Severe asthma: Advances in current management and future therapy
|
|
|
- Jasper Shaw
- 8 years ago
- Views:
Transcription
1 Asthma: Current status and future directions Severe asthma: Advances in current management and future therapy Peter J. Barnes, FMedSci, FRS London, United Kingdom Effective treatment of severe asthma is a major unmet need because patients symptoms are not controlled on maximum treatment with inhaled therapy. Asthma symptoms can be poorly controlled because of poor adherence to controller therapy, and this might be addressed by using combination inhalers that contain a corticosteroid and long-acting b 2 -agonist as reliever therapy in addition to maintenance treatment. New bronchodilators with a longer duration of action are in development, and recent studies have demonstrated the benefit of a long-acting anticholinergic bronchodilator in addition to b 2 -agonists in patients with severe asthma. Anti-IgE therapy is beneficial in selected patients with severe asthma. Several new blockers of specific mediators, including prostaglandin D 2, IL-5, IL-9, and IL-13, are also in clinical trials and might benefit patients with subtypes of severe asthma. Several broadspectrum anti-inflammatory therapies that target neutrophilic inflammation are in clinical development for the treatment of severe asthma, but adverse effects after oral administration might necessitate inhaled delivery. Macrolides might benefit some patients with infection by atypical bacteria, but recent results are not encouraging, although there could be an effect in patients with predominant neutrophilic asthma. Corticosteroid resistance is a major problem in patients with severe asthma, and several molecular mechanisms have been described that might lead to novel therapeutic approaches, including drugs that could reverse this resistance, such as theophylline and nortriptyline. In selected patients with severe asthma, bronchial thermoplasty might be beneficial, but thus far, clinical studies have not been encouraging. Finally, several subtypes of severe asthma are now recognized, and in the future, it will be necessary to find biomarkers that predict responses to specific forms of therapy. (J Allergy Clin Immunol 2012;129:48-59.) Key words: Corticosteroids, bronchodilator, cytokine, chemokine, IgE, kinase, p38 mitogen-activated protein kinase, bronchial thermoplasty, corticosteroid resistance, macrolide Severe asthma is defined by a failure to achieve control with maximum doses of inhaled therapies and represents one of the major unmet therapeutic needs in asthma. Although current From the National Heart and Lung Institute, Imperial College. Disclosure of potential conflict of interest: P. J. Barnes receives research support from GlaxoSmithKline, AstraZeneca, Novartis, Boehringer Ingelheim, and Pfizer. Received for publication October 18, 2011; revised November 8, 2011; accepted for publication November 10, Corresponding author: Peter J. Barnes, FMedSci, FRS, National Heart and Lung Institute, Imperial College School of Medicine, Dovehouse St, London SW3 6LY, United Kingdom. p.j.barnes@imperial.ac.uk /$36.00 Ó 2012 American Academy of Allergy, Asthma & Immunology doi: /j.jaci Abbreviations used COPD: Chronic obstructive pulmonary disease CRTH2: Chemoattractant homologous receptor expressed on T H 2 cells 59-LO: 59-Lipoxygenase HDAC2: Histone deacetylase-2 ICS: Inhaled corticosteroid LABA: Long-acting b 2 -agonist LAMA: Long-acting muscarinic antagonist LT: Leukotriene MAPK: Mitogen-activated protein kinase MIF: Migratory inhibitory factor NF-kB: Nuclear factor kb Nrf2: Nuclear factor erythroid 2 related factor 2 PDE: Phosphodiesterase PG: Prostaglandin PI3K: Phosphoinositide 3-kinase PPAR: Peroxisome proliferator activated receptor Syk: Spleen tyrosine kinase TSLP: Thymic stromal lymphopoietin management of asthma is highly effective, most patients symptoms are well controlled if they take regular inhaled corticosteroids (ICSs) with or without long-acting b 2 -agonists (LABAs) in combination inhalers. Yet despite the availability of highly effective therapies, more than half of the patients with asthma in the real world have disease that is apparently poorly controlled, largely because of poor adherence to controller therapy. 1,2 In patients with difficult-to-treat asthma, more than 80% show poor adherence with regular inhaled therapy. 3 Even in the patients with the most severe asthma treated with maintenance oral prednisolone (steroid-dependent asthma), only about half of the patients take the oral steroid based on plasma prednisolone assays. This suggests that poor adherence is a major factor contributing to poor control of asthma. In patients with refractory asthma with persistent sputum eosinophilia despite prescription of high doses of ICSs or maintenance oral steroids, treatment with high-dose intramuscular injection of triamcinolone results in disappearance of sputum eosinophilia in the majority of patients. 4 This suggests that poor compliance with inhaled and even oral corticosteroids might be a major factor contributing to difficult-to-treat asthma and that poor compliance with controller therapy is an important determinant of asthma severity. The reasons for poor compliance with regular therapy, especially in patients with severe asthma, are not well understood, but the lack of immediate symptom relief, as seen with antiinflammatory treatments, such as corticosteroids, is probably important. Steps need to be taken to more accurately determine adherence to therapy, and strategies to overcome this problem 48
2 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES 49 need to be devised. These findings also indicate that patients with poorly controlled asthma might need additional antiinflammatory therapy. This review discusses some of the currently available and developing approaches to the management of severe or refractory asthma. Several new classes of drugs are currently in development for the treatment of severe asthma, but it has proved challenging to find effective and safe therapies. 5 Although severe asthma comprises only approximately 5% to 10% of all asthmatic patients, it accounts for more than half of the health care spending on asthma because patients with severe asthma consume more expensive drugs and are more likely to be hospitalized or require additional medical attention. SMART STRATEGIES Several studies have shown that in patients with moderate-tosevere asthma, there is an improvement in asthma control and significant reduction in severe exacerbations if a budesonide/ formoterol combination inhaler is used as a reliever instead of a short-acting b 2 -agonist, whereas maintenance therapy with budesonide/formoterol is administered twice daily as usual. 6 This strategy is now known as single inhaler maintenance and reliever therapy (SMART) and could presumably be used with any combination inhaler containing formoterol, irrespective of the corticosteroid used. However, this strategy is not possible with salmeterol or the once-daily b 2 -agonists, such as indacaterol and vilanterol, all of which have cumulative side effects. The scientific rationale for SMART is now well understood because the ICS used as rescue therapy has a rapid onset of its antiinflammatory effect and prevents the build-up of inflammation that precedes an acute exacerbation. 7,8 The SMART strategy is effective in patients with moderate and severe asthma, although studies confined to severe asthma have not yet been conducted. 6 This strategy might also be effective even when patients forget doses of their maintenance therapy and therefore addresses the key issue of poor adherence with controller therapy discussed above. Indeed, studies are now needed looking at inhaled formoterol/steroid combination inhalers as rescue therapy, even in the absence of the maintenance dose. 9 NEW CORTICOSTEROIDS Several ICSs are currently available for clinical use, and all have similar clinical efficacy, but there are differences in pharmacodynamic properties so that systemic exposure might differ. Because patients with severe asthma might require higher doses of ICSs, there is an advantage in developing systemic corticosteroids with fewer systemic side effects. Ciclesonide is a recently developed ICS and appears to have the least systemic effects and local side effects because the prodrug is activated in the lungs to the active principle des-ciclesonide by esterases, whereas there is little activation in the oropharynx. 10 This suggests that high doses of ciclesonide might be useful in the treatment of severe asthma. ICSs in pressurized metered-dose inhalers are now administered with hydrofluoroalkane 134a rather than chlorofluorocarbon as a propellant, and this results in smaller particle sizes, so that the drugs are more likely to be deposited in the small airways. 11 Theoretically, this should more effectively treat patients with severe asthma in whom there is inflammation of peripheral airways with evidence of small-airway inflammation. 12 More studies are needed on ICSs with hydrofluoroalkane 134a propellants in patients with severe asthma. All currently available ICSs are absorbed from the lungs and thus have the potential for systemic side effects. This has led to a search for safer ICSs with reduced oral bioavailability, reduced absorption from the lungs, or inactivation in the circulation because this would allow higher doses to be administered safely in patients with severe asthma. Dissociated steroids attempt to separate the side-effect mechanisms from the anti-inflammatory mechanisms. This is theoretically possible because side effects are largely mediated through transactivation and the binding of glucocorticoid receptors to DNA, whereas anti-inflammatory effects are largely mediated through transrepression of transcription factors through a nongenomic effect. 13 Dissociated steroids are designed to have a greater effect on transactivation than on transrepression and thus might have a better therapeutic ratio and might even be suitable for oral administration. 14 Nonsteroidal selective glucocorticoid receptor activators, such as AL-438 and mapracorat, are in clinical development. However, some of the anti-inflammatory effects of corticosteroids might be due to transactivation of anti-inflammatory genes, and therefore selective glucocorticoid receptor activators might not be as efficacious as existing ICSs. 15 Corticosteroids switch off inflammatory genes by recruiting the nuclear enzyme histone deacetylase-2 (HDAC2) to the activated inflammatory gene initiation site so that activators of this enzyme might also have antiinflammatory effects or might enhance the anti-inflammatory effects of corticosteroids. 13 NEW BRONCHODILATORS Bronchodilators play an important role in reducing symptoms in patients with severe asthma, and currently, LABAs are the bronchodilators of choice, usually given in combination with ICSs in a fixed-dose inhaler. Bronchodilators are essential in the management of asthma because they relieve and prevent bronchoconstriction. There have been several advances in the development of bronchodilators for the treatment of severe asthma. Once-daily b 2 -agonists b 2 -Agonists are the most effective bronchodilators because they act as functional antagonists of airway smooth muscle contraction, irrespective of the constricting stimulus. The LABAs salmeterol and formoterol have been a major advance in the management of severe asthma and are usually administered through combination inhalers with corticosteroids. There have been concerns about the safety of LABAs, and there is convincing evidence that LABAs used without a corticosteroid cover increase severe exacerbations and mortality. However, there is no clear evidence that LABAs pose any risk if combined with corticosteroids and therefore should only be used in the form of combination inhalers. 16,17 Several once-daily b 2 -agonists ( ultra-labas ) are in clinical studies, including indacaterol (already available for chronic obstructive pulmonary disease [COPD] in several countries), carmoterol, vilanterol, and olodaterol. 18 For asthmatic patients, these ultra-labas should only be available with a corticosteroid in a fixed combination. Currently, fluticasone furoate/vilanterol and mometasone/indacaterol are in clinical development for asthma as once-daily combination inhalers. 18
3 50 BARNES J ALLERGY CLIN IMMUNOL JANUARY 2012 Long-acting muscarinic antagonists Antimuscarinic (anticholinergic) bronchodilators are the preferred first-line therapy in patients with COPD, but in patients with asthma, they are less effective than b 2 -agonists because they block only the cholinergic component of bronchoconstriction, whereas b 2 -agonists reverse all bronchoconstrictors, including the direct effects of inflammatory mediators, such as histamine, leukotriene (LT) D 4, and prostaglandin (PG) D 2. Animal studies have recently demonstrated an important role for cholinergic mechanisms in the late response to inhaled allergen in sensitized guinea pigs because the long-acting muscarinic antagonist (LAMA) tiotropium bromide completely blocks the late response in nonanesthetized animals. 19 This response is also blocked by drugs that block TRPA1, an activating ion channel on airway sensory nerves, suggesting that allergens release a mediator (thus far unidentified) that activates TRPA1, leading to cholinergic reflex bronchoconstriction. There is also increasing evidence that muscarinic receptors can be activated by acetylcholine released from nonneuronal cells, such as epithelial and inflammatory cells. 20,21 Choline acetyltransferase can be induced in epithelial cells by inflammatory mediators, such as TNF-a, suggesting that acetylcholine synthesis might be increased in the airways of asthmatic patients. In sensitized guinea pigs tiotropium inhibits eosinophilic inflammation in the airways and airway hyperresponsiveness, even in vagotomized animals, suggesting that tiotropium is blocking the effects of nonneuronally released acetylcholine on muscarinic M 3 receptors and that tiotropium also blocks eosinophilic inflammatory mechanisms. 22 Tiotropium also inhibits T H 2 cytokine release in allergen-exposed sensitized mice and that from human PBMCs. 23 It also reduces eosinophilic inflammation, mucin gene expression, and airway remodeling in a murine model of asthma, possibly through a direct effect on fibroblasts. 24 Tiotropium also inhibits neutrophilic inflammation and airway fibrosis after repeated LPS challenge in guinea pigs. 25 These experimental studies suggest that tiotropium might have antiinflammatory effects through antagonism of neuronally and extraneuronally released acetylcholine on M 3 receptors on inflammatory cells. There is also evidence that blocking M 3 receptors with tiotropium inhibits acetylcholine-induced release of neutrophil chemotactic factors (mainly LTB 4 ) from human macrophages. 26 These in vitro and experimental studies have paved the way to recent clinical studies of tiotropium in patients with asthma, particularly in those with severe disease. Recent studies have shown that once-daily tiotropium provides useful additional bronchodilatation when added to a LABA in some patients with severe asthma. In one study approximately 30% of patients with severe asthma showed a good additional response when tiotropium was added. 27 Addition of tiotropium significantly improves lung function in patients whose symptoms are not controlled by high doses of ICSs and LABAs, although there is no improvement in symptoms or health status. 28 Another study showed that tiotropium was comparable with salmeterol in terms of bronchodilator response when added to an ICS in patients who show a good response to a short-acting anticholinergic. 29 In asthmatic patients with the Arg16/Arg16 genotype of the b 2 -receptor, who have previously been reported to be less responsive to b 2 -agonists, once-daily tiotropium was no less effective than twicedaily salmeterol in patients whose symptoms are not controlled with ICSs alone. 30 These studies suggest that addition of a LAMA to existing therapy in patients with severe asthma not controlled with ICSs and LABAs is beneficial and might be indicated, particularly in elderly patients with an element of fixed airway obstruction, who have similarities to patients with COPD. There are several other LAMAs in clinical development for COPD, including once-daily glycopyrrolate and GSK and twice-daily aclidinium bromide. 31 There appears to be additivity between LABAs and LAMAs, suggesting that a triple combination of a LABA plus a LAMA plus an ICS might be useful in some patients with severe asthma, although the development of such inhalers might prove difficult technically and for regulatory reasons. 32 Several bifunctional molecules that have LABA and LAMA activity are also in development, but it might prove difficult to balance the b-agonist and anticholinergic activities. 33 It would be logistically easier to combine a bifunctional molecule that has LABA and LAMA activity and an ICS in a combination inhaler to provide triple activity. Novel classes of bronchodilator In view of the recent concerns about the long-term safety of LABAs in asthmatic patients, there has been a search for alternative classes of bronchodilator. Novel bronchodilators have proved difficult to develop, and new drugs, such as vasoactive intestinal peptide analogs and potassium-channel openers, have had side effects due to more potent vasodilator than bronchodilator effects. A stable vasoactive intestinal peptide analog, Ro , has bronchodilator activity in asthmatic patients but is less effective than inhaled formoterol. 34 b 2 -Agonists and theophylline relax human airway smooth muscle by activating large-conductance Ca 21 -activated potassium channels, leading to a search for direct large-conductance Ca 21 -activated potassium channel activators, but although activating drugs were discovered, they have not been tested in clinical studies in asthma. Rho kinase inhibitors also have potential as bronchodilators but are likely to have significant toxicity. Recently, it has been found that agonists of bitter taste receptors (TAS2Rs), such as quinine, chloroquine, and saccharine, relax human airways in vitro by increasing local Ca 21 release, resulting in the opening and hyperpolarization of airway smooth muscle cells. 35 In murine models inhaled bitter tastants appear to be more effective than a b-agonist, although this species is not very responsive to b 2 -agonists. Theophylline relaxes human airway smooth muscle by inhibiting phosphodiesterase (PDE) 3 in airway smooth muscle cells, so that selective PDE3 inhibitors, such as cilostazol and milrinone, are potential bronchodilators. However, there has been concern that PDE3 inhibitors were associated with increased cardiovascular mortality in previous clinical trials. Combined PDE3/ 4 inhibitors are currently in development as inhaled therapy for asthma and COPD. 36 PGE 2 relaxes human airway smooth muscle through EP 4 receptors, 37 suggesting that EP 4 -selective agonists might be useful bronchodilators and might avoid the coughing induced by PGE 2 through EP 3 receptors on sensory nerve endings. ANTI-IgE Omalizumab is the only novel therapy that has specifically been approved for the treatment of severe asthma. Omalizumab is an mab that binds the Fc portion of IgE and thus prevents activating its high-affinity IgE receptor (FcεRI) on mast cells, basophils, and dendritic cells, as well as a low-affinity receptor
4 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES 51 (FcεRII) expressed on several immune and inflammatory cells, including macrophages, eosinophils, and T and B lymphocytes. Numerous clinical trials have demonstrated the clinical efficacy of omalizumab in reducing maintenance doses of oral corticosteroids and ICSs and in reducing exacerbations in patients (including children) with severe asthma In a large study of patients with severe asthma whose symptoms are not controlled with high doses of ICSs and LABAs, omalizumab significantly reduced exacerbations (by 25%) and improved symptoms and asthma-related quality-of-life scores. 39 Only a proportion of allergic asthmatic patients with the target total serum IgE concentration of 70 to 300 IU/mL show a good response, and because of the high cost, a trial of therapy over 3 to 4 months is often recommended to identify good responders. Unfortunately, despite extensive analyses, no clinically measurable biomarkers have been found to predict a good response. Patients with nonatopic (intrinsic) asthma are currently excluded, but there is evidence for local IgE production in the airways of at least some of these patients, 41 and therefore future studies should investigate this group of patients who often have difficult-to-control asthma. Similarly, there are patients with severe uncontrolled asthma with total IgE levels of greater than 300 IU/mL who are currently excluded because it is not feasible to give enough antibody to effectively block IgE. In the future, antibodies with a higher affinity for IgE might be developed so that it could be possible to treat patients with very high total IgE levels. An mab (lumiliximab) directed against FcεRII (CD23) reduces total IgE levels, probably by reducing synthesis by B lymphocytes, but has little clinical benefit, even in patients with mild asthma, and therefore is no longer in clinical development. 42 TARGETING INFLAMMATORY MEDIATORS More than 100 mediators are involved in the complex inflammation of asthma, making it unlikely that blocking the synthesis or receptor for a single mediator could be very effective. ICSs are highly effective in suppressing the synthesis of multiple inflammatory mediators, but in patients with severe asthma, they appear to be less effective, making it possible that adding a mediator antagonist to high doses of ICSs might be beneficial. In addition, the inflammation seen in some patients with severe asthma has a different pattern, with a predominance of neutrophils, suggesting that targeting mediators of neutrophilic inflammation might be effective in these patients. 43 Lipid mediator blockade The only mediator antagonists currently used in asthma therapy are antileukotrienes, which block cysteinyl leukotriene receptors, but these drugs are much less effective than ICSs and have little place as add-on therapy in patients with severe asthma. 44 LTB 4 is a chemoattractant of neutrophils, mast cells, and T cells, including effector CD8 1 memory T cells, and its levels are increased in patients with severe asthma. 45 An LTB 4 receptor (BLT 1 ) antagonist had no effect in patients with mild asthma 46 but has not been tested in patients with more severe disease, in whom it would be more likely to be effective. A low-affinity BLT 2 receptor is expressed on several cell types, including T cells and mast cells, and when inhibited by oligonucleotides, there is a reduction in allergic inflammation in a murine model. 47 BLT 2 receptors are upregulated on FIG 1. PGD 2 might play a role in severe asthma. It is synthesized mainly in mast cells by PDGD synthase (PGDS) and acts on DP 1 receptors on vessels to mediate vasodilatation and on dendritic cells to enhance their activation through DP 2 receptors (also known as CRTH2) to attract T H 2 lymphocytes and eosinophils and on thromboxane (TP) receptors to cause bronchoconstriction. DP 2 (CRTH2) antagonists are now in a clinical trial in patients with severe asthma. Antagonists of DP 1 and receptors and inhibitors of PGDS are now in clinical development for asthma therapy. Adapted from Barnes. 5 mast cells after allergen challenge and mediate the synthesis of T H 2 cytokines. 48 To target both BLT 1 and BLT 2,LTB 4 synthesis can be reduced by an inhibitor of LTA 4 hydrolase, and such an approach is effective in a murine model of asthma. 49 Phospholipase A 2 inhibits the generation of all lipid mediators (prostaglandins, leukotrienes, and platelet-activating factor) from membrane phospholipids and therefore theoretically should be effective in patients with severe asthma, although there is uncertainty about whether to block the secretory or cytosolic isoforms of phospholipase A 2, and it has been difficult to discover safe and selective inhibitors Lipoxygenase (59-LO) works through 59-LO activating protein, and several novel 59-LO and 59-LO activating protein inhibitors are currently in clinical development. These drugs could be more effective than BLT 1 antagonists because they block production of additional mediators, such as 5-HETE and 5-oxo- ETE, which acts through a specific OXE receptor Oxo-ETE is generated by oxidative stress and therefore is likely to be generated in patients with severe asthma. It is a potent attractant of eosinophils but also attracts neutrophils and T cells. PGD 2 is released from mast cells, T H 2 cells, and dendritic cells and activates DP 2 receptors, also known as chemoattractant homologous receptor expressed on T H 2 cells (CRTH2), which mediate chemotaxis of T H 2 cells and eosinophils (Fig 1). 5,52 There is increased expression of PGD 2 in patients with severe asthma. 53 Several CRTH2 antagonists are now in clinical development for asthma, including AMG-853, OC000459, and MK-7246, which have shown early clinical efficacy as oral treatments for asthma and rhinitis. A study of OC00049 in steroidnaive asthmatic patients showed no improvement in lung function but a small reduction in symptoms and no significant reduction in sputum eosinophil numbers compared with those values after placebo. 54 PGD 2 also activates DP 1 receptors, which mediate vasodilatation and enhance T H 2 cell polarization by dendritic cells, so that a dual DP 1 /DP 2 antagonist might be more effective, whereas an inhibitor of PGD synthase would block PGD 2 synthesis and also prevent the bronchoconstrictor effects of PGD 2 that are mediated through thromboxane receptors on airway smooth muscle.
5 52 BARNES J ALLERGY CLIN IMMUNOL JANUARY 2012 Cytokine blockade Cytokines play a key role in orchestrating chronic inflammation and remodeling airway structure and therefore have become important targets for blockade in asthmatic patients, particularly patients with severe disease whose symptoms are not controlled with high doses of ICSs. 55 More than 50 cytokines have been implicated in asthma, and several have already been targeted in clinical studies, often with disappointing results. 56 There is a great redundancy of cytokines, and therefore it might be difficult to inhibit an inflammatory process effectively with a selective blocker. Another problem is the high cost of blocking mabs, and therefore these drugs are likely to be cost-effective only in patients with severe disease. It is possible that production costs might be reduced by the development of higher-affinity antibodies or the use of fragments, such as domain antibodies, that are cheaper to produce. Another problem is that there has been a major focus on T H 2 cytokines in the belief that T H 2 cells drive allergic inflammation. 57 Corticosteroids are very effective in suppressing T H 2 cell driven inflammation, at least in part because they are very potent inhibitors of the T H 2 regulating transcription factor GATA3. 58 Animal models of asthma have also been developed that highlight T H 2 cell driven inflammation, and these models might be inappropriate for the development of treatments for severe asthma. Because different immune mechanisms are likely operate in many patients with severe asthma, it might be necessary to target different sets of cytokines, such as those involving T H 1 and T H 17 cells. T H 17 cells have been implicated in patients with severe asthma, particularly those patients with a predominantly neutrophilic pattern of inflammation. 59 Interestingly, T H 17 cells appear to be corticosteroid resistant and might therefore contribute to the corticosteroid resistance seen in patients with severe asthma. 60 Inhibiting T H 2 cytokines Inhibition of IL-4 by using inhaled soluble receptors proved to be disappointing, but there is continued interest in blocking IL- 13, a related cytokine that regulates IgE formation, particularly in patients with severe asthma. IL-13 can also induce corticosteroid resistance and therefore appears to be an appropriate target for patients with severe asthma. 61,62 Pitrakinra is a mutated form of IL-4 that blocks IL-4 receptor a, the common receptor for IL-4 and IL-13, and significantly reduces the late response to inhaled allergen in patients with mild asthma when administered subcutaneously or by means of nebulization, 63 and larger clinical trials are currently in progress with this protein. Several IL-13 and IL-4 receptor a blocking antibodies are also in clinical development, but thus far, clinical studies in patients with severe asthma have been disappointing. A blocking mab to IL-13, lebrikizumab, has been studied in asthmatic patients whose symptoms are not controlled with high doses of ICSs and showed a small increase in FEV 1 (approximately 5%) compared with placebo after 12 weeks but no significant effect at 24 weeks. 64 There are no significant improvements in symptoms or asthma-related health status and no reduction in exacerbations. Interestingly, increased concentrations of the plasma biomarker periostin, which was discovered by means of proteomic analysis of IL-13 stimulated epithelial cells, showed a slightly better response (approximately 8%) than low concentrations, suggesting that it can be used as a biomarker to predict greater responses. An mab targeting IL-4 receptor a (AMG317), which therefore blocks the effects of IL-4 and IL-13, has been ineffective in controlling asthma symptoms or lung function in 3 different doses over a 12-week period in patients with mild asthma. 65 One question about the poor efficacy of anti IL-13 strategies might be whether the dose is sufficient to block endogenous IL-13 in the airways. In a recent study a blocking anti IL-13 mab profoundly suppressed IL-13 in nasal secretions after local allergen challenge, yet there was no significant reduction in eosinophil numbers or nasal symptoms. 66 IL-4 and IL-13 signal through the transcription factor signal transducer and activator of transcription 6, and small-molecule inhibitors, such as AS , have now been developed that are active in a murine model of asthma but have yet to be developed clinically. 67 IL-5 is of critical importance for eosinophilic inflammation, and a blocking antibody to IL-5 (mepolizumab) depletes eosinophils from the circulation and sputum of asthmatic patients but disappointingly has no effect on the response to inhaled allergen, airway hyperresponsiveness, symptoms, lung function, or exacerbation frequency in asthmatic patients. 68,69 However, more recent studies show that mepolizumab reduces exacerbations in highly selected patients who have persistent sputum eosinophilia despite high doses of ICSs, although there is no improvement in symptoms, lung function, or airway hyperresponsiveness. 70,71 Another IL-5 blocking antibody, reslizumab, failed to improve asthma control over 12 weeks in patients with sputum eosinophilia despite high doses of ICSs, but there was some reduction in symptoms and sputum eosinophils. 72 An antibody against the IL-5 receptor a (benralizumab, MEDI-563) might more effectively deplete airway eosinophils than blocking IL-5 itself through antibody-dependent cytotoxicity of eosinophils and is currently being studied in clinical trials. 73 Inhaled antisense oligonucleotides that block the common b chain of IL-5 and GM-CSF receptors together with the chemokine receptor CCR3 (TPI ASM8) have a small effect in reducing allergen responses and airway inflammation. 74 Overall, blocking IL-5, although effective in reducing eosinophilic inflammation, has been disappointing, although it might be effective in highly selected patients, as well as in patients with other hypereosinophilic diseases, such as Churg-Strauss syndrome and eosinophilic esophagitis. 75,76 Another T H 2 cytokine that is currently being targeted is IL-9, which plays a role in mast cell proliferation, although there is recent evidence that it is produced particularly by a subset of CD4 1 T cells designated T H 9 cells. 77 Clinical studies have been encouraged by animal studies showing that inhibition of IL-9 leads to reduced allergic inflammation and mucus hypersecretion, and a blocking IL-9 antibody (MEDI-528) has been shown to be safe after weekly subcutaneous injections, with a trend toward reduction in exercise-induced asthma, which is mediated through mast cell activation. 78 Larger clinical trials are now in progress. There has been considerable interest in thymic stromal lymphopoietin (TSLP), an IL-7 related cytokine that is secreted by airway epithelial cells, because it instructs dendritic cells to secrete chemokines that attract T H 2 cells into the airways and potentiates the activation of these cells. 79 TSLP expression by airway epithelial cells is increased in a subset of patients with severe asthma treated with high doses of ICSs, suggesting that
6 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES 53 this might be a good target, especially because it acts as an upstream cytokine. 80 Several pharmaceutical companies are developing antibodies to TSLP and its receptor, as well as to OX40 and OX40 ligand, which act as costimulatory molecules to TSLP, although bronchial OX40/OX40 ligand expression is not increased in patients with severe asthma compared with that seen in patients with mild asthma. 81 Other cytokines Another cytokine targeted in asthmatic patients is TNF-a, which might play a significant role in those with severe asthma. Several uncontrolled or small studies suggested that anti-tnf therapies (TNF blocking antibodies infliximab or soluble receptor etanercept) might be useful in reducing symptoms, exacerbations, and airway hyperresponsiveness in patients with severe asthma, 82,83 but a recent large multicenter trial with the humanized antibody golimumab showed no beneficial effect on lung function, symptoms, or exacerbations, and there were increased reports of pneumonia and cancer. 84 A study of etanercept over 4 weeks in patients with moderate-to-severe asthma showed no clinical efficacy, but there were no safety problems. 85 Several other cytokine blockers are currently being targeted in asthmatic patients, including IL-17, IL-25, IL-33, GM-CSF, and stem cell factor, but thus far, no clinical studies in patients with severe asthma have been reported. 56 Chemokine receptor antagonists Chemokines are small cytokines that attract inflammatory cells, including mast cells, eosinophils, and T H 2 cells, into the airways and are therefore appropriate targets for therapy, particularly because they signal through G protein coupled receptors for which small-molecule antagonists can be developed. 86 The major focus of interest in asthmatic patients has been the chemokine receptor CCR3, which is predominantly expressed on eosinophils and mediates the chemotactic response to CXCL11 (eotaxin), which is secreted in asthma. CCR3 is also expressed on mast cells and some T H 2 cells. Several small-molecule inhibitors of CCR3 have been in clinical development, but their effects in asthmatic patients have not yet been reported because they have usually been discontinued because of toxicology problems. An inhaled antisense oligonucleotide that targets CCR3 has some effect in reducing sputum eosinophils, but results are difficult to interpret because IL-5 and GM-CSF b chain antisense were coadministered. 87 Other chemokine receptors that are targeted for asthma therapy are CCR2 on monocytes and T cells and CCR4, CCR8, and CXCR4 on T H 2 cells. A defucosylated antibody to CCR4 (mogamulizumab, also known as KW-0761 and AMG- 761) results in prolonged cytotoxic effects on T H 2 cells, marked and prolonged depletion of T H 2 cells, and reduced lung inflammation in animal models. This antibody is now in early clinical trials for asthma and adult T-cell leukemia-lymphoma. 88 CXCR2 is expressed on neutrophils and monocytes and might be involved in the recruitment of neutrophils into the airways of patients with severe (neutrophilic) asthma. Several small-molecule inhibitors of CXCR2 are now in clinical development. 89 An oral CXCR1/ CXCR2 antagonist, navarixin (SCH ), is effective in blocking ozone-induced sputum neutrophilia in healthy subjects 90 and is currently in clinical trials in patients with severe asthma. BROAD-SPECTRUM ANTI-INFLAMMATORY TREATMENTS The fact that the symptoms of patients with severe asthma might not be controlled by high doses of ICSs plus LABAs and sometimes even oral corticosteroids has prompted a search for alternative anti-inflammatory therapies that can be added to existing therapies to provide additional control. In addition, inflammation in some patients with severe asthma is predominantly neutrophilic so that inhibitors of neutrophilic inflammation are needed, and corticosteroids are poorly effective against neutrophilic inflammation. Several approaches to treating neutrophilic inflammation might be applicable to the treatment of severe asthma. Although several classes of broad-spectrum noncorticosteroid anti-inflammatory treatments have been in development, there have usually been problems with side effects when the drugs are administered orally, and this has had limited clinical development. This suggests that it might be necessary to develop potent topically active anti-inflammatory treatments that avoid systemic exposure, but thus far, this has proved to be a major challenge. PDE4 inhibitors The most advanced of the anti-inflammatory therapies are PDE4 inhibitors, which have a wide spectrum of antiinflammatory effects that are relevant to severe asthma, inhibiting T cells, eosinophils, neutrophils, mast cells, airway smooth muscle, epithelial cells, and nerves and are highly effective in animal models of asthma. 91 PDE4 inhibitors are effective against neutrophilic inflammation, making them an attractive potential therapy for severe asthma when there is neutrophilic inflammation. An oral PDE4 inhibitor, roflumilast, has an inhibitory effect on allergen-induced responses in patients with mild asthma and also reduces symptoms and lung function similar to a low dose of ICS. 92 Roflumilast is currently licensed for use in patients with severe COPD, and therefore there has been increased interest in its potential for the treatment of severe asthma. However, a major limitation to this class of drug is the mechanism-based side-effect profile, including nausea, headaches, and diarrhea, which is dose limiting. On the basis of animal models, the antiinflammatory effects appear to be mediated by inhibition of PDE4B, whereas nausea and vomiting are mediated through PDE4D inhibition, suggesting that PDE4B-selective inhibitors might be better tolerated. 93 Another approach is to deliver PDE4 inhibitors by means of inhalation, but thus far, these drugs have had no efficacy. Inhaled PDE3/4 inhibitors are also in development and might have the advantage of bronchodilatation through PDE3 inhibition. 36 Kinase inhibitors Kinases play a key role in regulating the expression of inflammatory genes in asthmatic patients and might amplify inflammation in patients with severe asthma. 94 There are now several kinase inhibitors that might be useful in the treatment of severe asthma (Fig 2). The transcription factor nuclear factor kb (NF-kB) regulates many of the inflammatory genes that are abnormally expressed in asthmatic patients and is activated in asthmatic airways. Small-molecule inhibitors of the key enzyme IKK2/IKKb (inhibitor of kb kinase) block inflammation induced by NF-kB activation and are now in preclinical testing. 95
7 54 BARNES J ALLERGY CLIN IMMUNOL JANUARY 2012 FIG 2. Inhibition of proinflammatory kinase pathways for severe asthma. Several kinases activate the expression of multiple inflammatory genes and might therefore amplify the inflammation in asthmatic patients, leading to more severe disease. Selective inhibitors have been developed for several kinases, including spleen tyrosine kinase (SYK), which activates several signaling pathways, including phospholipase Cg (PLCg); inhibitor of NFkB kinase (IKK2), which activates NF-kB; p38 MAPK, which activates MAPK-activated protein kinase 2 (MAPKAPK2); Jun kinase (JNK), which activates activator protein 1 (AP-1); and PI3K, which activates Akt. Selective inhibitors have now been developed for all of these enzyme targets. p38 mitogen-activated protein kinase (MAPK) activates similar inflammatory genes to NF-kB, is activated in cells from patients with severe asthma, 96 and has been linked to corticosteroid resistance. 97 A p38 MAPK inhibitor appears to improve corticosteroid responsiveness in cells from patients with severe asthma. 98 p38 MAPK also plays a key role in activation of GATA3, a transcription factor that regulates T H 2 cell differentiation and expression of T H 2 cytokines. 99 Corticosteroids block GATA3 activation and are mimicked by p38 MAPK inhibitors. 58 An antisense that blocks p38 MAPK demonstrated efficacy in a murine asthma model. 100 Several small-molecule p38 inhibitors are now in clinical development for the treatment of inflammatory diseases, but side effects after systemic administration have proved to be a major problem. 101 Phosphoinositide 3-kinase (PI3K) also regulates inflammation and has several isoforms, but nonselective inhibitors are likely to be toxic. 102 The isoenzyme PI3Kg is important in chemotactic responses, and selective inhibitors are in development, whereas PI3Kd activation results in reduced corticosteroid responsiveness through reduced HDAC2 activity, so that PI3Kd inhibitors might potentially reverse corticosteroid resistance in patients with severe asthma. 103 Theophylline is a selective inhibitor of PI3Kd, and theophylline derivatives that lack PDE inhibition or selective PI3Kd inhibitors might therefore be of therapeutic value. A general concern about novel kinase inhibitors is that they might have side effects because they target mechanisms that are found in many cell types. Therefore it might be necessary to develop inhaled formulations for use in asthmatic patients in the future, as proved necessary for corticosteroids. Spleen tyrosine kinase (Syk) is involved in activation of mast cells and other immune cells, and several small-molecule Syk kinase inhibitors are in development, particularly for patients with severe asthma. 104 An antisense inhibitor of Syk kinase is effective in an animal model of asthma, 105 and the small-molecule inhibitor R112 administered nasally reduces nasal symptoms in patients with hay fever. 106 More potent inhibitors, such as R343 and Bay , are in development for inhalation in asthmatic FIG 3. Inhibition of mast cells in asthmatic patients. Mast cell activation can be inhibited by blocking IgE binding to FcεRI; by inhibiting c-kit, which is activated by stem cell factor (SCF); or by inhibiting spleen tyrosine kinase (SYK). Mast cell stabilizers, such as cromones and furosemide, might work through specific ion channels or G protein coupled receptors for which novel modulators can be developed. Adapted from Barnes. 5 patients. Because Syk is widely distributed in immune and neuronal cells, there are concerns about side effects. As with other kinase inhibitors, there can be side effects with systemic administration, and therefore inhalation might be preferred. Peroxisome proliferator activated receptor g agonists Peroxisome proliferator activated receptor (PPAR) g agonists have a wide spectrum of anti-inflammatory effects, including inhibitory effects on macrophages and T cells and neutrophilic inflammation, and polymorphisms of the PPARg gene have been linked to increased risk of asthma. 107 The PPARg agonist rosiglitazone produced a small improvement in lung function in smoking asthmatic patients in whom ICSs were ineffective 108 and a modest (15%) reduction in late response to inhaled allergen in patients with mild asthma. 109 This suggests that PPARg agonists, such as thiazolidinediones, have little therapeutic potential in asthma therapy. MAST CELL INHIBITORS Mast cell activation is important as a driving mechanism in some patients with severe asthma. 53 There are several approaches to inhibiting mast cell activation (Fig 3), 5 and anti-ige has already been shown to be of value in the treatment of some patients with severe asthma. Stem cell factor is a key regulator of mast cell survival in the airways and acts through the receptor c-kit on mast cells. 110 Plasma concentrations of stem cell factor are increased in patients with severe asthma. 111 Blockade of stem cell factor or c-kit is effective in animal models of asthma, suggesting that this pathway might be a good target for new asthma therapies. Masitinib is a potent tyrosine kinase inhibitor that blocks c-kit (as well as platelet-derived growth factor receptors) and provides some symptomatic benefit in patients with severe asthma. 112 More selective c-kit inhibitors are in development. Cromones (cromolyn sodium and nedocromil sodium) inhibit the activation of human mucosal mast cells and are very effective against allergen and other indirect challenges that involve mast cell activation. 113 The effects of cromones are closely mimicked
8 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES 55 FIG 4. Corticosteroid resistance in some patients with severe asthma is due to a reduction in HDAC2 activity and expression as a result of oxidative stress through activation of PI3Kd. This can be reversed by antioxidants, including Nrf2 activators, theophylline, nortriptyline, and selective PI3Kd inhibitors. Macrolides also reverse corticosteroid resistance by acting further down the pathway. In the future, selective HDAC2 activators might be developed. by the diuretic furosemide, suggesting that they might act through ion channels. However, the molecular target for cromones was never identified, although recent studies suggest that an orphan G protein coupled receptor called GPR35 might be a target. 114 THE PROBLEM OF CORTICOSTEROID RESISTANCE Resistance to the anti-inflammatory effects of corticosteroids might be an important factor in determining asthma severity. Several molecular mechanisms have now been described to account for corticosteroid resistance in asthmatic patients, including activation of p38 MAPK activity (as described above), increased expression of an alternatively spliced variant of the glucocorticoid receptor GRb, increased production of macrophage migratory inhibitory factor (MIF), and reduced expression of HDAC This suggests that there might be therapies that could potentially reverse corticosteroid resistance and that there might be different phenotypes of corticosteroid resistance in asthma that could require different therapeutic approaches. p38 MAPK inhibitors have been shown to increase the antiinflammatory responses to corticosteroids in PBMCs from patients with severe asthma, 98 and as discussed above, p38 MAPK inhibitors are in clinical development for the treatment of severe asthma. MIF is reported to be increased in patients with severe asthma and block the anti-inflammatory effects of corticosteroids, 116 but the molecular mechanisms are poorly understood, and it has been difficult to find drugs that block its actions. 117 MIF can signal and cause corticosteroid resistance through the activation of p38 MAPK. 118 HDAC2 activation There is increasing evidence that corticosteroid resistance in patients with COPD is due to a reduction in HDAC2 activity and expression as a result of oxidative and nitrative stress. 119 This results in increased acetylation of the glucocorticoid receptor, which prevents it from inhibiting NF-kB driven inflammation. 120 There is evidence that a similar mechanism might underlie corticosteroid resistance in patients with severe asthma, in whom there is increased oxidative stress from endogenously generated oxidants. 121,122 A novel therapeutic strategy is reversal of this corticosteroid resistance by increasing the expression and activity of HDAC2, and this can be achieved in several ways (Fig 4). Low doses of oral theophylline increase HDAC2 expression in alveolar macrophages from patients with COPD and thereby restore steroid responsiveness. 123,124 It has previously been shown that addition of low-dose theophylline to moderate doses of ICSs is more effective in patients with severe asthma than increasing the dose of ICS to the maximum tolerated dose 125 and that withdrawal of low-dose theophylline causes a loss of asthma control in patients with severe asthma. 126 In smoking asthmatic patients who become refractory to corticosteroids, low-dose theophylline is effective when added to a dose of ICS, which is ineffective alone. 127 The molecular mechanism of action of theophylline in increasing HDAC2 levels is independent of PDE inhibition and appears to be mediated by inhibition of oxidant-activated PI3Kd. 103,128 The tricyclic antidepressant nortriptyline also reverses corticosteroid resistance by inhibiting PI3Kd and therefore might have clinical benefit as an add-on therapy, although clinical trials have not yet been done in patients with severe asthma. 129 Selective PI3Kd inhibitors might be of potential value in patients with severe asthma in combination with ICSs. Selective PI3Kd inhibitors are now in clinical development for the treatment of B-cell leukemia but might also be useful in patients with severe asthma, especially if administered by means of inhalation to avoid any hematologic side effects. Antioxidants Oxidative stress is increased in patients with severe asthma, 130 particularly during exacerbations, and reactive oxygen species are likely to amplify inflammation and contribute to its
9 56 BARNES J ALLERGY CLIN IMMUNOL JANUARY 2012 pathophysiology. Oxidative stress also reduces steroid responsiveness through a reduction in HDAC2 activity and expression. This suggests that antioxidants might reverse corticosteroid resistance and also reduce inflammation. Unfortunately, currently available antioxidants based on glutathione are relatively weak and are inactivated by oxidative stress, and therefore new and more potent and stable antioxidants are needed, such as superoxide dismutase mimics and NADPH oxidase inhibitors. 131 The transcription factor nuclear factor erythroid 2 related factor 2 (Nrf2) plays a key role in the regulation of endogenous antioxidant genes and might be dysfunctional in patients with severe asthma. Several Nrf2 activators, such as sulforaphane (which occurs naturally in broccoli) and the synthetic triterpenoid 1-(2- cyano-3-,12-dioxooleana-1,9-dien-28-oyl)imidazole-methyl ester, have now been identified, 132 and Nrf2 activators are now in clinical development. MACROLIDES There is evidence that some patients with severe asthma are chronically infected with atypical bacteria, such as Mycoplasma pneumoniae and Chlamydia pneumoniae. 133 In patients with infection confirmed by means of PCR and culture, there was a significant improvement in FEV 1 after a 6-week course of clarythromycin. 134 However, in a larger trial of patients with poorly controlled asthma, treatment with clarithromycin over a 16-week period did not produce any clinically meaningful improvement in asthma control, even in the patients who had positive PCR results for atypical bacteria, although there was a significant reduction in airway hyperresponsiveness. 135 It has long been recognized that macrolides have anti-inflammatory effects that might be independent of their antibiotic effects. 136 Macrolides appear to inhibit inflammation by inhibiting NF-kB and other transcription factors, but the precise molecular mechanisms have not yet been determined. In patients with severe neutrophilic asthma, a course of azithromycin significantly reduced sputum neutrophil numbers and CXCL8 concentrations, with some improvement in symptoms. 137 This suggests that it might be worth using a therapeutic trial of macrolide antibiotics in patients with severe asthma who have predominantly neutrophilic inflammation. A nonantibiotic macrolide (EM-703) reverses corticosteroid resistance caused by oxidative stress by increasing HDAC2 activity. 138 Several nonantibiotic macrolides are now in development as anti-inflammatory therapies. 139 BRONCHIAL THERMOPLASTY Bronchial thermoplasty delivers controlled thermal energy to the bronchial wall to selectively reduce the amount of airway smooth muscle and has been studied in patients with severe asthma. It is usually administered as 3 outpatient bronchoscopic procedures separated by 3 weeks. In a large controlled trial of almost 200 patients with severe asthma, bronchial thermoplasty compared with a sham procedure produced a small improvement in asthma-specific quality-of-life scores (although this was far less than the minimal clinically significant difference for this test) and a small reduction in exacerbations after treatment. 140 However, significantly more patients were hospitalized, and therefore it is uncertain whether the small clinical benefit is justifiable. In another study asthma control was improved compared with that seen in a control group in patients taking ICSs in whom longacting b 2 -agonists were withdrawn, 141 suggesting that it would provide no greater benefit than a bronchodilator. The safety of the procedure has been followed for up to 5 years with no loss of lung function, suggesting that there are no structural changes as a consequence of the therapy. 142 It is still unclear how much benefit this procedure provides in patients with severe asthma, and the clinical outcomes show little change and might not even be apparent when patients are treated with long-acting bronchodilators. It is possible that this procedure is indicated in carefully selected patients in whom airway smooth muscle hypertrophy is predominant, as evidenced by pronounced airway hyperresponsiveness. The mechanism of action of bronchial thermoplasty has been determined from studies in normal dogs, and it is uncertain how the procedure affects the airways of asthmatic patients or whether it leads to reduced inflammation by reducing airway smooth muscle cell secretion of inflammatory mediators in the airways of asthmatic patients. FUTURE DIRECTIONS It is now becoming clear that there are several distinct phenotypes of severe asthma and that these might require different therapeutic approaches. For example, patients whose symptoms were not controlled on maximal inhaled therapies that have high sputum eosinophilia and frequent exacerbations might benefit from anti IL-5 therapy with mepolizumab or reslizumab. By contrast, neutrophilic asthma might respond to antiinflammatory therapies that target neutrophilic inflammation, including PDE4 inhibitors, p38 MAPK inhibitors, CXCR2 antagonists, or macrolides. Corticosteroid resistance is likely to be an important mechanism contributing to poor treatment control in patients with severe asthma and might respond to therapies that target the molecular mechanisms of corticosteroid resistance, such as p38 MAPK inhibitors in some patients, or treatments that increase HDAC2 levels, such as theophylline, nortriptyline, and PI3Kd inhibitors among others. Analysis of large datasets of adults and children with severe asthma is now beginning to recognize distinct phenotypes. 143,144 It will be important to identify biomarkers that predict response to identify therapeutic subphenotypes of asthma, and this area requires more research so that therapy can be personalized, particularly for therapies that target specific mediators or mechanisms, because only a small proportion of patients with severe asthma are likely to respond adequately. REFERENCES 1. Partridge MR, van der Molen T, Myrseth SE, Busse WW. Attitudes and actions of asthma patients on regular maintenance therapy: the INSPIRE study. BMC Pulm Med 2006;6: Chapman KR, Boulet LP, Rea RM, Franssen E. Suboptimal asthma control: prevalence, detection and consequences in general practice. Eur Respir J 2008;31: Gamble J, Stevenson M, McClean E, Heaney LG. The prevalence of nonadherence in difficult asthma. Am J Respir Crit Care Med 2009;180: ten Brinke A, Zwinderman AH, Sterk PJ, Rabe KF, Bel EH. Refractory eosinophilic airway inflammation in severe asthma: effect of parenteral corticosteroids. Am J Respir Crit Care Med 2004;170: Barnes PJ. New drugs for asthma: is there any progress? Trends Pharmacol Sci 2010;31: Cates CJ, Lasserson TJ. Combination formoterol and budesonide as maintenance and reliever therapy versus inhaled steroid maintenance for chronic asthma in adults and children. Cochrane Database Syst Rev 2009;(2):CD Barnes PJ. Scientific rationale for using a single inhaler for asthma control. Eur Respir Dis 2007;29:
10 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES Erin EM, Zacharasiewicz AS, Nicholson GC, Tan AJ, Neighbour H, Engelstatter R, et al. Rapid anti-inflammatory effect of inhaled ciclesonide in asthma: a randomised, placebo-controlled study. Chest 2008;134: Papi A, Caramori G, Adcock IM, Barnes PJ. Rescue treatment in asthma. More than as-needed bronchodilation. Chest 2009;135: Nave R. Clinical pharmacokinetic and pharmacodynamic profile of inhaled ciclesonide. Clin Pharmacokinet 2009;48: Gentile DA, Skoner DP. New asthma drugs: small molecule inhaled corticosteroids. Curr Opin Pharmacol 2010;10: Contoli M, Bousquet J, Fabbri LM, Magnussen H, Rabe KF, Siafakas NM, et al. The small airways and distal lung compartment in asthma and COPD: a time for reappraisal. Allergy 2010;65: Barnes PJ. Glucocorticosteroids: current and future directions. Br J Pharmacol 2011;163: Schacke H, Schottelius A, Docke WD, Strehlke P, Jaroch S, Schmees N, et al. Dissociation of transactivation from transrepression by a selective glucocorticoid receptor agonist leads to separation of therapeutic effects from side effects. Proc Natl Acad Sci U S A 2004;101: De Bosscher K. Selective glucocorticoid receptor modulators. J Steroid Biochem Mol Biol 2010;120: Jaeschke R, O Byrne PM, Mejza F, Nair P, Lesniak W, Brozek J, et al. The safety of long-acting beta-agonists among patients with asthma using inhaled corticosteroids: systematic review and metaanalysis. Am J Respir Crit Care Med 2008;178: Sears MR. Safety of long-acting beta-agonists: are new data really required? Chest 2009;136: Cazzola M, Calzetta L, Matera MG. Beta(2)-adrenoceptor agonists: current and future direction. Br J Pharmacol 2011;163: Raemdonck J, de Alba J, Birrell MA, Grace M, Maher SA, Irvin CG, et al. A role for sensory nerves in the late asthmatic response. Thorax 2011[Epub ahead of print]. 20. Kummer W, Lips KS, Pfeil U. The epithelial cholinergic system of the airways. Histochem Cell Biol 2008;130: Bateman ED, Rennard S, Barnes PJ, Dicpinigaitis PV, Gosens R, Gross NJ, et al. Alternative mechanisms for tiotropium. Pulm Pharmacol Ther 2009;22: Buels KS, Jacoby DB, Fryer AD. Non-bronchodilating mechanisms of tiotropium prevent airway hyperreactivity in a guinea pig model of allergic asthma. Br J Pharmacol 2011[Epub ahead of print]. 23. Ohta S, Oda N, Yokoe T, Tanaka A, Yamamoto Y, Watanabe Y, et al. Effect of tiotropium bromide on airway inflammation and remodelling in a mouse model of asthma. Clin Exp Allergy 2010;40: Bos IS, Gosens R, Zuidhof AB, Schaafsma D, Halayko AJ, Meurs H, et al. Inhibition of allergen-induced airway remodelling by tiotropium and budesonide: a comparison. Eur Respir J 2007;30: Pera T, Zuidhof A, Valadas J, Smit M, Schoemaker RG, Gosens R, et al. Tiotropium inhibits pulmonary inflammation and remodelling in a guinea pig model of COPD. Eur Respir J 2011;38: Buhling F, Lieder N, Kuhlmann UC, Waldburg N, Welte T. Tiotropium suppresses acetylcholine-induced release of chemotactic mediators in vitro. Respir Med 2007;101: Park HW, Yang MS, Park CS, Kim TB, Moon HB, Min KU, et al. Additive role of tiotropium in severe asthmatics and Arg16Gly in ADRB2 as a potential marker to predict response. Allergy 2009;64: Kerstjens HA, Disse B, Schroder-Babo W, Bantje TA, Gahlemann M, Sigmund R, et al. Tiotropium improves lung function in patients with severe uncontrolled asthma: a randomized controlled trial. J Allergy Clin Immunol 2011;128: Peters SP, Kunselman SJ, Icitovic N, Moore WC, Pascual R, Ameredes BT, et al. Tiotropium bromide step-up therapy for adults with uncontrolled asthma. N Engl J Med 2010;363: Bateman ED, Kornmann O, Schmidt P, Pivovarova A, Engel M, Fabbri LM. Tiotropium is noninferior to salmeterol in maintaining improved lung function in B16-Arg/Arg patients with asthma. J Allergy Clin Immunol 2011;128: Joos GF. Potential for long-acting muscarinic antagonists in chronic obstructive pulmonary disease. Expert Opin Investig Drugs 2010;19: Barnes PJ. Triple inhalers for obstructive airways disease: will they be useful? Expert Rev Respir Med 2011;5: Ray NC, Alcaraz L. Muscarinic antagonist-beta-adrenergic agonist dual pharmacology molecules as bronchodilators: a patent review. Expert Opin Ther Pat 2009; 19: Linden A, Hansson L, Andersson A, Palmqvist M, Arvidsson P, Lofdahl CG, et al. Bronchodilation by an inhaled VPAC(2) receptor agonist in patients with stable asthma. Thorax 2003;58: Deshpande DA, Wang WC, McIlmoyle EL, Robinett KS, Schillinger RM, An SS, et al. Bitter taste receptors on airway smooth muscle bronchodilate by localized calcium signaling and reverse obstruction. Nat Med 2010;16: Banner KH, Press NJ. Dual PDE3/4 inhibitors as therapeutic agents for chronic obstructive pulmonary disease. Br J Pharmacol 2009;157: Buckley J, Birrell MA, Maher SA, Nials AT, Clarke DL, Belvisi MG. EP4 receptor as a new target for bronchodilator therapy. Thorax 2011[Epub ahead of print]. 38. Busse WW, Morgan WJ, Gergen PJ, Mitchell HE, Gern JE, Liu AH, et al. Randomized trial of omalizumab (anti-ige) for asthma in inner-city children. N Engl J Med 2011;364: Hanania NA, Alpan O, Hamilos DL, Condemi JJ, Reyes-Rivera I, Zhu J, et al. Omalizumab in severe allergic asthma inadequately controlled with standard therapy: a randomized trial. Ann Intern Med 2011;154: Rodrigo GJ, Neffen H, Castro-Rodriguez JA. Efficacy and safety of subcutaneous omalizumab vs placebo as add-on therapy to corticosteroids for children and adults with asthma: a systematic review. Chest 2011;139: Takhar P, Corrigan CJ, Smurthwaite L, O Connor BJ, Durham SR, Lee TH, et al. Class switch recombination to IgE in the bronchial mucosa of atopic and nonatopic patients with asthma. J Allergy Clin Immunol 2007;119: Rosenwasser LJ, Meng J. Anti-CD23. Clin Rev Allergy Immunol 2005;29: Barnes PJ. New molecular targets for the treatment of neutrophilic diseases. J Allergy Clin Immunol 2007;119: Robinson DS, Campbell DA, Barnes PJ. Addition of an anti-leukotriene to therapy in chronic severe asthma in a clinic setting: a double-blind, randomised, placebo-controlled study. Lancet 2001;357: Ohnishi H, Miyahara N, Gelfand EW. The role of leukotriene B(4) in allergic diseases. Allergol Int 2008;57: Evans DJ, Barnes PJ, Coulby LJ, Spaethe SM, van Alstyne EC, Pechous PA, et al. The effect of a leukotriene B 4 antagonist LY on allergen-induced responses in asthma. Thorax 1996;51: Cho KJ, Seo JM, Shin Y, Yoo MH, Park CS, Lee SH, et al. Blockade of airway inflammation and hyperresponsiveness by inhibition of BLT2, a low-affinity leukotriene B4 receptor. Am J Respir Cell Mol Biol 2010;42: Cho KJ, Seo JM, Lee MG, Kim JH. BLT2 Is upregulated in allergen-stimulated mast cells and mediates the synthesis of Th2 cytokines. J Immunol 2010;185: Rao NL, Riley JP, Banie H, Xue X, Sun B, Crawford S, et al. Leukotriene A(4) hydrolase inhibition attenuates allergic airway inflammation and hyperresponsiveness. Am J Respir Crit Care Med 2010;181: Magrioti V, Kokotos G. Phospholipase A2 inhibitors as potential therapeutic agents for the treatment of inflammatory diseases. Expert Opin Ther Pat 2010; 20: Grant GE, Rokach J, Powell WS. 5-Oxo-ETE and the OXE receptor. Prostaglandins Other Lipid Mediat 2009;89: Pettipher R, Hansel TT, Armer R. Antagonism of the prostaglandin D2 receptors DP1 and CRTH2 as an approach to treat allergic diseases. Nat Rev Drug Discov 2007;6: Balzar S, Fajt ML, Comhair SA, Erzurum SC, Bleecker E, Busse WW, et al. Mast cell phenotype, location, and activation in severe asthma: data from the severe asthma research program. Am J Respir Crit Care Med 2011;183: Barnes N, Pavord I, Chuchalin A, Bell J, Hunter M, Lewis T, et al. A randomized, double-blind, placebo-controlled study of the CRTH2 antagonist OC in moderate persistent asthma. Clin Exp Allergy 2011[Epub ahead of print]. 55. Barnes PJ. Cytokine networks in asthma and chronic obstructive pulmonary disease. J Clin Invest 2008;118: Hansbro PM, Kaiko GE, Foster PS. Cytokine/anti-cytokine therapy novel treatments for asthma? Br J Pharmacol 2011;163: Barnes PJ. Pathophysiology of allergic inflammation. Immunol Rev 2011;242: Maneechotesuwan K, Yao X, Ito K, Jazrawi E, Usmani OS, Adcock IM, et al. Suppression of GATA-3 nuclear import and phosphorylation: a novel mechanism of corticosteroid action in allergic disease. PLoS Med 2009;6:e Alcorn JF, Crowe CR, Kolls JK. TH17 cells in asthma and COPD. Annu Rev Physiol 2010;72: McKinley L, Alcorn JF, Peterson A, Dupont RB, Kapadia S, Logar A, et al. TH17 cells mediate steroid-resistant airway inflammation and airway hyperresponsiveness in mice. J Immunol 2008;181: Spahn JD, Szefler SJ, Surs W, Doherty DE, Nimmagadda SR, Leung DY. A novel action of IL-13: induction of diminished monocyte glucocorticoid receptorbinding affinity. J Immunol 1996;157: Matthews JG, Ito K, Barnes PJ, Adcock IM. Defective glucocorticoid receptor nuclear translocation and altered histone acetylation patterns in glucocorticoidresistant patients. J Allergy Clin Immunol 2004;113: Wenzel S, Wilbraham D, Fuller R, Getz EB, Longphre M. Effect of an interleukin-4 variant on late phase asthmatic response to allergen challenge in asthmatic patients: results of two phase 2a studies. Lancet 2007;370:
11 58 BARNES J ALLERGY CLIN IMMUNOL JANUARY Corren J, Lemanske RF, Hanania NA, Korenblat PE, Parsey MV, Arron JR, et al. Lebrikizumab treatment in adults with asthma. N Engl J Med 2011;365: Corren J, Busse W, Meltzer EO, Mansfield L, Bensch G, Fahrenholz J, et al. A randomized, controlled, phase 2 study of AMG 317, an IL-4Ralpha antagonist, in patients with asthma. Am J Respir Crit Care Med 2010;181: Nicholson GC, Kariyawasam HH, Tan AJ, Hohlfeld JM, Quinn D, Walker C, et al. The effects of an anti-il-13 monoclonal antibody on cytokine levels and nasal symptoms following nasal allergen challenge. J Allergy Clin Immunol 2011; 128:800-7, e Chiba Y, Todoroki M, Nishida Y, Tanabe M, Misawa M. A novel STAT6 inhibitor AS ameliorates antigen-induced bronchial hypercontractility in mice. Am J Respir Cell Mol Biol 2009;41: Leckie MJ, ten Brincke A, Khan J, Diamant Z, O Connor BJ, Walls CM, et al. Effects of an interleukin-5 blocking monoclonal antibody on eosinophils, airway hyperresponsiveness and the late asthmatic response. Lancet 2000;356: Flood-Page P, Swenson C, Faiferman I, Matthews J, Williams M, Brannick L, et al. A study to evaluate safety and efficacy of mepolizumab in patients with moderate persistent asthma. Am J Respir Crit Care Med 2007;176: Haldar P, Brightling CE, Hargadon B, Gupta S, Monteiro W, Sousa A, et al. Mepolizumab and exacerbations of refractory eosinophilic asthma. N Engl J Med 2009;360: Nair P, Pizzichini MM, Kjarsgaard M, Inman MD, Efthimiadis A, Pizzichini E, et al. Mepolizumab for prednisone-dependent asthma with sputum eosinophilia. N Engl J Med 2009;360: Castro M, Mathur S, Hargreave F, Boulet LP, Xie F, Young J, et al. Reslizumab for poorly controlled, eosinophilic asthma: a randomized, placebo-controlled study. Am J Respir Crit Care Med 2011[Epub ahead of print]. 73. Kolbeck R, Kozhich A, Koike M, Peng L, Andersson CK, Damschroder MM, et al. MEDI-563, a humanized anti-il-5 receptor alpha mab with enhanced antibody-dependent cell-mediated cytotoxicity function. J Allergy Clin Immunol 2010;125: Gauvreau GM, Boulet LP, Cockcroft DW, Baatjes A, Cote J, Deschesnes F, et al. Antisense therapy against CCR3 and the common beta chain attenuates allergen-induced eosinophilic responses. Am J Respir Crit Care Med 2008; 177: Kim S, Marigowda G, Oren E, Israel E, Wechsler ME. Mepolizumab as a steroidsparing treatment option in patients with Churg-Strauss syndrome. J Allergy Clin Immunol 2010;125: Straumann A, Conus S, Grzonka P, Kita H, Kephart G, Bussmann C, et al. Antiinterleukin-5 antibody treatment (mepolizumab) in active eosinophilic oesophagitis: a randomised, placebo-controlled, double-blind trial. Gut 2010;59: Xing J, Wu Y, Ni B. Th9: a new player in asthma pathogenesis? J Asthma 2011; 48: Parker JM, Oh CK, Laforce C, Miller SD, Pearlman DS, Le C, et al. Safety profile and clinical activity of multiple subcutaneous doses of MEDI-528, a humanized anti-interleukin-9 monoclonal antibody, in two randomized phase 2a studies in subjects with asthma. BMC Pulm Med 2011;11: Ziegler SF, Artis D. Sensing the outside world: TSLP regulates barrier immunity. Nat Immunol 2010;11: Shikotra A, Choy DF, Ohri CM, Doran E, Butler C, Hargadon B, et al. Increased expression of immunoreactive thymic stromal lymphopoietin in patients with severe asthma. J Allergy Clin Immunol 2011[Epub ahead of print]. 81. Siddiqui S, Mistry V, Doe C, Stinson S, Foster M, Brightling C. Airway wall expression of OX40/OX40L and interleukin-4 in asthma. Chest 2010;137: Berry MA, Hargadon B, Shelley M, Parker D, Shaw DE, Green RH, et al. Evidence of a role of tumor necrosis factor alpha in refractory asthma. N Engl J Med 2006;354: Howarth PH, Babu KS, Arshad HS, Lau L, Buckley M, McConnell W, et al. Tumour necrosis factor (TNFalpha) as a novel therapeutic target in symptomatic corticosteroid dependent asthma. Thorax 2005;60: Wenzel SE, Barnes PJ, Bleecker ER, Bousquet J, Busse W, Dahlen SE, et al. A randomized, double-blind, placebo-controlled study of TNF-a blockade in severe persistent asthma. Am J Respir Crit Care Med 2009;179: Holgate ST, Noonan M, Chanez P, Busse W, Dupont L, Pavord I, et al. Efficacy and safety of etanercept in moderate-to-severe asthma: a randomised, controlled trial. Eur Respir J 2011;37: Proudfoot AE, Power CA, Schwarz MK. Anti-chemokine small molecule drugs: a promising future? Expert Opin Investig Drugs 2010;19: Gauvreau GM, Boulet LP, Cockcroft DW, Baatjes A, Cote J, Deschesnes F, et al. Antisense therapy against CCR3 and the common beta chain attenuates allergeninduced eosinophilic responses. Am J Respir Crit Care Med 2008;177: Antoniu SA. Mogamulizumab, a humanized mab against C-C chemokine receptor 4 for the potential treatment of T-cell lymphomas and asthma. Curr Opin Mol Ther 2010;12: Donnelly LE, Barnes PJ. CXCR2 antagonism to prevent airway inflammation. Drugs Future 2011[Epub ahead of print]. 90. Holz O, Khalilieh S, Ludwig-Sengpiel A, Watz H, Stryszak P, Soni P, et al. SCH527123, a novel CXCR2 antagonist, inhibits ozone-induced neutrophilia in healthy subjects. Eur Respir J 2010;35: Diamant Z, Spina D. PDE4-inhibitors: a novel, targeted therapy for obstructive airways disease. Pulm Pharmacol Ther 2011;24: Bousquet J, Aubier M, Sastre J, Izquierdo JL, Adler LM, Hofbauer P, et al. Comparison of roflumilast, an oral anti-inflammatory, with beclomethasone dipropionate in the treatment of persistent asthma. Allergy 2006;61: Houslay MD, Schafer P, Zhang KY. Keynote review: phosphodiesterase-4 as a therapeutic target. Drug Discov Today 2005;10: Adcock IM, Chung KF, Caramori G, Ito L. Kinase inhibitors and airway inflammation. Eur J Pharmacol 2006;533: Karin M, Yamamoto Y, Wang QM. The IKK NF-kappa B system: a treasure trove for drug development. Nat Rev Drug Discov 2004;3: Bhavsar P, Hew M, Khorasani N, Alfonso T, Barnes PJ, Adcock I, et al. Relative corticosteroid insensitivity of alveolar macrophages in severe asthma compared to non-severe asthma. Thorax 2008;63: Irusen E, Matthews JG, Takahashi A, Barnes PJ, Chung KF, Adcock IM. p38 Mitogen-activated protein kinase-induced glucocorticoid receptor phosphorylation reduces its activity: role in steroid-insensitive asthma. J Allergy Clin Immunol 2002;109: Bhavsar P, Khorasani N, Hew M, Johnson M, Chung KF. Effect of p38 MAPK inhibition on corticosteroid suppression of cytokine release in severe asthma. Eur Respir J 2010;35: Maneechotesuwan K, Xin Y, Ito K, Jazrawi E, Lee KY, Usmani OS, et al. Regulation of Th2 cytokine genes by p38 MAPK-mediated phosphorylation of GATA-3. J Immunol 2007;178: Duan W, Chan JH, McKay K, Crosby JR, Choo HH, Leung BP, et al. Inhaled p38alpha mitogen-activated protein kinase antisense oligonucleotide attenuates asthma in mice. Am J Respir Crit Care Med 2005;171: Cuenda A, Rousseau S. p38 MAP-kinases pathway regulation, function and role in human diseases. Biochim Biophys Acta 2007;1773: Rommel C, Camps M, Ji H. PI3K delta and PI3K gamma: partners in crime in inflammation in rheumatoid arthritis and beyond? Nat Rev Immunol 2007;7: To Y, Ito K, Kizawa Y, Failla M, Ito M, Kusama T, et al. Targeting phosphoinositide-3-kinase-d with theophylline reverses corticosteroid insensitivity in COPD. Am J Respir Crit Care Med 2010;182: Denyer J, Patel V. Syk kinase inhibitors in allergic diseases. Drug News Perspect 2009;22: Stenton GR, Ulanova M, Dery RE, Merani S, Kim MK, Gilchrist M, et al. Inhibition of allergic inflammation in the airways using aerosolized antisense to Syk kinase. J Immunol 2002;169: Meltzer EO, Berkowitz RB, Grossbard EB. An intranasal Syk-kinase inhibitor (R112) improves the symptoms of seasonal allergic rhinitis in a park environment. J Allergy Clin Immunol 2005;115: Oh SH, Park SM, Lee YH, Cha JY, Lee JY, Shin EK, et al. Association of peroxisome proliferator-activated receptor-gamma gene polymorphisms with the development of asthma. Respir Med 2009;103: Spears M, Donnelly I, Jolly L, Brannigan M, Ito K, McSharry C, et al. Bronchodilatory effect of the PPAR-g agonist rosiglitazone in smokers with asthma. Clin Pharmacol Ther 2009;86: Richards DB, Bareille P, Lindo EL, Quinn D, Farrow SN. Treatment with a peroxisomal proliferator activated receptor gamma agonist has a modest effect in the allergen challenge model in asthma: a randomised controlled trial. Respir Med 2009;104: Reber L, Da Silva CA, Frossard N. Stem cell factor and its receptor c-kit as targets for inflammatory diseases. Eur J Pharmacol 2006;533: Makowska JS, Cieslak M, Kowalski ML. Stem cell factor and its soluble receptor (c-kit) in serum of asthmatic patients correlation with disease severity. BMC Pulm Med 2009;9: Humbert M, de Blay F, Garcia G, Prud homme A, Leroyer C, Magnan A, et al. Masitinib, a c-kit/pdgf receptor tyrosine kinase inhibitor, improves disease control in severe corticosteroid-dependent asthmatics. Allergy 2009;64: Norris AA. Pharmacology of sodium cromoglycate. Clin Exp Allergy 1996; 26(suppl 4): Yang Y, Lu JY, Wu X, Summer S, Whoriskey J, Saris C, et al. G-protein-coupled receptor 35 is a target of the asthma drugs cromolyn disodium and nedocromil sodium. Pharmacology 2010;86: Barnes PJ, Adcock IM. Glucocorticoid resistance in inflammatory diseases. Lancet 2009;342:
12 J ALLERGY CLIN IMMUNOL VOLUME 129, NUMBER 1 BARNES Mizue Y, Ghani S, Leng L, McDonald C, Kong P, Baugh J, et al. Role for macrophage migration inhibitory factor in asthma. Proc Natl Acad Sci U S A 2005; 102: Hoi AY, Iskander MN, Morand EF. Macrophage migration inhibitory factor: a therapeutic target across inflammatory diseases. Inflamm Allergy Drug Targets 2007;6: Ayoub S, Hickey MJ, Morand EF. Mechanisms of disease: macrophage migration inhibitory factor in SLE, RA and atherosclerosis. Nat Clin Pract Rheumatol 2008; 4: Barnes PJ. Role of HDAC2 in the pathophysiology of COPD. Ann Rev Physiol 2009;71: Ito K, Yamamura S, Essilfie-Quaye S, Cosio B, Ito M, Barnes PJ, et al. Histone deacetylase 2-mediated deacetylation of the glucocorticoid receptor enables NFkB suppression. J Exp Med 2006;203: Hew M, Bhavsar P, Torrego A, Meah S, Khorasani N, Barnes PJ, et al. Relative corticosteroid insensitivity of peripheral blood mononuclear cells in severe asthma. Am J Respir Crit Care Med 2006;174: Cosio BG, Mann B, Ito K, Jazrawi E, Barnes PJ, Chung KF, et al. Histone acetylase and deacetylase activity in alveolar macrophages and blood monocytes in asthma. Am J Respir Crit Care Med 2004;170: Cosio BG, Tsaprouni L, Ito K, Jazrawi E, Adcock IM, Barnes PJ. Theophylline restores histone deacetylase activity and steroid responses in COPD macrophages. J Exp Med 2004;200: Barnes PJ. Theophylline for COPD. Thorax 2006;61: Evans DJ, Taylor DA, Zetterstrom O, Chung KF, O Connor BJ, Barnes PJ. A comparison of low-dose inhaled budesonide plus theophylline and high-dose inhaled budesonide for moderate asthma. New Engl J Med 1997;337: Kidney J, Dominguez M, Taylor PM, Rose M, Chung KF, Barnes PJ. Immunomodulation by theophylline in asthma: demonstration by withdrawal of therapy. Am J Respir Crit Care Med 1995;151: Spears M, Donnelly I, Jolly L, Brannigan M, Ito K, McSharry C, et al. Effect of theophylline plus beclometasone on lung function in smokers with asthma a pilot study. Eur Respir J 2009;33: Marwick JA, Caramori G, Stevenson CC, Casolari P, Jazrawi E, Barnes PJ, et al. Inhibition of PI3Kd restores glucocorticoid function in smoking-induced airway inflammation in mice. Am J Respir Crit Care Med 2009;179: Mercado N, To Y, Ito K, Barnes PJ. Nortriptyline reverses corticosteroid insensitivity by inhibition of PI3K-d. J Pharmacol Exp Ther 2011;337: Montuschi P, Ciabattoni G, Corradi M, Nightingale JA, Collins JV, Kharitonov SA, et al. Increased 8-Isoprostane, a marker of oxidative stress, in exhaled condensates of asthmatic patients. Am J Respir Crit Care Med 1999;160: Kirkham P, Rahman I. Oxidative stress in asthma and COPD: antioxidants as a therapeutic strategy. Pharmacol Ther 2006;111: Sussan TE, Rangasamy T, Blake DJ, Malhotra D, El Haddad H, Bedja D, et al. Targeting Nrf2 with the triterpenoid CDDO-imidazolide attenuates cigarette smoke-induced emphysema and cardiac dysfunction in mice. Proc Natl Acad Sci U S A 2009;106: Metz G, Kraft M. Effects of atypical infections with Mycoplasma and Chlamydia on asthma. Immunol Allergy Clin North Am 2010;30: Kraft M, Torvik JA, Trudeau JB, Wenzel SE, Martin RJ. Theophylline: potential antiinflammatory effects in nocturnal asthma. J Allergy Clin Immunol 1996;97: Sutherland ER, King TS, Icitovic N, Ameredes BT, Bleecker E, Boushey HA, et al. A trial of clarithromycin for the treatment of suboptimally controlled asthma. J Allergy Clin Immunol 2010;126: Friedlander AL, Albert RK. Chronic macrolide therapy in inflammatory airways diseases. Chest 2010;138: Simpson JL, Powell H, Boyle MJ, Scott RJ, Gibson PG. Clarithromycin targets neutrophilic airway inflammation in refractory asthma. Am J Respir Crit Care Med 2008;177: Charron C, Sumakuza T, Oomura S, Ito K. EM-703, a non-antibacterial erythromycin derivative, restores HDAC2 activation diminished by hypoxia and oxidative stress. Proc Am Thorac Soc 2007;175:A Sugawara A, Sueki A, Hirose T, Nagai K, Gouda H, Hirono S, et al. Novel 12- membered non-antibiotic macrolides from erythromycin A; EM900 series as novel leads for anti-inflammatory and/or immunomodulatory agents. Bioorg Med Chem Lett 2011;21: Castro M, Rubin AS, Laviolette M, Fiterman J, De Andrade LM, Shah PL, et al. Effectiveness and safety of bronchial thermoplasty in the treatment of severe asthma: a multicenter, randomized, double-blind, sham-controlled clinical trial. Am J Respir Crit Care Med 2010;181: Cox L, Platts-Mills TA, Finegold I, Schwartz LB, Simons FE, Wallace DV. American Academy of Allergy, Asthma & Immunology/American College of Allergy, Asthma and Immunology Joint Task Force Report on omalizumab-associated anaphylaxis. J Allergy Clin Immunol 2007;120: Thomson NC, Rubin AS, Niven RM, Corris PA, Siersted HC, Olivenstein R, et al. Long-term (5 year) safety of bronchial thermoplasty: Asthma Intervention Research (AIR) trial. BMC Pulm Med 2011;11: Brasier AR, Victor S, Ju H, Busse WW, Curran-Everett D, Bleecker E, et al. Predicting intermediate phenotypes in asthma using bronchoalveolar lavage-derived cytokines. Clin Transl Sci 2010;3: Fitzpatrick AM, Teague WG, Meyers DA, Peters SP, Li X, Li H, et al. Heterogeneity of severe asthma in childhood: confirmation by cluster analysis of children in the National Institutes of Health/National Heart, Lung, and Blood Institute Severe Asthma Research Program. J Allergy Clin Immunol 2011;127:
Asthma (With a little SCID to start) Disclosures Outline Starting with the Immune System The Innate Immune System The Adaptive Immune System
 1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
9/16/2014. Anti-Immunoglobulin E (IgE) Omalizumab (Xolair ) Dosing Guidance
 Disclosure Statement of Financial Interest New Therapies for Asthma Including Omalizumab and Anti-Cytokine Therapies Marsha Dangler, PharmD, BCACP Clinical Pharmacy Specialist James H. Quillen VA Medical
Disclosure Statement of Financial Interest New Therapies for Asthma Including Omalizumab and Anti-Cytokine Therapies Marsha Dangler, PharmD, BCACP Clinical Pharmacy Specialist James H. Quillen VA Medical
Prof. Florian Gantner. Vice President Respiratory Diseases Research Boehringer Ingelheim
 Prof. Florian Gantner Vice President Respiratory Diseases Research Boehringer Ingelheim Research and Development in Practice: COPD Chronic Obstructive Pulmonary Disease (COPD) Facts Main cause of COPD
Prof. Florian Gantner Vice President Respiratory Diseases Research Boehringer Ingelheim Research and Development in Practice: COPD Chronic Obstructive Pulmonary Disease (COPD) Facts Main cause of COPD
understanding the professional guidelines
 SEVERE ASTHMA understanding the professional guidelines This guide includes information on what the European Respiratory Society (ERS) and the American Thoracic Society (ATS) have said about severe asthma.
SEVERE ASTHMA understanding the professional guidelines This guide includes information on what the European Respiratory Society (ERS) and the American Thoracic Society (ATS) have said about severe asthma.
Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis, and asthma
 Chapter 31 Drugs Used to Treat Lower Respiratory Disease Learning Objectives Describe the physiology of respirations Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis,
Chapter 31 Drugs Used to Treat Lower Respiratory Disease Learning Objectives Describe the physiology of respirations Compare the physiologic responses of the respiratory system to emphysema, chronic bronchitis,
Prevention of Acute COPD exacerbations
 December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
Drugs for treatment of respiratory diseases. Huifang Tang Department of pharmacology Zhejiang University, school of medicine tanghuifang@zju.edu.
 Drugs for treatment of respiratory diseases Huifang Tang Department of pharmacology Zhejiang University, school of medicine tanghuifang@zju.edu.cn Antiasthmatic drugs Immunological and non-immunological
Drugs for treatment of respiratory diseases Huifang Tang Department of pharmacology Zhejiang University, school of medicine tanghuifang@zju.edu.cn Antiasthmatic drugs Immunological and non-immunological
Pharmacology of the Respiratory Tract: COPD and Steroids
 Pharmacology of the Respiratory Tract: COPD and Steroids Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Pharmacology of the Respiratory Tract: COPD and Steroids Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
DRUG UTILISATION STUDY IN BRONCHIAL ASTHMA IN A TERTIARY CARE HOSPITAL
 International Journal of Pharmaceutical Applications ISSN 0976-2639, Online ISSN 2278 6023 Vol 3, Issue 2, 2012, pp 297-305 http://www.bipublication.com DRUG UTILISATION STUDY IN BRONCHIAL ASTHMA IN A
International Journal of Pharmaceutical Applications ISSN 0976-2639, Online ISSN 2278 6023 Vol 3, Issue 2, 2012, pp 297-305 http://www.bipublication.com DRUG UTILISATION STUDY IN BRONCHIAL ASTHMA IN A
Drug therapy SHORT-ACTING BETA AGONISTS SHORT-ACTING ANTICHOLINERGICS LONG-ACTING BETA AGONISTS LONG-ACTING ANTICHOLINERGICS
 Drug therapy 6 6.1 What is the role of bronchodilators in COPD? 52 SHORT-ACTING BETA AGONISTS 6.2 How do short-acting beta agonists work? 52 6.3 What are the indications for their use? 52 6.4 What is the
Drug therapy 6 6.1 What is the role of bronchodilators in COPD? 52 SHORT-ACTING BETA AGONISTS 6.2 How do short-acting beta agonists work? 52 6.3 What are the indications for their use? 52 6.4 What is the
From the Text. Clinical Indications. Clinical Indications. RSPT 2217 Non-steroidal Anti-asthma Agents. RSPT 2317 Non-steroidal Antiasthma Agents
 From the Text RSPT 2317 Non-steroidal Antiasthma Agents Gardenhire Chapter 12 Key Terms and Definitions Page 226 Nonsteroidal Antiasthma Meds Table 12-1; page 228 Comparative Features of Antileukotriene
From the Text RSPT 2317 Non-steroidal Antiasthma Agents Gardenhire Chapter 12 Key Terms and Definitions Page 226 Nonsteroidal Antiasthma Meds Table 12-1; page 228 Comparative Features of Antileukotriene
Hypersensitivity. TYPE I Hypersensitivity Classic allergy. Allergens. Characteristics of allergens. Allergens. Mediated by IgE attached to Mast cells.
 Gel and Coombs classification of hypersensitivities. Hypersensitivity Robert Beatty Type I Type II Type III Type IV MCB150 IgE Mediated IgG/IgM Mediated IgG Mediated T cell Classic Allergy rbc lysis Immune
Gel and Coombs classification of hypersensitivities. Hypersensitivity Robert Beatty Type I Type II Type III Type IV MCB150 IgE Mediated IgG/IgM Mediated IgG Mediated T cell Classic Allergy rbc lysis Immune
Background information
 Background information Asthma Asthma is a complex disease affecting the lungs that can be managed but cannot be cured. 1 Asthma can be controlled well in most people most of the time, although some people
Background information Asthma Asthma is a complex disease affecting the lungs that can be managed but cannot be cured. 1 Asthma can be controlled well in most people most of the time, although some people
RSPT 2317 Non-steroidal anti-asthma agents
 RSPT 2317 Non-steroidal Anti-asthma Agents Mechanisms of Inflammation in Asthma Mechanisms of Inflammation in Asthma Asthma is a chronic inflammatory disorder of the airways It is divided into extrinsic
RSPT 2317 Non-steroidal Anti-asthma Agents Mechanisms of Inflammation in Asthma Mechanisms of Inflammation in Asthma Asthma is a chronic inflammatory disorder of the airways It is divided into extrinsic
Topic: New Treatment = Better Outcome?
 Session on COPD: Novel Concepts and Promising New Drugs Topic: New Treatment = Better Outcome? Through a CME Grant sponsored by New Treatment = Better Outcome? Tim S. Trinidad, MD Disclosure Present: COPD
Session on COPD: Novel Concepts and Promising New Drugs Topic: New Treatment = Better Outcome? Through a CME Grant sponsored by New Treatment = Better Outcome? Tim S. Trinidad, MD Disclosure Present: COPD
VPM 152. INFLAMMATION: Chemical Mediators
 General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
Pathophysiology of asthma
 CHAPTER 5 Pathophysiology of asthma P.J. Barnes Correspondence: P.J. Barnes, Dept of Thoracic Medicine, National Heart and Lung Institute, Dovehouse St, London SW3 6LY, UK. Asthma is characterised by a
CHAPTER 5 Pathophysiology of asthma P.J. Barnes Correspondence: P.J. Barnes, Dept of Thoracic Medicine, National Heart and Lung Institute, Dovehouse St, London SW3 6LY, UK. Asthma is characterised by a
B Cell Generation, Activation & Differentiation. B cell maturation
 B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
The Annual Direct Care of Asthma
 The Annual Direct Care of Asthma The annual direct health care cost of asthma in the United States is approximately $11.5 billion; indirect costs (e.g. lost productivity) add another $4.6 billion for a
The Annual Direct Care of Asthma The annual direct health care cost of asthma in the United States is approximately $11.5 billion; indirect costs (e.g. lost productivity) add another $4.6 billion for a
COPD and Asthma Differential Diagnosis
 COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
Monoclonal Antibodies in Asthma Therapy. Yehia El-Gamal MD, PhD
 Monoclonal Antibodies in Asthma Therapy Yehia El-Gamal MD, PhD Conflict of Interest Nothing to disclose Objectives Following this presentation, the audience should be able to: Recognize some important
Monoclonal Antibodies in Asthma Therapy Yehia El-Gamal MD, PhD Conflict of Interest Nothing to disclose Objectives Following this presentation, the audience should be able to: Recognize some important
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Immunology and immunotherapy in allergic disease
 Immunology and immunotherapy in allergic disease Jing Shen, MD Faculty Advisor: Matthew Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation February 2005
Immunology and immunotherapy in allergic disease Jing Shen, MD Faculty Advisor: Matthew Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation February 2005
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma
 Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE
 PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE The content of this booklet was developed by Allergy UK. MSD reviewed this booklet to comment
PATIENT INFORMATION ABOUT TREATMENTS FOR ASTHMA AND ALLERGIC RHINITIS, PRESCRIPTIONS & OVER THE COUNTER MEDICINE The content of this booklet was developed by Allergy UK. MSD reviewed this booklet to comment
Severe asthma Definition, epidemiology and risk factors. Mina Gaga Athens Chest Hospital
 Severe asthma Definition, epidemiology and risk factors Mina Gaga Athens Chest Hospital Difficult asthma Defined as asthma, poorly controlled in terms of chronic symptoms, with episodic exacerbations,
Severe asthma Definition, epidemiology and risk factors Mina Gaga Athens Chest Hospital Difficult asthma Defined as asthma, poorly controlled in terms of chronic symptoms, with episodic exacerbations,
BSc in Medical Sciences with PHARMACOLOGY
 BSc in Medical Sciences with PHARMACOLOGY Course Director Dr Christopher John Module Leaders Dr Robert Dickinson (Module 1) Dr Anabel Varela Carver (Module 2) Dr Sohag Saleh (Module 3) Course Administrator
BSc in Medical Sciences with PHARMACOLOGY Course Director Dr Christopher John Module Leaders Dr Robert Dickinson (Module 1) Dr Anabel Varela Carver (Module 2) Dr Sohag Saleh (Module 3) Course Administrator
How to use FENO-guided asthma control in routine clinical practice
 How to use FENO-guided asthma control in routine clinical practice Asthma is a chronic inflammatory disease of the airways. This has implications for the diagnosis, management and potential prevention
How to use FENO-guided asthma control in routine clinical practice Asthma is a chronic inflammatory disease of the airways. This has implications for the diagnosis, management and potential prevention
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
5. Treatment of Asthma in Children
 Treatment of sthma in hildren 5. Treatment of sthma in hildren 5.1 Maintenance Treatment 5.1.1 rugs Inhaled Glucocorticoids. Persistent wheezing in children under the age of three can be controlled with
Treatment of sthma in hildren 5. Treatment of sthma in hildren 5.1 Maintenance Treatment 5.1.1 rugs Inhaled Glucocorticoids. Persistent wheezing in children under the age of three can be controlled with
Montelukast Sodium. -A new class of seasonal allergic rhinitis therapy
 Montelukast Sodium -A new class of seasonal allergic rhinitis therapy Symptoms of Seasonal Allergic Rhinitis Nasal itch Sneezing Rhinorrhoea Nasal stuffiness Pathogenesis of Allergic Rhinitis Mast cells,
Montelukast Sodium -A new class of seasonal allergic rhinitis therapy Symptoms of Seasonal Allergic Rhinitis Nasal itch Sneezing Rhinorrhoea Nasal stuffiness Pathogenesis of Allergic Rhinitis Mast cells,
A Genetic Analysis of Rheumatoid Arthritis
 A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
Stacie L. Penkova, PharmD, MHSA, BCPS Clinical Pharmacy Manager Critical Care Pharmacy Specialist Drug Information Coordinator Pharmacology Summit
 Stacie L. Penkova, PharmD, MHSA, BCPS Clinical Pharmacy Manager Critical Care Pharmacy Specialist Drug Information Coordinator Pharmacology Summit July 26, 2014 Objectives Classify asthma by severity Prescribe
Stacie L. Penkova, PharmD, MHSA, BCPS Clinical Pharmacy Manager Critical Care Pharmacy Specialist Drug Information Coordinator Pharmacology Summit July 26, 2014 Objectives Classify asthma by severity Prescribe
medicineupdate to find out more about this medicine
 medicineupdate Asking the right questions about new medicines Seretide for chronic obstructive pulmonary disease What this medicine is 1 What this medicine treats 2 Other medicines available for this condition
medicineupdate Asking the right questions about new medicines Seretide for chronic obstructive pulmonary disease What this medicine is 1 What this medicine treats 2 Other medicines available for this condition
YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST...
 YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST... ...HERE S WHAT TO EXPECT You have been referred to an allergist because you have or may have asthma. The health professional who referred you wants you to
YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST... ...HERE S WHAT TO EXPECT You have been referred to an allergist because you have or may have asthma. The health professional who referred you wants you to
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
Chronic obstructive pulmonary disease (COPD)
 Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
DRUG TREATMENT OF ASTHMA Asrar B. Malik, Ph.D. 312-996-7635 abmalik@uic.edu
 DRUG TREATMENT OF ASTHMA Asrar B. Malik, Ph.D. 312-996-7635 abmalik@uic.edu DRUGS USEFUL IN ASTHMA LEARNING OBJECTIVES 1. Know the working definitions of asthma and basic pathology of the disease. 2. Understand
DRUG TREATMENT OF ASTHMA Asrar B. Malik, Ph.D. 312-996-7635 abmalik@uic.edu DRUGS USEFUL IN ASTHMA LEARNING OBJECTIVES 1. Know the working definitions of asthma and basic pathology of the disease. 2. Understand
Objectives. Asthma Management
 Objectives Asthma Management BREATHE Conference Allergy and Asthma Specialists PC Christine Malloy MD March 22, 2013 Review the role of inflammation in asthma Discuss the components of the EPR-3 management
Objectives Asthma Management BREATHE Conference Allergy and Asthma Specialists PC Christine Malloy MD March 22, 2013 Review the role of inflammation in asthma Discuss the components of the EPR-3 management
Glucocorticoids, Inhaled Therapeutic Class Review (TCR)
 Glucocorticoids, Inhaled Therapeutic Class Review (TCR) July 31, 2015 No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying,
Glucocorticoids, Inhaled Therapeutic Class Review (TCR) July 31, 2015 No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying,
Montelukast Sodium Singulair, Merck. Development and Pharmacology: 1
 Montelukast Sodium Singulair, Merck Development and Pharmacology: 1 Asthma is a chronic inflammatory disease of the airways that is complicated by episodes of acute inflammation. Even patients with mild
Montelukast Sodium Singulair, Merck Development and Pharmacology: 1 Asthma is a chronic inflammatory disease of the airways that is complicated by episodes of acute inflammation. Even patients with mild
Chapter 20. Drugs Used in Asthma
 Nitric Oxide (INOmax) Inhalation: 100, 800 ppm gas Katzung PHARMACOLOGY, 9e > Section IV. Drugs with Important Actions on Smooth Muscle > Chapter 19. Nitric Oxide, Donors, & Inhibitors > Chapter 20. Drugs
Nitric Oxide (INOmax) Inhalation: 100, 800 ppm gas Katzung PHARMACOLOGY, 9e > Section IV. Drugs with Important Actions on Smooth Muscle > Chapter 19. Nitric Oxide, Donors, & Inhibitors > Chapter 20. Drugs
Disclosures. Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
 Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
Treatment of Asthma. Talk to your doctor about the various medications available to treat asthma.
 Please call 911 if you think you have a medical emergency. Treatment of Asthma The goals of asthma therapy are to prevent your child from having chronic and troublesome symptoms, to maintain your child's
Please call 911 if you think you have a medical emergency. Treatment of Asthma The goals of asthma therapy are to prevent your child from having chronic and troublesome symptoms, to maintain your child's
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Pre-Operative Services Teaching Rounds 2 Jan 2011
 Pre-Operative Services Teaching Rounds 2 Jan 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Pre-Operative Services Teaching Rounds 2 Jan 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
O ρόλος της ακετυλοχολίνης στη σύσπαση και τον πολλαπλασιασµό των ΛΜΚ (του αναπνευστικού) Απ. Χατζηευθυµίου 2015
 O ρόλος της ακετυλοχολίνης στη σύσπαση και τον πολλαπλασιασµό των ΛΜΚ (του αναπνευστικού) Απ. Χατζηευθυµίου 2015 Σύσπαση ΛΜΙ An increase in free intracellular calcium can result from either increased flux
O ρόλος της ακετυλοχολίνης στη σύσπαση και τον πολλαπλασιασµό των ΛΜΚ (του αναπνευστικού) Απ. Χατζηευθυµίου 2015 Σύσπαση ΛΜΙ An increase in free intracellular calcium can result from either increased flux
Breathe Easy: Asthma and FMLA
 This article was published in the FMLA Policy, Practice, and Legal Update newsletter, by Business & Legal Reports, Inc. (BLR). BLR is a nationally recognized publisher of regulatory and legal compliance
This article was published in the FMLA Policy, Practice, and Legal Update newsletter, by Business & Legal Reports, Inc. (BLR). BLR is a nationally recognized publisher of regulatory and legal compliance
Management of Asthma
 Federal Bureau of Prisons Clinical Practice Guidelines May 2013 Clinical guidelines are made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does not warrant
Federal Bureau of Prisons Clinical Practice Guidelines May 2013 Clinical guidelines are made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does not warrant
Medicines Use Review Supporting Information for Asthma Patients
 Medicines Use Review Supporting Information for Asthma Patients What is asthma? Asthma is a chronic inflammatory disorder of the airways. The inflammation causes an associated increase in airway hyper-responsiveness,
Medicines Use Review Supporting Information for Asthma Patients What is asthma? Asthma is a chronic inflammatory disorder of the airways. The inflammation causes an associated increase in airway hyper-responsiveness,
InetCE 146-000-01-001-H01
 The National Asthma Education Prevention Program (NAEPP II) Guidelines for the Treatment of Asthma: Implications for the Pharmacist (Manuscript Updated December 2000) InetCE 146-000-01-001-H01 Theresa
The National Asthma Education Prevention Program (NAEPP II) Guidelines for the Treatment of Asthma: Implications for the Pharmacist (Manuscript Updated December 2000) InetCE 146-000-01-001-H01 Theresa
4 Pharmacological management
 4 Pharmacological management The aim of asthma management is control of the disease. Control of asthma is defined as: no daytime symptoms no night time awakening due to asthma no need for rescue medication
4 Pharmacological management The aim of asthma management is control of the disease. Control of asthma is defined as: no daytime symptoms no night time awakening due to asthma no need for rescue medication
COPD is a multicomponent disease that includes. Inhaled Combination Therapy With Long-Acting 2 -Agonists and Corticosteroids in Stable COPD*
 Inhaled Combination Therapy With Long-Acting 2 -Agonists and Corticosteroids in Stable COPD* Mario Cazzola, MD, FCCP; and Ronald Dahl, MD Long-acting 2 -agonists (LABAs) have been shown to be effective
Inhaled Combination Therapy With Long-Acting 2 -Agonists and Corticosteroids in Stable COPD* Mario Cazzola, MD, FCCP; and Ronald Dahl, MD Long-acting 2 -agonists (LABAs) have been shown to be effective
Actions of Hormones on Target Cells Page 1. Actions of Hormones on Target Cells Page 2. Goals/ What You Need to Know Goals What You Need to Know
 Actions of Hormones on Target Cells Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Actions of Hormones on Target Cells Hormones
Actions of Hormones on Target Cells Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Actions of Hormones on Target Cells Hormones
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
Understanding the immune response to bacterial infections
 Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Glucocorticoids, Inhaled Therapeutic Class Review (TCR) February 7, 2012
 Glucocorticoids, Inhaled Therapeutic Class Review (TCR) February 7, 2012 No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying,
Glucocorticoids, Inhaled Therapeutic Class Review (TCR) February 7, 2012 No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying,
BIOM 255 - Firestein, Winter 2009. Rheumatoid arthritis. Page 1
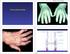 Rheumatoid arthritis Page 1 Vascular events in RA Synovium in rheumatoid arthritis Non-extra articular RA Extra articular RA Turesson, et al. Ann Rheum Dis. 2007;66:60 Normal Rheumatoid Arthritis Major
Rheumatoid arthritis Page 1 Vascular events in RA Synovium in rheumatoid arthritis Non-extra articular RA Extra articular RA Turesson, et al. Ann Rheum Dis. 2007;66:60 Normal Rheumatoid Arthritis Major
COPD PROTOCOL CELLO. Leiden
 COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
Guideline on the clinical investigation of medicinal products for the treatment of asthma
 22 October 2015 CHMP/EWP/2922/01 Rev.1 Committee for Medicinal Products for Human Use (CHMP) Guideline on the clinical investigation of medicinal products for the treatment of Draft Agreed by Respiratory
22 October 2015 CHMP/EWP/2922/01 Rev.1 Committee for Medicinal Products for Human Use (CHMP) Guideline on the clinical investigation of medicinal products for the treatment of Draft Agreed by Respiratory
The Most Common Autoimmune Disease: Rheumatoid Arthritis. Bonita S. Libman, M.D.
 The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
Medications for Managing COPD in Hospice Patients. Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources
 Medications for Managing COPD in Hospice Patients Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources Goal of medications in COPD Decrease symptoms and/or complications Reduce frequency
Medications for Managing COPD in Hospice Patients Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources Goal of medications in COPD Decrease symptoms and/or complications Reduce frequency
Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007
 Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007 The cardiometabolic risk syndrome is increasingly recognized
Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007 The cardiometabolic risk syndrome is increasingly recognized
Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age
 Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age Components of Severity Symptoms Intermittent 2 days/week Classification of Asthma Severity (0 4 years of age) Persistent
Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age Components of Severity Symptoms Intermittent 2 days/week Classification of Asthma Severity (0 4 years of age) Persistent
1. The potential sites of action for sympathomimetics and the difference between a direct and indirect acting agonist.
 1 OBI 836 The Autonomic Nervous System-Sympathomimetics M.T. Piascik August 29, 2012 Learning Objectives Lecture II The student should be able to explain or describe 1. The potential sites of action for
1 OBI 836 The Autonomic Nervous System-Sympathomimetics M.T. Piascik August 29, 2012 Learning Objectives Lecture II The student should be able to explain or describe 1. The potential sites of action for
Rheumatoid arthritis: an overview. Christine Pham MD
 Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines.
 Formulary Guidance for Management of COPD patients Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines. For inhaler
Formulary Guidance for Management of COPD patients Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines. For inhaler
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
RES/006/APR16/AR. Speaker : Dr. Pither Sandy Tulak SpP
 RES/006/APR16/AR Speaker : Dr. Pither Sandy Tulak SpP Definition of Asthma (GINA 2015) Asthma is a common and potentially serious chronic disease that imposes a substantial burden on patients, their families
RES/006/APR16/AR Speaker : Dr. Pither Sandy Tulak SpP Definition of Asthma (GINA 2015) Asthma is a common and potentially serious chronic disease that imposes a substantial burden on patients, their families
Tests. Pulmonary Functions
 Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Summary and conclusion 2013
 The work presented in the thesis is focused on the problems related to the prostate gland. Benign prostatic hyperplasia (BPH) and prostate cancer (PCa) are the two major problems associated with prostate.
The work presented in the thesis is focused on the problems related to the prostate gland. Benign prostatic hyperplasia (BPH) and prostate cancer (PCa) are the two major problems associated with prostate.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
Nursing 113. Pharmacology Principles
 Nursing 113 Pharmacology Principles 1. The study of how drugs enter the body, reach the site of action, and are removed from the body is called a. pharmacotherapeutics b. pharmacology c. pharmacodynamics
Nursing 113 Pharmacology Principles 1. The study of how drugs enter the body, reach the site of action, and are removed from the body is called a. pharmacotherapeutics b. pharmacology c. pharmacodynamics
HUNTINGTON S DISEASE THERAPIES RESEARCH UPDATE
 HUNTINGTON S DISEASE MULTIDISCIPLINARY CLINIC HUNTINGTON S DISEASE THERAPIES RESEARCH UPDATE From gene to treatments The gene that causes Huntington s disease (HD) was discovered in 1993. Since then, enormous
HUNTINGTON S DISEASE MULTIDISCIPLINARY CLINIC HUNTINGTON S DISEASE THERAPIES RESEARCH UPDATE From gene to treatments The gene that causes Huntington s disease (HD) was discovered in 1993. Since then, enormous
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
INTERNATIONAL CONFERENCE ON HARMONISATION OF TECHNICAL REQUIREMENTS FOR REGISTRATION OF PHARMACEUTICALS FOR HUMAN USE S1A. Current Step 4 version
 INTERNATIONAL CONFERENCE ON HARMONISATION OF TECHNICAL REQUIREMENTS FOR REGISTRATION OF PHARMACEUTICALS FOR HUMAN USE ICH HARMONISED TRIPARTITE GUIDELINE GUIDELINE ON THE NEED FOR CARCINOGENICITY STUDIES
INTERNATIONAL CONFERENCE ON HARMONISATION OF TECHNICAL REQUIREMENTS FOR REGISTRATION OF PHARMACEUTICALS FOR HUMAN USE ICH HARMONISED TRIPARTITE GUIDELINE GUIDELINE ON THE NEED FOR CARCINOGENICITY STUDIES
Bronchodilators in COPD
 TSANZSRS Gold Coast 2015 Can average outcomes in COPD clinical trials guide treatment strategies? Long live the FEV1? Christine McDonald Dept of Respiratory and Sleep Medicine Austin Health Institute for
TSANZSRS Gold Coast 2015 Can average outcomes in COPD clinical trials guide treatment strategies? Long live the FEV1? Christine McDonald Dept of Respiratory and Sleep Medicine Austin Health Institute for
Future strategies for myeloma: An overview of novel treatments In development
 Future strategies for myeloma: An overview of novel treatments In development Dr. Matthew Streetly Guys and St. Thomas NHS Trust How far have we come? Melphalan and prednisolone VAD Autologous SCT Thalidomide
Future strategies for myeloma: An overview of novel treatments In development Dr. Matthew Streetly Guys and St. Thomas NHS Trust How far have we come? Melphalan and prednisolone VAD Autologous SCT Thalidomide
Doncaster & Bassetlaw Medicines Formulary
 Doncaster & Bassetlaw Medicines Formulary Section 3.2: Corticosteroids Beclometasone 50, 100 and 250micrograms/dose Clickhaler Clenil Modulite (Beclometasone CFC free) 50, 100, and 250micrograms/dose MDI
Doncaster & Bassetlaw Medicines Formulary Section 3.2: Corticosteroids Beclometasone 50, 100 and 250micrograms/dose Clickhaler Clenil Modulite (Beclometasone CFC free) 50, 100, and 250micrograms/dose MDI
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD)
 Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Longitudinal Modeling of Lung Function in Respiratory Drug Development
 Longitudinal Modeling of Lung Function in Respiratory Drug Development Fredrik Öhrn, PhD Senior Clinical Pharmacometrician Quantitative Clinical Pharmacology AstraZeneca R&D Mölndal, Sweden Outline A brief
Longitudinal Modeling of Lung Function in Respiratory Drug Development Fredrik Öhrn, PhD Senior Clinical Pharmacometrician Quantitative Clinical Pharmacology AstraZeneca R&D Mölndal, Sweden Outline A brief
Basics of Immunology
 Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
ICH Topic S 1 A The Need for Carcinogenicity Studies of Pharmaceuticals. Step 5
 European Medicines Agency July 1996 CPMP/ICH/140/95 ICH Topic S 1 A The Need for Carcinogenicity Studies of Pharmaceuticals Step 5 NOTE FOR GUIDANCE ON THE NEED FOR CARCINOGENICITY STUDIES OF PHARMACEUTICALS
European Medicines Agency July 1996 CPMP/ICH/140/95 ICH Topic S 1 A The Need for Carcinogenicity Studies of Pharmaceuticals Step 5 NOTE FOR GUIDANCE ON THE NEED FOR CARCINOGENICITY STUDIES OF PHARMACEUTICALS
Drug Development Services
 Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Corticosteroid Resistance in Airway Disease
 Corticosteroid Resistance in Airway Disease Peter J. Barnes National Heart and Lung Institute, Imperial College, London, United Kingdom Resistance to the antiinflammatory effects of corticosteroids is
Corticosteroid Resistance in Airway Disease Peter J. Barnes National Heart and Lung Institute, Imperial College, London, United Kingdom Resistance to the antiinflammatory effects of corticosteroids is
ASTHMA< Observation about treatment and education of patients in San Pablo Clinic, Heredia Costa Rica
 ASTHMA< Observation about treatment and education of patients in San Pablo Clinic, Heredia Costa Rica Rachel Borovina, MSIV Lisa Troeger, MSIV University of California San Francisco IHCAI FOUNDATION 2001
ASTHMA< Observation about treatment and education of patients in San Pablo Clinic, Heredia Costa Rica Rachel Borovina, MSIV Lisa Troeger, MSIV University of California San Francisco IHCAI FOUNDATION 2001
Note for guidance on clinical investigation of medicinal products for treatment of asthma
 1 2 3 27 June 2013 CHMP/EWP/2922/01 Rev.1 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 Note for guidance on clinical investigation of medicinal products for treatment of asthma Draft Draft
1 2 3 27 June 2013 CHMP/EWP/2922/01 Rev.1 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 Note for guidance on clinical investigation of medicinal products for treatment of asthma Draft Draft
HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES JASON CYSTER SECTION 13
 SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
Version 1 2015. Module guide. Preliminary document. International Master Program Cardiovascular Science University of Göttingen
 Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Inflammatory cells in asthma: Mechanisms and implications for therapy
 Inflammatory cells in asthma: Mechanisms and implications for therapy Qutayba Hamid, MD, PhD, a Meri K. Tulic, PhD, a Mark C. Liu, MD, b and Redwan Moqbel, PhD c Montreal, Quebec, Canada, Baltimore, Md,
Inflammatory cells in asthma: Mechanisms and implications for therapy Qutayba Hamid, MD, PhD, a Meri K. Tulic, PhD, a Mark C. Liu, MD, b and Redwan Moqbel, PhD c Montreal, Quebec, Canada, Baltimore, Md,
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY
 GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
Adrenergic receptors lec 9, part 2. 16/10/2014 Dr. Laila M. Matalqah Rama Kamal Ali Treany
 Adrenergic receptors lec 9, part 2 16/10/2014 Dr. Laila M. Matalqah Rama Kamal Ali Treany Pharmacology of ANS Adrenergic Agonists Adrenergic receptors:- - It is a receptor which is located in the peripheral
Adrenergic receptors lec 9, part 2 16/10/2014 Dr. Laila M. Matalqah Rama Kamal Ali Treany Pharmacology of ANS Adrenergic Agonists Adrenergic receptors:- - It is a receptor which is located in the peripheral
PHYSIOLOGY IN MEDICINE: A SERIES OF ARTICLES LINKING MEDICINE WITH SCIENCE
 PHYSIOLOGY IN MEDICINE: A SERIES OF ARTICLES LINKING MEDICINE WITH SCIENCE Physiology in Medicine Dennis A. Ausiello, MD, Editor; Dale J. Benos, PhD, Deputy Editor; Francois Abboud, MD, Associate Editor;
PHYSIOLOGY IN MEDICINE: A SERIES OF ARTICLES LINKING MEDICINE WITH SCIENCE Physiology in Medicine Dennis A. Ausiello, MD, Editor; Dale J. Benos, PhD, Deputy Editor; Francois Abboud, MD, Associate Editor;
Dear Provider: Sincerely,
 Asthma Toolkit Dear Provider: L.A. Care is pleased to present this updated asthma toolkit. Our goal is to promote the highest level of asthma care, based on the 2007 National Asthma Education and Prevention
Asthma Toolkit Dear Provider: L.A. Care is pleased to present this updated asthma toolkit. Our goal is to promote the highest level of asthma care, based on the 2007 National Asthma Education and Prevention
RELAPSE MANAGEMENT. Pauline Shaw MS Nurse Specialist 25 th June 2010
 RELAPSE MANAGEMENT Pauline Shaw MS Nurse Specialist 25 th June 2010 AIMS OF SESSION Relapsing/Remitting MS Definition of relapse/relapse rate Relapse Management NICE Guidelines Regional Clinical Guidelines
RELAPSE MANAGEMENT Pauline Shaw MS Nurse Specialist 25 th June 2010 AIMS OF SESSION Relapsing/Remitting MS Definition of relapse/relapse rate Relapse Management NICE Guidelines Regional Clinical Guidelines
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal. Drugs for the treatment of pulmonary arterial hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
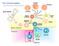 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
POCKET GUIDE FOR ASTHMA MANAGEMENT AND PREVENTION
 POCKET GUIDE FOR ASTHMA MANAGEMENT AND PREVENTION (for Adults and Children Older than 5 Years) A Pocket Guide for Physicians and Nurses Updated 2015 BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND
POCKET GUIDE FOR ASTHMA MANAGEMENT AND PREVENTION (for Adults and Children Older than 5 Years) A Pocket Guide for Physicians and Nurses Updated 2015 BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND
