Corneal Collagen Cross-Linking for Ectasia after LASIK and Photorefractive Keratectomy
|
|
|
- Madeleine Jenkins
- 8 years ago
- Views:
Transcription
1 Corneal Collagen Cross-Linking for Ectasia after LASIK and Photorefractive Keratectomy Long-Term Results Olivier Richoz, MD, 1 Nikolaos Mavrakanas, MD, 1 Bojan Pajic, MD, PhD, 1 Farhad Hafezi, MD, PhD 1,2 Purpose: To report the long-term results of corneal collagen cross-linking (CXL) in ectasia after LASIK and photorefractive keratectomy (PRK). Design: Retrospective, interventional cases series. Participants: Twenty-six eyes of 26 patients (18 male, 8 female) with postoperative ectasia after LASIK (23 eyes) and PRK (3 eyes) were included with a mean age of 35 9 years at the time of treatment and a mean follow-up of 25 months (range, months). Methods: All consecutive patients treated with CXL for progressive ectasia after LASIK or PRK at the Institute for Refractive and Ophthalmic Surgery, Zurich, Switzerland between 2004 and 2010 were included. Main Outcome Measures: Corrected distance visual acuity (CDVA), maximum keratometry readings (K max ), minimum radius of curvature (R min ), and 6 corneal topography indices were assessed in this study. Results: Mean CDVA before CXL was 0.5 logarithm of the minimum angle of resolution (logmar) units, which improved to a mean of 0.3 logmar units (P 0.001). Corrected distance visual acuity improved 1 line or more in 19 cases and remained unchanged in 7 patients. Mean K max after CXL of diopters (D) was significantly lower (P 0.001) than mean pre-cxl K max of D. The R min after CXL was increased significantly (P 0.006), whereas the index of surface variance (P 0.03), the index of vertical asymmetry (P 0.04), the keratoconus index (P 0.03), and the central keratoconus index (P 0.016) were reduced significantly. Conclusions: Ectasia after LASIK and PRK was arrested by CXL with stabilization or improvement of CDVA and K max after a mean follow-up of 25 months. There were improvements in 4 topography indices, suggesting a more regular corneal surface. Financial Disclosure(s): The author(s) have no proprietary or commercial interest in any materials discussed in this article. Ophthalmology 2013;120: by the American Academy of Ophthalmology. Iatrogenic ectasia after refractive laser surgery, a progressive stromal thinning and steepening of the cornea resulting in refractive aberrations and visual loss, increasingly has been reported since its first description by Seiler et al 1 in All excimer laser procedures remove corneal tissue, weakening corneal biomechanics. Iatrogenic keratectasia is a sightthreatening complication after LASIK, occurring in 0.1 % of cases, 2,3 and is less frequent after photorefractive keratectomy (PRK). 4 The major risk factors for ectasia after refractive laser surgery are deep ablation, residual stromal thickness of less than 250 m, 5 retreatments, and pre-existing abnormal corneal topography such as forme fruste keratoconus and pellucid marginal degeneration. 2,6 Corneal collagen cross-linking (CXL) has emerged as an effective technique to delay or arrest progression of keratoconus 7 9 and postoperative ectasia Corneal collagen crosslinking increases the stromal biomechanical stability by creating additional chemical bonds using ultraviolet A light and riboflavin as photomediator. 14 These biomechanical changes can be detected either directly 15 or via changes in corneal topography. 16 Corneal collagen cross-linking also improves stromal collagen resistance to endogenous protease, 17 a proposed cause of ectasia. 18 Before CXL emerged, treatment options for iatrogenic ectasia were limited to intracorneal ring segments to try to stabilize the cornea mechanically and to lamellar or penetrating keratoplasty. 22 Hafezi et al 10 investigated the effect of CXL on iatrogenic keratectasia and observed an improvement in corrected distance visual acuity (CDVA) in 9 of 10 cases, improved keratometric readings in 5 of 10 cases, and reduction in cylinder in all patients. Salgado et al 13 similarly showed regression of corneal ectasia and improvement of spherical equivalent with a 6-month follow-up. Recently, Hersh et al 11 reported 1-year outcomes of a prospective, randomized clinical trial on CXL in both keratoconus and ectasia patients, showing significant improvement in CDVA and reduced maximum keratometric values; however, the CXL results were less notable in ectasia patients. The results of these studies, evaluating the efficacy, stability, and safety of corneal CXL for ectasia, are limited by short follow-up. The study evaluated the effect of CXL in the treatment of ectasia after LASIK and PRK with a follow-up period of up to 62 months (mean, 25 months). Patients and Methods This was a retrospective study of all consecutive patients treated with CXL for progressive ectasia after LASIK or PRK at the Institute for Refractive and Ophthalmic Surgery, Zurich, Switzer by the American Academy of Ophthalmology ISSN /13/$ see front matter Published by Elsevier Inc.
2 Richoz et al Corneal Collagen CXL for Ectasia after LASIK and PRK land, between 2004 and The study was approved by the local institutional review board and adhered to the tenets of the Declaration of Helsinki. All patients provided written informed consent. Ectasia was defined as topographic steepening of 5 diopters (D) or more compared with immediate postoperative appearance, loss of 2 lines or more of Snellen acuity, and a change in manifest refraction of2dormore of either sphere or cylinder. 6 Progression was defined by an increase of maximum keratometry readings (K max ) of the anterior corneal surface, at 3.0 mm from the apex, of at least 1.0 D in corneal topographies over a maximum of 12 months. Central corneal thickness (CCT) by optical and ultrasonic pachymetry was at least 300 ìm, with the exception of 1 patient with CCT of 297 ìm. None of the patients had a history of corneal surgery, chemical injury, or delayed epithelial healing or was pregnant or lactating during the treatment. The main outcome measures were: CDVA, K max, minimum radius of curvature, and 6 quantitative descriptors of corneal topography (Pentacam topography; Oculus Instruments, Wetzlar, Germany), including index of surface variance, index of vertical asymmetry, keratoconus index, central keratoconus index, center keratoconus index, index of height asymmetry, and index of height decentration. Corneal Collagen Cross-Linking Surgical Technique Corneal collagen cross-linking was performed using the standard protocol 10 except for 8 patients with CCT thinner than 400 m, in whom hypo-osmolar riboflavin solution was used before surgery. 23 After topical anesthesia with tetracaine 1% and oxybuprocaine 0.4%, the central 8.0 mm of corneal epithelium were debrided using a hockey knife. Riboflavin solution (0.1% solution 10 mg riboflavin-5-phosphate in 10 ml dextran-t % solution) was instilled every 3 minutes for 30 minutes for complete stromal penetration, confirmed by green aqueous fluorescence with blue light slit-lamp biomicroscopy. Ultraviolet A irradiation then was applied using UV-X (Peschke Meditrade, Cham, Switzerland). Before treatment, the intended 3-mW/cm 2 surface irradiance (5.4 J/cm 2 surface dose after 30 minutes) was calibrated using an ultraviolet A meter (LaserMate-Q, LASER 2000; Coherent Inc, Santa Clara, CA) at a working distance of 10 cm. During treatment, riboflavin solution was applied every 5 minutes; tetracaine 1% and oxybuprocaine 0.4% drops were given if necessary. At the end of the procedure, ofloxacin ointment (Floxal; Bausch & Lomb, Madison, NJ) was applied every 2 hours and at night until full corneal re-epithelialization occurred. Then, fluorometholone 0.1% drops (FML Liquifilm; Allergan Inc., Irvine, CA) were administered twice daily for 6 weeks. Examination Preoperative and postoperative examinations included CDVA, slitlamp evaluation, Goldmann applanation tonometry, corneal topography, and minimal and central corneal thickness by Scheimpflug imaging (Pentacam; Oculus Instruments, Wetzlar, Germany), ultrasonic pachymetry (Tomey Corporation, Nahoya, Japan). Visual acuity was recorded and analyzed as the logarithm of the minimum angle of resolution (logmar) value. Scheimpflug imaging was not available at the beginning of the study, but was performed in the last 18 of 26 cases. The K max reading was performed in all cases using corneal topography. Because of high intraindividual variation associated with K max, 3 keratometry readings were performed and the highest of the 3 was chosen. For ultrasound pachymetry, the thinnest measurement was chosen, with each single measurement representing the mean of 5 consecutive measurements. Statistical Analysis Statistical analysis was performed using PASW Statistics software version 18 (SPSS, Inc, Chicago, IL). A paired 2-tailed Student t test was performed to analyze the postoperative outcome changes compared with baseline values. A P value less than 0.05 was used to determine statistical significance. The Wilcoxon test was used for keratoconus index and index of height asymmetry. Results Twenty-six eyes of 26 patients (18 male, 8 female) with progressive ectasia after LASIK (23 eyes) and PRK (3 eyes) were included. The mean standard deviation (SD) patient age at CXL treatment was 35 9 years (range, years). Twenty-five of 26 eyes had a central CCT by optical and ultrasonic pachymetry of at least 300 m; 1 eye had a CCT of 297 m. Fifteen patients (58%) had undiagnosed keratoconus, 3 patients (12%) had undiagnosed pellucid marginal degeneration, and 3 patients (12%) had a deep stromal ablation. In 4 cases (15%), the cause of the ectasia was not clear. Mean SD follow-up was months (range, months). Mean SD CDVA was logmar before CXL (range, ) and improved to logmar (range, logmar) after treatment. Total mean SD CDVA improved to logmar (P 0.001). Corrected distance visual acuity improved (gain of 1 line) in 19 cases and remained stable in 7 patients. No patient showed deterioration (lost 1 line). Mean SD K max after CXL of diopters (D) (range, D) was significantly lower (P 0.001) than mean K max before CXL ( D; range, D). Mean SD K max improvement was D (range, 0.6 to 7.7 D). There was no significant correlation between K max and CDVA before (r 0.12, P 0.53) or after (r 0.1, P 0.6) treatment. In 19 patients, K max improved (more than 1 D improvement) and in 7 patients was stable (less than 1-D change). In the 4 cases with followup longer than 3 years, both K max and CDVA remained stable. Mean SD CCT was 9 17 m thinner (range, 27 to 32 m) after CXL (P 0.007). The 3 cases of ectasia occurring after PRK all showed forme fruste keratoconus before surgery and the following characteristics after CXL: mean preoperative K max improved from 50.1 D to 49.7 D. Corrected distance visual acuity remained stable in 2 patients and improved by 0.03 logmar for the third patient. Statistical comparisons between the groups of LASIK and PRK patients are limited by the small number of the latter. The minimum radius of curvature was increased significantly after CXL. The index of surface variance, the index of vertical asymmetry, the keratoconus index, and the central keratoconus index were reduced significantly. There was no significant change in the index of height asymmetry or index of height decentration. The results and P values are summarized in Table 1. Figures 1 and 2 show preoperative and postoperative topographies and their difference maps. No serious complications were reported during the follow-up period. A corneal demarcation line was observed at a depth of approximately 250 to 300 m in all cases undergoing CXL after 2005, when the initial observation on the existence of such a line was submitted. 24 A haze was visible in the anterior stroma, up to 80% of thickness, in all eyes, but disappeared within 12 months after CXL. One case with preoperative CCT by ultrasonic pachymetry of 400 m had endothelial irregularity and endothelial opacities at presentation that cleared within 12 months after CXL with a stable endothelial cell count of 2350 cells/mm. The patient showing a preoperative thickness of 297 m was treated using 1355
3 Ophthalmology Volume 120, Number 7, July 2013 Table 1. Results and P Values of Minimum Radius of Curvature and 6 Corneal Topography Indices Before Corneal Collagen Cross-Linking After Corneal Collagen Cross-Linking Change Standard Deviation P Value KI * IHA ISV * IVA * CKI * IHD R min * CKI central keratoconus index; IHA index of height asymmetry; IHD index of height decentration; ISV index of surface variance; IVA index of vertical asymmetry; KI keratoconus index; R min minimum radius of curvature. *Statistically significant. hypo-osmolar riboflavin solution and showed no signs of endothelial damage. Discussion This study of CXL for ectasia after refractive surgery, with 23 cases occurring after LASIK and 3 cases occurring after PRK, offers a longer follow-up (mean, 25 months; maximum, 62 months) when compared with the existing literature. Results of CXL for PRK-induced ectasia have not been published previously. This study found an improvement in CDVA in 19 of 26 patients after CXL, with a mean improvement of 0.2 log- MAR. In a previous report, an improvement in CDVA was shown in 9 of 10 patients after CXL, but a recent report by Hersh et al 11 showed only a 0.07-logMAR increase in CDVA at 1 year after CXL. Corneal collagen cross-linking has been proven very effective in halting the progression of keratoconus and iatrogenic ectasia, but visual recovery, Figure 1. Topographies obtained (Top left) before and (Top middle, Bottom left, and Bottom middle) after corneal collagen cross-linking (CXL) showing regression of maximum keratometry reading (K max ) over 3 years. The difference map visualizes the regression over more than 5 diopters. OD right eye. 1356
4 Richoz et al Corneal Collagen CXL for Ectasia after LASIK and PRK Figure 2. Topographies obtained before and after corneal collagen cross-linking (CXL) in a patient with bilateral iatrogenic ectasia and their respective difference maps for (Top row) the right eye (OD) and (Bottom row) the left eye (OS). N nasal; T temporal. although statistically significant, usually is modest. 11,25,26 It also seems that the visual outcome in patients with iatrogenic ectasia has been inferior compared with that of keratoconus patients after CXL. 11 Mean K max was significantly lower at 50.9 D (P 0.001) when compared with mean K max before CXL of 52.8 D. In 19 eyes, K max improved by more than 1 D, and in 7 eyes, it was stable. This is consistent with a previous report of 10 ectasia patients treated with CXL that showed a K max reduction from 54.5 D to 52.6 D. However, another report of 22 eyes with ectasia that had undergone LASIK showed no significant difference in K max before or after treatment (1.00 D decrease in K max ; P 0.08). Vinciguerra et al 27 also reported no significant topographic changes (average keratometry, flat keratometry, or steep keratometry) in patients with iatrogenic keratectasia. Those results suggest that ectatic corneas may have a less robust response to CXL as opposed to keratoconic corneas. Although the cause for this potential difference in not clear, several explanations have been suggested. One is that CXL preferentially strengthens the anterior stroma, including the LASIK flap, which does not contribute to the mechanical stability of the cornea. The riboflavin diffusion may be reduced in corneas that have undergone LASIK, affecting the CXL result. Differences in the pathophysiologic features of keratoconus and ectasia occurring after refractive surgery also may account for a less pronounced CXL effect. 11,28 Corneal topography indices are elevated in ectasia patients with the exception of the minimum radius of curvature, the inverse of corneal steepness, and therefore are expected to decrease. A decrease in corneal indices after CXL may indicate improvement of the corneal irregularities. In 18 of 26 eyes for which Scheimpflug imaging was available, the results showed a statistically significant increase in the minimum radius of curvature and statistically significant decreases in the index of surface variance, the index of vertical asymmetry, the keratoconus index, and the central keratoconus index after CXL therapy. There were no significant changes in the index of height asymmetry or index of height decentration. The increase in the minimum radius of curvature in the present study is consistent with decreases in K max after CXL in many studies. 8,26,27,29 31 Decreases in the index of surface variance indicate a decrease in the curvature variation compared with the mean curvature of the cornea, and decreases in the index of vertical asymmetry suggest a reduction of the difference between the superior and inferior corneal curvature. The decrease of this index may correspond to a decrease of the inferior-to-superior ratio The significant improvement in the keratoconus and central 1357
5 Ophthalmology Volume 120, Number 7, July 2013 keratoconus indices reflect the reduction of the corneal steepening after CXL. Improvement in those parameters may explain the visual recovery and reverse of refractive aberrations in some ectasia patients. Previous studies from Koller et al 16 and Greenstein et al 29 showed similar results. Koller et al found significant improvement in 4 of 7 Pentacam topography indices (central keratoconus index, keratoconus index, index of height asymmetry, and minimum radius of curvature) 1 year after CXL. Greenstein et al 29 found changes in the index of surface variance, index of vertical asymmetry, keratoconus index, and minimum radius of curvature at 1 year after CXL, but the results were significant only in the subgroup of keratoconus patients, and not in the ectasia patients. No serious complications were reported during the follow-up period, apart from an early corneal haze, which disappeared within 12 months after CXL, and a patient with an endothelial irregularity and preoperative CCT of 400 m, which cleared after 12 months with a normal endothelial cell count. The direct irradiation by ultraviolet A light normally is limited to the anterior 300 m of corneal stroma, protecting the endothelium, iris, and lens. 35 No permanent haze, stromal scars, sterile infiltrates, corneal edema, lamellar keratitis, infectious or herpetic keratitis, or iritis were described. The overall risk of corneal infection with CXL is low, possibly because of a bactericidal effect and an antibiotic prophylaxis occurring after CXL. 36 In conclusion, CXL arrested the progression of ectasia occurring after LASIK and PRK and improved the CDVA and K max, with a mean follow-up of 25 months. There were improvements in 4 topography indices, suggesting a more regular corneal surface. In the light of these results and the absence of major complications, but also in the absence of other minimally invasive therapeutic options, the use of CXL in iatrogenic ectasia is recommended without restrictions. References 1. Seiler T, Koufala K, Richter G. Iatrogenic keratectasia after laser in situ keratomileusis. J Refract Surg 1998;14: Binder PS. Ectasia after laser in situ keratomileusis. J Cataract Refract Surg 2003;29: Pallikaris IG, Kymionis GD, Astyrakakis NI. Corneal ectasia induced by laser in situ keratomileusis. J Cataract Refract Surg 2001;27: Hamilton DR, Johnson RD, Lee N, Bourla N. Differences in the corneal biomechanical effects of surface ablation compared with laser in situ keratomileusis using a microkeratome or femtosecond laser. J Cataract Refract Surg 2008;34: Kim TH, Lee D, Lee HI. The safety of 250 microm residual stromal bed in preventing keratectasia after laser in situ keratomileusis (LASIK). J Korean Med Sci 2007;22: Randleman JB, Russell B, Ward MA, et al. Risk factors and prognosis for corneal ectasia after LASIK. Ophthalmology 2003;110: Coskunseven E, Jankov MR II, Hafezi F. Contralateral eye study of corneal collagen cross-linking with riboflavin and UVA irradiation in patients with keratoconus. J Refract Surg 2009;25: Raiskup-Wolf F, Hoyer A, Spoerl E, Pillunat LE. Collagen crosslinking with riboflavin and ultraviolet-a light in keratoconus: long-term results. J Cataract Refract Surg 2008; 34: Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-Ainduced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol 2003;135: Hafezi F, Kanellopoulos J, Wiltfang R, Seiler T. Corneal collagen crosslinking with riboflavin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis. J Cataract Refract Surg 2007;33: Hersh PS, Greenstein SA, Fry KL. Corneal collagen crosslinking for keratoconus and corneal ectasia: one-year results. J Cataract Refract Surg 2011;37: Kohlhaas M, Spoerl E, Speck A, et al. A new treatment of keratectasia after LASIK by using collagen with riboflavin/ UVA light cross-linking [in German]. Klin Monatsbl Augenheilkd 2005;222: Salgado JP, Khoramnia R, Lohmann CP, Winkler von Mohrenfels C. Corneal collagen crosslinking in post-lasik keratectasia. Br J Ophthalmol 2011;95: Spoerl E, Seiler T. Techniques for stiffening the cornea. J Refract Surg 1999;15: Vinciguerra P, Albe E, Mahmoud AM, et al. Intra- and postoperative variation in ocular response analyzer parameters in keratoconic eyes after corneal cross-linking. J Refract Surg 2010;26: Koller T, Iseli HP, Hafezi F, et al. Scheimpflug imaging of corneas after collagen cross-linking. Cornea 2009;28: Spoerl E, Wollensak G, Seiler T. Increased resistance of crosslinked cornea against enzymatic digestion. Curr Eye Res 2004;29: Balasubramanian SA, Pye DC, Willcox MD. Are proteinases the reason for keratoconus? Curr Eye Res 2010;35: Kymionis GD, Siganos CS, Kounis G, et al. Management of post-lasik corneal ectasia with Intacs inserts: one-year results. Arch Ophthalmol 2003;121: Siganos CS, Kymionis GD, Astyrakakis N, Pallikaris IG. Management of corneal ectasia after laser in situ keratomileusis with INTACS. J Refract Surg 2002;18: Lovisolo CF, Fleming JF. Intracorneal ring segments for iatrogenic keratectasia after laser in situ keratomileusis or photorefractive keratectomy. J Refract Surg 2002;18: Seitz B, Rozsival P, Feuermannova A, et al. Penetrating keratoplasty for iatrogenic keratoconus after repeat myopic laser in situ keratomileusis: histologic findings and literature review. J Cataract Refract Surg 2003;29: Hafezi F, Mrochen M, Iseli HP, Seiler T. Collagen crosslinking with ultraviolet-a and hypoosmolar riboflavin solution in thin corneas. J Cataract Refract Surg 2009;35: Seiler T, Hafezi F. Corneal cross-linking-induced stromal demarcation line. Cornea 2006;25: Asri D, Touboul D, Fournie P, et al. Corneal collagen crosslinking in progressive keratoconus: multicenter results from the French National Reference Center for Keratoconus. J Cataract Refract Surg 2011;37: Caporossi A, Mazzotta C, Baiocchi S, Caporossi T. Longterm results of riboflavin ultraviolet A corneal collagen crosslinking for keratoconus in Italy: the Siena Eye Cross Study. Am J Ophthalmol 2010;149: Vinciguerra P, Camesasca FI, Albe E, Trazza S. Corneal collagen cross-linking for ectasia after excimer laser refractive surgery: 1-year results. J Refract Surg 2010;26: Cheema AS, Mozayan A, Channa P. Corneal collagen crosslinking in refractive surgery. Curr Opin Ophthalmol 2012;23: Greenstein SA, Fry KL, Hersh PS. Corneal topography indices after corneal collagen crosslinking for keratoconus and cor- 1358
6 Richoz et al Corneal Collagen CXL for Ectasia after LASIK and PRK neal ectasia: one-year results. J Cataract Refract Surg 2011; 37: Grewal DS, Brar GS, Jain R, et al. Corneal collagen crosslinking using riboflavin and ultraviolet-a light for keratoconus: one-year analysis using Scheimpflug imaging. J Cataract Refract Surg 2009;35: Vinciguerra P, Albe E, Trazza S, et al. Refractive, topographic, tomographic, and aberrometric analysis of keratoconic eyes undergoing corneal cross-linking. Ophthalmology 2009;116: Rabinowitz YS. Videokeratographic indices to aid in screening for keratoconus. J Refract Surg 1995;11: Jafri B, Li X, Yang H, Rabinowitz YS. Higher order wavefront aberrations and topography in early and suspected keratoconus. J Refract Surg 2007;23: Li X, Yang H, Rabinowitz YS. Keratoconus: classification scheme based on videokeratography and clinical signs. J Cataract Refract Surg 2009;35: Spoerl E, Mrochen M, Sliney D, et al. Safety of UVAriboflavin cross-linking of the cornea. Cornea 2007;26: Moren H, Malmsjo M, Mortensen J, Ohrstrom A. Riboflavin and ultraviolet A collagen crosslinking of the cornea for the treatment of keratitis. Cornea 2010;29: Footnotes and Financial Disclosures Originally received: July 9, Final revision: November 8, Accepted: December 13, Available online: April 10, Manuscript no Division of Ophthalmology, Department of Clinical Neurosciences, Geneva University Hospitals, Geneva, Switzerland. 2 Doheny Eye Institute, Keck School of Medicine, University of Southern California, Los Angeles, California. Financial Disclosure(s): The author(s) have no proprietary or commercial interest in any materials discussed in this article. Correspondence: Farhad Hafezi, MD, PhD, Department of Ophthalmology, Geneva University Hospitals, Rue Alcide Jentzer 22, 1211 Geneva, Switzerland. farhad.hafezi@hcuge.ch 1359
Journal of American Science 2014;10(8) http://www.jofamericanscience.org
 Management of Early Post LASIK Ectasia by using Corneal Collagen Cross-Linking Abdalla M. Elamin MD. Ophthalmology Department, Faculty of Medicine, Al Azhar University, Cairo, Egypt Abstract: Purpose:
Management of Early Post LASIK Ectasia by using Corneal Collagen Cross-Linking Abdalla M. Elamin MD. Ophthalmology Department, Faculty of Medicine, Al Azhar University, Cairo, Egypt Abstract: Purpose:
Corneal collagen crosslinking with riboflavin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis
 ARTICLE Corneal collagen crosslinking with riboflavin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis Farhad Hafezi, MD, John Kanellopoulos, MD, Rainer Wiltfang, MD,
ARTICLE Corneal collagen crosslinking with riboflavin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis Farhad Hafezi, MD, John Kanellopoulos, MD, Rainer Wiltfang, MD,
Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking
 Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking Kay Lam, MD, Dan B. Rootman, MSc, Alejandro Lichtinger, and David S. Rootman, MD, FRCSC Author affiliations:
Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking Kay Lam, MD, Dan B. Rootman, MSc, Alejandro Lichtinger, and David S. Rootman, MD, FRCSC Author affiliations:
Corneal topography indices after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results
 ARTICLE Corneal topography indices after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Kristen L. Fry, OD, MS, Peter S. Hersh, MD PURPOSE:
ARTICLE Corneal topography indices after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Kristen L. Fry, OD, MS, Peter S. Hersh, MD PURPOSE:
Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus
 Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus George D. Kymionis, MD, PhD; Georgios A. Kontadakis, MD, MSc; George A. Kounis, PhD; Dimitra M. Portaliou,
Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus George D. Kymionis, MD, PhD; Georgios A. Kontadakis, MD, MSc; George A. Kounis, PhD; Dimitra M. Portaliou,
(Mazzotta et al, 2007) Human corneal rigidity increases 329 % (Wollensak, 2006)
 Simultaneous PRK and CXL Corneal Crosslinking (CXL): UV-A light, 365 nm, causes riboflavin, 0.1 %, to release oxygen radicals which create new cross-linking bonds between collagen lameller fibres and within
Simultaneous PRK and CXL Corneal Crosslinking (CXL): UV-A light, 365 nm, causes riboflavin, 0.1 %, to release oxygen radicals which create new cross-linking bonds between collagen lameller fibres and within
CXL With the Epithelium on or off: Which Is Better?
 CXL With the Epithelium on or off: Which Is Better? Transepithelial CXL Is Gaining Ground By Roy S. Rubinfeld, MD, and the CXL-USA Study Group At its simplest, corneal collagen cross-linking (CXL) is a
CXL With the Epithelium on or off: Which Is Better? Transepithelial CXL Is Gaining Ground By Roy S. Rubinfeld, MD, and the CXL-USA Study Group At its simplest, corneal collagen cross-linking (CXL) is a
Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation
 Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation Mohammad Naser Hashemian, MD 1 Mahdi AliZadeh, MD 2 Hassan Hashemi, MD 1,3 Firoozeh Rahimi, MD 4 Abstract Purpose: To present
Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation Mohammad Naser Hashemian, MD 1 Mahdi AliZadeh, MD 2 Hassan Hashemi, MD 1,3 Firoozeh Rahimi, MD 4 Abstract Purpose: To present
Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus
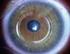 SURGICAL TECHNIQUE Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus Waleed Al-Tuwairqi, MD; Mazen M. Sinjab, MD,
SURGICAL TECHNIQUE Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus Waleed Al-Tuwairqi, MD; Mazen M. Sinjab, MD,
Transepithelial Crosslinking vs. Corneal Pocket Crosslinking. Christoph Kranemann MD Anna Yu OD
 Transepithelial Crosslinking vs. Corneal Pocket Crosslinking Christoph Kranemann MD Anna Yu OD Rome 2013 We have no financial interests in this presentation. Corneal collagen cross linking Creates new
Transepithelial Crosslinking vs. Corneal Pocket Crosslinking Christoph Kranemann MD Anna Yu OD Rome 2013 We have no financial interests in this presentation. Corneal collagen cross linking Creates new
How To Test For Cxl
 ARTICLE Complication and failure rates after corneal crosslinking Tobias Koller, MD, Michael Mrochen, PhD, Theo Seiler, MD, PhD PURPOSE: To evaluate the complication rate of corneal crosslinking (CXL)
ARTICLE Complication and failure rates after corneal crosslinking Tobias Koller, MD, Michael Mrochen, PhD, Theo Seiler, MD, PhD PURPOSE: To evaluate the complication rate of corneal crosslinking (CXL)
Surgical Advances in Keratoconus. Keratoconus. Innovations in Ophthalmology. New Surgical Advances. Diagnosis of Keratoconus. Scheimpflug imaging
 Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
Keratoconus. Progressive bilateral ectasia. Onset puberty. Prevalence 1:2000. 20% progress to transplantation. Pathogenesis unclear
 Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Validation of a New Scoring System for the Detection of Early Forme of Keratoconus
 10.5005/jp-journals-10025-1019 Alain Saad, Damien Gatinel ORIGINAL ARTICLE Validation of a New Scoring System for the Detection of Early Forme of Keratoconus Alain Saad, Damien Gatinel ABSTRACT Purpose:
10.5005/jp-journals-10025-1019 Alain Saad, Damien Gatinel ORIGINAL ARTICLE Validation of a New Scoring System for the Detection of Early Forme of Keratoconus Alain Saad, Damien Gatinel ABSTRACT Purpose:
Ectasia after laser in-situ keratomileusis (LASIK)
 Ectasia after laser in-situ keratomileusis (LASIK) 長 庚 紀 念 醫 院 眼 科 蕭 靜 熹 Post-LASIK ectasia A rare complication of LASIK Manhattan jury awarded a former investment banker a record $7.25 million for post-lasik
Ectasia after laser in-situ keratomileusis (LASIK) 長 庚 紀 念 醫 院 眼 科 蕭 靜 熹 Post-LASIK ectasia A rare complication of LASIK Manhattan jury awarded a former investment banker a record $7.25 million for post-lasik
Elsevier Editorial System(tm) for Journal of Cataract & Refractive Surgery Manuscript Draft
 Elsevier Editorial System(tm) for Journal of Cataract & Refractive Surgery Manuscript Draft Manuscript Number: Title: Keratoconus exacerbation after cross-linking and surface ablation - a case report Article
Elsevier Editorial System(tm) for Journal of Cataract & Refractive Surgery Manuscript Draft Manuscript Number: Title: Keratoconus exacerbation after cross-linking and surface ablation - a case report Article
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus
 Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
KERATOCONUS IS A BILATERAL, ASYMMETRIC, CHRONIC,
 Comparison of and Intacs for Keratoconus and Post-LASIK Ectasia MUNISH SHARMA, MD, AND BRIAN S. BOXER WACHLER, MD PURPOSE: To evaluate the efficacy of single-segment Intacs and compare with double-segment
Comparison of and Intacs for Keratoconus and Post-LASIK Ectasia MUNISH SHARMA, MD, AND BRIAN S. BOXER WACHLER, MD PURPOSE: To evaluate the efficacy of single-segment Intacs and compare with double-segment
ORIGINAL ARTICLES. Anastasios John Kanellopoulos, MD; Perry S. Binder, MS, MD
 ORIGINAL ARTICLES Management of Corneal Ectasia After LASIK With Combined, Same-day, Topographyguided Partial Transepithelial PRK and Collagen Cross-linking: The Athens Protocol Anastasios John Kanellopoulos,
ORIGINAL ARTICLES Management of Corneal Ectasia After LASIK With Combined, Same-day, Topographyguided Partial Transepithelial PRK and Collagen Cross-linking: The Athens Protocol Anastasios John Kanellopoulos,
Diego Fernando Suárez Sierra, MD Fellow Cornea and Refractive Surgery Fellow Lens and Ocular Surface Vejarano Laser Vision Center
 Corneal crosslinking with riboflavin and ultraviolet light before or after subepithelial keratectomy laser-assisted (LASEK) in patients with thin corneas. Diego Fernando Suárez Sierra, MD Fellow Cornea
Corneal crosslinking with riboflavin and ultraviolet light before or after subepithelial keratectomy laser-assisted (LASEK) in patients with thin corneas. Diego Fernando Suárez Sierra, MD Fellow Cornea
Short and long term complications of combined. Protocol) in 412 keratoconus eyes (2 7 years follow up)
 Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results
 ARTICLE Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Vinnie P. Shah, MD, Kristen L. Fry, OD, MS, Peter S.
ARTICLE Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Vinnie P. Shah, MD, Kristen L. Fry, OD, MS, Peter S.
Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus.
 Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus. Mahmoud M Saleh, Ahmed I Galhoom, Mohamed A El-Malah, Abdelgany Ib Abdelgany Department
Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus. Mahmoud M Saleh, Ahmed I Galhoom, Mohamed A El-Malah, Abdelgany Ib Abdelgany Department
BY A. JOHN KANELLOPOULOS, MD
 Sequential Versus Simultaneous CXL and Topography-Guided PRK Simultaneous treatment appears to provide superior rehabilitation of keratoconus. BY A. JOHN KANELLOPOULOS, MD * Editor s note: The following
Sequential Versus Simultaneous CXL and Topography-Guided PRK Simultaneous treatment appears to provide superior rehabilitation of keratoconus. BY A. JOHN KANELLOPOULOS, MD * Editor s note: The following
Post LASIK Ectasia. Examination: Gina M. Rogers, MD and Kenneth M. Goins, MD
 Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis
 ARTICLE Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis Steven A. Greenstein, Kristen L. Fry, OD, MS, Jalpa Bhatt,
ARTICLE Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis Steven A. Greenstein, Kristen L. Fry, OD, MS, Jalpa Bhatt,
UPDATE ON AVEDRO CROSSLINKING STUDIES
 UPDATE ON AVEDRO CROSSLINKING STUDIES Peter S. Hersh, M.D. Director, Cornea & Laser Eye Institute CLEI Center for Keratoconus Clinical Professor of Ophthalmology, Rutgers Medical School Visiting Researcher,
UPDATE ON AVEDRO CROSSLINKING STUDIES Peter S. Hersh, M.D. Director, Cornea & Laser Eye Institute CLEI Center for Keratoconus Clinical Professor of Ophthalmology, Rutgers Medical School Visiting Researcher,
How To Implant A Keraring
 Corneal Remodeling Using the Keraring A variety of thicknesses, arc lengths, and optical zone sizes allows tailoring of the procedure to the individual patient. BY DOMINIQUE PIETRINI, MD; AND TONY GUEDJ
Corneal Remodeling Using the Keraring A variety of thicknesses, arc lengths, and optical zone sizes allows tailoring of the procedure to the individual patient. BY DOMINIQUE PIETRINI, MD; AND TONY GUEDJ
Collagen cross-linking should be done separately. Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey
 Collagen cross-linking should be done separately Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey Collagen cross linking 1st established tx addressing the pathophysiology of corneal
Collagen cross-linking should be done separately Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey Collagen cross linking 1st established tx addressing the pathophysiology of corneal
Keratoconus is a bilateral, nonsymmetric, and noninflammatory
 CASE REPORT Collagen Cross-Linking (CCL) With Sequential Topography-Guided PRK A Temporizing Alternative for Keratoconus to Penetrating Keratoplasty A. John Kanellopoulos, MD* and Perry S. Binder, MS,
CASE REPORT Collagen Cross-Linking (CCL) With Sequential Topography-Guided PRK A Temporizing Alternative for Keratoconus to Penetrating Keratoplasty A. John Kanellopoulos, MD* and Perry S. Binder, MS,
Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up
 Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up Ramon Gutiérrez, MD, PhD; Inma Lopez, MD; Cesar Villa-Collar, OD, PhD; José Manuel González-Méijome, OD, PhD ABSTRACT PURPOSE:
Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up Ramon Gutiérrez, MD, PhD; Inma Lopez, MD; Cesar Villa-Collar, OD, PhD; José Manuel González-Méijome, OD, PhD ABSTRACT PURPOSE:
Sri Ganesh and Sheetal Brar. 1. Introduction. 2. Materials and Methods
 Ophthalmology Volume 215, Article ID 263412, 7 pages http://dx.doi.org/1.1155/215/263412 Clinical Study Clinical Outcomes of Small Incision Lenticule Extraction with Accelerated Cross-Linking (ReLEx SMILE
Ophthalmology Volume 215, Article ID 263412, 7 pages http://dx.doi.org/1.1155/215/263412 Clinical Study Clinical Outcomes of Small Incision Lenticule Extraction with Accelerated Cross-Linking (ReLEx SMILE
Cross-Linking with Refractive Surgery: Pros and Cons
 Cross-Linking with Refractive Surgery: Pros and Cons Raj K. Rajpal, M.D. Medical Director and Founder See Clearly Vision Group Mclean, Virginia Clinical Associate Professor Georgetown University Washington,
Cross-Linking with Refractive Surgery: Pros and Cons Raj K. Rajpal, M.D. Medical Director and Founder See Clearly Vision Group Mclean, Virginia Clinical Associate Professor Georgetown University Washington,
Irregular astigmatism can occur naturally or due to
 Combined Topography- Guided Transepithelial PRK and CXL in Patients With Keratoconus The combined procedure strengthens the cornea and regularizes the anterior surface. BY MIRKO R. JANKOV II, MD, PHD;
Combined Topography- Guided Transepithelial PRK and CXL in Patients With Keratoconus The combined procedure strengthens the cornea and regularizes the anterior surface. BY MIRKO R. JANKOV II, MD, PHD;
Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9
 Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9 COMPARISON OF RAPID AND CONVENTIONAL CORNEAL COLLAGEN CROSS LINKING IN PATIENTS HAVING KERATOCONUS Intisar ul Haq,
Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9 COMPARISON OF RAPID AND CONVENTIONAL CORNEAL COLLAGEN CROSS LINKING IN PATIENTS HAVING KERATOCONUS Intisar ul Haq,
Single-Segment and Double-Segment INTACS for Post-LASIK Ectasia. Received: 8 Mar. 2013; Accepted: 8 Oct. 2013
 ORIGINAL ARTICLE Single-Segment and Double-Segment INTACS for Post-LASIK Ectasia Hassan Hashemi 1, Ali Gholaminejad 1, Kazem Amanzadeh 1, Maryam Hashemi 2, and Mehdi Khabazkhoob 3 1 Noor Ophthalmology
ORIGINAL ARTICLE Single-Segment and Double-Segment INTACS for Post-LASIK Ectasia Hassan Hashemi 1, Ali Gholaminejad 1, Kazem Amanzadeh 1, Maryam Hashemi 2, and Mehdi Khabazkhoob 3 1 Noor Ophthalmology
CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD
 CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD From: BOGOTA LASER REFRACTIVE INSTITUTE Bogota, Colombia DISCLOSURES FOR GUSTAVO TAMAYO
CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD From: BOGOTA LASER REFRACTIVE INSTITUTE Bogota, Colombia DISCLOSURES FOR GUSTAVO TAMAYO
Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years
 Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years Hassan Hashemi, MD 1,2 Mehrdad Mohammadpour, MD 3 Abstract Purpose: To describe a case of successful laser in situ
Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years Hassan Hashemi, MD 1,2 Mehrdad Mohammadpour, MD 3 Abstract Purpose: To describe a case of successful laser in situ
By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA.
 By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA Rome, Italy 2013 بسم الرحمن الرحيم In the name of Allah, Most Gracious, Most Merciful
By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA Rome, Italy 2013 بسم الرحمن الرحيم In the name of Allah, Most Gracious, Most Merciful
How do we use the Galilei for cataract and refractive surgery?
 How do we use the Galilei for cataract and refractive surgery? Douglas D. Koch, MD Mariko Shirayama, MD* Li Wang, MD, PhD* Mitchell P. Weikert, MD Cullen Eye Institute Baylor College of Medicine Houston,
How do we use the Galilei for cataract and refractive surgery? Douglas D. Koch, MD Mariko Shirayama, MD* Li Wang, MD, PhD* Mitchell P. Weikert, MD Cullen Eye Institute Baylor College of Medicine Houston,
Long-term stability of the posterior cornea after laser in situ keratomileusis
 ARTICLE Long-term stability of the posterior cornea after laser in situ keratomileusis Joseph B. Ciolino, MD, Stephen S. Khachikian, MD, Michael J. Cortese, OD, Michael W. Belin, MD PURPOSE: To study long-term
ARTICLE Long-term stability of the posterior cornea after laser in situ keratomileusis Joseph B. Ciolino, MD, Stephen S. Khachikian, MD, Michael J. Cortese, OD, Michael W. Belin, MD PURPOSE: To study long-term
Corneal Collagen Cross-Linking (CXL) With Riboflavin
 Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Comparison of Sequential vs Same-day Simultaneous Collagen Cross-linking and Topography-guided PRK for Treatment of Keratoconus
 Comparison of Sequential vs Same-day Simultaneous Collagen Cross-linking and Topography-guided PRK for Treatment of Keratoconus Anastasios John Kanellopoulos, MD ABSTRACT PURPOSE: The safety and effi cacy
Comparison of Sequential vs Same-day Simultaneous Collagen Cross-linking and Topography-guided PRK for Treatment of Keratoconus Anastasios John Kanellopoulos, MD ABSTRACT PURPOSE: The safety and effi cacy
Alain Saad, MD, Alice Grise-Dulac, MD, Damien Gatinel, MD, PhD
 CASE REPORT Bilateral loss in the quality of vision associated with anterior corneal protrusion after hyperopic LASIK followed by intrastromal femtolaser-assisted incisions Alain Saad, MD, Alice Grise-Dulac,
CASE REPORT Bilateral loss in the quality of vision associated with anterior corneal protrusion after hyperopic LASIK followed by intrastromal femtolaser-assisted incisions Alain Saad, MD, Alice Grise-Dulac,
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery
 Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Medical Director, Shinagawa LASIK Center, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China
 Medical Director,, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China Financial disclosure: Ziemer Group AG, Switzerland AcuFocus, CA Schwind Eye-Tech-Solutions,
Medical Director,, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China Financial disclosure: Ziemer Group AG, Switzerland AcuFocus, CA Schwind Eye-Tech-Solutions,
Refractive Surgery Issue. Inlays and Presbyopia: On the Horizon P. 24. Crack a SMILE or Raise a Flap? P. 30. LASIK Xtra: Who Should Get It? P.
 MULTIMODAL IMAGING OF PLACOID DISORDERS P. 42 WILLS RESIDENT CASE SERIES P. 67 NTG: THE NOCTURNAL BLOOD PRESSURE FACTOR P. 54 WISE CHOICES FOR OCULAR DIAGNOSES P. 50 NEW WAYS TO DETECT KERATOCONUS P. 58
MULTIMODAL IMAGING OF PLACOID DISORDERS P. 42 WILLS RESIDENT CASE SERIES P. 67 NTG: THE NOCTURNAL BLOOD PRESSURE FACTOR P. 54 WISE CHOICES FOR OCULAR DIAGNOSES P. 50 NEW WAYS TO DETECT KERATOCONUS P. 58
Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia
 Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia Robert L. Epstein, MD, MSEE; Yi-Lin Chiu, PhD; Greg L. Epstein, BS ABSTRACT PURPOSE: To determine criteria for keratoconus
Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia Robert L. Epstein, MD, MSEE; Yi-Lin Chiu, PhD; Greg L. Epstein, BS ABSTRACT PURPOSE: To determine criteria for keratoconus
Keratoconus Detection Using Corneal Topography
 Keratoconus Detection Using Corneal Topography Jack T. Holladay, MD, MSEE, FACS ABSTRACT PURPOSE: To review the topographic patterns associated with keratoconus suspects and provide criteria for keratoconus
Keratoconus Detection Using Corneal Topography Jack T. Holladay, MD, MSEE, FACS ABSTRACT PURPOSE: To review the topographic patterns associated with keratoconus suspects and provide criteria for keratoconus
Unilateral Corneal Ectasia after Bilateral LASIK: The Thick Flap Counts
 10.5005/jp-journals-10025-1056 Case Report IJKECD Unilateral Corneal Ectasia after Bilateral LASIK: The Thick Flap Counts Bruno Freitas Valbon, Renato Ambrosio Jr, Juliana Glicéria, Rodrigo Santos, Allan
10.5005/jp-journals-10025-1056 Case Report IJKECD Unilateral Corneal Ectasia after Bilateral LASIK: The Thick Flap Counts Bruno Freitas Valbon, Renato Ambrosio Jr, Juliana Glicéria, Rodrigo Santos, Allan
Efficacy of Intacs Intrastromal Corneal Ring Segments in Patients with Post-LASIK Corneal Ectasia
 Efficacy of Intacs Intrastromal Corneal Ring Segments in Patients with Post-LASIK Corneal Ectasia Amirhushang Beheshtnejad, MD 1 Alireza Yazdani-Abyaneh, MD 2 Hassan Hashemi, MD 3,4 Mahmoud Jabbarvand,
Efficacy of Intacs Intrastromal Corneal Ring Segments in Patients with Post-LASIK Corneal Ectasia Amirhushang Beheshtnejad, MD 1 Alireza Yazdani-Abyaneh, MD 2 Hassan Hashemi, MD 3,4 Mahmoud Jabbarvand,
Corneal ectasia induced by laser in situ keratomileusis. Ioannis G. Pallikaris, MD, PhD, George D. Kymionis, MD, PhD, Nikolaos I.
 Corneal ectasia induced by laser in situ keratomileusis Ioannis G. Pallikaris, D, PhD, George D. Kymionis, D, PhD, Nikolaos I. Astyrakakis, OD ABSTRACT Purpose: To identify factors that can lead to corneal
Corneal ectasia induced by laser in situ keratomileusis Ioannis G. Pallikaris, D, PhD, George D. Kymionis, D, PhD, Nikolaos I. Astyrakakis, OD ABSTRACT Purpose: To identify factors that can lead to corneal
Lasik Xtra in: Hyperopia AK Xtra Clear cornea cataract surgery
 Lasik Xtra in: Hyperopia AK Xtra Clear cornea cataract surgery A. John Kanellopoulos, M.D. Clinical Profesor of Ophthalmology New York University School of Medicine, New York, NY, USA Laservision.gr Institute,
Lasik Xtra in: Hyperopia AK Xtra Clear cornea cataract surgery A. John Kanellopoulos, M.D. Clinical Profesor of Ophthalmology New York University School of Medicine, New York, NY, USA Laservision.gr Institute,
Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps
 Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps Lingo Y. Lai, MD William G. Zeh, MD Clark L. Springs, MD The authors
Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps Lingo Y. Lai, MD William G. Zeh, MD Clark L. Springs, MD The authors
High Order Aberration Outcomes of Corneal Collagen Crosslinking in Eyes with 10.5005/jp-journals-10025-1088
 IJKECD High Order Aberration Outcomes of Corneal Collagen Crosslinking in Eyes with 10.5005/jp-journals-10025-1088 Keratoconus and Post-LASIK Ectasia ORIGINAL ARTICLE High Order Aberration Outcomes of
IJKECD High Order Aberration Outcomes of Corneal Collagen Crosslinking in Eyes with 10.5005/jp-journals-10025-1088 Keratoconus and Post-LASIK Ectasia ORIGINAL ARTICLE High Order Aberration Outcomes of
THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening
 THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening GALILEI G4 Clinical Applications Corneal Implant Planning The comes with a licensable corneal inlay software
THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening GALILEI G4 Clinical Applications Corneal Implant Planning The comes with a licensable corneal inlay software
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Διαθλαζηικη Χειροσργικη 2014
 Διαθλαζηικη Χειροσργικη 2014 Επιθηλιο Femto Κεραηοκωνος Διαζσνδεζη Κολλαγονοσ Anastasios John Kanellopoulos, MD Professor: NYU Medical School, New York, NY LaserVision.gr Eye Institute, Athens, Greece
Διαθλαζηικη Χειροσργικη 2014 Επιθηλιο Femto Κεραηοκωνος Διαζσνδεζη Κολλαγονοσ Anastasios John Kanellopoulos, MD Professor: NYU Medical School, New York, NY LaserVision.gr Eye Institute, Athens, Greece
Review Article Complications of Corneal Collagen Cross-Linking
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2011, Article ID 869015, 5 pages doi:10.1155/2011/869015 Review Article Complications of Corneal Collagen Cross-Linking Shikha Dhawan, Kavita
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2011, Article ID 869015, 5 pages doi:10.1155/2011/869015 Review Article Complications of Corneal Collagen Cross-Linking Shikha Dhawan, Kavita
Intacs for keratoconus Yaron S. Rabinowitz
 Intacs for keratoconus Yaron S. Rabinowitz Purpose of review The use of Intacs as a therapeutic modality in contact lens intolerant patients with mild to moderate keratoconus is increasingly gaining acceptance
Intacs for keratoconus Yaron S. Rabinowitz Purpose of review The use of Intacs as a therapeutic modality in contact lens intolerant patients with mild to moderate keratoconus is increasingly gaining acceptance
5/24/2013 ESOIRS 2013. Moderator: Alaa Ghaith, MD. Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD
 ESOIRS 2013 Moderator: Alaa Ghaith, MD Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD 1 A systematic approach to the management of Keratoconus through the presentation of different
ESOIRS 2013 Moderator: Alaa Ghaith, MD Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD 1 A systematic approach to the management of Keratoconus through the presentation of different
FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US
 FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US JON DISHLER, MD DENVER, COLORADO, USA INTRODUCTION AND STUDY OBJECTIVES This article summarizes the first US
FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US JON DISHLER, MD DENVER, COLORADO, USA INTRODUCTION AND STUDY OBJECTIVES This article summarizes the first US
9/15/2013. Naturally-existing Corneal Pathology Forme Fruste Keratoconus Keratoconus Pellucid Marginal Degeneration
 Bill Tullo, OD, FAAO Diplomate Vice-President of Clinical Services TLC Vision 33386-PO 1 Hour Bill Tullo, OD has no financial interests in any of the products or companies discussed in this program Naturally-existing
Bill Tullo, OD, FAAO Diplomate Vice-President of Clinical Services TLC Vision 33386-PO 1 Hour Bill Tullo, OD has no financial interests in any of the products or companies discussed in this program Naturally-existing
Topography guided custom ablation treatment for treatment of keratoconus
 Symposium: Keratoconus Topography guided custom ablation treatment for treatment of keratoconus Rohit Shetty, Sharon D Souza, Samaresh Srivastava 1, R Ashwini Keratoconus is a progressive ectatic disorder
Symposium: Keratoconus Topography guided custom ablation treatment for treatment of keratoconus Rohit Shetty, Sharon D Souza, Samaresh Srivastava 1, R Ashwini Keratoconus is a progressive ectatic disorder
Short and long term complications of combined. Protocol) in 412 keratoconus eyes (2 7 years follow up)
 Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Cornea and Refractive Surgery Update
 Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Photorefractive keratectomy in mild to moderate keratoconus: Outcomes in over 40 year old patients
 Original Article Photorefractive keratectomy in mild to moderate keratoconus: Outcomes in over 40 year old patients Hamid Khakshoor, Fatemeh Razavi, Alireza Eslampour 1, Arash Omdtabrizi 1 Background:
Original Article Photorefractive keratectomy in mild to moderate keratoconus: Outcomes in over 40 year old patients Hamid Khakshoor, Fatemeh Razavi, Alireza Eslampour 1, Arash Omdtabrizi 1 Background:
Macsai MS, Varley GA, Krachmer JH. Development of keratoconus after. contact lens wear. Arch Ophthalmol 1990;108:534 538.
 Lovisolo CF, Fleming JF. Intracorneal ring segments for iatrogenic keratectasia after laser in situ keratomileusis or photorefractive keratectomy. J Refract Surg. 2002; 18:535 541. Macsai MS, Varley GA,
Lovisolo CF, Fleming JF. Intracorneal ring segments for iatrogenic keratectasia after laser in situ keratomileusis or photorefractive keratectomy. J Refract Surg. 2002; 18:535 541. Macsai MS, Varley GA,
Collagen Cross-linking combined with PRK and LASIK
 Collagen Cross-linking combined with PRK and LASIK./*0&1#*!"#$%%&'&(%&)2*+,* +$345"%*,46$57&62*8")$694)4&#/:6*;#)%4#45"%*?6&@$))&62*ABC*8"#:&#$*+$345"%*D51&&%2*AB!"#$%%&'&(%&)*+,!
Collagen Cross-linking combined with PRK and LASIK./*0&1#*!"#$%%&'&(%&)2*+,* +$345"%*,46$57&62*8")$694)4&#/:6*;#)%4#45"%*?6&@$))&62*ABC*8"#:&#$*+$345"%*D51&&%2*AB!"#$%%&'&(%&)*+,!
Corneal intrastromal implantation surgery for the treatment of moderate and high myopia
 TECHNIQUE Corneal intrastromal implantation surgery for the treatment of moderate and high myopia Albert Daxer, MD, PhD I describe a corneal intrastromal implantation technique that uses a new type of
TECHNIQUE Corneal intrastromal implantation surgery for the treatment of moderate and high myopia Albert Daxer, MD, PhD I describe a corneal intrastromal implantation technique that uses a new type of
Lasik Xtra Provides Corneal Stability and Improved Outcomes
 DOI 10.1007/s40123-015-0039-x REVIEW Lasik Xtra Provides Corneal Stability and Improved Outcomes Rajesh K. Rajpal. Christine B. Wisecarver. Dawn Williams. Sachin D. Rajpal. Rhonda Kerzner. Nick Nianiaris.
DOI 10.1007/s40123-015-0039-x REVIEW Lasik Xtra Provides Corneal Stability and Improved Outcomes Rajesh K. Rajpal. Christine B. Wisecarver. Dawn Williams. Sachin D. Rajpal. Rhonda Kerzner. Nick Nianiaris.
Clinical Results of Topography-based Customized Ablations in Highly Aberrated Eyes and Keratoconus/Ectasia With Cross-linking
 Clinical Results of Topography-based Customized Ablations in Highly Aberrated Eyes and Keratoconus/Ectasia With Cross-linking David T.C. Lin, MD, FRCSC; Simon Holland, MD, FRCSC; Johnson C.H. Tan, MBBS,
Clinical Results of Topography-based Customized Ablations in Highly Aberrated Eyes and Keratoconus/Ectasia With Cross-linking David T.C. Lin, MD, FRCSC; Simon Holland, MD, FRCSC; Johnson C.H. Tan, MBBS,
Key Words: Aberration, LASEK, LASIK, Posterior corneal surface, Wavefront-guided ablation
 Department of Ophthalmology, Seoul National University College of Medicine 1, Seoul, Korea Seoul Artificial Eye Center, Seoul National University Hospital Clinical Research Institute 2, Seoul, Korea Department
Department of Ophthalmology, Seoul National University College of Medicine 1, Seoul, Korea Seoul Artificial Eye Center, Seoul National University Hospital Clinical Research Institute 2, Seoul, Korea Department
Comparison of Two Procedures: Photorefractive Keratectomy Versus Laser In Situ Keratomileusis for Low to Moderate Myopia
 Comparison of Two Procedures: Photorefractive Keratectomy Versus Laser In Situ Keratomileusis for Low to Moderate Myopia Jae Bum Lee, Jae Sung Kim, Chul-Myong Choe, Gong Je Seong and Eung Kweon Kim Institute
Comparison of Two Procedures: Photorefractive Keratectomy Versus Laser In Situ Keratomileusis for Low to Moderate Myopia Jae Bum Lee, Jae Sung Kim, Chul-Myong Choe, Gong Je Seong and Eung Kweon Kim Institute
Refractive errors, such as residual astigmatism after
 CLINICAL SCIENCE Intrastromal Corneal Ring Segment Implantation by Femtosecond Laser for the Correction of Residual Astigmatism After Penetrating Keratoplasty Tatiana Moura Bastos Prazeres, MD,* Allan
CLINICAL SCIENCE Intrastromal Corneal Ring Segment Implantation by Femtosecond Laser for the Correction of Residual Astigmatism After Penetrating Keratoplasty Tatiana Moura Bastos Prazeres, MD,* Allan
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments
 Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Collagen Cross-linking with Riboflavin in a Hypotonic Solution, with UV light, on Corneas Less Than 400 microns thick: an exploratory study
 Collagen Cross-linking with Riboflavin in a Hypotonic Solution, with UV light, on Corneas Less Than 400 microns thick: an exploratory study Chad Rostron. Corneal Collagen Cross-linking with Riboflavin
Collagen Cross-linking with Riboflavin in a Hypotonic Solution, with UV light, on Corneas Less Than 400 microns thick: an exploratory study Chad Rostron. Corneal Collagen Cross-linking with Riboflavin
Comparison Combined LASIK Procedure for Ametropic Presbyopes and Planned Dual Interface for Post-LASIK Presbyopes Using Small Aperture Corneal Inlay
 Comparison Combined LASIK Procedure for Ametropic Presbyopes and Planned Dual Interface for Post-LASIK Presbyopes Using Small Aperture Corneal Inlay Minoru Tomita, MD, PhD 1,2 1) Shinagawa LASIK, Tokyo,
Comparison Combined LASIK Procedure for Ametropic Presbyopes and Planned Dual Interface for Post-LASIK Presbyopes Using Small Aperture Corneal Inlay Minoru Tomita, MD, PhD 1,2 1) Shinagawa LASIK, Tokyo,
Ophthalmology. Department of Ophthalmology and Vision Sciences. FACULTY OF MEDICINE University of Toronto. Keratoconus
 2011 Volume 9, Issue 1 Ophthalmology ROUNDS AS PRESENTED IN THE ROUNDS OF THE DEPARTMENT OF OPHTHALMOLOGY AND VISION SCIENCES, FACULTY OF MEDICINE, UNIVERSITY OF TORONTO Corneal Collagen Crosslinking:
2011 Volume 9, Issue 1 Ophthalmology ROUNDS AS PRESENTED IN THE ROUNDS OF THE DEPARTMENT OF OPHTHALMOLOGY AND VISION SCIENCES, FACULTY OF MEDICINE, UNIVERSITY OF TORONTO Corneal Collagen Crosslinking:
Clinical Practice. Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results
 Clinical Practice JOHN E. SUTPHIN, MD, EDITOR Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results FREDERIK RAISKUP, MD, PHD, FEBO, AND EBERHARD SPOERL, PHD
Clinical Practice JOHN E. SUTPHIN, MD, EDITOR Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results FREDERIK RAISKUP, MD, PHD, FEBO, AND EBERHARD SPOERL, PHD
Financial Disclosure. LASIK Flap Parameters IntraLase Microkeratome 6/9/2008. Femtosecond LASIK Flaps: What Could We Customize Yesterday?
 Financial Disclosure Arturo Chayet, MD Tijuana, BC Mexico Perry S. Binder, MS, MD San Diego CA USA I have the following financial interests or relationships to disclose: AMO/IntraLase Corporation - C Acufocus
Financial Disclosure Arturo Chayet, MD Tijuana, BC Mexico Perry S. Binder, MS, MD San Diego CA USA I have the following financial interests or relationships to disclose: AMO/IntraLase Corporation - C Acufocus
Refractive Surgery. Evolution of Refractive Error Correction
 Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Page: 1 of 6. Corneal Topography/Computer-Assisted Corneal Topography/ Photokeratoscopy
 Section: Surgery Effective Date: July 15, 2015 Last Review Status/Date: June 2015 Page: 1 of 6 Corneal Topography/ Photokeratoscopy Description Computer-assisted topography/photokeratoscopy provides a
Section: Surgery Effective Date: July 15, 2015 Last Review Status/Date: June 2015 Page: 1 of 6 Corneal Topography/ Photokeratoscopy Description Computer-assisted topography/photokeratoscopy provides a
 Collagen Crosslinking and Management of Keratoconus Christopher Chow, M.D. Michigan Cornea Consultants Oakland University William Beaumont School of Medicine May 11, 2012 2 Keratoconus First described
Collagen Crosslinking and Management of Keratoconus Christopher Chow, M.D. Michigan Cornea Consultants Oakland University William Beaumont School of Medicine May 11, 2012 2 Keratoconus First described
This is the author s version of a work that was submitted/accepted for publication in the following source:
 This is the author s version of a work that was submitted/accepted for publication in the following source: Zeraid, Ferial M., Jawkhab, Asma A., Al-Tuwairqi, Waleed S., & Osuagwu, Uchechukwu L. (2014)
This is the author s version of a work that was submitted/accepted for publication in the following source: Zeraid, Ferial M., Jawkhab, Asma A., Al-Tuwairqi, Waleed S., & Osuagwu, Uchechukwu L. (2014)
Long-Term Outcomes of Flap Amputation After LASIK
 Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES
 Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Laser-assisted In Situ Keratomileusis for Correction of Astigmatism and Increasing Contact Lens Tolerance after Penetrating Keratoplasty
 pissn: -9 eissn: 9-9 Korean J Ophthalmol ;(5):59- http://dx.doi.org/./kjo...5.59 Original Article Laser-assisted In Situ Keratomileusis for Correction of Astigmatism and Increasing Contact Lens Tolerance
pissn: -9 eissn: 9-9 Korean J Ophthalmol ;(5):59- http://dx.doi.org/./kjo...5.59 Original Article Laser-assisted In Situ Keratomileusis for Correction of Astigmatism and Increasing Contact Lens Tolerance
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL
 REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
Corneal collagen cross-linking (CXL) was first described in
 CLINICAL SCIENCE Transepithelial Corneal Cross-Linking With Vitamin E-Enhanced Riboflavin Solution and Abbreviated, Low-Dose UV-A: 24-Month Clinical Outcomes Ciro Caruso, MD,* Carmine Ostacolo, PharmD,
CLINICAL SCIENCE Transepithelial Corneal Cross-Linking With Vitamin E-Enhanced Riboflavin Solution and Abbreviated, Low-Dose UV-A: 24-Month Clinical Outcomes Ciro Caruso, MD,* Carmine Ostacolo, PharmD,
A.M.Sherif,M.A.Ammar,Y.S.Mostafa,S.A.GamalEldin,andA.A.Osman. Department of Ophthalmology, Faculty of Medicine, Cairo University, Cairo 12411, Egypt
 Ophthalmology Volume 2015, Article ID 321953, 7 pages http://dx.doi.org/10.1155/2015/321953 Clinical Study One-Year Results of Simultaneous Topography-Guided Photorefractive Keratectomy and Corneal Collagen
Ophthalmology Volume 2015, Article ID 321953, 7 pages http://dx.doi.org/10.1155/2015/321953 Clinical Study One-Year Results of Simultaneous Topography-Guided Photorefractive Keratectomy and Corneal Collagen
Keratoconus surgery: what works best and why-
 Keratoconus surgery: what works best and why-./-0&1#-!"#$%%&'&(%&)*-+,-,23$45&3*-6")$372)2&#/83-9#):5(5$*-.51$#)*-;3$$4$-
Keratoconus surgery: what works best and why-./-0&1#-!"#$%%&'&(%&)*-+,-,23$45&3*-6")$372)2&#/83-9#):5(5$*-.51$#)*-;3$$4$-
Anterior Elevation Maps as the Screening Test for the Ablation Power of Previous Myopic Refractive Surgery
 Anterior Elevation Maps as the Screening Test for the Ablation Power of Previous Myopic Refractive Surgery Soo Yong Jeong, MD, Hee-Seung Chin, MD, PhD, Jung Hyub Oh, MD, PhD Department of Ophthalmology,
Anterior Elevation Maps as the Screening Test for the Ablation Power of Previous Myopic Refractive Surgery Soo Yong Jeong, MD, Hee-Seung Chin, MD, PhD, Jung Hyub Oh, MD, PhD Department of Ophthalmology,
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques
 Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
NEW SURGICAL APPROACHES TO THE MANAGEMENT OF KERATOCONUS AND POST-LASIK ECTASIA
 NEW SURGICAL APPROACHES TO THE MANAGEMENT OF KERATOCONUS AND POST-LASIK ECTASIA BY Bryan U. Tan MD, Tracy L. Purcell PhD, Luis F. Torres MD PhD, AND David J. Schanzlin MD* ABSTRACT Purpose: The objective
NEW SURGICAL APPROACHES TO THE MANAGEMENT OF KERATOCONUS AND POST-LASIK ECTASIA BY Bryan U. Tan MD, Tracy L. Purcell PhD, Luis F. Torres MD PhD, AND David J. Schanzlin MD* ABSTRACT Purpose: The objective
Laser in situ keratomileusis (LASIK) has been. Retreatment of Hyperopia After Primary Hyperopic LASIK REPORTS
 REPORTS Retreatment of Hyperopia After Primary Hyperopic LASIK Julio Ortega-Usobiaga, MD, PhD; Rosario Cobo-Soriano, MD, PhD; Fernando Llovet, MD; Francisco Ramos, MD; Jaime Beltrán, MD; Julio Baviera-Sabater,
REPORTS Retreatment of Hyperopia After Primary Hyperopic LASIK Julio Ortega-Usobiaga, MD, PhD; Rosario Cobo-Soriano, MD, PhD; Fernando Llovet, MD; Francisco Ramos, MD; Jaime Beltrán, MD; Julio Baviera-Sabater,
For approximately two decades photorefractive keratectomy. Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK.
 Cornea Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK Anders Ivarsen and Jesper Hjortdal PURPOSE. To examine long-term changes in corneal power and aberrations in myopic patients
Cornea Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK Anders Ivarsen and Jesper Hjortdal PURPOSE. To examine long-term changes in corneal power and aberrations in myopic patients
LASIK SURGERY OUTCOMES, VOLUME AND RESOURCES
 MOH Information Paper: 2006/17 LASIK SURGERY OUTCOMES, VOLUME AND RESOURCES By Dr. Ganga Ganesan 1 I INTRODUCTION LASIK stands for Laser-Assisted In Situ Keratomileusis and is a surgical procedure that
MOH Information Paper: 2006/17 LASIK SURGERY OUTCOMES, VOLUME AND RESOURCES By Dr. Ganga Ganesan 1 I INTRODUCTION LASIK stands for Laser-Assisted In Situ Keratomileusis and is a surgical procedure that
Trans-epithelial cross-linking with riboflavin solution: two-year clinical results
 Trans-epithelial cross-linking with riboflavin solution: two-year clinical results Authors: Ciro Caruso, M.D. 1,2, Luigi Pacente, M.D. 1, Robert L Epstein 5, Salvatore Troisi, M.D. 3, Gaetano Barbaro,
Trans-epithelial cross-linking with riboflavin solution: two-year clinical results Authors: Ciro Caruso, M.D. 1,2, Luigi Pacente, M.D. 1, Robert L Epstein 5, Salvatore Troisi, M.D. 3, Gaetano Barbaro,
SCHWIND CAM Perfect Planning wide range of applications
 SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PALK-CAM PTK-CAM 2 SCHWIND CAM the system solution The latest version of the modular SCHWIND CAM represents an even more efficient
SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PALK-CAM PTK-CAM 2 SCHWIND CAM the system solution The latest version of the modular SCHWIND CAM represents an even more efficient
