Dynamic stabilization of the lumbar spine Robert W. Molinari
|
|
|
- Lydia Chapman
- 8 years ago
- Views:
Transcription
1 Dynamic stabilization of the lumbar spine Robert W. Molinari Purpose of review This is a review of the recent literature involving dynamic posterior stabilization in the lumbar spine. Recent findings As an alternative to fusion, a mobile, dynamic stabilization restricting segmental motion would be advantageous in various indications, allowing greater physiological function and reducing the inherent disadvantages of rigid instrumentation and fusion. Dynamic stabilization may provide benefit by altering the transmission of abnormal loads across the degenerative disc space without the elimination of movement. Further study is required to determine optimal design, clinical indications, and clinical outcomes. Summary Much of the experience with dynamic lumbar stabilization is from Europe. There has been little experience with these devices in the USA and data on long-term clinical outcomes are lacking. Much of the European experience has been with two dynamic stabilization devices, the Graf ligament and Dynesys. Biomechanical testing of newer posterior fulcrum-assisted dynamic systems has been recently reported. Short-term follow-up data on the X-STOP device, which is another alternative to lumbar fusion, has been recently reported. Keywords dynamic stabilization, lumbar, soft stabilization, spine, X-STOP Curr Opin Orthop 18: ß 2007 Lippincott Williams & Wilkins. Department of Orthopaedic Surgery, Division of Spinal Surgery, University of Rochester, Rochester, New York, USA Correspondence to Robert W. Molinari, MD, University of Rochester Medical Center, Box 665, 601 Elmwood Ave, Rochester, NY 14642, USA Tel: ; fax: ; bobmol@aol.com Current Opinion in Orthopaedics 2007, 18: Abbreviation TOPS total posterior element-replacement system ß 2007 Lippincott Williams & Wilkins Introduction Spinal fusion remains the gold standard for surgical management of instability and mechanical low-back pain. However, even in carefully selected patients, successful clinical results can be difficult to achieve. Reasons for failure include pseudarthrosis and adjacent segment disease. Although dynamic stabilization seems promising in some clinical reports, one should take a cautious approach to any new spinal-implant system. An implant for fusion only has to serve a temporary stabilization until fusion has taken place; on the other hand, a dynamic stabilization system has to provide stability throughout its life. Implant loosening following fusion surgery is common in the presence of pseudarthrosis. With dynamic stabilization, the implant has to stay anchored to the bone despite allowing movement. Any mismatch between the kinematics of the implant system and the motion segment, in particular any discrepancy between their instantaneous axis of rotation, would result in the implant bearing unexpected load at certain ranges of motion. The need for strict bench testing in the laboratory, therefore, cannot be over-emphasized. The few dynamic stabilization systems that have had clinical applications so far have produced some clinical outcomes comparable to that of fusion. Most importantly, no prospective randomized controlled trial has been reported yet, which is an essential requirement for practice of evidence-based medicine. The need for more clinical outcomes data was recently emphasized by Nockels [1] in his review of dynamic lumbar stabilization in the management of painful lumbar disorders. Biomechanics Schmoelz et al. [2] investigated the Dynesys dynamic posterior nonfusion system to determine the magnitude of the stabilization and the effect of the stabilization on the adjacent lumbar segment. Six lumbar cadaver spines were fixed in a spine tester and loaded in pure moments in three main motion planes. For each spine, four different stages were tested: intact spine, defect in the middle segment, Dynesys stabilization, and fixation with rigid pedicle screws. Intersegmental motions were measured at all levels. For the bridged segment, Dynesys stabilized the spine and was more flexible than rigid internal fixation. This difference was most pronounced in extension, with the Dynesys restoring motion back to the level of the intact spine. Interestingly, the motion in the adjacent segments was not influenced by either stabilization method. The study suggests that Dynesys provides substantial stability in cases of degenerative 215
2 216 Thoracolumbar spine spinal pathologies but may not produce any difference on adjacent segment motion [2]. Schmoelz et al. [3] performed a study in vitro of intradiscal pressure to determine the influence of dynamic stabilization on the load bearing of the bridged disc. Using six cadaver spines, four different states of the specimens were studied: intact, destabilized, Dynesys-stabilized, and rigidly fixed with an internal fixator. In the neutral position, there were no significant differences in the disc pressure for the four conditions. During the course of loading, both the Dynesys and the internal fixator significantly reduced the pressure change from neutral to extension in comparison to the intact spine. However, there was no significant pressure changes noted from neutral to flexion. Only the internal fixator demonstrated slightly reduced discal pressure change in axial rotation. Dynesys showed no significant difference in axialrotation disc pressure when compared to the intact spine. No changes were seen in adjacent disc pressures for either Dynesys or the internal fixator. The results demonstrated that the intradiscal pressures for both Dynesys and rigid internal fixation were similar, but altered compared to the intact disc [3]. Recently Wilke et al. [4 ] reported the biomechanical evaluation of a new total posterior-element-replacement system at the L4 L5 segment in cadaver spines. The total posterior element-replacement system (TOPS) implant is designed to replace the entire posterior elements while providing flexible restabilization. It consists of bilateral pedicle screws attached to an elastic disc element capable of transmitting tensile and compressive loads (Fig. 1). In this study the implant almost ideally restored range of motion in lateral bending and axial rotation compared to the intact spine. In the sagittal plane, 85% of the intact range of motion could be obtained. The authors conclude that the TOPS implant almost ideally restored range of motion and loading of the anterior disc. The implant mimics the biomechanical behavior of the posterior complex of the spine after laminectomy and facetectomy [4 ]. Clinical outcomes of posterior dynamic stabilization There has been little clinical experience with posterior dynamic stabilization devices in the USA. Much of the reported European clinical experience has been with two dynamic stabilization devices, Dynesys and the Graf ligament. Dynesys In 1994, a dynamic transpedicular system (Dynesys) was introduced to the market, promoting the concept that stabilization is possible without bone grafting. This Figure 1 Schematic diagrams (a, b) and posterior view (c) of the total posterior element-replacement system (TOPS) implant, which is fixed with regular polyaxial transpedicular screws to the spinal segment Taken from [4 ]. dynamic neutralization system for the posterior spine is a pedicle screw system for mobile stabilization, consisting of titanium-alloy screws connected by an elastic synthetic compound, controlling motion in any plane (Fig. 2). Several recent European studies have reported shortterm clinical outcomes. Schnake et al. [5] evaluated whether elastic stabilization with the Dynesys system provides enough stability to prevent instability after decompression for spinal stenosis with degenerative spondylolisthesis. Twenty-six patients with lumbar spinal stenosis and degenerative spondylolisthesis underwent interlaminar decompression and dynamic stabilization with the Dynesys system. Minimum follow-up was 2 years. Mean leg pain decreased significantly (P < 0.01), and mean walking distance improved significantly to more than 1000 m (P < 0.01). There were five patients (21%) who still had some claudication. A total of 21 patients (87.5%) were satisfied and indicated that they would undergo the same procedure again. Radiographically, no significant progression of spondylolisthesis could be detected. The implant failure rate was 17%, and none of the implant failures was clinically symptomatic. In elderly patients with spinal stenosis with degenerative spondylolisthesis, dynamic stabilization with the Dynesys system in addition to decompression leads to similar clinical results as seen in established protocols using decompression and fusion with pedicle screws. Dynesys also maintains enough stability to prevent further progression of spondylolisthesis or instability [5].
3 Stabilization of the lumbar spine Molinari 217 Figure 2 Dynesys with the pedicle screws connected by the synthetic flexible cords, and spacers necessitated further surgery. Mean pain and function scores improved significantly from baseline to followup and Oswestry Disability Scores improved from 55.4 to 22.9%. These study results compare well with those obtained by conventional procedures. Dynamic neutralization may be a safe and effective alternative in the treatment of unstable lumbar conditions [6]. Dynamic stabilization may prevent further degeneration of the lumbar spine. Putzier et al. [7] evaluated the addition of dynamic stabilization to lumbar discectomy procedures in an attempt investigate the effect of dynamic stabilization on segmental degeneration after discectomy. Eighty-four patients with initial-stage disc degeneration (Modic 1) underwent discectomy for symptomatic disc herniation and 35 had the addition of Dynesys stabilization. At mean 34-month follow-up a significant increase in Oswestry Disability Scores and Visual Analog Scale results was observed only in the nonstabilized group. No progression of disc degeneration was noted in the Dynesys group at follow-up, whereas radiographic signs of accelerated degeneration were noted only in the discectomy group. The authors concluded that dynamic stabilization is useful to prevent progression of initial disc degeneration in segments after lumbar discectomy [7]. Taken from [2]. Stoll et al. [6] reported the results of a prospective, multicenter study evaluating the safety and efficacy of Dynesys in the treatment of lumbar instability conditions. The authors evaluated pre and postoperative pain, function, and radiographic data on a consecutive series of 83 patients. Indications consisted of unstable segmental conditions mainly combined with spinal stenosis (60.2%) and with degenerative discs (24.1%), in some cases with disc herniation (8.4%), and with revision surgery (6%). Thirty-nine patients had degenerative spondylolisthesis, and 30 patients had previous lumbar surgery. In 56 patients, the instrumentation was combined with direct decompression. The mean age at operation was 58 years and the mean follow-up time was 38 months. Additional surgery in the follow-up period included implant removal and conversion into spinal fusion with rigid instrumentation for persistent pain in three cases, laminectomy of an index segment in one case and screw removal due to loosening in one case. In seven cases, radiographic signs of screw loosening were observed. In seven cases, adjacent segment degeneration Although the Dynesys semirigid fixation system has been in clinical use for more than 5 years, only one study from a disinterested research group has reported on patientoriented outcome after surgery with Dynesys. Grob et al. [8] reported the clinical experience with Dynesys semirigid lumbar fixation in 31 patients with follow-up of more than 2 years. The primary indication for surgery was degenerative disc with stenosis and associated instability and 35% of the patients had prior spinal surgery. In 23% of cases, one level was instrumented, in 52% two levels, 13% three levels, and 3% four levels. Forty-two percent of the patients also had decompression. Within the 2-year follow-up period, six of 31 (19%) patients had required or were scheduled for further surgical intervention. The following global outcomes were reported: back symptoms, 67% improved, 30% same, 3% worse; leg symptoms, 64% improved, 21% same, 15% worse; ability to do physical activity and sports, 40% improved, 33% same, 27% worse; quality of life, 50% improved, 37% same, 13% worse; how much the operation helped, 29% helped a lot, 23% helped, 10% only helped a little, 35% didn t help, 3% made things worse. The results of this study indicate that both back and leg pain are, on average, still moderately high 2 years after instrumentation with the Dynesys system. Only half of the patients declared that the operation had helped and had improved their overall quality of life. Less than half of the patients reported improvement in their functional capacity. The reoperation rate after Dynesys was relatively high. The results
4 218 Thoracolumbar spine Figure 3 Radiograph with Dynesys of the lumbar spine Figure 4 Graf ligamentoplasty with the implant shown disassembled (top) and in situ (bottom) In the radiographs, only the pedicle screws are visible. Taken from [8]. The components include a nonelastic band, which is secured around two pedicle screw heads with a metal band. Taken from [1]. provide no support for the notion that dynamic fixation of the lumbar spine results in better patient-oriented outcomes than those typical of fusion [8] (Fig. 3). Graf ligamentoplasty The Graf ligament stabilizes the lumbar segment through the coaptation of the bilateral facet joints, and it is the first posterior dynamic stabilization device to be widely clinically evaluated. The Graf procedure reportedly has the potential to treat flexion instability but cannot correct vertebral slippage or deformity. The most common surgical indication is degenerative lumbar disorder with less than 25% of vertebral slip, minimal disc space narrowing, and facet arthrosis (Fig. 4). In the mid and long term, Graf ligamentoplasty may reduce the risk of adjacent segment degeneration. Kanayama et al. [9] reported the adjacent-segment morbidity after Graf ligamentoplasty compared to posterolateral lumbar fusion at a minimum of 5-year follow-up in 45 patients. Although there was no difference in the preoperative adjacent-segment disc condition between the two groups, radiographic evidence of adjacent-segment degeneration at final follow-up was more frequent in the posterolateral-lumbar-fusion group than the Graf group (25 and 6% at L1 L2, 38 and 6% at L2 L3, 38 and 18% at L3 L4, and 43 and 18% at L5 S1, respectively). One case in the Graf group (6%) and and five cases in the posterolateral-lumbar-fusion group (19%) required additional surgery for adjacent-segment degeneration. The authors concluded that in well selected patients, Graf ligamentoplasty lowers the rate of adjacent-segment degeneration [9]. Rigby et al. [10] reported the mid and long-term followup of Graf ligament stabilization. A retrospective review of 51 patients with a mean follow-up time of 4 years was reported. The average age of the patients was 41 years. The Oswestry Disability Score only improved an average of six points with longer follow-up. There were 12 complications and four required additional surgery. Seven patients (14%) went on to require bony-fusion procedures. Forty-one percent of the group would have chosen not to have the operation again. The authors concluded that longer-term results of this technique are not as encouraging as earlier studies and that the continued use of the procedure should be viewed with caution [10]. Although series have been reported showing encouraging results with the use of the Graf ligamentoplasty for lowback pain no comparative data are available on outcomes when compared with more conventional treatments. A retrospective case control study compared Graf ligamentoplasty and instrumented posterolateral fusion in a consecutive series of 83 patients operated on by a single surgeon. Patients underwent either soft-tissue stabilization using the Graf ligament or posterolateral fusion with
5 Stabilization of the lumbar spine Molinari 219 pedicle-screw instrumentation. There was a significantly better outcome, when measured by the Low Back Outcome Score, in the group of patients managed by posterolateral fusion at 1 year (P ¼ 0.02), although at 2 years the difference was less (P < 0.34). This study demonstrated that the outcome after soft-tissue stabilization was associated with a worse outcome at 1 year and a significantly higher revision rate at 2 years. Revision was associated with a poor outcome similar to that seen in revision after fusion [11]. Future direction Studies have demonstrated that soft stabililization with the Graf ligament restricts abnormal spinal segment motion but increases the segmental disc pressure. The Dynesys system, which uses a plastic cylinder around the ligament to prevent overloading the disc, has been shown to restrict extension. It can also cause loss of lordosis with excessive distraction. The ideal system for dynamic stabilization of the lumbar spine does not exist. Recently, Sengupta and Mulholland [12] described fulcrumassisted dynamic stabilization as a new concept in the surgical treatment of degenerative low-back pain. The device consisted of pedicle screws attached to a ligament with the addition of a fulcrum in front of the ligament to unload the disc. It was hypothesized that the fulcrum should transform the compressive force of the ligament behind into a distraction force in front and unload the disc. The new dynamic stabilization device was evaluated in cadaver spines. The results indicated that the fulcrums reduced disc pressure and maintained lordosis. Increasing fulcrum length resulted in progressive unloading of the disc. As the fulcrum length approximated the height of the motion segment, the lordosis was lost, and the disc was completely unloaded. The authors concluded that the novel fulcrum-assisted soft stabilization (FASS) system can unload the disc, control range of motion, and maintain lordosis. These parameters may be controlled with a suitable combination of ligament and fulcrum system. The study indicates the desirable biomechanical properties of the fulcrum and ligament for future development of a clinically applicable prototype [12] (Fig. 5). Figure 5 The concept of the fulcrum-assisted soft stabilization (FASS) system (a) A diagram of a normal-motion segment in the lumbar spine. Application of a ligament to the pedicle screws across the motion segment increases the load at the posterior aspect of the disc. (b) Introduction of a fulcrum in front of the ligaments in the FASS system may unload the disc. Taken from [12]. spinal stenosis. The mean improvement in Oswestry Disability Score was 29 points. The overall success rate of the X-STOP device was 78% (14 of 18 patients) and the rate of clinical success remained consistent with the 2-year follow-up results previously reported by the same authors. The authors concluded that the intermediateterm outcomes of X-STOP are stable over time [13]. Anderson et al. [14] reported the results of X-STOP for the treatment of neurogenic claudication in patients with degenerative spondylolisthesis. Forty-two patients underwent X-STOP surgery and 33 patients were treated nonoperatively. Two-year follow-up data were obtained in 70 of the 75 patients. There was statistically significant improvement in the SF-36 scores of the X-STOP devicetreated patients but not in those of the nonoperative controls. Overall clinical success occurred in 63% of the X-STOP-treated patients and only 13% of the controls. Spondylolisthesis and segmental kyphosis were unaltered. The authors concluded that the X-STOP Figure 6 The X-STOP rigid interspinous process distraction device and case example X-STOP Another alternative to lumbar fusion is the X-STOP interspinous process distraction device. The X-STOP implant is a rigid titanium-alloy device that is placed between the spinous processes to reduce the canal and foraminal narrowing that occurs in extension. The X-STOP device is designed to distract the posterior elements of the stenotic lumbar segment and place it in flexion to treat neurogenic claudication (Fig. 6). Kondrashov et al. [13] recently reported the 4-year followup outcomes of X-STOP in 18 patients with lumbar Taken from [13].
6 220 Thoracolumbar spine device was more effective than nonoperative management of neurogenic claudication secondary to degenerative lumbar spondylolisthesis [14]. Conclusion Many questions remain unanswered regarding the safety and efficacy of dynamic stabilization over the long term. Will dynamic stabilization be superior to lumbar decompression or fusion for a select group of patients? How long can we expect these devices to last before failing? While theoretical advantages exist, additional outcomes data are certainly required to establish the clinical efficacy of these devices. The few posterior dynamic stabilization systems that have had clinical applications so far have produced outcomes somewhat comparable with fusion. No severe adverse events caused by these implants have been reported. Long-term follow-up data and well controlled, prospective randomized studies do not exist, but are essential to prove the safety, efficacy, appropriateness, and economic viability of these methods. References and recommended reading Papers of particular interest, published within the annual period of review, have been highlighted as: of special interest of outstanding interest Additional references related to this topic can also be found in the Current World Literature section in this issue (p. 290). 1 Nockels RP. Dynamic stabilization in the surgical management of painful lumbar spinal disorders. Spine 2005; 30 (16 Suppl):S68 S72. 2 Schmoelz W, Huber JF, Nydegger T, et al. Dynamic stabilization of the lumbar spine and its effects on adjacent segments: an in vitro experiment. J Spinal Disord Tech 2003; 16: Schmoelz W, Huber JF, Nydegger T, et al. Influence of a dynamic stabilisation system on load bearing of a bridged disc: an in vitro study of intradiscal pressure. Eur Spine J 2006; 15: Wilke HJ, Schmidt H, Werner K, et al. Biomechanical evaluation of a new total posterior-element replacement system. Spine 2006; 31: The TOPS implant almost ideally restored range of motion and loading of the anterior disc. The implant mimics the biomechanical behavior of the posterior complex of the spine after laminectomy and facetectomy. 5 Schnake KJ, Schaeren S, Jeanneret B. Dynamic stabilization in addition to decompression for lumbar spinal stenosis with degenerative spondylolisthesis. Spine 2006; 31: Stoll TM, Dubois G, Schwarzenbach O. The dynamic neutralization system for the spine: a multicenter study of a novel nonfusion system. Eur Spine J 2002; 11 (suppl 2):S170 S Putzier M, Schneider SV, Funk JF, et al. The surgical treatment of the lumbar disc prolapse: nucleotomy with additional transpedicular dynamic stabilization versus nucleotomy alone. Spine 2005; 30:E109 E Grob D, Benini A, Junge A, Mannion AF. Clinical experience with the Dynesys semirigid fixation system for the lumbar spine: surgical and patient-oriented outcome in 50 cases after an average of 2 years. Spine 2005; 30: Kanayama M, Hashimoto T, Shigenobu K, et al. Nonfusion surgery for degenerative spondylolisthesis using artificial ligament stabilization: surgical indication and clinical results. Spine 2005; 30: Rigby MC, Selmon GP, Foy MA, Fogg AJ. Graf ligament stabilisation: mid- to long-term follow-up. Eur Spine J 2001; 10: Hadlow SV, Fagan AB, Hillier TM, Fraser RD. The Graf ligamentoplasty procedure. Comparison with posterolateral fusion in the management of low back pain. Spine 1998; 23: Sengupta DK, Mulholland RC. Fulcrum assisted soft stabilization system: a new concept in the surgical treatment of degenerative low back pain. Spine 2005; 30: Kondrashov DG, Hannibal M, Hsu KY, Zucherman JF. Interspinous process decompression with the X-STOP device for lumbar spinal stenosis: a 4-year follow-up study. J Spinal Disord Tech 2006; 19: Anderson PA, Tribus CB, Kitchel SH. Treatment of neurogenic claudication by interspinous decompression: application of the X STOP device in patients with lumbar degenerative spondylolisthesis. J Neurosurg Spine 2006; 4:
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA
 LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011
 1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
Motion Preservation. Hansen Yuan, MD President, Spine Arthroplasty Society
 Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
Minimum Four-Year Follow-up of Spinal Stenosis With Degenerative Spondylolisthesis Treated With Decompression and Dynamic Stabilization
 Minimum Four-Year Follow-up of Spinal Stenosis With Degenerative Spondylolisthesis Treated With Decompression and Dynamic Stabilization SPINE Volume 33, Number 18, pp E636 E642 2008, Lippincott Williams
Minimum Four-Year Follow-up of Spinal Stenosis With Degenerative Spondylolisthesis Treated With Decompression and Dynamic Stabilization SPINE Volume 33, Number 18, pp E636 E642 2008, Lippincott Williams
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
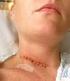 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Issued and entered this _6th_ day of October 2010 by Ken Ross Commissioner ORDER I PROCEDURAL BACKGROUND
 STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Biomechanics of the Lumbar Spine
 Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
1. Proposal Abstract. Table 1. Degeneration distribution of tested discs Grade I Grade II Grade III Grade IV Grade V # of discs tested 13 9 12 5 1
 1. Proposal Abstract Purpose: Chronic low back pain (LBP) is a common musculoskeletal disorder that significantly impacts public health. However the mechanism of chronic LBP is still not fully understood.
1. Proposal Abstract Purpose: Chronic low back pain (LBP) is a common musculoskeletal disorder that significantly impacts public health. However the mechanism of chronic LBP is still not fully understood.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of non-rigid stabilisation techniques for the treatment of low back pain Chronic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of non-rigid stabilisation techniques for the treatment of low back pain Chronic
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Medical Policy Manual. Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Date of Origin: October 2006.
 Medical Policy Manual Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Section: Surgery Date of Origin: October 2006 Last Reviewed Date: December 2015 Policy No: 155 Effective
Medical Policy Manual Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Section: Surgery Date of Origin: October 2006 Last Reviewed Date: December 2015 Policy No: 155 Effective
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Low Back Pain (LBP) Prevalence. Low Back Pain (LBP) Prevalence. Lumbar Fusion: Where is the Evidence?
 15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
Introduction to Non-fusion Technologies in the Lumbar and Cervical Spine
 Introduction to Non-fusion Technologies in the Lumbar and Cervical Spine Introduction The term motion-sparing technology has been used to describe newer surgical techniques designed to preserve spinal
Introduction to Non-fusion Technologies in the Lumbar and Cervical Spine Introduction The term motion-sparing technology has been used to describe newer surgical techniques designed to preserve spinal
Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures
 Interlaminar Technology Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures Coding Recommendations Overview Implant Description & Device Type Differentiation
Interlaminar Technology Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures Coding Recommendations Overview Implant Description & Device Type Differentiation
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
PARADIGM SPINE. Brochure. coflex Interlaminar Stabilization
 PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
Treatment pathways in lumbar spinal stenosis. By Prof. Dr. H. Michael Mayer
 Treatment pathways in lumbar spinal stenosis By Prof. Dr. H. Michael Mayer Content The pathology of spinal stenosis 4 The treatment of spinal stenosis 6 Spinal stenosis treatment options and outcomes 8
Treatment pathways in lumbar spinal stenosis By Prof. Dr. H. Michael Mayer Content The pathology of spinal stenosis 4 The treatment of spinal stenosis 6 Spinal stenosis treatment options and outcomes 8
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults
 Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Surgical Treatment for Lumbar Spinal Stenosis Dynamic Interspinous Distraction Interlaminar Stabilization Implant - Coflex
 International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis
 Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
The recent Spine Patient Outcomes Research Trial
 SPINE Volume 38, Number 18, pp 1529-1539 2013, Lippincott Williams & Wilkins RANDOMIZED TRIAL Decompression and Coflex Interlaminar Stabilization Compared With Decompression and Instrumented Spinal Fusion
SPINE Volume 38, Number 18, pp 1529-1539 2013, Lippincott Williams & Wilkins RANDOMIZED TRIAL Decompression and Coflex Interlaminar Stabilization Compared With Decompression and Instrumented Spinal Fusion
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Cervical Dynamic Stabilization
 PARADIGM SPINE Dynamic Cervical Implant Cervical Dynamic Stabilization 2 DCI Recurrent Neck Pain due to Adjacent Segment Disease: the Rationale for Motion Preservation The gold standard in stabilizing
PARADIGM SPINE Dynamic Cervical Implant Cervical Dynamic Stabilization 2 DCI Recurrent Neck Pain due to Adjacent Segment Disease: the Rationale for Motion Preservation The gold standard in stabilizing
SURGICAL TREATMENT FOR SPINE PAIN
 MEDICAL POLICY SURGICAL TREATMENT FOR SPINE PAIN Policy Number: 2012T0547C Effective Date: April 1, 2012 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG ADMINISTRATION...
MEDICAL POLICY SURGICAL TREATMENT FOR SPINE PAIN Policy Number: 2012T0547C Effective Date: April 1, 2012 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG ADMINISTRATION...
Moderator and Panelists
 Panelists Moderator and Panelists Moderator Dr. Hallett Mathews Executive Vice President Chief Medical Officer Paradigm Spine, LLC Panelist Dr. John Peloza Orthopedic Surgeon The Center for Spine Care
Panelists Moderator and Panelists Moderator Dr. Hallett Mathews Executive Vice President Chief Medical Officer Paradigm Spine, LLC Panelist Dr. John Peloza Orthopedic Surgeon The Center for Spine Care
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com
 Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010
 Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
SURGICAL TREATMENT FOR SPINE PAIN
 CLINICAL POLICY SURGICAL TREATMENT FOR SPINE PAIN Policy Number: SURGERY 075.11 T2 Effective Date: April 1, 2015 Table of Contents CONDITIONS OF COVERAGE... COVERAGE RATIONALE... BACKGROUND... CLINICAL
CLINICAL POLICY SURGICAL TREATMENT FOR SPINE PAIN Policy Number: SURGERY 075.11 T2 Effective Date: April 1, 2015 Table of Contents CONDITIONS OF COVERAGE... COVERAGE RATIONALE... BACKGROUND... CLINICAL
Surgical treatment of lumbar spinal stenosis with microdecompression and interspinous distraction device insertion. A case series
 Ploumis et al. Journal of Orthopaedic Surgery and Research 2012, 7:35 RESEARCH ARTICLE Open Access Surgical treatment of lumbar spinal stenosis with microdecompression and interspinous distraction device
Ploumis et al. Journal of Orthopaedic Surgery and Research 2012, 7:35 RESEARCH ARTICLE Open Access Surgical treatment of lumbar spinal stenosis with microdecompression and interspinous distraction device
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated And Fenestrated Pedicle
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
 Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach
 Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Instability concept. Symposium- Cervical Spine. Barcelona, February 2014
 Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Evidence-based lumbar spine surgery
 34 Acta Orthop Scand (Suppl 5) 02; 73 Evidence-based lumbar spine surgery The role of national registration Björn Strömqvist Department of Orthopedics, Lund University Hospital, SE-221 85 Lund, Sweden,
34 Acta Orthop Scand (Suppl 5) 02; 73 Evidence-based lumbar spine surgery The role of national registration Björn Strömqvist Department of Orthopedics, Lund University Hospital, SE-221 85 Lund, Sweden,
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Minimally Invasive Spine Surgery. David H Strothman, M.D.
 Minimally Invasive Spine Surgery David H Strothman, M.D. The Lumbar Spine Lumbar Disc Annulus Fibrosus High collagen content Concentric layers of intertwined annular bands Nucleus Pulposus Hydrated Proteoglycans
Minimally Invasive Spine Surgery David H Strothman, M.D. The Lumbar Spine Lumbar Disc Annulus Fibrosus High collagen content Concentric layers of intertwined annular bands Nucleus Pulposus Hydrated Proteoglycans
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Surgical Guideline for Lumbar Fusion (Arthrodesis)
 I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
Outcome of the L5-S1 Segment after Posterior Instrumented Spinal Surgery in Degenerative Lumbar Diseases
 Original Article 81 Outcome of the L5-S1 Segment after Posterior Instrumented Spinal Surgery in Degenerative Lumbar Diseases Jen-Chung Liao, MD; Wen-Jer Chen, MD; Lih-Huei Chen, MD; Chi-Chien Niu, MD Results:
Original Article 81 Outcome of the L5-S1 Segment after Posterior Instrumented Spinal Surgery in Degenerative Lumbar Diseases Jen-Chung Liao, MD; Wen-Jer Chen, MD; Lih-Huei Chen, MD; Chi-Chien Niu, MD Results:
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary?
 White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Subject: BlueCross BlueShield of North Carolina Lumbar Spine Fusion Surgery Notification
 , 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
, 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Our mission is to help you experience the greatest benefits possible. Our physicians and care staff are dedicated to your needs.
 What to Expect Our mission is to help you experience the greatest benefits possible. Our physicians and care staff are dedicated to your needs. You will most likely require 20-30 procedure sessions to
What to Expect Our mission is to help you experience the greatest benefits possible. Our physicians and care staff are dedicated to your needs. You will most likely require 20-30 procedure sessions to
Disc Replacement or Fusion: which is best for me?
 Disc Replacement or Fusion: which is best for me? After anterior discectomy in either the cervical or lumbar region there is a need to replace the removed disc with something and the choice lies between
Disc Replacement or Fusion: which is best for me? After anterior discectomy in either the cervical or lumbar region there is a need to replace the removed disc with something and the choice lies between
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Thoracolumbar Spine Fractures. Outline. Outline. Holmes Criteria. Disclosure:
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
The conservative surgical treatment of lumbar spinal stenosis in the elderly
 REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
Technology Breakthrough in Spinal Implants (Technical Insights)
 Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
MATERIALS AND METHODS
 REDISTRIBUTION OF LOAD OF INJURED LOWER CERVICAL SPINE UNDER AXIAL COMPRESSION USING FEM E. C. Teo 1 and H. W. Ng 1 1 School of Mechanical and Production Engineering, Nanyang Technological University,
REDISTRIBUTION OF LOAD OF INJURED LOWER CERVICAL SPINE UNDER AXIAL COMPRESSION USING FEM E. C. Teo 1 and H. W. Ng 1 1 School of Mechanical and Production Engineering, Nanyang Technological University,
The Surgical Spine. Sergio Rivero M.D.
 The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
 Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients
 CLINICAL ARTICLE Kor J Spine 5(2):83-88, 2008 Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients Il-Tae Jang, M.D., Sang-Won Lee, M.D., Paul M. Atienza, M.D., Jang-Seon You, M.D.
CLINICAL ARTICLE Kor J Spine 5(2):83-88, 2008 Decompressive Surgery Alone for Lumbar Spinal Stenosis in Elderly Patients Il-Tae Jang, M.D., Sang-Won Lee, M.D., Paul M. Atienza, M.D., Jang-Seon You, M.D.
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Effects of vertebral axial decompression on intradiscal pressure
 This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
Lumbar Stenosis Without Spondylolift - A Review
 J Neurosurg: Spine 2:686 691, 2005 Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 10: fusion following decompression in patients with stenosis without
J Neurosurg: Spine 2:686 691, 2005 Guidelines for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 10: fusion following decompression in patients with stenosis without
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
NEW HORIZONS IN SPINAL SURGERY: SPINE ARTHROPLASTY
 NEW HORIZONS IN SPINAL SURGERY: SPINE ARTHROPLASTY Viral B. Shah*, Appaji Krishnan* and Sajan K. Hegde** From the: Spine Fellows*, Consultant Spinal Surgeon**, Department of Spinal Surgery, Apollo Hospitals,
NEW HORIZONS IN SPINAL SURGERY: SPINE ARTHROPLASTY Viral B. Shah*, Appaji Krishnan* and Sajan K. Hegde** From the: Spine Fellows*, Consultant Spinal Surgeon**, Department of Spinal Surgery, Apollo Hospitals,
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
A Radiographic Assessment of the Ability of the Extreme Lateral Interbody Fusion Procedure to Indirectly Decompress the Neural Elements
 A Radiographic Assessment of the Ability of the Extreme Lateral Interbody Fusion Procedure to Indirectly Decompress the Neural Elements SPINE Volume 35, Number 26S, pp S331 S337 2010, Lippincott Williams
A Radiographic Assessment of the Ability of the Extreme Lateral Interbody Fusion Procedure to Indirectly Decompress the Neural Elements SPINE Volume 35, Number 26S, pp S331 S337 2010, Lippincott Williams
