization of ( 3 H)-morphine binding to interleukin-1 activated thymocyte. J Pharmacol Exp Ther 263: Roy S, Loh HH and Barke RA (1995) Morphine-induced suppression of thymocyte proliferation is mediated by inhibition of IL-2 synthesis. Adv Exp Med Biol 373: Roy S and Loh HH (1996) Effects of opioids on the immune system. Neurochem Res 21: Roy S, Ramakrishanan S, Loh HH and Lee NM (1991) Chronic morphine treatment selectively suppresses macrophage colony formation in bone marrow. Eur J Pharmacol 195: Roy S, Sedqi M, Ramakrishanan S, Barke RA and Loh HH (1996) Differential effects of opioids on the proliferation of macrophage cell line Bac1.2F5. Cell Immunol 2: Sacerdote P, Rubboli F, Locatelli L, Ciciliato I, Mantegazza P and Panerai AE (1991) Pharmacological modulation of neuropeptides in peripheral mononuclear cells. J Neuroimmunol 32: Sei Y, Yoshimoto K, Meintyre T, Skolnick P and Arora PK (1991) Morphine-induced thymic hypoplasia is glucocorticoid dependent. J Immunol 146: Sedqi M, Roy S, Ramakrishnan S, Elde R and Loh HH (1995) Complementary DNA cloning of a -opioid receptor from rat peritoneal macrophages. Biochem Biophys Res Commun 209: Shavit Y, Depaulis A and Martin FC (1986) Involvement of brain opiate receptors in the immune-suppressive effect of morphine. Proc Natl Acad Sci USA 83: Shine D, Moll B, Emeson E, Spigland I, Harris C, Small CB, Friedland G, Weiss SH and Bodner AJ (1987) Serologic immunologic and clinical features of parenteral drug users from contrasting populations. Am J Drug Alcohol Abuse 13: Sibinga NE and Goldstein A (1988) Opioid peptides and opioid receptors in cell of the immune system. Annu Rev Immunol 6: Wick MJ, Minnerath SR, Roy S, Ramakrishnan S and Loh HH (1996) Differential expression of opioid receptor genes in human lymphoid cell lines and peripheral blood lymphocytes. J Neuroimmunol 64: Weber RJ and Pert A (1989) The periaqueductal gray matter mediates opiateinduced immunosuppression. Science 245: Wongkhomthong SA, Kaime A and Ono K (1995) AIDS in the Developing World: A Case Study in Thailand. Holistic Publishing, Bangkok. Send reprint requests to: Piyarat Govitrapong, Ph.D., Neuro-Behavioural Biology Center, Institute of Science and Technology for Research and Development, Mahidol University at Salaya, Nakornpathom 73170, Thailand. grpkk@mahidol.ac.th
Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory
 Immunology and Cell Biology (1999) 77, 559 564 Special Feature Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory DA FULCHER
Immunology and Cell Biology (1999) 77, 559 564 Special Feature Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory DA FULCHER
CFSE Cell Division Assay Kit
 CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
STANDARD OPERATING PROCEDURE
 Title: Lymphocyte Proliferation Assay (LPA) Using 3 H- Thymidine Incorporation Assay Core Name: Lloyd Mayer, Mount Sinai Medical Center Effective Date: 02/16/2012 Trial Number: ITN047AI SOP # ITN2800 SOP
Title: Lymphocyte Proliferation Assay (LPA) Using 3 H- Thymidine Incorporation Assay Core Name: Lloyd Mayer, Mount Sinai Medical Center Effective Date: 02/16/2012 Trial Number: ITN047AI SOP # ITN2800 SOP
International Beryllium Conference, Montreal, Canada March 10, 2005
 Alternative Lymphocyte Proliferation Tests: BrdU and Flow Cytometry Based Tests International Beryllium Conference, Montreal, Canada March 10, 2005 Tim K. Takaro Department of Environmental and Occupational
Alternative Lymphocyte Proliferation Tests: BrdU and Flow Cytometry Based Tests International Beryllium Conference, Montreal, Canada March 10, 2005 Tim K. Takaro Department of Environmental and Occupational
RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method)
 Immune Tolerance Network RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method) Author: Paul Wallace, Director, RPCI Laboratory of Flow Cytometry Approved by: Paul
Immune Tolerance Network RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method) Author: Paul Wallace, Director, RPCI Laboratory of Flow Cytometry Approved by: Paul
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens
 www.iqproducts.nl PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens IFN- γ PURE [RUO] [REF] IQP-160P s 50 tests FITC [RUO] [REF] IQP-160F s 50 tests R-PE [RUO] [REF] IQP-160R s 50
www.iqproducts.nl PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens IFN- γ PURE [RUO] [REF] IQP-160P s 50 tests FITC [RUO] [REF] IQP-160F s 50 tests R-PE [RUO] [REF] IQP-160R s 50
Standardization, Calibration and Quality Control
 Standardization, Calibration and Quality Control Ian Storie Flow cytometry has become an essential tool in the research and clinical diagnostic laboratory. The range of available flow-based diagnostic
Standardization, Calibration and Quality Control Ian Storie Flow cytometry has become an essential tool in the research and clinical diagnostic laboratory. The range of available flow-based diagnostic
TITLE: TRU-COUNT ENUMERATION OF T-CELLS IN WHOLE
 TITLE: TRU-COUNT ENUMERATION OF T-CELLS IN WHOLE PRINCIPLES OF THE PROCEDURE: When whole blood is added to the reagent, the fluorochrome labeled antibodies in the reagent bind specifically to leukocyte
TITLE: TRU-COUNT ENUMERATION OF T-CELLS IN WHOLE PRINCIPLES OF THE PROCEDURE: When whole blood is added to the reagent, the fluorochrome labeled antibodies in the reagent bind specifically to leukocyte
Immunity and how vaccines work
 1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
Immunophenotyping peripheral blood cells
 IMMUNOPHENOTYPING Attune Accoustic Focusing Cytometer Immunophenotyping peripheral blood cells A no-lyse, no-wash, no cell loss method for immunophenotyping nucleated peripheral blood cells using the Attune
IMMUNOPHENOTYPING Attune Accoustic Focusing Cytometer Immunophenotyping peripheral blood cells A no-lyse, no-wash, no cell loss method for immunophenotyping nucleated peripheral blood cells using the Attune
Like cocaine, heroin is a drug that is illegal in some areas of the world. Heroin is highly addictive.
 Heroin Introduction Heroin is a powerful drug that affects the brain. People who use it can form a strong addiction. Addiction is when a drug user can t stop taking a drug, even when he or she wants to.
Heroin Introduction Heroin is a powerful drug that affects the brain. People who use it can form a strong addiction. Addiction is when a drug user can t stop taking a drug, even when he or she wants to.
Treatment of Opioid Dependence with Buprenorphine/Naloxone (Suboxone )
 Treatment of Opioid Dependence with Buprenorphine/Naloxone (Suboxone ) Elinore F. McCance-Katz, M.D., Ph.D. Professor and Chair, Addiction Psychiatry Virginia Commonwealth University Neurobiology of Opiate
Treatment of Opioid Dependence with Buprenorphine/Naloxone (Suboxone ) Elinore F. McCance-Katz, M.D., Ph.D. Professor and Chair, Addiction Psychiatry Virginia Commonwealth University Neurobiology of Opiate
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Heroin. How Is Heroin Abused? How Does Heroin Affect the Brain? What Other Adverse Effects Does Heroin Have on Health?
 Heroin Heroin is an opiate drug that is synthesized from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears as a white or brown
Heroin Heroin is an opiate drug that is synthesized from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears as a white or brown
1) Siderophores are bacterial proteins that compete with animal A) Antibodies. B) Red blood cells. C) Transferrin. D) White blood cells. E) Receptors.
 Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Heroin. How is Heroin Abused? What Other Adverse Effects Does Heroin Have on Health? How Does Heroin Affect the Brain?
 Heroin Heroin is a synthetic opiate drug that is highly addictive. It is made from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears
Heroin Heroin is a synthetic opiate drug that is highly addictive. It is made from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears
Application Note 10. Measurement of Cell Recovery. After Sorting with a Catcher-Tube-Based. Cell Sorter. Introduction
 Application Note 10 Measurement of Cell Recovery After Sorting with a Catcher-Tube-Based Cell Sorter Introduction In many experiments using sorted cells, it is important to be able to count the number
Application Note 10 Measurement of Cell Recovery After Sorting with a Catcher-Tube-Based Cell Sorter Introduction In many experiments using sorted cells, it is important to be able to count the number
Human CD4+T Cell Care Manual
 Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Basic Science in Medicine
 Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
Identification of T-cell epitopes of SARS-coronavirus for development of peptide-based vaccines and cellular immunity assessment methods
 RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES PKS Chan 陳 基 湘 S Ma 文 子 光 SM Ngai 倪 世 明 Key Messages 1. Subjects recovered from SARS-CoV infection retain memory of cellular immune response to epitopes
RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES PKS Chan 陳 基 湘 S Ma 文 子 光 SM Ngai 倪 世 明 Key Messages 1. Subjects recovered from SARS-CoV infection retain memory of cellular immune response to epitopes
Results: A plot showing propidium iodide and Annexin is used to determine apoptotic (Annexin only +) from necrotic (PI+ and Annexin +).
 Results: A plot showing propidium iodide and Annexin is used to determine apoptotic (Annexin only +) from necrotic (PI+ and Annexin +). This group should be a low percentage. Surface markers can then be
Results: A plot showing propidium iodide and Annexin is used to determine apoptotic (Annexin only +) from necrotic (PI+ and Annexin +). This group should be a low percentage. Surface markers can then be
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159. Date Submitted: 12-11-09
 Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
CD3/TCR stimulation and surface detection Determination of specificity of intracellular detection of IL-7Rα by flow cytometry
 CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
THE IMMUNE SYSTEM AND BREAST CANCER
 THE IMMUNE SYSTEM AND BREAST CANCER Moderator: Hope Nemiroff Panelists: David M. Brady, ND, DC, CCN, DACBN Elizabeth Boham, MD, MS, RD Examining the role of the immune system in breast cancer survival
THE IMMUNE SYSTEM AND BREAST CANCER Moderator: Hope Nemiroff Panelists: David M. Brady, ND, DC, CCN, DACBN Elizabeth Boham, MD, MS, RD Examining the role of the immune system in breast cancer survival
Considerations in Medication Assisted Treatment of Opiate Dependence. Stephen A. Wyatt, D.O. Dept. of Psychiatry Middlesex Hospital Middletown, CT
 Considerations in Medication Assisted Treatment of Opiate Dependence Stephen A. Wyatt, D.O. Dept. of Psychiatry Middlesex Hospital Middletown, CT Disclosures Speaker Panels- None Grant recipient - SAMHSA
Considerations in Medication Assisted Treatment of Opiate Dependence Stephen A. Wyatt, D.O. Dept. of Psychiatry Middlesex Hospital Middletown, CT Disclosures Speaker Panels- None Grant recipient - SAMHSA
Chapter 3. Immunity and how vaccines work
 Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS
 FOR IN-VITRO DIAGNOSTIC USE INVITROGEN CAL-LYSE TM Lysing Solution WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS CAL-LYSE TM CATALOG No. GAS-010 250 tests 25 ml CATALOG No. GAS-010S-100
FOR IN-VITRO DIAGNOSTIC USE INVITROGEN CAL-LYSE TM Lysing Solution WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS CAL-LYSE TM CATALOG No. GAS-010 250 tests 25 ml CATALOG No. GAS-010S-100
The Need for a PARP in vivo Pharmacodynamic Assay
 The Need for a PARP in vivo Pharmacodynamic Assay Jay George, Ph.D., Chief Scientific Officer, Trevigen, Inc., Gaithersburg, MD For further infomation, please contact: William Booth, Ph.D. Tel: +44 (0)1235
The Need for a PARP in vivo Pharmacodynamic Assay Jay George, Ph.D., Chief Scientific Officer, Trevigen, Inc., Gaithersburg, MD For further infomation, please contact: William Booth, Ph.D. Tel: +44 (0)1235
Uses of Flow Cytometry
 Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
Medication-Assisted Addiction Treatment
 Medication-Assisted Addiction Treatment Molly Carney, Ph.D., M.B.A. Executive Director Evergreen Treatment Services Seattle, WA What is MAT? MAT is the use of medications, in combination with counseling
Medication-Assisted Addiction Treatment Molly Carney, Ph.D., M.B.A. Executive Director Evergreen Treatment Services Seattle, WA What is MAT? MAT is the use of medications, in combination with counseling
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer
 Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Chapter 43: The Immune System
 Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Heroin. How Is Heroin Abused? How Does Heroin Affect the Brain? What Other Adverse Effects Does Heroin Have on Health?
 Heroin Heroin is an opiate drug that is synthesized from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears as a white or brown
Heroin Heroin is an opiate drug that is synthesized from morphine, a naturally occurring substance extracted from the seed pod of the Asian opium poppy plant. Heroin usually appears as a white or brown
MEDICALLY SUPERVISED OPIATE WITHDRAWAL FOR THE DEPENDENT PATIENT. An Outpatient Model
 MEDICALLY SUPERVISED OPIATE WITHDRAWAL FOR THE DEPENDENT PATIENT An Outpatient Model OBJECTIVE TO PRESENT A PROTOCOL FOR THE EVALUATION AND TREATMENT OF PATIENTS WHO ARE CHEMICALLY DEPENDENT ON OR SEVERLY
MEDICALLY SUPERVISED OPIATE WITHDRAWAL FOR THE DEPENDENT PATIENT An Outpatient Model OBJECTIVE TO PRESENT A PROTOCOL FOR THE EVALUATION AND TREATMENT OF PATIENTS WHO ARE CHEMICALLY DEPENDENT ON OR SEVERLY
OKT3. ~ The first mouse monoclonal antibody. used in clinical practice in the field of transplantation ~
 g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
CHAPTER 8 IMMUNOLOGICAL IMPLICATIONS OF PEPTIDE CARBOHYDRATE MIMICRY
 CHAPTER 8 IMMUNOLOGICAL IMPLICATIONS OF PEPTIDE CARBOHYDRATE MIMICRY Immunological Implications of Peptide-Carbohydrate Mimicry 8.1 Introduction The two chemically dissimilar molecules, a peptide (12mer)
CHAPTER 8 IMMUNOLOGICAL IMPLICATIONS OF PEPTIDE CARBOHYDRATE MIMICRY Immunological Implications of Peptide-Carbohydrate Mimicry 8.1 Introduction The two chemically dissimilar molecules, a peptide (12mer)
Treatment of Opioid Dependence: A Randomized Controlled Trial. Karen L. Sees, DO, Kevin L. Delucchi, PhD, Carmen Masson, PhD, Amy
 Category: Heroin Title: Methadone Maintenance vs 180-Day psychosocially Enriched Detoxification for Treatment of Opioid Dependence: A Randomized Controlled Trial Authors: Karen L. Sees, DO, Kevin L. Delucchi,
Category: Heroin Title: Methadone Maintenance vs 180-Day psychosocially Enriched Detoxification for Treatment of Opioid Dependence: A Randomized Controlled Trial Authors: Karen L. Sees, DO, Kevin L. Delucchi,
Low Cost CD4 Enumeration Using Generic Monoclonal Antibody Reagents and a Two-Color User-Defined MultiSET TM Protocol
 Cytometry Part B (Clinical Cytometry) 70B:355 360 (2006) Low Cost CD4 Enumeration Using Generic Monoclonal Antibody Reagents and a Two-Color User-Defined MultiSET TM Protocol Kovit Pattanapanyasat, 1 *
Cytometry Part B (Clinical Cytometry) 70B:355 360 (2006) Low Cost CD4 Enumeration Using Generic Monoclonal Antibody Reagents and a Two-Color User-Defined MultiSET TM Protocol Kovit Pattanapanyasat, 1 *
ENUMERATION OF LYMPHOCYTE SUBSETS USING FLOW CYTOMETRY: EFFECT OF STORAGE BEFORE AND AFTER STAINING IN A DEVELOPING COUNTRY SETTING
 ENUMERATION OF LYMPHOCYTE SUBSETS USING FLOW CYTOMETRY: EFFECT OF STORAGE BEFORE AND AFTER STAINING IN A DEVELOPING COUNTRY SETTING Sanju Jalla*, Sunil Sazawal***, Saikat Deb***, Robert E. Black**, Satya
ENUMERATION OF LYMPHOCYTE SUBSETS USING FLOW CYTOMETRY: EFFECT OF STORAGE BEFORE AND AFTER STAINING IN A DEVELOPING COUNTRY SETTING Sanju Jalla*, Sunil Sazawal***, Saikat Deb***, Robert E. Black**, Satya
Introduction to Tolerance, Physical Dependence and Withdrawal
 Introduction to Tolerance, Physical Dependence and Withdrawal Carrie G Markgraf, MD, PhD Safety Assessment Merck Research Laboratories 1 Overview Definitions Addiction, psychological dependence, physical
Introduction to Tolerance, Physical Dependence and Withdrawal Carrie G Markgraf, MD, PhD Safety Assessment Merck Research Laboratories 1 Overview Definitions Addiction, psychological dependence, physical
Supplemental Information. McBrayer et al. Supplemental Data
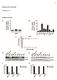 1 Supplemental Information McBrayer et al. Supplemental Data 2 Figure S1. Glucose consumption rates of MM cell lines exceed that of normal PBMC. (A) Normal PBMC isolated from three healthy donors were
1 Supplemental Information McBrayer et al. Supplemental Data 2 Figure S1. Glucose consumption rates of MM cell lines exceed that of normal PBMC. (A) Normal PBMC isolated from three healthy donors were
Human Peripheral Blood Mononuclear Cell (PBMC) Manual
 Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
EFFECTS OF IRON ON THE IMMUNE SYSTEM
 EFFECTS OF IRON ON THE IMMUNE SYSTEM Gert Mayer Department of Internal Medicine IV (Nephrology and Hypertension) Medical University Innsbruck Austria Conflicts of interest Research Support: Amgen, Roche,
EFFECTS OF IRON ON THE IMMUNE SYSTEM Gert Mayer Department of Internal Medicine IV (Nephrology and Hypertension) Medical University Innsbruck Austria Conflicts of interest Research Support: Amgen, Roche,
Lab 2. Isolation of mononuclear cells from peripheral blood and separation into subpopulations
 Lab 2 Isolation of mononuclear cells from peripheral blood and separation into subpopulations Supervisors: Sissela Broos sissela.broos@immun.lth.se tel: 222 96 78 Niclas Olsson niclas.olsson@immun.lth.se
Lab 2 Isolation of mononuclear cells from peripheral blood and separation into subpopulations Supervisors: Sissela Broos sissela.broos@immun.lth.se tel: 222 96 78 Niclas Olsson niclas.olsson@immun.lth.se
APPLICATION INFORMATION
 DRAFT: Rev. D A-2045A APPLICATION INFORMATION Flow Cytometry 3-COLOR COMPENSATION Raquel Cabana,* Mark Cheetham, Jay Enten, Yong Song, Michael Thomas,* and Brendan S. Yee Beckman Coulter, Inc., Miami FL
DRAFT: Rev. D A-2045A APPLICATION INFORMATION Flow Cytometry 3-COLOR COMPENSATION Raquel Cabana,* Mark Cheetham, Jay Enten, Yong Song, Michael Thomas,* and Brendan S. Yee Beckman Coulter, Inc., Miami FL
KMS-Specialist & Customized Biosimilar Service
 KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
Teriflunomide is the active metabolite of Leflunomide, a drug employed since 1994 for the treatment of rheumatoid arthritis (Baselt, 2011).
 Page 1 of 10 ANALYTE NAME AND STRUCTURE TERIFLUNOMIDE Teriflunomide TRADE NAME Aubagio CATEGORY Antimetabolite TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND sclerosis. The
Page 1 of 10 ANALYTE NAME AND STRUCTURE TERIFLUNOMIDE Teriflunomide TRADE NAME Aubagio CATEGORY Antimetabolite TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND sclerosis. The
Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells
 Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells Mary E. Kopechek Honor s Research Thesis May 17, 2007 Research Advisor: Dr. Jeff Lakritz, DVM, PhD The Ohio State
Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells Mary E. Kopechek Honor s Research Thesis May 17, 2007 Research Advisor: Dr. Jeff Lakritz, DVM, PhD The Ohio State
COMMUNITY BUPRENORPHINE PRESCRIBING IN OPIATE DEPENDENCE
 COMMUNITY BUPRENORPHINE PRESCRIBING IN OPIATE DEPENDENCE INTRODUCTION High dose sublingual buprenorphine (Subutex) tablets are available in the following strengths 0.4 mg, 2 mg, and 8 mg. Suboxone tablets,
COMMUNITY BUPRENORPHINE PRESCRIBING IN OPIATE DEPENDENCE INTRODUCTION High dose sublingual buprenorphine (Subutex) tablets are available in the following strengths 0.4 mg, 2 mg, and 8 mg. Suboxone tablets,
Naltrexone Pellet Treatment for Opiate, Heroin, and Alcohol Addiction. Frequently Asked Questions
 Naltrexone Pellet Treatment for Opiate, Heroin, and Alcohol Addiction Frequently Asked Questions What is Naltrexone? Naltrexone is a prescription drug that effectively blocks the effects of heroin, alcohol,
Naltrexone Pellet Treatment for Opiate, Heroin, and Alcohol Addiction Frequently Asked Questions What is Naltrexone? Naltrexone is a prescription drug that effectively blocks the effects of heroin, alcohol,
Stimulants Notes. What is heroin?
 What is heroin? Heroin is an opiate/depressant drug processed from morphine, a naturally occurring substance in the Asian poppy plant. Morphine has been used as a narcotic for thousands of years. According
What is heroin? Heroin is an opiate/depressant drug processed from morphine, a naturally occurring substance in the Asian poppy plant. Morphine has been used as a narcotic for thousands of years. According
Standard Operating Procedure
 1.0 Purpose: 1.1 The characterisation of of main leukocyte subsets in peripheral blood cells from mice by flow cytometry. Reliable values of frequencies of leukocyte clusters are very much dependent on
1.0 Purpose: 1.1 The characterisation of of main leukocyte subsets in peripheral blood cells from mice by flow cytometry. Reliable values of frequencies of leukocyte clusters are very much dependent on
One example: Chapman and Huygens, 1988, British Journal of Addiction
 This is a fact in the treatment of alcohol and drug abuse: Patients who do well in treatment do well in any treatment and patients who do badly in treatment do badly in any treatment. One example: Chapman
This is a fact in the treatment of alcohol and drug abuse: Patients who do well in treatment do well in any treatment and patients who do badly in treatment do badly in any treatment. One example: Chapman
Immunomodulatory Effects of Mycobacteria. Toh S.S. 1 and Seah G.T. 2
 Immunomodulatory Effects of Mycobacteria Toh S.S. 1 and Seah G.T. 2 Department of Microbiology, Faculty of Medicine, National University of Singapore MD4, 5 Science Drive 2, Singapore 117597 ABSTRACT It
Immunomodulatory Effects of Mycobacteria Toh S.S. 1 and Seah G.T. 2 Department of Microbiology, Faculty of Medicine, National University of Singapore MD4, 5 Science Drive 2, Singapore 117597 ABSTRACT It
OVERVIEW OF MEDICATION ASSISTED TREATMENT
 Sarah Akerman MD Assistant Professor of Psychiatry Director of Addiction Services Geisel School of Medicine/Dartmouth-Hitchcock Medical Center OVERVIEW OF MEDICATION ASSISTED TREATMENT Conflicts of Interest
Sarah Akerman MD Assistant Professor of Psychiatry Director of Addiction Services Geisel School of Medicine/Dartmouth-Hitchcock Medical Center OVERVIEW OF MEDICATION ASSISTED TREATMENT Conflicts of Interest
NCL Method ITA-6. Leukocyte Proliferation Assay
 NCL Method ITA-6 Leukocyte Proliferation Assay Nanotechnology Characterization Laboratory National Cancer Institute-Frederick SAIC-Frederick Frederick, MD 21702 (301) 846-6939 ncl@mail.nih.gov December
NCL Method ITA-6 Leukocyte Proliferation Assay Nanotechnology Characterization Laboratory National Cancer Institute-Frederick SAIC-Frederick Frederick, MD 21702 (301) 846-6939 ncl@mail.nih.gov December
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma
 Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
This module reviews the following: Opioid addiction and the brain Descriptions and definitions of opioid agonists,
 BUPRENORPHINE TREATMENT: A Training For Multidisciplinary Addiction Professionals Module II Opioids 101 Goals for Module II This module reviews the following: Opioid addiction and the brain Descriptions
BUPRENORPHINE TREATMENT: A Training For Multidisciplinary Addiction Professionals Module II Opioids 101 Goals for Module II This module reviews the following: Opioid addiction and the brain Descriptions
The Body s Defenses CHAPTER 24
 CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
Treatment Approaches for Drug Addiction
 Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call the
Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call the
Cell Cycle Phase Determination Kit
 Cell Cycle Phase Determination Kit Item No. 10009349 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 3 Safety
Cell Cycle Phase Determination Kit Item No. 10009349 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 3 Safety
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: CSD - Suboxone Therapeutic Class: Central Nervous System Agents Therapeutic Sub-Class: Analgesics and Antipyretics (Opiate Partial Agonists) Client: County of San
Prior Authorization Guideline Guideline: CSD - Suboxone Therapeutic Class: Central Nervous System Agents Therapeutic Sub-Class: Analgesics and Antipyretics (Opiate Partial Agonists) Client: County of San
Prospects for Vaccines against Hepatitis C Viruses. T. Jake Liang. M.D. Liver Diseases Branch NIDDK, NIH, HHS
 Prospects for Vaccines against Hepatitis C Viruses T. Jake Liang. M.D. Liver Diseases Branch NIDDK, NIH, HHS HCV Vaccine Prevention strategies Protective immunity Barriers and solutions Vaccine candidates
Prospects for Vaccines against Hepatitis C Viruses T. Jake Liang. M.D. Liver Diseases Branch NIDDK, NIH, HHS HCV Vaccine Prevention strategies Protective immunity Barriers and solutions Vaccine candidates
Treatment Approaches for Drug Addiction
 Treatment Approaches for Drug Addiction [NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call
Treatment Approaches for Drug Addiction [NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call
Substitution Therapy for Opioid Dependence The Role of Suboxone. Mandy Manak, MD, ABAM, CCSAM Methadone 101-Hospitalist Workshop, October 3, 2015
 Substitution Therapy for Opioid Dependence The Role of Suboxone Mandy Manak, MD, ABAM, CCSAM Methadone 101-Hospitalist Workshop, October 3, 2015 Objectives Recognize the options available in treating opioid
Substitution Therapy for Opioid Dependence The Role of Suboxone Mandy Manak, MD, ABAM, CCSAM Methadone 101-Hospitalist Workshop, October 3, 2015 Objectives Recognize the options available in treating opioid
DrugFacts: Treatment Approaches for Drug Addiction
 DrugFacts: Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please
DrugFacts: Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please
ArC Amine Reactive Compensation Bead Kit
 ArC Amine Reactive Compensation Bead Kit Catalog no. A1346 Table 1. Contents and storage information. Material Amount Composition Storage Stability ArC reactive beads (Component A) ArC negative beads (Component
ArC Amine Reactive Compensation Bead Kit Catalog no. A1346 Table 1. Contents and storage information. Material Amount Composition Storage Stability ArC reactive beads (Component A) ArC negative beads (Component
How Does a Doctor Test for AIDS?
 Edvo-Kit #S-70 How Does a Doctor Test for AIDS? S-70 Experiment Objective: The Human Immunodefi ciency Virus (HIV) is an infectious agent that causes Acquired Immunodefi ciency Syndrome (AIDS) in humans.
Edvo-Kit #S-70 How Does a Doctor Test for AIDS? S-70 Experiment Objective: The Human Immunodefi ciency Virus (HIV) is an infectious agent that causes Acquired Immunodefi ciency Syndrome (AIDS) in humans.
Joanna L. Starrels. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VIII, 2003-2004. A. Study Purpose and Rationale
 Outpatient Treatment of Opiate Dependence with Sublingual Buprenorphine/Naloxone versus Methadone Maintenance: a Randomized Trial of Alternative Treatments in Real Life Settings Joanna L. Starrels A. Study
Outpatient Treatment of Opiate Dependence with Sublingual Buprenorphine/Naloxone versus Methadone Maintenance: a Randomized Trial of Alternative Treatments in Real Life Settings Joanna L. Starrels A. Study
Hoechst 33342 HSC Staining and Stem Cell Purification Protocol (see Goodell, M., et al. (1996) J Exp Med 183, 1797-806)
 Hoechst 33342 HSC Staining and Stem Cell Purification Protocol (see Goodell, M., et al. (1996) J Exp Med 183, 1797-86) The Hoechst purification was established for murine hematopoietic stem cells (HSC)
Hoechst 33342 HSC Staining and Stem Cell Purification Protocol (see Goodell, M., et al. (1996) J Exp Med 183, 1797-86) The Hoechst purification was established for murine hematopoietic stem cells (HSC)
Developing Medications to Treat Addiction: Implications for Policy and Practice. Nora D. Volkow, M.D. Director National Institute on Drug Abuse
 Developing Medications to Treat Addiction: Implications for Policy and Practice Nora D. Volkow, M.D. Director National Institute on Drug Abuse Medications Currently Available For Nicotine Addiction Nicotine
Developing Medications to Treat Addiction: Implications for Policy and Practice Nora D. Volkow, M.D. Director National Institute on Drug Abuse Medications Currently Available For Nicotine Addiction Nicotine
CLINICAL POLICY Department: Medical Management Document Name: Vivitrol Reference Number: NH.PHAR.96 Effective Date: 03/12
 Page: 1 of 7 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 7 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Generation of EBV-immortalized B cell lines
 UCANU 0014 Version November 01, 2011 Page 1 van 6 Generation of EBVimmortalized B cell lines CMCI (Center for molecular and Cellular Intervention) University Medical Center Utrecht Written by Name Function
UCANU 0014 Version November 01, 2011 Page 1 van 6 Generation of EBVimmortalized B cell lines CMCI (Center for molecular and Cellular Intervention) University Medical Center Utrecht Written by Name Function
Integrating Medication- Assisted Treatment (MAT) for Opioid Use Disorders into Behavioral and Physical Healthcare Settings
 Integrating Medication- Assisted Treatment (MAT) for Opioid Use Disorders into Behavioral and Physical Healthcare Settings All-Ohio Conference 3/27/2015 Christina M. Delos Reyes, MD Medical Consultant,
Integrating Medication- Assisted Treatment (MAT) for Opioid Use Disorders into Behavioral and Physical Healthcare Settings All-Ohio Conference 3/27/2015 Christina M. Delos Reyes, MD Medical Consultant,
PROTOCOL. Immunostaining for Flow Cytometry. Background. Materials and equipment required.
 PROTOCOL Immunostaining for Flow Cytometry 1850 Millrace Drive, Suite 3A Eugene, Oregon 97403 Rev.0 Background The combination of single cell analysis using flow cytometry and the specificity of antibody-based
PROTOCOL Immunostaining for Flow Cytometry 1850 Millrace Drive, Suite 3A Eugene, Oregon 97403 Rev.0 Background The combination of single cell analysis using flow cytometry and the specificity of antibody-based
HuCAL Custom Monoclonal Antibodies
 HuCAL Custom Monoclonal HuCAL Custom Monoclonal Antibodies Highly Specific, Recombinant Antibodies in 8 Weeks Highly Specific Monoclonal Antibodies in Just 8 Weeks HuCAL PLATINUM (Human Combinatorial Antibody
HuCAL Custom Monoclonal HuCAL Custom Monoclonal Antibodies Highly Specific, Recombinant Antibodies in 8 Weeks Highly Specific Monoclonal Antibodies in Just 8 Weeks HuCAL PLATINUM (Human Combinatorial Antibody
No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer
 APPLICATION NOTE Attune NxT Flow Cytometer No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer Introduction Standard methods for isolating and detecting leukocytes
APPLICATION NOTE Attune NxT Flow Cytometer No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer Introduction Standard methods for isolating and detecting leukocytes
Custom Antibody Services
 prosci-inc.com Custom Antibody Services High Performance Antibodies and More Broad Antibody Catalog Extensive Antibody Services CUSTOM ANTIBODY SERVICES Established in 1998, ProSci Incorporated is a leading
prosci-inc.com Custom Antibody Services High Performance Antibodies and More Broad Antibody Catalog Extensive Antibody Services CUSTOM ANTIBODY SERVICES Established in 1998, ProSci Incorporated is a leading
Rheumatoid arthritis: an overview. Christine Pham MD
 Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
Using Drugs to Treat Drug Addiction How it works and why it makes sense
 Using Drugs to Treat Drug Addiction How it works and why it makes sense Jeff Baxter, MD University of Massachusetts Medical School May 17, 2011 Objectives Biological basis of addiction Is addiction a chronic
Using Drugs to Treat Drug Addiction How it works and why it makes sense Jeff Baxter, MD University of Massachusetts Medical School May 17, 2011 Objectives Biological basis of addiction Is addiction a chronic
Mouse IFN-gamma ELISpot Kit
 Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
Update and Review of Medication Assisted Treatments
 Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Introduction to flow cytometry
 Introduction to flow cytometry Flow cytometry is a popular laser-based technology. Discover more with our introduction to flow cytometry. Flow cytometry is now a widely used method for analyzing the expression
Introduction to flow cytometry Flow cytometry is a popular laser-based technology. Discover more with our introduction to flow cytometry. Flow cytometry is now a widely used method for analyzing the expression
Treatment Approaches for Drug Addiction
 Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call 1-800-662-HELP(4357)
Treatment Approaches for Drug Addiction NOTE: This is a fact sheet covering research findings on effective treatment approaches for drug abuse and addiction. If you are seeking treatment, please call 1-800-662-HELP(4357)
低 剂 量 辐 射 对 脐 血 T 淋 巴 细 胞 膜 分 子 表 达 的 影 响 EFFECT OF LOW DOSE IRRADIATION ON EXPRESSION OF MEMBRANE MOLECULES OF T LYMPHOCYTES IN CORD BLOOD
 CNIC-01513 PUTH-0001 低 剂 量 辐 射 对 脐 血 T 淋 巴 细 胞 膜 分 子 表 达 的 影 响 EFFECT OF LOW DOSE IRRADIATION ON EXPRESSION OF MEMBRANE MOLECULES OF T LYMPHOCYTES IN CORD BLOOD 中 国 核 情 报 中 心 China Nuclear Information
CNIC-01513 PUTH-0001 低 剂 量 辐 射 对 脐 血 T 淋 巴 细 胞 膜 分 子 表 达 的 影 响 EFFECT OF LOW DOSE IRRADIATION ON EXPRESSION OF MEMBRANE MOLECULES OF T LYMPHOCYTES IN CORD BLOOD 中 国 核 情 报 中 心 China Nuclear Information
Fighting the Battles: Conducting a Clinical Assay
 Fighting the Battles: Conducting a Clinical Assay 6 Vocabulary: In Vitro: studies in biology that are conducted using components of an organism that have been isolated from their usual biological surroundings
Fighting the Battles: Conducting a Clinical Assay 6 Vocabulary: In Vitro: studies in biology that are conducted using components of an organism that have been isolated from their usual biological surroundings
Dependence and Addiction. Marek C. Chawarski, Ph.D. Yale University David Metzger, Ph.D. University of Pennsylvania
 Dependence and Addiction Marek C. Chawarski, Ph.D. Yale University David Metzger, Ph.D. University of Pennsylvania Overview Heroin and other opiates The disease of heroin addiction or dependence Effective
Dependence and Addiction Marek C. Chawarski, Ph.D. Yale University David Metzger, Ph.D. University of Pennsylvania Overview Heroin and other opiates The disease of heroin addiction or dependence Effective
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS
 CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: immune_cell_function_assay 11/2009 3/2016 3/2017 3/2016 Description of Procedure or Service Careful monitoring
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: immune_cell_function_assay 11/2009 3/2016 3/2017 3/2016 Description of Procedure or Service Careful monitoring
Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual
 Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual INSTRUCTION MANUAL ZBM0065.03 SHIPPING CONDITIONS Human Umbilical Cord Blood CD34+ Progenitor Cells, cryopreserved Cryopreserved human umbilical
Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual INSTRUCTION MANUAL ZBM0065.03 SHIPPING CONDITIONS Human Umbilical Cord Blood CD34+ Progenitor Cells, cryopreserved Cryopreserved human umbilical
Pulling the Plug on Cancer Cell Communication. Stephen M. Ansell, MD, PhD Mayo Clinic
 Pulling the Plug on Cancer Cell Communication Stephen M. Ansell, MD, PhD Mayo Clinic Why do Waldenstrom s cells need to communicate? Waldenstrom s cells need activating signals to stay alive. WM cells
Pulling the Plug on Cancer Cell Communication Stephen M. Ansell, MD, PhD Mayo Clinic Why do Waldenstrom s cells need to communicate? Waldenstrom s cells need activating signals to stay alive. WM cells
OPIOIDS. Petros Levounis, MD, MA Chair Department of Psychiatry Rutgers New Jersey Medical School
 OPIOIDS Petros Levounis, MD, MA Chair Department of Psychiatry Rutgers New Jersey Medical School Rutgers New Jersey Medical School Fundamentals of Addiction Medicine Summer Series Newark, NJ July 24, 2013
OPIOIDS Petros Levounis, MD, MA Chair Department of Psychiatry Rutgers New Jersey Medical School Rutgers New Jersey Medical School Fundamentals of Addiction Medicine Summer Series Newark, NJ July 24, 2013
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
Asthma (With a little SCID to start) Disclosures Outline Starting with the Immune System The Innate Immune System The Adaptive Immune System
 1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
SUMMARY OF RECOMMENDATIONS
 SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
SUMMARY OF RECOMMENDATIONS FOR THE LONG- TERM TREATMENT OF RLS/WED from AN IRLSSG TASK FORCE Members of the Task Force Diego Garcia- Borreguero, MD, Madrid, Spain* Richard Allen, PhD, Baltimore, MD, USA*
Developmental Validation of a Novel Lateral Flow Strip Test for Rapid Identification of Human Blood, Rapid Stain Identification-Blood, RSID -Blood
 Developmental Validation of a Novel Lateral Flow Strip Test for Rapid Identification of Human Blood, Rapid Stain Identification-Blood, RSID -Blood Dr. Brett A. Schweers, Dr. Jennifer Old, Dr. P.W. Boonlayangoor
Developmental Validation of a Novel Lateral Flow Strip Test for Rapid Identification of Human Blood, Rapid Stain Identification-Blood, RSID -Blood Dr. Brett A. Schweers, Dr. Jennifer Old, Dr. P.W. Boonlayangoor
CONTENT. Chapter 1 Review of Literature. List of figures. List of tables
 Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
