First human experience with endoscopically delivered and retrieved duodenal-jejunal bypass sleeve
|
|
|
- Ruby Porter
- 8 years ago
- Views:
Transcription
1 Surgery for Obesity and Related Diseases 4 (2008) Original article with video First human experience with endoscopically delivered and retrieved duodenal-jejunal bypass sleeve Leonardo Rodriguez-Grunert, M.D. a, Manoel Passos Galvao Neto, M.D. b, Munir Alamo, M.D. a, Almino Cardoso Ramos, M.D. b, Percy Brante Baez, M.D. a, Michael Tarnoff, M.D., F.A.C.S. c, * a Centro de Cirugía de la Obesidad, Hospital DIPRECA, Las Condes, Santiago de Chile b Gastro Obeso Center, São Pãulo, Brazil c Department of Surgery, Tufts-New England Medical Center, Boston, Massachusetts Received May 11, 2007; revised June 26, 2007; accepted July 6, 2007 Abstract Keywords: Background: We report the first human experience with an endoscopic duodenal-jejunal bypass sleeve (DJBS) in a community hospital. Methods: The DJBS is a 60-cm sleeve anchored in the duodenum to create a duodenal-jejunal bypass. In a 12-patient prospective, open-label, single-center, 12-week study, the device was endoscopically implanted, left in situ, and retrieved. The study included 5 men and 7 women, with a mean body mass index of 43 kg/m 2. Of the 12 patients, 4 had type 2 diabetes. The primary endpoints were the incidence and severity of adverse events. The secondary outcomes included the percentage of excess weight loss and changes in co-morbid status. Results: The DJBS was endoscopically delivered and retrieved in all patients (mean implant/ explant time of 26.6 and 43.3 min, respectively). Of the 12 patients, 10 were able to maintain the device for 12 weeks and 2 underwent explantation after 9 days secondary to poor device placement. Several self-limited adverse events were possibly or definitely related to the device, including 6 episodes of abdominal pain, 18 of nausea, and 16 of vomiting, mainly within 2 weeks of implantation. Two partial pharyngeal tears occurred during explantation. Implant site inflammation was encountered in all patients. No device-related event was considered severe. The average percentage of excess weight loss for the 10 patients with the device in place for 12 weeks was 23.6%, with all patients achieving at least 10% excess weight loss. All 4 diabetic patients had normal fasting plasma glucose levels without hypoglycemic medication for the entire 12 weeks. Of these 4 patients, 3 had decreased hemoglobin A 1c of.5% by week 12. Conclusion: The DJBS can be safely delivered and removed endoscopically and left in situ for 12 weeks. The device had a favorable safety and encouraging efficacy profile. Randomized prospective trials are warranted. (Surg Obes Relat Dis 2008;4:55 59.) 2008 American Society for Metabolic and Bariatric Surgery. All rights reserved. Bariatric; Endoluminal; Diabetes; Obesity; Duodenum The 1998 National Institutes of Heath Panel on Weight Loss recommended that patients attempt to lose 10% of their body weight before undergoing surgery for weight loss [1]. Current strategies range from commercial diets to *Reprint requests: Michael Tarnoff, M.D., F.A.C.S., Tufts-England Medical Center, Box 900, Boston, MA staged approaches [2]. Although each of these methods has merit, considerable limitations exist. Diets carry little risk but are invariably unsuccessful. Staged approaches are paradoxical in that high-risk patients are exposed to two surgical procedures rather than one. Given these limitations, novel preoperative weight loss strategies are desirable. We recently reported our animal experience with an endoscopically delivered and retrieved, reversible duodenal-jeju /08/$ see front matter 2008 American Society for Metabolic and Bariatric Surgery. All rights reserved. doi: /j.soard
2 56 L. Rodriguez-Grunert et al. / Surgery for Obesity and Related Diseases 4 (2008) nal bypass sleeve (DJBS) [3]. The DJBS contains an implant that is endoscopically delivered and anchored in the proximal duodenum and a sleeve that is extended into the jejunum (Fig. 1). Chyme passes through the sleeve, creating an intestinal bypass/biliopancreatic diversion without the need for stapling or anastomosis. The device has not yet received Food and Drug Administration approval. This report details our first human experience with the DJBS. Methods Fig. 1. DJBS implant. In a 12-patient, prospective, open-label study, the device was endoscopically placed, left in situ for 12 weeks, and endoscopically retrieved. Patients were enrolled in the study after they were deemed candidates for gastric bypass in accordance with the 1991 National Institutes of Health guidelines [1]. The device was used to enhance the preoperative weight loss. The primary endpoints were the incidence and severity of adverse events. The secondary endpoints included the percentage of excess weight loss and changes in co-morbid status. Type 2 diabetes mellitus (T2DM) was considered improved if the patient had a reduction in fasting plasma glucose or hemoglobin A 1c or a decrease in the frequency or dosing of medications. T2DM was considered to have resolved if the fasting plasma glucose and hemoglobin A 1c had normalized and the patient no longer needed diabetes medication. Hypertension was considered improved if the systolic and/or diastolic pressure components had decreased or the patients had been able to reduce or discontinue medical therapy. Hypertension was considered to have resolved if the systolic and diastolic components were normal and the patient no longer required medication. Hyperlipidemia was considered improved if the patient had a decrease in laboratory values or a reduction or discontinuation of medical therapy. It was considered to have resolved if the laboratory values were normal and the patient no longer required medication. All patients provided written informed consent, and the hospital ethics committee approved the study. All participants had undergone a baseline evaluation, including history and physical examination, upper endoscopy, fasting blood tests, and a nutritional assessment. During all studyspecific visits, the safety and efficacy data were recorded using approved study forms. All 12 patients underwent general anesthesia. During the procedure, fluoroscopy and endoscopy were used to deliver the device. The implant was delivered using an over-thewire catheter system and was contained within a capsule at the distal end of the catheter. Once the capsule was placed in the duodenum, an inner catheter was pushed and the bowel negotiated with the aid of an atraumatic ball attached to the distal end of the catheter. The sleeve was attached to the catheter, which pulls the sleeve out of the capsule. Once the sleeve was fully deployed, the anchor was deployed from the capsule to sit within the duodenal bulb. The anchor is self-expanding, and the barbs engage the tissue to prevent movement. Contrast was flushed to ensure patency of the sleeve (Fig. 2). The sleeve and ball were detached from the catheter, and the catheter was removed from the bowel, leaving the implant in place. The total procedure and fluoroscopy times were recorded, as were any procedure-related adverse events. All patients were hospitalized for 24 hours and maintained on a liquid diet for 1 week. The diet was then advanced to puree and then solid food at weeks 2 and 4, respectively. After discharge, the patients were evaluated weekly for the first 8 weeks, at 10 and 12 weeks after implantation, and then again 72 hours after device removal. For the 12-week follow-up period, the patients were closely evaluated with a combination of serum testing, history, physical examination, and adverse event monitoring. Plain abdominal films and upper gastrointestinal studies with contrast were occasionally used to evaluate device position and assess for patency. Fig. 2. Contrast study showing patency of sleeve.
3 L. Rodriguez-Grunert et al. / Surgery for Obesity and Related Diseases 4 (2008) The patients received weight loss counseling before implantation and at each follow-up visit during the in vivo period. All patients were advised to consume a 1000-calorie low-fat diet. Although no food logs were used, the patients were asked to rate their desire for food and feelings of satiety at each visit compared with before implantation. No patient was lost to follow-up. During the explantation procedure, a combination of fluoroscopy and endoscopy was used for retrieval. Retrieval was accomplished by first collapsing the anchor by grabbing 1 of the proximal drawstrings using a custom grasper. Once collapsed, the anchor was pulled inside a custom retrieval hood placed on the end of the endoscope. The hood served to protect the tissue from the barbs during withdrawal, thus precluding the need for an overtube. The total procedure and fluoroscopy times were recorded, as were any adverse events. Follow-up endoscopy and clinical assessment were performed 72 hours after removal of the implant. Surveillance was done of the stomach and the duodenum. Results Of the 12 patients, 5 (41.7%) were men and 7 (58.3%) were women. The mean age was 41 years (range 28 54), and the mean body mass index (BMI) was 43 kg/m 2 (range 35 51). The mean starting weight was kg (range ). Of the patients who completed the study, 6 had at least 1 co-morbid condition. Of these 6 patients, 4 had T2DM, 4 had hypertension, and 3 had hyperlipidemia. Twelve implants were attempted and completed. The mean implant time was 26.6 minutes (range 20 51), with a mean fluoroscopy time of 14.5 minutes (range ). The time required for implanting the device was relatively constant across all 12 implants. Twelve explants were performed. The mean explant time was 43.3 minutes (range ), with a mean fluoroscopy time of 10.7 minutes (range ). Two procedure-related adverse events occurred in 2 patients: 1 oral-pharyngeal mucosal tear and 1 esophageal mucosal tear. These events both occurred during device removal. No event was considered serious by the investigator. A total of 71 adverse events were reported in the 12 patients during the in vivo period. Of these events, 55 (78%) were possibly or definitely related to the device. These events included 6 reports of abdominal pain, 1 of diarrhea, 1 of a gastrointestinal mucosal disorder/esophageal tear, 12 of implant site inflammation, 18 of nausea, 16 of vomiting, and 1 of a oral-pharyngeal mucosal tear. Most episodes of abdominal pain, nausea, or vomiting occurred during the first week of the study. None of these events were considered severe by the investigator. All events were rated mild or moderate, and all were self-limited. Tissue inflammation was uniformly present in all 12 patients at explantation. The inflammation was limited to the site of the anchor. These changes were noted only on endoscopy. Inflammatory pseudopolyps were a frequent finding at the 72-hour surveillance endoscopy after explantation. Of the 12 patients, 2 underwent explantation before their scheduled removal date (9 days into the implant) because of excessive abdominal pain and discomfort. No patient in the study experienced migration or obstruction. Similarly, no clinically significant abnormal blood values were reported. No serious adverse events related to the device or the procedure occurred. All events were anticipated in both occurrence and severity. Weight loss data were available for all 10 patients completing the study. The average percentage of excess weight loss for the 10 patients was 23.6% (range %; Fig. 3). All 10 patients were able to achieve 10% excess weight loss. The average total weight loss was 10.2 kg (range ). The average baseline BMI was 43 kg/m 2. The average ending BMI was 38.7, for an average decrease in BMI from baseline of 3.8 kg/m 2 (range ). All patients reported greater satiety and less food volume intake after the device was implanted. Of the 12 patients, 4 had T2DM, all of whom completed the study. All 4 patients had required oral medication to control their condition at baseline. In 3 of the 4 patients, T2DM had resolved within 24 hours of implantation. One patient showed no improvement. Of the 4 patients with a history of hypertension at baseline, all 4 completed the study. All patients had required oral medication at baseline to control their hypertension. By the end of the study, the hypertension of 1 patient had resolved, 1 patient had improvement, and 2 patients no change. Of the 3 patients with hyperlipidemia, all completed the study. At the end of the study, 2 had improvement and 1 showed no change. Additional blood tests relevant to safety included measures of serum amylase, liver function tests, complete blood count, routine chemistry, vitamins D and B 12, folate, iron, ferritin, and albumin. All laboratory values were normal during the study period, with the exception of transient alterations in serum bilirubin in select patients. Discussion Gastric bypass surgery results in anatomic alterations that each may play a role in its mechanism of action. Although continually debated, the restrictive (pouch), hormonal (gastric/duodenal bypass), malabsorptive (jejunal bypass), and neural (partial vagotomy) effects may all variably contribute to the known efficacy profile. Several studies have sought to further delineate these relative contributions. In the attempt to better understand the role of duodenal bypass, Rubino et al. [4] studied duodenal jejunal exclusion in a spontaneous, nonobese rat model of T2DM. That study
4 58 L. Rodriguez-Grunert et al. / Surgery for Obesity and Related Diseases 4 (2008) Mean %EWL Weeks Fig. 3. Percentage of excess weight loss with time for each patient; overall mean also shown. showed that bypassing the duodenum directly ameliorated T2DM, independently of effects on food intake, body weight, malabsorption, or nutrient delivery to the hindgut. Although still poorly understood, this concept could serve as the physiologic explanation for the rapid restoration of glycemic control seen after gastric bypass and other bariatric procedures. Others have studied the effect of jejunal bypass, for which an alternative, but related, theory is that the enhanced delivery of undigested nutrients to the distal small bowel plays a major role in the improved glycemic control and/or weight loss seen after gastric bypass surgery [5,6]. The time required for implanting the device was relatively constant. One delivery required additional time because of misplacement and replacement of the device. However, the consistent delivery time signifies the simplicity of the procedure, especially when considering that three different physicians with distinct skill sets placed the devices at differing times. All implants in this study were performed under general anesthesia; however, we believe that conscious sedation will be a viable option as our comfort level with the procedure increases. Of the 12 implants, 2 were removed before their scheduled date (9 days after implant). We believe this resulted from initial misplacement of the devices during implantation. In both cases, the device was placed too close to the pylorus. In 1 of these 2 patients, we unsuccessfully attempted to push the device distally with the end of the endoscope. Ultimately, both patients complained of persistent and moderate nausea, vomiting, and abdominal discomfort, and the devices were removed. All remaining patients completed the study per the protocol. Only 1 severe adverse event occurred during the study, which consisted of a report of severe abdominal pain related to preexisting kidney stones. Several other adverse events were noted, all of which were self-limited. The most common of these events included abdominal pain, nausea, and vomiting. We believe that the occurrence of these symptoms in the first 14 days is most reliably explained by early expansion of the anchor. After the first 14 days, the symptoms were most often associated with dietary indiscretion. The device was patent and stable in all 10 patients. No interference occurred with the ampulla of Vater, as evidenced by the normalcy of the blood test results and the lack of associated symptoms. Several patients had isolated, selflimited abnormalities in the total bilirubin measurements. The significance of this is unknown, but the self-limited nature and lack of associated laboratory abnormalities implies a lack of clinical relevance. Twelve endoscopic explantations were performed. The mean explant time in the first 2 and last 10 cases was 112 and 29 minutes, respectively. The 2 early cases were associated with difficulty dislodging the anchor from the duodenal wall. The 1 partial oral-pharyngeal tear and 1 esophageal tear that occurred during explantation each occurred in 1 of these first 2 cases. In each instance, failure to properly secure the anchor within the confines of the flexible hood resulted in tearing of the tissue. These events underscore the importance of proper hooding of the anchor. The 72-hour tissue response was consistent and ranged from mild focal inflammatory changes to diffuse inflammation and superficial mucosal erosions. All patients were noted to have small benign biopsy-proven pseudopolyps of unclear etiology. The stability of the anchor diameter after the first 14 days and the acceptable tissue response
5 L. Rodriguez-Grunert et al. / Surgery for Obesity and Related Diseases 4 (2008) indicates that the anchor provides an appropriate balance of mucosal erosion, tissue healing, and device stability. The 23.6% average excess weight loss and that all 10 patients had 10% excess weight loss are interesting results in the context of a 12-week study that also included counseling. All patients reported enhanced satiety and reduced food volume. This could be explained by any number of mechanisms, including, but not limited to, delayed gastric emptying or other alterations of gastrointestinal physiology. The changes in hypertension and hyperlipidemia were consistent with the degree of weight loss. The T2DM data could have resulted from the effect of the weight loss, but the rapid restoration to normalcy without medications might have been an independent effect of the duodenal bypass. Conclusion The results of our study indicate that the DJBS can be safely implanted and explanted during a 12-week period. The preliminary efficacy profile is encouraging and warrants additional investigation. Disclosures Supported by GI Dynamics, Incorporated, Watertown, Massachusetts. Supplementary data Supplementary data associated with this article can be found, in the online version, at References [1] National Institutes of Health. Clinical guidelines on the identification, evaluation and treatment of overweight and obesity in adults. Available from: Accessed May [2] Ault A. Two stage gastric surgery is safer for high risk patients. Presented April 3, 2004 at the Sages Annual Meeting (abstract). [3] Gersin K, Lembo A, Tarnoff M. Chronic in-vivo experience with an endoscopcically delivered and retrieved duodenal jejunal bypass sleeve in a porcine model. Presented April 22, 2007 at the Sages Annual Meeting. [4] Rubino F, Forgione A, Cummings DE, et al. The mechanism of diabetes control after gastrointestinal bypass surgery reveals a role of the proximal small intestine in the pathophysiology of type 2 diabetes. Ann Surg 2006;244: [5] Patriti A, Facchiano E, Annetti C, et al. Early improvement of glucose tolerance after ileal transposition in a non-obese type 2 diabetes rat model. Obes Surg 2005;15: [6] de Paula A, Macedo AL, Prudente AS, et al. Laparoscopic sleeve gastrectomy with ileal transposition pilot study of a new operation. Surg Obes Relat Dis 2006;2:464 7.
Transoral gastric volume reduction for weight management: technique and feasibility in 18 patients
 Surgery for Obesity and Related Diseases 6 (2010) 689 694 Video original article Transoral gastric volume reduction for weight management: technique and feasibility in 18 patients Stacy A. Brethauer, M.D.
Surgery for Obesity and Related Diseases 6 (2010) 689 694 Video original article Transoral gastric volume reduction for weight management: technique and feasibility in 18 patients Stacy A. Brethauer, M.D.
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
The first endoscopically-delivered device therapy for obese patients with type 2 diabetes
 DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach
 Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Treatment for Severely Obese Patients
 Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Obesity When to Recommend Surgery. Lily Chang, MD September 27, 2013
 Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 (IPG518) NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of implantation of a duodenal jejunal bypass liner for managing type 2 diabetes
(IPG518) NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of implantation of a duodenal jejunal bypass liner for managing type 2 diabetes
M. Tarnoff Æ L. Rodriguez Æ A. Escalona Æ A. Ramos Æ M. Neto Æ M. Alamo Æ E. Reyes Æ F. Pimentel Æ L. Ibanez
 DOI 10.1007/s00464-008-0125-4 Open label, prospective, randomized controlled trial of an endoscopic duodenal-jejunal bypass sleeve versus low calorie diet for pre-operative weight loss in bariatric surgery
DOI 10.1007/s00464-008-0125-4 Open label, prospective, randomized controlled trial of an endoscopic duodenal-jejunal bypass sleeve versus low calorie diet for pre-operative weight loss in bariatric surgery
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS
 GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Diabetes? Does Metabolic Surgery. Experts disagree about how surgery treats diabetes but agree more research needs to be done.
 Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium jacques.deviere@erasme.ulb.ac.be Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium jacques.deviere@erasme.ulb.ac.be Obesity Affects 300 millions
Understanding Obesity
 Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
Nutrition Management After Bariatric Surgery
 Nutrition Management After Bariatric Surgery Federal Bureau of Prisons Clinical Practice Guidelines October 2013 Clinical guidelines are made available to the public for informational purposes only. The
Nutrition Management After Bariatric Surgery Federal Bureau of Prisons Clinical Practice Guidelines October 2013 Clinical guidelines are made available to the public for informational purposes only. The
HOUSTON METHODIST SURGICAL WEIGHT LOSS
 HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary?
 White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
White Paper: Treating Clinical Obesity: When is Bariatric Surgery or Bariatric Surgery Revision Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Introduction More than one
Bariatric Surgery Guide
 One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of
 Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Bariatric Patients, Nutritional Intervention for
 SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Grupo CHRISTUS MUGUERZA
 Grupo CHRISTUS MUGUERZA Information about: Laparoscopic Adjustable Gastric Banding (Lap Band Surgery) For International Patients Grupo CHRISTUS MUGUERZA / Pág. 1 INDEX About Lap Band Surgery.... 3 Characteristics..
Grupo CHRISTUS MUGUERZA Information about: Laparoscopic Adjustable Gastric Banding (Lap Band Surgery) For International Patients Grupo CHRISTUS MUGUERZA / Pág. 1 INDEX About Lap Band Surgery.... 3 Characteristics..
5. Conversion Procedures that change from an index procedure to a different type of procedure.
 Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Gastric Surgery for Clinically Severe (Morbid) Obesity
 Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
The weight of the world.
 The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
Why a loop and new approach makes sense!
 IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS Prime Surgicare Morbid Obesity and Treatment Options Qualifying for Bariatric Surgery Co-morbid Conditions Coping with Concerns Life After Surgery Morbid Obesity and Treatment
FREQUENTLY ASKED QUESTIONS Prime Surgicare Morbid Obesity and Treatment Options Qualifying for Bariatric Surgery Co-morbid Conditions Coping with Concerns Life After Surgery Morbid Obesity and Treatment
ICD-9-CM/ICD-10-CM Codes for MNT
 / Codes for MNT ICD (International Classification of Diseases) codes are used by physicians and medical coders to assign medical diagnoses to individual patients. It is not within the scope of practice
/ Codes for MNT ICD (International Classification of Diseases) codes are used by physicians and medical coders to assign medical diagnoses to individual patients. It is not within the scope of practice
12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16
 HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
Transmittal 54 Date: APRIL 28, 2006. SUBJECT: Bariatric Surgery for Treatment of Morbid Obesity
 CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 54 Date: APRIL 28, 2006 Change
CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 54 Date: APRIL 28, 2006 Change
Bariatric Surgery: What the Internist Needs to Know
 Bariatric Surgery: What the Internist Needs to Know Richard Stahl, MD, FACS Assistant Professor of Surgery Medical Director of Bariatric Surgery Disclosures None (sadly) Objectives Describe several myths
Bariatric Surgery: What the Internist Needs to Know Richard Stahl, MD, FACS Assistant Professor of Surgery Medical Director of Bariatric Surgery Disclosures None (sadly) Objectives Describe several myths
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
really help your physical, social and emotional wellbeing helping you do more of the things you want and feel more confident and relaxed.
 Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Sudbury Bariatric Regional Assessment & Treatment Centre
 Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
. 2000 : 2.9 million WORLDWIDE deaths. Diabetes Mortality COST 2007 * Types II Diabetes (T2DM) Type II Diabetes Mellitus: medical or surgical disease?
 Type II Diabetes Mellitus: medical or surgical disease? Conference presented at 4-th National Congress of Romanian Association for Endoscopic Surgery, October 30-th, 2008, Iaşi, Romania Gianfranco Silecchia
Type II Diabetes Mellitus: medical or surgical disease? Conference presented at 4-th National Congress of Romanian Association for Endoscopic Surgery, October 30-th, 2008, Iaşi, Romania Gianfranco Silecchia
Emerging Concepts in Bariatric Surgery
 Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Dieting and Gallstones
 Dieting and Gallstones WIN Weight-control Information Network What are Gallstones are clusters of solid material that form in the gallbladder. The most common type is made mostly of cholesterol. Gallstones
Dieting and Gallstones WIN Weight-control Information Network What are Gallstones are clusters of solid material that form in the gallbladder. The most common type is made mostly of cholesterol. Gallstones
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Weight Loss Surgery. Malabsorptive: Your intestines are rearranged to reduce the amount of food absorbed into the system
 The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
Gastric Imbrication: The Future or Fantasy?
 Opinions General Surgery News. Issue: July 2011 Volume 38:7 Gastric Imbrication: The Future or Fantasy? Expert Panel Meets To Discuss Major Questions About New Procedure for Weight Loss by Daniel Cottam,
Opinions General Surgery News. Issue: July 2011 Volume 38:7 Gastric Imbrication: The Future or Fantasy? Expert Panel Meets To Discuss Major Questions About New Procedure for Weight Loss by Daniel Cottam,
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery
 Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Southcoast Center for Weight Loss
 Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Comparison of Nutritional Deficiencies after Rouxen-Y Gastric Bypass and after Biliopancreatic Diversion with Roux-en-Y Gastric Bypass
 Obesity Surgery, 12, 551-558 Comparison of Nutritional Deficiencies after Rouxen-Y Gastric Bypass and after Biliopancreatic Diversion with Roux-en-Y Gastric Bypass George Skroubis, MD 1 ; George Sakellaropoulos,
Obesity Surgery, 12, 551-558 Comparison of Nutritional Deficiencies after Rouxen-Y Gastric Bypass and after Biliopancreatic Diversion with Roux-en-Y Gastric Bypass George Skroubis, MD 1 ; George Sakellaropoulos,
Weight Loss Surgery: Pre- and Post-Operative Care
 Weight Loss Surgery: Pre- and Post-Operative Care Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine Daniel.Bessesen@ucdenver.edu
Weight Loss Surgery: Pre- and Post-Operative Care Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine Daniel.Bessesen@ucdenver.edu
Patient Information Guide for the ReShape Procedure
 Patient Information Guide for the ReShape Procedure Please review this information before your procedure. Please talk to your doctor if you have any questions or do not understand any of this information.
Patient Information Guide for the ReShape Procedure Please review this information before your procedure. Please talk to your doctor if you have any questions or do not understand any of this information.
Roux-en-Y Gastric Bypass
 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
What is the Sleeve Gastrectomy?
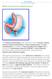 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Endoluminal and Laparoscopic Bariatric & Metabolic Surgery Advanced Course
 Endoluminal and Laparoscopic Bariatric & Metabolic Surgery Advanced Course Directors of the course: Jacques MARESCAUX Michel VIX Manoel GALVAO NETO Silvana PERRETTA France France Brazil Italy Faculty:
Endoluminal and Laparoscopic Bariatric & Metabolic Surgery Advanced Course Directors of the course: Jacques MARESCAUX Michel VIX Manoel GALVAO NETO Silvana PERRETTA France France Brazil Italy Faculty:
When, Why, and How to Revise a Failed Sleeve Gastrectomy
 When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Endoluminal Bariatric Revision. Todd David Wilson, MD
 Endoluminal Bariatric Revision Todd David Wilson, MD Surgical Endoscopy and the Bariatric Surgeon Preoperative Endoscopy Postoperative Endoscopy Revisional Endoscopy Primary Endoluminal Bariatrics Preoperative
Endoluminal Bariatric Revision Todd David Wilson, MD Surgical Endoscopy and the Bariatric Surgeon Preoperative Endoscopy Postoperative Endoscopy Revisional Endoscopy Primary Endoluminal Bariatrics Preoperative
2013 RN.ORG, S.A., RN.ORG, LLC
 Obesity: Bariatric Surgical Options WWW.RN.ORG Reviewed September, 2013, Expires September, 2015 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2013 RN.ORG,
Obesity: Bariatric Surgical Options WWW.RN.ORG Reviewed September, 2013, Expires September, 2015 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2013 RN.ORG,
Surgical Associates of Ithaca Guide to Weight-loss Surgery
 Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
Laparoscopic Adjustable Gastric Banding as a Type of Weight Loss
 Laparoscopic Adjustable Gastric Banding as a Type of Weight Loss Abstract Obesity has become a global health crisis. Traditional treatments try to modify behavior in regard to diet and exercise. Laparoscopic
Laparoscopic Adjustable Gastric Banding as a Type of Weight Loss Abstract Obesity has become a global health crisis. Traditional treatments try to modify behavior in regard to diet and exercise. Laparoscopic
Bariatric Surgery. Beth A. Ryder, MD FACS. Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University
 Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Weight Loss Surgery. Our Surgeons. A Patient s Guide
 Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Endoscopic Management of Strictures and Leaks. Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center
 Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Chapter 6 Gastrointestinal Impairment
 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
BARIATRIC SURGERY. Prerequisites. Authorization, Notification and Referral
 BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
Subject: Weight Loss Surgery Policy. Effective Date: 1/00 Revision Date: 10/15
 Subject: Weight Loss Surgery Policy Effective Date: 1/00 Revision Date: 10/15 DESCRIPTION OSU Health Plans supports covered members with a spectrum of service for obesity and weight loss attempts. The
Subject: Weight Loss Surgery Policy Effective Date: 1/00 Revision Date: 10/15 DESCRIPTION OSU Health Plans supports covered members with a spectrum of service for obesity and weight loss attempts. The
Metabolic and Bariatric Surgery Center
 Metabolic and Bariatric Surgery Center www.bannerhealth.com/universitytucsonsurgicalweightloss 1 Welcome to Banner University Medical Center s Metabolic and Bariatric Surgery Center Thank you for choosing
Metabolic and Bariatric Surgery Center www.bannerhealth.com/universitytucsonsurgicalweightloss 1 Welcome to Banner University Medical Center s Metabolic and Bariatric Surgery Center Thank you for choosing
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS. Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence
 PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
Weight Loss Surgery A Patient s Guide
 Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Scott A. Shikora, MD, FACS. Sleeve Gastrectomy. Sleeve Gastrectomy. Sleeve Gastrectomy 11/8/2013
 DISCLOSURE Scott A. Shikora, MD, FACS Scott A. Shikora, MD, FACS Associate Professor of Surgery Harvard Medical School Director, Center for Metabolic and Bariatric Surgery Brigham and Women s Hospital
DISCLOSURE Scott A. Shikora, MD, FACS Scott A. Shikora, MD, FACS Associate Professor of Surgery Harvard Medical School Director, Center for Metabolic and Bariatric Surgery Brigham and Women s Hospital
BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY)
 BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY) WHAT IS OBESITY? Obesity is the condition whereby the individual sustains the body weight that is significantly higher than ideal body weight for
BARIATRIC SURGERY (SURGERY FOR THE TREATMENT OF OBESITY) WHAT IS OBESITY? Obesity is the condition whereby the individual sustains the body weight that is significantly higher than ideal body weight for
Bariatric Surgery Guide Dr. Stewart s Weight Loss Specialists of North Texas
 Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
BARIATRIC SURGERY. Personalized Weight Loss Program
 BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types:
 INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
Metabolic & Bariatric Surgery
 Metabolic & Bariatric Surgery Are you...tired of struggling with your weight? aware those extra pounds are putting your health at risk? ready to start a new path to take charge of your life again? If so,
Metabolic & Bariatric Surgery Are you...tired of struggling with your weight? aware those extra pounds are putting your health at risk? ready to start a new path to take charge of your life again? If so,
