Risk Stratification of Patients With Syncope
|
|
|
- Sandra Adelia Stephens
- 3 years ago
- Views:
From this document you will learn the answers to the following questions:
What were potential predictor variables?
What was the goal of the study?
Transcription
1 GENERAL CLINICAL INVESTIGATION/ORIGINAL CONTRIBUTION Risk Stratification of Patients With Syncope From the University of Pittsburgh, Pittsburgh, Pennsylvania. Received for publication January 29, Revisions received June 27 and September 30, Accepted for publication October i8, Supported in part by a grant from the National Heart, Lung, and Blood Institute (ROI HL36735). Dr Kapoor is a recipient of a Research Career Development Award from the National Heart, Lung, and Blood Institute (KO4L 01899). Copyright by the American College of Emergency Physicians. Thomas P Martin, MD Barbara H Hanusa, PhD Wishwa N Kapoor, MD, MPH See related editorial, p 540. Study objective: To develop and validate a risk classification system for patients presenting to emergency departments with syncope. Methods: Two prospective studies were carried out at a large urban teaching hospital ED. One cohort of 252 patients with syncope who reported to the ED was used to develop the risk classification system; a second cohort of 374 patients with syncope was used to validate the system. Data from the patient's history, physical examination, and ED ECG were used to identify predictors of arrhythmias or mortality within the first year. Arrhythmias were detected by cardiac monitoring or electrophysiologic studies. Logistic regression and Cox proportional hazards models were used to identify the important risk factors for the classification system. Performance of the system was measured by comparing the proportion of patients with arrhythmias or death at various levels of the risk and receiver operating characteristic curves. Results: Multivariate predictors of arrhythmia or 1-year mortality were an abnormal ED ECG (odds ratio [OR], 3.2; 95% confidence interval [CI], 1.6 to 6.4); history of ventricular arrhythmia (OR, 4.8; 95% CI, 1.7 to 13.9); history of congestive heart failure (OR, 3.1; 95% CI, 1.3 to 7.4); and age greater than 45 years (OR, 3.2; 95% CI, 1.3 to 8.1). Arrhythmias or death within 1 year occurred in 7.3% (derivation cohort) to 4.4% (validation cohort) of patients without any risk factors and in 80.4% (derivation) to 57.6% (validation) of patients with three or four risk factors. Conclusion: Historical and EGG factors available at the time of presentation can be used to stratify risk of arrhythmias or mortality within 1 year in ED patients presenting with syncope. [Martin TP, Hanusa BH, Kapoor WN: Risk stratification of patients with syncope. Ann Emerg Med April 1997;29: ] APRIL :4 ANNALS OF EMERGENCY MEDICINE 4 5 9
2 Martin, Hanusa & Kapoor INTRODUCTION Syncope is a common medical problem accounting for 1% to 6% of medical admissions and up to 3% of emergency department visits. 1-5 This symptom is often difficult to evaluate because of a broad differential diagnosis and the low yield of many diagnostic studies. 1-5 Further, patients presenting with syncope represent a heterogeneous population with respect to demographic and clinical characteristics. In patients with a definite cause of syncope, management depends on the cause identified. However, because the cause frequently is not certain when the patient is seen in the ED, hospital admission is often necessary. A major reason for admission in syncope patients is concern about arrhythmias and sudden death. Identification of patients who are at low risk for arrhythmias and sudden death could help ED personnel make informed decisions about safe discharges for outpatient diagnostic evaluation and treatment. The primary goals of this study were (1) to identify predictors of arrhythmias and mortality within the first year for patients presenting to the ED with syncope and (2) to develop and validate clinical prediction rules that can be used to separate ED patients into low- and high-risk groups. METHODS Syncope was defined as a sudden transient loss of consciousness associated with an inability to maintain postural tone that was not compatible with a seizure disorder, vertigo, dizziness (lightheadedness without loss of consciousness), coma, shock, or other states of altered consciousness. Patients must have regained consciousness spontaneously; those who required pharmacologic or electrical treatment at initial presentation were excluded. Two cohorts of patients with syncope were evaluated and followed prospectively. One group (derivation cohort) was enrolled between March 1981 and February 1984; the second group (validation cohort) was enrolled between August 1987 and February The study methodology for the two cohorts was similar. Patients were accrued from an exhaustive search at the University of Pittsburgh Medical Center ED, a teaching, tertiary and primary care hospitalassociated department that had an average annual census of 36,000 visits during the study periods. Patients presenting to the ED with symptoms possibly compatible with syncope were identified from daily review of ED visits and contacted. If these patients met the criteria for having had a syncopal episode, they were asked to participate in this study. There were two differences between the protocols for patients in the two cohorts. First, in the validation cohort, end points in addition to mortality and arrhythmias were collected, including stroke and myocardial infarction. Second, patients in the validation cohort underwent additional diagnostic testing systematically for orthostatic hypotension and psychiatric disorders. A few patients in the validation cohort underwent tilt-table testing when it became available in late 1980s. All patients enrolled in the study underwent a standardized assessment. Patients were interviewed and previous medical charts were reviewed. Assessment consisted of a complete history and physical examination; a baseline laboratory evaluation including a complete blood count, urinalysis, electrolytes, blood urea nitrogen, creatinine, and glucose; a 12-lead ECG; prolonged ECG monitoring of at least 24 hours' duration, by either ambulatory Holter monitoring or bedside monitoring in a CCU; and definitive evaluation of any clinical or historical findings suggestive of a cause of syncope. For example, cerebral angiography was required to establish a diagnosis of subclavian steal when clinical findings compatible with that entity were present. Other diagnostic studies, such as EEG, head computed tomography scans, and glucose tolerance tests were not routinely performed because previous studies have documented a low yield for these tests. >5 These studies were used selectively for consideration of specific diagnoses based on data from the initial history, physical examination, and ECG. Electrophysiologic studies were performed at the discretion of the patient's attending physician or on the recommendation of a consulting cardiologist. Upright tilt testing was not available for the derivation cohort and during the developmental phases in the validation cohort; therefore, few patients underwent tilt testing. Patients were monitored by their personal physicians. Follow-up information regarding recurrence of syncope, new cardiovascular events, subsequent diagnoses of significant arrhythmias, and mortality were obtained from patients, their personal physicians, family, or caregivers. Follow-up information was obtained at 3-month intervals for 3 years. All attempts were made to obtain records of subsequent evaluations, hospital admissions, and other events. A cause of death was assigned on the basis of information obtained from the family, patients' physicians, records from the Bureau of Vital Statistics, and autopsy reports if available. Death was classified as sudden or nonsudden by specific criteria. 6 Sudden death was defined as unexpected death occurring within 1 hour after onset of acute symptoms. Death was also classified as sudden if it occurred in a person known to be alive and functioning in his or her usual health within 24 hours of an unwitnessed death. This category included patients who were found dead or died during sleep. In addition, deaths were classified as sudden if unexpected ANNALS OF EMERGENCY MEDIOINE 29:4 APRIL 1997
3 Martirt, Hanusa &, Kapoor cardiac arrest occurred and resuscitation was successful but the cardiac arrest initiated a chain of events that led to death. Causes of syncope were assigned based on strict adherence to previously reported diagnostic criteria. 4 ECG reports and tracings (from ED ECG, Holter monitoring, or bedside ECG monitoring in the CCU) were reviewed for identification and verification of arrhythmias. Two definitions of clinically important arrhythmias were considered. It was not required that these arrhythmias were the cause of the syncope. A broad definition, designed to be inclusive, included the following: ventricular tachycardia (VT) of three or more beats; sinus pauses of 2 seconds or longer and those pauses that were symptomatic; symptomatic sinus bradycardia ("symptomatic" for the purposes of this study refers to the simultaneous occurrence of dizziness, lightheadedness, or Table 1. Demographic and clinical characteristics of derivation and validation cohorts. Derivation Cohort Validation Cohort Characteristic (n=252) 1n=374) Age (years) Mean Range No. >45 (%} 183 (73) 262 (70} No. female (%) 139 (55) 199 (53) No. nonwhite (%)* 63 (25) 79 (21) No. with prior syncoi0~e (%) Any previous episode 157 (62) 19T (55) >1 Episode in preceding year 107 (42) 92* (26) No. with comorbid cnnditions (%) High blood pressure 77 (31) 121 (32) Diabetes mellitus 33 (13) 37 (10) Ventricular arrhythmias 32 (13) 10 (3) Coronary artery disease 71 (28) 72 (19) Congestive heart failure 42 ( (9) Cerebravascular disease 34 (14) 37 (10) ECG results (%) Normal 70 (28) 154 {41 ) NST only 44 (18} 32 (9) Abnormal ~ 138 (55) 188 (50) Conduction disorders 68 (27) 104 (28) 01d myocardial infarction 40 (16) 36 (10) Ventricular hypertrophy u 29 (12) 30 (8) Rhythm abnormalities 30 (12) 29 (8) Other 25 (10) 22 (6} NST, nonspecific ST- and T- wave abnormalities. *Patients in the derivation cohort were either white or black; in the validation cohort there were four patients of Asian/Pacif c Islander ancestry tonly 356 patients had data available for this variable. *Only 360 patients had data available for this variable. ~Some patients had mare than one abnormality. t/oee patient in the derivation cohort and five patients in the validation cohort had right ventricular hypertrophy; the remainder had left ventricular hypertrophy, syncope and an arrhythmia on ECG monitoring); supraventricular tachycardia (SVT) with symptoms or associated with hypotension (systolic blood pressure less than 90 mm Hg); atrial fibrtllation with slow ventricular response (RR interval longer than 3 seconds); complete atrioventricular block; Mobitz II atrioventricular block; and evidence of pacemaker malfunction. Isolated, asymptomatic premature ventricular contractions (PVCs), couplets, asymptomatic premature atrial contractions, brief asymptomatic runs of SVT, chronic atrial fibrillation, and atrial flutter were not included in our definition of arrhythmias unless they were associated with symptoms (dizziness, lightheadedness, or syncope). In addition, findings at the time of e]ectrophysiologic studies of prolonged corrected sinus node recovery time; inducible, sustained monomorphic VT; HV intervals longer than i00 msec; symptomatic SVT or SVT associated with hypotension; and carotid sinus hypersensitivity were also considered evidence for clinically important arrhythmias. Table 2. Clinically important arrhythmias iden@ed in study populations in the presentation. Characteristic No. in No. in Derivation Cohort Validation Cohort (%) [n=252] (%) [n=374] Any arrhythmia Broad definition* 65 (26) 49 (13} Strict definition 43 (17) 29 (8) Ventricular tachycardia Broad definition ~ 41 (16) 32 (9) Strict definition* 15 (6) 10 (3) Sinus pause Broad definition (_>2.0 seconds) 13 (5) 9 (2) Strict definition (_>3.8 seconds) 5 (2) 2 (.5) Pacemaker malfunction 6 (2) 5 (1) Sinus bradycardia with symptoms 6 (2) 4 (1) Atrioventricular block ~ 6" (2) 7 (2) Supraventricular tachycardia 4 (2) 3 (1) with symptoms Atrial fibrillation with 111 (,4) 1 # (.3) slow ventricular response *Seven patients in the derivation cohort and 11 patients in the validation cohort had more than. one arrhythmia. qn the derivation cohort, diagnosis in one patient was made on the basis of electrophysiologic findings only and three by E0S findings only; in the validation cohort, diagnosis was made in two patients by electrophysielogic findings any and one by EOG findings only. *Strict definition: duration >lg0 beats or >30 sec, or with symptoms. ~lncludes complete heart block, Mobitz II on ECG, and prolonged ECG monitoring. UFive patients had complete heart block on Hotter, I had Mobitz II, seven had complete heart block on prolonged ECG monitoring. ~Atrial fibrillation with pauses ef 4.5 sac; also prolonged HV interval on electrophysialogic studies. #Atrial fibrillation with pauses of 3 seconds. APRIL :4 ANNALS OF EMfiRGENCY MEDICINE 4 6 I
4 Mart~n, Hanusa & Kapoor The strict definition for clinically important arrhythmias included symptomatic or sustained VT (duration longer than 30 seconds or 100 beats), symptomatic SVT, symptomatic bradycardia, pauses of longer than 3.0 seconds, atrial fibrillation with slow ventdcular response (RR interval longer than 3.0 seconds), complete atrioventricular block, Mobitz II atrioventricular block, and pacemaker malfunction. The electrophysiologic abnormalities defined previously were maintained. Results are reported for all-cause mortality and, in a more focused analysis, for cardiac causes of mortality. Cardiac mortality included deaths resulting from atherosclerotic heart disease (eg, myocardial infarction, coronary artery disease); myocardial, pericardial, or valvular heart disease; congestive heart failure (CHF); congenital heart disease; restrictive cardiomyopathy; and cardiac arrhythmias. All sudden deaths were classified as cardiac deaths. Potential predictor variables included demographic information (ie, age, sex, race), comorbid conditions, history of prior syncope, and ED ECGs. This information was obtainable from the patients or from medical records at the time of presentation for the index episode. The comorbid conditions considered were current or past history of high blood pressure, diabetes mellitus, cerebrovascular disease, coronary artery disease, CHE or ventricular arrhythmias (VA). VA included past history of frequent (more than 10 per hour), repetitive (two or more consecutive), or multifocal PVCs. ED ECGs were classified into three groups: normal (including patients with only sinus bradycardia or sinus tachycardia); nonspecific ST- and T-wave abnormalities (NST) for patients with NST as the only abnormality; and abnormal. The abnormal group included rhythm abnormalities (eg, atrial fibrillation or flutter, multifocal atrial tachycardia, junctional or paced rhythms); frequent or repetitive PVCs (including VT), conduction disorders (ie, left axis deviation, bundle branch block, intraventricular conduction delay), left or right ventricular hypertrophy (LVH or RVH), short PR interval (less than. 10 see), old myocardial infarction, and atrioventricular block (ie, complete atrioventricular block, Mobitz II, or Mobitz I with other abnormalities present). Univariate predictors of clinically important arrhythmias were identified using X 2 analysis for categorical data and Student's t test for continuous data. Univariate predictors of death within 1 year of study enrollment were identified with Kaplan-Meier methods and the Wilcoxon statistics. Those variables with probability values lower than. 10 were entered m a multivariate logistic regression model to identify predictors of important arrhythmias and in a Cox proportional hazards model to identify multivariate predictors of 1-year mortality. After multivariate models were identified for each study end point, a joint logistic regression model was developed by using the multivariate predictors of either arrhythmias or death in the first year. For this model, death in the first year was coded as "yes" or "no." Significant multivariate predictors were then identified as risks for arrhythmias or death. Predictors identified by the final logistic regression model were used to define a risk index for either arrhythmias or mortality within 1 year based on the number of risk factors present. The usefulness of the risk index was measured by comparing the proportion of death or arrhythmias across the risk index in the derivation and validation cohorts. In addition, its usefulness for identifying patients with the more strictly defined arrhythmias or cardiac deaths was measured. Performance of the risk index in all analyses was also evaluated by comparison of areas under receiver operating Table 3. Significant multivariate predictors of arrhythmias and death within 1 yea~* Broad-Definition Arrhythmias Mortality Combined Arrhythmias or Mortality Predictor OR 95% CI RR 95% CI OR 95% CI Abnormal ECG , History ef ventricular arrhythmia , History of congestive heart failure Age >45 years , ,1 Nonwhite race No prior history of syncope , *Logistic regression models result in OR estimates, and Oex proportional hazards models result in RR estimates. OR compares the odds of occurrence of an event when a risk factor is present with the odds of occurrence when the risk factor is not present. RR compares the proportion of those with a risk factor who have an event to the proportion of those without the risk factor who have the event. If the occurrence of the event is rare, the RR is estimated by the OR. The 95% CI of the OR or RR is shown in each instance. 462 ANNALS OF EMERGENCY MEDICINE 29:4 APRIL 1997
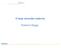
5 RiSK STRATIFICATION Martin, Hanusa & Kapoor characteristic (ROC) curves. BMDP Statistical Software r was used for logistic regression and survival analyses; ROCFIT software s was used for the ROC analysis. RESULTS In the derivation cohort, 253 palients with syncope presented to the ED. One patient did not have an ED ECG, leaving 252 patients in the derivation cohort. In the validation cohort, 378 patients were seen in the ED, and 4 did not have an ED ECG, leaving 374 patients in the validation cohort. No patients in the derivation cohort were Iost to follow-up at 1 year; three patients (.8%) in the validation cohort were lost to follow-up in the first year. As shown in Table 1, patients in the derivation cohort had greater cardiac comorbidity (ie, more coronary artery disease, CHE and history of VA) and were less likely to have a nolmal ED ECG (P<.01 for all comparisons). A larger proportion of patients in the derivation cohort had had more than one episode of syncope within the last year. Results from ED ECGs indicated that the most frequent abnormalities in both cohorts were conduction disorders, old myocardial infarction, and LVH or RVH. In the derivation cohort, there were 65 patients with arrhythmias (broad definition) and 39 deaths within the first year. Descriptions of the arrhythmias are presented in Table 2. Significant univariate predictors of arrhyhmias were an abnormal ECG, male sex, age greater than 45 years, nonwhite race, hist0~y of CHE history of myocardial infarction, and history of VA. As displayed in Table 3, multivariate predictors of arrhythmia were an abnormal ECG, history of VA, history of CHE age greater than 45 years, and nonwhite race. Univariate predictors of death in the first year were abnormal ECG, NST on ECG, LVH on ECG, age greater than 45 years, history of CHE history of VA, and having no prior history of syncope. LVH on ECG was not included in the multivariate modeling because it was a type of abnormality on the ECG. As displayed in Table 3, the multivariate predictors of death were an abnormal ECG, history of CHE age greater than 45 years, and having no prior history of syncope. The combined multivariate model for arrhythmia or death showed four significant factors (Table 3). These included an abnormal ECG, age greater than 45 years, history of VA, and history of CHE The odds ratios of these factors ranged from 3.1 to 4.8, but, for simplicity, they were treated as equivalent in the identification of risk groups. Four groups were identified, defined by the number of risk factors present (none, one, two, and three or four). The validation cohort had a smaller proportion of patients with three or four risk factors than the derivation cohort (P=.007). In the derivation cohort, the incidence of arrhythmias (broad definition) identified in the first year ranged from 5.5% in patients with no risk factors to 63.0% in patients with three or four risk factors (Figure, A). In the validation cohort, the model identified similar proportions of patients with arrhythmias in each risk group, ranging from 3.3% in those patients with no risk factors to 45.5% in patients with three or four risk factors. When the more strict definition of arrhythmia was employed, rates of arrhythmias decreased in all risk categories (Figure, B). However, in both the derivation and validation cohorts, the proportion of patients with arrhythmias increased as the number of risk factors increased. There were 1.8% and 0% in the lowest risk group and 43.5% to 18.2% in the highest risk group of the derivation and validation cohorts, respectively. One-year mortality rates in the derivation cohort ranged from 1.8% in patients with no risk factors to 37.0% in patients with three or four risk factors (Figure, C). In the validation cohort, mortality ranged from 1.1% in the lowest risk category to 27.3% in patients with three or four risk factors. When only cardiac causes of mortality were considered (Figure, D), mortality rates decreased in all risk groups. Cardiac mortality rates ranged from 0% to 28.3% in the derivation cohort and from 0% to 15.1% in the validation cohort. Figure part E displays the number of arrhythmias (broad definition) and deaths in the first year in the derivation and validation cohorts. In the derivation cohort, these ranged from 7.3% in patients with no risk factors to 80.4% in patients with three or four risk factors. In the validation cohort, they ranged from 4.4% in the lowest risk category to 57.6% in patients with three or four risk factors. When only strict-definition arrhythmias or cardiac causes of mortality were considered (Figure, F), the rates ranged from 1.8% Table 4. Distribution of patients across rfsl~ strata. No. From No. From No. of Derivation Cohort Validation Cohort Risk Factors (%) [n=252] (%) [n=374] 0 55 (22] 91 (24) T 63 (25) 108 (29) 2 88 (35) 142 (38} 3 or 4 46 (18) 33 {9) APRIL :4 AENALS OF EMERGENCY MEDICINE 48 3
6 RISK STRATIFICATION Martfn, Hanusa & Kapoor Figure. Performance of the syncope risk classification system. Graphs show the proportion of patients at each number of risk factors who A, had broadly defined cardiac arrhythmias; B, strictly defined cardiac arrhythmias; C, died within a year of the enrolling episode; D, died of a cardiac cause in the the enrolling episode; E, had broadly defined arrhythmias or died within the first year; and F, had strictly d@ned arrhythmias or died of a cardiac cause in the first year. A Proportion Proportion 1 IZZ] Derivation cohort E~ Derivation cohort I Validation cohort.9-- I Validation cohort C E Proportion Derivation cohort I Validation cohort,8- Lajl [~ Ii B Proportion D Proportion F Proportion,9- EZ] mi Derivation cohort Validation cohort.9- I Derivation cohort Validation cohort.9- I---I I Derivation cohort Validation cohort, , / li No of Risk Factors ANNALS OF EMERGENCY MEDICINE 29:4 APRIL 1997
7 Ma~tin, Hanusa S, Kapoor to 52.2% in the derivation cohort and from 0% to 27.3% in the validation cohort. Areas under the ROC curves range from.77 to.83 for the derivation cohort and from.73 to.80 for the validation cohort. All 12 ROC curves had areas significantly greater than.5. There were no significant differences in areas under the ROC curves in any comparison between derivation and validation cohorts; probability values ranged from.2 to.8. DISCUSSION This study showed that information available at the time of presentation to the ED can be used to stratify the risk of arrhythmias and death within 1 year in patients with syncope. We found four factors useful for risk stratification: age greater than 45 years, history of VA, history of CHE and abnormal ECG. Our model performed well whether a broadly inclusiw, definition of arrhythmias or a strict definition was used. Furthermore, when only cardiac death was considered, the mortality rates in the lower-risk strata approached zero. Our results apply to patients presenting with syncope to an ED. The proportions of patients with cardiac syncope (31% in the derivation cohort and 17% in the validation cohort) in this study were similar to or higher than those reported in unselected populations in other studies (approximately 16%). >3 Studies of syncope patients referred to electrophysiology practices report a higher proportion of patients with cardiac syncope (arrhythmias) 9-I6; our results may not be entirely applicable to these selected populations. Syq~cope is often difficult to evaluate in the ED. Patients are usually free of symptoms when they are seen after an episode, and the clinical assessment and initial ECG may be unremarkable. If a cause of syncope can be determined on the basis of initial clinical assessment (eg, symptomatic orthostatic hypotension), management decisions are relatively straightforward. However, in approximately 60% of patients a cause is not apparent on initial history, physical examination, and ECGJ Under these circumstances, the focus of evaluation is directed toward finding serious and life-threatening arrhythmias that may be inapparent on initiai clinical assessment. The concerns for arrhythmias and sudden death frequently lead to hospital admission and performance of many diagnostic tests. There are no published studies of stratification of risk of arrhythmias and death in patients with syncope using clinical and ECG data available at the time of initial presentation. Studies of risk stratification are important in devising more cost-effective management strategies for subgroups of patients. Previous prognostic studies of syncope have iden- tiffed high-risk causes, mainly cardiac causes >5, as being associated with high risk of mortality and sudden death. Although these studies have been important for determining prognosis, they are not applicable to patients presenting to the ED, because assignment of a cause of syncope often requires extensive diagnostic testing that cannot be performed in the ED. The factors used in risk stratification in this study are consistent with those reported in previous clinical and epidemiologic studies of risk of arrhythmias and mortality in patients with syncope. A recent study showed that syncope in patients with left ventricular dysfunction was associated with a particularly poor prognosis. 17 In addition, studies of the natural history of CHF showed 5-year survival rates of 25% in men and 38% in women is, clearly identifying this condition as a determinant of poor outcome. The history of CHF undoubtedly represented left ventricular dysfunction in most of our patients. Previous studies have correlated both a risk of sudden death and inducibility of sustained monomorphic VT at the time of electrophysiologic studies with left ventricular dysfunction in patients presenting with syncope. 9-st Our finding that a history of VA identified patients at risk for arrhythmias and death is consistent with results of studies documenting higher rates of sudden death and all-cause mortality in syncope patients with VT. 11,12,14,19 It is also clinically plausible that a history of VA in a patient with syncope implies a high likefihood that VT was the cause of patient's symptoms. Other studies have shown that negative predictors of abnormal electrophysiologic studies are the absence of structural heart disease and normal ECG. 15,16 These findings are consistent with our results, which showed CHF and abnormal ECG to be predictors of arrhythmias. An abnormal resting ECG may serve as a marker for underlying structural heart disease, explaining its correlation with mortality and arrhythmias. Finally, although no previous study has identified age alone as an independent risk factor for adverse outcome after a syncopal episode, data from the Framingham Heart Study documented increasing rates of sudden death in males as age increased, after controlling for cardiac risk factors. ~8 Further, age may serve as a marker for the presence of comorbid disease processes that may affect the likelihood of arrhythmias and mortality We acknowledge several limitations of this study First, the derivation and validation phases of the study were performed at a single institution which serves as a tertiary referral center for a large patient population. The generalizability of our findings needs to be tested in other clinical APRIL :4 ANNALS OF EMERGENCY MEDICINE 4 S 5
8 Martin, Hanuaa & Kapoor settings. Second, electrophysiologic testing was not performed in a large fraction of patients. Although we might have diagnosed more arrhythmias by wider use of electrophysiologic testing, our findings that structural heart disease, particularly CHE and abnormal ECG are predictors of arrhythmias probably would not have changed, because previous studies have shown these to be predictors of abnormal electrophysiologic results. 15,16 Similarly, wider use of tilt testing would not have altered the results of our study, because patients with positive tilt-test results are at low risk for arrhythmias and death. 12,2-22 REFERENCES 1. Day SC, Cook EF, Funkenstoin H, et ah Evaluation and outcome of emergency room patients with transient loss of consciousness. Am J Med 1982;73: Silverstein MD, Singer DE, Mulley A, et ah Patients with syncope admitted to medical intern sive care units. JAMA 1982;248: Martin G J, Adams SL, Martin HG, et al: Prospective evaluation of syncope. Ann Emerg Med 1984;13: Kapoor WN, Karpf M, Wieand S, et el: A prospective evaluation and follow-up of patients with syncope. N Engt J Med 1983;309: Kapoor W: Evaluation and outcome of patients with syncope. Medicine fbaltimore) 1990;69: Cupples LA, Gagnen DR, Kennel WB: Long- and short4erm risk of sudden coronary death. Circulation 1992;85 (suppl)fll Dickson WJ (edl: BMDP Statistical Software Manual Berkeley: University of California Press, Metz CE, Shen JH, Wang PL, et ah ROCFIE Chicago: University of Chicago, Bachinsky WB, Linzer M, Weld L, et ah Usefulness of clinical characteristics in predicting the outcome of electrophysiologic studies in unexplained syncope. Am J Cardio11992;69: Teichman SL, Felder SD, Mates JA, et al: The value of electrophysiologic studies in syncope of undetermined origin: Report of 150 cases. Am Heart J 1988;110: E}oherty JU, Pembrook-Regers D, Grogan EW, et el: Electrephysiologic evaluation and followup characteristics of patients with recurrent unexplained syncope and presyncope. Am J Cardiol 1985;55: Sra JS, Anderson A J, Sheikh SH, et ah Unexplained syncope evaluated by e[ectrophysiologic studies and head-up tilt testing. Ann Intern Meal1991;114: Moazez F, Peter T, Simonson J, et ah Syncope of unknown origin: Clinical noninvasive and electrophysiologic determinants of arrhythmia induction and symptom recurrence during longterm follow-up. Am Heart J 1991 ;121: Bass EB, Elson J J, Fogoros RN, et ah Long-term prognosis of patients undergoing electrophysiologic studies for syncope of unknown origin. Am J Cardio11988;62: Krol RB, Merady F, Flaker GC, et ah Electrophysiologic testing in patients with unexplained syncope: Clinical and noninvasive predictors of outcome. JAm Coil Cardio11997;lg: Denes P, Vretz E, Ezr MD, et L: Clinical predictors of electrophysielogic findings in patients with syncope of unknown origin. Arch Intern Mef11988;148: Middlekauff HR, Stevenson WG, Stevenson LW, et el: Syncope in advanced heart failure: High risk of sudden death regardless of origin of syncope. J Am Cod Cardiol 1993;21: He KK, Anderson KM, Kannel WB, et ah Survival after the onset of congestive heart failure in Framingham Heart Study subjects. Circulation 1993;88: Kapoar WN, Cha R, Peterson J, et ah Prolonged electrocardiographic monitoring in patients with syncope: Importance of frequent or repetitive ventricular ectopy. Am J Med 1987;82: Almquist A, Goldenberg IF, Milstein S, et ah Provocation of hradycardia and hypotension by isopreterenol and upright posture in patients with unexplained syncope. N EnglJ Med 1989;320: Grubb BP, Temesy-Armos P, Hahn H, et al: Utility of upright tilt-table testing in the evaluation and management of syncope of unknown origin. Am J Med 1991 ;90; Kapoor WN, Smith M, Miller NL: Upright tilt testing in evaluating syncope: A comprehensive literature review. Am J Meal 1994;97: Reprint no. 47/1/79922 Address for reprints: Wishwa N Kapoor, MD Suite 9W-933, 200 Lothrop Street Mantefiore University Hospital Pittsburgh, Pennsylvania Fax ANNALS OF EMERGENCY MEDICINE 29:4 APRIL 1997
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
510(k) Summary May 7, 2012
 510(k) Summary Medicalgorithmics 510(k) Premarket Notification 510(k) Summary May 7, 2012 1. Submitter Name and Address Medicalgorithmics LLC 245 West 107th St., Suite 11A New York, NY 10025, USA Contact
510(k) Summary Medicalgorithmics 510(k) Premarket Notification 510(k) Summary May 7, 2012 1. Submitter Name and Address Medicalgorithmics LLC 245 West 107th St., Suite 11A New York, NY 10025, USA Contact
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout.
 Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ABSTRACT Background Little is known about the epidemiology and prognosis of syncope in the general population.
 INCIDENCE AND PROGNOSIS OF SYNCOPE ELPIDOFOROS S. SOTERIADES, M.D., JANE C. EVANS, D.SC., MARTIN G. LARSON, SC.D., MING HUI CHEN, M.D., LEWAY CHEN, M.D., EMELIA J. BENJAMIN, M.D., AND DANIEL LEVY, M.D.
INCIDENCE AND PROGNOSIS OF SYNCOPE ELPIDOFOROS S. SOTERIADES, M.D., JANE C. EVANS, D.SC., MARTIN G. LARSON, SC.D., MING HUI CHEN, M.D., LEWAY CHEN, M.D., EMELIA J. BENJAMIN, M.D., AND DANIEL LEVY, M.D.
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Electrocardiographic Issues in Williams Syndrome
 Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
In general, causes of syncope are addressed as entities
 414 Multiple Causes of Syncope Original Article Prevalence and Clinical Outcomes of Patients With Multiple Potential Causes of Syncope LIN Y. CHEN, MD; BERNARD J. GERSH, MB, CHB, DPHIL; DAVID O. HODGE,
414 Multiple Causes of Syncope Original Article Prevalence and Clinical Outcomes of Patients With Multiple Potential Causes of Syncope LIN Y. CHEN, MD; BERNARD J. GERSH, MB, CHB, DPHIL; DAVID O. HODGE,
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Prognostic impact of uric acid in patients with stable coronary artery disease
 Prognostic impact of uric acid in patients with stable coronary artery disease Gjin Ndrepepa, Siegmund Braun, Martin Hadamitzky, Massimiliano Fusaro, Hans-Ullrich Haase, Kathrin A. Birkmeier, Albert Schomig,
Prognostic impact of uric acid in patients with stable coronary artery disease Gjin Ndrepepa, Siegmund Braun, Martin Hadamitzky, Massimiliano Fusaro, Hans-Ullrich Haase, Kathrin A. Birkmeier, Albert Schomig,
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm
 CHAPTER 6 Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm JW Haveman, A Karliczek, ELG Verhoeven, IFJ Tielliu, R de Vos, JH Zwaveling, JJAM
CHAPTER 6 Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm JW Haveman, A Karliczek, ELG Verhoeven, IFJ Tielliu, R de Vos, JH Zwaveling, JJAM
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
2320-6691 2015; 3(3B):1132-1136 ISSN 2347-954X
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3B):1132-1136 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3B):1132-1136 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Wyatt Decker, M.D., FACEP Mayo Clinic College of Medicine, 200 First Street SW, Rochester, MN 55905
 WHICH PATIENTS WITH SYNCOPE NEED TO BE ADMITTED TO THE HOSPITAL Wyatt Decker, M.D., FACEP Mayo Clinic College of Medicine, 200 First Street SW, Rochester, MN 55905 Case Unresponsive 82 y.o. male - found
WHICH PATIENTS WITH SYNCOPE NEED TO BE ADMITTED TO THE HOSPITAL Wyatt Decker, M.D., FACEP Mayo Clinic College of Medicine, 200 First Street SW, Rochester, MN 55905 Case Unresponsive 82 y.o. male - found
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Il loop recorder esterno. Roberto Maggi
 Il loop recorder esterno Roberto Maggi ECG monitoring and syncope In-hospital monitoring Holter Monitoring Event recorder External loop recorder Remote (at home) telemetry Implantable loop recorder External
Il loop recorder esterno Roberto Maggi ECG monitoring and syncope In-hospital monitoring Holter Monitoring Event recorder External loop recorder Remote (at home) telemetry Implantable loop recorder External
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
DISCLOSURES RISK ASSESSMENT. Stroke and Heart Disease -Is there a Link Beyond Risk Factors? Daniel Lackland, MD
 STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
Main Effect of Screening for Coronary Artery Disease Using CT
 Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Acquired, Drug-Induced Long QT Syndrome
 Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Clinical Glidepath TM Tools Syncope Frail Life expectancy less than five years or significant functional impairment
 Robust Elderly greater ALL GROUPS 1 SYMPTOMS a) wth, nausea b) postural symptoms c) chest pain, dyspnea, post-exercise, dizziness, history of heart disease, palpitations, family history (prolonged QT)
Robust Elderly greater ALL GROUPS 1 SYMPTOMS a) wth, nausea b) postural symptoms c) chest pain, dyspnea, post-exercise, dizziness, history of heart disease, palpitations, family history (prolonged QT)
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Osama Jarkas. in Chest Pain Patients. STUDENT NAME: Osama Jarkas DATE: August 10 th, 2015
 STUDENT NAME: Osama Jarkas DATE: August 10 th, 2015 PROJECT TITLE: Analysis of ECG Exercise Stress Testing and Framingham Risk Score in Chest Pain Patients PRIMARY SUPERVISOR NAME: Dr. Edward Tan DEPARTMENT:
STUDENT NAME: Osama Jarkas DATE: August 10 th, 2015 PROJECT TITLE: Analysis of ECG Exercise Stress Testing and Framingham Risk Score in Chest Pain Patients PRIMARY SUPERVISOR NAME: Dr. Edward Tan DEPARTMENT:
Tips for surviving the analysis of survival data. Philip Twumasi-Ankrah, PhD
 Tips for surviving the analysis of survival data Philip Twumasi-Ankrah, PhD Big picture In medical research and many other areas of research, we often confront continuous, ordinal or dichotomous outcomes
Tips for surviving the analysis of survival data Philip Twumasi-Ankrah, PhD Big picture In medical research and many other areas of research, we often confront continuous, ordinal or dichotomous outcomes
Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD
 92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
FULL COVERAGE FOR PREVENTIVE MEDICATIONS AFTER MYOCARDIAL INFARCTION IMPACT ON RACIAL AND ETHNIC DISPARITIES
 FULL COVERAGE FOR PREVENTIVE MEDICATIONS AFTER MYOCARDIAL INFARCTION IMPACT ON RACIAL AND ETHNIC DISPARITIES Niteesh K. Choudhry, MD, PhD Harvard Medical School Division of Pharmacoepidemiology and Pharmacoeconomics
FULL COVERAGE FOR PREVENTIVE MEDICATIONS AFTER MYOCARDIAL INFARCTION IMPACT ON RACIAL AND ETHNIC DISPARITIES Niteesh K. Choudhry, MD, PhD Harvard Medical School Division of Pharmacoepidemiology and Pharmacoeconomics
Sleep Heart Health Study (SHHS) ECG Protocol
 Sleep Heart Health Study (SHHS) ECG Protocol SHHS 1 Electrocardiography (ECG) Baseline ECG is performed in all parent study clinic visits preceding the PSG. All sites perform a standard resting 12-lead
Sleep Heart Health Study (SHHS) ECG Protocol SHHS 1 Electrocardiography (ECG) Baseline ECG is performed in all parent study clinic visits preceding the PSG. All sites perform a standard resting 12-lead
How do you decide on rate versus rhythm control?
 Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
Signal-averaged electrocardiography late potentials
 SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Translating Science to Health Care: the Use of Predictive Models in Decision Making
 Translating Science to Health Care: the Use of Predictive Models in Decision Making John Griffith, Ph.D., Associate Dean for Research Bouvé College of Health Sciences Northeastern University Topics Clinical
Translating Science to Health Care: the Use of Predictive Models in Decision Making John Griffith, Ph.D., Associate Dean for Research Bouvé College of Health Sciences Northeastern University Topics Clinical
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
Professor Rose Anne Kenny, St James Hospital &Trinity College, Dublin
 Syncope Presentation and Investigation in the Acute Setting Professor Rose Anne Kenny, St James Hospital &Trinity College, Dublin Definition- Presentation Syncope is a syndrome consisting of a relatively
Syncope Presentation and Investigation in the Acute Setting Professor Rose Anne Kenny, St James Hospital &Trinity College, Dublin Definition- Presentation Syncope is a syndrome consisting of a relatively
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Impact of Massachusetts Health Care Reform on Racial, Ethnic and Socioeconomic Disparities in Cardiovascular Care
 Impact of Massachusetts Health Care Reform on Racial, Ethnic and Socioeconomic Disparities in Cardiovascular Care Michelle A. Albert MD MPH Treacy S. Silbaugh B.S, John Z. Ayanian MD MPP, Ann Lovett RN
Impact of Massachusetts Health Care Reform on Racial, Ethnic and Socioeconomic Disparities in Cardiovascular Care Michelle A. Albert MD MPH Treacy S. Silbaugh B.S, John Z. Ayanian MD MPP, Ann Lovett RN
38 year old female with mild obesity. She is planning an exercise program to loose weight. She has no other known risk factors for CAD.
 Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Coronary Heart Disease (CHD) Brief
 Coronary Heart Disease (CHD) Brief What is Coronary Heart Disease? Coronary Heart Disease (CHD), also called coronary artery disease 1, is the most common heart condition in the United States. It occurs
Coronary Heart Disease (CHD) Brief What is Coronary Heart Disease? Coronary Heart Disease (CHD), also called coronary artery disease 1, is the most common heart condition in the United States. It occurs
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
4/7/2015. Cardiac Rehabilitation: From the other side of the glass door. Chicago, circa 1999. Objectives. No disclosures, no conflicts
 Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
Conflicts of interest: None
 Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
The Role Of Early Stress Testing In Assessing Low Risk Chest Pain Patients Admitted Through The Emergency Department
 The Role Of Early Stress Testing In Assessing Low Risk Chest Pain Patients Admitted Through The Emergency Department Simbo Chiadika LAY ABSTRACT A. Study purpose Cardiac stress testing has been recommended
The Role Of Early Stress Testing In Assessing Low Risk Chest Pain Patients Admitted Through The Emergency Department Simbo Chiadika LAY ABSTRACT A. Study purpose Cardiac stress testing has been recommended
MADIT-II CLINICAL SUMMARY
 CAUTION: Federal law restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY MADIT-II Boston Scientific Corporation
CAUTION: Federal law restricts this device to sale by or on the order of a physician trained or experienced in device implant and follow-up procedures. CLINICAL SUMMARY MADIT-II Boston Scientific Corporation
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics. Yen Tibayan, M.D. Division of Cardiovascular Medicine
 Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Independent Contribution of Electrocardiographic Abnormalities to Risk of Death from Coronary Heart Disease, Cardiovascular Diseases and All Causes
 Independent Contribution of Electrocardiographic Abnormalities to Risk of Death from Coronary Heart Disease, Cardiovascular Diseases and All Causes Findings of Three Chicago Epidemiologic Studies BLANCO
Independent Contribution of Electrocardiographic Abnormalities to Risk of Death from Coronary Heart Disease, Cardiovascular Diseases and All Causes Findings of Three Chicago Epidemiologic Studies BLANCO
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Cardiovascular Endpoints
 The Malmö Diet and Cancer Study Department of Clinical Sciences Skåne University Hospital, Malmö Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 30
The Malmö Diet and Cancer Study Department of Clinical Sciences Skåne University Hospital, Malmö Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 30
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Malmö Preventive Project. Cardiovascular Endpoints
 Malmö Preventive Project Department of Clinical Sciences Malmö University Hospital Lund University Malmö Preventive Project Cardiovascular Endpoints End of follow-up: 31 Dec 2008 * Report: 21 June 2010
Malmö Preventive Project Department of Clinical Sciences Malmö University Hospital Lund University Malmö Preventive Project Cardiovascular Endpoints End of follow-up: 31 Dec 2008 * Report: 21 June 2010
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
How to read the ECG in athletes: distinguishing normal form abnormal
 How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Elevated heart rate at twelve months after heart transplantation is an independent predictor of long term mortality
 Elevated heart rate at twelve months after heart transplantation is an independent predictor of long term mortality C. Tomas, MA Castel, E Roig, I. Vallejos, C. Plata, F. Pérez-Villa Cardiology Department,
Elevated heart rate at twelve months after heart transplantation is an independent predictor of long term mortality C. Tomas, MA Castel, E Roig, I. Vallejos, C. Plata, F. Pérez-Villa Cardiology Department,
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians
 Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Telecardiology Technical Innovations and Challegenes in Clinical Practice
 Telecardiology Technical Innovations and Challegenes in Clinical Practice Axel Müller Clinic of Internal Medicine I (Head of Department: Prof. Dr. med. J. Schweizer) Klinikum Chemnitz ggmbh June 24, 2015
Telecardiology Technical Innovations and Challegenes in Clinical Practice Axel Müller Clinic of Internal Medicine I (Head of Department: Prof. Dr. med. J. Schweizer) Klinikum Chemnitz ggmbh June 24, 2015
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
Ruchika D. Husa, MD, MS Assistant t Professor of Medicine in the Division of Cardiology The Ohio State University Wexner Medical Center
 Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Barriers to Healthcare Services for People with Mental Disorders. Cardiovascular disorders and diabetes in people with severe mental illness
 Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Provider Checklist-Outpatient Imaging. Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469)
 Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Malmö Preventive Project. Cardiovascular Endpoints
 Malmö Preventive Project Department of Clinical Sciences Skåne University Hospital, Malmö Lund University Malmö Preventive Project Cardiovascular Endpoints End of follow-up: 30 June 2009 Report: 7 October
Malmö Preventive Project Department of Clinical Sciences Skåne University Hospital, Malmö Lund University Malmö Preventive Project Cardiovascular Endpoints End of follow-up: 30 June 2009 Report: 7 October
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Autonomic Stress Test
 Autonomic Stress Test (The expanded head-up tilt test) Artur Fedorowski Syncope Unit Skåne University Hospital, Malmö, Sweden NordSync 2011, Malmö Disclosure None The expanded head-up tilt test When? Why?
Autonomic Stress Test (The expanded head-up tilt test) Artur Fedorowski Syncope Unit Skåne University Hospital, Malmö, Sweden NordSync 2011, Malmö Disclosure None The expanded head-up tilt test When? Why?
Cardiovascular Endpoints
 The Malmö Diet and Cancer Study Department of Clinical Sciences Malmö University Hospital Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 31 Dec * Report:
The Malmö Diet and Cancer Study Department of Clinical Sciences Malmö University Hospital Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 31 Dec * Report:
Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University
 Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Define exercise associated collapse (EAC) and exercise-associated postural hypotension
Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Define exercise associated collapse (EAC) and exercise-associated postural hypotension
Ngaire has Palpitations
 Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
RISK STRATIFICATION for Acute Coronary Syndrome in the Emergency Department
 RISK STRATIFICATION for Acute Coronary Syndrome in the Emergency Department Sohil Pothiawala FAMS (EM), MRCSEd (A&E), M.Med (EM), MBBS Consultant Dept. of Emergency Medicine Singapore General Hospital
RISK STRATIFICATION for Acute Coronary Syndrome in the Emergency Department Sohil Pothiawala FAMS (EM), MRCSEd (A&E), M.Med (EM), MBBS Consultant Dept. of Emergency Medicine Singapore General Hospital
MEDICAL POLICY No. 91104-R7 DETOXIFICATION I. POLICY/CRITERIA
 DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
A list of FDA-approved testosterone products can be found by searching for testosterone at http://www.accessdata.fda.gov/scripts/cder/drugsatfda/.
 FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
Physician and other health professional services
 O n l i n e A p p e n d i x e s 4 Physician and other health professional services 4-A O n l i n e A p p e n d i x Access to physician and other health professional services 4 a1 Access to physician care
O n l i n e A p p e n d i x e s 4 Physician and other health professional services 4-A O n l i n e A p p e n d i x Access to physician and other health professional services 4 a1 Access to physician care
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation
 A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
