NORTHWESTERN VEIN CENTER
|
|
|
- Winfred Poole
- 10 years ago
- Views:
Transcription
1 NORTHWESTERN VEIN CENTER
2 VEIN (8346) Northwestern Vein Center Chicago Division 675 N. St. Clair Street, Suite Chicago, Illinois Northwestern Vein Center Lake Forest Division 800 Westmoreland Road, Suite 102 Lake Forest, Illinois
3 P A T I E N T E D U C A T I O N VEINS T r e a t m e n t O p t i o n s NORTHWESTERN V E I N C E N T E R The circulatory system is made up of a network of blood vessels. Blood vessels are tube-like channels running throughout the body, which include arteries, veins, and capillaries. This handbook will help you understand the anatomy of leg veins, your treatment plan, and after care for: Endovascular Laser Ablation, Microphlebectomy, and Sclerotherapy. This information will answer many of your questions. Please use the notes section at the end of this booklet to record any unanswered questions you may have and discuss them with your doctor, physician assistant, or nurse. The following topics will be covered in this booklet: Anatomy...1 Endovenous Laser Ablation...3 Microphlebectomy...6 Sclerotherapy...8 Pelvic Congestion Syndrome...10 Notes...12 Arteries bring oxygen rich blood to all parts of the body. Veins return oxygen poor blood back to the heart. Anatomy The circulatory system is made up of a network of blood vessels. Blood vessels are tube-like channels running throughout the body, which include arteries, veins, and capillaries. Arteries bring oxygen rich blood to all parts of the body. Veins carry oxygen poor blood back to the heart. There are three vein groups found in the legs: The deep veins, enclosed by muscle, lie deep in the legs and return the majority of blood back to the heart. The superficial veins, which lie near the surface of the skin, make up an accessory system that carries only a small portion of blood back to the heart. The deep and the superficial veins are connected by perforator veins.
4 Anatomy Veins Normal Veins Varicose Long Saphenous Vein Valve Open Femoral Vein Popliteal Vein Short Saphenous Vein Valve Competent Perforating Veins Valve Incompetent D.C.Botos
5 Endovenous Laser Ablation What is endovascular laser venous ablation therapy? Your doctor is recommending endovascular laser venous ablation (ELVA) therapy because you have venous insufficiency in one or more of the larger superficial system veins in your legs. The vein most commonly associated with venous insufficiency is the great saphenous vein and its main branches. Venous insufficiency is a condition where the veins in the legs that are suppose to carry blood up, towards the heart, allow blood to reflux (or go the wrong way) down towards the feet. This causes pooling of blood in the legs and can lead to pain, swelling, or heaviness, as well as superficial varicose veins. Traditionally this malfunctioning vein has been treated with a surgical procedure in the operating room but ELVA is a less invasive way to fix the problem. Rather than remove the malfunctioning vein, as the surgical procedure would do, the vein is left in place but closed from the inside through a tiny nick in the skin. After a short recovery period, most people report a significant improvement in their physical symptoms because ELVA eliminates the conduit for refluxing blood. The maximal benefits from the procedure are measured at 6-8 weeks. Occasionally patients will need to have adjuvant treatments (microphlebectomy or sclerotherapy) to treat residual veins for persistent symptomatic or cosmetic reasons. What are the risks of this procedure? Bruising: Bruising is very common in the treated leg. It may be minimal, moderate, or even extensive. It can last for 1-2 weeks but in some cases can be visible for months. Phlebitis: A collection of blood in the treated vein(s) can become painful and/or tender, and cause some skin discoloration. This blood can be removed with a needle to speed the healing process but it may require several visits. Brown Stains on the Skin: Sometimes iron from the blood in bruises is deposited in the skin and leaves a brown stain (hyperpigmentation). It is usually subtle and resolves over the course of a few months. Occasionally it is darker brown and can last for several months to a couple years. In rare cases these brown stains may never completely fade. Scars: Visible scars are possible at the incision site(s). Though rare, these scars may appear lighter or darker than the surrounding skin when completely healed. Incomplete Closure: While the goal of treatment is closure of the greater saphenous vein and/or its major branches, occasionally the treated veins will not close completely. Wearing the prescriptive compression stockings as prescribed and complying with post-procedure activity restrictions will help to ensure complete closure. If there is incomplete closure, additional treatments may be necessary at additional expense to you and/or your insurance. Residual Veins: The goal of ELVA is relief of your symptoms of venous insufficiency, (i.e., leg swelling, heaviness, achiness, and chronic skin changes or ulcers). There may be residual veins you can see following ELVA. If you choose to treat these residual veins, there may be additional cost to you for these adjuvant treatments as they may not be covered by, or be billable to, your insurance. Blood Clots: While ELVA treatment involves the superficial venous system, there is risk of developing a blood clot in the deep system (a DVT or deep vein thrombosis). While this is very unlikely, should this occur, additional treatment may be necessary. Infection: Though unlikely, infection is possible at the incision site(s) and should infection occur, additional treatment may be necessary. Watch for signs of infection including redness, tenderness, pus, fever, nausea, and vomiting and call the Vein Center should any of these symptoms develop. During the day call and after hours call and ask for the Interventional Radiology Fellow on call. Nerve Problems: There are nerves that are occasionally irritated during the treatment. You may experience a brief twinge of pain or tingling if this occurs. Sometimes one or more of these sensory abnormalities may persist for a number of weeks or months. Though rare, there is a risk for permanent sensory (touch) or motor nerve damage from the ELVA procedure. 3
6 Allergic Reactions: Occasionally local allergies, (i.e., skin irritation from tape or skin cleanser) or systemic allergies (involving multiple organ systems) may occur in response to drugs or chemicals used during or after your treatment. No Relief of Symptoms: There are many causes of leg pain, swelling, and skin changes and there is no guarantee that this ELVT procedure will completely correct the symptoms you are experiencing. Will my insurance pay for ELVA? Most insurance companies will cover expenses for treatment of symptomatic venous insufficiency and varicose veins. Because this treatment can sometimes be considered cosmetic by the insurance industry, we will submit documentation to your insurance company prior to treatment to see if ELVA is a covered benefit. Once we have been notified of coverage for you, we will proceed with scheduling your procedure. Some insurance carriers or plans will only cover a predetermined percentage of such treatments. You may want to check with your carrier to determine what portion of the service provided you may be responsible for covering. While we will interact with your carrier, we cannot guarantee coverage, and you remain financially responsible for amounts not covered by your insurance. What are my pre-procedure instructions? 1. Fill any pre- and post-procedure medication prescriptions you may have gotten and be sure to get your compression stockings. You can purchase your compression stockings at a medical supply store. Please plan ahead and get your stockings well in advance of your procedure as the correct size often has to be ordered for you. Please also try your stockings on prior to your procedure to be sure they fit. They will be very snug and they ought to be long enough that they come to the very top of your leg (to your groin). 2. To decrease bruising avoid aspirin, ibuprofen, or other NSAIDS, for 5 days before the procedure. If another health care provider has prescribed these medications, please get his or her permission prior to stopping them. 3. You may eat, drink, and take all normal medications (except medications mentioned in #2) prior to your procedure. However, avoid caffeine and try to be well hydrated on the day of your procedure. 4. The pre-procedure medications can sometimes make people sleepy so we advise that you have someone with you to drive you home after the procedure. What can I expect on the day of my procedure? After you have had the opportunity to have all of your questions answered and have signed a consent form, you will lie on a procedure table and your leg will be prepped with a cleaning solution and wrapped in sterile towels. After numbing your skin with a local anesthetic, the doctor will make a small (2-4 mm) nick in the skin and then use an ultrasound machine to place a very small catheter into the problematic vein. Since the blood vessels do not have sensation (touch) nerves inside them, most patient do not feel the catheter passing through the vein. After placing a laser fiber into the vein through the catheter, the doctor will completely anesthetize the area around the entire length of the vein by injecting the local anesthetic with a small needle. The laser is then activated and pulled back, ablating the vein as it passes. Occasionally patients will feel a short pinch or twinge of pain when the laser is activated, but most patients feel nothing. Be sure to let your nurse and doctor know if you have any pain or are uncomfortable during the procedure. Your leg will be cleaned again and dressings will be placed over the small incision(s) and the injection sites. After getting your compression stockings on, you will be able to walk out of the procedure room and go home. While every patient s procedure is a little different, most ELVA procedures (including prep and clean-up time) are about 1 to 2 hours. 4
7 What are my post-procedure instructions? For the first 24 hours after the procedure most people rest and relax. Complete bed rest, however, is discouraged. Try to elevate your legs when you are sitting for the first hours after your procedure. Otherwise, carry on with all of your daily activities with a few exceptions: No heavy lifting (greater than pounds) for 2 weeks. Keep in mind that items like grocery bags, trash, laundry baskets, and children can weigh more than this. If you exercise regularly, please consult with the physician performing your procedure about your return to exercise activity. No tub baths, swimming, or soaking in water for 2 weeks after the procedure to prevent infection. Taking a shower is OK. You should NOT plan air-travel or long distance car travel for 2 weeks after the procedure. If you must travel within this time frame, please discuss this with the physician performing your procedure. Compression Stockings: Week One: Wear the stockings around the clock. Remove them once daily to shower and then put the stockings back on. Week Two: Wear the stockings during the day and in the evening, removing them only when you are sleeping. Week Three: Wear the stockings all day and remove in the evening if you will be inactive. If you will be active in the evening, keep them on until bedtime. REMEMBER: You can wear the stockings too little, but not too much. Dressing Care: Leave all dressings and compression stockings on for 24 hours after your procedure. You then can remove everything, with the exception of the steri-strips, and shower. (Steri-strips are white or brown and are placed directly on the skin, under the bulky white dressings. Leave the steri-strips on for up to 7 days. It is OK if they fall off sooner than that.) After you have dried your leg completely, put the compression stockings back on. What can I expect as I recover from my procedure? The majority of patients have a very easy recovery period with minimal pain. The following are normal and expected signs or symptoms after your procedure: Bruising, is sometimes quite extensive, along the length of the treated vein. The bruising can sometimes be painful as well, but your pain will improve as the bruising improves. Oozing of clear to pink red liquid from injection sites is normal. This is some of the anesthetic solution your doctor injected and it will stop oozing about a day after the procedure, or sooner. Tightness or stiffness (often described as a pulling sensation) along the treated vein can sometimes be felt beginning about a week after your procedure. This is normal. You may feel a cord (like a pencil) under the skin in this area as well. It can feel quite tender and even look red. This is normal as it is the vein that was treated in the ELVA procedure. This tightness and pain usually peaks at about 7-10 days after the procedure and then improves. You can apply warm compresses to the area twice a day, elevate the leg when sitting, and take Tylenol in addition to the NSAID you have been prescribed. Call the Vein Center if you have any questions or concerns ( or after hours and ask for the Interventional Radiology Fellow on call). Painful varicosities can persist after the ablation procedure particularly if they were large and tortuous prior to treatment. During your recovery these veins may feel tender, warm, and appear red. This is phlebitis and is treated via the same measures mentioned above (leg elevation, Tylenol, and warm compresses). Call the Vein Center with any questions or concerns ( or after hours and ask for the Interventional Radiology Fellow on call). 5
8 The following signs or symptoms may be signs of more serious problems. While rare, if they develop please call the Vein Center (or call and ask for the Interventional Radiology fellow on call if after hours): Fever, chills, nausea, or vomiting Pus draining from incision sites on the leg Redness extending beyond the incision sites on the leg Leg swelling and difficulty walking Follow-up: Patients return for a follow-up appointment 1 week after their procedure for a brief ultrasound exam sooner if there are problems or concerns. We encourage everyone to return for their follow-up visits even if you are feeling great, and especially if you are not. Though uncommon, occasionally patients will have residual pain but we can usually resolve this problem. Microphlebectomy What is a microphlebectomy? Microphlebectomy (pronounced mike-row-fle-beck-tomy) is a procedure to remove varicose veins on your legs. Varicose veins are thick, bulging, ropey veins that often throb or ache, especially when standing for prolonged periods. While varicose veins can be isolated in their occurrence, more often they are associated with venous insufficiency of an underlying superficial system vein. This is a condition where the larger veins in the legs allow some blood to leak (or reflux) towards your toes rather than flow upwards towards your heart. When the blood refluxes, it often fills and causes enlargement of smaller, more superficial vessels causing varicose veins. Even after the refluxing problem in the larger veins has been fixed (with a vein stripping or an ablation treatment), the varicose veins can remain. Microphlebectomy is a safe and effective way to remove these residual veins. Microphlebectomy is an outpatient procedure. After thoroughly numbing the areas around the veins, small nicks (2-4mm) are made in the skin, and the veins, or segments of the veins, are removed. Compression dressings and stockings will then be applied and you will be able to go home. What are my pre-procedure instructions? Unless told otherwise, you may eat and drink before your procedure. If possible, we advise that you avoid aspirin, ibuprofen, (i.e., Advil and Motrin), or other NSAIDS for 5 days prior to treatment, as they can be associated with increased bruising. If you have been advised by another physician to take these medications daily, please discuss this with him/her prior to stopping them. Please take any regular medications (other than those listed above) as you normally would on the day of your procedure. If you have not yet done so, you will need to get the prescribed compression stockings, as you will need to bring them with you on the day of your procedure. The stockings will be quite tight but their use is essential in the outcome of the procedure. It is very important that you have compression stockings that fit you properly. For this reason, it is a good idea to try them on prior to the day of your procedure. What can I expect on the day of my procedure? After you have had the opportunity ask all of your questions and sign a consent form, the physician performing your microphlebectomy will use a marker to map the skin over the areas of your varicose veins. The physician will have you stand while he/she does this because veins are better seen when you are standing. You will then lie down and your leg will be cleaned for the procedure with a sterilizing solution. The physician will completely anesthetize the areas around the veins and then proceed with making very small nicks (usually 2-4mm) in your skin through which he/she will remove the veins or segments of the veins. You should expect to have several incisions throughout the marked areas. While you may feel some pressure during this part of the procedure, you should not be in pain. If you are feeling uncomfortable during your procedure, be sure to let your nurse or physician know. When finished, your skin will again be cleaned, dressings and possible sutures will be applied, to close the incisions, and we will assist you with getting your compression stockings on. Procedure time varies but the average microphlebectomy takes about 1 hour. 6
9 What are my post-procedure instructions? While it is important to remain relatively active during your recovery most people find they are more comfortable resting and elevating their leg while sitting during the first 24 hours following a microphlebectomy. Complete bed rest is not recommended. Below are some specific guidelines for you to follow during your recovery. Leg Care: Leave the compression stockings and dressing in place for approximately 24 hours following your procedure. After 24 hours, remove the compression stocking and all the dressings except the steri-strips. (If you have them, the steri-strips will look like small pieces of tape applied directly on the skin over the small skin nicks.) Allow the steri-strips to fall off on their own (in 7-10 days). After you have bathed, dry your legs completely and reapply the compression stockings. No new dressings are needed. Bathing: You may shower but avoid baths or soaking (including swimming pools and spas) for at least 1 week after your procedure longer if the incisions have not yet completely healed. Compression Stockings: You will then wear the compression stockings around the clock for 1 week, removing only for bathing. The second week following your procedure, you will wear the stockings only during the day and can remove them at night while you are sleeping. During the third week you will only need to wear the stockings while engaged in significant physical activity. Exercise: We advise that you limit your exercising activity for 24 hours following your procedure and avoid lifting anything heavier than 15 pounds for 2 weeks following your procedure. Consult the physician performing your procedure regarding returning to exercise activity. Follow-up: Schedule a follow-up visit to the Vein Center 1 week following your microphlebectomy for a brief ultrasound exam and removal of any sutures placed. What can I expect as I recover from microphlebectomy? During the recovery period following microphlebectomy, the treated leg(s) may look quite bruised and mildly swollen. It is important to remember that the maximal outcome from this procedure will be realized at about 4-6 weeks following the procedure. You may or may not experience the following during your recovery: Bruising: Tenderness and bruising is expected following microphlebectomy. The use of the compression stockings as prescribed may decrease some bruising and pain and this will likely all resolve with time. Occasionally patients will get some hyperpigmentation over the areas of bruising or at the skin nicks. Wearing the compression stockings as prescribed and avoiding sun exposure to these areas will decrease (but not completely reduce) the likelihood of developing hyperpigmentation. Bleeding: Occasionally patients will experience some bleeding from one of the small nicks that were made in the skin. Should this happen, lie down and apply gentle pressure (or have someone else apply gentle pressure) to the area for 15 to 20 minutes. When the bleeding stops - reapply a clean dressing and continue to lie quietly for another 30 minutes. Although rare, if you are unable to get the bleeding to stop using these measures, go to your nearest emergency department. Swelling: Mild swelling at or near area of the microphlebectomy site is normal and will decrease with time. Widespread leg swelling and pain with walking can be a sign of a significant blood clot or infection. Should you have these symptoms, call the Vein Center (or and ask for the Interventional Radiology fellow on call if after hours). Scarring/Skin Changes: All skin may heal with some scarring. You will have small (2-3mm) scars that usually fade over time but may not completely go away. The scars may appear lighter or darker than the surrounding skin, even when completely healed. Please contact the Vein Center if you experience any of the following, as they may be a sign of infection: Red streaks around the skin nicks. Pus or any drainage that is not pink/red or clear. Swelling with extreme tenderness. Fever, chill, nausea, and vomiting. After hours for urgent or emergent issues call the hospital operator at and ask for the Interventional Radiology Fellow on call or go to your nearest emergency department. 7
10 Sclerotherapy What are spider veins and how did I get them? Spider veins are tiny, red or purple veins in the very superficial layers of the skin. They are often as wide as a human hair (although they can be larger), and can occur on the legs as threadlike isolated veins, fan-shaped areas, or in large clusters. They are harmless and pose no health risk, although to many people they are cosmetically unappealing. The causes of spider veins are not completely understood, but genetics, hormones, and pregnancy influence their development. Women are more likely to develop spider veins than men. Statistically 40-50% of women in western countries as compared to 10-20% of men develop some form of vein disorder by age 50. Other causes of vein development include standing for long periods of time, a traumatic leg injury that damaged leg valve structure, and multiple pregnancies. Spider veins are not varicose veins, although people can have either or both spider and varicose veins. Varicose veins are larger, ropey veins (often 5 mm in diameter or larger) and usually bulge from the skin. Varicose veins are associated with more severe symptoms (pain, heaviness, swelling, aching, skin changes, and open sores). Spider vein symptoms are usually minimal or nonexistent, and may include localized discomfort that often worsens during the menstrual cycle. Varicose and spider veins will not resolve without treatment, although the symptoms associated with them will often improve with regular use of prescription hosiery. What is sclerotherapy? Sclerotherapy is one of the most common, safe, and effective methods for treating unwanted spider or reticular veins on the legs. The treatment involves the injection of a small amount of an irritant solution, called a sclerosant, into the leg veins. Every patient is different, but several dozen injections may be needed for each leg during every session. Once injected, this sclerosant (i.e., concentrated salt water, diluted detergent, or glycerin) will irritate the inside of the vessel. After the injections are completed, compression dressings and stockings are applied. Over the next several weeks, the small veins will collapse, shrivel, and disappear. Bruising is common after injections are performed, and most patient s legs will look worse before better. The injection procedure may be mildly uncomfortable, but most patients tolerate the procedure without use of pre-treatment analgesics. Each sclerotherapy session is approximately 45 minutes, allowing for injections as well as dressing application. Sessions should not be scheduled less than 2 weeks apart, as your body will need time to heal the treated veins before additional treatment is done. Please schedule the recommended number of treatments 2-4 weeks apart to ensure optimal cosmetic outcome. Will it work for me? While there are no guarantees that sclerotherapy will work for everyone, our experience and evidence-based scientific data suggest that approximately 90% of the population will respond to sclerotherapy. Unfortunately, there is no way to predict who will and who will not respond to treatment, but if you have had successful sclerotherapy treatments in the past you will likely respond favorably to future treatments as well. It is unlikely that all unwanted veins will disappear after treatment. A successful course of sclerotherapy is a 75-80% improvement. It is important to note that most people will require several sclerotherapy sessions to achieve their optimal results. After each session, some treated veins will become smaller in diameter, and some will have resolved completely. The veins that remain will require additional treatments until they have markedly improved. Please be patient while undergoing sclerotherapy. Remember, these veins did not develop overnight, nor will they disappear overnight! Will my insurance pay for sclerotherapy? Spider vein treatment is considered cosmetic. This means that the medical providers of the Vein Center cannot and will not write letters of medical necessity for spider vein treatment. 8
11 What are the risks and alternatives to sclerotherapy? Below is a list of possible risks or outcomes of sclerotherapy: Bruising: temporary small black and blue marks Telangiectatic Matting: This is the growth of new, blush-like areas around veins that were injected. These veins usually resolve over several months but unresolved matted areas may be too small to be treated with additional sclerotherapy. Blood Clots: A collection of blood within a treated, superficial blood vessel is possible. It will feel like a small pea under your skin. This is not harmful and will resolve over time but if needed, a small nick can be made in the skin to help drain this trapped blood. Call the Vein Center if you are concerned you may have this problem. There is also a very small risk of developing a larger, more dangerous blood clot in larger veins (the deep veins) with sclerotherapy. However, this is usually associated with treatment of larger varicose veins and not spider veins. Hyperpigmentation: This is darkening of the skin. When you get a bruise, blood and the iron in the blood are deposited in the skin. It may look rusty brown in color and can get darker when exposed to the sun. Wearing the compression stockings as prescribed and avoiding sun exposure to any bruises you may get after the treatment might prevent or lessen hyperpigmentation. The hyperpigmentation usually fades with time, but it could take many months to years to fade, and may never completely fade away. Ulceration and Scarring: Though unlikely, small, open skin sores can develop in the areas treated. If not treated promptly and appropriately, these sores may enlarge, become infected, and leave a scar. If you are concerned you have a skin ulcer, contact the Vein Center immediately. Visual Changes: Patients will sometimes note vision changes during or after sclerotherapy including seeing floaters or small blind spots. If they occur, these symptoms are temporary and will resolve. Allergic Reactions: Though extremely rare, an allergic reaction to the solutions used in sclerotherapy is possible. It is essential that you communicate any allergies you may have to Vein Center providers. An allergic reaction can be as minor as a rash to something more severe, and potentially fatal anayphylaxis. For this reason, it is important that you communicate any discomfort you are experiencing during the treatment. If you experience any untoward symptoms after you leave the Vein Center (rash, throat tightness, difficulty breathing), you should report to the nearest hospital emergency department immediately. Alternative: Spider veins are harmless and not treating them certainly is an option. There are no creams or pills that have been shown to prevent or treat spider veins. While new laser systems are being introduced regularly, no surface laser system has been shown to be more effective than, or as safe as, sclerotherapy for spider veins on the legs. What kind of results can I expect after my sclerotherapy? Initially your legs will look worse following treatment. Redness and some mild tenderness at the treatment sites may persist for several days following your sclerotherapy session. Bruising is very common following the treatment and will resolve over several weeks. Once the redness and bruising have resolved, most people are very satisfied with the treatment. You will note the maximal outcome of sclerotherapy is effective in treating the spider veins that are present on your legs now. It will not prevent you from developing more spider veins in the future. Are there any pre-procedure directions I should follow? If possible, we advise that you avoid aspirin, ibuprofen, (i.e., Advil and Motrin), and vitamin E for 5 days prior to treatment, as they can be associated with increased bruising. If you have been advised by another physician to take these medications daily, please discuss this with him/her prior to stopping them. If you do not already have them, it is also important to get the prescribed compression stockings. You will need to bring them with you to your sclerotherapy session. Lastly, please do not shave your legs or apply creams, oils, or lotions on your legs the morning of your treatment. It is imperative that you are not pregnant or breast feeding if you are undergoing sclerotherapy. The medications used have not been tested in pregnant subjects, and the effects on a fetus are unknown. 9
12 What are my post-procedure instructions? Dressing Care: When you leave the Vein Center after your sclerotherapy session you will have compression dressings on as well as the compression stockings. Leave the entire cotton ball and tape dressings and the stockings in place until the following morning. In the morning, remove the stockings and all of the dressings. Leaving the dressing on longer will not give you a better outcome and in fact may increase your risk of infections. After you have showered and dried off completely, put only the stockings back on. No additional dressings are needed. Wound Care: Keep in mind that your legs could look quite bruised following sclerotherapy. It is important that you check your legs daily for signs of infection such as red streaks beyond the areas treated, extreme tenderness, pus or drainage. Though rare, should you see any of these signs call the Vein Center. When bruising is present, it is very important that you avoid exposing the area to sun (including artificial sun/ tanning) as you will increase your chances of getting hyperpigmentation skin changes. Widespread leg swelling and pain while walking is not normal. Call the Vein Center should you have these or any other concerning symptom. Compression Stockings: The purpose of the compression stockings as prescribed is very important to the success of the procedure. For the first 24 hours following the procedure, wear the compression stockings around the clock removing when you bathe. Reapply the stockings after bathing. For the remaining 6 days you can take the stockings off at night when you are sleeping but should otherwise wear the stockings all day. You will be wearing the stockings for a total of 1 week following the procedure. Bathing: Avoid swimming and soaking in water for the first week after the treatment to prevent infection. (This includes soaking in hot whirlpool tubs.) Exercise: For the first week after sclerotherapy, we advise that you avoid aerobic impact activities like running, jumping, and lifting weights with your legs. However, we do encourage you to walk a minimum of 30 minutes daily following your sclerotherapy to promote the growth of new healthy, veins. After 1 week you may return to you normal level of exercise. Follow-up: Allow 6-8 weeks after your final sclerotherapy session for most bruising to have resolved, and healing to have occurred. Some spider veins are likely to persist despite the most meticulous of sclerotherapy treatments. The expected result should be improvement, not perfection. We would be happy to see you to address additional questions or concerns after your sclerotherapy sessions are completed. Pelvic Congestion Syndrome (PCS) Chronic pelvic pain in women It is estimated that one-third of all women will experience chronic pelvic pain in their lifetime. Many of these women are told the problem is all in their head, but recent advancements now show the pain may be due to hard to detect varicose veins in the pelvis, a condition known as pelvic congestion syndrome. The causes of chronic pelvic pain are varied, but it is often associated with the presence of ovarian and pelvic varicose veins. Pelvic congestion syndrome is similar to varicose veins in the legs. In both cases, the valves in the veins that help return blood to the heart against gravity become weakened and don t close properly, which allows blood to flow backwards and pool in the vein causing pressure and bulging veins. In the pelvis, varicose veins can cause pain and affect the uterus, ovaries, and labia. Up to 15% of women, generally between the ages of 20 and 50, have varicose veins in the pelvis, although not all experience symptoms. The diagnosis is often missed because women lie down for a pelvic exam, relieving pressure from the ovarian veins, so that the veins no longer bulge with blood as they do while a woman is standing. Many women with pelvic congestion syndrome spend many years trying to get an answer as to why they have this chronic pelvic pain. Living with chronic pelvic pain is difficult and affects not only the woman directly, but also 10
13 her interactions with her family, friends, and her general outlook on life. Because the cause of the pelvic pain is not diagnosed, no therapy is provided even though therapeutic options are available. How common is PCS? Women with pelvic congestion syndrome are typically less than 45 years old and in their child bearing years. Ovarian veins increase in size related to previous pregnancies. Pelvic congestion syndrome is unusual in women who have not been pregnant. Chronic pelvic pain accounts for 15% of outpatient gynecologic visits. Studies show 30% of patients with chronic pelvic pain have pelvic congestion syndrome (PCS) as a sole cause of their pain and an additional 15% have PCS along with another pelvic pathology. What are the risk factors for PCS? Two or more pregnancies and pregnancy-associated hormonal increases Fullness of leg veins The chronic pain that is associated with this disease is usually dull and aching. The pain is usually felt in the lower abdomen and lower back. When is PCS pain most noticeable? Following intercourse Menstrual periods When tired or when standing (worse at end of day) Pregnancy What other symptoms are common with PCS? Irritable bladder Abnormal menstrual bleeding Varicose veins on labia, buttocks, or thigh Diagnosis and assessment Once other abnormalities or inflammation has been ruled out by a thorough pelvic exam, pelvic congestion syndrome can be diagnosed through several minimally invasive methods: Pelvic Venography: Thought to be the most accurate method for diagnosis, a venogram is performed by injecting contract dye in the veins of the pelvis to make them visible during an X-ray. MRI: May be the best non-invasive way of diagnosing pelvic congestion syndrome. The exam needs to be done in a way that is specifically adapted for looking at the pelvic blood vessels. A standard MRI may not show the abnormality. Pelvic Ultrasound: Usually not very helpful in diagnosing pelvic congestion syndrome unless done in a very specific manner with the patient standing while the study is being done. Ultrasound may be used to exclude other problems that might be causing pelvic pain. Transvaginal Ultrasound: This technique is used to see better inside the pelvic cavity. As with a pelvic ultrasound, it is not very good at visualizing the pelvic veins unless the woman is standing. However it may be used to exclude other problems. Treatment options Once a diagnosis is made, if the patient is symptomatic, an embolization should be done. Embolization is a minimally invasive procedure performed by interventional radiologists using X-ray imaging for guidance. During the outpatient procedure, the interventionalist inserts a thin catheter into a vein in the groin and guides it to the affected area using X-ray guidance. To seal the faulty, enlarged vein and relieve painful pressure, an interventional radiologist inserts tiny coils often with a sclerosing agent (the same type of material used to treat varicose veins) to close the vein. After treatment, patients can return to normal activities immediately. 11
14 Additional treatments are available depending on the severity of the woman s symptoms: Analgesics may be prescribed to reduce the pain. Hormones such as birth control pills decrease a woman s hormone level causing menstruation to stop and may be helpful in controlling her symptoms. Surgical options include a hysterectomy with removal of the ovaries, and tying off or removing the veins. Efficacy Embolization offers a safe, effective, minimally invasive treatment option that frequently relieves patient symptoms. The procedure is commonly successful in blocking the abnormal blood flow % of women have improvement in their symptoms after the procedure. Although women are usually improved, the veins are never normal and in some cases other pelvic veins are also affected, which may require further treatment. Notes 12
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
treatment of varicose and spider veins patient information SAMPLE a publication by advancing vein care
 treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
EndoVenous Laser Therapy (EVLT) Information Booklet. Dr. Dueck. Varicose Veins
 EndoVenous Laser Therapy (EVLT) Information Booklet Dr. Dueck Varicose Veins Varicose veins are abnormally large veins that protrude from under the skin in the legs. They can be associated with a brown
EndoVenous Laser Therapy (EVLT) Information Booklet Dr. Dueck Varicose Veins Varicose veins are abnormally large veins that protrude from under the skin in the legs. They can be associated with a brown
CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE
 Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Spotlight Series: Interventional Radiology. Varicose Veins and Venous Insufficiency
 Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Patient Information Understanding Varicose Veins
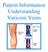 Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
What are spider veins? What is the best treatment for spider veins?
 Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
The Treatment of Varicose Veins and Spider Veins
 The Treatment of Varicose Veins and Spider Veins St. Joseph Vein Center Surgical Specialists of St. Joseph, P.C. Glen H. Hastings, M.D., F.A.C.S. 820 Lester Ave., Suite 105 St. Joseph, MI 49085 (269) 983-3368
The Treatment of Varicose Veins and Spider Veins St. Joseph Vein Center Surgical Specialists of St. Joseph, P.C. Glen H. Hastings, M.D., F.A.C.S. 820 Lester Ave., Suite 105 St. Joseph, MI 49085 (269) 983-3368
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
Varicose Vein Treatment (Endovenous Ablation of Varicose Veins)
 Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
THE VEIN CENTER. State-of-the-Art Treatment for Varicose Veins and Spider Veins
 THE VEIN CENTER State-of-the-Art Treatment for Varicose Veins and Spider Veins Vein Disorders Nearly 50 percent of the adult population suffers from undesirable, sometimes painful vein disease. The most
THE VEIN CENTER State-of-the-Art Treatment for Varicose Veins and Spider Veins Vein Disorders Nearly 50 percent of the adult population suffers from undesirable, sometimes painful vein disease. The most
Modern Varicose Vein Treatments: What Every Patient Should Know
 The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info
 TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins. Managing leg health during pregnancy
 Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins Managing leg health during pregnancy Common leg health problems during pregnancy Venous disorders
Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins Managing leg health during pregnancy Common leg health problems during pregnancy Venous disorders
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
V03 Varicose Veins Surgery
 V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
Varicose Veins and Spider Veins
 page 1 Varicose Veins and Spider Veins Q: What are varicose veins and spider A: Varicose (VAR-i-kos) veins are enlarged veins that can be blue, red, or fleshcolored. They often look like cords and appear
page 1 Varicose Veins and Spider Veins Q: What are varicose veins and spider A: Varicose (VAR-i-kos) veins are enlarged veins that can be blue, red, or fleshcolored. They often look like cords and appear
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose veins and spider veins
 Varicose veins and spider veins Summary Varicose veins are knobbly, twisted and darkish-blue in appearance, and are most commonly found on people s legs. Varicose veins are caused by faulty valves within
Varicose veins and spider veins Summary Varicose veins are knobbly, twisted and darkish-blue in appearance, and are most commonly found on people s legs. Varicose veins are caused by faulty valves within
Varicose veins - 1 -
 Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Patients First. Varicose Veins: Treatment Options. Deep veins, enclosed by muscle, lie deep in the legs and carry the most blood to the heart.
 Patient Education About your surgery Varicose Veins: Treatment Options Deep veins, enclosed by muscle, lie deep in the legs and carry the most blood to the heart. This handbook will help you understand
Patient Education About your surgery Varicose Veins: Treatment Options Deep veins, enclosed by muscle, lie deep in the legs and carry the most blood to the heart. This handbook will help you understand
Treatment for Varicose Veins
 Treatment for Varicose Veins Your blood vessels are made up of arteries and veins. Arteries bring blood rich in oxygen from the heart to all parts of your body. Veins carry blood back to the heart where
Treatment for Varicose Veins Your blood vessels are made up of arteries and veins. Arteries bring blood rich in oxygen from the heart to all parts of your body. Veins carry blood back to the heart where
F REQUENTLY A SKED Q UESTIONS. and Spider Veins
 page 1 Varicose Veins moves up the legs. If the one-way valves become weak, blood can leak back into the vein and collect there. This problem is called venous insufficiency. Pooled blood enlarges the vein
page 1 Varicose Veins moves up the legs. If the one-way valves become weak, blood can leak back into the vein and collect there. This problem is called venous insufficiency. Pooled blood enlarges the vein
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS)
 SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE
 CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Treatment by LASER. Understanding Varicose veins and. Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD)
 Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
Spider and Varicose Veins
 KRAMES. PATIENT EDUCATION Procedures for Spider and Varicose Veins How Vein Problems Develop Easing Symptoms with Self-Care Minimally Invasive and Surgical Treatment Options , J ;Yf 'i Understanding Problem
KRAMES. PATIENT EDUCATION Procedures for Spider and Varicose Veins How Vein Problems Develop Easing Symptoms with Self-Care Minimally Invasive and Surgical Treatment Options , J ;Yf 'i Understanding Problem
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Information for patients who require Foam Sclerotherapy for Varicose Veins.
 Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
INFORMATION DOCUMENT. Minimal Invasive Therapy of Leg Veins. Types of Veins. What is the mechanism by which veins develop?
 INFORMATION DOCUMENT Minimal Invasive Therapy of Leg Veins (Injection Microsclerotherapy / Ultrasound Guided Sclerotherapy / Endovenous Laser Therapy-EVLA and Modified Ambulatory Phlebectomy). This document
INFORMATION DOCUMENT Minimal Invasive Therapy of Leg Veins (Injection Microsclerotherapy / Ultrasound Guided Sclerotherapy / Endovenous Laser Therapy-EVLA and Modified Ambulatory Phlebectomy). This document
Percutaneous Abscess Drainage
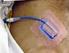 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
TheraSphere A Radiation Treatment Option for Liver Cancer
 TheraSphere A Radiation Treatment Option for Liver Cancer TheraSphere is a treatment which is done in the Interventional Radiology Clinic. If you have more questions after reading this handout, you can
TheraSphere A Radiation Treatment Option for Liver Cancer TheraSphere is a treatment which is done in the Interventional Radiology Clinic. If you have more questions after reading this handout, you can
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
LASER TREATMENT FOR VARICOSE VEINS
 LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
Muskegon Surgical Associates, P.C. 1316 Mercy Drive Muskegon, Michigan 49444 231-739-1932 231-739-9461 1-888-874-5892 (Toll Free) www.msapc.
 Muskegon Surgical Associates, P.C. 1316 Mercy Drive Muskegon, Michigan 49444 231-739-1932 231-739-9461 1-888-874-5892 (Toll Free) www.msapc.com www.msa-veincarecenter.com Welcome The Vein Care Center at
Muskegon Surgical Associates, P.C. 1316 Mercy Drive Muskegon, Michigan 49444 231-739-1932 231-739-9461 1-888-874-5892 (Toll Free) www.msapc.com www.msa-veincarecenter.com Welcome The Vein Care Center at
Venefit treatment for varicose veins
 Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Do you have any of these varicose vein symptoms?
 Do you have any of these varicose vein symptoms? Heaviness Achiness Swelling Throbbing Itching HASTI Symptoms Ask your doctor if Varithena is right for you Varithena (polidocanol injectable foam) is a
Do you have any of these varicose vein symptoms? Heaviness Achiness Swelling Throbbing Itching HASTI Symptoms Ask your doctor if Varithena is right for you Varithena (polidocanol injectable foam) is a
The veins of the lower limbs can be subdivided into three subtypes: deep veins, superficial veins, and connecting veins (figure 1).
 VEIN DISEASE Vein disease may seem insignificant and harmless at first, but if left untreated, it can develop into a major problem. It occurs when veins have trouble transporting blood back to the heart
VEIN DISEASE Vein disease may seem insignificant and harmless at first, but if left untreated, it can develop into a major problem. It occurs when veins have trouble transporting blood back to the heart
Chest Port Port-a-cath
 Patient Education Port-a-cath This handout explains what a chest port is and what to expect when you have one. What is a chest port? Your doctor has asked us to insert a chest port (also called a port-acath)
Patient Education Port-a-cath This handout explains what a chest port is and what to expect when you have one. What is a chest port? Your doctor has asked us to insert a chest port (also called a port-acath)
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Endovenous Laser Therapy
 Information for patients Endovenous Laser Therapy Northern General Hospital You have been given this leaflet because you will be having Endovenous Laser Therapy (EVLT). This leaflet explains more about
Information for patients Endovenous Laser Therapy Northern General Hospital You have been given this leaflet because you will be having Endovenous Laser Therapy (EVLT). This leaflet explains more about
Graduated compression hosiery (stockings)
 What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
Inferior Vena Cava Filter Placement and Removal
 Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
RENAL ANGIOMYOLIPOMA EMBOLIZATION
 RENAL ANGIOMYOLIPOMA EMBOLIZATION The information about renal angiomyolipomas on the next several pages includes questions commonly asked about the embolization procedure. Please take a few moments to
RENAL ANGIOMYOLIPOMA EMBOLIZATION The information about renal angiomyolipomas on the next several pages includes questions commonly asked about the embolization procedure. Please take a few moments to
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
MOHS MICROGRAPHIC SURGERY
 Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
Mary E. Maloney, MD Director Professor of Medicine David E. Geist, MD Assistant Professor of Medicine Dori Goldberg, MD Assistant Professor of Medicine Mark J. Scharf, MD Professor of Medicine Jason D.
After Your Gastric Bypass Surgery
 After Your Gastric Bypass Surgery UHN Information for patients and families Read this information to learn: what problems to look out for how to care for yourself at home about your follow-up appointment
After Your Gastric Bypass Surgery UHN Information for patients and families Read this information to learn: what problems to look out for how to care for yourself at home about your follow-up appointment
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Suffering from varicose veins? Patient Information. ELVeS Radial Minimally invasive laser therapy of venous insufficiency
 Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Cardiac Catheter Lab Information for patients having a Coronary Angiogram
 Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
SEDICO Newsletter Issue 8. Varicose veins
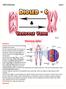 SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
Low Back Surgery. Remember to bring this handout to the hospital with you.
 Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Presence and extent of fatty liver or other metabolic liver diseases
 UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Blepharoplasty - Eyelid Surgery
 Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Breast Reduction Post-Operative Instructions
 Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions
 Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne
 VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne What are Varicose Veins Varicose veins are enlarged swollen veins. Most varicose veins are found in the legs. They are generally caused by a
VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne What are Varicose Veins Varicose veins are enlarged swollen veins. Most varicose veins are found in the legs. They are generally caused by a
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you.
 Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
The injection contains a local anesthetic for pain control and a steroid to reduce inflammation.
 Caudal Steroid Injection A Caudal Steroid Injection is done to provide pain relief. The injection provides pain relief by reducing swelling and irritation around nerve roots at the base of the spine or
Caudal Steroid Injection A Caudal Steroid Injection is done to provide pain relief. The injection provides pain relief by reducing swelling and irritation around nerve roots at the base of the spine or
Preparation for your vasectomy
 Preparation for your vasectomy You have been scheduled for a vasectomy with the SIU Division of Urology. Please read through this information carefully. Vasectomies are performed in the REI clinic, 751
Preparation for your vasectomy You have been scheduled for a vasectomy with the SIU Division of Urology. Please read through this information carefully. Vasectomies are performed in the REI clinic, 751
Liver Transarterial Chemoembolization (TACE) Cancer treatment
 Patient Education Liver Transarterial Chemoembolization (TACE) Cancer treatment This handout explains what liver transarterial chemoembolization (TACE) is and what to expect with this cancer treatment.
Patient Education Liver Transarterial Chemoembolization (TACE) Cancer treatment This handout explains what liver transarterial chemoembolization (TACE) is and what to expect with this cancer treatment.
POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION
 www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
Laser of the Vulva. This is a surgery where your doctor will use a laser light to remove unhealthy tissue.
 What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Information for you Treatment of venous thrombosis in pregnancy and after birth. What are the symptoms of a DVT during pregnancy?
 Information for you Treatment of venous thrombosis in pregnancy and after birth Published in September 2011 What is venous thrombosis? Thrombosis is a blood clot in a blood vessel (a vein or an artery).
Information for you Treatment of venous thrombosis in pregnancy and after birth Published in September 2011 What is venous thrombosis? Thrombosis is a blood clot in a blood vessel (a vein or an artery).
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION
 A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
A PATIENT S GUIDE TO CARDIAC CATHETERIZATION The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to cardiac catheterization. In the following pages, we will
Lumbar or Thoracic Fusion +/- Decompression
 Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Cardiac Catheterization Lab Procedures
 UW MEDICINE PATIENT EDUCATION Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed
UW MEDICINE PATIENT EDUCATION Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed
VASECTOMY What is Vasectomy? How is the procedure performed? What is the no-scalpel method of doing vasectomy? When can I go back to work?
 VASECTOMY What is Vasectomy? Every man has a basic right to a vasectomy, a valuable medical procedure. Before you actually have a vasectomy, you should think about it carefully, because a vasectomy is
VASECTOMY What is Vasectomy? Every man has a basic right to a vasectomy, a valuable medical procedure. Before you actually have a vasectomy, you should think about it carefully, because a vasectomy is
Hysteroscopy. What is a hysteroscopy? When is this surgery used? How do I prepare for surgery?
 What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Information for patients who require Foam Sclerotherapy for Varicose Veins
 Information for patients who require Foam Sclerotherapy for Varicose Veins Why do I need treatment for varicose veins? Deep veins Everybody has 2 sets of veins in their legs. These are called the superficial
Information for patients who require Foam Sclerotherapy for Varicose Veins Why do I need treatment for varicose veins? Deep veins Everybody has 2 sets of veins in their legs. These are called the superficial
