Model Coverage Policy
|
|
|
- Tiffany Greene
- 8 years ago
- Views:
Transcription
1 Model Coverage Policy Autonomic Testing Christopher H. Gibbons, MD, FAAN William P. Cheshire Jr., MD, FAAN Terry D. Fife, MD, FAAN BACKGROUND The conceptual framework for autonomic testing began at the turn of the 19 th century with a number of experiments in basic neurophysiology. These original tests were developed over time into a rigorously defined, standardized series of autonomic tests that are useful in the clinical assessment and care of patients with suspected autonomic disorders. Autonomic testing has been widely used in clinical practice for 50 years, with decades of extensive experience and thousands of studies published on its use. Comprehensive textbooks have been published on the purpose and methodology of autonomic testing. 1 4 Autonomic testing is an umbrella term that covers testing of the various branches of the nervous system: the sympathetic, parasympathetic, and enteric. It should be noted that the autonomic nervous system extends to nearly every organ system in the body; so many organ specific tests are in fact tests of autonomic function (such as urodynamic studies, gastric motility testing, pupillometry, tests of lacrimal and salivary gland production, etc.). For the purposes of this policy, we will focus on the standard tests of sudomotor (sympathetic cholinergic), cardiovagal (parasympathetic) and sympathetic adrenergic system function. As is true for other accepted tests of neurophysiologic function and clinical monitoring technologies, randomized controlled trials establishing the efficacy of autonomic testing have not been done. However, current data, accumulated through scientific research and clinical experience and published in peer-reviewed journals over the past 50 years, have defined the role of autonomic testing in the diagnosis and management of autonomic disorders in clinical practice and established the value of autonomic testing in the longitudinal study of disease. Autonomic testing is an integral component of the clinical evaluation of patients with autonomic disorders. Autonomic Disorders is an established subspecialty recognized by the United Council on Neurologic Subspecialties (UCNS), which certifies physicians and laboratories with training and expertise in this discipline. COMMON AUTONOMIC TESTING TERMS Autonomic Nervous System: The part of the nervous system that controls involuntary visceral actions. Cardiovagal: The parasympathetic response measured via cardiac function, which is under control of the vagus nerve, which influences heart rate variability. Heart Rate Variability: A test of parasympathetic function in which an individual undergoes a standard series of breathing exercises and the variability in the heart rate response is measured. Diminished heart rate variability (diminished respiratory sinus arrhythmia) is a sign of parasympathetic dysfunction. Quantitative Sudomotor Axon Reflex Test: A test to evaluate the integrity of postganglionic sudomotor nerves along the axon reflex to define the volume and distribution of sweat loss. This is accomplished by releasing acetylcholine into the skin, which activates distal postganglionic sudomotor nerves, when then activates receptors on the eccrine sweat gland. The sweat response is typically recorded from four sites (one forearm and three lower extremity sites) and the waveforms generated are assessed for deficits. Sudomotor: The sympathetic cholinergic component of the autonomic nervous system is responsible for sweat gland function and the production of thermoregulatory sweating. Sympathetic Skin Response: A test to measure a provoked change in the electrical potential of the skin. Thermoregulatory Sweat Test (TST): A test of sweat function and its neurologic regulation in which a generalized thermoregulatory sweating response is elicited by raising the core body temperature and monitoring sweat production by an indicator dye applied to the skin of the whole body (typically the anterior aspect). When the core temperature rises beyond a hypothalamic thermoregulatory set point, sweating occurs. TST investigates the integrity of the central and peripheral thermoregulatory sympathetic pathways, from Approved by AAN Board of Directors in October 2014 Autonomic Testing 1
2 the hypothalamus to the eccrine sweat gland, by use of an indicator powder mixture (typically alizarin red or iodinated corn starch). When a core temperature of 38 C is achieved, normal sweat production is visualized by a change in color in the indicator powder. Digital photography is used to document the sweat distribution, which can be characteristic of neuropathy, ganglionopathy, or generalized autonomic failure. Valsalva Maneuver: An autonomic testing maneuver in which the patient exhales against resistance and the blood pressure and heart rate are recorded, typically on a beatto-beat basis. This test evaluates the complex sympathetic adrenergic and parasympathetic responses to the transient reduction in cardiac preload caused by an increase in intrathoracic pressure. VARIATIONS IN METHODS OF TESTING, INCLUDING A DISCUSSION ABOUT AUTOMATED DEVICES Autonomic testing using automated devices, in which software automatically generates an interpretation, has not been validated. Automated autonomic testing devices perform a simplified battery of autonomic tests typically the heart rate response to deep breathing, the heart rate response to a Valsalva maneuver, and the blood pressure response to standing. Many devices are severely limited in the validity of the data they generate because they do not measure or control for expiratory pressure or include beat-to-beat blood pressure measurement, both of which are requirements, not only for scientifically accurate assessment, but also for billing of autonomic testing.5, 6 For example, by failing to measure the expiratory pressure and blood pressure responses to a Valsalva maneuver, these devices generate meaningless heart rate data, since it is not possible to interpret the heart rate without information about its stimulus. Most of these devices generate reports automatically and do not allow physician interpretation of the raw data, which is a serious design flaw when evaluating patients who have, for example, cardiac rhythm abnormalities that mislead the testing results. In contrast to state-of-the art autonomic testing (as discussed in detail below), a review of the scientific literature reveals that autonomic testing by automated devices has not been validated by any presentations to our knowledge at scientific sessions of the American Academy of Neurology or the American Autonomic Society, nor does a search of the literature on PubMed discover any published data demonstrating that such automated testing is clinically meaningful. Automated testing devices do not satisfy the conditions that are required for using the billing codes that were developed for autonomic testing. The CPT code requires a five-minute tilt table test and continuous beat-tobeat blood pressure monitoring in order to be billed. It is clear that the vast majority of bills from code using automated devices do not include beat-to-beat blood pressure testing and do not include a five-minute tilt table test. Furthermore, the new autonomic testing codes also require beat-tobeat blood pressure monitoring and a tilt table test. There are no automated devices currently on the market that, when used alone, are sufficient to bill for autonomic testing using Billing code is the only code appropriate for autonomic testing using automated devices. Autonomic testing (CPT codes and 95924) not using automated devices combines a battery of tests that typically includes the heart rate response to paced breathing, the heart rate response and continuous blood pressure response to a Valsalva maneuver, the heart rate response and beatto- beat blood pressure response to a five-minute stand, and the beat-to-beat blood pressure response to a passive tilt table test of five minutes or longer. The data is rigorously reviewed and interpreted by a physician with expertise in understanding and interpreting the data in the appropriate clinical context. A vast number of medications may influence autonomic test results, and physicians who perform autonomic testing must be aware of the potential for misinterpretation of results in the context of polypharmacy. All of the extensive data in the literature about autonomic testing is based on these testing methods; extrapolating this literature to automatic devices that omit essential elements of autonomic testing as described would be scientifically unjustifiable. In regard to the clinical utility of the well-established methods of autonomic testing discussed above, there has been no debate until recently. With the advent and increasing use of automated autonomic testing devices, physicians specializing in autonomic disorders are concerned that erroneous results obtained from devices of unproven scientific validity could adversely impact patient care. Additionally, payers have taken notice of increased billing for autonomic testing using these devices. Cost considerations have generated debate over autonomic testing in general. Whereas autonomic testing by the well-established methods in accordance with autonomic CPT codes is performed under carefully controlled conditions, can take minutes to perform correctly, and requires interpretation by a physician familiar with autonomic nervous system physiology; automated testing devices are designed to generate data after approximately minutes of testing and without physician interpretation. The automated testing devices are often utilized and billed for by physicians with no training in autonomic testing and no specialized expertise in Autonomic Testing 2
3 autonomic nervous system physiology. This has resulted in misuse of the autonomic billing codes. Code requires both a five-minute tilt table test and beat-to-beat blood pressure monitoring in order to be billed. It is clear that the vast majority of bills from code using automated devices do not include beat-to-beat blood pressure testing QUALIFICATIONS OF PHYSICIANS WHO PERFORM AUTONOMIC TESTING and do not include a five-minute tilt table test. Furthermore, the new combined autonomic testing code (95924) also requires beat-to-beat blood pressure monitoring and a tilt table test for use. All autonomic testing using automated devices should be billed using code effective January 1, A number of automated testing devices have been developed over the past several years and advertised directly to non-neurologists and general practitioners who do not have training or expertise in the autonomic nervous system. Some of these automated devices may also generate patient-specific recommendations for treatment. As a result, physicians who do perform full autonomic testing have seen a large increase in the number of patients erroneously diagnosed with an autonomic disorder (unpublished data from the authors practices). Prescribing unnecessary medications on the basis of an incorrect autonomic diagnosis could potentially harm patients because of the potential for serious adverse reactions. We have seen, for example, some patients treated with immune globulin for years for a diagnosis of autoimmune autonomic failure when all they had was a false positive automated autonomic test. Further, we have seen some patients who were told they have autonomic failure that is linked to a fatal neurologic disease (such as multiple system atrophy) when, in reality, they simply had an automated test that gave an incorrect result. Most physicians without training in the autonomic nervous system do not know enough about many of the rare autonomic disorders to integrate the information supplied by automated devices into the clinical history of the individual in front of them. Therefore, we strongly recommend that only physicians with the appropriate training perform and interpret clinical autonomic test results. Recommendations for required training are beyond the scope of this policy, but should follow the same guidelines for other tests of neurophysiology such as EMG, EEG, and evoked potentials. The United Council of Neurologic Subspecialties has established a board examination as one potential method to certify those individuals with expertise in autonomic disorders. In addition, some subspecialty societies are developing guidelines on what constitutes appropriate training for interpretation of autonomic test results. We also recommend that health insurance plans and exchanges allow for their patients to be covered for autonomic testing and consultation at centers where such expertise exists when it is not available within their network. TECHNIQUES USED IN AUTONOMIC TESTING Cardiovagal Autonomic Testing: Autonomic nervous system function testing for cardiovagal innervation has an enormous amount of clinical data supporting its use. It is the only reliable way to measure the function of the parasympathetic, or cardiovagal, nervous system. 5, 7 The American Diabetes Association (ADA) recommends that autonomic testing (including cardiovagal testing) be performed for all patients with type 2 diabetes mellitus at the time of diagnosis and five years after diagnosis in individuals with type 1 diabetes. 8, 9 Those recommendations are based on evidence showing that individuals with diabetes that have evidence of cardiac autonomic neuropathy have significantly higher rates of mortality and silent myocardial ischemia. Guidelines for anesthesia, surgery and medical therapies to affect outcomes have been established for diabetic patients based on autonomic test findings. 8, 10, 11 Cardiovagal testing has been demonstrated in a number of disease states to be an early marker of autonomic parasympathetic dysfunction Some disorders, such as amyloidosis and autoimmune autonomic ganglionopathy, preferentially affect autonomic nerve fibers and may not exhibit abnormalities of somatic nerve fiber tests (the latter detectable by nerve conduction tests and electromyography). 16, 17 Heart rate variability is a simple and reliable test of cardiovagal function. It has a sensitivity of 97.5 percent for detection of parasympathetic dysfunction in diabetes when age-adjusted normative values are used. 10, 18 The heart rate response to deep breathing, tilt table test, and the Valsalva maneuver are considered standard clinical tests of autonomic function and are sensitive, specific, and reproducible methods for grading the degree of autonomic dysfunction. 5 Evaluation of parasympathetic function through cardiovagal testing has been firmly established for clinical use for decades. Autonomic Testing 3
4 Vasomotor Adrenergic Autonomic Testing: Testing sympathetic adrenergic function is the primary method for evaluating patients with syncope, orthostatic hypotension, 14, postural tachycardia syndrome, and postural dizziness. Such testing is sensitive, specific, and clinically useful across diseases to diagnose patients with autonomic dysfunction. Sympathetic adrenergic testing (in conjunction with cardiovagal and sudomotor function testing) has been shown to aid in diagnosis, management, and outcomes in patients with autonomic dysfunction or syncope of unexplained cause. 6, 26 Sympathetic adrenergic testing, when normal, is clinically useful also in ruling out autonomic failure when the history and bedside examination alone are diagnostically insufficient. Autonomic testing (including adrenergic testing) is recommended for all patients with type 2 diabetes at the time of diagnosis and five years after diagnosis in individuals with type 1 diabetes. 8 Individuals with diabetes that have cardiac autonomic neuropathy have a significantly higher mortality, and guidelines for anesthesia, surgery, and medical 8, 10, 11 therapies to affect outcomes have been established. Vasomotor adrenergic autonomic testing has been firmly established for clinical use for decades. Sudomotor Testing: There are more than 60 years of data supporting the use of sudomotor testing in clinical practice. Following World War II, investigations of injuries to the nervous system involving sudomotor pathways led to the development of the quinizarin sweat test. The thermoregulatory sweat test (TST) is a sophisticated modification of the quinizarin sweat test that is widely used in the diagnosis of peripheral neuropathy. A large body of evidence exists to support its role in detecting and distinguishing among specific types of central nervous system disorders and peripheral neuropathies that impair sudomotor pathways, particularly when those disorders do not involve somatic sensory or motor nerve fibers. 27 The QSART device was first reported in detail in 1983 and has been in widespread clinical use ever since. 28 There are well established normative values and clinical guidelines for the use of this test. 27 The sympathetic skin response is another widely utilized test of sudomotor function The overwhelming amount of data supporting the use of QSART and SSR define these tests as medically necessary for the evaluation of autonomic dysfunction. QDIRT and silastic sweat imprint methods are also widely used, but they do not have the same level of clinical data supporting their use and at this time would be considered investigational. 32 All of these tests measure only post-ganglionic sudomotor function, whereas the TST also assesses central nervous system sudomotor pathways. Data from a considerable body of literature indicate that sudomotor testing may be the most sensitive means to detect a peripheral small fiber neuropathy. 33 Sudomotor testing is also the only way to detect isolated damage to sudomotor nerves, as it can occur in a number of specific disease states, including Ross syndrome, Harlequin syndrome, diabetes mellitus, multiple system atrophy, Parkinson s disease, autoimmune autonomic ganglionopathy, lepromatous leprosy, amyloid neuropathy, Sjögren syndrome, Fabry s disease, Lambert-Eaton myasthenic syndrome, pure autonomic failure, chronic idiopathic anhidrosis, and a host of other disorders that frequently come to the attention of the neurologist. 28, The clinical implications of testing and outcomes are reviewed in detail in a plethora of studies across numerous diseases. Autonomic testing (including sudomotor testing) is recommended for all patients with type 2 diabetes at the time of diagnosis and five years after diagnosis in individuals with type 1 diabetes. 8 10, 18, 38 Individuals with diabetes that have autonomic neuropathy have a significantly higher mortality, and guidelines for anesthesia, surgery and medical 8, 10, 11 therapies to affect outcomes have been established. WHAT TYPES OF PATIENTS WILL BENEFIT FROM AUTONOMIC TESTING? Examples of the many situations where autonomic testing is of clinical utility include: Patients with syncope: Autonomic testing is necessary to differentiate neurally mediated syncope from neurogenic orthostatic hypotension and other causes of syncope. 26, Patients with diabetes mellitus: All patients with diabetes are recommended to have autonomic testing (sudomotor, cardiovagal and adrenergic) at diagnosis (type 2 diabetes) 8 10, 18, 38, 44 or five years after diagnosis (type 1 diabetes). There is a high prevalence of cardiovascular autonomic neuropathy in the diabetic population The relationship between autonomic dysfunction and cardiovascular risk has been well documented and is important to monitor for patients planning major surgical procedures or considering moderate to high intensity physical exercise. This is the reason that the ADA recommends autonomic testing for all patients with type 2 diabetes at the time of diagnosis, and all patients with type 1 diabetes five years after diagnosis. The increased perioperative mortality in cardiovascular autonomic neuropathy is linked to greater blood pressure instability and hypothermia This information may prompt high-risk patients to forgo an elective procedure or allow the anesthesiologist to Autonomic Testing 4
5 prepare for potential hemodynamic changes, thereby 49, reducing the risks of morbidity and mortality. Patients with orthostatic dizziness: Patients with recurrent dizziness when standing may have autonomic dysfunction, postural tachycardia syndrome, or other autonomic neuropathy that can be treated if a diagnosis is made. 17, All autonomic tests (sudomotor, cardiovagal, and adrenergic) are appropriate to use in forming a differential diagnosis, defining the physiology of orthostatic intolerance in the individual patient, grading the severity of impairment, and directing appropriate therapy. Patients with disorders of sweating: Autonomic testing can provide a diagnosis which can lead to treatment of the underlying disorder and improvements in clinical outcomes Patients found to have global anhidrosis may be at risk for heat exhaustion or heat stroke and can benefit from interventions to restore sweating, when a reversible cause is diagnosed, or otherwise from management strategies to avoid heat stress. Although sudomotor testing will provide specific information about the problem with sweating, cardiovagal, and adrenergic testing will narrow the differential diagnosis and are therefore integral parts of the autonomic test (i.e., does the patient have an autonomic ganglionopathy, an isolated autonomic neuropathy such as Ross syndrome, a peripheral neuropathy causing distal anhidrosis and proximal hyperhidrosis, how severe or anatomically widespread is the deficit, etc.). Patients with peripheral neuropathy from a number of different causes such as (but not limited to) amyloidosis, Fabry s disease, Sjögren s syndrome, and autoimmune neuropathies. 73 CLINICAL INDICATIONS FOR TESTING The following indications are examples of appropriate situations in which to consider autonomic testing (note: this is not an exhaustive list): Evaluate orthostatic hypotension in a patient with dizziness, a drop in blood pressure, or syncope upon standing. Autonomic testing can assist the physician in distinguishing neurogenic from other causes of orthostatic hypotension, evaluate the severity of adrenergic failure, and assess for associated recumbent hypertension. In central neurodegenerative disorders, especially the synucleinopathies, distinguish multiple system atrophy from Parkinson s disease and diffuse Lewy body disease. Diagnose the presence of autonomic neuropathy in a patient with signs or symptoms suggesting a progressive autonomic neuropathy, including, but not limited to: Diabetic neuropathy Amyloid neuropathy Sjögren s syndrome Idiopathic neuropathy Pure autonomic failure Multiple system atrophy Evaluate the severity and distribution of a diagnosed progressive autonomic neuropathy. Differentiate certain complicated variants of syncope from other causes of loss of consciousness. Evaluate inadequate response to beta blockade in vasodepressor syncope. Evaluate distressing symptoms in the patient with a clinical picture suspicious for distal small fiber neuropathy in order to diagnose the condition when nerve conduction studies are normal. Diagnose and differentiate the cause of postural tachycardia syndrome. Evaluate change in type, distribution or severity of autonomic deficits in patients with autonomic failure. Evaluate the response to treatment in patients with autonomic failure who demonstrate a change in clinical exam. Diagnose axonal neuropathy or suspected autonomic neuropathy in the symptomatic patient. Evaluate and diagnose sympathetically maintained pain, as in reflex sympathetic dystrophy or causalgia. Evaluate and treat patients with recurrent unexplained syncope to demonstrate autonomic failure. Autonomic Testing 5
6 DIAGNOSES WHERE TESTING IS INDICATED The following disorders are known to impair the function of the autonomic nervous system. When clinically indicated, the following disorders may require testing of the autonomic nervous system (note: this is not an exhaustive list): Orthostatic hypotension Multiple system atrophy Lewy body disease Parkinson s disease Pure autonomic failure Cerebellar ataxia Syncope Orthostatic intolerance including postural tachycardia syndrome (POTS) Anhidrosis Autoimmune autonomic neuropathy/ganglionopathy Idiopathic autonomic neuropathy Paraneoplastic autonomic neuropathy Chagas disease Intestinal pseudo-obstruction (if generalized or cholinergic neuropathy is suspected) Autonomic dysreflexia Familial dysautonomia or Riley Day syndrome Baroreflex failure Hereditary sensory and autonomic neuropathies Ross syndrome Lambert Eaton myasthenic syndrome Morvan syndrome Guillain-Barré syndrome LIMITATIONS Autonomic testing evaluates the physiologic responses to various stimuli. It is not a test for a specific disease; instead it investigates the degree of dysfunction of this part of the nervous system. This can aid in localization of the dysfunction, narrowing of the differential diagnosis, and in some cases making a clear diagnosis. Autonomic testing may not be able to differentiate between similar disorders that both cause autonomic dysfunction, but can quantify the severity of autonomic dysfunction, in other cases exclude autonomic dysfunction, and thereby lead to specific recommendations for treatment. Autonomic testing can make a diagnosis of orthostatic hypotension, delayed orthostatic hypotension, neurally mediated syncope, or postural tachycardia syndrome. However, autonomic testing cannot always differentiate between the various disorders that cause these syndromes. The role of autonomic testing in this situation is to define, clarify, and gauge the severity of the problem so that the appropriate work-up and treatment can be instituted. INDICATIONS FOR WHICH DATA IS LIMITED The following are a list of indications for which data is limited at the time of writing this template policy (note: this is not an exhaustive list): Myofascial pain syndrome/fibromyalgia Raynaud s phenomenon Predicting foot ulcers Flushing syndrome Chronic fatigue NOS Generalized hyperhidrosis Palmoplantar hyperhidrosis Irritable bowel syndrome Somatization disorder Anxiety disorder CPT CODES CPT codes, descriptions, and other data are copyright 2014 American Medical Association. All Rights Reserved. Applicable FARS/DFARS Clauses Apply. Code should be reported only when both the parasympathetic function and the adrenergic function are tested together with the use of a tilt table * Testing of autonomic nervous system function; cardiovagal innervation (parasympathetic function), including two or more of the following: heart rate response to deep breathing with recorded R-R interval, Valsalva ratio, and 30:15 ratio To report autonomic function testing that does not include beat-tobeat recording, or for testing without use of a tilt table, use Autonomic Testing 6
7 95922 Vasomotor adrenergic innervation (sympathetic adrenergic function), including beat-to-beat blood pressure and R-R interval changes during Valsalva maneuver and at least 5 minutes of passive tilt Do not report in conjunction with sudomotor, including one or more of the following: quantitative sudomotor axon reflex test (QSART), silastic sweat imprint, thermoregulatory sweat test, and changes in sympathetic skin potential Simultaneous, independent, quantitative measures of both parasympathetic function and sympathetic function, based on time-frequency analysis of heart rate variability concurrent with time-frequency analysis of continuous respiratory activity, with mean heart rate and blood pressure measures, during rest, paced (deep) breathing, Valsalva maneuvers, and head-up postural change Do not report in conjunction with 93040, 95921, 95922, combined parasympathetic and sympathetic adrenergic function testing with at least 5 minutes of passive tilt DISCLAIMER Do not report in conjunction with or AAN s Model Coverage Policies must be used by AAN members in an appropriate manner and not for engaging in anti-competitive activities. Antitrust laws involve complex legal and economic analysis beyond the scope of Model Coverage Policies; but they are integral in the overall consideration of building payer relationships and advocating for improving payer policies. No material contained in AAN Model Coverage Policies should be construed as legal advice. Neurologists are encouraged to seek advice from attorneys with expertise in payer relations. The information in AAN s Model Coverage Policies: 1. should not be considered inclusive of all proper treatments, methods of care, or as a statement of the standard of care; 2. is not continually updated and may not reflect the most recent evidence (new evidence may emerge between the time information is developed and when it is published or read); 3. does not mandate any particular course of medical care or promote or not promote any particular device or product; and 4. is not intended to substitute for the independent professional judgment of the treating provider, as the information does not account for individual variation among patients. In all cases, the selected course of action should be considered by the treating provider in the context of treating the individual patient. Use of the information is voluntary. The AAN provides this information on an as is basis, and makes no warranty, expressed or implied, regarding the information. The AAN specifically disclaims any warranties of merchantability or fitness for a particular use or purpose. The AAN assumes no responsibility for any injury or damage to persons or property arising out of or related to any use of this information or for any errors or omissions. Autonomic Testing 7
8 APPENDIX A DIAGNOSES THAT SUPPORT MEDICAL NECESSITY Note: All ICD-9-CM and ICD-10-CM codes listed below may be viewed as medically necessary; however, there may be other diagnostic codes not included in this list that are deserving of consideration for coverage. Such instances may require individual consideration. ICD-9-CM Orthostatic hypotension Syncope , Diabetic neuropathy Idiopathic neuropathy Hereditary sensory neuropathy Idiopathic peripheral autonomic neuropathy Unspecified disorder of the autonomic nervous system Degenerative disease of the basal ganglia Postural tachycardia ICD-10-CM I95.1 Orthostatic hypotension R55 Syncope and collapse E11.40 Type 2 diabetes mellitus with diabetic E11.41 Type 2 diabetes mellitus with diabetic mononeuropathy E11.42 Type 2 diabetes mellitus with diabetic polyneuropathy E11.43 Type 2 diabetes mellitus with diabetic autonomic (poly)neuropathy E11.44 Type 2 diabetes mellitus with diabetic amyotrophy E11.49 Type 2 diabetes mellitus with other diabetic neurological complication E Type 2 diabetes mellitus with diabetic neuropathic arthropathy E13.40 Other specified diabetes mellitus with diabetic E13.41 Other specified diabetes mellitus with diabetic mononeuropathy E13.42 Other specified diabetes mellitus with diabetic polyneuropathy E13.43 Other specified diabetes mellitus with diabetic autonomic (poly)neuropathy E13.44 Other specified diabetes mellitus with diabetic amyotrophy E13.49 Other specified diabetes mellitus with other diabetic neurological complication E Other specified diabetes mellitus with diabetic neuropathic arthropathy E10.40 Type 1 diabetes mellitus with diabetic E10.41 Type 1 diabetes mellitus with diabetic mononeuropathy E10.42 Type 1 diabetes mellitus with diabetic polyneuropathy E10.43 Type 1 diabetes mellitus with diabetic autonomic (poly)neuropathy E10.44 Type 1 diabetes mellitus with diabetic amyotrophy E10.49 Type 1 diabetes mellitus with other diabetic neurological complication E Type 1 diabetes mellitus with diabetic neuropathic arthropathy E11.40 Type 2 diabetes mellitus with diabetic E11.65 Type 2 diabetes mellitus with hyperglycemia E10.40 Type 1 diabetes mellitus with diabetic E10.65 Type 1 diabetes mellitus with hyperglycemia E08.42 Diabetes mellitus due to underlying condition with diabetic polyneuropathy E09.42 Drug or chemical induced diabetes mellitus with neurological complications with diabetic polyneuropathy E10.42 Type 1 diabetes mellitus with diabetic polyneuropathy E11.42 Type 2 diabetes mellitus with diabetic polyneuropathy E13.42 Other specified diabetes mellitus with diabetic polyneuropathy E08.40 Diabetes mellitus due to underlying condition with diabetic E09.40 Drug or chemical induced diabetes mellitus with neurological complications with diabetic E10.40 Type 1 diabetes mellitus with diabetic E11.40 Type 2 diabetes mellitus with diabetic E13.40 Other specified diabetes mellitus with diabetic G60.9 Hereditary and idiopathic neuropathy, unspecified G60.0 Hereditary motor and sensory neuropathy G90.09 Other idiopathic peripheral autonomic neuropathy G90.9 Disorder of the autonomic nervous system, unspecified G90.8 Other disorders of autonomic nervous system G23.0 Hallervorden-Spatz disease G23.1 Progressive supranuclear ophthalmoplegia [Steele-Richardson-Olszewski] G23.2 Striatonigral degeneration G23.8 Other specified degenerative diseases of basal ganglia G23.9 Degenerative disease of basal ganglia, unspecified G90.3 Multi-system degeneration of the autonomic nervous system R00.0 Tachycardia, unspecified Autonomic Testing 8
9 REFERENCES 1. Mathias CJ, Bannister R. Autonomic Failure., 4 ed. Oxford: Oxford University Press, Low PA. Clinical autonomic disorders: evaluation and management, Second Edition ed. Philadelphia: Lippincott - Raven, Robertson D, Biaggioni I. Primer on the autonomic nervous system, 3 rd ed. Oxford: Academic, Low PA, Benarroch EE. Clinical autonomic disorders, 3 rd ed. Philadelphia: Lippincott Williams & Wilkins, Low PA. Testing the autonomic nervous system. SeminNeurol 2003;23: Freeman R. Assessment of cardiovascular autonomic function. ClinNeurophysiol 2006;117: Heart rate variability: standards of measurement, physiological interpretation and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology [see comments]. Circulation 1996;93: Boulton AJ, Vinik AI, Arezzo JC, et al. Diabetic neuropathies: a statement by the American Diabetes Association. Diabetes Care 2005;28: Tesfaye S, Boulton AJ, Dyck PJ, et al. Diabetic neuropathies: update on definitions, diagnostic criteria, estimation of severity, and treatments. Diabetes Care 2010;33: Spallone V, Ziegler D, Freeman R, et al. Cardiovascular autonomic neuropathy in diabetes: clinical impact, assessment, diagnosis, and management. Diabetes/metabolism research and reviews Vinik AI, Ziegler D. Diabetic cardiovascular autonomic neuropathy. Circulation 2007;115: Thaisetthawatkul P, Boeve BF, Benarroch EE, et al. Autonomic dysfunction in dementia with Lewy bodies. Neurology 2004;62: Low PA, Benrud-Larson LM, Sletten DM, et al. Autonomic Symptoms and Diabetic Neuropathy: A population-based study. Diabetes Care 2004;27: Gibbons CH, Freeman R. Delayed orthostatic hypotension: a frequent cause of orthostatic intolerance. Neurology 2006;67: Goldstein DS, Sharabi Y, Karp BI, et al. Cardiac sympathetic denervation preceding motor signs in Parkinson disease. CleveClinJMed 2009;76 Suppl 2:S47-S Wang AK, Fealey RD, Gehrking TL, Low PA. Patterns of neuropathy and autonomic failure in patients with amyloidosis. Mayo ClinProc 2008;83: Vernino S, Low PA, Fealey RD, Stewart JD, Farrugia G, Lennon VA. Autoantibodies to ganglionic acetylcholine receptors in autoimmune autonomic neuropathies. NEnglJMed 2000;343: Spallone V, Bellavere F, Scionti L, et al. Recommendations for the use of cardiovascular tests in diagnosing diabetic autonomic neuropathy. Nutrition, metabolism, and cardiovascular diseases : NMCD 2011;21: Faraji F, Kinsella LJ, Rutledge JC, Mikulec AA. The comparative usefulness of orthostatic testing and tilt table testing in the evaluation of autonomic-associated dizziness. Otology & neurotology : official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology 2011;32: Sundkvist G. Autonomic nervous function in asymptomatic diabetic patients with signs of peripheral neuropathy. Diabetes Care 1981;4: Sundkvist G, Alm:er LO, Lilja B. A sensitive orthostatic test on tilt table, useful in the detection of diabetic autonomic neuropathy. Acta MedScandSuppl 1981;656: Kenny RA, Ingram A, Bayliss J, Sutton R. Head-up tilt: a useful test for investigating unexplained syncope. Lancet 1986: Grubb BP, Gerard G, Roush K, et al. Differentiation of convulsive syncope and epilepsy with head-up tilt testing [see comments]. AnnInternMed 1991;115: Calkins H, Byrne M, el-atassi R, Kalbfleisch S, Langberg JJ, Morady F. The economic burden of unrecognized vasodepressor syncope. AmJMed 1993;95: Mathias CJ, Deguchi K, Schatz I. Observations on recurrent syncope and presyncope in 641 patients. Lancet 2001;357: Lahrmann H, Cortelli P, Hilz M, Mathias CJ, Struhal W, Tassinari M. EFNS guidelines on the diagnosis and management of orthostatic hypotension. EurJNeurol 2006;13: Illigens BM, Gibbons CH. Sweat testing to evaluate autonomic function. Clinical autonomic research: official journal of the Clinical Autonomic Research Society 2009;19: Low PA, Caskey PE, Tuck RR, Fealey RD, Dyck PJ. Quantitative sudomotor axon reflex test in normal and neuropathic subjects. AnnNeurol 1983;14: Soliven B, Maselli R, Jaspan J, et al. Sympathetic skin response in diabetic neuropathy. Muscle & Nerve 1987;10: Uncini A, Pullman SL, Lovelace RE, Gambi D. The sympathetic skin response: normal values, elucidation of afferent components and application limits. JNeurolSci 1988;87: Baser SM, Meer J, Polinsky RJ, Hallett M. Sudomotor function in autonomic failure. Neurology 1991;41: Gibbons CH, Illigens BM, Centi J, Freeman R. QDIRT: quantitative direct and indirect test of sudomotor function. Neurology 2008;70: Low VA, Sandroni P, Fealey RD, Low PA. Detection of small-fiber neuropathy by sudomotor testing. Muscle Nerve 2006;34: Low PA, Fealey RD. Sudomotor neuropathy. In: Dyck PJ, Thomas PK, Winegrad A, Porte D, eds. Diabetic neuropathy. Philadelphia: W.B.Saunders, 1987: Schondorf R, Low PA. Idiopathic postural orthostatic tachycardia syndrome: an attenuated form of acute pandysautonomia? Neurology 1993;43: Wolfe GI, Galetta SL, Teener JW, Katz JS, Bird SJ. Site of autonomic dysfunction in a patient with Ross syndrome and postganglionic Horner s syndrome. Neurology 1995;45: Sandroni P, Low PA, Ferrer T, Opfer-Gehrking TL, Willner CL, Wilson PR. Complex regional pain syndrome I (CRPS I): prospective study and laboratory evaluation. ClinJPain 1998;14: Autonomic Testing 9
10 38. Bernardi L, Spallone V, Stevens M, et al. Investigation methods for cardiac autonomic function in human research studies. Diabetes/ metabolism research and reviews Abi-Samra F, Maloney JD, Fouad-Tarazi FM, Castle LW. The usefulness of head-up tilt testing and hemodynamic investigations in the workup of syncope of unknown origin. PacingClinElectrophysiol 1988;11: Kochiadakis GE, Rombola AT, Kanoupakis EM, Simantirakis EN, Chlouverakis GI, Vardas PE. Assessment of autonomic function at rest and during tilt testing in patients with vasovagal syncope. AmHeart J 1997;134: Stewart JM. Autonomic nervous system dysfunction in adolescents with postural orthostatic tachycardia syndrome and chronic fatigue syndrome is characterized by attenuated vagal baroreflex and potentiated sympathetic vasomotion. PediatrRes 2000;48: Karas B, Grubb BP, Boehm K, Kip K. The postural orthostatic tachycardia syndrome: a potentially treatable cause of chronic fatigue, exercise intolerance, and cognitive impairment in adolescents. Pacing ClinElectrophysiol 2000;23: Freeman R, Wieling W, Axelrod FB, et al. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Clinical autonomic research : official journal of the Clinical Autonomic Research Society 2011;21: Spallone V, Morganti R, D Amato C, et al. Clinical correlates of painful diabetic neuropathy and relationship of neuropathic pain with sensorimotor and autonomic nerve function. European journal of pain 2011;15: Suarez GA, Clark VM, Norell JE, et al. Sudden cardiac death in diabetes mellitus: risk factors in the Rochester diabetic neuropathy study. JNeurolNeurosurgPsychiatry 2005;76: Astrup AS, Tarnow L, Rossing P, Hansen BV, Hilsted J, Parving HH. Cardiac autonomic neuropathy predicts cardiovascular morbidity and mortality in type 1 diabetic patients with diabetic nephropathy. Diabetes Care 2006;29: Ziegler D, Zentai CP, Perz S, et al. Prediction of mortality using measures of cardiac autonomic dysfunction in the diabetic and nondiabetic population: the MONICA/KORA Augsburg Cohort Study. Diabetes Care 2008;31: Kahn JK, Sisson JC, Vinik AI. Prediction of sudden cardiac death in diabetic autonomic neuropathy. Journal of Nuclear Medicine 1988;29: Burgos LG, Ebert TJ, Asiddao C, et al. Increased intraoperative cardiovascular morbidity in diabetics with autonomic neuropathy. Anesthesiology 1989;70: O Brien IA, McFadden JP, Corrall RJ. The influence of autonomic neuropathy on mortality in insulin- dependent diabetes. QJMed 1991;79: Baker SK, Morillo C, Vernino S. Autoimmune autonomic ganglionopathy with late-onset encephalopathy. AutonNeurosci 2009;146: Iodice V, Kimpinski K, Vernino S, Sandroni P, Low PA. Immunotherapy for autoimmune autonomic ganglionopathy. AutonNeurosci 2009;146: Gibbons CH, Centi J, Vernino S, Freeman R. Autoimmune Autonomic Ganglionopathy With Reversible Cognitive Impairment. Archives of neurology Vernino S, Adamski J, Kryzer TJ, Fealey RD, Lennon VA. Neuronal nicotinic ACh receptor antibody in subacute autonomic neuropathy and cancer-related syndromes. Neurology 1998;50: Low PA, Opfer-Gehrking TL, Textor SC, et al. Postural tachycardia syndrome (POTS). Neurology 1995;45:S19-S Gordon VM, Opfer-Gehrking TL, Novak V, Low PA. Hemodynamic and symptomatic effects of acute interventions on tilt in patients with postural tachycardia syndrome. ClinAutonRes 2000;10: Sandroni P, Novak V, Opfer-Gehrking TL, Huck CA, Low PA. Mechanisms of blood pressure alterations in response to the Valsalva maneuver in postural tachycardia syndrome. ClinAutonRes 2000;10: Low PA, Schondorf R, Rummans TA. Why do patients have orthostatic symptoms in POTS? ClinAutonRes 2001;11: Singer W, Spies JM, McArthur J, et al. Prospective evaluation of somatic and autonomic small fibers in selected autonomic neuropathies. Neurology 2004;62: Thieben MJ, Sandroni P, Sletten DM, et al. Postural orthostatic tachycardia syndrome: the Mayo clinic experience. Mayo ClinProc 2007;82: Gibbons CHF, R. Intense cardiovascular exercise as a treatment for postural tachycardia syndrome (POTS). Neurology 2011;76:A De Marinis M, Stocchi F, Testa SR, De PF, Agnoli A. Alterations of thermoregulation in Parkinson s disease. FunctNeurol 1991;6: Nolano M, Provitera V, Perretti A, et al. Ross syndrome: a rare or a misknown disorder of thermoregulation? A skin innervation study on 12 subjects. Brain 2006;129: Kimpinski K, Iodice V, Sandroni P, Fealey RD, Vernino S, Low PA. Sudomotor dysfunction in autoimmune autonomic ganglionopathy. Neurology 2009;73: Fisher DA, Maibach HI. Postural hypotension and anhidrosis. The autonomic insufficiency syndrome. ArchDermatol 1970;102: Spector RH, Bachman DL. Bilateral Adie s tonic pupil with anhidrosis and hyperthermia. ArchNeurol 1984;41: Kang WH, Chun SI, Lee S. Generalized anhidrosis associated with Fabry s disease. J Amer Acad Derm 1987;17: Mitchell J, Greenspan J, Daniels T, Whitcher JP, Maibach HI. Anhidrosis (hypohidrosis) in Sjogren s syndrome. J Amer Acad Derm 1987;16: Fealey RD, Low PA, Thomas JE. Thermoregulatory sweating abnormalities in diabetes mellitus. MayoClinProc 1989;64: Weller M, Wilhelm H, Sommer N, Dichgans J, Wietholter H. Tonic pupil, areflexia, and segmental anhidrosis: two additional cases of Ross syndrome and review of the literature. JNeurol 1992;239: Cheshire WP, Freeman R. Disorders of sweating. SeminNeurol 2003;23: Gibbons CH, Freeman R. Antibody titers predict clinical features of autoimmune autonomic ganglionopathy. AutonNeurosci Freeman R. Autonomic peripheral neuropathy. NeurolClin 2007;25: Autonomic Testing 10
Local Coverage Determination (LCD): Medicine: Autonomic Function Tests (L34500)
 Local Coverage Determination (LCD): Medicine: Autonomic Function Tests (L34500) Contractor Information Contractor Name Cahaba Government Benefit Administrators, LLC LCD Information Document Information
Local Coverage Determination (LCD): Medicine: Autonomic Function Tests (L34500) Contractor Information Contractor Name Cahaba Government Benefit Administrators, LLC LCD Information Document Information
What on Earth is the Autonomic Nervous System? Dysautonomia and Autonomic Dysfunction
 www.complexchild.com What on Earth is the Autonomic Nervous System? Dysautonomia and Autonomic Dysfunction Most people have never heard of the Autonomic Nervous System, even though it controls most of
www.complexchild.com What on Earth is the Autonomic Nervous System? Dysautonomia and Autonomic Dysfunction Most people have never heard of the Autonomic Nervous System, even though it controls most of
Medical Treatment Guidelines Washington State Department of Labor and Industries
 Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Autonomic Stress Test
 Autonomic Stress Test (The expanded head-up tilt test) Artur Fedorowski Syncope Unit Skåne University Hospital, Malmö, Sweden NordSync 2011, Malmö Disclosure None The expanded head-up tilt test When? Why?
Autonomic Stress Test (The expanded head-up tilt test) Artur Fedorowski Syncope Unit Skåne University Hospital, Malmö, Sweden NordSync 2011, Malmö Disclosure None The expanded head-up tilt test When? Why?
Copyright 2013 Renua Medical TM, A Health First Technologies, Inc. Company. All rights reserved.
 Copyright 2013 Renua Medical TM, A Health First Technologies, Inc. Company. All rights reserved. This document may not be reproduced in whole, or in part, stored in a retrieval system, or transmitted in
Copyright 2013 Renua Medical TM, A Health First Technologies, Inc. Company. All rights reserved. This document may not be reproduced in whole, or in part, stored in a retrieval system, or transmitted in
Diabetes Care 27:2942 2947, 2004
 Pathophysiology/Complications O R I G I N A L A R T I C L E Autonomic Symptoms and Diabetic Neuropathy A population-based study PHILLIP A. LOW, MD LISA M. BENRUD-LARSON, PHD DAVID M. SLETTEN TONETTE L.
Pathophysiology/Complications O R I G I N A L A R T I C L E Autonomic Symptoms and Diabetic Neuropathy A population-based study PHILLIP A. LOW, MD LISA M. BENRUD-LARSON, PHD DAVID M. SLETTEN TONETTE L.
How To Treat An Elderly Patient
 1. Introduction/ Getting to know our Seniors a. Identify common concepts and key terms used when discussing geriatrics b. Distinguish between different venues of senior residence c. Advocate the necessity
1. Introduction/ Getting to know our Seniors a. Identify common concepts and key terms used when discussing geriatrics b. Distinguish between different venues of senior residence c. Advocate the necessity
Multifocal Motor Neuropathy. Jonathan Katz, MD Richard Lewis, MD
 Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout.
 Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
Assessment, diagnosis and specialist referral of adults (>16 years) with an episode of transient loss of consciousness (TLoC) or a blackout. TLoC is common huge variation in management range of clinicians
EMG and the Electrodiagnostic Consultation for the Family Physician
 EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
Recommended Policy for Electrodiagnostic Medicine American Association of Neuromuscular & Electrodiagnostic Medicine
 Recommended Policy for Electrodiagnostic Medicine American Association of Neuromuscular & Electrodiagnostic Medicine Executive Summary The electrodiagnostic medicine (EDX) evaluation is an important and
Recommended Policy for Electrodiagnostic Medicine American Association of Neuromuscular & Electrodiagnostic Medicine Executive Summary The electrodiagnostic medicine (EDX) evaluation is an important and
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
December 29, 2012. Dear Acting Administrator Tavenner:
 December 29, 2012 Marilyn B. Tavenner Acting Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Attention: CMS-1590-FC P.O. Box 8013 Baltimore, MD 21244
December 29, 2012 Marilyn B. Tavenner Acting Administrator Centers for Medicare & Medicaid Services U.S. Department of Health and Human Services Attention: CMS-1590-FC P.O. Box 8013 Baltimore, MD 21244
Postural tachycardia syndrome following human papillomavirus vaccination
 European Journal of Neurology 2014, 21: 135 139 doi:10.1111/ene.12272 Postural tachycardia syndrome following human papillomavirus vaccination S. Blitshteyn Department of Neurology, State University of
European Journal of Neurology 2014, 21: 135 139 doi:10.1111/ene.12272 Postural tachycardia syndrome following human papillomavirus vaccination S. Blitshteyn Department of Neurology, State University of
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
D.U.C. Assist. Lec. Faculty of Dentistry General Physiology Ihsan Dhari. The Autonomic Nervous System
 The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
ELECTROMYOGRAPHY (EMG), NEEDLE, NERVE CONDUCTION STUDIES (NCS) AND QUANTITATIVE SENSORY TESTING (QST)
 AND QUANTITATIVE SENSORY TESTING (QST) Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical
AND QUANTITATIVE SENSORY TESTING (QST) Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical
Autonomic dysfunctions in Paralympic athletes.
 Sochi 2014, Russia Rosa Khutor, March 10, 2014 Autonomic dysfunctions in Paralympic athletes. Andrei Krassioukov MD, PhD, FRCPC Professor, Dep. of Medicine, Div. Physical Medicine & Rehabilitation, Associate
Sochi 2014, Russia Rosa Khutor, March 10, 2014 Autonomic dysfunctions in Paralympic athletes. Andrei Krassioukov MD, PhD, FRCPC Professor, Dep. of Medicine, Div. Physical Medicine & Rehabilitation, Associate
How To Find Out If The Gulf War And Health Effects Of Serving In The Gulf Wars Are Linked To Health Outcomes
 Gulf War and Health: Update of Health Effects of Serving in the Gulf War Statement of Stephen L. Hauser, M.D. Professor and Chair of Neurology University of California, San Francisco, School of Medicine
Gulf War and Health: Update of Health Effects of Serving in the Gulf War Statement of Stephen L. Hauser, M.D. Professor and Chair of Neurology University of California, San Francisco, School of Medicine
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing
 3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing Peter D. Donofrio, M.D. Professor of Neurology Vanderbilt University Medical Center
3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing Peter D. Donofrio, M.D. Professor of Neurology Vanderbilt University Medical Center
Chapter 15. The Autonomic Nervous. The Autonomic Nervous System. Autonomic Motor Pathways. ANS vs. SNS
 The Autonomic Nervous System Chapter 15 The subconscious involuntary nervous system Regulates activity of smooth muscle, cardiac muscle & certain glands The Autonomic Nervous System 1 2 ANS vs. SNS Somatic
The Autonomic Nervous System Chapter 15 The subconscious involuntary nervous system Regulates activity of smooth muscle, cardiac muscle & certain glands The Autonomic Nervous System 1 2 ANS vs. SNS Somatic
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Conflicts of interest: None
 Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Syncope in Athletes Thomas G. Allison, PhD, MPH Mayo Clinic Rochester, MN USA 13 th Annual Review Course in Clinical Cardiology Zurich 14 April, 2015 CP972908-1 Conflicts of interest: None Syncope: Definition
Criteria: CWQI HCS-123 (This criteria is consistent with CMS guidelines for External Infusion Insulin Pumps)
 Moda Health Plan, Inc. Medical Necessity Criteria Subject: Origination Date: 05/15 Revision Date(s): 05/2015 Developed By: Medical Criteria Committee 06/24/2015 External Infusion Insulin Pumps Page 1 of
Moda Health Plan, Inc. Medical Necessity Criteria Subject: Origination Date: 05/15 Revision Date(s): 05/2015 Developed By: Medical Criteria Committee 06/24/2015 External Infusion Insulin Pumps Page 1 of
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding Guidance Co-morbidities associated with morbid obesity
 Billing and Coding Guidance Co-morbidities associated with morbid obesity AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT only copyright 2002-2014 American Medical Association. All Rights Reserved.
Billing and Coding Guidance Co-morbidities associated with morbid obesity AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT only copyright 2002-2014 American Medical Association. All Rights Reserved.
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_cord_stimulation 3/1980 10/2015 10/2016 10/2015 Description of Procedure or Service Spinal cord stimulation
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Intra-operative Nerve Monitoring Coding Guide. March 1, 2011
 Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
2014 Neurologic Physical Therapy Professional Education Consortium Webinar Course Descriptions and Objectives
 Descriptions and Neuroplasticity Health care providers are facing greater time restrictions to render services to the individual with neurological dysfunction. However, the scientific community has recognized
Descriptions and Neuroplasticity Health care providers are facing greater time restrictions to render services to the individual with neurological dysfunction. However, the scientific community has recognized
Electroneuromyographic studies
 Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
Electroneuromyographic studies in the diagnosis of Pudendal Entrapment Syndrome BY NAGLAA ALI GADALLAH PROFESSOR OF PHYSICAL MEDICINE, RHEUMATOLOGY& REHABILITATION AIN SHAMS UNIVERSITY Pudendal neuralgia
The Autonomic Nervous System Physiology Study Guide, Chapter 9
 Name: The Autonomic Nervous System Physiology Study Guide, Chapter 9 Lab Time: 1 Part I. Clinical Applications and Short Essay 1. After surgery, patients are often temporarily unable to urinate, and bowel
Name: The Autonomic Nervous System Physiology Study Guide, Chapter 9 Lab Time: 1 Part I. Clinical Applications and Short Essay 1. After surgery, patients are often temporarily unable to urinate, and bowel
Chapter 15 Anatomy and Physiology Lecture
 1 THE AUTONOMIC NERVOUS SYSTEM Chapter 15 Anatomy and Physiology Lecture 2 THE AUTONOMIC NERVOUS SYSTEM Autonomic Nervous System (ANS) regulates the activity of smooth muscles, cardiac muscles, and certain
1 THE AUTONOMIC NERVOUS SYSTEM Chapter 15 Anatomy and Physiology Lecture 2 THE AUTONOMIC NERVOUS SYSTEM Autonomic Nervous System (ANS) regulates the activity of smooth muscles, cardiac muscles, and certain
Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole)
 EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
A Study on The Prevalence of Cardiac Autonomic Neuropathy in Type-2 Diabetes in Eastern India
 ORIGINAL ARTICLE JIACM 2010; 11(3): 190-4 A Study on The Prevalence of Cardiac Autonomic Neuropathy in Type-2 Diabetes in Eastern India Abstract AK Basu*, R Bandyopadhyay**, S Chakrabarti***, R Paul****,
ORIGINAL ARTICLE JIACM 2010; 11(3): 190-4 A Study on The Prevalence of Cardiac Autonomic Neuropathy in Type-2 Diabetes in Eastern India Abstract AK Basu*, R Bandyopadhyay**, S Chakrabarti***, R Paul****,
Please read chapter 15, The Autonomic Nervous System, complete this study guide, and study this material BEFORE coming to the first class.
 Please read chapter 15,, complete this study guide, and study this material BEFORE coming to the first class. I. Introduction to the autonomic nervous system: Briefly describe the autonomic nervous system.
Please read chapter 15,, complete this study guide, and study this material BEFORE coming to the first class. I. Introduction to the autonomic nervous system: Briefly describe the autonomic nervous system.
Chapter 15. Autonomic Nervous System (ANS) and Visceral Reflexes. general properties Anatomy. Autonomic effects on target organs
 Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Autonomic Dysfunction in Children with Cerebral Palsy, Static Encephalopathy, and Similar Conditions by Susan Agrawal
 www.complexchild.com Autonomic Dysfunction in Children with Cerebral Palsy, Static Encephalopathy, and Similar Conditions by Susan Agrawal Many children with cerebral palsy, static encephalopathy, and
www.complexchild.com Autonomic Dysfunction in Children with Cerebral Palsy, Static Encephalopathy, and Similar Conditions by Susan Agrawal Many children with cerebral palsy, static encephalopathy, and
 E08.621 Diabetes mellitus due to underlying condition with foot ulcer E09.621 Drug or chemical induced diabetes mellitus with foot ulcer E10.10 Type 1 diabetes mellitus with ketoacidosis without coma E10.11
E08.621 Diabetes mellitus due to underlying condition with foot ulcer E09.621 Drug or chemical induced diabetes mellitus with foot ulcer E10.10 Type 1 diabetes mellitus with ketoacidosis without coma E10.11
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
Basic ICD-10-CM Documentation and Coding. Effective date: October 1, 2015. Presented by: Jenna Glenn, CPC May 6, 2015 1
 Basic ICD-10-CM Documentation and Coding Effective date: October 1, 2015 Presented by: Jenna Glenn, CPC May 6, 2015 1 Objectives Overview on what is ICD-10-CM Changes from ICD-9-CM to ICD-10-CM Importance
Basic ICD-10-CM Documentation and Coding Effective date: October 1, 2015 Presented by: Jenna Glenn, CPC May 6, 2015 1 Objectives Overview on what is ICD-10-CM Changes from ICD-9-CM to ICD-10-CM Importance
Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale.
![Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale. Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale.](/thumbs/25/5563775.jpg) [Date] [Name of Contact] [Title] [Name of Health Insurance Company] [Address] [City, State, Zip Code] Insured: [Patient Name] Policy Number: [Number] Group Number: [Number] Diagnosis: [Diagnosis and ICD-9-CM
[Date] [Name of Contact] [Title] [Name of Health Insurance Company] [Address] [City, State, Zip Code] Insured: [Patient Name] Policy Number: [Number] Group Number: [Number] Diagnosis: [Diagnosis and ICD-9-CM
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Reflex Physiology. Dr. Ali Ebneshahidi. 2009 Ebneshahidi
 Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Diabetes ICD9-CM Crosswalk to ICD10-CM 2015
 ICD-9-CM 250.00 Diabetes mellitus w/o mention of complication, type II or unspecified type, not stated as 250.01 Diabetes mellitus w/o mention of complication, type I (juvenile type), not stated as 250.02
ICD-9-CM 250.00 Diabetes mellitus w/o mention of complication, type II or unspecified type, not stated as 250.01 Diabetes mellitus w/o mention of complication, type I (juvenile type), not stated as 250.02
Chapter 13. Sympathetic Nervous System. Basic Functions of the Nervous System. Divisions of the Peripheral Nervous System
 Chapter 13 Drugs Affecting the Autonomic Basic Functions of the Recognizing changes in Internal environment External environment Processing and integrating changes Reacting to changes Upper Saddle River,
Chapter 13 Drugs Affecting the Autonomic Basic Functions of the Recognizing changes in Internal environment External environment Processing and integrating changes Reacting to changes Upper Saddle River,
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
Ms. Jackson is the Manager of Health Finance and Reimbursement, Division of Health Policy and Practice Services, Washington, DC.
 Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
Electrodiagnostic Testing with Same Day Evaluation Management By: Shane J. Burr, MD; Scott I. Horn, DO; Jenny J. Jackson, MPH, CPC; Joseph P. Purcell, DO Dr. Burr practices general inpatient and outpatient
AUTONOMIC NERVOUS SYSTEM
 AUTONOMIC NERVOUS SYSTEM Somatic efferent and ANS Somatic Efferent Control is over skeletal muscles. External environment This division of the PNS responds to some change in the external environment. single
AUTONOMIC NERVOUS SYSTEM Somatic efferent and ANS Somatic Efferent Control is over skeletal muscles. External environment This division of the PNS responds to some change in the external environment. single
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
ASSESSMENT: CLINICAL AUTONOMIC TESTING
 ASSESSMENT: CLINICAL AUTONOMIC TESTING Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology Overview. The focus of this report is on noninvasive, quantitative
ASSESSMENT: CLINICAL AUTONOMIC TESTING Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology Overview. The focus of this report is on noninvasive, quantitative
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION. Robert Dobbins, M.D. Ph.D.
 TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
CHAPTER 16: THE AUTONOMIC NERVOUS SYSTEM
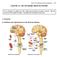 Unit 4: The Autonomic Nervous System 254 CHAPTER 16: THE AUTONOMIC NERVOUS SYSTEM Read: Chapter 16, pages 517-534. Read only the topics covered in lecture. We will not cover this chapter in detail. Complete
Unit 4: The Autonomic Nervous System 254 CHAPTER 16: THE AUTONOMIC NERVOUS SYSTEM Read: Chapter 16, pages 517-534. Read only the topics covered in lecture. We will not cover this chapter in detail. Complete
CLINICAL NEUROPHYSIOLOGY
 CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
CLINICAL NEUROPHYSIOLOGY Barry S. Oken, MD, Carter D. Wray MD Objectives: 1. Know the role of EMG/NCS in evaluating nerve and muscle function 2. Recognize common EEG findings and their significance 3.
Guidelines for Clinical Neurophysiology
 Guidelines for Clinical Neurophysiology These Guidelines have been drawn up along the lines of those of the Department of Clinical Radiology to help referring clinicians make the best use of Clinical Neurophysiology.
Guidelines for Clinical Neurophysiology These Guidelines have been drawn up along the lines of those of the Department of Clinical Radiology to help referring clinicians make the best use of Clinical Neurophysiology.
Alameda Alliance for Heath ICD-9 to ICD-10 TRANSLATION CODES E10.10
 DIABETES ICD-9 CM ICD-9 CM Volume 1 - Diagnosis Description ICD-10 CM - Diagnosis Code ICD-10 CM - Diagnosis Description 250.00 Diabetes mellitus without mention of complication, type II or unspecified
DIABETES ICD-9 CM ICD-9 CM Volume 1 - Diagnosis Description ICD-10 CM - Diagnosis Code ICD-10 CM - Diagnosis Description 250.00 Diabetes mellitus without mention of complication, type II or unspecified
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
trust clinical guideline
 CG23 VERSION 1.0 1/7 Guideline ID CG23 Version 1.0 Title Approved by Transient Loss of Consciousness Clinical Effectiveness Group Date Issued 01/01/2013 Review Date 31/12/2016 Directorate Authorised Staff
CG23 VERSION 1.0 1/7 Guideline ID CG23 Version 1.0 Title Approved by Transient Loss of Consciousness Clinical Effectiveness Group Date Issued 01/01/2013 Review Date 31/12/2016 Directorate Authorised Staff
6. 7. 8. 9. 10. 11. An overview EDX studies 12. 13. and inappropriate 14. 15. 16. 17. publication, EDX. from
 Recommendedd Policy for Electrodiagnostic Medicine Executive Summary The electrodiagnostic medicine (EDX) evaluation is an important and useful extensionn of the clinical evaluation of patients with disorders
Recommendedd Policy for Electrodiagnostic Medicine Executive Summary The electrodiagnostic medicine (EDX) evaluation is an important and useful extensionn of the clinical evaluation of patients with disorders
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]
![SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]](/thumbs/27/9667060.jpg) SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
Intraoperative Nerve Monitoring Coding Guide. March 1, 2010
 Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
Chapter 15. Neurotransmitters of the ANS
 Chapter 15 Neurotransmitters of the ANS Neurotransmitters and Receptors How can the same ANS neurons create different effects on different target tissue? Variety of neurotransmitters Secondly, different
Chapter 15 Neurotransmitters of the ANS Neurotransmitters and Receptors How can the same ANS neurons create different effects on different target tissue? Variety of neurotransmitters Secondly, different
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
Neuromuscular Medicine Fellowship Curriculum
 Neuromuscular Medicine Fellowship Curriculum General Review Goals and Objectives Attend weekly EMG sessions as assigned Take a Directed History and Exam of each EMG patient Attend every other week Muscle
Neuromuscular Medicine Fellowship Curriculum General Review Goals and Objectives Attend weekly EMG sessions as assigned Take a Directed History and Exam of each EMG patient Attend every other week Muscle
Common Surgical Procedures in the Elderly
 Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Common Surgical Procedures in the Elderly From hip and knee replacements to cataract and heart surgery, America s elderly undergo 20% of all surgical procedures. For a group that comprises only 13% of
Update and Review of Medication Assisted Treatments
 Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Relationship between fatigue, cognitive dysfunction and small fiber neuropathy. Elske Hoitsma
 Relationship between fatigue, cognitive dysfunction and small fiber neuropathy Elske Hoitsma Typical patient 45 year old male, Runs his own busy company, married, 4 young kids. Has always been very energetic
Relationship between fatigue, cognitive dysfunction and small fiber neuropathy Elske Hoitsma Typical patient 45 year old male, Runs his own busy company, married, 4 young kids. Has always been very energetic
MEDICAL POLICY No. 91104-R7 DETOXIFICATION I. POLICY/CRITERIA
 DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
ICD-10 IS COMING OCTOBER 1, 2014
 ICD-10 IS COMING OCTOBER 1, 2014 WHAT IS THE IMPACT ON THERAPY PRACTICES? CHET DESHMUKH, MBA, OTR/L, CPC, CHDA Overview Understanding the language of clinical diagnosis What is ICD? About ICD-9 CM Good
ICD-10 IS COMING OCTOBER 1, 2014 WHAT IS THE IMPACT ON THERAPY PRACTICES? CHET DESHMUKH, MBA, OTR/L, CPC, CHDA Overview Understanding the language of clinical diagnosis What is ICD? About ICD-9 CM Good
Nursing. Management of Spinal Trauma. Content. Objectives. Objectives
 7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
Status Active. Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015
 Status Active Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015 Anesthesia Policy Description: Definitions: This policy addresses
Status Active Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015 Anesthesia Policy Description: Definitions: This policy addresses
DNH 120 Management of Emergencies
 Revised: Fall 2015 DNH 120 Management of Emergencies COURSE OUTLINE Prerequisites: None Course Description: Studies the various medical emergencies and techniques for managing emergencies in the dental
Revised: Fall 2015 DNH 120 Management of Emergencies COURSE OUTLINE Prerequisites: None Course Description: Studies the various medical emergencies and techniques for managing emergencies in the dental
Overactive bladder is a common condition thought to. women, and is a serious condition that can lead to. significant lifestyle changes.
 Overactive bladder is a common condition thought to FADE UP TO WIDE SHOT OF FEMALE MODEL WITH TRANSPARENT SKIN. URINARY BLADDER VISIBLE IN PELVIC REGION affect over 16 percent of adults. It affects men
Overactive bladder is a common condition thought to FADE UP TO WIDE SHOT OF FEMALE MODEL WITH TRANSPARENT SKIN. URINARY BLADDER VISIBLE IN PELVIC REGION affect over 16 percent of adults. It affects men
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
ESC/EASD Pocket Guidelines Diabetes, pre-diabetes and cardiovascular disease
 Diabetes, prediabetes and cardiovascular disease Classes of recommendations Levels of evidence Recommended treatment targets for patients with diabetes and CAD Definition, classification and screening
Diabetes, prediabetes and cardiovascular disease Classes of recommendations Levels of evidence Recommended treatment targets for patients with diabetes and CAD Definition, classification and screening
WHEN TO ORDER; HOW TO INTERPRET
 ELECTROMYOGRAPHY AND 1 NERVE CONDUCTION TESTING: WHEN TO ORDER; HOW TO INTERPRET Ronald N. Kent, M.D., Ph.D. 2 ELECTROMYOGRAPHY AND NERVE CONDUCTION TESTING EMG/NCS Testing is a component of a complete
ELECTROMYOGRAPHY AND 1 NERVE CONDUCTION TESTING: WHEN TO ORDER; HOW TO INTERPRET Ronald N. Kent, M.D., Ph.D. 2 ELECTROMYOGRAPHY AND NERVE CONDUCTION TESTING EMG/NCS Testing is a component of a complete
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics. Yen Tibayan, M.D. Division of Cardiovascular Medicine
 Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Electrodiagnostic Testing
 Electrodiagnostic Testing Table of Contents Related Policies Policy Number 359 Policy Statement Purpose.. 1 2 Competency in Electrophysiologic Testing Original Effective Date: Current Approval Date: 1/1997
Electrodiagnostic Testing Table of Contents Related Policies Policy Number 359 Policy Statement Purpose.. 1 2 Competency in Electrophysiologic Testing Original Effective Date: Current Approval Date: 1/1997
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Nutrition. Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT
 1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
Multiple System Atrophy
 Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers
 Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers Introduction The health benefits of physical activity have been documented in numerous scientific
Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers Introduction The health benefits of physical activity have been documented in numerous scientific
Snoring and Obstructive Sleep Apnea (updated 09/06)
 Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
Dementia Episodes of Care
 A Guide for Bundled Payments This document reviews the considerations in establishing a bundled payment program for services provided to patients with dementia. In addressing dementia, there are two distinct
A Guide for Bundled Payments This document reviews the considerations in establishing a bundled payment program for services provided to patients with dementia. In addressing dementia, there are two distinct
Contractor Number 11302. Oversight Region Region IV
 Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Chemobrain. Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015
 Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
What are Dysautonomias?
 What are Dysautonomias? Dysautonomias are conditions where altered activity of the automatic nervous system (the autonomic nervous system) is harmful to health. -- 59 -- In Dysautonomias, What Goes Wrong?
What are Dysautonomias? Dysautonomias are conditions where altered activity of the automatic nervous system (the autonomic nervous system) is harmful to health. -- 59 -- In Dysautonomias, What Goes Wrong?
Documentation Guidelines for Physicians Interventional Pain Services
 Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
Documentation Guidelines for Physicians Interventional Pain Services Pamela Gibson, CPC Assistant Director, VMG Coding Anesthesia and Surgical Divisions 343.8791 1 General Principles of Medical Record
Kinesiology Graduate Course Descriptions
 Kinesiology Graduate Course Descriptions KIN 601 History of Exercise and Sport Science 3 credits Historical concepts, systems, patterns, and traditions that have influenced American physical activity and
Kinesiology Graduate Course Descriptions KIN 601 History of Exercise and Sport Science 3 credits Historical concepts, systems, patterns, and traditions that have influenced American physical activity and
Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW
 Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW Diagnosis of Dementia : DSM-IV criteria Loss of memory and one or more other cognitive abilities Aphasia Apraxia Agnosia
Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW Diagnosis of Dementia : DSM-IV criteria Loss of memory and one or more other cognitive abilities Aphasia Apraxia Agnosia
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
