Dizziness: A Diagnostic Approach
|
|
|
- Annabel Parks
- 8 years ago
- Views:
Transcription
1 Dizziness: A Diagnostic Approach ROBERT E. POST, MD, Virtua Family Medicine Residency, Voorhees, New Jersey LORI M. DICKERSON, PharmD, Medical University of South Carolina, Charleston, South Carolina Dizziness accounts for an estimated 5 percent of primary care clinic visits. The patient history can generally classify dizziness into one of four categories: vertigo, disequilibrium, presyncope, or lightheadedness. The main causes of vertigo are benign paroxysmal positional vertigo, Meniere disease, vestibular neuritis, and labyrinthitis. Many medications can cause presyncope, and regimens should be assessed in patients with this type of dizziness. Parkinson disease and diabetic neuropathy should be considered with the diagnosis of disequilibrium. Psychiatric disorders, such as depression, anxiety, and hyperventilation syndrome, can cause vague lightheadedness. The differential diagnosis of dizziness can be narrowed with easy-to-perform physical examination tests, including evaluation for nystagmus, the Dix-Hallpike maneuver, and orthostatic blood pressure testing. Laboratory testing and radiography play little role in diagnosis. A final diagnosis is not obtained in about 20 percent of cases. Treatment of vertigo includes the Epley maneuver (canalith repositioning) and vestibular rehabilitation for benign paroxysmal positional vertigo, intratympanic dexamethasone or gentamicin for Meniere disease, and steroids for vestibular neuritis. Orthostatic hypotension that causes presyncope can be treated with alpha agonists, mineralocorticoids, or lifestyle changes. Disequilibrium and lightheadedness can be alleviated by treating the underlying cause. (Am Fam Physician. 2010;82(4): Copyright 2010 American Academy of Family Physicians.) ILLUSTRATION BY TODD BUCK Patient information: A handout on dizziness, written by the authors of this article, is provided on page 369. Diagnosing the cause of dizziness can be difficult because symptoms are often nonspecific and the differential diagnosis is broad. However, a few simple questions and physical examination tests can help narrow the possible diagnoses. It is estimated that primary care physicians care for more than one half of all patients who present with dizziness. 1 Dizziness is the chief presenting symptom in about 3 percent of primary care visits for patients 25 years and older, and in nearly 3 percent of all emergency department visits. 2,3 Dizziness can be classified into four main types: vertigo, disequilibrium, presyncope, or lightheadedness. Although appropriate history and physical examination usually leads to a diagnosis, the final cause of dizziness is not identified in up to one in five patients. 4,5 Patient History The initial description of dizziness can be difficult to obtain because patient responses are not always consistent. 6 Therefore, the history should first focus on what type of sensation the patient is feeling. Table 1 includes descriptors for the main categories of dizziness. 4,5,7,8 It is important to note that some causes of dizziness can be associated with more than one set of descriptors. A medication history should be obtained because dizziness (especially from orthostatic hypotension) is a well-known adverse effect of many drugs 9 (Table 2 10,11 ). Patients should also be asked about caffeine, nicotine, and alcohol intake. 9 Head trauma and whiplash injuries can cause a variety of dizziness symptoms, from vertigo to lightheadedness. The incidence of dizziness with a head injury or vertigo initially after whiplash have been reported as high as 78 to 80 percent. 12 Selected causes of dizziness are summarized in Table 3. 4,7,8,13-20 VERTIGO Otologic or vestibular causes of vertigo are the most common causes of dizziness, 21,22 Downloaded from the American Family Physician Web site at Copyright 2010 American Academy of Family Physicians. For the private, noncommercial August 15, use 2010 of one Volume individual 82, user Number of the Web 4 site. All other rights reserved. Contact copyrights@aafp.org for copyright questions American and/or permission Family requests. Physician 361
2 Dizziness SORT: KEY RECCOMENDATIONS FOR PRACTICE Clinical recommendation The Dix-Hallpike maneuver should be performed to diagnose BPPV. Because they generally are not helpful diagnostically, laboratory testing and radiography are not routinely indicated in the workup of patients with dizziness when no other neurologic abnormalities are present. The Epley maneuver and vestibular rehabilitation are effective treatments for BPPV. BPPV = benign paroxysmal positional vertigo. and include benign paroxysmal positional vertigo (BPPV), vestibular neuritis (viral infection of the vestibular nerve), labyrinthitis (infection of the labyrinthine organs), and Meniere disease (increased endolymphatic fluid in the inner ear). 7,13 An estimated 35 percent of adults 40 years and older have vestibular dysfunction. 14 Hearing loss and duration of symptoms help narrow the differential diagnosis further in patients with vertigo. with hearing loss is usually caused by Meniere disease or labyrinthitis, whereas vertigo without hearing loss is more likely caused by BPPV or vestibular neuritis. 8 Unilateral auditory symptoms help localize the cause to an anatomic abnormality, particularly in patients with peripheral disease. 9 Episodic vertigo tends to be caused by BPPV or Meniere disease, whereas persistent vertigo can be caused by vestibular neuritis or labyrinthitis. 8 Migrainous vertigo, or vestibular migraine, is another underlying cause of vertigo that affects about 3 percent of the general population and about 10 percent of persons with migraine. 15 This diagnosis should be considered after other causes of vertigo have been ruled out. Diagnosis of migrainous vertigo is established in patients with a history of episodic vertigo with a current migraine or history of migraine and one of the following symptoms during at least two episodes of vertigo: migraine headache, photophobia, phonophobia, or aura. 15 PRESYNCOPE Evidence rating References C 7, 9, 16 C 7, 31, 32 B 40, 41, 42 A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to Cardiovascular causes of dizziness include arrhythmias, myocardial infarction, carotid artery stenosis, and orthostatic hypotension. 21 Of patients with supraventricular tachycardia, 75 percent experience dizziness and about 30 percent experience syncope. 23 Symptoms brought on Table 1. Main Categories of Dizziness Category Description False sense of motion, possibly spinning sensation Percentage of patients with dizziness 45 to 54 Disequilibrium Off-balance or wobbly Up to 16 Presyncope Lightheadedness Feeling of losing consciousness or blacking out Vague symptoms, possibly feeling disconnected with the environment Information from references 4, 5, 7, and 8. Up to 14 Approximately 10 Table 2. Medications Commonly Associated with Dizziness from Orthostatic Hypotension Cardiac medications Alpha blockers (e.g., doxazosin [Cardura], terazosin) Alpha/beta blockers (e.g., carvedilol [Coreg], labetalol) Angiotensin-converting enzyme inhibitors Beta blockers Clonidine (Catapres) Dipyridamole (Persantine) Diuretics (e.g., furosemide [Lasix]) Hydralazine Methyldopa Nitrates (e.g., nitroglycerin paste, sublingual nitroglycerin) Reserpine Central nervous system medications Antipsychotics (e.g., chlorpromazine, clozapine [Clozaril], thioridazine) Opioids Parkinsonian drugs (e.g., bromocriptine [Parlodel], levodopa/ carbidopa [Sinemet]) Skeletal muscle relaxants (e.g., baclofen [Lioresal], cyclobenzaprine [Flexeril], methocarbamol [Robaxin], tizanidine [Zanaflex]) Tricyclic antidepressants (e.g., amitriptyline, doxepin, trazodone) Urologic medications Phosphodiesterase type 5 inhibitors (e.g., sildenafil [Viagra]) Urinary anticholinergics (e.g., oxybutynin [Ditropan]) Information from references 10 and 11. by postural changes suggest a diagnosis of orthostatic hypotension. 9 A variety of cardiovascular medications increase the risk of orthostatic hypotension in older persons, including reserpine (at doses greater than 0.25 mg), doxazosin (Cardura), and clonidine (Catapres) American Family Physician Volume 82, Number 4 August 15, 2010
3 Table 3. Selected Causes of Dizziness Dizziness Cause Category of dizziness Pathophysiology Diagnostic criteria Benign paroxysmal positional vertigo Hyperventilation syndrome Lightheadedness Loose otolith in semicircular canals causing a false sense of motion Hyperventilation causing respiratory alkalosis; underlying anxiety may provoke the hyperventilation Positive findings with Dix-Hallpike maneuver; episodic vertigo without hearing loss Symptoms reproduced with voluntary hyperventilation Meniere disease Increased endolymphatic fluid in the inner ear Episodic vertigo with hearing loss Migrainous vertigo (vestibular migraine) Orthostatic hypotension Presyncope Uncertain; one hypothesis is that trigeminal nuclei stimulation causes nystagmus in persons with migraine Drop in blood pressure on position change causing decreased blood flow to the brain, adverse effect of multiple medications (see Table 2) Parkinson disease Disequilibrium Dysfunction in gait causing imbalance and falls Peripheral neuropathy Disequilibrium Decreased tactile response when walking causes patient to be unaware when feet touch the ground, leading to imbalance and falls Episodic vertigo with signs of migraine, plus photophobia, phonophobia, or aura during at least two episodes of vertigo Systolic blood pressure decrease of 20 mm Hg, diastolic blood pressure decrease of 10 mm Hg, or a pulse increase of 30 beats per minute Shuffling gait with reduced arm swing and possible hesitation Decreased sensation in lower extremities, particularly the feet Information from references 4, 7, 8, and 13 through 20. DISEQUILIBRIUM There are many underlying conditions that may cause a sense of imbalance. Stroke is an important and lifethreatening cause of dizziness that needs to be ruled out when the dizziness is associated with other symptoms of stroke. However, other neurologic findings are generally present. In a population-based study of more than 1,600 patients, 3.2 percent of those presenting to an emergency department with dizziness were diagnosed with a stroke or transient ischemic attack (TIA), but only 0.7 percent presenting with isolated dizziness were diagnosed with stroke or TIA. 25 Poor vision commonly accompanies a feeling of imbalance, 16 leading to falls. The physician should inquire about a history of other problems that may cause imbalance, such as Parkinson disease, peripheral neuropathy, and any musculoskeletal disorders that may affect gait. 17 Use of benzodiazepines and tricyclic antidepressants increase the risk of ataxia and falls in older persons. 24 LIGHTHEADEDNESS Psychiatric causes of lightheadedness are common, particularly anxiety; therefore, questions about anxiety and depression should be included in the patient history. In one study, about 28 percent of patients with dizziness reported symptoms of at least one anxiety disorder. 26 In another study, one in four patients with dizziness met criteria for panic disorder. 27 A study of patients with chronic dizziness showed that those with panic disorder were more likely to have neurotologic findings than those without panic disorder. 28 Up to 60 percent of patients with chronic subjective dizziness have been reported to have an anxiety disorder. 29 Depression and alcohol intoxication have also been found to overlap with dizziness. 21,30 Hyperventilation syndrome is an important cause of lightheadedness. Although the condition can be associated with anxiety disorders, many patients without anxiety experience hyperventilation. Hyperventilation is defined as breathing in excess of metabolic requirements, causing a respiratory alkalosis and lightheadedness. Patients may sigh repeatedly and may have associated symptoms, such as chest pain, paraesthesias, bloating, and epigastric pain. 18 Physical Examination The main goal of the physical examination is to reproduce the patient s dizziness in the office. There are a few simple physical examination tests that can be performed to aid in this goal. First, blood pressure should be measured while the patient is in a supine position and again at least one minute after the patient stands. A systolic blood pressure decrease of 20 mm Hg, diastolic blood pressure decrease of 10 mm Hg, or pulse increase of 30 beats per minute is indicative of orthostatic hypotension. 16,19 The Dix-Hallpike maneuver (Figure 1 9,16 ) is diagnostic for BPPV if positive, but does not rule it out if negative. The maneuver is performed on a flat examination table. While the patient is in a seated position, the physician August 15, 2010 Volume 82, Number 4 American Family Physician 363
4 ILLUSTRATION BY MARCIA HARSTOCK 45 A B Figure 1. Dix-Hallpike maneuver. While the patient is in a seated position, the physician (A) turns the patient s head 45 degrees to one side, then (B) rapidly lays the patient into a supine position with the head hanging about 20 degrees over the end of the table, observing the patient s eyes for approximately 30 seconds. The maneuver is repeated for the opposite side. Nystagmus is diagnostic of vestibular debris in the ear that is facing down, closest to the examination table. A video demonstration of this maneuver is available at Information from references 9 and 16. turns the patient s head 45 degrees to one side, then rapidly lays the patient into a supine position with the head hanging about 20 degrees over the end of the table and observes the patient s eyes for approximately 30 seconds. The maneuver is repeated with the head turned to the opposite side. Nystagmus is diagnostic of vestibular debris in the ear that is facing down, closest to the examination table. There is usually a latent period of a few seconds before the patient develops nystagmus, and a sensation of vertigo for up to one minute.9,16 The sensitivity of the Dix-Hallpike maneuver is 50 to 88 percent for BPPV.7 Lesions of the labyrinth and cranial nerve VIII (vestibulocochlear) commonly produce spontaneous nystagmus. Saccadic eye movements associated with a patient s smooth ocular pursuit of the physician s finger as it moves slowly left, right, up, and down may be associated with a central cause, such as brainstem or cerebellar disease. The head impulse test involves asking the patient to remain focused on a target while the physician moves the patient s head back and forth rapidly. Eye movement to one side with a refixation saccade (rapid oscillatory eye movement that occurs as the eye fixes on an object) is indicative of a lesion on the side to which the eyes move. Bilateral refixation movements commonly occur with ototoxicity. Another test that can elicit nystagmus involves the patient leaning forward 30 degrees while the physician shakes the patient s head back and forth vigorously for 20 seconds. The presence of nystagmus indicates a peripheral cause in the ipsilateral direction of the nystagmus American Family Physician Other physical examination tests include the Romberg test and observation of gait. Swaying toward one side with the Romberg test is indicative of vestibular dysfunction in the ipsilateral side. Also, a patient s gait will lean toward the side of a vestibular lesion. Ataxia is indicative of cerebellar dysfunction, and the patient s gait is usually slow, wide-based, and irregular.9,20 Observation of gait is also important to detect symptoms suggestive of parkinsonism in patients presenting with disequilibrium.4 In early Parkinson disease, gait is usually slower with smaller steps and reduced arm swing, and progresses to freezing and hesitation in later stages of the disease.20 Screening for peripheral neuropathy is also important in patients presenting with disequilibrium.4 If hyperventilation syndrome is suspected, the diagnosis can be confirmed by having the patient rapidly take 20 deep inhalations and exhalations, in an attempt to reproduce symptoms.9,18 A thorough cardiovascular examination should be performed in all patients with dizziness. However, tests such as electrocardiography, Holter monitor testing, and carotid Doppler testing should be performed only if an underlying cardiac cause is suspected based on other findings or known cardiac disease.7 Additional Testing In general, laboratory testing and radiography are not beneficial in the work-up of patients with dizziness when no other neurologic abnormalities are present.31,32 Laboratory studies, including complete blood count, Volume 82, Number 4 August 15, 2010
5 Approach to the Patient with Dizziness Dizziness Patient presents with dizziness Ask about medication regimen; caffeine, nicotine, and alcohol intake; and history of head trauma or whiplash What sensation does the patient describe? False sense of motion or spinning sensation Ask about migraine symptoms Migrainous vertigo is diagnosed with history of episodic vertigo with a current migraine or history of migraine and one of the following symptoms during at least two episodes of vertigo: migraine headache, photophobia, phonophobia, aura Off-balance or wobbly Dysequilibrium Consider possible underlying conditions, such as peripheral neuropathy and Parkinson disease Recheck medication regimen, especially in older patients Examine gait and vision, perform Romberg test, screen for neuropathy Feeling of losing consciousness or blacking out Presyncope Ask about history of arrhythmias and myocardial infarction Recheck medication regimen, especially in older patients Measure orthostatic blood pressures Vague symptoms, possibly feeling disconnected with the environment Lightheadedness Ask about history of anxiety or depression Perform hyperventilation provocation test Yes Hearing loss? No Consider cardiac testing in patients with relevant history Episodic vertigo? Episodic vertigo? Yes No Yes No Meniere disease Labyrinthitis Benign paroxysmal positional vertigo Vestibular neuritis Perform Dix-Hallpike maneuver (Figure 1) Figure 2. Algorithm for the initial evaluation of a patient with dizziness. metabolic panels, and thyroid function tests, have very low yield in diagnosing a cause of dizziness. In one meta-analysis, only 26 of 4,538 patients (0.6 percent) had laboratory abnormalities that explained their dizziness. 7 Electronystagmography tests vestibular function by using electrodes to detect nystagmus. The test has a reported sensitivity of 69 to 74 percent and specificity of 81 to 83 percent for peripheral vestibular disorders. For central vestibular disorders, sensitivity has been reported as high as 81 percent and specificity as high as 93 percent. 7 Approach to the Patient After obtaining the patient history, the physician can tailor the physical examination to best fit the differential diagnosis. One approach to the initial evaluation of patients with dizziness is presented in Figure 2. The initial history can help place the diagnosis into one of the four major categories of dizziness. Then, questions specific to that category can further narrow the possible diagnoses. A thorough neurologic and cardiovascular examination should be performed in all patients, as well as targeted components of the physical examination based on suspicion of the underlying diagnosis. Further testing, such as cardiac and radiologic testing, is only needed when specific causes are suspected. Treatment of vertigo has been addressed. 33 Table 4 summarizes the treatment of selected causes of dizziness, 10,18,34-49 and Figure 3 illustrates the Epley maneuver, an effective treatment for BPPV. 41 August 15, 2010 Volume 82, Number 4 American Family Physician 365
6 Table 4. Treatment for Selected Causes of Dizziness Cause Treatment Comments Benign paroxysmal positional vertigo Meniere disease Vestibular neuritis Meclizine (Antivert), 25 to 50 mg orally every four to six hours Epley maneuver (canalith repositioning; see Figure 3) Vestibular rehabilitation Salt restriction (less than 1 to 2 g of sodium per day) and/or diuretics (most commonly, hydrochlorothiazide/ triamterene [Dyazide]) Intratympanic dexamethasone or gentamicin Endolymphatic sac surgery Methylprednisolone (Depo-Medrol), initially 100 mg orally daily then tapered to 10 mg orally daily over three weeks Migrainous vertigo Migraine prophylaxis with serotonin 5-HT 1 receptor agonists (triptans) Presyncope Orthostatic hypotension Disequilibrium Lightheadedness Hyperventilation syndrome Review medication regimen Midodrine (Proamatine) titrated up to 10 mg orally three times daily Fludrocortisone, initially 0.1 mg orally daily, titrated up weekly until peripheral edema develops or to a maximal dosage of 1 mg daily Pseudoephedrine, 30 to 60 mg orally daily Paroxetine (Paxil), 20 mg orally daily Desmopressin (DDAVP), 5 to 40 mcg intranasally daily Treatment of underlying cause (e.g., peripheral neuropathy, Parkinson disease) Breathing control exercises, rebreathing into a small paper bag Beta blockers Antianxiety agents (e.g., selective serotonin reuptake inhibitors) or shortterm use of benzodiazepines Commonly used to reduce symptoms of acute episodes of vertigo, although there are no RCTs to support its use; use of vestibular suppressants can lead to brainstem compensation and prolong vertiginous symptoms Main benign paroxysmal positional vertigo treatment; safe and effective compared with placebo; video demonstration is available at Series of head and neck exercises that can be performed daily at home; video demonstration available at watch?v=hhinu_ou_hm Evidence for balance therapy (e.g., tai chi, Wii Fit) is accumulating No large-scale RCTs to support these therapies Referral to an otolaryngologist required; in one small study, dexameth asone resolved symptoms in 82 percent of patients; in a larger study, gentamicin resolved symptoms in 80.7 percent of patients 46,47 Referral to an otolaryngologist required In an RCT, methylprednisolone was more effective in improving peripheral vestibular function than valacyclovir (Valtrex) in patients with vestibular neuritis 49 Treatment based on expert opinion, not RCTs This is the first step, especially in older patients; rehydration (even increased water intake) can improve symptoms, especially in those with autonomic failure Alpha-1 agonist metabolite; to avoid supine hypertension, the third dose should be given by 6 p.m.; should be used only in severely impaired patients; in placebo-controlled trials, midodrine was associated with increased standing blood pressures and fewer orthostatic symptoms compared with placebo 36 Mineralocorticoids, such as fludrocortisone, are used to increase sodium and water retention; monitor blood pressure, potassium level, and for symptoms of heart failure Fludrocortisone and midodrine can be used in combination if either agent alone fails to control symptoms These drugs are options when midodrine and fludrocortisone are ineffective Nondrug therapy includes replacement of fluids, rising slowly from lying or sitting positions, sleeping with the head of the bed elevated, increasing salt intake, and regular exercise Because disequilibrium is generally a symptom of an underlying condition, treatment of the condition improves symptoms of disequilibrium Reverses hypocapnia-related symptoms Treats associated symptoms, such as palpitations and sweating; not for use in patients with asthma For use in patients with underlying anxiety RCT = randomized controlled trial. Information from references 10, 18, and 34 through 49.
7 45 A B ILLUSTRATION BY MARCIA HARSTOCK C D Figure 3. Epley maneuver (canalith repositioning). The technique involves a series of movements. (A) The maneuver begins with the patient sitting with the head rotated 45 degrees to the right. (B) The physician lays the patient into a supine position with the head hanging over the end of the table. (C) The head is then rotated 90 degrees to the left, (D) and the head and body are rotated together an additional 90 degrees until the patient is 135 degrees from the initial supine position. (E) The patient is brought to a sitting position while the head remains tilted. Finally, the head is brought forward and downward to an angle of 20 degrees. The physician should pause at each position until nystagmus resolves, and the whole series should be repeated until no nystagmus is present at any position. The maneuver can also begin with the patient in the supine position. A video demonstration of this maneuver is available at watch?v=zqokxzrbjfw&nr=1. E Information from reference 41. The Authors ROBERT E. POST, MD, is a faculty member with the Virtua Family Medicine Residency in Voorhees, N.J. At the time this article was written, he was an instructor in the Department of Family Medicine at the Medical University of South Carolina in Charleston. LORI M. DICKERSON, PharmD, is a professor in the Trident Medical Center/Medical University of South Carolina Family Medicine Residency Program. August 15, 2010 Volume 82, Number 4 Address correspondence to Robert E. Post, MD, 2225 Evesham Rd., Suite 101, Voorhees, NJ ( rpostmd@gmail.com). Reprints are not available from the authors. Author disclosure: Nothing to disclose. REFERENCES 1. Schappert SM, Burt CW. Ambulatory care visits to physician offices, hospital outpatient departments, and emergency departments. Vital Health Stat ;(159): American Family Physician 367
8 Dizziness 2. Sloane PD. Dizziness in primary care. J Fam Pract. 1989;29(1): Kerber KA, Meurer WJ, West BT, et al. Dizziness presentations in U.S. emergency departments, Acad Emerg Med. 2008; 15(8): Kroenke K, Lucas CA, Rosenberg ML, et al. Causes of persistent dizziness. Ann Intern Med. 1992;117(11): Herr RD, Zun L, Mathews JJ. A directed approach to the dizzy patient. Ann Emerg Med. 1989;18(6): Newman-Toker DE, Cannon LM, Stofferahn ME, et al. Imprecision in patient reports of dizziness symptom quality: a crosssectional study conducted in an acute care setting. Mayo Clin Proc. 2007;82(11): Hoffman RM, Einstadter D, Kroenke K. Evaluating dizziness. Am J Med. 1999;107(5): Kentala E, Rauch SD. A practical assessment algorithm for diagnosis of dizziness. Otolaryngol Head Neck Surg. 2003;128(1): Goebel JA. The ten-minute examination of the dizzy patient. Semin Neurol. 2001;21(4): Gupta V, Lipsitz LA. Orthostatic hypotension in the elderly: diagnosis and treatment. Am J Med. 2007;120(10): The seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Bethesda, Md.: National Heart, Lung, and Blood Institute; August NIH publication no jnc7full.pdf. Accessed September 2, Fitzgerald DC. Head trauma: hearing loss and dizziness. J Trauma. 1996;40(3): Hanley K, O Dowd T, Considine N. A systematic review of vertigo in primary care. Br J Gen Pract. 2001;51(469): Agrawal Y, Carey JP, Della Santina CC, et al. Disorders of balance and vestibular function in US adults: data from the National Health and Nutrition Examination Survey, [published correction appears in Arch Intern Med. 2009;169(15):1419]. Arch Intern Med. 2009;169(10): Lempert T, Neuhauser H, Daroff RB. as a symptom of migraine. Ann N Y Acad Sci. 2009;1164: Colledge NR, Barr-Hamilton RM, Lewis SJ, et al. Evaluation of investigations to diagnose the cause of dizziness in elderly people: a community based controlled study. BMJ. 1996;313(7060): Nedzelski JM, Barber HO, McIlmoyl L. Diagnoses in a dizziness unit. J Otolaryngol. 1986;15(2): Gardner WN. The pathophysiology of hyperventilation disorders. Chest. 1996;109(2): McGee S, Abernethy WB III, Simel DL. The rational clinical examination. Is this patient hypovolemic? JAMA. 1999;281(11): Ebersbach G, Sojer M, Valldeoriola F, et al. Comparative analysis of gait in Parkinson s disease, cerebellar ataxia and subcortical arteriosclerotic encephalopathy. Brain. 1999;122(pt 7): Newman-Toker DE, Hsieh YH, Camargo CA Jr, et al. Spectrum of dizziness visits to US emergency departments: cross-sectional analysis from a nationally representative sample. Mayo Clin Proc. 2008;83(7): Kroenke K, Hoffman RM, Einstadter D. How common are various causes of dizziness? A critical review. South Med J. 2000;93(2): Wood KA, Drew BJ, Scheinman MM. Frequency of disabling symptoms in supraventricular tachycardia. Am J Cardiol. 1997;79(2): Fick DM, Cooper JW, Wade WE, et al. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts [published correction appears in Arch Intern Med. 2004;164(3):298]. Arch Intern Med. 2003;163(22): Kerber KA, Brown DL, Lisabeth LD, et al. Stroke among patients with dizziness, vertigo, and imbalance in the emergency department: a population-based study. Stroke. 2006;37(10): Wiltink J, Tschan R, Michal M, et al. Dizziness: anxiety, health care utilization and health behavior. J Psychosom Res. 2009;66(5): Yardley L, Owen N, Nazareth I, et al. Panic disorder with agoraphobia associated with dizziness. J Nerv Ment Dis. 2001;189(5): Teggi R, Caldirola D, Bondi S, et al. Vestibular testing in patients with panic disorder and chronic dizziness. Acta Otorhinolaryngol Ital. 2007;27(5): Staab JP, Ruckenstein MJ. Expanding the differential diagnosis of chronic dizziness. Arch Otolaryngol Head Neck Surg. 2007;133(2): Nagy E, Claussen CF, Bencze G, et al. Depressive disorders in relation to neurootological complaints. Int Tinnitus J. 2004;10(1): Colledge N, Lewis S, Mead G, et al. Magnetic resonance brain imaging in people with dizziness: a comparison with non-dizzy people. J Neurol Neurosurg Psychiatry. 2002;72(5): Wasay M, Dubey N, Bakshi R. Dizziness and yield of emergency head CT scan: is it cost effective? Emerg Med J. 2005;22(4): Swartz R, Longwell P. Treatment of vertigo. Am Fam Physician. 2005; 71(6): Brignole M, Alboni P, Benditt DG, et al. Guidelines on management (diagnosis and treatment) of syncope. Europace. 2004;6(6): Shannon JR, Diedrich A, Biaggioni I, et al. Water drinking as a treatment for orthostatic syndromes. Am J Med. 2002;112(5): Low PA, Gilden JL, Freeman R, et al. Efficacy of midodrine vs placebo in neurogenic orthostatic hypotension. [published correction appears in JAMA. 1997;278(5):388]. JAMA. 1997;277(13): Freeman R. Clinical practice. Neurogenic orthostatic hypotension. N Engl J Med. 2008;358(6): Hain TC, Uddin M. Pharmacological treatment of vertigo. CNS Drugs. 2003;17(2): Kuo CH, Pang L, Chang R. - part 2 - management in general practice. Aust Fam Physician. 2008;37(6): Fife TD, Iverson DJ, Lempert T, et al. Practice parameter: therapies for benign paroxysmal positional vertigo (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2008;70(22): Hilton M, Pinder D. The Epley (canalith repositioning) manoeuvre for benign paroxysmal positional vertigo. Cochrane Database Syst Rev. 2004; (2):CD Yardley L, Donovan-Hall M, Smith HE, et al. Effectiveness of primary care-based vestibular rehabilitation for chronic dizziness. Ann Intern Med. 2004;141(8): Thirlwall AS, Kundu S. Diuretics for Ménière s disease or syndrome. Cochrane Database Syst Rev. 2006;3:CD van Deelen GW, Huizing EH. Use of a diuretic (Dyazide) in the treatment of Menière s disease. ORL J Otorhinolaryngol Relat Spec. 1986;48(5): Santos PM, Hall RA, Snyder JM, et al. Diuretic and diet effect on Menière s disease evaluated by the 1985 Committee on Hearing and Equilibrium guidelines. Otolaryngol Head Neck Surg. 1993;109(4): Garduño-Anaya MA, Couthino De Toledo H, Hinojosa-González R, et al. Dexamethasone inner ear perfusion by intratympanic injection in unilateral Ménière s disease. Otolaryngol Head Neck Surg. 2005;133(2): De Beer L, Stokroos R, Kingma H. Intratympanic gentamicin therapy for intractable Ménière s disease. Acta Otolaryngol. 2007;127(6): Wetmore SJ. Endolymphatic sac surgery for Ménière s disease. Arch Otolaryngol Head Neck Surg. 2008;134(11): Strupp M, Zingler VC, Arbusow V, et al. Methylprednisolone, valacyclovir, or the combination for vestibular neuritis. N Engl J Med. 2004; 351(4): American Family Physician Volume 82, Number 4 August 15, 2010
Benign Paroxysmal Positional Vertigo (BPPV)
 Benign Paroxysmal Positional Vertigo (BPPV) UHN Information for Patients Patient Education Improving Health Through Education You have been told by your doctor that you have Benign Paroxysmal Positional
Benign Paroxysmal Positional Vertigo (BPPV) UHN Information for Patients Patient Education Improving Health Through Education You have been told by your doctor that you have Benign Paroxysmal Positional
Vestibular Rehabilitation Therapy. Melissa Nelson
 Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Introduction to Dizziness and the Vestibular System
 Introduction to Dizziness and the Vestibular System David R Friedland, MD, PhD Professor and Vice-Chairman Chief, Division of Otology and Neuro-otologic Skull Base Surgery Chief, Division of Research Department
Introduction to Dizziness and the Vestibular System David R Friedland, MD, PhD Professor and Vice-Chairman Chief, Division of Otology and Neuro-otologic Skull Base Surgery Chief, Division of Research Department
Vestibular Rehabilitation
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
Vestibular Rehabilitation What s the Spin?
 Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Workup and Management of Vertigo
 Workup and Management of Vertigo S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 25, 2008 The speaker has no disclosures Two Key Questions 1. What do you
Workup and Management of Vertigo S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 25, 2008 The speaker has no disclosures Two Key Questions 1. What do you
Dizziness and Vertigo
 Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic
 Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Dizziness: More than BPPV or Meniere s. William J Garvis, MD Otology, Neurotology & Skull Base Surgery Ear, Nose & Throat SpecialtyCare of MN, PA
 Dizziness: More than BPPV or Meniere s William J Garvis, MD Otology, Neurotology & Skull Base Surgery Ear, Nose & Throat SpecialtyCare of MN, PA American Family Physician Dizziness: A Diagnostic Approach
Dizziness: More than BPPV or Meniere s William J Garvis, MD Otology, Neurotology & Skull Base Surgery Ear, Nose & Throat SpecialtyCare of MN, PA American Family Physician Dizziness: A Diagnostic Approach
Dizziness and balance problems
 Dizziness and balance problems Dizziness and balance problems, Action on Hearing Loss Information, May 2011 1 Dizziness and balance problems This factsheet is part of our Ears and ear problems range. It
Dizziness and balance problems Dizziness and balance problems, Action on Hearing Loss Information, May 2011 1 Dizziness and balance problems This factsheet is part of our Ears and ear problems range. It
Vestibular Injury. Vestibular Disorders Association www.vestibular.org Page 1 of 5
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Vestibular Injury Compensation, De-compensation, and Failure to Compensate By Thomas E. Boismier,
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Vestibular Injury Compensation, De-compensation, and Failure to Compensate By Thomas E. Boismier,
Clinical Glidepath TM Tools Syncope Frail Life expectancy less than five years or significant functional impairment
 Robust Elderly greater ALL GROUPS 1 SYMPTOMS a) wth, nausea b) postural symptoms c) chest pain, dyspnea, post-exercise, dizziness, history of heart disease, palpitations, family history (prolonged QT)
Robust Elderly greater ALL GROUPS 1 SYMPTOMS a) wth, nausea b) postural symptoms c) chest pain, dyspnea, post-exercise, dizziness, history of heart disease, palpitations, family history (prolonged QT)
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL
 BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Vestibular Injury: Compensation, Decompensation, and Failure to Compensate
 VESTIBULAR DISORDERS ASSOCIATION PO Box 13305 Portland, OR 97213 fax: (503) 229-8064 toll-free voice-mail: (800) 837-8428 info@vestibular.org http://www.vestibular.org/ VEDA Publication No. F-26 Vestibular
VESTIBULAR DISORDERS ASSOCIATION PO Box 13305 Portland, OR 97213 fax: (503) 229-8064 toll-free voice-mail: (800) 837-8428 info@vestibular.org http://www.vestibular.org/ VEDA Publication No. F-26 Vestibular
Benign Paroxysmal Positional Vertigo. By Mick Benson
 Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT
 Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
Vertigo, a type of dizziness, is the
 Treatment of Vertigo RANDY SWARTZ, M.D., University of California, San Diego, School of Medicine, La Jolla, California PAXTON LONGWELL, M.D., Corpus Christi, Texas Vertigo is the illusion of motion, usually
Treatment of Vertigo RANDY SWARTZ, M.D., University of California, San Diego, School of Medicine, La Jolla, California PAXTON LONGWELL, M.D., Corpus Christi, Texas Vertigo is the illusion of motion, usually
Nursing Care of Patients with Movement Disorders. Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014
 Nursing Care of Patients with Movement Disorders Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014 Types of Movement Disorders Parkinson s disease Huntington s disease Dystonia Tremors
Nursing Care of Patients with Movement Disorders Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014 Types of Movement Disorders Parkinson s disease Huntington s disease Dystonia Tremors
How To Treat An Elderly Patient
 1. Introduction/ Getting to know our Seniors a. Identify common concepts and key terms used when discussing geriatrics b. Distinguish between different venues of senior residence c. Advocate the necessity
1. Introduction/ Getting to know our Seniors a. Identify common concepts and key terms used when discussing geriatrics b. Distinguish between different venues of senior residence c. Advocate the necessity
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
National Hospital for Neurology and Neurosurgery. Inner ear balance problems. Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Inner ear balance problems Department of Neuro-otology If you would like this document in another language or format or if you require the services of an
National Hospital for Neurology and Neurosurgery Inner ear balance problems Department of Neuro-otology If you would like this document in another language or format or if you require the services of an
Post-Concussion Syndrome
 Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health & Science University, Portland, Oregon
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
Conflicts of interest: None
 Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling
 Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
Dallas Neurosurgical and Spine Associates, P.A Patient Health History
 Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Vestibular Migraine May 2013
 TITLE: Vestibular Migraine SOURCE: Grand Rounds Presentation, Department of Otolaryngology The University of Texas Medical Branch (UTMB Health) DATE: May 23, 2013 RESIDENT PHYSICIAN: Matthew Yantis, MD
TITLE: Vestibular Migraine SOURCE: Grand Rounds Presentation, Department of Otolaryngology The University of Texas Medical Branch (UTMB Health) DATE: May 23, 2013 RESIDENT PHYSICIAN: Matthew Yantis, MD
Trouble Getting a Diagnosis?
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG By the Vestibular Disorders Association Trouble Getting a Diagnosis? Many people who suffer from
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG By the Vestibular Disorders Association Trouble Getting a Diagnosis? Many people who suffer from
Low Blood Pressure. This reference summary explains low blood pressure and how it can be prevented and controlled.
 Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
II. VESTIBULAR SYSTEM OVERVIEW
 HM513 Vertigo and Dizziness; Vestibular System Disorders - Summary Eric Eggenberger*, DO and Kathryn Lovell, PhD *Co-Director, MSU Neuro-Visual Unit; *Director, MSU Ocular Motility Lab Department of Neurology
HM513 Vertigo and Dizziness; Vestibular System Disorders - Summary Eric Eggenberger*, DO and Kathryn Lovell, PhD *Co-Director, MSU Neuro-Visual Unit; *Director, MSU Ocular Motility Lab Department of Neurology
Chronic Subjective Dizziness
 Chronic Subjective Dizziness MichaelJ. Ruckenstein, MD, MSc, FACS, FRCSC a, *, Jeffrey P. Staab, MD, MS a,b KEYWORDS Dizziness Vertigo Anxiety Migraine The symptom of dizziness represents a nonspecific
Chronic Subjective Dizziness MichaelJ. Ruckenstein, MD, MSc, FACS, FRCSC a, *, Jeffrey P. Staab, MD, MS a,b KEYWORDS Dizziness Vertigo Anxiety Migraine The symptom of dizziness represents a nonspecific
Alcohol Withdrawal Syndromes
 Alcohol Withdrawal Syndromes Should You Treat This Patient s Alcohol Withdrawal With Benzodiazepines?! Meta-analysis of RCTs of benzodiazepines for the treatment of alcohol withdrawal! 11 RCTs identified,
Alcohol Withdrawal Syndromes Should You Treat This Patient s Alcohol Withdrawal With Benzodiazepines?! Meta-analysis of RCTs of benzodiazepines for the treatment of alcohol withdrawal! 11 RCTs identified,
Living with Low Blood Pressure
 Living with Low Blood Pressure Understand the medical jargon and tips on how to cope with low Blood Pressure (BP) What is low blood pressure? Blood pressure (BP) is measured in millimetres of mercury (mm
Living with Low Blood Pressure Understand the medical jargon and tips on how to cope with low Blood Pressure (BP) What is low blood pressure? Blood pressure (BP) is measured in millimetres of mercury (mm
SPECIALITY: AUDIOVESTIBULAR MEDICINE CLINICAL PROBLEMS: DIZZINESS, VERTIGO AND IMBALANCE. Introduction
 St Richard s Hospital SPECIALITY: AUDIOVESTIBULAR MEDICINE CLINICAL PROBLEMS: DIZZINESS, VERTIGO AND IMBALANCE Introduction Whilst dizziness, vertigo and imbalance may be due to systemic disease, they
St Richard s Hospital SPECIALITY: AUDIOVESTIBULAR MEDICINE CLINICAL PROBLEMS: DIZZINESS, VERTIGO AND IMBALANCE Introduction Whilst dizziness, vertigo and imbalance may be due to systemic disease, they
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Multiple System Atrophy
 Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Headaches in Children How to Manage Difficult Headaches
 Headaches in Children How to Manage Difficult Headaches Peter Procopis Childhood headaches Differential diagnosis Migraine Psychological Raised Pressure Childhood headaches Other causes: Constitutional
Headaches in Children How to Manage Difficult Headaches Peter Procopis Childhood headaches Differential diagnosis Migraine Psychological Raised Pressure Childhood headaches Other causes: Constitutional
Otologic (Ear) Dizziness. Fistula Other. SCD Bilateral. Neuritis. Positional Vertigo BPPV. Menieres
 Otologic Dizziness (Dizziness from Ear) Ear Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
Otologic Dizziness (Dizziness from Ear) Ear Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
Headaches and Kids. Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital
 Headaches and Kids Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital Overview Headache classifications and diagnosis Address common headache
Headaches and Kids Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital Overview Headache classifications and diagnosis Address common headache
A Flow Chart For Classification Of Nystagmus
 A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout.
 Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
St. Luke s MS Center New Patient Questionnaire. Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor?
 St. Luke s MS Center New Patient Questionnaire Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor? Who referred you to the MS Center? List any other doctors you see: Reason you have
St. Luke s MS Center New Patient Questionnaire Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor? Who referred you to the MS Center? List any other doctors you see: Reason you have
JAMES PETROS, M.D., INC. PHONE: (408) 528-8833 FAX: (408) 528-8557
 FIGHTING PAIN. TOUCHING LIVES. JAMES PETROS, M.D., INC. PHONE: (408) 528-8833 FAX: (408) 528-8557 Personal Information Emergency Contact Today s Date: Name: Patient: Realtionship: Birth Date: Age: Sex:
FIGHTING PAIN. TOUCHING LIVES. JAMES PETROS, M.D., INC. PHONE: (408) 528-8833 FAX: (408) 528-8557 Personal Information Emergency Contact Today s Date: Name: Patient: Realtionship: Birth Date: Age: Sex:
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Neck Pain & Cervicogenic Headache Integrating Research into Practice: San Luis Sports Therapy s Approach to Evidence-Based Practice
 Neck Pain & Cervicogenic Headache Integrating Research into Practice: San Luis Sports Therapy s Approach to Evidence-Based Practice PROBLEM: Neck Pain and Cervicogenic Headache 66% Proportion of individuals
Neck Pain & Cervicogenic Headache Integrating Research into Practice: San Luis Sports Therapy s Approach to Evidence-Based Practice PROBLEM: Neck Pain and Cervicogenic Headache 66% Proportion of individuals
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only)
 PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
Treatments for Major Depression. Drug Treatments The two (2) classes of drugs that are typical antidepressants are:
 Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA
 Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Depression in Older Persons
 Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
SYMPTOMS Heart failure symptoms may vary and can be hard to detect. Symptoms may include:
 Heart Failure Heart failure is a condition in which the heart has trouble pumping blood. This means your heart does not pump blood efficiently for your body to work well. In some cases of heart failure,
Heart Failure Heart failure is a condition in which the heart has trouble pumping blood. This means your heart does not pump blood efficiently for your body to work well. In some cases of heart failure,
How To Diagnose Stroke In Acute Vestibular Syndrome
 Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
Danica Dummer, PT, DPT, University of Utah Abigail Reid, PT, DPT, Kessler Institute for Rehabilitation Online Journal Club-Article Review Article Citation Study Objective/Purpose (hypothesis) Study Design
Chiari Malformation: Symptoms
 Chiari Malformation: Symptoms SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
Chiari Malformation: Symptoms SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
Medications and Falls
 Virginia Commonwealth University VCU Scholars Compass Case Studies from Age in Action Virginia Center on Aging 1998 Medications and Falls Patricia W. Slattum Virginia Commonwealth University, pwslattu@vcu.edu
Virginia Commonwealth University VCU Scholars Compass Case Studies from Age in Action Virginia Center on Aging 1998 Medications and Falls Patricia W. Slattum Virginia Commonwealth University, pwslattu@vcu.edu
Concussions and Mild Head Injury. Post Concussion Syndrome. Whiplash Injuries
 Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
Causes of Dizziness. Because of the many possible causes of dizziness, getting a correct diagnosis can be a long and frustrating experience.
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Causes of Dizziness Dizziness, vertigo, and disequilibrium are common symptoms reported by adults
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Causes of Dizziness Dizziness, vertigo, and disequilibrium are common symptoms reported by adults
Heart Failure: Diagnosis and Treatment
 Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Meniere s Disease. By David Foyt, M.D.
 Meniere s Disease By David Foyt, M.D. This paper covers basic information about Meniere s Disease, Its Possible Causes and Implications Meniere's disease is a disorder of the inner ear which causes episodes
Meniere s Disease By David Foyt, M.D. This paper covers basic information about Meniere s Disease, Its Possible Causes and Implications Meniere's disease is a disorder of the inner ear which causes episodes
Emergency Scenario. Chest Pain
 Emergency Scenario Chest Pain This emergency scenario reviews chest pain in a primary care patient, and is set up for roleplay and case review with your staff. 1) The person facilitating scenarios can
Emergency Scenario Chest Pain This emergency scenario reviews chest pain in a primary care patient, and is set up for roleplay and case review with your staff. 1) The person facilitating scenarios can
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
SLEEP AND PARKINSON S DISEASE
 A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
New England Pain Management Consultants At New England Baptist Hospital
 New England Pain Management Consultants At New England Baptist Hospital Pain Management Center Health Assessment Dear New Pain Management Patient, Welcome to the New England Pain Management Consultants
New England Pain Management Consultants At New England Baptist Hospital Pain Management Center Health Assessment Dear New Pain Management Patient, Welcome to the New England Pain Management Consultants
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Webinar title: Know Your Options for Treating Severe Spasticity
 Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
What Can I Do about Atrial Fibrillation (AF)?
 Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
A Definition of Multiple Sclerosis
 English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
The practice of lowering blood pressure (BP)
 Original Paper Treatment of Hypertension in the Inpatient Setting: Use of Intravenous Labetalol and Hydralazine Alan B. Weder, MD; 1 Steven Erickson, PharmD 2 Acute blood pressure elevations are commonly
Original Paper Treatment of Hypertension in the Inpatient Setting: Use of Intravenous Labetalol and Hydralazine Alan B. Weder, MD; 1 Steven Erickson, PharmD 2 Acute blood pressure elevations are commonly
Parkinson's s disease - a
 Parkinson's Disease Parkinson's s disease - a progressive disorder of the nervous system that affects movement. The most common perception of Parkinson s is the patient having tremors. Hands shaking, inability
Parkinson's Disease Parkinson's s disease - a progressive disorder of the nervous system that affects movement. The most common perception of Parkinson s is the patient having tremors. Hands shaking, inability
NEW PATIENT CLINICAL INFORMATION FORM. Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute
 NEW PATIENT CLINICAL INFORMATION FORM Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute Date: Name: Referring Doctor: How did you hear about us? NWPF Your Physician:
NEW PATIENT CLINICAL INFORMATION FORM Booth Gardner Parkinson s Care & Movement Disorders Center Evergreen Neuroscience Institute Date: Name: Referring Doctor: How did you hear about us? NWPF Your Physician:
Michigan Ear Institute. Dizziness and Balance Disturbances. www.michiganear.com
 Michigan Ear Institute Dizziness and Balance Disturbances www.michiganear.com DOCTORS Jack M. Kartush, MD Dennis I. Bojrab, MD Michael J. LaRouere, MD John J. Zappia, MD, FACS Eric W. Sargent, MD, FACS
Michigan Ear Institute Dizziness and Balance Disturbances www.michiganear.com DOCTORS Jack M. Kartush, MD Dennis I. Bojrab, MD Michael J. LaRouere, MD John J. Zappia, MD, FACS Eric W. Sargent, MD, FACS
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Treatment of cardiogenic shock
 ACUTE HEART FAILURE AND COMORBIDITY IN THE ELDERLY Treatment of cardiogenic shock Christian J. Wiedermann, M.D., F.A.C.P. Associate Professor of Internal Medicine, Medical University of Innsbruck, Austria
ACUTE HEART FAILURE AND COMORBIDITY IN THE ELDERLY Treatment of cardiogenic shock Christian J. Wiedermann, M.D., F.A.C.P. Associate Professor of Internal Medicine, Medical University of Innsbruck, Austria
Southwest General Surgical Associates General & Vascular Surgery 8230 Walnut Hill Lane Suite 408 Dallas, TX 75231 Phone-214)369-5432 Fax-214)369-5591
 Southwest General Surgical Associates General & Vascular Surgery 8230 Walnut Hill Lane Suite 408 Dallas, TX 75231 Phone-214)369-5432 Fax-214)369-5591 Andres U. Katz, M.D. Richard S. Anderson, M.D. G. Thomas
Southwest General Surgical Associates General & Vascular Surgery 8230 Walnut Hill Lane Suite 408 Dallas, TX 75231 Phone-214)369-5432 Fax-214)369-5591 Andres U. Katz, M.D. Richard S. Anderson, M.D. G. Thomas
Hospital-based SNF Coding Tip Sheet: Top 25 codes and ICD-10 Chapter Overview
 Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
What s new, and why, in Neurology 4?
 What s new, and why, in Neurology 4? All topics in Neurology 4 have been extensively reviewed and updated by the expert writing group, to provide concise evidence-based advice for the busy practitioner.
What s new, and why, in Neurology 4? All topics in Neurology 4 have been extensively reviewed and updated by the expert writing group, to provide concise evidence-based advice for the busy practitioner.
GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS
 GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
The McGee Law Firm. 213 Princess Street Wilmington, NC 28401 (910) 254-0400
 The McGee Law Firm 213 Princess Street Wilmington, NC 28401 (910) 254-0400 DWI CLIENT INTERVIEW Date of Interview: Name: Address: Phone numbers: Home: Work: Cell: e-mail address DOB: / / Offense Date:
The McGee Law Firm 213 Princess Street Wilmington, NC 28401 (910) 254-0400 DWI CLIENT INTERVIEW Date of Interview: Name: Address: Phone numbers: Home: Work: Cell: e-mail address DOB: / / Offense Date:
NEW PATIENT HISTORY Mark L. Prasarn, M.D.
 NEW PATIENT HISTORY Mark L. Prasarn, M.D. Date: Name: Age: Height: Weight: Pharmacy: Phar. Phone#: Primary Care M.D. Referring M.D.: What is your Chief Complaint? What makes the pain better? Neck Pain
NEW PATIENT HISTORY Mark L. Prasarn, M.D. Date: Name: Age: Height: Weight: Pharmacy: Phar. Phone#: Primary Care M.D. Referring M.D.: What is your Chief Complaint? What makes the pain better? Neck Pain
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
Fits, Faints and Funny Turns. Kate Ingram Geriatrician SCGH
 Fits, Faints and Funny Turns Kate Ingram Geriatrician SCGH 84 year old man presents to ED after falling overnight and being found the next morning by a carer on the floor in his hallway. After being treated
Fits, Faints and Funny Turns Kate Ingram Geriatrician SCGH 84 year old man presents to ED after falling overnight and being found the next morning by a carer on the floor in his hallway. After being treated
22/02/2015. Possible causes. Decisions decisions decisions. Challenging eye and ear conditions at underwriting and claim stage Dr Maritha van der Walt
 Challenges Underwriting symptoms rather than conditions- tinnitus, vertigo, blurred vision Requests for narrower rather than broad exclusions and consequences Pre existing condition and unrelated claims
Challenges Underwriting symptoms rather than conditions- tinnitus, vertigo, blurred vision Requests for narrower rather than broad exclusions and consequences Pre existing condition and unrelated claims
What to Know About. Atrial Fibrillation
 Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Vestibular Disorders: An Overview
 5018 NE 15 TH AVE, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG Vestibular Disorders: An Overview By the Vestibular Disorders Association The vestibular system includes
5018 NE 15 TH AVE, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG Vestibular Disorders: An Overview By the Vestibular Disorders Association The vestibular system includes
DISCLOSURES RISK ASSESSMENT. Stroke and Heart Disease -Is there a Link Beyond Risk Factors? Daniel Lackland, MD
 STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
Erectile Dysfunction (ED)
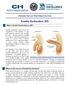 Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
One of the most common and frustrating
 Initial Evaluation of Vertigo RONALD H. LABUGUEN, M.D., University of Southern California, Los Angeles, California Benign paroxysmal positional vertigo, acute vestibular neuronitis, and Ménière s disease
Initial Evaluation of Vertigo RONALD H. LABUGUEN, M.D., University of Southern California, Los Angeles, California Benign paroxysmal positional vertigo, acute vestibular neuronitis, and Ménière s disease
Headaches in Children
 Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
