CMS does not have a National Coverage Determination for transarterial chemoembolization for primary liver cancer.
|
|
|
- Cleopatra Norman
- 8 years ago
- Views:
Transcription
1 Subject: Transarterial Chemoembolization (TACE) for Primary Liver Hepatocellular Carcinoma (HCC) Guidance Number: MCG-120 Revision Date(s): Original Effective Date: 10/31/2012 Medical Coverage Guidance Approval Date: 10/31/2012 PREFACE This Medical Guidance is intended to facilitate the Utilization Management process. It expresses Molina's determination as to whether certain services or supplies are medically necessary, experimental, investigational, or cosmetic for purposes of determining appropriateness of payment. The conclusion that a particular service or supply is medically necessary does not constitute a representation or warranty that this service or supply is covered (i.e., will be paid for by Molina) for a parti cular member. The member's benefit plan determines coverage. Each benefit plan defines which services are covered, which are excluded, and which are subject to dollar caps or other limits. Members and their providers will need to consult the member's benefit plan to determine if there are any exclusions or other benefit limitations applicable to this service or supply. If there is a discrepancy between this policy and a member's plan of benefits, the benefits plan will govern. In addition, coverage may be mandated by applicable legal requirements of a State, the Federal government or CMS for Medicare and Medicaid members. CMS's Coverage Database can be found on the following website: FDA INDICATIONS Transarterial chemoembolization is a procedure not subject to FDA regulation. CENTERS FOR MEDICARE AND MEDICAID SERVICES (CMS) The coverage directive(s) and criteria from an existing National Coverage Determination (NCD) or Local Coverage Determination (LCD) will supersede the contents of this Molina medical coverage guidance (MCG) document and provide the directive for all Medicare members. The directives from this MCG document may be followed if there are no available NCD or LCD documents available and outlined below. CMS does not have a National Coverage Determination for transarterial chemoembolization for primary liver cancer. INITIAL COVERAGE CRITERIA 1. Transarterial chemoembolization (TACE) is indicated for the treatment of primary hepatocellular liver carcinoma (HCC) when ALL of the following criteria are met 4 : Localized unresectable or multifocal tumor with all of the following: [ALL] o No vascular invasion o No extrahepatic spread o Tumor burden involving < 50 percent of the liver o Tumor size > 5 cm 3 21 No portal vein thrombus No encephalopathy Page 1 of 11
2 No biliary obstruction Serum bilirubin < 2 mg/dl Liver function preserved: [ANY] Child-Turcote-Pugh (CPT) score A (<7); OR Child-Turcote-Pugh (CPT) score B (7-9) * The Child-Turcote-Pugh (CPT) score determines short-term prognosis among groups of patients awaiting liver transplantation and has been widely adopted for risk-stratifying patients before transplantation. Child-Turcote-Pugh Score of Severity of Liver Disease 7 Points Encephalopathy None Ascites Absent Slight Moderate Bilirubin (mg/dl) < > 3 For PBC/PSC, < > 10 Bilirubin Albumin (g/dl) > < 2.8 INR* < > 2.3 PT (seconds prolonged) < > 6 The individual scores are summed and then grouped as a classification: < 7 = A 7-9 = B > 9 = C (forecasts a survival of less than 12 months) *INR = International Normalized Ratio; PT = prothrombin time. CONTINUATION OF THERAPY The TACE procedure may be repeated every 8-12 weeks if there is clear evidence of progressive tumor growth in the treated areas. 2 4 Note: Multiple courses of TACE, especially if spaced too closely together, can increase deaths from liver failure despite successful tumor shrinkage, and these excess deaths from deterioration of liver function may counterbalance any prolongation of survival that results from enhanced tumor control. TACE may cause hepatic artery damage, the likelihood of which is higher in patients with impaired liver function. Hepatic artery interruption by repeated TACE or arterial dissection also leads to the development of extrahepatic collateralization, which may create an alternative blood supply to the tumor, and contribute to treatment failure. 4 COVERAGE EXCLUSIONS TACE is contraindicated when any of the following clinical circumstances occur : Page 2 of 11
3 Thrombus in the main portal vein and portal vein obstruction Encephalopathy Biliary obstruction Child- Turcote-Pugh C cirrhosis Relative contraindications include any of the following : Serum bilirubin >2 mg/dl Lactate dehydrogenase >425 units/l Aspartate aminotransferase >100 units/l Tumor burden involving >50 percent of the liver Cardiac or renal insufficiency Ascites, recent variceal bleed, or significant thrombocytopenia Transjugular intrahepatic portosystemic shunt (TIPS) DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL Transarterial chemoembolization (TACE) is a procedure used to treat primary liver cancer that involves injection or infusion of a concentrated dose of antitumor or chemotherapeutic drugs into the hepatic artery or its branches followed by arterial embolization to block off or occlude the artery. Intra-arterial injection of antitumor drugs increases their local concentration and reduces systemic side effects, while intra-arterial embolization causes ischemic necrosis of the tumor, depriving it of nutrients and oxygen. The most commonly used chemotherapeutic drugs are doxorubicin, epirubicin, mitomycin, and cisplatin, either alone or in combination. Embolization is performed with gelatin sponge particles, or Gelfoam. Often lipiodol, or iodized poppy-seed oil (Lipiodol, Andre Guerbet, Aulnay-Sous-Bois, France; or Ethiodol, Savage Laboratories, Melville, NY), is added to the chemoembolization regimen, usually as an emulsion with the chemotherapeutic drugs, to enhance the antitumor effect of the drugs by prolonging their contact with tumor cells. The iodized oil, which is selectively deposited within the tumor, functions both as a carrier for the anticancer drugs, releasing the drugs gradually, and as an embolic material. The oil has the unique property of remaining within the tumor for several months after injection, whereas it disappears more rapidly from the nontumorous parenchyma. Chemoembolization is performed by an interventional radiologist and multiple treatments may be required to treat all lesions as well as recurrences. The treatment can be repeated every 8 to 12 weeks; however, the benefit of repetition of TACE needs to be balanced against the progressive liver damage associated with the treatment. 2 The most common adverse effect of TACE, which occurs in 60 to 80 percent of patients, is postembolization syndrome. This consists of varying degrees of right upper quadrant pain, nausea, a moderate degree of ileus, fatigue, fever, and transient elevation of AST, ALT and bilirubin values. Symptoms are usually self-limited, lasting three to four days; full recovery is typical within 7 to 10 days. 4 Hepatocellular Carcinoma General Information Page 3 of 11
4 The incidence of hepatocellular carcinoma (HCC), or primary liver cancer is increasing due to the spread of hepatitis virus infection. In the majority of patients, HCC is associated with cirrhosis of the liver, and survival rates for HCC are poor. Patients with primary liver cancer are broadly classified into those with localized resectable, localized unresectable and advanced disease. Surgery is the only potentially curative treatment but only in patients with localized resectable disease, where the tumor is confined to a solitary mass in a portion of the liver that allows its complete surgical removal with a margin of normal liver, and in the absence of cirrhosis and chronic hepatitis. In patients with localized unresectable disease, although the cancer appears to be confined to the liver, surgical resection of the entire tumor is not possible due to its location within the liver or the presence of concomitant medical conditions such as cirrhosis. While some of these patients may be candidates for liver transplantation, limited availability of donor livers remains a problem. In advanced liver cancer, the cancer is present in both lobes of the liver or has metastasized to distant sites. 2 For patients with localized unresectable HCC or multifocal HCC without extrahepatic metastases, transarterial chemoembolization (TACE) is one of several nonsurgical therapeutic approaches available; other approaches include percutaneous ethanol injection (PEI) and systemic chemotherapy. Chemoembolization involves injection of chemotherapeutic drugs and embolizing agents into the branch of the hepatic artery supplying the tumor. The goal of this procedure is to deliver the chemotherapeutic agents directly to the tumor, and then to block blood flow to the tumor, thereby reducing the size or growth rate of the tumor. 2 GENERAL INFORMATION Summary of Medical Evidence A meta-analysis by Wang and colleagues (2011) 19 to assess the evidence for improved outcomes in hepatocellular carcinoma (HCC) with transarterial chemoembolization (TACE) alone or with percutaneous ethanol injection (PEI) was done. Seven randomized trials were identified that included 623 patients. The results of the meta-analysis are as follows: the 6-month, 1-, 2-, and 3-year survival rates were significantly better in patients with the TACE+PEI group than TACE group; in the decline rates of the AFP level and the reduction rates of tumor size (>50%), the TACE+PEI group has better effects than TACE group; as adverse effects, TACE+PEI group has lower incidence rates than TACE group. In patients with HCC, the efficacy of TACE combined with PEI is significantly better than that of TACE alone. The authors concluded that although there is convincing evidence to confirm the results, large sample, multicenter, randomized, controlled trials need to be done to confirm these findings. Zhong and colleagues (2010) 17 performed a meta-analysis to evaluate the efficacy of postoperative adjuvant TACE for participants with HCC. Six RCT totaling 659 participants, of whom almost all were of stage IIIA HCC, were included. For the 1-year tumor recurrence rate, hepatectomy plus TACE showed statistically significant less incidence of recurrence, with a pooled risk ratio (RR) of For 1-year mortality, the trials were favorable for TACE with a pooled risk ratio of 0.48.For 3-year mortality, the trials also revealed statistically significant less incidence, with a pooled risk ratio of 0.76.However, for 5-year mortality, TACE did not demonstrate statistically significant less incidence. Transient fever and nausea/vomiting were reported as side-effects of TACE but were well tolerated by most participants. The authors concluded that postoperative Page 4 of 11
5 adjuvant TACE seems promising for participants with HCC with risk factors (multiple nodules of >5 vascular invasion) but requires further trial. cm or A systematic review of 18 studies including 3 randomized trials and 15 observational studies was completed by Chua et al. (2010) to identify published studies of TACE administered preoperatively as a neoadjuvant treatment for resectable HCC. This comprised of 3927 patients, of which, 1293 underwent neoadjuvant TACE. The median disease-free survival (DFS) in the TACE and non-tace group ranged from 10 to 46 and 8 to 52 months, respectively, with 67% of studies reporting similar DFS between groups despite higher extent of tumor necrosis from the resected specimens indicating a higher rate of pathological response (partial TACE 27-72% vs. non-tace 23-52%; complete TACE 0-28% vs. non-tace zero), with no difference in surgical morbidity and mortality outcome. No conclusion could be drawn with respect to overall survival (OS). Overall survival (OS), rate of pathological response, impact on surgical morbidity and mortality and pattern of recurrences were secondary endpoints of this review. Both randomized and non-randomized trials suggest the use of TACE preoperatively as a neoadjuvant treatment in resectable HCC is a safe and efficacious procedure with high rates of pathological responses. However, it does not appear to improve disease-free survival (DFS). 8 A systematic review by Llovet and colleagues (2003) 14 was done to assess the evidence of the impact of medical treatments for HCC on survival. Randomized controlled trials (RCTs) that were published as full papers assessing survival for primary treatments of HCC were included. The primary end point was survival, and the secondary end point was response to treatment. Estimates of effect were calculated according to the random effects model. Sensitivity analysis included methodological quality. 61 randomized trials were identified but only 14 met the criteria to perform a meta-analysis assessing arterial embolization (7 trials, 545 patients) or tamoxifen (7 trials, 898 patients). Arterial embolization improved 2-year survival compared with control (odds ratio [OR], 0.53; 95% confidence interval [CI], ; P =.017). Sensitivity analysis showed a significant benefit of chemoembolization with cisplatin or doxorubicin (OR, 0.42; 95% CI, ) but none with embolization alone (OR, 0.59; 95% CI, ). Overall, treatment induced objective responses in 35% of patients (range, 16%-61%). Tamoxifen showed no antitumoral effect and no survival benefits (OR, 0.64; 95% CI, ; P =.13), and only low-quality scale trials suggested 1-year improvement in survival. The authors concluded that chemoembolization improves survival of patients with unresectable HCC and may become the standard treatment. Treatment with tamoxifen does not modify the survival of patients with advanced disease. Marelli and colleagues (2007) 18 performed a systematic review of published cohort and randomized studies to evaluate whether specific patient characteristics and/or radiological transarterial techniques result in better outcomes. 175 articles were reviewed. Anticancer drugs were used as sole agent in 75% of cases (double 15% and triple 6%): doxorubicin (36%), cisplatin (31%), epirubicin (12%), mitoxantrone (8%), mitomycin (8%), and SMANCS (5%). Embolizing agents used were: gelatin sponge particles (71%), polyvinyl alcohol (PVA) particles (8%), degradable starch microspheres (DSM) (4%), and embospheres (4%). Sessions per patient were 2.5 +/- 1.5 (interval: 2 months). Objective response was 40 +/- 20%; survival rates at 1, 2, 3, and 5 years were: 62 +/- 20%, 42 +/- 17%, 30 +/- 15%, and 19 +/- 16%, respectively, and survival time was 18 +/- 9.5 months. Page 5 of 11
6 The post-tace complications were: acute liver failure, 7.5% (range 0-49%); acute renal failure, 1.8% (0-13%); encephalopathy, 1.8% (0-16%); ascites, 8.3% (0-52%); upper gastrointestinal bleeding; 3% (0-22%); and hepatic or splenic abscess, 1.3% (0-2.5%). Treatment-related mortality was 2.4% (0-9.5%), mainly due to acute liver failure. Our meta-analysis of nine randomized controlled trials (RCTs) confirmed that TACE improves survival; but a meta-analysis of TACE versus TAE alone (3 RCTs, 412 patients) demonstrated no survival difference. The authors concluded that no chemotherapeutic agent appears better than any other. There is no evidence for benefit with lipiodol. Gelatin sponge is the most used embolic agent, but PVA particles may be better. TAE appears as effective as TACE. New strategies to reduce the risk of post-tace complications are required. Takasu (2012) 10 reviewed the survival benefits of two randomized controlled trials for transcatheter arterial chemoembolization for patients with unresectable hepatocellular carcinoma. Chemoembolization accounted for initial treatment of 32% of patients and 58% for recurrent foci. The indications of chemoembolization are various: they are multinodular tumors in the Barcelona Clinic Liver Cancer staging system and two or three tumors >3 cm or four or more tumors in the Japanese guidelines, and both indications fulfill the Child-Pugh Class A/B or liver damage A/B and exclusion of vascular invasion or extrahepatic spread. Recently, both guidelines were identified to have almost similar content. The 4966 patients stratified to chemoembolization recommended by the Japanese guidelines showed that 3-year survival of patients with two or three tumors >3 cm or four or more tumors was 55 and 46% in Child-Pugh A, respectively, and 30 and 22% in Class B, respectively. Chemoembolization with drug-eluting beads and radioembolization with yttrium-90 microspheres have been introduced, and each of them showed similar tumor response and median survival compared with conventional chemoembolization. Morimoto and colleagues (2010) 16 randomly compared the efficacy of radiofrequency ablation (RFA) combined with transcatheter arterial chemoembolization (TACE) to RFA alone, for the treatment of intermediate-sized hepatocellular carcinomas (HCCs). The authors randomly assigned 37 patients with solitary HCCs (diameter, cm in the greatest dimension) to 2 groups: the TACE-RFA group, in which the patients received TACE followed by RFA on the same day, and the RFA group, in which the patients received only RFA. Technical success was achieved after 1.4±0.5 RFA sessions in the RFA group and after 1.1±0.2 RFA sessions in the TACE-RFA group (P<.01). The mean diameters of the longer and shorter axes of the RFAinduced ablated areas were 50±8.0 mm and 41±7.1 mm, respectively, in the RFA group and 58±13.2 mm and 50±11.3 mm, respectively, in the TACE-RFA group; the mean diameters of the shorter axes were significantly different (P=.012). The rates of local tumor progression at the end of the third year in the RFA and TACE-RFA groups were 39% and 6%, respectively (P=.012). The 3-year survival rates of the patients in the RFA and TACE-RFA groups were 80% and 93%, respectively (P=.369). The authors concluded that in patients with intermediate-sized HCCs, RFA combined with TACE is more effective than RFA alone for extending the ablated area in fewer treatment sessions and for decreasing the local tumor progression rate. Page 6 of 11
7 Hayes, Cochrane, UpToDate, MD Consult etc. A Cochrane review (2011) 9 was published to assess the beneficial and harmful effects of transarterial chemoembolization (TACE) or transarterial embolization (TAE). Nine trials with 645 participants were included. Six trials assessed TACE versus control and three trials assessed TAE versus control. Seven trials had low risk of selection bias based on adequate generation of allocation sequence and concealment - but all these trials had other risks of bias. Three trials were stopped early due to interim inspections and one due to slow accrual. For all-cause mortality, statistical heterogeneity between trials was low to moderate (I2= 30%). Metaanalysis of trials with low risk of selection bias showed that TACE or TAE versus control does not significantly increase survival. Two trials with low risk of selection bias, no early stopping, and no co-intervention did not establish any significant effect of TACE or TAE on overall survival. Trial sequential analysis confirmed the absence of evidence for a beneficial effect of TACE or TAE on survival indicating the need for future randomization of up to 383 additional participants. Substantial differences in criteria for assessing tumor response did not allow quantitative analyses. One trial investigated quality of life but did not detect any significant differences between the intervention groups. A range of adverse events including post-embolization syndrome and serious complications were reported. The conclusions were that firm evidence to support or refute TACE or TAE for patients with unresectable HCC cannot be made until additional bias protected trials are completed. UpToDate: Curley and colleagues 4 summarize that arterial embolization is a reasonable option for patients with an unresectable HCC that is either too large or multifocal for percutaneous ablation techniques such as RFA, with relatively preserved liver function (Child-Pugh A/B, and no extrahepatic tumor spread, vascular invasion, or main portal vein thrombus). TACE rather than bland embolization alone is recommended in guidelines from the American Association for the Study of Liver Disease (AASLD), and from an expert consensus group of the American Hepato-Pancreato-Biliary Association (weak evidence). Guidelines from the National Comprehensive Cancer Network (NCCN) recommend chemoembolization, bland embolization, or radioembolization in this setting. Doxorubicin as a single agent at a fixed dose is recommended for the procedure, although other centers add mitomycin and/or cisplatin; there is no evidence that either approach is better. Where available, DEBs may be preferred, although long-term outcomes using this technique are not available. Patient selection is critical to the success and safety of TACE. The best candidates for TACE are patients with unresectable lesions without vascular invasion or extrahepatic spread, and preserved liver function (i.e., Child-Pugh A or B cirrhosis). TACE is not recommended prior to a planned HCC resection. While it is commonly used as a bridging maneuver in patients awaiting liver transplantation, data proving benefit in this setting are lacking. Hayes Page 7 of 11
8 There is a Directory report called Chemoembolization for Primary Liver Cancer that was last updated in 2007 and archived in Professional Organizations American College of Radiology (ACR) 21 : The 2011 Appropriateness Criteria : radiologic management of hepatic malignancy recommends that transarterial chemoembolization is usually appropriate for patients who have: hepatocellular solitary tumors that are > 5cm more than one tumor with at least one > 5cm American Society for the Study of Liver Disease (AASLD): The AASLD Practice Guideline Management of Hepatocellular Carcinoma: An Update indicates that TACE is recommended as first line non-curative therapy for non-surgical patients with large/ multifocal HCC who do not have vascular invasion or extrahepatic spread. The AASLD notes that the development of polyvinyl chloride spheres that release chemotherapy after being injected (DEBs) have allowed a reduction of the side effects of the passage of chemotherapy into systemic circulation. 6 Cardiovascular and Interventional Radiological Society of Europe 11 (CIRSE) 2012: The CIRSE guidelines for hepatic transarterial chemoembolization indicate that for unresectable intermediate-stage HCC (BCLC stage B or Child-Pugh class A/B with large or multifocal HCC, no vascular invasion, or extrahepatic spread), the current standard treatment is TACE. General exclusion criteria for TACE based on laboratory assays have not been definitively established even though a bilirubin level >2 mg/dl, a lactate dehydrogenase level >425 mg/dl, and an aspartate aminotransferase (AST) level >100 IU/L have been reported to be strongly associated with increased post procedural mortality. In general, Child-Pugh class C is considered a contraindication for TACE. Indications for TACE in patients with HCC include all of the following: Tumor status: No extrahepatic localizations No main PV thrombosis Tumor involvement >50 % of the liver parenchyma Patients with HCC not suitable for curative treatments such as resection, liver transplantation, or percutaneous ablation according to BCLC staging classification and treatment schedule Patient performance status: Eastern Cooperative Oncology Group performance status < 3 or Karnofsky score > 70 Patient metabolic status Patients with well-preserved liver function (Child-Pugh class A/B) without encephalopathy and mild or severe ascites Serum creatinine <2 mg/dl (177 lmol/l) Platelet count >50,000/mm3 Prothrombin activity > 50 % Page 8 of 11
9 National Comprehensive Cancer Network (NCCN) : The 2012 NCCN guidelines for hepatocellular carcinoma indicate that all tumors may be amendable to embolization (chemo, bland or radio) provided that the arterial blood supply may be isolated without non-target embolization. Chemoembolization is contraindicated in patients with bilirubin > 3mg/dL and in cases of main portal vein thrombosis and Child-Pugh Class C. Unresectable or inoperable tumors > 5cm should be considered for treatment using embolic approaches or systemic therapy. Society of Interventional Radiology 20 : The 2009 position statement on chemoembolization of hepatic malignancies suggests that hepatic arterial chemoembolization is a safe, proven, and effective technique for the treatment of a number of malignancies, including hepatocellular carcinoma (HCC), neuroendocrine tumors, ocular melanoma, cholangiocarcinoma, and sarcoma. Furthermore, it has a palliative role for patients with colon carcinoma and may be useful with patients who have hepatic-dominant metastatic disease from other primary malignancies. However, the benefit of chemoembolization for these individuals should be evaluated on a caseby-case basis. CODING INFORMATION CPT Description Transcatheter occlusion or embolization (e.g., for tumor destruction, to achieve hemostasis, to occlude a vascular malformation), percutaneous, any method, non-central nervous system, non-head or neck Transcatheter therapy, embolization, any method, radiological supervision and interpretation HCPCS Description N/A ICD-9 Description Malignant neoplasm of liver, primary Malignant neoplasm of liver, not specified as primary or secondary Secondary malignant neoplasm of respiratory and digestive systems; liver, specified as secondary ICD-10 Description C22.0 Carcinoma malignant, hepatocellular Page 9 of 11
10 RESOURCE REFERENCES 1. Centers for Medicaid & Medicare Services (CMS). Search for National Coverage Determination (NCD) Accessed at: 2. Hayes Medical Technology Directory. Chemoembolization for Primary Liver Cancer. Winifred Hayes, Inc. Lansdale PA. July 2002, last updated April Archived Jan National Comprehensive Cancer Network (NCCN). NCCN Clinical Guidelines in Oncology. Clinical practice guidelines in oncology. Hepatobiliary Cancers. Version V UpToDate. Curley SA, Stuart KE, Schwartz JM. Nonsurgical therapies for localized hepatocellular carcinoma: Transarterial embolization, radiotherapy, and radioembolization. Aug 30, DynaMed. [Internet]. Ipswich (MA): EBSCO Publishing Hepatacellular Carcinoma. Updated June 27, Bruix J, Sherman M. American Association for the Study of Liver Diseases (AASLD) guideline on management of hepatocellular carcinoma: an update. HEPATOLOGY, Vol. 53, No. 3, Accessed at: te2010.pdf 7. American Association for the Study of Liver Disease (AASLD) Clinical Practice Guidelines. Evaluation of the patient for liver transplantation. Hepatology. 2005, June. Re-reviewed Accessed at: nsplant.pdf 8. Chua TC, Liauw W, Saxena A, Chu F, Glenn D, Chai A, Morris DL. Systematic review of neoadjuvant transarterial chemoembolization for resectable hepatocellular carcinoma. Liver International 2010; 30(2): Accessed at: 9. Oliveri RS, Wetterslev J, Gluud C. Transarterial (chemo)embolisation for unresectable hepatocellular carcinoma. Cochrane Database of Systematic Reviews 2011, Issue 3. Art. No.: CD DOI: / CD pub2 10. Takayasu K. Transarterial chemoembolization for hepatocellular carcinoma over three decades: current progress and perspective. Jpn J Clin Oncol Apr;42(4): Epub 2012 Mar 9. Accessed at: Basile A, Carrafiello G et al. Cardiovascular and Interventional Radiological Society of Europe (CIRSE) Standards of Practice Guidelines Quality Improvement Guidelines for Hepatic Transarterial Chemoembolization. Cardiovasc Intervent Radiol. 8 May Accessed at: Improvement%20Guidelines%20for%20Hepatic%20Transarterial%20Chemoembolization.pdf 12. MD Consult [website]: Hepatocellular Carcinoma. April 15, Llovet J, Real M, Montanya X, et al: Arterial embolization, chemoembolization versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: A randomized controlled trial. Lancet 2002; 359: Llovet J, Bruix J: Systematic review of randomized trials for unresectable hepatocellular carcinoma: Chemoembolization improves survival. Hepatology 2003; 37: Lo CM, Ngan H, Tso WK, et al: Randomized controlled trial of transarterial lipiodol chemoembolization for unresectable hepatocellular carcinoma. Hepatology 2002; 35: Morimoto M, Numata K, Kondou M, et al. Midterm outcomes in patients with intermediate-sized hepatocellular carcinoma: a randomized controlled trial for determining the efficacy of radiofrequency Page 10 of 11
11 ablation combined with transcatheter arterial chemoembolization. Cancer Dec 1;116(23): doi: /cncr Epub 2010 Jul Zhong JH, Li LQ. Postoperative adjuvant transarterial chemoembolization for participants with hepatocellular carcinoma: A meta-analysis. Hepatol Res. 2010;40(10): Marelli L, Stigliano R, Triantos C, et al. Transarterial therapy for hepatocellular carcinoma: Which technique is more effective? A systematic review of cohort and randomized studies. Cardiovasc Intervent Radiol. 2007;30(1):6-25. Accessed at: Wang N, Guan Q et al. TACE combined with PEI versus TACE alone in the treatment of HCC: a metaanalysis. Med Oncol Dec;28(4): Epub 2010 Jul Brown DB, Geschwind JF, Soulen MC, Millward SF, Sacks D. Society of Interventional Radiology position statement on chemoembolization of hepatic malignancies. J Vasc Interv Radiol 2009 Jul;20(7 Suppl):S Accessed at: Kouri BE, Funaki BS, Ray CE Jr, Abou-Alfa G, Burke CT et al. Expert Panel on Interventional Radiology. ACR Appropriateness Criteria radiologic management of hepatic malignancy. [online publication]. Reston (VA): American College of Radiology (ACR); Acessed at: Page 11 of 11
Hepatocellular Carcinoma Management Guidelines
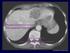 Hepatocellular Carcinoma Management Guidelines By Ashraf Omar M.D, Prof. of Hepatology & Tropical Medicine Cairo University Staging Strategy and Treatment for Patients With HCC HCC PST 0, Child-Pugh A
Hepatocellular Carcinoma Management Guidelines By Ashraf Omar M.D, Prof. of Hepatology & Tropical Medicine Cairo University Staging Strategy and Treatment for Patients With HCC HCC PST 0, Child-Pugh A
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Hepatocellular Carcinoma (HCC)
 Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
Hepatocellular Carcinoma Treatment Decision Tree
 Treatment Decision Tree Derek DuBay, MD Assistant Professor of Surgery Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery 1 UAB Liver Tumor Clinic Referrals: 205 996 5970 (phone) 205
Treatment Decision Tree Derek DuBay, MD Assistant Professor of Surgery Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery 1 UAB Liver Tumor Clinic Referrals: 205 996 5970 (phone) 205
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL HEPATOCELLULAR CARCINOMA GI Site Group Hepatocellular Carcinoma Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL HEPATOCELLULAR CARCINOMA GI Site Group Hepatocellular Carcinoma Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION
Treatment of Hepatic Neoplasm
 I. Policy University Health Alliance (UHA) will reimburse for treatment of hepatic neoplasm outside of systemic chemotherapy alone when determined to be medically necessary and within the medical criteria
I. Policy University Health Alliance (UHA) will reimburse for treatment of hepatic neoplasm outside of systemic chemotherapy alone when determined to be medically necessary and within the medical criteria
HEPATOCELLULAR CARCINOMA (HCC) RESECTION VERSUS TRANSPLANTATION. Francis Yao, M.D.
 UCSF TRANSPLANT CONFERENCE - 9/28/2012 HEPATOCELLULAR CARCINOMA (HCC) RESECTION VERSUS TRANSPLANTATION Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation
UCSF TRANSPLANT CONFERENCE - 9/28/2012 HEPATOCELLULAR CARCINOMA (HCC) RESECTION VERSUS TRANSPLANTATION Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation
SBRT (Elekta), 45 Gy in fractions of 3 Gy 3x/week for 5 weeks (N=22) vs.
 Uitgangsvraag 6: Wat is de plaats van stereotactische radiotherapiebehandeling (SBRT) bij HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary
Uitgangsvraag 6: Wat is de plaats van stereotactische radiotherapiebehandeling (SBRT) bij HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary
Name of Policy: Locoregional Therapies for Hepatocellular Carcinoma and Metastatic Liver Carcinoma and Metastatic Carcinoid Tumors of the Liver
 Name of Policy: Locoregional Therapies for Hepatocellular Carcinoma and Metastatic Liver Carcinoma and Metastatic Carcinoid Tumors of the Liver Policy #: 070 Latest Review Date: September 2015 Category:
Name of Policy: Locoregional Therapies for Hepatocellular Carcinoma and Metastatic Liver Carcinoma and Metastatic Carcinoid Tumors of the Liver Policy #: 070 Latest Review Date: September 2015 Category:
Locoregional Treatment of Hepatocellular Carcinoma. Cory Johnston and Sung Cho HPB Surgery Fellows Providence Portland, Oregon
 Locoregional Treatment of Hepatocellular Carcinoma Cory Johnston and Sung Cho HPB Surgery Fellows Providence Portland, Oregon Hepatocellular Carcinoma The 3 rd most common cause of cancer- related death
Locoregional Treatment of Hepatocellular Carcinoma Cory Johnston and Sung Cho HPB Surgery Fellows Providence Portland, Oregon Hepatocellular Carcinoma The 3 rd most common cause of cancer- related death
New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma. Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma
 New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma Riccardo Lencioni Author s Affiliation: Division of Diagnostic
New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma Riccardo Lencioni Author s Affiliation: Division of Diagnostic
Hepatocellular Carcinoma
 Hepatocellular Carcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Walter Kocha, MD, FRCPC (Medical Oncologist) Approval Date: October 2006 This guideline is a statement of
Hepatocellular Carcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Walter Kocha, MD, FRCPC (Medical Oncologist) Approval Date: October 2006 This guideline is a statement of
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: microwave_tumor_ablation 12/2011 11/2015 11/2016 11/2015 Description of Procedure or Service Microwave ablation
After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH
 After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH Professor of Medicine Department of Gastroenterology Director, Viral Hepatitis Center University of California San Francisco
After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH Professor of Medicine Department of Gastroenterology Director, Viral Hepatitis Center University of California San Francisco
Clinical Practice Guidelines for Hepatocellular Carcinoma, List of Clinical Questions/Recommendations. Chapter. Grade. CQ No. 1 Interferon Therapy
 Clinical Practice Guidelines for Hepatocellular Carcinoma, List of Clinical Questions/Recommendations Chapter Chapter 1 Prevention Sectio n CQ No. 1 Interferon Therapy Clinical Question 1 Does interferon
Clinical Practice Guidelines for Hepatocellular Carcinoma, List of Clinical Questions/Recommendations Chapter Chapter 1 Prevention Sectio n CQ No. 1 Interferon Therapy Clinical Question 1 Does interferon
Yttrium-90 Radioembolization
 Yttrium-90 Radioembolization Yttrium-90 radioembolization is generally used as a palliative therapy for selected patients with unresectable tumors of the liver including: Metastatic tumors from colorectal
Yttrium-90 Radioembolization Yttrium-90 radioembolization is generally used as a palliative therapy for selected patients with unresectable tumors of the liver including: Metastatic tumors from colorectal
Hepatocellular Carcinoma: What the hepatologist wants to know
 Hepatocellular Carcinoma: What the hepatologist wants to know Hélène Castel, MD Liver Unit Hôpital St-Luc CHUM? CAR Annual Scientific Meeting Saturday, April 27 th 2013 Disclosure statement I do not have
Hepatocellular Carcinoma: What the hepatologist wants to know Hélène Castel, MD Liver Unit Hôpital St-Luc CHUM? CAR Annual Scientific Meeting Saturday, April 27 th 2013 Disclosure statement I do not have
Drug-Eluting Bead TACE with DC Bead [DEBDOX ] in the Treatment of Hepatocellular Carcinoma (HCC) Review of Published Clinical Data
![Drug-Eluting Bead TACE with DC Bead [DEBDOX ] in the Treatment of Hepatocellular Carcinoma (HCC) Review of Published Clinical Data Drug-Eluting Bead TACE with DC Bead [DEBDOX ] in the Treatment of Hepatocellular Carcinoma (HCC) Review of Published Clinical Data](/thumbs/40/20786672.jpg) Bio Clinical Review piece Frenette v31_layout 1 28/09/2010 10:55 Page 4 Drug-Eluting Bead TACE with DC Bead [DEBDOX ] in the Treatment of Hepatocellular Carcinoma (HCC) Review of Published Clinical Data
Bio Clinical Review piece Frenette v31_layout 1 28/09/2010 10:55 Page 4 Drug-Eluting Bead TACE with DC Bead [DEBDOX ] in the Treatment of Hepatocellular Carcinoma (HCC) Review of Published Clinical Data
Liver Transplantation for Hepatocellular Carcinoma. John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco
 Liver Transplantation for Hepatocellular Carcinoma John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco Hepatocellular Carcinoma HCC is the 5th most common
Liver Transplantation for Hepatocellular Carcinoma John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco Hepatocellular Carcinoma HCC is the 5th most common
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 6
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 6 Contents 6. Hepatocellular carcinoma 64 6.1. Introduction: 65 6.2.
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 6 Contents 6. Hepatocellular carcinoma 64 6.1. Introduction: 65 6.2.
NATURAL HISTORY OF HEPATOCELLULAR CARCINOMA AND EFFECTS OF TREATMENTS
 DOTTORATO DI RICERCA IN BIOPATOLOGIA XXIII CICLO NATURAL HISTORY OF HEPATOCELLULAR CARCINOMA AND EFFECTS OF TREATMENTS Ph. D. Candidate Dr. Giuseppe Cabibbo Tutor Prof. Antonio Craxì (MED 012) Coordinator
DOTTORATO DI RICERCA IN BIOPATOLOGIA XXIII CICLO NATURAL HISTORY OF HEPATOCELLULAR CARCINOMA AND EFFECTS OF TREATMENTS Ph. D. Candidate Dr. Giuseppe Cabibbo Tutor Prof. Antonio Craxì (MED 012) Coordinator
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
Management of Hepatocellular
 Clinician s Guide version 08-05-09 Management of Hepatocellular Carcinoma (HCC) U.S. Department of Veterans Affairs Veterans Health Administration VA Hepatitis C Resource Center Program & VA National Clinical
Clinician s Guide version 08-05-09 Management of Hepatocellular Carcinoma (HCC) U.S. Department of Veterans Affairs Veterans Health Administration VA Hepatitis C Resource Center Program & VA National Clinical
Clinical Policy Bulletin: Liver and Other Neoplasms - Treatment Approaches
 Liver and Other Neoplasms - Treatment Approaches Page 1 of 29 Clinical Policy Bulletin: Liver and Other Neoplasms - Treatment Approaches Number: 0268 (Replaces CPB 338) Policy I. Percutaneous Ethanol Injection
Liver and Other Neoplasms - Treatment Approaches Page 1 of 29 Clinical Policy Bulletin: Liver and Other Neoplasms - Treatment Approaches Number: 0268 (Replaces CPB 338) Policy I. Percutaneous Ethanol Injection
Machine learning of patient similarity: a case study on predicting survival in cancer patient after locoregional chemotherapy.
 Title Machine learning of patient similarity: a case study on predicting survival in cancer patient after locoregional chemotherapy Author(s) Chan, LWC; Chan, T; Cheng, LF; Mak, WS Citation The 2010 IEEE
Title Machine learning of patient similarity: a case study on predicting survival in cancer patient after locoregional chemotherapy Author(s) Chan, LWC; Chan, T; Cheng, LF; Mak, WS Citation The 2010 IEEE
Hepatocellular Carcinoma and Y-90 Radioembolization
 Hepatocellular Carcinoma and Y-90 Radioembolization Radhika S. Kumar, MD Faculty Advisors: Ravi Shridhar, MD PhD, Michael Montejo, MD, Bela Kis, MD and Ghassan El- Haddad, MD H.L. Moffitt Cancer Center
Hepatocellular Carcinoma and Y-90 Radioembolization Radhika S. Kumar, MD Faculty Advisors: Ravi Shridhar, MD PhD, Michael Montejo, MD, Bela Kis, MD and Ghassan El- Haddad, MD H.L. Moffitt Cancer Center
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Non-coronary Brachytherapy
 Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
LIVER TUMORS PROFF. S.FLORET
 LIVER TUMORS PROFF. S.FLORET NEOPLASM OF LIVER PRIMARY 1)BENIGN 2)MALIGNANT METASTATIC/SECONDARY LIVER Primary Liver Cancer the Second Killer among tumors high morbidity and mortality(20.40/100,000) etiology
LIVER TUMORS PROFF. S.FLORET NEOPLASM OF LIVER PRIMARY 1)BENIGN 2)MALIGNANT METASTATIC/SECONDARY LIVER Primary Liver Cancer the Second Killer among tumors high morbidity and mortality(20.40/100,000) etiology
Treatment Advances for Liver Cancer
 Treatment Advances for Liver Cancer Guest Expert: Wasif, MD Associate Professor of Medical Oncology Mario Strazzabosco, MD Professor of Internal Medicine, Digestive Diseases www.wnpr.org www.yalecancercenter.org
Treatment Advances for Liver Cancer Guest Expert: Wasif, MD Associate Professor of Medical Oncology Mario Strazzabosco, MD Professor of Internal Medicine, Digestive Diseases www.wnpr.org www.yalecancercenter.org
Hepatocellular Carcinoma: A Guide to Screening and Diagnosis
 February 2012 Hepatocellular Carcinoma: A Guide to Screening and Diagnosis Reid Merryman, Harvard Medical School Year III Agenda Hepatocellular carcinoma (HCC) introduction Index patient: clinical presentation
February 2012 Hepatocellular Carcinoma: A Guide to Screening and Diagnosis Reid Merryman, Harvard Medical School Year III Agenda Hepatocellular carcinoma (HCC) introduction Index patient: clinical presentation
Evaluation and Prognosis of Patients with Cirrhosis
 Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
Case Study in the Management of Patients with Hepatocellular Carcinoma
 Management of Patients with Viral Hepatitis, Paris, 2004 Case Study in the Management of Patients with Hepatocellular Carcinoma Eugene R. Schiff This 50-year-old married man with three children has a history
Management of Patients with Viral Hepatitis, Paris, 2004 Case Study in the Management of Patients with Hepatocellular Carcinoma Eugene R. Schiff This 50-year-old married man with three children has a history
NP/PA Clinical Hepatology Fellowship Summary of Year-Long Curriculum
 OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
Ching-Yao Yang, Yu-Wen Tien
 Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Radioembolization for Primary and Metastatic Tumors of the Liver. Original Policy Date
 MP 8.01.21 Radioembolization for Primary and Metastatic Tumors of the Liver Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
MP 8.01.21 Radioembolization for Primary and Metastatic Tumors of the Liver Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
Comparative Effectiveness Review Number 114. Local Therapies for Unresectable Primary Hepatocellular Carcinoma
 Comparative Effectiveness Review Number 114 Local Therapies for Unresectable Primary Hepatocellular Carcinoma Comparative Effectiveness Review Number 114 Local Therapies for Unresectable Primary Hepatocellular
Comparative Effectiveness Review Number 114 Local Therapies for Unresectable Primary Hepatocellular Carcinoma Comparative Effectiveness Review Number 114 Local Therapies for Unresectable Primary Hepatocellular
What is liver cancer?
 Liver Cancer What is liver cancer? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines LIVER CANCER: A GUIDE FOR PATIENTS
Liver Cancer What is liver cancer? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines LIVER CANCER: A GUIDE FOR PATIENTS
Quality-Improvement Guidelines for Hepatic Transarterial Chemoembolization
 Cardiovasc Intervent Radiol DOI 10.1007/s00270-012-0423-z CIRSE STANDARDS OF PRACTICE GUIDELINES Quality-Improvement Guidelines for Hepatic Transarterial Chemoembolization Antonio Basile Gianpaolo Carrafiello
Cardiovasc Intervent Radiol DOI 10.1007/s00270-012-0423-z CIRSE STANDARDS OF PRACTICE GUIDELINES Quality-Improvement Guidelines for Hepatic Transarterial Chemoembolization Antonio Basile Gianpaolo Carrafiello
Selection Criteria for Hepatectomy in Patients with Hepatocellular Carcinoma and Portal Vein Tumor Thrombus
 ANNALS OF SURGERY Vol. 233, No. 3, 379 384 2001 Lippincott Williams & Wilkins, Inc. Selection Criteria for Hepatectomy in Patients with Hepatocellular Carcinoma and Portal Vein Tumor Thrombus Masami Minagawa,
ANNALS OF SURGERY Vol. 233, No. 3, 379 384 2001 Lippincott Williams & Wilkins, Inc. Selection Criteria for Hepatectomy in Patients with Hepatocellular Carcinoma and Portal Vein Tumor Thrombus Masami Minagawa,
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Diagnosis, staging and treatment of hepatocellular carcinoma
 Brazilian Hepatocellular Journal carcinoma of Medical and Biological Research (2004) 37: 1689-1705 ISSN 0100-879X Review 1689 Diagnosis, staging and treatment of hepatocellular carcinoma A.V.C. França
Brazilian Hepatocellular Journal carcinoma of Medical and Biological Research (2004) 37: 1689-1705 ISSN 0100-879X Review 1689 Diagnosis, staging and treatment of hepatocellular carcinoma A.V.C. França
The State of the Liver in the Adult Patient after Fontan Palliation
 The State of the Liver in the Adult Patient after Fontan Palliation Fred Wu, M.D. Boston Adult Congenital Heart Service Boston Children s Hospital/Brigham & Women s Hospital 7 th National Adult Congenital
The State of the Liver in the Adult Patient after Fontan Palliation Fred Wu, M.D. Boston Adult Congenital Heart Service Boston Children s Hospital/Brigham & Women s Hospital 7 th National Adult Congenital
Preoperative drainage is always indicated in malignant CBD strictures PRO. Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany
 Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
Lamivudine for Patients with hronic Hepatitis B and Advanced Liver Disease. From : New England Journal of Medicine
 Lamivudine for Patients with hronic Hepatitis B and Advanced Liver Disease From : New England Journal of Medicine Volume 351:1521-1531, Number 15, Oct 7, 2004 馬 偕 紀 念 醫 院 一 般 內 科, 肝 膽 腸 胃 科 新 竹 分 院 陳 重
Lamivudine for Patients with hronic Hepatitis B and Advanced Liver Disease From : New England Journal of Medicine Volume 351:1521-1531, Number 15, Oct 7, 2004 馬 偕 紀 念 醫 院 一 般 內 科, 肝 膽 腸 胃 科 新 竹 分 院 陳 重
Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment.
 1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
Introduction. Case History
 NAOSITE: Nagasaki University's Ac Title Author(s) A Case Report of Renal Cell Carcino Shimajiri, Shouhei; Shingaki, Yoshi Masaya; Tamamoto, Tooru; Toda, Taka Citation Acta Medica Nagasakiensia. 1992, 37
NAOSITE: Nagasaki University's Ac Title Author(s) A Case Report of Renal Cell Carcino Shimajiri, Shouhei; Shingaki, Yoshi Masaya; Tamamoto, Tooru; Toda, Taka Citation Acta Medica Nagasakiensia. 1992, 37
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
CME. Introduction. Methods. WM Yip HG Hung KH Lok KF Li KK Li ML Szeto. Study design O R I G I N A L A R T I C L E
 O R I G I N A L A R T I C L E WM Yip HG Hung KH Lok KF Li KK Li ML Szeto Outcome of inoperable hepatocellular carcinoma patients receiving transarterial chemoembolisation: a real-life retrospective analysis
O R I G I N A L A R T I C L E WM Yip HG Hung KH Lok KF Li KK Li ML Szeto Outcome of inoperable hepatocellular carcinoma patients receiving transarterial chemoembolisation: a real-life retrospective analysis
National Medical Policy
 National Medical Policy Subject: Policy Number: Ablation of Liver Tumors NMP124 Effective Date*: March 2004 Updated: February 2015 This National Medical Policy is subject to the terms in the IMPORTANT
National Medical Policy Subject: Policy Number: Ablation of Liver Tumors NMP124 Effective Date*: March 2004 Updated: February 2015 This National Medical Policy is subject to the terms in the IMPORTANT
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50
 General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
Section: Medicine Last Reviewed Date: August 2015. Policy No: 140 Effective Date: September 1, 2015
 Medical Policy Manual Topic: Radioembolization for Primary and Metastatic Tumors of the Liver Date of Origin: December 2, 2010 Section: Medicine Last Reviewed Date: August 2015 Policy No: 140 Effective
Medical Policy Manual Topic: Radioembolization for Primary and Metastatic Tumors of the Liver Date of Origin: December 2, 2010 Section: Medicine Last Reviewed Date: August 2015 Policy No: 140 Effective
New Treatment Options for Breast Cancer
 New Treatment Options for Breast Cancer Brandon Vakiner, PharmD., BCOP Clinical Pharmacy Specialist - Oncology The University of Iowa Hospitals and Clinics Assistant Professor (Clinical) University of
New Treatment Options for Breast Cancer Brandon Vakiner, PharmD., BCOP Clinical Pharmacy Specialist - Oncology The University of Iowa Hospitals and Clinics Assistant Professor (Clinical) University of
Localised Cancer Treatment. PCI Biotech. Amphinex a new product for localised cancer treatment
 Localised Cancer Treatment PCI Biotech Amphinex a new product for localised cancer treatment Disclaimer This document (the Presentation ) has been produced by PCI Biotech Holding ASA (the Company ). The
Localised Cancer Treatment PCI Biotech Amphinex a new product for localised cancer treatment Disclaimer This document (the Presentation ) has been produced by PCI Biotech Holding ASA (the Company ). The
La Malattia Metastatica Epatica Il Ruolo della radiologia Interventistica
 AIRO 2014 Padova 8-11 Novembre La Malattia Metastatica Epatica Il Ruolo della radiologia Interventistica Camillo Aliberti S.S.D.Radiologia Interventistica Oncologica Istituto Oncologico Veneto (IRCCS)
AIRO 2014 Padova 8-11 Novembre La Malattia Metastatica Epatica Il Ruolo della radiologia Interventistica Camillo Aliberti S.S.D.Radiologia Interventistica Oncologica Istituto Oncologico Veneto (IRCCS)
Optimal imaging surveillance schedules after liver directed therapy for hepatocellular carcinoma
 Optimal imaging surveillance schedules after liver directed therapy for hepatocellular carcinoma F. Edward Boas, MD, PhD; Bao Do, MD; John D. Louie, MD; Nishita Kothary, MD; Gloria L. Hwang, MD; William
Optimal imaging surveillance schedules after liver directed therapy for hepatocellular carcinoma F. Edward Boas, MD, PhD; Bao Do, MD; John D. Louie, MD; Nishita Kothary, MD; Gloria L. Hwang, MD; William
Hepatocellular carcinoma (HCC) is the sixth most common
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:604 611 Chemoembolization and Radioembolization for Hepatocellular Carcinoma RIAD SALEM and ROBERT J. LEWANDOWSKI Section of Interventional Radiology, Division
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:604 611 Chemoembolization and Radioembolization for Hepatocellular Carcinoma RIAD SALEM and ROBERT J. LEWANDOWSKI Section of Interventional Radiology, Division
Original Article Intervention
 Original Article Intervention http://dx.doi.org/10.3348/kjr.2014.15.4.464 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(4):464-471 Transcatheter Arterial Chemoembolization for Infiltrative Hepatocellular
Original Article Intervention http://dx.doi.org/10.3348/kjr.2014.15.4.464 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(4):464-471 Transcatheter Arterial Chemoembolization for Infiltrative Hepatocellular
A PATIENT S GUIDE TO ABLATION THERAPY
 A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
Evidence tabel Lokaal palliatieve behandelingen
 Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Hepatocellular carcinoma: Algorithms of diagnosis and options of therapy
 Hepatocellular carcinoma: Algorithms of diagnosis and options of therapy Alejandro Forner BCLC Group. Liver Unit. Hospital Clinic. University of Barcelona Pathogenesis and Clinical Practice in Gastroenterology
Hepatocellular carcinoma: Algorithms of diagnosis and options of therapy Alejandro Forner BCLC Group. Liver Unit. Hospital Clinic. University of Barcelona Pathogenesis and Clinical Practice in Gastroenterology
CANCER OF THE LIVER HEPATOCELLULAR CARCINOMA
 CANCER OF THE LIVER HEPATOCELLULAR CARCINOMA WHAT IS CANCER OF THE LIVER? Hepatocellular carcinoma is the most common form and it comes from the main type of liver cell, the hepatocyte. About 3 out 4
CANCER OF THE LIVER HEPATOCELLULAR CARCINOMA WHAT IS CANCER OF THE LIVER? Hepatocellular carcinoma is the most common form and it comes from the main type of liver cell, the hepatocyte. About 3 out 4
Treatment outcomes for hepatocellular carcinoma using chemoembolization in combination with other therapies
 Cancer Treatment Reviews (2006) 32, 594 606 available at www.sciencedirect.com journal homepage: www.elsevierhealth.com/journals/ctrv TUMOUR REVIEW Treatment outcomes for hepatocellular carcinoma using
Cancer Treatment Reviews (2006) 32, 594 606 available at www.sciencedirect.com journal homepage: www.elsevierhealth.com/journals/ctrv TUMOUR REVIEW Treatment outcomes for hepatocellular carcinoma using
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
THE SECOND VERSION of Evidence-based Clinical
 bs_bs_banner doi: 10.1111/hepr.12464 Special Report Evidence-based Clinical Practice Guidelines for Hepatocellular Carcinoma: The Japan Society of Hepatology 2013 update (3rd JSH-HCC Guidelines) Norihiro
bs_bs_banner doi: 10.1111/hepr.12464 Special Report Evidence-based Clinical Practice Guidelines for Hepatocellular Carcinoma: The Japan Society of Hepatology 2013 update (3rd JSH-HCC Guidelines) Norihiro
Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases
 I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
Hepatocellular carcinoma (HCC): a global perspective
 WGO Global Guideline HCC 1 World Gastroenterology Organisation Global Guideline Hepatocellular carcinoma (HCC): a global perspective November 2009 Review team: Peter Ferenci (chair) (Austria) Michael Fried
WGO Global Guideline HCC 1 World Gastroenterology Organisation Global Guideline Hepatocellular carcinoma (HCC): a global perspective November 2009 Review team: Peter Ferenci (chair) (Austria) Michael Fried
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Leading the Way to Treat Liver Cancer
 Leading the Way to Treat Liver Cancer Guest Expert: Sukru, MD Professor of Transplant Surgery Mario Strazzabosco, MD Professor of Internal Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale
Leading the Way to Treat Liver Cancer Guest Expert: Sukru, MD Professor of Transplant Surgery Mario Strazzabosco, MD Professor of Internal Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale
Summary of treatment benefits
 Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
1. Utility of transradial approach in endovascular management of chronic mesenteric ischemia
 PUBLICATIONS, ABSTRACTS AND PRESENTATIONS : 1. Utility of transradial approach in endovascular management of chronic mesenteric ischemia 2. Endovascular management of the suprarenal IVC agenesis 3. The
PUBLICATIONS, ABSTRACTS AND PRESENTATIONS : 1. Utility of transradial approach in endovascular management of chronic mesenteric ischemia 2. Endovascular management of the suprarenal IVC agenesis 3. The
Hepatocellular carcinoma: ESMO ESDO Clinical Practice Guidelines for diagnosis, treatment and follow-up
 Annals of Oncology 23 (Supplement 7): vii41 vii48, 2012 doi:10.1093/annonc/mds225 Hepatocellular carcinoma: ESMO ESDO Clinical Practice Guidelines for diagnosis, treatment and follow-up C. Verslype 1,2,
Annals of Oncology 23 (Supplement 7): vii41 vii48, 2012 doi:10.1093/annonc/mds225 Hepatocellular carcinoma: ESMO ESDO Clinical Practice Guidelines for diagnosis, treatment and follow-up C. Verslype 1,2,
Recent Progress in Understanding, Diagnosing, and Treating Hepatocellular Carcinoma
 Current Treatment Paradigms in Hepatocellular Carcinoma Recent Progress in Understanding, Diagnosing, and Treating Hepatocellular Carcinoma Mary Maluccio, MD, MPH 1 ; Anne Covey, MD 2 Hepatocellular carcinoma
Current Treatment Paradigms in Hepatocellular Carcinoma Recent Progress in Understanding, Diagnosing, and Treating Hepatocellular Carcinoma Mary Maluccio, MD, MPH 1 ; Anne Covey, MD 2 Hepatocellular carcinoma
Scottish Medicines Consortium
 Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
UK Guidelines for the management of suspected hepatocellular carcinoma (HCC) in adults
 UK Guidelines for the management of suspected hepatocellular carcinoma (HCC) in adults SD Ryder DM FRCP Consultant Hepatologist Queens Medical Centre Nottingham University Hospitals NHS Trust Wolfson Digestive
UK Guidelines for the management of suspected hepatocellular carcinoma (HCC) in adults SD Ryder DM FRCP Consultant Hepatologist Queens Medical Centre Nottingham University Hospitals NHS Trust Wolfson Digestive
Phone: 1-877-336-3736 Fax: 1-877-556-3737 M F 8:00 am 9:00 pm ET
 QUICK REFERENCE CODING & BILLING GUIDE PHYSICIAN OFFICE CMS National Coverage Determination and Q-Code for PROVENGE Simplifies patient coverage criteria Clarifies coding requirements Expedites electronic
QUICK REFERENCE CODING & BILLING GUIDE PHYSICIAN OFFICE CMS National Coverage Determination and Q-Code for PROVENGE Simplifies patient coverage criteria Clarifies coding requirements Expedites electronic
Interventional Oncology
 Interventional Oncology 23 September 2014 Imagine where we can go. Forward-looking statement This presentation and information communicated verbally to you may contain certain projections and other forward-looking
Interventional Oncology 23 September 2014 Imagine where we can go. Forward-looking statement This presentation and information communicated verbally to you may contain certain projections and other forward-looking
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
Approach to Abnormal Liver Tests
 Approach to Abnormal Liver Tests Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of Gastroenterology and Hepatology Indiana University School
Approach to Abnormal Liver Tests Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of Gastroenterology and Hepatology Indiana University School
Treatment options in hepatocellular carcinoma today
 Scandinavian Journal of Surgery 100: 22 29, 2011 Treatment options in hepatocellular carcinoma today T. Livraghi 1, H. Mäkisalo 2, P.-D. Line 3 1 Interventional Radiology Department, Istituto Clinico Humanitas,
Scandinavian Journal of Surgery 100: 22 29, 2011 Treatment options in hepatocellular carcinoma today T. Livraghi 1, H. Mäkisalo 2, P.-D. Line 3 1 Interventional Radiology Department, Istituto Clinico Humanitas,
GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER
 GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER Author: Dr Susan O Reilly On behalf of the Breast CNG Written: December 2008 Agreed at CNG: June 2009 & June 2010 Review due: June 2011 Guidelines Adjuvant Systemic
GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER Author: Dr Susan O Reilly On behalf of the Breast CNG Written: December 2008 Agreed at CNG: June 2009 & June 2010 Review due: June 2011 Guidelines Adjuvant Systemic
Stomach (Gastric) Cancer. Prof. M K Mahajan ACDT & RC Bathinda
 Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Management of Spontaneous Rupture of Liver Tumours
 Complications in Hepatobiliary Surgery Dig Surg 2002;19:109 113 P. Marini a V. Vilgrain b J. Belghiti a Departments of a Hepatopancreatobiliary Surgery and b Radiology, Beaujon Hospital, Assistance Publique,
Complications in Hepatobiliary Surgery Dig Surg 2002;19:109 113 P. Marini a V. Vilgrain b J. Belghiti a Departments of a Hepatopancreatobiliary Surgery and b Radiology, Beaujon Hospital, Assistance Publique,
Background. t 1/2 of 3.7 4.7 days allows once-daily dosing (1.5 mg) with consistent serum concentration 2,3 No interaction with CYP3A4 inhibitors 4
 Abstract No. 4501 Tivozanib versus sorafenib as initial targeted therapy for patients with advanced renal cell carcinoma: Results from a Phase III randomized, open-label, multicenter trial R. Motzer, D.
Abstract No. 4501 Tivozanib versus sorafenib as initial targeted therapy for patients with advanced renal cell carcinoma: Results from a Phase III randomized, open-label, multicenter trial R. Motzer, D.
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS
 YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
Uitgangsvraag 3: Welke prognostische factoren moeten er beschreven worden in het pa-verslag van het resectiepreparaat
 Uitgangsvraag 3: Welke prognostische factoren moeten er beschreven worden in het pa-verslag van het resectiepreparaat van HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics
Uitgangsvraag 3: Welke prognostische factoren moeten er beschreven worden in het pa-verslag van het resectiepreparaat van HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics
STE Report: Transarterial Radioembolization for the treatment of Hepatic Neoplasia
 STE Report: Transarterial Radioembolization for the treatment of Hepatic Neoplasia Laura Higgins, MSc Senior Analyst Sarah Rose, PhD Biostatistician Lloyd Sutherland, MD, MSc Project Director Tom Noseworthy,
STE Report: Transarterial Radioembolization for the treatment of Hepatic Neoplasia Laura Higgins, MSc Senior Analyst Sarah Rose, PhD Biostatistician Lloyd Sutherland, MD, MSc Project Director Tom Noseworthy,
Alcoholic Hepatitis (Teacher s Guide)
 Thomas Ormiston, M.D. Updated 5/5/15 2007-2015, SCVMC Alcoholic Hepatitis (Teacher s Guide) (30 minutes) I. Objectives Recognize the signs and symptoms of alcoholic hepatitis Understand the treatment options
Thomas Ormiston, M.D. Updated 5/5/15 2007-2015, SCVMC Alcoholic Hepatitis (Teacher s Guide) (30 minutes) I. Objectives Recognize the signs and symptoms of alcoholic hepatitis Understand the treatment options
Catheter Embolization and YOU
 Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
clinical practice guidelines
 Annals of Oncology 21 (Supplement 5): v59 v64, 2010 doi:10.1093/annonc/mdq166 Hepatocellular carcinoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up S. Jelic 1 & G. C. Sotiropoulos
Annals of Oncology 21 (Supplement 5): v59 v64, 2010 doi:10.1093/annonc/mdq166 Hepatocellular carcinoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up S. Jelic 1 & G. C. Sotiropoulos
Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer
 Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer David Josephson, MD FACS Fellowship Director, Urologic Oncology and Robotic Surgery Program Staging Most important in risk assessment and
Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer David Josephson, MD FACS Fellowship Director, Urologic Oncology and Robotic Surgery Program Staging Most important in risk assessment and
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Management of hepatitis C: pre- and post-liver transplantation. Piyawat Komolmit Bangkok
 Management of hepatitis C: pre- and post-liver transplantation Piyawat Komolmit Bangkok Liver transplantation and CHC Cirrhosis secondary to HCV is the leading cause of liver transplantation in the US
Management of hepatitis C: pre- and post-liver transplantation Piyawat Komolmit Bangkok Liver transplantation and CHC Cirrhosis secondary to HCV is the leading cause of liver transplantation in the US
Surgical Treatment of Various GI Tract Cancers
 Surgical Treatment of Various GI Tract Cancers By James Ouellette, DO, FACS, Surgical Oncology, Hepatobiliary Surgery Surgical treatment for most gastrointestinal (GI) cancers requires multidisciplinary
Surgical Treatment of Various GI Tract Cancers By James Ouellette, DO, FACS, Surgical Oncology, Hepatobiliary Surgery Surgical treatment for most gastrointestinal (GI) cancers requires multidisciplinary
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): 9/1/2011 Most Recent Review Date (Revised): 7/21/2015 Effective Date: 10/1/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS
Original Issue Date (Created): 9/1/2011 Most Recent Review Date (Revised): 7/21/2015 Effective Date: 10/1/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS
LIVER TRANSPLANTATION IN ALAGILLE SYNDROME
 LIVER TRANSPLANTATION IN ALAGILLE SYNDROME Ronald J. Sokol, MD Children s Hospital Colorado University of Colorado School of Medicine Treatment of Liver Disease in Improve bile flow ALGS Ursodeoxycholic
LIVER TRANSPLANTATION IN ALAGILLE SYNDROME Ronald J. Sokol, MD Children s Hospital Colorado University of Colorado School of Medicine Treatment of Liver Disease in Improve bile flow ALGS Ursodeoxycholic
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
