Clin Plastic Surg 32 (2005) Hair Restoration. Alfonso Barrera, MD, FACS
|
|
|
- Jacob Day
- 8 years ago
- Views:
Transcription
1 Clin Plastic Surg 32 (2005) Hair Restoration Alfonso Barrera, MD, FACS Baylor College of Medicine, 902 Frostwood, Suite #163, Houston, TX 77024, USA The use of micrografts (one or two hair follicular unit grafts) and minigrafts (three or four hair follicular unit grafts) in large numbers has revolutionized hair restoration in aesthetic and reconstructive cases and has rapidly become the technique of choice in most cases. The use of single-hair grafts is not a new concept. Tumura [1] in 1943 was the first to report the use of single-hair grafts to restore pubic hair. Fujita [2] in 1953 reconstructed eyebrows with single-hair grafts. The first reports on the use of single-hair grafts on the scalp were by Nordstrom [3] in 1980 and Marritt [4] in 1981 who introduced the use of single-hair grafts to the front hairline to camouflage plugs and scars from previous hair restoration procedures. This provided natural-looking hairlines by providing a transition zone in the front. It was, however, time consuming and at that time it did not seem to be a viable alternative to restore hair for larger areas of hair loss. In 1991, Uebel [5] introduced the use of micrografts (1 2 hair grafts) and minigrafts (3 4 hair grafts) in large numbers ( grafts) to cover large areas of hair loss, such as the entire top of the head in cases of male pattern baldness (MPB).The author has subsequently further increased the number of grafts transplanted in a single session up to 2500 and has described multiple other applications for micrografts and minigrafts, such as restoring naturallooking hair in the face and scalp (eg, restoring natural-looking sideburns, eyebrows, mustaches, beard) and, more recently, other body areas including lower legs [6 12]. address: abarrera@lookinggood.com In 1984, Headington [13] described an important concept in hair anatomy the follicular unit. When we study the histology of skin (scalp), traditionally we see vertical sections. Headington studied transverse microscopic sections of the human scalp and noticed that hair grows in follicular units of one, two, three, or four hair follicles with their independent neurovascular boundless, sebaceous glands, sweat glands, and pilo-erectile muscle surrounded by a sheath of collagen (Fig. 1). These follicular units seem to be true physiologic units. Mantaining them as intact as possible seems to increase the survival and ultimate hair growth of the grafts. The life-cycle phases of a hair follicle Anagen is the actively growing phase. In this phase, the follicular cells are actively multiplying and keratinizing. In a nonbalding scalp, normally about 90% of the hairs are in this phase, which lasts about 3 years. During the catagen phase, the base of the hair becomes keratinized, forming a club, and separates itself from the dermal papilla. It then moves toward the surface and is eventually connected to the dermal papilla only by a connective tissue strand. This phase lasts 2 to 3 weeks. During the telogen phase, also called the resting phase, the attachment at the base of the follicle becomes weaker until the hair finally sheds. During this period, the follicle is inactive, and hair growth ceases. This phase lasts 3 to 4 months and commonly occurs after hair transplantation. For this reason, significant growth of the hair grafts is not seen until this phase is over. Some of the native hair often goes into the catagen and then into the telogen phase from the insult of the surgery; this is called telogen effluvium /05/$ see front matter D 2005 Elsevier Inc. All rights reserved. doi: /j.cps plasticsurgery.theclinics.com
2 164 barrera I use one- and two-hair follicular units as micrografts and three- and four-hair follicular units as minigrafts (Fig. 2). When dissecting grafts I keep two, three, or four hair follicles together as a unit and preserve the tissue around the hair shaft of single hair grafts to make sure I preserve all the vital components. The appearance of fullness has to do with hair mass, which is related to the number of hairs, the thickness of the individual hair shafts, the texture and color of the hair, and the curliness of the hair. The contrast of colors between the scalp and the hair has a significant influence on the optical illusion of fullness. The average healthy nonbalding patient has a density of about 200 hairs/cm 2 (range ); only 50% of this number is needed to give an appearance of normal density, which is about 100 hairs/cm 2 (range ). This number can be transplanted in two sessions of micrografting and minigrafting. Patient selection Fig. 1. Transverse histologic section of scalp demonstrating follicular units. We have no method to create new hair. All current techniques for hair restoration involve redistributing the patient s existing hair. Therefore, candidates for hair transplantation are limited to those who have a favorable donor site surface area and density relative to the size of the area to be transplanted. Several centers worldwide are working on tissue engineering in an attempt to clone hair follicles or culture and multiply hair follicles in the laboratory setting. When successful, we will be able to treat patients with limited donor hair and need only harvest a sample of hair follicles. This would eliminate donor site morbidity and discomfort almost completely. MPB is a progressive condition. The rate of hair loss may slow down after 40 years of age, but it never stops completely. Therefore, the preoperative plan must ensure a natural-looking long-term result. Good communication with patients is essential to establish realistic expectations. Fig. 2. Drawing of follicular unit micrografts and minigrafts. (From Barrera A. Hair transplantation: the art of micrografting and minigrafting. 1st edition. St. Louis (MO): Quality Medical Publishing Inc.; 2002; with permission.)
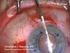
3 hair restoration 165 Reconstructive applications of micrografts and minigrafts Micrografts and minigrafts grow anywhere on the face and thus are useful for restoring sideburns, temporal hairline, eyebrows, mustache, beard, etc. The most common reasons for using micrografts and minigrafts in reconstructive cases include (1) revision of unfavorable results from previous hair transplantation procedures (eg, the plug look, corn field rows, and hairline scars); (2) post-surgical conditions, such as the lost sideburn and temporal hairline after facelift and other facial rejuvenating procedures; (3) post-traumatic injuries; (4) correction of hair loss burn injuries; and (5) certain congenital conditions, such as is the absence of hair on the prolabium in cases of bilateral cleft lips, hair loss due to excision of congenital hairy nevus, arterio-venous malformations, or after involution of strawberry hemangiomas. Technique For cases of MPB I normally do between 1000 and 2500 grafts per session (megasessions) depending on the degree of hair loss. This labor-intensive procedure requires an organized and efficient surgical team. My surgical team consists of three surgical assistants and myself. I remain in the operating room for the duration of the procedure and insert all grafts personally. Efficiency is the key when transplanting a large number of grafts in a single session. The patient is placed in the supine position and mildly sedated with midazolam (2 10 mg) and fentanyl (25 50 mg), which are titrated for each patient. I usually treat pediatric patients under general anesthesia. The patient s vital signs, EKG, and O 2 saturation are monitored throughout the procedure. Supraorbital and occipital nerve blocks are established with 0.5% bupivacaine with 1:200,000 epinephrine (~30 ml). This includes a ring block just below the proposed hairline. A tumescent solution of 0.5% lidocaine with 1:200,000 epinephrine is infiltrated in the donor site. The patient s head is turned to the left, and harvesting of the right half of the donor ellipse is begun immediately. Under 3.5 loupe magnification with Personna Prep Blades, thin slices ( mm) are dissected from the donor ellipse over a sterile wooden board and handed to the assistants. The assistants prepare the final grafts from these slices while the surgeon closes the right half of the donor strip. Careful dissection of the thin slices into micrographs and minigrafts is the most tedious part of the procedure and one of the most important steps. The incisions must be made precisely parallel to the hair shafts at all times to minimize the loss of hair follicles. Graft dissection To dissect the slices into micrografts and minigrafts, the assistants use 3.5 loupe magnification, Fig. 3. Technique of micrograft and minigraft transplantation: slit and slide. (From Barrera A. Hair transplantation: the art of micrografting and minigrafting. 1st edition. St. Louis (MO): Quality Medical Publishing Inc.; 2002; with permission.)
4 166 barrera no. 10 Bard Parker blades, and jeweler s forceps. They generally work over a wooden board that has been autoclaved. The darker and thicker the individual hair shafts, the easier it is to dissect the grafts. The ideal grafts have intact hair shafts all the way from the subcutaneous fatty tissue to the scalp surface, are somewhat thick, and contain from one to four hairs. They must be handled as atraumatically as possible. The grafts are held by the fatty tissue under the hair bulbs or by the tissue around them, not by the hair bulb or dermal hair papilla. In cases of very-light-colored or white hair, we use microscopes (10) for a safe dissection of the grafts (I prefer the Mantis Microscope). The surgeon turns the patient s head to the right for harvesting the left half of the donor ellipse. The surgeon closes the left side donor site and finishes slicing the remaining segment of the donor ellipse into slides. Several Fig. 4. A 28-year-old man with male pattern baldness V. (A) Before, front view. (B) One year after a 1783 micrograft and minigraft megasession, front view. (C) Side view, before. (D) Side view, after. (E) Top of the head, before. (F) Top of the head, after.
5 hair restoration 167 hundred grafts have been dissected at this point. They are lined up in rows on a wet green or blue towel and are ready for insertion. The process of graft dissection and insertion continues until all the grafts are transplanted. It is imperative to keep the grafts wet in normal saline solution and chilled to approximately 4 C until they are lined up for insertion. If the graft becomes desiccated, no hair growth will occur. Key points to remember in graft dissection are: Maintain the follicular units as intact as feasible. In patients with dark hair, 3.5 loupe magnification is sufficient to dissect most grafts as follicular units. In patients with light hair or gray hair, surgical microscopes and background lighting may be needed for more accurate dissection. Fig. 5. A 58-year-old woman who lost her sideburns due to a facelift procedure. (A) Before. (B) Planning the hairline to be restored. (C) At the end of surgery, she received 400 micrografts and minigrafts (200 per side); side view. (D) One year after, side view. (E) One year after, oblique view. Notice the direction of the hair growth and the absence of detectable scarring.
6 168 barrera Graft insertion Infiltration of tumescent solution into the recipient area is important for several reasons, the most important of which are to promote hemostasis and to produce temporary edema of the scalp, which facilitates graft insertion. I inject 150 ml of 0.5% lidocaine with 1:200,000 epinephrine when transplanting 2000 or more. If good hemostasis is not obtained with this amount of solution, I increase the epinephrine strength to 1:100,000. Optimal hemostasis is often achieved if the tumescent solution is infiltrated in thirds. I first inject the anterior region once a large number of grafts have been inserted. I proceed posteriorly, doing the same for the middle third and the posterior third. Doing this allows us to take advantage of the peak times of epinephrine effect. As fibrinogen turns into fibrin, the grafts adhere better to the recipient slits. We repetitively return anteriorly to insert more grafts, packing them densely to minimize popping out of neighboring grafts. The epinephrine effect is often still adequate when returning to the anterior region to place additional grafts; otherwise, we re-inject. I use a slit-and-insert technique, so there is no need for punch removal of scalp or dilators. A slit is created, and immediately a graft is inserted (Fig. 3). I use 22.5 sharp point blades at and 1 cm in front of the hairline to create a nice transition zone, intentionally making a slight irregularity to mimic nature. With these blades, the scars are undetectable. Posterior to that I prefer to use no. 11 Feather Personna blades. Fig. 4 shows an example of a 28-year-old man with MPB V before and a year after a single megasession of 1783 micrografts and minigrafts. On the face, the technique of graft insertion is similar but more difficult because there is much more tendency for grafts to pop out as others are inserted. My experience in restoring the eyebrows, mustache, or beard has shown that it is best to make most or all of the slits initially and insert the grafts later to minimize this problem. Fig. 6. A 39-year-old male third-degree burn victim. (A) Before. (B) Surgical planning of the hair to be restored outlined by marking pen. (C) One year after a single session of 180 micrografts and minigrafts. (D) Close up, after.
7 hair restoration 169 On small cases, the grafts are harvested from a small donor ellipse from the occipital area posterior to the mastoid prominence and dissected as for scalp transplantation. The size of the donor strip varies from very small to a large depending on the number of grafts needed and the donor site hair density. The slits on the face are made with a no Sharpoint blade. You can also use a NoKor 18-gauge needle, always inserting the blade at the angle of the desired direction of hair growth, laterally and upward following the direction of the natural eyebrows. In the case of sideburns or temporal hair line, mustache, or beard, we angle the blade with which we are making the slits so it orients the hair growth in the proper direction. Fig. 5 shows a 58-year-old woman who lost her sideburns secondary to a facelift procedure. She underwent 400 micrografts and minigrafts (200 per side). Fig. 6 shows an example of a 39-year-old male thirddegree burn victim with loss of moustache hair before and 1 year after a single session of 180 micrografts. For dressings I generally use one or two layers of adaptic, Kurlex, and a 3-in elastic Ace bandage for the scalp. I use adaptic, gauze, and 0.5-in SteriStrips or hypoallergenic paper tape (Micropore) on the face. The hair transplanted to the face is usually harvested from the scalp, so it has the characteristics of scalp hair and thus needs to be trimmed frequently. Axillary or pubic hair can be used but require a larger donor ellipse because these areas normally have less hair density. When revising previous hair transplantation if the plugs are large, I usually combine plug reduction (partial removal of the plugs) and recycle the plugs as micrografts and minigrafts and use additional grafts (if available) in front and between the plugs to obtain optimal improvement [14,15]. The plug reduction is done by coring out hair follicles with a 2- to 4-mm Punch biopsy forceps. The insertion of the grafts is done as described previously. Problems and complications As with a face-lift procedure, patients are told to expect dysesthesia and hypesthesia cephalad to the horizontal donor site closure. This resolves within a few weeks to months. I have encountered few complications. In 9 years I have treated over 500 patients without a single incidence of infection or hematoma. In one patient who had undergone four hair plug procedures elsewhere, a minor dehiscence occurred at the donor site closure (<1 in), but this granulated and healed spontaneously. In two patients, one who was African American and the other of Mediterranean origin, keloid scars developed at the donor site only. Initially, many patients had ingrown hairs and small inclusion cysts because I inserted the grafts too deep. I learned to prevent this by leaving the epidermis of the grafts slightly superficial to the epidermis of the recipient scalp, which also prevents small-diameter pitting. Summary For aesthetic and reconstructive hair restoration cases I prefer the use of micrografts and minigrafts for several reasons: There is a natural short-term and long-term result. There is minimal (usually undetectable) scarring. Minimal down time can often be accomplished in just one session or two sessions. There is quick healing and recovery. The direction of the hair can usually be controlled by angling the surgical blade (the most difficult areas include eyelashes and eyebrows). The desired hairline design can be controlled with precision. There are no worries about flap ischemia, tip necrosis, or expander exposures and extrusion. In my experience, micrografting and minigrafting provide a high level of patient satisfaction. References [1] Fujita K. Reconstruction of eyebrows. La Lepr 1953; 22:364. [2] Tamura H. Pubic hair transplantation. Jpn J Dermatol 1943;53:76. [3] Nordstrom REA. Micrigrafts for improvement of the frontal hairline after hair transplantation. Aesthetic Plast Surg 1981;5:97. [4] Marritt E. Single hair transplantation for hairline refinement: a practical solution. J Dermatol Surg Oncol 1984;10:962. [5] Uebel CO. Micrografts and minigrafts: a new approach to baldness surgery. Ann Plast Surg 1991;27:476. [6] Barrera A. Micrograft and minigraft megasession hair transplantation: review of 100 consecutive cases. Aesth Surg J 1997;17:165. [7] Barrera A. Micrograft and minigraft megasession hair transplantation results after a single session. Plast Reconstr Surg 1997;100:1524.
8 170 barrera [8] Barrera A. Refinements in hair transplantation: micro and minigraft megasession. Perspect Plast Surg 1998; 11:53. [9] Barrera A. The use of micrografts and minigrafts for the correction of the postrhytidectomy lost sideburn. Plast Reconstr Surg 1998;102:2273. [10] Barrera A. The use of micrografts and minigrafts for the treatment of burn alopecia. Plast Reconstr Surg 1999;103:581. [11] Barrera A. Hair grafting tips and techniques. Perspect Plast Surg 2001;15: [12] Barrera A. Hair transplantation: the art of micrografting and minigrafting. 1st edition. St. Louis (MO)7 Quality Medical Publishing Inc.; [13] Headington JT. Transverse microscopic anatomy of the human scalp. Arch Dermatol 1984;120:449. [14] Lucas MWG. Partial retransplantation: a new approach in hair transplantation. J Dermatol Surg Oncol 1994; 20:511. [15] Vogel JE. Correction of the cornrow transplant and other common problems in surgical hair restoration. Plast Reconstr Surg 2000;105:
STATE OF THE ART SURGICAL TECHNIQUE: FOLLICULAR UNIT HAIR GRAFTING
 STATE OF THE ART SURGICAL TECHNIQUE: FOLLICULAR UNIT HAIR GRAFTING Author: Jeffrey S. Epstein, M.D., F.A.C.S. Clinical Professor, University of Miami Private Practice, Miami, FL 305.666.1774 305.666.6708
STATE OF THE ART SURGICAL TECHNIQUE: FOLLICULAR UNIT HAIR GRAFTING Author: Jeffrey S. Epstein, M.D., F.A.C.S. Clinical Professor, University of Miami Private Practice, Miami, FL 305.666.1774 305.666.6708
where hair grows Hair Restoration NO SCARS NO PAIN NO STRIPS It s your Hair - 100% Natural Results
 where hair grows Hair Restoration NO SCARS NO PAIN NO STRIPS It s your Hair - 100% Natural Results GOING BALD? HAIR LOSS? THINNING? NO MORE! - HAIR RESTORATION FROM FUECLINICS Hair transplantation involves
where hair grows Hair Restoration NO SCARS NO PAIN NO STRIPS It s your Hair - 100% Natural Results GOING BALD? HAIR LOSS? THINNING? NO MORE! - HAIR RESTORATION FROM FUECLINICS Hair transplantation involves
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
FUNCTIONS OF THE SKIN
 FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FOLLICLAR UNIT TRANSPLANTATION. An Overview
 HAIR FOLLICLAR UNIT TRANSPLANTATION An Overview The desire for Increased Naturalness led to Follicular Unit Transplantation FOLLICULAR UNIT S FOLLICULAR UNIT TRANSPLANTATION Graft Type 1-3(4) Hair Fu
HAIR FOLLICLAR UNIT TRANSPLANTATION An Overview The desire for Increased Naturalness led to Follicular Unit Transplantation FOLLICULAR UNIT S FOLLICULAR UNIT TRANSPLANTATION Graft Type 1-3(4) Hair Fu
5 Upper eyelid blepharoplasty
 5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
How To Harvest Fat From The Infratemporal Fossila
 Techniques in Cosmetic Surgery Harvesting Fat from the Infratemporal Fossa Bahman Guyuron, M.D., and Kevin Rose, M.D. Cleveland, Ohio As part of forehead rejuvenation and surgical treatment of migraine
Techniques in Cosmetic Surgery Harvesting Fat from the Infratemporal Fossa Bahman Guyuron, M.D., and Kevin Rose, M.D. Cleveland, Ohio As part of forehead rejuvenation and surgical treatment of migraine
Lesions, and Masses, and Tumors Oh My!!
 Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
CHAPTER 47 STRUCTURAL FAT GRAFTING
 CHAPTER 47 STRUCTURAL FAT GRAFTING SYDNEY R. COLEMAN With the recent recognition of the importance of soft-tissue fillers, fat grafting has assumed an increasingly important roll as both an adjunctive
CHAPTER 47 STRUCTURAL FAT GRAFTING SYDNEY R. COLEMAN With the recent recognition of the importance of soft-tissue fillers, fat grafting has assumed an increasingly important roll as both an adjunctive
Chapter 12. Anatomy of Skin. Epidermis. Dermis
 Chapter 12 SKIN GRAFTS KEY FIGURES: Skin anatomy with graft thickness Humby knife Using the dermatome Using the Humby knife Mesher Skin graft Tying the dressing in place Defatting the FTSG A skin graft
Chapter 12 SKIN GRAFTS KEY FIGURES: Skin anatomy with graft thickness Humby knife Using the dermatome Using the Humby knife Mesher Skin graft Tying the dressing in place Defatting the FTSG A skin graft
Notes on Hair Analysis
 Notes on Hair Analysis I have found local veterinarians very uncooperative when trying to get samples of dog and cat fur. I have found neighbors, friends and relatives a much better source of fur. There
Notes on Hair Analysis I have found local veterinarians very uncooperative when trying to get samples of dog and cat fur. I have found neighbors, friends and relatives a much better source of fur. There
Not Your Father s Hair Restoration: The Latest Clinical Advancements from Lasers to Robots in Treating in Men and Women
 Not Your Father s Hair Restoration: The Latest Clinical Advancements from Lasers to Robots in Treating in Men and Women Robert T. Leonard, Jr., DO, FAACS, FISHRS Founder and Chief Surgeon Leonard Hair
Not Your Father s Hair Restoration: The Latest Clinical Advancements from Lasers to Robots in Treating in Men and Women Robert T. Leonard, Jr., DO, FAACS, FISHRS Founder and Chief Surgeon Leonard Hair
Blepharoplasty & Cosmetic eyelid surgery
 Our cosmetic surgery team at The USF Eye Institute offers a wide variety of cosmetic procedures of the eyelids and face with the goal of obtaining a natural and rejuvenated appearance. Dr.Leyngold has
Our cosmetic surgery team at The USF Eye Institute offers a wide variety of cosmetic procedures of the eyelids and face with the goal of obtaining a natural and rejuvenated appearance. Dr.Leyngold has
Chapter 11. Everting skin edges
 Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Preparing to Suture. 6 th Annual Pediatric Advanced Practice Conference Tuesday, February 9, 2016 1:30 pm. Workshop B: Suturing for Beginners
 Preparing to Suture Kristen Devick, MPAS, PA-C University of Colorado Department of Emergency Medicine NONE! Skin Anatomy Trott, 2012, p.11 Preparing to suture Initial evaluation Hemostasis Anesthesia
Preparing to Suture Kristen Devick, MPAS, PA-C University of Colorado Department of Emergency Medicine NONE! Skin Anatomy Trott, 2012, p.11 Preparing to suture Initial evaluation Hemostasis Anesthesia
PHaSES: Practical Hands-on Surgical Education System
 U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
U.S. Toll Free 866-GOLIMBS PHaSES Range PHaSES: Practical Hands-on Surgical Education System Limbs & Things is pleased to introduce the PHaSES Range. The range is based upon our well known basic & general
 no!no! Thermicon: A Novel, Home-based Hair Removal Device Dr. Mira Barki Yavne, Israel Introduction Lasers and intense pulsed light sources have become a popular method for long-term removal of unwanted
no!no! Thermicon: A Novel, Home-based Hair Removal Device Dr. Mira Barki Yavne, Israel Introduction Lasers and intense pulsed light sources have become a popular method for long-term removal of unwanted
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Breast Augmentation Amsterdam Plastic Surgery Breast Augmentation Overview
 Breast Augmentation Amsterdam Plastic Surgery Breast Augmentation Overview The long-lasting results of breast augmentation are not limited to just physical changes as data documents that many patients
Breast Augmentation Amsterdam Plastic Surgery Breast Augmentation Overview The long-lasting results of breast augmentation are not limited to just physical changes as data documents that many patients
www.healthoracle.org 1
 How does hair grow and should it recycle? A single hair follicle grows its hair strand over a period of four to six years (the anagen phase). It then rests for two to four months (the telogen phase), after
How does hair grow and should it recycle? A single hair follicle grows its hair strand over a period of four to six years (the anagen phase). It then rests for two to four months (the telogen phase), after
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
Before you know about your future see your past before improving your future hair see what has been and is the state of your hair now Ravi Bhanot
 Chapter 1 All you need to know about hair almost Before you know about your future see your past before improving your future hair see what has been and is the state of your hair now Ravi Bhanot Typically
Chapter 1 All you need to know about hair almost Before you know about your future see your past before improving your future hair see what has been and is the state of your hair now Ravi Bhanot Typically
Chapter 3 The Study of Hair By the end of the chapter you will be able to:
 Chapter 3 The Study of Hair By the end of the chapter you will be able to: identify the various parts of a hair describe variations in the structure of the medulla, cortex, and cuticle distinguish between
Chapter 3 The Study of Hair By the end of the chapter you will be able to: identify the various parts of a hair describe variations in the structure of the medulla, cortex, and cuticle distinguish between
Fat Injection to Correct Contour Deformities in the Reconstructed Breast
 Fat Injection to Correct Contour Deformities in the Reconstructed Breast Scott L. Spear, M.D., Henry B. Wilson, M.D., and Michelle D. Lockwood, M.D. Washington, D.C. Background: A ten-year, single-surgeon
Fat Injection to Correct Contour Deformities in the Reconstructed Breast Scott L. Spear, M.D., Henry B. Wilson, M.D., and Michelle D. Lockwood, M.D. Washington, D.C. Background: A ten-year, single-surgeon
Give us a table of facelift complications. How would you treat each? Answers from Cummings:
 Give us a table of facelift complications. How would you treat each? Answers from Cummings: Hematoma The most common perioperative complication of rhytidectomy is hematoma, which occurs in 1% to 10% of
Give us a table of facelift complications. How would you treat each? Answers from Cummings: Hematoma The most common perioperative complication of rhytidectomy is hematoma, which occurs in 1% to 10% of
Fundamental to breast reconstruction after mastectomy
 CASE REPORT Correction of Chest Wall Deformity After Implant- Based Breast Reconstruction Using poly-l-lactic Acid (Sculptra) Matthew R. Schulman, MD, Justin Lipper, BA, and Richard A. Skolnik, MD Division
CASE REPORT Correction of Chest Wall Deformity After Implant- Based Breast Reconstruction Using poly-l-lactic Acid (Sculptra) Matthew R. Schulman, MD, Justin Lipper, BA, and Richard A. Skolnik, MD Division
How To Improve Your Looks with Plastic Surgery
 How To Improve Your Looks with Plastic Surgery By Daniel Becker Plastic surgery is a special type of surgery that involves both a person's appearance and his or her ability to function. Plastic surgeons
How To Improve Your Looks with Plastic Surgery By Daniel Becker Plastic surgery is a special type of surgery that involves both a person's appearance and his or her ability to function. Plastic surgeons
MEDICAL MANAGEMENT POLICY
 TITLE: Scar Revision/Keloid PAGE: 1of 9 This Medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
TITLE: Scar Revision/Keloid PAGE: 1of 9 This Medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
TREATMENT 1. Control bleeding by applying pressure over wound with Gauze Pads (Surgical Supply-4). 2. Contact Surgeon for laceration repair options.
 Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
ABDOMINOPLASTY - FREQUENTLY ASKED QUESTIONS (FAQs)
 Executive Level E1, Excen Centre, 119 Willoughby Road, Crows Nest 2065 Tel: 02 9817 7585 www.mycosmeticclinic.net AFFORDABILITY WITH EXCELLENCE Liposuction Breast Augmentation Abdominoplasty Eyelids Surgery
Executive Level E1, Excen Centre, 119 Willoughby Road, Crows Nest 2065 Tel: 02 9817 7585 www.mycosmeticclinic.net AFFORDABILITY WITH EXCELLENCE Liposuction Breast Augmentation Abdominoplasty Eyelids Surgery
Open and Endoscopic Forehead Lift. Plastic Surgery. For All Brow and Forehead Lift Procedures. Revolutionizing. Soft-Tissue Fixation
 Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
Thomas T. Jeneby, M.D. 7272 Wurzbach Suite 801 San Antonio, TX. 78240 210-782-8269/210 270 8595
 Laser hair removal is one of the most popular cosmetic procedures performed. Unwanted hair grows on various regions of the body. Often, individuals find the presence of hair in certain regions of the body
Laser hair removal is one of the most popular cosmetic procedures performed. Unwanted hair grows on various regions of the body. Often, individuals find the presence of hair in certain regions of the body
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
F ORUM. Special Topic. Facial Reshaping Using Minimally Invasive Methods
 Special Topic Facial Reshaping Using Minimally Invasive Methods Q1 Richard Ellenbogen, MD; Gary Motykie, MD; nthony Youn, MD; Steven Svehlak, MD; and Dan Yamini, MD Dr. Ellenbogen, Dr. Motykie, Dr. Yamini,
Special Topic Facial Reshaping Using Minimally Invasive Methods Q1 Richard Ellenbogen, MD; Gary Motykie, MD; nthony Youn, MD; Steven Svehlak, MD; and Dan Yamini, MD Dr. Ellenbogen, Dr. Motykie, Dr. Yamini,
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
DESPITE THE FACT that cubital tunnel syndrome is
 SURGICAL TECHNIQUE Endoscopic Cubital Tunnel Release Tyson K. Cobb, MD A minimally invasive endoscopic approach has been successfully applied to surgical treatment of cubital tunnel syndrome. This procedure
SURGICAL TECHNIQUE Endoscopic Cubital Tunnel Release Tyson K. Cobb, MD A minimally invasive endoscopic approach has been successfully applied to surgical treatment of cubital tunnel syndrome. This procedure
Wound Management and Basic Suturing Techniques. Disclosures
 Wound Management and Basic Suturing Techniques 10 July 2016 Douglas Winstanley, DO FAAD FACMS West Michigan Dermatology Grand Rapids MI Hugh Greenway s 33 nd Annual Cutaneous Anatomy and Surgery Course
Wound Management and Basic Suturing Techniques 10 July 2016 Douglas Winstanley, DO FAAD FACMS West Michigan Dermatology Grand Rapids MI Hugh Greenway s 33 nd Annual Cutaneous Anatomy and Surgery Course
What is androgenetic alopecia?
 What is androgenetic alopecia? Androgenetic alopecia is also called male pattern alopecia. It refers to a symptom that develops after puberty, influenced by the androgen, where thinning and/or loss of
What is androgenetic alopecia? Androgenetic alopecia is also called male pattern alopecia. It refers to a symptom that develops after puberty, influenced by the androgen, where thinning and/or loss of
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
PROPERTIES OF THE HAIR AND SCALP
 PROPERTIES OF THE HAIR AND SCALP 1. The scientific study of hair, its diseases and care is called: a. dermatology c. biology b. trichology d. cosmetology 2. The two parts of a mature hair strand are the
PROPERTIES OF THE HAIR AND SCALP 1. The scientific study of hair, its diseases and care is called: a. dermatology c. biology b. trichology d. cosmetology 2. The two parts of a mature hair strand are the
Preputial Skin Grafts
 11 Preputial Skin Grafts Ahmet Bulent Dogrul 1 and Kaya Yorganci 2 1 Mus State Hospital, Clinic of General Surgery, MUS 2 Hacettepe University Medical School, Department of General Surgery, Ankara Turkey
11 Preputial Skin Grafts Ahmet Bulent Dogrul 1 and Kaya Yorganci 2 1 Mus State Hospital, Clinic of General Surgery, MUS 2 Hacettepe University Medical School, Department of General Surgery, Ankara Turkey
Oklahoma Facts CPT. Definitions. Mohs Micrographic Surgery. What Does That Mean? Billing and Coding for Mohs Surgery
 Billing and Coding for Mohs Surgery Cindy L. Wilson Dermatology Associates of Tulsa Oklahoma Facts Per square mile, Oklahoma has more tornadoes than any other place in the world. The highest wind speed
Billing and Coding for Mohs Surgery Cindy L. Wilson Dermatology Associates of Tulsa Oklahoma Facts Per square mile, Oklahoma has more tornadoes than any other place in the world. The highest wind speed
Around 30 participants joined the 4th FUE EUROPE meeting in Prague for a fruitful and interesting workshop.
 Special thanks have to be issued to Dr. Peter Hajduk, Monika Dočkalová and the team of in Prague for the excellent organisation of this event in the astounding historical city of Prague. Around 30 participants
Special thanks have to be issued to Dr. Peter Hajduk, Monika Dočkalová and the team of in Prague for the excellent organisation of this event in the astounding historical city of Prague. Around 30 participants
ELECTROLYSIS- INFORMATION AND FAQ s
 ELECTROLYSIS- INFORMATION AND FAQ s 1. How does Electrolysis work? A very fine sterilized filament is inserted into the hair follicle, which is a natural opening in the skin. The skin is not pierced or
ELECTROLYSIS- INFORMATION AND FAQ s 1. How does Electrolysis work? A very fine sterilized filament is inserted into the hair follicle, which is a natural opening in the skin. The skin is not pierced or
Influence of the skin mechanical and microbial properties on hair growth
 Call for Interdisciplinary Projects Sevres 2014 A General Information Project title Influence of the skin mechanical and microbial properties on hair growth Acronym TADDEI: The Ambiguous Dupond and Dupont
Call for Interdisciplinary Projects Sevres 2014 A General Information Project title Influence of the skin mechanical and microbial properties on hair growth Acronym TADDEI: The Ambiguous Dupond and Dupont
Breast Augmentation. If you are dissatisfied with your breast size, augmentation surgery is a choice to consider. Breast augmentation can:
 Breast Augmentation What is Breast Augmentation? Also known as augmentation mammaplasty, breast augmentation involves using implants to fulfill your desire for fuller breasts or to restore breast volume
Breast Augmentation What is Breast Augmentation? Also known as augmentation mammaplasty, breast augmentation involves using implants to fulfill your desire for fuller breasts or to restore breast volume
Plastic and Reconstructive Surgery
 Plastic and Reconstructive Surgery General Description Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 Elective Rotation This elective rotation in Plastic and Reconstructive Surgery (PRS)
Plastic and Reconstructive Surgery General Description Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 Elective Rotation This elective rotation in Plastic and Reconstructive Surgery (PRS)
Hair & Fiber. (Unit 5)
 37 Hair & Fiber (Unit 5) Morphology of Hair Hair is encountered as physical evidence in a wide variety of crimes. A review of the forensic aspects of hair examination must start with the observation that
37 Hair & Fiber (Unit 5) Morphology of Hair Hair is encountered as physical evidence in a wide variety of crimes. A review of the forensic aspects of hair examination must start with the observation that
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Facial Multilayered Micro Lipo-Augmentation KIRK BRANDOW, MD, AND JULIUS NEWMAN, MD
 International Journal of Aesthetic and Restorative Volume 4, Number 2, 1996, Pages 95-110 Surgery Facial Multilayered Micro Lipo-Augmentation KIRK BRANDOW, MD, AND JULIUS NEWMAN, MD ABSTRACT: Lipo-transfer
International Journal of Aesthetic and Restorative Volume 4, Number 2, 1996, Pages 95-110 Surgery Facial Multilayered Micro Lipo-Augmentation KIRK BRANDOW, MD, AND JULIUS NEWMAN, MD ABSTRACT: Lipo-transfer
Do I Need to Have Surgery for Urinary Incontinence? What Kinds of Surgery Can Treat Stress Incontinence?
 Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery
 Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Hair Loss: An Insider Guide to Hair Restoration and Replacement
 Hair Loss: An Insider Guide to Hair Restoration and Replacement November 2013 Why you may want more hair. Typically, people don t realize their hair is thinning until they ve lost 50% of it. By age 35,
Hair Loss: An Insider Guide to Hair Restoration and Replacement November 2013 Why you may want more hair. Typically, people don t realize their hair is thinning until they ve lost 50% of it. By age 35,
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
COPYRIGHT ASPS. Breast Augmentation. The Symbol of Excellence in Plastic Surgery
 Breast Augmentation The Symbol of Excellence in Plastic Surgery A public education service of the American Society of Plastic Surgeons and the American Society for Aesthetic Plastic Surgery. This brochure
Breast Augmentation The Symbol of Excellence in Plastic Surgery A public education service of the American Society of Plastic Surgeons and the American Society for Aesthetic Plastic Surgery. This brochure
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY
 STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
Understanding Hair Loss and the ARTAS Robotic Hair Transplant
 Understanding Hair Loss and the ARTAS Robotic Hair Transplant The ARTAS Robotic System Table of Contents PART 1: Understanding Hair Loss 5 6 7 Why am I losing my hair? Why is my hair thinning? How far
Understanding Hair Loss and the ARTAS Robotic Hair Transplant The ARTAS Robotic System Table of Contents PART 1: Understanding Hair Loss 5 6 7 Why am I losing my hair? Why is my hair thinning? How far
Descemet s Stripping Endothelial Keratoplasty (DSEK)
 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
SKIN REJUVENATION WITH FRAXEL LASER. Akhil Wadhera, M.D. Dermatology
 SKIN REJUVENATION WITH FRAXEL LASER By Akhil Wadhera, M.D. Dermatology Dr. Hendler: Hello and welcome to KP Healthcast. I m your host, Dr. Peter Hendler. Today our guest is Dr. Akhil Wadhera who s been
SKIN REJUVENATION WITH FRAXEL LASER By Akhil Wadhera, M.D. Dermatology Dr. Hendler: Hello and welcome to KP Healthcast. I m your host, Dr. Peter Hendler. Today our guest is Dr. Akhil Wadhera who s been
Hair. *credit to Anthony and Patti Bertino for image. Dec 2 8:10 PM
 Hair *credit to Anthony and Patti Bertino for image Dec 2 8:10 PM 1 Essential Question: How can hair be used to solve a crime? Dec 2 8:12 PM 2 History of hair evidence criminal evidence in 1800's 1883
Hair *credit to Anthony and Patti Bertino for image Dec 2 8:10 PM 1 Essential Question: How can hair be used to solve a crime? Dec 2 8:12 PM 2 History of hair evidence criminal evidence in 1800's 1883
ADVANCED SUTURING WORKSHOP ANN BECKER, APRN-CNP; TONI PRATT-REID, APRN-CNP
 ADVANCED SUTURING WORKSHOP ANN BECKER, APRN-CNP; TONI PRATT-REID, APRN-CNP SUTURING WORKSHOP! The technique of suturing, as a method for closing cutaneous wounds has been a part of medicine for hundreds
ADVANCED SUTURING WORKSHOP ANN BECKER, APRN-CNP; TONI PRATT-REID, APRN-CNP SUTURING WORKSHOP! The technique of suturing, as a method for closing cutaneous wounds has been a part of medicine for hundreds
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
Hair Chemistry. Chapter 1. Hair Relaxers Science, Design, and Application www.alluredbooks.com
 Hair Relaxers Science, Design, and Application www.alluredbooks.com Chapter 1 Hair Chemistry We all know that the hair on our head is dead, but underneath the scalp, within the hair follicle, is a surprisingly
Hair Relaxers Science, Design, and Application www.alluredbooks.com Chapter 1 Hair Chemistry We all know that the hair on our head is dead, but underneath the scalp, within the hair follicle, is a surprisingly
MOHS MICROGRAPHIC SURGERY
 MOHS MICROGRAPHIC SURGERY UMass Memorial Medical Center 55 Lake Avenue North Worcester, MA 01655 (508) 856-1666 Dr. Mary Maloney This booklet is intended to explain Mohs surgery to you. It is not, however,
MOHS MICROGRAPHIC SURGERY UMass Memorial Medical Center 55 Lake Avenue North Worcester, MA 01655 (508) 856-1666 Dr. Mary Maloney This booklet is intended to explain Mohs surgery to you. It is not, however,
Hair Restoration Update
 ١ Hair Restoration Update By Dr.Tarek Ahmed Said Lecturer of Plastic Surgery, Cairo University Hair on a man's head is an important emblem of health, youth and vitality (Vogel, 2000). For a long time physicians
١ Hair Restoration Update By Dr.Tarek Ahmed Said Lecturer of Plastic Surgery, Cairo University Hair on a man's head is an important emblem of health, youth and vitality (Vogel, 2000). For a long time physicians
To our knowledge, a long-term follow-up study COSMETIC
 COSMETIC Outcomes Article The Measure of Face-Lift Patient Satisfaction: The Owsley Facelift Satisfaction Survey with a Long-Term Follow-Up Study Michael T. Friel, M.D. Richard E. Shaw, Ph.D. Matthew J.
COSMETIC Outcomes Article The Measure of Face-Lift Patient Satisfaction: The Owsley Facelift Satisfaction Survey with a Long-Term Follow-Up Study Michael T. Friel, M.D. Richard E. Shaw, Ph.D. Matthew J.
Informed Consent For Laser Hair Removal
 Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity
 Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity Robert Cohen, MD, FACS* Paradise Valley, AZ Case summary A 41-year old woman with a history
Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity Robert Cohen, MD, FACS* Paradise Valley, AZ Case summary A 41-year old woman with a history
MOHS MICROGRAPHIC SURGERY
 Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
Auditory System. Chaos Healthcare
 Medical Coding Auditory System Chaos Healthcare AUDITORY SYSTEM: Anatomy AUDITORY SYSTEM: Physiology AUDITORY SYSTEM MYRINGOPLASTY: Myringoplasty is an operative procedure used in the reconstruction of
Medical Coding Auditory System Chaos Healthcare AUDITORY SYSTEM: Anatomy AUDITORY SYSTEM: Physiology AUDITORY SYSTEM MYRINGOPLASTY: Myringoplasty is an operative procedure used in the reconstruction of
Fat Grafting intrauma and Reconstructive Surgery
 Fat Grafting intrauma and Reconstructive Surgery Yadranko Ducic, MD,FRCS(C),FACS a,b,c,d KEYWORDS Fat grafting Lipotransfer Reconstructive surgery The Greeks long ago recognized the ideals of proportion
Fat Grafting intrauma and Reconstructive Surgery Yadranko Ducic, MD,FRCS(C),FACS a,b,c,d KEYWORDS Fat grafting Lipotransfer Reconstructive surgery The Greeks long ago recognized the ideals of proportion
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
1 of 6 2/10/12 10:15 AM
 Home Dr. Bitar About Us Events Media Specialties Non Surgical Gallery Fees Contact Us Plastic Surgery Products Magazine, October 2007 Issue Breast Augmentation: The Axillary Approach by George John Bitar,
Home Dr. Bitar About Us Events Media Specialties Non Surgical Gallery Fees Contact Us Plastic Surgery Products Magazine, October 2007 Issue Breast Augmentation: The Axillary Approach by George John Bitar,
Evaluation of the Cosmetic Patient
 APC Ophthalmology Conference Evaluation of the Cosmetic Patient David K. Isaacs, M.D. Clinical instructor Loma Linda University Clinial Staff Attending UCLA/Jules Stein Eye Institute Lecture Agenda Review
APC Ophthalmology Conference Evaluation of the Cosmetic Patient David K. Isaacs, M.D. Clinical instructor Loma Linda University Clinial Staff Attending UCLA/Jules Stein Eye Institute Lecture Agenda Review
The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches
 Cosmetic The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches Scott W. Mosser, M.D., Bahman Guyuron, M.D., Jeffrey E. Janis, M.D., and Rod J. Rohrich, M.D. Cleveland,
Cosmetic The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches Scott W. Mosser, M.D., Bahman Guyuron, M.D., Jeffrey E. Janis, M.D., and Rod J. Rohrich, M.D. Cleveland,
UROLOGY GROUP of PRINCETON
 UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
APPLICATION OF DRY DRESSING
 G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
Innovative Low Fluence-High Repetition Rate Technology for Hair Removal
 Innovative Low Fluence-High Repetition Rate Technology for Hair Removal Dr. Joseph Lepselter Alma Lasers Ltd. Caesarea, Israel Houten, Holland April 14, 2012 Terms LHR = laser hair removal SHR = super
Innovative Low Fluence-High Repetition Rate Technology for Hair Removal Dr. Joseph Lepselter Alma Lasers Ltd. Caesarea, Israel Houten, Holland April 14, 2012 Terms LHR = laser hair removal SHR = super
X-Plain Alopecia Reference Summary
 X-Plain Alopecia Reference Summary Introduction Hair loss is very common in both men and women. You or someone you love may be experiencing hair loss. Hair follicle Learning about normal hair growth is
X-Plain Alopecia Reference Summary Introduction Hair loss is very common in both men and women. You or someone you love may be experiencing hair loss. Hair follicle Learning about normal hair growth is
INFORMATION SHEET FAT TRANSFER
 INFORMATION SHEET FAT TRANSFER INTRODUCTION In the past surgeons have tried to enlarge women s breasts and to fill out contour hollows by cutting out a lump of fat from the abdomen or buttocks and embedding
INFORMATION SHEET FAT TRANSFER INTRODUCTION In the past surgeons have tried to enlarge women s breasts and to fill out contour hollows by cutting out a lump of fat from the abdomen or buttocks and embedding
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
Two main classes: Epithelial Connective (synovial) Epithelial. Cutaneous Mucous Serous
 Two main classes: Epithelial Connective (synovial) Epithelial Cutaneous Mucous Serous Epithelial Membranes = sheet of epithelia + connective tissue base 1. Cutaneous membrane: outer skin layer (stratified
Two main classes: Epithelial Connective (synovial) Epithelial Cutaneous Mucous Serous Epithelial Membranes = sheet of epithelia + connective tissue base 1. Cutaneous membrane: outer skin layer (stratified
Placement of an indwelling urinary catheter in female dogs
 Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
SILS. Port Insertion By Homero Rivas, MD, MBA, FACS. Single incision. Single port. Simple choice.
 SILS Port Insertion By Homero Rivas, MD, MBA, FACS Single incision. Single port. Simple choice. SILS Port Insertion By Homero Rivas, MD, MBA, FACS For the last 20 years, there has given surgical procedure.
SILS Port Insertion By Homero Rivas, MD, MBA, FACS Single incision. Single port. Simple choice. SILS Port Insertion By Homero Rivas, MD, MBA, FACS For the last 20 years, there has given surgical procedure.
Prepared By: The Professional Staff of the Appropriations Subcommittee on Health and Human Services REVISED:
 The Florida Senate BILL ANALYSIS AND FISCAL IMPACT STATEMENT (This document is based on the provisions contained in the legislation as of the latest date listed below.) Prepared By: The Professional Staff
The Florida Senate BILL ANALYSIS AND FISCAL IMPACT STATEMENT (This document is based on the provisions contained in the legislation as of the latest date listed below.) Prepared By: The Professional Staff
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Intracapsular Allogenic Dermal Grafts for Breast Implant Related Problems
 Cosmetic Intracapsular Allogenic Dermal Grafts for Breast Implant Related Problems Richard A. Baxter, M.D. Mountlake Terrace, Wash. Despite advances in surgical techniques and breast implant design, certain
Cosmetic Intracapsular Allogenic Dermal Grafts for Breast Implant Related Problems Richard A. Baxter, M.D. Mountlake Terrace, Wash. Despite advances in surgical techniques and breast implant design, certain
Please visit your examination provider s website for the most current bulletin prior to testing. IMPORTANT INSTRUCTIONS
 NATIONAL BARBER THEORY EXAMINATION CANDIDATE INFORMATION BULLETIN Please visit your examination provider s website for the most current bulletin prior to testing. The National Barber Theory Examination
NATIONAL BARBER THEORY EXAMINATION CANDIDATE INFORMATION BULLETIN Please visit your examination provider s website for the most current bulletin prior to testing. The National Barber Theory Examination
Facial Nerve Paralysis: Management of the Eye
 Facial Nerve Paralysis: Management of the Eye Facial Nerve Paralysis: Management of the Eye Introduction Anatomy Options Discussion of Literature Introduction-Facial Nerve Paralysis Functional and cosmetic
Facial Nerve Paralysis: Management of the Eye Facial Nerve Paralysis: Management of the Eye Introduction Anatomy Options Discussion of Literature Introduction-Facial Nerve Paralysis Functional and cosmetic
Bone Anchored Hearing Aids B.A.H.A
 Bone Anchored Hearing Aids B.A.H.A Dr. Abdulrahman Hagr MBBS FRCS(c) Assistant Professor King Saud University Otolaryngology Consultant Otologist, Neurotologist & Skull Base Surgeon King Abdulaziz Hospital
Bone Anchored Hearing Aids B.A.H.A Dr. Abdulrahman Hagr MBBS FRCS(c) Assistant Professor King Saud University Otolaryngology Consultant Otologist, Neurotologist & Skull Base Surgeon King Abdulaziz Hospital
Blepharoplasty - Eyelid Surgery
 Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Clinical Privileges Profile Plastic Surgery. Indu & Raj Soin Medical Center
 Printed Name Clinical Privileges Profile Plastic Surgery Indu & Raj Soin Medical Center Applicant: Check off the Requested box for each privilege requested. Applicants have the burden of producing information
Printed Name Clinical Privileges Profile Plastic Surgery Indu & Raj Soin Medical Center Applicant: Check off the Requested box for each privilege requested. Applicants have the burden of producing information
Corneal Collagen Cross-Linking (CXL) With Riboflavin
 Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
There are a wide range of factors that can impact on the health of the hair and hair growth.
 Welcome to Viviscal Viviscal, one of the best selling hair growth supplement in the US, is now available with TVSN. The Viviscal brand of hair care products is enjoying rapid and substantial growth in
Welcome to Viviscal Viviscal, one of the best selling hair growth supplement in the US, is now available with TVSN. The Viviscal brand of hair care products is enjoying rapid and substantial growth in
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
PRESS RELEASE from HAIR SCIENCE INSTITUTE
 PRESS RELEASE from HAIR SCIENCE INSTITUTE Amsterdam/Maastricht, 28 January 2010 Last Friday, 22 January 2010, a news item was posted on the internet (www.nieuwsbank.nl) with the headline "Doctors warn
PRESS RELEASE from HAIR SCIENCE INSTITUTE Amsterdam/Maastricht, 28 January 2010 Last Friday, 22 January 2010, a news item was posted on the internet (www.nieuwsbank.nl) with the headline "Doctors warn
STOP HAIR LOSS DR JOYCE LIM DERMATOLOGIST PARAGON MEDICAL CENTRE #11-16/20
 STOP HAIR LOSS DR JOYCE LIM DERMATOLOGIST PARAGON MEDICAL CENTRE #11-16/20 HAIR LOSS Types of Hair loss What causes them What are the solutions HAIR LOSS PATCHY HAIR LOSS PATCHY HAIR LOSS Single/ Multiple
STOP HAIR LOSS DR JOYCE LIM DERMATOLOGIST PARAGON MEDICAL CENTRE #11-16/20 HAIR LOSS Types of Hair loss What causes them What are the solutions HAIR LOSS PATCHY HAIR LOSS PATCHY HAIR LOSS Single/ Multiple
There has been a renewed interest in upper
 SPECIAL TOPIC An Algorithmic Approach to Upper Arm Contouring Eric A. Appelt, M.D. Jeffrey E. Janis, M.D. Rod. J. Rohrich, M.D. Dallas, Texas Summary: There has been a renewed interest in upper arm contouring
SPECIAL TOPIC An Algorithmic Approach to Upper Arm Contouring Eric A. Appelt, M.D. Jeffrey E. Janis, M.D. Rod. J. Rohrich, M.D. Dallas, Texas Summary: There has been a renewed interest in upper arm contouring
Hard work. PAL will take you. can get you 90% of the way there. over the finish line. Results instead of hype.
 Hard work can get you 90% of the way there. PAL will take you over the finish line. Results instead of hype. Power-Assisted Liposuction (PAL) offers meaningful patient benefits. Less bruising, swelling
Hard work can get you 90% of the way there. PAL will take you over the finish line. Results instead of hype. Power-Assisted Liposuction (PAL) offers meaningful patient benefits. Less bruising, swelling
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
