A thesis submitted for the degree of Doctor of Medicine at the Faculty of Medicine Ludwig-Maximilians-University Munich, Germany
|
|
|
- Jean Ford
- 8 years ago
- Views:
Transcription
1 In vitro generation of human monocyte-derived dendritic cells within 48 hours: functional characterisation and optimal activation in view of cellular-based immunotherapy A thesis submitted for the degree of Doctor of Medicine at the Faculty of Medicine Ludwig-Maximilians-University Munich, Germany Submitted by Véronique Lam Isong Plaines Wilhelms, Mauritius 2012 Completed at the Section of Gastroenterology, Medizinische Klinik Innenstadt, University of Munich
2 Aus der Medizinischen Klinik und Poliklinik IV-Innenstadt der Ludwig-Maximilians-Universität München Direktor : Prof. Dr. Martin Reincke Generierung dendritischer Zellen aus Monozyten innerhalb von 48 Stunden in vitro: funktionelle Charakterisierung und optimale Aktivierung im Hinblick auf die Tumor-Immuntherapie Dissertation zum Erwerb des Doktorgrades der Medizin an der Medizinischen Fakultät der Ludwig-Maximilians-Universität München vorgelegt von Véronique Lam Isong aus Plaines Wilhelms, Mauritius 2012
3 With permission of the Faculty of medicine of the University of Munich Supervisor/Examiner: Prof. Dr. Andreas Eigler Co-examiners: Prof. Dr. Monika Führer Priv. Doz. Dr. Peter Neth Dekan: Prof. Dr.med. Dr. h.c. Maximilian Reiser, FACR, FRCR Oral examination held on:
4 Mit Genehmigung der Medizinischen Fakultät der Universität München Berichtserstatter: Prof. Dr. Andreas Eigler Mitberichtserstatter: Prof. Dr. Monika Führer Priv. Doz. Dr. Peter Neth Dekan: Prof. Dr. Dr. h.c. Maximilian Reiser, FACR, FRCR Tag der mündlichen Prüfung:
5 Table of contents 1. INTRODUCTION DENDRITIC CELLS Dendritic cell subsets Functional plasticity of dendritic cells Antigen uptake, processing and presentation Maturation of dendritic cells Migration of dendritic cells DENDRITIC CELLS AND T-CELL MEDIATED IMMUNITY T-cell subsets Interleukin CLINICAL APPLICATIONS OF DENDRITIC CELLS Dendritic cells and tolerance Dendritic cells and clinical immunology Dendritic cell-based cancer immunotherapy ISOLATION OF DENDRITIC CELLS Stimuli used for dendritic cell maturation in vitro Pro-inflammatory mediators: Prostaglandin E 2, tumour necrosis factor- and interleukin Pathogen-derived signals: Toll-like receptors T-cell derived signals: CD40 ligand and interferon SHORT-TERM CULTURE PROTOCOLS QUESTIONS ADDRESSED METHODS REAGENTS AND MATERIALS Apparatus Plastic materials Reagents Frequently used buffers Reagents for cell culture Monoclonal antibodies Cytokines and chemokines Enzyme-linked immunosorbent assays (ELISA) Magnetic activated cell sorting (MACS) Peptides T2 cell line CELL ISOLATION AND CELL CULTURE Cell culture Counting of cells and cell viability Enrichment of monocytes by cell adhesion Generation of FastDC in vitro Standard protocol for the generation of monocytes-derived dendritic cells Immature DC Isolation of T-cells by magnetic cell sorting (MACS) ANALYTICAL METHODS Phase-contrast microscopy Enzyme-linked immunosorbent assay (ELISA) Fluorescent-activated cell-sorting (FACS) Staining of cell surface CD (cluster of differentiation) molecules Staining of intracellular interferon Streptamer Fluorescent T-labeling and isolation via FACS Endocytosis assay (FITC-dextran uptake) Pinocytosis assay (Panc-tumor-cells uptake) Cell migration assay Induction of antigen-specific T-cell responses Co-culture of FastDC with autologous T-cells Radiolabeling of target cells Standard 51 Cr release assay * Statistical analysis...28
6 3. RESULTS INFLUENCE OF INTERFERON-ALPHA ON FASTDC DIFFERENTIATION, TERMINAL MATURATION AND ANTIGEN UPTAKE Differentiation and terminal maturation Antigen uptake Uptake of FITC-labeled dextran Uptake of CFSE-labeled apoptotic pancreatic carcinoma cells by FastDC OPTIMISATION OF THE FASTDC PROTOCOL: USE OF TOLL-LIKE RECEPTOR AGONISTS FOR STIMULATION FastDC immunophenotype and IL-12p70 synthesis upon TLR-based activation Migration and CCR7 expression by FastDC upon TLR-based activation PGE 2 and TLR-based FastDC Generation of multifunctional FastDCs using pro-inflammatory mediators in combination with TLR agonists INDUCTION OF ANTIGEN-SPECIFIC T-CELL RESPONSES BY FASTDC DISCUSSION SUMMARY OF THE RESULTS COMPARISON WITH THE LITERATURE FastDC and short term protocols Determination of antigen-specific T-cell responses FastDC and interferon IL-12p70 deficiency and migration in conventional FastDC Maximum IL-12p70 secretion in TLR-derived FastDC Poor migration in TLR-stimulated FastDC Migration is restored and IL-12p70 secretion is not aborted in TLR-matured FastDC supplemented with PGE Migratory vs. pro-inflammatory dendritic cells Activation of an antigen-specific immunity IL-12p70 secretion and antitumour immunity CLINICAL RELEVANCE Minor success of first-generation DC vaccines Optimal DC quality with TLR ligands and PGE 2 for DC-based immunotherapy Future perspectives DC-based therapy and adjuvant antitumour therapy SUMMARY ZUSAMMENFASSUNG LIST OF REFERENCES ABBREVIATIONS ACKNOWLEDGEMENTS PUBLICATIONS CURRICULUM VITAE...82
7 1 1. Introduction Innate and adaptive immunity are the two branches of the immune system. Cells of the innate immune system sense microbial presence by recognizing non-processed antigens, known as pathogen-associated molecular patterns (PAMP) using invariant pattern recognition receptors (PRR) in an antigen-independent manner. Macrophages and granulocytes are subsequently activated, providing immediate care (within hours) while restricting the spreading of an infection. On the other hand, cells of the adaptive immune system, comprising the T and B lymphocytes, are stimulated in an antigen-specific manner, and rely on additional instructions from the cells of the innate immune system to get activated. The resulting adaptive response is directed against one specific antigen. Furthermore, it is characterised by its immunological memory functions, providing long-lasting protection against invading pathogens, and is responsible for the discrimination between self and non-self. Antigen-presenting cells (APCs) are critical for the initiation and modulation of adaptive immune responses. Dendritic cells (DCs), known as the most potent APCs, represent a crucial link between the innate and the adaptive immune system, playing a central role in T lymphocyte activation and differentiation into T helper and cytotoxic T cells. In brief, the life cycle DCs can be simplified as follows: immature DCs are ideally positioned as sentinels in the bloodstream, mucosa or residing in tissues, sampling for incoming pathogens. In their immature state, they are highly efficient in antigen capture, processing and presentation with major histocompatibility complex (MHC) molecules - a prerequisite for T-cell activation. Upon activation, they undergo a process of maturation, up-regulating co-stimulatory molecules and migrating to the T cell-rich regions of lymph nodes where priming of corresponding naïve T cells occurs, resulting in the initiation of a T cellmediated response. In addition to their pivotal role in bridging the innate to the adaptive immune system, DCs have been found to be involved in the pathology of autoimmune diseases, cancer, organ rejections and graft versus host reactions (Banchereau et al., 2006). In recent years, there has been an increasing interest to exploit DCs to launch a specific T cell-mediated immune response against cancer cells. However, poor results obtained in early clinical trials have dampened the initial enthusiasm about DC-based immunotherapy. In current studies, factors contributing to the minor success of DC-based immunotherapy against cancer are being identified. Continuous investigation of DC biology will not only be helpful in
8 2 understanding the pathophysiology of diseases, but also in improving target-oriented therapeutic approaches. Thus, the generation of highly effective DC eligible for anti-tumour therapy is the main objective of this doctoral thesis Dendritic cells Dendritic cell subsets Like all immune cells, DCs originate from hematopoietic stem cells. It is widely accepted that there are two main differentiation pathways of DCs, generating three major DC subsets: (i) myeloid DCs (also known as interstitial DCs), (ii) Langerhans cells (LC)-DCs, and (iii) plasmacytoid DCs (pdcs). Along the myeloid pathway, CD34 + haematopoietic stem cells differentiate in either CD11c + CD1a + Langerhans precursor cells or CD11c + CD1a - interstitial DC precursor cells (Liu et al., 2001). While epidermal Langerhans cells stimulate cytotoxic T cells, interstitial DCs are localized in the dermis and other tissues, and promote B cell differentiation. Furthermore, the common myeloid progenitor gives rise to monocytes, differentiating into myeloid interstitial DCs under the influence of granulocyte macrophage colony-stimulating factor (GM-CSF) and interleukin-4 (IL-4). CD pdcs, believed to be of lymphoid origin, are characterized by the secretion of large amounts of type I interferons (interferon- and interferon- ) in response to viral infections. Recent murine in vivo studies demonstrated that Langerhans cells are derived from monocyte precursors (Banchereau et al., 2006). Though some data support the theory that human monocytes also represent a relevant in vivo precursor population for DCs (Banchereau et al., 1998), it remains to be determined whether monocyte-derived DCs have biological significance in humans Functional plasticity of dendritic cells In contrast to the initial belief that the developmental origin exclusively defines the functional specialization of distinct DC subsets, it has become evident that the local microenvironment, antigen dose, nature of microbial stimulus and maturational status of DCs modulate the final outcome of a T-cell mediated response (Pulendran et al., 2004). In vitro studies demonstrated that neither a T H 1 (T helper) nor a T H 2 response was an intrinsic feature of specific DC subset (Vieira et al., 2000) : while DCs cultured with IL-10 induced T H 2 responses, interferon- -primed (IFN- ) DCs were found to be potent inducers of T H 1 responses. Similarly, monocyte-derived DCs (modcs)
9 3 matured with interleukin-1 1 and tumour necrosis factor- (TNF- ) were demonstrated to induce a T H 1 response, while the supplementation of prostaglandin E 2 (PGE 2 ) rapidly induced the secretion of T H 2 cytokines (Kalinski et al., 1998). Likewise, the influence of the microenvironment on DC differentiation was underlined in experiments demonstrating that DCs localized in different tissues elicited different responses. For instance, splenic DCs were found to induce the secretion of T H 1 cytokines, whereas DCs localised in Peyer's patches secreted T H 2 cytokines (Iwasaki et al., 1999) Antigen uptake, processing and presentation Immature DCs sense microbial presence via recognition of pathogen-associated molecular patterns (PAMPs) by means of their pattern recognition receptors (PRRs) or through inflammatory cytokines present in the microenvironment. PAMPs represent highly evolutionary conserved patterns found on all microorganisms, that are essential for their survival (and therefore difficult to alter) and distinct from the host s patterns. Following recognition, immature DCs capture antigens in vivo by phagocytosis, receptor-mediated endocytosis or macropinocytosis (Guermonprez et al., 2002). Experimentally, DCs have been shown additionally to internalise latex and zymosan beads (Inaba et al. 1993) as well as apoptotic bodies (Parr et al. 1991; Rescigno et al. 2000). In order to be recognised by T cells, the captured antigens need to be processed and displayed in association with self MHC molecules in a process known as antigen presentation. The presentation of antigenic peptides on either MHC class I or MHC class II molecules determines the type of T cells to be primed a feature described as the T-cell restriction of the immune system. MHC class I-restricted presentation of intracellular or endogenous antigens leads to activation of CD8 + cytotoxic T lymphocytes (CTL). In contrast, presentation of exogenous antigens on MHC class II molecules activates CD4 + T helper cells, thereby eliciting either a T H 1 or a T H 2 response. While a T H 1 response is characterised by the activation of macrophages, cytotoxic T cells and other effector cells, a T H 2 response results in the activation of B lymphocytes, with the subsequent formation of immunoglobulins. In addition to these classical pathways of antigen presentation, DCs are capable of presenting exogenous peptides on MHC class I molecules, a process called cross-presentation (Trombetta et al., 2005). It represents an important feature of DCs, resulting in the activation of CD8 + T cells against tumour and viral antigens that are otherwise not accessible to the classical MHC class I pathway. Furthermore, cross-presentation in DCs was reported to play an important role in transplantation and autoimmune diseases (Ackerman et al. 2004).
10 Maturation of dendritic cells DC maturation is characterised by the development of features optimising the efficacy of DCs in T- cell priming. It is a continuous process, initiated in the periphery following encounter to pathogens, and completed upon T-cell encounter. Microbial-derived stimuli (e.g. Toll-like receptors), proinflammatory mediators (PGE 2, TNF- ), T-cell derived signals (CD40 ligand), and immune complexes acting on Fc receptors as well as sensors for cell death are known to induce maturation in DCs. DC maturation is characterised by the up-regulation of membrane-associated co-stimulatory molecules, such as CD86 (cluster of differentiation) and CD80, as well as increased expression of the specific DC marker CD83 and MHC molecules (Banchereau et al., 1998). CD83 is one of the best-known maturation markers in DCs. Its functional role has not been completely elucidated, but it has been reported to influence T cell differentiation (Lechmann et al., 2002). Concomitant to the up-regulation of co-stimulatory molecules, DCs undergo co-ordinated changes in the expression of adhesion molecules accompanied by cytoskeletal re-organisations. For instance, mannose-receptors are down-regulated and DCs lose their capacity to capture antigens. Likewise, they become unresponsive to immature DC-associated chemokines such as macrophage inflammatory protein (MIP-) 1 and MIP-3 (Caux et al. 2002) Migration of dendritic cells To encounter and activate T lymphocytes, DCs migrate to secondary lymphoid organs. The process of DC maturation is closely related to DC migration: while up-regulating the chemokine receptors CCR7, DCs migrate to the lymph nodes via the afferent lymphatic system or highendothelial venules (HEV). Upon CCR7 expression, mature DCs respond to MIP-3 (also known as Exodus 3, ELC [EBI ligand chemokine], CCL 19 [chemokine ligand]) and 6Ckine (also known as SLC [secondary lymphoid tissue chemokine], Exodus 2 or CCL21), both highly expressed by stromal cells in the T cell rich zones of lymph nodes. Interestingly, CCR7 + naïve T cells were also reported to enter lymph nodes in response to 6Ckine (Willimann et al., 1998). Likewise, CCR7 expression was found in B cells as well as in non-immune cells in various malignancies (Förster et al., 2008). The key role of CCR7 in migration was demonstrated in a mouse knock-out model, whereby CCR7 - mice failed to migrate to lymph nodes while exhibiting an impaired immune response (Gunn
11 5 et al., 1999). In addition to its central role in chemotaxis, CCR7 was found to exert regulatory effects on DCs. Its expression has been associated with an extended longevity of DCs, caused by an inhibition of apoptosis. Furthermore, an increase in migratory speed was observed in CCR7 + DCs (Sanchez-Sanchez et al., 2004). Concomitant with the up-regulation of CCR7, changes in the cytoarchitecture of DCs were observed in terms of re-organisation of the actin cytoskeleton and the development of dendritic protrusions (Sanchez-Sanchez et al., 2006). However, in contrast to early assumptions, there is increasing evidence that migration is not limited to mature DCs: immature DCs expressing CCR7 in the absence of inflammatory signals were also found to home to the lymph nodes. These semi-mature DCs are believed to contribute to peripheral immunological tolerance against self-antigens (Sanchez-Sanchez et al., 2006) Dendritic cells and T-cell mediated immunity Naïve T lymphocytes rely on interactions with APCs for their differentiation and expansion in effector T cells. DCs deliver three key signals required for the clonal expansion and differentiation of T cells: Signal 1: MHC/peptide complex associated with T-cell receptor (TCR) Signal 2: co-stimulatory signals required for the survival and expansion of T cells Signal 3: co-stimulatory signals involved in directing the differentiation into different subsets of effector T cells T-cell subsets While the priming of CD8 + T cells results in a single set of effector cells, namely the cytotoxic T lymphocytes (CTL), the differentiation pathway of the CD4 + subpopulation is more complex giving rise to several types of T helper cells, namely the T H 1, T H 2 or T regulatory cells. T H 1 cells are characterised by the secretion of IFN-, IL-2, TNF- and TNF-, enhancing the bactericidal activity of macrophages for the eradication of intracellular pathogens. The predominant inducers of a T H 1 differentiation by DCs are IL-12 and IFN-. On the other hand, IL-4, IL-5, IL-6 and IL-13 are the major cytokines secreted by T H 2 cells, optimal for the production of antibodies, and are involved in the elimination of extracellular pathogens, including helminthes and nematodes. The differentiation of T H 2 cells is promoted by the presence of PGE 2, TNF-, IL-1 and TGF-
12 6 (transforming growth factor). With regard to T regulatory cells involved in immunological tolerance, the synthesis of IL-10 has been shown to promote their differentiation in the absence of costimulatory molecules by DCs Interleukin-12 Secretion of IL-12 is essential to resist infections against bacteria and parasites. Activation of an antigen-specific T H 1 response represents its major role. As a potent inducer of IFN- secretion by natural killer (NK) cells and T cells, it favours the differentiation and proliferation of precursor T helper cells into effector T cells. DCs have been found to be one of the main producers of IL-12. Recent studies have shown that IL-12 also possesses anti-tumour functions. However, the exact mechanisms involved are not fully understood. Unlike its effects on T helper cells, IL-12 exerts no polarising effects on the differentiation of CD8 + T cells, but was found to increase their cytotoxic potential and functional avidity (antigen sensitivity) - an important aspect to be considered in antitumour regimes (Xu et al., 2006). The bioactive form of IL-12 is a covalently linked heterodimer cytokine formed by a p35 subunit (also called IL-12, a 35 kda light chain) and a p40 subunit (the heavy 40 kda chain, also called IL-12 ), which is secreted by activated APCs, including macrophages, monocytes and DCs. Although IL-12 is predominantly produced by DCs upon CD40 ligation while interacting with T H 1 cells, IFN- or IL-4 have also been found to be required for its secretion (Snidjers et al., 1998). Regarding the IL-12 receptor, it consists of the IL-12R- 1 and the IL-12-2 polypeptide chains (Presky et al., 1996), mainly expressed by T cells and NK cells. They have been found lately to be additionally expressed by B cells. Interestingly, the IL-12 receptor is absent in most resting T cells, and is up-regulated upon its activation mediated by the T cell receptor.
13 Clinical applications of dendritic cells Steinman s publication about the potential roles of DCs in clinical medicine considered the following three aspects (Steinman et al. 2007): Roles of DCs in clinical medicine Modulation of immune responses - Resistance to infection - Resistance to cancer - Tolerance induction Disease development - Autoimmunity - Graft-vs-Host reaction - Immune evasion - Tumour pathogenesis Disease treatment - DC-based immunotherapy Dendritic cells and tolerance One of the fascinating features of the adaptive immune system is its ability to discriminate between self and non-self. DCs play an important role in central as well as peripheral tolerance. By inducing negative clonal selection during T cell development, they ensure the elimination of T lymphocytes recognising self-antigens on thymic cells. In the context of peripheral tolerance, tolerogenic DCs are involved in the induction of anergy (T cells are refractory to activation, due to the absence of co-stimulatory molecules) or deletion of autoreactive T cells (Hawiger et al., 2001) Dendritic cells and clinical immunology Considering their pivotal functions in controlling immunity, DCs also play a role in the development of autoimmune diseases, transplantation, immunodeficiency as well as resistance to infection and to tumours. For instance, increased numbers and activations of DCs have been observed in patients with psoriasis and rheumatoid arthritis. Moreover, DCs have been found to be the source of cytokine over-production associated with autoimmunity (Banchereau et al., 2006). Correspondingly, excessive TNF- was observed in rheumatoid arthritis and psoriasis (Lowes et al., 2005). Likewise, plasmocytoid DCs were found to release large amounts of type I IFN in systemic lupus erythematosus (Benett et al., 2003). In transplantation, DCs have been described
14 8 as the key initiators of T-cell induced responses in graft versus host reactions; recipient DCs were found to capture graft antigens and stimulate alloreactive T lymphocytes. Additionally, DCs are believed to participate in the development of cancer. Tumours suppress immunity by several pathways, and are capable of evading the immune system by exploiting DCs. For instance, tumours have been demonstrated to condition DCs to form suppressive T cells like FOXP3 + (Ghiringhelli et al., 2005) or IL-13-producing CD4 + T cells (Aspord et al., 2007). The secretion of IL-6, vascular endothelial growth factor (VEGF) and IL-10 by tumour cells have also been reported to exert inhibitory effects on DCs (Steinman et al., 2007). On the other hand, DCs infiltrating colon and basal-cell cancers were found to be CD80- and CD83-deficient, emphasizing the necessity of functional DCs to mount an antigen-t cell anti-tumour response Dendritic cell-based cancer immunotherapy In comparison to conventional anti-tumour regimes, the advantages of immunotherapy lie in their non-toxic and specific effects. T-cell mediated immunity is thus a potent therapeutical approach to consider in the treatment of cancer. DCs represent optimal candidates for the treatment of cancer based on the following facts (Steinman et al., 2007): DCs have been detected in tumours tumour cells express molecularly defined antigens DCs are capable of presenting tumour antigens and activating different arms of cell-mediated resistance, namely NK cells and T cells ex vivo generated DCs retain their immuno-stimulatory capacity in cancer patients DC-based vaccines can induce long-term immunity and tumour protection in vivo The induction of a T-cell mediated anti-tumour response can be achieved by two DC-based approaches. In the first approach, ex vivo generated DCs are loaded with tumour antigens, and reinjected in the patient. The second strategy is based on the direct targeting of DCs in vivo. However, despite the induction of T-cell responses and some cases of tumour regression observed in early clinical trials with DC vaccines, relevant clinical responses and effects on survival are reported only very rarely (Steinman et al., 2007).
15 Isolation of dendritic cells DCs can be isolated directly from peripheral blood, or generated in vitro from CD34 + hematogenic stem cells or from CD14 + monocytes. Monocytes can be isolated from peripheral blood, buffy coats or leukapheresis by plastic adherence, immunomagnetic selection or elutriation. Alternatively, DCs can be expanded in vivo by injections with cytokines termed DC-poietins including Flt3-ligand, GM-CSF and G-CSF (Maraskovsky et al., 1996; Pulendran et al., 1999). Their scarcity (accounting for only 0.1 % of the mononuclear cells) and the difficulty encountered in isolating and maintaining them in culture represented the two major obstacles for experimental and clinical use of peripheral blood DCs in early trials. To date, the gold standard is based on the generation of monocyte-derived DCs in vitro from peripheral blood : monocytes are isolated from the peripheral blood mononuclear cells and cultured for 5-7 days with GM-CSF and IL-4 (Sallutsto et al., 1994; Romani et al., 1994), followed by stimulation for another two days with pro-inflammatory mediators (Jonuleit et al., 1997) Stimuli used for dendritic cell maturation in vitro Pro-inflammatory mediators: Prostaglandin E 2, tumour necrosis factor- and interleukin-1 Physiologically, pro-inflammatory mediators are secreted mainly by monocytes and macrophages at inflammatory sites. Previous studies of our group demonstrated that single pro-inflammatory mediators were incapable of inducing phenotypic maturation of monocyte-derived DCs. However, PGE 2 and TNF- acted synergistically in inducing full DC maturation, and the supplementation with IL1- enhanced the IL-12 secretory potential of DCs (Dauer et al., 2003). On the other hand, IL-6 was found to be indispensable in the differentiation of FastDC. PGE 2 is one of the most reliable and powerful mediators known to induce maturation of DCs. More importantly, it has been shown to be indispensable for the development of migratory capacities of DCs by regulating the sensitivity of CCR7; the exact mechanisms involved are not fully understood. Its signalling cascade involves G-proteins, mediated by the subunits EP4 (prostaglandin E receptor) and EP2 receptors in humans (Legler et al., 2006). IFN- is a cytokine with antiviral properties secreted predominantly by plasmacytoid DCs. Excessive IFN- in the serum of systemic lupus erythematosus patients was reported to induce the
16 10 differentiation of monocytes into DCs (Blanco et al., 2001). In vitro studies with monocyte-derived DCs showed that IFN- induced maturation when supplemented with other cytokines (Luft et al., 2002). Furthermore, the supplementation of IFN- was shown to enhance survival and prevent the reversion of DCs to an immature phenotype (Dauer et al., 2006) Pathogen-derived signals: Toll-like receptors Toll-like receptors (TLRs) are innate receptors that sense microbial products and trigger DC maturation and cytokine production. To date, twelve TLRs have been identified in mammals, and each of them is stimulated by a distinct set of microbial compounds. TLRs are composed of integral membrane glycoproteins with extracellular domains containing varying numbers of leucinerich repeats and a cytoplasmic signalling domain homologous to the IL-1 receptor, called the Toll/IL-1R domain (TIR domain) (Bowie et al., 2000). Although TLRs are expressed by a large variety of cells including macrophages, B cells, T cells, and non-immune cells such as fibroblasts and epithelial cells, DCs exhibit the broadest repertoire of TLRs. Unlike other receptors recognising microbial ligands, only TLRs are capable of inducing DC maturation directly. Localised in different cellular compartments, they are expressed in a differential manner in distinct DC subsets. Myeloid DCs express all TLRs except TLR7 and TLR9, which are expressed selectively by plasmacytoid DCs (Jarossay et al., 2001). While most of the TLRs are expressed at the cell surface, TLR7, TLR8 and TLR9 are localised in endosomes. However, the exact intracellular localisation of TLR3 remains to be determined (Napolitani et al., 2005). Table 1 gives a summary of the different TLRs as well as their corresponding ligands.
17 11 Table 1: Microbial components Species TLR usage Bacteria LPS Gram negative bacteria TLR4 Diacyl lipopeptides Mycoplasma TLR6/TLR2 LTA Group B Streptococcus TLR6/TLR2 Triacyl lipopeptides Bacteria and mycobacteria TLR1/TLR2 Porins Neisseria TLR2 Flagellin Flagellated bacteria TLR5 CpG-DNA Bacteria and mycobacteria TLR9 Not determined Uropathogenic bacteria TLR11 Viruses DNA Viruses TLR9 dsrna Viruses TLR3 ssrna RNA viruses TLR7 and TLR8 Hemagglutinin protein Measles virus TLR2 Envelope proteins RSV TLR4 Fungi Mannan Candida albicans TLR4 Zymosan Saccharomyces cerevisiae TLR6/TRL2 Glucuronoxylomannan Cryptococcus neoformans TLR2 and TLR4 Parasites Glycoinositolphospholipids Trypanosoma TLR2 Hemozoin Plasmodium TLR9 Profilin-like molecule Toxoplasma gondii TLR11 (modified from Akira et al., 2006) The engagement of TLRs by microbial components triggers the activation of signalling cascades, which initiates the induction of the gene expression of pro-inflammatory mediators, involved in antimicrobial host defence. The two signalling pathways identified in TLRs are the inflammatory MyD88-dependent pathway and the interferon-dependent pathway. The inflammatory signalling
18 12 pathway acts via the adapter molecule, MyD88 (myeloid differentiation factor 88), binding to the cytoplasmic portion of all TLRs except TLR3, or TIRAP (Toll-like receptor adaptor protein), which binds only TLR2 and TLR4. Both lead eventually to the activation of NF- B (nuclear factor kappalight-chain-enhancer of activated B cells) (Fitzgerald et al., 2001). The activation of NF- B via TLRs results in the secretion of mediators such as IL1, IL6, IL12 and TNF-. On the other hand, via the MyD88-independent pathway, IFN- or IFN- are secreted in response to stimulation with TLR3, 4, 7, and 9 (Akira et al., 2006). The release of these cytokines is a key process channelling signals of the innate system to the induction of a cellular response. The set of TLRs stimulated determines the cytokine profile induced, resulting in diverse adaptive immune responses. Interestingly, it has been demonstrated that the maximum cytokine production was induced by a combination of TLR agonists as compared with single TLR agonists. TLR synergy was equally observed in the T H 1 polarising capacity of DCs (Napolitani et al., 2005). In the experiments described below, the TLR agonists R848 and LPS were used as microbialderived signals for DC maturation. The physiological ligands for human TLR8 have been identified as GU-rich ssrna (Heil et al., 2004; Diebold et al., 2004), whereas the synthetic nucleoside analogs binding to TLR7/8 comprise imiquimod (R837) and resiquimod (R848), as well as the guanine nucleotide analogs like loxoribine. Showing high homology, TLR7 and TLR8, recognise viral ssrna with different but overlapping specificities. TLR8-activation results in the induction of type I IFN secretion, acting antivirally. Additionally, their intracellular localization reflects their optimisation in detecting micro-organisms reaching the cytosolic compartments, as it is in the case in viral invasion. Clinically, TLR8 agonists are used for their antiviral properties. Lipopolysaccharides (LPS), recognised by the extracellular TLR4, were originally known as endotoxins, are compounds consisting of a lipid and polysaccharide part, found in the structural cell wall of Gram-negative bacteria. During infections, LPS is liberated from bacterial cell walls T-cell derived signals: CD40 ligand and interferon- CD40 ligand (CD40L) is a 50 kda glycoprotein of the TNF receptor superfamily, which is primarily expressed by T cells. It activates CD40-expressing DCs leading to the expression of high levels of co-stimulatory molecules. CD40-CD40 ligand interaction is additionally associated with an enhanced survival in DCs (Caux et al., 1994) and is indispensable in the priming and expansion of antigen-specific CD4 + T cells. IFN- is a potent antiviral cytokine, blocking viral replication and eliminating viruses from infected cells. Early studies have demonstrated that mice deficient in IFN- had impaired immune
19 13 responses in vivo, with an increased susceptibility to microbial pathogens and viruses (Szabo et al., 2003). While NK cells and T cells are the most potent sources of IFN-, macrophages, B cells and DCs have also been identified as IFN- -secreting cells. IFN- has been demonstrated to enhance the production of IL-12 by DCs, matured with either LPS or pro-inflammatory mediators (Vieira et al., 2000). IFN- polarises immature DCs to stimulate T H 1 cells. T H 1 cells secreting IFN- activate macrophages, thereby potentiating the resulting inflammatory response (Grewal et al., 1998) Short-term culture protocols During the past few years, it has been shown repeatedly that monocyte-derived DCs can be generated in a shorter time span than above. Short-term protocols using calcium-mobilising agents for maturation (Czerniecki et al., 1997) or maturation with IL-4 or IFN- (Dauer et al., 2003; Xu et al., 2003) have been described. The interest in short-term protocol is based on the assumption that a more rapid differentiation process represents more closely physiological conditions in vivo. On the other hand, in terms of methodology, short-term protocols confer the advantages of reducing costs and labour as well as the risks of contamination. Previously, in our working group, a novel protocol was established, whereby monocyte-derived DCs undergoing all the processes of DC-differentiation were generated within only 48 hours, referred to as FastDCs (Dauer et al., 2003). In this work, higher levels of co-stimulatory molecules were measured when moncocytes were incubated for 24 hours with GM-CSF and IL-4, and the conventional stimulatory combination, PGE 2, TNF- and IL1-, was added for further 24 hours of incubation, as compared with a single-step differentiation (GM-CSF and IL-4 plus conventional stimulatory combination added at the beginning of the culture for 48 hours). Additionally, it was found that monocytes cultured with GM-CSF or GM-CSF and pro-inflammatory mediators in the absence of IL-4 failed to develop DC features. Comparative analysis between the different pro-inflammatory mediators revealed that complete immunophenotypic DC maturation (CD83> 50%) was elicited only in combinations including PGE 2 and TNF-, or when IL-1 was substituted for TNF- in the presence of PGE 2. Moreover, IL-1 was found to synergise with PGE 2 and TNF- to induce the secretion of IL-12. In contrast, IL-6 was found to be superfluous in the maturation of FastDCs. IL-12 secretion is a key event in the activation of T cells and a critical requirement in DC-based immunotherapy. Low levels ofil-12 could be detected in mature FastDC, which was enhanced
20 14 upon addition of CD40L and IFN-. On the other hand, no IL-12p70 secretion could be induced unless supplemented by CD40 ligand and IFN-. With respect to their ability in activating CD8 + T cells in an antigen-specific manner, FastDCs and modcs were found to be equally capable of inducing T cell proliferation using tetanus toxoid (TT) as a model antigen. While comparable levels of IFN- were measured in the supernatants of both FastDC and modc, no IL-4 was detected in all supernatants. The functional characteristics of FastDCS and monocyte-derived DCs were further analysed in a comparative study (Dauer et al., 2005). Interestingly, in comparison to modcs, a higher yield with more than 95% purity and viability was obtained with FastDCs. Regarding their migratory capacities, both populations were readily capable of migrating in response to 6ckine. Likewise, FastDCs were found to be capable of equally priming tumour-antigen specific cytotoxic T cell responses as shown in a melanoma antigen model: While a higher lytic activity was observed in the FastDC population in the chromium release assay, comparable levels of IFN- -producing CD8 + T cells were measured in monocyte-derived DCs and FastDC. Though superior in FastDCs, only low levels of IL-12p70 could be detected. Considering that the maintenance of a mature DC phenotype while homing to the lymph node is a pre-requisite for T cell priming, the following set of experiments were performed : DC viability and immunophenotype were assessed in modcs cultured for additional 6 days without further supplementation of growth factors or cytokines (wash-out cultures) following maturation. Moreover, comparative studies were conducted to analyse the influence of CD40L, IFN- and IFN-. To this end, monocytes were cultured for 24 hours with GM-CSF and IL-4 on day 1, while maturation was induced with PGE 2, TNF-, IL-6 and IL1- for 36 hours. CD40 ligand and IFN- were added during the last 24 hours of maturation whereas IFN- was added on day 1: after 24 hours of maturation, 90% of DCs were alive and exhibited the typical mature DC immunophenotype CD83 + CD80 + CD86 high MHC high. An increased viability and enhanced maturational degree were observed in mature DCs supplemented with CD40 ligand and IFN-. Furthermore, their supplementation was associated with a lower re-expression of CD14 (monocytic phenotype). Supplementation with IFN- did not affect DC yield and survival, neither its ability to prime autologous naïve T cells or migratory potential. In contrast, a higher expression of co-stimulatory molecules was observed while CD14 re-expression was delayed. Both effects were more pronounced when CD40L and IFN- were added in the last 24 hours of incubation. IL-12p70 deficiency was observed in all wash-out cultures, independent of IFN- supplementation (Dauer et al., 2006).
Dendritic Cells: A Basic Review *last updated May 2003
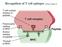
 *last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
*last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
TABLE OF CONTENT. Page ACKNOWLEDGEMENTS. iii ENGLISH ABSTRACT THAI ABSTRACT. vii LIST OF TABLES LIST OF FIGURES. xvi ABBREVIATIONS.
 x TABLE OF CONTENT ACKNOWLEDGEMENTS ENGLISH ABSTRACT THAI ABSTRACT LIST OF TABLES LIST OF FIGURES ABBREVIATIONS iii iv vii xv xvi xviii CHAPTER I: INTRODUCTION 1.1 Statement of problems 1 1.2 Literature
x TABLE OF CONTENT ACKNOWLEDGEMENTS ENGLISH ABSTRACT THAI ABSTRACT LIST OF TABLES LIST OF FIGURES ABBREVIATIONS iii iv vii xv xvi xviii CHAPTER I: INTRODUCTION 1.1 Statement of problems 1 1.2 Literature
Mouse IFN-gamma ELISpot Kit
 Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
Recognition of T cell epitopes (Abbas Chapter 6)
 Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
ELISA BIO 110 Lab 1. Immunity and Disease
 ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
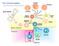 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
CFSE Cell Division Assay Kit
 CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens
 www.iqproducts.nl PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens IFN- γ PURE [RUO] [REF] IQP-160P s 50 tests FITC [RUO] [REF] IQP-160F s 50 tests R-PE [RUO] [REF] IQP-160R s 50
www.iqproducts.nl PRODUCT INFORMATION SHEET Monoclonal antibodies detecting human antigens IFN- γ PURE [RUO] [REF] IQP-160P s 50 tests FITC [RUO] [REF] IQP-160F s 50 tests R-PE [RUO] [REF] IQP-160R s 50
Hapten - a small molecule that is antigenic but not (by itself) immunogenic.
 Chapter 3. Antigens Terminology: Antigen: Substances that can be recognized by the surface antibody (B cells) or by the TCR (T cells) when associated with MHC molecules Immunogenicity VS Antigenicity:
Chapter 3. Antigens Terminology: Antigen: Substances that can be recognized by the surface antibody (B cells) or by the TCR (T cells) when associated with MHC molecules Immunogenicity VS Antigenicity:
2) Macrophages function to engulf and present antigen to other immune cells.
 Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Human CD4+T Cell Care Manual
 Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Chapter 43: The Immune System
 Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma
 On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
Drug Development Services
 Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
NCL Method ITA-14. Analysis of Nanoparticle Effects on Maturation of Monocyte Derived Dendritic Cells In Vitro
 NCL Method ITA-14 Analysis of Nanoparticle Effects on Maturation of Monocyte Derived Dendritic Cells In Vitro Nanotechnology Characterization Laboratory Frederick National Laboratory for Cancer Research
NCL Method ITA-14 Analysis of Nanoparticle Effects on Maturation of Monocyte Derived Dendritic Cells In Vitro Nanotechnology Characterization Laboratory Frederick National Laboratory for Cancer Research
Activation and effector functions of HMI
 Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Understanding the immune response to bacterial infections
 Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Introduction to flow cytometry
 Introduction to flow cytometry Flow cytometry is a popular laser-based technology. Discover more with our introduction to flow cytometry. Flow cytometry is now a widely used method for analyzing the expression
Introduction to flow cytometry Flow cytometry is a popular laser-based technology. Discover more with our introduction to flow cytometry. Flow cytometry is now a widely used method for analyzing the expression
International Beryllium Conference, Montreal, Canada March 10, 2005
 Alternative Lymphocyte Proliferation Tests: BrdU and Flow Cytometry Based Tests International Beryllium Conference, Montreal, Canada March 10, 2005 Tim K. Takaro Department of Environmental and Occupational
Alternative Lymphocyte Proliferation Tests: BrdU and Flow Cytometry Based Tests International Beryllium Conference, Montreal, Canada March 10, 2005 Tim K. Takaro Department of Environmental and Occupational
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159. Date Submitted: 12-11-09
 Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
B cell activation and Humoral Immunity
 B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
Basic Science in Medicine
 Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
Introduction to Flow Cytometry
 Outline Introduction to Flow Cytometry Basic Concept of Flow Cytometry Introduction to Instrument Subsystems Daisy Kuo Assistant Product Manager E-mail: daisy_kuo@bd.com BDBiosciences Application Examples
Outline Introduction to Flow Cytometry Basic Concept of Flow Cytometry Introduction to Instrument Subsystems Daisy Kuo Assistant Product Manager E-mail: daisy_kuo@bd.com BDBiosciences Application Examples
CONTENT. Chapter 1 Review of Literature. List of figures. List of tables
 Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
The Body s Defenses CHAPTER 24
 CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS
 CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Chapter 18: Applications of Immunology
 Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES JASON CYSTER SECTION 13
 SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
B Cell Generation, Activation & Differentiation. B cell maturation
 B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
STANDARD OPERATING PROCEDURE
 Title: Lymphocyte Proliferation Assay (LPA) Using 3 H- Thymidine Incorporation Assay Core Name: Lloyd Mayer, Mount Sinai Medical Center Effective Date: 02/16/2012 Trial Number: ITN047AI SOP # ITN2800 SOP
Title: Lymphocyte Proliferation Assay (LPA) Using 3 H- Thymidine Incorporation Assay Core Name: Lloyd Mayer, Mount Sinai Medical Center Effective Date: 02/16/2012 Trial Number: ITN047AI SOP # ITN2800 SOP
Human Peripheral Blood Mononuclear Cell (PBMC) Manual
 Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
PROTOCOL. Immunostaining for Flow Cytometry. Background. Materials and equipment required.
 PROTOCOL Immunostaining for Flow Cytometry 1850 Millrace Drive, Suite 3A Eugene, Oregon 97403 Rev.0 Background The combination of single cell analysis using flow cytometry and the specificity of antibody-based
PROTOCOL Immunostaining for Flow Cytometry 1850 Millrace Drive, Suite 3A Eugene, Oregon 97403 Rev.0 Background The combination of single cell analysis using flow cytometry and the specificity of antibody-based
Uses of Flow Cytometry
 Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer
 APPLICATION NOTE Attune NxT Flow Cytometer No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer Introduction Standard methods for isolating and detecting leukocytes
APPLICATION NOTE Attune NxT Flow Cytometer No-wash, no-lyse detection of leukocytes in human whole blood on the Attune NxT Flow Cytometer Introduction Standard methods for isolating and detecting leukocytes
Instructions. Torpedo sirna. Material. Important Guidelines. Specifications. Quality Control
 is a is a state of the art transfection reagent, specifically designed for the transfer of sirna and mirna into a variety of eukaryotic cell types. is a state of the art transfection reagent, specifically
is a is a state of the art transfection reagent, specifically designed for the transfer of sirna and mirna into a variety of eukaryotic cell types. is a state of the art transfection reagent, specifically
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
Lab 2. Isolation of mononuclear cells from peripheral blood and separation into subpopulations
 Lab 2 Isolation of mononuclear cells from peripheral blood and separation into subpopulations Supervisors: Sissela Broos sissela.broos@immun.lth.se tel: 222 96 78 Niclas Olsson niclas.olsson@immun.lth.se
Lab 2 Isolation of mononuclear cells from peripheral blood and separation into subpopulations Supervisors: Sissela Broos sissela.broos@immun.lth.se tel: 222 96 78 Niclas Olsson niclas.olsson@immun.lth.se
Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells
 Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells Mary E. Kopechek Honor s Research Thesis May 17, 2007 Research Advisor: Dr. Jeff Lakritz, DVM, PhD The Ohio State
Expression of CD163 on Bovine Alveolar Macrophages and Peripheral Blood Mononuclear Cells Mary E. Kopechek Honor s Research Thesis May 17, 2007 Research Advisor: Dr. Jeff Lakritz, DVM, PhD The Ohio State
ArC Amine Reactive Compensation Bead Kit
 ArC Amine Reactive Compensation Bead Kit Catalog no. A1346 Table 1. Contents and storage information. Material Amount Composition Storage Stability ArC reactive beads (Component A) ArC negative beads (Component
ArC Amine Reactive Compensation Bead Kit Catalog no. A1346 Table 1. Contents and storage information. Material Amount Composition Storage Stability ArC reactive beads (Component A) ArC negative beads (Component
KMS-Specialist & Customized Biosimilar Service
 KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
The Four Pillars of Cancer Therapy
 Improving the Overall Understanding of Immunotherapy in Multiple Myeloma Webinar 2, August 19, 2015 Myeloma Vaccines: A New Use of a Time-Tested Treatment The Four Pillars of Cancer Therapy Surgery Radiation
Improving the Overall Understanding of Immunotherapy in Multiple Myeloma Webinar 2, August 19, 2015 Myeloma Vaccines: A New Use of a Time-Tested Treatment The Four Pillars of Cancer Therapy Surgery Radiation
Basics of Immunology
 Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Chapter 3. Immunity and how vaccines work
 Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 16: Innate Immunity
 Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Application Note 10. Measurement of Cell Recovery. After Sorting with a Catcher-Tube-Based. Cell Sorter. Introduction
 Application Note 10 Measurement of Cell Recovery After Sorting with a Catcher-Tube-Based Cell Sorter Introduction In many experiments using sorted cells, it is important to be able to count the number
Application Note 10 Measurement of Cell Recovery After Sorting with a Catcher-Tube-Based Cell Sorter Introduction In many experiments using sorted cells, it is important to be able to count the number
The Immune System. 2 Types of Defense Mechanisms. Lines of Defense. Line of Defense. Lines of Defense
 The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES
 Introduction to immunology. LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES Today we will get to know: The antibodies How antibodies are produced, their classes and their maturation processes Antigen recognition
Introduction to immunology. LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES Today we will get to know: The antibodies How antibodies are produced, their classes and their maturation processes Antigen recognition
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer
 Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Minimal residual disease detection in Acute Myeloid Leukaemia on a Becton Dickinson flow cytometer Purpose This procedure gives instruction on minimal residual disease (MRD) detection in patients with
Introduction to Flow Cytometry
 Introduction to Flow Cytometry presented by: Flow Cytometry y Core Facility Biomedical Instrumentation Center Uniformed Services University Topics Covered in this Lecture What is flow cytometry? Flow cytometer
Introduction to Flow Cytometry presented by: Flow Cytometry y Core Facility Biomedical Instrumentation Center Uniformed Services University Topics Covered in this Lecture What is flow cytometry? Flow cytometer
Transfection reagent for visualizing lipofection with DNA. For ordering information, MSDS, publications and application notes see www.biontex.
 METAFECTENE FluoR Transfection reagent for visualizing lipofection with DNA For ordering information, MSDS, publications and application notes see www.biontex.com Description Cat. No. Size METAFECTENE
METAFECTENE FluoR Transfection reagent for visualizing lipofection with DNA For ordering information, MSDS, publications and application notes see www.biontex.com Description Cat. No. Size METAFECTENE
Classic Immunoprecipitation
 292PR 01 G-Biosciences 1-800-628-7730 1-314-991-6034 technical@gbiosciences.com A Geno Technology, Inc. (USA) brand name Classic Immunoprecipitation Utilizes Protein A/G Agarose for Antibody Binding (Cat.
292PR 01 G-Biosciences 1-800-628-7730 1-314-991-6034 technical@gbiosciences.com A Geno Technology, Inc. (USA) brand name Classic Immunoprecipitation Utilizes Protein A/G Agarose for Antibody Binding (Cat.
Core Topic 2. The immune system and how vaccines work
 Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
Final Review. Aptamers. Making Aptamers: SELEX 6/3/2011. sirna and mirna. Central Dogma. RNAi: A translation regulation mechanism.
 Central Dogma Final Review Section Week 10 DNA RNA Protein DNA DNA replication DNA RNA transcription RNA Protein translation **RNA DNA reverse transcription http://bass.bio.uci.edu/~hudel/bs99a/lecture20/lecture1_1.html
Central Dogma Final Review Section Week 10 DNA RNA Protein DNA DNA replication DNA RNA transcription RNA Protein translation **RNA DNA reverse transcription http://bass.bio.uci.edu/~hudel/bs99a/lecture20/lecture1_1.html
1) Siderophores are bacterial proteins that compete with animal A) Antibodies. B) Red blood cells. C) Transferrin. D) White blood cells. E) Receptors.
 Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Generation of EBV-immortalized B cell lines
 UCANU 0014 Version November 01, 2011 Page 1 van 6 Generation of EBVimmortalized B cell lines CMCI (Center for molecular and Cellular Intervention) University Medical Center Utrecht Written by Name Function
UCANU 0014 Version November 01, 2011 Page 1 van 6 Generation of EBVimmortalized B cell lines CMCI (Center for molecular and Cellular Intervention) University Medical Center Utrecht Written by Name Function
Standard Operating Procedure
 1.0 Purpose: 1.1 The characterisation of of main leukocyte subsets in peripheral blood cells from mice by flow cytometry. Reliable values of frequencies of leukocyte clusters are very much dependent on
1.0 Purpose: 1.1 The characterisation of of main leukocyte subsets in peripheral blood cells from mice by flow cytometry. Reliable values of frequencies of leukocyte clusters are very much dependent on
TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS.
 TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS. The nomenclature of cytokines partly reflects their first-described function and also the order of their discovery. There is no single unified nomenclature,
TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS. The nomenclature of cytokines partly reflects their first-described function and also the order of their discovery. There is no single unified nomenclature,
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
Immunophenotyping peripheral blood cells
 IMMUNOPHENOTYPING Attune Accoustic Focusing Cytometer Immunophenotyping peripheral blood cells A no-lyse, no-wash, no cell loss method for immunophenotyping nucleated peripheral blood cells using the Attune
IMMUNOPHENOTYPING Attune Accoustic Focusing Cytometer Immunophenotyping peripheral blood cells A no-lyse, no-wash, no cell loss method for immunophenotyping nucleated peripheral blood cells using the Attune
CD3/TCR stimulation and surface detection Determination of specificity of intracellular detection of IL-7Rα by flow cytometry
 CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
SCANTIBODIES Laboratory, Inc. Contract Monoclonal Antibody Production
 A Technical Publication of SCANTIBODIES Laboratory, Inc. Volume 1 Number 4 9336 Abraham Way Santee, CA 92071 USA (619) 258-9300 fax (619) 258-9366 www.scantibodies.com SCANTIBODIES Laboratory, Inc. Contract
A Technical Publication of SCANTIBODIES Laboratory, Inc. Volume 1 Number 4 9336 Abraham Way Santee, CA 92071 USA (619) 258-9300 fax (619) 258-9366 www.scantibodies.com SCANTIBODIES Laboratory, Inc. Contract
Immunity and how vaccines work
 1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
Your partner in immunology
 Your partner in immunology Expertise Expertise Reactivity Reactivity Quality Quality Advice Advice Who are we? Specialist of antibody engineering Covalab is a French biotechnology company, specialised
Your partner in immunology Expertise Expertise Reactivity Reactivity Quality Quality Advice Advice Who are we? Specialist of antibody engineering Covalab is a French biotechnology company, specialised
HBV Quantitative Real Time PCR Kit
 Revision No.: ZJ0002 Issue Date: Aug 7 th, 2008 HBV Quantitative Real Time PCR Kit Cat. No.: HD-0002-01 For Use with LightCycler 1.0/LightCycler2.0/LightCycler480 (Roche) Real Time PCR Systems (Pls ignore
Revision No.: ZJ0002 Issue Date: Aug 7 th, 2008 HBV Quantitative Real Time PCR Kit Cat. No.: HD-0002-01 For Use with LightCycler 1.0/LightCycler2.0/LightCycler480 (Roche) Real Time PCR Systems (Pls ignore
EdU Flow Cytometry Kit. User Manual
 User Manual Ordering information: (for detailed kit content see Table 2) EdU Flow Cytometry Kits for 50 assays: Product number EdU Used fluorescent dye BCK-FC488-50 10 mg 6-FAM Azide BCK-FC555-50 10 mg
User Manual Ordering information: (for detailed kit content see Table 2) EdU Flow Cytometry Kits for 50 assays: Product number EdU Used fluorescent dye BCK-FC488-50 10 mg 6-FAM Azide BCK-FC555-50 10 mg
Flow Cytometry. What is Flow Cytometry? What Can a Flow Cytometer Tell Us About a Cell? Particle Size. Flow = Fluid Cyto = Cell Metry = Measurement
 What is Flow Cytometry? Flow Cytometry Basic Principle and Applications BD Biosciences Daisy Kuo (daisy_kuo@bd.com) Flow = Fluid Cyto = Cell Metry = Measurement A variety of measurements are made on cells,
What is Flow Cytometry? Flow Cytometry Basic Principle and Applications BD Biosciences Daisy Kuo (daisy_kuo@bd.com) Flow = Fluid Cyto = Cell Metry = Measurement A variety of measurements are made on cells,
The role of IBV proteins in protection: cellular immune responses. COST meeting WG2 + WG3 Budapest, Hungary, 2015
 The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types:
 Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Immuno-Oncology Therapies to Treat Lung Cancer
 Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Modelling and analysis of T-cell epitope screening data.
 Modelling and analysis of T-cell epitope screening data. Tim Beißbarth 2, Jason A. Tye-Din 1, Gordon K. Smyth 1, Robert P. Anderson 1 and Terence P. Speed 1 1 WEHI, 1G Royal Parade, Parkville, VIC 3050,
Modelling and analysis of T-cell epitope screening data. Tim Beißbarth 2, Jason A. Tye-Din 1, Gordon K. Smyth 1, Robert P. Anderson 1 and Terence P. Speed 1 1 WEHI, 1G Royal Parade, Parkville, VIC 3050,
Overview. Transcriptional cascades. Amazing aspects of lineage plasticity. Conventional (B2) B cell development
 Overview B cell development Transcriptional cascades Amazing aspects of lineage plasticity Conventional (B2) B cell development What happens to an autoreactive B cell? B1 vs B2 cells Key anatomical sites
Overview B cell development Transcriptional cascades Amazing aspects of lineage plasticity Conventional (B2) B cell development What happens to an autoreactive B cell? B1 vs B2 cells Key anatomical sites
Enhancing Anti-Tumor Activity of Checkpoint Inhibition
 Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual
 Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual INSTRUCTION MANUAL ZBM0065.03 SHIPPING CONDITIONS Human Umbilical Cord Blood CD34+ Progenitor Cells, cryopreserved Cryopreserved human umbilical
Human Umbilical Cord Blood CD34 + Progenitor Cell Care Manual INSTRUCTION MANUAL ZBM0065.03 SHIPPING CONDITIONS Human Umbilical Cord Blood CD34+ Progenitor Cells, cryopreserved Cryopreserved human umbilical
STEMCELL Quality Control Kits
 STEMCELL Quality Control Kits i Table of Contents 1.0 Introduction...1 2.0 Thawing Cells, Plating and Colony Enumeration...2 2.1 Supplies and reagents included in the QC kit...2 2.2 Additional reagents
STEMCELL Quality Control Kits i Table of Contents 1.0 Introduction...1 2.0 Thawing Cells, Plating and Colony Enumeration...2 2.1 Supplies and reagents included in the QC kit...2 2.2 Additional reagents
MACS cell separation - the faster way to ultrapure, Dr. Katharina Winnemoeller katharinaw@miltenyibiotec.com.au
 MACS cell separation - the faster way to ultrapure, viable cells + Dr. Katharina Winnemoeller katharinaw@miltenyibiotec.com.au About us Germany's largest independent, privately owned biotech company 1300
MACS cell separation - the faster way to ultrapure, viable cells + Dr. Katharina Winnemoeller katharinaw@miltenyibiotec.com.au About us Germany's largest independent, privately owned biotech company 1300
RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method)
 Immune Tolerance Network RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method) Author: Paul Wallace, Director, RPCI Laboratory of Flow Cytometry Approved by: Paul
Immune Tolerance Network RPCI 004 v.002 Staining Procedure For all Directly Conjugated Reagents (Whole Blood Method) Author: Paul Wallace, Director, RPCI Laboratory of Flow Cytometry Approved by: Paul
Serology: Fluorescent antibody tests and other tests employing conjugated antibodies
 Serology: Fluorescent antibody tests and other tests employing conjugated antibodies Authors: Adapted by Prof M van Vuuren. Originally compiled by Dr RW Worthington. (Retired) Licensed under a Creative
Serology: Fluorescent antibody tests and other tests employing conjugated antibodies Authors: Adapted by Prof M van Vuuren. Originally compiled by Dr RW Worthington. (Retired) Licensed under a Creative
LAB 14 ENZYME LINKED IMMUNOSORBENT ASSAY (ELISA)
 STUDENT GUIDE LAB 14 ENZYME LINKED IMMUNOSORBENT ASSAY (ELISA) GOAL The goal of this laboratory lesson is to explain the concepts and technique of enzyme linked immunosorbent assay (ELISA). OBJECTIVES
STUDENT GUIDE LAB 14 ENZYME LINKED IMMUNOSORBENT ASSAY (ELISA) GOAL The goal of this laboratory lesson is to explain the concepts and technique of enzyme linked immunosorbent assay (ELISA). OBJECTIVES
Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory
 Immunology and Cell Biology (1999) 77, 559 564 Special Feature Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory DA FULCHER
Immunology and Cell Biology (1999) 77, 559 564 Special Feature Carboxyfluorescein succinimidyl ester-based proliferative assays for assessment of T cell function in the diagnostic laboratory DA FULCHER
WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS
 FOR IN-VITRO DIAGNOSTIC USE INVITROGEN CAL-LYSE TM Lysing Solution WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS CAL-LYSE TM CATALOG No. GAS-010 250 tests 25 ml CATALOG No. GAS-010S-100
FOR IN-VITRO DIAGNOSTIC USE INVITROGEN CAL-LYSE TM Lysing Solution WHOLE BLOOD LYSING SOLUTION FOR FLOW CYTOMETRIC APPLICATIONS CAL-LYSE TM CATALOG No. GAS-010 250 tests 25 ml CATALOG No. GAS-010S-100
Assays to evaluate cell-mediated immunity. Guus Rimmelzwaan Department of Virology Erasmus Medical Center Rotterdam The Netherlands
 Assays to evaluate cell-mediated immunity Guus Rimmelzwaan Department of Virology Erasmus Medical Center Rotterdam The Netherlands CBER/NIAID/WHO, Bethesda MD, December 11 2007 A working model of an antiviral
Assays to evaluate cell-mediated immunity Guus Rimmelzwaan Department of Virology Erasmus Medical Center Rotterdam The Netherlands CBER/NIAID/WHO, Bethesda MD, December 11 2007 A working model of an antiviral
Human Adult Mesothelial Cell Manual
 Human Adult Mesothelial Cell Manual INSTRUCTION MANUAL ZBM0025.01 SHIPPING CONDITIONS Human Adult Mesothelial Cells Orders are delivered via Federal Express courier. All US and Canada orders are shipped
Human Adult Mesothelial Cell Manual INSTRUCTION MANUAL ZBM0025.01 SHIPPING CONDITIONS Human Adult Mesothelial Cells Orders are delivered via Federal Express courier. All US and Canada orders are shipped
ΔΕΝΤΡΙΤΙΚΑ ΚΥΤΤΑΡΑ ΚΑΙ ΕΜΒΟΛΙΑ ΓΙΑ ΤΟΝ ΚΑΡΚΙΝΟ DENDRITIC CELLS AND CANCER VACCINES
 ΔΕΝΤΡΙΤΙΚΑ ΚΥΤΤΑΡΑ ΚΑΙ ΕΜΒΟΛΙΑ ΓΙΑ ΤΟΝ ΚΑΡΚΙΝΟ DENDRITIC CELLS AND CANCER VACCINES David Hunt. Cell Systems Initiative, U. of Washington. Βαίος Καρανίκας EU Marie Curie Fellow Μοναδα Ανοσολογίας Καρκίνου
ΔΕΝΤΡΙΤΙΚΑ ΚΥΤΤΑΡΑ ΚΑΙ ΕΜΒΟΛΙΑ ΓΙΑ ΤΟΝ ΚΑΡΚΙΝΟ DENDRITIC CELLS AND CANCER VACCINES David Hunt. Cell Systems Initiative, U. of Washington. Βαίος Καρανίκας EU Marie Curie Fellow Μοναδα Ανοσολογίας Καρκίνου
3D Cell Culture mimsys G
 3D Cell Culture mimsys G xeno-free & nutrient permeable hydrogel for 3D cell culture mimsys G is a xeno-free and non-immunogenic, easy to handle hydrogel for cell encapsulation in 3D experiments in vitro
3D Cell Culture mimsys G xeno-free & nutrient permeable hydrogel for 3D cell culture mimsys G is a xeno-free and non-immunogenic, easy to handle hydrogel for cell encapsulation in 3D experiments in vitro
Diane Kadidlo MT(ASCP) SBB University of Minnesota Joanna Stanson, M.S. University of Pittsburgh
 Production Records & Documentation Diane Kadidlo MT(ASCP) SBB University of Minnesota Joanna Stanson, M.S. University of Pittsburgh Production Records This Session: Production Records Basic Elements Regulatory
Production Records & Documentation Diane Kadidlo MT(ASCP) SBB University of Minnesota Joanna Stanson, M.S. University of Pittsburgh Production Records This Session: Production Records Basic Elements Regulatory
Automation of Cell Staining Technical Information Bulletin
 Automation of Cell Staining Technical Information Bulletin Automation of Cell Staining Using the Biomek 4000 Laboratory Automation Workstation Amy N. Yoder, Sr. Development Scientist and Li Liu, Sr. Development
Automation of Cell Staining Technical Information Bulletin Automation of Cell Staining Using the Biomek 4000 Laboratory Automation Workstation Amy N. Yoder, Sr. Development Scientist and Li Liu, Sr. Development
Interim Progress Report R&D Project 348. Development of a Field Test Kit for Detection of Blue-Green Algal Toxins
 Interim Progress Report R&D Project 348 Development of a Field Test Kit for Detection of Blue-Green Algal Toxins Biocode Limited November 1992 R&D 348/04/A ENVIRONMENT AGENCY 135357 CONTENTS SUMMARY KEYWORDS
Interim Progress Report R&D Project 348 Development of a Field Test Kit for Detection of Blue-Green Algal Toxins Biocode Limited November 1992 R&D 348/04/A ENVIRONMENT AGENCY 135357 CONTENTS SUMMARY KEYWORDS
Welcome to Mini Med School at the Child & Family Research Institute
 Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
Cytotoxic T Lymphocytes (CTLs) and NK Cells. Effector T cells. After activation, naïve T cells differentiate into effector and memory T cells
 After activation, naïve T cells differentiate into effector and memory T cells Cytotoxic T Lymphocytes (CTLs) and NK Cells After activation, T cells remain in lymph nodes for 5-6 days Effector T cells
After activation, naïve T cells differentiate into effector and memory T cells Cytotoxic T Lymphocytes (CTLs) and NK Cells After activation, T cells remain in lymph nodes for 5-6 days Effector T cells
Amaxa Mouse T Cell Nucleofector Kit
 Amaxa Mouse T Cell Nucleofector Kit For T cells isolated from C57BL/6 & BALB/c mice Evaluated for murine T cells isolated from C57BL/6 & BALB/c mice This protocol is designed for murine lymphocytes or
Amaxa Mouse T Cell Nucleofector Kit For T cells isolated from C57BL/6 & BALB/c mice Evaluated for murine T cells isolated from C57BL/6 & BALB/c mice This protocol is designed for murine lymphocytes or
The Most Common Autoimmune Disease: Rheumatoid Arthritis. Bonita S. Libman, M.D.
 The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
Enumeration and Viability of Nucleated Cells from Bone Marrow, Cord Blood, and Mobilized Peripheral Blood
 Application Note Primary Cell Analysis Enumeration and Viability of Nucleated Cells from Bone Marrow, Cord Blood, and Mobilized Peripheral Blood Cell Viability Introduction: Bone Marrow, Cord Blood, Stem
Application Note Primary Cell Analysis Enumeration and Viability of Nucleated Cells from Bone Marrow, Cord Blood, and Mobilized Peripheral Blood Cell Viability Introduction: Bone Marrow, Cord Blood, Stem
