RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF UNIVERSITY OF NORTH CAROLINA HOSPITALS
|
|
|
- Iris O’Brien’
- 8 years ago
- Views:
Transcription
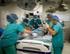
1 RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF UNIVERSITY OF NORTH CAROLINA HOSPITALS Approved by the Executive Committee of the Medical Staff, November 5, Approved and adopted by the Board of Directors, University of North Carolina Health Care System, November 16, 2001, effective December 5, Amended effective January 22, Amended effective May 20, Amended effective July 15, Amended effective March 17, Amended effective May 19, Amended effective January 18, Amended effective September 26, Amended effective March 19, Amended effective November 8, 2010 Amended effective March 19, 2012 Amended effective November 11, 2013 Amended effective March 10, 2014 Amended effective May 18,
2 RULES AND REGULATIONS OF THE BYLAWS OF THE MEDICAL STAFF THE UNIVERSITY OF NORTH CAROLINA HOSPITALS 1. The meetings of the Medical Staff shall be held as provided in Article XII of the Bylaws of the Medical Staff. 2. Patients may be treated only by physicians and dentists who have been duly appointed to membership on the Medical Staff and by Allied Health Professionals with practice privileges. All hospitalized patients shall be attended by a member of the Medical Staff and shall be assigned to the service concerned with the treatment of the patient s disease. The Medical Staff shall be responsible for supervising Housestaff in the provision of care to patients under their care. 2(a) All individuals presenting to a UNC Hospitals dedicated emergency department (as defined by law and in policy) for examination or treatment shall be given an appropriate medical screening examination (MSE) by qualified medical personnel (QMP) to determine if an emergency medical condition exists. QMP include physicians, physician assistants, nurse practitioners, and midwives (for labor and delivery patients only). 3. Each member of the Medical Staff who is not a resident in the city or immediate vicinity shall name a member of the Medical Staff who is a resident of the city or immediate vicinity, who may be called to attend his/her patients in an emergency. In case of failure to name such an associate, the Department Chair involved or the Chief Medical Officer shall have authority to request any member of the Medical Staff to substitute. In the anticipated absence of a member of the Medical Staff, s/he shall designate another member of the Medical Staff to attend his/her patients. In the case of failure to do so, the Department Chair involved or the Chief Medical Officer shall have the authority and responsibility to designate a member of the Medical Staff to substitute. 4. Except in emergency situations, no patient shall be admitted to the Hospital until a provisional diagnosis has been stated. In case of emergency, the provisional diagnosis shall be stated as soon as possible after admission. 5. Medical Staff members admitting patients shall be held responsible for giving such information as may be necessary to assure the protection of other patients from potential sources of danger from any causes whatsoever, or to assure protection of the patient from self-harm. All Medical Staff and Housestaff physicians and Allied Health Professionals will practice according to Hospitals policies on restraint and seclusion. 6. Each patient admitted for inpatient care or outpatient surgery shall have a history taken and a comprehensive physical examination (H&P) performed by an attending physician or by a Housestaff physician or Allied Health Professional with such privileges and authenticated by the attending physician. Qualified oral surgeons who admit patients without medical problems may perform the history and physical examination on those patients. An H&P shall be completed for the electronic medical record no more than twenty-four (24) hours prior to a scheduled admission or outpatient surgery or within twenty-four (24) hours after emergency surgery (the Required Period ). In an emergency when there is no time to record a complete H&P, a progress or admission note describing a brief history and appropriate physical findings and the preoperative - 2 -
3 diagnosis is recorded in the medical record before surgery. If all or part of the H&P is dictated, then a brief note shall be written in the record on the progress notes or typed directly in the electronic medical record upon admission to provide pertinent information until the dictated H&P is transcribed. An H&P may be performed outside the Required Period, but within thirty (30) days prior to a scheduled admission or outpatient surgery, if an updated assessment is subsequently both performed and documented during the Required Period that identifies any changes in the patient s medical status or that no changes have occurred. 7. When a history and physical examination is not recorded before the time stated for a surgical operation, the operation shall be canceled unless the attending surgeon documents in the patient s medical record that such a delay would constitute a hazard to the patient. 8. Standing orders are pre-written physician orders to address specific clinical scenarios involving the administration of medications and/or biologicals which have been approved as meeting nationally recognized evidence-based guidelines by the Medical Staff Executive Committee. Upon implementation of a standing order by authorized clinical personnel, the patient s physician is notified, and a licensed independent practitioner must authenticate the order with signature, date, and time within three (3) business days of implementation. In the inpatient setting, the only exceptions to authentication are standing orders for influenza and pneumococcal vaccines. In the outpatient setting, standing orders for immunizations do not require physician authentication. 9. Standing orders, order sets, physician protocols, automatic stop orders, and routine laboratory and radiographic studies shall be formulated, approved or modified by the Executive Committee for the Medical Staff upon recommendations by Department Chairs or Medical Staff Committees. Physician protocols for routine laboratory tests and/or radiographic studies may be performed by appropriate healthcare personnel as per the protocol, but do not require authentication by a licensed independent practitioner. 10. All orders for treatment shall be in writing and signed by the physician, dentist, allied health professional with such privileges, or the designated member of the Housestaff responsible for the patient. Signature stamps are prohibited. Entries in the medical record by Housestaff or allied health professionals that require countersigning by supervisory or attending Medical Staff members include: operative reports, procedure notes, admission history and physical, daily progress notes, discharge summaries, 48- hour final progress notes, pre-anesthesia record, anesthesia record, post-anesthesia note, pre-op note, and post-op note if stay is greater than 48 hours. A verbal order shall be considered to be in writing if it is dictated by a licensed physician, dentist, or allied health professional with such privileges to a licensed nurse or other licensed or registered person functioning in his/her sphere of competence; i.e., Occupational Therapist for Occupational Therapy treatment; Physical Therapist for Physical Therapy treatment; Respiratory Therapist for Respiratory Therapy treatment, and signed by an appropriate licensed Practitioner. Orders dictated over the telephone shall be signed by the appropriate authorized person to whom dictated and should indicate the name of the Practitioner who gave the order. The Practitioner giving the order shall authenticate such verbal orders within forty-eight (48) hours. If automated systems are introduced, these requirements shall be considered met if the approved system is used
4 10(a) Before a patient may be transferred from one inpatient service (i.e. physician care team) to another, whether or not there is a change in acuity level of care, either the transferring team or the accepting team must write a new, full set of treatment orders. Which team will write transfer orders should be determined on a case-by-case basis, after considering the needs of both the patient being transferred and any patient known to need the vacated bed. In those instances when orders are written by the transferring team, when the patient arrives on the receiving Hospital unit the nursing staff of that unit will promptly notify a physician on the accepting team. The accepting team is expected to countersign, and/or amend as deemed appropriate, the treatment orders in a timely manner that meets the care needs of the transferred patient. The accepting team will notify the nursing staff as soon as it has countersigned the orders. Until the accepting team countersigns the treatment orders, the transferring team will remain responsible for the patient s orders and will remain the first point of contact for the receiving unit nursing staff. EXCEPTION: In those instances when a patient is transferred from one inpatient service (i.e. physician care team) to another AND both the prior Hospital unit and the receiving Hospital unit use the computerized provider order entry (CPOE) system the accepting care team may simply enter a transfer order. It is expected that this accepting care team will amend orders as appropriate. This exception applies whether or not there is a concomitant change in acuity level of care. 10(b) In those instances when a patient is transferred from one acuity level to another but continues to receive care from the same service, the care team must write a new, full set of treatment orders, UNLESS both the prior Hospital unit and the receiving Hospital unit use the computerized provider order entry (CPOE) system. In that case the care team may simply enter a transfer order. It is expected that the team will amend orders as appropriate in the context of the change in acuity level. 11. In all cases, except as noted below, surgical procedures shall be performed only with the prior informed written consent of the patient or his/her legal representative. Obtaining such consent shall be the responsibility of the surgeon. Generally, such consent shall be in writing. However, consent may be obtained by witnessed telephone authorization. In cases of emergency operations, when consent cannot be obtained, such operations will be performed only in accordance with the Hospital s policy on Consent for Emergency Surgical and/or Medical Treatment. The surgeon shall record in writing in the patient s medical record the reasons why consent could not be obtained and the need for the operation, with the need concurred with by one (1) other attending physician and so documented in the patient s medical record. 12. All operations performed shall be fully described in writing by the operating surgeon. All specimens removed during a surgical procedure, or tissue passed vaginally in the case of a miscarriage, shall be properly labeled and shall be sent to the pathologist (except as covered in a-g below), who shall make such examinations as are considered necessary and record his/her observations and interpretations in a signed report. In certain cases where special studies are indicated, arrangements will be made between the pathologist, surgeon, and special laboratory concerned, with appropriate notation made in the medical record. A signed copy of the pathology report shall be filed timely in the medical record. Exceptions to the requirement of pathologic examination of specimens removed during a surgical procedure are made only when the quality of care has not been compromised by the exception, when another suitable means of verification of the removal has been routinely used, and when there is an authenticated operative or other official report that documents the removal. The limited categories of - 4 -
5 specimens that may be exempted from pathologic examination include, but are not necessarily limited to, the following: (It should be noted that any specimen on which pathologic examination is requested will be examined by Surgical Pathology irrespective of the exclusions). a. Specimens that by their nature or condition do not permit fruitful examination, such as an orthopedic or other exogenous appliance, foreign body, or portion of bone or cartilage removed only to enhance operative exposure; (however, it is strongly recommended that where such specimen(s) constitute a component(s) of a specimen requiring pathologic examination, all of this material should be submitted); b. Therapeutic radioactive sources, the removal of which should be guided by radiation safety monitoring requirements; c. Foreign bodies (e.g., bullets) that for legal reasons are given directly in the chain of custody to law enforcement representatives; d. Certain specimens known rarely, if ever, to show pathological change, and the removal of which is highly visible post-operative, (e.g., foreskin from circumcision of newborn infants, tissue removed during nasal septoplasty, cosmetic surgery involving removal of essentially non-pathologic material); e. Placentas that are grossly normal and have been removed in the course of operative and non-operative obstetrics; f. Teeth, provided the number, including fragments, are recorded in the medical record; and g. Crystalline lenses removed following either intracapsular or extracapsular cataract removal; and in cases where no specimen was removed, the surgical case review is the responsibility of the individual department. Documentation should include the indications for surgery and all cases in which there is a major discrepancy between the preoperative and postoperative diagnosis. 13. Surgeons and all other personnel involved must be in the operating rooms and ready to begin operating at the time scheduled. The operating room will not be held longer than fifteen (15) minutes after the time scheduled. 14. Patients shall be discharged only on written order of the responsible physician or his/her designee. At the time of discharge the attending physician or his/her designee shall take appropriate action to resolve all active orders, see that the record is complete, state the final diagnosis, and sign the record. 15. All inpatients must be seen and reevaluated within 24 hours of admission and then daily by a Licensed Independent Practitioner (LIP) (e.g., attending physician, resident physician, nurse practitioner, physician assistant). A progress note shall be entered in the medical record daily, and countersigned by the attending physician. The note should include the plan of care and reflect the active involvement of the attending physician
6 16. For each outpatient clinic visit, the attending physician or Allied Health Professional is responsible for the preparation of a complete visit record for each patient in accordance with the completion requirements established by the Clinical Documentation Committee (CDC). The attending physician will ensure that s/he and all Housestaff under the attending physician s supervision have completed all chart requirements within three (3) business days after the date of service. The Allied Health Professional will complete all chart requirements within three (3) business days after the date of service. 17. The attending physician shall be held responsible for the preparation of a complete medical record for each patient in accordance with the completion requirements established by the Clinical Documentation Committee. The attending physician shall insure that s/he and all Housestaff under his/her supervision have completed all chart requirements within at most fourteen (14) days after discharge. The Clinical Documentation Committee, with approval by the Medical Staff Executive Committee may institute time requirements for the completion of medical records which define delinquent records at a time prior to fourteen (14) days after discharge. A clinical summary shall be dictated in the medical record at discharge by the responsible physician for all patients, except as specified below. A Final Progress Note may be substituted for a discharge summary in the case of patients with problems of a minor nature who require less than a forty-eight (48) hour period of hospitalization and in the case of newborn infants and uncomplicated obstetrical deliveries. It will be the responsibility of the Clinical Documentation Committee to determine those specific situations which may be considered to be in this minor category. Operative reports shall be dictated or written in the medical record immediately after surgery and contain a description of the findings, the technical procedures used, the specimen removed, the postoperative diagnosis, and the name of the primary surgeon and any assistants. If the dictation is not done, the Department Chair or Division Chief will be notified. A brief Operative Note shall be written in the Progress Notes immediately after surgery to provide pertinent information until the dictated Operative Report is transcribed. When an autopsy is performed, a provisional anatomic diagnosis is forwarded within two (2) working days to the Medical Information Management Department for inclusion in the medical record. The final autopsy report will be considered delinquent if it has not been dictated and signed by the responsible pathologist within sixty (60) days after the death of the patient. 18. Each clinical Department Chair, or his/her designee, may administratively reassign the clinical duties of Medical Staff and Housestaff physicians and Allied Health Professionals to enable those Practitioners with delinquent medical records, as defined by the Medical Information Management Committee, to complete such delinquent records. Each Clinical Department Chair, or his/her designee, may also administratively reassign the clinical duties of Medical Staff and Housestaff physicians and Allied Health Professionals to enable those Practitioners who have not demonstrated compliance with OSHA, CDC or other Hospital safety requirements to demonstrate such compliance. This procedure is an administrative mechanism, distinct from corrective action as authorized by Article V of the Policy on Appointment and Corrective Action. Such administrative reassignment shall not be considered Corrective Action against Medical Staff physicians, or disciplinary action against a Housestaff physician or Allied Health Professional. However, repeated administrative reassignments which have the effect of being detrimental to the operations of the Hospital may subject a Medical Staff physician to Corrective Action or a Housestaff physician or Allied Health Professional to disciplinary action. Pursuant to an administrative reassignment, Medical Staff and Housestaff physicians and Allied Health Professionals shall not be permitted to schedule new clinic - 6 -
7 appointments and admissions, to schedule new surgical procedures or to use the Emergency Department until all delinquent medical records are completed. A Housestaff physician shall, among other appropriate actions, be removed from all clinical activities and be required to utilize annual leave until all delinquent medical records are completed. 19. No autopsy shall be performed without consent of the legally authorized individual. Generally, such permission should be in writing. However, consent may be obtained by recorded and witnessed telephone authorization. The Chair of the Department of Pathology and Laboratory Medicine, or his/her designated assistant, shall be responsible for the performance of all autopsies on patients dying in the Hospital, except in those cases where the Medical Examiner has jurisdiction. 20. Postmortem tissue and organ donation will be conducted in accordance with the Uniform Anatomical Gift Act. When a tissue or organ of the donor is to be removed for transplantation pursuant to the Uniform Anatomical Gift Act, and the death of the donor is established by a determination that the person has suffered a total and irreversible cessation of brain function, the pronouncement of death is made by the patient s attending physician, or his/her substitute attending physician, or the Housestaff in consultation with an attending physician. The physicians making the determination of death shall not participate in the procedures for removing or transplanting a tissue or organ. 21. Consultation with the Obstetrical service is required when a known pregnant woman is admitted to a service other than Family Medicine or Obstetrics and Gynecology. A preoperative consultation with the Obstetrical service is also required when an inpatient or outpatient operative or other interventional procedure requiring moderate or deep sedation or anesthesia is planned for a known pregnant woman. This consultation should be requested at the time of surgical scheduling. 22. Except in an emergency, consultations with another qualified physician are required in: a. Curettages or other procedures by which a known or suspected pregnancy of greater than 20 weeks duration from the last menstrual cycle may be interrupted; b. Cases in which according to the judgment of the physician: (1) The patient is not a good risk for operation or treatment; (2) The diagnosis is obscure; or (3) There is doubt as to the best therapeutic measure to be utilized. In general, only physicians who are members of the Medical Staff of the Hospital or properly supervised designees shall serve as consultants. However, in special situations, qualified physicians not on the Medical Staff of this Hospital may be invited to visit a patient, as well as observe the course of treatment, provided the Chair of the appropriate Department, the Chief Medical Officer or his/her designee, gives permission. Such a consultant shall not assume responsibilities for the patient. A member of the Medical Staff inviting such a consultant shall notify the Chair of the appropriate Department or the Chief Medical Officer in each case and shall assume responsibility for adherence to this rule
8 The patient s physician is responsible for requesting consultations when indicated. It is the duty of the Medical Staff through its Department Chairs or Service Heads and Executive Committee to make certain that members of the Staff do not fail in the matter of requesting consultations when needed. All patients for whom an inpatient consultation is requested shall be seen and examined by a Licensed Independent Practitioner (LIP) (e.g., attending physician, resident physician, nurse practitioner, physician assistant). A written opinion must be documented in the medical record within 24 hours of the request. The consultant s assessment should reflect the active involvement of the attending physician, which may be in person or by phone. When operative procedures are involved, the consultation note, except in emergency, shall be recorded prior to the operation. 23. Each Clinical Department must ensure the availability of schedules or instructions in WebXchange that inform all members of the health care team of attending physicians and residents currently responsible for each patient s care. 24. Drugs used shall be among those listed in the Hospital Formulary as amended by the Pharmacy and Therapeutics Committee, with the exception of drugs for bona fide clinical investigations. Deviation from this rule shall be well justified and shall be reported to the Pharmacy and Therapeutics Committee for review. The metric system shall be used in prescription and drug orders. Nonproprietary (generic) rather than trade and proprietary nomenclature shall be used. However, certain products of multiple composition are metered in the Formulary under a recognized generic or trade name titled with the composition listed. The Department of Pharmacy may dispense the exact chemical equivalent (labeled in non proprietary terms) for those drugs ordered under a trade or proprietary name in the treatment of inpatients and outpatients. However, if any physician or dentist considers an exception to this policy is indicated for a particular patient, s/he should consult with the senior pharmacist on duty. Only those abbreviations which have been approved by the Clinical Documentation Committee shall be used in medication orders. 25. All Schedule II controlled substances and other drugs as recommended by the Pharmacy and Therapeutics Committee that are ordered without time limitations of dosage shall be automatically discontinued after seven (7) days. Drugs should not be discontinued without notifying the physician or dentist. If the order expires in the night, it should be continued until the next morning and called to the attention of the physician or dentist the following morning. 26. Mass Casualty Assignments. Physicians shall be assigned responsibilities as defined in the Hospital s Disaster Plan. 27. Other rules which have been adopted by the Executive Committee of the Medical Staff will be found in the Hospital Policy Manual. Amendments These Rules and Regulations may be amended as provided in Article XVI of the Medical Staff Bylaws
9 - 9 -
AKRON CHILDREN'S HOSPITAL MEDICAL STAFF BYLAWS, POLICIES, AND RULES AND REGULATIONS MEDICAL STAFF RULES AND REGULATIONS
 AKRON CHILDREN'S HOSPITAL MEDICAL STAFF BYLAWS, POLICIES, AND RULES AND REGULATIONS MEDICAL STAFF RULES AND REGULATIONS July 1, 2012 GENERAL RULES G1. Patients shall be attended by their own private Medical
AKRON CHILDREN'S HOSPITAL MEDICAL STAFF BYLAWS, POLICIES, AND RULES AND REGULATIONS MEDICAL STAFF RULES AND REGULATIONS July 1, 2012 GENERAL RULES G1. Patients shall be attended by their own private Medical
Canyon Vista Medical Center
 Department: MEDICAL STAFF Page 1 of 14 INTRODUCTION: 1. This document sets forth the Rules and Regulations of the Medical Staff and is subject to the provisions of the Medical Staff Bylaws. The terms defined
Department: MEDICAL STAFF Page 1 of 14 INTRODUCTION: 1. This document sets forth the Rules and Regulations of the Medical Staff and is subject to the provisions of the Medical Staff Bylaws. The terms defined
How To Write A Medical Record
 RULES AND REGULATIONS OF THE MEDICAL STAFFS OF NORTH BROWARD HOSPITAL DISTRICT April 2006 RULES AND REGULATIONS OF THE MEDICAL STAFFS OF THE NORTH BROWARD HOSPITAL DISTRICT TABLE OF CONTENTS PAGE I. RULES
RULES AND REGULATIONS OF THE MEDICAL STAFFS OF NORTH BROWARD HOSPITAL DISTRICT April 2006 RULES AND REGULATIONS OF THE MEDICAL STAFFS OF THE NORTH BROWARD HOSPITAL DISTRICT TABLE OF CONTENTS PAGE I. RULES
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION
 LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION Hospital Policy Manual Purpose: To define the components of the paper and electronic medical record
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT MEDICAL RECORDS CONTENT/DOCUMENTATION Hospital Policy Manual Purpose: To define the components of the paper and electronic medical record
Medical Staff Rules & Regulations Last Updated: January 2013. University Hospital Medical Staff. Rules & Regulations
 University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
University Hospital Medical Staff Rules & Regulations 1 UNIVERSITY HOSPITAL MEDICAL STAFF RULES AND REGULATIONS The Medical Staff shall adopt Rules and Regulations as may be necessary to implement the
SAINT FRANCIS HOSPITAL AND MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS
 SAINT FRANCIS HOSPITAL AND MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS: ARTICLE I INTRODUCTION 1.1 Definitions 1.2 Applicability 1.3 Conflict with Hospital Policies 1.4 Departmental
SAINT FRANCIS HOSPITAL AND MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS: ARTICLE I INTRODUCTION 1.1 Definitions 1.2 Applicability 1.3 Conflict with Hospital Policies 1.4 Departmental
CAROLINAS REHABILITATION
 CAROLINAS REHABILITATION CURRENT LANGUAGE ORGANIZATIONAL MANUAL OF BYLAWS OF CAROLINAS REHABILITATION (TAB 2) New Language ORGANIZATIONAL MANUAL OF BYLAWS OF CAROLINAS REHABILITATION (TAB 2) ARTICLE II
CAROLINAS REHABILITATION CURRENT LANGUAGE ORGANIZATIONAL MANUAL OF BYLAWS OF CAROLINAS REHABILITATION (TAB 2) New Language ORGANIZATIONAL MANUAL OF BYLAWS OF CAROLINAS REHABILITATION (TAB 2) ARTICLE II
SECTION IV RULES AND REGULATIONS SECTION OF THE BYLAWS MEDICAL AND DENTAL STAFF CAROLINAS MEDICAL CENTER-UNIVERSITY
 SECTION IV RULES AND REGULATIONS SECTION OF THE BYLAWS MEDICAL AND DENTAL STAFF CAROLINAS MEDICAL CENTER-UNIVERSITY APPROVED BY THE BYLAWS COMMITTEE - 08-14-96 APPROVED BY THE MEDICAL AND DENTAL STAFF
SECTION IV RULES AND REGULATIONS SECTION OF THE BYLAWS MEDICAL AND DENTAL STAFF CAROLINAS MEDICAL CENTER-UNIVERSITY APPROVED BY THE BYLAWS COMMITTEE - 08-14-96 APPROVED BY THE MEDICAL AND DENTAL STAFF
RULES AND REGULATIONS OF THE MEDICAL STAFF UNIVERSITY OF COLORADO HOSPITAL
 RULES AND REGULATIONS OF THE MEDICAL STAFF UNIVERSITY OF COLORADO HOSPITAL I. PREAMBLE... 2 II. INDIVIDUAL RESPONSIBILITIES... 2 A. CARE OF PATIENTS... 2 B. ANESTHESIA AND SEDATION... 5 C. EMERGENCY CARE...
RULES AND REGULATIONS OF THE MEDICAL STAFF UNIVERSITY OF COLORADO HOSPITAL I. PREAMBLE... 2 II. INDIVIDUAL RESPONSIBILITIES... 2 A. CARE OF PATIENTS... 2 B. ANESTHESIA AND SEDATION... 5 C. EMERGENCY CARE...
POLICY and PROCEDURE. TITLE: Documentation Requirements for the Medical Record. TITLE: Documentation Requirements for the Medical Record
 POLICY and PROCEDURE TITLE: Documentation Requirements for the Medical Record Number: 13289 Version: 13289.1 Type: Administrative - Medical Staff Author: Joan Siler Effective Date: 8/16/2011 Original Date:
POLICY and PROCEDURE TITLE: Documentation Requirements for the Medical Record Number: 13289 Version: 13289.1 Type: Administrative - Medical Staff Author: Joan Siler Effective Date: 8/16/2011 Original Date:
STANFORD HOSPITAL AND CLINICS Medical Staff Rules and Regulations. Last Approval Date: May 2014
 STANFORD HOSPITAL AND CLINICS Medical Staff Rules and Regulations Last Approval Date: May 2014 The Medical Staff is responsible to the Stanford Hospital and Clinics (SHC) Board of Directors for the professional
STANFORD HOSPITAL AND CLINICS Medical Staff Rules and Regulations Last Approval Date: May 2014 The Medical Staff is responsible to the Stanford Hospital and Clinics (SHC) Board of Directors for the professional
THE ORTHOPEDIC HOSPITAL RULES & REGULATIONS INDEX
 P a g e 1 THE ORTHOPEDIC HOSPITAL RULES & REGULATIONS INDEX PAGES ARTICLE I ADMISSION & DISCHARGE OF PATIENTS 1.1 ADMISSION OF PATIENTS 3 1.2 ADMITTING POLICY 4 1.3 SUICIDAL PATIENTS 4 1.4 DISCHARGE OF
P a g e 1 THE ORTHOPEDIC HOSPITAL RULES & REGULATIONS INDEX PAGES ARTICLE I ADMISSION & DISCHARGE OF PATIENTS 1.1 ADMISSION OF PATIENTS 3 1.2 ADMITTING POLICY 4 1.3 SUICIDAL PATIENTS 4 1.4 DISCHARGE OF
Rehabilitation Hospital Rules and Regulations
 Rehabilitation Hospital Rules and Regulations REHABILITATION HOSPITAL OF FORT WAYNE MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS A. ADMISSION AND DISCHARGE OF PATIENTS...2 B. MEDICAL RECORDS...4
Rehabilitation Hospital Rules and Regulations REHABILITATION HOSPITAL OF FORT WAYNE MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS A. ADMISSION AND DISCHARGE OF PATIENTS...2 B. MEDICAL RECORDS...4
FAIRFIELD MEDICAL CENTER MEDICAL STAFF RULES, REGULATIONS AND POLICIES MANUAL
 FAIRFIELD MEDICAL CENTER MEDICAL STAFF RULES, REGULATIONS AND POLICIES MANUAL RULES, REGULATIONS AND POLICIES MANUAL OF THE MEDICAL STAFF FAIRFIELD MEDICAL CENTER TABLE OF CONTENTS PART ONE DEFINITIONS...
FAIRFIELD MEDICAL CENTER MEDICAL STAFF RULES, REGULATIONS AND POLICIES MANUAL RULES, REGULATIONS AND POLICIES MANUAL OF THE MEDICAL STAFF FAIRFIELD MEDICAL CENTER TABLE OF CONTENTS PART ONE DEFINITIONS...
How To Get A Medical License In The United States
 RULES AND REGULATIONS OF THE MEDICAL STAFF 1. Only physicians who have submitted proper credentials and have been duly appointed to membership on the Medical Staff shall be permitted to admit and treat
RULES AND REGULATIONS OF THE MEDICAL STAFF 1. Only physicians who have submitted proper credentials and have been duly appointed to membership on the Medical Staff shall be permitted to admit and treat
MEDICAL STAFF RULES & REGULATIONS
 MEDICAL STAFF RULES & REGULATIONS PURPOSE: Rules and Regulations shall set standards of practice that are to be required of each individual exercising clinical privileges in the hospital, and shall act
MEDICAL STAFF RULES & REGULATIONS PURPOSE: Rules and Regulations shall set standards of practice that are to be required of each individual exercising clinical privileges in the hospital, and shall act
1. PATIENT TYPES AND ADMISSION OF PATIENTS. A. Description
 LUCILE PACKARD CHILDREN S HOSPITAL Medical Staff Rules and Regulations Last Approval Date: Jan 2014 The purpose of the Lucile Packard Children's Hospital (LPCH) is to furnish quality medical care, treatment
LUCILE PACKARD CHILDREN S HOSPITAL Medical Staff Rules and Regulations Last Approval Date: Jan 2014 The purpose of the Lucile Packard Children's Hospital (LPCH) is to furnish quality medical care, treatment
JOHN C LINCOLN MEDICAL STAFF RULES AND REGULATIONS
 JOHN C LINCOLN MEDICAL STAFF RULES AND REGULATIONS Jan 2016 0 Table of Contents 1.0 RESPONSIBILITY 1 1.1 General 1 1.2 Patient Safety 2 1.3 Consideration for Suicidal Patients 2 1.4 Consideration for Suspected
JOHN C LINCOLN MEDICAL STAFF RULES AND REGULATIONS Jan 2016 0 Table of Contents 1.0 RESPONSIBILITY 1 1.1 General 1 1.2 Patient Safety 2 1.3 Consideration for Suicidal Patients 2 1.4 Consideration for Suspected
ARTICLE X: RULES AND REGULATIONS
 ARTICLE X: RULES AND REGULATIONS The Medical Staff shall adopt such rules and regulations as necessary for the proper conduct of its work. Such rules and regulations may be a part of these bylaws except
ARTICLE X: RULES AND REGULATIONS The Medical Staff shall adopt such rules and regulations as necessary for the proper conduct of its work. Such rules and regulations may be a part of these bylaws except
MEDICAL STAFF RULES AND REGULATIONS
 MEDICAL STAFF RULES AND REGULATIONS Approved by Board of Directors: TABLE OF CONTENTS PAGE 1. GENERAL... 3 2. ADMISSION AND DISCHARGE... 3 3. CRITICAL CARE UNITS... 4 4. EMERGENCY SERVICES... 5 5. MEDICAL
MEDICAL STAFF RULES AND REGULATIONS Approved by Board of Directors: TABLE OF CONTENTS PAGE 1. GENERAL... 3 2. ADMISSION AND DISCHARGE... 3 3. CRITICAL CARE UNITS... 4 4. EMERGENCY SERVICES... 5 5. MEDICAL
RULES AND REGULATIONS
 MEMORIAL HOSPITAL UNIVERSITY OF COLORADO HEALTH MEDICAL, DENTAL AND PODIATRIC STAFF BYLAWS, POLICIES, AND RULES AND REGULATIONS RULES AND REGULATIONS Updated March 23, 2011 This update reflects all revisions
MEMORIAL HOSPITAL UNIVERSITY OF COLORADO HEALTH MEDICAL, DENTAL AND PODIATRIC STAFF BYLAWS, POLICIES, AND RULES AND REGULATIONS RULES AND REGULATIONS Updated March 23, 2011 This update reflects all revisions
RULES AND REGULATIONS OF THE MEDICAL STAFF OF FORT HAMILTON HOSPITAL
 RULES AND REGULATIONS OF THE MEDICAL STAFF OF FORT HAMILTON HOSPITAL M E D I C A L S T F F R U L E S & Revised and Approved by the Board of Trustees 1-15-13 R E G U L A T I O N S MEDICAL STAFF RULES AND
RULES AND REGULATIONS OF THE MEDICAL STAFF OF FORT HAMILTON HOSPITAL M E D I C A L S T F F R U L E S & Revised and Approved by the Board of Trustees 1-15-13 R E G U L A T I O N S MEDICAL STAFF RULES AND
(HEALTH INFORMATION MANAGEMENT SERVICES (HIMS)) MEDICAL RECORDS POLICY AND PROCEDURE
 (HEALTH INFORMATION MANAGEMENT SERVICES (HIMS)) MEDICAL RECORDS POLICY AND PROCEDURE Adopted by the Medical Staff: July 27, 2009 Adopted by the Board of Directors: July 31, 2009 Amended by the Medical
(HEALTH INFORMATION MANAGEMENT SERVICES (HIMS)) MEDICAL RECORDS POLICY AND PROCEDURE Adopted by the Medical Staff: July 27, 2009 Adopted by the Board of Directors: July 31, 2009 Amended by the Medical
Interdisciplinary Admission Assessment and
 06/20/14 - Effective Definitions Policy Licensed Independent Practioner (LIP): Any individual permitted by law and UTMB to provide care and services without direction or supervision within the scope of
06/20/14 - Effective Definitions Policy Licensed Independent Practioner (LIP): Any individual permitted by law and UTMB to provide care and services without direction or supervision within the scope of
POLICY and PROCEDURE. TITLE: Documentation Requirements for the Medical Record
 POLICY and PROCEDURE TITLE: Documentation Requirements for the Medical Record Number: 13424 Version: 13424.5 Type: Administrative - Medical Staff Author: Martha Hoover Effective Date: 9/24/2014 Original
POLICY and PROCEDURE TITLE: Documentation Requirements for the Medical Record Number: 13424 Version: 13424.5 Type: Administrative - Medical Staff Author: Martha Hoover Effective Date: 9/24/2014 Original
RULES AND REGULATIONS. of the YALE-NEW HAVEN HOSPITAL, INC. for the MEDICAL STAFF JANUARY 27, 1982. (Revised to October 20 May 18, 20101)
 RULES AND REGULATIONS of the YALE-NEW HAVEN HOSPITAL, INC. for the MEDICAL STAFF JANUARY 27, 1982 (Revised to October 20 May 18, 20101) TABLE OF CONTENTS RULES & REGULATIONS ACCEPTANCE OF PATIENTS... -3-
RULES AND REGULATIONS of the YALE-NEW HAVEN HOSPITAL, INC. for the MEDICAL STAFF JANUARY 27, 1982 (Revised to October 20 May 18, 20101) TABLE OF CONTENTS RULES & REGULATIONS ACCEPTANCE OF PATIENTS... -3-
ALABAMA BOARD OF NURSING ADMINISTRATIVE CODE CHAPTER 610-X-5 ADVANCED PRACTICE NURSING COLLABORATIVE PRACTICE TABLE OF CONTENTS
 ALABAMA BOARD OF NURSING ADMINISTRATIVE CODE CHAPTER 610-X-5 ADVANCED PRACTICE NURSING COLLABORATIVE PRACTICE TABLE OF CONTENTS 610-X-5-.01 610-X-5-.02 610-X-5-.03 610-X-5-.04 610-X-5-.05 610-X-5-.06 610-X-5-.07
ALABAMA BOARD OF NURSING ADMINISTRATIVE CODE CHAPTER 610-X-5 ADVANCED PRACTICE NURSING COLLABORATIVE PRACTICE TABLE OF CONTENTS 610-X-5-.01 610-X-5-.02 610-X-5-.03 610-X-5-.04 610-X-5-.05 610-X-5-.06 610-X-5-.07
CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS
 I. INTRODUCTION CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS Advance registered nurse practitioners (ARNPs) and clinical nurse practitioners (CNPs) have their scope
I. INTRODUCTION CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS Advance registered nurse practitioners (ARNPs) and clinical nurse practitioners (CNPs) have their scope
TITLE: Processing Provider Orders: Inpatient and Outpatient
 POLICY and PROCEDURE TITLE: Processing Provider Orders: Inpatient and Outpatient Number: 13211 Version: 13211.3 Type: Patient Care Author: Janice Dinner; Provider Order Policy Committee Effective Date:
POLICY and PROCEDURE TITLE: Processing Provider Orders: Inpatient and Outpatient Number: 13211 Version: 13211.3 Type: Patient Care Author: Janice Dinner; Provider Order Policy Committee Effective Date:
MEDICAL STAFF RULES AND REGULATIONS
 MEDICAL STAFF RULES AND REGULATIONS ARTICLE I. PROFESSIONALISM 1.1 These rules and regulations are intended to provide comprehensive information to members of the Ambulatory Surgery Center in order for
MEDICAL STAFF RULES AND REGULATIONS ARTICLE I. PROFESSIONALISM 1.1 These rules and regulations are intended to provide comprehensive information to members of the Ambulatory Surgery Center in order for
PHYSICIAN ORDER POLICY
 PURPOSE: To clarify requirements and assure all physician orders are complete and valid for safe patient care SUPPORTIVE DATA: Medication: Prescribing and Ordering Procedure #790.25 RCW 18.164.011 and
PURPOSE: To clarify requirements and assure all physician orders are complete and valid for safe patient care SUPPORTIVE DATA: Medication: Prescribing and Ordering Procedure #790.25 RCW 18.164.011 and
South West Nova District Health Authority Medical Staff Rules and Regulations
 South West Nova District Health Authority Medical Staff Rules and Regulations These Rules and Regulations, adopted by the Medical Staff, have been developed by the District Medical Advisory Committee and
South West Nova District Health Authority Medical Staff Rules and Regulations These Rules and Regulations, adopted by the Medical Staff, have been developed by the District Medical Advisory Committee and
St. Luke's University Health Network RULES AND REGULATIONS OF THE MEDICAL STAFFS
 St. Luke's University Health Network RULES AND REGULATIONS OF THE MEDICAL STAFFS St. Luke's Hospital - Anderson St. Luke's Hospital Allentown-Bethlehem St. Luke's Hospital - Miners St. Luke's Hospital
St. Luke's University Health Network RULES AND REGULATIONS OF THE MEDICAL STAFFS St. Luke's Hospital - Anderson St. Luke's Hospital Allentown-Bethlehem St. Luke's Hospital - Miners St. Luke's Hospital
ALABAMA BOARD OF MEDICAL EXAMINERS ADMINISTRATIVE CODE CHAPTER 540-X-8 ADVANCED PRACTICE NURSES: COLLABORATIVE PRACTICE TABLE OF CONTENTS
 Medical Examiners Chapter 540-X-8 ALABAMA BOARD OF MEDICAL EXAMINERS ADMINISTRATIVE CODE CHAPTER 540-X-8 ADVANCED PRACTICE NURSES: COLLABORATIVE PRACTICE TABLE OF CONTENTS 540-X-8-.01 540-X-8-.02 540-X-8-.03
Medical Examiners Chapter 540-X-8 ALABAMA BOARD OF MEDICAL EXAMINERS ADMINISTRATIVE CODE CHAPTER 540-X-8 ADVANCED PRACTICE NURSES: COLLABORATIVE PRACTICE TABLE OF CONTENTS 540-X-8-.01 540-X-8-.02 540-X-8-.03
PLEASE NOTE. For more information concerning the history of these regulations, please see the Table of Regulations.
 PLEASE NOTE This document, prepared by the Legislative Counsel Office, is an office consolidation of this regulation, current to February 12, 2011. It is intended for information and reference purposes
PLEASE NOTE This document, prepared by the Legislative Counsel Office, is an office consolidation of this regulation, current to February 12, 2011. It is intended for information and reference purposes
RULES AND REGULATIONS
 DESERT REGIONAL MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS ADOPTED: MAY 1993 REVISED: November 2014 Page 1 of 19 CONTENTS INTRODUCTION... 3 A. ADMISSION AND TREATMENT OF PATIENTS... 3 B. ALLIED
DESERT REGIONAL MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS ADOPTED: MAY 1993 REVISED: November 2014 Page 1 of 19 CONTENTS INTRODUCTION... 3 A. ADMISSION AND TREATMENT OF PATIENTS... 3 B. ALLIED
YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE
 YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE Nurse Midwives are licensed in Connecticut pursuant to CGS Section 20 75a et seq. recognizes that actual midwife function will vary with training
YALE NEW HAVEN HOSPITAL CORE PRIVILEGES LICENSED NURSE MIDWIFE Nurse Midwives are licensed in Connecticut pursuant to CGS Section 20 75a et seq. recognizes that actual midwife function will vary with training
Delegation of Services Agreements Change in Regulations
 Delegation of Services Agreements Change in Regulations Title 16, Division 13.8, Article 4, section 1399.540 was amended to include several requirements for the delegation of medical services to a physician
Delegation of Services Agreements Change in Regulations Title 16, Division 13.8, Article 4, section 1399.540 was amended to include several requirements for the delegation of medical services to a physician
HIPAA Notice of Privacy Practices
 HIPAA Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW IT CAREFULLY. This Notice
HIPAA Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW IT CAREFULLY. This Notice
11/01/15 STATE OF OKLAHOMA PHYSICIAN ASSISTANT ACT Title 59 O.S., Sections 519-524 INDEX
 11/01/15 STATE OF OKLAHOMA PHYSICIAN ASSISTANT ACT Title 59 O.S., Sections 519-524 INDEX 519. Repealed 519.1. Short title 519.2. Definitions 519.3. Physician Assistant Committee--Powers and duties 519.4.
11/01/15 STATE OF OKLAHOMA PHYSICIAN ASSISTANT ACT Title 59 O.S., Sections 519-524 INDEX 519. Repealed 519.1. Short title 519.2. Definitions 519.3. Physician Assistant Committee--Powers and duties 519.4.
MEDICAL CENTER POLICY NO. 0094. A. SUBJECT: Documentation of Patient Care (Electronic Medical Record)
 Clinical Staff Executive Committee MEDICAL CENTER POLICY NO. 0094 A. SUBJECT: Documentation of Patient Care (Electronic Medical Record) B. EFFECTIVE DATE: April 1, 2012 (R) C. POLICY: The University of
Clinical Staff Executive Committee MEDICAL CENTER POLICY NO. 0094 A. SUBJECT: Documentation of Patient Care (Electronic Medical Record) B. EFFECTIVE DATE: April 1, 2012 (R) C. POLICY: The University of
Health Professions Act BYLAWS SCHEDULE F. PART 3 Residential Care Facilities and Homes Standards of Practice. Table of Contents
 Health Professions Act BYLAWS SCHEDULE F PART 3 Residential Care Facilities and Homes Standards of Practice Table of Contents 1. Application 2. Definitions 3. Supervision of Pharmacy Services in a Facility
Health Professions Act BYLAWS SCHEDULE F PART 3 Residential Care Facilities and Homes Standards of Practice Table of Contents 1. Application 2. Definitions 3. Supervision of Pharmacy Services in a Facility
CLINICAL PRIVILEGES- NURSE MIDWIFE
 Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: Applicant: Check off the Requested
Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: Applicant: Check off the Requested
2 nd Floor CS&E Building A current UMHS identification badge is required to obtain medical records
 Location Hours 2 nd Floor CS&E Building A current UMHS identification badge is required to obtain medical records The Health Information Services Department is open to the public Monday through Friday,
Location Hours 2 nd Floor CS&E Building A current UMHS identification badge is required to obtain medical records The Health Information Services Department is open to the public Monday through Friday,
Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses
 Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses PROTOCOL FOR PHYSICIAN ASSISTANTS AND ADVANCED PRACTICE NURSES 1. POLICY Advanced
Community Center Readiness Guide Additional Resource #17 Protocol for Physician Assistants and Advanced Practice Nurses PROTOCOL FOR PHYSICIAN ASSISTANTS AND ADVANCED PRACTICE NURSES 1. POLICY Advanced
He then needs to work closely with the Quality Management Director or Leader and the Risk Manager to monitor the provision of patient care.
 Chapter II Introduction The Director has a major role in the effort to provide high quality medical care with a high degree of clinical safety. He is ultimately responsible for the professional conduct
Chapter II Introduction The Director has a major role in the effort to provide high quality medical care with a high degree of clinical safety. He is ultimately responsible for the professional conduct
DQA Hospital Q&A Page 1 of 24 Created on 03/10/2010 1:15:00 PM
 DQA Hospital Q&A Page 1 of 24 Created on 03/10/2010 1:15:00 PM 1. Is there a specific regulation or an interpretation of a regulation, in which soiled utility room doors must be locked? No. There is not
DQA Hospital Q&A Page 1 of 24 Created on 03/10/2010 1:15:00 PM 1. Is there a specific regulation or an interpretation of a regulation, in which soiled utility room doors must be locked? No. There is not
MEDICAL STAFF RULES & REGULATIONS. St. Ann's Medical Staff
 SUBJECT: RESPONSIBLE PERSONS: Medical Records St. Ann's Medical Staff POLICY: It is the policy of the medical staff to ensure timely completion of medical records in accordance with regulations and quality-of-care.
SUBJECT: RESPONSIBLE PERSONS: Medical Records St. Ann's Medical Staff POLICY: It is the policy of the medical staff to ensure timely completion of medical records in accordance with regulations and quality-of-care.
Regulatory Compliance Policy No. COMP-RCC 4.03 Title:
 I. SCOPE: Regulatory Compliance Policy No. COMP-RCC 4.03 Page: 1 of 10 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
I. SCOPE: Regulatory Compliance Policy No. COMP-RCC 4.03 Page: 1 of 10 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
MEDICAL STAFF RULES AND REGULATIONS MC KEE MEDICAL CENTER. Loveland, Colorado
 MEDICAL STAFF RULES AND REGULATIONS MC KEE MEDICAL CENTER Loveland, Colorado January 2014 MC KEE MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS PART 1 ADMISSION OF PATIENTS 1 1.2
MEDICAL STAFF RULES AND REGULATIONS MC KEE MEDICAL CENTER Loveland, Colorado January 2014 MC KEE MEDICAL CENTER MEDICAL STAFF RULES AND REGULATIONS TABLE OF CONTENTS PART 1 ADMISSION OF PATIENTS 1 1.2
MUNICIPAL REGULATIONS FOR NURSE- MIDWIVES
 MUNICIPAL REGULATIONS FOR NURSE- MIDWIVES CHAPTER 58 NURSE-MIDWIVES Secs. 5800 Applicability 5801 General Requirement 5802 Term of Certificate 5803 Renewal of Certificate 5804 Educational and Experience
MUNICIPAL REGULATIONS FOR NURSE- MIDWIVES CHAPTER 58 NURSE-MIDWIVES Secs. 5800 Applicability 5801 General Requirement 5802 Term of Certificate 5803 Renewal of Certificate 5804 Educational and Experience
ALASKA. Downloaded January 2011
 ALASKA Downloaded January 2011 7 AAC 12.255. SERVICES REQUIRED A nursing facility must provide nursing, pharmaceutical, either physical or occupational therapy, social work services, therapeutic recreational
ALASKA Downloaded January 2011 7 AAC 12.255. SERVICES REQUIRED A nursing facility must provide nursing, pharmaceutical, either physical or occupational therapy, social work services, therapeutic recreational
MUNICIPAL REGULATIONS for NURSE- ANESTHETISTS
 MUNICIPAL REGULATIONS for NURSE- ANESTHETISTS CHAPTER 57 CERTIFIED REGISTERED NURSE-ANESTHETISTS Secs. 5700 Applicability 5701 General Requirement 5702 Term of Certificate 5703 Renewal of Certificate 5704
MUNICIPAL REGULATIONS for NURSE- ANESTHETISTS CHAPTER 57 CERTIFIED REGISTERED NURSE-ANESTHETISTS Secs. 5700 Applicability 5701 General Requirement 5702 Term of Certificate 5703 Renewal of Certificate 5704
In the Hospital Setting
 In the Hospital Setting 2013 PENNSYLVANIA HOSPITAL QUALITY: Achieving More Together Use of Physician Assistants, Certified Registered Nurse Practitioners, Certified Nurse Midwives, Certified Registered
In the Hospital Setting 2013 PENNSYLVANIA HOSPITAL QUALITY: Achieving More Together Use of Physician Assistants, Certified Registered Nurse Practitioners, Certified Nurse Midwives, Certified Registered
02- DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION. Chapter 8 REGULATIONS RELATING TO ADVANCED PRACTICE REGISTERED NURSING
 02- DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 8 REGULATIONS RELATING TO ADVANCED PRACTICE REGISTERED NURSING SUMMARY: This chapter identifies the role of a registered
02- DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 8 REGULATIONS RELATING TO ADVANCED PRACTICE REGISTERED NURSING SUMMARY: This chapter identifies the role of a registered
Allied Health Care Provider: Appointment and Re-appointment
 Allied Health Care Provider: Appointment and Re-appointment Document Owner: Lawson, Louise Version: 8 Effective Date: 10/23/2013 Revision Date: 4/26/2015 Approvers: Calkins, Paul; Del Boccio, Suzanne;
Allied Health Care Provider: Appointment and Re-appointment Document Owner: Lawson, Louise Version: 8 Effective Date: 10/23/2013 Revision Date: 4/26/2015 Approvers: Calkins, Paul; Del Boccio, Suzanne;
APP PRIVILEGES IN ORTHOPEDICS
 APP PRIVILEGES IN ORTHOPEDICS Education/Training Licensure (Initial and Reappointment) Required Successful completion of a PA or NP program Current Licensure as a PA or RN in the state of CA Current certification
APP PRIVILEGES IN ORTHOPEDICS Education/Training Licensure (Initial and Reappointment) Required Successful completion of a PA or NP program Current Licensure as a PA or RN in the state of CA Current certification
Health Information Technology & Management Chapter 2 HEALTH INFORMATION SYSTEMS
 Health Information Technology & Management Chapter 2 HEALTH INFORMATION SYSTEMS INFORMATION SYSTEM *Use of computer hardware and software to process data into information. *Healthcare information system
Health Information Technology & Management Chapter 2 HEALTH INFORMATION SYSTEMS INFORMATION SYSTEM *Use of computer hardware and software to process data into information. *Healthcare information system
North Shore LIJ Health System, Inc. Facility Name
 North Shore LIJ Health System, Inc. Facility Name POLICY TITLE: The Medical Record POLICY #: 200.10 Approval Date: 2/14/13 Effective Date: Prepared by: Elizabeth Lotito, HIM Project Manager ADMINISTRATIVE
North Shore LIJ Health System, Inc. Facility Name POLICY TITLE: The Medical Record POLICY #: 200.10 Approval Date: 2/14/13 Effective Date: Prepared by: Elizabeth Lotito, HIM Project Manager ADMINISTRATIVE
Rules and Regulations Of the. Medical Staff. Coaldale, Pennsylvania
 Rules and Regulations Of the Medical Staff Coaldale, Pennsylvania Article I PREAMBLE...4 General Statement...4 Adoption and Amendment...4 Article II APPLICABILITY...4 Article III STATEMENT OF PURPOSE...4
Rules and Regulations Of the Medical Staff Coaldale, Pennsylvania Article I PREAMBLE...4 General Statement...4 Adoption and Amendment...4 Article II APPLICABILITY...4 Article III STATEMENT OF PURPOSE...4
BYLAWS OF THE MEDICAL STAFF
 (EFFECTIVE 6.25.12) BYLAWS OF THE MEDICAL STAFF CENTRAL MAINE MEDICAL CENTER LEWISTON, MAINE With updates adopted by the Medical Staff on June 25, 2012 Edmund Claxton, M.D. President Approved by the Governing
(EFFECTIVE 6.25.12) BYLAWS OF THE MEDICAL STAFF CENTRAL MAINE MEDICAL CENTER LEWISTON, MAINE With updates adopted by the Medical Staff on June 25, 2012 Edmund Claxton, M.D. President Approved by the Governing
Regulatory Compliance Policy No. COMP-RCC 4.20 Title:
 I. SCOPE: Regulatory Compliance Policy No. COMP-RCC 4.20 Page: 1 of 11 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
I. SCOPE: Regulatory Compliance Policy No. COMP-RCC 4.20 Page: 1 of 11 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
UW School of Dentistry Comprehensive Medication Policy
 UNIVERSITY OF WASHINGTON SCHOOL OF DENTISTRY Subject: UW School of Dentistry Comprehensive Medication Policy Policy Number: Effective Date: December 2014 Revision Dates: June 2015 PURPOSE This policy provides
UNIVERSITY OF WASHINGTON SCHOOL OF DENTISTRY Subject: UW School of Dentistry Comprehensive Medication Policy Policy Number: Effective Date: December 2014 Revision Dates: June 2015 PURPOSE This policy provides
ALLOW NATURAL DEATH/WITHHOLDING AND/OR WITHDRAWING L I F E - S U S T A I N I N G T R E A T M E N T / NON-BENEFICIAL CARE AND RESUSCITATION POLICY
 PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
Ontario Hospital Association/Ontario Medical Association Hospital Prototype Board-Appointed Professional Staff By-law
 Ontario Hospital Association/Ontario Medical Association Hospital Prototype Board-Appointed Professional Staff By-law 2011 ONTARIO HOSPITAL ASSOCIATION/ ONTARIO MEDICAL ASSOCIATION HOSPITAL PROTOTYPE BOARD-APPOINTED
Ontario Hospital Association/Ontario Medical Association Hospital Prototype Board-Appointed Professional Staff By-law 2011 ONTARIO HOSPITAL ASSOCIATION/ ONTARIO MEDICAL ASSOCIATION HOSPITAL PROTOTYPE BOARD-APPOINTED
BOARD OF PHARMACY DIVISION 41 OPERATION OF PHARMACIES (RETAIL AND INSTITUTIONAL DRUG OUTLETS) CONSULTING PHARMACISTS AND OPERATION OF DRUG ROOMS
 BOARD OF PHARMACY DIVISION 41 OPERATION OF PHARMACIES (RETAIL AND INSTITUTIONAL DRUG OUTLETS) CONSULTING PHARMACISTS AND OPERATION OF DRUG ROOMS 855-041-6050 Definitions Hospitals with Pharmacies (1) In
BOARD OF PHARMACY DIVISION 41 OPERATION OF PHARMACIES (RETAIL AND INSTITUTIONAL DRUG OUTLETS) CONSULTING PHARMACISTS AND OPERATION OF DRUG ROOMS 855-041-6050 Definitions Hospitals with Pharmacies (1) In
Title 30: Professions and Occupations. Part 2630 Collaboration. Part 2630 Chapter 1: Collaboration with Nurse Practitioners
 Title 30: Professions and Occupations Part 2630 Collaboration Part 2630 Chapter 1: Collaboration with Nurse Practitioners Rule 1.1 Scope. These rules apply to all individuals licensed to practice medicine
Title 30: Professions and Occupations Part 2630 Collaboration Part 2630 Chapter 1: Collaboration with Nurse Practitioners Rule 1.1 Scope. These rules apply to all individuals licensed to practice medicine
JOB DESCRIPTION NURSE PRACTITIONER
 JOB DESCRIPTION NURSE PRACTITIONER Related documents: Nurse Practitioner Process Protocol Authorization for Individuals to Provide Services as Allied Health Personnel in the LPCH/SCH Administrative Manual
JOB DESCRIPTION NURSE PRACTITIONER Related documents: Nurse Practitioner Process Protocol Authorization for Individuals to Provide Services as Allied Health Personnel in the LPCH/SCH Administrative Manual
Deleted Elements of Performance for Rehabilitation and Psychiatric Distinct Part Units in Critical Access Hospitals
 Deleted Elements of Performance for Rehabilitation and Psychiatric Distinct Part Units in Critical Access Hospitals Effective January 1, 2010 Critical Access Hospital Accreditation Program Standard EC.0001
Deleted Elements of Performance for Rehabilitation and Psychiatric Distinct Part Units in Critical Access Hospitals Effective January 1, 2010 Critical Access Hospital Accreditation Program Standard EC.0001
KENTUCKY ADMINISTRATIVE REGULATIONS TITLE 201. GENERAL GOVERNMENT CABINET CHAPTER 9. BOARD OF MEDICAL LICENSURE
 KENTUCKY ADMINISTRATIVE REGULATIONS TITLE 201. GENERAL GOVERNMENT CABINET CHAPTER 9. BOARD OF MEDICAL LICENSURE 201 KAR 9:260. Professional standards for prescribing and dispensing controlled substances.
KENTUCKY ADMINISTRATIVE REGULATIONS TITLE 201. GENERAL GOVERNMENT CABINET CHAPTER 9. BOARD OF MEDICAL LICENSURE 201 KAR 9:260. Professional standards for prescribing and dispensing controlled substances.
MEDICAL STAFF RULES AND REGULATIONS. Sturgeon Bay, Wisconsin
 MEDICAL STAFF RULES AND REGULATIONS Sturgeon Bay, Wisconsin Rules and Regulations Table of Contents Admission and Discharge of Patients...3 Informed Consent...4 Hand Off Communication...4 General Orders
MEDICAL STAFF RULES AND REGULATIONS Sturgeon Bay, Wisconsin Rules and Regulations Table of Contents Admission and Discharge of Patients...3 Informed Consent...4 Hand Off Communication...4 General Orders
MEDICAL STAFF RULES & REGULATIONS
 MEDICAL STAFF RULES & REGULATIONS 1 Table of Contents Rule 1: General... 4 Rule 2: Patient Rights and Responsibilities... 5 Rule 3: Responsibility for Care... 6 3.1 Conduct of Care... 6 3.2 Consultations:...
MEDICAL STAFF RULES & REGULATIONS 1 Table of Contents Rule 1: General... 4 Rule 2: Patient Rights and Responsibilities... 5 Rule 3: Responsibility for Care... 6 3.1 Conduct of Care... 6 3.2 Consultations:...
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner
 Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Health Professions Act BYLAWS SCHEDULE F. PART 2 Hospital Pharmacy Standards of Practice. Table of Contents
 Health Professions Act BYLAWS SCHEDULE F PART 2 Hospital Pharmacy Standards of Practice Table of Contents 1. Application 2. Definitions 3. Drug Distribution 4. Drug Label 5. Returned Drugs 6. Drug Transfer
Health Professions Act BYLAWS SCHEDULE F PART 2 Hospital Pharmacy Standards of Practice Table of Contents 1. Application 2. Definitions 3. Drug Distribution 4. Drug Label 5. Returned Drugs 6. Drug Transfer
AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Verificatoin Criterea EFFECTIVE JANUARY 1, 2015. Criterion. Level (1 or 2) Number
 Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
THE LONG ISLAND HOME MEDICAL STAFF BYLAWS
 THE LONG ISLAND HOME MEDICAL STAFF BYLAWS South Oaks Hospital A Comprehensive Behavioral Health Center Broadlawn Manor Nursing and Rehabilitation Center A Comprehensive Long-Term And Sub-Acute Care Facility
THE LONG ISLAND HOME MEDICAL STAFF BYLAWS South Oaks Hospital A Comprehensive Behavioral Health Center Broadlawn Manor Nursing and Rehabilitation Center A Comprehensive Long-Term And Sub-Acute Care Facility
Guidelines for the Operation of Burn Centers
 C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
TABLE OF CONTENTS RULES & REGULATIONS
 TABLE OF CONTENTS RULES & REGULATIONS Preamble... 2 General Information... 2 Section One - Adoption and Amendment... 2 Section Two - Orders... 4 Section Three - Progress Notes... 5 Section Four - Consultations...
TABLE OF CONTENTS RULES & REGULATIONS Preamble... 2 General Information... 2 Section One - Adoption and Amendment... 2 Section Two - Orders... 4 Section Three - Progress Notes... 5 Section Four - Consultations...
Credentials Policy Manual. Reviewed & Approved by MEC 8/13/2012 Reviewed & Approved by Board of Commissioners 9/11/12
 Credentials Policy Manual Reviewed & Approved by MEC 8/13/2012 Reviewed & Approved by Board of Commissioners 9/11/12 Credentialing Policy Manual Table of Contents I. Application for Appointment to Staff...1
Credentials Policy Manual Reviewed & Approved by MEC 8/13/2012 Reviewed & Approved by Board of Commissioners 9/11/12 Credentialing Policy Manual Table of Contents I. Application for Appointment to Staff...1
UNMH Certified Nurse-Midwife (CNM) Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
PSYCHIATRIC MENTAL HEALTH NURSE PRACTITIONER CLINICAL PRIVILEGES
 Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: 6/3/15 Applicant: Check off
Name: Page 1 Initial Appointment Reappointment Department Specialty Area All new applicants must meet the following requirements as approved by the governing body effective: 6/3/15 Applicant: Check off
CRAIG HOSPITAL ENGLEWOOD, COLORADO BYLAWS OF THE MEDICAL STAFF ADOPTED AS AMENDED: MARCH 26, 2015
 CRAIG HOSPITAL ENGLEWOOD, COLORADO BYLAWS OF THE MEDICAL STAFF ADOPTED AS AMENDED: MARCH 26, 2015 BYLAWS OF THE MEDICAL STAFF 48355590.5 TABLE OF CONTENTS PAGE PREAMBLE... 1 DEFINITIONS...1 ARTICLE I.
CRAIG HOSPITAL ENGLEWOOD, COLORADO BYLAWS OF THE MEDICAL STAFF ADOPTED AS AMENDED: MARCH 26, 2015 BYLAWS OF THE MEDICAL STAFF 48355590.5 TABLE OF CONTENTS PAGE PREAMBLE... 1 DEFINITIONS...1 ARTICLE I.
58-13-1. Title. This chapter is known as the "Health Care Providers Immunity from Liability Act."
 58-13-1. Title. This chapter is known as the "Health Care Providers Immunity from Liability Act." Enacted by Chapter 253, 1996 General Session 58-13-2. Emergency care rendered by licensee. (1) A person
58-13-1. Title. This chapter is known as the "Health Care Providers Immunity from Liability Act." Enacted by Chapter 253, 1996 General Session 58-13-2. Emergency care rendered by licensee. (1) A person
Part 2630 Chapter 1: Collaboration/Consultation with Nurse Practitioners
 Title 30: Professions and Occupations Part 2630 Collaboration/Consultation Part 2630 Chapter 1: Collaboration/Consultation with Nurse Practitioners Rule 1.1 Scope. These rules apply to all individuals
Title 30: Professions and Occupations Part 2630 Collaboration/Consultation Part 2630 Chapter 1: Collaboration/Consultation with Nurse Practitioners Rule 1.1 Scope. These rules apply to all individuals
8.310.12.1 ISSUING AGENCY: New Mexico Human Services Department (HSD). [8.310.12.1 NMAC - N, 11-1-14]
![8.310.12.1 ISSUING AGENCY: New Mexico Human Services Department (HSD). [8.310.12.1 NMAC - N, 11-1-14] 8.310.12.1 ISSUING AGENCY: New Mexico Human Services Department (HSD). [8.310.12.1 NMAC - N, 11-1-14]](/thumbs/27/12237818.jpg) TITLE 8 SOCIAL SERVICES CHAPTER 310 HEALTH CARE PROFESSIONAL SERVICES PART 12 INDIAN HEALTH SERVICE AND TRIBAL 638 FACILITIES 8.310.12.1 ISSUING AGENCY: New Mexico Human Services Department (HSD). [8.310.12.1
TITLE 8 SOCIAL SERVICES CHAPTER 310 HEALTH CARE PROFESSIONAL SERVICES PART 12 INDIAN HEALTH SERVICE AND TRIBAL 638 FACILITIES 8.310.12.1 ISSUING AGENCY: New Mexico Human Services Department (HSD). [8.310.12.1
MUNICIPAL REGULATIONS for CLINICAL NURSE SPECIALISTS
 MUNICIPAL REGULATIONS for CLINICAL NURSE SPECIALISTS CHAPTER 60 CLINICAL NURSE SPECIALIST Secs. 6000 Applicability 6001 General Requirements 6002 Term of Certificate 6003 Renewal of Certificate 6004 Educational
MUNICIPAL REGULATIONS for CLINICAL NURSE SPECIALISTS CHAPTER 60 CLINICAL NURSE SPECIALIST Secs. 6000 Applicability 6001 General Requirements 6002 Term of Certificate 6003 Renewal of Certificate 6004 Educational
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Center for Medicaid and State Operations/Survey & Certification Group
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
LONG ISLAND JEWISH MEDICAL CENTER RULES AND REGULATIONS THE MEDICAL STAFF
 LONG ISLAND JEWISH MEDICAL CENTER RULES AND REGULATIONS OF THE MEDICAL STAFF Signed Chairman of the Medical Board As Amended through April 29, 2015. INDEX A. GENERAL POLICIES...1 B. QUALIFICATIONS FOR
LONG ISLAND JEWISH MEDICAL CENTER RULES AND REGULATIONS OF THE MEDICAL STAFF Signed Chairman of the Medical Board As Amended through April 29, 2015. INDEX A. GENERAL POLICIES...1 B. QUALIFICATIONS FOR
CHAPTER 101 (HB 500)
 AN ACT relating to crime victims. CHAPTER 101 1 CHAPTER 101 (HB 500) Be it enacted by the General Assembly of the Commonwealth of Kentucky: Section 1. KRS 216B.400 is amended to read as follows: (1) Where
AN ACT relating to crime victims. CHAPTER 101 1 CHAPTER 101 (HB 500) Be it enacted by the General Assembly of the Commonwealth of Kentucky: Section 1. KRS 216B.400 is amended to read as follows: (1) Where
Ambulatory Surgical Centers Frequently Asked Questions
 Ambulatory Surgical Centers Frequently Asked Questions Index Top General Definitions Compliance with State Licensure Laws Governing Body and Management Surgical Services Quality Assessment and Performance
Ambulatory Surgical Centers Frequently Asked Questions Index Top General Definitions Compliance with State Licensure Laws Governing Body and Management Surgical Services Quality Assessment and Performance
WEST VIRGINIA ~ STATUTE
 WEST VIRGINIA ~ STATUTE STATUTE West Virginia Code 30-3-16, 30-3-13, 30-3-5 DATE Enacted 1976 REGULATORY BODY PA DEFINED SCOPE OF PRACTICE PRESCRIBING/DISPENSING SUPERVISION DEFINED PAs PER PHYSICIAN APPLICATION
WEST VIRGINIA ~ STATUTE STATUTE West Virginia Code 30-3-16, 30-3-13, 30-3-5 DATE Enacted 1976 REGULATORY BODY PA DEFINED SCOPE OF PRACTICE PRESCRIBING/DISPENSING SUPERVISION DEFINED PAs PER PHYSICIAN APPLICATION
12 LC 33 4683S. The House Committee on Health and Human Services offers the following substitute to HB 972: A BILL TO BE ENTITLED AN ACT
 The House Committee on Health and Human Services offers the following substitute to HB 972: A BILL TO BE ENTITLED AN ACT 1 2 3 4 5 6 7 8 9 10 11 12 13 To amend Chapter 34 of Title 43 of the Official Code
The House Committee on Health and Human Services offers the following substitute to HB 972: A BILL TO BE ENTITLED AN ACT 1 2 3 4 5 6 7 8 9 10 11 12 13 To amend Chapter 34 of Title 43 of the Official Code
(A) Information needed to identify and classify the hospital, include the following: (b) The hospital number assigned by the department;
 3701-59-05 Hospital registration and reporting requirements. Every hospital, public or private, shall, by the first of March of each year, register with and report to the department of health the following
3701-59-05 Hospital registration and reporting requirements. Every hospital, public or private, shall, by the first of March of each year, register with and report to the department of health the following
Overview of the Florida Medicaid Therapy Services Coverage and Limitations Handbook
 Overview of the Florida Medicaid Therapy Services Coverage and Limitations Handbook 2 Introduction Medicaid reimburses for physical therapy (PT), occupational therapy (OT), respiratory therapy (RT), and
Overview of the Florida Medicaid Therapy Services Coverage and Limitations Handbook 2 Introduction Medicaid reimburses for physical therapy (PT), occupational therapy (OT), respiratory therapy (RT), and
Physician Assistant Licensing Act
 45:9-27.10. Short title 1. This act shall be known and may be cited as the "Physician Assistant Licensing Act." L.1991,c.378,s.1. 45:9-27.11. Definitions 2. As used in this act: "Approved program" means
45:9-27.10. Short title 1. This act shall be known and may be cited as the "Physician Assistant Licensing Act." L.1991,c.378,s.1. 45:9-27.11. Definitions 2. As used in this act: "Approved program" means
Notice of Privacy Practices. Introduction
 Notice of Privacy Practices Introduction At Ohio Valley Medical Center and East Ohio Regional Hospital, we are committed to using and disclosing protected health information about you responsibly. This
Notice of Privacy Practices Introduction At Ohio Valley Medical Center and East Ohio Regional Hospital, we are committed to using and disclosing protected health information about you responsibly. This
ARTICLE 4. MEDICAL RECORD POLICIES
 A. General Rules ARTICLE 4. MEDICAL RECORD POLICIES 4.1 General - A Medical Record is established and maintained for each patient who has been treated or evaluated at the Medical Center. The Medical Record,
A. General Rules ARTICLE 4. MEDICAL RECORD POLICIES 4.1 General - A Medical Record is established and maintained for each patient who has been treated or evaluated at the Medical Center. The Medical Record,
Collaborative Practice Agreement for Nurse Practitioner Management of Patients in the Specialty of Pediatric Critical Care
 Collaborative Practice Agreement for Nurse Practitioner Management of Patients in the Specialty of Pediatric Critical Care Purpose Section I Introduction/Overview This document authorizes the nurse practitioner
Collaborative Practice Agreement for Nurse Practitioner Management of Patients in the Specialty of Pediatric Critical Care Purpose Section I Introduction/Overview This document authorizes the nurse practitioner
MedStar Family Choice Benefits Summary District of Columbia- Healthy Families WHAT YOU GET WHO CAN GET THIS BENEFIT BENEFIT
 Primary Care Services Specialist Services Laboratory & X-ray Services Hospital Services Pharmacy Services (prescription drugs) Emergency Services Preventive, acute, and chronic health care Services generally
Primary Care Services Specialist Services Laboratory & X-ray Services Hospital Services Pharmacy Services (prescription drugs) Emergency Services Preventive, acute, and chronic health care Services generally
