Therapist s Management of Distal Radius Fractures
|
|
|
- Stephanie Ramsey
- 8 years ago
- Views:
Transcription
1 Therapist s Management of Distal Radius Fractures SUSAN MICHLOVITZ, PT, PhD, CHT AND LYNN FESTA, OTR, CHT CHAPTER 70 SURGEON S MANAGEMENT OF DRFs EXAMINATION OF THE PATIENT WITH A DRF THERAPY GUIDELINES AND PROGRESSION MOBILIZATION/MOTION PHASE FUNCTION AND STRENGTHENING PHASE PATIENT EDUCATION AND HOME EXERCISE PROGRAMS THERAPY GUIDELINES BASED ON FRACTURE MANAGEMENT TECHNIQUE CONCLUDING STATEMENTS CRITICAL POINTS Therapy techniques and activities are based on principles of fracture healing and fixation. Validated self-report outcome questionnaires capture dimensions of the patient that are not always obvious by more traditional physical measures such as range of motion (ROM) with a goniometer. Pain can be a major obstacle to the return of motion and function. The goal during the mobilization phase is to restore as much motion as possible, but at least functional wrist range of motion. Management of distal radius fractures (DRFs) has evolved considerably over the past decade, mostly due to stable fixation techniques that permit early motion of the wrist (e.g., during the first 2 to 4 weeks after fracture reduction). Therapy goals after wrist fracture are to control edema and pain, restore (realistic) ROM, and promote the use of the involved extremity for grip, torque, and weight-bearing activities. This chapter discusses the therapy strategies to optimize motion and function after DRF. Surgeon s Management of DRFs There are a vast number of classification systems for surgeons to use to describe the nature of DRFs, and these are generally based on fracture fragment patterns. Using these classifications should theoretically serve as a foundation for the surgeon s intervention. Some knowledge of the most popular fracture classification paradigms can be helpful when communicating with surgeons. Fracture management by the surgeon may be done with the intent to reduce and stabilize fracture fragments and include the following: orthosis or plaster cast for minimally displaced fractures, 1 bridging external fixation devices with or without pinning and arthroscopically assisted reduction for intra-articular fracture fragments, 2 indirect reduction and percutaneous fixation 3 and open reduction and internal fixation with volar fixedangle plates with or without locking mechanisms, 4 and a low-profile dorsal plate (fragment-specific fixation or intermedullary nailing). 5 The preceding chapter and this chapter should be used together to understand a comprehensive approach to the treatment of a patient with a DRF. Progression of activity related to specific fracture management techniques is detailed later in this chapter. Examination of the Patient With a DRF The principles for examining the patient and selecting outcome questionnaires for patients with hand and wrist disorders are well covered in Chapter 16. Results of an examination assist the hand therapist in establishing goals for rehabilitation and determining prognosis for functional recovery. Patient values and expectations should be 949
2 950 PART 12 COMMON WRIST INJURIES Figure 70-1 Volar forearm bruising in a woman who is taking warfarin. considered when developing goals and therapy strategies. Patients with minimal complications who are self-directed and motivated and have an understanding of body functioning may be best served with one or two supervised therapy sessions with instruction in a home exercise program. Those with less body awareness, more severe injury, and complications usually require a supervised therapy program. During evaluation and treatment planning, these factors should be kept in mind. Patient Factors Including Medical History The therapist should collect information from the patient regarding work and daily demands including avocations, particularly those activities involving weight-bearing such as pushing up from the floor or pushing heavy loads and torquerelated activities or working with heavy equipment. Patients who had a high-impact injury such as a fall while snowboarding or riding a motorcycle may have a significant number of related soft-tissue injuries such as scapholunate ligament or triangular fibrocartilage complex tears. Co-morbidities such as diabetes mellitus, low hemoglobin, systemic lupus erythematosus, and immunosuppressive disorders should be documented because these conditions can delay healing or reduce expectations for the final outcome. Medication use should be documented and any side effects noted (e.g., blood thinners can result in excessive bruising) (Fig. 70-1). Patient-Rated Self-Report Measures/Questionnaires When assessing the patient who has had a DRF, outcomes measures should be selected that are representative of the limitations and disabilities associated with consequences of this injury. Pain scales such as the visual analogue scale, which reflects pain during rest and activity, should be administered. Pain can be a major obstacle to the return of motion and function. 6 Region-specific outcomes questionnaires such as the Patient-Rated Wrist Evaluation (PRWE) have a certain percentage of questions that directly assess pain. The PRWE has 5 questions related to pain and 10 questions related to function (usual and specific activities). The pain questions address pain at rest, during activity requiring repeated wrist motion, and when lifting a heavy object and ask when the pain is worst. The frequency of pain is also rated on the same 0 to 10 Likert scale. The specific activities include such items as turning a doorknob and pushing up from a chair using the involved wrist and hand. The usual activities include personal care, household chores, work, and recreational activities. Pain and function are weighted at 50% each, and the scale is graded from 0 (not disabled) to 100 (most disabled). 7,8 Validated questionnaires such as the PRWE, Disabilities of the Arm, Shoulder, and Hand (DASH) questionnaire, 6 and the Michigan Hand Outcomes Questionnaire 9 can capture dimensions of the patient that are not always obvious by more traditional physical measures such as ROM with a goniometer. 10 These measures are responsive to changes in the patient during early (within the first few months) and late (at 1 year after injury) recovery. 11 The greatest changes in DASH 12 and PRWE 11 scores occur during the 3- to 6-month period after fracture but will continue to improve over the first year. These region-specific questionnaires can be more responsive and specific in measuring recovery after DRF than a global measure such as the SF-36 Health Survey. 13 Knowledge of these time frames can assist the therapist in educating the patient about expected milestones for recovery of function and often alleviate some of the patient s concerns about recovery. ROM Passive and active motion measures are indicators of impairment after wrist fracture. It is important to discern which structures are involved in limiting motion. Differential motion loss (e.g., active versus passive) is addressed in this chapter in the Mobilization/Motion Phase section. Particular attention should be paid to wrist extension, supination, and pronation motions that may be most difficult to restore after DRF. Restoration of those motions has been correlated with higher function as measured by DASH scores. 14 Therapy strategies should focus on restoration of functional wrist and forearm motion. Hand function, as measured by the Jebson Taylor Hand Function Test, has been shown in normal persons to be reduced when elbow, forearm, wrist, and finger motions are limited. 15 We may be able to extrapolate these results to patients after wrist fracture. Digital motion can be markedly limited after high-impact injuries, after falls in the elderly, and in patients who have osteoarthritis (Fig. 70-2). Therefore, careful monitoring of finger and thumb motion is important. Loading Across the Wrist: Grip, Pinch, and Push-off Reduction in the ability to grip and twist and to bear weight on the palm, needed when pushing open a door or pushing up from a chair, are common functional complaints in persons recovering from wrist fractures. Grip and pinch strength can be tested when fracture healing has progressed to the point where weight-bearing activities are permitted on the hand. Testing can usually begin 6 to 8 weeks after
3 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 951 A B Figure 70-2 A, Limited finger flexion after distal radius fracture in a woman with osteoarthritis affecting the hand. B, Side view of fingers during attempted flexion. fracture, if the fracture is healed. It is prudent to check with the surgeon regarding the status of fracture healing. The push-off test 16 is used to quantify the ability to bear weight through the palm (Fig. 70-3). This has been tested and found to be reliable in normal subjects and also in a patient population after wrist and elbow fractures. 17 The uninjured side can be used for comparison because weightbearing ability is not dependent on hand dominance. Figure 70-3 Push-off test using a Jamar dynamometer. The therapist must stabilize the dynamometer on the table while the patient is applying weight on the palm onto the device. Radiographic Outcome There is some evidence that the amount of wrist 18 and forearm motion 19 as well as functional outcomes gained after fracture is related to the success of anatomic reduction. In the patient who may have less demand during activities of daily living, failure to restore anatomy may not be as critical to the final outcome. 7 Therefore, each patient s outcome must be assessed individually and goals established with the patient s input, particularly in younger adults. It is not clear whether this is as important in an elderly population. 20,21 Measuring Outcome of Intervention After Wrist Fracture To compare therapy interventions, each clinic should consider a standardized battery of measures (e.g., a core outcome dataset). 22 These measures should be selected from those that reflect the problems of patients with the injury, are reliable (e.g., can be reproduced with minimum amount of error), and are responsive to change (e.g., will change in response to change in patient status). A suggested testing paradigm is presented in Box Some measures may be better to use during certain time periods after injury. For example, volumetric or girth measures can be useful to monitor edema during the early motion phase, but are less useful later in recovery when edema has stabilized or resolved. Before it is safe to test grip strength, patient-reported outcomes such as those included on the PRWE or DASH may give information that highlights areas of concern that should be included in goal setting and addressed during therapy. 13 Most recovery can be expected to occur within the first 6 months after fracture, 11 although supervised therapy is often provided only during the early period after immobilization (e.g., 4 to 6 weeks). When assessing long-term outcomes in patients who have had surgical treatment for DRF, it is important to be aware of factors that have been shown to have adverse affects on recovery such as increased age and
4 952 PART 12 COMMON WRIST INJURIES Box 70-1 Suggested Therapist Examination Components After Distal Radius Fracture EARLY TESTING AFTER DRF Pain using VAS or PRWE Function with self-report outcomes questionnaires (PRWE or DASH) Light touch with monofilaments to screen for nerve compression (median, ulnar, dorsal radial nerve) Figure-of-eight measurement or volume displacement (if no external fixation device or cast) ROM (if wrist is still immobilized measure adjacent joints) LATER TESTING AFTER DRF (FROM 6 TO 8 WEEKS ONWARD) ROM Grip strength Pinch strength Push-off test Function with outcomes questionnaires (PRWE or DASH) DASH, Disability Arm, Shoulder, and Hand questionnaire; DRF, distal radius fracture; PRWE, Patient-Related Wrist Evaluation; ROM, range of motion. lower income. 23 The injured worker should be assessed based on physical work demands. Those who have jobs that involve heavy lifting, pushing, and pulling may be expected to have a longer time out of work. 24 Overall outcomes can be expected to be better in patients who have higher DASH scores or patient perceived outcomes, greater grip strength, and better radiographic evidence of restoration of anatomy. 25 Therapy Guidelines and Progression DRFs are not all the same; therefore, why should therapy be all the same? Progression of activities is discussed in each phase of rehabilitation with guidelines, techniques, and precautions. These, of course, should be used as guidelines and modified for particular circumstances. Initiation of motion and progression to joint mobilization techniques, strengthening, and weight-bearing activities should be undertaken when fracture healing permits. This is a determination made by the surgeon during successive follow-up office visits and reexamination and communicated to the therapist with an updated therapy referral. Realistic goal planning for improvements in wrist ROM and hand function requires assessment of any residual deformities. The DRF may be a well-healed, essentially nondisplaced extra-articular fracture, but it may also be a dorsally displaced DRF with a combination of displacement, radial shortening, dorsal angulation, and even intra-articular involvement. Implications for ultimate outcome and use of therapy techniques may be different in both examples. In the latter, it may be less likely to restore as much ROM. Therapy techniques and activities are based on principles of fracture healing and fixation. We must consider progression on an individual basis, and this can be influenced by a number of factors. These can include some of the following: Success of reduction of fracture and restoration of anatomy. There is some evidence that the amount of wrist 18 and forearm 19 motion and the functional outcomes gained after fracture are related to the success of anatomic reduction in younger adults. It is not clear whether this is as important in an elderly population. 20,21 The time frame for healing (e.g., when can wrist motion begin and when can resisted and weight-bearing exercises begin)? Complications such as nerve compression, tendon rupture, stiffness, and pain can reduce function and can lower final outcome. Some complications that occur after DRF can be addressed through a therapy program (e.g., stiffness) and some may not (e.g., fracture malunion or delayed union), resulting in debilitating pain and decreased strength. More details about complications are addressed later in this chapter. Pain can be a major obstacle to return of motion and function. 6 The source of pain, whether it be physiologic or psychosocial, should be addressed by the appropriate practitioner. If there is evidence of complex regional pain syndrome (CRPS), then pharmacologic intervention managed by a physician pain specialist may be used in conjunction with therapy modalities such as heat, cold, and electrical stimulation. Phases of Rehabilitation Activities during healing can be divided into the following phases: early protective phase (or during immobilization or protected motion), motion or mobilization, and function and strengthening. These are summarized in Table Educating the patient regarding the healing process should be done in a way that will be meaningful to that person s status and daily life requirements. Patient compliance and its importance in the rehabilitation partnership need to be emphasized. The roles of joint mobilization and orthotic wear to increase ROM are included in the discussion. Early Protective Phase Ideally a hand therapist can see a patient within the first week after wrist fracture management for home instruction for symptom management (e.g., pain, edema, finger stiffness) and education regarding functional limitations and abilities. Due to a number of circumstances, we often see a patient after the first follow-up visit at the surgeon s office and that patient has fingers that are stiff and swollen and well on the way to residual loss of motion (see Fig. 70-2). Early on after fracture, it can be common for the patient to hold the injured upper extremity in a protected position with the shoulder adducted and internally rotated and the
5 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 953 Table 70-1 Phases of Therapy After Distal Radius Fracture Early Protective Phase Motion/Mobilization Phase Function/Strength Phase Time frame Goals and priorities Techniques Comments and precautions 1 6 weeks depending on fracture fragment stability Protect fracture, control swelling and pain, avoid pin-site infections Cast, orthosis, surgical fixation/stabilization; edema control (elevation including overhead fisting, retrograde massage, compression wraps); regular pin-site cleaning (for percutanous pinning); tendon-gliding exercises, particularly after ORIF Digit ROM should be attained in this phase; signs of CRPS (significant edema and/or pain, redness) should be monitored and addressed; abnormal paresthesias should be recorded Starts immediately after immobilization AROM and PROM of digits, elbow, shoulder; AROM of wrist; forearm rotation AROM of shoulder, elbow, forearm, wrist, digits; AROM/ gentle PROM of forearm, wrist, digits; dynamic orthoses Pain, swelling due to excessively vigorous ROM exercises; avoid excessive ROM if there are indicators of delayed healing or instability; wrist extension with digit flexion is a priority Begun with proven healing/bone fixation Increase ROM to WFLs; increase strength to WFLs for activities of daily living Isometric progressing to isotonic exercises; resisted exercises with putty or grippers Excessive overload, irritated tissues, increased pain after exercises, functional activities AROM, active range of motion; CRPS, complex regional pain syndrome; ORIF, open reduction and internal fixation; PROM, passive range of motion; WFL, within functional limits. Adapted from LaStayo PC, Michlovitz SM, Lee M. Wrist and hand. In: Kolt G, Snyder-Macker L, eds. Physical Therapies in Sport and Exercise. 2nd ed elbow flexed. The use of a sling should be minimized because it does not properly elevate the extremity; it promotes shoulder and elbow stiffness and discourages functional use of the hand and arm. Slings may be used for short periods when protection is needed in crowded public situations. Active motion of the digits, elbow, and shoulder (and wrist and forearm, if permitted) and overhead fisting should be encouraged to be performed several times daily. A stringent effort of elevating the hand and wrist above heart level may be successful in controlling pain and edema. 26 If necessary, retrograde massage and compression wraps may be used for edema control. Cold packs or wraps may also be used after exercise if swelling has increased. But if swelling increases after each exercise session, then perhaps the vigor of the exercises should be reduced to alleviate undue stress on already inflamed tissues. It is important to acknowledge that the pain is real for the patient. Most patients have never experienced a DRF. In addition to being frightened and in pain, the sudden interference with loss of independence increases the patient s anxiety level. Along with reassurances that the pain will get better, it is important to reinforce strategies that will decrease the pain, such as elevation, massage, heat or cold modalities, and active exercises. In most patients, pain will fade as stable fracture fixation is achieved. 11 However, treatment of pain is given priority if it seems to be a greater problem than the stiffness. It is difficult to use treatment techniques to address the stiffness and dysfunction if the pain cannot be controlled. Attempts should be made to determine whether the pain stems from possible median nerve compression, is sympathetically mediated, or is related to joint tightness or an illfitting immobilization cast or orthosis. If a program of early wrist motion (e.g., within 2 to 4 weeks) is instituted, an orthosis that fits and allows full digit mobility should be worn between exercise sessions. If a wellfitted prefabricated orthosis cannot be supplied, then the therapist has the option of a custom-molded thermoplastic orthosis (Figs and 70-5). The orthosis may require the therapist to monitor and modify on a regular basis (e.g., weekly) to accommodate changes in edema and motion. How do you know early on if things are not going so well for the patient? Early predictors of difficulty in recovery can include the following: metacarpophalangeal (MCP) or proximal interphalangeal (PIP) joint pain and swelling, tingling in digits, and rapid change in swelling with position change. We have observed that patients who have osteoarthritis may notice their first difficulty with finger stiffness after a fall on an outstretched hand. The common comment that we hear from patients is Well, I did not have arthritis before my injury. In some patients, palmar nodules and bands may develop with a subsequent decrease in palmar mobility. This may be indicative of Dupuytren s contracture. 27 A B Figure 70-4 Dorsal view (A) and side view (B) of a custom circumferential wrist orthosis.
6 954 PART 12 COMMON WRIST INJURIES Figure 70-5 Custom volar forearm-based wrist orthosis. An early sign of trouble observed by the authors is the patient who has red and painful PIP joints and fluctuating hand edema. We have observed that CRPS develops in some of these patients. Pin insertion on the radial side of the wrist may irritate the superficial branch of the radial nerve 27 and result in hyperesthesia or causalgia. Mobilization/Motion Phase The goal during this phase is to restore as much motion as possible, but at least functional wrist ROM, defined as 40 degrees of flexion and 40 degrees of extension of the wrist and a total of 40 degrees of radial and ulnar deviation. 28 Supination and wrist extension can be challenging to restore after DRF. However, regaining finger flexion can be equally if not more challenging, particularly in the person who has osteoarthritis. Most motion gains will be made during the first 3 months after fracture. 25 There can be motion gains up to 1 year, but the rate and magnitude of these changes lessen and patients would rarely need to be in supervised therapy for such an extended period of time. Techniques to Restore Motion A summary table (Table 70-2) is provided to assist in decision making related to restoring motion after DRF. When determining and prioritizing therapy strategies for improving motion, the techniques selected should to be matched with the tissues restricting motion. For example, if passive and active motion values are equally limited, then this more likely can implicate a joint as a source for the loss of motion. The motion can be lost due to obliteration of the joint space or an adaptively shortened joint capsule. The former cannot be improved by therapy, but the latter can. Selective tissuetensioning maneuvers must be done to differentiate loss of motion. If passive PIP joint flexion is restricted, it can be caused by stiffness from osteoarthritis (which may be exacerbated after trauma), joint contracture, or reduction of extensor tendon excursion (i.e., lengthening). Scar or pin sites on the dorsum of the hand can limit extensor tendon gliding and lead to intrinsic muscle tightness. Selective tissue tensioning is discussed in more detail in Chapters 6 and 67. Wrist extension may be reduced because of adaptive shortening of the joint capsule, scar, or reduced flexor tendon gliding on the volar wrist. Supination loss may be attributed to volar soft-tissue injury or shortening, potentially involving the pronator quadratus, joint capsular adhesions, or distal radioulnar joint (DRUJ) malalignment. The former two can be addressed through exercise and orthotic wear. DRUJ malalignment or subluxation that limits supination and/or pronation and results in protracted pain may be addressed at a later time by surgery. Subluxation of the DRUJ can decrease forearm rotation. In particular, a severe positive ulnar variance will limit supination. 19 Active motion of the wrist, forearm, and digits should be emphasized early in the motion phase. Wrist extension without concurrent finger extension may be difficult to achieve early on. A priority in therapy is to overcome this substitution pattern because finger flexion, grip strength, and hand function cannot improve until the wrist extensors relearn to work alone without help from the digital extensors. If active exercise and verbal cues are not sufficient to activate wrist extensors, then neuromuscular electrical stimulation isolated to the wrist extensors may be helpful for muscle reeducation and to enhance tissue extensibility (Fig. 70-6). 29 The electrodes would be placed over the wrist extensors near the elbow and middorsal forearm, the latter electrode to complete the circuit. A pulse rate of 25 to 35 pulses per second should be sufficient to cause a smooth titanic muscle contraction. A cycle of 10 seconds on and 20 seconds Table 70-2 Decision Making Related to Restoring Motion After Distal Radius Fracture Testing Characteristic Findings Suggested Intervention to Increase Motion Joints Tendons Intrinsic muscles Passive ROM (and compare with uninjured side) Compare passive with active ROM Bunnell Littler test Active and passive motion may be equal With loss of tendon gliding, active motion will be less than passive motion in the direction of the motion measured; flexor tendon adherence can limit passive extension More PIP joint flexion with MCP joints flexed, then with MCP joints extended Joint mobilization grades 3 and 4 glides; traction grade 3 (if there was an intra-articular fracture, check imaging studies for joint space) Active motion of agonist; NMES of agonist muscle; resisted exercise of agonist Intrinsic muscle stretching (MCP joints extended and PIP joints flexed) MCP, metacarpophalangeal; NMES, neuromuscular electrical stimulation; PIP, proximal interphalangeal; ROM, range of motion.
7 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 955 Figure 70-8 Exercises for passive stretch. Figure 70-6 Neuromuscular electrical nerve stimulator to increase wrist extension. off, with a ramp up of 3 seconds should suffice to produce a good contraction and minimize muscle fatigue. As training progresses, 10-second on and 10-second off cycling can be used. Amplitude should be set to achieve a fair plus (3+/5) muscle contraction. Electromyographic biofeedback may also be helpful for muscle reeducation of the wrist extensors, but isolated placement may be challenging because of the overlapping muscles. However, most patients can achieve independent wrist extension without the help of these modalities, but they can be useful adjuncts in selected patients. Active wrist flexion should be performed with the fingers relaxed or extended. Radial and ulnar deviation should be done with the wrist in neutral position in the sagittal plane and the forearm pronated. It is also helpful to have the patient use the opposite hand to stabilize the forearm to prevent the elbow from moving. Forearm rotation should be done with the elbow at approximately a 90-degree angle and tucked into the side to prevent shoulder substitution. Exercises can be repeated 10 times each 3 to 4 times per day. Emphasis should be placed on moving to the end of the available range, rather than just wiggling fingers and flapping the hand about in the air. ROM exercises through multiple planes of motion can be done with the assistance of a wand (Fig. 70-7, online). The results of a systematic review indicated that the strongest evidence for techniques to restore passive ROM in the upper extremity include active exercise, joint mobilization, and the use of an orthosis. 30 There were limited or no studies that examined the contribution of heat, cold, ultrasound, or electrical stimulation modalities and the use of continuous passive motion or passive stretch to increase joint motion due to joint contracture in the upper extremity. The application of heat can have positive short-term effects on pain and tissue elasticity to facilitate ease of exercise. Thermal agents such as moist heat packs, Fluidotherapy, and paraffin may help some patients follow their rehabilitation program with less discomfort and can easily be incorporated into a home program. There is support in the literature for the use of heat to increase tissue extensibility in joint contracture. 31 Passive stretch exercises are incorporated into the exercise program when tolerated or when fracture healing permits, as determined by radiographs and the referring surgeon. Each stretch should be held for 30 seconds for one or more repetitions 32 several times per day. Recommendations for specific doses of passive stretch vary in the literature, and the recommendations are extrapolated from literature on stretching of leg muscles. Examples of passive stretches are shown in Figures 70-8 to The therapeutic benefits and differences of both active ROM and passive stretch exercises should be explained to the patient so that there is an understanding that one is not a substitute for the other type of exercise. For patients with persistent joint stiffness, joint mobilization techniques can be used to assist in restoration of normal joint play or accessory motion when ROM is limited. 33,34 This technique has also been used as an adjunct in relieving pain. Translatory glide mobilizations of grade 3 or 4 are used to Figure 70-9 Exercises for passive stretch.
8 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 955.e1 A B Figure 70-7 Use of a wand for range of motion exercises.
9 956 PART 12 COMMON WRIST INJURIES Figure Exercises for passive stretch. increase motion, and grades 1 and 2 are oscillations to reduce pain. Manual traction should be applied across the joint concurrent with the glide (e.g., manual traction to the radiocarpal joint while performing a volar glide of the carpus on the distal radius to restore wrist extension). To restore wrist extension, the radiocarpal traction is accompanied by a dorsal glide of the carpus on the distal radius. Therapists using joint mobilization need to be skilled in the technique and need to make sure that there are no contraindications such as intra-articular incongruency and osteoporosis. Other contraindications for passive stretch and joint mobilization include incomplete bony union. It is not prudent to use joint mobilization in the presence of sharp, acute pain with motion and/or hypermobility. 33 Further details on joint mobilization may be found in Chapter 120. Mobilization with movement, a recently popularized technique by physical therapist Brian Mulligan, may also be used to enhance passive motion and reduce pain. This combines principles of active or passive motion and joint mobilization. The therapist combines mobilization with active motion or passive motion. The goal is to increase motion in a pain-free way. 33,35 Role of Orthotic Devices for Adaptively Shortened Connective Tissue When wrist or forearm ROM plateaus before reaching an acceptable functional level, several dynamic or static progressive orthotic approaches to improve passive ROM may be considered. Joint tightness is improved by sustained gentle stress at the end of available ROM over long periods instead of by short periods of high-intensity stretch. Low-load prolonged stress (LLPS) is more effective than high-load brief stress. 36 Knowledge of scar-tissue response to stress and biomechanics of the hand and wrist has led to advances in orthotic techniques that can be effective in improving wrist ROM limitations after DRF. Static progressive orthosis use applies LLPS to the scar tissue through adjustable force application. A static progressive orthosis may be more effective than a dynamic orthosis when the passive ROM does not exceed the active ROM. Several types of orthoses can be fabricated with the goal of holding tissue at end ROM (Figs to 70-14). Dynamic orthoses work by the mechanical principle of creep and static Figure Orthosis to increase range of motion of wrist and finger extension. (Courtesy of Kristen Valdes, OTR/L, OTD, CHT, Hand Works Therapy LC, Sarasota, Florida.) progressive orthoses by stress relaxation. Dynamic or static progressive forearm rotation orthoses can also be fabricated. Orthoses that increase wrist or forearm motion are also commercially available. In a retrospective review of patients after DRF, 38 of 249 patients were treated with static progressive orthoses for wrist and forearm motion. Those patients who gained wrist extension and supination had a better functional outcome as measured by grip strength and the DASH. 14 Further details on specific orthotic techniques for mobilization of joints are found in Chapters 123 and 124. Patient selection and knowledge of the healed position of the fracture are important when considering the use of one of these dynamic or static progressive orthoses. These orthotic approaches can be considered when the loss of motion is related to soft-tissue tightness due to joint capsular or musculotendinous unit adaptive shortening and not bony blockage or joint instability. Good patient compliance and clear wearing instructions are required because the orthoses need to be worn several hours each day to be effective. For static progressive orthoses, wearing times of 30 to 60 minutes a few times each day had a positive effect on increasing wrist flexion and extension motions in a case series of patients with wrist stiffness due to DRF or other injuries who had residual joint contracture after other therapy techniques. 37 Note that wear schedules in this series began for one session per day and built up to three sessions per day by 3 to 5 days. Similar positive findings were Figure Orthosis to increase range of motion of wrist extension. (Courtesy of Paul Brach, MS, PT, CHT, Hand Center of Pittsburgh, Pittsburgh, Pennsylvania.)
10 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 957 Figure Intrinsic muscle stretching exercise. Note metacarpophalangeal joints are extended while proximal and distal interphalangeal joints are flexed. Figure Orthosis to increase range of motion of wrist extension. (Courtesy of William W. Walsh, MBA, MHA, OTR/L, CHT, Hand and Rehabilitation Specialists of North Carolina, Greensboro, North Carolina.) reported for patients who used a static progressive orthosis to restore forearm rotation. 38 Orthotic devices are expensive and time-consuming to fabricate or can be costly to rent when a commercial device is used. It takes a significant commitment on the part of the patient to be compliant with wear schedules. If the patient has not been compliant in the other aspects of DRF rehabilitation, the provision of one of these orthoses may not be indicated or justified. What About the Hand? Active ROM exercises of the uninvolved joints act to maintain joint mobility, prevent tendon adherence, and help reduce edema by the pumping action of the muscles transporting the fluid proximally. Full excursion of the flexor and extensor tendons can be prohibited by the flexed position of the wrist in the cast or external fixation device. The accompanying pain and edema may further restrict tendon gliding. Patients need to be instructed in specific exercises that need to be sustained for 10 seconds, repeated 5 to 10 times each, and performed several times each day. It must be emphasized Figure Orthosis to increase range of motion wrist flexion. (Courtesy of Paul Brach, MS, PT, CHT, Hand Center of Pittsburgh, Pittsburgh, Pennsylvania.) that nonspecific, fluttering movements of the fingers are not effective. In addition to active flexion and extension exercises for the fingers, patients should be instructed in individual tendon-gliding exercises for the superficialis and profundus tendons. The hook-fist position isolates the digital extensors and aids interphalangeal joint flexion as well as stretches the intrinsic muscles. Particular attention needs to be paid to stretching the intrinsic muscles by extending the MCP joints while flexing the PIP and distal interphalangeal joints (Fig ). Passive stretching of the joints should target MCP joint flexion, PIP joint extension, and stretching of the thumb webspace. There should be no painful forceful passive manipulations. The patient needs to understand the differences between active ROM and passive stretch exercises and that one type of exercise is not a substitute for the other one. Like the wrist, resistant contractures of the fingers may benefit from orthotic use to provide an LLPS. Chapter 67 addresses management of the stiff hand in more detail. Function and Strengthening Phase When fracture healing has progressed, exercises that apply stress or load to the wrist can be initiated. It is important to emphasize that the determination of fracture healing adequate for initiation of stress loading and strengthening is made by the surgeon based on reexamination of the patient, either clinically or radiographically. In general, at approximately 8 weeks, the wrist can typically handle progressive loading 39 from light grip to wrist isometrics to progressive resisted exercises (Figs to 70-21) to closed chain activities. It is important to keep in mind that the patient has not used his or her involved upper extremity for any more than light activities for a considerable time. Therefore, upper extremity conditioning exercises are appropriate in both open and closed chain activities. Closed kinetic chain activities include exercises performed in weight bearing such as wall push-ups, plyoball exercises, and pushing or pulling activities. Exercise tools that are used for proximal stabilization (Fig ) such as the Body Blade ( com) or the B.O.I.N.G. Arm Exerciser ( may
11 958 PART 12 COMMON WRIST INJURIES Figure Progressive resisted exercises using an exercise band for wrist extension. be useful additions to the person with high functional demands of the upper extremity. These exercise tools and devices can be used in a supervised therapy session and then used on a home program basis. Patient Education and Home Exercise Programs Patients are usually concerned about the course of recovery from a DRF, the ultimate outcome, and whether their aches and pains are normal. The therapist can educate the patient about recovery milestones. MacDermid 25 and colleagues provided a general framework for recovery. It seems prudent for the therapist to spend considerable time and effort designing and implementing a home program for edema control, pain modulation, and exercise. Written instructions should be in language that is not therapy speak but which is understandable to the specific patient. Figures or photographs that enhance the written instructions are beneficial. Digital images of the exercise session can be taken for the patient with a digital camera or with the patient s cellular phone if it is equipped with a camera (Fig ). Therapists must be good educators, and patients with DRFs must effectively perform their home programs and accept Figure Progressive resisted exercises using an exercise band for wrist flexion. responsibility for their rehabilitation. Evidence in the literature supports the importance of a home exercise program in patients after DRF for promoting optimal recovery. 40 Therapy Guidelines Based on Fracture Management Technique There are a myriad of techniques used by surgeons to anatomically reduce and stabilize DRFs. Much has been written about the advantages and disadvantages of each, and new Figure Progressive resisted exercises using a free weight for wrist extension. Figure Progressive resisted exercises using a free weight for wrist flexion.
12 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 959 Figure Progressive resisted exercises for forearm rotation. techniques are ever evolving. Some of the more common techniques and postsurgical management are discussed in the following section. For individual cases, the surgeon who managed and referred the patient should be contacted to discuss specifics of fracture care and therapy management. Closed Reduction and Cast Immobilization When a fracture is considered stable with good alignment and does not require surgery, a cast is applied for approximately 4 to 6 weeks, depending on healing and the overall health of the patient. A properly applied cast should allow full active flexion of all digits and should be applied proximal to the distal palmar crease. When a cast is applied improperly, edema of the digits can occur, as well as intrinsic tightness, resulting in a stiff hand and potentially CRPS, even before the cast is removed. If this patient is referred to hand therapy with the cast still applied, a properly fitted cast is important. If the cast material cannot be cut down in the clinic, the patient should be referred back to the physician to have the cast reapplied. Edema control measures are introduced such as elevation above the level of the heart, retrograde massage, use of self-adherent elastic wrap, and active Figure Use of an exercise device (Body Blade) for proximal stabilization exercises. exercise to facilitate muscle pumping. Tendon-gliding exercises and those to facilitate intrinsic stretching should be taught to the patient. Shoulder and elbow ROM should also be examined, and ROM exercises for these joints should be reviewed as part of the home exercise program. There are some patients who are managed in this fashion who do not need formal supervised therapy. Those in whom complications develop may need ongoing supervised therapy. The older patient who did not have surgery and has a malunion and osteoarthritis will likely have prolonged wrist pain and stiff fingers. There are also patients whose therapy may be more focused on increasing tolerance of functional demand to allow return to premorbid activity. An example is a patient who is a violinist who required general upper extremity Figure Grip exercises for hand strengthening. Figure Use of camera to document home exercise program.
13 960 PART 12 COMMON WRIST INJURIES Figure Use of a therapy ball for upper extremity and core stabilization and endurance exercises. conditioning and core strengthening exercises after a nondisplaced DRF. Therapy focused on conditioning and stabilization exercises including activities using a therapy ball (Fig ). External Fixation With or Without Percutaneous Pinning Bridging (e.g., across the radiocarpal articulation) or nonbridging external fixation devices 41 (Figs and 70-26) are sometimes the treatment of choice for high-energy impact injuries. The therapist must take the extent of soft-tissue injury into account when planning therapy. When a DRF is treated with external fixation, the complications most commonly seen are pin-site infection, edema, first webspace tightness, and intrinsic tightness of the digits. If a patient is referred to hand therapy with the external fixation device still in place, examination should include the following: ROM of shoulder, elbow, and digits and edema measurement using a tape measure. Treatment is the same as with casting: retrograde massage, use of self-adherent elasticized wrap, and active ROM. Pin-site care should also be reviewed with the A Figure A, Radiograph of distal radius fracture. B, Radiograph of external fixation device with percutaneous pinning for a distal radius fracture. (Courtesy of Daniel DiCristino, MD, Fayetteville, New York.) patient. The patient should be instructed to keep the pin sites dry and clean at all times because the pin is a conduit of infection. 42 Daily cleaning using saline solution or diluted hydrogen peroxide applied with a clean cotton-tipped applicator is recommended by some, but newer evidence suggests that this may not be necessary. 42 Tendon-gliding exercises performed on an hourly basis should also be emphasized. Special attention should be placed on the index finger because the dorsal pins are usually in close proximity to the extensor indicis proprius and extensor digitorum communis. Another problem seen is dorsal radial sensory nerve involvement, B A B C D Figure Radiographs of volar fixed-angle plate for a distal radius fracture. A, Lateral view of distal radius fracture. B, Lateral view of volar plate. C, Anteroposterior view of distal radius fracture. D, Anteroposterior view of volar plate. (Courtesy of Michael Nancollas, MD, Orthopedic Associates of Central New York, Syracuse, New York.)
14 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 961 Table 70-3 More Common Complications After a Distal Radius Fracture Complication Early Late Median nerve compression/ x x Test for diminished sensibility in median distribution of hand carpal tunnel syndrome Complex regional pain syndrome x Early signs may be more pain than expected after injury, vasomotor instability, pain and redness in PIP joints, burning sensation in hand Tendinitis, tenosynovitis x During remobilization may have focal pain at wrist (ulnar-sided wrist pain can implicate the ECU tendon) Superficial branch of radial nerve x Hyperesthesia from wrist to dorsum of thumb, index and middle fingers (to level of PIP joint) compression/neuropathy Tendon adhesions and scarring x Active motion lags behind passive motion; examine for scar adherence and observe skin for puckering Ulnar nerve compression x Paresthesia in ulnar distribution of hand and/or ulnar innervated intrinsic weakness and atrophy Distal radioulnar joint problems x x Failure to gain forearm rotation can indicate DRUJ incongruity; note pain during forearm rotation Ruptured EPL/FPL tendon x Symptoms of weakening of thumb extension or flexion can indicate impending rupture; loss of active extension or flexion at interphalangeal joint Early, within the first month; late, after the first month. (Note: These are only relative time frames and can be different for each patient.) DRUJ, distal radioulnar joint; ECU, extensor carpi ulnaris; EPL, extensor pollicis longus; FPL, flexor pollicis longus. Adapted from McKay SD, MacDermid JC, Roth JH, Richards RS. Assessment of complications of distal radius fractures and development of a complication check list. J Hand Surg 2001;26A: most typically caused by placement of the proximal pin site too close to this nerve. This can lead to CRPS; therefore, a sensory examination should also include the dorsoradial aspect of the hand. Acute carpal tunnel syndrome can also be experienced in this population, due to trauma caused by the injury and/or the position of the wrist in the fixation device. The surgeon should be contacted immediately by the patient or hand therapist if he or she experiences any sensory changes. Open Reduction and Internal Fixation Volar Fixed-Angle Plating The bonus of applying a volar plate is the fixation that can be attained that allows early motion, which is advocated and encouraged by most physicians using this technique. However, literature supporting early wrist motion is equivocal. 43 Postoperative edema can be addressed early before tendon tightness, either intrinsic or extrinsic, becomes an issue. If early motion is suggested by the surgeon, then a wrist orthosis should be worn between therapy sessions until 6 weeks after fracture. This orthosis can be prefabricated or custom fabricated depending on the fit. Scar management may be necessary using techniques such as scar massage followed by application of silicone gel pads. Complications after volar fixed-angle plating reported in the literature include ruptures of the flexor pollicis longus and extensor tendons, but this is uncommon. If interphalangeal joint motion of the thumb in either flexion or extension is difficult to attain, the thumb joint should be monitored closely to avoid this complication. Dorsal Plating This is an alternative to volar plate fixation, and in one case series, the patients were satisfied with the procedure and gained 80% of their ROM of the wrist. 44 Others also reported positive results using a dorsal Pi plate. 45,46 The most common and disappointing complication seen with dorsal plate fixation is rupture of the extensor pollicis longus and/or the extensor digitorum communis tendon. Complications: When Things Do Not Go Well There are a variety of complications that can occur after DRF. These are outlined in Table McKay and colleagues 27 developed a complications checklist that the practitioner uses to score complications as mild (symptoms only with no specific treatment), moderate (requiring diagnostic procedure and/or therapeutic intervention), and severe (requiring surgery). The highest number of complications reported in one series included median nerve compression, CRPS, tendonitis, extensor pollicis longus rupture occurring with or without dorsal plating, dorsoradial sensory neuritis, DRUJ problems, tendon adhesions, and ulnar nerve compression. Other complications to be aware of include flexor pollicis longus tendon rupture, 46 carpal instability or subluxation, trigger finger, Dupuytren s contracture, compartment syndrome, delayed union, and pin-site infection. In the small numbers of patients in whom CRPS develops, therapy in conjunction with pharmacologic management of pain may be prolonged. The care of the patient with CPRS is discussed in Chapters 115 and 116. A common problem experienced is ulnar-sided wrist pain, which can affect strength and functional outcome. Most often this is due to tendinitis of the extensor carpi ulnaris tendon, DRUJ instability, or triangular fibrocartilage complex involvement. This pain most frequently occurs during gripping or rotational strengthening activities. Forearm pronation during gripping and loading activities increases ulnar-sided load
15 962 PART 12 COMMON WRIST INJURIES and, if painful, should be modified and performed with the forearm in neutral rotation. Most ulnar-sided wrist pain will resolve itself within 1 year, but this problem can be debilitating to the patient s progress, and the etiology should be determined. Because pain is the most debilitating obstacle with DRF, ulnar-sided wrist pain needs to be assessed and treated appropriately. Some ulnar-sided pain can be attributed to the change in load bearing across the wrist if there is malunion or significant shortening of the radius. If there is malalignment of fracture fragments, including a dorsal tilt of the radius, DRUJ subluxation or instability, or significant radial shortening that results in disabling pain, then the patient may be a candidate for a surgical procedure. This malalignment is treated with corrective osteotomy of the radius 47,48 and/or ulnar shortening osteotomy to alleviate ulnar impaction. 49 Therapy is often required after these procedures (see Chapter 76). Do Patients Get Better With Hand Therapy After DRF? Therapists recognize the value of the care and guidance that is provided to a patient through supervised therapy after a wrist fracture. Some patients with uncomplicated fractures may figure it out on their own, but, according to the expert clinical opinion and experience of hand therapists, patients with the typical sequelae of stiffness, edema, pain, and disrupted function do better with a guided and supervised program of therapy to improve the outcome. The challenge is to show which techniques are most effective through controlled clinical studies. As Handoll and colleagues 50 wrote in their 2006 Cochrane Database Systematic Review, there was not enough evidence available to determine the best form of rehabilitation after DRF. It is important to note that Handoll reviewed cases where just cast immobilization had been used, and many of these patients do not require ongoing supervised therapy, rather, a well-structured home exercise plan. Exploring Further Information on DRFs Technologies in surgery and therapy for treating DRFs are evolving. For clinicians to remain knowledgeable, it is important to use resources from current peer-reviewed journals and keep up with the evidence. Sites such as PubMed ( can be used to do searches on a periodic basis. Medical Subject Headings are searched using terminology related to DRF management. PubMed provides a tutorial for those unfamiliar with this resource. There are also ratings, reviews, and articles on websites such as Physiotherapy Evidence Database (PEDro) ( and McMaster University s Rehab + ( Openaccess journals such as BMC Musculoskeletal Disorders ( can also be accessed for information. The importance of using current and past evidence, expert clinical opinion, and patient values to make care decisions is addressed by MacDermid in Chapter 143 ( Evidence-Based Practice ), the final chapter of this textbook. Concluding Statements Treatment of DRFs with better predictability, fewer complications, and improved functional outcomes continues to challenge surgeons and therapists alike. There have been numerous attempts to describe and classify them and form treatment algorithms. Enhanced understanding of the anatomy and biomechanics of the wrist in the past two decades has aided the evolution of treatment for these fractures. The once well-established belief that deformity from this fracture can be tolerated because there are no long-term functional consequences is changing. Restoration of the anatomy can be critical to the final radiographic and functional outcome in many patients, particularly those with high physical demands on the involved extremity. Surgeons continue to develop and refine fixation techniques to restore the distal radius anatomy with better predictability and fewer complications. Therapists must be knowledgeable about the anatomy of the distal radius and the ramifications of any residual deformities and the expected time for healing after fracture. The functional effect of the accompanying soft-tissue injuries must also be factored into treatment planning because it may be just as significant as the fracture. It is the combination of soft-tissue injury, edema, and ischemia of the intrinsic muscles that leads to finger stiffness and hand dysfunction, which can remain long after the fracture has healed. Maximum improvement from most DRFs does not occur for many months. Patients usually do not continue with therapy until maximum improvement is reached. Therefore, therapists must be good educators and patients with DRF must effectively perform their home programs and accept responsibility for their rehabilitation. REFERENCES The complete reference list is available online at com.
16 CHAPTER 70 THERAPIST S MANAGEMENT OF DISTAL RADIUS FRACTURES 962.e1 REFERENCES 1. O Connor D, Mullett H, Doyle M, et al. Minimally displaced Colles fractures: a prospective randomized trial of treatment with a wrist splint or a plaster cast. J Hand Surg. 2003;28B(1): Guofen C, Doi K, Hattori Y, Kitajima I. Arthroscopically assisted reduction and immobilization of intraarticular fracture of the distal end of the radius: several options of reduction and immobilization. Tech Hand Up Extrem Surg. 2005;9(2): Ellis A, Weiland AJ. Indirect reduction and percutaneous fixation led to a rapid recovery and better function than open reduction for intra-articular fractures of the distal end of the radius. J Bone Joint Surg Am. 2006;88: Chung KC, Watt AJ, Kotsis SV, et al. Treatment of unstable distal radial fractures with the volar locking plating system. J Bone Joint Surg Am. 2006;88: Simic PM, Robison J, Gardner MJ, et al. Treatment of distal radius fractures with a low-profile dorsal plating system: an outcomes assessment. J Hand Surg. 2006;31A: Souer JS, Lozano-Calderón SA, Ring D. Predictors of wrist function and health status after operative treatment of fractures of the distal radius. J Hand Surg. 2008;33A(2): MacDermid JC. Development of a scale for patient rating of wrist pain and disability. J Hand Ther. 1996;9: MacDermid JC, Tottingham V. Responsiveness of the DASH and PRWE in wrist of hand injured patients referred for rehabilitation. J Hand Ther. 2004;17: Kotsis SV, Lau FH, Chung KC. Responsiveness of the Michigan Hand Outcomes Questionnaire and physical measurements in outcome studies of distal radius fracture treatment. J Hand Surg. 2007;32A(1): MacDermid J, Michlovitz S. Outcomes in evidence-based practice. In: Law M, MacDermid J, eds. Evidence-Based Rehabilitation: A Guide to Practice. 2nd ed. Thorofare, NJ: Slack; MacDermid JC, Roth JH, Richards RS. Pain and disability reported in the year following a distal radius fracture: a cohort study. BMC Musculoskelet Disord Oct 31;4: Abramo A, Kopylov P, Tagil M. Evaluation of a treatment protocol in distal radius fractures: a prospective study in 581 patients using DASH as outcome. Acta Orthop. 2008;79(3): MacDermid JC, Richards RS, Donner A, et al. Responsiveness of the Short Form-36, Disability of the Arm, Shoulder, and Hand Questionnaire, Patient-Rated Wrist Evaluation, and physical impairment measurements in evaluating recovery after a distal radius fracture. J Hand Surg. 2000;25A(2): Lucado A, Li Z, Russel GB, et al. Changes in impairment and function after static progressive splinting for stiffness after distal radius fracture. J Hand Ther. 2008;21: Bland MD, Beebe JA, Hardwick DD, Lang CE. Restricted active range of motion at the elbow, forearm, wrist or fingers decreases hand function. J Hand Ther. 2008;21: Michlovitz SL, Ashton B, Butler M, et al. The push off test: assessing wrist function after fracture. Poster at American Physical Therapy Association Combined Sections Meeting, San Antonio, Texas, Feb MacDermid JC, Michlovitz S, Rafuse R, et al. Does a push-off test or other physical impairments explain disability in daily activities and work in patients with wrist and elbow pathology? Canadian Orthopaedic Conference, Montreal, Quebec, Canada, June 3-5, Karnezis IA, Panagiotopoulos E, Tyllianakis M, et al. Correlation between radiological parameters and patient-rated wrist dysfunction following fractures of the distal radius. Injury. 2005;36(12): Ishikawa J, Iwasaki N, Minami A. Influence of distal radioulnar joint subluxation on restricted forearm rotation after distal radius fracture. J Hand Surg. 2005;30A(6): Grewal R, MacDermid JC. The risk of adverse outcomes in extraarticular distal radius fractures is increased with malalignment in patients of all ages but mitigated in older patients. J Hand Surg. 2007;32A: Jaremko JL, Lambert RG, Rowe BH, et al. Do radiographic indices of distal radius fracture reduction predict outcomes in older adults receiving conservative treatment? Clin Radiol. 2007; 62(1): Handoll HH, Madhok R. Conservative interventions for treating distal radial fractures in adults. Cochrane Database Syst Rev. 2003;2:CD Chung KC, Kotsis SV, Kim HM. Predictors of functional outcomes after surgical treatment of distal radius fractures. J Hand Surg. 2007;32A(1): MacDermid JC, Roth JH, McMurtry R. Predictors of time lost from work following a distal radius fracture. J Occup Rehabil. 2007;17: MacDermid JC, Richard RS, Roth JH. Distal radius fracture: a prospective outcome study of 275 patients. J Hand Ther. 2001; 14: MacDermid JC. Hand therapy management of intra-articular fractures with open reduction and Pi plate fixation: a therapist s perspective. Tech Hand Up Extrem Surg. 2004;8: McKay SD, MacDermid JC, Roth JH, Richards RS. Assessment of complications of distal radius fractures and development of a complication checklist. J Hand Surg. 2001;26A: Ryu JY, Cooney WP 3rd, Askew LJ, et al. Functional ranges of motion of the wrist joint. J Hand Surg. 1991;16A: Johnston TE. Muscle weakness and loss of motor performance. In: Michlovitz SL, Nolan TP. Modalities for Therapeutic Intervention. 4th ed. Philadelphia: FA Davis; 2005: Michlovitz SL, Harris BA, Watkins MP: Interventions for loss of range of motion of the upper extremity: a systematic review. J Hand Ther. 2004;17(2): Usuba M, Miyanaga Y, Miyakawa S, et al. Effect of heat in increasing the range of knee motion after development of a joint contracture. Arch Phys Med Rehabil. 2006;87: Youdas JW, Krause DA, Egan KS, et al. The effect of static stretching of the calf muscle-tendon unit on active ankle dorsiflexion range of motion. J Orthop Sports Phys Ther. 2003;33: Hertling D, Kessler RM. Wrist and hand complex. In: Hertling D, Kessler RM. Management of Common Musculoskeletal Disorders: Physical Therapy Principles and Methods. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2006: Kisner C, Colby LA. Therapeutic Exercise: Foundations and Techniques. 5th ed. Philadelphia: FA Davis; 2007: Vicenzino B, Branjerdporn M, Teys P, Jordan K. Initial changes in posterior talar glide and dorsiflexion of the ankle after mobilization with movement in individuals with recurrent ankle sprain. J Orthop Sports Phys Ther. 2006;36(7): Cyr LM, Ross RG. How controlled stress affects healing tissues. J Hand Ther. 1998;11(2): McGrath MS, Ulrich SD, Bonutti PM, et al. Evaluation of static progressive stretch for the treatment of wrist stiffness. J Hand Surg. 2008;33A: McGrath MS, Ulrich SD, Bonutti PM, et al. Static progressive splinting for restoration of rotational motion of the forearm. J Hand Ther. 2009;22: Slutsky DJ, Herman M. Rehabilitation of distal radius fractures: a biomechanical guide. Hand Clin. 2005;21(3): Lyngcoln A, Taylor N, Pizzari T, Baskus K. The relationship between adherence to hand therapy and short-term outcome after distal radius fracture. J Hand Ther. 2005;18: Capo JT, Swan KG Jr, Tan V. External fixation techniques for distal radius fractures. Clin Orthop Relat Res Apr;445: Egol KA, Paksima N, Puopolo S, et al. Treatment of external fixation pins about the wrist: a prospective, randomized trial. J Bone Joint Surg. 2006;88A:
17 962.e2 PART 12 COMMON WRIST INJURIES 43. Lozano-Calderón SA, Souer S, Mudgal C, et al. Wrist mobilization following volar plate fixation of fractures of the distal part of the radius. J Bone Joint Surg. 2008;90A(6): Kamath AF, Zurakowski D, Day CS. Low-profile dorsal plating for dorsally angulated distal radius fractures: an outcomes study. J Hand Surg. 2006;31A(7): Keller M, Steiger R. The [pi] plate: an implant for unstable extension fractures of the distal radius in patients with osteoporotic bone. Tech Hand Up Extrem Surg. 2004;8(4): Sánchez T, Jakubietz M, Jakubietz R, et al. Complications after Pi Plate osteosynthesis. Plast Reconstr Surg. 2006;118(1): Prommersberger KJ, Ring DR, González del Pino J, et al. Corrective osteotomy for intra-articular malunion of the distal part of the radius: surgical technique. J Bone Joint Surg. 2006;88A: Viegas SF. A new modification of corrective osteotomy for treatment of distal radius malunion. Tech Hand Up Extrem Surg. 2006;10(4): Petersen K, Breddam M, Jorgsholm P, Schroder H. Ulnar shortening osteotomy after Colles fracture. Scand J Plast Reconstr Surg Hand Surg. 2005;39(3): Handoll HHG, Madhok R, Howe TE. Rehabilitation for distal radial fractures in adults. Cochrane Database Syst Rev. 2006;3: CD DOI: / CD pub2.
Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma. Magee, 2008. pg.
 PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
LSU Health Sciences Center Occupational Therapy Flexor Tendon Injury Treatment Protocol
 . LSU Health Sciences Center Occupational Therapy Flexor Tendon Injury Treatment Protocol DIP PIP MCP Zone 1 Zone 2 T 1 T 2 Zone 3 T 3 Zone 4 Zone 5 Zone 5 cs Carla M. Saulsbery LOTR, CHT Dr. A. Hollister,
. LSU Health Sciences Center Occupational Therapy Flexor Tendon Injury Treatment Protocol DIP PIP MCP Zone 1 Zone 2 T 1 T 2 Zone 3 T 3 Zone 4 Zone 5 Zone 5 cs Carla M. Saulsbery LOTR, CHT Dr. A. Hollister,
THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014
 THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014 ELBOW FUNCTION 1. Required to provide stability for power and precision tasks for both open and closed kinetic chain
THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014 ELBOW FUNCTION 1. Required to provide stability for power and precision tasks for both open and closed kinetic chain
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
Radial Head Fracture Repair and Rehabilitation
 1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Distal Radius Fractures. Lee W Hash, MD Affinity Orthopedics and Sports Medicine
 Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Hand Injuries and Disorders
 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327
 K-W URGENT CARE CLINICS INC. Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327 OPEN Mon-Fri 8am-5pm, Sa
K-W URGENT CARE CLINICS INC. Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327 OPEN Mon-Fri 8am-5pm, Sa
Fractures around wrist
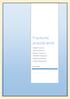 Fractures around wrist Colles Fracture Smiths fracture Barton s fracture Chauffer s fracture Scaphoid fracture Lunate dislocation Vivek Pandey Colles fracture Definition: Fracture of the distal end radius
Fractures around wrist Colles Fracture Smiths fracture Barton s fracture Chauffer s fracture Scaphoid fracture Lunate dislocation Vivek Pandey Colles fracture Definition: Fracture of the distal end radius
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Chapter 7 The Wrist and Hand Joints
 Chapter 7 The Wrist and Hand Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Many Archery, Relate wrist require sports require precise functioning of flexion, & hand & hand functional combined
Chapter 7 The Wrist and Hand Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Many Archery, Relate wrist require sports require precise functioning of flexion, & hand & hand functional combined
.org. Distal Radius Fracture (Broken Wrist) Description. Cause
 Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463
 Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Chapter 30. Rotational deformity Buddy taping Reduction of metacarpal fracture
 Chapter 30 FINGER FRACTURES AND DISLOCATIONS KEY FIGURES: Rotational deformity Buddy taping Reduction of metacarpal fracture Because we use our hands for so many things, finger fractures and dislocations
Chapter 30 FINGER FRACTURES AND DISLOCATIONS KEY FIGURES: Rotational deformity Buddy taping Reduction of metacarpal fracture Because we use our hands for so many things, finger fractures and dislocations
WRIST EXAMINATION. Look. Feel. Move. Special Tests
 WRIST EXAMINATION Look o Dorsum, side, palmar- palmar flex wrist to exacerbate dorsal swellings o Deformity e.g. radial deviation after colles, prominent ulna o Swellings e.g. ganglion o Scars, muscle
WRIST EXAMINATION Look o Dorsum, side, palmar- palmar flex wrist to exacerbate dorsal swellings o Deformity e.g. radial deviation after colles, prominent ulna o Swellings e.g. ganglion o Scars, muscle
NOW PLAYING THE WRIST. David Costa, OTR/L October 20, 2007
 NOW PLAYING THE WRIST David Costa, OTR/L October 20, 2007 Starring Radius Ulna Scaphoid Lunate Triquetrum Trapezium Trapezoid Capitate Hamate Pisiform TFCC Transverse Carpal Ligament Scapholunate Ligament
NOW PLAYING THE WRIST David Costa, OTR/L October 20, 2007 Starring Radius Ulna Scaphoid Lunate Triquetrum Trapezium Trapezoid Capitate Hamate Pisiform TFCC Transverse Carpal Ligament Scapholunate Ligament
Pediatric Sports Injuries of the Wrist and Hand. Sunni Alford, OTR/L,CHT Preferred Physical Therapy
 Pediatric Sports Injuries of the Wrist and Hand Sunni Alford, OTR/L,CHT Preferred Physical Therapy Wrist injuries TFCC ECU/ FCU tendonitis Instability Growth Plate Fractures Ulnar abutment syndrome Triangular
Pediatric Sports Injuries of the Wrist and Hand Sunni Alford, OTR/L,CHT Preferred Physical Therapy Wrist injuries TFCC ECU/ FCU tendonitis Instability Growth Plate Fractures Ulnar abutment syndrome Triangular
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Examination of the Elbow. Elbow Examination. Structures to Examine. Active Range of Motion. Active Range of Motion 8/22/2012
 Examination of the Elbow The elbow is a complex modified hinge joint The humero-ulnar joint is a hinge joint allowing flexion and extension The radio-ulnar joint allows for pronation and supination of
Examination of the Elbow The elbow is a complex modified hinge joint The humero-ulnar joint is a hinge joint allowing flexion and extension The radio-ulnar joint allows for pronation and supination of
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ESSENTIALPRINCIPLES. Wrist Pain. Radial and Ulnar Collateral Ligament Injuries. By Ben Benjamin
 ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
Elbow, Forearm, Wrist, & Hand. Bony Anatomy. Objectives. Bones. Bones. Bones
 Objectives Elbow, Forearm, Wrist, & Hand Chapter 19 Identify and discuss the functional anatomy of the elbow and forearm Discuss the common injuries associated with these anatomical structures Bones Humerus
Objectives Elbow, Forearm, Wrist, & Hand Chapter 19 Identify and discuss the functional anatomy of the elbow and forearm Discuss the common injuries associated with these anatomical structures Bones Humerus
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
NERVE COMPRESSION DISORDERS
 Common Disorders of the Hand and Wrist Ryan Klinefelter, MD Associate Professor of Orthopaedics Department of Orthopaedics The Ohio State University Medical Center NERVE COMPRESSION DISORDERS 1 Carpal
Common Disorders of the Hand and Wrist Ryan Klinefelter, MD Associate Professor of Orthopaedics Department of Orthopaedics The Ohio State University Medical Center NERVE COMPRESSION DISORDERS 1 Carpal
Hand and Wrist Injuries and Conditions
 Hand and Wrist Injuries and Conditions Julia Wild Hand Therapist www.southernhandtherapy.com.au 02 9553 8597 POSI Position of Safe Immobilisation So everything is balanced Wrist 30⁰ ext MCP 70⁰ flex for
Hand and Wrist Injuries and Conditions Julia Wild Hand Therapist www.southernhandtherapy.com.au 02 9553 8597 POSI Position of Safe Immobilisation So everything is balanced Wrist 30⁰ ext MCP 70⁰ flex for
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com
 North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a
A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a
International Standards for the Classification of Spinal Cord Injury Motor Exam Guide
 C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
.org. Tennis Elbow (Lateral Epicondylitis) Anatomy. Cause
 Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Total Elbow Arthroplasty and Rehabilitation
 Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Integra. MCP Joint Replacement PATIENT INFORMATION
 Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
.org. Clavicle Fracture (Broken Collarbone) Anatomy. Description. Cause. Symptoms
 Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Arthroscopy of the Hand and Wrist
 Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA
 Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
ASOP Exams PO Box 7440 Seminole, FL 33775. The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title. Address. City State Zip.
 The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title Address City State Zip Tel# Email Certification Organization Cert# Mail a copy of your completed exam to: ASOP Exams PO Box 7440
The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title Address City State Zip Tel# Email Certification Organization Cert# Mail a copy of your completed exam to: ASOP Exams PO Box 7440
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
2. Repair of the deltoid - the amount deltoid was released and security of repair
 Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
Ergonomics Monitor Training Manual
 Table of contents I. Introduction Ergonomics Monitor Training Manual II. Definition of Common Injuries Common Hand & Wrist Injuries Common Neck & Back Injuries Common Shoulder & Elbow Injuries III. Ergonomics
Table of contents I. Introduction Ergonomics Monitor Training Manual II. Definition of Common Injuries Common Hand & Wrist Injuries Common Neck & Back Injuries Common Shoulder & Elbow Injuries III. Ergonomics
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Median Nerve Injuries in, Fractures in the Region of the Wrist
 252 Median Nerve Injuries in, Fractures in the Region of the Wrist N. MEADOFF, M.D., Bakersfield SUMMARY Injuries of the median nerve in fractures in the region of the wrist are not uncommon. Median nerve
252 Median Nerve Injuries in, Fractures in the Region of the Wrist N. MEADOFF, M.D., Bakersfield SUMMARY Injuries of the median nerve in fractures in the region of the wrist are not uncommon. Median nerve
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
Common wrist injuries in sport. Chris Milne Sports Physician Hamilton,NZ
 Common wrist injuries in sport Chris Milne Sports Physician Hamilton,NZ Overview / Classification Acute injuries Simple - wrist sprain Not so simple 1 - Fracture of distal radius/ulna 2 - Scaphoid fracture
Common wrist injuries in sport Chris Milne Sports Physician Hamilton,NZ Overview / Classification Acute injuries Simple - wrist sprain Not so simple 1 - Fracture of distal radius/ulna 2 - Scaphoid fracture
Lean-Ergonomic methods to reduce workers compensation costs (Part 2 of 2) Cumulative trauma disorders can be classified as: What is CTD?
 #425 Lean-ergonomic methods to reduce workers compensation costs, Part 2 of 2 Lean-Ergonomic methods to reduce workers compensation costs (Part 2 of 2) Govid Bharwani, Ph.D, Biomedical Engineering Thursday,
#425 Lean-ergonomic methods to reduce workers compensation costs, Part 2 of 2 Lean-Ergonomic methods to reduce workers compensation costs (Part 2 of 2) Govid Bharwani, Ph.D, Biomedical Engineering Thursday,
Wrist Fractures. Wrist Defined: Carpal Bones Distal Radius Distal Ulna
 Wrist Fractures Wrist Fractures Wrist Defined: Carpal Bones Distal Radius Distal Ulna Wrist Fractures Wrist Joints: CMC Intercarpal Radiocarpal DRUJ drudge Wrist Fractures Wrist Fractures: (that we are
Wrist Fractures Wrist Fractures Wrist Defined: Carpal Bones Distal Radius Distal Ulna Wrist Fractures Wrist Joints: CMC Intercarpal Radiocarpal DRUJ drudge Wrist Fractures Wrist Fractures: (that we are
Elbow Examination. Haroon Majeed
 Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
UPPER EXTREMITY INJURIES IN SPORTS
 UPPER EXTREMITY INJURIES IN SPORTS Wrist and Hand Injuries in the Athlete Tim L. Uhl, PhD, ATC, PT Philip Blazar, MD Greg Pitts, MS, OTR/L, CHT Kelly Ramsdell, ATC CHAPTER 2 Sports Physical Therapy Section
UPPER EXTREMITY INJURIES IN SPORTS Wrist and Hand Injuries in the Athlete Tim L. Uhl, PhD, ATC, PT Philip Blazar, MD Greg Pitts, MS, OTR/L, CHT Kelly Ramsdell, ATC CHAPTER 2 Sports Physical Therapy Section
Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath
 Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath Difficult Balance Many hand conditions can be managed non-operatively / simply Missed injury or delayed diagnosis not uncommon Common Problems
Common Hand and Wrist Conditions: When to Refer? Dr Tim Heath Difficult Balance Many hand conditions can be managed non-operatively / simply Missed injury or delayed diagnosis not uncommon Common Problems
CONSTRUCTION WORK and CUMULATIVE TRAUMA DISORDERS
 Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES
 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
TENDON INJURIES OF THE HAND KEY FIGURES:
 Chapter 32 TENDON INJURIES OF THE HAND KEY FIGURES: Extensor surface of hand Mallet finger Mallet splints Injured finger in stack splint Repair of open mallet Most hand specialists believe that the earlier
Chapter 32 TENDON INJURIES OF THE HAND KEY FIGURES: Extensor surface of hand Mallet finger Mallet splints Injured finger in stack splint Repair of open mallet Most hand specialists believe that the earlier
Systemic condition affecting synovial tissue Hypertrohied synovium destroys. Synovectomy. Tenosynovectomy Tendon Surgery Arthroplasty Arthrodesis
 Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons
 Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Active Range of Motion: A. Flexion: Gently try to bend your wrist forward. Hold for 5 seconds. Repeat for 3 sets of 10.
 Rehabilitation Exercises for Wrist and Hand Injuries If instructed by your medical doctor, you may begin these exercises when the pain has started to decrease. Active Range of Motion: A. Flexion: Gently
Rehabilitation Exercises for Wrist and Hand Injuries If instructed by your medical doctor, you may begin these exercises when the pain has started to decrease. Active Range of Motion: A. Flexion: Gently
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Injuries to Upper Limb
 Injuries to Upper Limb 1 The following is a list of common sporting conditions and injuries. The severity of each condition may lead to different treatment protocols and certainly varying levels of intervention.
Injuries to Upper Limb 1 The following is a list of common sporting conditions and injuries. The severity of each condition may lead to different treatment protocols and certainly varying levels of intervention.
Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
 LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Below is a diagram showing the main bones together with written text on their order of compilation.
 Below is a diagram showing the main bones together with written text on their order of compilation. The hand and wrist contain twenty-seven bones and tendons, eight carpals, five metacarpals and fourteen
Below is a diagram showing the main bones together with written text on their order of compilation. The hand and wrist contain twenty-seven bones and tendons, eight carpals, five metacarpals and fourteen
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients This leaflet has been developed to answer any questions you may have regarding
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients This leaflet has been developed to answer any questions you may have regarding
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
Get Rid of Elbow Pain
 Get Rid of Elbow Pain Self Regional Healthcare Optimum Life Center 115 Academy Avenue Greenwood, SC 29646 Office: (864) 725-7088 Self Regional Healthcare Physical Therapy Savannah Lakes 207 Holiday Road
Get Rid of Elbow Pain Self Regional Healthcare Optimum Life Center 115 Academy Avenue Greenwood, SC 29646 Office: (864) 725-7088 Self Regional Healthcare Physical Therapy Savannah Lakes 207 Holiday Road
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
The Elbow, Forearm, Wrist, and Hand
 Elbow - Bones The Elbow, Forearm, Wrist, and Hand Chapters 23 & 24 Humerus Distal end forms the medial & lateral condyles Lateral: capitulum Medial: trochlea Radius Ulna Sports Medicine II Elbow - Bones
Elbow - Bones The Elbow, Forearm, Wrist, and Hand Chapters 23 & 24 Humerus Distal end forms the medial & lateral condyles Lateral: capitulum Medial: trochlea Radius Ulna Sports Medicine II Elbow - Bones
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF)
 ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
RADIOGRAPHIC EVALUATION
 Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
The wrist and hand are constructed of a series of complex, delicately balanced joints whose function is essential to almost every act of daily living.
 TOPIC OUTLINE 9- THE WRIST AND HAND. Introduction. The wrist and hand are constructed of a series of complex, delicately balanced joints whose function is essential to almost every act of daily living.
TOPIC OUTLINE 9- THE WRIST AND HAND. Introduction. The wrist and hand are constructed of a series of complex, delicately balanced joints whose function is essential to almost every act of daily living.
Fact Sheet: Occupational Overuse Syndrome (OOS)
 Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
Treatment Guide Understanding Elbow Pain. Using this Guide. Choosing Your Care. Table of Contents:
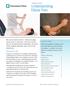 Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior
 Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
The Rehabilitation Team
 Considerations in Designing a Rehab Program Philosophy of Sports Medicine Healing Process Pathomechanics of Injury Psychological Aspects Goals of Rehab Chapter 1 Group effort The Rehabilitation Team AEP/Athletic
Considerations in Designing a Rehab Program Philosophy of Sports Medicine Healing Process Pathomechanics of Injury Psychological Aspects Goals of Rehab Chapter 1 Group effort The Rehabilitation Team AEP/Athletic
VIRGINIA SPORTSMEDICINE INSTITUTE 1715 N. GEORGE MASON DR. SUITE 503 ARLINGTON, VA 22205 703-525-5542 WWW.VASPORTSMEDICINE.
 VIRGINIA SPORTSMEDICINE INSTITUTE 1715 N. GEORGE MASON DR. SUITE 503 ARLINGTON, VA 22205 703-525-5542 WWW.VASPORTSMEDICINE.COM ELBOW PAIN Elbow tendonitis/tendinosis is an overuse injury resulting from
VIRGINIA SPORTSMEDICINE INSTITUTE 1715 N. GEORGE MASON DR. SUITE 503 ARLINGTON, VA 22205 703-525-5542 WWW.VASPORTSMEDICINE.COM ELBOW PAIN Elbow tendonitis/tendinosis is an overuse injury resulting from
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
CUMMULATIVE DISORDERS OF UPPER EXTIMITY DR HABIBOLLAHI
 CUMMULATIVE DISORDERS OF UPPER EXTIMITY DR HABIBOLLAHI Definition Musculoskeletal disorder (MSD) is an injury or disorder of the muscles, nerves, tendons, joints, cartilage,ligament and spinal discs. It
CUMMULATIVE DISORDERS OF UPPER EXTIMITY DR HABIBOLLAHI Definition Musculoskeletal disorder (MSD) is an injury or disorder of the muscles, nerves, tendons, joints, cartilage,ligament and spinal discs. It
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Repetitive Strain Injury (RSI)
 Carpal Tunnel Syndrome and Other Musculoskeletal Problems in the Workplace: What s the Solution? by Richard N. Hinrichs, Ph.D. Dept. of Kinesiology Arizona State University Repetitive Strain Injury (RSI)
Carpal Tunnel Syndrome and Other Musculoskeletal Problems in the Workplace: What s the Solution? by Richard N. Hinrichs, Ph.D. Dept. of Kinesiology Arizona State University Repetitive Strain Injury (RSI)
Shoulder Replacement Surgery
 In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
by joe muscolino body mechanics
 by joe muscolino body mechanics carpal tunnel syndrome The word carpal means wrist. Therefore, the carpal tunnel is a tunnel that is formed by the structural configuration of the wrist (carpal) bones.
by joe muscolino body mechanics carpal tunnel syndrome The word carpal means wrist. Therefore, the carpal tunnel is a tunnel that is formed by the structural configuration of the wrist (carpal) bones.
THORACIC OUTLET SYNDROME
 THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called

 Full version is >>> HERE
Full version is >>> HERE